The PAIN Pathway for the Management of Acute Coronary Syndrome
|
|
|
- Jared Wells
- 6 years ago
- Views:
Transcription
1 2 The PAIN Pathway for the Management of Acute Coronary Syndrome Eyal Herzog, Emad Aziz, and Mun K. Hong Acute coronary syndrome (ACS) subsumes a spectrum of clinical entities, ranging from unstable angina to ST-elevation myocardial infarction [1]. The management of ACS is deservedly scrutinized, as it accounts for 2 million hospitalizations and a remarkable 30% of all deaths in the Unites States each year [2]. Clinical guidelines on the management of ACS, which are based on clinical trials, have been updated and published [3, 4]. Large-scale registries the NRMI [5], CRUSADE [6], and GRACE [7] registries have consistently demonstrated a major gap between ACS management guidelines and their practical application in the real world. Accordingly, a major message that emerges from these quality-improvement registries is that there is an urgent need to incorporate the evidence-based guidelines into our daily management of ACS. In an attempt to achieve this goal, we have developed a new pathway for the management of ACS at our institution, St. Luke s Roosevelt Hospital Center (SLRHC), which is a university hospital of Columbia University College of Physicians and Surgeons. The necessity to develop such a pathway at our institution is compelling yet typical of the need at many similar medical centers. The evidence-based information obtained from the large-scale clinical trials and from the guidelines is increasingly complex. Specifically, it has become exceedingly difficult for all house staff and emergency room staff to grasp all of the subtleties in the management of ACS patients. To address this problem, we have developed a unified pathway for the management of patients presenting with acute chest pain or its equivalent. The pathway has been designated by the acronym PAIN (Priority risk, Advanced risk, Intermediate risk and Negative/low risk), which reflects a patient s most immediate risk stratification upon admission (Fig. 2.1). This risk stratification reflects a patient s 30-day risks for death and myocardial infarction after the initial ACS event. The PAIN pathway is color-coded (P, red; A, yellow; I, yellow; N, green) and will guide patient management according to a patient s risk stratification. These colors similar to the road traffic light code have been chosen as an easy reference for the provider about the sequential risk level of patients with ACS [8]. 9
2 10 E. Herzog et al. FIGURE 2.1. The PAIN pathway for the management of ACS.
3 2. The PAIN Pathway for the Management of ACS 11 FIGURE 2.2. Chest pain and chest pain equivalent symptoms. The Goals of the PAIN Pathway and a Road Map to this Acute Coronary Syndrome Book Initial Assessment of Patients with Chest Pain or Chest Pain Equivalent Patients who present to emergency departments with chest pain or chest pain equivalent will be enrolled into this pathway. Figure 2.2 shows the chest pain equivalent symptoms. The initial assessment is seen in Figure 2.3. A detailed description of emergency department assessment is provided in Chapter 5. All patients should have an electrocardiogram (ECG) performed within 10 minutes as well as detailed history and physical exam. Non-ACS chest pain should be excluded urgently. This includes aortic dissection, pericarditis and pericardial effusion, pulmonary emboli, aortic stenosis, and hypertrophic cardiomyopathy. If any of these emergency conditions is suspected, we recommend obtaining immediate echocardiogram or computed tomography (CT) and to treat accordingly. Our recommended initial laboratory tests include complete blood count, basic metabolic panel, cardiac markers (to include CPK, CPK-MB, troponin), BNP, PT, PTT, INR, magnesium, and a lipid profile. FIGURE 2.3. Initial assessment of patients with chest pain.
4 12 E. Herzog et al. Initial Management of PRIORITY Patients (Patients with ST-Elevation Myocardial Infarction) PRIORITY patients are those with symptoms of chest pain or chest pain equivalent lasting longer than 30 minutes with one of the following ECG criteria for acute myocardial infarction: 1. ST elevation 1 mm in two contiguous leads; or 2. New left bundle branch block; or 3. Acute posterior wall myocardial infarction (ST-segment depression in leads V 1 V 3 ). The initial treatment of these patients includes obtaining an intravenous line, providing oxygen, treating patients with oral aspirin (chewable 325 mg, stat), clopidogrel (300 mg or 600 mg loading dose), and intravenous beta-blocker (if no contraindication), heparin (unfractionated or enoxaparin), nitroglycerin, and oral high-dose statin (Fig. 2.4). A detailed dosing and the rationale for this management appear in Chapter 6. The key question for further management of these patients is the duration of the patients symptoms. For patients whose symptoms exceed 12 hours, presence of persistent or residual chest pain determines the next strategy. If there is no evidence of continued symptoms, these patients will be treated as if they had been risk stratified with the Advanced Risk group. For patients whose symptoms are less than 12 hours or with ongoing chest pain, the decision for further management is based on the availability of on-site FIGURE 2.4. The initial management of PRIORITY patients (patient with ST-elevation myocardial infarction).
5 2. The PAIN Pathway for the Management of ACS 13 FIGURE 2.5. Advanced management of PRIORITY myocardial infarction patients with expected door to balloon time of less than 90 minutes. angioplasty (PCI) capability with expected door to balloon time of less than 90 minutes or the presence of cardiogenic shock. A detailed discussion of cardiogenic shock appears in Chapter 13. Patients with expected door to balloon time of less than 90 minutes should be started on intravenous treatment of glycoprotein IIb/IIIa inhibitors and they should be transferred immediately to the cardiac catheterization lab for revascularization. The myocardial infarction (MI) team is activated for this group of patients (Fig. 2.5). At our institution, a single call made by the emergency department physician to the page operator activates the MI team, which includes the following health care providers: 1. The interventional cardiologist on-call 2. The director of the cardiac care unit (CCU) 3. The cardiology fellow on-call 4. The interventional cardiology fellow on-call 5. The cath lab nurse on-call 6. The cath lab technologist on-call 7. The CCU nursing manager on-call 8. The senior internal medicine resident on-call. Activating this group of people has been extremely successful at our institution and has reduced markedly our door to balloon time. These strategies have been recently shown to decrease door to balloon time in the range of 8 to 19 minutes [9].
6 14 E. Herzog et al. FIGURE 2.6. CCU management and secondary prevention for patients with PRIORITY myocardial infarction. For hospitals with no PCI capability or in situations when door to balloon time is expected to exceed 90 minutes, we recommend thrombolytic therapy if there are no contraindications. CCU Management and Secondary Prevention for Patients with PRIORITY Myocardial Infarction Patients with PRIORITY myocardial infarction should be admitted to the CCU (Fig. 2.6). A detailed description of CCU management appears in Chapter 6. All patients should have an echocardiogram to evaluate left ventricle systolic and diastolic function and to exclude valvular abnormality and pericardial involvement (as described in Chapter 14). We recommend a minimum CCU stay of 24 hours to exclude arrhythmia complication (as described in Chapters 16 to 18) or mechanical complication (as described in Chapter 11). For patients with no evidence of mechanical complications or significant arrhythmia, secondary prevention drugs should be started, including aspirin, clopidogrel, high-dose statin, beta-blocker, and angiotensin-converting enzyme (ACE) inhibitor or angiotensin receptor blocker. Most patients can be discharge within 48 hours with recommendation for lifestyle modification including exercise, weight and diet control, smoking cessation (Chapter 26), and cardiac rehabilitation. Secondary prevention drugs should be continued on discharge as discussed in Chapter 25. Management of Advanced Risk ACS Typical anginal symptoms are required to be present in patients, who will enroll into the Advanced Risk or the Intermediate Risk groups. These symptoms include: 1. Prolonged chest pain (>20 minutes) relieved by nitroglycerine or rest; 2. Chest pain at rest; or 3. Accelerated chest pain within 48 hours.
