NONLINEAR DYNAMICS OF HEART RHYTHMS
|
|
|
- Cora Byrd
- 6 years ago
- Views:
Transcription
1 Proceedings of COBEM 007 Copyright 007 by ABCM 9th International Congress of Mechanical Engineering November -9, 007, Brasília, DF NONLINEAR DYNAMICS OF HEART RHYTHMS Sandra R.F.S.M. Gois, Marcelo A. Savi, Universidade Federal do Rio de Janeiro COPPE Department of Mechanical Engineering.9.97 Rio de Janeiro RJ Brazil, P.O. Box 8.0 Abstract. Rhythmic phenomena represent one of the most striking manifestations of dynamic behavior in biological systems. Understanding the mechanisms responsible for biological rhythms is crucial for the comprehension of the dynamics of life. Natural rhythms could be either periodic or irregular over time and space. Each kind of dynamical behavior related to biomedical systems may be related with both normal and pathological physiological functioning. The cardiac conducting system can be treated as a network of self-excitatory elements. Since these elements exhibit oscillatory behavior, they can be modeled as nonlinear oscillators. This article proposes a mathematical model to describe heart rhythms. Three modified Van der Pol oscillators are connected considering time delay coupling in order to reproduce electrocardiogram (ECG) signals. Numerical simulations are carried out reproducing normal and pathological rhythms represented by ECG signals. Keywords: Chaos, heart, natural rhythms, nonlinear dynamics.. INTRODUCTION Natural rhythms could be either periodic or irregular over time and space. Each kind of dynamical behavior related to biomedical systems may be related to both normal and pathological physiological functioning. Extremely regular dynamics may be associated with diseases including periodic breathing, certain abnormally heart rhythms, cyclical blood diseases, epilepsy, neurological tics and tremors. On the other hand, there are phenomena where regular dynamics reflect healthy behavior as sleep-wake cycle and menstrual rhythms. Moreover, irregular rhythms can also reflect disease: cardiac arrhythmias, such as fibrillation, and different neurological disorders (Savi, 00, 00; Glass, 00; Ferriere & Fox, 99). Rhythmic changes of blood pressure, heart rate and other cardiovascular measures indicate the importance of dynamical aspects in the comprehension of cardiovascular rhythms. Several studies are pointing to the fact that certain cardiac arrhythmias are instances of chaos (Witkowski et al., 99; Radhakrishna et al., 000). This is important because it may suggest different therapeutic strategies, changing classical approaches. Among cardiac arrhythmia, one can cite premature beats, atrial fibrillation, bradycardia, tachycardia and ventricular arrhythmias, as fibrillations and tachycardia, which are the most severe and life-threatening arrhythmias being the cause of many deaths. There are different forms to evaluate the heart functioning by the measurement of some signal. An electrocardiogram (ECG) records the electrical activity of the heart being used to measure the rate and regularity of heartbeats as well as the size and position of the chambers. The electrical impulses related to heart functioning are recorded in the form of waves, which represents the electrical current in different areas of heart. The clinical arrhythmias that have the greatest potential for therapeutic applications of chaos theory are the aperiodic tachyarrhythmias, including atrial and ventricular fibrillation. Garfinkel et al. (99) and Garfinkel et al. (99) discuss the application of chaos control techniques in order to avoid heart arrhythmic responses. This approach may be incorporated into pacemakers, avoiding ventricular fibrillation, for example. Since chaotic responses may be controlled by an efficient way using OGY method or its variants, this may inspire some interesting approaches in order to stabilize unstable orbits associated with the normal heart rhythm. This article proposes a mathematical model to describe heart rhythms. Since the qualitative features of the heart actuation potential is close related to the dynamical response of the classical Van der Pol (VdP) oscillator, this oscillator may be considered as the starting point of this modeling. Actually, the classical article due to Van der Pol & Van der Mark (9) describes the heart behavior from coupled VdP oscillators. Afterwards, Hodkin & Huxley (9) describes the heartbeat behavior by considering different models. Recently, Grudzinski & Zebrowski (00) proposes a variation of the classical Van der Pol oscillator in order to capture some important aspects regarding the heart action potential. Santos et al. (00) use coupled oscillators in order to describe general aspects of heartbeat rhythms discussing different coupling terms. Campbell & Wang (998) presents a discussion dealing with some coupling characteristics of these oscillators highlighting the importance to consider time delay coupling. Here, three modified VdP oscillators are connected considering time delay coupling in order to reproduce ECG signals. Normal and pathological rhythms are reproduced altering coupling terms.
