Anesthetic management of Wolff-Parkinson-White Syndrome. Daniel Crosby, BSN Westminster College. December 13, 2013
|
|
|
- Christine Knight
- 6 years ago
- Views:
Transcription
1 Anesthetic management of Wolff-Parkinson-White Syndrome Daniel Crosby, BSN Westminster College December 13, 2013 Keywords: Wolff-Parkinson-White syndrome, accessory pathway, arrhythmia, general anesthesia, ventricular pre-excitation Wolff-Parkinson White syndrome (WPW) is a ventricular pre-excitation syndrome resulting from an aberrant conduction pathway between the atria and ventricles known as "bundle of Kent." 1 Undiagnosed WPW can be worrisome under anesthesia because some anesthetic drugs have a tendency to alter the physiology of atrioventricular (AV) conduction resulting in lifethreatening arrhythmias. Also, any increase in sympathetic activity can be arrhythmogenic in patients with WPW. 2,3 Therefore, anesthetic management of these patients should be customized according to the surgical procedure and the presenting condition of the patient. The following is a case report for WPW under general anesthesia for diagnostic laparoscopy. Case Report A 19-year-old female with a past medical history significant for mild congestive heart failure, cerebrovascular accident, ventricular septal defect (VSD), WPW, gastroesophageal reflux disease (GERD), and a five pack-year smoking history presented for diagnostic laparoscopy due to chronic pelvic pain and severe dysmenorrhea unresponsive to medical treatment. The patient had undergone general anesthesia once previously for repair of VSD without any anesthetic or surgical complications. The patient's medication regime included only omeprazole 20 mg daily. She did not have any drug allergies. On pre-anesthetic evaluation, the patient was comfortable with a heart rate of 100 beats per minute, blood pressure of 129/84 mm Hg, SpO 2 was 98%, and respirations were unlabored at 14 breaths per minute. A complete blood count and a type and cross match were drawn with no abnormal results. The patient was premedicated with midazolam 2 mg and fentanyl 50 mcg intravenously (IV) in the preoperative holding area. Once in the operating room, one hundred percent oxygen was administered via facemask and standard AANA monitors were applied in addition to a Zoll monitor with defibrillator pads. Antiarrhythmic drugs including adenosine, esmolol, lidocaine, and amiodarone were also available and prepared for use. Following preoxygenation, IV fentanyl 100 mcg, lidocaine 80 mg, propofol 170 mg, and rocuronium 45 mg were administered for induction of anesthesia. Placement of a 7.0 mm oral endotracheal tube was confirmed by the presence of bilateral breath sounds, and end tidal CO 2 on capnography.
2 General anesthesia was maintained with delivery of 2.5% expired Sevoflurane in combination with oxygen 1 L/min and air 1 L/min. Fentanyl was administered in 50 mcg intervals and IV morphine was titrated to a respiratory rate of 11 breaths per minute towards the end of the case with a total of 4 mg given. Lead II was used for intraoperative electrocardiograph (ECG) monitoring which sustained the expected findings of a shortened PR interval, delta wave, and widened QRS as seen on the preoperative 12-lead ECG. Neuromuscular blockade was antagonized with administration of IV glycopyrrolate and neostigmine. An uneventful deep extubation was performed and the patient had a smooth emergence. An agreeable postoperative recovery without any adverse events or anesthetic complaints ensued. In post-anesthesia recovery, she was comfortable, alert, and oriented. Vital signs included a pulse rate of 99 beats per minute, blood pressure of 121/84 mm Hg, respiratory rate of 12 breaths per minute, and 100% SpO 2. Discussion WPW syndrome is the most common form of preexcitation, which refers to early depolarization of the ventricles by an abnormal conduction pathway from the atria. However, WPW, with an incidence of approximately 0.3%, is not extremely common in the general population. 4 This cardiac conduction disorder may not always be detected preoperatively, as it is rarely recognized without an accompanying arrhythmia. Diagnosis may be accomplished via a thorough history along with telltale ECG changes which include a slurring of the QRS complex known as a delta wave, a shortened PR interval, and a lengthened QRS complex. These notorious ECG changes are the result of ventricular contraction being triggered by the confluence of a faster, aberrant pathway impulse with the normal AV nodal pathway impulse. When an action potential follows the deviant pathway, it bypasses the AV node and its physiologic delay in impulse transmission, resulting in early depolarization of the part of the ventricle where the accessory pathway ends. This is the source of the short PR interval and slurring of the QRS complex. The rest of the ventricular muscle is usually depolarized as the normal pathway impulse catches up, resulting in a widened QRS complex. 