Management of Patients With Coronary Vascular Disorders
|
|
|
- Thomasina Franklin
- 5 years ago
- Views:
Transcription
1 Management of Patients With Coronary Vascular Disorders
2 Coronary Artery Disease
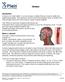
3 CORONARY ATHEROSCLEROSIS Is an abnormal accumulation of lipid, or fatty substances and fibrous tissue in the vessel wall These substances create blockages or narrow the vessel in a way that reduces blood flow to the myocardium Atherosclerosis is a progressive disease that can be curtailed and, in some cases, reversed
4
5
6 Pathophysiology Atherosclerosis begins as fatty streaks, lipids that are deposited in the intima of the arterial wall T lymphocytes and monocytes (that become macrophages) infiltrate the area to ingest the lipids and then die; this causes smooth muscle cells within the vessel to proliferate and form a fibrous cap over the dead fatty core These deposits, called atheromas or plaques, protrude into the lumen of the vessel, narrowing it and obstructing blood flow
7 Pathophysiology If The fibrous cap of the plaque is thick & The lipid pool remains relatively stable it can resist the stress from blood flow and vessel movement If The cap is thin The lipid core may grow Causing it to rupture and hemorrhage into the plaque Allowing a thrombus to develop The thrombus may obstruct blood flow leading to sudden cardiac death or an acute myocardial infarction (MI), which is the death of heart tissue
8
9
10
11
12 Pathophysiology Angles of the coronary arteries The many angles and curves of the coronary arteries contribute to the vessels susceptibility to atheromatous plaques Arteries shown as dashed lines supply the posterior wall of the heart
13 Causes of heart disease Is most often caused by atherosclerosis of the coronary arteries Decrease blood flow to the heart 1. vasospasm (sudden constriction or narrowing) of a coronary artery 2. myocardial trauma from internal or external forces, structural disease 3. Congenital anomalies 4. Decreased oxygen supply (eg, from acute blood loss, anemia, or low blood pressure) 5. Increased demand for oxygen (eg, from rapid heart rate, thyrotoxicosis, or ingestion of cocaine)
14 Clinical Manifestations Symptoms and complications according to: 1. Location and degree of narrowing of the arterial lumen 2. Thrombus formation 3. Obstruction of blood flow to the myocardium
15 Clinical Manifestations Angina pectoris refers to Chest pain that is brought about by myocardial ischemia If the ischemia is great enough, of long duration, or both Irreversible damage and death of myocardial cells, or MI Over time, irreversibly damaged myocardium undergoes degeneration and is replaced by scar tissue, causing various degrees of myocardial dysfunction
16
17 Significant myocardial damage may cause: Inadequate cardiac output The heart cannot support the body s needs for blood which is called heart failure (HF) A decrease in blood supply from CAD may even cause the heart to stop abruptly Called sudden cardiac death
18 Clinical Manifestations of CAD Acute onset of chest pain May be asymptomatic (in those older, women, have diabetes, a history of heart failure) Typical symptoms: shortness of breath Nausea unusual fatigue changes on the (ECG) high levels of cardiac enzymes Dysrhythmias sudden death
19 Risk Factors Use of tobacco Hypertension Elevated blood lipid levels Family history of premature cardiovascular disease Age (first-degree relative with cardiovascular disease at age 55 or younger for men and at age 65 or younger for women) >45 years for men >55 years for women
20 Nonmodifiable Risk Factors for Coronary Artery Disease Family history of coronary heart disease Increasing age Gender (heart disease occurs three times more often in men than in premenopausal women) Race (higher incidence of heart disease in African Americans than in Caucasians)
21 Modifiable Risk Factors for Coronary Artery Disease High blood cholesterol level Cigarette smoking, tobacco use Hypertension Diabetes mellitus Lack of estrogen in women Physical inactivity Obesity
22 Coronary Artery Disease Risk Equivalents Individuals at highest risk for a cardiac event within 10 years are hose with existing (CAD) & those with any of the following diseases, which are called CAD risk equivalents: Diabetes Peripheral arterial disease Abdominal aortic aneurysm Carotid artery disease
23 Prevention of Coronary Artery Disease CONTROLLING CHOLESTEROL ABNORMALITIES: The desired goal is to have low LDL values and high HDL values The desired level of LDL depends on the patient: Patients with one or no risk factors Less than 160 mg/dl Patients with two or more risk factors Less than 130 mg/dl Patients with CAD or a CAD risk equivalent Less than 100 mg/dl
24 Control of LDL Serum cholesterol and LDL levels can usually be controlled by diet and physical activity Medication therapy
25 CONTROLLING CHOLESTEROL ABNORMALITIES The level of HDL should exceed 40 mg/dl and should ideally be more than 60mg/dL A high HDL level is a strong negative risk factor (is protective) for heart disease
26 Controlling TG Abnormalities Triglyceride is another fatty substance, made up of fatty acids, that is transported through the blood by a lipoprotein Although an elevated triglyceride level (>200 mg/dl) may be due to: 1. Genetic in origin 2. Obesity 3. physical inactivity 4. excessive alcohol intake 5. high-carbohydrate diets 6. diabetes mellitus 7. kidney disease 8. Medications ( birth control pills, corticosteroids, and beta-adrenergic blockers when given in higher doses(
27 Management of elevated triglyceride Weight reduction Increased physical activity Medications
28 Dietary Measures Soluble fibers, which are found in fresh fruit, cereal grains, vegetables, and legumes, enhance the excretion of metabolized cholesterol
29 Physical Activity Regular, moderate physical activity increases HDL levels and reduces triglyceride levels The goal for the average person is a total of 30 minutes of exercise, three to four times per week
30 Physical Activity Patients should begin with a 5-minute warm-up period to stretch and prepare the body for the exercise The nurse should inform patients to stop any activity if they develop Chest pain Unusual shortness of breath Dizziness Lightheadedness Nausea
31 PROMOTING CESSATION OF TOBACCO USE Effects of smoking: The inhalation of smoke Increases the blood carbon monoxide level Hemoglobin to combine with CO than with O 2 Decreased amount of available oxygen Decrease the heart s ability to pump
32 Effects of smoking: The nicotinic acid in tobacco Triggers the release of catecholamines Raise the heart rate and blood pressure Coronary arteries to constrict May be a factor in the increased incidence of sudden cardiac death
33 Effects of smoking: Use of tobacco Increases platelet adhesion Higher probability of thrombus formation People who stop smoking reduce their risk of heart disease by 30% to 50% within the first year, and the risk continues to decline as long as they refrain from smoking
34 Managing Hypertension Hypertension is defined Blood pressure measurements that repeatedly exceed 140/90 mm Hg Long-standing elevated blood pressure may Increased stiffness of the vessel walls Leading to vessel injury Resulting inflammatory response within the intima
35 Hypertension can also Increase the work of the left ventricle pump harder to eject blood into the arteries Over time Heart to enlarge and thicken (HYPERTROPHY) condition that may eventually lead to cardiac failure