7 2. The PAIN Pathway for the Management of ACS 15 FIGURE 2.7. Risk stratification as Advanced Risk ACS. In order to qualify for the Advanced Risk group, patients must have either dynamic ST changes on the electrocardiogram (>0.5 mm) and/or elevated troponin (>0.2 ng/ml) (Fig. 2.7). A detailed description of the management of Advanced Risk patients appears in Chapter 7. We recommend that patients be admitted to the CCU and be treated with aspirin, clopidogrel, heparin, glycoprotein IIb/IIIa inhibitor, betablocker, statin, and nitroglycerin if there are no contraindications (Fig. 2.8). FIGURE 2.8. Management of patients with Advanced Risk ACS.
8 16 E. Herzog et al. FIGURE 2.9. Management of patients with Intermediate Risk ACS. These patients should have early cardiac catheterization within 12 to 48 hours and revascularization by PCI or coronary artery bypass surgery (CABG) if necessary. All patients should have an echocardiogram to evaluate left ventricular function. Recommendation for secondary prevention medication, lifestyle modification, and cardiac rehabilitation should be provided similar to the patients in the PRIORITY risk group (Fig. 2.6). Management of Intermediate Risk Group Both Intermediate Risk group and Advanced Risk patients present to the hospital with typical anginal symptoms. Compared with the Advanced Risk patients, the Immediate Risk patients do not have evidence of dynamic ST changes on the electrocardiogram or evidence of positive cardiac markers (see Chapter 8). These patients should be admitted to the telemetry floor and be given aspirin, heparin, and beta-blocker (Fig. 2.9). We recommend a minimum telemetry stay of 12 to 24 hours. If during this period of time there is evidence of dynamic ST changes on the electrocardiogram or evidence for positive cardiac markers, the patients should be treated as if they had been stratified to the Advanced Risk group. The Intermediate Risk group patients are assessed again for the following high risk features: 1. New or worsening heart failure symptoms; 2. Malignant ventricular arrhythmias; 3. Hemodynamic instability; or 4. Recent (<6 months) PCI or CABG.
9 2. The PAIN Pathway for the Management of ACS 17 If there is evidence of any of these high-risk features, we recommend to transfer the patient for cardiac catheterization within 12 to 48 hours and for revascularization by PCI or CABG if necessary. Patients with no evidence of high-risk features should be referred for cardiac imaging stress testing (stress echocardiography or stress nuclear test). Management of Negative or Low Risk Group Patients These patients have atypical symptoms and do not have significant ischemic ECG changes during pain and do not have elevated cardiac markers. These patients should be treated only with aspirin and given sublingual nitroglycerin if needed. If a decision was made to admit them to the hospital, they should be admitted to a chest pain unit or to a regular medical floor. They should be followed up for 12 to 24 hours with repeated ECG and cardiac markers (Fig. 2.10). If there is evidence of evolving ST changes on the electrocardiogram or evidence of positive cardiac markers, the patients would be treated aggressively as with the Advanced Risk patients. If there are no significant ECG changes and all cardiac markers are negative, we recommend cardiac imaging stress testing (by stress echocardiography or stress nuclear test) (Fig. 2.11). Evidence of significant ischemia on any of these stress imaging modalities will be followed by a referral for cardiac catheterization. FIGURE Initial management of patients with Negative or Low Risk ACS.
10 18 E. Herzog et al. FIGURE Risk stratification of Low Risk patients by using cardiac imaging stress testing. FIGURE Primary prevention for Low Risk patients. If there is no evidence of significant ischemia on stress testing, the patients will be discharged home with a recommendation for risk-factor modification to include primary prevention medication and lifestyle modification (Fig. 2.12). In summary, we believe that this comprehensive yet simple pathway will be able to bridge the gap between the complex evidence-based guidelines and practical management of patients with ACS. References 1. Herzog E, Saint-Jacques H, Rozanski A. The PAIN pathway as a tool to bridge the gap between evidence and management of acute coronary syndrome. Crit Pathways Cardiol 2004;3:20 24.
11 2. The PAIN Pathway for the Management of ACS Califf RM. Acute coronary syndromes: ACS essentials. Royal Oak, MI: Physicians Press; Braunwald E, Antman EM, Beasley JW, et al. ACC/AHA guidelines update for the management of patients with unstable angina and non-st elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on the Management of Patients with Unstable Angina). J Am Coll Cardiol 2000;36: Antman EM, Anbe DT, Armstrong PW, et al. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction. J Am Coll Cardiol 2004;44: Spencer FA, Meyer TE, Gore JM, et al. Heterogeneity in the management and outcomes of patients with acute myocardial infarction complicated by heart failure: the National Registry of Myocardial Infarction. Circulation 2002;105: Hoekstra JW, Pollack CV Jr, Roe MY, et al. Improving the care of patients with non- ST-elevation acute coronary syndromes in the emergency department: the CRUSADE initiative. Acad Emerg Med 2002;9: Fox KA, Goodman SG, Klein W, et al. Management of acute coronary syndromes. Variations in practice and outcomes; findings from the Global Registry of Acute Coronary Events (GRACE). Eur Heart J 2002;23: Saint-Jacques H, Burroughs VJ, Watowska J, et al. Acute coronary syndrome critical pathway: chest PAIN caremap a qualitative research study-provider-level intervention. Crit Pathways Cardiol 2005;4: Bradley EH, Herrin J, Wang YF, et al. Strategies for reducing the door-to-balloon time in acute myocardial infarction. N Engl J Med 2006;355:
12
Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA
 Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA Case History A 50-year-old man with type 1 diabetes mellitus and hypertension presents after experiencing 1 hour of midsternal chest pain that began after
Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA Case History A 50-year-old man with type 1 diabetes mellitus and hypertension presents after experiencing 1 hour of midsternal chest pain that began after
Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist. Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI
 Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist physician Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI Outcome objectives of the discussion: At the end of the
Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist physician Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI Outcome objectives of the discussion: At the end of the
CLINICIAN INTERVIEW RECOGNIZING ACS AND STRATIFYING RISK IN PRIMARY CARE. An interview with A. Michael Lincoff, MD, and Eric R. Bates, MD, FACC, FAHA
 RECOGNIZING ACS AND STRATIFYING RISK IN PRIMARY CARE An interview with A. Michael Lincoff, MD, and Eric R. Bates, MD, FACC, FAHA Dr Lincoff is an interventional cardiologist and the Vice Chairman for Research
RECOGNIZING ACS AND STRATIFYING RISK IN PRIMARY CARE An interview with A. Michael Lincoff, MD, and Eric R. Bates, MD, FACC, FAHA Dr Lincoff is an interventional cardiologist and the Vice Chairman for Research