1,4 These patients are susceptible to life threatening tachyarrhythmias such as paroxysmal supraventricular tachycardia, atrial fibrillation (A-fib), atrial flutter, ventricular tachycardia, and vetricular fibrillation. 3,4 In addition, preexcitation can be associated with other cardiac anomolies, including Ebstein's anomoly, mitral valve prolapse, and cardiomyopathies. Situations and factors which can trigger arrhythmias related to the delivery of anesthesia include drug administration, direct laryngoscopy, tracheal intubation, surgical stimulation, light plane of anesthesia, pain, hypercapnia, acidosis, and even transient hypoxia. 1,2,3,4 Therefore, regional anesthesia is the preferred anesthetic technique when appropriate, due to the avoidance of direct laryngoscopy and anesthetic drugs that can alter AV nodal physiology. Epidural is preferred over spinal anesthesia due to controlled, segmental block, avoidance of polypharmacy, and better hemodynamic stability. 2,3
3 Drugs which precipitate tachycardia such as the antimuscarinics (atropine, glycopyrrolate), histamine releasing agents (atracurium), vagolytics (pancuronium) and sympathomimetics (ketamine, ephedrine), particularly beta-1 agonists, can be disadvantageous in patients with WPW and should be avoided when possible. 2 Sevoflurane and isoflurane have no effect on accessory pathway conduction, and isoflurane is the preferred volatile agent for WPW as it actually suppresses the accessory pathway. 3 Other drugs that have either a beneficial effect or no effect on aberrant pathway conduction and can be safely used include propofol, fentanyl, droperidol, thiopental, rocuronium, cis-atracurium, mivacurium, benzodiazepines, and nitrous oxide. Additional drugs that can be detrimental and should be avoided include halothane, neostigmine, digitalis, verapamil, and oxytocin. Digitals and verapamil can dangerously accelerate the ventricular response in A-fib and atrial flutter because they decrease conduction through the AV node, thus favoring conduction via the accessory pathway. 1,2,3,4 Laparoscopic surgery usually necessitates general anesthesia and endotracheal intubation in order to prevent aspiration and respiratory compromise from induction of pneumoperitoneum. There are however, several case reports of laparoscopic surgery being performed under regional anesthesia including spinal and epidural blockade. With this particular patient's history of GERD, it was determined that a balanced general anesthetic with modified rapid sequence induction and endotracheal intubation with cricoid pressure was the safest option. Had isoflurane been available at this particular facility, it would have been the agent of choice for maintenance of general anesthesia. Sevoflurane was the next best available option. The risks and benefits of reversing neuromuscular blockade were weighed judiciously. A slightly lower dose of glycopyrrolate (0.4 mg) with neostigmine 3 mg was given, which produced no significant change in heart rate and sufficient reversal of neuromuscular blockade as evidenced by 4:4 train of four response with sustained tetany. Until a more ideal drug is available, glycopyrrolate is preferred over atropine when antimuscarinic administration is necessary. 4 Deep extubation is a prudent option to avert the negative consequences of sympathetic stimulation on emergence from general anesthesia. Use of a larngyotracheal anesthesia kit would also be beneficial in that respect. Patients who are hemodynamically stable and comfortable usually do not require any treatment pre-operatively. 5 However, thoughtful preparation, as with most anesthetics, can mean the difference between life and death for patients with WPW. Drugs such as adenosine, phenylephrine, beta blockers, and antiarrhythmics should be available and ready. A defibrillator should also be on hand. If an arrhythmia arises resulting in hemodynamic instability, direct cardioversion is indicated. 6 In hemodynamically stable patients, class-1 antiarrhythmics such as disopyramide, lidocaine, and procainamide, as well as the calcium channel blocker, diltiazem can be used to interrupt re-entrant tachycardias. 2,4 Despite its infrequent occurrence in the general population, WPW will likely be encountered by all anesthesia professionals at some point in their careers. Commonly, patients will not have been diagnosed with WPW, and a sudden manifestation of WPW under anesthesia can be life
4 threatening. Therefore, it is important for the anesthesia provider to know and understand WPW, the effects of anesthetic drugs, and how to safely manage these patients. Mentors: James Stimpson CRNA, DNP Dee Bambrough CRNA
