Collage of medicine Cardiovascular Physiology 3- Arterial and venous blood Pressure.
|
|
|
- Phoebe Phelps
- 5 years ago
- Views:
Transcription
1 University of Babylon Collage of medicine Dr. Ghafil Seyhood Hassan Al-Shujiari Cardiovascular Physiology 3- Arterial and venous blood Pressure. UArterial blood pressureu: Arterial pressure = COP X Peripheral resistance. Mean blood pressure = Diastolic pressure + 1/3 pulse pressure. Pulse pressure = Systolic pressure diastolic pressure. (Figure 1). The pressure falls very slightly in the large and medium-sized arteries because their resistance to flow is small, but it fall rapidly in the small arteries and arterioles, which are the main sites of peripheral resistance. Normal blood pressure is 120/ 70 mmhg. The pressure in any vessel below heart level is increased and above heart level is decreased by effect of the gravity 0.77 mmhg for each one cm. Figure (1): Arterial blood pressure curve. In general the blood pressure is lower in children than adult and women than men. Blood pressure may increase by exercise, emotion and pregnancy. Increase cardiac output lead to increase the systolic pressure. The blood pressure is higher in systemic than pulmonary circulation because pulmonary circulation is under lower resistance UMethods of measuring arterial blood pressure: 1- Direct method ( invasive method): A cannula is inserted into an artery, the arterial pressure can be measured directly with a mercury manometer. The wave recorded by this method is called pulse wave. Pressure at the highest point of each pulse is systolic pressure and the lowest point is diastolic pressure. 2- Indirect method (non invasive method): A- UPalpation method:u Letting the pressure fall and determining the pressure at which the radial pulse become palpable. This is a systolic pressure. This method is usually 2-5 mmhg, pressure lower than those measured by ausculatory method.
2 A-UAusculatory methodu: Inflatable cuff attached to mercury manometer (sphygmomanometer) is wrapped around the arm and a stethoscope is placed over the brachial artery at elbow. The cuff is rapidly inflated until pressure in it above expected systolic pressure. Artery is occluded by cuff and no sound is heard with stethoscope. The pressure in cuff is then lowered slowly, at point a tapping sound heard (Korotkoff sound phase 1), systolic pressure is recorded. Cuff pressure is lowest further, the sound become louder, dull, and muffled then disappear (Korotkoff sound phase 5), at this point diastolic pressure is recorded. A number of precautions must be obtained in measurement of arterial BP: 1- The cuff must be at heart level to obtain a pressure that is uninfluenced by gravity. 2- The size of the cuff suitable, as small cuff use in children and large cuff use in obese. 3- Do not leave the cuff inflate for long time as it may cause generalized reflex vasoconstriction. 4-Measure blood pressure from right and left arm. Regulation of arterial blood pressure I- Nervous mechanism: UA- Baroreceptor mechanism:u This is fast neural mechanism. Baroreceptors are stretch receptors located with in the wall of the carotid sinus near the bifurcation of the common carotid arteries and aortic arch in adventitia of vessels. Figure (2). Figure (2): Carotid sinus and aortic arch paroreceptors. UB- The chemoreceptors mechanism:u Chemoreceptors present in the carotid and aortic bodies. They have very high rate of O2 consumption and therefore are very
3 sensitive to hypoxia. A decrease in arterial pressure causes a decrease in O2 delivery to the chemoreceptors. Information is sent to vasomotor center. UC- Vasomotor center (VMC)U: It is group of neurons located in the medulla oblongata. It is composed of vasoconstrictor, vasodilator and sensory area. When blood pressure decreases, the informations reach VMC via vagus and glosopharyngeal nerves to increase sympathetic discharge to blood vessels and heart to increase HR, stroke volume and TPR. Conversely increase in blood pressure causes decrease in sympathetic and increase in parasympathetic discharge to cause vasodilatation of vessels and decrease heart rat. UII-Hormonal Mechanism: 1- URenin-angiotensin-aldosterone system:u It is a slow mechanism. Blood pressure regulated by blood volume. Renin is an enzyme that catalyzes the conversion of angiotensinogen to angiotensin I in plasma. It is secreted from the juxtaglomerular cells of the afferent arteriole in kidney during decrease in renal perfusion pressure. Angiotensin I is inactive. The angiotensin I is converted to angiotensin II by angiotensin converting enzyme (ACE), primarily in the lungs. Angiotensin II is physiologically active. It is degraded by angiotensinase. Angiotensin II has two effects: 1- It stimulates the synthesis and secretion of the aldosterone by the adrenal cortex. Aldosterone increases sodium chloride ( Nacl) reabsorption by renal distal tubule, thereby increasing blood volume and arterial pressure. This action of aldosterone is slow because it requires new protein synthesis. 