I. Cardiac Output Chapter 14
|
|
|
- Emily Kennedy
- 6 years ago
- Views:
Transcription
1 10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac Output Volume of blood pumped each minute by each ventricle: cardiac output = stroke volume X heart rate (ml/minute) (ml/beat) (beats/min) Average heart rate = 70 bpm Average stroke volume = ml/beat Average cardiac output = 5,500 ml/minute Regulation of Cardiac Rate Regulation of Cardiac Rate Spontaneous depolarization occurs at SA node when HCN channels open, allowing Na+ in. Sympathetic norepinephrine (vagus nerve) and adrenal epinephrine keep HCN channels open, increasing heart rate. Regulation of Cardiac Rate Parasympathetic acetylcholine opens K+ channels, slowing heart rate. Controlled by cardiac center of medulla oblongata 1
2 Regulation of Stroke Volume Regulated by three variables: 1. End diastolic volume (EDV): volume of blood in the ventricles at the end of diastole - Sometimes called preload - Stroke volume increases with increased EDV. Regulation of Stroke Volume Regulated by three variables: 2. Total peripheral resistance: Frictional resistance in the arteries - Inversely related to stroke volume 3. Contractility: strength of ventricular contraction - Stroke volume increases with contractility. Frank-Starling Law Increased EDV results in increased contractility and thus increased stroke volume. Intrinsic Control of Contraction Strength Due to myocardial stretch Increased EDV stretches the myocardium, which increases contraction strength. Due to increased myosin and actin overlap and increased sensitivity to Ca 2+ in cardiac muscle cells Intrinsic Control of Contraction Strength Extrinsic Control of Contractility Sympathetic norepinephrine and adrenal epinephrine can increase contractility by making more Ca 2+ available to sarcomeres. 2
3 Venous Return Venous Return End diastolic volume is controlled by factors that affect venous return: Total blood volume Venous pressure Veins are compliant = stretch at a given pressure. They hold more blood than arteries but maintain lower pressure. Factors in Venous Return 1. Highest pressure in venules vs. lowest pressure in veins closest to heart 2. Sympathetic nerve activity to stimulate smooth muscles and lower compliance Factors in Venous Return 3. Skeletal muscle pumps 4. Pressure difference between abdominal and thoracic cavities 5. Blood volume Factors in Venous Return II. Blood Volume 3
4 Body Water Distribution Body Water Distribution 2/3 of our body water is found in the cells. Of the remaining, 80% exists in interstitial spaces and 20% is in the blood plasma. Osmotic forces control the movement of water between the interstitial spaces and the capillaries, affecting blood volume. Urine formation and water intake (drinking) also play a role in blood volume. Tissue/Capillary Fluid Exchange Net filtration pressure is the hydrostatic pressure of the blood in the capillaries minus the hydrostatic pressure of the fluid outside the capillaries: =36 mmhg at arteriole end =16 mmhg at venule end Tissue/Capillary Fluid Exchange Colloid osmotic pressure: due to proteins dissolved in fluid Blood plasma has higher colloid osmotic pressure than interstitial fluid. This difference is called oncotic pressure. Oncotic pressure = 25 mmhg This favors the movement of fluid into the capillaries. Tissue/Capillary Fluid Exchange Starling Forces: combination of hydrostatic pressure and oncotic pressure that predicts movement of fluid across capillary membranes Fluid movement is proportional to: (p c + π i ) - (p i + π p ) fluid out fluid in p c = Hydrostatic pressure in capillary π i s = Colloid osmotic pressure of interstitial fluid p i s = Hydrostatic pressure of interstitial fluid π p = Colloid osmotic pressure of blood plasma Tissue/Capillary Fluid Exchange Starling Forces predict the movement of fluid into the capillaries at the arteriole end and out of the capillaries at the venule end. 4
5 Tissue/Capillary Fluid Exchange Edema Excessive accumulations of interstitial fluids May be the result of: High arterial blood pressure Venous obstruction Leakage of plasma proteins into interstitial space Myxedema (excessive production of mucin in extracellular spaces caused by hypothyroidism) Decreased plasma protein concentration Obstruction of lymphatic drainage Edema The formation of urine begins with filtration of fluid through capillaries in the kidneys called glomeruli. 180 L of filtrate is moved across the glomeruli per day, yet only about 1.5 L is actually removed as urine. The rest is reabsorbed into the blood. The amount of fluid reabsorbed is controlled by several hormones in response to the body s needs. Antidiuretic hormone (ADH): produced by hypothalamus and released when osmoreceptors there detect increased plasma osmolarity. Plasma osmolarity can increase due to excessive salt intake or dehydration. Increased plasma osmolarity also increases thirst. ADH stimulates water reabsorption. Increased water intake and decreased urine formation increase blood volume. Blood becomes dilute, and ADH is no longer released. Stretch receptors in left atrium, carotid sinus, and aortic arch also inhibit ADH release. 5
