Emergency Endovascular Stent-Grafting for Life-Threatening Acute Type B Aortic Dissections
|
|
|
- Annabella Mason
- 6 years ago
- Views:
Transcription
1 Emergency Endovascular Stent-Grafting for Life-Threatening Acute Type B Aortic Dissections Lennart F. Duebener, MD, Peter Lorenzen, MD, Gert Richardt, MD, Martin Misfeld, MD, Axel Nötzold, MD, Franz Hartmann, MD, Hans-Hinrich Sievers, MD, and Volker Geist, MD Departments of Cardiac Surgery and Cardiology, University Hospital of Schleswig-Holstein, Campus Luebeck, Luebeck, Germany, and Department of Cardiology, Heart Center Bad Segeberg, Bad Segeberg, Germany Background. There is still a considerable controversy regarding optimal treatment for patients with acute type B aortic dissection. Patients with complicated disease are particularly challenging for cardiovascular treatment. Early surgery for acute dissections of the descending aorta with life-threatening complications is known to carry a high mortality. Endovascular stent grafting is developing as an alternative treatment mainly for chronic stages of type B aortic dissection. It is not clear whether endovascular stent grafting is safe and effective in emergency treatment of acute type B aortic dissection. Methods. In 10 patients (7 men, 3 women; mean age, 59.2 years; range, 46 to 65 years), endovascular stent grafting was performed within hours (range, 4 to 24 hours) of diagnosis of complications. Indications for acute intervention included contained rupture, hematothorax, life-threatening malperfusion, and refractory pain. Using a retrograde endovascular route after surgical exposure of the femoral artery, self-expanding stent prostheses consisting of polyester-covered Nitinol (Talent, World Medical; mean diameter, 40 4 mm; length, 10 cm) were placed into the descending aorta distal to the subclavian artery. Before discharge and on follow-up visits, imaging of the aorta was performed using computed tomography. Results. In 9 of 10 patients (90%), the primary entry could be completely occluded with the endovascular stent. Early mortality was 20% (2 of 10): 1 patient died after disruption of the intimal layer distal to the stent, and 1 patient died in hemorrhagic shock after surgical fenestration of the abdominal aorta for persistent malperfusion. Three patients (30%) required consecutive surgical treatment: indications included acute development of retrograde type A aortic dissection, acute stent dislocation by fractured wires and secondary leakage, and late formation of an aneurysm of the descending aorta 6 months after endovascular stent grafting. There were no surgical or late deaths. Conclusions. Our experience provides some evidence that early mortality of life-threatening acute type B aortic dissection may be reduced by emergency endovascular stent grafting and that this form of treatment is a promising therapeutic option. Refinements, especially in stent design and application, may further improve the prognosis of patients in the life-threatening situation of complicated acute type B aortic dissection. (Ann Thorac Surg 2004;78:1261 7) 2004 by The Society of Thoracic Surgeons Accepted for publication March 16, Address reprint requests to Dr Sievers, Department of Cardiac Surgery, University Hospital of Schleswig-Holstein, Campus Luebeck, Ratzeburger Allee 160, Luebeck, Germany; sievers@medinf.muluebeck.de. The optimal therapy for acute type B aortic dissection has not yet been clearly defined [1, 2]. Two groups of patients with dissection of the descending aorta have been differentiated: patients with uncomplicated disease and patients with life-threatening complications [3]. There is consensus that in patients with uncomplicated acute type B aortic dissection, medical therapy is preferred to open surgical treatment, although there are ongoing prospective randomized trials to define the role of endovascular stent grafting (EVSG) in this setting. Patients with life-threatening complications of acute dissection of the descending aorta are therapeutically more challenging. The definition of life-threatening complications is still a matter of debate, but usually includes contained rupture, malperfusion of visceral organs or extremities, rapid increase of aortic diameter, and refractory pain. So far the only effective treatment option was open emergency surgical intervention with replacement of the descending aorta. Early mortality in this group used to be very high (more than 50%) [4]. Although it could be reduced in recent years to 21% to 40% [5, 6], there is still a significant morbidity and mortality after surgical repair of complicated acute type B aortic dissections. For this high-risk group of patients, a safer and equally effective form of treatment is desirable. Recently EVSG has become an alternative form of treatment with promising midterm results for patients with aneurysms and chronic dissections of the descending aorta [7, 8]. Endovascular stent grafting might be a potential option because of its less invasive character. It 2004 by The Society of Thoracic Surgeons /04/$30.00 Published by Elsevier Inc doi: /j.athoracsur
2 1262 DUEBENER ET AL Ann Thorac Surg EMERGENCY ENDOVASCULAR STENT-GRAFTING 2004;78: Table 1. Demographic Data, Indications for Emergency Stent Grafting, and Stent Diameter Patient No. Age (y) Sex Complication of Aortic Dissection Interval of Complication to Stent Grafting (h) Proximal Diameter of Stent (mm) 1 57 Male Refractory pain Male Extension of dissection, obstruction of 6 42 branch vessels 3 65 Male Obstruction of branch vessels (left kidney, left leg) 4 64 Female Obstruction of branch vessels (left kidney, 4 42 right leg) 5 63 Male Acute aortic rupture, hematothorax Male Refractory pain Female Contained rupture Female Rapid increase of aortic diameter Male Dysathria, neurologic deficit lower 9 42 extremities, loss of bladder control Male Obstruction of branch vessels (right kidney) is effective because it closes the entry and reroutes the blood into the true lumen, thereby ameliorating lifethreatening malperfusion. The endoluminal approach can avoid the major trauma of surgical therapy. This should help to bring the patients out of the acute lifethreatening phase of this devastating disease. Nevertheless, this presumably less-invasive method has its inherent risks. Rupture of the aorta might occur during the stent implantation. Perivascular leakage is reported in up to 25% of patients with type B aortic dissection after EVSG [9]. Dislocation of stents, leading to side branch occlusion and subsequent ischemia, is another potential complication [10]. Because of embolization of emboli from the atherosclerotic aorta or malperfusion of the spinal cord, neurologic complications may occur in up to 8% of patients [11]. The incidence of these adverse effects of stent grafting might be higher in the acute stage of complicated type B aortic dissections because the intima is weaker in these patients. Little experience exists with acute endoluminal therapy in this high-risk group of patients within a few hours after diagnosis. We report the experience of emergency stent grafting in patients with acute life-threatening complications of type B aortic dissection at our institution. Patients and Methods Patients Between October 2000 and October 2003, 10 patients (7 men, 3 women) with a mean age of 59.2 years (range, 46 to 65 years) underwent emergency EVSG for complicated acute type B aortic dissection within 11 6 hours of diagnosis of complications. Spiral computed tomography of the chest and abdomen in combination with transesophageal echocardiography was used to confirm the diagnosis. All patients were admitted to the emergency room because of persistent chest pain despite prior strong analgesic and multidrug antihypertensive medication. Indications for acute intervention besides refractory pain included rapid progression of aortic dilatation (2 cm in 8 hours), contained rupture, hematothorax, and lifethreatening malperfusion. Exclusion criteria for endovascular stent treatment were a distance of less than 0.5 cm between the subclavian artery and the entry and disease of the femoral or iliac arteries that precluded the introduction of the stent delivery system. None of the patients had Marfan s syndrome or a known history of aortic disease. Arterial hypertension as a cardiovascular risk factor was found in all patients. In all patients the entry of the type B dissection was found in a typical location just distal to the left subclavian artery. A cardiac catheterization was performed in all patients to rule out concomitant coronary artery disease. Demographic data and the intervals between the diagnosis of complications and stent grafting, as well as indications for acute endoluminal stent placement, are listed in Table 1. Stent Placement The mean time between diagnosis of complications and stent grafting was hours (range, 4 to 24 hours). The in-hospital availability of a variety of endovascular stents in different diameters made an emergency approach feasible. Using a retrograde endovascular route after surgical exposure of the femoral artery, selfexpanding stent prostheses consisting of polyestercovered Nitinol (Talent; Medtronics, Sunrise, FL; mean diameter, 40 4 mm; covered length, 100 mm) were placed into the descending aorta at the entry of dissection distal of the left subclavian artery. Only a short stent was used to avoid unnecessary side branch (eg, intercostal artery) occlusion. A pigtail catheter was advanced through the left brachial artery into the ascending aorta for angiography during the procedure and visualization of the true lumen. Emergency stent grafting was performed under general anesthesia in the cardiac catheterization laboratory by a team of interventional cardiolo-