2- It causes vasoconstriction of the arterioles, thereby increasing TPR and mean arterial pressure. U2-Vasopressin or Antidiuretic hormone (ADHU): Atrial receptors respond to a decrease in blood pressure and cause the release of vasopressin from the posterior pituitary gland. Vasopressin has two effects that tend to increase BP toward normal. 1- It is a potent vasoconstrictor that increases TPR by activating V1 receptors on the arterioles. 2- It increases water reabsorption by the renal distal tubule and collecting ducts by activating V2 receptors. U3- Atrial natriuretic peptide (AVP):U It is released from the atria in response to an increase in atrial pressure, causes relaxation of vascular smooth muscle, dilatation of arterioles and decreased TPR. It causes increased excretion of salt and water by the kidney III- Capillary fluid shift mechanism: Any change in the arterial pressure usually associated with change in capillary pressure resulting in the movement of fluid across the capillary membrane between the blood and interstitial compartment so a new state of equilibrium will be achieved.
4 Venous blood pressure The pressure in the venules is about mmhg. It fails in the larger veins to about 5.5 mmhg in the great veins outside the thorax and 4.5 mmhg (central venous pressure) at their entrance the thorax. Peripheral venous pressure is affected by gravity. It is increased by 0.77 mmhg for each cm below the right atrium and decrease by 0.77 mmhg for each 1cm above the right atrium. UJugular venous pulses:u The changes in atrial pressure are transmitted to the great veins, producing three characteristic positive waves. The (a) wave is due to atria systole. The (c) wave concides with the onset of ventricular systole and results from tricuspid valve closure (Tricuspid bulging). The (v) wave indicates arise in pressure as venous blood return continously while tricuspid valve is closed. Figure (3). Figure (3): Normal jugular venous pulse. Effect of gravity on the body The following changes occur when an individual move from a supine position to standing position: 1- A significant volume of blood pools in the lower extremities due to of high compliance of the vein. Muscular activity would prevent this pooling. 2- Increase venous pressure in legs, increase filtered fluid into interstitium. Edema will occur. 3- Decrease venous return, both stroke volume and COP decrease (Frank-Starling relationship). 4- If COP decrease cerebral blood pressure becomes low, fainting may occur. Compensatory mechanism will attempt to increase blood pressure to normal. The carotid sinus baroreceptors respond to the decrease in arterial pressure by decreasing the firing of the carotid sinus nerves. Vasomotor center then increases sympathetic outflow to the heart and blood vessels and decreases parasympathetic outflow to heart. As a result, heart rate and TPR increase and blood pressure increases toward normal
5 from Effect of altitude on the body 1- The oxygen partial pressure decreases, hypoxia beginning at altitude of about 12,000 feet, symptoms of hypoxia are drowsiness, lassitude, mental and muscle fatigue, sometime headache. 2- Hypoxia stimulates arterial chemoreceptors to Uincrease alveolar ventilationu to a maximum of about 1.65 times 0f normal. This is an immediate compensation with in seconds. 3- It Uincreases red blood cell productionu, UhematocitU from a normal value of to an average of about UIncrease concentration of hemoglobin U a normal value 15 gm /dl to about 20 gm /dl. 5- It Uincreases diffusing capacity for O2 through the pulmonary membraneu 3 fold as much as during exercise. Normal capacity 21 ml / mmhg / minute. 6- UCOP increaseu as much as 30% immediately after a person ascends to high altitude but then decrease back toward normal as the blood hematocrit increases. 7- UIncrease in number of systemic circulatory capillaries U. 8- In animals native to altitude of 13,000 to 17,000 feet, Ucell mitochondria and cellular oxidative enzyme systems are slightly more plentiful than in sea-level inhabitants. Venous return Venous flow is aided by; 1- The heart beat. 2-The increase in the negative intrathoracic pressure during each inspiration. 3- Contraction of skeletal muscles that compress the vein (muscle pump) figure (4). 4-Venous valves prevent reverse flow, the blood moves toward the heart. 5-The diaphragm descend during inspiration, intra-abdominal pressure rises, and this also squeezes blood toward the heart. 6-During inspiration the intrapleural pressure falls from to 6 mmhg. This negative pressure is transmitted to great veins; venous pressure fluctuates from about 6 mmhg during expiration to 2 mmhg during inspiration. The drop in venous pressure during inspiration aids venous return. Figure (4): Venus return.