6 Aldosterone: secreted by adrenal cortex indirectly when blood volume and pressure are reduced Stimulates reabsorption of salt in kidneys Regulated by renin-angiotensin-aldosterone system Renin-angiotensin-aldosterone system: When blood pressure is low, cells in the kidneys (juxtaglomerular apparatus) secrete the enzyme renin: Angiotensinogen is converted to angiotensin I. Angiotensin I is converted to angiotensin II by ACE enzyme. Angiotensin II has many effects that result in a raise in blood pressure: Vasoconstriction of small arteries and arterioles Stimulates thirst center in hypothalamus Stimulates production of aldosterone in adrenal cortex Atrial natriuretic peptide: produced by the atria of the heart when stretch is detected Promotes salt and water excretion in urine in response to increased blood volume Inhibits ADH secretion 6
7 III. Vascular Resistance to Blood Flow Blood Flow to the Organs Blood Flow to the Organs Cardiac output is distributed unequally to different organs due to unequal resistance to blood flow through the organs. Physical Laws Regulating Blood Flow Physical Laws Regulating Blood Flow Blood flows from a region of higher pressure to a region of lower pressure. The rate of blood flow is proportional to the differences in pressure. 7
8 Physical Laws Regulating Blood Flow The rate of blood flow is also inversely proportional to the frictional resistance to blood flow within the vessels. ΔP blood flow = resistance ΔP = pressure difference between the two ends of the tube Physical Laws Regulating Blood Flow Resistance is measured as: Lη resistance = r 4 L = length of the vessel η = viscosity of the blood r = radius of the blood vessel Physical Laws Regulating Blood Flow Physical Laws Regulating Blood Flow Poiseuille s Law adds in physical constraints: ΔPr 4 (π) blood flow = ηl(8) Physical Laws Regulating Blood Flow Physical Laws Regulating Blood Flow Vessel length (L) and blood viscosity (η) do not vary normally. Mean arterial pressure and vessel radius (r) are therefore the most important factors in blood flow. Vasoconstriction of arterioles provides the greatest resistance to blood flow and can redirect flow to/from particular organs. 8
9 10/24/11 Physical Laws Regulating Blood Flow Total Peripheral Resistance The sum of all vascular resistance in systemic circulation Blood flow to organs runs parallel to each other, so a change in resistance within one organ does not affect another. Vasodilation in a large organ may decrease total peripheral resistance and mean arterial pressure. Increased cardiac output and vasoconstriction elsewhere make up for this. Extrinsic Regulation of Blood Flow Extrinsic Control of Blood Flow Autonomic and endocrine control of blood flow Sympathetic nerves: Increases total peripheral resistance through release of norepinephrine onto smooth muscles of arterioles in the viscera and skin to stimulate vasoconstriction. Acetylcholine is released onto skeletal muscles, resulting in increased vasodilation to these tissues (due in part to adrenal epinephrine). Extrinsic Regulation of Blood Flow Extrinsic Regulation of Blood Flow Parasympathetic nerves: Acetylcholine stimulates vasodilation. Limited to digestive tract, external genitalia, and salivary glands Less important in controlling total peripheral resistance due to limited influence Paracrine control: Molecules produced by one tissue control another tissue within the same organ. Example: The tunica intima produces signals to influence smooth muscle activity in the tunica media. 9
10 Extrinsic Regulation of Blood Flow Intrinsic Regulation of Blood Flow Smooth muscle relaxation influenced by bradykinin, nitric oxide, and prostaglandin I 2 to produce vasodilation Endothelin-1 stimulates smooth muscle contraction to produce vasoconstriction and raise total peripheral resistance. Used by some organs (brain and kidneys) to promote constant blood flow when there is fluctuation of blood pressure; also called autoregulation. Myogenic control mechanisms: Vascular smooth muscle responds to changes in arterial blood pressure. Intrinsic Regulation of Blood Flow Metabolic control mechanisms: Vasodilation is controlled by changes in: Decreased oxygen concentrations due to increased metabolism Increased carbon dioxide concentrations Decreased tissue ph (due to CO 2, lactic oxide, etc.) Release of K + and paracrine signals IV. Blood Flow to the Heart and Skeletal Muscles Aerobic Requirements of the Heart Aerobic Requirements of the Heart The coronary arteries supply blood to a massive number of capillaries (2,500 4,000 per cubic mm tissue). Cardiac tissue also has lots of mitochondria and respiratory enzymes, thus is metabolically very active. Unlike most organs, blood flow is restricted during systole. Cardiac tissue therefore has myoglobin to store oxygen during diastole to be released in systole. During exercise, the coronary arteries increase blood flow from 80 ml to 400 ml/ minute/100 g tissue. 10
