Pulmonary hypertension is a significant cause of morbidity
|
|
|
- Clyde Page
- 6 years ago
- Views:
Transcription
1 Randomized Controlled Study of Inhaled Nitric Oxide After Operation for Congenital Heart Disease Ronald W. Day, MD, John A. Hawkins, MD, Edwin C. McGough, MD, Kevin L. Crezeé, RRT, and Garth S. Orsmond, MD Divisions of Pediatric Cardiology and Cardiothoracic Surgery, University of Utah and Primary Children s Medical Center, Salt Lake City, Utah Background. Inhaled nitric oxide selectively decreases pulmonary vascular resistance. This study was performed to determine whether inhaled nitric oxide decreases the incidence of pulmonary hypertensive crises after corrective procedures for congenital heart disease. Methods. Patients with a systolic pulmonary arterial pressure of 50% or more of the systolic systemic arterial pressure during the early postoperative period were randomized to receive 20 parts per million inhaled nitric oxide (n 20) or conventional therapy alone (n 20). Acute hemodynamic and blood gas measurements were performed at the onset of therapy. The efficacy of sustained therapy was determined by comparing the number of patients in each group who experienced a pulmonary hypertensive crisis. Results. In comparison to controls, there were no significant differences in the baseline and 1-hour measurements of patients who were treated with nitric oxide. Four patients in the control group and 3 patients in the nitric oxide group experienced a pulmonary hypertensive crisis. Conclusions. Nitric oxide did not substantially improve pulmonary hemodynamics and gas exchange immediately after operation for congenital heart disease. Nitric oxide also failed to significantly decrease the incidence of pulmonary hypertensive crises. (Ann Thorac Surg 2000;69: ) 2000 by The Society of Thoracic Surgeons Pulmonary hypertension is a significant cause of morbidity and mortality after corrective procedures and heart transplantation in patients with congenital heart disease [1, 2]. Pulmonary endothelial function is decreased with advanced stages of pulmonary vascular disease [3, 4]. The production of nitric oxide by the pulmonary circulation is further impaired during the early postoperative period [5]. When inhaled, nitric oxide selectively decreases the pulmonary vascular resistance of many patients with congenital heart disease and pulmonary hypertension [6, 7]. For this reason, nitric oxide may prevent complications from right ventricular failure or decrease the incidence of pulmonary hypertensive crises after operation when the heart and pulmonary circulation are recovering from the effects of cardiopulmonary bypass. In previous studies [8 18], nitric oxide has been used to acutely decrease pulmonary vascular resistance in patients after surgical palliation or repair. However, previous studies have lacked controls during sustained therapy to determine whether a specific outcome could potentially be improved by treating all patients with moderately severe pulmonary hypertension. Thus, we performed a randomized, controlled study of Accepted for publication Dec 22, Address reprint requests to Dr Day, Division of Pediatric Cardiology, Primary Children s Medical Center, 100 North Medical Dr, Salt Lake City, UT 84113; ron.day@hsc.utah.edu. patients with congenital heart disease after corrective operation or heart transplantation to determine [1] whether inhaled nitric oxide acutely improves blood gases and pulmonary hemodynamics, and [2] whether sustained therapy prevents pulmonary hypertensive crises. Material and Methods This study was approved by the Research and Human Subjects Committee of Primary Children s Medical Center (July 29, 1993). Informed consent was obtained from the patients ( 18 years of age) or their parents. An Investigational New Drug application for the use of inhaled nitric oxide for postoperative pulmonary hypertension was approved by the US Food and Drug Administration (March 12, 1993). This study was performed from August 1993 to August Patients Patients with congenital heart disease who underwent a biventricular repair or heart transplantation were eligible for enrollment if their systolic pulmonary arterial pressure was 50% or more of the systolic systemic arterial pressure when they were successfully removed from cardiopulmonary bypass. Patients with lower pulmonary arterial pressures are less likely to have problems with 2000 by The Society of Thoracic Surgeons /00/$20.00 Published by Elsevier Science Inc PII S (00)
2 1908 DAY ET AL Ann Thorac Surg POSTOPERATIVE INHALED NITRIC OXIDE 2000;69: postoperative pulmonary hypertension [17]. Modified ultrafiltration was performed in all patients immediately after cardiopulmonary bypass. Pulmonary arterial catheters were placed in all patients before they were transferred from the surgical suite to the intensive care unit. Preoperative hemodynamics were not used to enroll patients because heart catheterization was not a prerequisite for operation; however, all patients had at least echocardiographic evidence of pulmonary hypertension before operation. Consent was generally not obtained until an increased pulmonary arterial pressure was confirmed at the completion of operation, although many families were informed of the study before operation. Patients were randomly assigned to a control group that received conventional therapy or a treatment group that received 20 parts per million (ppm) inhaled nitric oxide. Patients were randomized by a blind draw from sequential groups containing six assignments. Conventional therapy was determined by each patient s attending cardiothoracic surgeon. The research committee of Primary Children s Medical Center required that conventional therapy was not restricted by the study to avoid any conflict with the clinical judgment of the patients physicians. Acute Hemodynamic and Blood Gas Measurements Heart rate, systemic arterial pressure, pulmonary arterial pressure, atrial pressures, and pulse oximetry were monitored continuously by care providers. Baseline hemodynamic and blood gas measurements were performed when patients were clinically stable after admission to the intensive care unit. Inhaled nitric oxide was then administered to patients in the treatment group in an open labeled, or unblinded manner as previously described [19, 20]. The control group was not given a placebo gas of nitrogen. After a period of approximately 1 hour, the hemodynamic and blood gas measurements were repeated. Pulmonary Hypertensive Crises During Sustained Therapy The primary outcome of sustained therapy was determined by comparing the number of patients in each group who experienced a pulmonary hypertensive crisis. For this study, a pulmonary hypertensive crisis was defined as an acute episode of suprasystemic pulmonary arterial pressure associated with a decrease in blood pressure, heart rate, or oxygenation that required a change in medical therapy or ventilatory support. Death was not used to evaluate outcome because a previous study reported a potential lifesaving benefit from nitric oxide therapy [8]. Thus, control patients who experienced a pulmonary hypertensive crisis were allowed to crossover and receive inhaled nitric oxide after failing conventional therapy. Nitric oxide was not discontinued in treated patients who experienced a pulmonary hypertensive crisis unless there was a concern of drug toxicity because life-threatening events may occur when therapy is abruptly withdrawn [21]. Nitric oxide was administered at a concentration of 20 Table 1. Patient Diagnoses Diagnoses Control Nitric Oxide Cardiac Atrioventricular 5 7 septal defect Atrial or ventricular 5 6 septal defect Total anomalous 3 3 pulmonary venous return Partial anomalous 1 0 pulmonary venous return Pulmonary venous 3 2 obstruction Mitral valve stenosis 0 1 Single ventricle with 1 0 aortic hypoplasia Tetralogy of Fallot 1 0 Stenosis of the 1 0 aortic and pulmonary valves Cor triatriatum 0 1 Other Down syndrome 7 8 Lung disease before operation ppm until care providers decided to wean the patient from assisted ventilation. Before extubation, nitric oxide was gradually withdrawn by decreasing the dose during a period of 6 to 12 hours. The amount of supplemental oxygen was transiently increased when nitric oxide was discontinued. Statistical Analysis Numerical values are expressed as mean standard error of the mean. Serial hemodynamic and blood gas measurements were compared by analysis of variance for repeated measures. A factorial analysis of variance or Fisher s exact test was used for comparisons between patient groups. Significant results were determined by p less than 0.05 using a Scheffé s F test (Statview II, Abacus Concepts, Berkeley, CA). Results Patients Nineteen patients were enrolled into each patient group. Two patients were enrolled on two separate occasions; both underwent operation for pulmonary venous obstruction after an initial repair of total anomalous pulmonary venous return. The patients diagnoses are listed in Table 1. A similar number of patients had Down syndrome in each group. Table 1 also indicates that several patients in each group had radiographic evidence of lung disease before operation. The median age was 6 months (range, 1 day to 3 years) in control patients and 7 months