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
4. Which survey program does your facility use to get your program designated by the state?
 STEMI SURVEY Please complete one survey for each TCD designation you have in your facility. There would be a maximum of three surveys completed if your facility was designated as a trauma, stroke and STEMI
STEMI SURVEY Please complete one survey for each TCD designation you have in your facility. There would be a maximum of three surveys completed if your facility was designated as a trauma, stroke and STEMI
Acute Coronary Syndrome. Emergency Department Updated Jan. 2017
 Acute Coronary Syndrome Emergency Department Updated Jan. 2017 Goals and Objectives To reduce mortality and morbidity for people who have cardiovascular disease, with a focus on those who experience an
Acute Coronary Syndrome Emergency Department Updated Jan. 2017 Goals and Objectives To reduce mortality and morbidity for people who have cardiovascular disease, with a focus on those who experience an
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Severe Hypertension. Pre-referral considerations: 1. BP of arm and Leg 2. Ambulatory BP 3. Renal causes
 Severe Hypertension *Prior to making a referral, call office or Doc Halo, to speak with a Cardiologist or APP to discuss patient and possible treatment options. Please only contact the patient's cardiologist.
Severe Hypertension *Prior to making a referral, call office or Doc Halo, to speak with a Cardiologist or APP to discuss patient and possible treatment options. Please only contact the patient's cardiologist.
Acute Coronary Syndromes
 Overview Acute Coronary Syndromes Rabeea Aboufakher, MD, FACC, FSCAI Section Chief of Cardiology Altru Health System Grand Forks, ND Epidemiology Pathophysiology Clinical features and diagnosis STEMI management
Overview Acute Coronary Syndromes Rabeea Aboufakher, MD, FACC, FSCAI Section Chief of Cardiology Altru Health System Grand Forks, ND Epidemiology Pathophysiology Clinical features and diagnosis STEMI management
Appendix: ACC/AHA and ESC practice guidelines
 Appendix: ACC/AHA and ESC practice guidelines Definitions for guideline recommendations and level of evidence Recommendation Class I Class IIa Class IIb Class III Level of evidence Level A Level B Level
Appendix: ACC/AHA and ESC practice guidelines Definitions for guideline recommendations and level of evidence Recommendation Class I Class IIa Class IIb Class III Level of evidence Level A Level B Level
ST-elevation myocardial infarctions (STEMIs)
 Guidelines for Treating STEMI: Case-Based Questions As many as 25% of eligible patients presenting with STEMI do not receive any form of reperfusion therapy. The ACC/AHA guidelines highlight steps to improve
Guidelines for Treating STEMI: Case-Based Questions As many as 25% of eligible patients presenting with STEMI do not receive any form of reperfusion therapy. The ACC/AHA guidelines highlight steps to improve
Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg
 Rotation: or: Faculty: Coronary Care Unit (CVICU) Dr. Jeff Rottman Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg Duty Hours: Mon Fri, 7 AM to 7 PM, weekend call shared with consult
Rotation: or: Faculty: Coronary Care Unit (CVICU) Dr. Jeff Rottman Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg Duty Hours: Mon Fri, 7 AM to 7 PM, weekend call shared with consult
Acute Myocardial Infarction
 Acute Myocardial Infarction Hafeza Shaikh, DO, FACC, RPVI Lourdes Cardiology Services Asst.Program Director, Cardiology Fellowship Associate Professor, ROWAN-SOM Acute Myocardial Infarction Definition:
Acute Myocardial Infarction Hafeza Shaikh, DO, FACC, RPVI Lourdes Cardiology Services Asst.Program Director, Cardiology Fellowship Associate Professor, ROWAN-SOM Acute Myocardial Infarction Definition:
DISCUSSION QUESTION - 1
 CASE PRESENTATION 87 year old male No past history of diabetes, HTN, dyslipidemia or smoking Very active Medications: omeprazole for heart burn Admitted because of increasing retrosternal chest pressure
CASE PRESENTATION 87 year old male No past history of diabetes, HTN, dyslipidemia or smoking Very active Medications: omeprazole for heart burn Admitted because of increasing retrosternal chest pressure
Acute Myocardial Infarction. Willis E. Godin D.O., FACC
 Acute Myocardial Infarction Willis E. Godin D.O., FACC Acute Myocardial Infarction Definition: Decreased delivery of oxygen and nutrients to the myocardium Myocardial tissue necrosis causing irreparable
Acute Myocardial Infarction Willis E. Godin D.O., FACC Acute Myocardial Infarction Definition: Decreased delivery of oxygen and nutrients to the myocardium Myocardial tissue necrosis causing irreparable
Educational Goals and Objectives for Rotations on: Cardio Inpatient
 Educational Goals and Objectives for Rotations on: Cardio Inpatient Residents will rotate through cardiology inpatient rotations to: Develop skills to evaluate and manage patients with diseases of the
Educational Goals and Objectives for Rotations on: Cardio Inpatient Residents will rotate through cardiology inpatient rotations to: Develop skills to evaluate and manage patients with diseases of the
Non ST Elevation-ACS. Michael W. Cammarata, MD
 Non ST Elevation-ACS Michael W. Cammarata, MD Case Presentation 65 year old man PMH: CAD s/p stent in 2008 HTN HLD Presents with chest pressure, substernally and radiating to the left arm and jaw, similar
Non ST Elevation-ACS Michael W. Cammarata, MD Case Presentation 65 year old man PMH: CAD s/p stent in 2008 HTN HLD Presents with chest pressure, substernally and radiating to the left arm and jaw, similar
STEMI, Non-STEMI, Chest Pain?
