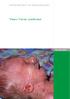
SWISS SOCIETY OF NEONATOLOGY. Fatal pulmonary embolism in a premature neonate after twin-twin transfusion syndrome
|
|
|
- Nathaniel Walters
- 6 years ago
- Views:
Transcription
1 SWISS SOCIETY OF NEONATOLOGY Fatal pulmonary embolism in a premature neonate after twin-twin transfusion syndrome February 2010
2 2 Schlapbach LJ, Riedel T, Genitsch V, Nelle M, McDougall FJ, Department of Pediatrics (LJ, RT, NM, McDFJ), Department of Pathology (GV), University of Berne, Switzerland Swiss Society of Neonatology, Thomas M Berger, Webmaster
3 3 While pulmonary embolism (PE) represents a frequent emergency in adults, PE occurs very rarely in the pedia tric age group (1). However, it is increasingly being recognized that thrombotic disease may frequently be under diagnosed (2). The incidence of thromboembolic events in children is highest during the neonatal period (3), which is characterised by a delicate equilibrium of pro- versus anticoagulant factors. Over the past years, thrombotic complications in newborns have received broader attention (4), in part thanks to improved diagnostic procedures. We present a case of a premature infant with fatal PE. INTRODUCTION A premature baby girl weighing 1400 grams was born at 29 weeks of gestation by caesarean section because of maternal chorioamnionitis. The monozygotic twin pregnancy had been complicated by twinto-twin transfusion syndrome (TTTS) with the girl presented here being the recipient. The baby was intubated for respiratory distress syndrome after birth and umbilical venous and arterial lines were placed. The umbilical artery line was immediately removed following the x-ray as the tip was malpositioned in the iliac artery. CBC on admission showed borderline polycythemia (hemoglobin 202 g/l, hematocrit 58%) and a normal platelet count (320x109/l). After receiving porcine surfactant (Curosurf ) for radiologically evident hyaline membrane disease, the infant was extubated and did well on room air without additional respiratory assistance. The umbilical venous catheter CASE REPORT
4 4 was removed on day three, and peripheral catheters on day nine when full enteral feeds were reached. At 10 days of age, the baby started requiring supplemental oxygen (25-30%). Radiologially, patchy pulmonary markings were noted and interpreted as early manifestation of bronchopulmonary dysplasia (Fig. 1). Therefore, diuretic therapy with spironolactone and hydrochlorothiazide was initiated with no clear improvement. Arterial blood pressure and electrolytes, including calcium, were always within normal range. On day 14 of life, directly following capillary heel stick blood sampling, the ipsilateral leg became pale and cooler with no peripheral pulses palpable. The baby was otherwise well, and showed no other signs of compromised perfusion. Within an hour, the perfusion of the right leg normalized spontaneously. Duplex sonography of the abdominal, pelvic and lower extremity vessels excluded arterial or venous thromboses, including renal vein thrombosis. In order to rule out a cardiac origin of a possible thromboembolic event, echocardiography was performed. There was no evidence of congenital heart disease, pulmonary hypertension or thrombotic disease. Given the spontaneous rapid resolution and the normal radiographic findings, arterial vasospasm triggered by the painful stimulus was diagnosed.
5 5 Fig. 1 Chest x-ray on day 10 showing increased pulmonary markings.
6 6 On day 20 of life, while lying comfortably in bed, the baby became acutely cyanotic with oxygen saturations around 60%, and manifested respiratory distress with tachypnea and subcostal retractions. Blood pressure was 42/22 mmhg (mean 30 mmhg) with a heart rate of 184 bpm. There was no improvement in oxygenation with 100% oxygen. She was intubated and mechanically ventilated. Emergency thoracocentesis of both pleural spaces ruled out a tension pneumothorax. Dopamine was started to treat arterial hypotension. On the CXR, diminished pulmonary vasculature was noted. Echocardiography showed suprasystemic pulmonary arterial pressure with severe tricuspid regurgitation, a flattened interventricular septum, right-sided ventricular dilatation with almost no flow across the pulmonary arteries, and right-to-left shunting across the foramen ovale. There was severe lactic acidosis (ph 6.8, lactate 14.8 mmol/l). In spite of maximal intensive care support with catecholamines, high-frequency oscillatory ventilation and inhaled nitric oxide, the baby further deteriorated and died approximately 2 hours after the onset of the sudden event. At autopsy, large emboli were found extending into both pulmonary arteries (Fig. 2). The right lower lobe showed a large area of infarction (Fig. 3). Microscopic examination revealed several peripheral pulmonary artery emboli (Fig. 4) and several extensively calcified renal vein thromboses (RVT) (Fig. 5). Due to the high degree of calcification and signs of beginning thrombus
7 7 organi sation, the age of the RVT was estimated to be >1 week, in contrast to the more recent, smaller pulmonary artery emboli estimated to be aged several days. A renal origin of the PEs was thought probable. Family history revealed that the maternal grandfather had experienced PE at the age of 78 years. Exten sive thrombophilia screening was performed with DNA of the deceased baby, her surviving monozygotic twin sister and the parents. Coagulation studies including Protein C and S levels, antithrombin III, homocystein concentration, and antiphospholipid antibodies were negative. Genetic screening for factor V Leiden (R506Q) and prothrombin mutation (20210G>A) and methylene-tetrahydrafolate reductase variant (C677T) was negative. Apart from intubation and ventilation for hyaline membrane disease, the surviving twin (birth weight 1245 gram, hemoglobin 112 g/l, hematocrit 33% on admission), had an uneventful course. Echocardiography and abdominal Doppler studies were normal.
8 8 Fig. 2 Post-mortem specimen of the right lung with opened main pulmonary artery showing a large embolus (arrow).
9 9 Fig. 3 Post-mortem specimen showing bilateral pulmonary emboli (arrowhead) and infarction in the right lower lobe (asterisk).
10 10 Fig. 4 Post-mortem histology of the pulmonary vascular bed showing a pulmonary embolus (A: artery, B: bronchus).
