Figure 2. Normal ECG tracing. Table 1.
|
|
|
- Eleanore Gardner
- 6 years ago
- Views:
Transcription
1
2 Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are embedded in the entire thickness of the myocardium and activate the entire myocardial mass from the endocardial surface to the 2 epicardial surface. Normal ECG Figure 2 depicts the normal ECG wave form. Each waveform may be simplified as below: P wave atrial depolarization PR interval time interval from beginning of P wave to beginning of QRS. QRS Ventricular depolarization (duration of ventricular muscle depolarization). ST-T segment Ventricular repolarisation. QT interval duration of ventricular depolarisation and repolarisation. T wave ventricular repolarisation. U wave Purkinje system repolarisation. RR interval suggests ventricular rate. Table 1. Indications of cardiac pacing Arrhythmia with hemodynamic compromise I n a p p r o p r i a t e s l o w r a t e w i t h hemodynamic compromise I n a p p r o p r i a t e f a s t r a t e w i t h hemodynamic compromise Reasons for arrhythmias requiring pacing Short term these might require temporary cardiac pacemaker (TCP) o Conduction pathway damage during surgery o Edema surrounding surgical site o o Electrolyte imbalances VSD/ASD patches Long term these usually require permanent cardiac pace maker (PCP) o Congenital arrhythmias o Chamber hypertrophy VOL 1 NO.2 April June
3 Types of cardiac pacing Invasive electrical pacing is used to initiate myocardial contraction when intrinsic stimulation is insufficient, the intrinsic impulses are not being conducted or the heart rate is too slow to maintain an 3 adequate cardiac output. Electrical impulses of sufficient strength are delivered to and which then stimulate the myocardium to depolarize at a 4 preselected rate. There are a number of various routes and methods available to deliver cardiac pacing (figure 3). The common goal of each approach to pacing is to contribute to hemodynamic stability and to correct symptoms of reduced cardiac output through support of the heart rate by providing safe, potentially life-saving therapy in a variety of 1 clinical situations. Temporary cardiac pacing sites Epicardial Epicardial pacing is the most commonly used pacing in post-op cardiac patients. During cardiac surgery, electrodes (epicardial wires) are attached directly to the epicardial surface of the atrium and/or the ventricle. The wires then exit through the patient's sternum where they are then connected to a pulse generator. Epicardial pacing is often used following cardiac surgery for the management of surgically 1 related bradydysrrhythmias. Transvenous (Endocardial) Transvenous leads may be balloon-tipped which will allow for floating placement in the ICU, or nonfloating pacing catheters which require fluoroscopic 1 guidance for placement. A Swan-Ganz balloontipped floating bipolar transvenous pacing wire is a commonly used example. This is advanced via a vein (usually the subclavian routed through to the superior venacava) to the endocardial surface of right atrium (RA), or most commonly, the right ventricle. The presence of pacing spikes and restoration of a fixed heart rate on the ECG will confirm placement of the wire. Transesophageal This method is used when there are no epicardial wires or when wires do not adequately pace the heart. Transcutaneous (External) External transcutaneous pacing is temporary means Figure 3. Types of cardiac pacing VOL 1 NO.2 April June
4 of pacing a patient's heart during an emergency as it 6 can be rapidly achieved. Adhesive skin pads (electrodes) are applied to the patient's chest and back, which are then connected to a defibrillator unit. A fixed rate is set and the output current is dialed up until capture is displayed on the ECG. Current between 0-10 milliampere (ma), depending upon the size of the patient and transthoracic impedence, are usually sufficient. This procedure can be painful for the patient, therefore, sedation and analgesia should always be considered. Indications for temporary cardiac pacing (TCP) Table 2. Indications of temporary cardiac pacing (TCP) Bradydysrhythmias/Heart blocks a. Second degree AV bock: Type I (occasionally) & Type II b. Bifascicular or trifascicular block c. Complete AV block d. Complete asystole Sick sinus syndrome a. Symptomatic sinus arrest b. Atrial fibrillation (fast or slow) c. Bradycardias/tachycardias d. Symptomatic sinus bradycardia Cardiovascular surgery a. Prophylactic use during cardiac surgery in patients with history of Acute Coronary Syndrome or cardiac dysrhythmias b. Treatment for heart blocks developing during or after surgery c. Cardiac output augmentation post-operatively Drugs a. Digoxin b. Amiodarone Temporary Pacing Temporary pacing of the myocardium is used for a 3 variety of emergency and elective conditions (table 2). Sinus bradycardia and AV block are common early postoperative dysrhythmias and conduction block is more common and transient after valvular surgery as a result of direct injury and increased 1 edema to the myocardium. Heart blocks following surgery are usually transient. It may be caused by ischemia, manipulation of cardiac tissue with resultant edema, perioperative myocardial 7 infarction or mechanical injury during surgery. Unipolar and Bipolar pacing 'Unipolar' and 'bipolar' pacing is not synonymous as 'single-chamber' and 'dual chamber' pacing. Terms unipolar and bipolar refers to the pacing electrodes. Unipolar pacing is usually used in permanent pacing systems. In this there is only one conducting wire and electrode, electric current returns to the pacemaker via body fluids. Bipolar pacing is the method of choice for TCP. There are two conducting wires and two electrodes. The impulse from the pulse generator passes down one electrode, then passes through cardiac tissue to cause depolarization and the circuit is then completed via second electrode, which delivers the 8 current back to generator. Demand and Asynchronous pacing Demand pacing is most commonly used type of pacing. In this, pacing is provided on demand, when the patient's own rhythm falls below the set rate. If the pacemaker is sensing inappropriately, there is potential to deliver pacing stimulus during atrial or ventricular repolarisation, which could precipitate tachycardia and fibrillation as myocardial cells are vulnerable during this period. In asynchronous pacing, pacing stimulus is provided at a set rate regardless of underlying rhythm. It is safe only if there is no to minimal electrical activity. As soon as patient's native electrical activity reemerges, demand mode must be introduced, to prevent tachyarrythmias. VOL 1 NO.2 April June
