Extracorporeal life support (ECLS) supplements the
|
|
|
- Brandon Jenkins
- 6 years ago
- Views:
Transcription
1 CARDIOPULMONARY SUPPORT AND PHYSIOLOGY A PROSPECTIVE COMPARISON OF ATRIO-FEMORAL AND FEMORO-ATRIAL FLOW IN ADULT VENOVENOUS EXTRACORPOREAL LIFE SUPPORT Preston B. Rich, MD Samir S. Awad, MD Stefania Crotti, MD Ronald B. Hirschl, MD, MS Robert H. Bartlett, MD Robert J. Schreiner, MD Introduction: In the United States, venovenous extracorporeal life support has traditionally been performed with atrial drainage and femoral reinfusion (atrio-femoral flow). Although flow reversal (femoro-atrial flow) may alter recirculation and extracorporeal flow, no direct comparison of these 2 modes has been undertaken. Objective: Our goal was to prospectively compare atrio-femoral and femoro-atrial flow in adult venovenous extracorporeal life support for respiratory failure. Methods: A modified bridge enabling conversion between atrio-femoral and femoro-atrial flow was incorporated in the extracorporeal circuit. Bypass was initiated in the direction that provided the highest pulmonary arterial mixed venous oxygen saturation, and the following measurements were taken: (1) maximum extracorporeal flow, (2) highest achievable pulmonary arterial mixed venous oxygen saturation, and (3) flow required to maintain the same pulmonary arterial mixed venous oxygen saturation in both directions. Flow direction was then reversed, and the measurements were repeated. Data were compared with paired t tests and are presented as mean ± standard deviation. Results: Ten patients were studied, and 9 were included in the data analysis. Femoro-atrial bypass provided (1) higher maximal extracorporeal flow (femoro-atrial flow = 55.6 ± 9.8 ml/kg per minute, atrio-femoral flow = 51.1 ± 11.1 ml/kg per minute; P =.04) and (2) higher pulmonary arterial mixed venous oxygen saturation (femoroatrial flow = 89.9% ± 6.6%, atrio-femoral flow = 83.2% ± 4.2%; P =.006); (3) furthermore, it required less flow to maintain an equivalent pulmonary arterial mixed venous oxygen saturation (femoro-atrial flow = 37.0 ± 12.2 ml/kg per minute, atrio-femoral flow = 46.4 ± 8.8 ml/kg per minute; P =.04). Conclusions: During venovenous extracorporeal life support, femoro-atrial bypass provided higher maximal extracorporeal flow, higher pulmonary arterial mixed venous oxygen saturation, and required comparatively less flow to maintain an equivalent mixed venous oxygen saturation than did atrio-femoral bypass. (J Thorac Cardiovasc Surg 1998;116:628-32) From the Department of Surgery, University of Michigan Hospitals, Ann Arbor, Mich. Funded in part by National Institutes of Health RO1 grant HD Presented in part at the Extracorporeal Life Support Organization Annual Meeting, Detroit, Mich, September Received for publication April 6, 1998; revisions requested June 17, 1998; revisions received June 30, 1998; accepted for publication July 1, Address for reprints: Robert J. Schreiner, MD, University of Michigan Medical Center, 1500 E Medical Center Dr, 2920 Taubman Center, Box 0331, Ann Arbor, MI Copyright 1998 by Mosby, Inc /98 $ /1/92801 Extracorporeal life support (ECLS) supplements the failing cardiorespiratory system. 1 In the absence of significant cardiac failure, venovenous bypass has been an effective means of delivering supplemental oxygen to the circulation and has gradually replaced venoarterial support in this setting. 2,3 Because of the high extracorporeal flows frequently required during venovenous ECLS ( ml/kg per minute), currently cannulation of the venous system involves conduits of large caliber. Such adequate sites include the right atrium and the common femoral/common iliac system. These areas can be readily accessed 628
2 The Journal of Thoracic and Volume 116, Number 4 Rich et al 629 Fig 1. The modified ECLS bridge. This bridge was placed in the ECLS circuits of all patients studied. Flow was redirected from AF to FA by changing position of the tubing clamps as indicated. Arrows indicate the path of blood flow with the 2 modes of support. via the right internal jugular and right common femoral veins. Oxygen supplementation during ECLS depends on extracorporeal flow rate and the amount of oxygen available for systemic distribution. In contrast to venoarterial bypass, venovenous ECLS requires both drainage and infusion from prepulmonary capacitance veins. Because of this, a fraction of highly oxygenated ECLS blood is returned to the circuit and is not available for systemic use. Several factors govern extracorporeal flow and recirculation, including cannula position, venous diameter, thoracoabdominal pressure differential, and flow direction. The cumulative effects of these variables may significantly differ when atrial drainage and femoral reinfusion (AF ECLS) is compared with femoral drainage with atrial reinfusion (FA ECLS) and may result in distinctly different levels of support achieved during venovenous ECLS. Despite the routine use of opposite flow directions in the United States 3 and Europe (using FA access and a long atrial reinfusion catheter 4,5 ), no direct comparison between these 2 ECLS modes has been performed. This study was undertaken to prospectively compare the amount of extracorporeal support provided by FA and AF flow during venovenous ECLS using our standard access. Methods Adult patients subjected to venovenous ECLS for the treatment of severe respiratory failure were prospectively studied. In all patients, consent for ECLS and its related procedures was obtained before institution of bypass. A modified bridge was designed that allowed conversion between AF and FA bypass without the need for circuit modifications (Fig 1). With the exception of this bridge, the conduct of ECLS was routine and as previously described. 3 In all patients, access for cannulation was attempted percutaneously, via a modified dilatational Seldinger technique. This was possible in all but 1 patient who required a cervical incision for atrial catheter placement. The right internal jugular vein was instrumented for atrial access and the right common femoral vein for iliac vein inferior vena cava access. When possible, two 25 cm (tip to flare) 23F Bio-Medicus catheters (Medtronic Bio-Medicus, Eden Prairie, Minn) were placed. Tips were positioned in the right atrium and right common iliac vein inferior vena cava confluence. This was confirmed with radiography. After initiation of ECLS, standard pressure controlled rest ventilator settings were instituted. 3 These included pressure-
3 630 Rich et al The Journal of Thoracic and October 1998 Table I. FA and AF comparative data Flow required to Flow required to Maximum flow Maximum flow reach same reach same Maximum (L/min) (ml/kg/min) (L/min) (ml/kg/min) Patient Weight (kg) AF FA AF FA AF FA AF FA AF FA * Average Standard deviation P value Individual patient data comparing atrio-femoral (AF) and femoro-atrial (FA) flow during venovenous ECLS. Each paired set of measurements was obtained within 24 hours of initiating ECLS by changing clamp position on a modified bridge. P values represent FA and AF comparisons between individual patients by paired t tests. *Patient 10 was not included in data analysis because of 2 different cannula sizes. controlled inverse-ratio ventilation at a respiratory rate of 6 breaths/min with peak inspiratory pressures of 30 cm H 2 O at an end-expiratory pressure of 10 cm H 2 O ( P = 20 cm H 2 O). Patients were pharmacologically paralyzed. Fiberoptic pulmonary artery (PA) catheters (Oximetrix, Abbott Critical Care Systems, North Chicago, Ill) were placed in all patients to allow continuous monitoring during the study. An ultrasonic flow probe (Transonic Systems Inc, Ithaca, NY) was placed on the infusion limb of the ECLS circuit to obtain continuous flow measurements. Immediately after cannulation, bypass was conducted in an AF direction. Flow direction was briefly reversed to FA by changing clamp position. Patients were initially maintained on the form of bypass that provided the highest PA saturation during this preliminary comparison. Regardless of initial flow direction, formal measurements were not performed until stable venovenous bypass was attained; this was defined as no change in PA for 15 minutes. The following three measurements were collected on the direction of bypass originally selected. Highest ECLS flow. Extracorporeal flow was gradually advanced by increasing the speed of the roller pump until the compliance chamber on the drainage limb of the circuit intermittently collapsed. Speed was then reduced to allow continuous uninterrupted flow. Flow, measured ultrasonically from the infusion limb of the circuit, was recorded in liters per minute as the maximal flow and corrected for body weight (milliliters per kilogram per minute). Highest PA. ECLS flow was increased until the highest obtainable PA was reached. This point occurred invariably at the maximum ECLS flow. Amount of extracorporeal flow required to maintain equivalent PA saturation. ECLS flow was adjusted to attain a patient-specific PA oxygen saturation (based on the level of PA achieved with initial bypass) obtainable with both modes of bypass. Circuit flow was then reversed by changing clamp position on the modified bridge (Fig 1). After stable bypass was achieved in the opposite direction, a similar set of data was collected. The patient continued to receive the form of bypass that provided the higher PA. This procedure was performed once in each patient, within the first 24 hours of ECLS. Twotailed paired t tests compared data from the 2 bypass directions. Data are expressed as mean ± standard deviation. Results Ten adult patients with severe respiratory failure unresponsive to conventional ventilation were treated with an ECLS circuit containing a modified bridge. Comparative AF and FA data are presented in Table I. Two 23F Bio-Medicus catheters of equal length (25 cm from tip to cannula flare) were inserted in 9 patients. Two cannulas of different calibers were inserted in another patient, and this patient was therefore excluded from the data analysis. Flow was maintained in the FA direction in 9 patients and in the AF direction in 1 patient because of the initial flow comparison. In all patients, the initial comparison based on PA was consistent with subsequent formal measurements. For each set of formal paired measurements, FA bypass provided the same or higher maximal flow (Fig 2). Overall, when corrected for body weight, FA bypass provided significantly higher extracorporeal flow (FA = 55.6 ± 9.8 ml/kg per minute, AF = 51.1 ± 11.1 ml/kg per minute; P =.04).