11 11 Fig. 5 Post-mortem histology of the kidney showing a calcified renal vein thrombosis (V: vein with thrombus, A: artery).
12 12 DISCUSSION To the best of our knowledge, this is the first case report on a fatal PE in a premature infant. In the absence of inherited thrombophilia and disseminated intravascular coagulation, the extensive renal and pulmonary thromboses were thought to have arisen either in relation to the umbilical venous catheter or as an indirect consequence of TTTS. We assume that the combination of polycythemia, prematurity and other triggers such as diminished intravascular volume due to diuretics, may have further propagated the fatal thrombotic event. Recipient twins may be at particular risk due to chronic hyperviscosity associated with polycythemia and thrombocytosis (5). TTTS was shown to be an inde pendent risk factor in a study on neonatal ischemic stroke (6). In contrast to adults where PE represents a frequent cardiovascular emergency, the condition is exceedingly rare in children. A prospective Dutch registry in children aged 0 to 18 years has reported an incidence of 0.14 per children (1). However, the true incidence of PE in the pediatric population is probably underestimated. In neonates, several case reports on PE have been published (7-11) usually describing term infants with persistent pulmonary hypertension of the newborn or severe respiratory failure. Presentation of PE may range from mild respiratory distress to severe pulmonary hypertension and acute right-sided heart failure leading to severe hypoxemia and death (12). Diagnosis of PE in infants is difficult, since experience
13 13 with ventilation-perfusion lung scanning and spiral computed tomography is limited in this age group, while pulmonary angiography is invasive (11). Consequently, most cases are diagnosed either by echocardiography or during the post-mortem examination (10, 13). Smaller PEs may frequently be missed or misinterpreted as respiratory diseases such as pneumonia or pulmonary edema. In our case, moderate hypoxemia probably caused by smaller PEs was mistaken as an early sign of bronchopulmonary dysplasia. RVT is the most common non-catheter related thrombosis in neonates, occurring in 0.5/1000 neonatal inten sive care unit admissions and accounting for 20% of neonatal thrombotic events (2, 3). Classic symptoms are hematuria, palpable abdominal mass, thrombocytopenia and frequently arterial hypertension, but only a minority of patients present with the complete triad (4). The recent review by Lau et al. confirmed that RVT occurs frequently in the absence of prothrombotic risk factors (4). Doppler ultrasound studies of the renal vessels is considered gold standard for diagnosis of RVT and advances in radiologic technique have improved diagnostic accuracy over recent years. Within the pediatric population, neonates are at the greatest risk for venous thromboembolism (5.1/ live births per year), with a second peak in incidence during puberty and adolescence (14). The risk
14 14 factors differ between neonates and older children, with sepsis or necrotising enterocolitis, dehydration or hypovolemia, maternal diabetes, asphyxia, congenital heart disease and central venous catheters being the most frequent clinical risk factors in neonates (2). Although vitamin-k-dependent procoagulant clotting factors are decreased in neonates, particularly if born preterm, coagulation inhibitor concentrations are signi ficantly lower compared to adults as well (3). In addition, levels and activity of both pro- and anticoagulant factors undergo significant changes during the neonatal period. This delicate and dynamic equilibrium between coagulation and fibrinolysis is easily disturbed by perinatal or iatrogenic factors. In the presented case, no inherited cause of thrombophlia was found. A recent meta-analysis by Young et al. showed that in herited deficiencies of the natural anticoagulants protein C, protein S, and antithrombin are present in less than 10% of pediatric patients with venous thromboembolism (14). In conclusion, the present case illustrates that both renal and smaller pulmonary thromboses may progress asymptomatically. The incidence of PE and of RVT may therefore be underestimated. Considering the potentially lethal course of PE, pediatricians and neonatologists should maintain a high degree of suspicion for thrombotic events in infants with sudden deterioration of oxygenation, acute signs of respiratory distress or unexplained pulmonary hypertension.
15 15 The authors thank Manuela Albisetti, MD, Department of Hematology, University Children s Hospital Zurich, Switzerland, for her critical comments and review of the manuscript. ACKNOW- LEDGEMENT
16 16 REFERENCES 1. Van Ommen CH, Peters M. Acute pulmonary embolism in childhood. Thromb Res 2006;118: Saracco P, Parodi E, Fabris C, et al. Management and investigation of neonatal thromboembolic events: genetic and acquired risk factors. Thromb Res 2009;123: Thornburg C, Pipe S. Neonatal thromboembolic emergencies. Semin Fetal Neonatal Med 2006;11: Lau KK, Stoffman JM, Williams S, et al. Neonatal renal vein thrombosis: review of the English-language literature between 1992 and Pediatrics 2007;120:e Lopriore E, Oepkes D. Fetal and neonatal haematological complications in monochorionic twins. Semin Fetal Neonatal Med 2008;13: Benders MJ, Groenendaal F, Uiterwaal CS, et al. Maternal and infant characteristics associated with perinatal arterial stroke in the preterm infant. Stroke 2007;38: De Blanche LE, Schmitz ML, Johnson CE, et al. Successful surgical management of a neonate with a saddle pulmonary embolus. Ann Thorac Surg 2004;78:e Goble MM, Gomez CA. Neonatal pulmonary artery thrombosis: echocardiographic characteristics and possible contributing factors. J Am Soc Echocardiography 2005;18: Kenny D, Tsai-Goodman B. Neonatal arterial thrombus mimicking congenital heart disease. Arch Dis Child Fetal Neonatal Ed 2007;92:F Allred L, Ruiz R, Jones D, et al. Intractable respiratory failure in a term newborn. Am J Perinatol 2008;25: Sawyer T, Antle A, Studer M, et al. Neonatal pulmonary artery thrombosis presenting as persistent pulmonary hypertension of the newborn. Pediatr Cardiol 2009;30:
17 Biss TT, Brandao LR, Kahr WH, et al. Clinical features and outcome of pulmonary embolism in children. Br J Haematol 2008;142: Champ C, Byard R. W. Pulmonary thromboembolism and unexpected death in infancy. J Paediatr Child Health 1994;30: Young G, Albisetti M, Bonduel M, et al. Impact of inherited thrombophilia on venous thromboembolism in children: a systematic review and meta-analysis of observational studies. Circulation 2008;118:
18 concept & design by mesch.ch SUPPORTED BY CONTACT Swiss Society of Neonatology
SWISS SOCIETY OF NEONATOLOGY. Neonatal cerebral infarction
 SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
SWISS SOCIETY OF NEONATOLOGY. Local fibrinolysis with r-tpa in a newborn with brachial artery thrombosis
 SWISS SOCIETY OF NEONATOLOGY Local fibrinolysis with r-tpa in a newborn with brachial artery thrombosis January 2001 2 Dyroff C, Berger TM, Treumann T, Neonatal and Pediatric Intensive Care Unit (DC, BTM),
SWISS SOCIETY OF NEONATOLOGY Local fibrinolysis with r-tpa in a newborn with brachial artery thrombosis January 2001 2 Dyroff C, Berger TM, Treumann T, Neonatal and Pediatric Intensive Care Unit (DC, BTM),
SWISS SOCIETY OF NEONATOLOGY. Congenital ductus arteriosus aneurysm: serious or common?