11 Regulation of Coronary Blood Flow Norepinephrine from sympathetic nerve fibers stimulates vasoconstriction, raising vascular resistance at rest. Adrenal epinephrine stimulates vasodilation and thus vascular resistance during exercise. Vasodilation is enhanced by intrinsic metabolic control mechanisms Regulation of Blood Flow Through Skeletal Muscles Arterioles have high vascular resistance at rest. Even at rest, skeletal muscles still receive 20 25% of the body s blood supply. Regulation of Blood Flow Through Skeletal Muscles Regulation of Blood Flow Through Skeletal Muscles Vasodilation is stimulated by both adrenal epinephrine and sympathetic acetylcholine. Intrinsic metabolic controls enhance vasodilation during exercise Circulatory Changes During Exercise Vascular resistance to skeletal and cardiac muscles decreases due to: Increased cardiac output Metabolic vasodilation Diversion of blood away from viscera and skin Circulatory Changes During Exercise Cardiac output can increase 5X due to increased cardiac rate. Stroke volume can increase some due to increased venous return. Blood flow to brain increases a small amount with moderate exercise and decreases a small amount during intense exercise. 11
12 10/24/11 Circulatory Changes During Exercise Circulatory Changes During Exercise Cerebral Circulation V. Blood Flow to the Brain and Skin The brain cannot tolerate much variation in blood flow. Unless mean arterial pressure becomes very high, there is little sympathetic control of blood flow to the brain. At high pressure, vasoconstriction occurs to protect small vessels from damage and stroke. Myogenic Control of Cerebral Blood Flow When blood pressure falls, cerebral vessels automatically dilate. When blood pressure rises, cerebral vessels automatically constrict. Metabolic Control of Cerebral Blood Flow The most active regions of the brain must receive increased blood flow due to arteriole sensitivity to metabolic changes. Astrocytes may play a role Decreased ph of cerebrospinal fluid (buildup of CO2) also causes arteriole dilation. 12
13 Metabolic Control of Cerebral Blood Flow Cutaneous Blood Flow The skin can tolerate the greatest fluctuations in blood flow. The skin helps control body temperature in a changing environment by regulating blood flow = thermoregulation. Increased blood flow to capillaries in the skin releases heat when body temperature increases. Sweat is also produced to aid in heat loss. Bradykinins in the sweat glands also stimulate vasodilation in the skin. Cutaneous Blood Flow Vasoconstriction of arterioles keeps heat in the body when ambient temperatures are low. This is aided by arteriovenous anastomoses, which shunt blood from arterioles directly to venules. Cold temperatures activate sympathetic vasoconstriction. This is tolerated due to decreased metabolic activity in the skin. Cutaneous Blood Flow At average ambient temperatures, vascular resistance in the skin is high, and blood flow is low. Sympathetic stimulation reduces blood flow further. With continuous exercise, the need to regulate body temperature overrides this, and vasodilation occurs. Cutaneous Blood Flow Cutaneous Blood Flow May result in lowered total peripheral resistance if not for increased cardiac output However, if a person exercises in very hot weather, he or she may experience extreme drops in blood pressure after reduced cardiac output. This condition can be very dangerous. 13
14 Blood Pressure VI. Blood Pressure Affected by blood volume/stroke volume, total peripheral resistance, and cardiac rate Increase in any of these will increase blood pressure. Vasoconstriction of arterioles raises blood pressure upstream in the arteries. Blood Pressure Blood Pressure Capillary blood pressure is low because of large total cross-sectional area. Blood Pressure Regulation Baroreceptor Reflex Kidneys can control blood volume and thus stroke volume. The sympathoadrenal system stimulates vasoconstriction of arterioles (raising total peripheral resistance) and increased cardiac output. Activated by changes in blood pressure detected by baroreceptors in the aortic arch and carotid sinuses 14
15 Baroreceptor Reflex Baroreceptor Reflex Increased blood pressure stretches these receptors, increasing action potentials to the vasomotor and cardiac control centers in the medulla. Most sensitive to drops in blood pressure Baroreceptor Reflex Baroreceptor Reflex The vasomotor center controls vasodilation and constriction. The cardiac center controls heart rate. Baroreceptor Reflex Baroreceptor Reflex Fall in blood pressure = sympathetic and parasympathetic activity, resulting in increased heart rate and total peripheral resistance Rise in BP has the opposite effects. Good for quick beat-by-beat regulation 15