4 The Journal of Thoracic and Volume 116, Number 4 Rich et al 631 Fig 2. Maximum ECLS flow. When corrected for body weight, FA bypass provided significantly higher extracorporeal flow (FA = 55.6 ± 9.8 ml/kg per minute, AF = 51.1 ± 11.1 ml/kg per minute; P =.04). Fig 3. Maximum. FA ECLS provided statistically higher levels of (FA = 89.9% ± 6.6%, AF = 83.2% ± 4.2%, P =.006). Eight of 9 patients had higher maximal PA oxygen saturations while in the FA mode (Fig 3). Overall, FA ECLS provided statistically higher levels of (FA = 89.9% ± 6.6%, AF = 83.2% ± 4.2%; P =.006). FA bypass provided similar levels of PA at lower ECLS flows in 8 of 9 patients (Fig 4). Overall, significantly less flow (adjusted for patient weight) was required during FA ECLS to achieve comparatively similar levels of (FA = 37.0 ± 12.2 ml/kg per minute, AF = 46.4 ± 8.8 ml/kg per minute; P =.04). Fig 4. Flow required to maintain equivalent. Significantly less flow (adjusted for patient weight) was required during FA ECLS to achieve comparatively similar levels of (FA = 37.0 ± 12.2 ml/kg per minute, AF = 46.4 ± 8.8 ml/kg per minute; P =.04). Discussion This study demonstrated that FA flow during venovenous ECLS is safe and can adequately support gas exchange. When compared directly with atriovenous flow in patients serving as their own controls, higher absolute levels of were achieved, and significantly less flow was required to maintain equivalent levels of extracorporeal support for the group. Contrary to our former belief, FA bypass provided comparably higher maximum flow for the group. Historically, our practice has been to direct ECLS flow in an AF direction, draining deoxygenated blood from the atrium and reinfusing it into the femoral vein. This is predicated on the notion that the large caliber of the atrial chamber may afford greater drainage and therefore translate into higher flows when compared with drainage from the smaller femoral vein. When AF ECLS was initially chosen as the primary direction to conduct flow, ventilator rest settings included low-volume ventilation with pressure limits and short inspiratory times. Current ECLS rest settings routinely use pressurecontrolled inverse-ratio ventilation in an effort to maintain pulmonary recruitment. The increased intrathoracic pressures that accompany this technique may significantly reduce atrial drainage and, by reciprocally shunting blood toward the lower extremities, thereby increase femoral drainage. These pressure relationships may account for our finding FA ECLS to provide significantly higher flows than AF ECLS. We used changes in PA as an approximation of ECLS support. PA reflects the mixing of oxygen saturations that occurs from returning systemic blood combining with that of the ECLS circuit. Additionally, PA is not directly affected by contributions from the native lungs, as is arterial saturation. Although this value does not represent true native because of extracorporeal augmentation, we believe it does accu-
5 632 Rich et al The Journal of Thoracic and October 1998 rately reflect relative changes in ECLS support. PA is routinely relied on at our institution to assess adequacy of support during venovenous ECLS. During venovenous ECLS, both drainage and infusion occur via the same prepulmonary vasculature, and therefore a certain fraction of ECLS affluent unavoidably consists of recently delivered extracorporeally oxygenated blood. The magnitude of this recirculation directly affects peripheral oxygen delivery. During traditional AF ECLS, flow is directed from the infusion cannula directly toward the drainage cannula, and the systemic distribution of ECLS effluent necessitates passage of oxygenated blood past the orifice of the drainage cannula. Femoral drainage with atrial infusion (FA bypass) may reduce recirculation by directing oxygenated blood through the tricuspid valve for subsequent systemic distribution. Although not directly measured, reduced recirculation likely accounted for the significantly higher PA observed with FA bypass, as well as the provision of similar levels of support at lower circuit flow rates. Although for a given paired comparison FA bypass usually provided higher PA, higher maximal flow, and required less flow to maintain similar support, this was not universal. As governed by Poiseuille s law, flow is greatly influenced by cannula diameter and length. All patients with equivalent cannulas in both access sites demonstrated higher flows in the FA direction. The 1 patient dropped from analysis because of cannula size discrepancy (atrial 23F, femoral 21F) had predictably higher flows with AF bypass. However, even with lower flows, PA s in this patient were significantly higher in the FA direction. Another patient (included in data analysis) demonstrated higher PA and required less flow to maintain with AF bypass, while having lower maximal flow in this direction. Radiography revealed appropriate cannula placement in this patient. Despite this isolated exception, FA bypass provided significantly higher, higher flow, and required less flow to maintain an equivalent in the group as a whole. Although ECLS may be required for weeks in patients with respiratory failure, we compared differences in flow direction only on the first day of bypass. It is unclear how flow and recirculation relationships will change over time. Although not tested in this study, it is possible that FA flow may be compromised to a greater degree than AF flow by intravascular volume depletion, thereby limiting the application of the current findings. To our knowledge, no complication resulted from the conduct of FA bypass. Routine circuit examinations did reveal a higher incidence of thrombus formation adjacent to Y connectors. Inasmuch as the modified bridge contains 2 more of these connectors than the standard bridge, it may increase the potential for embolic events. In routine ECLS any clot that dislodged during stable flow in either direction would be directed at the oxygenators. However, flow reversal under these circumstances could have resulted in free intravascular clot being directed toward the native pulmonary circulation. It is for this reason that flow reversals were not routinely performed after the first day of bypass. The modified bridge is more complex than the standard one and requires the manipulation of 2 tubing clamps rather than 1. Because of the added tubing, the bridge is larger and can be more difficult to transport without kinking. Regardless, after adequate staff training we found the device to be manageable and to require little additional care. In summary, FA support during adult venovenous ECLS provided higher maximum flow, higher PA, and required less flow to maintain a given than did traditional AF bypass. Although we no longer routinely use the modified bridge, it permitted safe conversion between the 2 modes of support and allowed for direct comparisons within individual patients. On the basis of this study, it has become our practice to initiate flow in the FA direction in adult venovenous ECLS. REFERENCES 1. Anderson HL, Delius RE, Sinard JM, McCurry KR, Shanley CJ, Chapman RA, et al. Early experience with adult ECMO in the modern era. Ann Thorac Surg 1992;53: Anderson H, Steimle C, Shapiro M, Delius R, Chapman R, Hirschl R, et al. Extracorporeal life support for adult cardiorespiratory failure. Surgery 1993;114: Kolla S, Awad SS, Rich PB, Schreiner RJ, Hirschl RB, Bartlett RH. Extracorporeal life support for 100 patients with severe respiratory failure. Ann Surg 1997;226: Brunet F, Belghith M, Mira J, Lanore JJ, Vaxelaire JF, Santucci JD, et al. Extracorporeal carbon dioxide removal and low-frequency positive-pressure ventilation: improvement in arterial oxygenation with reduction of risk of pulmonary barotrauma in patients with adult respiratory distress syndrome. Chest 1993; 104: Gattinoni L, Pesenti A, Mascheroni D, Marcolin R, Fumagalli R, Rossi F, et al. Low frequency positive pressure ventilation with extracorporeal CO 2 removal in severe acute respiratory failure. JAMA 1986;256:881-6.
