of Aorta-to-Coronary Artery
|
|
|
- Baldric Merritt
- 5 years ago
- Views:
Transcription
1 Reoperation Following Clinical Failure of Aorta-to-Coronary Artery Bypass Vein Grafts Maurice Adam, M.D., Gerald F. Geisler, M.D., Cary J. Lambert, M.D., and Ben F. Mitchel, Jr., M.D. ABSTRACT In the past four years the authors have used 1,360 saphenous vein grafts (SVG) in the treatment of 600 patients with coronary artery disease. In 19 patients reoperation was carried out. The SVG occlusions were related to distal obstructions or to fibrotic and inflammatory changes around the SVG and at times were unrelated to detectable causes. The presence of both closed and open vein grafts in some of the patients suggests that SVG obstructions are probably due to local causes and, it is hoped, are nonrecurring in most instances. Primary SVG failure may be related to local vein factors such as ischemic or mechanical trauma, and efforts to avoid these are strongly recommended. Of the 17 survivors, 14 had excellent results or were improved clinically following reoperation, and we have concluded that reoperation is safe and effective in achieving ultimate success in those patients in whom distal arterial runoff is adequate. Recurring angina demands prompt restudy and corrective operation when possible. Treatment of postpericardiotomy syndromes with corticoids and avoidance or evacuation of mediastinal hematomas are important. R eversed autogenous saphenous vein bypass grafting has become the procedure of choice in the treatment of myocardial ischemia in both established angina and preinfarction syndromes [l, 2, 81. It serves to alleviate angina, it improves myocardial work load tolerance, and it may protect against later myocardial infarction. Some subsequent clinical failures must inevitably occur on the basis of progression of the patient s arterial disease. However, primary failure of the saphenous vein graft (SVG) also occurs. The prevention of such failures is an important surgical goal, but solution awaits clear definition of the etiology of SVG closure. Studies done over a number of years in femoral-to-popliteal artery bypass graft procedures [3-61 indicate that though clinical failure may often be due to pathological conditions within the vein graft rather than to progressive arterial disease, vein bypass grafts in fact have considerable resistance to failure under such adverse circumstances as distal arterial obstruction. More recently, Johnson, Auer, and Tector [71 have described changes of intimal thickening within vein grafts leading to their obstruc- From the Departments of Thoracic and Cardiovascular Surgery, Baylor University Medical Center, St. Paul Hospital, and The University of Texas Southwestern Medical School, Dallas, Tex. Presented at the Eighth Annual Meeting of The Society of Thoracic Surgeons, San Francisco, Calif., Jan , Address reprint requests to Dr. Adam, 3434 Swiss Ave., Dallas, Tex THE ANNALS OF THORACIC SURGERY
2 Reoperation Following Vein Graft Failure tion, and this has been suggested by Vlodaver and Edwards [lo] to be due to a water hammer effect secondary to poor runoff under conditions of unaccustomed pressure within the veins. Other modes of failure include SVG thrombosis, suture granulomas, and technical errors. Clinical Material In the past four years the authors have used 1,360 aorta-to-coronary artery bypass vein grafts in the treatment of 600 patients with coronary artery disease. Of these, 82% have had good long-term results [2]. Interestingly, some of these patients have one or more occluded vein grafts but have maintained a good clinical status on the basis of residual patent grafts or infarction. The exact number is not known because the asymptomatic patients are not routinely studied by repeat coronary angiography. On the other hand, those becoming symptomatic again are restudied. In a few of these, all grafts were found to be open and the condition of the arteries unchanged. In others, vein graft narrowing or occlusion had appeared in one of several grafts or in all the grafts. Arterial disease had progressed in some patients. In 19 of the 600 patients we believed reoperation was indicated. The purpose of this study is to analyze this group of 19 patients in order to establish the results obtainable by reoperation techniques, to try to get some idea of the incidence of arterial disease progression, and to determine the reasons for graft failure when possible. The patients, 3 women and 16 men, ranged in age from 34 to 64 years. The reoperations were done from 1 to 28 months following the initial procedure. The criteria for operability were the same as those established for the initial procedure in these patients [I, 81, namely, the presence of angina, the presence of significant anatomical arterial or SVG obstruction, and the demonstration of an adequate runoff below an area suitable for grafting. Most of the patients had good ventricular contractility and were in reasonably stable condition, but there were exceptions. Table 1 groups the patients according to what was considered their most noteworthy characteristic immediately preceding the second operation. Reoperation was performed in a manner basically identical to the ini- TABLE 1. STATUS BEFORE REOPERATION IN 19 PATIENTS WITH FAILURE OF CORONARY SVG No. of Status Patients Reasonably stable, good ventricular contractility 13 Reasonably stable, poor ventricular contractility 1 Preinfarction syndrome 1 Acute myocardial infarction 12 to 24 hours previously 2 Healed dehiscence of sternotomy 1 VOL. 14, NO. 3, SEPTEMBER,
3 ADAM ET AL. tial procedure. This consisted of using total cardiopulmonary bypass, with hemodilution technique maintaining the hematocrit at 30% or better; moderate hypothermia of 30" to 32 C.; intentional electric fibrillation; the use of left ventricular apical venting as necessary; and anastomosis with either continuous 6-0 Ethiflex or interrupted 6-0 silk sutures. Aortic cross-clamping for periods up to 20 minutes was also used. The operating time and the time spent on bypass are both increased in reoperation. Besides the presence of the expected adhesions and the care necessary to insure protection of the functioning vein grafts, there may be a problem in reopening the sternum. The right atrium or right ventricle may be densely adherent to the sternum, leading to severe blood loss from opening these chambers. By prior exposure of the femoral artery and heparinization, cannulation of the femoral artery may be done, if needed, to return all the collected blood encountered at this awkward moment. Such a system was necessary in 3 of our patients. The findings at reoperation were interesting. In some, only light adhesions were present. Occasionally, dense scar had formed, possibly representing organized mediastinal hematoma. Those veins which were patent at the time of reoperation were soft and very similar in appearance to fresh veins. Some were thicker, yet soft and flexible. Closed vein grafts were firm, full-feeling, and rubbery or sometimes were found to be flattened and soft, as if collapsed. The entire length of an occluded vein was not always demonstrable. The sites of anastomosis were usually patent, especially at the veinto-coronary artery end. Restoration of flow in closed grafts was by interposition of a new vein graft into the patent stub of the occluded graft or into a new site on the same artery as before. The choice was dictated by arteriographic and operative findings. Treatment after operation included continuing endotracheal intubation and respirator support overnight, antibiotic coverage, digitalis and diuretic therapy, and antiarrhythmic management as necessary. After oral intake was resumed, aspirin and Persantine were used for their action in minimizing platelet agglutination and associated thrombosis. The course of events in the 19 patients was extremely varied and complex. In order to properly assess and study the problems leading to reoperation, one must consider the status of the original 58 arteries and the initial management of the 38 diseased arteries, then follow the changes which took place with the passage of time and at the time of reoperation (Table 2). Of 12 arteries that had been considered normal at the original operation, 5 demonstrated advancing obstructive disease which led to treatment by vein grafting at the second operation (see Table 2). Eight arteries listed as untreated were recognized as having disease thought to be subcritical or which was treated by internal mammary artery implantation. At the subsequent operation, 7 of these had either demonstrated progression of the obstructive phenomena or were still considered to need a proper revascular- 274 THE ANNALS OF THORACIC SURGERY