16 Atrial Stretch Reflexes Blood Pressure Measurement Activated by increased venous return to: Stimulate tachycardia Inhibit ADH release Results in excretion of more urine Stimulate secretion of atrial natriuretic peptide Results in excretion of more salts and water in urine Measured in mmhg by an instrument called a sphygmomanometer. A blood pressure cuff produces turbulent flow of blood in the brachial artery, which can be heard using a stethoscope; called sounds of Korotkoff. Blood Pressure Measurement Blood Pressure Measurement The cuff is first inflated to beyond systolic blood pressure to pinch off an artery. As pressure is released, the first sound is heard at systole and a reading can be taken. The average blood pressure is 120/80. The last Korotkoff sound is heard when the pressure in the cuff reaches diastolic pressure and a second reading can be taken. Pulse Pressure Taking the pulse is a measure of heart rate. What the health professional feels is increased blood pressure in that artery at systole. The difference between blood pressure at systole and at diastole is the pulse pressure. If your blood pressure is 120/80, your pulse pressure is 40 mmhg. Mean Arterial Pressure The average pressure in the arteries in one cardiac cycle is the mean arterial pressure. This is significant because it is the difference between mean arterial pressure and venous pressure that drives the blood into the capillaries. Calculated as: diastolic pressure + 1/3 pulse pressure 16
17 Hypertension VII. Hypertension, Shock, and Congestive Heart Failure Hypertension is high blood pressure. 20% of Americans have hypertension. It can increase the risk of cardiac diseases and stroke. Hypertension can be classified as essential or secondary. Secondary hypertension is a symptom of another disease, such as kidney disease. Secondary Hypertension Essential Hypertension Most people fall in this category. The cause is difficult to determine and may involve any of the following: Increased salt intake coupled with decreased kidney filtering ability Increased sympathetic nerve activity, increasing heart rate Responses to paracrine regulators from the endothelium Dangers of Hypertension Vascular damage within organs, especially dangerous in the cerebral vessels and leading to stroke Ventricular overload to eject blood, leading to arrhythmias and cardiac arrest Contributes to the development of atherosclerosis Treatments for Hypertension Lifestyle modification: limit salt intake; limit smoking and drinking; lose weight; exercise K + (and possibly calcium) supplements Diuretics to increase urine formation Beta blockers to decrease cardiac rate ACE inhibitors to block angiotensin II production 17
18 Circulatory Shock Circulatory Shock Occurs when there is inadequate blood flow to match oxygen usage in the tissues Symptoms result from inadequate blood flow and how our circulatory system changes to compensate. Sometimes shock leads to death. Hypovolemic Shock Due to low blood volume from an injury, dehydration, or burns Characterized by decreased cardiac output and blood pressure Blood is diverted to the heart and brain at the expense of other organs. Compensation includes baroreceptor reflex, which lowers blood pressure, raises heart rate, raises peripheral resistance, and produces cold, clammy skin and low urine output. Septic Shock Dangerously low blood pressure due to an infection (sepsis) Bacterial toxins induce NO production, causing widespread vasodilation. Mortality rate is high (50 70%). Other Causes of Circulatory Shock Severe allergic reactions can cause anaphylactic shock due to production of histamine and resulting vasodilation. Spinal cord injury or anesthesis can cause neurogenic shock due to loss of sympathetic stimulation. Cardiac failure can cause cardiogenic shock due to significant myocardial loss. Congestive Heart Failure Occurs when cardiac output is not sufficient to maintain blood flow required by the body Caused by myocardial infarction, congenital defects, hypertension, aortic valve stenosis, or disturbances in electrolyte levels (K + and Ca 2+ ) Similar to hypovolemic shock in symptoms 18
Physiology of Circulation
 Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Cardiovascular system: Blood vessels, blood flow. Latha Rajendra Kumar, MD
 Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
CHAPTER 14 CARDIAC OUTPUT, BLOOD FLOW, AND BLOOD PRESSURE
 CHAPTER 14 CARDIAC OUTPUT, BLOOD FLOW, AND BLOOD PRESSURE CHAPTER SCOPE The last chapter introduced the blood, the structure and function of the heart and the blood vessels. Logically, this chapter follows
CHAPTER 14 CARDIAC OUTPUT, BLOOD FLOW, AND BLOOD PRESSURE CHAPTER SCOPE The last chapter introduced the blood, the structure and function of the heart and the blood vessels. Logically, this chapter follows
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
During exercise the heart rate is 190 bpm and the stroke volume is 115 ml/beat. What is the cardiac output?