36
37 Witch of them are more compliant?
38
39 CONTROLLING DIABETES MELLITUS 2/3 to ¾ of diabetic patient death related to Cardiovascular Disease Hyperglycemia Fosters dyslipidemia Increased platelet aggregation Altered red blood cell function All of above factor can lead to thrombus formation
40 Gender and Estrogen Level Women tend not to recognize the symptoms as early as men and to wait longer to report their symptoms and seek medical assistance!!! In women younger than age 55, the incidence of CAD is significantly lower than in men After age 55, the incidence in women is approximately equal to that in men
41 Gender and Estrogen Level Hormone replacement therapy (HRT) has decreased postmenopausal symptoms and the risk for osteoporosis related bone fractures but HRT also has been associated with: CAD BC DVT CVA PE
42 ANGINA PECTORIS
43 Angina Pectoris Angina pectoris is Clinical syndrome usually characterized by episodes or paroxysms of pain or pressure in the anterior chest The cause usually insufficient coronary blood flow Supply Demand
44
45 factors associated with typical anginal pain: Physical exertion increasing myocardial oxygen demand Exposure to cold vasoconstriction elevated blood pressure increased oxygen demand Eating a heavy meal increases the blood flow to the mesenteric area for digestion reducing the blood supply available to the heart muscle Stress or any emotion-provoking situation Release of adrenaline Increasing BP accelerate the HR increase the myocardial workload
46 Types of Angina Stable angina: o predictable and consistent pain that occurs on exertion and is relieved by rest Unstable angina:(also called pre infarction angina or crescendo angina) o symptoms occur more frequently and last longer than stable angina o The threshold for pain is lower, and pain may occur at rest Intractable or refractory angina: o severe incapacitating chest pain
47 Types of Angina (Cont) Variant angina (also called Prinzmetal s angina): Pain at rest with reversible ST-segment elevation Thought to be caused by coronary artery vasospasm Silent ischemia: Objective evidence of ischemia (such as ECG changes with a stress test) Patient reports no symptoms
48 Clinical Manifestations A feeling of indigestion to a choking Heavy sensation in the upper chest Pain accompanied by severe apprehension Feeling of impending death. Retrosternal pain, tightness The pain or discomfort is poorly localized and May radiate to the neck, jaw, shoulders, and inner aspects of the upper arms, usually the left arm
49 Clinical Manifestations A feeling of weakness or numbness Arms, wrists, and hands may accompany the pain shortness of breath, Pallor Diaphoresis Dizziness or lightheadedness nausea and vomiting
50 Assessment and Diagnostic Findings o Clinical manifestations of ischemia o Patient s history o A 12-lead ECG o Blood laboratory values o Echocardiogram o C-reactive protein (CRP): High blood levels of CRP have been associated with increased coronary artery calcification and risk of an acute cardiovascular event (eg, MI) in seemingly healthy individuals
51 Medical Management The objectives of the medical management of angina: Decrease the oxygen demand of the myocardium Increase the oxygen supply Medically, these objectives are met through Pharmacologic therapy Control of risk factors Supply Demand
52 Revascularization procedures Percutaneous coronary interventional (PCI) procedures: percutaneous transluminal coronary angioplasty [PTCA] Intracoronary stents Atherectomy CABG Percutaneous transluminal myocardial revascularization (PTMR)
53 PHARMACOLOGIC THERAPY Nitroglycerin: Actions: 1. Reduce myocardial oxygen consumption Decreases ischemia and relieves pain 2. Dilates primarily the veins 3. Dilates the arteries (High Dose) 4. Increase coronary blood flow by o o Preventing vasospasm Increasing perfusion through the collateral vessels
54 Nitroglycerin Dilation of the veins venous pooling of blood throughout the body decrease venous returns Decreasing filling pressure (preload) is reduced If the patient is hypovolemic the decrease in filling pressure can cause a significant decrease in cardiac output and blood pressure
55 Route of administration o Sublingual tablet or spray: Alleviates the pain of ischemia within 3 minutes o Topical agent: Fast acting and is a convenient way to administer the medication o Intravenous administration: According patient symptom
56 After the patient is symptom free, the nitroglycerin may be switched to a topical preparation within 24 hours Precautions on IV administration The amount of nitroglycerin administered is based on the patient s symptoms Observe BP for hypotension It usually is not given if the systolic blood pressure is 90 mm Hg or less
57 Beta-Adrenergic Blocking Agents Propranolol (Inderal) Atenolol (Tenormin)
58 Actions o Reduce myocardial oxygen consumption Blocking the beta-adrenergic sympathetic stimulation to the heart The result is a reduction in HR Slowed conduction of an impulse through the heart Decreased BP Reduced myocardial contractility (force of contraction) Establishes a more favorable balance between (demands) and available (supply) o Reduce the incidence of recurrent angina, infarction, and cardiac mortality
59 Cardiac side effects and possible contraindication o Hypotension o Bradycardia o Advanced atrioventricular block o Decompensated heart failure
60 Precautions on administration: If a beta-blocker is given intravenously, Monitor o ECG o Blood pressure o heart rate o Contraindicated in Pt. with bronchial asthma o Should not be stopped abruptly o Patients with diabetes who take beta-blockers are instructed to assess their blood glucose levels more often and to observe for signs and symptoms of hypoglycemia
61 Precautions on administration Beta Blocker Agents: Hypoglycemic S&S o Sweating o Nervousness o Tremor o Tachycardia o Hunger o Neurologic symptoms ranging from Bizarre behavior and confusion ======== Seizures and coma
62 Calcium Channel Blocking Agents: (diltiazem) Decrease: SA node automaticity and AV node conduction Resulting in: 1. Slower HR (negative Chronotrop effect) 2. Decrease in the strength of the heart muscle contraction (negative inotropic effect) 3. Decrease the workload of the heart
63 Calcium Channel Blocking Agents: (diltiazem) Relax the blood vessels Decrease in BP Increase in coronary artery perfusion Dilating the smooth muscle wall of the coronary arterioles Increase myocardial oxygen supply Reducing systemic arterial pressure and the workload of the LV Decrease myocardial oxygen demand
64 Antiplatelet o Aspirin: It prevents platelet activation Reduces the incidence of MI Reduce Death in patients with CAD o Dose: o 160- to 325-mg should be given to the patient with angina (as soon as the diagnosis is made) o Continued with 81 to 325 mg daily
65 Antiplatelet o Clopidogrel (Plavix): Given to patients who are allergic to aspirin Given in addition to aspirin in patients at high risk for MI Take a few days to achieve their antiplatelet effect They also cause gastrointestinal upset, including: Nausea Vomiting Diarrhea