5 Pacing codes The North American and British Group (NBG) generic pace maker codes are used for easy identification of pacing modes. The table 3 shows five pacing codes, however, in clinical practice the first three letters are predominantly used. Terminology Table 3 Threshold the least amount of electrical current required to cause depolarisation of myocardium Capture the ability of the pacing box's electrical impulse to initiate a cardiac response (indicated by pacing spike followed by respective wave, P or QRS, on ECG) Sensitivity the ability of the pacemaker to sense the intrinsic (patients own) cardiac electrical activity. This prevents pacemaker from competing with the patient's own rhythm. The pacemaker should initiate a contraction if does not sense the patients own rhythm. Triggered the atrial rate can be measured (sensed) by the box and the ventricle will be paced at the same rate, even if that is higher than the rate set in the box. Position I Position II Position III Position IV Position V Chamber (s) Chamber (s) Response to Rate modulation Multisite pacing paced sensed sensing O = None O = None O = None O = None O = None A = Atrium A = Atrium T = Triggered R = rate A = Atrium modulation V = Ventricle V = Ventricle I = inhibited V = Ventricle D = Dual (A+V) D = Dual (A+V) D = Dual (T+I) D = Dual (A+V) Figure 4 a VOL 1 NO.2 April June
6 Figure 4 b Inhibition the patient can inhibit the pacing box. This means that if the patient's heart rate is faster than the box, the box should not pace the chamber. However, the box should not allow the patient's rate to go below the rate set on the box. Depending upon first three positions (Table 3?), cardiac chambers can be paced independently (Figure 4 a) or simultaneously (Figure 4 b), hence pacing modes may be described accordingly. Hemodynamic effects of TCP The common goal of all techniques of cardiac pacing is to contribute to hemodynamic stability by resuming cardiac output through support of heart rate, as cardiac output depends upon the heart rate and stroke volume. Single chamber pacing Atrial pacing (AOO or AAI) is preferable to ventricular pacing (VOO or VVI) as this maintains AV synchrony. However, for applying atrial pacing, AV nodal pathway must be intact with normal 9 functionality. Ventricular single chamber pacing can reduce cardiac output significantly as AV synchrony is absent. Dual chamber pacing Stimulation of both atria and ventricles can be accomplished by using a dual chamber pacing mode (DDD) with a set interval between atrial and ventricular stimulation (AV interval). AV interval must be set as close as possible to the normal PR interval, which is normally 140 to 200 msec. This allows optimization of cardiac filling for ventricular contraction. As, DDD pacing ensures synchrony, it is superior to VVI pacing. Capturing and sensing Capturing is the ability of an electrical impulse to initiate a cardiac response and is detected by 3 examining an ECG. It is both an electrical and mechanical event. Capture is indicated by a pacer spike followed by a corresponding P wave in atrial pacing and QRS complex in ventricular pacing or both in dual chamber pacing. When a pacing stimulus successfully generates ECG wave (P or QRS), it is said to have captured the corresponding chamber (atria or ventricles). Sensing refers to ability of the generator to detect and recognize the myocardial intrinsic activity. In demand pacing, sensing of an intrinsic QRS complex will inhibit the pacemaker from delivering an impulse so as not to interfere with patient's own electrical activity. The sensitivity is measured in millivolts (mv) and is initially set to about 2- mv. Failure to sense means pulse generator is undersensing and has not seen the heart's intrinsic beat and VOL 1 NO.2 April June
7 so continues to pace, even when not required, causing dysrhythmias such as ventricular fibrillations. This can be managed by decreasing the sensitivity threshold (making the pacer more sensitive). If pacemaker is over sensing then it may be detecting beats that are not actually occurring, from electronic devices which causes electromechanical interference. This is bad because patient will not get a pacing stimulus when one is required and will be hemodynamically compromised. In this scenario, sensitivity threshold should to be increased to block out the artifacts (thus making the pacer less sensitive). Commonly used pacing modes with their indications VOO used in emergency situation in complete heart block or severe bradycardia VVI used as backup in sudden unexpected bradycardia or in patients with identified AV conduction block in whom AV synchrony is not thought to be necessary or achievable. Atrial pacing used in patients with sinus bradycardia or sinus arrest with intact AV conduction AOO advantage of simplicity, may cause arrhythmia as asynchronous AAI advantage of adding atrial systolic contribution to cardiac output DVI (AV sequential) usual indication is AV conduction block DDD (AV universal) paces and senses the atrium and ventricle and can act in different modes depending on the underlying rhythm. Ventricular wires The two wires, for positive and negative electrodes, exiting on left side of sternum are ventricular wires. Connecting pacing wires to a bipolar pacing cable The two metal pins (positive and negative electrodes) of pacing wires (both atrial and ventricular wires separately) are plugged in the pacing cables, which are then connected to pacing box (Figure ). Figure 6 demonstrates operational instructions of TCP. Setting the pacing box