5 References 1. Sahu S, Karna S, Karna A, Lata I, Kapoor D. Anaesthetic management of Wolff-Parkinson- White syndrome for hysterectomy. Indian J Anaesth [serial online]. August 2011; 55(4): Available from: Academic Search Premier, Ipswich, MA. Accessed August 8, Kabade S, Sheikh S, Periyadka B. Anaesthetic management of a case of Wolff-Parkinson- White syndrome. Indian J Anaesth [serial online]. August 2011;55(4): Available from: Academic Search Premier, Ipswich, MA. Accessed August 8, Rahul A, Patel R. Anaesthetic Management of W.P.W. Syndrome. Internet Journal Of Anesthesiology [serial online]. February 5, 2007;11(2):10. Available from: CINAHL with Full Text, Ipswich, MA. Accessed August 9, Morgan E, Mikhail M, Murray M. Clinical Anesthesiology. 4th ed. New York: Lange Medical Books/McGraw Hill Medical Pub. Division; 2006: Shora A, Gurkoo S, Farooqi A, Qazi M, Nisa W. Anaesthetic management of Wolff Parkinson White syndrome for cesarean section. Internet Journal Of Anesthesiology [serial online]. June 26, 2008;16(2):24. Available from: CINAHL with Full Text, Ipswich, MA. Accessed August 8, Namshikar V, Bharne S. Anesthesia for Wolff-Parkinson-White syndrome: A report of two cases. Saudi J Anaesth [serial online]. July 2013;7(3): Available from: MEDLINE, Ipswich, MA. Accessed August 29, 2013
6 Abstract Wolff-Parkinson White syndrome (WPW) is an electrophysiological abnormality in which an aberrant conduction pathway exists between the atria and ventricles of the heart. With an incidence of 0.3% in the general population, it is likely that WPW will be encountered by almost all anesthesia providers at some point in their careers. 4 Fundamentally, the safe management of these patients necessitates a sound understanding of the pathophysiology of WPW, the effects of anesthetic and adjuvant drugs on cardiac impulse conduction, factors that may precipitate lifethreatening arrhythmias, and how these arrhythmias should be treated. Although regional, specifically epidural, anesthesia is the most ideal anesthetic technique for patients who have WPW, these patients can be safely managed under general anesthesia. The anesthetic technique should be suited to the individual patient as well as the procedure requiring anesthesia services. The following case report demonstrates safe management of a 19 year old female with WPW undergoing general anesthesia for diagnostic laparoscopy, provides a review of WPW pathophysiology, and includes a discussion on the essentials of delivering a safe anesthetic and better patient outcomes.
7 Three objectives that utilize a higher level of learning in Bloom's Taxonomy: Objective #1- Students will differentiate between Wolff-Parkinson White syndrome and other cardiac conduction abnormalities based on electrocardiogram findings and explain these specific changes related to its pathophysiology. Objective #2- Students will tailor, revise, and justify modifications in their anesthetic plan to improve patient safety and outcomes for patients with Wolff-Parkinson White syndrome. Objective #3- Students will appraise the safety of anesthetic drugs, adjuvant medications, and treatment options for patients with Wolff-Parkinson White syndrome to determine the most appropriate medications, techniques and interventions.
8 Multiple Choice Questions: #1- Wolff-Parkinson White syndrome may be identified on an electrocardiogram by all of the following, except: A. a delta wave B. a shortened PR interval C. a prolonged PR interval D. a lengthened QRS complex Answer- C: Diagnosis may be accomplished via a thorough history along with telltale ECG changes which include a slurring of the QRS complex known as a delta wave, a shortened PR interval, and a lengthened QRS complex. #2- The anesthetic technique of choice for a patient with Wolff-Parkinson White syndrome undergoing a total vaginal hysterectomy would be: A. Regional spinal B. Regional epidural C. General ETT D. General LMA Answer- B: Regional anesthesia is the preferred anesthetic technique when appropriate, due to the avoidance of direct laryngoscopy and anesthetic drugs that can alter AV nodal physiology. Epidural is preferred over spinal anesthesia due to controlled, segmental block, avoidance of polypharmacy, and better hemodynamic stability. #3- Factors that can trigger arrhythmias related to the delivery of anesthesia in patients who have Wolff-Parkinson White syndrome include (select five that apply): A. direct laryngoscopy, B. light plane of anesthesia C. adequate analgesia D. hypoxia E. hypercapnia F. tracheal intubation G. alkalosis Answer- A,B,D,E,F: Situations and factors that can trigger arrhythmias related to the delivery of anesthesia include drug administration, direct laryngoscopy, tracheal intubation, surgical stimulation, light plane of anesthesia, pain, hypercapnia, acidosis, and even transient hypoxia. #4- All of the following may be deleterious when administered to a patient with Wolff-Parkinson White syndrome, except: A. beta-1 antagonists B. antimuscarinics C. histamine releasing agents D. ketamine