3 Ann Thorac Surg DAY ET AL 2000;69: POSTOPERATIVE INHALED NITRIC OXIDE 1909 Table 2. Inotropic and Vasodilatory Agents Agents Control Nitric Oxide Dopamine Dobutamine Nitroprusside Milrinone 9 9 Amrinone 5 5 Epinephrine 7 6 Isoproterenol 1 0 Prostaglandin E (range, 1 day to 20 years) in patients who received inhaled nitric oxide. All patients were treated with a narcotic for pain control and a benzodiazepine for sedation. Neuromuscular blockade was used from the onset of enrollment in 16 control patients and 15 patients who were treated with nitric oxide. Table 2 lists the inotropic and vasodilatory agents that were used at the time of baseline hemodynamic and blood gas measurements. Corrective operation was attempted in all but 1 patient who underwent heart transplantation for a single ventricle and aortic hypoplasia, and 1 patient who was left with a small residual atrial septal defect after closure of a ventricular septal defect. Anatomic obstruction of the pulmonary circulation was identified in 5 patients during the postoperative period. In the control group, 1 patient had residual pulmonary venous obstruction, 1 patient had branch pulmonary artery stenosis, and 1 patient had mild mitral valve stenosis. In the group of patients who received inhaled nitric oxide, 2 patients had residual pulmonary venous obstruction. Acute Hemodynamic and Blood Gas Measurements Table 3 lists the mean hemodynamic and blood gas measurements for each group of patients. There were no significant differences in baseline measurements between patient groups. In comparison to baseline measurements, significant changes in heart rate, pulmonary arterial pressure, left atrial pressure, ph, arterial carbon dioxide tension, and the ratio of arterial oxygen tension and fraction of inspired oxygen were observed only in Fig 1. Ratio of systolic pulmonary and systolic systemic arterial pressures. In comparison to baseline, patients developed a small improvement in the ratio of systolic pulmonary and systolic systemic arterial pressures (systolic PAP/systolic SAP) after the onset of inhaled nitric oxide therapy (*p 0.011). However, there were no differences between patient groups at baseline or after 1 hour of observation. patients who received inhaled nitric oxide. The change in right atrial pressure for treated patients was not statistically significant (p 0.065). Figure 1 shows a small, but significant, decrease in the ratio of systolic pulmonary and systemic arterial pressures. There were no measured differences between patient groups after 1 hour of observation. However, the difference between the changes in ratio of systolic pulmonary and systemic arterial pressures for the two patient groups approached statistical significance (p 0.066). Two control patients and 4 patients who were treated with inhaled nitric oxide acutely experienced a 20% or more decrease in the ratio of systolic pulmonary and systemic arterial pressures. Six control patients and 9 patients who were treated with inhaled nitric oxide acutely experienced a 10% or more decrease in the ratio of systolic pulmonary and systemic arterial pressures. The sample size was large enough to conclude that nitric oxide did not decrease the ratio of systolic pulmonary and systemic arterial pressures by 20% in comparison to controls with a power (1- ) more than Table 3. Acute Hemodynamic and Blood Gas Measurements Variables Control Group Nitric Oxide Group Baseline 1-Hour Baseline 1-Hour Heart rate (min 1 ) a Systolic pulmonary pressure a Systolic systemic pressure Right atrial pressure Left atrial pressure a ph a PaCO a PaO 2 /FIO a PaCO 2 arterial carbon dioxide tension; PaO 2 /FIO 2 ratio between the arterial oxygen tension and the fraction of inspired oxygen. a p 0.05 versus baseline. There were no differences between patient groups at baseline or after 1 hour of therapy.
4 1910 DAY ET AL Ann Thorac Surg POSTOPERATIVE INHALED NITRIC OXIDE 2000;69: Table 4. Characteristics of Patients Who Developed Pulmonary Hypertensive Crises Patient Age Diagnosis Onset of Crisis Lung Disease Neuromuscular Blockade Control group 1 4 months Aortic and pulmonary valve stenosis 2 hours Yes Yes 2 5 months Atrioventricular septal defect 5 days Yes No 3 7 months Tetralogy of Fallot, branch pulmonary stenosis 3 days Yes Yes 4 6 months Atrial and ventricular septal defects 2 days Yes No Nitric oxide group 1 7 months Pulmonary venous obstruction 12 hours No No 2 7 months Atrioventricular septal defect 16 hours No No 3 12 months Ventricular septal defect 2 hours Yes No Arterial blood gas, right atrial pressure, pulmonary arterial pressure, and systemic arterial pressure measurements and comparisons were performed in all patients. Heart rate comparisons were limited to 17 control patients and 13 patients who received inhaled nitric oxide because heart rate was determined by temporary pacing in 10 patients. Left atrial pressure comparisons were limited to 17 patients in each group because 6 patients did not have a catheter placed in the left atrium. Matching sets of systemic and pulmonary arterial blood gas measurements were inadvertently not performed in all patients at baseline and after 1 hour of observation. However, there was no significant change in the difference between systemic and pulmonary arterial oxygen saturations for 11 patients in the control group or 15 patients in the group of patients who received inhaled nitric oxide. Patients with and without radiographic evidence of lung disease before operation had similar baseline hemodynamic and blood gas measurements. The presence of lung disease also had no significant effect on these measurements after 1 hour of observation. However, there was a significantly greater increase in the ratio of arterial oxygen tension and fraction of inspired oxygen in patients without lung disease than in patients with lung disease who were treated with inhaled nitric oxide (68 20 mm Hg versus 13 8mmHg,p 0.012). Pulmonary Hypertensive Crises During Sustained Therapy Pulmonary hypertensive crises occurred in 4 control patients and in 3 patients who were treated with inhaled nitric oxide. The characteristics of these patients are listed in Table 4. A life-threatening episode of pulmonary hypertension occurred in 1 control patient. This episode was refractory to hyperventilation with 100% oxygen, sedation, and neuromuscular blockade. However, when treated with inhaled nitric oxide, a marked increase in the ratio of arterial oxygen tension and fraction of inspired oxygen (136 to 240 mm Hg), and a 47% reduction in the ratio of systolic pulmonary and systemic arterial pressures occurred. In other patients, the crises were less severe. Using a power analysis for contingency tables, more than 2,000 patients may be needed to determine whether nitric oxide decreases the incidence of pulmonary hypertensive crises with a power (1- ) more than The acute hemodynamic and blood gas effects of inhaled nitric oxide in the 4 control patients who experienced a pulmonary hypertensive crisis are listed in Table 5. In each patient, the pulmonary hemodynamics or oxygenation improved. The patient with branch pulmonary artery stenosis even developed an increase in the ratio of arterial oxygen tension and fraction of inspired oxygen (142 to 208 mm Hg) and a 20% reduction in the ratio of systolic pulmonary and systemic arterial pressures when treated with inhaled nitric oxide. No additional patient with anatomic obstruction experienced a pulmonary hypertensive crisis. None of the control patients experienced a pulmonary hypertensive crisis after being treated with inhaled nitric oxide. None of the patients who were initially randomized to the nitric oxide group experienced a subsequent pulmonary hypertensive crisis when neuromuscular blockade and sedation were gradually decreased over a period of 4 to 6 days. Table 5. Acute Hemodynamic and Blood Gas Measurements of the Four Control Patients Who Were Treated With Inhaled Nitric Oxide After Experiencing a Pulmonary Hypertensive Crisis Variables Baseline After Pulmonary Hypertensive Crisis Nitric Oxide (1 hour) Heart rate (min 1 ) a Systolic pulmonary pressure a Systolic systemic pressure Right atrial pressure Left atrial pressure ph PaCO PaO 2 /FIO a PaCO 2 arterial carbon dioxide tension; PaO 2 /FIO 2 ratio between the arterial oxygen tension and the fraction of inspired oxygen. a p 0.05 versus baseline.