66 Other Clopidogrel Side effects: o o o o o o o o o o o Bloody or black, tarry stools Nosebleeds Pinpoint red or purple spots on your skin or in mouth Problems with vision, speech, or walking Red or dark brown urine Seizures Severe stomach pain Shortness of breath, tiredness, uneven heartbeat Yellowing of skin or the whites of eyes Unusual bleeding, bruising, or weakness Vomiting of blood or vomit that looks like coffee grounds
67 Anticoagulant Medications Heparin: Unfractionated heparin prevents the formation of new blood clots The amount of heparin administered is based on o The results of (aptt) Heparin therapy is usually considered therapeutic when o The aptt is 1.5 to 2 times the normal aptt value
68 Signs and symptoms indicate a significant risk for a cardiac event: Patient is hospitalized May be given an intravenous bolus of heparin and Started on a continuous infusion or Given an intravenous bolus every 4 to 6 hours 5000u Bolus 25000/50 cc 1cc 500 u 1h 2cc
69 low-molecular-weight heparin (LMWH): may be used instead of intravenous unfractionated heparin to treat patients with unstable angina or non ST-segment elevation MIs
70 Patient is monitored for signs and symptoms of external and internal bleeding, such as: Low BP Increased HR Decrease in serum Hgb and HCT values
71 Oxygen Administration Usually initiated at the onset of chest pain Increase oxygen delivered to the myocardium Decrease pain The therapeutic effectiveness of oxygen is determined by observing the rate and rhythm of respirations Blood oxygen saturation is monitored by pulse oximetry, the normal oxygen saturation (SpO2) level is greater than 93%
72
73 MYOCARDIAL INFARCTION
74 Definition Its the death of apportion of heart muscle in an area where there is sudden loss of blood supply
75 Clinical Manifestations Chest pain Occurs suddenly and continues despite rest and medication is the presenting symptom in most patients with an MI Shortness of breath Anxiety and restless Cool, pale, and moist skin Tachypnea bradycardia dyshythmia May be a symptomatic Increase B.P or decrease B.P Decrease U.O Nausea and vomiting Anxiety, fear, headache, visual disturbances, altered speech
76 Diagnoses of M.I o ECG (electrocardiogram) o Laboratory test: cardiac enzyme o Creatinine kinase (ck) isoenzymes o CK-MB (heart muscle) o Troponin : regulate the myocardial contractility o LDH
77 ELECTROCARDIOGRAM o It should be obtained within 10 minutes from the time a patient reports pain or arrives in the emergency department o The classic ECG changes are o T-wave inversion o ST-segment elevation o Development of an abnormal Q wave The injured myocardial cells depolarize normally But repolarize more rapidly than normal cells ST segment to rise at least 1 mm above the isoelectric line
78
79 Electrocardiographic Criterion The most frequently used electrocardiographic criterion for identifying acute myocardial infarction is ST segment elevation (two or more anatomically contiguous leads)
80 Electrocardiographic Criterion Early stages of AMI the ECG May be normal or near normal!!! Less than half Of Patients With AMI Have clear diagnostic Changes On Their First trace About 10% of patients with a proved AMI (on the basis of clinical history and enzymatic markers) Fail to Develop ST segment Elevation or depression In Most cases, however, Serial Electrocardiograms Show Evolving Changes that tend To Follow Well Recognized patterns
81
82 LABORATORY TESTS Creatine Kinase and Its Isoenzymes. There are 3 CK isoenzymes: o CK-MM (skeletal muscle) o CK-MB (heart muscle): CK-MB is the cardiac-specific isoenzyme found mainly in cardiac cells and rises only when there has been damage to these cells o CK-BB (brain tissue)
83 Laboratory Test (Myoglobin ) o Myoglobin is a heme protein that helps to transport oxygen o It is found in cardiac and skeletal muscle o The myoglobin level o Starts to increase within 1 to 3 hours o Peaks within 12 hours after the onset of symptoms o If the first myoglobin test results are negative, the test may be repeated 3 hours later o Another negative test result confirms that the patient did not have an MI
84 Laboratory Test (Troponin) o Protein found in the myocardium, regulates the myocardial contractile process o Troponins I and T for cardiac muscle, used to identify myocardial injury (unstable angina or acute MI) o The increase in the level of troponin in the serum o Starts and peaks at approximately the same time as CK-MB. o However, it remains elevated for a longer period, often up to 3 weeks Cannot be used to identify subsequent extension or expansion of an MI
85
86 Medical management for MI M.I can treat by open the blocked artery & restore blood flow to the affected area of the heart muscle by: Reperfusion: Established in the first 4-6 hrs of heart attack by using (percutanous transluminal coronary angioplasty (PTCA) Thrombolytic medication
87 Pharmacological Treatment Thrombolytic agents: The purpose of thrombolytics Dissolve and lyse the thrombus in a coronary artery (thrombolysis) Allowing blood to flow through the coronary artery again (reperfusion) Minimizing the size of the infarction Preserving ventricular function
88 Antiplatelets Aspirin to reduce tendency of platelets in the blood to clump & clot Nitroglycerine: Vasodilator Analgesics: The analgesic of choice for acute MI is morphine sulfate
89 Potential Complications o Acute pulmonary edema o Heart failure o Cardiogenic shock o Dysrhythmias and cardiac arrest o Pericardial effusion and cardiac tamponade o Myocardial rupture
90 Nursing Process Myocardial Infarction Assessment A systemic assessment include careful history, particularly as it related to symptom Each symptom must be evaluated with regard to Time Duration Factors that precipitate the symptom Factor that elieve it
91 NURSING DIAGNOSES 1. Ineffective cardiopulmonary perfusion related to reduced coronary blood flow 2. Potential impaired gas exchange related to fluid overload from L.V 3. Potential altered peripheral tissue perfusion related to decreased cardiac output 4. Anxiety related to fear of death
92 Planning and Goals 1. Relief the pain The major goals of the Patient include: 2. Prevention of further myocardial damage 3. Absence of respiratory dysfunction 4. Reducing anxiety 5. Absence of or recognition of complications 6. Maintenance or attainment of adequate tissue Perfusion by decreasing the heart s workload
93 Nursing Interventions RELIEVING PAIN AND OTHER SIGNS AND SYMPTOMS OF ISCHEMIA: Administration of oxygen Elevate head of the bed: is beneficial for the following reasons: Tidal volume improves because of reduced pressure from abdominal contents on the diaphragm and better lung expansion and gas exchange Drainage of the upper lung lobes improves Venous return to the heart (preload) decreases, which reduces the work of the heart.