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Therefore MAP=CO x TPR = HR x SV x TPR
 Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Physiology lecture 15 Hemodynamic
 Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Blood pressure control Contin. Reflex Mechanisms. Dr. Hiwa Shafiq
 Blood pressure control Contin. Reflex Mechanisms Dr. Hiwa Shafiq 17-12-2018 A. Baroreceptor reflexes Baroreceptors (stretch receptors) located in the walls of several large systemic arteries( specially
Blood pressure control Contin. Reflex Mechanisms Dr. Hiwa Shafiq 17-12-2018 A. Baroreceptor reflexes Baroreceptors (stretch receptors) located in the walls of several large systemic arteries( specially
BIOH122 Session 6 Vascular Regulation
 BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
Cardiovascular system: Blood vessels, blood flow. Latha Rajendra Kumar, MD
 Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
 Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide 1 Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical Application
Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide 1 Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical Application
Presenter: Tom Mulvey
 Slides are from Level 3 Biology Course Content Day, 7 th November 2012 Presenter: Tom Mulvey Teachers are free to use these for teaching purposes with appropriate acknowledgement Blood Pressure Ways of
Slides are from Level 3 Biology Course Content Day, 7 th November 2012 Presenter: Tom Mulvey Teachers are free to use these for teaching purposes with appropriate acknowledgement Blood Pressure Ways of
Physiology of Circulation
 Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
CASE 13. What neural and humoral pathways regulate arterial pressure? What are two effects of angiotensin II?
 CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
I. Cardiac Output Chapter 14
 10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
Blood Pressure Regulation -1
 CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
Heart. Large lymphatic vessels Lymph node. Lymphatic. system Arteriovenous anastomosis. (exchange vessels)
 Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Cardiovascular System. Heart
 Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation
 Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation I. General Features of Blood Vessel Structure A. General Pattern of Circulation 1. Ventricles pump blood into 2. These arteries
Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation I. General Features of Blood Vessel Structure A. General Pattern of Circulation 1. Ventricles pump blood into 2. These arteries
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D.
 Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
PHYSIOLOGY MeQ'S (Morgan) All the following statements related to blood volume are correct except for: 5 A. Blood volume is about 5 litres. B.
 PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
The Cardiovascular System. The Structure of Blood Vessels. The Structure of Blood Vessels. The Blood Vessels. Blood Vessel Review
 The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
Blood Pressure. a change in any of these could cause a corresponding change in blood pressure
 Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Chapter 24 Vital Signs. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
3/10/2009 VESSELS PHYSIOLOGY D.HAMMOUDI.MD. Palpated Pulse. Figure 19.11
 VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Cardiovascular System. Blood Vessel anatomy Physiology & regulation
 Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
1. Distinguish among the types of blood vessels on the basis of their structure and function.
 Blood Vessels and Circulation Objectives This chapter describes the structure and functions of the blood vessels Additional subjects contained in Chapter 13 include cardiovascular physiology, regulation,
Blood Vessels and Circulation Objectives This chapter describes the structure and functions of the blood vessels Additional subjects contained in Chapter 13 include cardiovascular physiology, regulation,
Special Lecture 11/08/2013. Hypertension Dr. HN Mayrovitz
 Special Lecture 11/08/2013 Hypertension Dr. HN Mayrovitz Arterial Blood Pressure (ABP) Major Factors Summarized Sympathetic Hormones Arteriole MAP ~ Q x TPR + f (V / C) SV x HR Renal SBP Hypertension =
Special Lecture 11/08/2013 Hypertension Dr. HN Mayrovitz Arterial Blood Pressure (ABP) Major Factors Summarized Sympathetic Hormones Arteriole MAP ~ Q x TPR + f (V / C) SV x HR Renal SBP Hypertension =
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM 1. Resting membrane potential of the ventricular myocardium is: A. -55 to-65mv B. --65 to-75mv C. -75 to-85mv D. -85 to-95 mv E. -95 to-105mv 2. Regarding myocardial contraction:
CARDIOVASCULAR SYSTEM 1. Resting membrane potential of the ventricular myocardium is: A. -55 to-65mv B. --65 to-75mv C. -75 to-85mv D. -85 to-95 mv E. -95 to-105mv 2. Regarding myocardial contraction:
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Chapter 21 Peripheral circulation and Regulation
 Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
Physiology of the Circulatory System modified from
 Physiology of the Circulatory System modified from http://www.ekcsk12.org/science/aplabreview/aplab10.htm Introduction The circulatory system functions to deliver oxygen and nutrients to tissues for growth
Physiology of the Circulatory System modified from http://www.ekcsk12.org/science/aplabreview/aplab10.htm Introduction The circulatory system functions to deliver oxygen and nutrients to tissues for growth
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
Cardiovascular regulation. Neural and hormonal Regulation Dr Badri Paudel GMC. 1-Local factors (autoregulation) Control of Blood Flow
 Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
During exercise the heart rate is 190 bpm and the stroke volume is 115 ml/beat. What is the cardiac output?
 The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
Physiology of Circulation. Dr. Hiwa Shafiq 16/12/2018
 Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Lab #10 Physiology of the Circulatory System
 Lab #10 Physiology of the Circulatory System Introduction The circulatory system functions to deliver oxygen an nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart
Lab #10 Physiology of the Circulatory System Introduction The circulatory system functions to deliver oxygen an nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions
 Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapters 9 & 10. Cardiorespiratory System. Cardiovascular Adjustments to Exercise. Cardiovascular Adjustments to Exercise. Nervous System Components
 Cardiorespiratory System Chapters 9 & 10 Cardiorespiratory Control Pulmonary ventilation Gas exchange Left heart Arterial system Tissues Right heart Lungs Pulmonary ventilation Cardiovascular Regulation-
Cardiorespiratory System Chapters 9 & 10 Cardiorespiratory Control Pulmonary ventilation Gas exchange Left heart Arterial system Tissues Right heart Lungs Pulmonary ventilation Cardiovascular Regulation-
Mechanism: 1- waterretention from the last part of the nephron which increases blood volume, venous return EDV, stroke volume and cardiac output.
 Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM
 Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Chapter 15: The Cardiovascular System
 Chapter 15: The Cardiovascular System McArdle, W. D., Katch, F. I., & Katch, V. L. (2010). Exercise Physiology: Nutrition, Energy, and Human Performance (7 ed.). Baltimore, MD.: Lippincott Williams and
Chapter 15: The Cardiovascular System McArdle, W. D., Katch, F. I., & Katch, V. L. (2010). Exercise Physiology: Nutrition, Energy, and Human Performance (7 ed.). Baltimore, MD.: Lippincott Williams and
Cardiovascular Physiology
 Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Contents. Page 1. Homework 11 Chapter Blood Vessels Due: Week 6 Lec 11
 Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
The Circulatory System. Lesson Overview. Lesson Overview The Circulatory System
 33.1 THINK ABOUT IT More than one-third of the 1.2 million Americans who suffer a heart attack each year die. This grim evidence shows that the heart and the circulatory system it powers are vital to life.
