Sinus rhythm with premature atrial beats 2 and 6 (see Lead II).
|
|
|
- Georgia Phillips
- 5 years ago
- Views:
Transcription
1 Cardiac Pacemaker
2 Premature Beats When one of ectopic foci becomes irritable, it may spontaneously fire, leading to one or more premature beats. Atrial and junctional foci may become irritable from excess epinephrine or norepinephrine. Ventricular focus may become irritable when they experience either hypoxemia (low oxygen) or hypokalaemia (low serum potassium).when one premature beat follows and is coupled to a sinus beat, the group of two beats is called bigeminy. When two premature beats follow the sinus beat, the group of three beats is called trigeminy. Sinus rhythm with premature atrial beats 2 and 6 (see Lead II). A premature atrial beat can be identified by the change in heart rate and P-wave shape. After that, the original heart rate continues.
3 Premature Beats Two junctional beats, followed by nine sinus beats and then two premature junctional beats. Ventricular bigeminy in patient with atrial fibrillation. A premature junctional beat can be identified by the change in heart rate and the lack of an associated P wave. After that, the original heart rate continues. A premature ventricular contraction (PVC) can be identified by the change in heart rate and larger beat height and duration. A very wide ventricular complex is produced. After the PVC, a pause is observed because the SA node is not reset.
4 Heart Blocks Sinus block. A sick sinus (SA) node temporarily stop pacing for at least one beat, may lead to an escape beat from one of the ectopic foci. Sinus block is characterized by identical P waves before and after the pause. Sinus block printed from Rivertek RSIM-1500 Simulator
5 Heart Blocks First-degree (1 ) AV block. The impulse from the atria to ventricles is delayed, resulting in a longer than normal pause before ventricular stimulation(p-r interval). In 1 AV block, normal sinus rhythm is present, but the P-R interval exceeds 0.2 s 1 AV block with heart rate of 88 bpm and P-R interval of 0.28 s
6 Heart Blocks Second-degree (2 ) AV block, there is a periodic dropped beat. Type I (Wenckebach) 2 AV block, the P-R interval becomes progressively longer with each beat, until the AV node no longer conducts an impulse from the atria. Type I 2 AV block is caused by parasympathetic excess or by drugs that mimic these parasympathetic effects. In both cases, AV conduction is slowed. Type I 2 AV block. P-R intervals for beats 36 are 0.23, 0.33, 0.37, and 0.41 s.
7 Heart Blocks Type II (Mobitz II) 2 AV block, the P-R interval remains consistent, but a QRS complex does not follow every P wave. Two to four P waves may occur before ventricular. depolarization and a QRS complex are observed. The number of P waves and resulting conduction ratio of P waves to QRS complex relate to the increasing severity of the block. Type II 2 AV block, with a 2:1 conduction ratio.
8 Heart Blocks Ventricular third-degree AV block, or complete AV block, The atrial rate becomes completely dissociated from the ventricular rate, or R-R interval. No atria signal reaches the ventricles; so an ectopic focus below the block escapes overdrive suppression. If R-R interval is bpm, then the AV junctional focus is pacing. If the R-R interval is bpm, the ventrical focus is pacing. When a slower ventricular rate occurs in ventricular 3 AV block, blood flow to the brain becomes inadequate, which causes the patient to lose consciousness (Stokes-Adams syndrome).
9 Heart Failure Heart failure: the reduced pumping capacity of the heart, may causes by bundle branch block. It is a consequence of coronary artery disease, high blood pressure, or diabetes. The body compensates by increasing sympathetic nervous stimulation. When this compensation is insufficient to balance outgoing versus returning blood flow, chronic heart failure occurs. - increased QRS duration (>0.13s) - chronic low blood pressure - resting tachycardia - left ventricle remodels : changes in sphericity, wall thinning, functional mitral regurgitation (backflow of blood through the mitral valve), and increased wall stress
10 Heart Failure
11 Heart Failure Left BBB, with QRS duration of 0.16 s and two R peaks visible in V4 and V5.
12 Heart Failure Right BBB, with QRS duration of 0.15 s and two R peaks visible in V1
13 Pacemakers Direct electrical stimulation of the ventricle may act as therapy to elicit ventricle contraction. The earliest implantable pacemakers were designed to control the Stokes-Adams syndrome. Sensor-based enhancements, which include an accelerometer, can detect motion and cause the heart rate to be adjusted during physical activity. Other optional sensors can detect respiration, the presence of thoracic fluid, or pressure.
14 Leads Outer jacket: polyurethane or a polyurethane hybrid, silicone rubber or polyurethane insulation. Conductor: one or two metal coils of titanium or platinum/iridium that terminate as textured-surface electrodes unipolar lead administers a voltage between one electrode as the catheter and a portion of the pulse generator can as the anode. bipolar lead administers a voltage between a so-called tip electrode (cathode) and a ring electrode (anode), spaced about mm apart at the end of the lead.
