Magnesium potentiates neuromuscular blockade with cisatracurium during cardiac surgery
|
|
|
- Laureen Chase
- 6 years ago
- Views:
Transcription
1 172 Cardiothoracic Anesthesia, Respiration and Airway Magnesium potentiates neuromuscular blockade with cisatracurium during cardiac surgery [Le magnésium potentialise le blocage neuromusculaire réalisé avec du cisatracurium en cardiochirurgie] Anne Marie Pinard MD FRCPC,* François Donati MD PhD FRCPC, Raymond Martineau MD FRCPC, André Y. Denault MD CSPQ FRCPC, Jean Taillefer MD, Michel Carrier MD Purpose: Magnesium potentiates the effect of nondepolarizing neuromuscular blocking agents. It is used in cardiac anesthesia to prevent hypertension and arrhythmias. This study was performed to measure the interaction between magnesium and cisatracurium in cardiac surgery. Methods: Twenty patients scheduled for elective cardiac surgery were randomly assigned to receive magnesium sulfate (70 mg kg 1 at induction followed by 30 mg kg 1 hr 1 ) or placebo. The ulnar nerve was stimulated and the electromyographic response of the adductor pollicis was measured. Cisatracurium 0.1 mg kg 1 was given at induction, followed by 0.05 mg kg 1 when the first twitch in the train-of-four reached 25%. Results: Ionized magnesium was 1.32 ± 0.24 mmol L 1 in the treatment group vs 0.47 ± 0.4 mmol L 1 in the control group. Duration of action of the intubating dose was longer in the magnesium group (74 ± 20 min) than in the placebo group (42 ± 6 min, P = ). Duration of the first maintenance dose was 69 ± 16 min in the magnesium group vs 35 ± 7 min in the placebo group (P = ). Total dose of cisatracurium administered throughout surgery was 0.19 ± 0.07 mg kg 1 in the magnesium group compared with 0.29 ± 0.01 mg kg 1 in the placebo group (P = 0.017). Hemodynamic variables and temperature were similar in both groups. Conclusion: In patients undergoing cardiac surgery, administration of magnesium sulfate, resulting in ionized levels of 1.3 mmol L 1, results in a min prolongation of the neuromuscular blockade induced with intubating and maintenance doses of cisatracurium and does not alter hemodynamic stability. Objectif : Le magnésium est utilisé en clinique pour traiter les arythmies et prévenir l hypertension. Le but de cette étude est de mesurer l interaction entre le cisatracurium et le magnésium en chirurgie cardiaque. Méthode : Vingt patients devant subir une intervention cardiaque programmée ont été randomisés pour recevoir du sulfate de magnésium (70 mg kg 1 à l induction puis 30 mg kg 1 h 1 ) ou un placebo. Le nerf ulnaire était stimulé et la réponse électromyographique du muscle adducteur du pouce était enregistrée. Pour l intubation, 0,1 mg kg 1 de cisatracurium était utilisé et les doses suivantes de 0,05 mg kg 1 ont été administrées lorsque T1 atteignait 25 %. Résultats : Le magnésium ionisé était de 1,32 ± 0,24 mmol L 1 dans le groupe traité vs 0,47 ± 0,4 mmol L 1 dans le groupe placebo. La durée d action des doses d intubation et de maintien dans le groupe traité au magnésium (74 ± 20 min et 69 ± 16) était plus longue que dans le groupe placebo (42 ± 6 et 35 ± 7, P = 0,0001). Les variables hémodynamiques et la température sont restés similaires dans les deux groupes. La quantité de cisatracurium administrée durant l'opération était moins grande dans le groupe ayant reçu du magnésium comparé au placebo (0,19 ± 0,07 mg kg 1 vs 0,29 ± 0,01 mg kg 1, P = 0,017). Conclusion : Chez des patients subissant une intervention cardiaque, une magnésémie de 1,3 mmol L 1 produit peu de changements hémodynamiques mais augmente la durée du bloc neuromusculaire produit par le cisatracurium d environ min. From the Department of Anesthesiology, Maisonneuve-Rosemont Hospital,* University of Montreal, and the Departments of Anesthesiology, and Surgery, Montreal Heart Institute, Montreal, Quebec, Canada. Address correspondence to: Dr. Anne-Marie Pinard, Department of Anesthesiology, Maisonneuve-Rosemont Hospital, 5415 L Assomption Boulevard, Montreal, Quebec H1T 2M4, Canada. Phone: ; Fax: ; ampinard@sympatico.ca This study was supported by the Plan de Pratique des Anesthésistes de l Institut de Cardiologie de Montréal. Accepted for publication June 18, Revision accepted November 4, CAN J ANESTH 2003 / 50: 2 / pp
2 Pinard et al.: MAGNESIUM POTENTIATES CISATRACURIUM BLOCKADE 173 INTRAVENOUS magnesium sulfate has many uses in clinical practice. Initially reported as a sole anesthetic agent in 1916, 1 it has been used more recently for its antiarrhythmic, anticonvulsant, and antihypertensive properties, especially in the anesthetic, obstetrical, and cardiac fields. 2 7 During cardiac surgery, magnesium sulfate is frequently used to control ventricular arrhythmias or to lower systemic or coronary vascular resistance. 4,8,9 An interaction between magnesium sulfate and nondepolarizing neuromuscular blocking agents (NMBAs) has been documented for many years. In 1968, a prolongation in duration of neuromuscular blockade was described in obstetrical patients when they were treated with magnesium for pre-eclampsia. 10 Several reports have since confirmed this interaction with vecuronium, rocuronium, pancuronium, and mivacurium, but it has not been determined for cisatracurium The doses of magnesium used in these studies were variable and serum concentrations of magnesium were not measured. Furthermore, none of these investigations were performed in cardiac surgery, where magnesium might be useful and widely used and none used cisatracurium, which has an elimination profile suitable for cardiac patients who are at risk of renal and hepatic failure. The purpose of this study was to quantify the interaction between magnesium sulfate and cisatracurium by measuring the duration of neuromuscular blockade in a randomized, double-blind controlled study in cardiac surgery patients, using a standardized dosage of magnesium to obtain stable levels throughout the procedure. Methods The protocol was approved by the Institutional Review Board and patients gave written informed consent. Twenty American Society of Anesthesiology (ASA) physical status class II or III patients between 18 and 80-yr-old, undergoing elective cardiac surgery, were included in this study. Patients with any of the following criteria were excluded: morbid obesity (body mass index over 30 kg m 2 ), history of neuromuscular disease, diabetic neuropathy, or abnormal renal function (serum creatinine > 176 µmol L 1 ), and patients receiving magnesium supplementation or drugs known to have a significant interaction with NMBAs. Premedication included morphine 0.15 mg kg 1 im, scopolamine mg im and the patient s usual cardiac medication. When the patient arrived in the operating room (OR), oxygen was administered by nasal cannula and standard monitors (electrocardiogram, pulse oximeter, noninvasive blood pressure) TABLE I Demographic data (mean ± SD when applicable) Placebo Magnesium P-value n = 10 n = 10 Gender (M/F) 7/3 9/1 0.3 Age (yr) 62 ± ± Weight (kg) 77 ± ± Height (cm) 165 ± ± Type of surgery (CABG/others) 7/3 7/3 1 Unstable angina 3 (30%) 3 (30%) 1 Hypertension 6 (60%) 6 (60%) 1 Heart failure 2 (20%) 4 (40%) 0.3 Diabetes 1 (10%) 1 (10%) 1 COPD 1 (10%) 1 (10%) 1 Beta-blockers 8 (80%) 5 (50%) 0.2 ACE inhibitors 3 (30%) 4 (40%) 0.6 Calcium channel blockers 5 (50%) 7 (70%) 0.4 Diuretics 1 (10%) 1 (10%) 1 ACE = angiotensin-converting enzyme; CABG = coronary artery bypass graft; COPD = chronic obstructive pulmonary disease. were applied. Sedation with midazolam 1 2 mg iv boluses and/or propofol mg iv were administered as required to maintain sedation during insertion, under local anesthesia, of a radial artery cannula and the introduction of a pulmonary artery catheter via the internal jugular route. Neuromuscular function was monitored with a relaxograph (Datex, Helsinki, Finland), which uses an electromyographic technique. The response of the adductor pollicis muscle was recorded over the thenar eminence after supramaximal train-of-four (2 Hz for 2 sec) stimulation of the ulnar nerve at the wrist every 20 sec. The neuromuscular monitor was calibrated before administration of the study drug (magnesium or placebo) and induction of anesthesia. Skin temperature was measured using a temperature monitor (Shiley, CA, USA) applied to the skin surface of the hypothenar site of the same hand. Following calibration of the neuromuscular monitor, patients were randomly allocated to receive either magnesium 70 mg kg 1 over ten minutes prior to induction of anesthesia, followed by an infusion of 30 mg kg 1 hr 1 (Group A), or an equal volume of normal saline solution (Group B). The study drug infusion was maintained until the beginning of sternal closure towards the end of surgery. Randomization was made by the pharmacist, who was the only unblinded person in the study, from sealed envelopes. The investigator was blinded to the contents of the perfusion syringe and to the results of plasma magnesium levels. There were ten patients in each group.