4 Reoperation Following Vein Graft Failure TABLE 2. FLOW SHEET OF GRAFT AND ARTERY CHANGES IN 19 REOPERATED PATIENTS Initial Management Preoperative Management Status Just Prior at Second Status of at First to Second Operation Artery Operation Operation If Treated 12 normal arteries No treatment 7 normal 5 critical stenoses 4 vein grafts; 1 vein graft & distal endarterectomy 8 subcritical stenoses No treatment 1 subcritical (< 75%) stenosis 7 critical stenoses 8 vein grafts 38 critical stenoses 35 vein grafts 12 open vein (> 75%) grafts 23 closed vein 21 vein grafts; 2 grafts not treatedarteries too diseased 2 endarterectomies 1 open endarterectomy 1 closed 1 vein graft endarterectomy 1 endarterectomy 1 open vein graft and proximal into distal vein graft endarterectomy ization procedure, and these were treated in 6 instances with vein bypass grafts and in 1 instance by distal endarterectomy with proximal vein bypass graft. Of the 35 arteries initially treated by vein grafting, 12 had remained open and 23 showed vein graft closure. Twenty-one of these were treated by repeat vein grafting and 2 were left untreated due to severely advancing distal arterial disease. Two vessels initially had been endarterectomized; 1 of these had remained open and 1 had closed, and the latter was managed successfully with a vein graft. The 1 vessel originally treated by endarterectomy and proximal vein grafting was open at the time of the second operation. Thus, failures were attributable to advancing arterial disease in untreated arteries, advancing arterial disease in treated arteries, and to vein graft failure occurring primarily. It was noted frequently that in a single patient, vein graft closure had occurred in only 1 of 2 or in 2 of 3 vein grafts. Among the 23 SVG failures, it was frequently noted that the aortic and arterial ends of the vein grafts were still widely patent; and, in most instances, the closure of the SVG could and did occur in such a way as to leave uncompromised the preexisting arterial situation. Although occluded veins VOL. 14, NO. 3, SEPTEMBER,
5 ADAM ET AL. TABLE 3. TYPE OF VEIN GRAFT FAILURE AND RELATED FACTORS IN 19 REOPERATED PATIENTS FIP & Encased Pathological Condition Thrombosis Thrombosis in Scar Obstruction distal to vein graft Severe fibrosis & inflammation around graft Neither of above FIP = fibrous intimal proliferation. usually were obstructed throughout their entire length except at each end, there was some variation in the gross and microscopical appearance of the veins. Two veins were encased in extremely heavy mediastinal scar tissue and were not identifiable within this mass of scar. Of the remaining vessels, 7 appeared to show thrombosis as the major occluding factor and 14 showed various degrees of fibrous intimal proliferative change, usually with some thrombus centrally. Table 3 lists the number of patients having each observed occlusive process, divided into three categories representing associated phenomena observed in the patients, One sees that both distal runoff obstruction and severe inflammatory disease or fibrosis around the graft appear to be related to the formation of severe fibrous intimal proliferative changes. R esu 1 ts The results of reoperation (Table 4) are comparable to the results obtained with the initial Of the 19 patients, 14 showed excellent or improved results and 2 were unchanged; there were 2 operative deaths and 1 late death. Both operative deaths occurred in patients who had had acute infarction 12 to 24 hours previously and who thus would have been difficult patients for an initial operation as well as a reoperation. The late death occurred in a patient with severe congestive heart failure who had improved clinically following triple bypass vein grafting but in whom failure had recurred; restudy had demonstrated closure of 1 of the 3 grafts. Reoperation was followed by sternal dehiscence, continuing congestive heart failure, and death three months postoperatively. A postmortem examination was not obtained, but it was believed that a myocardiopathy had probably been a significant component in the patient s clinical difficulties. The 2 patients not helped by reoperation were both men with early, severe, and rapidly progressive arteriosclerosis. One, aged 34, had had early closure of 2 vein grafts at two months postoperatively. An endarterectomy, initially open, had closed at twenty-one months. Severe progression of his distal arterial disease was shown at restudy, and at reoperation, severe mediastinal fibrosis was observed and reaction about the graft was extreme. 276 THE ANNALS OF THORACIC SURGERY
6 Reoperation Following Vein Graft Failure TABLE 4. RESULTS OF REOPERATION IN 19 PATIENTS WITH FAILURE OF CORONARY SVG No. of Result Patients Remarks Excellent 11 Asymptomatic without medication & working Improved 3 Working, some symptoms, some Unchanged 2 medication Rapid progression of arteriosclerotic heart disease Operative deaths 2 Acute preoperative infarctions Late deaths 1 Congestive heart failure Total 19 After reoperation, mediastinitis and sternal dehiscence occurred, and very early reclosure of his grafts was observed. The other unaided patient was 47 years old. Restudy showed extreme stenosis distal to the left anterior descending coronary artery graft with patency of the right coronary and circumflex grafts. Reoperation with bridging of the distal lesion was done, but a later study showed marked further progression of distal disease and closure of the grafts. Treatment with streptokinase was undertaken; it failed to reopen the grafts but, surprisingly, did partly reopen 2 of the 3 blocked arteries. One wonders if disseminated intravascular coagulation in a mild form might not have been present. Comment When autogenous vein grafts are placed in the arterial tree in human beings, they undergo changes of thickening, or arterialization. This thickening tends to involve all the coats of the vessel but is primarily intimal and chiefly composed of fibrous tissue [5]. Wyatt and Taylor [11] have clearly shown the deleterious effects of trauma, either of a mechanical nature or that produced by 90 minutes of irrigation with saline solution, in producing increased amounts of fibrous intimal proliferation. Overton and Owen [91 have demonstrated that ischemia can produce fibrous intimal proliferation and fibrous medial proliferation as well. Downs [6], in examining 7 patients undergoing femoropopliteal reoperation for stenosis and obstruction of vein grafts, found fibrous intimal proliferation to be the cause of obstruction in 2 of his 7 patients, while in 5 others the cause was listed as valve stenosis and described as being fibrosis of the valve cusps. This would seem to us to be a localized form of the same process of fibrous intimal proliferation. Interestingly, the degree of fibrous intimal proliferation seen in arterialized vein grafts has not frequently been reported as the chief cause of failure except by Johnson and associates [7]. Downs [6] believes this is a more likely primary VOL. 14, NO. 3, SEPTEMBER,
7 ADAM ET AL. cause when the veins are small, and he, as well as others, tends to find a degree of fibrous intimal proliferation together with a final thrombosis as the ultimate cause for obstruction. Vlodaver and Edwards [lo] have described the pathological features of the process of intimal proliferation, and from their study of postmortem specimens and the consistent finding of distal arterial disease, they have concluded that the distal obstruction produces a water hammer effect which aggravates the effect of the arterial pressure to produce unusual degrees of fibrous intimal proliferation and subsequent vein obstruction. If this theory is true, subsequent study should show an increased incidence of fibrous intimal proliferation in hypertensive patients. On theoretical grounds only, it is our belief that injury to the vein wall-chiefly to the intima-is the primary cause of serious intimal proliferative obstructive phenomena and that probably ischemia is the chief type of trauma encountered in coronary surgery patients. We propose that ischemia may be produced by drying and by excessively long soaking of the vein in saline solution prior to use or that it may be produced by scarring around the SVG through interference with the vasa vasorum and the partial failure to develop an adequate blood supply to the vein wall. Distal obstructive disease may also be contributory, but the data seem weak in this regard. In line with these thoughts, we have increasingly tried to avoid trauma in the harvesting of veins for use as grafts. We try to avoid drying the veins, we make every attempt to tie branches in such a way that the closed branch provides no pocket or puckering, and we try to see that valves are not cut in any way when the veins are trimmed for anastomosis. In order to minimize inflammatory changes around the SVG, we treat diagnosed postpericardiotomy syndrome with steroids in a vigorous manner and try to avoid mediastinal hematoma by extremely careful hemostasis and by using minimal dissection upon entering. There is some likelihood that increasing attention should be given to arteries which have less than critical stenosis present at the time of operation. Placing a graft about such a stenosed vessel before the condition become more critical may minimize the number of patients needing to be reoperated upon for advancing arterial changes in untreated subcritically stenotic vessels. Those patients requiring only single and double bypass grafts and with apparently normal remaining vessels will undoubtedly continue to show some degeneration due to advancing arterial disease in the untreated vessels. Reoperation fortunately is available for these people and can prevent possibly disastrous consequences when done promptly. Early restudy of all patients in whom angina recurs is strongly recommended. The use in the postoperative period of antiplatelet-agglutination agents such as aspirin and Persantine may contribute to a diminution in thrombotic failure of vein grafts and may minimize local buildup of platelet and 278 THE ANNALS OF THORACIC SURGERY