2 . HEART AND ITS ELECTRICAL ACTIVITY The heart walls are composed of cardiac muscle, called myocardium, and also striations that is similar to skeletal muscle. Basically, the heart consists of four compartments: the right and left atria (upper part) and the right and left ventricles (lower part) (Figure ). The blood returns from the systemic circulation to the right atrium and from there goes to the right ventricle. It is ejected from the right ventricle to the lungs. Oxygenated blood returns from the lungs to the left atrium, and from there to the left ventricle. Finally blood is pumped through the aortic valve to the aorta and to the systemic circulation. The heart muscle cell (myocyte) has an electric activation that takes place by means of the inflow of sodium ions across the cell membrane. A plateau phase follows cardiac depolarization, and thereafter repolarization takes place, which is a consequence of the outflow of potassium ions. The mechanical contraction of the heart is associated with the electric activation of cardiac muscle cell. An important distinction between cardiac muscle tissue and skeletal muscle is that the activation of the cardiac muscle can propagate from one cell to another in any direction. Therefore, the activation wave-fronts are of rather complex shape. The only exception is the boundary between the atria and ventricles, where the activation wave usually cannot cross except along a special conduction system, since there is a nonconducting barrier of fibrous tissue. All heart rhythms are governed by activation potentials controlled by specialized cells. The sinus node (sinoatrial or node) is located in the right atrium at the superior vena cava (Figure ). The nodal cells are self-excitatory, pacemaker cells, which generate an action potential at the rate of about 70 pulses per minute. Activation propagates from the node throughout the atria, but cannot propagate directly across the boundary between atria and ventricles. The atrioventricular node ( node) is located at the boundary between the atria and ventricles (Figure ). It has an intrinsic frequency about 0 pulses/min, however, this node follows higher frequencies when it is triggered. In a normal heart, the node provides the only conducting path from atria to ventricles. Therefore, under normal conditions, ventricles can be excited only by pulses that propagate through it. Propagation from the node to the ventricles is provided by a specialized conduction system. Proximally, this system is composed of a common bundle, called the bundle of His. More distally, it separates into two bundle branches propagating along each side of the septum, constituting the right and left bundle branches. Even more distally the bundles ramify into Purkinje fibers that diverge to the inner sides of the ventricular walls. Because the intrinsic rate of the node is the highest, it sets the activation frequency of the whole heart. If the connection from the atria to the node fails, the node adopts its intrinsic frequency. If the conduction system fails at the bundle of His, the ventricles will beat at the rate determined by their own region that has the highest intrinsic frequency... Activation Potential Figure Schematic picture of the heart. The heart electric activity is closely related to cellular rhythms known as Na-K pump. The concentration of sodium ions (Na+) is about 0 times higher outside the cellular membrane than inside, whereas the concentration of the potassium (K+) ions is about 0 times higher inside as compared to outside. When the membrane is stimulated the transmembrane potential rises about 0mV and reaches the threshold that is, when the membrane voltage changes from 70 mv to about 0 mv the sodium and potassium ionic permeability of the membrane change. Figure presents a schematic picture of the ionic flow that generates the activation potential. The sodium ion permeability increases very rapidly at first, allowing sodium ions to flow from outside to inside, increasing the inside positive potential, reaching about +0 mv. After that, there is a slowly increasing of potassium ion permeability allowing potassium ions to flow from inside to outside, causing the return of the intracellular potential to its resting value. The
3 Proceedings of COBEM 007 Copyright 007 by ABCM 9th International Congress of Mechanical Engineering November -9, 007, Brasília, DF maximum excursion of the membrane voltage during activation is about 00mV; the duration of the impulse is around 00ms. While at rest, following activation, the Na-K pump restores the ion concentrations inside and outside the membrane to their original values. Figure The Na-K pump and the activation potential (Malmivuo & Plonsey, 99). Once activation has been initiated, the membrane is insensitive to new stimuli, no matter how large the magnitude. This phase is called the absolute refractory period. The activation process encompasses certain characteristics such as currents, potentials, conductivities, concentrations and ion flows. The term action impulse describes the whole process. The bioelectric measurements focus on the electric potential difference across the membrane. Therefore, the electric measurement of the action impulse is called the action potential that describes the behavior of the membrane potential during the activation. Different groups of cells present different configurations of ionic channels, which lead to different action impulse velocities. Therefore, cells are classified as slow or fast response action potential cells, which present different shapes for the action potential signal, represented in Figure. The first group (slow response) includes the atrial and ventricular muscle, His bundle and Purkinje fibers while the second (fast response) are the and nodes. Figure Wave shape action potential response: slow response (left side) and fast response (right side). The cellular rhythms produces electric activity that is related to depolarization and repolarization waves. The sodium influx is triggered by the very large and rapid rise in sodium permeability. This current is confined to a zone called the depolarization zone. The current outflow is the local circuit current that initially depolarizes the resting tissue, and which is advancing in the direction of propagation. When a cell depolarizes, it produces an electric field which triggers the depolarization phenomenon in another cell close to it, which then depolarizes. Therefore, the depolarization may be understood as a propagating wave within cardiac tissue. The nature of the repolarization wave is different from that of the depolarization wave. Unlike depolarization, the repolarization is not a propagating phenomenon, however, by
4 examining the location of repolarizing cells at consecutive time instances, it is possible to approximate the repolarization with a proceeding wave phenomenon.. ELECTROCARDIOGRAM (ECG) Cardiac electric signals on an intracellular level may be recorded with a microelectrode, which is inserted inside a cardiac muscle cell. On the other hand, it is possible to record the electric potential generated by the heart electrical activity on the surface of the thorax. The electrocardiogram (ECG) is a measure of the extra-cellular electric behavior of the cardiac muscle tissue. The propagation wave-front of the cardiac electrical signal through the body presents a very complicated shape due to different conductivity values of the tissues composing the human body and their complex spatial distribution. Besides, as the depolarization and repolarization phenomena propagate through heart conducting system, the electric field has a periodic response. Many cardiac signal measurement systems are already proposed, where leads are used to measure potential difference between points on the body surface. Actually, the measured signal is the projection of the dipole along the line defined by the leads. Therefore, depending on the leads configuration, different measurements are obtained but, in general, the signal contains the following waves: P-Wave: It is the first wave registered in the ECG, representing the atrium activation just after the sinus stimulation. It normally lasts between 0 and 90 ms in adults, has a round shape with maximal amplitude between 0. and 0.0mV. PR-Interval: measured from the start of the P-wave to the start of the QRS-Complex and lasts 90ms. QRS-Complex: It corresponds to the ventricular activation and is measured from the start of the first wave (no matter if it is Q or R-wave), to the last wave (R or S-wave). In normal adults, the complex lasts about 80 ms and presents a sharp shape, because of the high frequencies of the signal; however its shape varies a lot, depending on the lead system used. ST-Interval: It lasts from the end of the QRS-complex to the star of the T-wave and corresponds to part of the ventricular re-polarization process. T-Wave: It represents the ventricular activation, has a round shape with amplitude about 0.0mV. Some characteristics of the electric cardiac events and their related waves are summarized in the Table. From such characteristics it is possible to state the shape of each wave, and their combination result in the amplitude signal of the dipole, as shown in Figure. The ECG is the projection of such signal according to a variable angle (the dipole orientation). Table Electric Events in the Heart Location in the heart Event Time ECG Conduction [ms] Terminology velocity [m/s] node impulse generated Right atrium depolarization P Left atrium depolarization node arrival of impulse 0 P-Q node departure of impulse interval Bundle of His activated Bundle Branches activated.0-. Purkinje Fibers activated Septum depolarization 7 Endocardium 0. Left Ventricle depolarization 90 QRS Left Ventricle depolarization 0.8 Right Ventricle depolarization 0 Epicardium Left Ventricle repolarization 00 Right Ventricle repolarization 0. T Endocardium Left Ventricle repolarization 00