3 174 CANADIAN JOURNAL OF ANESTHESIA TABLE II Core and cutaneous temperature Time (min) Skin temperature ( C) P-value Core temperature ( C) P-value Placebo Magnesium Placebo Magnesium n = 10 n = 10 n = 10 n = NS NA NA NA NS NS NS NS NS NS NS NS NS NS NS NS NS NS NS NS NS NS NA = not applicable; NS = not significant. TABLE III Pharmacodynamics of cisatracurium and plasma potassium levels (mean ± SD) Placebo Magnesium P-value n = 10 n = 10 Duration to 25% (first dose) (min) 42.6 ± ± Duration to 25% (second dose) (min) 35.3 ± ± Total dose, cisatracurium (mg kg 1 ) 0.29 ± ± Ionized Mg, arrival ICU (mmol L 1 ) 0.53 ± ± Ionized K, arrival ICU (mmol L 1 ) 4.09 ± ± Duration of surgery (min) 271 ± ± ICU = intensive care unit. After preoxygenation, anesthesia was induced and maintained with iv midazolam, propofol and sufentanil with the dosages being at the anesthesiologist s discretion. Cisatracurium 0.1 mg kg 1 (2 ED 95 ) iv was administered to facilitate tracheal intubation. Laryngoscopy was performed when first twitch height (T1) was < 15%. Mechanical ventilation with oxygen at a FIO 2 of 1.0 was set at a tidal volume of 9 12 ml kg 1 at a rate of 8 10 breaths min 1. No volatile anesthetic agents were allowed at any time throughout the surgery. Muscle relaxation was maintained by administering repeated boluses of cisatracurium 0.05 mg kg 1 (1 ED 95 ) iv when neuromuscular function recovered to 25% of T1 until the beginning of sternal closure at which time neuromuscular function was allowed to recover spontaneously. At the end of surgery, reversal of blockade was achieved with neostigmine 0.05 mg kg 1 and glycopyrrolate 10 µg kg 1 iv, administered only when four twitches were present on the train-of-four stimulation. After surgery, patients were transferred to the intensive care unit (ICU), where mechanical ventilation was continued until normothermia, stable hemodynamics, spontaneous breathing, and consciousness were achieved. Neuromuscular blockade was measured every 20 sec from induction of anesthesia until the end of the skin closure. The following variables were recorded after each dose of cisatracurium: time to 90% T1 depression, maximum block and time from injection to 25% T1 recovery. After the last dose, duration to 75% spontaneous T1 recovery was also recorded. Systolic blood pressure and heart rate were taken on arrival in the OR, prior to bolus of study medication, at the end of the bolus, and following tracheal intubation. Systolic blood pressure, heart rate, skin and core temperature were also recorded every 15 min after the administration of cisatracurium. Blood samples for magnesium, electrolytes and arterial blood gases were drawn before and after the initial bolus of study drug, after induction of anesthesia and on arrival in the ICU. Ionized magnesium was measured (NOVA STAT Profile Ultra C Analyzer, [ion selective electrode technique], NOVA Biomedical, Waltham, MA, USA - normal range mmol L 1 of ionized magnesium in whole blood) and the results of the test were not disclosed to the investigator.
4 Pinard et al.: MAGNESIUM POTENTIATES CISATRACURIUM BLOCKADE 175 usage were analyzed using Chi-square and Fisher exact tests where appropriate. Blood pressure, heart rate, temperature, ionized plasma magnesium, and duration of neuromuscular blockade analysis were performed using comparison of the mean with one-way ANOVA and were adjusted for inequality of variance when needed. A P-value less than 0.05 was considered to indicate a statistically significant difference. FIGURE 1 Systolic blood blood pressure (SBP) and heart rate (HR) in placebo (pl) and magnesium-treated (Mg) groups. Values are expressed as means ± standard deviations. FIGURE 2 Whole blood ionized magnesium throughout surgery and on arrival in intensive care unit (ICU). Values are expressed as means ± standard deviations Statistical analysis Sample size was determined from a pilot study on five patients who received magnesium. The expected duration of neuromuscular block was estimated at 46 ± 10 min [mean ± standard deviation (SD)] from the study by Searle et al. 19 in the same hospital. Using Student s t test, we calculated a sample size of ten patients per group to detect a clinically significant difference, due to magnesium, of 30% with an alpha value of 0.05 and a power of 0.8. Results are presented as mean ± SD. Comparison of demographic data (age, weight, and height) was performed using two-sided Student s t test. Frequency of coexisting diseases and medication Results There were no differences between the study groups with respect to demographic data, ASA physical status, coexisting disease, preoperative medication, type of surgery or duration of cardiopulmonary bypass (Table I). Total doses of midazolam, propofol, and sufentanil were 1 19 mg, mg, and µg respectively. Systolic blood pressure and heart rate are shown in Figure 1. There were no statistical differences in these variables between the two groups on arrival in the OR, at baseline, prior to bolus of study medication, at the end of the bolus of study medication or at the end of surgery, and prior to transfer to the ICU. Core and cutaneous temperatures were similar in both groups throughout the whole surgery (Table II). Ionized magnesium levels were similar between the two groups at baseline (0.48 ± 0.04 mmol L 1 in Group A vs 0.49 ± 0.04 mmol L 1 in Group B, P = 0.7), but significantly higher in the magnesium-treated group (1.32 ± 0.2 mmol L 1 vs 0.47 ± 0.3 mmol L 1, P = ) following bolus administration and remained higher throughout surgery and on arrival in the ICU (Figure 2). There was no statistically significant difference in plasma potassium levels on arrival in the ICU between both groups (Table III). Single twitch remained stable at the end of bolus administration (T1 = 98% of control in both groups). Maximum blockade was 100% in all patients. When compared with the control group, there was a significant prolongation in neuromuscular blockade in the group receiving magnesium. The duration to 25% recovery after the intubating dose (0.1 mg kg 1 ) was 32 min longer in the magnesium-treated group compared with the placebo group (P = , Table III). The effects of the first maintenance dose of cisatracurium (0.05 mg kg 1 ) also lasted 34 min longer (P = , Table III). Comparisons were made only for the first maintenance dose because some magnesiumtreated patients received only one maintenance dose. Patients given magnesium received 2.5 ± 0.5 maintenance doses, whereas those in the control group were given 4.8 ± 1.9 maintenance doses. Total dose of cisatracurium was significantly less in the magnesium group (0.19 ± 0.07 mg kg 1 ) compared with the place-
5 176 CANADIAN JOURNAL OF ANESTHESIA bo group (0.29 ± 0.01 mg kg 1, P = 0.017). Because several patients did not receive reversal of NMBA and single twitch did not recover to control values, evaluation of neuromuscular blockade to full recovery at the end of surgery was not possible. Discussion At dosages commonly used in cardiac patients, this study demonstrates that magnesium causes a significant prolongation of the effects of cisatracurium on the neuromuscular junction without cardiovascular effects. The dosage of magnesium selected is commonly used in cardiac surgery when treating shivering or pre- and postoperative arrhythmia, 8 and in obstetrical patients. In this study, pharmacological agents such as volatile agents or aminoglycosides were avoided because of their significant potentiation of the effects of nondepolarizing NMBA. 19 Other drugs such as calcium channel blockers and beta-blockers may have an effect on muscle relaxation. However, this effect is not clinically important, 20 and patients already taking these medications were equally distributed between both groups. The dosage of magnesium sulfate was chosen in an attempt to obtain plasma concentrations which preserve cardiovascular stability and prevent arrhythmia. In cardiology, the therapeutic level to prevent and treat arrhythmia is generally in the range of 3 6 meq L 1, or mmol L 1 total plasma magnesium, of which two thirds are ionized. The mean ionized magnesium level was 1.2 mmol L 1 in the treatment group, which suggests that the dose given was adequate to achieve a level close to the one required for treatment of arrhythmia. No significant effect was observed on heart rate and blood pressure. The number of patients was too small to determine whether magnesium was effective in preventing arrhythmia, and this was not the purpose of this investigation. Body temperature can have an influence on neuromuscular function. Buzello et al. have found that hypothermic cardiopulmonary bypass induces reversible twitch depression, 21 but the central and peripheral temperature of the patients during bypass were not reported. Recently, Cammu et al. studied the effects of hypothermic cardiopulmonary bypass on dose requirements of cisatracurium and rocuronium. 