9 Answer- A: Drugs that precipitate tachycardia such as the antimuscarinics (atropine, glycopyrrolate), histamine releasing agents (atracurium), vagolytics (pancuronium) and sympathomimetics (ketamine, ephedrine), particularly beta-1 agonists, can be disadvantageous in patients with WPW and should be avoided when possible. Beta-1 antagonists may be used to treat tachyarrhythmias associated with WPW. #5- The volatile anesthetic which suppresses the accessory pathway conduction and is the volatile agent of choice in patients with Wolff-Parkinson White syndrome is: A. Sevoflurane B. Desflurane C. Halothane D. Isoflurane Answer- D: Sevoflurane and isoflurane have no effect on accessory pathway conduction, and isoflurane is the preferred volatile agent for Wolff-Parkinson White syndrome as it actually suppresses the accessory pathway. #6- Two drugs that should be strictly avoided because they can dangerously accelerate the ventricular response to atrial fibrillation and atrial flutter in patients with Wolff-Parkinson White syndrome by decreasing conduction through the AV node are: A. ketamine and ephedrine B. verapamil and digoxin C. benzodiazepines and mivacurium D. disopyramide and diltiazem Answer- B: Digitals and verapamil can dangerously accelerate the ventricular response in atrial fibrillation and atrial flutter because they decrease conduction through the AV node, thus favoring conduction via the accessory pathway. #7- If administration of an antimuscarinic is necessary, which agent is preferred for patients with Wolff-Parkinson White syndrome: A. ipratropium B. atropine C. glycopyrrolate D. scopolamine Answer- C: Until a more ideal drug is available, glycopyrrolate is the agent of choice when antimuscarinic administration is necessary. #8- The incidence of Wolff-Parkinson White syndrome in the general population is approximately: A. 13% B % C. 5% D. 0.3%
10 Answer- D: With an incidence of approximately 0.3%, WPW is not extremely common in the general population. #9 You are managing a 19 year old female who has Wolff-Parkinson White syndrome under general anesthesia for a laparoscopic cholecystectomy. Suddenly, a supraventricular tachyarrhythmia arises, resulting in significant hemodynamic instability. Which of the following is indicated: A. direct cardioversion B. a diltiazem drip C. no treatment is required D. IV lidocaine 1.5 mg/kg Answer- A: If an arrhythmia arises resulting in hemodynamic instability, direct cardioversion is indicated. 6 In hemodynamically stable patients, class-1 antiarrhythmics such as disopyramide, lidocaine, and procainamide, as well as the calcium channel blocker diltiazem, can be used to interrupt re-entrant tachycardias. #10- Which of the following statements is not true regarding Wolff-Parkinson White syndrome: A. Patients who are hemodynamically stable and comfortable usually do not require any treatment pre-operatively. B. WPW may not always be detected preoperatively as it is rarely recognized without an accompanying arrhythmia. C. WPW is so extremely rare that most anesthesia providers will not encounter it during their career. D. WPW can be associated with other cardiac anomolies, including Ebstein's anomoly, mitral valve prolapse, and cardiomyopathies. Answer- C: Despite its infrequent occurrence in the general population, WPW will likely be encountered by all anesthesia professionals at some point in their career. A,B, & D are all true statements.
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Sustained tachycardia with wide QRS
 Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Paramedic Rounds. Tachyarrhythmia's. Sean Sutton Dallas Wood
 Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
EKG Abnormalities. Adapted from:
 EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
Patient with Wolff-Parkinson-White syndrome with intermittent pre-excitation under subarachnoid block for urological surgery
 Case Report Patient with Wolff-Parkinson-White syndrome with intermittent pre-excitation under subarachnoid block for urological surgery Address for correspondence: Dr. Rakesh Garg, 58-E, Kavita Colony,
Case Report Patient with Wolff-Parkinson-White syndrome with intermittent pre-excitation under subarachnoid block for urological surgery Address for correspondence: Dr. Rakesh Garg, 58-E, Kavita Colony,
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD
 Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
ANESTHESIA DRUG REVIEW
 ANESTHESIA REVIEW CAPA S 39 TH ANNUAL CONFERENCE PALM SPRINGS OCTOBER 10, 2015 ROBERT F. KOPEL, MD, FACP, FCCP HOAG HOSPITAL CARDIAC ANESTHESIOLOGIST ASSISTANT CLINICAL PROFESSOR UCLA SCHOOL OF MEDICINE
ANESTHESIA REVIEW CAPA S 39 TH ANNUAL CONFERENCE PALM SPRINGS OCTOBER 10, 2015 ROBERT F. KOPEL, MD, FACP, FCCP HOAG HOSPITAL CARDIAC ANESTHESIOLOGIST ASSISTANT CLINICAL PROFESSOR UCLA SCHOOL OF MEDICINE
ANTI - ARRHYTHMIC DRUGS
 ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
4/14/15 HTEC 91. Topics for Today. Guess That Rhythm. Premature Ventricular Contractions (PVCs) Ventricular Rhythms
 4/14/15 Topics for Today HTEC 91 Medical Office Diagnostic Tests Week 5 Ventricular Rhythms PVCs: Premature Ventricular Contractions VT: Ventricular Tachycardia VF: Ventricular Fibrillation Asystole Study
4/14/15 Topics for Today HTEC 91 Medical Office Diagnostic Tests Week 5 Ventricular Rhythms PVCs: Premature Ventricular Contractions VT: Ventricular Tachycardia VF: Ventricular Fibrillation Asystole Study
ARRHYTHMIAS IN THE ICU
 ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
Arrhythmias. Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium.
 Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Ventricular Tachycardia Basics
 Ventricular Tachycardia Basics OVERVIEW Ventricular refers to the ventricles of the heart; tachycardia is the medical term for rapid heart rate The heart of the dog or cat is composed of four chambers;
Ventricular Tachycardia Basics OVERVIEW Ventricular refers to the ventricles of the heart; tachycardia is the medical term for rapid heart rate The heart of the dog or cat is composed of four chambers;
CHAPTER 11. General and Local Anesthetics. Anesthetics. Anesthesia. Eliza Rivera-Mitu, RN, MSN NDEG 26 A
 CHAPTER 11 General and Local Anesthetics Eliza Rivera-Mitu, RN, MSN NDEG 26 A Anesthetics Agents that depress the central nervous system (CNS) Depression of consciousness Loss of responsiveness to sensory
CHAPTER 11 General and Local Anesthetics Eliza Rivera-Mitu, RN, MSN NDEG 26 A Anesthetics Agents that depress the central nervous system (CNS) Depression of consciousness Loss of responsiveness to sensory
Atrial fibrillation in the ICU
 Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
Review Packet EKG Competency This packet is a review of the information you will need to know for the proctored EKG competency test.
 Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
CSI Skills Lab #5: Arrhythmia Interpretation and Treatment
 CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
Patient Examination. Objectives for Presentation RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS 9/8/2016
 RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS Ryan Fries, DVM, DACVIM (Cardiology) Clinical Assistant Professor University of Illinois Department of Clinical Veterinary Medicine
RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS Ryan Fries, DVM, DACVIM (Cardiology) Clinical Assistant Professor University of Illinois Department of Clinical Veterinary Medicine
Sudden cardiac death: Primary and secondary prevention
 Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
MEDICATIONS CARDIOVASCULAR URGENCIES & EMERGENCIES 12/29/14. Cardiovascular Emergency Medications. Cardiovascular Emergency Medications
 CARDIOVASCULAR URGENCIES & EMERGENCIES Steven Ganzberg, DMD, MS Director of Anesthesiology, Century City Outpatient Surgery Center Clinical Professor of Anesthesiology, UCLA School of Dentistry sganzberg@ucla.edu
CARDIOVASCULAR URGENCIES & EMERGENCIES Steven Ganzberg, DMD, MS Director of Anesthesiology, Century City Outpatient Surgery Center Clinical Professor of Anesthesiology, UCLA School of Dentistry sganzberg@ucla.edu
ECGs and Arrhythmias: Family Medicine Board Review 2009
 Rate Rhythm Intervals Hypertrophy ECGs and Arrhythmias: Family Medicine Board Review 2009 Axis Jess (Fogler) Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Ischemia Overview
Rate Rhythm Intervals Hypertrophy ECGs and Arrhythmias: Family Medicine Board Review 2009 Axis Jess (Fogler) Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Ischemia Overview
TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT
 Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Supraventricular Tachycardia: From Fetus to Adult. Mohamed Hamdan, MD
 Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
PHARMACOLOGY OF ARRHYTHMIAS
 PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Northwest Community Healthcare Paramedic Education Program AV Conduction Defects/AV Blocks Connie J. Mattera, M.S., R.N., EMT-P
 Northwest Community Healthcare Paramedic Education Program AV Conduction Defects/ Connie J. Mattera, M.S., R.N., EMT-P Reading assignments: Bledsoe Vol. 3: pp. 88-93; 120-121 (atropine, norepinephrine,
Northwest Community Healthcare Paramedic Education Program AV Conduction Defects/ Connie J. Mattera, M.S., R.N., EMT-P Reading assignments: Bledsoe Vol. 3: pp. 88-93; 120-121 (atropine, norepinephrine,
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Anesthetic concerns when paralyzing is not an option. By: Ashley Evick, BSN, SRNA
 Anesthetic concerns when paralyzing is not an option By: Ashley Evick, BSN, SRNA Introduction Neuromuscular blockade is utilized in many of the surgeries performed today. There are two types of neuromuscular
Anesthetic concerns when paralyzing is not an option By: Ashley Evick, BSN, SRNA Introduction Neuromuscular blockade is utilized in many of the surgeries performed today. There are two types of neuromuscular
Atrial Fibrillation 10/2/2018. Depolarization & ECG. Atrial Fibrillation. Hemodynamic Consequences
 Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
physiology 6 Mohammed Jaafer Turquoise team
 15 physiology 6 Mohammed Jaafer 22-3-2016 Turquoise team Cardiac Arrhythmias and Their Electrocardiographic Interpretation Today, we are going to talk about the abnormal excitation. As we said before,
15 physiology 6 Mohammed Jaafer 22-3-2016 Turquoise team Cardiac Arrhythmias and Their Electrocardiographic Interpretation Today, we are going to talk about the abnormal excitation. As we said before,
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
WOLFF PARKINSON WHITE SYNDROME. Katarzyna Bigaj PGY-1
 WOLFF PARKINSON WHITE SYNDROME Katarzyna Bigaj PGY-1 Preexcitation is defined as a premature activation of the ventricular myocardium by an impulse that travels by an anomalous path and avoids physiologic
WOLFF PARKINSON WHITE SYNDROME Katarzyna Bigaj PGY-1 Preexcitation is defined as a premature activation of the ventricular myocardium by an impulse that travels by an anomalous path and avoids physiologic
Case #1. 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136
 Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ.