33.1 THINK ABOUT IT More than one-third of the 1.2 million Americans who suffer a heart attack each year die. This grim evidence shows that the heart and the circulatory system it powers are vital to life.
Blood Pressure and its Regulation
 Blood Pressure and its Regulation Blood pressure in your blood vessels is closely monitored by baroreceptors; they send messages to the cardio regulatory center of your medulla oblongata to regulate your
Blood Pressure and its Regulation Blood pressure in your blood vessels is closely monitored by baroreceptors; they send messages to the cardio regulatory center of your medulla oblongata to regulate your
Cardiac Output 1 Fox Chapter 14 part 1
 Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
Chapter 9, Part 2. Cardiocirculatory Adjustments to Exercise
 Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Figure ) The specific chamber of the heart that is indicated by letter A is called the. Diff: 1 Page Ref: 364
 Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Types of Blood Vessels
 Chapter 21 Peripheral Circulation and Regulation 21-1 Types of Blood Vessels Capillaries: site of exchange with tissue Arteries in dif. Types & sizes Elastic Muscular Arterioles Veins: thinner walls than
Chapter 21 Peripheral Circulation and Regulation 21-1 Types of Blood Vessels Capillaries: site of exchange with tissue Arteries in dif. Types & sizes Elastic Muscular Arterioles Veins: thinner walls than
Cardiovascular Responses to Exercise
 CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
BIOL 219 Spring Chapters 14&15 Cardiovascular System
 1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
AS OCR PHYSICAL EDUCATION The Vascular System
 AS OCR PHYSICAL EDUCATION The Vascular System Learning Objectives: - Distribution of Cardiac output at rest and during exercise - Role of the Vasomotor centre, arterioles and pre-capillary sphincters -
AS OCR PHYSICAL EDUCATION The Vascular System Learning Objectives: - Distribution of Cardiac output at rest and during exercise - Role of the Vasomotor centre, arterioles and pre-capillary sphincters -
LAB 9: Metabolic Rates
 LAB 9: Metabolic Rates Introduction: The cardiovascular (circulatory) system functions to deliver oxygen and nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart pumps
LAB 9: Metabolic Rates Introduction: The cardiovascular (circulatory) system functions to deliver oxygen and nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart pumps
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
The Cardiovascular system: physiology of circulation
 Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
d) Cardiovascular System Higher Human Biology
 d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
Chapter 17: Urinary System
 Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Chapter 15 Fluid and Acid-Base Balance
 Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
PHYSIOLOGY WEEK 9. vascular physiology - ED Primary Exam Teaching
 PHYSIOLOGY WEEK 9 vascular physiology - ED Primary Exam Teaching CONCEPTS OF BLOOD FLOW Vascular distensibility - when pressure in the arterioles is increased, this dilates the arterioles and therefore
PHYSIOLOGY WEEK 9 vascular physiology - ED Primary Exam Teaching CONCEPTS OF BLOOD FLOW Vascular distensibility - when pressure in the arterioles is increased, this dilates the arterioles and therefore
Control of Heart Rate
 Control of Heart Rate Control of Heart Rate The beating of your heart is an involuntary movement one that is beyond your direct control. The nerve impulse that causes the heart to beat originates within
Control of Heart Rate Control of Heart Rate The beating of your heart is an involuntary movement one that is beyond your direct control. The nerve impulse that causes the heart to beat originates within
PART I: HEART ANATOMY
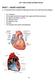 Lab 7: Heart Sounds and Blood Pressure PART I: HEART ANATOMY a) You should be able to identify the following structures on an adult human heart diagram. the 4 chambers the bicuspid (mitral) and tricuspid
Lab 7: Heart Sounds and Blood Pressure PART I: HEART ANATOMY a) You should be able to identify the following structures on an adult human heart diagram. the 4 chambers the bicuspid (mitral) and tricuspid
Responses to Changes in Posture QUESTIONS. Case PHYSIOLOGY CASES AND PROBLEMS
 64 PHYSIOLOGY CASES AND PROBLEMS Case 12 Responses to Changes in Posture Joslin Chambers is a 27-year-old assistant manager at a discount department store. One morning, she awakened from a deep sleep and
64 PHYSIOLOGY CASES AND PROBLEMS Case 12 Responses to Changes in Posture Joslin Chambers is a 27-year-old assistant manager at a discount department store. One morning, she awakened from a deep sleep and
What would be the response of the sympathetic system to this patient s decrease in arterial pressure?