5 Proceedings of COBEM 007 Copyright 007 by ABCM 9th International Congress of Mechanical Engineering November -9, 007, Brasília, DF Figure Different waveforms for each of the specialized cells found in the heart (Malmivuo & Plonsey, 99).. MATHEMATICAL MODELLING The Van der Pol (VdP) equation was originally employed to describe relaxation oscillators in electronic circuits, and has been frequently used in theoretical models of the cardiac rhythm. This equation is very useful in the phenomenological modeling of natural systems, especially the heartbeat, since it displays many of those features supposed to occur in the biological setting as limit cycle, synchronization and chaotic behavior. The general form of this equation is presented below: ( bx ) x + cx = Γ() t + a & () & where a, b and c are system parameters and Γ(t) is an external forcing. The qualitative features of an isolated VdP oscillator present a close similarity to the features of the heart actuation potential. Both kinds of actuation potential response (slow and fast) can be easily reproduced by VdP oscillator. Grudzinski & Zebrowski (00) proposed a modified oscillator in order to simulate important physiological features of the action potentials. In general, the new equation has two fixed points and a damping term asymmetric with respect to the voltage: x( x ) & + a ) ) = Γ( t) () ed here a, d and e are system parameters and Γ(t) is an external forcing. As already mentioned, the normal cardiac rhythm is primarily generated by the node, which is considered the normal pacemaker. In addition, there is another pacemaker, the node. Each of these instances presents an actuation potential, which is fundamental to the heart dynamics, but not necessarily the most expressive to compose the ECG signal. Each activation (depolarization followed by repolarization) corresponds to a different region of the heart and therefore to a different tissue mass generating currents of different magnitudes. Therefore, the combination of activation waves coming from each region of the heart is responsible for the ECG form and is not exactly as sketched in Figure. Some of these signals may be preponderant in this composition, like the waves originated in the atrium and ventricle. On the other hand, as these regions follow very close the activation of the and nodes, their signature on the ECG signal is representative of the pacemakers signals, and it is possible to associate these signals atrium and ventricle, respectively. Therefore, it is expected that coupled oscillators, each one representing a different heart region signal, may represent the general heartbeat dynamics. Usually, two oscillators are considered representing the and nodes, however, it is observed that these two oscillators are not enough to reproduce the ECG signal. This is because the signal of the first oscillator corresponds to the activation of the node and atrium, and the signal of the second oscillator corresponds just to the ventricle depolarization. Under this assumption, it is possible to reproduce the P-curve but not the QRScomplex, because this interval mainly corresponds to the ventricle repolarization. This observation motivate the inclusion of a third oscillator that represent the pulse propagation through the ventricles, which physiologically represents the His-Purkinje complex, composed by the His bundle and the Purkinje fibers. Figure presents the conceptual model showing either the oscillators or the coupling among them. In order to
6 build a general model, bidirectional asymmetric couplings are assumed among all oscillators. Moreover, an external pacemaker is incorporated to the system, considering a periodic driving term on the oscillators, Γ(t). Node Node Complex Figure Conceptual model with three coupled oscillators. = x = x = x x x x ) ) ) ) x ) x ) x ) ) ) sin( ω t) sin( ω sin( ω t) t) x ) x ) x ) x ) x ) x ) () These governing equations may be rewritten in a compact form as follows: & y = f ( y, y& ) + Γ ( t) + Ky () y = Γ = T [ x x x ] y& = [ x x x ] [ ρ sin( ω t) ρ sin( ω t) ρ sin( ω t) ] T T () k K = k k Notice that the governing equations have a general form f ( y, y& ) (related to the modified VdP oscillator), Γ(t) is the forcing term and K represents the coupling matrix. Time delays in signal transmission are unavoidable and, since even small delays may alter the system dynamics, it is necessary to understand how conduction delays change the behavior of coupled oscillators. The inclusion of time delays in differential equations can cause drastic changes and can make chaos emerges in a system that would otherwise be described by a regular behavior (Campbell & Wang, 998). On this basis, the proposed mathematical model is changed in order to consider delay aspects in coupling terms. Therefore, governing equations are changed as follows: = x = x = x x w x x w w ) w ) ) w w ) x ) x ) x ) ) ) sin( ω t) sin( ω t) sin( ω t) x τ x x ) τ τ ) ) x τ x ) x τ τ ) ) (7) τ where xi = xi ( t τ ) and τ represents the time delay. Notice that, actually, there are different delays depending on the connection type. The classical fourth order Runge-Kutta method is adapted in order to deal with difference differential equation. Basically, it is assumed a function equivalent to the delayed system and, for time instants t < τ, the function y 0 provides values corresponding to time delays prior to the initial instant of observation (Boucekkine et al., 997):
7 Proceedings of COBEM 007 Copyright 007 by ABCM 9th International Congress of Mechanical Engineering November -9, 007, Brasília, DF y ( t) = y( t ) (8) 0 τ The determination of y 0 (t) may be done using Taylor s series, approximating the exact solution (Cunningham, 9): τ y ( t τ ) y( t) τ y& ( t) + & y ( t) (9) Under this assumption, it is possible to obtain approximated values for y(t-τ) in the time interval t < τ. After this, it is possible to use the integrated values in order to construct the time delayed function.. NUMERICAL SIMULATIONS This section considers numerical simulations performed with the proposed heart model. Parameter values suggested by Grudzinski & Zebrowski (00) are used as reference values for the normal ECG. The other parameters are adjusted in oder to qualitatively match the normal ECG. The following parameters are adopted to represent the normal heart functioning: a =, w = 0., w =. 9, d =, e = ; a =, w = 0., w = 0., d =, e = ; a =, w =, w =, d =, e = 7. Concerning coupling aspects, it is assumed that the normal heart has a unidirectional coupling from to nodes and also from to. Therefore, k - = and k - = 0 are nonvanishing terms and all others coupling vanishes. Moreover, it is necessary to establish proper coupling time delay parameters. If there is no coupling, the time delay does not matter, since it represents the elapsed time when the signal travels from a pacemaker node to another. Therefore, the following parameters are assumed: τ - = 0.8 and τ AS- = 0., vanishing all others. Under this condition, the ECG simulation is presented in Figure. As it is shown in its enlargement, the simulated ECG captures its general characteristics, presenting the important waves: P, QRS, T. Figure Normal ECG. The forthcoming analysis treats different coupling terms in order to simulate some heart pathologies identified from ECG. At first, it is considered the case where there is no communication between the and nodes, what is simulated by eliminating the coupling between the first and second oscillators (k - = 0). Under this condition, the system is driven by the node, presenting a higher frequency rhythm when compared with the normal ECG. This pathology is named ventricular flutter presenting a typical ECG form shown in Figure 7.