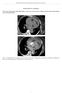
3 Ann Thorac Surg DUEBENER ET AL 2004;78: EMERGENCY ENDOVASCULAR STENT-GRAFTING 1263 and on follow-up visits, imaging of the aorta was performed using computed tomography. Fig 1. (A) Aortic angiogram depicts contrast media filling of false lumen through an entry site distal to the left subclavian artery. (B) Closure of the entry site by the stent graft resulted in redirection of flow into the true aortic lumen. gists and cardiac surgeons. During the release of the stent, the systolic arterial pressure was lowered to 60 mm Hg. The stents were expanded at the proximal end by balloon dilatation to anchor the stents in the aortic wall. At the end of the procedure in all patients, angiography was used to demonstrate the location of the stent and perfusion of the aorta and its branches (eg, left subclavian, mesenteric, renal arteries; Fig 1). Before discharge Results In all patients the stent grafts were successfully deployed in the intended position. With the exception of patient number 5, the primary entry could be occluded with the endovascular stent in all patients. Only one stent was used per patient. None of the patients had vascular problems at the arterial site of access for EVSG. Early mortality was 20% (2 of 10 patients). In patient number 3, the proximal entry of the dissection was successfully occluded by placement of an endovascular stent. However, renal ischemia persisted, and 1 day after EVSG surgical fenestration of the abdominal aorta was performed. Two days postoperatively the patient died in hemorrhagic shock as a result of massive intraabdominal bleeding after surgical fenestration of the abdominal aorta for persistent malperfusion. Patient number 6 had symptoms of mesenteric and lower extremity ischemia the morning after the intervention. With the exception of the right renal artery, no flow could be demonstrated in any of the visceral arteries of the infradiaphragmatic aorta by angiography. There was a complete disruption of the intimal layer distal to the stent. Surgical fenestration of the abdominal aorta did not lead to reperfusion. After resection of the ascending and transverse colon for complete necrosis, the postoperative course was complicated by renal failure, abdominal hematoma, necrosis of the pancreas, and retroperitoneal infection. The patient expired in multiorgan failure 5 weeks after EVSG. Three patients (30%) required consecutive surgical treatment: indications included in patient number 4 acute development of retrograde type A aortic dissection, in patient number 5 persistent leakage and late formation of an aneurysm of the descending aorta 6 months after EVSG, and in patient number 8 acute stent dislocation by fractured wires and a distal aneurysm. Surgical mortality was zero. Patient number 4 experienced hemiplegia with leftsided symptoms 12 hours after initially uneventful EVSG. Echocardiography showed an acute type A aortic dissection with involvement of the aortic arch and occlusion of the right internal carotid artery. In addition, there was severe aortic regurgitation. Intraoperatively a fresh entry tear was detected between the brachiocephalic trunk and the left internal carotid artery. The former entry in the descending aorta was found to be sealed by the stent. An aortic valve reconstruction was performed; the ascending aorta and partial aortic arch were replaced. The right internal carotid artery was revascularized by direct anastomosis of the dissected layers. Postoperatively symptoms of the hemiplegia were resolving. The patient was discharged on postoperative day 29 in stable condition. In patient number 5 emergency stent grafting was performed for aortic rupture with hematothorax. After EVSG only minimal flow into the false lumen could be demonstrated. The postinterventional course was com-
4 1264 DUEBENER ET AL Ann Thorac Surg EMERGENCY ENDOVASCULAR STENT-GRAFTING 2004;78: Table 2. Morbidity and Mortality of Acute Stent Grafting in Life-Threatening Type B Aortic Dissection Patient No. Complication of Stent Placement Secondary Surgery Outcome Duration of Follow-up (mo) 1 None None Good long-term result 38 2 None None Good long-term result 34 3 Persistent visceral ischemia Surgical fenestration of Death 1 day (died) abdominal aorta, fatal bleeding 4 Acute retrograde type A dissection, carotid artery occlusion, aortic valve regurgitation Surgical replacement of ascending aorta and arch, carotid revascularization, aortic valve repair Good long-term result 33 5 Only partial occlusion of entry-tear, persistent leakage 6 Intima disruption at distal end of stent, complete occlusion of distal aorta 6 mo postinterventional surgical replacement of descending aorta Unsuccessful surgical revascularization, bowel resection Good long-term result 33 Death 35 days (died) 7 None None Good long-term result 30 8 Stent dislocation caused by 6 mo postinterventional Good long-term result 27 fractured wires, secondary leakage distal descending aortic aneurysm, surgical replacement 9 Cerebral infarction (left middle None Slow recovery from neurologic 5 cerebral artery) morbidity 10 None None Good short-term result 1 plicated by renal failure and pneumonia necessitating tracheotomy. The patient was discharged 1 month after EVSG. Follow-up computed tomographic scans revealed persistent flow in the false lumen and an aneurysm of the descending aorta of 8 cm. An uneventful elective surgical replacement of the descending aorta was performed 6 months after stent grafting. In patient number 8 the primary entry was initially successfully occluded by the stent. However, fracture of the distal stent wires caused a dislocation of the endovascular stent with secondary leakage. An aneurysm was the indication for replacement of the descending aorta and later the infrarenal abdominal aorta. Two patients suffered from neurologic morbidity periinterventionally. In patient number 4, left-sided hemiplegia was caused by occlusion of the internal carotid artery secondary to retrograde type A aortic dissection after stent grafting. It resolved completely after surgical revascularization as described earlier. Patient number 9 had emergency stent grafting for acute type B aortic dissection with motor deficit of the lower extremities and loss of bladder control. In addition the patient suffered from marked dysarthria before EVSG. The stent placement was uneventful. The primary entry tear could be successfully occluded. Postinterventionally the patient demonstrated right-sided hemiplegia. Computed tomographic scans showed ischemia in the area of the left middle cerebral artery. Neurologic deficits resolved slowly, and on postinterventional day 27 the patient was transferred to a neurologic rehabilitation center. No neurologic deficits or sequelae were detectable periinterventionally or during follow-up in any of the other patients. Table 2 summarizes the stent-related complications, secondary operation, and outcomes of all patients. Mean follow-up was months (range, 1 to 38 months) and was complete. None of the patients died during the follow-up period. Comment Endovascular stent grafting was developed in the early 1990s, and the initial clinical use was in patients with abdominal aortic aneurysms [12, 13]. Shortly after, endoluminal stent placement was applied to patients with aneurysms of the thoracic aorta [7, 14]. Later this new approach was used in patients with aortic dissections as well [8, 15, 16]. During the last several years, evidence has accumulated that the outcome after EVSG in patients with chronic dissections of the descending aorta has favorable midterm results [16]. This is especially true for the elderly patient population with relevant comorbidities including hypertension, diabetes mellitus, renal disease, coronary artery disease, and obstructive lung disease. However, similar to any treatment option, endovascular stenting has its potential side effects. The risks of the endoluminal approach include a secondary intimal tear as a result of the stent wires, stent dislocation, perivascular leakage, branch occlusion, vascular problems at the arterial site of access, and, rarely, rupture of the aorta. Although endovascular stent placement for acute aor-
