Royal Wolverhampton Hospital Adult Lipid Lowering Therapy Guidelines Lipid Lowering Therapy for the Prevention of Cardiovascular Disease
|
|
|
- Crystal Sullivan
- 5 years ago
- Views:
Transcription
1 Royal Wolverhampton Hospital Adult Lipid Lowering Therapy Guidelines 1 This guideline is intended to assist rational and cost-effective prescribing of lipid regulating medications across both primary and secondary care. It represents an evidence based consensus of opinion of healthcare professionals involved in prescribing lipid regulating therapy. Before any treatment is initiated, lifestyle advice should be given regarding: - Smoking cessation - Attainment of a healthy weight - Diet - Alcohol intake - Exercise, in particular increasing aerobic exercise activity. The following should also be addressed: - Exclusion of secondary causes of hyperlipidaemia, including diabetes, hypothyroidism, nephrotic syndrome, renal disease, excessive alcohol intake - Optimisation of blood pressure management in hypertensive patients. - Optimisation of glycaemic control in patients with diabetes Lipid Lowering Therapy for the Prevention of Cardiovascular Disease Primary Prevention Primary prevention is appropriate for patients without known cardiovascular disease (CVD) who have: 1. A calculated CVD risk 10% over the next 10 years. Use QRISK2 risk engine to estimate CVD risk in people up to < 84 yrs. Interpretation of CVD risk should reflect informed clinical judgment. 2. Familial Hypercholesterolaemia (see familial hypercholesterolaemia) 3. Diabetes (see below for specific guidance) 4. Chronic Kidney Disease (CKD): People with egfr <60ml/min/1.73m 2 and/or microalbuminuria 5. An age >84 yrs, especially those who smoke and have hypertension Primary prevention for patients with a calculated CV risk < 10% over the next 10 years Step 1: Lifestyle advice regarding smoking cessation, attaining a healthy weight, diet, exercise and reducing alcohol consumption should be offered. Dietary modifications alone may reduce serum cholesterol by approximately 5%. (2) Step 2: Ongoing risk assessment in those >40yrs. Primary prevention for patients with a calculated CV risk > 10% over the next 10 years Step 1: Identify and address lifestyle and modifiable risk factors Step 2: Offer atorvastatin 20mg daily and aim to reduce non-hdl cholesterol by >40% Step 3: For patients who are still not able to achieve their target cholesterol levels: - Check compliance and review life-style measures - In those with type 2 diabetes optimise glycaemic control - Consider step-wise dose optimisation to Atorvastatin mg daily
2 Primary prevention for patients with diabetes Type 2 diabetes: Use QRISK2 tool to assess CVD risk and manage as above Type 1 diabetes: Risk assessment is not helpful to assess CVD risk in people with Type-1 diabetes. - Consider statin treatment in all adults with type-1 diabetes - Offer statin treatment in adults with type 1 diabetes who are 40 years or older, have diabetes for > 10 years duration, have evidence of CKD or other CV risk factors Primary prevention in patients with Chronic Kidney Disease (egfr <60ml/min/1.73m 2 and/or microalbuminuria) Step 1: Identify and address lifestyle and modifiable risk factors Step 2: Initiate atorvastatin 20mg daily and aim to reduce non-hdl cholesterol by >40% Step 3: For patients who are still not able to achieve their target cholesterol levels: - Check compliance and review life-style measures - In those with diabetes, optimise glycaemic control - Consider step-wise dose optimisation to Atorvastatin 40-80mg daily - In patients with CKD, whose egfr is <30mls/min seek specialist advice before increasing the dose of Atorvastatin Secondary Prevention Secondary Prevention is appropriate for patients with known CV disease (coronary artery disease/ischaemic stroke/tia or peripheral vascular disease) Step 1: Lifestyle advice should be issued in addition to initiation of statin therapy Lifestyle advice regarding smoking cessation, diet, exercise and reducing alcohol consumption should be offered. Dietary modifications alone can reduce serum cholesterol by approximately 5%. (1) Manage other cardiovascular factors Step 2: Initiate atorvastatin 80mg daily at the same time as issuing life-style advice In older patients (>75years) or those with low body weight (<60kg) consider a dose reduction to atorvastatin 40mg daily to mitigate against potential side effects e.g myopathy. Step 3: Once treatment has been initiated re-assess the patient s lipid profile at 3 months aiming for a greater than 40% reduction in non-hdl cholesterol. Should baseline non-hdl cholesterol not be available, patients should be treated to achieve a total cholesterol of <4 mmol/l or non-hdl cholesterol of <2.5 mmol/l. Step 4: If target reduction in non-hdl cholesterol or target total cholesterol levels are not achieved: - discuss adherence and timing of the dose - Review adherence with lifestyle measures - Optimisation to atorvastatin 80mg daily if on a lower dose - Consider addition of Ezetimibe 10mg daily if already on maximum tolerated statin dose
3 Acute Coronary Syndromes Intensive lipid lowering therapy is recommended by NICE for all patients following an acute coronary syndrome (including ST elevation MI, non-st elevation MI and Unstable Angina) Step 1: Initiate atorvastatin 40-80mg daily irrespective of baseline lipid levels, in addition to dietary advice and lifestyle modifications delivered as part of a local cardiac rehabilitation programme. For older patients or those with reduced body weight, a lower dose of atorvastatin 40mg daily may be prescribed. Step 2: Once treatment has been initiated re-assess the patient s lipid profile at 3 months aiming for a greater than 40% reduction in non-hdl cholesterol. Should baseline non-hdl cholesterol not be available, patients should be treated to achieve a total cholesterol of <4mmol/L and non-hdl cholesterol of <2.5 mmol/l. Step 3: If this reduction in non-hdl cholesterol or target total cholesterol levels are not achieved: - discuss adherence and timing of the dose - review adherence with lifestyle measures - Optimisation to atorvastatin 80mg daily if already on a lower dose - Consider addition of Ezetimibe 10mg daily if already on maximum tolerated statin dose - Consider referral for specialist advice. MHRA advice regarding high dose Simvastatin (3) Prescribers treating patients who are taking Simvastatin 80mg or who are being considered for uptitration to that dose may need to review their treatment during the next visit, to take into account the new evidence, as outlined above. Patients who are currently taking Simvastatin 80mg should not stop taking their medicine. However, they should be advised to contact their doctor immediately if they experience unexplained muscle pain, tenderness or weakness. Alternative Treatment Options For patients who are intolerant of statins, an alternative treatment options includes: - Ezetimibe 10mg daily as monotherapy - Seek specialist advice. o Fenofibrate 200mg daily o Cholestyramine 12-24g daily in divided doses. Other drugs should be taken at least one hour before or four hours after Cholestyramine to reduce the possible interference with absorption. o The concomitant use of Ezetimibe with Fibrates increases the risk of cholelithiasis and gall bladder disease. (4) Of note, NICE CG 181 recommends that bile acid sequestrants, nicotinic acid, or fibrates should NOT be offered for primary or secondary prevention of cardiovascular disease alone or in combination with a statin, including in people with chronic kidney disease or type 1 or type 2 diabetes. Ezetimibe may be considered as an adjunct in patients failing to achieve treatment targets despite maximal statin dose or where higher statin doses are not tolerated. If targets are still not achieved with a statin plus Ezetimibe, the patient should be referred to a Specialist for the possible addition of a fibrate. Concurrent prescribing of statins with fibrates increases the likelihood of myopathy/rhabdomylosis and therefore should be undertaken under specialist supervision. Ezetimibe remains a treatment option for primary hypercholesterolaemia as per NICE TA132, however, it is not licensed for the reduction of cardiovascular events in the context of the acute coronary syndromes. Although the IMPROVE-IT study (simvastatin 40mg plus ezetemibe 10mg vs simvastatin 40mg) demonstrates a modest benefit in reducing cardiovascular events in post-acs patients, it achieved significance after only 7 years of use with no reduction in total mortality. Since atorvastatin is now the default