 Minnesota Chest Pain / Acute Coronary Syndrome Tool-Kit Patient with Chest Pain Or Potential Acute Coronary Syndrome STEMI, n-stemi, Chest Pain? Follow MN STEMI Guideline Follow MN n-stemi Guideline Follow
Minnesota Chest Pain / Acute Coronary Syndrome Tool-Kit Patient with Chest Pain Or Potential Acute Coronary Syndrome STEMI, n-stemi, Chest Pain? Follow MN STEMI Guideline Follow MN n-stemi Guideline Follow
APPENDIX F: CASE REPORT FORM
 APPENDIX F: CASE REPORT FORM Instruction: Complete this form to notify all ACS admissions at your centre to National Cardiovascular Disease Registry. Where check boxes are provided, check ( ) one or more
APPENDIX F: CASE REPORT FORM Instruction: Complete this form to notify all ACS admissions at your centre to National Cardiovascular Disease Registry. Where check boxes are provided, check ( ) one or more
University of Wisconsin - Madison Cardiovascular Medicine Fellowship Program UW CCU Rotation Goals and Objectives Goals
 Goals Learn to coordinate a variety of data from multiple cardiovascular sub-disciplines, e.g. catheterization laboratory, hemodynamic study, non-invasive imaging, nuclear, electrophysiologic, and in combination
Goals Learn to coordinate a variety of data from multiple cardiovascular sub-disciplines, e.g. catheterization laboratory, hemodynamic study, non-invasive imaging, nuclear, electrophysiologic, and in combination
Cindy Stephens, MSN, ANP Kelly Walker, MS, ACNP Peter Cohn, MD, FACC
 Cindy Stephens, MSN, ANP Kelly Walker, MS, ACNP Peter Cohn, MD, FACC Define Acute Coronary syndromes Explain the Cause Assessment, diagnosis and therapy Reperfusion for STEMI Complications to look for
Cindy Stephens, MSN, ANP Kelly Walker, MS, ACNP Peter Cohn, MD, FACC Define Acute Coronary syndromes Explain the Cause Assessment, diagnosis and therapy Reperfusion for STEMI Complications to look for
Acute Coronary Syndrome. Sonny Achtchi, DO
 Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
Continuing Medical Education Post-Test
 Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
Results of Ischemic Heart Disease
 Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Chest Pain Acute Coronary Syndrome Version 4 4/10/17 This order set is designed to be used with an admission set or for a patient already admitted
 Patient Name: Diagnosis: Allergies with reaction type: Chest Pain Acute Coronary Syndrome Version 4 4/10/17 This order set is designed to be used with an admission set or for a patient already admitted
Patient Name: Diagnosis: Allergies with reaction type: Chest Pain Acute Coronary Syndrome Version 4 4/10/17 This order set is designed to be used with an admission set or for a patient already admitted
UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME. DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18
 UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18 INTRODUCTION The clinical entities that comprise acute coronary syndromes (ACS)-ST-segment
UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18 INTRODUCTION The clinical entities that comprise acute coronary syndromes (ACS)-ST-segment
UCLA Chest Pain and Unstable Angina Patient Management Guideline
 UCLA Clinical Practice Guideline-2001 1 I. Introduction UCLA Chest Pain and Unstable Angina Patient Management Guideline Unstable angina and acute myocardial infarction most often result from disruption
UCLA Clinical Practice Guideline-2001 1 I. Introduction UCLA Chest Pain and Unstable Angina Patient Management Guideline Unstable angina and acute myocardial infarction most often result from disruption
Assessing Cardiac Risk in Noncardiac Surgery. Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington
 Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Acute Coronary Syndrome in Phrae Hospital
 Acute Coronary Syndrome in Phrae Hospital Cardiovascular Unit, Department of Medicine, Phrae hospital, Phrae Thailand. Objective: To study the epidemiology, management and outcome of patients with acute
Acute Coronary Syndrome in Phrae Hospital Cardiovascular Unit, Department of Medicine, Phrae hospital, Phrae Thailand. Objective: To study the epidemiology, management and outcome of patients with acute
The importance of follow-up after a cardiac event: CARDIAC REHABILITATION. Dr. Guy Letcher
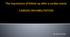 The importance of follow-up after a cardiac event: CARDIAC REHABILITATION Dr. Guy Letcher The National Medicare Experience Mortality After Angioplasty 225,915 patients Mortality After Bypass Surgery 357,885
The importance of follow-up after a cardiac event: CARDIAC REHABILITATION Dr. Guy Letcher The National Medicare Experience Mortality After Angioplasty 225,915 patients Mortality After Bypass Surgery 357,885
Acute Coronary Syndrome. Cindy Baker, MD FACC Director Peripheral Vascular Interventions Division of Cardiovascular Medicine
 Acute Coronary Syndrome Cindy Baker, MD FACC Director Peripheral Vascular Interventions Division of Cardiovascular Medicine Topics Timing is everything So many drugs to choose from What s a MINOCA? 2 Acute
Acute Coronary Syndrome Cindy Baker, MD FACC Director Peripheral Vascular Interventions Division of Cardiovascular Medicine Topics Timing is everything So many drugs to choose from What s a MINOCA? 2 Acute
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Awealth of research in acute coronary syndrome
 CLINICAL TRIAL SUPPORT OF THE USE OF CRITICAL PATHWAYS IN IMPROVING PATIENT OUTCOMES Judy W. M. Cheng, PharmD, MPH, BCPS, FCCP * ABSTRACT Acute coronary syndrome (ACS) is a common condition encountered
CLINICAL TRIAL SUPPORT OF THE USE OF CRITICAL PATHWAYS IN IMPROVING PATIENT OUTCOMES Judy W. M. Cheng, PharmD, MPH, BCPS, FCCP * ABSTRACT Acute coronary syndrome (ACS) is a common condition encountered
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina
 Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Program Metrics. New Unique ID. Old Unique ID. Metric Set Metric Name Description. Old Metric Name
 Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
Acute coronary syndrome (ACS) is a potentially
 DIAGNOSING ACUTE CORONARY SYNDROME AND DETERMINING PATIENT RISK Edith A. Nutescu, PharmD* ABSTRACT Acute coronary syndrome is a form of coronary artery disease and has a broad range of clinical presentations.
DIAGNOSING ACUTE CORONARY SYNDROME AND DETERMINING PATIENT RISK Edith A. Nutescu, PharmD* ABSTRACT Acute coronary syndrome is a form of coronary artery disease and has a broad range of clinical presentations.
Practitioner Education Course
 2015 Practitioner Education Course ST Elevation Myocardial Infarction 2 Pathology Concept of vulnerable plaque Mild Atheroma Diagnosis IVUS OCT 3 Diagnosis This is based on : Clinical History ECG Changes.
2015 Practitioner Education Course ST Elevation Myocardial Infarction 2 Pathology Concept of vulnerable plaque Mild Atheroma Diagnosis IVUS OCT 3 Diagnosis This is based on : Clinical History ECG Changes.