Extracorporeal Membrane Oxygenation (ECMO)
 Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/01/2014 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/01/2014 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO)
 Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2017 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2017 Section: Other/Miscellaneous
Initial Experience With Single Cannulation for Venovenous Extracorporeal Oxygenation in Adults
 Initial Experience With Single Cannulation for Venovenous Extracorporeal Oxygenation in Adults Christian A. Bermudez, MD, Rodolfo V. Rocha, MD, Penny L. Sappington, MD, Yoshiya Toyoda, MD, PhD, Holt N.
Initial Experience With Single Cannulation for Venovenous Extracorporeal Oxygenation in Adults Christian A. Bermudez, MD, Rodolfo V. Rocha, MD, Penny L. Sappington, MD, Yoshiya Toyoda, MD, PhD, Holt N.
Position of draining venous cannula in extracorporeal membrane oxygenation for respiratory and respiratory/circulatory support in adult patients
 Frenckner et al. Critical Care (2018) 22:163 https://doi.org/10.1186/s13054-018-2083-0 VIEWPOINT Position of draining venous cannula in extracorporeal membrane oxygenation for respiratory and respiratory/circulatory
Frenckner et al. Critical Care (2018) 22:163 https://doi.org/10.1186/s13054-018-2083-0 VIEWPOINT Position of draining venous cannula in extracorporeal membrane oxygenation for respiratory and respiratory/circulatory
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Cite this article as:
 doi: 10.21037/acs.2018.08.06 Cite this article as: Loforte A, Baiocchi M, Gliozzi G, Coppola G, Di Bartolomeo R, Lorusso R. Percutaneous pulmonary artery venting via jugular vein while on peripheral extracorporeal
doi: 10.21037/acs.2018.08.06 Cite this article as: Loforte A, Baiocchi M, Gliozzi G, Coppola G, Di Bartolomeo R, Lorusso R. Percutaneous pulmonary artery venting via jugular vein while on peripheral extracorporeal
Artificial Lung: A New Inspiration
 Artificial Lung: A New Inspiration Joseph B. Zwischenberger MD Johnston-Wright Professor and Chairman: Department of Surgery j.zwische@uky.edu The University of Kentucky Lexington, Kentucky Presenter Disclosure
Artificial Lung: A New Inspiration Joseph B. Zwischenberger MD Johnston-Wright Professor and Chairman: Department of Surgery j.zwische@uky.edu The University of Kentucky Lexington, Kentucky Presenter Disclosure
Troubleshooting Adult ECMO
 The Journal of ExtraCorporeal Technology Troubleshooting Adult ECMO David Sidebotham, FANZCA Departments of Anaesthesia and Intensive Care, Auckland City Hospital, Auckland, New Zealand Presented at Perfusion
The Journal of ExtraCorporeal Technology Troubleshooting Adult ECMO David Sidebotham, FANZCA Departments of Anaesthesia and Intensive Care, Auckland City Hospital, Auckland, New Zealand Presented at Perfusion
Comparison of Flow Differences amoiig Venous Cannulas
 Comparison of Flow Differences amoiig Venous Cannulas Edward V. Bennett, Jr., MD., John G. Fewel, M.S., Jose Ybarra, B.S., Frederick L. Grover, M.D., and J. Kent Trinkle, M.D. ABSTRACT The efficiency of
Comparison of Flow Differences amoiig Venous Cannulas Edward V. Bennett, Jr., MD., John G. Fewel, M.S., Jose Ybarra, B.S., Frederick L. Grover, M.D., and J. Kent Trinkle, M.D. ABSTRACT The efficiency of
Innovative ECMO Configurations in Adults
 Innovative ECMO Configurations in Adults Practice at a Single Center with Platinum Level ELSO Award for Excellence in Life Support Monika Tukacs, BSN, RN, CCRN Columbia University Irving Medical Center,
Innovative ECMO Configurations in Adults Practice at a Single Center with Platinum Level ELSO Award for Excellence in Life Support Monika Tukacs, BSN, RN, CCRN Columbia University Irving Medical Center,
ECLS as Bridge to Transplant
 ECLS as Bridge to Transplant Marcelo Cypel MD, MSc Assistant Professor of Surgery Division of Thoracic Surgery Toronto General Hospital University of Toronto Application of ECLS Bridge to lung recovery
ECLS as Bridge to Transplant Marcelo Cypel MD, MSc Assistant Professor of Surgery Division of Thoracic Surgery Toronto General Hospital University of Toronto Application of ECLS Bridge to lung recovery