 «Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology
 Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
Wolff-Parkinson-White Syndrome
 Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
ECGs and Arrhythmias: Family Medicine Board Review 2012
 Overview ECGs and Arrhythmias: Family Medicine Board Review 2012 Jess Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Bundle branch blocks Quick review of ischemia Arrhythmias
Overview ECGs and Arrhythmias: Family Medicine Board Review 2012 Jess Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Bundle branch blocks Quick review of ischemia Arrhythmias
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT
 ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
Dysrhythmias. Dysrythmias & Anti-Dysrhythmics. EKG Parameters. Dysrhythmias. Components of an ECG Wave. Dysrhythmias
 Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Final Written Exam ASHI ACLS
 Final Written Exam ASHI ACLS Instructions: Identify the choice that best completes the statement or answers the question. Questions 1 and 2 pertain to the following scenario: A 54-year-old man has experienced
Final Written Exam ASHI ACLS Instructions: Identify the choice that best completes the statement or answers the question. Questions 1 and 2 pertain to the following scenario: A 54-year-old man has experienced
Evaluation and Initial Treatment of Supraventricular Tachycardia
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical practice Evaluation and Initial Treatment of Supraventricular Tachycardia Mark S. Link, M.D. This Journal feature begins with a case vignette
T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical practice Evaluation and Initial Treatment of Supraventricular Tachycardia Mark S. Link, M.D. This Journal feature begins with a case vignette
Antiarrhythmic Drugs 1/31/2018 1
 Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif
 2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
Practical Approach to Arrhythmias
 Outline Practical Approach to Arrhythmias Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Conduction System ECG Acquisition ECG Interpretation Heart rate Rhythm Arrhythmias Tachyarrhythmias Supraventricular
Outline Practical Approach to Arrhythmias Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Conduction System ECG Acquisition ECG Interpretation Heart rate Rhythm Arrhythmias Tachyarrhythmias Supraventricular
WHAT DO YOU SEE WHEN YOU STIMULATE BETA
 CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Mr. Eknath Kole M.S. Pharm (NIPER Mohali)
 M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
HST-151 Clinical Pharmacology in the Operating Room
 Harvard-MIT Division of Health Sciences and Technology HST.151: Principles of Pharmocology Instructors: Dr. Carl Rosow, Dr. David Standaert and Prof. Gary Strichartz 1 HST-151 Clinical Pharmacology in
Harvard-MIT Division of Health Sciences and Technology HST.151: Principles of Pharmocology Instructors: Dr. Carl Rosow, Dr. David Standaert and Prof. Gary Strichartz 1 HST-151 Clinical Pharmacology in
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Course Objectives. Proper Lead Placements. Review the ECG print paper. Review the mechanics of the Myocardium. Review basics of ECG Rhythms
 ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
Hypotension after induction, corrected with 20 mg ephedrine x cc LR EBL 250cc Urine output:
 Terry C. Wicks, CRNA, MHS Catawba Valley Medical Center Hickory, North Carolina 63 y.o., 5 2, 88 kg female for hand assisted laparoscopic tranversecolectomy Co-morbidities include: Hypertension controlled
Terry C. Wicks, CRNA, MHS Catawba Valley Medical Center Hickory, North Carolina 63 y.o., 5 2, 88 kg female for hand assisted laparoscopic tranversecolectomy Co-morbidities include: Hypertension controlled
General anesthetics. Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine
 General anesthetics Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine Rationale General anesthesia is essential to surgical practice, because it renders patients analgesic,
General anesthetics Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine Rationale General anesthesia is essential to surgical practice, because it renders patients analgesic,
TACHYARRHYTHMIAs. Pawel Balsam, MD, PhD
 TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
ARRHYTHMIAS IN THE INTENSIVE CARE UNIT
 ARRHYTHMIAS IN THE INTENSIVE CARE UNIT Nicole Van Israël, DVM, CESOpht, CertSAM, CertVC, DECVIM-CA (Cardiology), MSc, MRCVS European Specialist in Veterinary Cardiology Animal CardioPulmonary Consultancy
ARRHYTHMIAS IN THE INTENSIVE CARE UNIT Nicole Van Israël, DVM, CESOpht, CertSAM, CertVC, DECVIM-CA (Cardiology), MSc, MRCVS European Specialist in Veterinary Cardiology Animal CardioPulmonary Consultancy
Management of ATRIAL FIBRILLATION. in general practice. 22 BPJ Issue 39
 Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Advanced Cardiac Life Support G 2010
 Advanced Cardiac Life Support G 2010 Produced by the Advanced Cardiac Life Support Council of the Irish Heart Foundation March 2012 Introduction: The Arrhythmia and ACLS Councils of the Irish Heart Foundation
Advanced Cardiac Life Support G 2010 Produced by the Advanced Cardiac Life Support Council of the Irish Heart Foundation March 2012 Introduction: The Arrhythmia and ACLS Councils of the Irish Heart Foundation
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Arrhythmic Complications of MI. Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine
 Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
! YOU NEED TO MONITOR QT INTERVALS IN THESE PATIENTS.