8 Figure 7 ECG without - coupling (ventricular flutter). The - coupling is now in focus, assuming k - = 0. Under this condition, the contribution of the oscillator vanishes and the ECG signal is related to the and activation, which means that ventricles do not perform their function. Figure 8 presents the ECG of this pathological functioning corresponding to the atrial activation. Figure 8 ECG without - coupling (sinus bradycardia). At this point, the normal ECG is considered again, however, an external pacemaker is exciting the heartbeat. Therefore, it is considered the same parameters related to Figure together with the following forcing parameters: ρ =, ρ =, ρ = 0, ω = ω = ω = π/(0/70). Under this condition, a ventricular fibrillation is induced. This pathological response is caused by different ventricle stimulation being characterized by irregular ECG with fast QRS response. mv ms Figure 9 ECG with external pacemaker excitation (ventricular fibrillation).. CONCLUSIONS A mathematical modeling of heart rhythms is developed considering three coupled modified Van der Pol oscillators. Each oscillator represents one of the main important heart activation potentials: sinoatrial node (), atrioventricular node () and His-Purkinje complex (). Numerical simulations of the proposed model shown that it is capable to capture the general heartbeat dynamics, representing the general ECG form with P, QRS and T curves. Afterwards, some pathological rhythms are of concern by establishing different coupling situations. Basically, it is assumed some communication interruption in the heart electric system. Under this condition, it is possible to simulate cardiopatologies as ventricular flutter. Moreover, external pacemaker excitation is of concern representing ventricular fibrillation. These results may encourage the identification of different pathological rhythms. 7. ACKNOWLEDGEMENTS The author acknowledges the support of Brazilian Research Council (CNPq).
9 Proceedings of COBEM 007 Copyright 007 by ABCM 9th International Congress of Mechanical Engineering November -9, 007, Brasília, DF 8. REFERENCES Boucekkine, R., Licandro, O. & Paul, C. (997), Differential-difference equations in economics: On the numerical solution of vintage capital growth models, Journal of Economic Dynamics and Control, v., pp. 7-. Campbell, S.R. & Wang, D. (998), Relaxation oscillators with time delay coupling, Physica D, v., pp.-78. Cunningham, W.J. (9), A Nonlinear Differential-Difference Equation of Growth Proceedings of the National Academy of Sciences of the United States of America, v.0, n.8, pp Dubin, D. (99), Interpretação Rápida do ECG, Editora de Publições Biomédicas EPUB, Rio de Janeiro. Ferriere, R. & Fox, G. A. (99), Chaos and evolution, Trends in Ecology and Evolution, v.0, n., pp Garfinkel, A., Spano, M. L., Ditto, W. L. & Weiss, J. N. (99), Controlling cardiac chaos, Science, v.7, pp.0-. Garfinkel, A., Weiss, J. N., Ditto, W. L. & Spano, M. L. (99), Chaos control of cardiac arrhythmias, Trends in Cardiovascular Medicine, v., n., pp Glass, L. (00), Synchronization and Rhythmic Processes in Physiology, Nature, v.0, March, pp Hodkin, A. L. & Huxley, A. F. (9). A quantitative description of membrane current and its application to conduction and excitation in nerve, J. Physiology,v.7, pp.00-. Malmivuo, J. & Plonsey, R. (99), Bioelectromagnetism - Principles and applications of bioelectric and biomagnetic fields, Oxford University Press, New York. Moffa, P.J. & Sanches, P.C.R. (00) Eletrocardiograma Normal e Patológico, Editora Roca. Radhakrishna, R. K. A., Dutt, D. N., Yeragani, V. K. (000), Nonlinear measures of heart rate time series: Influence of posture and controlled breathing, Autonomic Neuroscience: Basic and Clinical, v.8, pp.8 8. Santos, A.M., Lopes, S.R. & Viana, R.L. (00), Rhythm synchronization and chaotic modulation of coupled Van der Pol oscillators in a model for the heartbeat, Physica A, v.8, pp.-. Savi, M.A. (00), Chaos and order in biomedical rhythms, Journal of the Brazilian Society of Mechanical Sciences and Engineering, v.xxvii, n., pp.7-9. Savi, M.A. (00), Nonlinear dynamics and chaos, Editora E-papers (in portuguese). Van Der Pol, B. (9), On relaxation oscillations, Philosophical Magazine, v., pp.978. Van Der Pol, B. & Van Der Mark, J. (98), The heartbeat considered as a relaxation oscillator, and an electrical model of the heart, Philosophical Magazine, v. suppl., pp.7. Witkowski, F. X., Kavanagh, K. M., Penkoske, P. A., Plonsey, R., Spano, M. L., Ditto, W. L. & Kaplan, D. T. (99), Evidence for determinism in ventricular fibrillation, Physical Review Letters, v.7, n., pp.0-. Witkowski, F. X., Leon, L. J., Penkoske, P. A., Giles, W. R., Spano, M. L., Ditto, W. L. & Winfree, A. T. (998), Spatiotemporal evolution of ventricular fibrillation, Nature, v.9, March, pp RESPONSIBILITY NOTICE The authors are the only responsible for the printed material included in this paper.
PART I. Disorders of the Heart Rhythm: Basic Principles
 PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
Cardiac Cycle. Each heartbeat is called a cardiac cycle. First the two atria contract at the same time.