Rate set according to age and physiological needs of patient Output start with 10 milli ampere (ma) and increase until the capture is gained Sensitivity start at 0. mv for atria and 2- mv for ventricles and adjust according to sensing AV sensing set AV interval to ms (pulse generator defaults to 170 ms) The intensivist should recognize the pacemaker generated cardiac rhythm and associated problems and their solutions (figure 7 a & b). Initiating TCP Epicardial wire identification During cardiac surgery, epicardial wires are pulled through the skin and secured to the external chest wall, ready to be attached to a temporary pulse generator. The patient may have only atrial wires or ventricular wires or both atrial and ventricular wires. Atrial wires The wires exiting the sternum on the right side are always atrial wires, one each for positive and negative electrode. Figure. Medtronic 388 dual chamber temporary pacemaker VOL 1 NO.2 April June
8 Figure 6. Operational instructions of Medtronic 388 dual chamber temporary pacemaker Figure 7a An ECG of a paced rhythm VOL 1 NO.2 April June
9
Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC
 Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC Pacemaker: An electric device implanted in the body to regulate the heart beat. Delivers electrical stimuli over leads with electrodes in contact
Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC Pacemaker: An electric device implanted in the body to regulate the heart beat. Delivers electrical stimuli over leads with electrodes in contact
Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO
 Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! What is a
Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! What is a
RN-BC, MS, CCRN, FAHA
 Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! 1 A. Atropine
Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! 1 A. Atropine
Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS
 Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS NBG Codes 1st Letter 2nd Letter 3rd Letter A V D Chamber(s) Paced = atrium = ventricle = dual (both atrium and ventricle) Chamber(s) Sensed A = atrium
Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS NBG Codes 1st Letter 2nd Letter 3rd Letter A V D Chamber(s) Paced = atrium = ventricle = dual (both atrium and ventricle) Chamber(s) Sensed A = atrium
Pediatric pacemakers & ICDs:
 Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I
 1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 PROFESSIONAL NURSING PRACTICE CAN ONLY ADVANCE AS MUCH AS INDIVIDUAL
1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 PROFESSIONAL NURSING PRACTICE CAN ONLY ADVANCE AS MUCH AS INDIVIDUAL
SARASOTA MEMORIAL HOSPITAL
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE PACEMAKERS AND DETERMINING PACEMAKER DATE: REVIEWED: PAGES: 10/99 11/18 1 of 7 PS1094 ISSUED FOR: Nursing RESPONSIBILITY: *Qualified RN PURPOSE: To establish
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE PACEMAKERS AND DETERMINING PACEMAKER DATE: REVIEWED: PAGES: 10/99 11/18 1 of 7 PS1094 ISSUED FOR: Nursing RESPONSIBILITY: *Qualified RN PURPOSE: To establish
Pacing Codes and Modes Concepts
 Pacing Codes and Modes Concepts Pacing codes and modes concepts Objectives Upon completion of this program the participant will be able to: State what the first four positions of the NBG code represent.
Pacing Codes and Modes Concepts Pacing codes and modes concepts Objectives Upon completion of this program the participant will be able to: State what the first four positions of the NBG code represent.
TEMPORARY PACEMAKERS HINTS ( DUAL CHAMBER 5392 PACER)
 TEMPORARY PACEMAKERS HINTS ( DUAL CHAMBER 5392 PACER) TYPES OF PACERS 2018 1 TRANSCUTANEOUS: ( VENTRICULAR pacing only) Through the skin via gel electrode pads placed on the chest and back. Disadvantage:
TEMPORARY PACEMAKERS HINTS ( DUAL CHAMBER 5392 PACER) TYPES OF PACERS 2018 1 TRANSCUTANEOUS: ( VENTRICULAR pacing only) Through the skin via gel electrode pads placed on the chest and back. Disadvantage:
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ
 ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ ΤΖΩΡΤΖ ΔΑΔΟΥΣ ΕΠΙΚΟΥΡΟΣ ΚΑΘΗΓΗΤΗΣ Α.Π.Θ. ΜΑΡΙΑ ΚΑΡΑΛΙΟΛΙΟΥ ΕΙΔΙΚΕΥΟΜΕΝΗ ΙΑΤΡΟΣ ΚΑΡΔΙΟΛΟΓΟΣ Β ΚΑΡΔΙΟΛΟΓΙΚΗ ΚΛΙΝΙΚΗ Α.Π.Θ. ΙΠΠΟΚΡΑΤΕΙΟ Γ.Ν.Θ. 5 Why a Pacemaker is Implanted
ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ ΤΖΩΡΤΖ ΔΑΔΟΥΣ ΕΠΙΚΟΥΡΟΣ ΚΑΘΗΓΗΤΗΣ Α.Π.Θ. ΜΑΡΙΑ ΚΑΡΑΛΙΟΛΙΟΥ ΕΙΔΙΚΕΥΟΜΕΝΗ ΙΑΤΡΟΣ ΚΑΡΔΙΟΛΟΓΟΣ Β ΚΑΡΔΙΟΛΟΓΙΚΗ ΚΛΙΝΙΚΗ Α.Π.Θ. ΙΠΠΟΚΡΑΤΕΙΟ Γ.Ν.Θ. 5 Why a Pacemaker is Implanted
Temporary Pacemakers
 07 Part I Anaesthesia Refresher Course 2018 University of Cape Town Dr Owen Porrill Private Practice Honorary lecturer- University of Cape Town Temporary pacemakers are usually inserted as part of the
07 Part I Anaesthesia Refresher Course 2018 University of Cape Town Dr Owen Porrill Private Practice Honorary lecturer- University of Cape Town Temporary pacemakers are usually inserted as part of the
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Review of Pacemakers and ICD Therapy: Overview and Patient Management
 Review of Pacemakers and ICD Therapy: Overview and Patient Management Pacing Systems Charles J. Love, MD FACC FAHA FHRS CCDS Professor of Medicine Director, Cardiac Rhythm Device Services OSU Division
Review of Pacemakers and ICD Therapy: Overview and Patient Management Pacing Systems Charles J. Love, MD FACC FAHA FHRS CCDS Professor of Medicine Director, Cardiac Rhythm Device Services OSU Division
MONITORING PATIENTS WITH A TEMPORARY EXTERNAL EPICARDIAL PACEMAKER PURPOSE POLICY STATEMENTS SITE APPLICABILITY PRACTICE LEVEL/COMPETENCIES
 PURPOSE Guidelines for caring for and monitoring patients with a temporary external epicardial pacemaker. Epicardial pacemaker monitoring is performed on a continuous basis by a nurse to evaluate the effectiveness
PURPOSE Guidelines for caring for and monitoring patients with a temporary external epicardial pacemaker. Epicardial pacemaker monitoring is performed on a continuous basis by a nurse to evaluate the effectiveness
The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node.