 Antiarrhythmic Pharmacopoeia Powerful drugs, split into 4 major classes, according to the predominant receptor they effect. Some fit into several classes at once, like sotolol. Some don t fit at all, owing
Antiarrhythmic Pharmacopoeia Powerful drugs, split into 4 major classes, according to the predominant receptor they effect. Some fit into several classes at once, like sotolol. Some don t fit at all, owing
Step by step approach to EKG rhythm interpretation:
 Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Core Content In Urgent Care Medicine
 Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Antiarrhythmic Drugs Öner Süzer
 Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
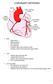 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS)
 Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
EKG Rhythm Interpretation Exam
 as EKG Rhythm Interpretation Exam Name: Date: ID# Unit Assume each strip is a 6 second strip. Passing is 80%. 1. Identify the following rhythm: a. Asystole b. Ventricular fibrillation c. Atrial fibrillation
as EKG Rhythm Interpretation Exam Name: Date: ID# Unit Assume each strip is a 6 second strip. Passing is 80%. 1. Identify the following rhythm: a. Asystole b. Ventricular fibrillation c. Atrial fibrillation
ANESTHESIA EXAM (four week rotation)
 SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University. OBHG Education Subcommittee
 -RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
(living in the fast lane)
 (living in the fast lane) Presented by M.D. Cardiology IT S A group of ECG and Electrophysiological abnormalities in which The atrial impulses are conducted partly or completely, PREMATURELY, to the ventricles
(living in the fast lane) Presented by M.D. Cardiology IT S A group of ECG and Electrophysiological abnormalities in which The atrial impulses are conducted partly or completely, PREMATURELY, to the ventricles
Benztropine and trihexyphenidyl: Centrally acting antimuscarinic agents used for treatment of Parkinson disease & extrapyramidal symptoms.
 Scopolamine: Tertiary amine plant alkaloid. Produces peripheral effects similar to those of atropine. Unlike atropine, scopolamine has greater action on the CNS (observed at therapeutic doses). It has
Scopolamine: Tertiary amine plant alkaloid. Produces peripheral effects similar to those of atropine. Unlike atropine, scopolamine has greater action on the CNS (observed at therapeutic doses). It has
Diploma in Electrocardiography
 The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
Electrocardiography. How to obtain an ECG. The Cardiac Conduction System. The Cardiac Conduction System 10/14/2015
 Electrocardiography Sarah Lehman, VMD Resident in Cardiology, CVCA The Veterinary Forum presented by The LifeCentre October 18, 2015 The Cardiac Conduction System The Cardiac Conduction System How to obtain
Electrocardiography Sarah Lehman, VMD Resident in Cardiology, CVCA The Veterinary Forum presented by The LifeCentre October 18, 2015 The Cardiac Conduction System The Cardiac Conduction System How to obtain
Clinical Problem. Management. Discussion
 Optimum management of atrial fibrillation in the Intensive Care Unit Clinical Problem A 61 year old man, PD, presented to the Intensive Care Unit (ICU) after angiography and intra arterial thrombolysis
Optimum management of atrial fibrillation in the Intensive Care Unit Clinical Problem A 61 year old man, PD, presented to the Intensive Care Unit (ICU) after angiography and intra arterial thrombolysis
ARTICLE. Supraventricular Tachycardia in Infancy. Catherine D. DeAngelis, MD. In most infants, SVT is due to an accessory atrioventricular
 Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
Chapter 03: Sinus Mechanisms Test Bank MULTIPLE CHOICE
 Instant download and all chapters Tesst Bank ECGs Made Easy 5th Edition Barbara J Aehlert https://testbanklab.com/download/tesst-bank-ecgs-made-easy-5th-edition-barbara-jaehlert/ Chapter 03: Sinus Mechanisms
Instant download and all chapters Tesst Bank ECGs Made Easy 5th Edition Barbara J Aehlert https://testbanklab.com/download/tesst-bank-ecgs-made-easy-5th-edition-barbara-jaehlert/ Chapter 03: Sinus Mechanisms
a lecture series by SWESEMJR
 Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
Cardiac Arrhythmias. Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company
 Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
ECG Interpretation Made Easy
 ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
CRITICAL CARE OF THE CARDIAC PATIENT WEBINAR VET 2017
 CRITICAL CARE OF THE CARDIAC PATIENT WEBINAR VET 2017 The Heart The heart is undoubtedly the most important organ in the body. Unfortunately, when it is not functioning properly, it can have dire consequences.