8 Reoperation Following Vein Graft Failure fibrous tissue at the site of local vein injury, particularly if used during the period prior to establishment of a completely smooth inner lining of the vein. References 1. Adam, M., Mitchel, B. F., and Lambert, C. J. Immediate revascularization of the heart. Circulation (Suppl. II):73, Adam, M., Mitchel, B. F., Lambert, C. J., and Geisler, G. F. Long-term results with aorta-to-coronary artery bypass vein grafts. Ann. Thorac. Surg. 14:1, Beebe, H. G., Clark, W. F., and DeWeese, J. A. Atherosclerotic change occurring in an autogenous venous arterial graft. Arch. Surg. 101:85, DeWeese, J. A., and Rob, C. G. Autogenous venous bypass grafts five years later. Ann. Surg. 174:3, DeWeese, J. A., Terry, R., Barner, H. B., and Rob, C. G. Autogenous venous femoropopliteal bypass grafts. Surgery 59:28, Downs, A. R. Repair of late vein graft occlusions. Arch. Surg. 103:639, Johnson, W. D., Auer, J. E., and Tector, A. J. Late changes in coronary vein grafts. Am. J. Cardiol. 26:640, Mitchel, B. F., Adam, M., Lambert, C. J., Sungu, U., and Shiekh, S. Ascending aorta-to-coronary artery saphenous vein bypass grafts. J. Thorac. Cardiovase. Surg. 60:457, Overton, J. H., and Owen, E. R. The successful replacement of minute arteries. Surgery 68 : 7 13, Vlodaver, Z., and Edwards, J. E. Pathologic changes in aortic-coronary arterial saphenous vein grafts. Circulation 44:719, Wyatt, A. P., and Taylor, G. W. Vein grafts: Changes in the endothelium of autogenous free vein grafts used as arterial replacements. Br. J. Surg. 53:945, Discussion DR. ROBERT G. CARISON (New York, N.Y.): It takes a brave surgeon to stand up and talk about his bad results. Actually, he had very good results with reoperations. At Cornell University we had one lesson that we would like to share with you. My SVG patency rate at two weeks is 90% in coronary arteries with a lumen of 1.5 mm. or greater. One patient who had patent double vein grafts two weeks postoperatively had routine follow-u angiograms six months later. This asymptomatic patient demonstrated a pseu Ioaneurysm f of the ascending aorta at the site of the aorta-to-vein graft anastomosis, and the left coronary artery was occluded. I excised the pseudoaneurysm. When the aneurysm and the segment of occluded SVG had been removed, the distal portion of that same graft to the anterior descending coronary artery was widely patent. Copious blood flowed retrogradely through this previously occluded SVG. A 1-inch-long vein graft was anastomosed between the ascending aorta and the previously occluded vein graft. At the same time, I bypassed a mild stenosis of the right vein graft. Two weeks after reoperation, the grafts were patent by angiogram. This pseudoaneurysm may have been due to slippery polyethylene sutures used for the anastomosis or to weakening of the aortic wall by the partially occluding clamp. Another possibility was that the angiography catheter may have weakened or pierced the anastomosis site two weeks postoperatively and allowed the pseudoaneurysm to form. VOL. 14, NO. 3, SEPTEMBER,
9 ADAM ET AL. DR. WILLIAM J. KERTH (San Francisco, Calif.): There is no doubt that aortato-coronary artery bypass SVG is a quantum step in coronary artery surgery. Until they are eliminated, however, late occlusions will probably preclude the extension of this procedure to the essentially asymptomatic patient who is at high risk of sudden death from severe coronary atherosclerosis. Information like that presented by the authors may well give clues to the reasons for late closure and lead to its prevention. I have some data on 8 patients who were reoperated upon at Pacific Medical Center in San Francisco following venous aorta-to-coronary artery bypass grafting. When we first began doing this work in February, 1968, we excised the valves in the veins of the first 7 patients, and I think that was the cause of occlusion in 1 patient, who had to be operated upon twice. In the second reoperation a reversed graft was used, and I believe this patient s vein is still open, as she has a normal treadmill test. One cause of proximal stenosis, particularly of a left bypass, is inadequate size of the proximal anastomosis. Initially we did not excise a large button of aortic tissue but only a small triangle. In January of 1970 we began to do arteriograms about two weeks after operation on all patients who had this operation, followed a year later by another bypass arteriogram and coronary arteriogram. Therefore, in all these patients except the first, we have early postoperative studies showing the technical adequacy of both the proximal and the distal anastomosis. One patient, the same one whose bypass was wide open both proximally and distally, developed a very severe proximal stenosis of the vein, down to only a pinpoint opening. The distal vein was wide open on early restudy; the distal anastomosis was fine. There was, however, intense intimal hyperplasia of the aortic anastomosis site eight months postoperatively. For the past two years we have examined control veins. We take a segment of vein at the time of coronary bypass and send it to the pathologist so we have something to compare the graft with if there is subsequent trouble. Also, by analyzing the early and late postoperative studies on patients whose grafts have remained opened, we have found that the vein does tend to shrink and that the left anterior descending SVG generally gets pulled up to some extent. On the right side we believe that the SVG does tend to tent up the distal right coronary artery unless the vein is made redundant at the initial operation. This tenting then may well lead to some funneling or turbulence at the distal anastomosis. We now make, as I indicated earlier, a very large proximal anastomosis, as large as the diameter of the vein or perhaps a little larger. We have seen at least 1 patient with a very intense external fibrous reaction around the proximal site of the aortic anastomosis, so much that the vein was encased in cement and was, I believe, kinked by intense scar. There are other reasons which we are not aware of now for this condition. We hope that with further study this will be a solvable problem. We are currently treating all our patients with aspirin postoperatively to attempt to prevent platelet deposition on the anastomosis. We have abandoned the use of heparin and Coumadin in the postoperative period, as they did not seem to make any difference. We also have a series of more than 20 patients in whom we kept the vein in situ until just before the anastomosis was made, thinking that ischemia may have been the cause for this reaction. The postoperative studies in these patients really are quite comparable as far as the amount of narrowing or shrinking of the veins, so I don t believe that that is the problem. DR. ADAM: As far as this search for the cause of SVG failure, I see that we are not the only ones still baffled. The pseudoaneurysm demonstrated by Dr. Carlson was well managed. Anas- 280 THE ANNALS OF THORACIC SURGERY