Ischemic Heart Disease Interventional Treatment
 Ischemic Heart Disease Interventional Treatment Cardiac Catheterization Laboratory Procedures (N = 11,61) is a regional and national referral center for percutaneous coronary intervention (PCI). A total
Ischemic Heart Disease Interventional Treatment Cardiac Catheterization Laboratory Procedures (N = 11,61) is a regional and national referral center for percutaneous coronary intervention (PCI). A total
Coronary Artery Disease: Revascularization (Teacher s Guide)
 Stephanie Chan, M.D. Updated 3/15/13 2008-2013, SCVMC (40 minutes) I. Objectives Coronary Artery Disease: Revascularization (Teacher s Guide) To review the evidence on whether percutaneous coronary intervention
Stephanie Chan, M.D. Updated 3/15/13 2008-2013, SCVMC (40 minutes) I. Objectives Coronary Artery Disease: Revascularization (Teacher s Guide) To review the evidence on whether percutaneous coronary intervention
Unstable angina and NSTEMI
 Issue date: March 2010 Unstable angina and NSTEMI The early management of unstable angina and non-st-segment-elevation myocardial infarction This guideline updates and replaces recommendations for the
Issue date: March 2010 Unstable angina and NSTEMI The early management of unstable angina and non-st-segment-elevation myocardial infarction This guideline updates and replaces recommendations for the
Acute Coronary Syndrome
 Acute Coronary Syndrome Clinical Manifestation of CAD Silent Ischemia/asymptomatic Stable Angina Acute Coronary Syndrome (Non- STEMI/UA and STEMI) Arrhythmias Heart Failure Sudden Death Pain patterns with
Acute Coronary Syndrome Clinical Manifestation of CAD Silent Ischemia/asymptomatic Stable Angina Acute Coronary Syndrome (Non- STEMI/UA and STEMI) Arrhythmias Heart Failure Sudden Death Pain patterns with
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM. General Instructions: ID NUMBER: FORM NAME: H F A DATE: 10/13/2017 VERSION: CONTACT YEAR NUMBER:
 ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
2018 HPN Provider Summary Guide. Adult Cardiology Patients (18 Years and Older) Referral Guidelines
 12.2 CARDIOLOGY REFERRAL GUIDELINES Contracted Group: Southwest Medical Associates For Appointments: 888 S. Rancho Las Vegas, NV 89109 Phone: (702) 877-8654 Fax: (702) 242-7998 Adult Cardiology Patients
12.2 CARDIOLOGY REFERRAL GUIDELINES Contracted Group: Southwest Medical Associates For Appointments: 888 S. Rancho Las Vegas, NV 89109 Phone: (702) 877-8654 Fax: (702) 242-7998 Adult Cardiology Patients
Measuring Natriuretic Peptides in Acute Coronary Syndromes
 Measuring Natriuretic Peptides in Acute Coronary Syndromes Peter A. McCullough, MD, MPH, FACC, FACP, FAHA, FCCP Consultant Cardiologist Chief Academic and Scientific Officer St. John Providence Health
Measuring Natriuretic Peptides in Acute Coronary Syndromes Peter A. McCullough, MD, MPH, FACC, FACP, FAHA, FCCP Consultant Cardiologist Chief Academic and Scientific Officer St. John Providence Health
Disclosures. Inpatient Management of Non-ST Elevation Acute Coronary Syndromes. Edward McNulty MD, FACC. None
 Inpatient Management of Non-ST Elevation Acute Coronary Syndromes Edward McNulty MD, FACC Assistant Clinical Professor UCSF Director, SF VAMC Cardiac Catheterization Laboratory Disclosures None New Guidelines
Inpatient Management of Non-ST Elevation Acute Coronary Syndromes Edward McNulty MD, FACC Assistant Clinical Professor UCSF Director, SF VAMC Cardiac Catheterization Laboratory Disclosures None New Guidelines
Management of Acute Myocardial Infarction
 Management of Acute Myocardial Infarction Prof. Hossam Kandil Professor of Cardiology Cairo University ST Elevation Acute Myocardial Infarction Aims Of Management Emergency care (Pre-hospital) Early care
Management of Acute Myocardial Infarction Prof. Hossam Kandil Professor of Cardiology Cairo University ST Elevation Acute Myocardial Infarction Aims Of Management Emergency care (Pre-hospital) Early care
Transfer in D2B. Scott D Friedman, MD FACC Medical Director, Cardiology Services Shore Health System of Maryland. The Problem
 Transfer in D2B Scott D Friedman, MD FACC Medical Director, Cardiology Services Shore Health System of Maryland The Problem NRMI-5: North Carolina, July 2003- June 2004 NC Nation Guidelines N 2,738 79,927
Transfer in D2B Scott D Friedman, MD FACC Medical Director, Cardiology Services Shore Health System of Maryland The Problem NRMI-5: North Carolina, July 2003- June 2004 NC Nation Guidelines N 2,738 79,927
Angina Luis Tulloch, MD 03/27/2012
 Angina Luis Tulloch, MD 03/27/2012 Acute coronary syndromes ACS STE > 1 mm, new LBBB* Increased cardiac enzymes STEMI Yes Yes NSTEMI No Yes UA No No *Recognize Wellen s sign/syndrome, posterior wall MI,
Angina Luis Tulloch, MD 03/27/2012 Acute coronary syndromes ACS STE > 1 mm, new LBBB* Increased cardiac enzymes STEMI Yes Yes NSTEMI No Yes UA No No *Recognize Wellen s sign/syndrome, posterior wall MI,
New Guidelines for Evaluating Acute Coronary Syndrome
 New Guidelines for Evaluating Acute Coronary Syndrome The American College of Cardiology and the American Heart Association [Clinician Reviews 11(1):73-86, 2001. 2001 Clinicians Publishing Group] Introduction
New Guidelines for Evaluating Acute Coronary Syndrome The American College of Cardiology and the American Heart Association [Clinician Reviews 11(1):73-86, 2001. 2001 Clinicians Publishing Group] Introduction
Acute Coronary Syndrome (ACS) Initial Evaluation and Management
 Acute Coronary Syndrome (ACS) Initial Evaluation and Management Symptoms of Possible ACS Chest discomfort with or without radiation to the arm(s), jaw, or epigastrium Short of breath Weakness Diaphoresis
Acute Coronary Syndrome (ACS) Initial Evaluation and Management Symptoms of Possible ACS Chest discomfort with or without radiation to the arm(s), jaw, or epigastrium Short of breath Weakness Diaphoresis
Exhibit EP16.h University of Virginia Medical Center Clinical Decision Tool
 TITLE: Emergency Management for Suspicion of Cardiac Event PURPOSE: Increasingly, patients have multiple morbidities and are at risk of adverse events related or unrelated to the condition for which they
TITLE: Emergency Management for Suspicion of Cardiac Event PURPOSE: Increasingly, patients have multiple morbidities and are at risk of adverse events related or unrelated to the condition for which they
B. Paudel *, 1, K. Paudel* *Department of Medicine, Gandaki Medical College - Charak Hospital, Pokhara, Nepal 1
 Original Article: Western Nepal acute coronary syndrome (WestNP-ACS) registry: Characteristics, management and in- hospital outcome of patients admitted with acute coronary syndrome in western Nepal. B.
Original Article: Western Nepal acute coronary syndrome (WestNP-ACS) registry: Characteristics, management and in- hospital outcome of patients admitted with acute coronary syndrome in western Nepal. B.