 PACEMAKER Natural pacemaker: The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node. Artificial pacemaker: It is a small, battery-operated device that helps the heart beat in
PACEMAKER Natural pacemaker: The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node. Artificial pacemaker: It is a small, battery-operated device that helps the heart beat in
Title and contents page 1 Who should read this document 2 Scope of the Guideline 2 Background 2 What is new in this version 2
 Temporary Transvenous Pacing Guideline Classification: Clinical Guideline Lead Author: Dr Peter Woolfson Additional author(s): Dr Alan Fitchet Sister Joanne Hughes, Matron Julie Winstanley Authors Division:
Temporary Transvenous Pacing Guideline Classification: Clinical Guideline Lead Author: Dr Peter Woolfson Additional author(s): Dr Alan Fitchet Sister Joanne Hughes, Matron Julie Winstanley Authors Division:
Review Packet EKG Competency This packet is a review of the information you will need to know for the proctored EKG competency test.
 Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
Transcutaneous Pacing on Zoll Defibrillator Version 4 Related Documents SOP-Zoll defibrillator ; Phillips MRX SOP Dr Randal McRoberts
 Emergency Medical Retrieval Service (EMRS) www.emrs.scot.nhs.uk Standard Operating Procedure Public Distribution Title Transcutaneous Pacing on Zoll Defibrillator Version 4 Related Documents SOP-Zoll defibrillator
Emergency Medical Retrieval Service (EMRS) www.emrs.scot.nhs.uk Standard Operating Procedure Public Distribution Title Transcutaneous Pacing on Zoll Defibrillator Version 4 Related Documents SOP-Zoll defibrillator
Temporary pacemaker : Programming &Trouble shooting
 2015 춘계심장학회 Temporary pacemaker : Programming &Trouble shooting 서울아산병원 한두영 Temporary Pacemaker Overview Indication of Temporary Pacemaker Programming ; NBG Code, Pacing/Sensing Device Trouble shooting
2015 춘계심장학회 Temporary pacemaker : Programming &Trouble shooting 서울아산병원 한두영 Temporary Pacemaker Overview Indication of Temporary Pacemaker Programming ; NBG Code, Pacing/Sensing Device Trouble shooting
Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale
 Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale Jason Collinson & Stuart Tan Essex Cardiothoracic Centre, Basildon and Thurrock University Hospital. Contact: jason.collinson@nhs.net
Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale Jason Collinson & Stuart Tan Essex Cardiothoracic Centre, Basildon and Thurrock University Hospital. Contact: jason.collinson@nhs.net
Cardiac Pacing. Learning outcomes. Introduction. The cardiac impulse - its formation and its failure CHAPTER. To understand:
 Cardiac Pacing CHAPTER 10 Learning outcomes To understand: The indications for cardiac pacing in the peri-arrest setting How to perform percussion pacing How to apply non-invasive, transcutaneous electrical
Cardiac Pacing CHAPTER 10 Learning outcomes To understand: The indications for cardiac pacing in the peri-arrest setting How to perform percussion pacing How to apply non-invasive, transcutaneous electrical
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists
 PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
CORONARY ARTERIES HEART
 CARDIAC/ECG MODULE THE HEART CORONARY ARTERIES FIBRILLATING HEART CORONARY ARTERIES HEART PRACTICE RHYTHMS PRACTICE RHYTHMS ELECTRICAL CONDUCTION SA Node (60 100) Primary pacemaker AV Node (40 60) ***Creates
CARDIAC/ECG MODULE THE HEART CORONARY ARTERIES FIBRILLATING HEART CORONARY ARTERIES HEART PRACTICE RHYTHMS PRACTICE RHYTHMS ELECTRICAL CONDUCTION SA Node (60 100) Primary pacemaker AV Node (40 60) ***Creates
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS
 PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS DR SUSAN CORCORAN CARDIOLOGIST ONCE UPON A TIME.. Single chamber pacemakers Programmed at 70/min VVI 70 UNIPOLAR SYSTEMS A Unipolar Pacing
PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS DR SUSAN CORCORAN CARDIOLOGIST ONCE UPON A TIME.. Single chamber pacemakers Programmed at 70/min VVI 70 UNIPOLAR SYSTEMS A Unipolar Pacing
Essentials of Pacemakers and ICD s. Rajesh Banker, MD, MPH
 Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