A. Incorrect! The left ventricle receives oxygenated blood from the lungs via the left atrium.
 DAT Biology - Problem Drill 10: The Circulatory System Question No. 1 of 10 1. What is the flow of deoxygenated blood through the heart as it returns from the body? Question #01 (A) Vena cava; right ventricle;
DAT Biology - Problem Drill 10: The Circulatory System Question No. 1 of 10 1. What is the flow of deoxygenated blood through the heart as it returns from the body? Question #01 (A) Vena cava; right ventricle;
Indications. The AngioVac cannula is intended for use as a venous drainage cannula and for the removal of fresh, soft thrombi or emboli
 Indications Straight Cannula or Cannula with 20 O Angle 17F Working Channel The AngioVac cannula is intended for use as a venous drainage cannula and for the removal of fresh, soft thrombi or emboli Radiopaque
Indications Straight Cannula or Cannula with 20 O Angle 17F Working Channel The AngioVac cannula is intended for use as a venous drainage cannula and for the removal of fresh, soft thrombi or emboli Radiopaque
THE HEART. Unit 3: Transportation and Respiration
 THE HEART Unit 3: Transportation and Respiration The Circulatory System Also called the Cardiovascular System Circulates blood in the body Transports nutrients, oxygen, carbon dioxide, hormones, and blood
THE HEART Unit 3: Transportation and Respiration The Circulatory System Also called the Cardiovascular System Circulates blood in the body Transports nutrients, oxygen, carbon dioxide, hormones, and blood
2018 CANNULAE CATALOGUE
 CANNULAE CATALOGUE 2018 Process The RHEOPAX synthetic albumin coating is a surface refinement which is carried out as a final manufacturing step before the sterilization and can not only improve the surface
CANNULAE CATALOGUE 2018 Process The RHEOPAX synthetic albumin coating is a surface refinement which is carried out as a final manufacturing step before the sterilization and can not only improve the surface
FOCUS CONFERENCE 2018
 FOCUS CONFERENCE 2018 Current Practice in Pediatric and Neonatal Extracorporeal Life Support Daniel W. Chipman, RRT Assistant Director of Respiratory Care Massachusetts General Hospital Boston, Massachusetts
FOCUS CONFERENCE 2018 Current Practice in Pediatric and Neonatal Extracorporeal Life Support Daniel W. Chipman, RRT Assistant Director of Respiratory Care Massachusetts General Hospital Boston, Massachusetts
Multislice CT Scans in Patients on Extracorporeal Membrane Oxygenation: Emphasis on Hemodynamic Changes and Imaging Pitfalls
 Pictorial Essay Cardiovascular Imaging http://dx.doi.org/10.3348/kjr.2014.15.3.322 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(3):322-329 Multislice CT Scans in Patients on Extracorporeal Membrane
Pictorial Essay Cardiovascular Imaging http://dx.doi.org/10.3348/kjr.2014.15.3.322 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(3):322-329 Multislice CT Scans in Patients on Extracorporeal Membrane
Migrated Avalon Veno-Venous Extracorporeal Membrane Oxygenation Cannula: How to Adjust Without Interruption of Flow.
 Thomas Jefferson University Jefferson Digital Commons Department of Surgery Faculty Papers Department of Surgery 11-1-2015 Migrated Avalon Veno-Venous Extracorporeal Membrane Oxygenation Cannula: How to
Thomas Jefferson University Jefferson Digital Commons Department of Surgery Faculty Papers Department of Surgery 11-1-2015 Migrated Avalon Veno-Venous Extracorporeal Membrane Oxygenation Cannula: How to
Case scenario V AV ECMO. Dr Pranay Oza
 Case scenario V AV ECMO Dr Pranay Oza Case Summary 53 y/m, k/c/o MVP with myxomatous mitral valve with severe Mitral regurgitation underwent Mitral valve replacement with mini thoracotomy Pump time nearly
Case scenario V AV ECMO Dr Pranay Oza Case Summary 53 y/m, k/c/o MVP with myxomatous mitral valve with severe Mitral regurgitation underwent Mitral valve replacement with mini thoracotomy Pump time nearly
ISPUB.COM. Concepts Of Neonatal ECMO. D Thakar, A Sinha, O Wenker HISTORY PATIENT SELECTION AND ECMO CRITERIA
 ISPUB.COM The Internet Journal of Emergency and Intensive Care Medicine Volume 5 Number 2 D Thakar, A Sinha, O Wenker Citation D Thakar, A Sinha, O Wenker.. The Internet Journal of Emergency and Intensive
ISPUB.COM The Internet Journal of Emergency and Intensive Care Medicine Volume 5 Number 2 D Thakar, A Sinha, O Wenker Citation D Thakar, A Sinha, O Wenker.. The Internet Journal of Emergency and Intensive
The Role of ECMO in Thoracic Surgery. Matthew Hartwig, MD
 The Role of ECMO in Thoracic Surgery Matthew Hartwig, MD Disclosure Slide Consultant for Mallincrodkt and Quark Pharmaceuticals Case #1 28 y.o. female with tracheal mass No previous medical or surgical
The Role of ECMO in Thoracic Surgery Matthew Hartwig, MD Disclosure Slide Consultant for Mallincrodkt and Quark Pharmaceuticals Case #1 28 y.o. female with tracheal mass No previous medical or surgical
ECLS. The Basics. Jeannine Hermens Intensive Care Center UMC Utrecht
 ECLS The Basics Jeannine Hermens Intensive Care Center UMC Utrecht Conflict of interest None Terminology ECMO - ExtraCorporeal Membrane Oxygenation ECLS - ExtraCorporeal Life Support PLS - Veno-venous
ECLS The Basics Jeannine Hermens Intensive Care Center UMC Utrecht Conflict of interest None Terminology ECMO - ExtraCorporeal Membrane Oxygenation ECLS - ExtraCorporeal Life Support PLS - Veno-venous
Cardiovascular Physiology
 Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
Cardiovascular Institute
 Allegheny Health Network Cardiovascular Institute Extracorporeal Membrane Oxygenation (ECMO) Program Our patient survival rate is higher than the national average. ECMO experts. Multidisciplinary team.
Allegheny Health Network Cardiovascular Institute Extracorporeal Membrane Oxygenation (ECMO) Program Our patient survival rate is higher than the national average. ECMO experts. Multidisciplinary team.
Amphotericin B Pharmacokinetics During Extracorporea/ Membrane Oxygenation: A Case Report
 Case Report Amphotericin B Pharmacokinetics During Extracorporea/ Membrane Oxygenation: A Case Report James H. Hertzog, MD; Ellen Brackett, MD; Mark Sale, MD; Gabriel J. Hauser, MD; Heidi J. Dalton, MD
Case Report Amphotericin B Pharmacokinetics During Extracorporea/ Membrane Oxygenation: A Case Report James H. Hertzog, MD; Ellen Brackett, MD; Mark Sale, MD; Gabriel J. Hauser, MD; Heidi J. Dalton, MD
Extra Corporeal Life Support for Acute Heart failure
 Extra Corporeal Life Support for Acute Heart failure Benjamin Medalion, MD Director Heart and Lung Transplantation Department of Cardiothoracic Surgery Rabin Medical Center, Beilinson Campus, Israel Mechanical
Extra Corporeal Life Support for Acute Heart failure Benjamin Medalion, MD Director Heart and Lung Transplantation Department of Cardiothoracic Surgery Rabin Medical Center, Beilinson Campus, Israel Mechanical
Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart. O Wenker, L Chaloupka, R Joswiak, D Thakar, C Wood, G Walsh
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
9/17/2014. Good Morning! 14th Annual Western Kansas Respiratory Care Seminar. 14th Annual Western Kansas Respiratory Care Seminar 28th
 Good Morning! 14th Annual Western Kansas Respiratory Care Seminar Current Status of Extracorporeal Membrane Oxygenation (ECMO) in Infants and Adults Kelly D. Hedlund, MS, CCP Chief Perfusionist Michael
Good Morning! 14th Annual Western Kansas Respiratory Care Seminar Current Status of Extracorporeal Membrane Oxygenation (ECMO) in Infants and Adults Kelly D. Hedlund, MS, CCP Chief Perfusionist Michael
Prolonged Extracorporeal Membrane Oxygenation Support for Acute Respiratory Distress Syndrome
 CASE REPORT Prolonged Extracorporeal Membrane Oxygenation Support for Acute Respiratory Distress Syndrome Wen-Je Ko,* Hsao-Hsun Hsu, Pi-Ru Tsai When all conventional treatments for respiratory failure
CASE REPORT Prolonged Extracorporeal Membrane Oxygenation Support for Acute Respiratory Distress Syndrome Wen-Je Ko,* Hsao-Hsun Hsu, Pi-Ru Tsai When all conventional treatments for respiratory failure
Long Term Support for Respiratory Failure: VV ECMO or Oxygenated RVAD?