15 Leads a bipolar lead positioned in the atrium records the atrial P wave with greater amplitude than a far field R wave from the ventricles a unipolar lead positioned in the atrium may record a far-field R wave of greater amplitude than the atrial P wave
16 Leads To minimize impedance increase, cause by scar tissue development, steroid-eluting electrodes have been developed. In an early design, each electrode consists of a silicone core, impregnated with a small dose of dexamethasone sodium phosphate, in contact with porous titanium, coated with platinum (Stokes, 1987). The mechanism by which dexamethasone sodium phosphate prevents an impedance increase is not fully understood..
17 Pulse Generator Pulse generator is sealed titanium can containing a battery and circuitry. It is implanted in a small-incision, subcutaneous pocket in the pectoralis fascia below the clavicle, on the patient s nondominant side.
18 Capture Tests For these pulses to be therapeutic, the voltage must be sufficient to capture the heart, that is, to generate depolarization. During implantation, a capture test is conducted for each lead. For each test, assuming a constant preselected pulse width, the pulse amplitude voltage is decreased from a maximum setting to the point at which depolarization no longer occurs. The last pulse amplitude of capture is known as the capture threshold. Typically, the pacing threshold is then set at twice the capture threshold. An empirical applied current density adequate for stimulation is 5.0 ma/cm² which, assuming a tissue resistivity of 500 Ωcm, gives an applied field of 2.5 V/cm Electrogram from two patients, measured from tip of a pacemaker lead placed at right ventricle apex, referenced to the can. These patients were at high risk for acute coronary syndromes
19 Pacemaker Sensing Parameters and Modes Atrial and ventricular sensitivities: the minimum voltage thresholds for sensing a P wave and R wave, respectively. These waves are sensed from the bandpass-filtered electrogram. AV delay: the time interval after an atrial pacing pulse at A, during which an R wave may be detected. If an R wave is not detected, a ventricular pulse, V, is fired. PV delay: the time interval after a P wave, during which an R wave may be detected. If an R wave is not detected, a ventricular pulse is fired. PVARP: the time interval after R wave or ventricular stimulus, which atrial sensing is disabled. PVARP prevents retrograde P waves (which often occur following paced beats) from being sensed by the atrial amplifier and causing a pacemaker mediated tachycardia. ventricular refractory period (VRP): the time after R wave or ventricular stimulus, which ventricular sensing is disabled. VRP prevents T waves from being sensed by the ventricular amplifier.
20 Revised NBG Pacemaker Code (Bernstein et al., 2002) Position I II III IV V Category Chamber(s) paced Chamber(s) sensed Response to sensing Rate Modulation Multiside O = None O = None O = None O = None O = None A = Atrium A = Atrium T = Trigger R = Rate Modulation V = Ventricle V = I = Inhibited Ventricle D = Dual (A+V) D = Dual (A+V) D = Dual (T+I) A = Atrium V = Ventricle D = Dual (A+V) Rate modulation: adaptive pacing to achieve more realistic physiological behavior.
21 Pacemaker Modes Two pacemaker modes. A: DDDxx. Both the right atrium and right ventricle are sensed and paced. B: VVIxx. Only the right ventricle is sensed and paced. In these beats, which occur during atrial fibrillation, the first two ventricular depolarization are spontaneous (S), but the third ventricular depolarization is paced (P)
22 Key Features To address unknown lead failure mechanisms, leads may undergo three tests, according to British Standard EN :2003 Active Implantable Medical Devices Part 2-1: Particular Requirements for Active Implantable Medical Devices Intended to Treat Bradyarrhythmia (Cardiac Pacemakers) (BSI, 2003). Battery. A pacemaker system is only as good as its battery, which typically lasts about 7-10 years. The battery is replaced by replacing the pulse generator. Sensitivity. According to British Standard EN :2003, sensitivity error must be within ±10%. Minimum Susceptibility to Electromagnetic Interference. Modern pulse generators are designed to minimize the effect of EMI radiating from 16.6 Hz, which is present on some European railways, to 3 GHz, the radiation field from cell phones. EN :2003 specifies seven tests to assess the effects of electromagnetic nonionizing radiation.
23 References 1. Fundamental of Anatomy and Physiology, Frederic H. Martini 2. Biomedical Instrumentation: Application and Design, John G. Webster 3. Medical Device Technologies: A Systems Based Overview Using Engineering Standards, Gail D. Baura 4. The Biomedical Engineering Handbook, Joseph D. Bronzino
24 clavicle
The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node.