22 They demonstrated that temperature had an important effect on the dose of cisatracurium needed to maintain adequate neuromuscular blockade. This is probably due to breakdown of cisatracurium, which is more dependent on ph and temperature compared with other NMBA. 23 In our study, central and cutaneous temperatures were recorded throughout the surgery, and were not different in the two groups. The duration of neuromuscular blockade associated with the initial bolus of cisatracurium was measured before the onset of cardiopulmonary bypass, that is before the lower body temperature could produce a significant confounding effect. In 1954, Del Castillo et al. described three effects of magnesium on the neuromuscular junction: decreased release of acetylcholine at the motor nerve terminal, 9 diminished depolarizing action of acetylcholine, and depressed excitability of the muscle fibre membrane, with the first effect being the most important. 24 In 1968, Giesecke et al. confirmed these observations in cats and further found that magnesium sulfate potentiates the effects of succinylcholine or d-tubocurarine. 10 Others have also demonstrated an interaction between magnesium and NMBAs. Ghoneim and Long observed magnesium-treated toxemic patients and wrote that when magnesium was combined with a subliminal blood level of d-tubocurarine, severe paralysis ensued. 15 In an attempt to speed up the onset of NMBA, magnesium has been given before pancuronium, but its effects were marginal in this setting. 16 Fuchs-Buder et al. showed that the onset time of vecuronium was faster in the presence of magnesium, and the duration of vecuronium induced neuromuscular blockade was almost doubled. 12,13 Administration of MgSO 4 after return of neuromuscular function leads to recurarization profound enough to compromise respiration. Rocuronium 17 and mivacurium 11 are also known to have longer lasting effects with concurrent administration of magnesium. In our study, the duration of action of cisatracurium in patients not given magnesium was comparable to that reported in studies where the same dose (0.1 mg kg 1 ) was given. In magnesium-treated subjects, the duration of a bolus dose of cisatracurium 0.1 mg kg 1 was increased by 76% (74 vs 42 min) and this is comparable to what would be expected with cisatracurium 0.2 mg kg Our finding suggests that an increased ionized-magnesium plasma concentration to 1.2 mmo L 1 is associated with an increase in the sensitivity of the neuromuscular junction by a factor of approximately 2. Ionized magnesium corresponds to approximately 65 72% of total magnesium in blood. 25 Total magnesium is more often measured than ionized magnesium. An ionized whole blood magnesium of 1.2 mmol L 1 corresponds to a plasma level of approximately 1.7 mmol L 1 of total magnesium. The NMBAs affect the neuromuscular function by binding to the postsynaptic receptors. An excess of acetylcholine enhances neuromuscular transmission,
6 Pinard et al.: MAGNESIUM POTENTIATES CISATRACURIUM BLOCKADE 177 and this is the mechanism involved when reversing neuromuscular blockade with neostigmine. On the other hand, magnesium, as mentioned, decreases the amount of acetylcholine released by the nerve terminals at the neuromuscular junction. Consequently, in the presence of magnesium, competition between acetylcholine and NMBA to bind postsynaptic receptors is tilted in favour of NMBA; thus, the duration of the neuromuscular blockade is enhanced. Magnesium is known to lower systemic blood pressure by directly acting on blood vessels and by inhibiting many vasoconstrictor substances such as calcium, acetylcholine, angiotensin and epinephrine In our study, the magnesium sulfate bolus (70 mg kg 1 ) was administered over ten minutes and we did not observe any significant decrease in systolic and diastolic blood pressure or any significant increase in heart rate compared with placebo. Therefore, we conclude that neuromuscular transmission is impaired significantly at blood magnesium levels which have virtually no hemodynamic effects. 26 In conclusion, we observed a clinically significant increase in duration of cisatracurium induced neuromuscular blockade during cardiac surgery. We feel this finding is important because this interaction is clinically significant when magnesium is given to treat or prevent arrhythmia, systemic hypertension, low cardiac output with high systemic vascular resistance, or postoperative shivering. In these situations, recovery of neuromuscular function must be assessed more carefully when magnesium has been administered. On the other hand, giving magnesium with cisatracurium allows us to use approximately half the dose of cisatracurium to achieve and maintain the desired level of neuromuscular blockade. References 1 Peck CH, Meltzer SJ. Anesthesia in human beings by intravenous injection of magnesium sulfate. JAMA 1916; 67: Delhumeau A, Granry JC, Monrigal JP, Costerousse F. Therapeutic use of magnesium in anaesthesia and intensive care (French). Ann Fr Anesth Reanim 1995; 14: Fawcett WJ, Haxby EJ, Male DA. Magnesium: physiology and pharmacology. Br J Anaesth 1999; 83: Gomez MN. Magnesium and cardiovascular disease. Anesthesiology 1998; 89: Idama TO, Lindow SW. Magnesium sulphate: a review of clinical pharmacology applied to obstetrics. Br J Obstet Gynaecol 1998; 105: James MFM. Clinical use of magnesium infusions in anesthesia. Anesth Analg 1992; 74: Witlin AG, Sibai BM. Magnesium sulfate therapy in preeclampsia and eclampsia. Obstet Gynecol 1998; 92: England MR, Gordon G, Salem M, Chernow B. Magnesium administration and dysrhythmias after cardiac surgery. A placebo-controlled, double-blind, randomized trial. JAMA 1992; 268: Horner SM. Magnesium and arrhythmias in acute myocardial infarction. Coron Artery Dis 1996; 7: Giesecke AH Jr, Morris RE, Dalton MD, Stephen CR. Of magnesium, muscle relaxants, toxemic parturients, and cats. Anesth Analg 1968; 47: Ahn EK, Bai SJ, Cho BJ, Shin YS. The infusion rate of mivacurium and its spontaneous neuromuscular recovery in magnesium-treated parturients. Anesth Analg 1998; 86: Fuchs-Buder T, Wilder-Smith OHG, Borgeat A, Tassonyi E. Interaction of magnesium sulphate with vecuronium-induced neuromuscular block. Br J Anaesth 1995; 74: Fuchs-Buder T, Tassonyi E. Magnesium sulphate enhances residual neuromuscular block induced by vecuronium. Br J Anaesth 1996; 76: Fuchs-Buder T, Ziegenfub T, Lysakowski K, Tassonyi E. Antagonism of vecuronium-induced neuromuscular block in patients pretreated with magnesium sulphate: dose-effect relationship of neostigmine. Br J Anaesth 1999; 82: Ghoneim MM, Long JP. The interaction between magnesium and other neuromuscular blocking agents. Anesthesiology 1970; 32: James MFM, Schenk PA, Van Der Veen BW. Priming of pancuronium with magnesium. Br J Anaesth 1991; 66: Kussman B, Shorten G, Uppington J, Comunale ME. Administration of magnesium sulphate before rocuronium: effects on speed of onset and duration of neuromuscular block. Br J Anaesth 1997; 79: Stacey MRW, Barclay K, Asai T, Vaughan RS. Effects of magnesium sulphate on suxamethonium-induced complications during rapid-sequence induction of anaesthesia. Anaesthesia 1995; 50: Searle NR, Thomson I, Dupont C, et al. A two-center study evaluating the hemodynamic and pharmacodynamic effects of cisatracurium and vecuronium in patients undergoing coronary artery bypass surgery. J Cardiothorac Vasc Anesth 1999; 13: Feldman S, Karalliedde L. Drug interactions with neuromuscular blockers. Drug Saf 1996; 15: Buzello W, Pollmaecher T, Schluermann D, Urbanyi B. The influence of hypothermic cardiopulmonary bypass
7 178 CANADIAN JOURNAL OF ANESTHESIA on neuromuscular transmission in the absence of muscle relaxants. Anesthesiology 1986; 64: Cammu G, Coddens J, Hendrickx J, Deloof T. Dose requirements of infusions of cisatracurium or rocuronium during hypothermic cardiopulmonary bypass. Br J Anaesth 2000; 84: Kisor DF, Schmith VD. Clinical pharmacokinetics of cisatracurium besilate. Clin Pharmacokinet 1999; 36: Del Castillo J, Engbaek L. The nature of the neuromuscular block produced by magnesium. J Physiol 1954; 124: Altura BM, Altura BT. Role of magnesium in pathophysiological processes and the clinical utility of magnesium ion selective electrodes. Scand J Clin Lab Invest 1996; 56(Suppl 224): Somjen GG, Baskerville EN. Effect of excess magnesium on vagal inhibition and acetylcholine sensitivity of the mammalian heart in situ and in vitro. Nature 1968; 217: Altura BM, Altura BT. Magnesium and vascular tone and reactivity. Blood Vessels 1978; 15: Altura BM, Altura BT, Carella A, Gebrewold A, Murakawa T, Nishio A. Mg 2+ -Ca 2+ interaction in contractility of vascular smooth muscle: Mg 2+ versus organic calcium channel blockers on myogenic tone and agonist-induced responsiveness of blood vessels. Can J Physiol Pharmacol 1987; 65:
Magnesium sulfate; Laryngoscopy; Sternotomy; Hemodynamic response; Coronary artery bypass graft
 Acad J Surg, 1 10 Dec. 2015 10 Aug. 2016 4 Mar. 2016 This study was designed to evaluate the effectiveness of low and high dose magnesium sulfate in reducing pressure responses to laryngoscopy and sternotomy.
Acad J Surg, 1 10 Dec. 2015 10 Aug. 2016 4 Mar. 2016 This study was designed to evaluate the effectiveness of low and high dose magnesium sulfate in reducing pressure responses to laryngoscopy and sternotomy.