 The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
ELECTROCARDIOGRAPHY (ECG)
 ELECTROCARDIOGRAPHY (ECG) The heart is a muscular organ, which pumps blood through the blood vessels of the circulatory system. Blood provides the body with oxygen and nutrients, as well as assists in
ELECTROCARDIOGRAPHY (ECG) The heart is a muscular organ, which pumps blood through the blood vessels of the circulatory system. Blood provides the body with oxygen and nutrients, as well as assists in
Cardiovascular System
 Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
Outline. Electrical Activity of the Human Heart. What is the Heart? The Heart as a Pump. Anatomy of the Heart. The Hard Work
 Electrical Activity of the Human Heart Oguz Poroy, PhD Assistant Professor Department of Biomedical Engineering The University of Iowa Outline Basic Facts about the Heart Heart Chambers and Heart s The
Electrical Activity of the Human Heart Oguz Poroy, PhD Assistant Professor Department of Biomedical Engineering The University of Iowa Outline Basic Facts about the Heart Heart Chambers and Heart s The
Cardiovascular System Notes: Physiology of the Heart
 Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
Lab 2. The Intrinsic Cardiac Conduction System. 1/23/2016 MDufilho 1
 Lab 2 he Intrinsic Cardiac Conduction System 1/23/2016 MDufilho 1 Figure 18.13 Intrinsic cardiac conduction system and action potential succession during one heartbeat. Superior vena cava ight atrium 1
Lab 2 he Intrinsic Cardiac Conduction System 1/23/2016 MDufilho 1 Figure 18.13 Intrinsic cardiac conduction system and action potential succession during one heartbeat. Superior vena cava ight atrium 1
4. The two inferior chambers of the heart are known as the atria. the superior and inferior vena cava, which empty into the left atrium.
 Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Full file at
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
Where are the normal pacemaker and the backup pacemakers of the heart located?
 CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
EKG Abnormalities. Adapted from:
 EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
Modeling Chaos in the Heart
 Modeling Chaos in the Heart S. M. Haider Aejaz haider_aejaz@yahoo.com PIMCS, Lahore, Pakistan Abstract: Chaos theory describes the dynamics of a deterministic system whose dynamics show extreme dependence
Modeling Chaos in the Heart S. M. Haider Aejaz haider_aejaz@yahoo.com PIMCS, Lahore, Pakistan Abstract: Chaos theory describes the dynamics of a deterministic system whose dynamics show extreme dependence
Chapter 20 (2) The Heart
 Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Comparison of Different ECG Signals on MATLAB
 International Journal of Electronics and Computer Science Engineering 733 Available Online at www.ijecse.org ISSN- 2277-1956 Comparison of Different Signals on MATLAB Rajan Chaudhary 1, Anand Prakash 2,
International Journal of Electronics and Computer Science Engineering 733 Available Online at www.ijecse.org ISSN- 2277-1956 Comparison of Different Signals on MATLAB Rajan Chaudhary 1, Anand Prakash 2,
Department of medical physiology 7 th week and 8 th week
 Department of medical physiology 7 th week and 8 th week Semester: winter Study program: Dental medicine Lecture: RNDr. Soňa Grešová, PhD. Department of medical physiology Faculty of Medicine PJŠU Cardiovascular
Department of medical physiology 7 th week and 8 th week Semester: winter Study program: Dental medicine Lecture: RNDr. Soňa Grešová, PhD. Department of medical physiology Faculty of Medicine PJŠU Cardiovascular
Chapter 13 The Cardiovascular System: Cardiac Function
 Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Shock-induced termination of cardiac arrhythmias
 Shock-induced termination of cardiac arrhythmias Group members: Baltazar Chavez-Diaz, Chen Jiang, Sarah Schwenck, Weide Wang, and Jinglei Zhang Abstract: Cardiac arrhythmias occur when blood flow to the
Shock-induced termination of cardiac arrhythmias Group members: Baltazar Chavez-Diaz, Chen Jiang, Sarah Schwenck, Weide Wang, and Jinglei Zhang Abstract: Cardiac arrhythmias occur when blood flow to the
Test Review Circulatory System Chapters
 Test Review Circulatory System Chapters 13-2010 1. The tissue that forms the tight fitting sac around the heart is the a. parietal pericardium c. myocardium b. visceral pericardium d. endocardium 2. Which
Test Review Circulatory System Chapters 13-2010 1. The tissue that forms the tight fitting sac around the heart is the a. parietal pericardium c. myocardium b. visceral pericardium d. endocardium 2. Which
Collin County Community College
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 5 The Heart 1 The Heart Beat and the EKG 2 1 The Heart Beat and the EKG P-wave = Atrial depolarization QRS-wave = Ventricular depolarization
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 5 The Heart 1 The Heart Beat and the EKG 2 1 The Heart Beat and the EKG P-wave = Atrial depolarization QRS-wave = Ventricular depolarization
Shock-induced termination of cardiac arrhythmias
 Shock-induced termination of cardiac arrhythmias Group members: Baltazar Chavez-Diaz, Chen Jiang, Sarah Schwenck, Weide Wang, and Jinglei Zhang Cardiac arrhythmias, also known as irregular heartbeat, occur
Shock-induced termination of cardiac arrhythmias Group members: Baltazar Chavez-Diaz, Chen Jiang, Sarah Schwenck, Weide Wang, and Jinglei Zhang Cardiac arrhythmias, also known as irregular heartbeat, occur
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Cardiac physiology. b. myocardium -- cardiac muscle and fibrous skeleton of heart
 I. Heart anatomy -- general gross. A. Size/orientation - base/apex B. Coverings D. Chambers 1. parietal pericardium 2. visceral pericardium 3. Layers of heart wall a. epicardium Cardiac physiology b. myocardium
I. Heart anatomy -- general gross. A. Size/orientation - base/apex B. Coverings D. Chambers 1. parietal pericardium 2. visceral pericardium 3. Layers of heart wall a. epicardium Cardiac physiology b. myocardium
Electrocardiography I Laboratory
 Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits:
 1 The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits: pulmonary and systemic. The pulmonary goes out to the
1 The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits: pulmonary and systemic. The pulmonary goes out to the
Introduction. Circulation
 Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
BIPN100 F15 Human Physiology I (Kristan) Problem set #5 p. 1
 BIPN100 F15 Human Physiology I (Kristan) Problem set #5 p. 1 1. Dantrolene has the same effect on smooth muscles as it has on skeletal muscle: it relaxes them by blocking the release of Ca ++ from the
BIPN100 F15 Human Physiology I (Kristan) Problem set #5 p. 1 1. Dantrolene has the same effect on smooth muscles as it has on skeletal muscle: it relaxes them by blocking the release of Ca ++ from the
ECG. Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13
 ECG Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13 The Concept When the cardiac impulse passes through the heart, electrical current
ECG Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13 The Concept When the cardiac impulse passes through the heart, electrical current
Collin County Community College. ! BIOL Anatomy & Physiology! WEEK 5. The Heart
 Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
The Electrocardiogram
 The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
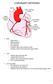 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
The Heart. Happy Friday! #takeoutyournotes #testnotgradedyet
 The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
Chapter 18 - Heart. I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity)
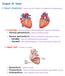 Chapter 18 - Heart I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity) A. Coverings: heart enclosed in double walled sac called the pericardium 1. Fibrous pericardium: dense connective
Chapter 18 - Heart I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity) A. Coverings: heart enclosed in double walled sac called the pericardium 1. Fibrous pericardium: dense connective
Cardiovascular System Notes: Heart Disease & Disorders
 Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 20 The Cardiovascular System: The Heart Introduction The purpose of the chapter is to: 1. Learn about the components of the cardiovascular system
Principles of Anatomy and Physiology 14 th Edition CHAPTER 20 The Cardiovascular System: The Heart Introduction The purpose of the chapter is to: 1. Learn about the components of the cardiovascular system
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
Heart. Heart 2-Tunica media: middle layer (media ='middle') muscle fibers (smooth or cardiac).