5 Ann Thorac Surg DUEBENER ET AL 2004;78: EMERGENCY ENDOVASCULAR STENT-GRAFTING 1265 tic dissections with complications (eg, ischemic) has been performed before [15, 17], it is not a well-established procedure yet. In the majority of theses cases the interval between diagnosis and stent grafting was longer than 24 hours, usually several days. Thus, there is little information available about the safety and effectiveness of endovascular stent grafting for complicated, life-threatening acute type B aortic dissection within 24 hours or less of diagnosis. Previously, the open surgical approach resulted in a high morbidity and mortality (more than 50%) in patients with life-threatening type B aortic dissections [4]. In our institution a total of 13 patients underwent surgery for acute complicated type B aortic dissection between 2000 and Seven of these patients died (in-hospital mortality of 54%): 2 died intraoperatively, and 5 died during the postoperative course. Causes of death included multiorgan failure, pulmonary complications, and cardiac low output syndrome. Because of the very high surgical mortality and the promising early results with stent grafting, in 2001 emergency stent placement became the procedure of choice for complicated acute type B aortic dissection in our institution. Recently surgical mortality could be reduced to 21% to 40% in some centers [5, 6], but there is still a significant morbidity and mortality after emergency surgical repair of complicated type B aortic dissection. Our study indicates that stent placement is a feasible and effective approach even in the emergency treatment (within 24 hours) of patients with complicated acute type B dissection. This is in keeping with a recent literature report [18] about emergent EVSG for perforated acute type B dissections (n 4) and ruptured thoracic aortic aneurysms (n 7). They concluded that emergency EVSG is technically feasible with less morbidity and mortality than conventional open surgery in high-risk patients. Stent grafting is effective by occlusion of the primary entry tear, which could be achieved in a majority of patients even in this acute setting. Our results also indicate that the mortality in this high-risk group may be reduced when compared with surgical series; however, it remains high (20%) in this EVSG series. Nienaber and colleagues [8] reported in 1999 an early mortality of 0 in 12 patients with descending aortic aneurysm. However, in their series patient profiles and selection were different. Endovascular stent grafting was not performed as an emergency treatment in a lifethreatening situation. This might in part explain the difference in mortality. However, according to a more recent report by the same group, emergency stent graft placement was successful without any periprocedural mortality and morbidity in 11 patients with acute type B aortic dissection with leakage and evolving rupture [19]. This shows that with a lot of expertise there is a potential for very low mortality after emergency stent grafting even in patients with complicated acute type B aortic dissections. In our series the cause of death in 1 patient was a presumably procedure-related distal disruption of the intimal layer leading to a complete abdominal ischemia. In these high-risk patients the creation of a secondary intimal tear by emergency EVSG is particularly of concern because the intima in patients with acute dissections tends to be weak. The bare spring wires at the distal end of the stent were thought to be responsible for the damage of the intima. Thereafter the protocol was changed, and only stents without distal bare springs were applied. One patient died in hemorrhagic shock after surgical fenestration for persistent mesenteric malperfusion. The malperfusion might have been caused by a so-called static flap of the dissection membrane that occluded mesenteric branches. This type of malperfusion is not easily reversible by the increase of flow in the true lumen and decline of flow in the false lumen. This problem has also been described after surgical repair of acute type B aortic dissection [4]. The problem of persistent malperfusion is an important issue in the care of patients with acute type B aortic dissections. Early diagnosis by selective angiography is crucial. Treatment remains difficult. As demonstrated by our experience, stent grafting of the descending aorta is not always sufficient to improve malperfusion of vital abdominal organs caused by local branch vessel obstruction. Newer treatment options include additional selective endoluminal stenting of important aortic branch vessels (such as the mesenteric or renal arteries). Three patients (30%) required consecutive surgical treatment: indications included acute development of retrograde type A aortic dissection, acute stent dislocation by fractured wires and secondary leakage, and late formation of an aneurysm of the descending aorta 6 months after EVSG. There were no surgical deaths, indicating that surgery in more chronic (nonemergency) stages provides more predictable results. In the patient with retrograde type A aortic dissection after emergency EVSG of the descending aorta, the cause of this complication might have been a secondary tear at the proximal end of the stent [20]. This was possibly the result of the rigidity of the stent graft [21]. Fracture of stent wires leading to dislocation of the stent and secondary leakage is a device-related complication. Refinements in stent design and application may prevent this complication. This should further improve the prognosis of patients with acute type B aortic dissections. Our experience provides some evidence that early mortality of life-threatening acute type B aortic dissection may be reduced by emergency EVSG. Complications after stent grafting were primarily caused by stentrelated factors potentially amendable by improved stent design. Nevertheless, the principle of this therapeutic approach seems promising and warrants further careful evaluation. References 1. Umana JP, Miller DC, Mitchell RS. What is the best treatment for patients with acute type B aortic dissections
6 1266 DUEBENER ET AL Ann Thorac Surg EMERGENCY ENDOVASCULAR STENT-GRAFTING 2004;78: medical, surgical or endovascular stent grafting? Ann Thorac Surg 2002;74: Umana JP, Lai DT, Mitchell RS, et al. Is medical therapy still the optimal treatment strategy for patients with acute type B aortic dissections? J Thorac Cardiovasc Surg 2002;124: Elefteriades JA, Hartleroad J, Gusberg RJ, et al. Long-term experience with descending aortic dissection: the complication-specific approach. Ann Thorac Surg 1992;53: Miller DC, Mitchell RS, Oyer PS, et al. Independent determinants of operative mortality for patients with aortic dissections. Circulation 1984;70(Suppl 1):I Gysi J, Schaffner T, Mohacsi P, Aeschbacher B, Althaus U, Carrel T. Early and late outcome of operated and nonoperated acute dissection of the descending aorta. Eur J Cardiothorac Surg 1997;11: Kouchoukos NT, Masetti P, Rokkas CK, Murphy SF, Blackstone EH. Safety and efficacy of hypothermic cardiopulmonary bypass and circulatory arrest for operations on the descending thoracic and thoracoabdominal aorta. Ann Thorac Surg 2001;73: Dake MD, Miller DC, Semba CP, et al. Transluminal placement of endovascular stent-grafts for the treatment of descending thoracic aortic aneurysms. N Engl J Med 1994;331: Nienaber CA, Fattori R, Lund G, et al. Nonsurgical reconstruction of thoracic aortic dissection by stent-graft placement. N Engl J Med 1999;340: Dake MD, Miller DC, Mitchell RS, Semba CP, Moore KA, Sakai T. The first generation of endovascular stent-grafts for patients with aneurysms of the descending thoracic aorta. J Thorac Cardiovasc Surg 1998;116: Resch T, Koul B, Dias NV. Changes in aneurysm morphology and stent graft confirmation after endovascular repair of aneurysms of the descending aorta. J Thorac Cardiovasc Surg 2001;122: Safi HJ, Miller CC III, Reardon MJ, et al. Operations for acute and chronic dissection: recent outcomes in regard to neurological deficit and early death. Ann Thorac Surg 1998;66: Parodi JC, Palmaz JC, Barone HD. Transfemoral intraluminal graft implantation for abdominal aortic aneurysms. Ann Vasc Surg 1991;5: Blum U, Voshage G, Lammer J, et al. Endoluminal stentgrafts for infrarenal abdominal aortic aneurysms. N Engl J Med 1997;336: Mitchell RS, Miller DC, Dake MD, et al. Thoracic aortic aneurysm repair with an endovascular stent graft: the first generation. Ann Thorac Surg 1999;67: Slonim SM, Nyman U, Semba CP, et al. Aortic dissection: percutaneous management of ischemic complications with endovascular stents and balloon fenestration. J Vasc Surg 1996;23: Dake MD, Kato N, Mitchell RS, et al. Endovascular stentgraft placement for the treatment of acute aortic dissection. N Engl J Med 1999;340: Williams DM, Lee DY, Hamilton BH, et al. The dissected aorta: percutaneous treatment of ischemic complications principles and results. J Vasc Interv Radiol 1997;8: Doss M, Balzer J, Martens S, et al. Emergent endovascular stent grafting for perforated acute type B and ruptured thoracic aortic aneurysms. Ann Thorac Surg 2003;76: Nienaber CA, Ince