Ass. Prof. Tomon Thongsri, MD Buddhachinaraj Phitsanuloke Hospital
 Treatment Bradyarrhythmia Ass. Prof. Tomon Thongsri, MD Buddhachinaraj Phitsanuloke Hospital 1 What is the rhythm? Sinus Bradycardia What s rhythm Sinus Bradycardia Treatment Asymptomatic No treatment
Treatment Bradyarrhythmia Ass. Prof. Tomon Thongsri, MD Buddhachinaraj Phitsanuloke Hospital 1 What is the rhythm? Sinus Bradycardia What s rhythm Sinus Bradycardia Treatment Asymptomatic No treatment
Cardiac Telemetry Self Study: Part One Cardiovascular Review 2017 THINGS TO REMEMBER
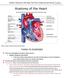 Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
Chapter 80 Implantable Cardiac Devices
 Chapter 80 Implantable Cardiac Devices Episode Overview: 1. List 5 Indications for permanent pacing 2. Pacemaker nomenclature - what do the 5 letters mean a. What are common Pacemaker types? 3. List the
Chapter 80 Implantable Cardiac Devices Episode Overview: 1. List 5 Indications for permanent pacing 2. Pacemaker nomenclature - what do the 5 letters mean a. What are common Pacemaker types? 3. List the
BEDSIDE ECG INTERPRETATION
 BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
ECG. Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13
 ECG Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13 The Concept When the cardiac impulse passes through the heart, electrical current
ECG Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13 The Concept When the cardiac impulse passes through the heart, electrical current
By the end of this lecture, you will be able to: Understand the 12 lead ECG in relation to the coronary circulation and myocardium Perform an ECG
 By the end of this lecture, you will be able to: Understand the 12 lead ECG in relation to the coronary circulation and myocardium Perform an ECG recording Identify the ECG changes that occur in the presence
By the end of this lecture, you will be able to: Understand the 12 lead ECG in relation to the coronary circulation and myocardium Perform an ECG recording Identify the ECG changes that occur in the presence
Non-Invasive Transcutaneous Pacing
 Non-Invasive Transcutaneous Pacing Application Note Introduction This Application Note provides an overview of non-invasive transcutaneous pacing. It includes a brief history of pacing, describes the electrical
Non-Invasive Transcutaneous Pacing Application Note Introduction This Application Note provides an overview of non-invasive transcutaneous pacing. It includes a brief history of pacing, describes the electrical
Project Title Temporary Pacemaker Training Simulator
 Project Title Temporary Pacemaker Training Simulator Project Description Problem: There is no available training device for temporary pacemakers (pacemakers). A training device will have to essentially
Project Title Temporary Pacemaker Training Simulator Project Description Problem: There is no available training device for temporary pacemakers (pacemakers). A training device will have to essentially
Pacing Lead Implant Testing. Document Identifier
 Pacing Lead Implant Testing 1 Objectives Upon completion of this presentation, the participant should be able to: Name the two primary surgical options for implanting pacing leads Describe three significant
Pacing Lead Implant Testing 1 Objectives Upon completion of this presentation, the participant should be able to: Name the two primary surgical options for implanting pacing leads Describe three significant
The Electrocardiogram
 The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
Lab Activity 24 EKG. Portland Community College BI 232
 Lab Activity 24 EKG Reference: Dubin, Dale. Rapid Interpretation of EKG s. 6 th edition. Tampa: Cover Publishing Company, 2000. Portland Community College BI 232 Graph Paper 1 second equals 25 little boxes
Lab Activity 24 EKG Reference: Dubin, Dale. Rapid Interpretation of EKG s. 6 th edition. Tampa: Cover Publishing Company, 2000. Portland Community College BI 232 Graph Paper 1 second equals 25 little boxes
OBJECTIVE. 1. Define defibrillation. 2. Describe Need and history of defibrillation. 3. Describe the principle and mechanism of defibrillation.