 t. innermost lumenal General Circulatory system heart and blood vessels walls have 3 layers (inside to outside) 1-Tunica interna: aka tunica intima layer--lumenal layer epithelium--endothelium simple squamous
t. innermost lumenal General Circulatory system heart and blood vessels walls have 3 layers (inside to outside) 1-Tunica interna: aka tunica intima layer--lumenal layer epithelium--endothelium simple squamous
Chapter 12: Cardiovascular Physiology System Overview
 Chapter 12: Cardiovascular Physiology System Overview Components of the cardiovascular system: Heart Vascular system Blood Figure 12-1 Plasma includes water, ions, proteins, nutrients, hormones, wastes,
Chapter 12: Cardiovascular Physiology System Overview Components of the cardiovascular system: Heart Vascular system Blood Figure 12-1 Plasma includes water, ions, proteins, nutrients, hormones, wastes,
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Objectives of the Heart
 Objectives of the Heart Electrical activity of the heart Action potential EKG Cardiac cycle Heart sounds Heart Rate The heart s beat separated into 2 phases Relaxed phase diastole (filling of the chambers)
Objectives of the Heart Electrical activity of the heart Action potential EKG Cardiac cycle Heart sounds Heart Rate The heart s beat separated into 2 phases Relaxed phase diastole (filling of the chambers)
Lab Activity 24 EKG. Portland Community College BI 232
 Lab Activity 24 EKG Reference: Dubin, Dale. Rapid Interpretation of EKG s. 6 th edition. Tampa: Cover Publishing Company, 2000. Portland Community College BI 232 Graph Paper 1 second equals 25 little boxes
Lab Activity 24 EKG Reference: Dubin, Dale. Rapid Interpretation of EKG s. 6 th edition. Tampa: Cover Publishing Company, 2000. Portland Community College BI 232 Graph Paper 1 second equals 25 little boxes
BME 5742 Bio-Systems Modeling and Control. Lecture 41 Heart & Blood Circulation Heart Function Basics
 BME 5742 Bio-Systems Modeling and Control Lecture 41 Heart & Blood Circulation Heart Function Basics Dr. Zvi Roth (FAU) 1 Pumps A pump is a device that accepts fluid at a low pressure P 1 and outputs the
BME 5742 Bio-Systems Modeling and Control Lecture 41 Heart & Blood Circulation Heart Function Basics Dr. Zvi Roth (FAU) 1 Pumps A pump is a device that accepts fluid at a low pressure P 1 and outputs the
10/23/2017. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]
![QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]](/thumbs/96/126998162.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
37 1 The Circulatory System
 H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
The Heart. Size, Form, and Location of the Heart. 1. Blunt, rounded point; most inferior part of the heart.
 12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
Lab #3: Electrocardiogram (ECG / EKG)
 Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
Electrocardiography Abnormalities (Arrhythmias) 7. Faisal I. Mohammed, MD, PhD
 Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
The Circulatory System. The Heart, Blood Vessels, Blood Types
 The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
Circulatory system ( 循环系统 )
 Circulatory system ( 循环系统 ) Circulatory system: heart + blood vessels Function: nutrient transportation and metabolites returning Blood: carrier Heart: pump Blood vessels: route, substance communications
Circulatory system ( 循环系统 ) Circulatory system: heart + blood vessels Function: nutrient transportation and metabolites returning Blood: carrier Heart: pump Blood vessels: route, substance communications
Rhythmical Excitation of the Heart
 Rhythmical Excitation of the Heart KALEB HOOD AND JIMMY JOHNSON Special Excitory and Conductive System of the Heart Sinus Node (or sinoatrial node or S-A): A small node with almost no contractile muscle,
Rhythmical Excitation of the Heart KALEB HOOD AND JIMMY JOHNSON Special Excitory and Conductive System of the Heart Sinus Node (or sinoatrial node or S-A): A small node with almost no contractile muscle,
Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC
 Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC Who am I? Class Outline Gross anatomy of the heart Trip around the heart Micro anatomy: cellular and tissue level Introduction
Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC Who am I? Class Outline Gross anatomy of the heart Trip around the heart Micro anatomy: cellular and tissue level Introduction
Approximately the size of your fist Location. Pericardial physiology
 Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
Cardiac Telemetry Self Study: Part One Cardiovascular Review 2017 THINGS TO REMEMBER
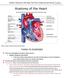 Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
SAMPLE CHAPTER CHAPTER
 2.1 Introduction CHAPTER 2 Cardiovascular Structure and Function One may question why it is important for a biomedical engineer to study physiology. To answer this question, we can begin by recognizing
2.1 Introduction CHAPTER 2 Cardiovascular Structure and Function One may question why it is important for a biomedical engineer to study physiology. To answer this question, we can begin by recognizing
Electrocardiography Biomedical Engineering Kaj-Åge Henneberg
 Electrocardiography 31650 Biomedical Engineering Kaj-Åge Henneberg Electrocardiography Plan Function of cardiovascular system Electrical activation of the heart Recording the ECG Arrhythmia Heart Rate
Electrocardiography 31650 Biomedical Engineering Kaj-Åge Henneberg Electrocardiography Plan Function of cardiovascular system Electrical activation of the heart Recording the ECG Arrhythmia Heart Rate
Chapter 20: Cardiovascular System: The Heart
 Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
WHAT S THAT RHYTHM I AM HEARING? GUIDE TO AUSCULTATION OF ARRHYTHMIAS IN HORSES