H, Weber F, et al. Emergency stent-graft placement in thoracic aortic dissection and evolving rupture. J Card Surg 2003;18: Misfeld M, Noetzold A, Geist V, Richardt G, Sievers HH. Retrograde type A dissection after endovascular stent grafting of type B dissection. Z Kardiol 2002;91: Suzuki T, Shimono T, Kato N, et al. Extended total arch replacement by means of the open stent-grafting method to treat intimal tears after transluminal stent-graft placement for a ruptured acute type B aortic dissection. J Thorac Cardiovasc Surg 2002;123: INVITED COMMENTARY During the second half of the last century, all areas of thoracic aorta became accessible to the thoracic surgeon for repair. Despite tremendous advances in surgical techniques and care, surgical repair of an acute aortic dissection remains a high-risk procedure. Acute aortic dissection is a complicated manifestation of aortic wall pathology. The prognosis of acute aortic dissection rests mainly on the anatomic location of the dissection and patient specific characteristics. At the Methodist DeBakey Heart Center, we continue to follow the teachings of Drs Michael E. DeBakey and E. Stanley Crawford, who developed our thoracic aortic program, operating acutely on DeBakey type I and II (Stanford type A) aortic dissections, and treating De- Bakey type III (Stanford type B) acute dissections medically unless they are complicated. Our definition of complicated descending thoracic aortic dissection matches that of the author, including contained rupture, hemothorax, life-threatening malperfusion, and refractory pain. We agree with the Stanford group that the prognosis in uncomplicated descending thoracic aortic dissection is similar for medically and successfully surgically treated patients [1]. The problematic point is the difficulty in achieving a successful surgical outcome in cases of acute descending thoracic aortic dissection. The current paper by Duebener and colleagues describes their experience with 10 patients undergoing emergency stent graft placement for complicated descending thoracic aortic dissection within 24 hours of diagnosis. This represents an extremely high-risk group and a very rapid turnaround time for stent placement. They have an early mortality rate of 2 of 10 patients (20%) compared with 7 of 13 patients (54%) treated with open surgical repair at their institution during the same time frame. Although the mortality rate associated with open surgical repair of complicated acute dissection continues to decline, and there is even a series reporting zero mortality [2], it remains a substantial surgical challenge, and a 50% mortality is closer to what most surgical groups are likely to achieve with open repair. Three patients did require consecutive surgical repair for complications of the stent or stent placement. There are currently three thoracic stent graft clinical trials in the United States, and no commercially available thoracic stent grafts. At the Methodist DeBakey Heart Center, we are participating in one of these trials. All surgeons who have operated on patients with a complicated acute descending thoracic aortic dissection know 2004 by The Society of Thoracic Surgeons /04/$30.00 Published by Elsevier Inc doi: /j.athoracsur
Thoracic aortic aneurysms are life threatening and
 Thoracic Aortic Aneurysms: Treatment With Endovascular Self-Expandable Stent Grafts Martin Grabenwöger, MD, Doris Hutschala, MD, Marek P. Ehrlich, MD, Fabiola Cartes-Zumelzu, MD, Siegfried Thurnher, MD,
Thoracic Aortic Aneurysms: Treatment With Endovascular Self-Expandable Stent Grafts Martin Grabenwöger, MD, Doris Hutschala, MD, Marek P. Ehrlich, MD, Fabiola Cartes-Zumelzu, MD, Siegfried Thurnher, MD,
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Transluminal Stent-graft Placement endovascular surgery
 13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when?
 Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome
 Case Report 1 Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome Marat. ripov, Ildar Z. bdyldaev, Semen D. Chevgun, ektur S. Daniyarov, Dinara. Toktosunova,
Case Report 1 Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome Marat. ripov, Ildar Z. bdyldaev, Semen D. Chevgun, ektur S. Daniyarov, Dinara. Toktosunova,
B myonephropathic metabolic syndrome MNMS 33 CT DeBakey IIIb MNMS
 13 603 607 2004 B B myonephropathic metabolic syndrome MNMS33 CT DeBakey IIIb MNMS 20 A MNMSMNMS 13 603 607 2004 MNMS B malperfusion myonephropathic metabolic syndrome MNMS MNMS Haimovici 1 3 MNMS B MNMS
13 603 607 2004 B B myonephropathic metabolic syndrome MNMS33 CT DeBakey IIIb MNMS 20 A MNMSMNMS 13 603 607 2004 MNMS B malperfusion myonephropathic metabolic syndrome MNMS MNMS Haimovici 1 3 MNMS B MNMS
I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical Department National Taiwan University Hospital
 Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Emergency Endovascular Treatment for Ruptured Type B Dissection in the Abdominal Aorta
 Brief Reports Emergency Endovascular Treatment for Ruptured Type B Dissection in the Abdominal Aorta Mikolaj Wojtaszek, MD, PhD, Krzysztof Milczarek, MD, PhD, Jacek Szmidt, MD, PhD, and Olgierd Rowinski,
Brief Reports Emergency Endovascular Treatment for Ruptured Type B Dissection in the Abdominal Aorta Mikolaj Wojtaszek, MD, PhD, Krzysztof Milczarek, MD, PhD, Jacek Szmidt, MD, PhD, and Olgierd Rowinski,
Management of Acute Aortic Syndromes. M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria
 Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Fate of Aneurysms of the Distal Arch and Proximal Descending Thoracic Aorta After Transaortic Endovascular Stent-Grafting
 CARDIOVASCULAR Fate of Aneurysms of the Distal Arch and Proximal Descending Thoracic Aorta After Transaortic Endovascular Stent-Grafting Taijiro Sueda, MD, Kazumasa Orihashi, MD, Kenji Okada, MD, Yuji
CARDIOVASCULAR Fate of Aneurysms of the Distal Arch and Proximal Descending Thoracic Aorta After Transaortic Endovascular Stent-Grafting Taijiro Sueda, MD, Kazumasa Orihashi, MD, Kenji Okada, MD, Yuji
Open fenestration for complicated acute aortic B dissection
 Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Treatment of acute type B aortic dissection: Current status
 MEET Cannes, 18. - 21.06.2009 Treatment of acute type B aortic dissection: Current status Christoph A. Nienaber, MD, FACC University of Rostock Department of Internal Medicine, Cardiology christoph.nienaber@med.uni-rostock.de
MEET Cannes, 18. - 21.06.2009 Treatment of acute type B aortic dissection: Current status Christoph A. Nienaber, MD, FACC University of Rostock Department of Internal Medicine, Cardiology christoph.nienaber@med.uni-rostock.de
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion
 Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection
 Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Indications for stent grafts in type B aortic dissection
 expert opinion I Akin C A Nienaber Indications for stent grafts in type B aortic dissection ibrahim akin christoph a nienaber Department of Medicine, Divisions of Cardiology, Pulmology and Intensive Care
expert opinion I Akin C A Nienaber Indications for stent grafts in type B aortic dissection ibrahim akin christoph a nienaber Department of Medicine, Divisions of Cardiology, Pulmology and Intensive Care
The New England Journal of Medicine ENDOVASCULAR STENT GRAFT PLACEMENT FOR THE TREATMENT OF ACUTE AORTIC DISSECTION
 ENDOVASCULAR STENT GRAFT PLACEMENT FOR THE TREATMENT OF ACUTE AORTIC DISSECTION MICHAEL D. DAKE, M.D., NORIYUKI KATO, M.D., R. SCOTT MITCHELL, M.D., CHARLES P. SEMBA, M.D., MAHMOOD K. RAZAVI, M.D., TAKATSUGU
ENDOVASCULAR STENT GRAFT PLACEMENT FOR THE TREATMENT OF ACUTE AORTIC DISSECTION MICHAEL D. DAKE, M.D., NORIYUKI KATO, M.D., R. SCOTT MITCHELL, M.D., CHARLES P. SEMBA, M.D., MAHMOOD K. RAZAVI, M.D., TAKATSUGU
The morbidity and mortality rates associated with the. Outcome of Surgical Treatment in Patients With Acute Type B Aortic Dissection
 Outcome of Surgical Treatment in Patients With Acute Type B Aortic Dissection Tomoki Shimokawa, MD, Kazutaka Horiuchi, MD, Naomi Ozawa, MD, Kenu Fumimoto, MD, Susumu Manabe, MD, Tetsuya Tobaru, MD, and
Outcome of Surgical Treatment in Patients With Acute Type B Aortic Dissection Tomoki Shimokawa, MD, Kazutaka Horiuchi, MD, Naomi Ozawa, MD, Kenu Fumimoto, MD, Susumu Manabe, MD, Tetsuya Tobaru, MD, and
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns
 CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
TEVAR for complicated acute type B dissection with malperfusion
 Masters of Cardiothoracic Surgery TEVR for complicated acute type dissection with malperfusion Guido H.W. van ogerijen 1, David M. Williams 2, Himanshu J. Patel 1 Departments of 1 Cardiac Surgery and 2
Masters of Cardiothoracic Surgery TEVR for complicated acute type dissection with malperfusion Guido H.W. van ogerijen 1, David M. Williams 2, Himanshu J. Patel 1 Departments of 1 Cardiac Surgery and 2
Endovascular therapy for Ischemic versus Nonischemic complicated acute type B aortic dissection (catbad).