5 Ann Thorac Surg DAY ET AL 2000;69: POSTOPERATIVE INHALED NITRIC OXIDE 1911 The patients who experienced a pulmonary hypertensive crisis had similar baseline hemodynamic and blood gas measurements in comparison to the patients who did not experience a pulmonary hypertensive crisis. However, there was a tendency for these patients to have increased baseline differences between systemic and pulmonary arterial oxygen saturations (43% 2% versus 32% 2%, p 0.062). Five patients with and 2 patients without preoperative lung disease experienced pulmonary hypertensive crises. One of the 4 patients with lung disease who experienced a pulmonary hypertensive crises was being treated with inhaled nitric oxide. Patients who experienced a pulmonary hypertensive crisis required an increased duration of paralysis ( days versus days, p 0.007). They did not require a significantly increased duration of assisted ventilation ( days versus days) or inotropic support ( days versus days). If the patients who experienced a pulmonary hypertensive crisis were excluded from statistical analysis, control patients and patients who received inhaled nitric oxide required a similar duration of paralysis ( days versus days), assisted ventilation ( days versus days), and inotropic support ( days versus days). Maximum methemoglobin values were slightly increased in patients who were treated with inhaled nitric oxide (1.4% 0.1% versus 1.1% 0.1%, p 0.023). There were no known complications or adverse effects associated with nitric oxide inhalation or the gradual withdrawal of nitric oxide before extubation. All patients completed the study and were weaned from assisted ventilation. Comment In this study, nitric oxide did not acutely improve pulmonary hemodynamics and arterial blood gases in comparison to conventional therapy. Nitric oxide also failed to significantly decrease the incidence of pulmonary hypertensive crises. This study is clearly limited by its size; however, it provides an estimate of the number of patients needed to exclude, with greater power, the possibility that inhaled nitric oxide prevents clinically significant pulmonary hypertensive crises after operation for congenital heart disease. Patients Only patients with relatively high pulmonary arterial pressures were enrolled in this study. All patients underwent a biventricular repair or heart transplantation. We may have failed to identify all patients with a systolic pulmonary arterial pressure of 50% or more of the systolic systemic pressure, and some patients with an initially low pulmonary arterial pressure may have developed a subsequent increase in pressure that was not monitored. Thus, we can only speculate that the majority of eligible patients were included in this study. Our patient groups were reasonably well matched with respect to diagnosis, drug therapy, and baseline hemodynamic and blood gas measurements. The groups were also managed similarly with respect to the duration of neuromuscular blockade, inotropic support, and assisted ventilation. Patients with anatomic obstruction in the pulmonary circulation were not excluded to report our complete results. Adatia and associates [15] have reported that these patients may not respond to inhaled nitric oxide. However, anatomic obstruction may be associated with an element of pulmonary vasoconstriction that is responsive to therapy, particularly if the obstruction is not severe bilaterally. Only 1 patient with residual anatomic obstruction experienced a pulmonary hypertensive crisis. The criteria for patient selection may have influenced the outcome of our study. Additional studies will need to determine whether the acute and sustained effects of inhaled nitric oxide are more pronounced in patient groups defined by higher pulmonary arterial pressure, lung disease, or systolic right ventricular dysfunction. Acute Hemodynamic and Blood Gas Measurements Our study supports previous claims that nitric oxide acutely causes significant hemodynamic and blood gas improvements in comparison to baseline measurements. Unfortunately, none of our acute measurements in treated patients improved significantly in comparison to controls. It is possible that a larger study may identify a statistically significant difference in hemodynamic and blood gas measurements. However, our study indicates with a power (1- ) more than 0.75 that it is unlikely for an acute improvement in pulmonary hemodynamics to exceed 20% in comparison to controls. Thus, nitric oxide may not improve pulmonary hemodynamics enough to justify therapy for all patients with a postoperative pulmonary arterial pressure of 50% or more of the systemic arterial pressure. Inhaled nitric oxide has decreased the pulmonary vascular resistance of patients with congenital heart disease during heart catheterization [6, 7]. Nitric oxide has also decreased mean pulmonary arterial pressure in comparison to conventional therapy when additional vasodilatory agents were not being used during a 20- minute period after repair of congenital heart disease [17]. Russell and associates [17] used different statistical methods; however, it is also possible that a significant decrease in pulmonary arterial pressure was not observed in our study because an intravenous nitric oxide donor was being used for systemic afterload reduction in the majority of patients. Pulmonary Hypertensive Crises During Sustained Therapy Pulmonary hypertensive crises occurred in both patient groups. Our results suggest that a very large study will be required to definitely exclude a benefit from sustained therapy. A larger study will also be needed to determine whether lung disease is a predisposing factor for pulmonary hypertensive crises. Our study is being closed because several institutions will need to collaborate to enroll an adequate number of patients to address these questions.
6 1912 DAY ET AL Ann Thorac Surg POSTOPERATIVE INHALED NITRIC OXIDE 2000;69: In contrast to our findings, a preliminary report of a case-control study [18] indicates that inhaled nitric oxide does decrease the incidence of pulmonary hypertensive crises after operation for congenital heart disease. This study will need to be evaluated in greater detail to determine whether the postoperative care and clinical characteristics of patients were similar in each group. It is possible that no crisis would have occurred in our treated patients if neuromuscular blockade or an increased level of pain management and sedation were used in all patients throughout the initial postoperative day. Our ability to identify a potential benefit from sustained therapy may have been improved by enforcing uniform standards for all aspects of conventional therapy. However, we agreed with our research committee that it would not be appropriate to impose restrictions on the judgment of care providers during a potential period of several days. Our findings may reflect the actual efficacy of sustained nitric oxide therapy in a true clinical setting where rigid strategies of assisted ventilation and drug therapy would not be enforced. We did not attempt to grade the severity of pulmonary hypertensive crises. In 1 control patient, however, an episode was refractory to conventional therapy and death appeared inevitable until the onset of nitric oxide inhalation. Goldman and associates [14] have reported that nitric oxide may reduce the need for extracorporeal support in children with critical postoperative pulmonary hypertension. We agree that a trial of nitric oxide may be justified in patients who experience a pulmonary hypertensive crisis. Nitric oxide did not have a significant impact on the duration of neuromuscular blockade, assisted ventilation, or inotropic support in patients whose postoperative course was not complicated by a pulmonary hypertensive crisis. In conclusion, nitric oxide did not substantially improve pulmonary hemodynamics and gas exchange after operation for congenital heart disease. It also failed to significantly decrease the incidence of pulmonary hypertensive crises. Nitric oxide may have a role in the treatment of severe pulmonary hypertension; however, at this time there is no evidence that a specific outcome will be improved by empirically treating all patients who have increased pulmonary arterial pressure after operation. We thank each member of the Department of Respiratory Care Services at Primary Children s Medical Center who assisted in the delivery of inhaled nitric oxide. References 1. Hopkins RA, Bull C, Haworth SG, de Leval MR, Stark J. Pulmonary hypertensive crises following surgery for congenital heart defects in young children. Eur J Cardiothorac Surg 1991;5: Murali S, Kormos RL, Uretsky BF, et al. Preoperative pulmonary hemodynamics and early mortality after orthotopic cardiac transplantation: the Pittsburg experience. Am Heart J 1993;126: Dinh Xuan AT, Higenbottam