94 Improve Respiratory Function: - Changing position - Deep breathing Promoting Adequate Tissue Perfusion - Checking skin temperature and peripheral pulses frequently is important to ensure adequate tissue perfusion - Oxygen may be administered to enrich the supply of circulating oxygen
95 Reducing Anxiety Developing a trusting and caring relationship with the patient Providing information to the patient and family Ensuring a quiet environment, preventing interruptions that disturb sleep MONITORING AND MANAGING POTENTIAL COMPLICATIONS
96 Invasive Coronary Artery Procedures Percutaneous Transluminal Coronary Angioplasty (PTCA): uses: In patient who do not experience angina but are at high risk for a cardiac event as identified by noninvasive testing In patient with recurrent chest pain that is unresponsive to medical therapy In patient with a significant amount of myocardium at risk but are poor surgical candidates In patient with an acute MI (as an alternate to thrombolysis and after thrombolysis
97
98
99
Results of Ischemic Heart Disease
 Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 26 Caring for Clients with Coronary Heart Disease and Dysrhythmias Coronary Heart Disease (CHD) Leading
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 26 Caring for Clients with Coronary Heart Disease and Dysrhythmias Coronary Heart Disease (CHD) Leading
Coronary Heart Disease. Raja Nursing Instructor RN, DCHN, Post RN. BSc.N
 Coronary Heart Disease Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives Define coronary heart disease (CHD). Identify the causes and risk factors of CHD Discuss the pathophysiological
Coronary Heart Disease Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives Define coronary heart disease (CHD). Identify the causes and risk factors of CHD Discuss the pathophysiological
Diagnosis and Management of Acute Myocardial Infarction
 Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United
 Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Cardiac Emergencies. A Review of Cardiac Compromise. Lawrence L. Lambert
 Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
Cardiovascular Diseases and Diabetes
 Cardiovascular Diseases and Diabetes LEARNING OBJECTIVES Ø Identify the components of the cardiovascular system and the various types of cardiovascular disease Ø Discuss ways of promoting cardiovascular
Cardiovascular Diseases and Diabetes LEARNING OBJECTIVES Ø Identify the components of the cardiovascular system and the various types of cardiovascular disease Ø Discuss ways of promoting cardiovascular
Can be felt where an artery passes near the skin surface and over a
 1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
Acute Myocardial Infarction. Willis E. Godin D.O., FACC
 Acute Myocardial Infarction Willis E. Godin D.O., FACC Acute Myocardial Infarction Definition: Decreased delivery of oxygen and nutrients to the myocardium Myocardial tissue necrosis causing irreparable
Acute Myocardial Infarction Willis E. Godin D.O., FACC Acute Myocardial Infarction Definition: Decreased delivery of oxygen and nutrients to the myocardium Myocardial tissue necrosis causing irreparable
Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since.
 1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina
 Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Lecture 8 Cardiovascular Health Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors
 Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
10/8/2018. Lecture 9. Cardiovascular Health. Lecture Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor
 Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
AIMS: CHEST PAIN. Causes of chest pain. Causes of chest pain: Cardiac causes: Acute coronary syndromes pericarditis thoracic aortic dissection
 CHEST PAIN Dr Susan Hertzberg Emergency Department Prince of Wales Hospital AIMS: To identify causes of chest pain in patients presenting to the ED. To identify and risk stratify patients presenting with
CHEST PAIN Dr Susan Hertzberg Emergency Department Prince of Wales Hospital AIMS: To identify causes of chest pain in patients presenting to the ED. To identify and risk stratify patients presenting with
MWLCEMS SYSTEM Continuing Education Packet Management of the Acute MI Patient
 MWLCEMS SYSTEM Continuing Education Packet Management of the Acute MI Patient In this CE we will discuss the patient presenting with an acute ST-Elevation Myocardial Infarction (STEMI) Definition: Myocardial
MWLCEMS SYSTEM Continuing Education Packet Management of the Acute MI Patient In this CE we will discuss the patient presenting with an acute ST-Elevation Myocardial Infarction (STEMI) Definition: Myocardial
Cardiac Pathophysiology
 Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Heart Disease. Signs and Symptoms
 Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
Acute coronary syndromes
 Acute coronary syndromes 1 Acute coronary syndromes Acute coronary syndromes results primarily from diminished myocardial blood flow secondary to an occlusive or partially occlusive coronary artery thrombus.
Acute coronary syndromes 1 Acute coronary syndromes Acute coronary syndromes results primarily from diminished myocardial blood flow secondary to an occlusive or partially occlusive coronary artery thrombus.