4 statin of choice, the results of IMPROVE-IT may not apply to current clinical practice since simvastatin 40mg is no longer considered to a clinically effective therapeutic option. Monitoring Statin Therapy (1,4) Lipid Levels Total cholesterol (TC) HDL Cholesterol Non-HDL cholesterol Triglycerides Thyroid Function Tests Renal Function Liver Function Tests (LFTs) Creatine kinase (CK) Other adverse effects Primary and Secondary Prevention: Lipid levels should be measured before therapy is initiated and at 3 months following the initiation or change of dose and 12 monthly intervals thereafter. At 3 months, aim for a greater than 40% reduction in non-hdl cholesterol; if levels remains persistently raised despite optimising statin therapy, consider specialist referral. Check before initiating a statin to exclude hypothyroidism Seek specialist advice regarding atorvastatin dosing >20mg od if egfr <30 ml/minute. Baseline ALT should be measured before starting a statin. Liver function (transaminases) should be measured within 3 months of starting treatment and at 12 monthly but not again unless clinically indicated. If transaminases >3x upper limit of normal (ULN) discontinue statin and refer. For lesser increases in transaminases, which remain elevated at 6 months consider specialist advice. Routine CK monitoring after initiation is not recommended. CK should be measured during treatment when clinically indicated i.e. where there are symptoms of muscle pain or tenderness, muscle weakness or muscle cramps. Patients should be counselled on initiation of statin to report any unusual muscle pain, tenderness or weakness during treatment IF MYOSITIS IS PRESENT OR SUSPECTED DISCONTINUE IMMEDIATELY If muscle soreness occurs: Rule out common causes (e.g. exercise) Check TFTs (hypothyroidism predisposes to myopathy) Measure CK - If CK elevated > 5 x ULN stop and seek advice - If CK elevated < 5 x ULN a) Monitor carefully by repeating CK level in one month b) If remains elevated, reduce dose and recheck CK level in one month c) If still remains elevated consider seeking advice If symptoms continue STOP statin and consult a specialist before re-initiating Note: Some Black African and Caribbeans have elevated baseline levels of CK. This is not a contra-indication to statin therapy. In these patients, after initiation if the CK > 5 x baseline - seek advice Headache, dyspepsia or insomnia. Evaluate symptoms at each visit. If symptoms not tolerated: Consider changing time of dose (after food if nauseous, morning if sleep disturbed) Consider decreasing dose Consider using an alternative agent Statin Interactions (5,6) Interacting Agents Potent CYP3A4 Inhibitors e.g. HIV protease inhibitors Azole antifungal agents Macrolides Fusidic Acid Ciclosporin Gemfibrozil Danazol Amiodarone Amlodipine Verapamil Diltiazem Niacin > 1g daily Grapefruit Juice Prescribing Recommendation Avoid Simvastatin and Atorvastatin Consider usual doses of Rosuvastatin or Pravastatin. For short course treatments of antibiotics or antifungals, stop the statin for the duration of antibiotic treatment and restart later. For patients treated with Fusidic Acid, statin therapy should resume seven days after course completion. Simvastatin is contraindicated Do not exceed Simvastatin 20mg; higher doses will increase the likelihood of myopathy/rhabdomylosis. Do not exceed Simvastatin 10mg Avoid grapefruit juice while taking Simvastatin or Atorvastatin.
5 2. Lipid Lowering Therapy for the Management of Moderate to Severe Hypertriglyceridaemia. A fasting serum triglyceride concentration below 2.0mmol/l is normal. In the range of mmol/L no specific intervention will be needed unless there are co-existing cardiovascular risk factors, and in particular a strong family history of early myocardial infarction or based a 10yr CVD risk >10% Identify and address secondary causes of hypertriglyceridaemia including diabetes and excessive alcohol intake. Patients should be given advice regarding weight loss and correction of any other modifiable cardiovascular risk factors they may have. Manage CVD risk as in primary and secondary prevention of cardiovascular disease. Serum triglyceride levels > 6.0mmol/L carry a risk of acute pancreatitis and retinal vein thrombosis. Patients should be advised to reduce their weight if overweight and start a formal lipid lowering diet A proportion of patients may have hypertriglyceridaemia secondary to even moderate alcohol intake. If hypertriglyceridaemia persists, lipid levels should be measured before and after a 4-week interval of complete abstinence from alcohol. If a considerable improvement results, lifelong abstinence should be considered. Other drugs, such as thiazides, oestrogens and glucocorticoids, may have a similar effect to alcohol in susceptible patients. If the triglyceride levels remain elevated above 6.0mmol/L, despite the above measures, drug therapy is warranted. Treatment Options: 1. A fibric acid derivative is the agent of first choice. 2. Fish oil capsules which contain omega-3 long chain fatty acids are also effective in lowering triglyceride concentrations. 3. Nicotinic acid may be used in addition, but its side effects are often a problem. First Line Treatment Fenofibrate 200mg daily Monitoring Fibrate Therapy Monitor LFTs at beginning of treatment and at 1-3 months, 6 months, 12 months, then annually. Check CK if patient complains of musculoskeletal symptoms. Discontinue Fibrate is ALT persists > 3 x ULN, or serum Creatinine continues to rise progressively. It is often difficult to normalize serum triglycerides. Successful treatment of triglycerides may paradoxically increase total and LDL cholesterol. If, after fibrate therapy, serum cholesterol is persistently > 5mmol/L in patients with established or at high risk of developing CVD consider specialist referral for additive statin therapy. If, after fibrate therapy, serum triglycerides are persistently > 5mmol/L consider referral for addition of a statin and/or fish oils.
6 3. Lipid Lowering Therapy for the Management of Familial Hypercholesterolaemia Guidelines for the diagnosis and management of FH were published by NICE in (7) A clinical diagnosis of FH should be suspected in adults who have markedly elevated total cholesterol (>7.5mmol/L), particularly if there is a positive family or personal history of premature coronary artery disease (CAD).. Clinical diagnosis of definite or possible FH is based on the Simon Broome Criteria: (7) Definite FH - TC> 7.5mmol/L (LDL > 4.9mmol/L), pretreatment (or highest on treatment), and presence of tendon xanthomas in the patient or first/second degree relative. OR - DNA-based evidence of an LDL-receptor mutation, familial defective apo B-100, or a PCSK9 mutation. Possible FH - TC>7.5mmol/L (LDL > 4.9mmol/L), pretreatment (or highest on treatment) And one of the following: - Family history of MI (<50 years in 2 nd -degree relative or < 60 years in first degree relative) - Family history of raised cholesterol ( >7.5mmol/L in adult 1 st or 2 nd -degree relative; >6.7mmol/L in child or sibling aged < 16 years) Patients with suspected or confirmed FH should be referred to a specialist lipid clinic and cascade testing of relatives. First line treatment is with statins, aiming for 50% reduction in LDL-C, although dual treatment with a statin and Ezetimibe may be required to meet this target. If initial treatment is contra-indicated, not tolerated or ineffective, fibrates, bile acid sequestrants, and nicotinic acid may be initiated by a specialist in FH. Treatment Options (7) Drug Therapy Statins - Use as initial treatment - To achieve a recommended reduction in LDL-C concentration of greater than 50% from baseline: Consider prescribing a high-intensity statin Increase to the maximum licensed or tolerated dose - When an adult who does not have coronary heart disease, is diagnosed with FH after the age of 60 years, offer a statin with a low acquisition cost. - Measure baseline liver and muscle enzymes (including transaminases and creatine kinase) before starting treatment. - Raised liver or muscle enzymes should not routinely exclude a person from therapy. - Do not routinely monitor creatine kinase levels in asymptomatic patients. Ezetimibe - Is an option for adults with heterozygous FH if statins are contra-indicated or not tolerated. - Is an option for adults with heterozygous FH when co-administered with initial statin therapy, If: Serum or LDL-C concentration is not appropriately controlled with initial statin therapy after appropriate dose optimization or because of intolerance to the statin, and Consideration is being given to changing from initial statin therapy to an alternative statin. Bile Acid Sequestrant - For long-term treatment, consider offering fat-soluble vitamins (A,D and K) and Folic Acid supplementation. Fibrate - Do not use Gemfibrozil and statins together. - Consider if statin or Ezetemibe are contra-indicated or not tolerated. - Offer a referral to a specialist in FH for consideration of this treatment.