10 Reoperation Following Vein Graft Failure tomotic bleeding more often results in early reexploration for suture control or, as in 1 of our patients, in death from hemorrhage. Dr. Kerth s demonstration of excised valves and other local problems tends to strengthen my feeling about vein trauma being the cause of difficulties. With regard to the proximal anastomosis, we use a rather large cobra-head anastomosis with a slit in the aorta, and we think two factors are important in this. One is not to have the incision too long in the aorta, because that stretches the cobra head flat when it opens up; so one has to make it short enough to suit if the vein is small. Second, one can see when it is finished that the full lumen of the vein is available for entry, and we have not had much trouble with proximal anastomoses. We too believe that shrinkage of the vein is likely and have therefore used the loop application of vein with a generous length. We also use aspirin and Persantine postoperatively (for an indeterminate period as yet) and hope this will prevent early failure until the veins develop a smooth inner lining. VOL. 14, NO. 3, SEPTEMBER,
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Results of Reoperation
 Results of Reoperation for Recurrent Angina Pectoris William I. Norwood, M.D., Lawrence H. Cohn, M.D., and John J. Collins, Jr., M.D. ABSTRACT Although a coronary bypass operation improves the quality
Results of Reoperation for Recurrent Angina Pectoris William I. Norwood, M.D., Lawrence H. Cohn, M.D., and John J. Collins, Jr., M.D. ABSTRACT Although a coronary bypass operation improves the quality
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST
 CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
Arterial Diseases & Grafts What Can Go Wrong and How to Fix It
 Arterial Diseases & Grafts What Can Go Wrong and How to Fix It Lecture #9 Ref: Harloff, Jan, Are Biomaterials the Limiting Factor in the Progress of Arterial Prosthesis? Termpaper, BE 512, introduction
Arterial Diseases & Grafts What Can Go Wrong and How to Fix It Lecture #9 Ref: Harloff, Jan, Are Biomaterials the Limiting Factor in the Progress of Arterial Prosthesis? Termpaper, BE 512, introduction
Tehnique for Using Soft, Flexible Catheter Stents in Aortocoronary Vein Bypass Operations
 Tehnique for Using Soft, Flexible Catheter Stents in Aortocoronary Vein Bypass Operations Louis G. Ludington, M.D., George Kafrouni, M.D., Merle H. Peterson, M.D., Joseph J. Verska, M.D., G. Arnold Mulder,
Tehnique for Using Soft, Flexible Catheter Stents in Aortocoronary Vein Bypass Operations Louis G. Ludington, M.D., George Kafrouni, M.D., Merle H. Peterson, M.D., Joseph J. Verska, M.D., G. Arnold Mulder,
Surgical Management of the Preinfarction Syndrome
 Surgical Management of the Preinfarction Syndrome Ernest A. Traad, M.D., Parry B. Larsen, M.D., Thomas 0. Gentsch, M.D., Arthur J. Gosselin, M.D., and Paul S. Swaye, M.D. ABSTRACT The indications for coronary
Surgical Management of the Preinfarction Syndrome Ernest A. Traad, M.D., Parry B. Larsen, M.D., Thomas 0. Gentsch, M.D., Arthur J. Gosselin, M.D., and Paul S. Swaye, M.D. ABSTRACT The indications for coronary
Mechanical Bleeding Complications During Heart Surgery
 Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
CORONARY ARTERY BYPASS GRAFT
 CORONARY ARTERY BYPASS GRAFT Coronary artery disease develops because of hardening of the arteries (arteriosclerosis) that supply blood to the heart muscle. In the diagnosis of coronary artery disease,
CORONARY ARTERY BYPASS GRAFT Coronary artery disease develops because of hardening of the arteries (arteriosclerosis) that supply blood to the heart muscle. In the diagnosis of coronary artery disease,
ATHEROSCLEROSIS. Secondary changes are found in other coats of the vessel wall.
 ATHEROSCLEROSIS Atherosclerosis Atherosclerosis is a disease process affecting the intima of the aorta and large and medium arteries, taking the form of focal thickening or plaques of fibrous tissue and
ATHEROSCLEROSIS Atherosclerosis Atherosclerosis is a disease process affecting the intima of the aorta and large and medium arteries, taking the form of focal thickening or plaques of fibrous tissue and
Disease of the aortic valve is frequently associated with
 Stentless Aortic Bioprosthesis for Disease of the Aortic Valve, Root and Ascending Aorta John R. Doty, MD, and Donald B. Doty, MD Disease of the aortic valve is frequently associated with morphologic abnormalities
Stentless Aortic Bioprosthesis for Disease of the Aortic Valve, Root and Ascending Aorta John R. Doty, MD, and Donald B. Doty, MD Disease of the aortic valve is frequently associated with morphologic abnormalities
Management during Reoperation of Aortocoronary Saphenous Vein Grafts with Minimal Atherosclerosis by Angiography
 Management during Reoperation of ortocoronary Saphenous Vein Grafts with therosclerosis by ngiography William G. Marshall, Jr., M.D., Jeffrey Saffitz, M.D., and Nicholas T. Kouchoukos, M.D. STRCT The proper
Management during Reoperation of ortocoronary Saphenous Vein Grafts with therosclerosis by ngiography William G. Marshall, Jr., M.D., Jeffrey Saffitz, M.D., and Nicholas T. Kouchoukos, M.D. STRCT The proper
Further Evaluation. Technique of Coronary Artery Bypass. of the Circular Sequential Vein Graft
 Further Evaluation of the Circular Sequential Vein Graft Technique of Coronary Artery Bypass Joseph C. Cleveland, M.D., Ira M. Lebenson, M.D., Robert J. Twohey, M.D., Joseph G. Ellis, M.D., Daniel B. Nelson,
Further Evaluation of the Circular Sequential Vein Graft Technique of Coronary Artery Bypass Joseph C. Cleveland, M.D., Ira M. Lebenson, M.D., Robert J. Twohey, M.D., Joseph G. Ellis, M.D., Daniel B. Nelson,
TSDA ACGME Milestones
 TSDA ACGME Milestones Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short
TSDA ACGME Milestones Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short
Angiographic 5-Year Follow-up Study of Right Gastroepiploic Artery Grafts
 Angiographic 5-Year Follow-up Study of Right Gastroepiploic Artery Grafts Sari Voutilainen, MD, Kalervo Verkkala, MD, PhD, Antero J~irvinen, MD, PhD, and Pekka Keto, MD, PhD Departments of Thoracic and
Angiographic 5-Year Follow-up Study of Right Gastroepiploic Artery Grafts Sari Voutilainen, MD, Kalervo Verkkala, MD, PhD, Antero J~irvinen, MD, PhD, and Pekka Keto, MD, PhD Departments of Thoracic and
Combat Extremity Vascular Trauma
 Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Direct Coronary Surgery Utilizing Multiple-Vein Bypass Grafts
 Direct Coronary Surgery Utilizing Multiple-Vein Bypass Grafts W. Dudley Johnson, M.D., Robert J. Flemma, M.D., and Derward Lepley, Jr., M.D. P revious angiographic and pathological studies have shown that
Direct Coronary Surgery Utilizing Multiple-Vein Bypass Grafts W. Dudley Johnson, M.D., Robert J. Flemma, M.D., and Derward Lepley, Jr., M.D. P revious angiographic and pathological studies have shown that
Calcified Aortic Sinotubular Ridge: A Source of Coronary Ostial Stenosis or Embolism
 1510 JACC Vol. 12, No, 6 December 1988:1510--4 Calcified Aortic Sinotubular Ridge: A Source of Coronary Ostial Stenosis or Embolism KEVIN J. TVETER, MD, JESSE E. EDWARDS, MD, FACC St, Paul, Minnesota This
1510 JACC Vol. 12, No, 6 December 1988:1510--4 Calcified Aortic Sinotubular Ridge: A Source of Coronary Ostial Stenosis or Embolism KEVIN J. TVETER, MD, JESSE E. EDWARDS, MD, FACC St, Paul, Minnesota This
A Loeys-Dietz Patient with a Trans-Atlantic Odyssey. Repeated Aortic Root Surgery ending with a Huge Left Main Coronary Aneurysm 4
 1 2 3 A Loeys-Dietz Patient with a Trans-Atlantic Odyssey Repeated Aortic Root Surgery ending with a Huge Left Main Coronary Aneurysm 4 5 6 7 8 9 Thierry Carrel 1, Florian Schoenhoff 1 and Duke Cameron
1 2 3 A Loeys-Dietz Patient with a Trans-Atlantic Odyssey Repeated Aortic Root Surgery ending with a Huge Left Main Coronary Aneurysm 4 5 6 7 8 9 Thierry Carrel 1, Florian Schoenhoff 1 and Duke Cameron
Management of Fusiform Ascending Aortic Aneurysms
 Management of Fusiform Ascending Aortic Aneurysms Stuart Houser, M.D., Jose Mijangos, M.D., Amarenda Sengupta, M.D., Lawrence Zaroff, M.D., Robert Weiner, M.D., and James A. DeWeese, M.D. ABSTRACT Thirteen
Management of Fusiform Ascending Aortic Aneurysms Stuart Houser, M.D., Jose Mijangos, M.D., Amarenda Sengupta, M.D., Lawrence Zaroff, M.D., Robert Weiner, M.D., and James A. DeWeese, M.D. ABSTRACT Thirteen
Pathophysiology of Cardiovascular System. Dr. Hemn Hassan Othman, PhD
 Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
1 Description. 2 Indications. 3 Warnings ASPIRATION CATHETER
 Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
Aneurysms & a Brief Discussion on Embolism
 Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
14 Valvular Stenosis
 14 Valvular Stenosis 14-1. Valvular Stenosis unicuspid valve FIGUE 14-1. This photograph shows severe valvular stenosis as it occurs in a newborn. There is a unicuspid, horseshoe-shaped leaflet with a
14 Valvular Stenosis 14-1. Valvular Stenosis unicuspid valve FIGUE 14-1. This photograph shows severe valvular stenosis as it occurs in a newborn. There is a unicuspid, horseshoe-shaped leaflet with a
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D.
 CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
Ischemic heart disease
 Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Distal Coronary Artery Dissection Following Percutaneous Transluminal Coronary Angioplasty
 Distal Coronary rtery Dissection Following Percutaneous Transluminal Coronary ngioplasty Douglas. Murphy, M.D., Joseph M. Craver, M.D., and Spencer. King 111, M.D. STRCT The most common cause of acute
Distal Coronary rtery Dissection Following Percutaneous Transluminal Coronary ngioplasty Douglas. Murphy, M.D., Joseph M. Craver, M.D., and Spencer. King 111, M.D. STRCT The most common cause of acute
The Healing Characteristics of Autogenous Saphenous Vein Used in the Reconstruction of Previouslv Implanted Arterial Saphenous Vein Grafts
 The Healing Characteristics of Autogenous Saphenous Vein Used in the Reconstruction of Previouslv Implanted Arterial Saphenous Vein Grafts Karl J. Karlson, M.D., M.M.S., Robert Brescia, M.D., and Hassan
The Healing Characteristics of Autogenous Saphenous Vein Used in the Reconstruction of Previouslv Implanted Arterial Saphenous Vein Grafts Karl J. Karlson, M.D., M.M.S., Robert Brescia, M.D., and Hassan
The arterial switch operation has been the accepted procedure
 The Arterial Switch Procedure: Closed Coronary Artery Transfer Edward L. Bove, MD The arterial switch operation has been the accepted procedure for the repair of transposition of the great arteries (TGA)
The Arterial Switch Procedure: Closed Coronary Artery Transfer Edward L. Bove, MD The arterial switch operation has been the accepted procedure for the repair of transposition of the great arteries (TGA)
10/8/2018. Lecture 9. Cardiovascular Health. Lecture Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor
 Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
Coronary Artery from the Wrong Sinus of Valsalva: A Physiologic Repair Strategy
 Coronary Artery from the Wrong Sinus of Valsalva: A Physiologic Repair Strategy Tom R. Karl, MS, MD he most commonly reported coronary artery malformation leading to sudden death in children and young
Coronary Artery from the Wrong Sinus of Valsalva: A Physiologic Repair Strategy Tom R. Karl, MS, MD he most commonly reported coronary artery malformation leading to sudden death in children and young
and Paul C. Taylor, M.D. ORIGINAL ARTICLES
 ORIGINAL ARTICLES Trends in Selection and Results of Coronary Artery Reoperations Floyd D. Loop, M.D., Bruce W. Lytle, M.D., Carl C. Gill, M.D., Leonard A. R. Golding, M.D., Delos M. Cosgrove, M.D., and
ORIGINAL ARTICLES Trends in Selection and Results of Coronary Artery Reoperations Floyd D. Loop, M.D., Bruce W. Lytle, M.D., Carl C. Gill, M.D., Leonard A. R. Golding, M.D., Delos M. Cosgrove, M.D., and
Right Coronary Artery With Anomalous Origin and Slit Ostium
 Right Coronary Artery With Anomalous Origin and Slit Ostium Raul Garcia Rinaldi, MO, Jorge Carballido, MO, Richard Giles, MO, Emilio Del Taro, MO, and Raul Porro, MO Departments of Cardiovascular Surgery
Right Coronary Artery With Anomalous Origin and Slit Ostium Raul Garcia Rinaldi, MO, Jorge Carballido, MO, Richard Giles, MO, Emilio Del Taro, MO, and Raul Porro, MO Departments of Cardiovascular Surgery
Carotid Stenosis (carotid artery disease)
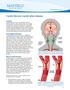 1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
The management of chronic thromboembolic pulmonary
 Technique of Pulmonary Thromboendarterectomy Isabelle Opitz, MD, and Marc de Perrot, MD, MSc, FRCSC Toronto Pulmonary Endarterectomy Program, Toronto General Hospital, Ontario, Canada. Address reprint
Technique of Pulmonary Thromboendarterectomy Isabelle Opitz, MD, and Marc de Perrot, MD, MSc, FRCSC Toronto Pulmonary Endarterectomy Program, Toronto General Hospital, Ontario, Canada. Address reprint
False Aneurvsm and Pseudo-False Aneurysm of the Left qentricle: ~tiology, Pathology; Diagnosis, and Operative Management
 False Aneurvsm and Pseudo-False Aneurysm of the Left qentricle: ~tiology, Pathology; Diagnosis, and Operative Management S. Stewart, M.D., R. Huddle, M.D., I. Stuard, M.D., B. F. Schreiner, M.D., and J.
False Aneurvsm and Pseudo-False Aneurysm of the Left qentricle: ~tiology, Pathology; Diagnosis, and Operative Management S. Stewart, M.D., R. Huddle, M.D., I. Stuard, M.D., B. F. Schreiner, M.D., and J.
Review of 131 Consecutive Patients Gerald F. Geisler, M.D., Maurice Adam, M.D., Ben F. Mitchel, M.D., Cary J. Lambert, M.D., and J. Peter Thiele, M.D.
 Treatment of Severe Coronary Artery Disease with 5, 6, and 7 Saphenous Vein Bypasses: Review of 131 Consecutive Patients Gerald F. Geisler, M.D., Maurice Adam, M.D., Ben F. Mitchel, M.D., Cary J. Lambert,
Treatment of Severe Coronary Artery Disease with 5, 6, and 7 Saphenous Vein Bypasses: Review of 131 Consecutive Patients Gerald F. Geisler, M.D., Maurice Adam, M.D., Ben F. Mitchel, M.D., Cary J. Lambert,
Late Results with Autogenous
 Late Results with Autogenous Tissue Heart Valves W. Sterling Edwards, M.D. ABSTRACT Five years of experience using unsupported and mounted fascia lata and pericardial heart valves in human beings is summarized.