 Endovascular therapy for Ischemic versus Nonischemic complicated acute type B aortic dissection (catbad). AS. Eleshra, MD 1, T. Kölbel, MD, PhD 1, F. Rohlffs, MD 1, N. Tsilimparis, MD, PhD 1,2 Ahmed Eleshra
Endovascular therapy for Ischemic versus Nonischemic complicated acute type B aortic dissection (catbad). AS. Eleshra, MD 1, T. Kölbel, MD, PhD 1, F. Rohlffs, MD 1, N. Tsilimparis, MD, PhD 1,2 Ahmed Eleshra
AORTIC DISSECTIONS Current Management. TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida
 AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
Endovascular Treatment of Malperfusion Syndrome
 Endovascular Treatment of Malperfusion Syndrome in Type B Aortic Dissection Department of Cardiology, Pusan National luniveristy i Hospital, Han Cheol Lee Endovascular Treatment Indication of Type B Aortic
Endovascular Treatment of Malperfusion Syndrome in Type B Aortic Dissection Department of Cardiology, Pusan National luniveristy i Hospital, Han Cheol Lee Endovascular Treatment Indication of Type B Aortic
The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations
 The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations Joseph V. Lombardi, MD Professor & Chief, Division of Vascular & Endovascular Surgery Department of Surgery,
The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations Joseph V. Lombardi, MD Professor & Chief, Division of Vascular & Endovascular Surgery Department of Surgery,
Vascular Intervention
 10 : 389-393, 2001 B Vascular Intervention 1 1 2 1 1 1 1 3 2 1 1997 7 2000 4 B 29 19 10 50 84 66.1 stent graft S/G primary entry stenting S/G 12 4 2 1 1 40 mm 8 1 MOF 1 endoleak + 11 91.6% 10 stenting
10 : 389-393, 2001 B Vascular Intervention 1 1 2 1 1 1 1 3 2 1 1997 7 2000 4 B 29 19 10 50 84 66.1 stent graft S/G primary entry stenting S/G 12 4 2 1 1 40 mm 8 1 MOF 1 endoleak + 11 91.6% 10 stenting
AORTIC DISSECTION. DISSECTING ANEURYSMS OF THE AORTA or CLASSIFICATION
 DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR
 Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR William J. Quinones-Baldrich MD Professor of Surgery Director UCLA Aortic Center UCLA Medical Center Los Angeles,
Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR William J. Quinones-Baldrich MD Professor of Surgery Director UCLA Aortic Center UCLA Medical Center Los Angeles,
Aortic dissection is one of the most catastrophic events that affects
 Surgery for Acquired Cardiovascular Disease Midterm results of stent-graft repair of acute and chronic aortic dissection with descending tear: The complicationspecific approach Noriyuki Kato, MD a Takatsugu
Surgery for Acquired Cardiovascular Disease Midterm results of stent-graft repair of acute and chronic aortic dissection with descending tear: The complicationspecific approach Noriyuki Kato, MD a Takatsugu
Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure
 Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosure Speaker name: Tilo Kölbel, MD I
Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosure Speaker name: Tilo Kölbel, MD I
No Disclosure. Aortic Dissection in Japan. This. The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair
 No Disclosure The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair Toru Kuratani Department of Cardiovascular Surgery Osaka University Graduate School of Medicine,
No Disclosure The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair Toru Kuratani Department of Cardiovascular Surgery Osaka University Graduate School of Medicine,
Descending aorta replacement through median sternotomy
 Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques
 Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept
 The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept Professor Christoph A. Nienaber The Royal Brompton and Harefield NHS Trust Cardiology and Aortic Centre
The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept Professor Christoph A. Nienaber The Royal Brompton and Harefield NHS Trust Cardiology and Aortic Centre
SUPPLEMENTAL MATERIAL
 SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
Animesh Rathore, MD 4/22/17. The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management
 Animesh Rathore, MD 4/22/17 The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management Disclosures Just a young vascular surgeon who would like to keep his job My opponent
Animesh Rathore, MD 4/22/17 The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management Disclosures Just a young vascular surgeon who would like to keep his job My opponent
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury. Conflict of Interest. Hypotensive shock 5/5/2014. none
 EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation
 Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation Vallabhajosyula, P: Szeto, W; Desai, N; Pulsipher, A;
Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation Vallabhajosyula, P: Szeto, W; Desai, N; Pulsipher, A;
Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta
 02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
Distal False Lumen Occlusion in Aortic Dissection With a Homemade Extra-Large Vascular Plug: The Candy-Plug Technique
 484 J ENDOVASC THER 2013;20:484 489 TECHNICAL NOTE Distal False Lumen Occlusion in Aortic Dissection With a Homemade Extra-Large Vascular Plug: The Candy-Plug Technique Tilo Kölbel, MD, PhD; Christina
484 J ENDOVASC THER 2013;20:484 489 TECHNICAL NOTE Distal False Lumen Occlusion in Aortic Dissection With a Homemade Extra-Large Vascular Plug: The Candy-Plug Technique Tilo Kölbel, MD, PhD; Christina
Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D.
 Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D. Gil Hospital, Gachon University Incheon, Korea Classification of AD Acute vs. Chronic (2weeks) (IIIa, b) type
Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D. Gil Hospital, Gachon University Incheon, Korea Classification of AD Acute vs. Chronic (2weeks) (IIIa, b) type
Transluminal placement of endovascular stentgrafts for the treatment of type A aortic dissection with an entry tear in the descending thoracic aorta
 CLINICAL RESEARCH STUDIES Transluminal placement of endovascular stentgrafts for the treatment of type A aortic dissection with an entry tear in the descending thoracic aorta Noriyuki Kato, MD, a Takatsugu
CLINICAL RESEARCH STUDIES Transluminal placement of endovascular stentgrafts for the treatment of type A aortic dissection with an entry tear in the descending thoracic aorta Noriyuki Kato, MD, a Takatsugu
Treatment of Thoracoabdominal Aneurysms Is there a need for custom-made devices?