7 Nicotinic Acid - Offer advice on strategies that reduce flushing, including taking: Low initial doses with meals, and/or Aspirin 75mg 30 minutes before first daily dose. - The specialist should make the decision as to whether any of these treatments should be added to initial statin therapy. References 1. NICE Clinical Guideline 181. Lipid modification: cardiovascular risk assessment and the modification of blood lipids for the primary and secondary of cardiovascular disease. (2015) guidance.nice.org.uk/cg Cleemant JL, Lenfant C, The National Cholesterol Education Programme. Progress and Prospects. JAMA 1998;290: /12/2015> /12/2015> 5. MHRA Drug Safety Update Simvastatin: updated advice on drug interactions - updated contraindications<accessed 24/09/12> 6. Drug Interactions <accessed 20/09/12> 7. NICE Clinical Guideline 71: Familial Hypercholesterolaemia (2008)
FORTH VALLEY. LIPID LOWERING GUIDELINE v5 2016
 FORTH VALLEY LIPID LOWERING GUIDELINE v5 2016 This guideline applies to people over 16 years of age. This guideline is not intended to serve as a standard of medical care or be applicable in every situation.
FORTH VALLEY LIPID LOWERING GUIDELINE v5 2016 This guideline applies to people over 16 years of age. This guideline is not intended to serve as a standard of medical care or be applicable in every situation.
Primary Prevention Patients aged 85yrs and over
 Rotherham Guideline for the management of Non-Familial Hypercholesterolaemia Type 1 Diabetes Offer lifestyle advice Over 40yrs of age? Diabetic for more than 10 years? Established nephropathy? Other CVD
Rotherham Guideline for the management of Non-Familial Hypercholesterolaemia Type 1 Diabetes Offer lifestyle advice Over 40yrs of age? Diabetic for more than 10 years? Established nephropathy? Other CVD
APPENDIX 2F Management of Cholesterol
 Patients with established CVD: Coronary heart disease Cerebrovascular disease Peripheral vascular disease APPEDIX 2F Management of Cholesterol Patients at high risk of cardiovascular events: Chronic kidney
Patients with established CVD: Coronary heart disease Cerebrovascular disease Peripheral vascular disease APPEDIX 2F Management of Cholesterol Patients at high risk of cardiovascular events: Chronic kidney
Helen Williams Consultant Pharmacist for CV Disease - South London
 Helen Williams Consultant Pharmacist for CV Disease - South London CVD remains the leading cause of death in the UK Accounts for a third of all deaths 46,000 deaths in people < 75 years (70% of these
Helen Williams Consultant Pharmacist for CV Disease - South London CVD remains the leading cause of death in the UK Accounts for a third of all deaths 46,000 deaths in people < 75 years (70% of these
Volume 2; Number 11 July 2008
 Volume 2; Number 11 July 2008 CONTENTS Page 1 NICE Clinical Guideline 67: Lipid Modification (May 2008) Page 7 NICE Technology Appraisal 132: Ezetimibe for the treatment of primary (heterozygous familial
Volume 2; Number 11 July 2008 CONTENTS Page 1 NICE Clinical Guideline 67: Lipid Modification (May 2008) Page 7 NICE Technology Appraisal 132: Ezetimibe for the treatment of primary (heterozygous familial
Coronary Heart Disease and Stroke, Primary and Secondary Prevention Guidelines (Cholesterol)
 CLINICAL GUIDELINE Coronary Heart Disease and Stroke, Primary and Secondary Prevention Guidelines (Cholesterol) A guideline is intended to assist healthcare professionals in the choice of disease-specific
CLINICAL GUIDELINE Coronary Heart Disease and Stroke, Primary and Secondary Prevention Guidelines (Cholesterol) A guideline is intended to assist healthcare professionals in the choice of disease-specific
Identification and management of familial hypercholesterolaemia (FH) - An overview
 Identification and management of familial hypercholesterolaemia (FH) - An overview National Collaborating Centre for Primary Care and Royal College of General Practitioners NICE Guideline CG 71 (August
Identification and management of familial hypercholesterolaemia (FH) - An overview National Collaborating Centre for Primary Care and Royal College of General Practitioners NICE Guideline CG 71 (August
Lecture 36 Dyslipidemia Therapeutics Barry LIPIDS:
 LIPIDS: PATHOPHYSIOLOGY: TC or LDL-C = CVD HDL-C = CVD Association between TG and CVD not established o HyperTG associated with pancreatitis o Reducing TG w/ drug therapy doesn t CVD TYPES OF DYSLIPIDEMIA:
LIPIDS: PATHOPHYSIOLOGY: TC or LDL-C = CVD HDL-C = CVD Association between TG and CVD not established o HyperTG associated with pancreatitis o Reducing TG w/ drug therapy doesn t CVD TYPES OF DYSLIPIDEMIA:
This is a lipid lowering drug strategy which should only be used within an overall lifestyle and clinical management strategy.
 Treatment Guideline Statin Prescribing Objective These guidelines represent the views of the Gloucestershire Hospitals NHS Foundation Trust, which were arrived at after consideration of the available evidence
Treatment Guideline Statin Prescribing Objective These guidelines represent the views of the Gloucestershire Hospitals NHS Foundation Trust, which were arrived at after consideration of the available evidence
Hyperlipidaemia, dyslipidaemia and hypercholesterolaemia
 Medicine > Cardiology > Hyperlipidaemia, dyslipidaemia and Background information Patient information including patient decision aid Key messages for this pathway FH specialist nurse contact details Local
Medicine > Cardiology > Hyperlipidaemia, dyslipidaemia and Background information Patient information including patient decision aid Key messages for this pathway FH specialist nurse contact details Local
SIGN 149 Risk estimation and the prevention of cardiovascular disease. Quick Reference Guide July Evidence
 SIGN 149 Risk estimation and the prevention of cardiovascular disease Quick Reference Guide July 2017 Evidence ESTIMATING CARDIOVASCULAR RISK R Individuals with the following risk factors should be considered
SIGN 149 Risk estimation and the prevention of cardiovascular disease Quick Reference Guide July 2017 Evidence ESTIMATING CARDIOVASCULAR RISK R Individuals with the following risk factors should be considered
Type 2 Diabetes. Stopping Smoking. Consider referral to smoking cessation. Consider referring for weight management advice.
 Type 2 Diabetes Stopping Smoking Consider referral to smoking cessation BMI > 25 kg m² Set a weight loss target of a 5-10% reduction Consider referring for weight management advice Control BP to
Type 2 Diabetes Stopping Smoking Consider referral to smoking cessation BMI > 25 kg m² Set a weight loss target of a 5-10% reduction Consider referring for weight management advice Control BP to
SECONDARY PREVENTION OF CORONARY HEART DISEASE AND ISCHAEMIC STROKE/TIA
 PRIMARY PREVENTION OF CHD AND STROKE IN HIGH RISK PATIENTS Random non fasting test for total cholesterol, HDL cholesterol (TC:HDL ratio) and LFTs If cholesterol > 7.5 mmol/l or LDL C 5mmol/l exclude secondary
PRIMARY PREVENTION OF CHD AND STROKE IN HIGH RISK PATIENTS Random non fasting test for total cholesterol, HDL cholesterol (TC:HDL ratio) and LFTs If cholesterol > 7.5 mmol/l or LDL C 5mmol/l exclude secondary
Southern Derbyshire Shared Care Pathology Guidelines. Dyslipidaemia
 Southern Derbyshire Shared Care Pathology Guidelines Dyslipidaemia This guideline applies to patients with significantly abnormal lipid profiles, which may be primary (genetic), secondary to other diseases
Southern Derbyshire Shared Care Pathology Guidelines Dyslipidaemia This guideline applies to patients with significantly abnormal lipid profiles, which may be primary (genetic), secondary to other diseases
Cardiovascular risk reduction in diabetes Lipids (NICE CG181)
 Cardiovascular risk reduction in diabetes Lipids (NICE CG181) Primary Prevention T1DM Offer Atorvastatin 20mg if >40 years old Diabetes duration >10 years Established nephropathy Other CVS risk factors
Cardiovascular risk reduction in diabetes Lipids (NICE CG181) Primary Prevention T1DM Offer Atorvastatin 20mg if >40 years old Diabetes duration >10 years Established nephropathy Other CVS risk factors
NICE QIPP about Lipitor. Robert Trotter. Clinical Effectiveness Consultant
 NICE QIPP about Lipitor Robert Trotter Clinical Effectiveness Consultant LIP2894c Date of preparation: April 2009 Prescribing information for atorvastatin is available on the last slide Roadmap Background
NICE QIPP about Lipitor Robert Trotter Clinical Effectiveness Consultant LIP2894c Date of preparation: April 2009 Prescribing information for atorvastatin is available on the last slide Roadmap Background
Approach to Dyslipidemia among diabetic patients
 Approach to Dyslipidemia among diabetic patients Farzad Hadaegh, MD, Professor of Internal Medicine & Endocrinology Prevention of Metabolic Disorders Research Center, Research Institute for Endocrine Sciences
Approach to Dyslipidemia among diabetic patients Farzad Hadaegh, MD, Professor of Internal Medicine & Endocrinology Prevention of Metabolic Disorders Research Center, Research Institute for Endocrine Sciences
Death is inevitable but premature death is not. Sir Richard Doll
 Welcome to the Diabetes Care for You webinar Please log onto the conference call so you can hear our presenter From any SCFT Cisco phone dial 800800 From a mobile phone or any other phone dial 01273 242
Welcome to the Diabetes Care for You webinar Please log onto the conference call so you can hear our presenter From any SCFT Cisco phone dial 800800 From a mobile phone or any other phone dial 01273 242
In 2008 NICE issued guidelines on lipid modification. Key points are summarised below.