 PACEMAKER Natural pacemaker: The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node. Artificial pacemaker: It is a small, battery-operated device that helps the heart beat in
PACEMAKER Natural pacemaker: The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node. Artificial pacemaker: It is a small, battery-operated device that helps the heart beat in
Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC
 Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC Pacemaker: An electric device implanted in the body to regulate the heart beat. Delivers electrical stimuli over leads with electrodes in contact
Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC Pacemaker: An electric device implanted in the body to regulate the heart beat. Delivers electrical stimuli over leads with electrodes in contact
Step by step approach to EKG rhythm interpretation:
 Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
EKG Abnormalities. Adapted from:
 EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
Electrocardiography Biomedical Engineering Kaj-Åge Henneberg
 Electrocardiography 31650 Biomedical Engineering Kaj-Åge Henneberg Electrocardiography Plan Function of cardiovascular system Electrical activation of the heart Recording the ECG Arrhythmia Heart Rate
Electrocardiography 31650 Biomedical Engineering Kaj-Åge Henneberg Electrocardiography Plan Function of cardiovascular system Electrical activation of the heart Recording the ECG Arrhythmia Heart Rate
The Electrocardiogram
 The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
Practice Questions.
 IBHRE Prep Practice Questions Question 1 The relative refractory yperiod of the ventricular myocardium corresponds to which of the following phases of the action potential? A. (0) B. (1) C. (2) D. (3)
IBHRE Prep Practice Questions Question 1 The relative refractory yperiod of the ventricular myocardium corresponds to which of the following phases of the action potential? A. (0) B. (1) C. (2) D. (3)
2017 BDKA Review. Regularity Rate P waves PRI QRS Interpretation. Regularity Rate P waves PRI QRS Interpretation 1/1/2017
 1. 2017 BDKA Review 2. 3. 4. Interpretation 5. QT 6. 7. 8. 9. 10. QT 11. 12. 13. 14. 15. 16. 17. 18. QT 19. 20. QT 21. 22. QT 23. 24. Where are pacer spikes? Before the P wave or before the QRS complex?
1. 2017 BDKA Review 2. 3. 4. Interpretation 5. QT 6. 7. 8. 9. 10. QT 11. 12. 13. 14. 15. 16. 17. 18. QT 19. 20. QT 21. 22. QT 23. 24. Where are pacer spikes? Before the P wave or before the QRS complex?
Electrocardiography Abnormalities (Arrhythmias) 7. Faisal I. Mohammed, MD, PhD
 Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University. OBHG Education Subcommittee
 -RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS
 INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS BEFORE INTERPRETING THE ECG: Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS. Cardiology San Francisco General Hospital UCSF Disclosures: None 1 2 QUESTIONS
INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS BEFORE INTERPRETING THE ECG: Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS. Cardiology San Francisco General Hospital UCSF Disclosures: None 1 2 QUESTIONS
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists
 PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE. Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology
 PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH
 ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
Basic EKG Interpretation. Nirja Parikh, PT, DPT
 Basic EKG Interpretation Nirja Parikh, PT, DPT Electrocardiogram (EKG) Using surface electrodes record the electrical activity of the heart electrical activity (usually) correlates to mechanical function
Basic EKG Interpretation Nirja Parikh, PT, DPT Electrocardiogram (EKG) Using surface electrodes record the electrical activity of the heart electrical activity (usually) correlates to mechanical function
TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT
 Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Timing cycles. Objectives Upon completion of this program the participant will be able to:
 Timing Cycles Timing cycles Objectives Upon completion of this program the participant will be able to: Identify the basic timing cycles of a single and dual chamber pacemaker. Describe the characteristics
Timing Cycles Timing cycles Objectives Upon completion of this program the participant will be able to: Identify the basic timing cycles of a single and dual chamber pacemaker. Describe the characteristics
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ
 ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ ΤΖΩΡΤΖ ΔΑΔΟΥΣ ΕΠΙΚΟΥΡΟΣ ΚΑΘΗΓΗΤΗΣ Α.Π.Θ. ΜΑΡΙΑ ΚΑΡΑΛΙΟΛΙΟΥ ΕΙΔΙΚΕΥΟΜΕΝΗ ΙΑΤΡΟΣ ΚΑΡΔΙΟΛΟΓΟΣ Β ΚΑΡΔΙΟΛΟΓΙΚΗ ΚΛΙΝΙΚΗ Α.Π.Θ. ΙΠΠΟΚΡΑΤΕΙΟ Γ.Ν.Θ. 5 Why a Pacemaker is Implanted
ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ ΤΖΩΡΤΖ ΔΑΔΟΥΣ ΕΠΙΚΟΥΡΟΣ ΚΑΘΗΓΗΤΗΣ Α.Π.Θ. ΜΑΡΙΑ ΚΑΡΑΛΙΟΛΙΟΥ ΕΙΔΙΚΕΥΟΜΕΝΗ ΙΑΤΡΟΣ ΚΑΡΔΙΟΛΟΓΟΣ Β ΚΑΡΔΙΟΛΟΓΙΚΗ ΚΛΙΝΙΚΗ Α.Π.Θ. ΙΠΠΟΚΡΑΤΕΙΟ Γ.Ν.Θ. 5 Why a Pacemaker is Implanted
CRC 431 ECG Basics. Bill Pruitt, MBA, RRT, CPFT, AE-C
 CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
Pacing Lead Implant Testing. Document Identifier
 Pacing Lead Implant Testing 1 Objectives Upon completion of this presentation, the participant should be able to: Name the two primary surgical options for implanting pacing leads Describe three significant
Pacing Lead Implant Testing 1 Objectives Upon completion of this presentation, the participant should be able to: Name the two primary surgical options for implanting pacing leads Describe three significant
Pacing and Device Jargon Made Simple. Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital
 Pacing and Device Jargon Made Simple Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital Disclosure Dr Jonathan Timperley Honorarium from Bayer Arne Larson (1915
Pacing and Device Jargon Made Simple Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital Disclosure Dr Jonathan Timperley Honorarium from Bayer Arne Larson (1915
Chapter 20 (2) The Heart
 Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Rhythmical Excitation of the Heart
 Rhythmical Excitation of the Heart KALEB HOOD AND JIMMY JOHNSON Special Excitory and Conductive System of the Heart Sinus Node (or sinoatrial node or S-A): A small node with almost no contractile muscle,
Rhythmical Excitation of the Heart KALEB HOOD AND JIMMY JOHNSON Special Excitory and Conductive System of the Heart Sinus Node (or sinoatrial node or S-A): A small node with almost no contractile muscle,
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Is This Thing Working?
 Is This *#@!* Thing Working? Pacemaker (and ICD) ECG and Telemetry Pitfalls Wayne O. Adkisson, MD adki0004@umn.edu Disclosures I currently receive research support from Medtronic, Inc. I have been compensated
Is This *#@!* Thing Working? Pacemaker (and ICD) ECG and Telemetry Pitfalls Wayne O. Adkisson, MD adki0004@umn.edu Disclosures I currently receive research support from Medtronic, Inc. I have been compensated
Rate: The atrial and ventricular rates are equal; heart rate is greater than 100 bpm (usually between bpm).
 Sinus Bradycardia Regularity: The R-R intervals are constant; the rhythm is regular. Rate: The atrial and ventricular rates are equal; heart rate is less than 60 bpm. P wave: There is a uniform P wave
Sinus Bradycardia Regularity: The R-R intervals are constant; the rhythm is regular. Rate: The atrial and ventricular rates are equal; heart rate is less than 60 bpm. P wave: There is a uniform P wave
Outline. Electrical Activity of the Human Heart. What is the Heart? The Heart as a Pump. Anatomy of the Heart. The Hard Work
 Electrical Activity of the Human Heart Oguz Poroy, PhD Assistant Professor Department of Biomedical Engineering The University of Iowa Outline Basic Facts about the Heart Heart Chambers and Heart s The
Electrical Activity of the Human Heart Oguz Poroy, PhD Assistant Professor Department of Biomedical Engineering The University of Iowa Outline Basic Facts about the Heart Heart Chambers and Heart s The
Biomedical Instrumentation
 Biomedical Instrumentation Prof. Dr. Nizamettin AYDIN naydin@yildiz.edu.tr naydin@ieee.org http://www.yildiz.edu.tr/~naydin Therapeutic and Prosthetic Devices 1 Figure 13.1 Block diagram of an asynchronous
Biomedical Instrumentation Prof. Dr. Nizamettin AYDIN naydin@yildiz.edu.tr naydin@ieee.org http://www.yildiz.edu.tr/~naydin Therapeutic and Prosthetic Devices 1 Figure 13.1 Block diagram of an asynchronous
Cardiac Arrhythmias in Sleep
 Cardiac Arrhythmias in Sleep Only 53 Slides! Gauresh H Kashyap, MD, FACP, FCCP, FAASM 1 2 Cardiac Arrhythmias in Sleep Out of 400 Patients with OSA, 48% had some Arrhythmias 20% - 2 PVCs/min 7% - Bradycardia
Cardiac Arrhythmias in Sleep Only 53 Slides! Gauresh H Kashyap, MD, FACP, FCCP, FAASM 1 2 Cardiac Arrhythmias in Sleep Out of 400 Patients with OSA, 48% had some Arrhythmias 20% - 2 PVCs/min 7% - Bradycardia
Contents. Example: Pacemaker in DDD Mode. I. Introduction II. Website and Relevant Documents III. Background Information IV.
 Contents I. Introduction II. Website and Relevant Documents III. Background Information IV. Pacemaker System V. i. Components ii. Operating Modes iii. Parameters Example: Pacemaker in DDD Mode Pacemaker
Contents I. Introduction II. Website and Relevant Documents III. Background Information IV. Pacemaker System V. i. Components ii. Operating Modes iii. Parameters Example: Pacemaker in DDD Mode Pacemaker
Figure 2. Normal ECG tracing. Table 1.
 Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I
 1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 PROFESSIONAL NURSING PRACTICE CAN ONLY ADVANCE AS MUCH AS INDIVIDUAL
1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 PROFESSIONAL NURSING PRACTICE CAN ONLY ADVANCE AS MUCH AS INDIVIDUAL
Basic Dysrhythmia Interpretation
 Basic Dysrhythmia Interpretation Objectives 2 To understand the Basic ECG To understand the meaning of Dysrhythmia To describe the normal heart conduction system. To describe the normal impulse pathways.
Basic Dysrhythmia Interpretation Objectives 2 To understand the Basic ECG To understand the meaning of Dysrhythmia To describe the normal heart conduction system. To describe the normal impulse pathways.
Cardiovascular System
 Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
BEDSIDE ECG INTERPRETATION
 BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
Essentials of Pacemakers and ICD s. Rajesh Banker, MD, MPH
 Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS
 PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS DR SUSAN CORCORAN CARDIOLOGIST ONCE UPON A TIME.. Single chamber pacemakers Programmed at 70/min VVI 70 UNIPOLAR SYSTEMS A Unipolar Pacing
PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS DR SUSAN CORCORAN CARDIOLOGIST ONCE UPON A TIME.. Single chamber pacemakers Programmed at 70/min VVI 70 UNIPOLAR SYSTEMS A Unipolar Pacing
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC
 Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
ISO INTERNATIONAL STANDARD. Implants for surgery Active implantable medical devices Part 2: Cardiac pacemakers
 INTERNATIONAL STANDARD ISO 14708-2 Second edition 2012-08-15 Implants for surgery Active implantable medical devices Part 2: Cardiac pacemakers Implants chirurgicaux Dispositifs médicaux implantables actifs
INTERNATIONAL STANDARD ISO 14708-2 Second edition 2012-08-15 Implants for surgery Active implantable medical devices Part 2: Cardiac pacemakers Implants chirurgicaux Dispositifs médicaux implantables actifs
Conduction System of the Heart. Faisal I. Mohammed, MD, PhD
 Conduction System of the Heart Faisal I. Mohammed, MD, PhD 1 Objectives l List the parts that comprise the conduction system l Explain the mechanism of slow response action potential (pacemaker potential)
Conduction System of the Heart Faisal I. Mohammed, MD, PhD 1 Objectives l List the parts that comprise the conduction system l Explain the mechanism of slow response action potential (pacemaker potential)
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2
Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2
8/20/2012. Learning Outcomes (Cont d)
 1 2 3 4 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2 Identify premature junctional complexes
1 2 3 4 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2 Identify premature junctional complexes
The ECG Course. Boone County Fire Protection District EMS Education
 The ECG Course Level I G rated material AV Blocks What Causes AV Block? Long list of bad things that includes ischemia and.. Old age / disease Medications or drugs Electrolyte imbalances Physiologic Blocks
The ECG Course Level I G rated material AV Blocks What Causes AV Block? Long list of bad things that includes ischemia and.. Old age / disease Medications or drugs Electrolyte imbalances Physiologic Blocks
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
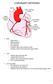 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
Course Objectives. Proper Lead Placements. Review the ECG print paper. Review the mechanics of the Myocardium. Review basics of ECG Rhythms
 ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
Arrhythmia Study Guide 3 Junctional and Ventricular Rhythms
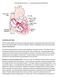 Arrhythmia Study Guide 3 Junctional and Ventricular Rhythms JUNCTIONAL RHYTHMS The AV Junction (Bundle of His and surrounding cells) only acts as pacemaker of the heart when the SA Node is not firing normally
Arrhythmia Study Guide 3 Junctional and Ventricular Rhythms JUNCTIONAL RHYTHMS The AV Junction (Bundle of His and surrounding cells) only acts as pacemaker of the heart when the SA Node is not firing normally
BIPN100 F15 Human Physiology I (Kristan) Problem set #5 p. 1
 BIPN100 F15 Human Physiology I (Kristan) Problem set #5 p. 1 1. Dantrolene has the same effect on smooth muscles as it has on skeletal muscle: it relaxes them by blocking the release of Ca ++ from the
BIPN100 F15 Human Physiology I (Kristan) Problem set #5 p. 1 1. Dantrolene has the same effect on smooth muscles as it has on skeletal muscle: it relaxes them by blocking the release of Ca ++ from the
Conduction System of the Heart 4. Faisal I. Mohammed, MD, PhD
 Conduction System of the Heart 4 Faisal I. Mohammed, MD, PhD 1 Objectives List the parts that comprise the conduction system Explain the mechanism of slow response action potential (pacemaker potential)
Conduction System of the Heart 4 Faisal I. Mohammed, MD, PhD 1 Objectives List the parts that comprise the conduction system Explain the mechanism of slow response action potential (pacemaker potential)
a lecture series by SWESEMJR
 Electrolyte disturbances Hypokalaemia Decreased extracellular potassium increases excitability in the myocardial cells and consequently the effect of very severe hypokalaemia is ventricular arrhythmia.