Acute Myocardial Infarction
 Acute Myocardial Infarction Hafeza Shaikh, DO, FACC, RPVI Lourdes Cardiology Services Asst.Program Director, Cardiology Fellowship Associate Professor, ROWAN-SOM Acute Myocardial Infarction Definition:
Acute Myocardial Infarction Hafeza Shaikh, DO, FACC, RPVI Lourdes Cardiology Services Asst.Program Director, Cardiology Fellowship Associate Professor, ROWAN-SOM Acute Myocardial Infarction Definition:
Objectives. Identify early signs and symptoms of Acute Coronary Syndrome Initiate proper protocol for ACS patient 10/2013 2
 10/2013 1 Objectives Identify early signs and symptoms of Acute Coronary Syndrome Initiate proper protocol for ACS patient 10/2013 2 Purpose of this Education Module: Chest Pain Center Accreditation involves
10/2013 1 Objectives Identify early signs and symptoms of Acute Coronary Syndrome Initiate proper protocol for ACS patient 10/2013 2 Purpose of this Education Module: Chest Pain Center Accreditation involves
Pharmacology. Drugs affecting the Cardiovascular system (Antianginal Drugs)
 Lecture 7 (year3) Dr Noor Al-Hasani Pharmacology University of Baghdad College of dentistry Drugs affecting the Cardiovascular system (Antianginal Drugs) Atherosclerotic disease of the coronary arteries,
Lecture 7 (year3) Dr Noor Al-Hasani Pharmacology University of Baghdad College of dentistry Drugs affecting the Cardiovascular system (Antianginal Drugs) Atherosclerotic disease of the coronary arteries,
Ischemic heart disease
 Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
12 Lead EKG Chapter 4 Worksheet
 Match the following using the word bank. 1. A form of arteriosclerosis in which the thickening and hardening of the vessels walls are caused by an accumulation of fatty deposits in the innermost lining
Match the following using the word bank. 1. A form of arteriosclerosis in which the thickening and hardening of the vessels walls are caused by an accumulation of fatty deposits in the innermost lining
Cardiovascular Disorders. Heart Disorders. Diagnostic Tests for CV Function. Bio 375. Pathophysiology
 Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Ischemic Heart Disease
 Ischemic Heart Disease Definition: Ischemic heart disease (IHD) is a condition in which there is an inadequate supply of blood and oxygen to a portion of the myocardium; it typically occurs when there
Ischemic Heart Disease Definition: Ischemic heart disease (IHD) is a condition in which there is an inadequate supply of blood and oxygen to a portion of the myocardium; it typically occurs when there
Angina Pectoris. Edward JN Ishac, Ph.D. Smith Building, Room
 Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University
Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University
Chapter 14. Cardiovascular Emergencies
 Chapter 14 Cardiovascular Emergencies Introduction (1 of 2) Cardiovascular disease has been leading killer of Americans since 1900. Accounts for 1 of every 2.8 deaths Introduction (2 of 2) EMS can help
Chapter 14 Cardiovascular Emergencies Introduction (1 of 2) Cardiovascular disease has been leading killer of Americans since 1900. Accounts for 1 of every 2.8 deaths Introduction (2 of 2) EMS can help
Coronary Artery Disease & Acute Coronary Syndrome
 Coronary Artery Disease & CAD & ACS Coronary Artery Disease Cardiovascular diseases are the major cause of death in the United States Heart attacks are still the leading cause of all cardiovascular disease
Coronary Artery Disease & CAD & ACS Coronary Artery Disease Cardiovascular diseases are the major cause of death in the United States Heart attacks are still the leading cause of all cardiovascular disease
CHAPTER-I MYOCARDIAL INFARCTION
 CHAPTER-I MYOCARDIAL INFARCTION Definition A myocardial infarction, more commonly known as MI or acute myocardial infarction (AMI) or heart attack is a condition where there is interruption of blood supply
CHAPTER-I MYOCARDIAL INFARCTION Definition A myocardial infarction, more commonly known as MI or acute myocardial infarction (AMI) or heart attack is a condition where there is interruption of blood supply
Ischemic Heart Disease
 Ischemic Heart Disease Dr Rodney Itaki Lecturer Division of Pathology University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology General Consideration Results from partial
Ischemic Heart Disease Dr Rodney Itaki Lecturer Division of Pathology University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology General Consideration Results from partial
Ischaemic heart disease. IInd Chair and Clinic of Cardiology
 Ischaemic heart disease IInd Chair and Clinic of Cardiology Definition Syndrome due to chronic insufficient oxygen supply to myocardial cells Nomenclature: ischaemic heart disease (IHD), coronary artery
Ischaemic heart disease IInd Chair and Clinic of Cardiology Definition Syndrome due to chronic insufficient oxygen supply to myocardial cells Nomenclature: ischaemic heart disease (IHD), coronary artery
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
MYOCARDIALINFARCTION. By: Kendra Fischer
 MYOCARDIALINFARCTION By: Kendra Fischer Outline Definition Epidemiology Clinical Aspects Treatment Effects of Exercise Exercise Testing Exercise Rx Summary and Conclusions References Break it down MYOCARDIAL
MYOCARDIALINFARCTION By: Kendra Fischer Outline Definition Epidemiology Clinical Aspects Treatment Effects of Exercise Exercise Testing Exercise Rx Summary and Conclusions References Break it down MYOCARDIAL
Heart Disease (Coronary Artery Disease)
 Heart Disease (Coronary Artery Disease) Understanding how the heart works To understand heart disease, you must first know how the heart works. The heart is like any other muscle, requiring blood to supply
Heart Disease (Coronary Artery Disease) Understanding how the heart works To understand heart disease, you must first know how the heart works. The heart is like any other muscle, requiring blood to supply
2.5 Circulatory Emergencies. Congestive Heart Failure. Cardiovascular Disease (CVD) Health Services: Unit 2 Circulatory System
 2.5 Circulatory Emergencies In Canada, thousands of people die every year from heart disease and stroke; half of these deaths occur before the patient reaches the hospital. The three major factors contributing
2.5 Circulatory Emergencies In Canada, thousands of people die every year from heart disease and stroke; half of these deaths occur before the patient reaches the hospital. The three major factors contributing
ANGINA PECTORIS. angina pectoris is a symptom of myocardial ischemia in the absence of infarction
 Pharmacology Ezra Levy, Pharm.D. ANGINA PECTORIS A. Definition angina pectoris is a symptom of myocardial ischemia in the absence of infarction angina usually implies severe chest pain or discomfort during
Pharmacology Ezra Levy, Pharm.D. ANGINA PECTORIS A. Definition angina pectoris is a symptom of myocardial ischemia in the absence of infarction angina usually implies severe chest pain or discomfort during