 SWISS SOCIETY OF NEONATOLOGY Congenital ductus arteriosus aneurysm: serious or common? AUGUST 2011 * 2 Beauport L, Meijboom E, Vial Y, Gudinchet F, Truttmann AC, CHUV, Lausanne, Neonatology Unit (BL, TAC),
SWISS SOCIETY OF NEONATOLOGY Congenital ductus arteriosus aneurysm: serious or common? AUGUST 2011 * 2 Beauport L, Meijboom E, Vial Y, Gudinchet F, Truttmann AC, CHUV, Lausanne, Neonatology Unit (BL, TAC),
SWISS SOCIETY OF NEONATOLOGY. Classical presentation of a newborn infant with renal vein thrombosis
 SWISS SOCIETY OF NEONATOLOGY Classical presentation of a newborn infant with renal vein thrombosis December 2017 Wendelspiess M, Schifferli A, Rudin C, Kaempfen S, Department of Neonatology (WM, KS), Department
SWISS SOCIETY OF NEONATOLOGY Classical presentation of a newborn infant with renal vein thrombosis December 2017 Wendelspiess M, Schifferli A, Rudin C, Kaempfen S, Department of Neonatology (WM, KS), Department
SWISS SOCIETY OF NEONATOLOGY. Vein of Galen aneurysm: Aneurysmal characteristics and clinical features as predictive factors
 SWISS SOCIETY OF NEONATOLOGY Vein of Galen aneurysm: Aneurysmal characteristics and clinical features as predictive factors April 2010 2 Pronzini F, Fontijn J, Fauchère JC, Bucher HU, Clinic of Neonatology,
SWISS SOCIETY OF NEONATOLOGY Vein of Galen aneurysm: Aneurysmal characteristics and clinical features as predictive factors April 2010 2 Pronzini F, Fontijn J, Fauchère JC, Bucher HU, Clinic of Neonatology,
SWISS SOCIETY OF NEONATOLOGY. Prolonged arterial hypotension due to propofol used for endotracheal intubation in a newborn infant
 SWISS SOCIETY OF NEONATOLOGY Prolonged arterial hypotension due to propofol used for endotracheal intubation in a newborn infant July 2001 2 Wagner B, Intensive Care Unit, University Children s Hospital
SWISS SOCIETY OF NEONATOLOGY Prolonged arterial hypotension due to propofol used for endotracheal intubation in a newborn infant July 2001 2 Wagner B, Intensive Care Unit, University Children s Hospital
SWISS SOCIETY OF NEONATOLOGY. Potentially fatal complications of peripherally inserted central venous catheters (PICCs)
 SWISS SOCIETY OF NEONATOLOGY Potentially fatal complications of peripherally inserted central venous catheters (PICCs) October 2001 2 Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital
SWISS SOCIETY OF NEONATOLOGY Potentially fatal complications of peripherally inserted central venous catheters (PICCs) October 2001 2 Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants?
 Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
SWISS SOCIETY OF NEONATOLOGY. Selective bronchial intubation for unilateral PIE
 SWISS SOCIETY OF NEONATOLOGY Selective bronchial intubation for unilateral PIE October 2000 2 Berger TM, Jöhr M, Neonatal and Pediatric Intensive Care Unit (BTM), Kinderspital Luzern, Department of Anesthesiology
SWISS SOCIETY OF NEONATOLOGY Selective bronchial intubation for unilateral PIE October 2000 2 Berger TM, Jöhr M, Neonatal and Pediatric Intensive Care Unit (BTM), Kinderspital Luzern, Department of Anesthesiology
Cor pulmonale. Dr hamid reza javadi
 1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
SWISS SOCIETY OF NEONATOLOGY. Supercarbia in an infant with meconium aspiration syndrome
 SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
VTE in Children: Practical Issues
 VTE in Children: Practical Issues Wasil Jastaniah MBBS,FAAP,FRCPC Consultant Pediatric Hem/Onc/BMT May 2012 Top 10 Reasons Why Pediatric VTE is Different 1. Social, ethical, and legal implications. 2.
VTE in Children: Practical Issues Wasil Jastaniah MBBS,FAAP,FRCPC Consultant Pediatric Hem/Onc/BMT May 2012 Top 10 Reasons Why Pediatric VTE is Different 1. Social, ethical, and legal implications. 2.