 Defibrillators OBJECTIVE 1. Define defibrillation. 2. Describe Need and history of defibrillation. 3. Describe the principle and mechanism of defibrillation. 4. Types and classes of defibrillator 5. Describe
Defibrillators OBJECTIVE 1. Define defibrillation. 2. Describe Need and history of defibrillation. 3. Describe the principle and mechanism of defibrillation. 4. Types and classes of defibrillator 5. Describe
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
Full file at
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
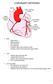 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Chapter 9: Ventricular Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 9.1 Describe the various ventricular dysrhythmias 9.2
Electrocardiography for Healthcare Professionals Chapter 9: Ventricular Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 9.1 Describe the various ventricular dysrhythmias 9.2
INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS
 INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS BEFORE INTERPRETING THE ECG: Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS. Cardiology San Francisco General Hospital UCSF Disclosures: None 1 2 QUESTIONS
INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS BEFORE INTERPRETING THE ECG: Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS. Cardiology San Francisco General Hospital UCSF Disclosures: None 1 2 QUESTIONS
Chapter 20 (2) The Heart
 Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Cardiac Rhythm Device Management. PBL STOP Your acronym for a standardized follow-up
 Cardiac Rhythm Device Management PBL STOP Your acronym for a standardized follow-up What s in it for you? What do you need to feel comfortable with a pacemaker/icd follow-up? 2 CORE OBJECTIVE Provide a
Cardiac Rhythm Device Management PBL STOP Your acronym for a standardized follow-up What s in it for you? What do you need to feel comfortable with a pacemaker/icd follow-up? 2 CORE OBJECTIVE Provide a
MODEL EPG SINGLE CHAMBER TEMPORARY EXTERNAL PACEMAKER
 MODEL 53401 EPG SINGLE CHAMBER TEMPORARY EXTERNAL PACEMAKER In-service Guide 53401 TRAINING LEARNING OBJECTIVES Identify the control knobs and be able to explain how to use them to program device. Distinguish
MODEL 53401 EPG SINGLE CHAMBER TEMPORARY EXTERNAL PACEMAKER In-service Guide 53401 TRAINING LEARNING OBJECTIVES Identify the control knobs and be able to explain how to use them to program device. Distinguish
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Model 5392 EPG Temporary Pacer
 Model 5392 EPG Temporary Pacer Compatible Components Reference Card 5392 Surgical Cables 5487 Disposable, short 5487L Disposable, long 5832S Reusable, small clip 5833S 5833SL Disposable, small clip, short
Model 5392 EPG Temporary Pacer Compatible Components Reference Card 5392 Surgical Cables 5487 Disposable, short 5487L Disposable, long 5832S Reusable, small clip 5833S 5833SL Disposable, small clip, short
a lecture series by SWESEMJR
 Electrolyte disturbances Hypokalaemia Decreased extracellular potassium increases excitability in the myocardial cells and consequently the effect of very severe hypokalaemia is ventricular arrhythmia.
Electrolyte disturbances Hypokalaemia Decreased extracellular potassium increases excitability in the myocardial cells and consequently the effect of very severe hypokalaemia is ventricular arrhythmia.
PART I. Disorders of the Heart Rhythm: Basic Principles
 PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
Timing cycles. Objectives Upon completion of this program the participant will be able to:
 Timing Cycles Timing cycles Objectives Upon completion of this program the participant will be able to: Identify the basic timing cycles of a single and dual chamber pacemaker. Describe the characteristics
Timing Cycles Timing cycles Objectives Upon completion of this program the participant will be able to: Identify the basic timing cycles of a single and dual chamber pacemaker. Describe the characteristics
Where are the normal pacemaker and the backup pacemakers of the heart located?
 CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
Pacemaker Concepts and Terminology*
 Pacemaker Concepts and Terminology* BAROUH V BERKOVITS, E.E., Ing. Associate in Surgery, Harvard Medical School, Boston, Mass., Associate in Electrophysiology, Miami University, Miami, Fla., Senior Research
Pacemaker Concepts and Terminology* BAROUH V BERKOVITS, E.E., Ing. Associate in Surgery, Harvard Medical School, Boston, Mass., Associate in Electrophysiology, Miami University, Miami, Fla., Senior Research
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
ECG Interpretation. Introduction to Cardiac Telemetry. Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services
 ECG Interpretation Introduction to Cardiac Telemetry Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services Disclosures Nothing to disclose Objectives Describe the electrical conduction pathway in
ECG Interpretation Introduction to Cardiac Telemetry Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services Disclosures Nothing to disclose Objectives Describe the electrical conduction pathway in
CRC 431 ECG Basics. Bill Pruitt, MBA, RRT, CPFT, AE-C
 CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
HTEC 91. Performing ECGs: Procedure. Normal Sinus Rhythm (NSR) Topic for Today: Sinus Rhythms. Characteristics of NSR. Conduction Pathway
 HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
DEFIBRILLATORS. Prof. Yasser Mostafa Kadah
 DEFIBRILLATORS Prof. Yasser Mostafa Kadah Basics Defibrillation is definitive treatment for life-threatening cardiac arrhythmias such as ventricular fibrillation Defibrillation consists of delivering therapeutic
DEFIBRILLATORS Prof. Yasser Mostafa Kadah Basics Defibrillation is definitive treatment for life-threatening cardiac arrhythmias such as ventricular fibrillation Defibrillation consists of delivering therapeutic
ABCs of ECGs. Shelby L. Durler
 ABCs of ECGs Shelby L. Durler Objectives Review the A&P of the cardiac conduction system Placement and obtaining 4-lead and 12-lead ECGs Overview of the basics of ECG rhythm interpretation Intrinsic
ABCs of ECGs Shelby L. Durler Objectives Review the A&P of the cardiac conduction system Placement and obtaining 4-lead and 12-lead ECGs Overview of the basics of ECG rhythm interpretation Intrinsic
Lab #3: Electrocardiogram (ECG / EKG)
 Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT
 Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Pacing and Device Jargon Made Simple. Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital
 Pacing and Device Jargon Made Simple Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital Disclosure Dr Jonathan Timperley Honorarium from Bayer Arne Larson (1915
Pacing and Device Jargon Made Simple Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital Disclosure Dr Jonathan Timperley Honorarium from Bayer Arne Larson (1915
Cardiac Cycle. Each heartbeat is called a cardiac cycle. First the two atria contract at the same time.