 Hyperlipidaemia: management In 2008 NICE issued guidelines on lipid modification. Key points are summarised below. Primary prevention A systematic strategy should be used to identify people aged 40-74
Hyperlipidaemia: management In 2008 NICE issued guidelines on lipid modification. Key points are summarised below. Primary prevention A systematic strategy should be used to identify people aged 40-74
PIEDMONT ACCESS TO HEALTH SERVICES, INC. Guidelines for Screening and Management of Dyslipidemia
 PIEDMONT ACCESS TO HEALTH SERVICES, INC. Policy Number: 01-09-021 SUBJECT: Guidelines for Screening and Management of Dyslipidemia EFFECTIVE DATE: 04/2008 REVIEWED/REVISED: 04/12/10, 03/17/2011, 4/10/2012,
PIEDMONT ACCESS TO HEALTH SERVICES, INC. Policy Number: 01-09-021 SUBJECT: Guidelines for Screening and Management of Dyslipidemia EFFECTIVE DATE: 04/2008 REVIEWED/REVISED: 04/12/10, 03/17/2011, 4/10/2012,
Case Discussions: Treatment Strategies for High Risk Populations. Most Common Reasons for Referral to the Baylor Lipid Clinic
 Case Discussions: Treatment Strategies for High Risk Populations Peter H. Jones MD, FNLA Associate Professor Methodist DeBakey Heart and Vascular Center Baylor College of Medicine Most Common Reasons for
Case Discussions: Treatment Strategies for High Risk Populations Peter H. Jones MD, FNLA Associate Professor Methodist DeBakey Heart and Vascular Center Baylor College of Medicine Most Common Reasons for
Lipid Therapy: Statins and Beyond. Ivan Anderson, MD RIHVH Cardiology
 Lipid Therapy: Statins and Beyond Ivan Anderson, MD RIHVH Cardiology Outline The cholesterol hypothesis and lipid metabolism The Guidelines 4 Groups that Benefit from Lipid therapy Initiation and monitoring
Lipid Therapy: Statins and Beyond Ivan Anderson, MD RIHVH Cardiology Outline The cholesterol hypothesis and lipid metabolism The Guidelines 4 Groups that Benefit from Lipid therapy Initiation and monitoring
New Guidelines in Dyslipidemia Management
 The Fourth IAS-OSLA Course on Lipid Metabolism and Cardiovascular Risk Muscat, Oman, February 2018 New Guidelines in Dyslipidemia Management Dr. Khalid Al-Waili, MD, FRCPC, DABCL Senior Consultant Medical
The Fourth IAS-OSLA Course on Lipid Metabolism and Cardiovascular Risk Muscat, Oman, February 2018 New Guidelines in Dyslipidemia Management Dr. Khalid Al-Waili, MD, FRCPC, DABCL Senior Consultant Medical
Pharmacology Challenges: Managing Statin Myalgia
 Clinical Case: RM is a 50 year-old African American woman with a past medical history of type diabetes, dyslipidemia, hypertension and peripheral arterial disease. She had been prescribed simvastatin 80
Clinical Case: RM is a 50 year-old African American woman with a past medical history of type diabetes, dyslipidemia, hypertension and peripheral arterial disease. She had been prescribed simvastatin 80
Elements for a Public Summary. Overview of disease epidemiology. Cardiovascular Events
 VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Cardiovascular Events Each year cardiovascular disease (CVD) causes 3.9 million deaths in Europe and over 1.8 million deaths in
VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Cardiovascular Events Each year cardiovascular disease (CVD) causes 3.9 million deaths in Europe and over 1.8 million deaths in
Conflicts of interest. What's the Skinny on the Lipid Guidelines? Key Differences. Are you applying the new ACC/AHA Lipid guidelines in your practice?
 Conflicts of interest What's the Skinny on the Lipid Guidelines? The presenter has no relevant conflicts of interest to disclose. Kathleen Vest, PharmD, CDE, BCACP At the end of this presentation, pharmacist
Conflicts of interest What's the Skinny on the Lipid Guidelines? The presenter has no relevant conflicts of interest to disclose. Kathleen Vest, PharmD, CDE, BCACP At the end of this presentation, pharmacist
Lipids & Hypertension Update
 Lipids & Hypertension Update No financial disclosures Michael W. Cullen, MD, FACC Senior Associate Consultant, Assistant Professor of Medicine Mayo Clinic Department of Cardiovascular Diseases 34 th Annual
Lipids & Hypertension Update No financial disclosures Michael W. Cullen, MD, FACC Senior Associate Consultant, Assistant Professor of Medicine Mayo Clinic Department of Cardiovascular Diseases 34 th Annual
Elements for a public summary
 VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Cardiovascular disease (CVD) is responsible for one-third of global deaths and is a leading and increasing contributor to the
VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Cardiovascular disease (CVD) is responsible for one-third of global deaths and is a leading and increasing contributor to the
New Guidelines in Dyslipidemia Management
 The Third IAS-OSLA Course on Lipid Metabolism and Cardiovascular Risk Muscat, Oman, February 2017 New Guidelines in Dyslipidemia Management Dr. Khalid Al-Waili, MD, FRCPC, DABCL Senior Consultant Medical
The Third IAS-OSLA Course on Lipid Metabolism and Cardiovascular Risk Muscat, Oman, February 2017 New Guidelines in Dyslipidemia Management Dr. Khalid Al-Waili, MD, FRCPC, DABCL Senior Consultant Medical
2017 Cardiovascular Summit for Primary Care Thursday 30th & Friday 31st March Crowne Plaza, Dublin
 2017 Cardiovascular Summit for Primary Care Thursday 30th & Friday 31st March 2017 - Crowne Plaza, Dublin 2016 ESC Guidelines on Cardiovascular Risk and elevated lipids Carlos Brotons Sardenya Primary
2017 Cardiovascular Summit for Primary Care Thursday 30th & Friday 31st March 2017 - Crowne Plaza, Dublin 2016 ESC Guidelines on Cardiovascular Risk and elevated lipids Carlos Brotons Sardenya Primary
Antihyperlipidemic Drugs
 Antihyperlipidemic Drugs Lipid disorders: Disorders of lipid metabolism are manifest by elevation of the plasma concentrations of the various lipid and lipoprotein fractions (total and LDL cholesterol,
Antihyperlipidemic Drugs Lipid disorders: Disorders of lipid metabolism are manifest by elevation of the plasma concentrations of the various lipid and lipoprotein fractions (total and LDL cholesterol,
Learning Objectives. Patient Case
 Joseph Saseen, Pharm.D., FASHP, FCCP, BCPS Professor and Vice Chair, Department of Clinical Pharmacy University of Colorado Anschutz Medical Campus Learning Objectives Identify the 4 patient populations
Joseph Saseen, Pharm.D., FASHP, FCCP, BCPS Professor and Vice Chair, Department of Clinical Pharmacy University of Colorado Anschutz Medical Campus Learning Objectives Identify the 4 patient populations
Familial hypercholesterolaemia
 Familial hypercholesterolaemia Jaimini Cegla MRCP FRCPath PhD Consultant in Chemical Pathology and Metabolic Medicine Hammersmith Hospital Lipid Clinic 20 April 2017 An unrecognised, potentially fatal,
Familial hypercholesterolaemia Jaimini Cegla MRCP FRCPath PhD Consultant in Chemical Pathology and Metabolic Medicine Hammersmith Hospital Lipid Clinic 20 April 2017 An unrecognised, potentially fatal,
MOLINA HEALTHCARE OF CALIFORNIA
 MOLINA HEALTHCARE OF CALIFORNIA HIGH BLOOD CHOLESTEROL IN ADULTS GUIDELINE Molina Healthcare of California has adopted the Third Report of the National Cholesterol Education Program (NCEP) Expert Panel
MOLINA HEALTHCARE OF CALIFORNIA HIGH BLOOD CHOLESTEROL IN ADULTS GUIDELINE Molina Healthcare of California has adopted the Third Report of the National Cholesterol Education Program (NCEP) Expert Panel