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY. Catastrophic gastrointestinal event in a 10-week-old extremely growth restricted preterm infant
 SWISS SOCIETY OF NEONATOLOGY Catastrophic gastrointestinal event in a 10-week-old extremely growth restricted preterm infant APRIL 2011 2 Häberli So, Hausladen Si, Hürlimann Sa, Caduff JH, Esslinger P,
SWISS SOCIETY OF NEONATOLOGY Catastrophic gastrointestinal event in a 10-week-old extremely growth restricted preterm infant APRIL 2011 2 Häberli So, Hausladen Si, Hürlimann Sa, Caduff JH, Esslinger P,
SWISS SOCIETY OF NEONATOLOGY. Prenatal closure of the ductus arteriosus
 SWISS SOCIETY OF NEONATOLOGY Prenatal closure of the ductus arteriosus March 2007 Leone A, Fasnacht M, Beinder E, Arlettaz R, Neonatal Intensive Care Unit (LA, AR), University Hospital Zurich, Cardiology
SWISS SOCIETY OF NEONATOLOGY Prenatal closure of the ductus arteriosus March 2007 Leone A, Fasnacht M, Beinder E, Arlettaz R, Neonatal Intensive Care Unit (LA, AR), University Hospital Zurich, Cardiology
Risk factors for DVT. Venous thrombosis & pulmonary embolism. Anticoagulation (cont d) Diagnosis 1/5/2018. Ahmed Mahmoud, MD
 Risk factors for DVT Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
Risk factors for DVT Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
Venous thrombosis & pulmonary embolism. Ahmed Mahmoud, MD
 Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Risk factors for DVT Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Risk factors for DVT Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
SWISS SOCIETY OF NEONATOLOGY. Preterm infant with. pulmonary hypertension and hypopituitarism
 SWISS SOCIETY OF NEONATOLOGY Preterm infant with pulmonary hypertension and hypopituitarism November 2007 2 Pilgrim S, Stocker M, Neonatal and Pediatric Intensiv Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY Preterm infant with pulmonary hypertension and hypopituitarism November 2007 2 Pilgrim S, Stocker M, Neonatal and Pediatric Intensiv Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY. Spontaneous intestinal perforation or necrotizing enterocolitis?
 SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY. Delayed-onset right-sided congenital diaphragmatic hernia and group B streptococcal septicemia
 SWISS SOCIETY OF NEONATOLOGY Delayed-onset right-sided congenital diaphragmatic hernia and group B streptococcal septicemia September 2003 2 Saner C, Burtscher R, Hunziker U, Zimmermann-Bär U, Department
SWISS SOCIETY OF NEONATOLOGY Delayed-onset right-sided congenital diaphragmatic hernia and group B streptococcal septicemia September 2003 2 Saner C, Burtscher R, Hunziker U, Zimmermann-Bär U, Department
SWISS SOCIETY OF NEONATOLOGY. Neonatal gastric perforation
 SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
SWISS SOCIETY OF NEONATOLOGY. Pulmonary complications of congenital listeriosis in a preterm infant
 SWISS SOCIETY OF NEONATOLOGY Pulmonary complications of congenital listeriosis in a preterm infant April 2009 2 Mészàros A, el Helou S, Zimmermann U, Berger TM, Neonatal and Pediatric Intensive Care Unit
SWISS SOCIETY OF NEONATOLOGY Pulmonary complications of congenital listeriosis in a preterm infant April 2009 2 Mészàros A, el Helou S, Zimmermann U, Berger TM, Neonatal and Pediatric Intensive Care Unit
THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO
 THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO DISCLAIMER I m a pediatrician I will be discussing this issue primarily from a pediatric perspective
THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO DISCLAIMER I m a pediatrician I will be discussing this issue primarily from a pediatric perspective
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine
 Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
A 50-year-old woman with syncope
 Hira Shahzad 1, Ali Bin Sarwar Zubairi 2 1 Medical College, Aga Khan University Hospital, Karachi 2 Department of Medicine, Aga Khan University Hospital, Karachi, Pakistan Ali Bin Sarwar Zubairi Associate
Hira Shahzad 1, Ali Bin Sarwar Zubairi 2 1 Medical College, Aga Khan University Hospital, Karachi 2 Department of Medicine, Aga Khan University Hospital, Karachi, Pakistan Ali Bin Sarwar Zubairi Associate
Shock, Hemorrhage and Thrombosis
 Shock, Hemorrhage and Thrombosis 1 Shock Systemic hypoperfusion due to: Reduction in cardiac output Reduction in effective circulating blood volume Hypotension Impaired tissue perfusion Cellular hypoxia
Shock, Hemorrhage and Thrombosis 1 Shock Systemic hypoperfusion due to: Reduction in cardiac output Reduction in effective circulating blood volume Hypotension Impaired tissue perfusion Cellular hypoxia
SWISS SOCIETY OF NEONATOLOGY. Peripartal management of a prenatally diagnosed large oral cyst
 SWISS SOCIETY OF NEONATOLOGY Peripartal management of a prenatally diagnosed large oral cyst May 2007 2 Fontana M, Berger TM, Winiker H, Jöhr M, Nagel H, Neonatal and Pediatric Intensive Care Unit (FM,
SWISS SOCIETY OF NEONATOLOGY Peripartal management of a prenatally diagnosed large oral cyst May 2007 2 Fontana M, Berger TM, Winiker H, Jöhr M, Nagel H, Neonatal and Pediatric Intensive Care Unit (FM,
Epidermiology Early pulmonary embolism
 Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
SWISS SOCIETY OF NEONATOLOGY. Prenatal diagnosis and postnatal management of meconium pseudocysts
 SWISS SOCIETY OF NEONATOLOGY Prenatal diagnosis and postnatal management of meconium pseudocysts September 2007 2 Burch E, Caduff JH, Hodel M, Berger TM, Neonatal and Pediatric Intensive Care Unit (BE,
SWISS SOCIETY OF NEONATOLOGY Prenatal diagnosis and postnatal management of meconium pseudocysts September 2007 2 Burch E, Caduff JH, Hodel M, Berger TM, Neonatal and Pediatric Intensive Care Unit (BE,
SWISS SOCIETY OF NEONATOLOGY. Cantrell s pentalogy: an unusual midline defect
 SWISS SOCIETY OF NEONATOLOGY Cantrell s pentalogy: an unusual midline defect October 2004 2 Cevey-Macherel MN, Meijboom EJ, Di Bernardo S, Truttmann AC, Division of Neonatology and Division of Pediatric
SWISS SOCIETY OF NEONATOLOGY Cantrell s pentalogy: an unusual midline defect October 2004 2 Cevey-Macherel MN, Meijboom EJ, Di Bernardo S, Truttmann AC, Division of Neonatology and Division of Pediatric
Successful Pulmonary Embolectomy of a Saddle Pulmonary Thromboembolism in a Preterm Neonate
 Successful Pulmonary Embolectomy of a Saddle Pulmonary Thromboembolism in a Preterm Neonate Kaarthigeyan Kalaniti, MBBS, MD a, Mauro Lo Rito, MD b, Edward J. Hickey, MD b,c, V. Ben Sivarajan, MD, MS c,d,e
Successful Pulmonary Embolectomy of a Saddle Pulmonary Thromboembolism in a Preterm Neonate Kaarthigeyan Kalaniti, MBBS, MD a, Mauro Lo Rito, MD b, Edward J. Hickey, MD b,c, V. Ben Sivarajan, MD, MS c,d,e
Thrombosis and emboli. Peter Nagy
 Thrombosis and emboli Peter Nagy A thrombus is any solid object developing from the blood in vivo within the vascular system or heart. Thrombosis is hemostasis in the wrong place. Major components, forms:
Thrombosis and emboli Peter Nagy A thrombus is any solid object developing from the blood in vivo within the vascular system or heart. Thrombosis is hemostasis in the wrong place. Major components, forms:
Hemodynamic Disorders, Thrombosis, and Shock. Richard A. McPherson, M.D.