S. SAKURABA (*), R. SERITA (**), S. KOSUGI**, L. I. ERIKSSON (***), S. G. E. LINDAHL (***) and J. TAKEDA (*)
 (Acta Anaesth. Belg., 2006, 57, 253-257) Pretreatment with magnesium sulphate is associated with less succinylcholine-induced fasciculation and subsequent tracheal intubation-induced hemodynamic changes
(Acta Anaesth. Belg., 2006, 57, 253-257) Pretreatment with magnesium sulphate is associated with less succinylcholine-induced fasciculation and subsequent tracheal intubation-induced hemodynamic changes
Effect of Magnesium Sulphate on the Speed of Onset and Duration of Neuromuscular Block Produced by Rocuronium Bromide
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 2 Ver. VI (February. 2017), PP 54-58 www.iosrjournals.org Effect of Magnesium Sulphate on the
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 2 Ver. VI (February. 2017), PP 54-58 www.iosrjournals.org Effect of Magnesium Sulphate on the
PRE-TREATMENT WITH MAGNESIUM SULPHATE BEFORE NON-DEPOLARIZING MUSCLE RELAXANTS: EFFECT ON SPEED ON ONSET, INDUCTION AND RECOVERY
 PRE-TREATMENT WITH MAGNESIUM SULPHATE BEFORE NON-DEPOLARIZING MUSCLE RELAXANTS: EFFECT ON SPEED ON ONSET, INDUCTION AND RECOVERY Suresh Singh 1, Deepak Malviya 2, Sujeet Rai 1, Birendra Yadav 3, Sanjeev
PRE-TREATMENT WITH MAGNESIUM SULPHATE BEFORE NON-DEPOLARIZING MUSCLE RELAXANTS: EFFECT ON SPEED ON ONSET, INDUCTION AND RECOVERY Suresh Singh 1, Deepak Malviya 2, Sujeet Rai 1, Birendra Yadav 3, Sanjeev
Sevoflurane and isoflurane, but not propofol, decrease mivacurium requirements over time
 907 General Anesthesia Sevoflurane and isoflurane, but not propofol, decrease mivacurium requirements over time [Le sévoflurane et l isoflurane, mais pas le propofol, diminuent les besoins en mivacurium
907 General Anesthesia Sevoflurane and isoflurane, but not propofol, decrease mivacurium requirements over time [Le sévoflurane et l isoflurane, mais pas le propofol, diminuent les besoins en mivacurium
Chapter 18. Skeletal Muscle Relaxants (Neuromuscular Blocking Agents)
 Chapter 18 Skeletal Muscle Relaxants (Neuromuscular Blocking Agents) Uses of Neuromuscular Blocking Facilitate intubation Surgery Agents Enhance ventilator synchrony Reduce intracranial pressure (ICP)
Chapter 18 Skeletal Muscle Relaxants (Neuromuscular Blocking Agents) Uses of Neuromuscular Blocking Facilitate intubation Surgery Agents Enhance ventilator synchrony Reduce intracranial pressure (ICP)
INTUBATING CONDITIONS AND INJECTION PAIN
 INTUBATING CONDITIONS AND INJECTION PAIN - Cisatracurium or Rocuronium versus Rocuronium-Cisatracurium Combination - AHED ZEIDAN *, NAZIH NAHLE *, HILAL MAALIKI ** AND ANIS BARAKA *** Summary The present
INTUBATING CONDITIONS AND INJECTION PAIN - Cisatracurium or Rocuronium versus Rocuronium-Cisatracurium Combination - AHED ZEIDAN *, NAZIH NAHLE *, HILAL MAALIKI ** AND ANIS BARAKA *** Summary The present
Priming with rocuronium accelerates neuromuscular block in children: a prospective randomized study
 538 REPORTS CANADIAN OF JOURNAL ORIGINAL OF INVESTIGATIONS ANESTHESIA Priming with rocuronium accelerates neuromuscular block in children: a prospective randomized study [L amorçage avec le rocuronium
538 REPORTS CANADIAN OF JOURNAL ORIGINAL OF INVESTIGATIONS ANESTHESIA Priming with rocuronium accelerates neuromuscular block in children: a prospective randomized study [L amorçage avec le rocuronium
Comparison of continuous infusion and intermittent bolus administration of Cisatracurium in cardiac surgery: a randomized clinical trial
 Original Article Comparison of continuous infusion and intermittent bolus administration of Cisatracurium in cardiac surgery: a randomized clinical trial Moosa Mirinejad, Ali Reza Yaghoubi, Rasoul Azarfarin,
Original Article Comparison of continuous infusion and intermittent bolus administration of Cisatracurium in cardiac surgery: a randomized clinical trial Moosa Mirinejad, Ali Reza Yaghoubi, Rasoul Azarfarin,
CISATRACURIUM IN CARDIAC SURGERY
 CISATRACURIUM IN CARDIAC SURGERY - Continuous Infusion vs. Bolus Administration - MOOSA MIRINEJAD *, RASOUL AZARFARIN * AND AZIN ALIZADEH ASL * Abstract The aim of this study was the comparison of infusion
CISATRACURIUM IN CARDIAC SURGERY - Continuous Infusion vs. Bolus Administration - MOOSA MIRINEJAD *, RASOUL AZARFARIN * AND AZIN ALIZADEH ASL * Abstract The aim of this study was the comparison of infusion
HST-151 Clinical Pharmacology in the Operating Room
 Harvard-MIT Division of Health Sciences and Technology HST.151: Principles of Pharmocology Instructors: Dr. Carl Rosow, Dr. David Standaert and Prof. Gary Strichartz 1 HST-151 Clinical Pharmacology in
Harvard-MIT Division of Health Sciences and Technology HST.151: Principles of Pharmocology Instructors: Dr. Carl Rosow, Dr. David Standaert and Prof. Gary Strichartz 1 HST-151 Clinical Pharmacology in
The effect of desflurane on rocuronium onset, clinical duration and maintenance requirements
 (Acta Anaesth. Belg., 2006, 57, 349-353) The effect of desflurane on rocuronium onset, clinical duration and maintenance requirements R. G. STOUT (*), T. J. GAN (**), P. S. A. GLASS (***), D. G. SILVERMAN
(Acta Anaesth. Belg., 2006, 57, 349-353) The effect of desflurane on rocuronium onset, clinical duration and maintenance requirements R. G. STOUT (*), T. J. GAN (**), P. S. A. GLASS (***), D. G. SILVERMAN
University of Mississippi Medical Center University of Mississippi Health Care. Pharmacy and Therapeutics Committee Medication Use Evaluation
 University of Mississippi Medical Center University of Mississippi Health Care Pharmacy and Therapeutics Committee Medication Use Evaluation Cisatracurium (Nimbex ) and Vecuronium (Norcuron ) PURPOSE The
University of Mississippi Medical Center University of Mississippi Health Care Pharmacy and Therapeutics Committee Medication Use Evaluation Cisatracurium (Nimbex ) and Vecuronium (Norcuron ) PURPOSE The
FOR REPRESENTATIVE EDUCATION
 Neuromuscular Blockade in the ICU NIMBEX Indication 1 NIMBEX (cisatracurium besylate) is indicated as an adjunct to general anesthesia to facilitate tracheal intubation in adults and in pediatric patients
Neuromuscular Blockade in the ICU NIMBEX Indication 1 NIMBEX (cisatracurium besylate) is indicated as an adjunct to general anesthesia to facilitate tracheal intubation in adults and in pediatric patients
(PP XI) Dr. Samir Matloob
 DRUGS ACTING ON THE CHOLINERGIC SYSTEM AND THE NEUROMUSCULAR BLOCKING DRUGS IV (NICOTINIC ANTAGONISTS) (PP XI) Dr. Samir Matloob Dept. of Pharmacology Baghdad College of Medicine Drugs acting on the cholinergic
DRUGS ACTING ON THE CHOLINERGIC SYSTEM AND THE NEUROMUSCULAR BLOCKING DRUGS IV (NICOTINIC ANTAGONISTS) (PP XI) Dr. Samir Matloob Dept. of Pharmacology Baghdad College of Medicine Drugs acting on the cholinergic
TRANSPARENCY COMMITTEE OPINION. 21 January 2009
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 21 January 2009 BRIDION 100 mg/ml, solution for injection Box containing 10 x 2 ml bottles, CIP: 573 553-9 Box containing
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 21 January 2009 BRIDION 100 mg/ml, solution for injection Box containing 10 x 2 ml bottles, CIP: 573 553-9 Box containing
Neuromuscular Junction
 Muscle Relaxants Neuromuscular Junction Cholinergic antagonists Neuromuscular-blocking agents (mostly nicotinic antagonists): interfere with transmission of efferent impulses to skeletal muscles. These
Muscle Relaxants Neuromuscular Junction Cholinergic antagonists Neuromuscular-blocking agents (mostly nicotinic antagonists): interfere with transmission of efferent impulses to skeletal muscles. These
Muscle relaxation and increasing doses of propofol improve intubating conditions
 GENERAL ANESTHESIA 121 Muscle relaxation and increasing doses of propofol improve intubating conditions [Les myorelaxants et des doses élevées de propofol améliorent les conditions d'intubation] Thomas
GENERAL ANESTHESIA 121 Muscle relaxation and increasing doses of propofol improve intubating conditions [Les myorelaxants et des doses élevées de propofol améliorent les conditions d'intubation] Thomas
Effect of Vecuronium in different age group
 Original Research Article Effect of Vecuronium in different age group Bharti Rajani 1, Hitesh Brahmbhatt 2, Hemlata Chaudhry 2, Hiren Parmar 3* 1 Associate Professor, Department of Anesthesiology, GMERS
Original Research Article Effect of Vecuronium in different age group Bharti Rajani 1, Hitesh Brahmbhatt 2, Hemlata Chaudhry 2, Hiren Parmar 3* 1 Associate Professor, Department of Anesthesiology, GMERS
The cholinesterase inhibitors, neostigmine and edrophonium,
 Reversal of Rocuronium-Induced Neuromuscular Blockade: A Comparison with Glycopyrrolate and Atropine Ozlem Sacan, MD Paul F. White, MD, PhD Burcu Tufanogullari, MD Kevin Klein, MD BACKGROUND: is a modified
Reversal of Rocuronium-Induced Neuromuscular Blockade: A Comparison with Glycopyrrolate and Atropine Ozlem Sacan, MD Paul F. White, MD, PhD Burcu Tufanogullari, MD Kevin Klein, MD BACKGROUND: is a modified
The Neuromuscular Effects and Tracheal Intubation Conditions After Small Doses of Succinylcholine
 The Neuromuscular Effects and Tracheal Intubation Conditions After Small Doses of Succinylcholine Mohammad I. El-Orbany, MD, Ninos J. Joseph, BS, M. Ramez Salem, MD, and Arthur J. Klowden, MD Department
The Neuromuscular Effects and Tracheal Intubation Conditions After Small Doses of Succinylcholine Mohammad I. El-Orbany, MD, Ninos J. Joseph, BS, M. Ramez Salem, MD, and Arthur J. Klowden, MD Department
Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant
 Original Article Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant Mirmohammad Taghi Mortazavi, 1 Masood Parish, 1 Naghi Abedini, 2
Original Article Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant Mirmohammad Taghi Mortazavi, 1 Masood Parish, 1 Naghi Abedini, 2
Journal of Anesthesia & Clinical
 Journal of Anesthesia & Clinical Research ISSN: 2155-6148 Journal of Anesthesia & Clinical Research Balasubramanian and Menaha, J Anesth Clin Res 2017, 8:12 DOI: 10.4172/2155-6148.1000791 Research Article
Journal of Anesthesia & Clinical Research ISSN: 2155-6148 Journal of Anesthesia & Clinical Research Balasubramanian and Menaha, J Anesth Clin Res 2017, 8:12 DOI: 10.4172/2155-6148.1000791 Research Article
The Latest Approaches to Reversal of Neuromuscular Blocking Agents
 The Latest Approaches to Reversal of Neuromuscular Blocking Agents Janay Bailey, Pharm.D. Anesthesiology 2017; 126:173-90 Objectives Pharmacists Determine optimal paralytic choices in knowing if reversal
The Latest Approaches to Reversal of Neuromuscular Blocking Agents Janay Bailey, Pharm.D. Anesthesiology 2017; 126:173-90 Objectives Pharmacists Determine optimal paralytic choices in knowing if reversal
A Nondepolarizing Neuromuscular Blocking (NMB) Agent
 DOSING GUIDE A Nondepolarizing Neuromuscular Blocking (NMB) Agent Easy to remember dosing for the 0.20 mg/kg adult intubating doses of NIMBEX 1 *: For every 10 kg, give 1 ml of NIMBEX (2 mg/ml concentration)
DOSING GUIDE A Nondepolarizing Neuromuscular Blocking (NMB) Agent Easy to remember dosing for the 0.20 mg/kg adult intubating doses of NIMBEX 1 *: For every 10 kg, give 1 ml of NIMBEX (2 mg/ml concentration)
Benztropine and trihexyphenidyl: Centrally acting antimuscarinic agents used for treatment of Parkinson disease & extrapyramidal symptoms.