ST-segment Elevation Myocardial Infarction (STEMI): Optimal Antiplatelet and Anti-thrombotic Therapy in the Emergency Department
 ST-segment Elevation Myocardial Infarction (STEMI): Optimal Antiplatelet and Anti-thrombotic Therapy in the Emergency Department decision-making. They have become the cornerstone of many ED protocols for
ST-segment Elevation Myocardial Infarction (STEMI): Optimal Antiplatelet and Anti-thrombotic Therapy in the Emergency Department decision-making. They have become the cornerstone of many ED protocols for
Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year
![Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year](/thumbs/76/74263761.jpg) PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
CHEST PAIN CDU INCLUSION CRITERIA
 CHEST PAIN CDU INCLUSION CRITERIA No clinical criteria for ACS Stable vital signs Initial ECG and cardiac biomarkers not consistent with ACS Low to intermediate ACS risk (HEART score 0-6) [Ref 1, 2] Plan
CHEST PAIN CDU INCLUSION CRITERIA No clinical criteria for ACS Stable vital signs Initial ECG and cardiac biomarkers not consistent with ACS Low to intermediate ACS risk (HEART score 0-6) [Ref 1, 2] Plan
Life Science Journal 2016;13(5) Acute Coronary Syndrome Process In Geriatric Population: One Year Follow-Up Study
 Acute Coronary Syndrome Process In Geriatric Population: One Year Follow-Up Study Samim Emet, MD 1, Fatih Akdogan 2, Yucel Arman 2, Murat Kose, MD 3, Basak Saracoglu, MD 4, Tufan Tukek, MD 3 1 Istanbul
Acute Coronary Syndrome Process In Geriatric Population: One Year Follow-Up Study Samim Emet, MD 1, Fatih Akdogan 2, Yucel Arman 2, Murat Kose, MD 3, Basak Saracoglu, MD 4, Tufan Tukek, MD 3 1 Istanbul
Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008.
 Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008. ST Elevation Myocardial Infarction (STEMI)-Acute Coronary Syndrome Guidelines:
Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008. ST Elevation Myocardial Infarction (STEMI)-Acute Coronary Syndrome Guidelines:
Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines)
 Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines) Authors: Dr. M. Love, Dr. I. Bata, K. Harrigan
Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines) Authors: Dr. M. Love, Dr. I. Bata, K. Harrigan
Objectives. Acute Coronary Syndromes; The Nuts and Bolts. Overview. Quick quiz.. How dose the plaque start?
 Objectives Acute Coronary Syndromes; The Nuts and Bolts Michael P. Gulseth, Pharm. D., BCPS Pharmacotherapy II Spring 2006 Compare and contrast pathophysiology of unstable angina (UA), non-st segment elevation
Objectives Acute Coronary Syndromes; The Nuts and Bolts Michael P. Gulseth, Pharm. D., BCPS Pharmacotherapy II Spring 2006 Compare and contrast pathophysiology of unstable angina (UA), non-st segment elevation
Ischemic Heart Disease Interventional Treatment
 Ischemic Heart Disease Interventional Treatment Cardiac Catheterization Laboratory Procedures (N = 89) is a regional and national referral center for percutaneous coronary intervention (PCI). A total of
Ischemic Heart Disease Interventional Treatment Cardiac Catheterization Laboratory Procedures (N = 89) is a regional and national referral center for percutaneous coronary intervention (PCI). A total of
Improving the Outcomes of
 Improving the Outcomes of STEMI Shelley Valaire, ACP; and Robert Welsh, MD, FRCPC Presented at the University of Alberta s 6th Annual Cardiology Update for General Practitioners and Internists, Edmonton,
Improving the Outcomes of STEMI Shelley Valaire, ACP; and Robert Welsh, MD, FRCPC Presented at the University of Alberta s 6th Annual Cardiology Update for General Practitioners and Internists, Edmonton,
2010 ACLS Guidelines. Primary goals of therapy for patients
 2010 ACLS Guidelines Part 10: Acute Coronary Syndrome Present : 內科 R1 鍾伯欣 Supervisor: F1 吳亮廷 991110 Primary goals of therapy for patients of ACS Reduce the amount of myocardial necrosis that occurs in
2010 ACLS Guidelines Part 10: Acute Coronary Syndrome Present : 內科 R1 鍾伯欣 Supervisor: F1 吳亮廷 991110 Primary goals of therapy for patients of ACS Reduce the amount of myocardial necrosis that occurs in
Percutaneous Coronary Interventions Without On-site Cardiac Surgery
 Percutaneous Coronary Interventions Without On-site Cardiac Surgery Hassan Al Zammar, MD,FESC Consultant & Interventional Cardiologist Head of Cardiology Department European Gaza Hospital Palestine European
Percutaneous Coronary Interventions Without On-site Cardiac Surgery Hassan Al Zammar, MD,FESC Consultant & Interventional Cardiologist Head of Cardiology Department European Gaza Hospital Palestine European
Acute coronary syndromes
 Acute coronary syndromes 1 Acute coronary syndromes Acute coronary syndromes results primarily from diminished myocardial blood flow secondary to an occlusive or partially occlusive coronary artery thrombus.
Acute coronary syndromes 1 Acute coronary syndromes Acute coronary syndromes results primarily from diminished myocardial blood flow secondary to an occlusive or partially occlusive coronary artery thrombus.
An update on the management of UA / NSTEMI. Michael H. Crawford, MD
 An update on the management of UA / NSTEMI Michael H. Crawford, MD New ACC/AHA Guidelines 2007 What s s new in the last 5 years CT imaging advances Ascendancy of troponin and BNP Clarification of ACEI/ARB
An update on the management of UA / NSTEMI Michael H. Crawford, MD New ACC/AHA Guidelines 2007 What s s new in the last 5 years CT imaging advances Ascendancy of troponin and BNP Clarification of ACEI/ARB
Prehospital and Hospital Care of Acute Coronary Syndrome
 Ischemic Heart Diseases Prehospital and Hospital Care of Acute Coronary Syndrome JMAJ 46(8): 339 346, 2003 Katsuo KANMATSUSE* and Ikuyoshi WATANABE** * Professor, Second Internal Medicine, Nihon University,
Ischemic Heart Diseases Prehospital and Hospital Care of Acute Coronary Syndrome JMAJ 46(8): 339 346, 2003 Katsuo KANMATSUSE* and Ikuyoshi WATANABE** * Professor, Second Internal Medicine, Nihon University,
University of Wisconsin - Madison Cardiovascular Medicine Fellowship Program UW CICU Rotation Goals and Objectives
 Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Belinda Green, Cardiologist, SDHB, 2016
 Acute Coronary syndromes All STEMI ALL Non STEMI Unstable angina Belinda Green, Cardiologist, SDHB, 2016 Thrombus in proximal LAD Underlying pathophysiology Be very afraid for your patient Wellens
Acute Coronary syndromes All STEMI ALL Non STEMI Unstable angina Belinda Green, Cardiologist, SDHB, 2016 Thrombus in proximal LAD Underlying pathophysiology Be very afraid for your patient Wellens
Safety of Single- Versus Multi-vessel Angioplasty for Patients with AMI and Multi-vessel CAD
 Safety of Single- Versus Multi-vessel Angioplasty for Patients with AMI and Multi-vessel CAD Mun K. Hong, MD Associate Professor of Medicine Director, Cardiovascular Intervention and Research Weill Cornell
Safety of Single- Versus Multi-vessel Angioplasty for Patients with AMI and Multi-vessel CAD Mun K. Hong, MD Associate Professor of Medicine Director, Cardiovascular Intervention and Research Weill Cornell