Angina Pectoris Dr. Shariq Syed
 Angina Pectoris Dr. Syed 1 What is Angina Pectoris (AP)? Commonly known as angina is chest pain often due to ischemia of the heart muscle, Because of obstruction or spasm of the coronary arteries 2 What
Angina Pectoris Dr. Syed 1 What is Angina Pectoris (AP)? Commonly known as angina is chest pain often due to ischemia of the heart muscle, Because of obstruction or spasm of the coronary arteries 2 What
Instruct patient and caregivers: Need for constant monitoring Potential complications of drug therapy
 Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Acute Coronary Syndrome. Emergency Department Updated Jan. 2017
 Acute Coronary Syndrome Emergency Department Updated Jan. 2017 Goals and Objectives To reduce mortality and morbidity for people who have cardiovascular disease, with a focus on those who experience an
Acute Coronary Syndrome Emergency Department Updated Jan. 2017 Goals and Objectives To reduce mortality and morbidity for people who have cardiovascular disease, with a focus on those who experience an
Coronary Artery Disease
 Coronary Artery Disease This information is at http://www.nhlbi.nih.gov/health/dci/diseases/cad/cad_all.html and is provided by the NHLBI, one of the Institutes of the National Institutes of Health. To
Coronary Artery Disease This information is at http://www.nhlbi.nih.gov/health/dci/diseases/cad/cad_all.html and is provided by the NHLBI, one of the Institutes of the National Institutes of Health. To
Cardiovascular System and Health. Chapter 15
 Cardiovascular System and Health Chapter 15 Cardiovascular Disease Leading cause of death in U.S. Claims 1 life every 43 seconds Often, the first sign is a fatal heart attack Death Rates #1 CVD #2 Cancer
Cardiovascular System and Health Chapter 15 Cardiovascular Disease Leading cause of death in U.S. Claims 1 life every 43 seconds Often, the first sign is a fatal heart attack Death Rates #1 CVD #2 Cancer
Acute coronary syndrome. Dr LM Murray Chemical Pathology Block SA
 Acute coronary syndrome Dr LM Murray Chemical Pathology Block SA13-2014 Acute myocardial infarction (MI) MI is still the leading cause of death in many countries It is characterized by severe chest pain,
Acute coronary syndrome Dr LM Murray Chemical Pathology Block SA13-2014 Acute myocardial infarction (MI) MI is still the leading cause of death in many countries It is characterized by severe chest pain,
Guide to Cardiology Care at Scripps
 Guide to Cardiology Care at Scripps Cardiology is the word in health care associated with heart, but the body s vascular system is also an important part of heart care. Your body has more than 60,000 miles
Guide to Cardiology Care at Scripps Cardiology is the word in health care associated with heart, but the body s vascular system is also an important part of heart care. Your body has more than 60,000 miles
YOUR GUIDE TO. Understanding Your Angina Diagnosis and Treatment
 YOUR GUIDE TO Understanding Your Angina Diagnosis and Treatment Our goal at the Mercy Health Heart Institute is to help you be well. Our experienced team includes cardiologists, cardiovascular surgeons,
YOUR GUIDE TO Understanding Your Angina Diagnosis and Treatment Our goal at the Mercy Health Heart Institute is to help you be well. Our experienced team includes cardiologists, cardiovascular surgeons,
Myocardial infarction
 CHAPTER-I CARDIOVASCULAR SYSTEM Myocardial infarction SUB: PHARMACOTHERAPEUTICS-I CODE:T0820006 Dr. Venugopal Pharm.D Assistant Professor Department of Pharm.D Kriahna Teja Pharmacy College,Tirupati. Definition
CHAPTER-I CARDIOVASCULAR SYSTEM Myocardial infarction SUB: PHARMACOTHERAPEUTICS-I CODE:T0820006 Dr. Venugopal Pharm.D Assistant Professor Department of Pharm.D Kriahna Teja Pharmacy College,Tirupati. Definition
Chp. 5 The cardiovascular system. What are the function of the cardiovascular system? Arteries and arterioles:
 5.1 Overview of the cardiovascular system Chp. 5 The cardiovascular system Includes the heart and blood vessels Brings nutrients to cells and helps get rid of wastes Blood is refreshed in the lung, kidneys,
5.1 Overview of the cardiovascular system Chp. 5 The cardiovascular system Includes the heart and blood vessels Brings nutrients to cells and helps get rid of wastes Blood is refreshed in the lung, kidneys,
Cardiovascular Concerns in Intermediate Care
 Cardiovascular Concerns in Intermediate Care GINA ST. JEAN RN, MSN, CCRN-CSC CLINICAL NURSE EDUCATOR HEART AND & CRITICAL AND INTERMEDIATE CARE Objectives: Identify how to do a thorough assessment of the
Cardiovascular Concerns in Intermediate Care GINA ST. JEAN RN, MSN, CCRN-CSC CLINICAL NURSE EDUCATOR HEART AND & CRITICAL AND INTERMEDIATE CARE Objectives: Identify how to do a thorough assessment of the
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to
 Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
BUSINESS. Articles? Grades Midterm Review session
 BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
Management of Stable Ischemic Heart Disease. Vinay Madan MD February 10, 2018
 Management of Stable Ischemic Heart Disease Vinay Madan MD February 10, 2018 1 Disclosure No financial disclosure. 2 Overview of SIHD Diagnosis Outline of talk Functional vs. Anatomic assessment Management
Management of Stable Ischemic Heart Disease Vinay Madan MD February 10, 2018 1 Disclosure No financial disclosure. 2 Overview of SIHD Diagnosis Outline of talk Functional vs. Anatomic assessment Management
Quinn Capers, IV, MD
 Heart Attacks Mended Hearts Presentation, January, 2017 Quinn Capers, IV, MD Associate Professor of Medicine (Cardiovascular Medicine) Director, Transradial Coronary Interventions Division of Cardiovascular
Heart Attacks Mended Hearts Presentation, January, 2017 Quinn Capers, IV, MD Associate Professor of Medicine (Cardiovascular Medicine) Director, Transradial Coronary Interventions Division of Cardiovascular
THE HEART THE CIRCULATORY SYSTEM
 THE HEART THE CIRCULATORY SYSTEM There are three primary closed cycles: 1) Cardiac circulation pathway of blood within the heart 2) Pulmonary circulation blood from the heart to lungs and back 3) Systemic
THE HEART THE CIRCULATORY SYSTEM There are three primary closed cycles: 1) Cardiac circulation pathway of blood within the heart 2) Pulmonary circulation blood from the heart to lungs and back 3) Systemic
Pathophysiology of Cardiovascular System. Dr. Hemn Hassan Othman, PhD
 Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
When the learner has completed this module, she/he will be able to:
 Thrombolytics and Myocardial Infarction WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017
Thrombolytics and Myocardial Infarction WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017
Cardiac Emergencies. Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington
 Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