 Scopolamine: Tertiary amine plant alkaloid. Produces peripheral effects similar to those of atropine. Unlike atropine, scopolamine has greater action on the CNS (observed at therapeutic doses). It has
Scopolamine: Tertiary amine plant alkaloid. Produces peripheral effects similar to those of atropine. Unlike atropine, scopolamine has greater action on the CNS (observed at therapeutic doses). It has
NERVOUS SYSTEM NERVOUS SYSTEM. Somatic nervous system. Brain Spinal Cord Autonomic nervous system. Sympathetic nervous system
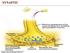 SYNAPTIC NERVOUS SYSTEM NERVOUS SYSTEM CENTRAL NERVOUS SYSTEM PERIPHERAL NERVOUS SYSTEM Brain Spinal Cord Autonomic nervous system Somatic nervous system Sympathetic nervous system Parasympathetic nervous
SYNAPTIC NERVOUS SYSTEM NERVOUS SYSTEM CENTRAL NERVOUS SYSTEM PERIPHERAL NERVOUS SYSTEM Brain Spinal Cord Autonomic nervous system Somatic nervous system Sympathetic nervous system Parasympathetic nervous
Nothing to Disclose. Severe Pulmonary Hypertension
 Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Effects of thiopental sodium, ketamine, and propofol on the onset time of rocuronium in children
 Anesth Pain Med 2017; 12: 47-51 https://doi.org/10.17085/apm.2017.12.1.47 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2017.12.1.47&domain=pdf&date_stamp=2017-1-25 pissn 1975-5171
Anesth Pain Med 2017; 12: 47-51 https://doi.org/10.17085/apm.2017.12.1.47 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2017.12.1.47&domain=pdf&date_stamp=2017-1-25 pissn 1975-5171
Effect of magnesium sulfate with propofol induction of anesthesia on succinylcholine-induced fasciculations and myalgia
 Original Article Effect of magnesium sulfate with propofol induction of anesthesia on succinylcholine-induced fasciculations and myalgia Mahendra Kumar, Nalin Talwar, Ritu Goyal, Usha Shukla, AK Sethi
Original Article Effect of magnesium sulfate with propofol induction of anesthesia on succinylcholine-induced fasciculations and myalgia Mahendra Kumar, Nalin Talwar, Ritu Goyal, Usha Shukla, AK Sethi
of end-tidal sevoflurane concentration for the smooth exchange of the tracheal tube for a laryngeal mask airway is 2.97%
 184 CARDIOTHORACIC ANESTHESIA, RESPIRATION AND AIRWAY The ED 95 of end-tidal sevoflurane concentration for the smooth exchange of the tracheal tube for a laryngeal mask airway is 2.97% [La DE 95 de la
184 CARDIOTHORACIC ANESTHESIA, RESPIRATION AND AIRWAY The ED 95 of end-tidal sevoflurane concentration for the smooth exchange of the tracheal tube for a laryngeal mask airway is 2.97% [La DE 95 de la
Core Safety Profile. Pharmaceutical form(s)/strength: Solution for Injection CZ/H/PSUR/0005/002 Date of FAR:
 Core Safety Profile Active substance: Rocuronium bromide Pharmaceutical form(s)/strength: Solution for Injection P-RMS: CZ/H/PSUR/0005/002 Date of FAR: 31.05.2012 4.3 Contraindications Hypersensitivity
Core Safety Profile Active substance: Rocuronium bromide Pharmaceutical form(s)/strength: Solution for Injection P-RMS: CZ/H/PSUR/0005/002 Date of FAR: 31.05.2012 4.3 Contraindications Hypersensitivity
*Author for Correspondence
 COMPARATIVE EVALUATION OF ONSET TIME INTUBATING CONDITION JUDGED BY CLINICAL CRITERIA AND HAEMODYNAMIC RESPONSE AFTER THE INTUBATING DOSE OF ROCURONIUM AND VECURONIUM *Namita Gupta 1, Mamta Sharma 2, Pusplata
COMPARATIVE EVALUATION OF ONSET TIME INTUBATING CONDITION JUDGED BY CLINICAL CRITERIA AND HAEMODYNAMIC RESPONSE AFTER THE INTUBATING DOSE OF ROCURONIUM AND VECURONIUM *Namita Gupta 1, Mamta Sharma 2, Pusplata
New York Science Journal 2017;10(6) Efficacy And Safety Of Sugammadex In Reversing Nmb (Rocuronium) In Adults
 Efficacy And Safety Of Sugammadex In Reversing Nmb (Rocuronium) In Adults Mahmoud Abd Elrahman El Sherbeny; Ehab Ahmed Abd Elrahman; Reda Khalil Kamal; Mohamed Ahmed Mohamed Abozena Anesthesia and ICU
Efficacy And Safety Of Sugammadex In Reversing Nmb (Rocuronium) In Adults Mahmoud Abd Elrahman El Sherbeny; Ehab Ahmed Abd Elrahman; Reda Khalil Kamal; Mohamed Ahmed Mohamed Abozena Anesthesia and ICU
Pharmacology of the Neuromuscular Junction (NMJ)
 Pharmacology of the Neuromuscular Junction (NMJ) Edward JN Ishac, Ph.D. Professor Smith Building, Room 742 eishac@vcu.edu 828 2127 Department of Pharmacology and Toxicology Medical College of Virginia
Pharmacology of the Neuromuscular Junction (NMJ) Edward JN Ishac, Ph.D. Professor Smith Building, Room 742 eishac@vcu.edu 828 2127 Department of Pharmacology and Toxicology Medical College of Virginia
Pharmacology of the Neuromuscular Junction (NMJ)
 Pharmacology of the Neuromuscular Junction (NMJ) Edward JN Ishac, Ph.D. Professor Smith Building, Room 742 eishac@vcu.edu 828 2127 Department of Pharmacology and Toxicology Medical College of Virginia
Pharmacology of the Neuromuscular Junction (NMJ) Edward JN Ishac, Ph.D. Professor Smith Building, Room 742 eishac@vcu.edu 828 2127 Department of Pharmacology and Toxicology Medical College of Virginia
Type of intervention Anaesthesia. Economic study type Cost-effectiveness analysis.
 Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Xiaochong Fan, Minyu Ma, Zhisong Li, Shengkai Gong, Wei Zhang, Yuanyuan Wen
 Int J Clin Exp Med 2015;8(9):16369-16373 www.ijcem.com /ISSN:1940-5901/IJCEM0008198 Original Article The relationship between the target effective site concentration of rocuronium and the degree of recovery
Int J Clin Exp Med 2015;8(9):16369-16373 www.ijcem.com /ISSN:1940-5901/IJCEM0008198 Original Article The relationship between the target effective site concentration of rocuronium and the degree of recovery
Chapter 18 Neuromuscular Blocking Agents Study Guide and Application Exercise
 Chapter 18 Neuromuscular Blocking Agents Study Guide and Application Exercise 1. Read chapter 2. Review objectives (p.305) 3. Review key terms and definitions (p.305) Add: Cholinesterase inhibitor Vagal
Chapter 18 Neuromuscular Blocking Agents Study Guide and Application Exercise 1. Read chapter 2. Review objectives (p.305) 3. Review key terms and definitions (p.305) Add: Cholinesterase inhibitor Vagal
Comparative evaluation of atracurium dosed on ideal body weight vs. total body weight in morbidly obese patients
 British Journal of Clinical Pharmacology DOI:1.1111/j.1365-2125.21.383.x Comparative evaluation of atracurium dosed on ideal body weight vs. total body weight in morbidly obese patients Simone van Kralingen,
British Journal of Clinical Pharmacology DOI:1.1111/j.1365-2125.21.383.x Comparative evaluation of atracurium dosed on ideal body weight vs. total body weight in morbidly obese patients Simone van Kralingen,
CHAPTER 11. General and Local Anesthetics. Anesthetics. Anesthesia. Eliza Rivera-Mitu, RN, MSN NDEG 26 A
 CHAPTER 11 General and Local Anesthetics Eliza Rivera-Mitu, RN, MSN NDEG 26 A Anesthetics Agents that depress the central nervous system (CNS) Depression of consciousness Loss of responsiveness to sensory
CHAPTER 11 General and Local Anesthetics Eliza Rivera-Mitu, RN, MSN NDEG 26 A Anesthetics Agents that depress the central nervous system (CNS) Depression of consciousness Loss of responsiveness to sensory
The Effect of Intraoperative Magnesium Sulphate Infusion on The Course of Neuromuscular Blockade of Atracurium
 Journal of the Egyptian Nat. Cancer Inst., Vol. 14, No. 2, June: 137144, 2002 The Effect of Intraoperative Magnesium Sulphate Infusion on The Course of Neuromuscular Blockade of Atracurium NIVIN FAHMY
Journal of the Egyptian Nat. Cancer Inst., Vol. 14, No. 2, June: 137144, 2002 The Effect of Intraoperative Magnesium Sulphate Infusion on The Course of Neuromuscular Blockade of Atracurium NIVIN FAHMY
Propofol or etomidate: Does it genuinely matter for induction in cardiac surgical procedures?