Late Results with Autogenous Tissue Heart Valves W. Sterling Edwards, M.D. ABSTRACT Five years of experience using unsupported and mounted fascia lata and pericardial heart valves in human beings is summarized.
Ab H. Boontje, M.D., Ph.D., Groningen, Holland
 Aneurysm formation in human umbilical vein grafts used as arterial substitutes Ab H. Boontje, M.D., Ph.D., Groningen, Holland A series of 257 human umbilical vein grafts for femoropopliteal bypass in 203
Aneurysm formation in human umbilical vein grafts used as arterial substitutes Ab H. Boontje, M.D., Ph.D., Groningen, Holland A series of 257 human umbilical vein grafts for femoropopliteal bypass in 203
AN ATOMY OF THE CARDIOVASCULAR SYSTEM
 Student Name CHAPTER 18 AN ATOMY OF THE CARDIOVASCULAR SYSTEM T he heart is actually two pumps one moves blood to the lungs, the other pushes it out into the body. These two functions seem rather elementary
Student Name CHAPTER 18 AN ATOMY OF THE CARDIOVASCULAR SYSTEM T he heart is actually two pumps one moves blood to the lungs, the other pushes it out into the body. These two functions seem rather elementary
Surgical Options for revascularisation P E T E R S U B R A M A N I A M
 Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Pathology of Cardiovascular Interventions. Body and Disease 2011
 Pathology of Cardiovascular Interventions Body and Disease 2011 Coronary Artery Atherosclerosis Intervention Goals: Acute Coronary Syndromes: Treat plaque rupture and thrombosis Significant Disease: Prevent
Pathology of Cardiovascular Interventions Body and Disease 2011 Coronary Artery Atherosclerosis Intervention Goals: Acute Coronary Syndromes: Treat plaque rupture and thrombosis Significant Disease: Prevent
Transluminal Stent-graft Placement endovascular surgery
 13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
Lecture 8 Cardiovascular Health Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors
 Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Heart may be rotated but not compressed
 Tips And Techniques For Multivessel OPCAB John D. Puskas, MD, Emory University, Atlanta AATS Adult Cardiac Skills April 28, 2012 San Francisco, CA Beating Heart Surgery vs Beat The Heart Surgery OPCAB
Tips And Techniques For Multivessel OPCAB John D. Puskas, MD, Emory University, Atlanta AATS Adult Cardiac Skills April 28, 2012 San Francisco, CA Beating Heart Surgery vs Beat The Heart Surgery OPCAB
Aberrant Right Subclavian Artery Aneurysm
 Aberrant Right Subclavian Artery William S. Stoney, M.D., William C. Alford, Jr., M.D., George R. Burrus, M.D., and Clarence S. Thomas, Jr., M.D. ABSTRACT Ten patients with aneurysm of an aberrant right
Aberrant Right Subclavian Artery William S. Stoney, M.D., William C. Alford, Jr., M.D., George R. Burrus, M.D., and Clarence S. Thomas, Jr., M.D. ABSTRACT Ten patients with aneurysm of an aberrant right
Post-Op Aorta: Differentiating Normal Post-Op vs. Complications. Linda C. Chu, MD Assistant Professor of Radiology Johns Hopkins University
 Post-Op Aorta: Differentiating Normal Post-Op vs. Complications Linda C. Chu, MD Assistant Professor of Radiology Johns Hopkins University No disclosures Disclosures Goals and Objectives To review CT technique
Post-Op Aorta: Differentiating Normal Post-Op vs. Complications Linda C. Chu, MD Assistant Professor of Radiology Johns Hopkins University No disclosures Disclosures Goals and Objectives To review CT technique
Aortocoronary Bypass in the Treatment of Left Main Coronary Artery Stenosis
 Aortocoronary Bypass in the Treatment of Left Main Coronary Artery Stenosis W. C. Alford, Jr., M.D., I. J. Shaker, M.D., C. S. Thomas, Jr., M.D., W. S. Stoney, M.D., G. R. Burrus, M.D., and H. L. Page,
Aortocoronary Bypass in the Treatment of Left Main Coronary Artery Stenosis W. C. Alford, Jr., M.D., I. J. Shaker, M.D., C. S. Thomas, Jr., M.D., W. S. Stoney, M.D., G. R. Burrus, M.D., and H. L. Page,
Complete Proximal Occlusion of All Three Main Coronary Arteries Complicated With a Left Main Coronary Aneurysm: A Case Report
 J Cardiol 2004 Nov; 44 5 : 201 205 Complete Proximal Occlusion of All Three Main Coronary Arteries Complicated With a Left Main Coronary Aneurysm: A Case Report Takatoshi Hiroshi Akira Takahiro Masayasu
J Cardiol 2004 Nov; 44 5 : 201 205 Complete Proximal Occlusion of All Three Main Coronary Arteries Complicated With a Left Main Coronary Aneurysm: A Case Report Takatoshi Hiroshi Akira Takahiro Masayasu
Management of Ascending Aortic
 Management of Ascending Aortic Aneurysm Complicating Coarctation of the Aorta Ramanathan Sampath, M.D., William N. O'Connor, M.D., Jacqueline A. Noonan, M.D., and Edward P. Todd, M.D., Ph.D. ABSTRACT Four
Management of Ascending Aortic Aneurysm Complicating Coarctation of the Aorta Ramanathan Sampath, M.D., William N. O'Connor, M.D., Jacqueline A. Noonan, M.D., and Edward P. Todd, M.D., Ph.D. ABSTRACT Four
Ascending Aortic Associated Aortic. Aneurysms with Regurgitation. Koger K. Stenlund, M.D., Charles K. Peterson, M.D.
 Ascending Aortic Associated Aortic Aneurysms with Regurgitation Hovald K. Helseth, M.D., John J. Haglin, M.D., Koger K. Stenlund, M.D., Charles K. Peterson, M.D., and David W. Gauger, M.D. ABSTRACT A safe
Ascending Aortic Associated Aortic Aneurysms with Regurgitation Hovald K. Helseth, M.D., John J. Haglin, M.D., Koger K. Stenlund, M.D., Charles K. Peterson, M.D., and David W. Gauger, M.D. ABSTRACT A safe
1 Functions of endothelial cells include all the following EXCEPT. 2 Response to vascular injury is characterised by
 airns ase Hospital mergency epartment Part 1 FM MQs 1 Functions of endothelial cells include all the following XPT Formation of von-willebrand factor Formation of collagen and proteoglycans Formation of
airns ase Hospital mergency epartment Part 1 FM MQs 1 Functions of endothelial cells include all the following XPT Formation of von-willebrand factor Formation of collagen and proteoglycans Formation of
CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY
 Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
Adult Cardiac Surgery
 Adult Cardiac Surgery Mahmoud ABU-ABEELEH Associate Professor Department of Surgery Division of Cardiothoracic Surgery School of Medicine University Of Jordan Adult Cardiac Surgery: Ischemic Heart Disease
Adult Cardiac Surgery Mahmoud ABU-ABEELEH Associate Professor Department of Surgery Division of Cardiothoracic Surgery School of Medicine University Of Jordan Adult Cardiac Surgery: Ischemic Heart Disease
and Coronary Artery Surgery George M. Callard, M.D., John B. Flege, Jr., M.D., and Joseph C. Todd, M.D.