Our Commitment to Quality and Patient Safety Core Measures
 Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
Wellness: Concepts and Applications 8 th Edition Anspaugh, Hamrick, Rosato
 Wellness: Concepts and Applications 8 th Edition Anspaugh, Hamrick, Rosato Preventing Cardiovascular Disease Chapter 2 Cardiovascular Disease the leading cause of death in the U.S. 35.3% of all deaths
Wellness: Concepts and Applications 8 th Edition Anspaugh, Hamrick, Rosato Preventing Cardiovascular Disease Chapter 2 Cardiovascular Disease the leading cause of death in the U.S. 35.3% of all deaths
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Section 5.1 The heart and heart disease
 Section 5.1 The heart and heart disease Mammals are too large to rely on diffusion. They need a circulatory system to move substances around the body. Blood moves down pressure gradients, from high to
Section 5.1 The heart and heart disease Mammals are too large to rely on diffusion. They need a circulatory system to move substances around the body. Blood moves down pressure gradients, from high to
CORONARY ARTERY DISEASE OVERVIEW
 CORONARY ARTERY DISEASE OVERVIEW Your heart is a strong muscular pump that is responsible for moving about 3,000 gallons of blood through your body every day. Like other muscles, your heart requires a
CORONARY ARTERY DISEASE OVERVIEW Your heart is a strong muscular pump that is responsible for moving about 3,000 gallons of blood through your body every day. Like other muscles, your heart requires a
Cardiac Pathology & Rehabilitation
 Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
Care of the Patient with a Cardiovascular or a Peripheral Vascular Disorder
 Care of the Patient with a Cardiovascular or a Peripheral Vascular Disorder 1 Slide 1 human heart Slide 2 MECHANICAL: PUSHES BLOOD FROM HEAD TO TOES AND BACK Slide 3 1 ELECTRICAL SYSTEM: TRIGGERS THE MECHANICAL
Care of the Patient with a Cardiovascular or a Peripheral Vascular Disorder 1 Slide 1 human heart Slide 2 MECHANICAL: PUSHES BLOOD FROM HEAD TO TOES AND BACK Slide 3 1 ELECTRICAL SYSTEM: TRIGGERS THE MECHANICAL
Cho et al., 2009 Journal of Cardiology (2009), 54:
 Endothelial Dysfunction, Increased Carotid Artery Intima-media Thickness and Pulse Wave Velocity, and Increased Level of Inflammatory Markers are Associated with Variant Angina Cho et al., 2009 Journal
Endothelial Dysfunction, Increased Carotid Artery Intima-media Thickness and Pulse Wave Velocity, and Increased Level of Inflammatory Markers are Associated with Variant Angina Cho et al., 2009 Journal
HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM
 REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900.
 1 2 3 4 5 6 Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900. Accounts for of every 3 deaths Cardiovascular disease
1 2 3 4 5 6 Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900. Accounts for of every 3 deaths Cardiovascular disease
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist. Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI
 Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist physician Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI Outcome objectives of the discussion: At the end of the
Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist physician Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI Outcome objectives of the discussion: At the end of the
Cardiovascular Disease in Women over 50. Jessie Fazel, Kristin Jeschke, and Teresa Taylor. University of Kansas School of Nursing
 Cardiovascular Disease in Women over 50 Jessie Fazel, Kristin Jeschke, and Teresa Taylor University of Kansas School of Nursing 48 Cardiovascular Disease in Women over 50 Cardiovascular disease is the
Cardiovascular Disease in Women over 50 Jessie Fazel, Kristin Jeschke, and Teresa Taylor University of Kansas School of Nursing 48 Cardiovascular Disease in Women over 50 Cardiovascular disease is the
Acute Coronary Syndrome. Sonny Achtchi, DO
 Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
Drug Treatment of Ischemic Heart Disease
 Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE School of Medicine, The University of Jordan November, 2017 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE School of Medicine, The University of Jordan November, 2017 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Cardiovascular Disease Risk Factors:
 Cardiovascular Disease Risk Factors: Risk factors are traits or habits that increase a person's chances of having cardiovascular disease. Some risk factors can be changed. These risk factors are high blood
Cardiovascular Disease Risk Factors: Risk factors are traits or habits that increase a person's chances of having cardiovascular disease. Some risk factors can be changed. These risk factors are high blood
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI).
 1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
Cardiovascular Emergencies. Chapter 12
 Cardiovascular Emergencies Chapter 12 Cardiovascular Emergencies Cardiovascular disease (CVD) claimed 931,108 lives in the US during 2001. 2,551 per day Almost two people per minute! CVD accounts for 38.5%
Cardiovascular Emergencies Chapter 12 Cardiovascular Emergencies Cardiovascular disease (CVD) claimed 931,108 lives in the US during 2001. 2,551 per day Almost two people per minute! CVD accounts for 38.5%
BLOOD PRESSURE. Unit 3: Transportation and Respiration
 BLOOD PRESSURE Unit 3: Transportation and Respiration Blood Pressure The force of your blood pushing on the walls of your arteries. How is Blood Pressure Measured? Measured at an artery in the arm and
BLOOD PRESSURE Unit 3: Transportation and Respiration Blood Pressure The force of your blood pushing on the walls of your arteries. How is Blood Pressure Measured? Measured at an artery in the arm and
1. What additional information needs to be collected to properly treat this client?
 CASE 1 A 45-year-old male presents to the emergency department with a complaint of chest pain for the past two hours. 1. What additional information needs to be collected to properly treat this client?
CASE 1 A 45-year-old male presents to the emergency department with a complaint of chest pain for the past two hours. 1. What additional information needs to be collected to properly treat this client?
Acute Coronary Syndromes
 Overview Acute Coronary Syndromes Rabeea Aboufakher, MD, FACC, FSCAI Section Chief of Cardiology Altru Health System Grand Forks, ND Epidemiology Pathophysiology Clinical features and diagnosis STEMI management
Overview Acute Coronary Syndromes Rabeea Aboufakher, MD, FACC, FSCAI Section Chief of Cardiology Altru Health System Grand Forks, ND Epidemiology Pathophysiology Clinical features and diagnosis STEMI management
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
WHI Form Report of Cardiovascular Outcome Ver (For items 1-11, each question specifies mark one or mark all that apply.