Utilization and Impact of Pre-Hospital Electrocardiograms for Patients With Acute ST-Segment Elevation Myocardial Infarction
 Journal of the American College of Cardiology Vol. 53, No. 2, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.09.030
Journal of the American College of Cardiology Vol. 53, No. 2, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.09.030
My Patient Needs a Stress Test
 My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
UCLA CHEST PAIN AND ACS PATIENT MANAGEMENT GUIDELINE UCLA Medical Center Los Angeles, California
 UCLA CHEST PAIN AND ACS PATIENT MANAGEMENT GUIDELINE 2005 UCLA Medical Center Los Angeles, California Page 2 Inside front cover BLANK 2 UCLA CHEST PAIN AND ACS PATIENT MANAGEMENT GUIDELINE 2005 UCLA Medical
UCLA CHEST PAIN AND ACS PATIENT MANAGEMENT GUIDELINE 2005 UCLA Medical Center Los Angeles, California Page 2 Inside front cover BLANK 2 UCLA CHEST PAIN AND ACS PATIENT MANAGEMENT GUIDELINE 2005 UCLA Medical
Guideline Number: NIA_CG_024 Last Review Date: January 2011 Responsible Department: Last Revised Date: May 2, 2011 Clinical Operations
 National Imaging Associates, Inc. Clinical guidelines NUCLEAR CARDIAC IMAGING (MYOCARDIAL PERFUSION STUDY) CPT Codes: 78451, 78452, 78453, 78454, 78466, 78468, 78469, 78481, 78483, 78494, 78499 Original
National Imaging Associates, Inc. Clinical guidelines NUCLEAR CARDIAC IMAGING (MYOCARDIAL PERFUSION STUDY) CPT Codes: 78451, 78452, 78453, 78454, 78466, 78468, 78469, 78481, 78483, 78494, 78499 Original
Know the Quality of our Care at Every Step. Kansas City ACS Summit BI-State Cardiovascular Education Consortium
 Know the Quality of our Care at Every Step Kansas City ACS Summit BI-State Cardiovascular Education Consortium Welcome to the Kansas City ACS Summit Objectives: Follow the flow and care of an ACS patient
Know the Quality of our Care at Every Step Kansas City ACS Summit BI-State Cardiovascular Education Consortium Welcome to the Kansas City ACS Summit Objectives: Follow the flow and care of an ACS patient
Measurement Name Beta-Blocker Therapy Prior Myocardial Infarction (MI)
 Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for Artery, Atrial Fibrillation, Hypertension
Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for Artery, Atrial Fibrillation, Hypertension
DIFFERENTIATING THE PATIENT WITH UNDIFFERENTIATED CHEST PAIN
 DIFFERENTIATING THE PATIENT WITH UNDIFFERENTIATED CHEST PAIN Objectives Gain competence in evaluating chest pain Recognize features of moderate risk unstable angina Review initial management of UA and
DIFFERENTIATING THE PATIENT WITH UNDIFFERENTIATED CHEST PAIN Objectives Gain competence in evaluating chest pain Recognize features of moderate risk unstable angina Review initial management of UA and
Clinical Investigations
 Clinical Investigations The Usage Patterns of Cardiac Bedside Markers Employing Point-of-Care Testing for Troponin in Non-ST-Segment Elevation Acute Coronary Syndrome: Results from CRUSADE Address for
Clinical Investigations The Usage Patterns of Cardiac Bedside Markers Employing Point-of-Care Testing for Troponin in Non-ST-Segment Elevation Acute Coronary Syndrome: Results from CRUSADE Address for
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Learning Objectives. Epidemiology of Acute Coronary Syndrome
 Cardiovascular Update: Antiplatelet therapy in acute coronary syndromes PHILLIP WEEKS, PHARM.D., BCPS-AQ CARDIOLOGY Learning Objectives Interpret guidelines as they relate to constructing an antiplatelet
Cardiovascular Update: Antiplatelet therapy in acute coronary syndromes PHILLIP WEEKS, PHARM.D., BCPS-AQ CARDIOLOGY Learning Objectives Interpret guidelines as they relate to constructing an antiplatelet
Journal of the American College of Cardiology Vol. 45, No. 6, by the American College of Cardiology Foundation ISSN /05/$30.
 Journal of the American College of Cardiology Vol. 45, No. 6, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.11.055
Journal of the American College of Cardiology Vol. 45, No. 6, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.11.055
William D. Salerno, M.D. Director, Coronary Care Unit Hackensack University Medical Center Clinical Associate Professor of Medicine, UMDNJ
 William D. Salerno, M.D. Director, Coronary Care Unit Hackensack University Medical Center Clinical Associate Professor of Medicine, UMDNJ PROBLEM: blood supply to the heart has been compromised and heart
William D. Salerno, M.D. Director, Coronary Care Unit Hackensack University Medical Center Clinical Associate Professor of Medicine, UMDNJ PROBLEM: blood supply to the heart has been compromised and heart
OVERVIEW ACUTE CORONARY SYNDROME SYMPTOMS 9/30/14 TYPICAL WHAT IS ACUTE CORONARY SYNDROME? SYMPTOMS, IDENTIFICATION, MANAGEMENT
 OVERVIEW ACUTE CORONARY SYNDROME SYMPTOMS, IDENTIFICATION, MANAGEMENT OCTOBER 7, 2014 PETE PERAUD, MD SYMPTOMS TYPICAL ATYPICAL IDENTIFICATION EKG CARDIAC BIOMARKERS STEMI VS NON-STEMI VS USA MANAGEMENT
OVERVIEW ACUTE CORONARY SYNDROME SYMPTOMS, IDENTIFICATION, MANAGEMENT OCTOBER 7, 2014 PETE PERAUD, MD SYMPTOMS TYPICAL ATYPICAL IDENTIFICATION EKG CARDIAC BIOMARKERS STEMI VS NON-STEMI VS USA MANAGEMENT
Acute coronary syndromes (ACS), including unstable
 n report n Acute Coronary Syndromes: Morbidity, Mortality, and Pharmacoeconomic Burden Daniel M. Kolansky, MD Abstract Acute coronary syndromes (ACS), which include unstable angina and myocardial infarction
n report n Acute Coronary Syndromes: Morbidity, Mortality, and Pharmacoeconomic Burden Daniel M. Kolansky, MD Abstract Acute coronary syndromes (ACS), which include unstable angina and myocardial infarction
LAC-USC Cardiology Consult Service
 LAC-USC Cardiology Consult Service RESIDENT ORIENTATION First Day of Rotation: Report to 1 st day at LAC + USC Hospital 4 th floor Cardiology units Page Fellow day before rotation for more information
LAC-USC Cardiology Consult Service RESIDENT ORIENTATION First Day of Rotation: Report to 1 st day at LAC + USC Hospital 4 th floor Cardiology units Page Fellow day before rotation for more information
Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines)
 Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines) Authors: Dr. M. Love, Dr. I. Bata, K. Harrigan
Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines) Authors: Dr. M. Love, Dr. I. Bata, K. Harrigan
INTRODUCTION. Key Words:
 Original Article Acta Cardiol Sin 2017;33:377 383 doi: 10.6515/ACS20170126A Percutaneous Coronary Intervention Predictors of Mortality in Elderly Patients with Non-ST Elevation Acute Coronary Syndrome
Original Article Acta Cardiol Sin 2017;33:377 383 doi: 10.6515/ACS20170126A Percutaneous Coronary Intervention Predictors of Mortality in Elderly Patients with Non-ST Elevation Acute Coronary Syndrome
Chest Pain: To Cath or Not? Part I
 Chest Pain: To Cath or Not? Part I Georgios Papaioannou, MD Ioannis Karavas, MD Newton-Wellesley Hospital 5/3/2000 1 A Typical Scenario... 57 year old female, Mrs. X., presents to your office with a 2
Chest Pain: To Cath or Not? Part I Georgios Papaioannou, MD Ioannis Karavas, MD Newton-Wellesley Hospital 5/3/2000 1 A Typical Scenario... 57 year old female, Mrs. X., presents to your office with a 2
The life after myocardial infarction: a long quiet river?