 Long Term Support for Respiratory Failure: VV ECMO or Oxygenated RVAD? Mechanical Circulatory Support Symposium 2018 (Houston, TX) Charles Hoopes, MD Professor of Surgery University of Alabama (Birmingham)
Long Term Support for Respiratory Failure: VV ECMO or Oxygenated RVAD? Mechanical Circulatory Support Symposium 2018 (Houston, TX) Charles Hoopes, MD Professor of Surgery University of Alabama (Birmingham)
Clinical Applications of Femoral Vein-to-Artery Cannulation for Mechanical Cardiopulmonary Support and Bypass
 Clinical Applications of Femoral Vein-to-Artery Cannulation for Mechanical Cardiopulmonary Support and Bypass Robert L. Berger, M.D., Virender K. Saini, M.D., and Everett L. Dargan, M.D. ABSTRACT Femoral
Clinical Applications of Femoral Vein-to-Artery Cannulation for Mechanical Cardiopulmonary Support and Bypass Robert L. Berger, M.D., Virender K. Saini, M.D., and Everett L. Dargan, M.D. ABSTRACT Femoral
Recirculation during veno-venous extra-corporeal membrane oxygenation a simulation study
 IJAO ISSN 0391-3988 Int J Artif Organs 2015; 38 (1): 23-30 DOI: 10.5301/ijao.5000373 ORIGINAL ARTICLE Recirculation during veno-venous extra-corporeal membrane oxygenation a simulation study Mikael Broman
IJAO ISSN 0391-3988 Int J Artif Organs 2015; 38 (1): 23-30 DOI: 10.5301/ijao.5000373 ORIGINAL ARTICLE Recirculation during veno-venous extra-corporeal membrane oxygenation a simulation study Mikael Broman
i INTERACTIVE CATALOG FIND YOUR IDEAL CANNULAE
 i INTERACTIVE CATALOG FIND YOUR IDEAL CANNULAE Catalog 2017 i USER TIPS Easily navigate through the pages in our 2017 Cannula Catalog by using the mini-menu shown on upper right of each page. Navigate
i INTERACTIVE CATALOG FIND YOUR IDEAL CANNULAE Catalog 2017 i USER TIPS Easily navigate through the pages in our 2017 Cannula Catalog by using the mini-menu shown on upper right of each page. Navigate
CIE Biology GCSE. 9: Transport in animals. Notes.
 CIE Biology GCSE 9: Transport in animals Notes The circulatory system acts as the main transport system in animals. It is made up of blood vessels such as arteries, veins and capillaries, in which blood
CIE Biology GCSE 9: Transport in animals Notes The circulatory system acts as the main transport system in animals. It is made up of blood vessels such as arteries, veins and capillaries, in which blood
Adult Extracorporeal Life Support (ECLS)
 Adult Extracorporeal Life Support (ECLS) Steven Scott, M.D., F.A.C.S. Piedmont Heart Institute Cardiothoracic Surgery Disclosures None ECMO = ECLS A technique of life support that involves a continuous
Adult Extracorporeal Life Support (ECLS) Steven Scott, M.D., F.A.C.S. Piedmont Heart Institute Cardiothoracic Surgery Disclosures None ECMO = ECLS A technique of life support that involves a continuous
Artificial Lungs: A New Inspiration
 Artificial Lungs: A New Inspiration Joseph B. Zwischenberger MD Johnston-Wright Professor and Chairman: Department of Surgery j.zwische@uky.edu The University of Kentucky Lexington, Kentucky Presenter
Artificial Lungs: A New Inspiration Joseph B. Zwischenberger MD Johnston-Wright Professor and Chairman: Department of Surgery j.zwische@uky.edu The University of Kentucky Lexington, Kentucky Presenter
ECMO Experience from ECMO-ICU, Karolinska
 ECMO Experience from ECMO-ICU, Karolinska X Curso de Ventilacion Mecanica en Anestesia, Cuidados Criticos y Transplantes Madrid 2012 International numbers Totally since 1989; 46500 patients as of July
ECMO Experience from ECMO-ICU, Karolinska X Curso de Ventilacion Mecanica en Anestesia, Cuidados Criticos y Transplantes Madrid 2012 International numbers Totally since 1989; 46500 patients as of July
Extracorporeal support in acute respiratory failure. Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London
 Extracorporeal support in acute respiratory failure Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London Objectives By the end of this session, you will be able to: Describe different
Extracorporeal support in acute respiratory failure Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London Objectives By the end of this session, you will be able to: Describe different
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Hemodynamic Monitoring and Circulatory Assist Devices
 Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation.
 Chapter 1: Principles of Mechanical Ventilation TRUE/FALSE 1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation. F
Chapter 1: Principles of Mechanical Ventilation TRUE/FALSE 1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation. F
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
Management of refractory ARDS. Saurabh maji
 Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator
 Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
ACTIVITY: The Heart Cycle
 ACTIVITY: The Heart Cycle In this activity, you will follow the flow of blood through the heart. Your heart has two jobs to do, and its two sides have separate responsibilities: The left side pumps oxygen-enriched
ACTIVITY: The Heart Cycle In this activity, you will follow the flow of blood through the heart. Your heart has two jobs to do, and its two sides have separate responsibilities: The left side pumps oxygen-enriched
Percutaneously Inserted AngioVac Suction Thrombectomy for the Treatment of Filter-Related. Iliocaval Thrombosis
 Percutaneously Inserted AngioVac Suction Thrombectomy for the Treatment of Filter-Related Iliocaval Thrombosis Faiz D. Francis, DO; Gianvito Salerno, MD; Sabbah D. Butty, MD Abstract In the setting of
Percutaneously Inserted AngioVac Suction Thrombectomy for the Treatment of Filter-Related Iliocaval Thrombosis Faiz D. Francis, DO; Gianvito Salerno, MD; Sabbah D. Butty, MD Abstract In the setting of
NUTRITION SUPPORT DURING EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) IN CRITICALLY ILL ADULT PATIENTS. Haley Murrell, March 19, 2015
 NUTRITION SUPPORT DURING EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) IN CRITICALLY ILL ADULT PATIENTS Haley Murrell, March 19, 2015 Objectives Provide an overview of Extracorporeal Membrane Oxygenation
NUTRITION SUPPORT DURING EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) IN CRITICALLY ILL ADULT PATIENTS Haley Murrell, March 19, 2015 Objectives Provide an overview of Extracorporeal Membrane Oxygenation
Partial anomalous pulmonary venous connection to superior
 Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
HLS CANNULAE SOLUTIONS FROM TIP TO TIP
 HLS CANNULAE SOLUTIONS FROM TIP TO TIP HLS CANNULAE SETS VESSEL ACCESS BECOMES EASIER MAQUET THE GOLD STANDARD MAQUET is an international synonym for innovative and technological advances in operating
HLS CANNULAE SOLUTIONS FROM TIP TO TIP HLS CANNULAE SETS VESSEL ACCESS BECOMES EASIER MAQUET THE GOLD STANDARD MAQUET is an international synonym for innovative and technological advances in operating
LV Distension and ECLS Lungs
 LV Distension and ECLS Lungs Kevin W. Hatton, MD, FCCM Interim Vice-Chair for Anesthesiology Research Division Chief, Anesthesiology Critical Care Medicine Program Director, Anesthesiology Critical Care
LV Distension and ECLS Lungs Kevin W. Hatton, MD, FCCM Interim Vice-Chair for Anesthesiology Research Division Chief, Anesthesiology Critical Care Medicine Program Director, Anesthesiology Critical Care
An emerging problem: Vascular access for ECMO
 An emerging problem: Vascular access for ECMO Dott.ssa Maria Grazia Calabrò U.O. Anestesia e Terapia Intensiva Cardio-Toraco-Vascolare Ospedale San Raffaele, Milano Impossibile visualizzare l'immagine.