 Original Research Article DOI: 10.18231/2394-4994.2016.0012 Propofol or etomidate: Does it genuinely matter for induction in cardiac surgical procedures? Manjunath Ratnakara Kamath 1,*, Suchitha Kamath
Original Research Article DOI: 10.18231/2394-4994.2016.0012 Propofol or etomidate: Does it genuinely matter for induction in cardiac surgical procedures? Manjunath Ratnakara Kamath 1,*, Suchitha Kamath
Reports of Investigation A rapid precurarization technique using rocuronium
 397 Ban C.H. Tsui MD MSc,* Susan Reid MD, t Sunil Gupta MD,* Ramona Kearney MD,* Tom Mayson MD,t Brendan Finucane MD* Reports of Investigation A rapid precurarization technique using rocuronium Purpose:
397 Ban C.H. Tsui MD MSc,* Susan Reid MD, t Sunil Gupta MD,* Ramona Kearney MD,* Tom Mayson MD,t Brendan Finucane MD* Reports of Investigation A rapid precurarization technique using rocuronium Purpose:
Managing Hypertension in the Perioperative Arena
 Managing Hypertension in the Perioperative Arena Optimizing Perioperative Management Strategies for Hypertension in the Cardiac Surgical Patient Objectives: Treatment of hypertensive emergencies. ALBERT
Managing Hypertension in the Perioperative Arena Optimizing Perioperative Management Strategies for Hypertension in the Cardiac Surgical Patient Objectives: Treatment of hypertensive emergencies. ALBERT
NEUROMUSCULAR BLOCKING AGENTS
 NEUROMUSCULAR BLOCKING AGENTS Edward JN Ishac, Ph.D. Associate Professor, Pharmacology and Toxicology Smith 742, 828-2127, Email: eishac@vcu.edu Learning Objectives: 1. Understand the physiology of the
NEUROMUSCULAR BLOCKING AGENTS Edward JN Ishac, Ph.D. Associate Professor, Pharmacology and Toxicology Smith 742, 828-2127, Email: eishac@vcu.edu Learning Objectives: 1. Understand the physiology of the
Neuromuscular Monitoring and Patient Safety:
 Neuromuscular Monitoring and Patient Safety: Pulmonary Complications of Residual Block CEEA Course Tuesday, Sept 4, 2012 Târgu Mureş, Romania Sorin J. Brull, MD, FCARCSI (Hon) Editor, Patient Safety Section
Neuromuscular Monitoring and Patient Safety: Pulmonary Complications of Residual Block CEEA Course Tuesday, Sept 4, 2012 Târgu Mureş, Romania Sorin J. Brull, MD, FCARCSI (Hon) Editor, Patient Safety Section
Neuromuscular Blockers
 Neuromuscular Blockers Joanne Leung joanneleung22@hotmail.com Oct 14, 2014 Objectives After this lecture, you should be able to: Describe the physiology of the neuromuscular junction Differentiate the
Neuromuscular Blockers Joanne Leung joanneleung22@hotmail.com Oct 14, 2014 Objectives After this lecture, you should be able to: Describe the physiology of the neuromuscular junction Differentiate the
Comparative study of intubating conditions after Rocuronium and Suxamethonium (study of 80 cases)
 ISPUB.COM The Internet Journal of Anesthesiology Volume 20 Number 1 Comparative study of intubating conditions after Rocuronium and Suxamethonium (study of 80 cases) K Bhati, V Parmar Citation K Bhati,
ISPUB.COM The Internet Journal of Anesthesiology Volume 20 Number 1 Comparative study of intubating conditions after Rocuronium and Suxamethonium (study of 80 cases) K Bhati, V Parmar Citation K Bhati,
PRETREATMENT WITH NON-DEPOLARIZING NEUROMUSCULAR BLOCKING AGENTS AND SUXAMETHONIUM-INDUCED INCREASES IN RESTING JAW TENSION IN CHILDREN
 British Journal of Anaesthesia 1990; 64: 577-581 PRETREATMENT WITH NON-DEPOLARIZING NEUROMUSCULAR BLOCKING AGENTS AND SUXAMETHONIUM-INDUCED INCREASES IN RESTING JAW TENSION IN CHILDREN C. E. SMITH, J.
British Journal of Anaesthesia 1990; 64: 577-581 PRETREATMENT WITH NON-DEPOLARIZING NEUROMUSCULAR BLOCKING AGENTS AND SUXAMETHONIUM-INDUCED INCREASES IN RESTING JAW TENSION IN CHILDREN C. E. SMITH, J.
Childhood Obesity: Anesthetic Implications
 Childhood Obesity: Anesthetic Implications The Changing Practice of Anesthesia 2015 UCSF Department of Anesthesia and Perioperative Care Marla Ferschl, MD Associate Professor of Anesthesia University of
Childhood Obesity: Anesthetic Implications The Changing Practice of Anesthesia 2015 UCSF Department of Anesthesia and Perioperative Care Marla Ferschl, MD Associate Professor of Anesthesia University of
British Journal ofanaesthesia 85 (2): (2000)
 British Journal ofanaesthesia 85 (2): 251-5 (2000) Comparison of succinylcholine with two doses of rocuronium using a new method of monitoring neuromuscular block at the laryngeal muscles by surface laryngeal
British Journal ofanaesthesia 85 (2): 251-5 (2000) Comparison of succinylcholine with two doses of rocuronium using a new method of monitoring neuromuscular block at the laryngeal muscles by surface laryngeal
A comparison of fentanyl, sufentanil, and remifentanil for fast-track cardiac anesthesia Engoren M, Luther G, Fenn-Buderer N
 A comparison of fentanyl, sufentanil, and remifentanil for fast-track cardiac anesthesia Engoren M, Luther G, Fenn-Buderer N Record Status This is a critical abstract of an economic evaluation that meets
A comparison of fentanyl, sufentanil, and remifentanil for fast-track cardiac anesthesia Engoren M, Luther G, Fenn-Buderer N Record Status This is a critical abstract of an economic evaluation that meets
HEMODYNAMIC PROFILE DURING LAPAROSCOPIC CHOLECYSTECTOMY VERSUS LAPAROSCOPIC BARIATRIC SURGERY
 HEMODYNAMIC PROFILE DURING LAPAROSCOPIC CHOLECYSTECTOMY VERSUS LAPAROSCOPIC BARIATRIC SURGERY - The Impact of Morbid Obesity - ABDELAZEEM ALI EL-DAWLATLY * Abstract The present study investigated the hemodynamic
HEMODYNAMIC PROFILE DURING LAPAROSCOPIC CHOLECYSTECTOMY VERSUS LAPAROSCOPIC BARIATRIC SURGERY - The Impact of Morbid Obesity - ABDELAZEEM ALI EL-DAWLATLY * Abstract The present study investigated the hemodynamic
Evaluation of intubation condition following administration of rocuronium in comparison to atracurium in paediatric patients
 Original Article Evaluation of intubation condition following administration of rocuronium in comparison to atracurium in paediatric Abdul Kuddus Khan 1*, MM Abdul Wadud 2, Azizul Gafur 3, Rafayetullah
Original Article Evaluation of intubation condition following administration of rocuronium in comparison to atracurium in paediatric Abdul Kuddus Khan 1*, MM Abdul Wadud 2, Azizul Gafur 3, Rafayetullah
TANAFFOS. Original Article. Key words: Magnesium sulfate, Lidocaine, Laryngoscopy, Intubation, Hemodynamics INTRODUCTION
 Original Article 2013 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran ISSN: 1735-0344 TANAFFOS Effects of Intravenous Magnesium Sulfate and Lidocaine on Hemodynamic Variables
Original Article 2013 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran ISSN: 1735-0344 TANAFFOS Effects of Intravenous Magnesium Sulfate and Lidocaine on Hemodynamic Variables
EPO 2 Evaluation of the preoxygenation in! morbidly obese. Optimal position and ventilation mode!