 : FETURED TECHNOLOGY: JOTEC E-XTR DESIGN ENGINEERING Treatment of Thoracoabdominal neurysms Is there a need for custom-made devices? INTERVIEW ND CSE PRESENTTIONS WITH DNIEL RNZN, MD, ND NDREJ SCHMIDT,
: FETURED TECHNOLOGY: JOTEC E-XTR DESIGN ENGINEERING Treatment of Thoracoabdominal neurysms Is there a need for custom-made devices? INTERVIEW ND CSE PRESENTTIONS WITH DNIEL RNZN, MD, ND NDREJ SCHMIDT,
Optimised management of type A aortic dissection with visceral malperfusion concept to reconsider
 Optimised management of type A aortic dissection with visceral malperfusion concept to reconsider Matthias Thielmann, MD, PhD, FAHA Thoracic and Cardiovascular Surgery, West-German Heart and Vascular Center
Optimised management of type A aortic dissection with visceral malperfusion concept to reconsider Matthias Thielmann, MD, PhD, FAHA Thoracic and Cardiovascular Surgery, West-German Heart and Vascular Center
Optimal repair of acute aortic dissection
 Optimal repair of acute aortic dissection Dept. of Vascular Surgery, The 2nd Xiang-Yale Hospital, Central-South University, China Hunan Major Vessels Diseases Clinical Center Chang Shu Email:changshu01@yahoo.com
Optimal repair of acute aortic dissection Dept. of Vascular Surgery, The 2nd Xiang-Yale Hospital, Central-South University, China Hunan Major Vessels Diseases Clinical Center Chang Shu Email:changshu01@yahoo.com
Challenges. 1. Sizing. 2. Proximal landing zone 3. Distal landing zone 4. Access vessels 5. Spinal cord ischemia 6. Endoleak
 Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
Total Endovascular Repair Type A Dissection. Eric Herget Interventional Radiology
 Total Endovascular Repair Type A Dissection Eric Herget Interventional Radiology 65 year old male Acute Type A Dissection Severe Aortic Regurgitation No co-morbidities Management? Part II Evolving Global
Total Endovascular Repair Type A Dissection Eric Herget Interventional Radiology 65 year old male Acute Type A Dissection Severe Aortic Regurgitation No co-morbidities Management? Part II Evolving Global
Endovascular Treatment of Thoracic Aortic Disease. Four Years of Experience
 Endovascular Treatment of Thoracic Aortic Disease Four Years of Experience Alessandro S. Bortone, MD, PhD, FESC; Emanuela De Cillis, MD; Donato D Agostino, MD; Luigi de Luca Tupputi Schinosa, MD Background
Endovascular Treatment of Thoracic Aortic Disease Four Years of Experience Alessandro S. Bortone, MD, PhD, FESC; Emanuela De Cillis, MD; Donato D Agostino, MD; Luigi de Luca Tupputi Schinosa, MD Background
1 7 central operation SMA SMA
 12 521 527 2003 198913 Stanford A 159 8 5.0 B 139 6 4.3 A SMA SMA A 8 1 7 central operation 3 1 SMA 1 1 5 1 14 8 3 38 B 6 1 5 2 +SMA 3 1 0 2910.3 SMA 3 50 A 5 B 5 SMA SMA SMA SMA SMA 12 521 527 2003 SMA
12 521 527 2003 198913 Stanford A 159 8 5.0 B 139 6 4.3 A SMA SMA A 8 1 7 central operation 3 1 SMA 1 1 5 1 14 8 3 38 B 6 1 5 2 +SMA 3 1 0 2910.3 SMA 3 50 A 5 B 5 SMA SMA SMA SMA SMA 12 521 527 2003 SMA
Animesh Rathore, MD 4/21/17. Penetrating atherosclerotic ulcers of aorta
 Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair
 583 Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair Frank R. Arko, MD; W. Anthony Lee, MD; Bradley B. Hill, MD; Paul Cipriano,
583 Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair Frank R. Arko, MD; W. Anthony Lee, MD; Bradley B. Hill, MD; Paul Cipriano,
Abdominal and thoracic aneurysm repair
 Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Peter I. Kalmar, 1 Peter Oberwalder, 2 Peter Schedlbauer, 1 Jürgen Steiner, 1 and Rupert H. Portugaller Introduction. 2.
 Case Reports in Medicine Volume 2013, Article ID 714914, 4 pages http://dx.doi.org/10.1155/2013/714914 Case Report Secondary Aortic Dissection after Endoluminal Treatment of an Intramural Hematoma of the
Case Reports in Medicine Volume 2013, Article ID 714914, 4 pages http://dx.doi.org/10.1155/2013/714914 Case Report Secondary Aortic Dissection after Endoluminal Treatment of an Intramural Hematoma of the
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui
 Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Neurological Complications of TEVAR. Frank J Criado, MD. Union Memorial-MedStar Health Baltimore, MD USA
 ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias. UCSF Vascular Symposium April 7-9, Acute Aortic Dissection
 Aortic Dissection: Natural History What is the Natural History of Aortic Dissection? UCSF Vascular Symposium April 7-9, 2011 Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias Stephen
Aortic Dissection: Natural History What is the Natural History of Aortic Dissection? UCSF Vascular Symposium April 7-9, 2011 Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias Stephen
Redo treatment and open conversion after TEVAR
 Redo treatment and open conversion after TEVAR Roberto Chiesa Vascular Surgery, Vita-Salute University Scientific Institute San Raffaele Milan, Italy Number of procedures Off-Label indications for TEVAR
Redo treatment and open conversion after TEVAR Roberto Chiesa Vascular Surgery, Vita-Salute University Scientific Institute San Raffaele Milan, Italy Number of procedures Off-Label indications for TEVAR
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011
 Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Understanding the Predictors of Aneurysmal Degeneration in Type B Dissection
 Understanding the Predictors of Aneurysmal Degeneration in Type B Dissection A case example illustrating when early endovascular intervention may provide the best outcome. BY DITTMAR BÖCKLER, MD, PhD;
Understanding the Predictors of Aneurysmal Degeneration in Type B Dissection A case example illustrating when early endovascular intervention may provide the best outcome. BY DITTMAR BÖCKLER, MD, PhD;
Development of a Branched LSA Endograft & Ascending Aorta Endograft
 Development of a Branched LSA Endograft & Ascending Aorta Endograft Frank R. Arko III, MD Sanger Heart & Vascular Institute Carolinas Medical Center Charlotte, North Carolina, USA Disclosures Proximal
Development of a Branched LSA Endograft & Ascending Aorta Endograft Frank R. Arko III, MD Sanger Heart & Vascular Institute Carolinas Medical Center Charlotte, North Carolina, USA Disclosures Proximal
THORACOABDOMINAL AORTIC ANEURYSMS HYBRID REPAIR
 Update on Open and Endovascular Therapeutic Option for Aortic Repair CENTRE CARDIO-TORACIQUE DE MONACO Friday November 7 th, 2014 THORACOABDOMINAL AORTIC ANEURYSMS HYBRID REPAIR Roberto Chiesa Vascular
Update on Open and Endovascular Therapeutic Option for Aortic Repair CENTRE CARDIO-TORACIQUE DE MONACO Friday November 7 th, 2014 THORACOABDOMINAL AORTIC ANEURYSMS HYBRID REPAIR Roberto Chiesa Vascular
Evolution of Thoracic Aortic Surgery A Rapidly Advancing Paradigm. October 15 th, 2014 Family Practice Evening Course University of Calgary
 Evolution of Thoracic Aortic Surgery A Rapidly Advancing Paradigm October 15 th, 2014 Family Practice Evening Course University of Calgary Jehangir Appoo Division of Cardiac Surgery Libin Cardiovascular
Evolution of Thoracic Aortic Surgery A Rapidly Advancing Paradigm October 15 th, 2014 Family Practice Evening Course University of Calgary Jehangir Appoo Division of Cardiac Surgery Libin Cardiovascular
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm
 Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
History of the Powerlink System Design and Clinical Results. Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ
 History of the Powerlink System Design and Clinical Results Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ Powerlink System: Unibody-Bifurcated Design Long Main Body Low-Porosity Proprietary eptfe
History of the Powerlink System Design and Clinical Results Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ Powerlink System: Unibody-Bifurcated Design Long Main Body Low-Porosity Proprietary eptfe
Surgery for Acquired Cardiovascular Disease
 Resch et al Changes in aneurysm morphology and stent-graft configuration after endovascular repair of aneurysms of the descending thoracic aorta Timothy Resch, MD, PhD a Bansi Koul, MD, PhD d Nuno V. Dias,
Resch et al Changes in aneurysm morphology and stent-graft configuration after endovascular repair of aneurysms of the descending thoracic aorta Timothy Resch, MD, PhD a Bansi Koul, MD, PhD d Nuno V. Dias,
What is the best treatment for False Lumen growth after type B Dissection
 What is the best treatment for False Lumen growth after type B Dissection Nikolaos Tsilimparis, Fiona Rohlffs, Yuk Law, Sebastian Debus, Tilo Kölbel N. Tsilimparis, MD, PhD, FEBVS Deputy Head of German
What is the best treatment for False Lumen growth after type B Dissection Nikolaos Tsilimparis, Fiona Rohlffs, Yuk Law, Sebastian Debus, Tilo Kölbel N. Tsilimparis, MD, PhD, FEBVS Deputy Head of German
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies. Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018
 Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
Midterm Results After Endovascular Treatment of Acute, Complicated Type B Aortic Dissection
 Midterm Results After Endovascular Treatment of Acute, Complicated Type B Aortic Dissection Marek P. Ehrlich, MD, Julia Dumfarth, MD, Maria Schoder, MD, Roman Gottardi, MD, Johannes Holfeld, MD, Andrzej
Midterm Results After Endovascular Treatment of Acute, Complicated Type B Aortic Dissection Marek P. Ehrlich, MD, Julia Dumfarth, MD, Maria Schoder, MD, Roman Gottardi, MD, Johannes Holfeld, MD, Andrzej
Residual Dissection and False Lumen Aneurysm After TEVAR
 WHAT WOULD YOU DO? Residual Dissection and False Lumen Aneurysm After MODERATOR: MARK FARBER, MD PANEL: YAZAN DUWAYRI, MD; MATTHEW J. EAGLETON, MD; WILLIAM D. JORDAN Jr, MD; TILO KÖLBEL, MD, PhD; AND ERIC
WHAT WOULD YOU DO? Residual Dissection and False Lumen Aneurysm After MODERATOR: MARK FARBER, MD PANEL: YAZAN DUWAYRI, MD; MATTHEW J. EAGLETON, MD; WILLIAM D. JORDAN Jr, MD; TILO KÖLBEL, MD, PhD; AND ERIC
UC SF An Algorithm to Choose Which Uncomplicated (Asymptomatic) Acute Type B Dissection Patients Should Undergo TEVAR. Disclosures.