An emerging problem: Vascular access for ECMO Dott.ssa Maria Grazia Calabrò U.O. Anestesia e Terapia Intensiva Cardio-Toraco-Vascolare Ospedale San Raffaele, Milano Impossibile visualizzare l'immagine.
ECLS Registry Form Extracorporeal Life Support Organization (ELSO)
 ECLS Registry Form Extracorporeal Life Support Organization (ELSO) Center ID: Center name: Run No (for this patient) Unique ID: Birth Date/Time Sex: (M, F) Race: (Asian, Black, Hispanic, White, Other)
ECLS Registry Form Extracorporeal Life Support Organization (ELSO) Center ID: Center name: Run No (for this patient) Unique ID: Birth Date/Time Sex: (M, F) Race: (Asian, Black, Hispanic, White, Other)
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of extracorporeal membrane carbon dioxide removal Using a blood-filtering machine
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of extracorporeal membrane carbon dioxide removal Using a blood-filtering machine
CVS Hemodynamics. Faisal I. Mohammed, MD,PhD.
 CVS Hemodynamics Faisal I. Mohammed, MD,PhD. Objectives point out the physical characteristics of the circulation: distribution of blood volume total cross sectional area velocity blood pressure List the
CVS Hemodynamics Faisal I. Mohammed, MD,PhD. Objectives point out the physical characteristics of the circulation: distribution of blood volume total cross sectional area velocity blood pressure List the
Despite recent advances in critical care, the overall
 ORIGINAL ARTICLES: GENERAL THORACIC Percutaneous Extracorporeal Arteriovenous CO 2 Removal for Severe Respiratory Failure Joseph B. Zwischenberger, MD, Steven A. Conrad, MD, PhD, Scott K. Alpard, MD, Laurie
ORIGINAL ARTICLES: GENERAL THORACIC Percutaneous Extracorporeal Arteriovenous CO 2 Removal for Severe Respiratory Failure Joseph B. Zwischenberger, MD, Steven A. Conrad, MD, PhD, Scott K. Alpard, MD, Laurie
Heart transplantation is the gold standard treatment for
 Organ Care System for Heart Procurement and Strategies to Reduce Primary Graft Failure After Heart Transplant Masaki Tsukashita, MD, PhD, and Yoshifumi Naka, MD, PhD Primary graft failure is a rare, but
Organ Care System for Heart Procurement and Strategies to Reduce Primary Graft Failure After Heart Transplant Masaki Tsukashita, MD, PhD, and Yoshifumi Naka, MD, PhD Primary graft failure is a rare, but
1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary.
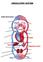 CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
How to face the challenge: contrast enhanced computed tomography scanning of patients under ExtraCorporeal Membrane Oxygenation - ECMO.
 How to face the challenge: contrast enhanced computed tomography scanning of patients under ExtraCorporeal Membrane Oxygenation - ECMO. Poster No.: C-2416 Congress: ECR 2017 Type: Educational Exhibit Authors:
How to face the challenge: contrast enhanced computed tomography scanning of patients under ExtraCorporeal Membrane Oxygenation - ECMO. Poster No.: C-2416 Congress: ECR 2017 Type: Educational Exhibit Authors:
Extracorporeal Life Support Organization (ELSO) General Guidelines for all ECLS Cases August, 2017
 Extracorporeal Life Support Organization (ELSO) Introduction General Guidelines for all ECLS Cases August, 2017 This guideline describes prolonged extracorporeal life support (ECLS, ECMO), applicable to
Extracorporeal Life Support Organization (ELSO) Introduction General Guidelines for all ECLS Cases August, 2017 This guideline describes prolonged extracorporeal life support (ECLS, ECMO), applicable to
Ch.15 Cardiovascular System Pgs {15-12} {15-13}
 Ch.15 Cardiovascular System Pgs {15-12} {15-13} E. Skeleton of the Heart 1. The skeleton of the heart is composed of rings of dense connective tissue and other masses of connective tissue in the interventricular
Ch.15 Cardiovascular System Pgs {15-12} {15-13} E. Skeleton of the Heart 1. The skeleton of the heart is composed of rings of dense connective tissue and other masses of connective tissue in the interventricular
Level 2 Anatomy and Physiology Bite size revision. Respiratory System. The order of the passage of oxygen into the body (inhalation/inspiration) is: -
 Respiratory System Function of the respiratory system The lungs are located in the chest cavity and their function is to intake oxygen and remove carbon dioxide from the body. Structure of the respiratory
Respiratory System Function of the respiratory system The lungs are located in the chest cavity and their function is to intake oxygen and remove carbon dioxide from the body. Structure of the respiratory
ECMO BASICS CHLOE STEINSHOUER, MD PULMONARY AND SLEEP CONSULTANTS OF KANSAS
 ECMO BASICS CHLOE STEINSHOUER, MD PULMONARY AND SLEEP CONSULTANTS OF KANSAS DISCLOSURES No financial disclosures or conflicts of interest OBJECTIVES Define ECMO/ECLS and be able to identify the main types
ECMO BASICS CHLOE STEINSHOUER, MD PULMONARY AND SLEEP CONSULTANTS OF KANSAS DISCLOSURES No financial disclosures or conflicts of interest OBJECTIVES Define ECMO/ECLS and be able to identify the main types
ECMO as a bridge to durable LVAD therapy. Jonathan Haft, MD Department of Cardiac Surgery University of Michigan
 ECMO as a bridge to durable LVAD therapy Jonathan Haft, MD Department of Cardiac Surgery University of Michigan Systolic Heart Failure Prevalence 4.8 million U.S. 287,000 deaths per year $39 billion spent
ECMO as a bridge to durable LVAD therapy Jonathan Haft, MD Department of Cardiac Surgery University of Michigan Systolic Heart Failure Prevalence 4.8 million U.S. 287,000 deaths per year $39 billion spent
CIRCULATION & GAS EXCHANGE
 AP BIOLOGY ACTIVITY2.13 Text:Campbell,v.8,chapter42 NAME DATE HOUR CIRCULATION & GAS EXCHANGE 1. In general, what is the function of transport systems? 2. What method/structure do most invertebrates use
AP BIOLOGY ACTIVITY2.13 Text:Campbell,v.8,chapter42 NAME DATE HOUR CIRCULATION & GAS EXCHANGE 1. In general, what is the function of transport systems? 2. What method/structure do most invertebrates use