 Combined Valvular and Coronary Artery Surgery George M. Callard, M.D., John B. Flege, Jr., M.D., and Joseph C. Todd, M.D. ABSTRACT Between July, 97, and March, 975,45 patients underwent combined valvular
Combined Valvular and Coronary Artery Surgery George M. Callard, M.D., John B. Flege, Jr., M.D., and Joseph C. Todd, M.D. ABSTRACT Between July, 97, and March, 975,45 patients underwent combined valvular
Pulmonary Valve Replacement
 Pulmonary Valve Replacement with Fascia Lata J. C. R. Lincoln, F.R.C.S., M. Geens, M.D., M. Schottenfeld, M.D., and D. N. Ross, F.R.C.S. ABSTRACT The purpose of this paper is to describe a technique of
Pulmonary Valve Replacement with Fascia Lata J. C. R. Lincoln, F.R.C.S., M. Geens, M.D., M. Schottenfeld, M.D., and D. N. Ross, F.R.C.S. ABSTRACT The purpose of this paper is to describe a technique of
CASE REPORT. Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea. G. A. Lopez, M.D., and A. R. C. Dobell, M.D.
 CASE REPORT Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea G. A. Lopez, M.D., and A. R. C. Dobell, M.D. ABSTRACT A patient developed a mycotic aneurysm of the aortic suture line after aortic
CASE REPORT Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea G. A. Lopez, M.D., and A. R. C. Dobell, M.D. ABSTRACT A patient developed a mycotic aneurysm of the aortic suture line after aortic
Importance of the third arterial graft in multiple arterial grafting strategies
 Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
Anatomic variants of the normal coronary artery circulation
 Diagnosis and Operation for Anomalous Circumflex Coronary Artery Keishi Ueyama, MD, PhD, Mahesh Ramchandani, MD, Arthur C. Beall, Jr, MD, and James W. Jones, MD, PhD Department of Surgery, Baylor College
Diagnosis and Operation for Anomalous Circumflex Coronary Artery Keishi Ueyama, MD, PhD, Mahesh Ramchandani, MD, Arthur C. Beall, Jr, MD, and James W. Jones, MD, PhD Department of Surgery, Baylor College
Coronary Artery Stenosis Following Aortic Valve Replacement and Intermittent Intracoronary Cardioplegia
 Coronary Artery Stenosis Following Aortic Valve Replacement and Intermittent Intracoronary Cardioplegia D. Glenn Pennington, M.D., Bulent Dincer, M.D., Hind Bashiti, M.D., Hendrick B. Barner, M.D., George
Coronary Artery Stenosis Following Aortic Valve Replacement and Intermittent Intracoronary Cardioplegia D. Glenn Pennington, M.D., Bulent Dincer, M.D., Hind Bashiti, M.D., Hendrick B. Barner, M.D., George
Distribution Of Grafts In Aortocoronary Bypass Surgery: Cardiovascular Surgery Fellowship Experience.
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 17 Number 1 Distribution Of Grafts In Aortocoronary Bypass Surgery: Cardiovascular Surgery Fellowship Experience. J C Eze Citation
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 17 Number 1 Distribution Of Grafts In Aortocoronary Bypass Surgery: Cardiovascular Surgery Fellowship Experience. J C Eze Citation
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Competitive Blood Flow in the- Coronary Circulation Simulating Progression of Proximal Coronary Artery Disease After Saphenous Vein Bypass Surgery*
 Clin. Cardiol. 7, 179-183 (1984) @ Clinical Cardiology Publishing Co., Inc. Competitive Blood Flow in the- Coronary Circulation Simulating Progression of Proximal Coronary Artery Disease After Saphenous
Clin. Cardiol. 7, 179-183 (1984) @ Clinical Cardiology Publishing Co., Inc. Competitive Blood Flow in the- Coronary Circulation Simulating Progression of Proximal Coronary Artery Disease After Saphenous
Use of polytetrafluoroethylene renal bypass
 Use of polytetrafluoroethylene renal bypass grafts for P. Lagneau, M.D., J. B. Michel, M.D., and J. M. Charrat, M.D., Paris, France Fifty-six revascularizations of the renal arteries were performed in
Use of polytetrafluoroethylene renal bypass grafts for P. Lagneau, M.D., J. B. Michel, M.D., and J. M. Charrat, M.D., Paris, France Fifty-six revascularizations of the renal arteries were performed in
Myocardial Infarction
 Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Further Studies on the Effect of Arteriovenous Fistulas and Elevations of Sinus Pressure
 Further Studies on the Effect of Arteriovenous Fistulas and Elevations of Sinus Pressure on Mortality Rates Following Acute Coronary Occlusions By GEORGE SMITH, F.R.C.S., JAMES DEMMING, MORTON ELEFF, AND
Further Studies on the Effect of Arteriovenous Fistulas and Elevations of Sinus Pressure on Mortality Rates Following Acute Coronary Occlusions By GEORGE SMITH, F.R.C.S., JAMES DEMMING, MORTON ELEFF, AND
THROMBOSIS. Dr. Nisreen Abu Shahin Assistant Professor of Pathology Pathology Department University of Jordan
 THROMBOSIS Dr. Nisreen Abu Shahin Assistant Professor of Pathology Pathology Department University of Jordan NORMAL BLOOD VESSEL HISTOLOGY THROMBOSIS Pathogenesis (called Virchow's triad): 1. Endothelial*
THROMBOSIS Dr. Nisreen Abu Shahin Assistant Professor of Pathology Pathology Department University of Jordan NORMAL BLOOD VESSEL HISTOLOGY THROMBOSIS Pathogenesis (called Virchow's triad): 1. Endothelial*
Carotid Stenosis 1/24/2019. Review of Primary Studies. NASCET- Moderate stenosis. ACAS (Asymptomatic Carotid Atherosclerosis Study) NASCET
 Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial
 An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial wall (intima, media, and adventitia) or the attenuated
An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial wall (intima, media, and adventitia) or the attenuated
Coronary artery anatomy:-
 ISCHEMIC HEART DISEASE- CORONARY ARTERY REVASCULARIZATION We will talk about coronary artery bypass grafting from surgical aspects, since the subject is mainly medical, in cardiac surgery the patient come
ISCHEMIC HEART DISEASE- CORONARY ARTERY REVASCULARIZATION We will talk about coronary artery bypass grafting from surgical aspects, since the subject is mainly medical, in cardiac surgery the patient come
REBEL. Platinum Chromium Coronary Stent System. Patient Information Guide
 REBEL Patient Information Guide REBEL PATIENT INFORMATION GUIDE You have recently had a REBEL bare metal stent implanted in the coronary arteries of your heart. The following information is important for
REBEL Patient Information Guide REBEL PATIENT INFORMATION GUIDE You have recently had a REBEL bare metal stent implanted in the coronary arteries of your heart. The following information is important for
Demonstration of Uneven. the infusion on myocardial temperature was insufficient
 Demonstration of Uneven in Patients with Coronary Lesions Rolf Ekroth, M.D., HAkan erggren, M.D., Goran Sudow, M.D., Josef Wojciechowski, M.D., o F. Zackrisson, M.D., and Goran William-Olsson, M.D. ASTRACT
Demonstration of Uneven in Patients with Coronary Lesions Rolf Ekroth, M.D., HAkan erggren, M.D., Goran Sudow, M.D., Josef Wojciechowski, M.D., o F. Zackrisson, M.D., and Goran William-Olsson, M.D. ASTRACT
AORTIC DISSECTIONS Current Management. TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida
 AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
In 1980, Bex and associates 1 first introduced the initial
 Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Distal radial artery lesion as a source of digital emboli