 The life after myocardial infarction: a long quiet river? Cardiac rehabilitation: for whom and how? Dr. Barnabas GELLEN MD, PhD, FESC Poitiers JESFC 2018 - Paris Conflicts of interest Speaker honoraria
The life after myocardial infarction: a long quiet river? Cardiac rehabilitation: for whom and how? Dr. Barnabas GELLEN MD, PhD, FESC Poitiers JESFC 2018 - Paris Conflicts of interest Speaker honoraria
Continuing Medical Education Post-Test
 Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
Pre Hospital and Initial Management of Acute Coronary Syndrome
 Pre Hospital and Initial Management of Acute Coronary Syndrome Dr. Muhammad Fadil, SpJP 3rd SymCARD 2013 Classification of ACS ESC Guidelines for the management of Acute Coronary Syndrome in patients without
Pre Hospital and Initial Management of Acute Coronary Syndrome Dr. Muhammad Fadil, SpJP 3rd SymCARD 2013 Classification of ACS ESC Guidelines for the management of Acute Coronary Syndrome in patients without
REFERRAL HOSPITAL. The Importance of Door In Door Out Time DIDO
 REFERRAL HOSPITAL The Importance of Door In Door Out Time DIDO Jean Skonhovd,RN,BSN,MSAS Emergency Department Director Avera Heart Hospital of South Dakota Time to Treatment is critical for STEMI patients
REFERRAL HOSPITAL The Importance of Door In Door Out Time DIDO Jean Skonhovd,RN,BSN,MSAS Emergency Department Director Avera Heart Hospital of South Dakota Time to Treatment is critical for STEMI patients
Cardiogenic Shock. Carlos Cafri,, MD
 Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
Daily practice of ACS management in the Gulf: Data from Gulf COAST
 Daily practice of ACS management in the Gulf: Data from Gulf COAST Mohammad Zubaid, MB, ChB, FRCPC, FACC Professor of Medicine, Kuwait University Head, Division of Cardiology Mubarak Alkabeer Hospital
Daily practice of ACS management in the Gulf: Data from Gulf COAST Mohammad Zubaid, MB, ChB, FRCPC, FACC Professor of Medicine, Kuwait University Head, Division of Cardiology Mubarak Alkabeer Hospital
ORIGINAL ARTICLE. Rescue PCI Versus a Conservative Approach for Failed Fibrinolysis in Patients with STEMI
 Heart Mirror Journal From Affiliated Egyptian Universities and Cardiology Centers Vol. 6, No. 3, 2012 ISSN 1687-6652 ORIGINAL ARTICLE for Failed Fibrinolysis in Patients with STEMI Mohamed Salem, MD, PhD;
Heart Mirror Journal From Affiliated Egyptian Universities and Cardiology Centers Vol. 6, No. 3, 2012 ISSN 1687-6652 ORIGINAL ARTICLE for Failed Fibrinolysis in Patients with STEMI Mohamed Salem, MD, PhD;
Supplementary Table 1. Details of the components of the primary composite endpoint
 Supplementary Table 1. Details of the components of the primary composite endpoint 1. Death The cause of death will be defined by the underlying cause, not the immediate mode of death. Death will be classified
Supplementary Table 1. Details of the components of the primary composite endpoint 1. Death The cause of death will be defined by the underlying cause, not the immediate mode of death. Death will be classified
A. BISOC 1,2 A.M. PASCU 1 M. RĂDOI 1,2
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 THE ctntg4 PLASMA LEVELS IN RELATION TO ELECTROCARDIOGRAPHIC AND ECHOCARDIOGRAPHIC ABNORMALITIES IN
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 THE ctntg4 PLASMA LEVELS IN RELATION TO ELECTROCARDIOGRAPHIC AND ECHOCARDIOGRAPHIC ABNORMALITIES IN
High Value Evaluation of Chest Pain. Zoom Tips
 High Value Evaluation of Chest Pain California Quality Collaborative s Cardiology Webinar Series Webinar 1 December 7, 2017 Zoom Tips Attendees are automatically MUTED upon entry Refrain from using the
High Value Evaluation of Chest Pain California Quality Collaborative s Cardiology Webinar Series Webinar 1 December 7, 2017 Zoom Tips Attendees are automatically MUTED upon entry Refrain from using the
03/07/ Background. + High Risk Features Are Prevalent in Dialysis Patients
 + When Does Cardiovascular Disease Preclude Consideration of Renal Transplantation? Kul Aggarwal, MD, MRCP (UK), FACC Professor of Clinical Medicine Division of Cardiology University of Missouri & Chief,
+ When Does Cardiovascular Disease Preclude Consideration of Renal Transplantation? Kul Aggarwal, MD, MRCP (UK), FACC Professor of Clinical Medicine Division of Cardiology University of Missouri & Chief,
Abstract Background: Methods: Results: Conclusions:
 Two-Year Clinical and Angiographic Outcomes of Overlapping Sirolimusversus Paclitaxel- Eluting Stents in the Treatment of Diffuse Long Coronary Lesions Kang-Yin Chen 1,2, Seung-Woon Rha 1, Yong-Jian Li
Two-Year Clinical and Angiographic Outcomes of Overlapping Sirolimusversus Paclitaxel- Eluting Stents in the Treatment of Diffuse Long Coronary Lesions Kang-Yin Chen 1,2, Seung-Woon Rha 1, Yong-Jian Li
Lahey Clinic Internal Medicine Residency Program: Curriculum for Cardiovascular Medicine Rotation
 Lahey Clinic Internal Medicine Residency Program: Curriculum for Cardiovascular Medicine Rotation Faculty representative: David Venesy, MD Resident representative: David Kahan, MD Revision date: June 29,
Lahey Clinic Internal Medicine Residency Program: Curriculum for Cardiovascular Medicine Rotation Faculty representative: David Venesy, MD Resident representative: David Kahan, MD Revision date: June 29,