Drug Prior Authorization Guideline PCSK9 Inhibitors -
 Drug Prior Authorization Guideline PCSK9 Inhibitors - REPATHA (evolocumab) PRALUENT (alirocumab) PA9911 Covered Service: Yes when meets criteria below Prior Authorization Required: Yes-as shown below Additional
Drug Prior Authorization Guideline PCSK9 Inhibitors - REPATHA (evolocumab) PRALUENT (alirocumab) PA9911 Covered Service: Yes when meets criteria below Prior Authorization Required: Yes-as shown below Additional
Antihyperlipidemic drugs
 Antihyperlipidemic drugs The clinically important lipoproteins are LDL low density lipoprotein, VLDL very low density lipoprotein, HDL high density lipoprotein. Hyperlipidemia may caused 1. by individual
Antihyperlipidemic drugs The clinically important lipoproteins are LDL low density lipoprotein, VLDL very low density lipoprotein, HDL high density lipoprotein. Hyperlipidemia may caused 1. by individual
VI.2 Elements for a public summary. VI.2.1 Overview of disease epidemiology
 VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology This medicine is used to lower levels of total cholesterol, LDL cholesterol ( bad cholesterol), and fatty substances called triglycerides
VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology This medicine is used to lower levels of total cholesterol, LDL cholesterol ( bad cholesterol), and fatty substances called triglycerides
Cardiovascular Risk and Dyslipidemia Management Clinician Guide SEPTEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Cardiovascular Risk and Dyslipidemia Management Clinician Guide SEPTEMBER 2017 Introduction This Clinician Guide is based on the 2017 KP National
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Cardiovascular Risk and Dyslipidemia Management Clinician Guide SEPTEMBER 2017 Introduction This Clinician Guide is based on the 2017 KP National
Lipids What s new? Meera Jain, MD Providence Portland Medical Center
 Lipids 2016- What s new? Meera Jain, MD Providence Portland Medical Center 1 Can I trust the ASCVD risk calculator? Do harms outweigh benefits in primary prevention? Is there anything besides a statin?
Lipids 2016- What s new? Meera Jain, MD Providence Portland Medical Center 1 Can I trust the ASCVD risk calculator? Do harms outweigh benefits in primary prevention? Is there anything besides a statin?
Major recommendations for statin therapy for ASCVD prevention
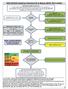 2013 A/AHA Guidelines holesterol Rx to Reduce ASVD Risk in Adults Major recommendations for statin therapy for ASVD prevention *% in LDL can be used as indication of response & adherence to Rx but is not
2013 A/AHA Guidelines holesterol Rx to Reduce ASVD Risk in Adults Major recommendations for statin therapy for ASVD prevention *% in LDL can be used as indication of response & adherence to Rx but is not
Clinical Practice Guideline
 Clinical Practice Guideline Secondary Prevention for Patients with Coronary and Other Vascular Disease Since the 2001 update of the American Heart Association (AHA)/American College of Cardiology (ACC)
Clinical Practice Guideline Secondary Prevention for Patients with Coronary and Other Vascular Disease Since the 2001 update of the American Heart Association (AHA)/American College of Cardiology (ACC)
Antihyperlipidemic Drugs
 Antihyperlipidemic Drugs Hyperlipidemias. Hyperlipoproteinemias. Hyperlipemia. Hypercholestrolemia. Direct relationship with acute pancreatitis and atherosclerosis Structure Lipoprotein Particles Types
Antihyperlipidemic Drugs Hyperlipidemias. Hyperlipoproteinemias. Hyperlipemia. Hypercholestrolemia. Direct relationship with acute pancreatitis and atherosclerosis Structure Lipoprotein Particles Types
DYSLIPIDEMIA PHARMACOLOGY. University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 DYSLIPIDEMIA PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Know normal cholesterol levels Understand what the role
DYSLIPIDEMIA PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Know normal cholesterol levels Understand what the role
Volume 2; Number 14 September 2008 NICE CLINICAL GUIDELINE 66: TYPE 2 DIABETES THE MANAGEMENT OF TYPE 2 DIABETES (MAY 2008)
 Volume 2; Number 14 September 2008 NICE CLINICAL GUIDELINE 66: TYPE 2 DIABETES THE MANAGEMENT OF TYPE 2 DIABETES (MAY 2008) The purpose of this special edition of the PACE Bulletin is to summarize the
Volume 2; Number 14 September 2008 NICE CLINICAL GUIDELINE 66: TYPE 2 DIABETES THE MANAGEMENT OF TYPE 2 DIABETES (MAY 2008) The purpose of this special edition of the PACE Bulletin is to summarize the
In the Know: Canadian Guidelines for Dyslipidemia, 2003
 In the Know: Canadian Guidelines for Dyslipidemia, 2003 In his reviews of Canadian dyslipidemia guidelines, Dr. Curnew explores the impact of major trials, the assessment and categories of risk, and both
In the Know: Canadian Guidelines for Dyslipidemia, 2003 In his reviews of Canadian dyslipidemia guidelines, Dr. Curnew explores the impact of major trials, the assessment and categories of risk, and both
Common Repatha Documentation Requirements for Patients With Primary Hyperlipidemia and Established CVD 1,2
 Established CVD Common Repatha Documentation Requirements for Patients With Primary Hyperlipidemia and Established CVD 1,2 Primary and Secondary Diagnosis Codes Primary Diagnosis: Primary hyperlipidemia
Established CVD Common Repatha Documentation Requirements for Patients With Primary Hyperlipidemia and Established CVD 1,2 Primary and Secondary Diagnosis Codes Primary Diagnosis: Primary hyperlipidemia
PREVENTION OF CARDIOVASCULAR DISEASE IN WOMEN
 PREVENTION OF CARDIOVASCULAR DISEASE IN WOMEN Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest EXPLAINING THE DECREASE
PREVENTION OF CARDIOVASCULAR DISEASE IN WOMEN Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest EXPLAINING THE DECREASE
High ( 50%) Restrictions mg 20-40mg PA; TS ⱡ 15 ⱡ
 MEDICATION COVERAGE POLICY PHARMACY AND THERAPEUTICS ADVISORY COMMITTEE POLICY: Cholesterol P&T DATE: 5/9/2017 THERAPEUTIC CLASS: Cardiovascular REVIEW HISTORY: 5/16, 5/15, 2/14, 5/12, LOB AFFECTED: Medi-Cal
MEDICATION COVERAGE POLICY PHARMACY AND THERAPEUTICS ADVISORY COMMITTEE POLICY: Cholesterol P&T DATE: 5/9/2017 THERAPEUTIC CLASS: Cardiovascular REVIEW HISTORY: 5/16, 5/15, 2/14, 5/12, LOB AFFECTED: Medi-Cal
2013 ACC/AHA Cholesterol Guidelines JULIE HAMMOND, D.O. PGY-2 MATTHEW PAOLI, D.O. PGY-2
 2013 ACC/AHA Cholesterol Guidelines JULIE HAMMOND, D.O. PGY-2 MATTHEW PAOLI, D.O. PGY-2 GOALS ACC/AHA as publisher of guidelines Determining which patients are appropriate for statin therapy The treatment
2013 ACC/AHA Cholesterol Guidelines JULIE HAMMOND, D.O. PGY-2 MATTHEW PAOLI, D.O. PGY-2 GOALS ACC/AHA as publisher of guidelines Determining which patients are appropriate for statin therapy The treatment
B. Patient has not reached the percentage reduction goal with statin therapy
 Managing Cardiovascular Risk: The Importance of Lowering LDL Cholesterol and Reaching Treatment Goals for LDL Cholesterol The Role of the Pharmacist Learning Objectives 1. Review the role of lipid levels
Managing Cardiovascular Risk: The Importance of Lowering LDL Cholesterol and Reaching Treatment Goals for LDL Cholesterol The Role of the Pharmacist Learning Objectives 1. Review the role of lipid levels
Younger adults with a family history of premature artherosclerotic disease should have their cardiovascular risk factors measured.