CRITICAL CARE OF THE CARDIAC PATIENT WEBINAR VET 2017 The Heart The heart is undoubtedly the most important organ in the body. Unfortunately, when it is not functioning properly, it can have dire consequences.
CVD: Cardiac Arrhythmias. 1. Final Cardiac Arrhythmias_BMP. 1.1 Cardiovascular Disease. Notes:
 CVD: Cardiac Arrhythmias 1. Final Cardiac Arrhythmias_BMP 1.1 Cardiovascular Disease 1.2 Directions for taking this course 1.3 Content Experts 1.4 Disclosures 1.5 Accreditation Information 1.6 Learning
CVD: Cardiac Arrhythmias 1. Final Cardiac Arrhythmias_BMP 1.1 Cardiovascular Disease 1.2 Directions for taking this course 1.3 Content Experts 1.4 Disclosures 1.5 Accreditation Information 1.6 Learning
Asymptomatic patient with WPW
 Asymptomatic patient with WPW Dimosthenis Avramidis, MD. Arrythmiologist Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital Athens Greece Preexcitation
Asymptomatic patient with WPW Dimosthenis Avramidis, MD. Arrythmiologist Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital Athens Greece Preexcitation
E.C.G. QUIZ. Case History
 Case History E.C.G. QUIZ Pages with reference to book, From 224 To 225 Asadullah Kundi, Azhar Faruqui ( National Institute of Cardio-Vascular Disease, Karachi. ) A 35 Years old female was brought to the
Case History E.C.G. QUIZ Pages with reference to book, From 224 To 225 Asadullah Kundi, Azhar Faruqui ( National Institute of Cardio-Vascular Disease, Karachi. ) A 35 Years old female was brought to the
ACLS. Advanced Cardiac Life Support Practice Test Questions. 1. The following is included in the ACLS Survey?
 1. The following is included in the ACLS Survey? a. Airway, Breathing, Circulation, Differential Diagnosis b. Airway, Breathing, Circulation, Defibrillation c. Assessment, Breathing, Circulation, Defibrillation
1. The following is included in the ACLS Survey? a. Airway, Breathing, Circulation, Differential Diagnosis b. Airway, Breathing, Circulation, Defibrillation c. Assessment, Breathing, Circulation, Defibrillation
Chapter 25. General Anesthetics
 Chapter 25 1. Introduction General anesthetics: 1. Analgesia 2. Amnesia 3. Loss of consciousness 4. Inhibition of sensory and autonomic reflexes 5. Skeletal muscle relaxation An ideal anesthetic: 1. A
Chapter 25 1. Introduction General anesthetics: 1. Analgesia 2. Amnesia 3. Loss of consciousness 4. Inhibition of sensory and autonomic reflexes 5. Skeletal muscle relaxation An ideal anesthetic: 1. A
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification
 Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
Palpitations.
 Palpitations http://www.heartfailurematters.org/en/understandingheartfailure/publishingimages/palpitations_lg.jpg Palpitations are the perception of cardiac activity. They are often described as a fluttering,
Palpitations http://www.heartfailurematters.org/en/understandingheartfailure/publishingimages/palpitations_lg.jpg Palpitations are the perception of cardiac activity. They are often described as a fluttering,
Routine Patient Care Guidelines - Adult
 Routine Patient Care Guidelines - Adult All levels of provider will complete an initial & focused assessment on every patient, and as standing order, use necessary and appropriate skills and procedures
Routine Patient Care Guidelines - Adult All levels of provider will complete an initial & focused assessment on every patient, and as standing order, use necessary and appropriate skills and procedures
CRC 431 ECG Basics. Bill Pruitt, MBA, RRT, CPFT, AE-C
 CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CASE 10. What would the ST segment of this ECG look like? On which leads would you see this ST segment change? What does the T wave represent?
 CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