 An Algorithm to Choose Which Uncomplicated (Asymptomatic) Acute Type B Dissection Patients Should Undergo TEVAR Disclosures Royalties and research grant support from Cook Medical, Inc. Jade S. Hiramoto,
An Algorithm to Choose Which Uncomplicated (Asymptomatic) Acute Type B Dissection Patients Should Undergo TEVAR Disclosures Royalties and research grant support from Cook Medical, Inc. Jade S. Hiramoto,
Femoral Versus Aortic Cannulation for Surgery of Chronic Ascending Aortic Aneurysm
 Femoral Versus Aortic Cannulation for Surgery of Chronic Ascending Aortic Aneurysm Fitsum Lakew, MD, Piotr Pasek, MD, Michael Zacher, MD, Anno Diegeler, MD, and Paul P. Urbanski, MD Department of Cardiovascular
Femoral Versus Aortic Cannulation for Surgery of Chronic Ascending Aortic Aneurysm Fitsum Lakew, MD, Piotr Pasek, MD, Michael Zacher, MD, Anno Diegeler, MD, and Paul P. Urbanski, MD Department of Cardiovascular
Current treatment of Aortic Aneurysms and Dissections. Adam Keefer, MD, FACS Sean Hislop, MD, FACS
 Current treatment of Aortic Aneurysms and Dissections Adam Keefer, MD, FACS Sean Hislop, MD, FACS Patient 1 69 year old well-educated man with reoccurring pain in his upper abdomen and a pulsatile mass.
Current treatment of Aortic Aneurysms and Dissections Adam Keefer, MD, FACS Sean Hislop, MD, FACS Patient 1 69 year old well-educated man with reoccurring pain in his upper abdomen and a pulsatile mass.
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
Dissection de type B: l étude Instead et corollaire stratégique
 Dissection de type B: l étude Instead et corollaire stratégique Christoph A. Nienaber, MD, FACC University Rostock Heartcenter Med. Clinic I Cardiology christoph.nienaber@med.uni-rostock.de Type B aortic
Dissection de type B: l étude Instead et corollaire stratégique Christoph A. Nienaber, MD, FACC University Rostock Heartcenter Med. Clinic I Cardiology christoph.nienaber@med.uni-rostock.de Type B aortic
Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely
 Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely Daniela Branzan, MD, Department of Vascular Surgery University Hospital Leipzig Disclosure
Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely Daniela Branzan, MD, Department of Vascular Surgery University Hospital Leipzig Disclosure
Acute aortic dissection frequently causes life-threatening SURGERY FOR ADULT CARDIOVASCULAR DISEASE
 SURGERY FOR ADULT CARDIOVASCULAR DISEASE PERCUTANEOUS BALLOON FENESTRATION AND STENTING FOR LIFE-THREATENING ISCHEMIC COMPLICATIONS IN PATIENTS WITH ACUTE AORTIC DISSECTION Suzanne M. Slonim, MD D. Craig
SURGERY FOR ADULT CARDIOVASCULAR DISEASE PERCUTANEOUS BALLOON FENESTRATION AND STENTING FOR LIFE-THREATENING ISCHEMIC COMPLICATIONS IN PATIENTS WITH ACUTE AORTIC DISSECTION Suzanne M. Slonim, MD D. Craig
ABERRANT RIGHT SUBCLAVIAN ARTERY AND CALCIFIED ANEURYSM OF. Jose Rubio-Alvarez, Juan Sierra-Quiroga, Belen Adrio Nazar and Javier Garcia Carro.
 ABERRANT RIGHT SUBCLAVIAN ARTERY AND CALCIFIED ANEURYSM OF KOMMERELL S DIVERTICULUM : AN ALTERNATIVE APPROACH. Jose Rubio-Alvarez, Juan Sierra-Quiroga, Belen Adrio Nazar and Javier Garcia Carro. Department
ABERRANT RIGHT SUBCLAVIAN ARTERY AND CALCIFIED ANEURYSM OF KOMMERELL S DIVERTICULUM : AN ALTERNATIVE APPROACH. Jose Rubio-Alvarez, Juan Sierra-Quiroga, Belen Adrio Nazar and Javier Garcia Carro. Department
Type II arch hybrid debranching procedure
 Safeguards and Pitfalls Type II arch hybrid debranching procedure Prashanth Vallabhajosyula, Wilson Y. Szeto, Nimesh Desai, Caroline Komlo, Joseph E. Bavaria Division of Cardiovascular Surgery, University
Safeguards and Pitfalls Type II arch hybrid debranching procedure Prashanth Vallabhajosyula, Wilson Y. Szeto, Nimesh Desai, Caroline Komlo, Joseph E. Bavaria Division of Cardiovascular Surgery, University
Abdominal Aortic Aneurysms. A Surgeons Perspective Dr. Derek D. Muehrcke
 Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Performance of the conformable GORE TAG device in Type B aortic dissection from the GORE GREAT real world registry
 University of Milan Thoracic Aortic Research Center Performance of the conformable GORE TAG device in Type B aortic dissection from the GORE GREAT real world registry Santi Trimarchi, MD, PhD Associate
University of Milan Thoracic Aortic Research Center Performance of the conformable GORE TAG device in Type B aortic dissection from the GORE GREAT real world registry Santi Trimarchi, MD, PhD Associate
Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic
 Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic Aneurysm History A 56-year-old gentleman, who had been referred
Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic Aneurysm History A 56-year-old gentleman, who had been referred
Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery
 Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery Are Young Patients More Likely to Develop Adverse Aortic Remodeling of the Remnant Aorta Over Time? Suk Jung Choo¹, Jihoon Kim¹,
Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery Are Young Patients More Likely to Develop Adverse Aortic Remodeling of the Remnant Aorta Over Time? Suk Jung Choo¹, Jihoon Kim¹,
Aortic Arch/ Thoracoabdominal Aortic Replacement
 Aortic Arch/ Thoracoabdominal Aortic Replacement Joseph S. Coselli, M.D. Vice Chair, Department of Surgery Professor, Chief, and Cullen Foundation Endowed Chair Division of Cardiothoracic Surgery Baylor
Aortic Arch/ Thoracoabdominal Aortic Replacement Joseph S. Coselli, M.D. Vice Chair, Department of Surgery Professor, Chief, and Cullen Foundation Endowed Chair Division of Cardiothoracic Surgery Baylor
SELECTIVE ANTEGRADE TECHNIQUE OF CHOICE
 SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
How to achieve a successful proximal sealing in TEVAR? Pr L Canaud
 How to achieve a successful proximal sealing in TEVAR? Pr L Canaud CHU de Montpellier France Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic. Proximal neck
How to achieve a successful proximal sealing in TEVAR? Pr L Canaud CHU de Montpellier France Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic. Proximal neck
Percutaneous Approaches to Aortic Disease in 2018
 Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Emerging Roles for Distal Aortic Interventions in Type A Dissection Surgery
 Emerging Roles for Distal Aortic Interventions in Type A Dissection Surgery Type A Dissection Workshop 2014 CCC Vancouver Oct 26 th, 2014 Jehangir Appoo Libin Cardiovascular Institute University of Calgary
Emerging Roles for Distal Aortic Interventions in Type A Dissection Surgery Type A Dissection Workshop 2014 CCC Vancouver Oct 26 th, 2014 Jehangir Appoo Libin Cardiovascular Institute University of Calgary
In recent years, the field of endovascular surgery has revolutionized
 Proven Performance cross Indications Device Selection and ase Planning for the Treatment of Type Dissections With the onformable GORE TG Thoracic Endoprosthesis What to know regarding stent-graft sizing
Proven Performance cross Indications Device Selection and ase Planning for the Treatment of Type Dissections With the onformable GORE TG Thoracic Endoprosthesis What to know regarding stent-graft sizing
Aortic Arch Treatment Open versus Endo Evidence versus Zeitgeist. M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria
 Aortic Arch Treatment Open versus Endo Evidence versus Zeitgeist M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Evidence Surgical aortic arch replacement with a Dacron
Aortic Arch Treatment Open versus Endo Evidence versus Zeitgeist M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Evidence Surgical aortic arch replacement with a Dacron
UC SF. Disclosures. Thoracic Endovascular Aortic Repair 4/24/2009. Management of Acute Dissections: Is There Still a Role for Open Surgery?