 EPO 2 Evaluation of the preoxygenation in! morbidly obese. Optimal position and ventilation mode! Antony Carrier-Boucher! PGY 3 Anesthesiology! Laval University! None! Conflict of interest! 2. Anesth Analg
EPO 2 Evaluation of the preoxygenation in! morbidly obese. Optimal position and ventilation mode! Antony Carrier-Boucher! PGY 3 Anesthesiology! Laval University! None! Conflict of interest! 2. Anesth Analg
POST-TETANIC COUNT AND PROFOUND NEUROMUSCULAR BLOCKADE WITH ATRACURIUM INFUSION IN PAEDIATRIC PATIENTS
 Br. J. Anaesth. (9), 60, 3-35 POST-TETANIC COUNT AND PROFOUND NEUROMUSCULAR BLOCKADE WITH ATRACURIUM INFUSION IN PAEDIATRIC PATIENTS S. A. RIDLEY AND D. J. HATCH Atracurium degrades rapidly and, because
Br. J. Anaesth. (9), 60, 3-35 POST-TETANIC COUNT AND PROFOUND NEUROMUSCULAR BLOCKADE WITH ATRACURIUM INFUSION IN PAEDIATRIC PATIENTS S. A. RIDLEY AND D. J. HATCH Atracurium degrades rapidly and, because
Running head: SUGAMMADEX AND MYASTHENIA GRAVIS 1
 Running head: SUGAMMADEX AND MYASTHENIA GRAVIS 1 Sugammadex in Patients with Myasthenia Gravis Jennifer A. Madsen University of Kansas SUGAMMADEX AND MYASTHENIA GRAVIS 2 Title of Proposed Research Project
Running head: SUGAMMADEX AND MYASTHENIA GRAVIS 1 Sugammadex in Patients with Myasthenia Gravis Jennifer A. Madsen University of Kansas SUGAMMADEX AND MYASTHENIA GRAVIS 2 Title of Proposed Research Project
200 mg/20 ml (10 mg/ml) in single-dose vials (3)
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use NIMBEX safely and effectively. See full prescribing information for NIMBEX. NIMBEX (cisatracurium
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use NIMBEX safely and effectively. See full prescribing information for NIMBEX. NIMBEX (cisatracurium
Neuromuscular block with vecuronium reduces the rapidly extracted auditory evoked potentials index during steady state anesthesia
 GENERAL ANESTHESIA 1017 Neuromuscular block with vecuronium reduces the rapidly extracted auditory evoked potentials index during steady state anesthesia [Un bloc neuromusculaire avec du vécuronium réduit
GENERAL ANESTHESIA 1017 Neuromuscular block with vecuronium reduces the rapidly extracted auditory evoked potentials index during steady state anesthesia [Un bloc neuromusculaire avec du vécuronium réduit
The Role of the Anaesthesiologist in the Perioperative Management of Preeclampsia. RA Dyer Interlaken 2017
 The Role of the Anaesthesiologist in the Perioperative Management of Preeclampsia RA Dyer Interlaken 2017 6 In preeclampsia - Understanding of pathophysiology Assessment of disease severity Prediction
The Role of the Anaesthesiologist in the Perioperative Management of Preeclampsia RA Dyer Interlaken 2017 6 In preeclampsia - Understanding of pathophysiology Assessment of disease severity Prediction
NEOSTIGMINE VERSUS SUGAMMADEX FOR REVERSAL OF NEUROMUSCULAR BLOCK
 EDITORIAL NEOSTIGMINE VERSUS SUGAMMADEX FOR REVERSAL OF NEUROMUSCULAR BLOCK Neostigmine is the classic acetylcholinesterase antagonist, which is widely used for reversal of neuromuscular block of all nondepolarising
EDITORIAL NEOSTIGMINE VERSUS SUGAMMADEX FOR REVERSAL OF NEUROMUSCULAR BLOCK Neostigmine is the classic acetylcholinesterase antagonist, which is widely used for reversal of neuromuscular block of all nondepolarising
International Journal of Medical and Health Sciences
 International Journal of Medical and Health Sciences Journal Home Page: http://www.ijmhs.net ISSN:2277-4505 Original article A Comparative Study Of Etomidate And Midazolam Induction In Patients Undergoing
International Journal of Medical and Health Sciences Journal Home Page: http://www.ijmhs.net ISSN:2277-4505 Original article A Comparative Study Of Etomidate And Midazolam Induction In Patients Undergoing
ANESTHESIA EXAM (four week rotation)
 SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
Ganglion blocking agents
 Ganglion blocking agents -out of date -Specifically act on the nicotinic receptors of both parasymphatetic and sympathetic ganglia - no selectivity toward PG or SG -These drugs are non-depolarizing, competitive
Ganglion blocking agents -out of date -Specifically act on the nicotinic receptors of both parasymphatetic and sympathetic ganglia - no selectivity toward PG or SG -These drugs are non-depolarizing, competitive
Comparison of Intubating Conditions of Succinylcholine and Rocuronium
 Comparison of Intubating Conditions of Succinylcholine and Rocuronium 1 Dr. Vaishali Kotambkar, 2 Dr. Sunil Tuljapure Abstract: The aim of study on neuromuscular drugs was to have nondepolarising muscle
Comparison of Intubating Conditions of Succinylcholine and Rocuronium 1 Dr. Vaishali Kotambkar, 2 Dr. Sunil Tuljapure Abstract: The aim of study on neuromuscular drugs was to have nondepolarising muscle
Hajime Iwasaki, MD Kenichi Takahoko, MD Shigeaki Otomo, MD Tomoki Sasakawa, MD Takayuki Kunisawa, MD, PhD Hiroshi Iwasaki, MD, PhD
 Can J Anesth/J Can Anesth (2013) 60:1222 1227 DOI 10.1007/s12630-013-0042-4 CASE REPORTS / CASE SERIES Monitoring of neuromuscular blockade in one muscle group alone may not reflect recovery of total muscle
Can J Anesth/J Can Anesth (2013) 60:1222 1227 DOI 10.1007/s12630-013-0042-4 CASE REPORTS / CASE SERIES Monitoring of neuromuscular blockade in one muscle group alone may not reflect recovery of total muscle
Comparison of Ease of Insertion and Hemodynamic Response to Lma with Propofol and Thiopentone.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IV (Dec. 2015), PP 22-30 www.iosrjournals.org Comparison of Ease of Insertion and Hemodynamic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IV (Dec. 2015), PP 22-30 www.iosrjournals.org Comparison of Ease of Insertion and Hemodynamic
Tracheal intubation after induction of anesthesia in children with propofol remifentanil or propofol-rocuronium
 854 REPORTS OF INVESTIGATION Tracheal intubation after induction of anesthesia in children with propofol remifentanil or propofol-rocuronium Ulla-Maija Klemola MD PhD, Arja Hiller MD PhD Purpose: To compare
854 REPORTS OF INVESTIGATION Tracheal intubation after induction of anesthesia in children with propofol remifentanil or propofol-rocuronium Ulla-Maija Klemola MD PhD, Arja Hiller MD PhD Purpose: To compare
Induction position for spinal anaesthesia: Sitting versus lateral position
 11 ORIGINAL ARTICLE Induction position for spinal anaesthesia: Sitting versus lateral position Khurrum Shahzad, Gauhar Afshan Abstract Objective: To compare the effect of induction position on block characteristics
11 ORIGINAL ARTICLE Induction position for spinal anaesthesia: Sitting versus lateral position Khurrum Shahzad, Gauhar Afshan Abstract Objective: To compare the effect of induction position on block characteristics
Materials and Methods
 Anesthesiology 2002; 97:616 21 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Duration of Anesthesia before Muscle Relaxant Injection Influences Level of Paralysis
Anesthesiology 2002; 97:616 21 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Duration of Anesthesia before Muscle Relaxant Injection Influences Level of Paralysis
Study Of Effects Of Varying Durations Of Pre-Oxygenation. J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh
 ISPUB.COM The Internet Journal of Anesthesiology Volume 20 Number 1 J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh Citation J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 20 Number 1 J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh Citation J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh.. The Internet
EVALUATION OF INTUBATING CONDITIONS WITH AND WITHOUT PRIMING DOSE OF ROCURONIUM BROMIDE
 EVALUATION OF INTUBATING CONDITIONS WITH AND WITHOUT PRIMING DOSE OF ROCURONIUM BROMIDE Revathy Jeevarathnam 1, Balasubramaniam Solaiappan 2 1Professor, Department of Anaesthesiology, Chengalpattu Medical
EVALUATION OF INTUBATING CONDITIONS WITH AND WITHOUT PRIMING DOSE OF ROCURONIUM BROMIDE Revathy Jeevarathnam 1, Balasubramaniam Solaiappan 2 1Professor, Department of Anaesthesiology, Chengalpattu Medical
Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006.
 Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006 Introduction Laparoscopic surgery started in the mid 1950s. In recent
Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006 Introduction Laparoscopic surgery started in the mid 1950s. In recent
ISSN X (Print) Research Article. *Corresponding author Kaushal RP
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2013; 1(6):943-950 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2013; 1(6):943-950 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
MD (Anaesthesiology) Title (Plan of Thesis) (Session )
 S.No. 1. COMPARATIVE STUDY OF CENTRAL VENOUS CANNULATION USING ULTRASOUND GUIDANCE VERSUS LANDMARK TECHNIQUE IN PAEDIATRIC CARDIAC PATIENT. 2. TO EVALUATE THE ABILITY OF SVV OBTAINED BY VIGILEO-FLO TRAC
S.No. 1. COMPARATIVE STUDY OF CENTRAL VENOUS CANNULATION USING ULTRASOUND GUIDANCE VERSUS LANDMARK TECHNIQUE IN PAEDIATRIC CARDIAC PATIENT. 2. TO EVALUATE THE ABILITY OF SVV OBTAINED BY VIGILEO-FLO TRAC
JMSCR Vol 04 Issue 01 Page January 2016
 www.jmscr.igmpublication.org Impact Factor 3.79 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i1.04 Haemodynamic Effects during Induction in
www.jmscr.igmpublication.org Impact Factor 3.79 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i1.04 Haemodynamic Effects during Induction in
POTENTIATION OF THE NEUROMUSCULAR BLOCKADE PRODUCED BY ALCURONIUM WITH HALOTHANE, ENFLURANE AND ISOFLURANE
 Br.J. Anaesth. (987), 9, 0-06 POTENTIATION OF THE NEUROMUSCULAR BLOCKADE PRODUCED BY ALCURONIUM WITH HALOTHANE, ENFLURANE AND ISOFLURANE S. J. KEENS, J. M. HUNTER, S. L. SNOWDON AND J. E. UTTING Volatile
Br.J. Anaesth. (987), 9, 0-06 POTENTIATION OF THE NEUROMUSCULAR BLOCKADE PRODUCED BY ALCURONIUM WITH HALOTHANE, ENFLURANE AND ISOFLURANE S. J. KEENS, J. M. HUNTER, S. L. SNOWDON AND J. E. UTTING Volatile
Anesthesia and Neuromuscular Blockade: A Guide for Hospital Pharmacists. Upon completion of this activity, participants will be better able to:
 Anesthesia and Neuromuscular Blockade: A Guide for Hospital Pharmacists EDUCATIONAL OBJECTIVES Upon completion of this activity, participants will be better able to: 1. Understand the use of neuromuscular
Anesthesia and Neuromuscular Blockade: A Guide for Hospital Pharmacists EDUCATIONAL OBJECTIVES Upon completion of this activity, participants will be better able to: 1. Understand the use of neuromuscular
DETERMINANTS OF THE REVERSAL TIME OF COMPETITIVE NEUROMUSCULAR BLOCK BY ANTICHOLINESTERASES
 British Journal of Anaesthesia 1991; 66: 469-45 DETERMINANTS OF THE REVERSAL TIME OF COMPETITIVE NEUROMUSCULAR BLOCK BY ANTICHOLINESTERASES G. H. BEEMER, A. R. BJORKSTEN, P. J. DAWSON, R. J. DAWSON, P.
British Journal of Anaesthesia 1991; 66: 469-45 DETERMINANTS OF THE REVERSAL TIME OF COMPETITIVE NEUROMUSCULAR BLOCK BY ANTICHOLINESTERASES G. H. BEEMER, A. R. BJORKSTEN, P. J. DAWSON, R. J. DAWSON, P.
P V Praveen Kumar 1*, P. Archana 2. Original Research Article. Abstract
 Original Research Article Comparative clinical study of attenuation of cardiovascular responses to laryngoscopy intubation diltiazem, lignocaine and combination of diltiazem and lignocaine P V Praveen
Original Research Article Comparative clinical study of attenuation of cardiovascular responses to laryngoscopy intubation diltiazem, lignocaine and combination of diltiazem and lignocaine P V Praveen
Materials and Methods
 Anesthesiology 2001; 95:96 101 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. The Corrugator Supercilii, Not the Orbicularis Oculi, Reflects Rocuronium Neuromuscular
Anesthesiology 2001; 95:96 101 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. The Corrugator Supercilii, Not the Orbicularis Oculi, Reflects Rocuronium Neuromuscular
Sugammadex: A Comprehensive Review of the Published Human Science, Including Renal Studies
 Sugammadex: A Comprehensive Review of the Published Human Science, Including Renal Studies Kelsey Martin, MD. CA3 Resident, Indiana University School of Medicine Department of Anesthesia Article Abstract
Sugammadex: A Comprehensive Review of the Published Human Science, Including Renal Studies Kelsey Martin, MD. CA3 Resident, Indiana University School of Medicine Department of Anesthesia Article Abstract
PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older)
 Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Rauf et al. The evidence for this effect is equivocal. Studies of volunteers and non-cardiac surgery patients have concluded that there is no toleranc
 British Journal of Anaesthesia 95 (5): 611 15 (2005) doi:10.1093/bja/aei237 Advance Access publication September 9, 2005 Remifentanil infusion in association with fentanyl propofol anaesthesia in patients
British Journal of Anaesthesia 95 (5): 611 15 (2005) doi:10.1093/bja/aei237 Advance Access publication September 9, 2005 Remifentanil infusion in association with fentanyl propofol anaesthesia in patients
COMPARISON OF SUFENTANIL-OXYGEN AND FENTANYL-OXYGEN ANAESTHESIA FOR CORONARY ARTERY BYPASS GRAFTING
 Br. J. Anaesth. (1988), 60, 530-535 COMPARISON OF SUFENTANIL-OXYGEN AND FENTANYL-OXYGEN ANAESTHESIA FOR CORONARY ARTERY BYPASS GRAFTING H. M. L. MATHEWS, G. FURNESS, I. W. CARSON, I. A. ORR, S. M. LYONS
Br. J. Anaesth. (1988), 60, 530-535 COMPARISON OF SUFENTANIL-OXYGEN AND FENTANYL-OXYGEN ANAESTHESIA FOR CORONARY ARTERY BYPASS GRAFTING H. M. L. MATHEWS, G. FURNESS, I. W. CARSON, I. A. ORR, S. M. LYONS
Sleep Apnea and ifficulty in Extubation. Jean Louis BOURGAIN May 15, 2016
 Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Use of the Intubating Laryngeal Mask Airway
 340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
DATE: 10 February 2016 CONTEXT AND POLICY ISSUES
 TITLE: Neuromuscular Monitoring for Patients Receiving Continuous Paralytic or Neuromuscular Blocking Agents: A Review of the Clinical Effectiveness and Guidelines DATE: 10 February 2016 CONTEXT AND POLICY
TITLE: Neuromuscular Monitoring for Patients Receiving Continuous Paralytic or Neuromuscular Blocking Agents: A Review of the Clinical Effectiveness and Guidelines DATE: 10 February 2016 CONTEXT AND POLICY
Neuromuscular blockade does not change the incidence or severity of pharyngolaryngeal discomfort after LMA anesthesia
 728 CARDIOTHORACIC ANESTHESIA, RESPIRATION AND AIRWAY Neuromuscular blockade does not change the incidence or severity of pharyngolaryngeal discomfort after LMA anesthesia [Le blocage neuromusculaire ne
728 CARDIOTHORACIC ANESTHESIA, RESPIRATION AND AIRWAY Neuromuscular blockade does not change the incidence or severity of pharyngolaryngeal discomfort after LMA anesthesia [Le blocage neuromusculaire ne
Hypertensives Emergency and Urgency
 Hypertensives Emergency and Urgency Budi Yuli Setianto Cardiology Divisision Department of Internal Medicine Faculty of Medicine UGM Sardjito Hospital Yogyakarta Background USA: Hypertension is 30% of
Hypertensives Emergency and Urgency Budi Yuli Setianto Cardiology Divisision Department of Internal Medicine Faculty of Medicine UGM Sardjito Hospital Yogyakarta Background USA: Hypertension is 30% of
= 0.002) 117 #!. 12, : = 0.45; P
 Background: Psychosocial factors governing the use of postoperative, intravenous patient-controlled analgesia (PCA) have received little attention in spite of the fact that PCA is the most common modality
Background: Psychosocial factors governing the use of postoperative, intravenous patient-controlled analgesia (PCA) have received little attention in spite of the fact that PCA is the most common modality
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Research Article. Shital S. Ahire 1 *, Shweta Mhambrey 1, Sambharana Nayak 2. Received: 22 July 2016 Accepted: 08 August 2016
 International Journal of Research in Medical Sciences Ahire SS et al. Int J Res Med Sci. 2016 Sep;4(9):3838-3844 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162824
International Journal of Research in Medical Sciences Ahire SS et al. Int J Res Med Sci. 2016 Sep;4(9):3838-3844 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162824
Onset of action and intubating conditions after administration of rocuronium or mivacurium in children
 79 Onset of action and intubating conditions after administration of rocuronium or mivacurium in children Papagiannopoulou Pinelopi, Sfyra Evaggelia, Georgiou Mary, Georgiadou Theodora, Kanakoudis Fotios
79 Onset of action and intubating conditions after administration of rocuronium or mivacurium in children Papagiannopoulou Pinelopi, Sfyra Evaggelia, Georgiou Mary, Georgiadou Theodora, Kanakoudis Fotios
POST-TETANIC COUNT AND INTENSE NEUROMUSCULAR BLOCKADE WITH VECURONIUM IN CHILDREN
 Br. J. Anaesth. (988), 6, 55-556 POST-TETANIC COUNT AND INTENSE NEUROMUSCULAR BLOCKADE WITH VECURONIUM IN CHILDREN S. A. RIDLEY AND N. BRAUDE Monitoring of profound neuromuscular blockade may be based
Br. J. Anaesth. (988), 6, 55-556 POST-TETANIC COUNT AND INTENSE NEUROMUSCULAR BLOCKADE WITH VECURONIUM IN CHILDREN S. A. RIDLEY AND N. BRAUDE Monitoring of profound neuromuscular blockade may be based
Ambulatory Anesthesia for the Obese Patient
 Ambulatory Anesthesia for the Obese Patient Disclosures I have nothing to disclose Brian M Keech, MD FAAP University of Colorado School of Medicine Director, Ambulatory Anesthesia Denver Health Medical
Ambulatory Anesthesia for the Obese Patient Disclosures I have nothing to disclose Brian M Keech, MD FAAP University of Colorado School of Medicine Director, Ambulatory Anesthesia Denver Health Medical