Electrolyte disturbances Hypokalaemia Decreased extracellular potassium increases excitability in the myocardial cells and consequently the effect of very severe hypokalaemia is ventricular arrhythmia.
PART I. Disorders of the Heart Rhythm: Basic Principles
 PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
1 st Degree Block Prolonged P-R interval caused by first degree heart block (lead II)
 AV Heart Blocks 1 st degree A condition of a rhythm, not a true rhythm Need to always state underlying rhythm 2 nd degree Type I - Wenckebach Type II Classic dangerous to the patient Can be variable (periodic)
AV Heart Blocks 1 st degree A condition of a rhythm, not a true rhythm Need to always state underlying rhythm 2 nd degree Type I - Wenckebach Type II Classic dangerous to the patient Can be variable (periodic)
Full file at
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
Cardiology Flash Cards
 Cardiology Flash Cards EKG in a nut shell www.brain101.info Conduction System www.brain101.info 2 Analyzing EKG Step by step Steps in Analyzing ECG'S 1. Rhythm: - Regular _ Sinus, Junctional or Ventricular.
Cardiology Flash Cards EKG in a nut shell www.brain101.info Conduction System www.brain101.info 2 Analyzing EKG Step by step Steps in Analyzing ECG'S 1. Rhythm: - Regular _ Sinus, Junctional or Ventricular.
Clinical Data Summary: Avoid FFS Study
 Atrial Pacing Lead with 1.1 mm Tip-to-Ring Spacing Clinical Data Summary: Avoid FFS Study A Multi-center, Randomized, Prospective Clinical Study Designed to Evaluate the 1699T Lead Clinical Data Summary:
Atrial Pacing Lead with 1.1 mm Tip-to-Ring Spacing Clinical Data Summary: Avoid FFS Study A Multi-center, Randomized, Prospective Clinical Study Designed to Evaluate the 1699T Lead Clinical Data Summary:
CORONARY ARTERIES HEART
 CARDIAC/ECG MODULE THE HEART CORONARY ARTERIES FIBRILLATING HEART CORONARY ARTERIES HEART PRACTICE RHYTHMS PRACTICE RHYTHMS ELECTRICAL CONDUCTION SA Node (60 100) Primary pacemaker AV Node (40 60) ***Creates
CARDIAC/ECG MODULE THE HEART CORONARY ARTERIES FIBRILLATING HEART CORONARY ARTERIES HEART PRACTICE RHYTHMS PRACTICE RHYTHMS ELECTRICAL CONDUCTION SA Node (60 100) Primary pacemaker AV Node (40 60) ***Creates
Electrical Conduction
 Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Intermittent episodes of paced tachycardia: what is the cause?
 Intermittent episodes of paced tachycardia: what is the cause? Lindsey Parkinson and Lucy Broadhurst, Rotherham NHS Foundation Trust Contact: Lindsey.Parkinson@rothgen.nhs.uk Introduction A hospital in-patient
Intermittent episodes of paced tachycardia: what is the cause? Lindsey Parkinson and Lucy Broadhurst, Rotherham NHS Foundation Trust Contact: Lindsey.Parkinson@rothgen.nhs.uk Introduction A hospital in-patient
Review of Pacemakers and ICD Therapy: Overview and Patient Management
 Review of Pacemakers and ICD Therapy: Overview and Patient Management Pacing Systems Charles J. Love, MD FACC FAHA FHRS CCDS Professor of Medicine Director, Cardiac Rhythm Device Services OSU Division
Review of Pacemakers and ICD Therapy: Overview and Patient Management Pacing Systems Charles J. Love, MD FACC FAHA FHRS CCDS Professor of Medicine Director, Cardiac Rhythm Device Services OSU Division
Lab 16. The Cardiovascular System Heart and Blood Vessels. Laboratory Objectives
 Lab 16 The Cardiovascular System Heart and Blood Vessels Laboratory Objectives Describe the anatomical structures of the heart to include the pericardium, chambers, valves, and major vessels. Describe
Lab 16 The Cardiovascular System Heart and Blood Vessels Laboratory Objectives Describe the anatomical structures of the heart to include the pericardium, chambers, valves, and major vessels. Describe
Cardiac Rhythm Device Management. PBL STOP Your acronym for a standardized follow-up
 Cardiac Rhythm Device Management PBL STOP Your acronym for a standardized follow-up What s in it for you? What do you need to feel comfortable with a pacemaker/icd follow-up? 2 CORE OBJECTIVE Provide a
Cardiac Rhythm Device Management PBL STOP Your acronym for a standardized follow-up What s in it for you? What do you need to feel comfortable with a pacemaker/icd follow-up? 2 CORE OBJECTIVE Provide a
Cardiac Telemetry Self Study: Part One Cardiovascular Review 2017 THINGS TO REMEMBER
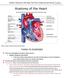 Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
Collin County Community College
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 5 The Heart 1 The Heart Beat and the EKG 2 1 The Heart Beat and the EKG P-wave = Atrial depolarization QRS-wave = Ventricular depolarization
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 5 The Heart 1 The Heart Beat and the EKG 2 1 The Heart Beat and the EKG P-wave = Atrial depolarization QRS-wave = Ventricular depolarization
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
The conduction system
 The conduction system In today s lecture we will discuss the conducting system of the heart. If we placed the heart in a special solution that contains Ca+ it will keep on contracting, keep in mind that
The conduction system In today s lecture we will discuss the conducting system of the heart. If we placed the heart in a special solution that contains Ca+ it will keep on contracting, keep in mind that
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc.
 Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
 Pacemaker Simulator ST2361 Learning Material Ver.1.1 An ISO 9001:2008 company Save paper, save trees, save earth Dear User, We request you to use the Learning material in the CD form provided with this
Pacemaker Simulator ST2361 Learning Material Ver.1.1 An ISO 9001:2008 company Save paper, save trees, save earth Dear User, We request you to use the Learning material in the CD form provided with this
Lab Activity 24 EKG. Portland Community College BI 232
 Lab Activity 24 EKG Reference: Dubin, Dale. Rapid Interpretation of EKG s. 6 th edition. Tampa: Cover Publishing Company, 2000. Portland Community College BI 232 Graph Paper 1 second equals 25 little boxes
Lab Activity 24 EKG Reference: Dubin, Dale. Rapid Interpretation of EKG s. 6 th edition. Tampa: Cover Publishing Company, 2000. Portland Community College BI 232 Graph Paper 1 second equals 25 little boxes
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
Practice Exercises for the Cardiovascular System
 Practice Exercises for the Cardiovascular System On the diagram below, color the oxygen-rich blood red and the oxygen-poor blood blue. Label the parts: Continued on the next page... Label the parts on
Practice Exercises for the Cardiovascular System On the diagram below, color the oxygen-rich blood red and the oxygen-poor blood blue. Label the parts: Continued on the next page... Label the parts on
Lab 2. The Intrinsic Cardiac Conduction System. 1/23/2016 MDufilho 1
 Lab 2 he Intrinsic Cardiac Conduction System 1/23/2016 MDufilho 1 Figure 18.13 Intrinsic cardiac conduction system and action potential succession during one heartbeat. Superior vena cava ight atrium 1
Lab 2 he Intrinsic Cardiac Conduction System 1/23/2016 MDufilho 1 Figure 18.13 Intrinsic cardiac conduction system and action potential succession during one heartbeat. Superior vena cava ight atrium 1
Cardiac Arrhythmias. Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company
 Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
4/14/15 HTEC 91. Topics for Today. Guess That Rhythm. Premature Ventricular Contractions (PVCs) Ventricular Rhythms
 4/14/15 Topics for Today HTEC 91 Medical Office Diagnostic Tests Week 5 Ventricular Rhythms PVCs: Premature Ventricular Contractions VT: Ventricular Tachycardia VF: Ventricular Fibrillation Asystole Study
4/14/15 Topics for Today HTEC 91 Medical Office Diagnostic Tests Week 5 Ventricular Rhythms PVCs: Premature Ventricular Contractions VT: Ventricular Tachycardia VF: Ventricular Fibrillation Asystole Study
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Basic ECG Interpretation Module Notebook
 Basic ECG Interpretation Module Notebook ECG_Notebook_04.27.05 Page 1 of 142 Basic ECG Interpretation Table of Contents Module Objectives... 3 Module Outline... 6 Lesson I... 6 Lesson II... 8 Lesson III...
Basic ECG Interpretation Module Notebook ECG_Notebook_04.27.05 Page 1 of 142 Basic ECG Interpretation Table of Contents Module Objectives... 3 Module Outline... 6 Lesson I... 6 Lesson II... 8 Lesson III...