 CASE 51 A 62-year-old man undergoes surgery to correct a herniated disc in his spine. The patient is thought to have an uncomplicated surgery until he complains of extreme abdominal distention and pain
CASE 51 A 62-year-old man undergoes surgery to correct a herniated disc in his spine. The patient is thought to have an uncomplicated surgery until he complains of extreme abdominal distention and pain
Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations
 ighapmlre33apg269_274 5/12/04 3:10 PM Page 269 impos03 302:bjighapmL:ighapmLrevshts:layouts: NAME Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations LAB TIME/DATE REVIEW SHEET exercise
ighapmlre33apg269_274 5/12/04 3:10 PM Page 269 impos03 302:bjighapmL:ighapmLrevshts:layouts: NAME Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations LAB TIME/DATE REVIEW SHEET exercise
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
The Cardiovascular System. Preview of Heart Action. The CV system provides oxygen & nutrients to tissues-removes wastes.
 The Cardiovascular System BIO 250 Human Anatomy & Physiology Preview of Heart Action http://www.youtube.com/watch?v=d3zdj gfddk0&nr=1 The CV system provides oxygen & nutrients to tissues-removes wastes.
The Cardiovascular System BIO 250 Human Anatomy & Physiology Preview of Heart Action http://www.youtube.com/watch?v=d3zdj gfddk0&nr=1 The CV system provides oxygen & nutrients to tissues-removes wastes.
1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary.
 CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
HEART SOUNDS & BLOOD PRESSURE
 LABORATORY HANDBOOK HEART SOUNDS & BLOOD PRESSURE For the course Systems Biology Karolinska Institutet Department of Physiology and Pharmacology Physiology Education Postal address: 171 77 Stockholm Visiting
LABORATORY HANDBOOK HEART SOUNDS & BLOOD PRESSURE For the course Systems Biology Karolinska Institutet Department of Physiology and Pharmacology Physiology Education Postal address: 171 77 Stockholm Visiting
Arteries AWAY. Branch. Typically oxygenated.
 Arteries AWAY Branch Typically oxygenated. Capillaries Smallest. Most abundant. 10 billion. Huge surface area. Exchange Veins TOWARDS Converge. Typically deoxygenated. 3 Layers of the Vascular Wall Tunica
Arteries AWAY Branch Typically oxygenated. Capillaries Smallest. Most abundant. 10 billion. Huge surface area. Exchange Veins TOWARDS Converge. Typically deoxygenated. 3 Layers of the Vascular Wall Tunica
Cardiac Output (C.O.) Regulation of Cardiac Output
 Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Control of blood tissue blood flow. Faisal I. Mohammed, MD,PhD
 Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
CHAPTER 14 CARDIAC OUTPUT, BLOOD FLOW, AND BLOOD PRESSURE
 CHAPTER 14 CARDIAC OUTPUT, BLOOD FLOW, AND BLOOD PRESSURE CHAPTER SCOPE The last chapter introduced the blood, the structure and function of the heart and the blood vessels. Logically, this chapter follows
CHAPTER 14 CARDIAC OUTPUT, BLOOD FLOW, AND BLOOD PRESSURE CHAPTER SCOPE The last chapter introduced the blood, the structure and function of the heart and the blood vessels. Logically, this chapter follows
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Unit 1: Human Systems. The Circulatory System
 Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