 Appendix 2A - Guidance on Management of Hypertension Measurement of blood pressure All adults from 40 years should have blood pressure measured as part of opportunistic cardiovascular risk assessment.
Appendix 2A - Guidance on Management of Hypertension Measurement of blood pressure All adults from 40 years should have blood pressure measured as part of opportunistic cardiovascular risk assessment.
Young high risk patients the role of statins Dr. Mohamed Jeilan
 Young high risk patients the role of statins Dr. Mohamed Jeilan KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures
Young high risk patients the role of statins Dr. Mohamed Jeilan KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures
Coronary Artery Disease Clinical Practice Guidelines
 Coronary Artery Disease Clinical Practice Guidelines Guidelines are systematically developed statements to assist patients and providers in choosing appropriate healthcare for specific clinical conditions.
Coronary Artery Disease Clinical Practice Guidelines Guidelines are systematically developed statements to assist patients and providers in choosing appropriate healthcare for specific clinical conditions.
Bibliographic Source(s) Guideline Status
 Lipid modification: cardiovascular risk assessment and the modification of blood lipids for the primary and secondary prevention of cardiovascular disease. Bibliographic Source(s) National Clinical Guideline
Lipid modification: cardiovascular risk assessment and the modification of blood lipids for the primary and secondary prevention of cardiovascular disease. Bibliographic Source(s) National Clinical Guideline
Praluent. Praluent (alirocumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.40.06 Subject: Praluent Page: 1 of 10 Last Review Date: September 20, 2018 Praluent Description Praluent
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.40.06 Subject: Praluent Page: 1 of 10 Last Review Date: September 20, 2018 Praluent Description Praluent
Elements for a public summary
 VI.2 VI.2.1 Elements for a public summary Overview of disease epidemiology Familial hypercholesterolemia (FH) is a genetic disorder characterized by high cholesterol levels, specifically very high levels
VI.2 VI.2.1 Elements for a public summary Overview of disease epidemiology Familial hypercholesterolemia (FH) is a genetic disorder characterized by high cholesterol levels, specifically very high levels
Cholesterol Management Roy Gandolfi, MD
 Cholesterol Management 2017 Roy Gandolfi, MD Goals Interpreting cholesterol guidelines Cholesterol treatment in diabetics Statin use and side effects therapy Reporting- Comparison data among physicians
Cholesterol Management 2017 Roy Gandolfi, MD Goals Interpreting cholesterol guidelines Cholesterol treatment in diabetics Statin use and side effects therapy Reporting- Comparison data among physicians
Rosuvastatin 5 mg, 10 mg and 20 mg Tablet
 Rosuvastatin 5 mg, 10 mg and 20 mg Tablet Description is a preparation of Rosuvastatin. Rosuvastatin is a member of the drug class of statins, used in combination with exercise, diet, and weight-loss to
Rosuvastatin 5 mg, 10 mg and 20 mg Tablet Description is a preparation of Rosuvastatin. Rosuvastatin is a member of the drug class of statins, used in combination with exercise, diet, and weight-loss to
ANTIHYPERLIPIDEMIA. Darmawan,dr.,M.Kes,Sp.PD
 ANTIHYPERLIPIDEMIA Darmawan,dr.,M.Kes,Sp.PD Plasma lipids consist mostly of lipoproteins Spherical complexes of lipids and specific proteins (apolipoproteins). The clinically important lipoproteins, listed
ANTIHYPERLIPIDEMIA Darmawan,dr.,M.Kes,Sp.PD Plasma lipids consist mostly of lipoproteins Spherical complexes of lipids and specific proteins (apolipoproteins). The clinically important lipoproteins, listed
How to Handle Statin Intolerance in the High Risk Patient
 How to Handle Statin Intolerance in the High Risk Patient Thomas D. Conley, MD FACC FSCAI Disclosures: None 1 Definition of High Risk Primary Prevention ASCVD Risk Calculator Adults >21 yrs, LDL 190 mg/dl
How to Handle Statin Intolerance in the High Risk Patient Thomas D. Conley, MD FACC FSCAI Disclosures: None 1 Definition of High Risk Primary Prevention ASCVD Risk Calculator Adults >21 yrs, LDL 190 mg/dl
Lipids What s new (and what s not)
 Lipids What s new (and what s not) Overview Background evidence Obesity Guidelines Treatment options Pragmatic lipidology Side effects Familial Hypercholesterolaemia Cases Summary Background evidence CHD
Lipids What s new (and what s not) Overview Background evidence Obesity Guidelines Treatment options Pragmatic lipidology Side effects Familial Hypercholesterolaemia Cases Summary Background evidence CHD
Lipid Guidelines Who, What, and How Low. Anita Ralstin, MS, CNP Next Step Health Consultant, LLC New Mexico Heart Institute
 Lipid Guidelines Who, What, and How Low Anita Ralstin, MS, CNP Next Step Health Consultant, LLC New Mexico Heart Institute Disclosures! None Objectives! List factors used in screening for dyslipidemia
Lipid Guidelines Who, What, and How Low Anita Ralstin, MS, CNP Next Step Health Consultant, LLC New Mexico Heart Institute Disclosures! None Objectives! List factors used in screening for dyslipidemia
ATP IV: Predicting Guideline Updates
 Disclosures ATP IV: Predicting Guideline Updates Daniel M. Riche, Pharm.D., BCPS, CDE Speaker s Bureau Merck Janssen Boehringer-Ingelheim Learning Objectives Describe at least two evidence-based recommendations
Disclosures ATP IV: Predicting Guideline Updates Daniel M. Riche, Pharm.D., BCPS, CDE Speaker s Bureau Merck Janssen Boehringer-Ingelheim Learning Objectives Describe at least two evidence-based recommendations
Long-Term Complications of Diabetes Mellitus Macrovascular Complication
 Long-Term Complications of Diabetes Mellitus Macrovascular Complication Sung Hee Choi MD, PhD Professor, Seoul National University College of Medicine, SNUBH, Bundang Hospital Diabetes = CVD equivalent
Long-Term Complications of Diabetes Mellitus Macrovascular Complication Sung Hee Choi MD, PhD Professor, Seoul National University College of Medicine, SNUBH, Bundang Hospital Diabetes = CVD equivalent
Management of Post-transplant hyperlipidemia
 Management of Post-transplant hyperlipidemia B. Gisella Carranza Leon, MD Assistant Professor of Medicine Lipid Clinic - Vanderbilt Heart and Vascular Institute Division of Diabetes, Endocrinology and
Management of Post-transplant hyperlipidemia B. Gisella Carranza Leon, MD Assistant Professor of Medicine Lipid Clinic - Vanderbilt Heart and Vascular Institute Division of Diabetes, Endocrinology and
What do the guidelines say about combination therapy?