TW, Clelland C, Pepke-Zaba J, Cremona G, Wallwork J. Impairment of pulmonary endothelium-dependent relaxation in patients with Eisenmenger s syndrome. Br J Pharmacol 1989;99: Celermajer DS, Cullen S, Deanfield JE. Impairment of endothelium-dependent pulmonary artery relaxation in children with congenital heart disease and abnormal pulmonary hemodynamics. Circulation 1993;87: Wessel DL, Adatia I, Giglia TM, Thompson JE, Kulik TJ. Use of inhaled nitric oxide and acetylcholine in the evaluation of pulmonary hypertension and endothelial function after cardiopulmonary bypass. Circulation 1993;88(Suppl 1): Roberts JD, Lang P, Bigatello LM, Vlahakes GJ, Zapol WM. Inhaled nitric oxide in congenital heart disease. Circulation 1993;87: Day RW, Lynch JM, Shaddy RE, Orsmond GS. Pulmonary vasodilatory effects of 12 and 60 parts per million inhaled nitric oxide in children with ventricular septal defect. Am J Cardiol 1995;75: Schranz D, Huth R, Wippermann CF, Ritzerfeld S, Schmitt FX, Oelert H. Nitric oxide and prostacyclin lower suprasystemic pulmonary hypertension after cardiopulmonary bypass. Eur J Pediatr 1993;152: Snow DJ, Gray SJ, Ghosh S, et al. Inhaled nitric oxide in patients with normal and increased pulmonary vascular resistance after cardiac surgery. Br J Anaesth 1994;72: Journois D, Pouard P, Mauriat P, Malhère T, Vouhé P, Safran D. Inhaled nitric oxide as a therapy for pulmonary hypertension after operations for congenital heart defects. J Thorac Cardiovasc Surg 1994;107: Miller OI, Celermajer DS, Deanfield JE, Macrae DJ. Very low-dose inhaled nitric oxide: a selective pulmonary vasodilator after operations for congenital heart disease. J Thorac Cardiovasc Surg 1994;108: Beghetti M, Habre W, Friedli B, Berner M. Continuous low dose inhaled nitric oxide for treatment of severe pulmonary hypertension after cardiac surgery in paediatric patients. Br Heart J 1995;73: Curran RD, Mavroudis C, Backer CL, Sautel M, Zales VR, Wessel DL. Inhaled nitric oxide for children with congenital heart disease and pulmonary hypertension. Ann Thorac Surg 1995;60: Goldman AP, Delius RE, Deanfield JE, de Leval MR, Sigston PE, Macrae DJ. Nitric oxide might reduce the need for extracorporeal support in children with critical postoperative pulmonary hypertension. Ann Thorac Surg 1996;62: Adatia I, Atz AM, Jonas RA, Wessel DL. Diagnostic use of inhaled nitric oxide after neonatal cardiac operations. J Thorac Cardiovasc Surg 1996;112: Schulze-Neick I, Bültmann M, Werner H, et al. Right ventricular function in patients treated with inhaled nitric oxide after cardiac surgery for congenital heart disease in newborns and children. Am J Cardiol 1997;80: Russell IAM, Zwass MS, Fineman JR, et al. The effects of inhaled nitric oxide on postoperative pulmonary hypertension in infants and children undergoing surgical repair of congenital heart disease. Anesth Analg 1998;87: Breuer J, Prein W, Gebhardt S, Sieverding L, Apitz J. Reduction of pulmonary hypertensive crises by inhaled NO in children after cardiac bypass surgery [Abstract]. Cardiol Young 1998;9(Suppl 1): Day RW, Guarín M, Lynch JM, Vernon DD, Dean JM. Inhaled nitric oxide in children with severe lung disease: results of acute and prolonged therapy with two concentrations. Crit Care Med 1996;24: Kirmse M, Hess D, Fujino Y, Kacmarek RM, Hurford WE. Delivery of inhaled nitric oxide using the Ohmeda INOvent Delivery System. Chest 1998;113: Cueto E, Lopéz-Herce J, Sánchez A, Carrillo A. Lifethreatening effects of discontinuing inhaled nitric oxide in children. Acta Paediatr 1997;86:
Inhaled Nitric Oxide Beyond the Evidence- Children
 Critical Care Canada Forum, Toronto 2014 Inhaled Nitric Oxide Beyond the Evidence- Children Ian Adatia, Pediatric Pulmonary Hypertension Service and Cardiac Intensive Care Unit, Stollery Children s Hospital,
Critical Care Canada Forum, Toronto 2014 Inhaled Nitric Oxide Beyond the Evidence- Children Ian Adatia, Pediatric Pulmonary Hypertension Service and Cardiac Intensive Care Unit, Stollery Children s Hospital,
DIPYRIDAMOLE ATTENUATES REBOUND PULMONARY HYPERTENSION AFTER INHALED NITRIC OXIDE WITHDRAWAL IN POSTOPERATIVE CONGENITAL HEART DISEASE
 DIPYRIDAMOLE ATTENUATES REBOUND PULMONARY HYPERTENSION AFTER INHALED NITRIC OXIDE WITHDRAWAL IN POSTOPERATIVE CONGENITAL HEART DISEASE D. Dunbar Ivy, MD a John P. Kinsella, MD b James W. Ziegler, MD d
DIPYRIDAMOLE ATTENUATES REBOUND PULMONARY HYPERTENSION AFTER INHALED NITRIC OXIDE WITHDRAWAL IN POSTOPERATIVE CONGENITAL HEART DISEASE D. Dunbar Ivy, MD a John P. Kinsella, MD b James W. Ziegler, MD d
ino in neonates with cardiac disorders
 ino in neonates with cardiac disorders Duncan Macrae Paediatric Critical Care Terminology PAP Pulmonary artery pressure PVR Pulmonary vascular resistance PHT Pulmonary hypertension - PAP > 25, PVR >3,
ino in neonates with cardiac disorders Duncan Macrae Paediatric Critical Care Terminology PAP Pulmonary artery pressure PVR Pulmonary vascular resistance PHT Pulmonary hypertension - PAP > 25, PVR >3,
SCVMC RESPIRATORY CARE PROCEDURE
 Page 1 of 7 New: 12/08 R: 4/11 R NC: 7/11, 7/12 B7180-63 Definitions: Inhaled nitric oxide (i) is a medical gas with selective pulmonary vasodilator properties. Vaso-reactivity is the evidence of acute
Page 1 of 7 New: 12/08 R: 4/11 R NC: 7/11, 7/12 B7180-63 Definitions: Inhaled nitric oxide (i) is a medical gas with selective pulmonary vasodilator properties. Vaso-reactivity is the evidence of acute
Inhaled Nitric Oxide for Children With Congenital Heart Disease and Pulmonary Hypertension
 Inhaled Nitric Oxide for Children With Congenital Heart Disease and Pulmonary Hypertension Ronald D. Curran, MD, Constantine Mavroudis, MD, Carl L. Backer, MD, Michael Sautel, BS, Vincent R. Zales, MD,
Inhaled Nitric Oxide for Children With Congenital Heart Disease and Pulmonary Hypertension Ronald D. Curran, MD, Constantine Mavroudis, MD, Carl L. Backer, MD, Michael Sautel, BS, Vincent R. Zales, MD,
In newborns with a functional single ventricle and
 Pulmonary Vascular Resistance of Children Treated With Nitrogen During Early Infancy Ronald W. Day, MD, Alan J. Barton, MD, Theodore J. Pysher, MD, and Robert E. Shaddy, MD Division of Pediatric Cardiology,
Pulmonary Vascular Resistance of Children Treated With Nitrogen During Early Infancy Ronald W. Day, MD, Alan J. Barton, MD, Theodore J. Pysher, MD, and Robert E. Shaddy, MD Division of Pediatric Cardiology,
Beneficial Effects of Inhaled Nitric Oxide in Adult Cardiac Surgical Patients
 Beneficial Effects of Inhaled Nitric Oxide in Adult Cardiac Surgical Patients Thomas S. Maxey, MD, Christopher D. Smith, MBBS, FRACS, John A. Kern, MD, Curtis G. Tribble, MD, David R. Jones, MD, Irving
Beneficial Effects of Inhaled Nitric Oxide in Adult Cardiac Surgical Patients Thomas S. Maxey, MD, Christopher D. Smith, MBBS, FRACS, John A. Kern, MD, Curtis G. Tribble, MD, David R. Jones, MD, Irving
USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014
 USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014 ino for Late Preterm and Term Infants with Severe PPHN Background:
USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014 ino for Late Preterm and Term Infants with Severe PPHN Background:
Perioperative Management of DORV Case
 Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Policy Specific Section: May 16, 1984 April 9, 2014
 Medical Policy Heart Transplant Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Transplant Original Policy Date: Effective Date: May 16, 1984 April 9, 2014 Definitions
Medical Policy Heart Transplant Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Transplant Original Policy Date: Effective Date: May 16, 1984 April 9, 2014 Definitions
Pulmonary Vasodilator Treatments in the ICU Setting
 Pulmonary Vasodilator Treatments in the ICU Setting Lara Shekerdemian Circulation 1979 Ann Thorac Surg 27 Anesth Analg 211 1 Factors in the ICU Management of Pulmonary Hypertension After Cardiopulmonary
Pulmonary Vasodilator Treatments in the ICU Setting Lara Shekerdemian Circulation 1979 Ann Thorac Surg 27 Anesth Analg 211 1 Factors in the ICU Management of Pulmonary Hypertension After Cardiopulmonary
Heart-lung transplantation: adult indications and outcomes
 Brief Report Heart-lung transplantation: adult indications and outcomes Yoshiya Toyoda, Yasuhiro Toyoda 2 Temple University, USA; 2 University of Pittsburgh, USA Correspondence to: Yoshiya Toyoda, MD,
Brief Report Heart-lung transplantation: adult indications and outcomes Yoshiya Toyoda, Yasuhiro Toyoda 2 Temple University, USA; 2 University of Pittsburgh, USA Correspondence to: Yoshiya Toyoda, MD,
Surgical Approaches to Advanced Pulmonary Vascular Disease. Historical Perspectives. Historical Perspectives
 5 th International Conference Neonatal and Childhood Pulmonary Vascular Disease, San Francisco, March 9-10, 2012 Surgical Approaches to Advanced Pulmonary Vascular Disease William M. Novick, M.D., M.S.