 Hemodynamic Disorders, Thrombosis, and Shock Richard A. McPherson, M.D. Edema The accumulation of abnormal amounts of fluid in intercellular spaces of body cavities. Inflammation and release of mediators
Hemodynamic Disorders, Thrombosis, and Shock Richard A. McPherson, M.D. Edema The accumulation of abnormal amounts of fluid in intercellular spaces of body cavities. Inflammation and release of mediators
PE and DVT. Dr Anzo William Adiga WatsApp or Call Medical Officer/RHEMA MEDICAL GROUP
 PE and DVT Dr Anzo William Adiga WatsApp or Call +256777363201 Medical Officer/RHEMA MEDICAL GROUP OBJECTIVES DEFINE DVT AND P.E PATHOPHYSIOLOGY OF DVT CLINICAL PRESENTATION OF DVT/PE INVESTIGATE DVT MANAGEMENT
PE and DVT Dr Anzo William Adiga WatsApp or Call +256777363201 Medical Officer/RHEMA MEDICAL GROUP OBJECTIVES DEFINE DVT AND P.E PATHOPHYSIOLOGY OF DVT CLINICAL PRESENTATION OF DVT/PE INVESTIGATE DVT MANAGEMENT
Screening for Critical Congenital Heart Disease
 Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Pathology of pulmonary vascular disease. Dr.Ashraf Abdelfatah Deyab. Assistant Professor of Pathology Faculty of Medicine Almajma ah University
 Pathology of pulmonary vascular disease Dr.Ashraf Abdelfatah Deyab Assistant Professor of Pathology Faculty of Medicine Almajma ah University Pulmonary vascular disease Type of pulmonary circulation: Types
Pathology of pulmonary vascular disease Dr.Ashraf Abdelfatah Deyab Assistant Professor of Pathology Faculty of Medicine Almajma ah University Pulmonary vascular disease Type of pulmonary circulation: Types
4. Which survey program does your facility use to get your program designated by the state?
 TRAUMA SURVEY Please complete one survey for each TCD designation you have in your facility. There would be a maximum of three surveys completed if your facility was designated as a trauma, stroke and
TRAUMA SURVEY Please complete one survey for each TCD designation you have in your facility. There would be a maximum of three surveys completed if your facility was designated as a trauma, stroke and
CARDIAC PROBLEMS IN PREGNANCY
 CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
How long to continue anticoagulation after DVT?
 How long to continue anticoagulation after DVT? Dr. Nihar Ranjan Pradhan M.S., DNB (Vascular Surgery), FVES(UK) Consultant Vascular Surgeon Apollo Hospital, Jubilee Hills, Hyderabad (Formerly Faculty in
How long to continue anticoagulation after DVT? Dr. Nihar Ranjan Pradhan M.S., DNB (Vascular Surgery), FVES(UK) Consultant Vascular Surgeon Apollo Hospital, Jubilee Hills, Hyderabad (Formerly Faculty in
A Study of Prevalence and Risk Factors of Polycythemia in Neonatal Nursery in Duhok
 ORIGINAL ARTICLE A Study of Prevalence and Risk Factors of Polycythemia in Neonatal Nursery in Duhok Akrem Mohammad Mostefa 1 ABSTRACT OBJECTIVE: To find the prevalence of neonatal polycythemia among neonates
ORIGINAL ARTICLE A Study of Prevalence and Risk Factors of Polycythemia in Neonatal Nursery in Duhok Akrem Mohammad Mostefa 1 ABSTRACT OBJECTIVE: To find the prevalence of neonatal polycythemia among neonates
October 2017 Pulmonary Embolism
 October 2017 Pulmonary Embolism Prof. Ahmed BaHammam, FRCP, FCCP Professor of Medicine College of Medicine King Saud University 1 Objectives Epidemiology Pathophysiology Diagnosis Massive PE Treatment
October 2017 Pulmonary Embolism Prof. Ahmed BaHammam, FRCP, FCCP Professor of Medicine College of Medicine King Saud University 1 Objectives Epidemiology Pathophysiology Diagnosis Massive PE Treatment
Are there still any valid indications for thrombophilia screening in DVT?
 Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
SWISS SOCIETY OF NEONATOLOGY. Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions
 SWISS SOCIETY OF NEONATOLOGY Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions July 2013 2 Anderson S, Rimensberger P, Service de Néonatologie et des Soins
SWISS SOCIETY OF NEONATOLOGY Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions July 2013 2 Anderson S, Rimensberger P, Service de Néonatologie et des Soins
Congenital heart disease in twin-to-twin transfusion syndrome treated with fetoscopic laser surgery
 Chapter 10 Congenital heart disease in twin-to-twin transfusion syndrome treated with fetoscopic laser surgery Enrico Lopriore MD Regina Bökenkamp MD Marry Rijlaarsdam MD Marieke Sueters MD Frank PHA Vandenbussche
Chapter 10 Congenital heart disease in twin-to-twin transfusion syndrome treated with fetoscopic laser surgery Enrico Lopriore MD Regina Bökenkamp MD Marry Rijlaarsdam MD Marieke Sueters MD Frank PHA Vandenbussche
Maternal and Fetal Physiology
 Background Maternal and Fetal Physiology Anderson Lo, DO Fellow, Maternal-Fetal Medicine Wayne State University School of Medicine SEMCME Fetal Assessment Course July 20, 2018 Oxygen pathway Mother Placenta
Background Maternal and Fetal Physiology Anderson Lo, DO Fellow, Maternal-Fetal Medicine Wayne State University School of Medicine SEMCME Fetal Assessment Course July 20, 2018 Oxygen pathway Mother Placenta
HEMODYNAMIC DISORDERS
 HEMODYNAMIC DISORDERS Normal fluid homeostasis requires vessel wall integrity as well as maintenance of intravascular pressure and osmolarity within certain physiologic ranges. Increases in vascular volume
HEMODYNAMIC DISORDERS Normal fluid homeostasis requires vessel wall integrity as well as maintenance of intravascular pressure and osmolarity within certain physiologic ranges. Increases in vascular volume
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Thrombophilia. Diagnosis and Management. Kevin P. Hubbard, DO, FACOI
 Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
How to Recognize a Suspected Cardiac Defect in the Neonate
 Neonatal Nursing Education Brief: How to Recognize a Suspected Cardiac Defect in the Neonate https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Neonatal Nursing Education Brief: How to Recognize a Suspected Cardiac Defect in the Neonate https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Mabel Labrada, MD Miami VA Medical Center
 Mabel Labrada, MD Miami VA Medical Center *1-Treatment for acute DVT with underlying malignancy is for 3 months. *2-Treatment of provoked acute proximal DVT can be stopped after 3months of treatment and
Mabel Labrada, MD Miami VA Medical Center *1-Treatment for acute DVT with underlying malignancy is for 3 months. *2-Treatment of provoked acute proximal DVT can be stopped after 3months of treatment and
The Blue Baby. Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin
 The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
SWISS SOCIETY OF NEONATOLOGY. Hypertrophic pyloric stenosis in a preterm infant
 SWISS SOCIETY OF NEONATOLOGY Hypertrophic pyloric stenosis in a preterm infant February 2014 2 Georgi R, Berger M, Schnyder I, Berger S, McDougall J, Division of Neonatology (GR, BM, McDJ), Department
SWISS SOCIETY OF NEONATOLOGY Hypertrophic pyloric stenosis in a preterm infant February 2014 2 Georgi R, Berger M, Schnyder I, Berger S, McDougall J, Division of Neonatology (GR, BM, McDJ), Department
Radiologic Features of The Pulmonary Embolus
 January 2003 Radiologic Features of The Pulmonary Embolus Travis McGlothin HMSIII Mr. J is a 51 y.o. male who presented to the BIDMC ED w/ acute onset of: Lft. Hemiparesis slurred speech mild dyspnea mild
January 2003 Radiologic Features of The Pulmonary Embolus Travis McGlothin HMSIII Mr. J is a 51 y.o. male who presented to the BIDMC ED w/ acute onset of: Lft. Hemiparesis slurred speech mild dyspnea mild
Lung diseases of Vascular Origin. By: Shefaa Qa qqa
 Lung diseases of Vascular Origin By: Shefaa Qa qqa Pulmonary Hypertension Pulmonary hypertension is defined as a mean pulmonary artery pressure greater than or equal to 25 mm Hg at rest. Based on underlying
Lung diseases of Vascular Origin By: Shefaa Qa qqa Pulmonary Hypertension Pulmonary hypertension is defined as a mean pulmonary artery pressure greater than or equal to 25 mm Hg at rest. Based on underlying
Pulmonary Embolism. Pulmonary Embolism. Pulmonary Embolism. PE - Clinical
 Pulmonary embolus - a practical approach to investigation and treatment Sam Janes Wellcome Senior Fellow and Respiratory Physician, University College London Background Diagnosis Treatment Common: 50 cases
Pulmonary embolus - a practical approach to investigation and treatment Sam Janes Wellcome Senior Fellow and Respiratory Physician, University College London Background Diagnosis Treatment Common: 50 cases
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
Physiologic Based Management of Circulatory Shock Kuwait 2018
 Physiologic Based Management of Circulatory Shock Kuwait 2018 Dr. Yasser Elsayed, MD, PhD Director of the Targeted Neonatal Echocardiography, Point of Care and Hemodynamics Program Staff Neonatologist
Physiologic Based Management of Circulatory Shock Kuwait 2018 Dr. Yasser Elsayed, MD, PhD Director of the Targeted Neonatal Echocardiography, Point of Care and Hemodynamics Program Staff Neonatologist
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM. Gordon Lowe Professor of Vascular Medicine University of Glasgow
 CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General
![OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General](/thumbs/85/91909911.jpg) OB Well Baby Nursery Admission (Term) [3040000234] For specialty focused order sets for your patient, refer to: 3040000424 Neonatal Circumcision Order Set 3040000522 Neonatal Herpes Viral Order Set 3040000524
OB Well Baby Nursery Admission (Term) [3040000234] For specialty focused order sets for your patient, refer to: 3040000424 Neonatal Circumcision Order Set 3040000522 Neonatal Herpes Viral Order Set 3040000524
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions
 Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS Pediatric Cardiology
 Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영
 When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
Venous thrombosis is common and often occurs spontaneously, but it also frequently accompanies medical and surgical conditions, both in the community
 Venous Thrombosis Venous Thrombosis It occurs mainly in the deep veins of the leg (deep vein thrombosis, DVT), from which parts of the clot frequently embolize to the lungs (pulmonary embolism, PE). Fewer
Venous Thrombosis Venous Thrombosis It occurs mainly in the deep veins of the leg (deep vein thrombosis, DVT), from which parts of the clot frequently embolize to the lungs (pulmonary embolism, PE). Fewer
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 16 December 1999 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 16 December 1999 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
SWISS SOCIETY OF NEONATOLOGY. Neonatal sinovenous thrombosis
 SWISS SOCIETY OF NEONATOLOGY Neonatal sinovenous thrombosis August 2006 2 Hauri-Hohl A, Zeilinger G, Pasquier S, Children s Hospital of Aarau, Switzerland Swiss Society of Neonatology, Thomas M Berger,
SWISS SOCIETY OF NEONATOLOGY Neonatal sinovenous thrombosis August 2006 2 Hauri-Hohl A, Zeilinger G, Pasquier S, Children s Hospital of Aarau, Switzerland Swiss Society of Neonatology, Thomas M Berger,
PULMONARY VENOLOBAR SYNDROME. Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital.