 WHAT S THAT RHYTHM I AM HEARING? GUIDE TO AUSCULTATION OF ARRHYTHMIAS IN HORSES Michelle Henry Barton DVM, PhD, DACVIM University of Georgia, Athens, GA INTRODUCTION The purpose of this talk is to review
WHAT S THAT RHYTHM I AM HEARING? GUIDE TO AUSCULTATION OF ARRHYTHMIAS IN HORSES Michelle Henry Barton DVM, PhD, DACVIM University of Georgia, Athens, GA INTRODUCTION The purpose of this talk is to review
Conduction System of the Heart 4. Faisal I. Mohammed, MD, PhD
 Conduction System of the Heart 4 Faisal I. Mohammed, MD, PhD 1 Objectives List the parts that comprise the conduction system Explain the mechanism of slow response action potential (pacemaker potential)
Conduction System of the Heart 4 Faisal I. Mohammed, MD, PhD 1 Objectives List the parts that comprise the conduction system Explain the mechanism of slow response action potential (pacemaker potential)
Health Science 20 Circulatory System Notes
 Health Science 20 Circulatory System Notes Functions of the Circulatory System The circulatory system functions mainly as the body s transport system. It transports: o Oxygen o Nutrients o Cell waste o
Health Science 20 Circulatory System Notes Functions of the Circulatory System The circulatory system functions mainly as the body s transport system. It transports: o Oxygen o Nutrients o Cell waste o
آالء العجرمي أسامة الخضر. Faisal Muhammad
 16 آالء العجرمي أسامة الخضر Faisal Muhammad 1. Summary for what taken : *changes in permeability of ions: 1. During phase 0: changes happen due to the influx of Na+, the permeability of Na ions increase
16 آالء العجرمي أسامة الخضر Faisal Muhammad 1. Summary for what taken : *changes in permeability of ions: 1. During phase 0: changes happen due to the influx of Na+, the permeability of Na ions increase
The conduction system
 The conduction system In today s lecture we will discuss the conducting system of the heart. If we placed the heart in a special solution that contains Ca+ it will keep on contracting, keep in mind that
The conduction system In today s lecture we will discuss the conducting system of the heart. If we placed the heart in a special solution that contains Ca+ it will keep on contracting, keep in mind that
The Heart and Heart Disease
 The Heart and Heart Disease Illustration of the heart by Leonardo DaVinci heart-surgeon.com/ history.html 2/14/2010 1 I. Location, Size and Position of the Heart A. Triangular organ located 1. of mass
The Heart and Heart Disease Illustration of the heart by Leonardo DaVinci heart-surgeon.com/ history.html 2/14/2010 1 I. Location, Size and Position of the Heart A. Triangular organ located 1. of mass
Circulation. Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body
 Circulation Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body Heart = muscular organ about the size of your fist which pumps blood.
Circulation Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body Heart = muscular organ about the size of your fist which pumps blood.
The Cardiovascular System
 11 PART A The Cardiovascular System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Cardiovascular
11 PART A The Cardiovascular System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Cardiovascular
CASE 10. What would the ST segment of this ECG look like? On which leads would you see this ST segment change? What does the T wave represent?
 CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The HEART. What is it???? Pericardium. Heart Facts. This muscle never stops working It works when you are asleep
 This muscle never stops working It works when you are asleep The HEART It works when you eat It really works when you exercise. What is it???? Located between the lungs in the mid thoracic region Apex
This muscle never stops working It works when you are asleep The HEART It works when you eat It really works when you exercise. What is it???? Located between the lungs in the mid thoracic region Apex
Paramedic Rounds. Tachyarrhythmia's. Sean Sutton Dallas Wood
 Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Cardiac Conduction System
 Cardiac Conduction System What causes the Heart to Beat? Heart contracts by electrical signals! Cardiac muscle tissue contracts on its own an electrical signal is sent out by the heart so that all cells
Cardiac Conduction System What causes the Heart to Beat? Heart contracts by electrical signals! Cardiac muscle tissue contracts on its own an electrical signal is sent out by the heart so that all cells
Cardiovascular System
 Cardiovascular System Purpose Transport oxygen and nutrients Take waste products away from tissues & organs Things we learned Blood pressure: the force of blood pushing against the walls of blood vessels
Cardiovascular System Purpose Transport oxygen and nutrients Take waste products away from tissues & organs Things we learned Blood pressure: the force of blood pushing against the walls of blood vessels
CARDIAC PHYSIOLOGY. Amelyn U. Ramos-Rafael,M.D. Functional Anatomy of the Heart
 CARDIAC PHYSIOLOGY Amelyn U. Ramos-Rafael,M.D. Functional Anatomy of the Heart 1 Functional Anatomy of The Heart The Atria relatively thin walled The Ventricles ventricular walls thicker than atrial walls
CARDIAC PHYSIOLOGY Amelyn U. Ramos-Rafael,M.D. Functional Anatomy of the Heart 1 Functional Anatomy of The Heart The Atria relatively thin walled The Ventricles ventricular walls thicker than atrial walls
CARDIAC CYCLE CONTENTS. Divisions of cardiac cycle 11/13/13. Definition. Badri Paudel GMC
 CARDIAC CYCLE Badri Paudel GMC CONTENTS Ø DEFINATION Ø DIVISION OF CARDIAC CYCLE Ø SUB DIVISION AND DURATION OF CARDIAC CYCLE Ø SYSTOLE Ø DIASTOLE Ø DESCRIPTION OF EVENTS OF CARDIAC CYCLE Ø SUMMARY Ø ELECTROCARDIOGRAPHY
CARDIAC CYCLE Badri Paudel GMC CONTENTS Ø DEFINATION Ø DIVISION OF CARDIAC CYCLE Ø SUB DIVISION AND DURATION OF CARDIAC CYCLE Ø SYSTOLE Ø DIASTOLE Ø DESCRIPTION OF EVENTS OF CARDIAC CYCLE Ø SUMMARY Ø ELECTROCARDIOGRAPHY