5 th International Conference Neonatal and Childhood Pulmonary Vascular Disease, San Francisco, March 9-10, 2012 Surgical Approaches to Advanced Pulmonary Vascular Disease William M. Novick, M.D., M.S.
Curricular Components for Cardiology EPA
 Curricular Components for Cardiology EPA 1. EPA Title 2. Description of the Activity Diagnosis and management of patients with acute congenital or acquired cardiac problems requiring intensive care. Upon
Curricular Components for Cardiology EPA 1. EPA Title 2. Description of the Activity Diagnosis and management of patients with acute congenital or acquired cardiac problems requiring intensive care. Upon
Extracorporeal Membrane Oxygenation (ECMO)
 Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/01/2014 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/01/2014 Section: Other/Miscellaneous
Does troponin-i measurement predict low cardiac output syndrome following cardiac surgery in children?
 Does troponin-i measurement predict low cardiac output syndrome following cardiac surgery in children? Norbert R Froese, Suvro S Sett, Thomas Mock and Gordon E Krahn Low cardiac output syndrome (LCOS)
Does troponin-i measurement predict low cardiac output syndrome following cardiac surgery in children? Norbert R Froese, Suvro S Sett, Thomas Mock and Gordon E Krahn Low cardiac output syndrome (LCOS)
Surgery for Congenital Heart Disease. How common is severe pulmonary hypertension after pediatric cardiac surgery?
 How common is severe pulmonary hypertension after pediatric cardiac surgery? L. Lindberg, MD, PhD A. K. Olsson, MD, PhD P. Jögi, MD C. Jonmarker, MD, PhD Background: Pulmonary hypertension may result in
How common is severe pulmonary hypertension after pediatric cardiac surgery? L. Lindberg, MD, PhD A. K. Olsson, MD, PhD P. Jögi, MD C. Jonmarker, MD, PhD Background: Pulmonary hypertension may result in
The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients
 The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
Cardiorespiratory Interactions:
 Cardiorespiratory Interactions: The Heart - Lung Connection Jon N. Meliones, MD, MS, FCCM Professor of Pediatrics Duke University Medical Director PCVICU Optimizing CRI Cardiorespiratory Economics O2:
Cardiorespiratory Interactions: The Heart - Lung Connection Jon N. Meliones, MD, MS, FCCM Professor of Pediatrics Duke University Medical Director PCVICU Optimizing CRI Cardiorespiratory Economics O2:
PPHN (see also ECMO guideline)
 Children s Acute Transport Service Clinical Guidelines PPHN (see also ECMO guideline) Document Control Information Author P Brooke E.Randle Author Position Medical Student Consultant Document Owner E.
Children s Acute Transport Service Clinical Guidelines PPHN (see also ECMO guideline) Document Control Information Author P Brooke E.Randle Author Position Medical Student Consultant Document Owner E.
The Journal of Thoracic and Cardiovascular Surgery
 Accepted Manuscript Dream Big in Every Small Step Lok Sinha, MD, Can Yerebakan, MD PII: S0022-5223(19)30013-3 DOI: https://doi.org/10.1016/j.jtcvs.2018.12.086 Reference: YMTC 13988 To appear in: The Journal
Accepted Manuscript Dream Big in Every Small Step Lok Sinha, MD, Can Yerebakan, MD PII: S0022-5223(19)30013-3 DOI: https://doi.org/10.1016/j.jtcvs.2018.12.086 Reference: YMTC 13988 To appear in: The Journal
Mechanical Ventilation & Cardiopulmonary Interactions: Clinical Application in Non- Conventional Circulations. Eric M. Graham, MD
 Mechanical Ventilation & Cardiopulmonary Interactions: Clinical Application in Non- Conventional Circulations Eric M. Graham, MD Background Heart & lungs work to meet oxygen demands Imbalance between supply
Mechanical Ventilation & Cardiopulmonary Interactions: Clinical Application in Non- Conventional Circulations Eric M. Graham, MD Background Heart & lungs work to meet oxygen demands Imbalance between supply
Surgical Repair of Transposition of the Great Arteries in Neonates With Persistent Pulmonary Hypertension
 Surgical Repair of Transposition of the Great Arteries in Neonates With Persistent Pulmonary Hypertension Giovanni Battista Luciani, MD, Anthony C. Chang, MD, and Vaughn A. Starnes, MD Divisions of Cardiothoracic
Surgical Repair of Transposition of the Great Arteries in Neonates With Persistent Pulmonary Hypertension Giovanni Battista Luciani, MD, Anthony C. Chang, MD, and Vaughn A. Starnes, MD Divisions of Cardiothoracic
Randomized, Double-Blind Trial of Inhaled Nitric Oxide in LVAD Recipients With Pulmonary Hypertension
 ORIGINAL ARTICLES: CARDIOVASCULAR Randomized, Double-Blind Trial of Inhaled Nitric Oxide in LVAD Recipients With Pulmonary Hypertension Michael Argenziano, MD, Asim F. Choudhri, BS, Nader Moazami, MD,
ORIGINAL ARTICLES: CARDIOVASCULAR Randomized, Double-Blind Trial of Inhaled Nitric Oxide in LVAD Recipients With Pulmonary Hypertension Michael Argenziano, MD, Asim F. Choudhri, BS, Nader Moazami, MD,
A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution
 Original Article A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution Ghassan Baslaim, MD, and Jill Bashore, RN Purpose: Adult patients with congenital
Original Article A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution Ghassan Baslaim, MD, and Jill Bashore, RN Purpose: Adult patients with congenital
Guideline for the Use of inhaled Nitric Oxide (NO) Catarina Silvestre Prof. Harish Vyas
 Inhaled Nitric Oxide Title of Guideline Guideline for the Use of inhaled Nitric Oxide (NO) 1a 2a 2b Contact Name and Job Title (author) Directorate & Speciality Date of submission October 2015 Date when
Inhaled Nitric Oxide Title of Guideline Guideline for the Use of inhaled Nitric Oxide (NO) 1a 2a 2b Contact Name and Job Title (author) Directorate & Speciality Date of submission October 2015 Date when
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Surgical Treatment for Atrioventricular Septal Defect. Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery
 Surgical Treatment for Atrioventricular Septal Defect Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Rastelli classification (Rastelli) Pulmonary artery banding (Muller & Dammann)
Surgical Treatment for Atrioventricular Septal Defect Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Rastelli classification (Rastelli) Pulmonary artery banding (Muller & Dammann)
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Perioperative Management of TAPVC
 Perioperative Management of TAPVC Professor Andrew Wolf Rush University Medical Center,Chicago USA Bristol Royal Children s Hospital UK I have no financial disclosures relevant to this presentation TAPVC
Perioperative Management of TAPVC Professor Andrew Wolf Rush University Medical Center,Chicago USA Bristol Royal Children s Hospital UK I have no financial disclosures relevant to this presentation TAPVC
Extracorporeal Membrane Oxygenation (ECMO)
 Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2017 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2017 Section: Other/Miscellaneous
Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia
 Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Congenital pulmonary vein (PV) stenosis with anatomically
 Pulmonary Vein Stenosis With Normal Connection: Associated Cardiac Abnormalities and Variable Outcome John P. Breinholt, BS, John A. Hawkins, MD, LuAnn Minich, MD, Lloyd Y. Tani, MD, Garth S. Orsmond,
Pulmonary Vein Stenosis With Normal Connection: Associated Cardiac Abnormalities and Variable Outcome John P. Breinholt, BS, John A. Hawkins, MD, LuAnn Minich, MD, Lloyd Y. Tani, MD, Garth S. Orsmond,
APPROACH TO THE ICCU PATIENT WITH PULMONARY HYPERTENSION
 APPROACH TO THE ICCU PATIENT WITH PULMONARY HYPERTENSION Rafael Hirsch, Adult Congenital Heart Unit Dept. of Cardiology Rabin Medical Center Beilinson Campus & Tel Aviv University Sackler School of Medicine,
APPROACH TO THE ICCU PATIENT WITH PULMONARY HYPERTENSION Rafael Hirsch, Adult Congenital Heart Unit Dept. of Cardiology Rabin Medical Center Beilinson Campus & Tel Aviv University Sackler School of Medicine,
PULMONARY HYPERTENSION AFTER OPERATIONS FOR CONGENITAL HEART DISEASE: ANALYSIS OF RISK FACTORS AND MANAGEMENT
 PULMONARY HYPERTENSION AFTER OPERATIONS FOR CONGENITAL HEART DISEASE: ANALYSIS OF RISK FACTORS AND MANAGEMENT Ko Bando, MD Mark W. Turrentine, MD Thomas G. Sharp, MD Yasuo Sekine, MD Thomas X. Aufiero,
PULMONARY HYPERTENSION AFTER OPERATIONS FOR CONGENITAL HEART DISEASE: ANALYSIS OF RISK FACTORS AND MANAGEMENT Ko Bando, MD Mark W. Turrentine, MD Thomas G. Sharp, MD Yasuo Sekine, MD Thomas X. Aufiero,
PFIZER INC. Study Center(s): A total of 6 centers took part in the study, including 2 in France and 4 in the United States.