 Distal radial artery lesion as a source of digital emboli G. Matthew Longo, MD, Andrew C. Friedman, MD, Ronald R. Hollins, MD, Cary J. Buresh, MD, and B. Timothy Baxter, MD, Omaha, Neb Ischemic changes
Distal radial artery lesion as a source of digital emboli G. Matthew Longo, MD, Andrew C. Friedman, MD, Ronald R. Hollins, MD, Cary J. Buresh, MD, and B. Timothy Baxter, MD, Omaha, Neb Ischemic changes
Partial anomalous pulmonary venous connection to superior
 Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Left Ventricular Wall Resection for Aneurysm and Akinesia due to Coronary Artery Disease: Fifty Consecutive Patients
 Left Ventricular Wall Resection for Aneurysm and Akinesia due to Coronary Artery Disease: Fifty Consecutive Patients Armand A. Lefemine, M.D., Rajagopalan Govindarajan, M.D., K. Ramaswamy, M.D., Harrison
Left Ventricular Wall Resection for Aneurysm and Akinesia due to Coronary Artery Disease: Fifty Consecutive Patients Armand A. Lefemine, M.D., Rajagopalan Govindarajan, M.D., K. Ramaswamy, M.D., Harrison
The most important advantage of CABG over PTCA is its
 Coronary Artery Bypass With Only In Situ Bilateral Internal Thoracic Arteries and Right Gastroepiploic Artery Hiroshi Nishida, MD; Yasuko Tomizawa, MD; Masahiro Endo, MD; Hitoshi Koyanagi, MD; Hiroshi
Coronary Artery Bypass With Only In Situ Bilateral Internal Thoracic Arteries and Right Gastroepiploic Artery Hiroshi Nishida, MD; Yasuko Tomizawa, MD; Masahiro Endo, MD; Hitoshi Koyanagi, MD; Hiroshi
Perfusion for Repair of Aneurysms of the Transverse Aortic Arch
 technique This new section is open for technicians to explore the unusual, the difficult, the innovative methods by which perfusion meets the challenge of the hour and produces the ultimate goal - a life
technique This new section is open for technicians to explore the unusual, the difficult, the innovative methods by which perfusion meets the challenge of the hour and produces the ultimate goal - a life
Χρόνιος διαχωρισμός. υπερηχοκαρδιογραφική. αορτής. παρακολούθηση ή άλλη; Α. Παπασπυρόπουλος ΕΠΙΜΕΛΗΤΗΣ ΓΝ.ΝΙΚΑΙΑΣ ΠΕΜΠΤΗ
 Χρόνιος διαχωρισμός αορτής υπερηχοκαρδιογραφική παρακολούθηση ή άλλη; Α. Παπασπυρόπουλος ΕΠΙΜΕΛΗΤΗΣ ΓΝ.ΝΙΚΑΙΑΣ ΠΕΜΠΤΗ 8-2-2018 The Normal Aorta (conduit function + control ) *Aortic expansion is about
Χρόνιος διαχωρισμός αορτής υπερηχοκαρδιογραφική παρακολούθηση ή άλλη; Α. Παπασπυρόπουλος ΕΠΙΜΕΛΗΤΗΣ ΓΝ.ΝΙΚΑΙΑΣ ΠΕΜΠΤΗ 8-2-2018 The Normal Aorta (conduit function + control ) *Aortic expansion is about
THE BLOOD VESSELS. Manar hajeer, MD University of Jordan Faculty of medicine, pathology department.
 THE BLOOD VESSELS Manar hajeer, MD University of Jordan Faculty of medicine, pathology department. Vascular pathology: 1- Narrowing or complete obstruction of vessel lumina, either progressively (e.g.,
THE BLOOD VESSELS Manar hajeer, MD University of Jordan Faculty of medicine, pathology department. Vascular pathology: 1- Narrowing or complete obstruction of vessel lumina, either progressively (e.g.,
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept
 The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept Professor Christoph A. Nienaber The Royal Brompton and Harefield NHS Trust Cardiology and Aortic Centre
The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept Professor Christoph A. Nienaber The Royal Brompton and Harefield NHS Trust Cardiology and Aortic Centre
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion
 Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Arthroplasty after previous surgery: previous vascular problems
 Arthroplasty after previous surgery: previous vascular problems Jacques Menetrey & Victoria B. Duthon Centre de médecine de l appareil locomoteur et du sport Swiss Olympic medical Center Unité d Orthopédie
Arthroplasty after previous surgery: previous vascular problems Jacques Menetrey & Victoria B. Duthon Centre de médecine de l appareil locomoteur et du sport Swiss Olympic medical Center Unité d Orthopédie
IMAGES. in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
CORONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW
 CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW 2015 PQRS OPTIONS F MEASURES GROUPS: 2015 PQRS MEASURES IN CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP: #43 Coronary Artery Bypass Graft (CABG):
CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW 2015 PQRS OPTIONS F MEASURES GROUPS: 2015 PQRS MEASURES IN CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP: #43 Coronary Artery Bypass Graft (CABG):
Publicado : Interactive CardioVascular Thoracic Surgery 2011;12:650.
 Pulmonary embolism due to biological glue after repair of type A aortic dissection Jose Rubio Alvarez,MD, PhD, 1 Juan Sierra Quiroga, MD, PhD, 1 Anxo Martinez de Alegria MD 2, Jose-Manuel Martinez Comendador,
Pulmonary embolism due to biological glue after repair of type A aortic dissection Jose Rubio Alvarez,MD, PhD, 1 Juan Sierra Quiroga, MD, PhD, 1 Anxo Martinez de Alegria MD 2, Jose-Manuel Martinez Comendador,
Mandatory knowledge about natural history of coronary grafts. P.Sergeant P. Maureira K.U.Leuven, Belgium
 Mandatory knowledge about natural history of coronary grafts P.Sergeant P. Maureira K.U.Leuven, Belgium Types of grafts Arterial ITA/IMA (internal thoracic/mammary artery) Radial artery Gastro-epiploïc
Mandatory knowledge about natural history of coronary grafts P.Sergeant P. Maureira K.U.Leuven, Belgium Types of grafts Arterial ITA/IMA (internal thoracic/mammary artery) Radial artery Gastro-epiploïc
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Introduction. Risk factors of PVD 5/8/2017
 PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
Animesh Rathore, MD 4/21/17. Penetrating atherosclerotic ulcers of aorta
 Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
Vasculature and innervation of the heart. A. Bendelic Human Anatomy Department
 Vasculature and innervation of the heart A. Bendelic Human Anatomy Department Plan: 1. Arterial blood supply of the heart. Coronary arteries 2. Venous drainage of the heart. Cardiac veins 3. Innervation
Vasculature and innervation of the heart A. Bendelic Human Anatomy Department Plan: 1. Arterial blood supply of the heart. Coronary arteries 2. Venous drainage of the heart. Cardiac veins 3. Innervation
Anomalous Left Main Coronary Artery: Not Always a Simple Surgical Reimplantation
 Cardiol Ther (2015) 4:77 82 DOI 10.1007/s40119-015-0039-x CASE REPORT Anomalous Left Main Coronary Artery: Not Always a Simple Surgical Reimplantation Asif H. Khan. Ian B. A. Menown. Alastair Graham. John
Cardiol Ther (2015) 4:77 82 DOI 10.1007/s40119-015-0039-x CASE REPORT Anomalous Left Main Coronary Artery: Not Always a Simple Surgical Reimplantation Asif H. Khan. Ian B. A. Menown. Alastair Graham. John
The pericardial sac is composed of the outer fibrous pericardium
 Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Intervention for Lower Extremity PAD: When, why and what?! Robert F Cuff, MD FACS RVT RPVI
 Intervention for Lower Extremity PAD: When, why and what?! Robert F Cuff, MD FACS RVT RPVI 1 Disclosures I have no financial disclosures related to this talk Objectives 1. Discuss indications for intervention
Intervention for Lower Extremity PAD: When, why and what?! Robert F Cuff, MD FACS RVT RPVI 1 Disclosures I have no financial disclosures related to this talk Objectives 1. Discuss indications for intervention