The Journal of Thoracic and Cardiovascular Surgery
 Accepted Manuscript Commentary: NO FLOW? QUICK, RE-SEW Ross M. Bremner, MD, PhD PII: S0022-5223(19)30560-4 DOI: https://doi.org/10.1016/j.jtcvs.2019.02.092 Reference: YMTC 14240 To appear in: The Journal
Accepted Manuscript Commentary: NO FLOW? QUICK, RE-SEW Ross M. Bremner, MD, PhD PII: S0022-5223(19)30560-4 DOI: https://doi.org/10.1016/j.jtcvs.2019.02.092 Reference: YMTC 14240 To appear in: The Journal
Hydrodynamic Evaluations of Four Mock Femoral Venous Cannulas
 ORIGINAL ARTICLE Hydrodynamic Evaluations of Four Mock Femoral Venous Türker Şahin 1, MD; Murat Tezer 2, MD; Levent Cerit 3, MD DOI: 10.21470/1678-9741-2018-0036 Abstract Objective: To report the results
ORIGINAL ARTICLE Hydrodynamic Evaluations of Four Mock Femoral Venous Türker Şahin 1, MD; Murat Tezer 2, MD; Levent Cerit 3, MD DOI: 10.21470/1678-9741-2018-0036 Abstract Objective: To report the results
Non-surgical extraction of right atrial mass by AngioVac aspiration device under fluoroscopic and transesophageal echocardiographic guidance
 Case Report Non-surgical extraction of right atrial mass by ngiovac aspiration device under fluoroscopic and transesophageal echocardiographic guidance Tariq H. Enezate, run Kumar, Kul ggarwal, Sudarshan
Case Report Non-surgical extraction of right atrial mass by ngiovac aspiration device under fluoroscopic and transesophageal echocardiographic guidance Tariq H. Enezate, run Kumar, Kul ggarwal, Sudarshan
Extracorporeal Life Support Organization (ELSO) General Guidelines for all ECLS Cases
 Extracorporeal Life Support Organization (ELSO) General Guidelines for all ECLS Cases Introduction This guideline describes prolonged extracorporeal life support (ECLS, ECMO). Related guidelines with more
Extracorporeal Life Support Organization (ELSO) General Guidelines for all ECLS Cases Introduction This guideline describes prolonged extracorporeal life support (ECLS, ECMO). Related guidelines with more
ELSA Extracorporeal Life Support Assurance
 ELSA Extracorporeal Life Support Assurance Optimize ECMO Therapy Detect Oxygenator Clotting Verify Delivered Blood Flow Optimize ECMO Therapy With Recirculation Percentage, Oxygenator Clot Detection, and
ELSA Extracorporeal Life Support Assurance Optimize ECMO Therapy Detect Oxygenator Clotting Verify Delivered Blood Flow Optimize ECMO Therapy With Recirculation Percentage, Oxygenator Clot Detection, and
CARDIORESPIRATORY DEVELOPMENT
 CARDIORESPIRATORY DEVELOPMENT Fahey/Insel/Roth, Fit & Well: Core Concepts and Labs in Physical Fitness and Wellness, Chapter 3 ANATOMY OF THE HEART O The heart is divided into right and left hand side
CARDIORESPIRATORY DEVELOPMENT Fahey/Insel/Roth, Fit & Well: Core Concepts and Labs in Physical Fitness and Wellness, Chapter 3 ANATOMY OF THE HEART O The heart is divided into right and left hand side
ELSA Extracorporeal Life Support Assurance
 ELSA Extracorporeal Life Support Assurance Optimize ECMO Therapy Detect Oxygenator Clotting Verify Delivered Blood Flow Optimize ECMO Therapy With Recirculation Percentage, Oxygenator Clot Detection, and
ELSA Extracorporeal Life Support Assurance Optimize ECMO Therapy Detect Oxygenator Clotting Verify Delivered Blood Flow Optimize ECMO Therapy With Recirculation Percentage, Oxygenator Clot Detection, and
Mechanical Bleeding Complications During Heart Surgery
 Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
Extracorporeal Life Support Organization (ELSO) Guidelines for Adult Respiratory Failure August, 2017
 Introduction Extracorporeal Life Support Organization (ELSO) Guidelines for Adult Respiratory Failure August, 2017 This guideline describes prolonged extracorporeal life support (ECLS, ECMO), applicable
Introduction Extracorporeal Life Support Organization (ELSO) Guidelines for Adult Respiratory Failure August, 2017 This guideline describes prolonged extracorporeal life support (ECLS, ECMO), applicable
Outline. Electrical Activity of the Human Heart. What is the Heart? The Heart as a Pump. Anatomy of the Heart. The Hard Work
 Electrical Activity of the Human Heart Oguz Poroy, PhD Assistant Professor Department of Biomedical Engineering The University of Iowa Outline Basic Facts about the Heart Heart Chambers and Heart s The
Electrical Activity of the Human Heart Oguz Poroy, PhD Assistant Professor Department of Biomedical Engineering The University of Iowa Outline Basic Facts about the Heart Heart Chambers and Heart s The
Clinical Commissioning Policy Statement: Patent Foramen Ovale (PFO) Closure. April Reference: NHSCB/A09/PS/a
 Clinical Commissioning Policy Statement: Patent Foramen Ovale (PFO) Closure April 2013 Reference: NHSCB/A09/PS/a NHS Commissioning Board Clinical Commissioning Policy Statement: Patent Foramen Ovale (PFO)
Clinical Commissioning Policy Statement: Patent Foramen Ovale (PFO) Closure April 2013 Reference: NHSCB/A09/PS/a NHS Commissioning Board Clinical Commissioning Policy Statement: Patent Foramen Ovale (PFO)
Bilateral Simultaneous Lung Lava
 Bilateral Simultaneous Lung Lava B e Utilizing Membrane Oxygenator or Pulmonary Alveolar Proteinosis in an &Month=Old Infant Loren F. Hiratzka, M.D., Davis M. Swan, M.D., Earl F. Rose, M.D., and Richard
Bilateral Simultaneous Lung Lava B e Utilizing Membrane Oxygenator or Pulmonary Alveolar Proteinosis in an &Month=Old Infant Loren F. Hiratzka, M.D., Davis M. Swan, M.D., Earl F. Rose, M.D., and Richard
Understanding the Cardiopulmonary Bypass Machine and Its Tubing
 Understanding the Cardiopulmonary Bypass Machine and Its Tubing Robert S. Leckie, MD Division of Cardiac Anesthesia, Beth Israel Deaconess Medical Center ABL 1/09 Reservoir Bucket This is a cartoon of
Understanding the Cardiopulmonary Bypass Machine and Its Tubing Robert S. Leckie, MD Division of Cardiac Anesthesia, Beth Israel Deaconess Medical Center ABL 1/09 Reservoir Bucket This is a cartoon of
Learning Objectives; 1. Identify the key features of the cardiovascular system. 2. Describe the function of the cardiovascular system.