 The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
Heart. Large lymphatic vessels Lymph node. Lymphatic. system Arteriovenous anastomosis. (exchange vessels)
 Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
BIOL 219 Spring Chapters 14&15 Cardiovascular System
 1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
Cardiac Output 1 Fox Chapter 14 part 1
 Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
Therefore MAP=CO x TPR = HR x SV x TPR
 Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide 1 Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical Application
Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide 1 Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical Application
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Cardiovascular System. Blood Vessel anatomy Physiology & regulation
 Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM
 Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
 Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation
 Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation I. General Features of Blood Vessel Structure A. General Pattern of Circulation 1. Ventricles pump blood into 2. These arteries
Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation I. General Features of Blood Vessel Structure A. General Pattern of Circulation 1. Ventricles pump blood into 2. These arteries
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions
 Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Chapter 21 Peripheral circulation and Regulation
 Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
3/10/2009 VESSELS PHYSIOLOGY D.HAMMOUDI.MD. Palpated Pulse. Figure 19.11
 VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Mechanism: 1- waterretention from the last part of the nephron which increases blood volume, venous return EDV, stroke volume and cardiac output.
 Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Presenter: Tom Mulvey
 Slides are from Level 3 Biology Course Content Day, 7 th November 2012 Presenter: Tom Mulvey Teachers are free to use these for teaching purposes with appropriate acknowledgement Blood Pressure Ways of
Slides are from Level 3 Biology Course Content Day, 7 th November 2012 Presenter: Tom Mulvey Teachers are free to use these for teaching purposes with appropriate acknowledgement Blood Pressure Ways of
The Cardiovascular system: physiology of circulation
 Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
PHYSIOLOGY MeQ'S (Morgan) All the following statements related to blood volume are correct except for: 5 A. Blood volume is about 5 litres. B.
 PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
The Cardiovascular System. The Structure of Blood Vessels. The Structure of Blood Vessels. The Blood Vessels. Blood Vessel Review
 The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
Blood Flow, Blood Pressure, Cardiac Output. Blood Vessels
 Blood Flow, Blood Pressure, Cardiac Output Blood Vessels Blood Vessels Made of smooth muscle, elastic and fibrous connective tissue Cells are not electrically coupled Blood Vessels Arteries arterioles
Blood Flow, Blood Pressure, Cardiac Output Blood Vessels Blood Vessels Made of smooth muscle, elastic and fibrous connective tissue Cells are not electrically coupled Blood Vessels Arteries arterioles
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Chapter 21! Chapter 21 Blood Vessels and Circulation! Blood Vessels and Circulation!
 Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
1. Distinguish among the types of blood vessels on the basis of their structure and function.
 Blood Vessels and Circulation Objectives This chapter describes the structure and functions of the blood vessels Additional subjects contained in Chapter 13 include cardiovascular physiology, regulation,
Blood Vessels and Circulation Objectives This chapter describes the structure and functions of the blood vessels Additional subjects contained in Chapter 13 include cardiovascular physiology, regulation,
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties!
 Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 1! Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 1! Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
BIOH122 Session 6 Vascular Regulation
 BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
*Generating blood pressure *Routing blood: separates. *Ensuring one-way blood. *Regulating blood supply *Changes in contraction
 *Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
*Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
Physiology of Circulation. Dr. Hiwa Shafiq 16/12/2018
 Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Vascular System Part One
 Vascular System Part One Objectives Trace the route taken by blood as it leaves, and then returns to the heart. Describe the structure of the walls of arteries and veins. Discuss the structure and function
Vascular System Part One Objectives Trace the route taken by blood as it leaves, and then returns to the heart. Describe the structure of the walls of arteries and veins. Discuss the structure and function
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Chapter 15 Fluid and Acid-Base Balance
 Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Collage of medicine Cardiovascular Physiology 3- Arterial and venous blood Pressure.
 University of Babylon Collage of medicine Dr. Ghafil Seyhood Hassan Al-Shujiari Cardiovascular Physiology 3- Arterial and venous blood Pressure. UArterial blood pressureu: Arterial pressure = COP X Peripheral
University of Babylon Collage of medicine Dr. Ghafil Seyhood Hassan Al-Shujiari Cardiovascular Physiology 3- Arterial and venous blood Pressure. UArterial blood pressureu: Arterial pressure = COP X Peripheral
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp , , , I. Major Functions of the Circulatory System
 P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
Cardiovascular regulation. Neural and hormonal Regulation Dr Badri Paudel GMC. 1-Local factors (autoregulation) Control of Blood Flow
 Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
CHAPTER 21 LECTURE OUTLINE
 CHAPTER 21 LECTURE OUTLINE I. INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated. B.
CHAPTER 21 LECTURE OUTLINE I. INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated. B.
Chapter 9, Part 2. Cardiocirculatory Adjustments to Exercise
 Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D.
 Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Chapter 21. Blood Vessels and Circulation
 Chapter 21 Blood Vessels and Circulation INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated.
Chapter 21 Blood Vessels and Circulation INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated.
Blood Pressure. a change in any of these could cause a corresponding change in blood pressure
 Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Types of Blood Vessels
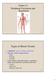 Chapter 21 Peripheral Circulation and Regulation 21-1 Types of Blood Vessels Capillaries: site of exchange with tissue Arteries in dif. Types & sizes Elastic Muscular Arterioles Veins: thinner walls than
Chapter 21 Peripheral Circulation and Regulation 21-1 Types of Blood Vessels Capillaries: site of exchange with tissue Arteries in dif. Types & sizes Elastic Muscular Arterioles Veins: thinner walls than
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the
 Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
Peripheral Circulation and Regulation
 Peripheral Circulation and Regulation Functions of Peripheral Circulation 1. Contain the blood 2. Exchange nutrients, waste products, and gases with tissues 3. Transport 4. Regulate blood pressure, along
Peripheral Circulation and Regulation Functions of Peripheral Circulation 1. Contain the blood 2. Exchange nutrients, waste products, and gases with tissues 3. Transport 4. Regulate blood pressure, along
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
IP: Regulation of Cardiac Output
 ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
Cardiovascular System B L O O D V E S S E L S 3
 Cardiovascular System B L O O D V E S S E L S 3 Fluid Shifts Between Capillaries and Tissue Permeable capillaries allow plasma and solutes to pass into interstitial space interstitial or extracellular
Cardiovascular System B L O O D V E S S E L S 3 Fluid Shifts Between Capillaries and Tissue Permeable capillaries allow plasma and solutes to pass into interstitial space interstitial or extracellular
Properties of Pressure
 OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
Cardiovascular System: The Heart
 Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
Cardiovascular System. Heart
 Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Homeostatic Regulation of the Vascular System *
 OpenStax-CNX module: m46603 1 Homeostatic Regulation of the Vascular System * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
OpenStax-CNX module: m46603 1 Homeostatic Regulation of the Vascular System * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
Chapter 12 Lecture Outline
 Chapter 12 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Chapter 12 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Means failure of heart to pump enough blood to satisfy the need of the body.
 Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Physiology lecture 15 Hemodynamic
 Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Circulation: Chapter 25. Cardiac Output. The Mammalian Heart Fig Right side of the heart
 Circulation: Chapter 25 1. Limits of Diffusion A. Small organisms use diffusion B. rapid over small distances 2. Most animals have circulatory systems A. Blood B. Pump (Heart) or propulsive structures
Circulation: Chapter 25 1. Limits of Diffusion A. Small organisms use diffusion B. rapid over small distances 2. Most animals have circulatory systems A. Blood B. Pump (Heart) or propulsive structures
Chapter 24 Vital Signs. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Cardiovascular System: Vessels and Circulation (Chapter 21)
 Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Blood Pressure Regulation -1
 CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
The Cardiovascular System: Vessels and Routes. Pulmonary Circulation H E A R T. Systemic Circulation
 The Cardiovascular System: Vessels and Routes 1. Overview of Blood Circulation A. Pulmonary Circulation Lung Arterioles Pulmonary Artery Capillaries Pulmonary Circulation Venules Pulmonary Veins H E A
The Cardiovascular System: Vessels and Routes 1. Overview of Blood Circulation A. Pulmonary Circulation Lung Arterioles Pulmonary Artery Capillaries Pulmonary Circulation Venules Pulmonary Veins H E A
THE HEART Dr. Ali Ebneshahidi
 THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
Cardiovascular Physiology
 Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
d) Cardiovascular System Higher Human Biology
 d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
Cardiac Output (C.O.) Regulation of Cardiac Output
 Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Circulation. Sinoatrial (SA) Node. Atrioventricular (AV) Node. Cardiac Conduction System. Cardiac Conduction System. Linked to the nervous system
 Circulation Cardiac Conduction System AHS A H S Your body resembles a large roadmap. There are routes or arteries that take you downtown to the heart of the city and veins that take you to the outskirts
Circulation Cardiac Conduction System AHS A H S Your body resembles a large roadmap. There are routes or arteries that take you downtown to the heart of the city and veins that take you to the outskirts
CASE 13. What neural and humoral pathways regulate arterial pressure? What are two effects of angiotensin II?
 CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
Function: Transportation of. Oxygen Nutrients Waste Hormones gases
 Function: Transportation of Oxygen Nutrients Waste Hormones gases Pericardium: double sac of serous membrane filled with fluid (pericardial fluid to be exact) that surrounds the heart. Parietal pericardium:
Function: Transportation of Oxygen Nutrients Waste Hormones gases Pericardium: double sac of serous membrane filled with fluid (pericardial fluid to be exact) that surrounds the heart. Parietal pericardium:
Six main classes of blood vessels (on handout) Wall structure of arteries and veins (on handout) Comparison: Arteries vs. Veins (on handout)
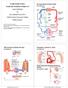 Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Six main classes of blood vessels Primary Sources
Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Six main classes of blood vessels Primary Sources
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
HYPERTENSION: Sustained elevation of arterial blood pressure above normal o Systolic 140 mm Hg and/or o Diastolic 90 mm Hg
 Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Control of blood tissue blood flow. Faisal I. Mohammed, MD,PhD
 Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Vasoconstriction if BP goes up. Vasodilation BP goes down. blood.. Vasodilation wastes detected, to move them away. None
 Shuster s A&P Notes Series Blood Vessels,, Perfusion & Capillary Dynamics 15 Summary of Controls on Perfusion and Systemic BP (short version): 1. Autoregulation of perfusion Control Category Short Term
Shuster s A&P Notes Series Blood Vessels,, Perfusion & Capillary Dynamics 15 Summary of Controls on Perfusion and Systemic BP (short version): 1. Autoregulation of perfusion Control Category Short Term
Chapter 13 The Cardiovascular System: Cardiac Function
 Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Cardiovascular Boot Camp April 2009
 Advanced Cardiac Dynamics Presented by: Karen Marzlin BSN, RN, CCRN-CMC CNEA 2009 1 Hemodynamics does not equal invasive monitoring Paradigm Shift 2 www.cardionursing.com 1 3 Circulation: Heart Arteries
Advanced Cardiac Dynamics Presented by: Karen Marzlin BSN, RN, CCRN-CMC CNEA 2009 1 Hemodynamics does not equal invasive monitoring Paradigm Shift 2 www.cardionursing.com 1 3 Circulation: Heart Arteries
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
Control of blood tissue blood flow. Faisal I. Mohammed, MD,PhD
 Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 25, 2013 Total POINTS: % of grade in class
 NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 25, 2013 Total POINTS: 100 20% of grade in class 1) During exercise, plasma levels of Renin increase moderately. Why should Renin levels be elevated during
NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 25, 2013 Total POINTS: 100 20% of grade in class 1) During exercise, plasma levels of Renin increase moderately. Why should Renin levels be elevated during
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co.
 Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co. Anatomy Views Label the diagrams of the heart below: Interactive Physiology Study
Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co. Anatomy Views Label the diagrams of the heart below: Interactive Physiology Study