 PULMONARY VENOLOBAR SYNDROME Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital. Presenting complaint: 10 yrs old girl with recurrent episodes of lower respiratory tract infection from infancy.
PULMONARY VENOLOBAR SYNDROME Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital. Presenting complaint: 10 yrs old girl with recurrent episodes of lower respiratory tract infection from infancy.
Valutazione del neonato con sospetta ipertensione polmonare
 Valutazione del neonato con sospetta ipertensione polmonare Cardiologia Pediatrica Seconda Università degli Studi di Napoli A.O. R.N. dei Colli-Monaldi Napoli Hypoxiemic infant Full or near-term neonate
Valutazione del neonato con sospetta ipertensione polmonare Cardiologia Pediatrica Seconda Università degli Studi di Napoli A.O. R.N. dei Colli-Monaldi Napoli Hypoxiemic infant Full or near-term neonate
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I. December 5, 2012
 SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
Pediatric Learning Solutions course alignment with the Neonatal/Pediatric Specialty Examination Detailed Content Outline.
 Pediatric Learning Solutions course alignment with the Neonatal/Pediatric Specialty Examination Detailed Content Outline. The following Pediatric Learning Solutions courses align to focus areas of the
Pediatric Learning Solutions course alignment with the Neonatal/Pediatric Specialty Examination Detailed Content Outline. The following Pediatric Learning Solutions courses align to focus areas of the
Late pulmonary hypertension in preterm infants How to sort things out? V.Gournay, FCPC, La Martinique, Nov 23,2015
 Late pulmonary hypertension in preterm infants How to sort things out? V.Gournay, FCPC, La Martinique, Nov 23,2015 Epidemiology Incidence of extreme prematurity (
Late pulmonary hypertension in preterm infants How to sort things out? V.Gournay, FCPC, La Martinique, Nov 23,2015 Epidemiology Incidence of extreme prematurity (
Pathophysiology. Tutorial 3 Hemodynamic Disorders
 Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Radiation Exposure in Pregnancy. John R. Mayo UNIVERSITY OF BRITISH COLUMBIA
 Radiation Exposure in Pregnancy John R. Mayo UNIVERSITY OF BRITISH COLUMBIA Illustrative Clinical Scenario 32 year old female 34 weeks pregnant with recent onset shortness of breath and central chest pain
Radiation Exposure in Pregnancy John R. Mayo UNIVERSITY OF BRITISH COLUMBIA Illustrative Clinical Scenario 32 year old female 34 weeks pregnant with recent onset shortness of breath and central chest pain
CongHeartDis.doc. Андрій Миколайович Лобода
 CongHeartDis.doc Андрій Миколайович Лобода 2015 Зміст 3 Зміст Зміст 4 A child with tetralogy of Fallot is most likely to exhibit: -Increased pulmonary blood flow -Increased pressure in the right ventricle
CongHeartDis.doc Андрій Миколайович Лобода 2015 Зміст 3 Зміст Зміст 4 A child with tetralogy of Fallot is most likely to exhibit: -Increased pulmonary blood flow -Increased pressure in the right ventricle
Disturbance of Circulation Hemodynamic Disorder
 Disturbance of Circulation Hemodynamic Disorder 2/17/2017 By Dr. Hemn Hassan Othman PhD, Pathology Fall 2016 1 Thrombosis Definition: Thrombosis is the formation of solid or semisolid blood clot within
Disturbance of Circulation Hemodynamic Disorder 2/17/2017 By Dr. Hemn Hassan Othman PhD, Pathology Fall 2016 1 Thrombosis Definition: Thrombosis is the formation of solid or semisolid blood clot within
CLINICAL CASE PRESENTATION
 European Winter School of Internal Medicine 2015 Riga, Latvia, 26-30 January CLINICAL CASE PRESENTATION Vasiliy Chulkov South Ural State Medical University (Chelyabinsk, Russia) CHELYABINSK CLINICAL HISTORY
European Winter School of Internal Medicine 2015 Riga, Latvia, 26-30 January CLINICAL CASE PRESENTATION Vasiliy Chulkov South Ural State Medical University (Chelyabinsk, Russia) CHELYABINSK CLINICAL HISTORY
Jessica Bryan, Natalia Evans, Karlyn Henderson, & Whitney Parks
 Jessica Bryan, Natalia Evans, Karlyn Henderson, & Whitney Parks 1. What is the most common cause of death in hospitalized patients? 1. Hospital-acquired infection 2. Pulmonary embolism 3. Myocardial infarction
Jessica Bryan, Natalia Evans, Karlyn Henderson, & Whitney Parks 1. What is the most common cause of death in hospitalized patients? 1. Hospital-acquired infection 2. Pulmonary embolism 3. Myocardial infarction
Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism
 Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Lectures 4 Early fetal assessment, screening, ultrasound and treatment modalities during pregnancy. II. Asphyxia and Resuscitation (3 lectures)...