 Learning Objectives; 1. Identify the key features of the cardiovascular system. 2. Describe the function of the cardiovascular system. https://www.youtube.com/watch?v=yaxna8lmoiy The Circulatory System
Learning Objectives; 1. Identify the key features of the cardiovascular system. 2. Describe the function of the cardiovascular system. https://www.youtube.com/watch?v=yaxna8lmoiy The Circulatory System
Cardioplegia Circuit Products { CARDIOPLEGIA ADAPTERS}
 Cardioplegia Circuit Products { CARDIOPLEGIA ADAPTERS} Cardioplegia adapters are designed to permit customization of the cardioplegia circuit. Medtronic adapters can be used to connect multiple cardioplegia
Cardioplegia Circuit Products { CARDIOPLEGIA ADAPTERS} Cardioplegia adapters are designed to permit customization of the cardioplegia circuit. Medtronic adapters can be used to connect multiple cardioplegia
Contents. Page 1. Homework 11 Chapter Blood Vessels Due: Week 6 Lec 11
 Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
The Physiology of the Fetal Cardiovascular System
 The Physiology of the Fetal Cardiovascular System Jeff Vergales, MD, MS Department of Pediatrics Division of Pediatric Cardiology jvergales@virginia.edu Disclosures I serve as the medical director for
The Physiology of the Fetal Cardiovascular System Jeff Vergales, MD, MS Department of Pediatrics Division of Pediatric Cardiology jvergales@virginia.edu Disclosures I serve as the medical director for
ECMO CPR. Ravi R. Thiagarajan MBBS, MPH. Cardiac Intensive Care Unit
 ECMO CPR Ravi R. Thiagarajan MBBS, MPH Staff Intensivist Cardiac Intensive Care Unit Children s Hospital Boston PCICS 2008, Miami, FL No disclosures Disclosures Outline Outcomes for Pediatric in-hospital
ECMO CPR Ravi R. Thiagarajan MBBS, MPH Staff Intensivist Cardiac Intensive Care Unit Children s Hospital Boston PCICS 2008, Miami, FL No disclosures Disclosures Outline Outcomes for Pediatric in-hospital
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Surviving Sepsis Campaign. Guidelines for Management of Severe Sepsis/Septic Shock. An Overview
 Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
The Mammalian Circulatory System
 The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
12.1 The Function of Circulation
 12.1 The Function of Circulation The Circulatory System Magnetic Resonance Angiography (MRA) Heart pump beats 100 000 times a day Deliver oxygen and nutrients Function of Circulation Multicellular organisms
12.1 The Function of Circulation The Circulatory System Magnetic Resonance Angiography (MRA) Heart pump beats 100 000 times a day Deliver oxygen and nutrients Function of Circulation Multicellular organisms
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
ECMO vs. CPB for Intraoperative Support: How do you Choose?
 ECMO vs. CPB for Intraoperative Support: How do you Choose? Shaf Keshavjee MD MSc FRCSC FACS Director, Toronto Lung Transplant Program Surgeon-in-Chief, University Health Network James Wallace McCutcheon
ECMO vs. CPB for Intraoperative Support: How do you Choose? Shaf Keshavjee MD MSc FRCSC FACS Director, Toronto Lung Transplant Program Surgeon-in-Chief, University Health Network James Wallace McCutcheon
MICS & FEMORAL CANNULAE
 MICS & FEMORAL CANNULAE Cannulae that can High performance cannulae for direct and femoral cannulation, either in conventional or minimally invasive cardiac surgery 1. Pfeiffer et al. Interactive Cardiovascular
MICS & FEMORAL CANNULAE Cannulae that can High performance cannulae for direct and femoral cannulation, either in conventional or minimally invasive cardiac surgery 1. Pfeiffer et al. Interactive Cardiovascular
Circulation.notebook March 07, Maintaining Dynamic Equilibrium. Oct 11 3:27 PM. Circulatory System p
 Unit 3 Maintaining Dynamic Equilibrium Circulatory system The heart Blood Blood Pressure Circulatory Disorders Oct 11 3:27 PM Circulatory System p.304 307 If an organism is small and flat it can transport
Unit 3 Maintaining Dynamic Equilibrium Circulatory system The heart Blood Blood Pressure Circulatory Disorders Oct 11 3:27 PM Circulatory System p.304 307 If an organism is small and flat it can transport
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Bellwork Define: hemostasis anticoagulation hemophilia (Then write the underline portion of the two state standards in your notes).
 Bellwork Define: hemostasis anticoagulation hemophilia (Then write the underline portion of the two state standards in your notes). A&P Standards 31) Identify the liquid and cellular components of blood
Bellwork Define: hemostasis anticoagulation hemophilia (Then write the underline portion of the two state standards in your notes). A&P Standards 31) Identify the liquid and cellular components of blood
THE CIRCULATORY SYSTEM
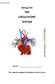 Biology 30S THE CIRCULATORY SYSTEM Name: This module adapted from bblearn.merlin.mb.ca 1 Introduction to Circulation The first organ to form, and the last organ to die. The heart is the pump of life. The
Biology 30S THE CIRCULATORY SYSTEM Name: This module adapted from bblearn.merlin.mb.ca 1 Introduction to Circulation The first organ to form, and the last organ to die. The heart is the pump of life. The
Girish M Nair, Seeger Shen, Pablo B Nery, Calum J Redpath, David H Birnie
 268 Case Report Cardiac Resynchronization Therapy in a Patient with Persistent Left Superior Vena Cava Draining into the Coronary Sinus and Absent Innominate Vein: A Case Report and Review of Literature
268 Case Report Cardiac Resynchronization Therapy in a Patient with Persistent Left Superior Vena Cava Draining into the Coronary Sinus and Absent Innominate Vein: A Case Report and Review of Literature
Respiration & Circulation
 Respiration & Circulation Objectives Describe the purpose of the respiratory system List & describe the structures of the respiratory system Describe the respiratory cycle, frequency, and factors that
Respiration & Circulation Objectives Describe the purpose of the respiratory system List & describe the structures of the respiratory system Describe the respiratory cycle, frequency, and factors that
Circulatory System Objective sheet 3
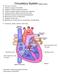 Circulatory System Objective sheet 3 10. Functions of blood 1) Transport oxygen and nutrients 2) Transport of carbon dioxide and waste 3) Protection against disease causing micro-organisms 4) Clotting
Circulatory System Objective sheet 3 10. Functions of blood 1) Transport oxygen and nutrients 2) Transport of carbon dioxide and waste 3) Protection against disease causing micro-organisms 4) Clotting
Cardiovascular System. Heart Anatomy
 Cardiovascular System Heart Anatomy 1 The Heart Location & general description: Atria vs. ventricles Pulmonary vs. systemic circulation Coverings Walls The heart is found in the mediastinum, the medial
Cardiovascular System Heart Anatomy 1 The Heart Location & general description: Atria vs. ventricles Pulmonary vs. systemic circulation Coverings Walls The heart is found in the mediastinum, the medial
Ultrasound Guidance for Extra-corporeal Membrane Oxygenation. General Guidelines
 Ultrasound Guidance for Extra-corporeal Membrane Oxygenation General Guidelines Authors: Vinodh Bhagyalakshmi Nanjayya MBBS, MD, EDIC, FCICM, DDU (Melbourne, Australia) Deirdre Murphy MB BCh BAO, MRCPI,
Ultrasound Guidance for Extra-corporeal Membrane Oxygenation General Guidelines Authors: Vinodh Bhagyalakshmi Nanjayya MBBS, MD, EDIC, FCICM, DDU (Melbourne, Australia) Deirdre Murphy MB BCh BAO, MRCPI,
Heart Facts. The average adult heart beats 72 times a min 100,000 times a day 3,600,000 times a year 2.5 billion times during a lifetime.
 Circulatory System Heart Facts The average adult heart beats 72 times a min 100,000 times a day 3,600,000 times a year 2.5 billion times during a lifetime. Heart Facts Weighs 11 oz A healthy heart pumps
Circulatory System Heart Facts The average adult heart beats 72 times a min 100,000 times a day 3,600,000 times a year 2.5 billion times during a lifetime. Heart Facts Weighs 11 oz A healthy heart pumps
Temporary circulatory support in the form of extracorporeal
 Preliminary In Vivo Testing of a Novel Pump for Short-Term Extracorporeal Life Support David J. Spurlock, MD, Kelly Koch, BS, Daniel E. Mazur, BS, Emilia M. Fracz, ME, Robert H. Bartlett, MD, and Jonathan
Preliminary In Vivo Testing of a Novel Pump for Short-Term Extracorporeal Life Support David J. Spurlock, MD, Kelly Koch, BS, Daniel E. Mazur, BS, Emilia M. Fracz, ME, Robert H. Bartlett, MD, and Jonathan