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Post-Cardiac Surgery Evaluation
 Post-Cardiac Surgery Evaluation 20th Annual Heart Conference October 15, 2016 Gary A Mayman PROFESSOR PEDIATRICS UNIVERSITY OF NEVADA Look Touch Listen Temperature, pulse, respiratory rate, & blood pressure
Post-Cardiac Surgery Evaluation 20th Annual Heart Conference October 15, 2016 Gary A Mayman PROFESSOR PEDIATRICS UNIVERSITY OF NEVADA Look Touch Listen Temperature, pulse, respiratory rate, & blood pressure
Inhaled epoprostenol vs inhaled nitric oxide for refractory hypoxemia in critically ill patients
 Journal of Critical Care (2013) 28, 844 848 Inhaled epoprostenol vs inhaled nitric oxide for refractory hypoxemia in critically ill patients Heather Torbic PharmD, BCPS a,, Paul M. Szumita PharmD, BCPS
Journal of Critical Care (2013) 28, 844 848 Inhaled epoprostenol vs inhaled nitric oxide for refractory hypoxemia in critically ill patients Heather Torbic PharmD, BCPS a,, Paul M. Szumita PharmD, BCPS
Deok Young Choi, Gil Hospital, Gachon University NEONATES WITH EBSTEIN S ANOMALY: PROBLEMS AND SOLUTION
 Deok Young Choi, Gil Hospital, Gachon University NEONATES WITH EBSTEIN S ANOMALY: PROBLEMS AND SOLUTION Carpentier classification Chauvaud S, Carpentier A. Multimedia Manual of Cardiothoracic Surgery 2007
Deok Young Choi, Gil Hospital, Gachon University NEONATES WITH EBSTEIN S ANOMALY: PROBLEMS AND SOLUTION Carpentier classification Chauvaud S, Carpentier A. Multimedia Manual of Cardiothoracic Surgery 2007
PULMONARY ARTERY HYPERTENSION (PAH) leading
 Inhaled Nitroglycerin Versus Inhaled Milrinone in Children with Congenital Heart Disease Suffering from Pulmonary Artery Hypertension Raveen Singh, MD,* Minati Choudhury, MD,* Anita Saxena, DM, Poonam
Inhaled Nitroglycerin Versus Inhaled Milrinone in Children with Congenital Heart Disease Suffering from Pulmonary Artery Hypertension Raveen Singh, MD,* Minati Choudhury, MD,* Anita Saxena, DM, Poonam
Original/Research Articles Analysis of Severe Pulmonary Hypertension
 Reced. : 24.11.09 Taken from CD. 10bhjj03 3rd proof Original/Research Articles Analysis of Severe Pulmonary Hypertension Shilpa Rao*, Manjula Sarkar**, Sarla Pandya*** Abstract Pulmonary hypertension may
Reced. : 24.11.09 Taken from CD. 10bhjj03 3rd proof Original/Research Articles Analysis of Severe Pulmonary Hypertension Shilpa Rao*, Manjula Sarkar**, Sarla Pandya*** Abstract Pulmonary hypertension may
INHALED NITRIC OXIDE AND PERSISTENT PULMONARY HYPERTENSION OF THE NEWBORN INHALED NITRIC OXIDE AND PERSISTENT PULMONARY HYPERTENSION OF THE NEWBORN
 INHALED NITRIC OXIDE AND PERSISTENT PULMONARY HYPERTENSION OF THE NEWBORN INHALED NITRIC OXIDE AND PERSISTENT PULMONARY HYPERTENSION OF THE NEWBORN JESSE D. ROBERTS, JR., M.D., JEFFREY R. FINEMAN, M.D.,
INHALED NITRIC OXIDE AND PERSISTENT PULMONARY HYPERTENSION OF THE NEWBORN INHALED NITRIC OXIDE AND PERSISTENT PULMONARY HYPERTENSION OF THE NEWBORN JESSE D. ROBERTS, JR., M.D., JEFFREY R. FINEMAN, M.D.,
Clinical Policy: Inhaled Nitric Oxide Reference Number: CP.MP.87
 Clinical Policy: Reference Number: CP.MP.87 Last Review Date: 09/17 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description (ino) is a
Clinical Policy: Reference Number: CP.MP.87 Last Review Date: 09/17 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description (ino) is a
Inhaled nitric oxide as a therapy for pulmonary hypertension after operations for congenital heart defects
 Inhaled nitric oxide as a therapy for pulmonary hypertension after operations for congenital heart defects Seventeen infants were treated with inhaled nitric oxide for critical pulmonary artery hypertension
Inhaled nitric oxide as a therapy for pulmonary hypertension after operations for congenital heart defects Seventeen infants were treated with inhaled nitric oxide for critical pulmonary artery hypertension
Keep. with life MEDICATION TECHNOLOGY SERVICES INSPIRED BY YOUR NEEDS
 Keep with life MEDICATION TECHNOLOGY SERVICES INSPIRED BY YOUR NEEDS 2 KINOX MEDICATION KINOX, inhaled nitric oxide, is a selective pulmonary vasodilator developed by Air Liquide Healthcare and characterized
Keep with life MEDICATION TECHNOLOGY SERVICES INSPIRED BY YOUR NEEDS 2 KINOX MEDICATION KINOX, inhaled nitric oxide, is a selective pulmonary vasodilator developed by Air Liquide Healthcare and characterized
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum
 Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Neal D. Hillman, MD a Ira M. Cheifetz, MD b Damian M. Craig, MS a Peter K. Smith, MD = Ross M. Ungerleider, MD a Jon N. Meliones, MD, FCCM b
 INHALED NITRIC OXIDE, RIGHT VENTRICULAR EFFICIENCY, AND PULMONARY VASCULAR MECHANICS: SELECTIVE VASODILATION OF SMALL PULMONARY VESSELS DURING HYPOXIC PULMONARY VASOCONSTRICTION Neal D. Hillman, MD a Ira
INHALED NITRIC OXIDE, RIGHT VENTRICULAR EFFICIENCY, AND PULMONARY VASCULAR MECHANICS: SELECTIVE VASODILATION OF SMALL PULMONARY VESSELS DURING HYPOXIC PULMONARY VASOCONSTRICTION Neal D. Hillman, MD a Ira
The Blue Baby. Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin
 The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
CongHeartDis.doc. Андрій Миколайович Лобода
 CongHeartDis.doc Андрій Миколайович Лобода 2015 Зміст 3 Зміст Зміст 4 A child with tetralogy of Fallot is most likely to exhibit: -Increased pulmonary blood flow -Increased pressure in the right ventricle
CongHeartDis.doc Андрій Миколайович Лобода 2015 Зміст 3 Зміст Зміст 4 A child with tetralogy of Fallot is most likely to exhibit: -Increased pulmonary blood flow -Increased pressure in the right ventricle
Cardiovascular Institute
 Allegheny Health Network Cardiovascular Institute Extracorporeal Membrane Oxygenation (ECMO) Program Our patient survival rate is higher than the national average. ECMO experts. Multidisciplinary team.