 WHI Form - Report of Cardiovascular Outcome Ver. 6. COMMENTS To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: OMB# 095-044 Exp: 4/06 -Affix label here- Clinical Center/ID:
WHI Form - Report of Cardiovascular Outcome Ver. 6. COMMENTS To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: OMB# 095-044 Exp: 4/06 -Affix label here- Clinical Center/ID:
Heart failure congestive heart failure, or CHF
 Heart failure Heart failure (also called congestive heart failure, or CHF) is a frequent end point of many of the conditions In the United States alone, CHF affects nearly 5 million individuals annually,
Heart failure Heart failure (also called congestive heart failure, or CHF) is a frequent end point of many of the conditions In the United States alone, CHF affects nearly 5 million individuals annually,
Ischemic Heart Diseases. Dr. Nabila Hamdi MD, PhD
 Ischemic Heart Diseases Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast the different types of angina regarding their pathogenesis, clinical manifestations and evolution. Discuss myocardial infarct,
Ischemic Heart Diseases Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast the different types of angina regarding their pathogenesis, clinical manifestations and evolution. Discuss myocardial infarct,
Term-End Examination December, 2009 MCC-006 : CARDIOVASCULAR EPIDEMIOLOGY
 MCC-006 POST GRADUATE DIPLOMA IN CLINICAL CARDIOLOGY (PGDCC) 00269 Term-End Examination December, 2009 MCC-006 : CARDIOVASCULAR EPIDEMIOLOGY Time : 2 hours Maximum Marks : 60 Note : There will be multiple
MCC-006 POST GRADUATE DIPLOMA IN CLINICAL CARDIOLOGY (PGDCC) 00269 Term-End Examination December, 2009 MCC-006 : CARDIOVASCULAR EPIDEMIOLOGY Time : 2 hours Maximum Marks : 60 Note : There will be multiple
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
Circulation and Cardiac Emergencies. Emergency Medical Response
 Circulation and Cardiac Emergencies Lesson 19: The Circulatory System and Cardiac Emergencies You Are the Emergency Medical Responder You are called to the home of a 50-year-old man whose wife called 9-1-1
Circulation and Cardiac Emergencies Lesson 19: The Circulatory System and Cardiac Emergencies You Are the Emergency Medical Responder You are called to the home of a 50-year-old man whose wife called 9-1-1
WHAT IS ATHEROSCLEROSIS?
 ATHEROSCLEROSIS WHAT IS ATHEROSCLEROSIS? Atherosclerosis is a narrowing of the arteries that can significantly reduce the blood supply to vital organs such as the heart, brain and intestines. In atherosclerosis,
ATHEROSCLEROSIS WHAT IS ATHEROSCLEROSIS? Atherosclerosis is a narrowing of the arteries that can significantly reduce the blood supply to vital organs such as the heart, brain and intestines. In atherosclerosis,
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
Cardiovascular System Notes: Heart Disease & Disorders
 Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
P F = R. Disorder of the Breast. Approach to the Patient with Chest Pain. Typical Characteristics of Angina Pectoris. Myocardial Ischemia
 Disorder of the Breast Approach to the Patient with Chest Pain Anthony J. Minisi, MD Department of Internal Medicine, Division of Cardiology Virginia Commonwealth University School of Medicine William
Disorder of the Breast Approach to the Patient with Chest Pain Anthony J. Minisi, MD Department of Internal Medicine, Division of Cardiology Virginia Commonwealth University School of Medicine William
Cardiovascular Disease
 Cardiovascular Disease Chapter 15 Introduction Cardiovascular disease (CVD) is the leading cause of death in the U.S. One American dies from CVD every 33 seconds Nearly half of all Americans will die from
Cardiovascular Disease Chapter 15 Introduction Cardiovascular disease (CVD) is the leading cause of death in the U.S. One American dies from CVD every 33 seconds Nearly half of all Americans will die from
Chest Pain Accreditation ACS Education
 Chest Pain Accreditation ACS Education Objectives Recognize the Typical and Atypical Signs and Symptoms of ACS Recognize Gender and Age Differences of ACS Recognize the Risk Factors of ACS Understand Early
Chest Pain Accreditation ACS Education Objectives Recognize the Typical and Atypical Signs and Symptoms of ACS Recognize Gender and Age Differences of ACS Recognize the Risk Factors of ACS Understand Early
Myocardial Infarction
 Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Chapter (9) Calcium Antagonists
 Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Unit 1: Human Systems. The Circulatory System
 Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Cardiovascular and Respiratory Disorders
 Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
CORONARY ARTERY BYPASS GRAFT
 CORONARY ARTERY BYPASS GRAFT Coronary artery disease develops because of hardening of the arteries (arteriosclerosis) that supply blood to the heart muscle. In the diagnosis of coronary artery disease,
CORONARY ARTERY BYPASS GRAFT Coronary artery disease develops because of hardening of the arteries (arteriosclerosis) that supply blood to the heart muscle. In the diagnosis of coronary artery disease,
It is what you will see most in practice and what you need to know thoroughly.
 Acute Myocardial Infarction: Pre-hospital Issues 2 CEUs By: Michelle E. Duffelmeyer, MD INTRODUCTION An in depth review of the pathophysiology, symptomatology, and treatment modalities for acute MI. It
Acute Myocardial Infarction: Pre-hospital Issues 2 CEUs By: Michelle E. Duffelmeyer, MD INTRODUCTION An in depth review of the pathophysiology, symptomatology, and treatment modalities for acute MI. It
Strokes , The Patient Education Institute, Inc. hp Last reviewed: 11/11/2017 1
 Strokes Introduction A stroke or a brain attack is a very serious condition that can result in death and significant disability. This disease is ranked as the third leading cause of death in the United
Strokes Introduction A stroke or a brain attack is a very serious condition that can result in death and significant disability. This disease is ranked as the third leading cause of death in the United
Cardiac Drugs: Chapter 9 Worksheet Cardiac Agents. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate.
 Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Health and Disease of the Cardiovascular system
 1 Health and Disease of the Cardiovascular system DR CHRIS MOORE Instructions 2 USE THE ARROWS TO NAVIGATE, OR TAP OUTLINE AT THE TOP TO BRING DOWN A SLIDE MENU Click these where you see them to zoom or
1 Health and Disease of the Cardiovascular system DR CHRIS MOORE Instructions 2 USE THE ARROWS TO NAVIGATE, OR TAP OUTLINE AT THE TOP TO BRING DOWN A SLIDE MENU Click these where you see them to zoom or