 Outline of a 2 year Neonatology educational course (80 lectures) PLUS 2 graduate level courses (GENETICS and BIOSTATISTICS & EPIDEMIOLOGY Approximate Percent in Examination I. Maternal-Fetal Medicine (6
Outline of a 2 year Neonatology educational course (80 lectures) PLUS 2 graduate level courses (GENETICS and BIOSTATISTICS & EPIDEMIOLOGY Approximate Percent in Examination I. Maternal-Fetal Medicine (6
SWISS SOCIETY OF NEONATOLOGY. Yunis-Varon syndrome
 SWISS SOCIETY OF NEONATOLOGY Yunis-Varon syndrome January 2003 2 Heyland K, Hodler C, Bänziger O, Neonatology, University Children s Hospital of Zurich, Switzerland Swiss Society of Neonatology, Thomas
SWISS SOCIETY OF NEONATOLOGY Yunis-Varon syndrome January 2003 2 Heyland K, Hodler C, Bänziger O, Neonatology, University Children s Hospital of Zurich, Switzerland Swiss Society of Neonatology, Thomas
Definition: HPS is a disease process with a triad of: 1- Liver disease. 2- Widespread intrapulmonary vasodilatation. 3- Gas exchange abnormality prese
 Hepatopulmonary syndrome (HPS) By Alaa Haseeb, MS.c Definition: HPS is a disease process with a triad of: 1- Liver disease. 2- Widespread intrapulmonary vasodilatation. 3- Gas exchange abnormality presenting
Hepatopulmonary syndrome (HPS) By Alaa Haseeb, MS.c Definition: HPS is a disease process with a triad of: 1- Liver disease. 2- Widespread intrapulmonary vasodilatation. 3- Gas exchange abnormality presenting
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Thrombolysis in PE. Outline. Disclosure. Overview on Pulmonary Embolism. Hot Topics in Emergency Medicine 2012 Midyear Clinical Meeting
 Disclosure Thrombolysis in PE Daniel P. Hays, PharmD, BCPS, FASHP reports no relevant financial relationships. Daniel P. Hays, PharmD, BCPS, FASHP Outline 55 YOF presents to ED with SOB PMH of DVT + noncompliance
Disclosure Thrombolysis in PE Daniel P. Hays, PharmD, BCPS, FASHP reports no relevant financial relationships. Daniel P. Hays, PharmD, BCPS, FASHP Outline 55 YOF presents to ED with SOB PMH of DVT + noncompliance
Acute Pulmonary Embolism and Deep Vein Thrombosis. Barbara LeVarge MD Beth Israel Deaconess Medical Center Pulmonary Hypertension Center COPYRIGHT
 Acute Pulmonary Embolism and Deep Vein Thrombosis Barbara LeVarge MD Beth Israel Deaconess Medical Center Pulmonary Hypertension Center Acute PE and DVT No disclosures. Acute PE and DVT Learning objectives
Acute Pulmonary Embolism and Deep Vein Thrombosis Barbara LeVarge MD Beth Israel Deaconess Medical Center Pulmonary Hypertension Center Acute PE and DVT No disclosures. Acute PE and DVT Learning objectives
NEONATAL CLINICAL PRACTICE GUIDELINE
 NEONATAL CLINICAL PRACTICE GUIDELINE Title: Brain Oxygen Monitoring in Newborns Using Near Infrared Spectroscopy (NIRS) Approval Date: Pages: June 2016 Approved by: Neonatal Patient Care Teams, HSC & SBH
NEONATAL CLINICAL PRACTICE GUIDELINE Title: Brain Oxygen Monitoring in Newborns Using Near Infrared Spectroscopy (NIRS) Approval Date: Pages: June 2016 Approved by: Neonatal Patient Care Teams, HSC & SBH
1
 1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant
 SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014
 USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014 ino for Late Preterm and Term Infants with Severe PPHN Background:
USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014 ino for Late Preterm and Term Infants with Severe PPHN Background:
How pregnancy impacts adult cyanotic congenital heart disease
 How pregnancy impacts adult cyanotic congenital heart disease Magalie Ladouceur Adult Congenital Heart Disease Unit, Hôpital Européen Georges Pompidou, Centre de reference des Malformations Cardiaques
How pregnancy impacts adult cyanotic congenital heart disease Magalie Ladouceur Adult Congenital Heart Disease Unit, Hôpital Européen Georges Pompidou, Centre de reference des Malformations Cardiaques
TACO CASE STUDIES RTC JUNE Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner
 TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
NEONATAL CLINICAL PRACTICE GUIDELINE
 NEONATAL CLINICAL PRACTICE GUIDELINE Title: Integrated Evaluation of Neonatal Hemodynamics (IENH) and Targeted Echocardiogram Approval Date: January 2015 Approved by: Neonatal Patient Care Teams, HSC &
NEONATAL CLINICAL PRACTICE GUIDELINE Title: Integrated Evaluation of Neonatal Hemodynamics (IENH) and Targeted Echocardiogram Approval Date: January 2015 Approved by: Neonatal Patient Care Teams, HSC &
Neonatal thrombosis. E A Chalmers
 J Clin Pathol 2000;53:419 423 419 Neonatal thrombosis Department of Haematology, Royal Hospital for Sick Children, Yorkhill, Glasgow G3 8SJ, UK E A Chalmers Correspondence to: Dr Chalmers e-mail: lizchalmers@btinternet.com
J Clin Pathol 2000;53:419 423 419 Neonatal thrombosis Department of Haematology, Royal Hospital for Sick Children, Yorkhill, Glasgow G3 8SJ, UK E A Chalmers Correspondence to: Dr Chalmers e-mail: lizchalmers@btinternet.com
DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients. David Liff MD Oklahoma Heart Institute Vascular Center
 DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients David Liff MD Oklahoma Heart Institute Vascular Center Overview Pathophysiology of DVT Epidemiology and risk factors for DVT in the
DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients David Liff MD Oklahoma Heart Institute Vascular Center Overview Pathophysiology of DVT Epidemiology and risk factors for DVT in the
Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study
 D-32084-2011 Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study Robert DiBlasi RRT-NPS, FAARC Respiratory Care Manager of Research & Quality
D-32084-2011 Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study Robert DiBlasi RRT-NPS, FAARC Respiratory Care Manager of Research & Quality