Allegheny Health Network Cardiovascular Institute Extracorporeal Membrane Oxygenation (ECMO) Program Our patient survival rate is higher than the national average. ECMO experts. Multidisciplinary team.
CARDIOVASCULAR SURGERY
 Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
Case Report. Stent Placement in a Neonate with Sano Modification of the Norwood using Semi-Elective Extracorporeal Membrane Oxygenation.
 Stent Placement in a Neonate with Sano Modification of the Norwood using Semi-Elective Extracorporeal Membrane Oxygenation Mustafa Gulgun and Michael Slack Associated Profesor Children National Medical
Stent Placement in a Neonate with Sano Modification of the Norwood using Semi-Elective Extracorporeal Membrane Oxygenation Mustafa Gulgun and Michael Slack Associated Profesor Children National Medical
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
3/13/2009. Disclosures. Novel Perioperative Therapies. Rick Barr, MD MSCI Vanderbilt Children s Hospital March 13, 2009
 1 Disclosures 2 Novel Perioperative Therapies Rick Barr, MD MSCI Children s Hospital March 13, 29 has filed for patents and licensed citrulline as a therapeutic agent with Asklepion Pharmaceuticals Dr.
1 Disclosures 2 Novel Perioperative Therapies Rick Barr, MD MSCI Children s Hospital March 13, 29 has filed for patents and licensed citrulline as a therapeutic agent with Asklepion Pharmaceuticals Dr.
Oral sildenafil for persistent pulmonary hypertension early after congenital cardiac surgery in children
 European Journal of Cardio-thoracic Surgery 38 (2010) 71 77 www.elsevier.com/locate/ejcts Oral sildenafil for persistent pulmonary hypertension early after congenital cardiac surgery in children Shintaro
European Journal of Cardio-thoracic Surgery 38 (2010) 71 77 www.elsevier.com/locate/ejcts Oral sildenafil for persistent pulmonary hypertension early after congenital cardiac surgery in children Shintaro
PREOPERATIVE CARDIOPULMONARY ASSESSMENT FOR LIVER TRANSPLANTATION James Y. Findlay Mayo Clinic College of Medicine, Rochester, MN, USA.
 PREOPERATIVE CARDIOPULMONARY ASSESSMENT FOR LIVER TRANSPLANTATION James Y. Findlay Mayo Clinic College of Medicine, Rochester, MN, USA Introduction Liver transplantation (LT) has gone from being a high-risk
PREOPERATIVE CARDIOPULMONARY ASSESSMENT FOR LIVER TRANSPLANTATION James Y. Findlay Mayo Clinic College of Medicine, Rochester, MN, USA Introduction Liver transplantation (LT) has gone from being a high-risk
Techniques for repair of complete atrioventricular septal
 No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
Pulmonary hypertension and right ventricular failure
 Pulmonary hypertension and right ventricular failure Sven-Erik Ricksten Dept. Anaesthesiology and Intensive Care, Sahlgrenska Academy, University of Gothenburg, Sahlgrenska University Hospital, Gothenburg,
Pulmonary hypertension and right ventricular failure Sven-Erik Ricksten Dept. Anaesthesiology and Intensive Care, Sahlgrenska Academy, University of Gothenburg, Sahlgrenska University Hospital, Gothenburg,
Surgical Management of TOF in Adults. Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital
 Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Heart Transplantation in Patients with Superior Vena Cava to Pulmonary Artery Anastomosis: A Single-Institution Experience
 Korean J Thorac Cardiovasc Surg 2018;51:167-171 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2018.51.3.167 Heart Transplantation in Patients with Superior
Korean J Thorac Cardiovasc Surg 2018;51:167-171 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2018.51.3.167 Heart Transplantation in Patients with Superior
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Lecture Notes. Chapter 2: Introduction to Respiratory Failure
 Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Adult Congenital Heart Disease: The New Reality. Disclosures
 Adult Congenital Heart Disease: The New Reality Kathryn Rouine-Rapp, MD Professor of Anesthesia Disclosures I have nothing to disclose 1 Outline Historic perspective Our reality Common lesions Guidelines
Adult Congenital Heart Disease: The New Reality Kathryn Rouine-Rapp, MD Professor of Anesthesia Disclosures I have nothing to disclose 1 Outline Historic perspective Our reality Common lesions Guidelines
3/14/2011 MANAGEMENT OF NEWBORNS CARDIAC INTENSIVE CARE CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 WITH HEART DEFECTS
 CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 MANAGEMENT OF NEWBORNS WITH HEART DEFECTS A NTHONY C. CHANG, MD, MBA, MPH M E D I C AL D I RE C T OR, HEART I N S T I T U T E C H I LDRE N
CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 MANAGEMENT OF NEWBORNS WITH HEART DEFECTS A NTHONY C. CHANG, MD, MBA, MPH M E D I C AL D I RE C T OR, HEART I N S T I T U T E C H I LDRE N
Congenital Heart Defects
 Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Clinicians and Facilities: RESOURCES WHEN CARING FOR WOMEN WITH ADULT CONGENITAL HEART DISEASE OR OTHER FORMS OF CARDIOVASCULAR DISEASE!!
 Clinicians and Facilities: RESOURCES WHEN CARING FOR WOMEN WITH ADULT CONGENITAL HEART DISEASE OR OTHER FORMS OF CARDIOVASCULAR DISEASE!! Abha'Khandelwal,'MD,'MS' 'Stanford'University'School'of'Medicine'
Clinicians and Facilities: RESOURCES WHEN CARING FOR WOMEN WITH ADULT CONGENITAL HEART DISEASE OR OTHER FORMS OF CARDIOVASCULAR DISEASE!! Abha'Khandelwal,'MD,'MS' 'Stanford'University'School'of'Medicine'
Nothing to Disclose. Severe Pulmonary Hypertension
 Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
WHY ADMINISTER CARDIOTONIC AGENTS?
 Cardiac Pharmacology: Ideas For Advancing Your Clinical Practice The image cannot be displayed. Your computer may not have enough memory to open the image, or Roberta L. Hines, M.D. Nicholas M. Greene
Cardiac Pharmacology: Ideas For Advancing Your Clinical Practice The image cannot be displayed. Your computer may not have enough memory to open the image, or Roberta L. Hines, M.D. Nicholas M. Greene
IMAGES. in PAEDIATRIC CARDIOLOGY. Abstract
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
Atrioventricular Valve Dysplasia
 Atrioventricular Valve Dysplasia How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job
Atrioventricular Valve Dysplasia How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job
The role of intraoperative TOE in congenital cardiac surgery
 The role of intraoperative TOE in congenital cardiac surgery Justiaan Swanevelder Dept of Anaesthesia Groote Schuur and Red Cross War Memorial Children s Hospitals University of Cape Town, South Africa
The role of intraoperative TOE in congenital cardiac surgery Justiaan Swanevelder Dept of Anaesthesia Groote Schuur and Red Cross War Memorial Children s Hospitals University of Cape Town, South Africa
Earlier Use of Inhaled Nitric Oxide in Term and Near-Term Neonates With Hypoxic Respiratory Failure (HRF) and Pulmonary Hypertension (PH)
 Earlier Use of Inhaled Nitric Oxide in Term and Near-Term Neonates With Hypoxic Respiratory Failure (HRF) and Pulmonary Hypertension (PH) 2013 Ikaria, Inc. 1 Disclosure Information This program is sponsored
Earlier Use of Inhaled Nitric Oxide in Term and Near-Term Neonates With Hypoxic Respiratory Failure (HRF) and Pulmonary Hypertension (PH) 2013 Ikaria, Inc. 1 Disclosure Information This program is sponsored
CYANOTIC CONGENITAL HEART DISEASES. PRESENTER: DR. Myra M. Koech Pediatric cardiologist MTRH/MU
 CYANOTIC CONGENITAL HEART DISEASES PRESENTER: DR. Myra M. Koech Pediatric cardiologist MTRH/MU DEFINITION Congenital heart diseases are defined as structural and functional problems of the heart that are
CYANOTIC CONGENITAL HEART DISEASES PRESENTER: DR. Myra M. Koech Pediatric cardiologist MTRH/MU DEFINITION Congenital heart diseases are defined as structural and functional problems of the heart that are
Subject: Inhaled Nitric Oxide
 07-00007-12 Original Effective Date: 04/15/01 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Inhaled Nitric Oxide THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION OF BENEFITS,
07-00007-12 Original Effective Date: 04/15/01 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Inhaled Nitric Oxide THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION OF BENEFITS,
Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension
 Tohoku J. Exp. Med., 1994, 174, 41-48 Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension KIYOSHI HANEDA, NAOSHI SATO, TAKAO TOGO, MAKOTO MIURA, MASAKI RATA and
Tohoku J. Exp. Med., 1994, 174, 41-48 Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension KIYOSHI HANEDA, NAOSHI SATO, TAKAO TOGO, MAKOTO MIURA, MASAKI RATA and
In 1980, Bex and associates 1 first introduced the initial
 Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Repair or Replacement
 Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
CARDIOTHORACIC TRANSPLANTATION
 CARDIOTHORACIC TRANSPLANTATION A prospective, randomized, crossover pilot study of inhaled nitric oxide versus inhaled prostacyclin in heart transplant and lung transplant recipients Tanveer A. Khan, MD,
CARDIOTHORACIC TRANSPLANTATION A prospective, randomized, crossover pilot study of inhaled nitric oxide versus inhaled prostacyclin in heart transplant and lung transplant recipients Tanveer A. Khan, MD,
Recent technical advances and increasing experience
 Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Although most patients with Ebstein s anomaly live
 Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE
 SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
Inhaled nitric oxide: clinical evidence for use in adults
 Inhaled nitric oxide: clinical evidence for use in adults Neill Adhikari Critical Care Medicine Sunnybrook Health Sciences Centre and University of Toronto 31 October 2014 Conflict of interest Ikaria provided
Inhaled nitric oxide: clinical evidence for use in adults Neill Adhikari Critical Care Medicine Sunnybrook Health Sciences Centre and University of Toronto 31 October 2014 Conflict of interest Ikaria provided
Septal Defects. How does the heart work?