 The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
Reviewed Date: Supersedes (Policy #/description & date): Prepared by: Jacque Callis, RN Approved by: D.R. Johnson, MD
 External Pacemaker Set-up and Revised Date: 11/13/2014 Page 1 of 5 POLICY: The transcutaneous external pacemaker will be used as a noninvasive method of delivering electrical stimuli to the myocardium
External Pacemaker Set-up and Revised Date: 11/13/2014 Page 1 of 5 POLICY: The transcutaneous external pacemaker will be used as a noninvasive method of delivering electrical stimuli to the myocardium
Electrocardiography Abnormalities (Arrhythmias) 7. Faisal I. Mohammed, MD, PhD
 Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH
 ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
4. The two inferior chambers of the heart are known as the atria. the superior and inferior vena cava, which empty into the left atrium.
 Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Interpreting Electrocardiograms (ECG) Physiology Name: Per:
 Interpreting Electrocardiograms (ECG) Physiology Name: Per: Introduction The heart has its own system in place to create nerve impulses and does not actually require the brain to make it beat. This electrical
Interpreting Electrocardiograms (ECG) Physiology Name: Per: Introduction The heart has its own system in place to create nerve impulses and does not actually require the brain to make it beat. This electrical
Cardiology. Objectives. Chapter
 1:44 M age 1121 Chapter Cardiology Objectives art 1: Cardiovascular natomy and hysiology, ECG Monitoring, and Dysrhythmia nalysis (begins on p. 1127) fter reading art 1 of this chapter, you should be able
1:44 M age 1121 Chapter Cardiology Objectives art 1: Cardiovascular natomy and hysiology, ECG Monitoring, and Dysrhythmia nalysis (begins on p. 1127) fter reading art 1 of this chapter, you should be able
Practice Questions.
 IBHRE Prep Practice Questions Question 1 The relative refractory yperiod of the ventricular myocardium corresponds to which of the following phases of the action potential? A. (0) B. (1) C. (2) D. (3)
IBHRE Prep Practice Questions Question 1 The relative refractory yperiod of the ventricular myocardium corresponds to which of the following phases of the action potential? A. (0) B. (1) C. (2) D. (3)
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology
 EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
Diploma in Electrocardiography
 The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
National Coverage Determination (NCD) for Cardiac Pacemakers (20.8)
 Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
3/26/15 HTEC 91. EKG Sign-in Book. The Cardiac Cycle. Parts of the ECG. Waves. Waves. Review of protocol Review of placement of chest leads (V1, V2)
 EKG Sign-in Book HTEC 91 Review of protocol Review of placement of chest leads (V1, V2) Medical Office Diagnostic Tests Week 2 http://www.cvphysiology.com/arrhythmias/a013c.htm The Cardiac Cycle Represents
EKG Sign-in Book HTEC 91 Review of protocol Review of placement of chest leads (V1, V2) Medical Office Diagnostic Tests Week 2 http://www.cvphysiology.com/arrhythmias/a013c.htm The Cardiac Cycle Represents
Implantable Cardioverter-Defibril. Defibrillators. Ratko Magjarević
 Implantable Cardioverter-Defibril Defibrillators Ratko Magjarević University of Zagreb Faculty of Electrical Engineering and Computing Croatia ratko.magjarevic@fer.hr Ventricular Fibrillation Ventricular
Implantable Cardioverter-Defibril Defibrillators Ratko Magjarević University of Zagreb Faculty of Electrical Engineering and Computing Croatia ratko.magjarevic@fer.hr Ventricular Fibrillation Ventricular
Is This Thing Working?
 Is This *#@!* Thing Working? Pacemaker (and ICD) ECG and Telemetry Pitfalls Wayne O. Adkisson, MD adki0004@umn.edu Disclosures I currently receive research support from Medtronic, Inc. I have been compensated
Is This *#@!* Thing Working? Pacemaker (and ICD) ECG and Telemetry Pitfalls Wayne O. Adkisson, MD adki0004@umn.edu Disclosures I currently receive research support from Medtronic, Inc. I have been compensated
Family Medicine for English language students of Medical University of Lodz ECG. Jakub Dorożyński
 Family Medicine for English language students of Medical University of Lodz ECG Jakub Dorożyński Parts of an ECG The standard ECG has 12 leads: six of them are considered limb leads because they are placed
Family Medicine for English language students of Medical University of Lodz ECG Jakub Dorożyński Parts of an ECG The standard ECG has 12 leads: six of them are considered limb leads because they are placed
Electrical Conduction
 Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
EKG Abnormalities. Adapted from:
 EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
Step by step approach to EKG rhythm interpretation:
 Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
2017 BDKA Review. Regularity Rate P waves PRI QRS Interpretation. Regularity Rate P waves PRI QRS Interpretation 1/1/2017
 1. 2017 BDKA Review 2. 3. 4. Interpretation 5. QT 6. 7. 8. 9. 10. QT 11. 12. 13. 14. 15. 16. 17. 18. QT 19. 20. QT 21. 22. QT 23. 24. Where are pacer spikes? Before the P wave or before the QRS complex?
1. 2017 BDKA Review 2. 3. 4. Interpretation 5. QT 6. 7. 8. 9. 10. QT 11. 12. 13. 14. 15. 16. 17. 18. QT 19. 20. QT 21. 22. QT 23. 24. Where are pacer spikes? Before the P wave or before the QRS complex?
