A Clinical Review of Implantable Cardioverter Defibrillators and Bi-Ventricular Pacemakers at one Institute
|
|
|
- Frank Sparks
- 5 years ago
- Views:
Transcription
1 A Clinical Review of Implantable Cardioverter Defibrillators and Bi-Ventricular Pacemakers at one Institute Author Nasir, Ahmad, Batra, Ravinder, Jayasinghe, Satyajit Published 200 Journal Title Australasian Medical Journal DOI Copyright Statement The Author(s) 200. The attached file is reproduced here in accordance with the copyright policy of the publisher. For information about this journal please refer to the journal's website or contact the authors. Downloaded from Griffith Research Online
2 Australasian Medical Journal 200,,, A Clinical Review of Implantable Cardioverter Defibrillators and Bi-Ventricular Pacemakers at one Institute Ahmad Nasir, Ravinder Batra 2, Rohan Jayasinghe 3 Gold Coast Hospital, Southport, 2 Griffith University School of Medicine, Queensland, Australia CLINICAL AUDIT Please cite this paper as: Nasir A, Batra R and Jayasingle R. A Clinical Review of Implantable Cardioverter Defibrillators and Bi-Ventricular Pacemakers at one Institute. AMJ 200,,, Doi /AMJ Corresponding Author: Ahmad Nasir Gold Coast Hospital Southport radhiahmad@hotmail.com Abstract Background: ICD/BVP indications are expanding. They are expensive devices and historically, morbidities associated with their use were high. The starting experience at the Gold Coast Hospital is being reviewed. Methods: A retrospective chart review of all the ICD/BVPs implanted in the Gold Coast Hospital from 06/07/2007 7/06/2008, with special emphasis on device indications and complications. Results: Devices implanted were (3). Primary prevention devices (67%), secondary prevention devices (33%). Indications were; Non-ischemic Dilated Cardiomyopathy (35%), Out-of-hospital Cardiac Arrest (26%), Conscious VT (3%), Ischemic Dilated Cardiomyopathy (0%), In-hospital Cardiac Arrest (6%), Long-QT Syndrome (6%) and Catecholamine-related Polymorphic VT (3%). Major complications reported; lung contusion (), left haemothorax (), failed coronary sinus lead positioning (2), lead repositioning (2), atrial lead removal (), left subclavian vein thrombosis (), lead malfunction leading to VT under sensing and syncope (). Device-administered therapies were eight; Inappropriate discharges (5), Appropriate discharges (), successful Anti-tachycardia Pacing (2). Conclusions: We believe that ICDs are very effective lifesaving devices but unfortunately they still are very expensive and their use can be associated with significant morbidities especially during the learning curve. Introduction ICDs are very effective in the secondary prevention of sudden cardiac death; their effectiveness over placebo and antiarrhythmic drugs has been demonstrated in major multicentre randomised controlled trials (6, 7, 8, and 9). The indications for the implantation of ICDs have quickly expanded from the secondary prevention of sudden cardiac death in persons who suffered a VT/ VF cardiac arrest to be used more in the primary prevention of sudden cardiac death in persons at risk of arrhythmic cardiac death after their effectiveness was shown in big trials (6,0,,2,3) the factor which had the largest impact on the increase in their use in recent years, the benefit is claimed to be a 20 30% relative reduction in mortality at one year, which is maintained over 3 5 years of follow-up, the absolute mortality benefit was approximately 3% per year compared to standard medical treatment (). BVPs is another area of device therapy which is quickly developing; BVPs reduce symptoms and frequency of hospitalisation when carried out in patients with symptomatic dilated CHF and prolonged QRS duration. A recent study has also demonstrated a mortality benefit of BVPs in patients with heart failure (, 3). We wanted to present our own registry in the first year of our institute s experience with ICD/BVPs implantation, looking mainly at the implantation indications and all complications that we could trace. Methods A list of all ICDs and BVPs was taken from the catheter laboratory at the Gold Coast Hospital from the start of the program with the first ICD implanted on 6 th July 2007 till the end of analysis period on the 7 th July 2008 which included a total of thirty one devices, charts were requested and reviewed. Excel tables were created with the patients characteristics, device indications, device type by function, device manufacturer, device cost, procedure time, hospital stay, use of antibiotics, use of chest x-ray to check for device position and procedure complication, device check by manufacturer, documented immediate complications, follow up including all device related re-admissions, device check-up and all adjustments, referrals to another institute and their outcomes. Results A total of 3 devices in 3 patients were implanted (25 male, 6 female), Mean patient s age was 58 years (20-75 years), and mean follow-up period was 9 months (3-5 months). Primary prevention devices were 2 (67%), secondary prevention devices were 0 (33%), the commonest single indication in our series was nonischemic dilated cardiomyopathy ( patients 35%), the second most common indication was out-of-hospital cardiac arrest which occurred in 8 patients (26%) while conscious VT was next (4 patients 3%), ischemic dilated cardiomyopathy 3 patients (0%), 2 patients (6%) had inhospital-cardiac arrest, 2 patients had congenital long QT syndrome (6%) and patient had catecholamine-related polymorphic VT (3%), table (). 23