 What do the guidelines say about combination therapy? Christie M. Ballantyne, MD Center for Cardiovascular Disease Prevention Methodist DeBakey Heart & Vascular Center Baylor College of Medicine Houston,
What do the guidelines say about combination therapy? Christie M. Ballantyne, MD Center for Cardiovascular Disease Prevention Methodist DeBakey Heart & Vascular Center Baylor College of Medicine Houston,
Prescribing Policy: Lipid Modification - Primary Prevention
 Prescribing Policy: Lipid Modification - Primary Prevention Policy Statement: Date of Approval: 11 th February 2010 This policy defines the decision made by the NHS Western Cheshire Clinical Commissioning
Prescribing Policy: Lipid Modification - Primary Prevention Policy Statement: Date of Approval: 11 th February 2010 This policy defines the decision made by the NHS Western Cheshire Clinical Commissioning
hyperlipidemia in CKD DR MOJGAN MORTAZAVI ASSOCIATE PROFESSOR OF NEPHROLOGY ISFAHAN KIDNEY DISEASES RESEARCH CENTER
 Management of hyperlipidemia in CKD DR MOJGAN MORTAZAVI ASSOCIATE PROFESSOR OF NEPHROLOGY ISFAHAN KIDNEY DISEASES RESEARCH CENTER Background on Dyslipidemia in CKD In advanced chronic kidney disease (CKD),
Management of hyperlipidemia in CKD DR MOJGAN MORTAZAVI ASSOCIATE PROFESSOR OF NEPHROLOGY ISFAHAN KIDNEY DISEASES RESEARCH CENTER Background on Dyslipidemia in CKD In advanced chronic kidney disease (CKD),
ESC/EAS Guidelines for the Management of Dyslipidaemias
 ESC/EAS Guidelines for the Management of Dyslipidaemias Professor Željko Reiner, MD, PhD, FRCP(Lond), FESC, FACC University Hospital Center Zagreb School of Medicine, University of Zagreb, Croatia Declaration
ESC/EAS Guidelines for the Management of Dyslipidaemias Professor Željko Reiner, MD, PhD, FRCP(Lond), FESC, FACC University Hospital Center Zagreb School of Medicine, University of Zagreb, Croatia Declaration
Drug Class Monograph
 Drug Class Monograph Class: Proprotein Convertase Subtilisin/Kexin Type 9 (PCSK9) Inhibitor Drugs: Praluent (alirocumab), Repatha (evolocumab) Line of Business: Medi-Cal Effective Date: February 17, 2016
Drug Class Monograph Class: Proprotein Convertase Subtilisin/Kexin Type 9 (PCSK9) Inhibitor Drugs: Praluent (alirocumab), Repatha (evolocumab) Line of Business: Medi-Cal Effective Date: February 17, 2016
Elements for a Public Summary
 Rosuvastatin Stada 5 mg film-coated tablets Rosuvastatin Stada 10 mg film-coated tablets Rosuvastatin Stada 20 mg film-coated tablets Rosuvastatin Stada 40 mg film-coated tablets 25.8.2014, V1.1 PUBLIC
Rosuvastatin Stada 5 mg film-coated tablets Rosuvastatin Stada 10 mg film-coated tablets Rosuvastatin Stada 20 mg film-coated tablets Rosuvastatin Stada 40 mg film-coated tablets 25.8.2014, V1.1 PUBLIC
An update on lipidology and cardiovascular risk management. Lipids, Metabolism & Vascular Risk Section - Royal Society of Medicine
 An update on lipidology and cardiovascular risk management Lipids, Metabolism & Vascular Risk Section - Royal Society of Medicine National and international lipid modification guidelines: A critical appraisal
An update on lipidology and cardiovascular risk management Lipids, Metabolism & Vascular Risk Section - Royal Society of Medicine National and international lipid modification guidelines: A critical appraisal
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Overview
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Overview Ezetimibe for the treatment of primary (heterozygous familial and non-familial) hypercholesterolaemia The overview is written by members of
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Overview Ezetimibe for the treatment of primary (heterozygous familial and non-familial) hypercholesterolaemia The overview is written by members of
Repatha. Repatha (evolocumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.40.08 Subject: Repatha Page: 1 of 9 Last Review Date: September 15, 2017 Repatha Description Repatha
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.40.08 Subject: Repatha Page: 1 of 9 Last Review Date: September 15, 2017 Repatha Description Repatha
Request for Prior Authorization for PCSK9 inhibitor therapy Website Form Submit request via: Fax
 Request for Prior Authorization for PCSK9 inhibitor therapy Website Form www.highmarkhealthoptions.com Submit request via: Fax - 1-855-476-4158 PCSK9 is a protein that reduces the hepatic removal of low-density
Request for Prior Authorization for PCSK9 inhibitor therapy Website Form www.highmarkhealthoptions.com Submit request via: Fax - 1-855-476-4158 PCSK9 is a protein that reduces the hepatic removal of low-density
Repatha. Repatha (evolocumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.40.08 Subject: Repatha Page: 1 of 9 Last Review Date: November 30, 2018 Repatha Description Repatha (evolocumab)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.40.08 Subject: Repatha Page: 1 of 9 Last Review Date: November 30, 2018 Repatha Description Repatha (evolocumab)
Drug regulation of serum lipids
 Drug regulation of serum lipids Foundations of Biomedical Science MEDS90001 Dr Michelle Hansen Pharmacology & Therapeutics mjhansen@unimelb.edu.au References Katzung, Basic & Clinical Pharmacology Ch 35
Drug regulation of serum lipids Foundations of Biomedical Science MEDS90001 Dr Michelle Hansen Pharmacology & Therapeutics mjhansen@unimelb.edu.au References Katzung, Basic & Clinical Pharmacology Ch 35
Non-Statin Lipid-Lowering Agents M Holler - Last updated: 10/2016
 Drug/Class Cholestyramine (Questran) Bile acid sequestrant Generic? Lipid Effects Y/N (monotherapy) Y LDL : 9% (4 g to 8 ; 21% (16 g to 20 ; 23% to 28% (>20 HDL : 4% to 8% (16 to 24 TG : 11% to 28% (4
Drug/Class Cholestyramine (Questran) Bile acid sequestrant Generic? Lipid Effects Y/N (monotherapy) Y LDL : 9% (4 g to 8 ; 21% (16 g to 20 ; 23% to 28% (>20 HDL : 4% to 8% (16 to 24 TG : 11% to 28% (4
Hyperlipidemia. Prepared by : Muhannad Mohammed Supervisor professor : Dr. Ahmed Yahya Dallalbashi
 Hyperlipidemia Prepared by : Muhannad Mohammed Supervisor professor : Dr. Ahmed Yahya Dallalbashi Outline The story of lipids Definition of hyperlipidemia Classification of hyperlipidemia Causes of hyperlipidemia
Hyperlipidemia Prepared by : Muhannad Mohammed Supervisor professor : Dr. Ahmed Yahya Dallalbashi Outline The story of lipids Definition of hyperlipidemia Classification of hyperlipidemia Causes of hyperlipidemia
Lipid Lowering in patients with High Risk of Cardiovascular Disease (Primary Prevention)
 Lipid Lowering in patients with High Risk of Cardiovascular Disease (Primary Prevention) Policy Statement: October 2010 This policy defines the decision made by NHS Wirral following an evidence review
Lipid Lowering in patients with High Risk of Cardiovascular Disease (Primary Prevention) Policy Statement: October 2010 This policy defines the decision made by NHS Wirral following an evidence review
Appendix F Simon Broome Diagnostic criteria for index individuals and relatives
 Appendix F Simon Broome Diagnostic criteria for index individuals and relatives 1 SIMON BROOME DIAGNOSTIC CRITERIA FOR INDEX INDIVIDUALS (PROBANDS) 2 2 GENDER- AND AGE-SPECIFIC LDL-C CRITERIA FOR THE DIAGNOSIS
Appendix F Simon Broome Diagnostic criteria for index individuals and relatives 1 SIMON BROOME DIAGNOSTIC CRITERIA FOR INDEX INDIVIDUALS (PROBANDS) 2 2 GENDER- AND AGE-SPECIFIC LDL-C CRITERIA FOR THE DIAGNOSIS
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Primary prevention of CVD Potential output:
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Primary prevention of CVD Potential output:
Disclosure. No relevant financial relationships. Placebo-Controlled Statin Trials
 MANAGEMENT OF HYPERLIPIDEMIA AND CARDIOVASCULAR RISK IN WOMEN: Balancing Benefits and Harms Disclosure Robert B. Baron, MD MS Professor and Associate Dean UCSF School of Medicine No relevant financial
MANAGEMENT OF HYPERLIPIDEMIA AND CARDIOVASCULAR RISK IN WOMEN: Balancing Benefits and Harms Disclosure Robert B. Baron, MD MS Professor and Associate Dean UCSF School of Medicine No relevant financial
Case Studies The Role of Non-Statin Therapies for LDL-C Lowering in the Management of ASCVD Risk
 Case Studies The Role of Non-Statin Therapies for LDL-C Lowering in the Management of ASCVD Risk Kim K. Birtcher, PharmD, MS, AACC Clinical Professor University of Houston College of Pharmacy Houston,
Case Studies The Role of Non-Statin Therapies for LDL-C Lowering in the Management of ASCVD Risk Kim K. Birtcher, PharmD, MS, AACC Clinical Professor University of Houston College of Pharmacy Houston,
DYSLIPIDEMIA. Michael Brändle, Stefan Bilz
 DYSLIPIDEMIA Michael Brändle, Stefan Bilz Cardiovascular risk in patients with DM Current guidelines with emphasis on patients with DM Familial Hypercholesterolemia PCSK9-inhibitors Primary Prevention
DYSLIPIDEMIA Michael Brändle, Stefan Bilz Cardiovascular risk in patients with DM Current guidelines with emphasis on patients with DM Familial Hypercholesterolemia PCSK9-inhibitors Primary Prevention
Drug Class Prior Authorization Criteria PCSK9 Inhibitors
 Drug Class Prior Authorization Criteria PCSK9 Inhibitors Line of Business: Medicaid P & T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has been developed through review of
Drug Class Prior Authorization Criteria PCSK9 Inhibitors Line of Business: Medicaid P & T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has been developed through review of
Package leaflet: Information for the user. Pravastatin Actavis 20 mg and 40 mg tablets (pravastatin sodium)
 PACKAGE LEAFLET Package leaflet: Information for the user Pravastatin Actavis 20 mg and 40 mg tablets (pravastatin sodium) Read all of this leaflet carefully before you start taking this medicine because
PACKAGE LEAFLET Package leaflet: Information for the user Pravastatin Actavis 20 mg and 40 mg tablets (pravastatin sodium) Read all of this leaflet carefully before you start taking this medicine because
Diabetes Complications Guideline Based Screening, Management, and Referral
 Diabetes Complications Guideline Based Screening, Management, and Referral Eric L. Johnson, M.D. Associate Professor Department of Family and Community Medicine Assistant Medical Director Altru Diabetes
Diabetes Complications Guideline Based Screening, Management, and Referral Eric L. Johnson, M.D. Associate Professor Department of Family and Community Medicine Assistant Medical Director Altru Diabetes
DYSLIPIDEMIA RECOMMENDATIONS
 DYSLIPIDEMIA RECOMMENDATIONS Α. DIAGNOSIS Recommendation 1 INITIAL LIPID PROFILING (Level of evidence II) It is recommended to GPs and other PHC Physicians to assess the lipid profile {total cholesterol
DYSLIPIDEMIA RECOMMENDATIONS Α. DIAGNOSIS Recommendation 1 INITIAL LIPID PROFILING (Level of evidence II) It is recommended to GPs and other PHC Physicians to assess the lipid profile {total cholesterol
Diabetic Dyslipidemia
 Diabetic Dyslipidemia Dr R V S N Sarma, M.D., (Internal Medicine), M.Sc., (Canada), Consultant Physician Cardiovascular disease (CVD) is a significant cause of illness, disability, and death among individuals
Diabetic Dyslipidemia Dr R V S N Sarma, M.D., (Internal Medicine), M.Sc., (Canada), Consultant Physician Cardiovascular disease (CVD) is a significant cause of illness, disability, and death among individuals
No relevant financial relationships
 MANAGEMENT OF LIPID DISORDERS Balancing Benefits and harms Disclosure Robert B. Baron, MD MS Professor and Associate Dean UCSF School of Medicine No relevant financial relationships baron@medicine.ucsf.edu
MANAGEMENT OF LIPID DISORDERS Balancing Benefits and harms Disclosure Robert B. Baron, MD MS Professor and Associate Dean UCSF School of Medicine No relevant financial relationships baron@medicine.ucsf.edu
Disclosures. Diabetes and Cardiovascular Risk Management. Learning Objectives. Atherosclerotic Cardiovascular Disease
 Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
Repatha. Repatha (evolocumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.40.08 Subject: Repatha Page: 1 of 8 Last Review Date: December 2, 2016 Repatha Description Repatha (evolocumab)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.40.08 Subject: Repatha Page: 1 of 8 Last Review Date: December 2, 2016 Repatha Description Repatha (evolocumab)
Cholesterol. Medicines To Help You
 Medicines To Help You Cholesterol Use this guide to help you talk to your doctor, pharmacist, or nurse about your cholesterol medicines. The guide lists all of the FDA-approved products now available to
Medicines To Help You Cholesterol Use this guide to help you talk to your doctor, pharmacist, or nurse about your cholesterol medicines. The guide lists all of the FDA-approved products now available to
REPATHA (PCSK9 INHIBITORS)
 REPATHA (PCSK9 INHIBITS) Indications: PCSK9 Inhibitors are indicated for treatment of adults with heterozygous familial hypercholesterolemia (HeFH) or clinical atherosclerotic cardiovascular disease as
REPATHA (PCSK9 INHIBITS) Indications: PCSK9 Inhibitors are indicated for treatment of adults with heterozygous familial hypercholesterolemia (HeFH) or clinical atherosclerotic cardiovascular disease as
Dyslipidemia. (Med-341)
 Dyslipidemia (Med-341) Anwar A Jammah, MD, FRCPC, FACP, CCD, ECNU. Associate Professor of Medicine Consultant Medicine, Endocrinology, Thyroid Oncology Department of Medicine, King Saud University The
Dyslipidemia (Med-341) Anwar A Jammah, MD, FRCPC, FACP, CCD, ECNU. Associate Professor of Medicine Consultant Medicine, Endocrinology, Thyroid Oncology Department of Medicine, King Saud University The
Cardiovascular risk assessment and the modification of blood lipids for the primary and secondary prevention of cardiovascular disease
 Issue date: May 2008 Lipid modification Cardiovascular risk assessment and the modification of blood lipids for the primary and secondary prevention of cardiovascular disease NICE clinical guideline 67
Issue date: May 2008 Lipid modification Cardiovascular risk assessment and the modification of blood lipids for the primary and secondary prevention of cardiovascular disease NICE clinical guideline 67
Pharmacy Management Drug Policy
 SUBJECT: ; Praluent (alirocumab), Repatha (evolocumab) POLICY NUMBER: Pharmacy-61 EFFECTIVE DATE: 8/15 LAST REVIEW DATE: 9/22/2017 If the member s subscriber contract excludes coverage for a specific service
SUBJECT: ; Praluent (alirocumab), Repatha (evolocumab) POLICY NUMBER: Pharmacy-61 EFFECTIVE DATE: 8/15 LAST REVIEW DATE: 9/22/2017 If the member s subscriber contract excludes coverage for a specific service
PCSK9 Agents Drug Class Prior Authorization Protocol
 PCSK9 Agents Drug Class Prior Authorization Protocol Line of Business: Medicaid P & T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has been developed through review of medical
PCSK9 Agents Drug Class Prior Authorization Protocol Line of Business: Medicaid P & T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has been developed through review of medical