 UC SF Management of Acute Dissections: Is There Still a Role for Open Surgery? Darren B. Schneider, M.D. Assistant Professor of Surgery and Radiology Division of Vascular Surgery University of California
UC SF Management of Acute Dissections: Is There Still a Role for Open Surgery? Darren B. Schneider, M.D. Assistant Professor of Surgery and Radiology Division of Vascular Surgery University of California
Department of Cardiovascular Surgery, Beijing Anzhen Hospital of Capital Medical University, Beijing Aortic Disease Center, Beijing, China;
 Featured Article Sun s procedure of total arch replacement using a tetrafurcated graft with stented elephant trunk implantation: analysis of early outcome in 398 patients with acute type A aortic dissection
Featured Article Sun s procedure of total arch replacement using a tetrafurcated graft with stented elephant trunk implantation: analysis of early outcome in 398 patients with acute type A aortic dissection
Surgical treatment for retrograde type A aortic dissection after endovascular stent graft placement for type B dissection
 Interactive CardioVascular and Thoracic Surgery Advance Access published February 22, 2012 Interactive CardioVascular and Thoracic Surgery 0 (2012) 1 5 doi:10.1093/icvts/ivs043 INSTITUTIONAL REPORT Surgical
Interactive CardioVascular and Thoracic Surgery Advance Access published February 22, 2012 Interactive CardioVascular and Thoracic Surgery 0 (2012) 1 5 doi:10.1093/icvts/ivs043 INSTITUTIONAL REPORT Surgical
F. Terzi, S. Gianstefani, R. Fattori. cardiology and interventional cardiology unit, ospedali riuniti Marche nord, pesaro.
 14_14 03/02/17 14.16 Pagina 101 Type B aortic dissection: it should Be TreaTed F. Terzi, S. Gianstefani, R. Fattori cardiology and interventional cardiology unit, ospedali riuniti Marche nord, pesaro.
14_14 03/02/17 14.16 Pagina 101 Type B aortic dissection: it should Be TreaTed F. Terzi, S. Gianstefani, R. Fattori cardiology and interventional cardiology unit, ospedali riuniti Marche nord, pesaro.
TEVAR. (Thoracic Endovascular Aortic Repair) for Aneurysm and Dissection. Bruce Tjaden MD Vascular Surgery Fellow
 Department of Cardiothoracic & Vascular Surgery McGovern Medical School / The University of Texas Health Science Center at Houston TEVAR (Thoracic Endovascular Aortic Repair) for Aneurysm and Dissection
Department of Cardiothoracic & Vascular Surgery McGovern Medical School / The University of Texas Health Science Center at Houston TEVAR (Thoracic Endovascular Aortic Repair) for Aneurysm and Dissection
Is it time to stent the ascending aorta? Martin Czerny
 Is it time to stent the ascending aorta? Martin Czerny Content Basic insights into pathological process Dissection induced geometry changes Initial attempts Dedicated programme Future developments Summary
Is it time to stent the ascending aorta? Martin Czerny Content Basic insights into pathological process Dissection induced geometry changes Initial attempts Dedicated programme Future developments Summary
A Case of Acute Type B Aortic Dissection: Limited Role of Laboratory Testing for the Diagnosis of Mesenteric Ischemia
 Case Report A Case of Acute Type B Aortic Dissection: Limited Role of Laboratory Testing for the Diagnosis of Mesenteric Ischemia Koichi Akutsu, MD, 1 Hitoshi Matsuda, MD, 2 Hiroaki Sasaki, MD, 2 Kenji
Case Report A Case of Acute Type B Aortic Dissection: Limited Role of Laboratory Testing for the Diagnosis of Mesenteric Ischemia Koichi Akutsu, MD, 1 Hitoshi Matsuda, MD, 2 Hiroaki Sasaki, MD, 2 Kenji
Diseases of the Aorta
 Diseases of the Aorta ASE Review 2018 Susan E Wiegers, MD, FASE, FACC Professor of Medicine My great friend Dr. Roberto Lang Disclosure None related to this presentation 1 Objectives Aneurysm Dissection
Diseases of the Aorta ASE Review 2018 Susan E Wiegers, MD, FASE, FACC Professor of Medicine My great friend Dr. Roberto Lang Disclosure None related to this presentation 1 Objectives Aneurysm Dissection
INNOVATION IN CARDIOVASCULAR MEDICINE. AORTA CLINIC. Dr. Jaime Camacho M. Director, Aorta Clinic
 AORTA CLINIC Aorta Clinic Calle 163 A # 13 B- 60 Fundadores Building, 3rd floor Bogota D.C. Colombia Direct Telephone: 6672791 PBX: 667-2727 ext. 3149 e-mail: clinicadeaorta@cardioinfantil.org AORTA CLINIC.
AORTA CLINIC Aorta Clinic Calle 163 A # 13 B- 60 Fundadores Building, 3rd floor Bogota D.C. Colombia Direct Telephone: 6672791 PBX: 667-2727 ext. 3149 e-mail: clinicadeaorta@cardioinfantil.org AORTA CLINIC.
Case Report International Journal of Basic and Clinical Studies (IJBCS) 2013;1(1): Elbey MA et al.
 Treatment of Interrupted Aorta in Adult Patients; a Challenge Both in Surgery and Transcatheter Intervention Mehmet Ali Elbey MD 1, Ahmet Caliskan MD 2, Ferhat Isık MD 1, Faruk Ertas MD 1, Mehmet Serdar
Treatment of Interrupted Aorta in Adult Patients; a Challenge Both in Surgery and Transcatheter Intervention Mehmet Ali Elbey MD 1, Ahmet Caliskan MD 2, Ferhat Isık MD 1, Faruk Ertas MD 1, Mehmet Serdar
State of Art Hybrid Approach
 State of Art Hybrid Approach for Complex Aorta Diseases Won Ho Kim, MD Division of Cardiology, Eulji University Hospital Eulji University School of Medicine, Daejeon, Korea Introduction.Hybrid procedure
State of Art Hybrid Approach for Complex Aorta Diseases Won Ho Kim, MD Division of Cardiology, Eulji University Hospital Eulji University School of Medicine, Daejeon, Korea Introduction.Hybrid procedure
Case 9799 Stanford type A aortic dissection: US and CT findings
 Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD
 Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD Foeke JH Nauta, MD, PhD Resident Cardiothoracic Surgery, Academic Medical Center, Amsterdam Disclosure
Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD Foeke JH Nauta, MD, PhD Resident Cardiothoracic Surgery, Academic Medical Center, Amsterdam Disclosure