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
Atlantic Health System
 Atlantic Health System Morristown Medical Center Newton Medical Center Overlook Medical Center Basic Dysrhythmia Course Day 1 1 2 Chapter 1 Anatomy and Physiology Learning Objectives 1) Identify electrophysiology
Atlantic Health System Morristown Medical Center Newton Medical Center Overlook Medical Center Basic Dysrhythmia Course Day 1 1 2 Chapter 1 Anatomy and Physiology Learning Objectives 1) Identify electrophysiology
NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS
 NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS OBJECTIVES Discuss history of ICDs Review the indications for ICD and CRT therapy Describe basic lead and device technology Discuss different therapies
NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS OBJECTIVES Discuss history of ICDs Review the indications for ICD and CRT therapy Describe basic lead and device technology Discuss different therapies
Basic ECG Interpretation Module Notebook
 Basic ECG Interpretation Module Notebook ECG_Notebook_04.27.05 Page 1 of 142 Basic ECG Interpretation Table of Contents Module Objectives... 3 Module Outline... 6 Lesson I... 6 Lesson II... 8 Lesson III...
Basic ECG Interpretation Module Notebook ECG_Notebook_04.27.05 Page 1 of 142 Basic ECG Interpretation Table of Contents Module Objectives... 3 Module Outline... 6 Lesson I... 6 Lesson II... 8 Lesson III...
Electrocardiography Normal 5. Faisal I. Mohammed, MD, PhD
 Electrocardiography Normal 5 Faisal I. Mohammed, MD, PhD 1 Objectives 2 1. Describe the different waves in a normal electrocardiogram. 2. Recall the normal P-R and Q-T interval time of the QRS wave. 3.
Electrocardiography Normal 5 Faisal I. Mohammed, MD, PhD 1 Objectives 2 1. Describe the different waves in a normal electrocardiogram. 2. Recall the normal P-R and Q-T interval time of the QRS wave. 3.
Introduction to Electrocardiography
 Introduction to Electrocardiography Class Objectives: Introduction to ECG monitoring Discuss principles of interpretation Identify the components and measurements of the ECG ECG analysis ECG Monitoring
Introduction to Electrocardiography Class Objectives: Introduction to ECG monitoring Discuss principles of interpretation Identify the components and measurements of the ECG ECG analysis ECG Monitoring
Newer pacemakers also can monitor your blood temperature, breathing, and other factors and adjust your heart rate to changes in your activity.
 Pacemakers & Defibrillators A pacemaker system consists of a battery, a computerized generator and wires with sensors called electrodes on one end. The battery powers the generator, and both are surrounded
Pacemakers & Defibrillators A pacemaker system consists of a battery, a computerized generator and wires with sensors called electrodes on one end. The battery powers the generator, and both are surrounded
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE. Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology
 PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
Electrocardiogram ECG. Hilal Al Saffar FRCP FACC College of medicine,baghdad University
 Electrocardiogram ECG Hilal Al Saffar FRCP FACC College of medicine,baghdad University Tuesday 29 October 2013 ECG introduction Wednesday 30 October 2013 Abnormal ECG ( ischemia, chamber hypertrophy, heart
Electrocardiogram ECG Hilal Al Saffar FRCP FACC College of medicine,baghdad University Tuesday 29 October 2013 ECG introduction Wednesday 30 October 2013 Abnormal ECG ( ischemia, chamber hypertrophy, heart
ECG interpretation basics
 ECG interpretation basics Michał Walczewski, MD Krzysztof Ozierański, MD 21.03.18 Electrical conduction system of the heart Limb leads Precordial leads 21.03.18 Precordial leads Precordial leads 21.03.18
ECG interpretation basics Michał Walczewski, MD Krzysztof Ozierański, MD 21.03.18 Electrical conduction system of the heart Limb leads Precordial leads 21.03.18 Precordial leads Precordial leads 21.03.18
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
TIP CARD. Model Temporary External Pacemaker
 TIP CARD Model 5392 Temporary External Pacemaker PRE-USE What to do... What NOT to do... Battery Replace the battery for each new patient. Do NOT reuse battery. Physical Check case for cracks/damage.**
TIP CARD Model 5392 Temporary External Pacemaker PRE-USE What to do... What NOT to do... Battery Replace the battery for each new patient. Do NOT reuse battery. Physical Check case for cracks/damage.**
CARDIOVASCULAR SYSTEM Worksheet
 CARDIOVASCULAR SYSTEM Worksheet NAME Section A: Blood Basics http://www.psbc.org/hematology/01_index.htm Although blood appears to be red liquid it is actually composed of yellowish liquid called plasma
CARDIOVASCULAR SYSTEM Worksheet NAME Section A: Blood Basics http://www.psbc.org/hematology/01_index.htm Although blood appears to be red liquid it is actually composed of yellowish liquid called plasma
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Pacemakers 12/04. Pacemakers. 1. What is a pacemaker?
 Pacemakers 12/04 1-What is a pacemaker? 2- What does intrinsic mean? 3- How exactly do pacemakers work on the heart? 4- What are the parts of a pacemaker? 5- Are there different kinds of pacemakers? 6-
Pacemakers 12/04 1-What is a pacemaker? 2- What does intrinsic mean? 3- How exactly do pacemakers work on the heart? 4- What are the parts of a pacemaker? 5- Are there different kinds of pacemakers? 6-
CASE 10. What would the ST segment of this ECG look like? On which leads would you see this ST segment change? What does the T wave represent?
 CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