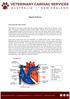 Septal Defects How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right side
Septal Defects How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right side
Paediatric addendum to CHMP guideline on the clinical investigations of medicinal products for the treatment of pulmonary arterial hypertension
 5 December 2011 EMA/CHMP/213972/2010 Committee for Medicinal Products for Human use (CHMP) Paediatric addendum to CHMP guideline on the clinical investigations of medicinal products for the treatment of
5 December 2011 EMA/CHMP/213972/2010 Committee for Medicinal Products for Human use (CHMP) Paediatric addendum to CHMP guideline on the clinical investigations of medicinal products for the treatment of
Assessment of Pulmonary Endothelial Function During Invasive Testing in Children and Adolescents With Idiopathic Pulmonary Arterial Hypertension
 Journal of the American College of Cardiology Vol. 60, No. 2, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2012.04.010
Journal of the American College of Cardiology Vol. 60, No. 2, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2012.04.010
Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications
 Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications Madhav Swaminathan, MD, FASE Professor of Anesthesiology Division of Cardiothoracic Anesthesia & Critical Care Duke University
Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications Madhav Swaminathan, MD, FASE Professor of Anesthesiology Division of Cardiothoracic Anesthesia & Critical Care Duke University
Patients at Risk for Low Systemic Oxygen Delivery After the Norwood Procedure
 Patients at Risk for Low Systemic Oxygen Delivery After the Norwood Procedure James S. Tweddell, MD, George M. Hoffman, MD, Raymond T. Fedderly, MD, Nancy S. Ghanayem, MD, John M. Kampine, MD, Stuart Berger,
Patients at Risk for Low Systemic Oxygen Delivery After the Norwood Procedure James S. Tweddell, MD, George M. Hoffman, MD, Raymond T. Fedderly, MD, Nancy S. Ghanayem, MD, John M. Kampine, MD, Stuart Berger,
Research Presentation June 23, Nimish Muni Resident Internal Medicine
 Research Presentation June 23, 2009 Nimish Muni Resident Internal Medicine Research Question In adult patients with repaired Tetralogy of Fallot, how does Echocardiography compare to MRI in evaluating
Research Presentation June 23, 2009 Nimish Muni Resident Internal Medicine Research Question In adult patients with repaired Tetralogy of Fallot, how does Echocardiography compare to MRI in evaluating
Clinical Policy: Inhaled Nitric Oxide Reference Number: CP.MP.87
 Clinical Policy: Reference Number: CP.MP.87 Last Review Date: 09/18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description (ino) is a
Clinical Policy: Reference Number: CP.MP.87 Last Review Date: 09/18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description (ino) is a
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Cardiac Emergencies in Infants. Michael Luceri, DO
 Cardiac Emergencies in Infants Michael Luceri, DO October 7, 2017 I have no financial obligations or conflicts of interest to disclose. Objectives Understand the scope of congenital heart disease Recognize
Cardiac Emergencies in Infants Michael Luceri, DO October 7, 2017 I have no financial obligations or conflicts of interest to disclose. Objectives Understand the scope of congenital heart disease Recognize
Pheochromocytoma Crisis Presenting as Fulminant Cardiopulmonary Failure: A Case Report
 170 Pheochromocytoma Crisis Presenting as Fulminant Cardiopulmonary Failure: A Case Report Chun-Wen Chiu 1, Cheng-Hsiung Chen 2 Fulminant cardiopulmonary failure in a patient with pheochromocytoma is a
170 Pheochromocytoma Crisis Presenting as Fulminant Cardiopulmonary Failure: A Case Report Chun-Wen Chiu 1, Cheng-Hsiung Chen 2 Fulminant cardiopulmonary failure in a patient with pheochromocytoma is a
AORTIC COARCTATION. Synonyms: - Coarctation of the aorta
 AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
CONGENITAL HEART LESIONS ((C.H.L
 CONGENITAL HEART LESIONS ((C.H.L BY THE BOOKS: 0.8 IN FACT: 3-5% INCLUDING: - BICUSPID AORTIC VALVE MITRAL VALVE PROLAPSE LATE DIAGNOSIS - :INCREASED INCIDENCE IN ADULTS BETTER DIAGNOSIS IN INFANCY BETTER
CONGENITAL HEART LESIONS ((C.H.L BY THE BOOKS: 0.8 IN FACT: 3-5% INCLUDING: - BICUSPID AORTIC VALVE MITRAL VALVE PROLAPSE LATE DIAGNOSIS - :INCREASED INCIDENCE IN ADULTS BETTER DIAGNOSIS IN INFANCY BETTER
The Impact of Length of Post-Operative Ventilator Support on Outcome of the Arterial Switch Operation Report from a Single Institute
 Original Article Post-Operative Ventilator Support after Arterial Switch Operation Acta Cardiol Sin 2010;26:173 8 Cardiovascular Surgery The Impact of Length of Post-Operative Ventilator Support on Outcome
Original Article Post-Operative Ventilator Support after Arterial Switch Operation Acta Cardiol Sin 2010;26:173 8 Cardiovascular Surgery The Impact of Length of Post-Operative Ventilator Support on Outcome
F that many congenital cardiac anomalies can be detected
 Fetal Cardiac Bypass: Improved Placental Function With Moderately High Flow Rates John A. Hawkins, MD, Steven M. Clark, MD, Robert E. Shaddy, MD, and William A. Gay, Jr, MD Divisions of Cardiothoracic
Fetal Cardiac Bypass: Improved Placental Function With Moderately High Flow Rates John A. Hawkins, MD, Steven M. Clark, MD, Robert E. Shaddy, MD, and William A. Gay, Jr, MD Divisions of Cardiothoracic
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
ino_rmp version 4.1_2016 Module Risk-management system NO-RMP-V 2.1
 VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Persistent pulmonary hypertension of the newborn (PPHN) Persistent pulmonary hypertension of the newborn is a life threatening
VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Persistent pulmonary hypertension of the newborn (PPHN) Persistent pulmonary hypertension of the newborn is a life threatening
ACCEPTED MANUSCRIPT. Title: Vasoactive-Ventilation-Renal Score Reliably Predicts Hospital Length-of- Stay after Surgery for Congenital Heart Disease
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 Title: Vasoactive-Ventilation-Renal Score Reliably Predicts Hospital
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 Title: Vasoactive-Ventilation-Renal Score Reliably Predicts Hospital