Diploma in Electrocardiography
 The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
Comparison of Different ECG Signals on MATLAB
 International Journal of Electronics and Computer Science Engineering 733 Available Online at www.ijecse.org ISSN- 2277-1956 Comparison of Different Signals on MATLAB Rajan Chaudhary 1, Anand Prakash 2,
International Journal of Electronics and Computer Science Engineering 733 Available Online at www.ijecse.org ISSN- 2277-1956 Comparison of Different Signals on MATLAB Rajan Chaudhary 1, Anand Prakash 2,
Cardiovascular System: The Heart
 Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
Introduction. Circulation
 Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Chapter 9: Ventricular Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 9.1 Describe the various ventricular dysrhythmias 9.2
Electrocardiography for Healthcare Professionals Chapter 9: Ventricular Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 9.1 Describe the various ventricular dysrhythmias 9.2
Collin County Community College. ! BIOL Anatomy & Physiology! WEEK 5. The Heart
 Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
Pacemaker Concepts and Terminology*
 Pacemaker Concepts and Terminology* BAROUH V BERKOVITS, E.E., Ing. Associate in Surgery, Harvard Medical School, Boston, Mass., Associate in Electrophysiology, Miami University, Miami, Fla., Senior Research
Pacemaker Concepts and Terminology* BAROUH V BERKOVITS, E.E., Ing. Associate in Surgery, Harvard Medical School, Boston, Mass., Associate in Electrophysiology, Miami University, Miami, Fla., Senior Research
If the P wave > 0.12 sec( 3 mm) usually in any lead. Notched P wave usually in lead I,aVl may be lead II Negative terminal portion of P wave in V1, 1
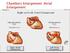 If the P wave > 0.12 sec( 3 mm) usually in any lead. Notched P wave usually in lead I,aVl may be lead II Negative terminal portion of P wave in V1, 1 mm depth and 3 mm width( most specific) Since Mitral
If the P wave > 0.12 sec( 3 mm) usually in any lead. Notched P wave usually in lead I,aVl may be lead II Negative terminal portion of P wave in V1, 1 mm depth and 3 mm width( most specific) Since Mitral
Diagnostic capabilities of the implantable therapeutic systems
 Cardiac pacing 2012 and beyound Monday August 27, 2012 Diagnostic capabilities of the implantable therapeutic systems Pekka Raatikainen Heart Center Co. Tampere University Hospital and University of Tampere
Cardiac pacing 2012 and beyound Monday August 27, 2012 Diagnostic capabilities of the implantable therapeutic systems Pekka Raatikainen Heart Center Co. Tampere University Hospital and University of Tampere
Human Anatomy and Physiology II Laboratory Cardiovascular Physiology
 Human Anatomy and Physiology II Laboratory Cardiovascular Physiology 1 This lab involves two exercises: 1) Conduction System of the Heart and Electrocardiography and 2) Human Cardiovascular Physiology:
Human Anatomy and Physiology II Laboratory Cardiovascular Physiology 1 This lab involves two exercises: 1) Conduction System of the Heart and Electrocardiography and 2) Human Cardiovascular Physiology:
ECG Interpretation. Introduction to Cardiac Telemetry. Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services
 ECG Interpretation Introduction to Cardiac Telemetry Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services Disclosures Nothing to disclose Objectives Describe the electrical conduction pathway in
ECG Interpretation Introduction to Cardiac Telemetry Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services Disclosures Nothing to disclose Objectives Describe the electrical conduction pathway in
Pacing Codes and Modes Concepts
 Pacing Codes and Modes Concepts Pacing codes and modes concepts Objectives Upon completion of this program the participant will be able to: State what the first four positions of the NBG code represent.
Pacing Codes and Modes Concepts Pacing codes and modes concepts Objectives Upon completion of this program the participant will be able to: State what the first four positions of the NBG code represent.
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]
![QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]](/thumbs/96/126998162.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
The Cardiac Pacemaker Case Study and its implementation in Safety-Critical Java and Ravenscar Ada
 The Cardiac Pacemaker Case Study and its implementation in Safety-Critical Java and Ravenscar Ada Neeraj Kumar Singh, Andy Wellings, Ana Cavalcanti University of York, United Kingdom JTRES, 24-26 October
The Cardiac Pacemaker Case Study and its implementation in Safety-Critical Java and Ravenscar Ada Neeraj Kumar Singh, Andy Wellings, Ana Cavalcanti University of York, United Kingdom JTRES, 24-26 October
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
Understanding the 12-lead ECG, part II
 Bundle-branch blocks Understanding the 12-lead ECG, part II Most common electrocardiogram (ECG) abnormality Appears as a wider than normal S complex Occurs when one of the two bundle branches can t conduct
Bundle-branch blocks Understanding the 12-lead ECG, part II Most common electrocardiogram (ECG) abnormality Appears as a wider than normal S complex Occurs when one of the two bundle branches can t conduct
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
4. The two inferior chambers of the heart are known as the atria. the superior and inferior vena cava, which empty into the left atrium.
 Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer: The electrical current has difficulty traveling down the normal conduction pathway.
 1 Electrocardiography for Healthcare Professionals Chapter 8: Heart Block Dysrhythmias 2 3 4 5 6 Learning Outcomes 8.1 Describe the various heartblock dysrhythmias 8.2 Identify first degree heartblock
1 Electrocardiography for Healthcare Professionals Chapter 8: Heart Block Dysrhythmias 2 3 4 5 6 Learning Outcomes 8.1 Describe the various heartblock dysrhythmias 8.2 Identify first degree heartblock
Pediatric pacemakers & ICDs:
 Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