A. Incorrect! The left ventricle receives oxygenated blood from the lungs via the left atrium.
 Anatomy and Physiology - Problem Drill 16: The Cardiovascular System No. 1 of 10 Instruction: (1) Read the problem statement and answer choices carefully (2) Work the problems on paper as needed (3) Pick
Anatomy and Physiology - Problem Drill 16: The Cardiovascular System No. 1 of 10 Instruction: (1) Read the problem statement and answer choices carefully (2) Work the problems on paper as needed (3) Pick
Enhanced Cellular Automation Model For Detecting Heart Fibrillation
 Enhanced Cellular Automation Model For Detecting Heart Fibrillation R. Touqan, A. Nasser & N. Hamdy Arab Academy for Science and Technology (AAST), email< rtouqan@hotmail.com Abstract: A new technique
Enhanced Cellular Automation Model For Detecting Heart Fibrillation R. Touqan, A. Nasser & N. Hamdy Arab Academy for Science and Technology (AAST), email< rtouqan@hotmail.com Abstract: A new technique
Practice Exercises for the Cardiovascular System
 Practice Exercises for the Cardiovascular System On the diagram below, color the oxygen-rich blood red and the oxygen-poor blood blue. Label the parts: Continued on the next page... Label the parts on
Practice Exercises for the Cardiovascular System On the diagram below, color the oxygen-rich blood red and the oxygen-poor blood blue. Label the parts: Continued on the next page... Label the parts on
The Cardiovascular System
 Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
*Generating blood pressure *Routing blood: separates. *Ensuring one-way blood. *Regulating blood supply *Changes in contraction
 *Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
*Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
Cardiac Properties MCQ
 Cardiac Properties MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Cardiac Valves: a- Prevent backflow of blood from the ventricles to the atria during
Cardiac Properties MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Cardiac Valves: a- Prevent backflow of blood from the ventricles to the atria during
The Cardiovascular System (Heart)
 The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
The Mammalian Circulatory System
 The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
االء العجرمي. Not corrected. Faisal Muhammad
 61 االء العجرمي Not corrected Faisal Muhammad 1. Summary for what taken : *changes in permeability of ions : 1. During phase 0 : changes happen due to the influx of Na+, the permeability of Na ions increase
61 االء العجرمي Not corrected Faisal Muhammad 1. Summary for what taken : *changes in permeability of ions : 1. During phase 0 : changes happen due to the influx of Na+, the permeability of Na ions increase
Interpreting Electrocardiograms (ECG) Physiology Name: Per:
 Interpreting Electrocardiograms (ECG) Physiology Name: Per: Introduction The heart has its own system in place to create nerve impulses and does not actually require the brain to make it beat. This electrical
Interpreting Electrocardiograms (ECG) Physiology Name: Per: Introduction The heart has its own system in place to create nerve impulses and does not actually require the brain to make it beat. This electrical
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Unit 10 ~ Learning Guide
 Unit 10 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 10 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
ECG Interpretation Cat Williams, DVM DACVIM (Cardiology)
 ECG Interpretation Cat Williams, DVM DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian. GOAL: Reduce Anxiety about ECGs Back to
ECG Interpretation Cat Williams, DVM DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian. GOAL: Reduce Anxiety about ECGs Back to
TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT
 Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Heart: Cardiac Function & ECGs. The Heart and Circulatory System
 Heart: Cardiac Function & ECGs Adapted From: Textbook Of Medical Physiology, 11 th Ed. Arthur C. Guyton, John E. Hall Chapters 9, 10, 11, 12, & 13 John P. Fisher The Heart and Circulatory System Introduction
Heart: Cardiac Function & ECGs Adapted From: Textbook Of Medical Physiology, 11 th Ed. Arthur C. Guyton, John E. Hall Chapters 9, 10, 11, 12, & 13 John P. Fisher The Heart and Circulatory System Introduction
Ch 19: Cardiovascular System - The Heart -
 Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
Electrical Conduction
 Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Arrhythmias. Pulmonary Artery
 Arrhythmias Introduction Cardiac arrhythmia is an irregularity of the heart beat that causes the heart to beat too slowly, too fast, or irregularly. There are different types of arrhythmias. Most arrhythmias
Arrhythmias Introduction Cardiac arrhythmia is an irregularity of the heart beat that causes the heart to beat too slowly, too fast, or irregularly. There are different types of arrhythmias. Most arrhythmias
CIRCULATION. Cardiovascular & lymphatic systems Functions. Transport Defense / immunity Homeostasis
 CIRCULATION CIRCULATION Cardiovascular & lymphatic systems Functions Transport Defense / immunity Homeostasis 2 Types of Circulatory Systems Open circulatory system Contains vascular elements Mixing of
CIRCULATION CIRCULATION Cardiovascular & lymphatic systems Functions Transport Defense / immunity Homeostasis 2 Types of Circulatory Systems Open circulatory system Contains vascular elements Mixing of
Electrocardiogram and Heart Sounds
 Electrocardiogram and Heart Sounds Five physiologic properties of cardiac muscle Automaticity: SA node is the primary pacemaker of the heart, but any cells in the conduction system can initiate their
Electrocardiogram and Heart Sounds Five physiologic properties of cardiac muscle Automaticity: SA node is the primary pacemaker of the heart, but any cells in the conduction system can initiate their
PROBLEM SET 3. Assigned: February 19, 2004 Due: February 26, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
12.2 Monitoring the Human Circulatory System
 12.2 Monitoring the Human Circulatory System Video 1: 3D Animation of Heart Pumping Blood blood flow through the heart... Video 2: Hank Reviews Everything on the Heart https://www.youtube.com/watch?v=x9zz6tcxari
12.2 Monitoring the Human Circulatory System Video 1: 3D Animation of Heart Pumping Blood blood flow through the heart... Video 2: Hank Reviews Everything on the Heart https://www.youtube.com/watch?v=x9zz6tcxari