3 Australasian Medical Journal 200,,, For patient s characteristics, co-morbidities and medications refer to tables (2, 3, 4) 2 devices (70%) were single chamber ICDs with a single right ventricular sensing pacing and defibrillating lead, 4 devices (3%) were double chamber ICDs with an additional atrial sensing and pacing lead as well, 5 devices (6%) were BVPs with the addition of a coronary sinus lead to the double chamber ICD to pace the left ventricle to achieve cardiac resynchronization function and finally, one patient had an ICD pulse generator replaced only (because of battery run out). Devices manufacturers were; St. Jude Medical 7 devices (55%), Medtronic devices (35%) and Guidant 3 devices (0%). All devices were implanted subcutaneously in the left pectoral area; all patients had prophylactic antibiotics intra-operatively with intra-venous Cephazolin plus intra-venous Gentamycin in selected patients. All patients had prophylactic oral antibiotics with Cephalexin for 5 days post-procedure. All patients in our series had a check chest X-ray the first post-procedure day, all devices were checked by manufacturer, all patients had device check at 6 weeks and then at 6 monthly intervals thereafter except one patient. The majority of the devices were implanted in a day procedure, 8 (58%), 8 patients (26%) had a hospital stay from 2-7 days, of them 3 patients had a conscious VT within the same hospital admission and 5 patients (6%) had a hospital stay of more than 7 days all of them had a cardiac arrest within the same hospital admission and a prolonged intensive care unit stay prior to the implantation procedure. Procedure duration was properly documented in 25 patients (80%), in the majority it was less than 90 minutes (7 procedures 54%), only 4 (3%) procedures lasted longer than 80 minutes and they were all BVPs. Twenty one patients (67%) in our series had reported some complications, ten had reported none, and around thirty complication occurrences were documented. These were procedure related or device related. Procedural complications were; significant pain requiring narcotic analgesics in six patients, significant bleeding from implantation wound which required local pressure in two patients plus intra-venous desmopressin infusion in one patient, local hematoma in one patient which happened on the 8 th post-procedure day secondary to minor trauma, minor haemoptysis on the 3 rd post-procedure day in one patient (CT scan of the chest confirmed lung contusion which was managed conservatively) and one patient was admitted with left sided haemothorax on the 4 th post-procedure day despite the fact that chest X-ray taken on the st post-procedure day was normal, required two inter-costal chest drains and video-assisted thoracoscopic procedure to stop the bleeding, two patients failed coronary sinus lead positioning for BVP, one patient eventually had an epicardial lead placed on mini-thoracotomy at another hospital to achieve BV pacing, the other was changed to single chamber ICD mode and the atrial lead was retrieved at a later date because that patient developed atrial fibrillation and failed cardio-version, one patient developed left subclavian vein thrombosis on the 0 th post-procedure day, one patient developed persistent left shoulder and ICD pocket pain and was referred to another hospital to consider submuscular implantation of the ICD. As far as the device complications are concerned, Inappropriate discharges occurred in four patients, in the first patient it was for a supraventricular tachycardia falling in the VT detection zone for that the ICD was reprogrammed, in the second patient it was for a nonsustained VT after anti-tachycardia pacing mode failure secondary to under-rate detection for which ICD was reprogrammed but inappropriate discharge recurred for a non-sustained VT as well which failed to respond to antitachycardia pacing therapy appropriately delivered by the device this patient was started on treatment with amiodarone to suppress the non-sustained VTs, in a third patient it was for an atrial flutter falling in the VT detection zone in whom a trial of radiofrequency catheter ablation of the atrial flutter was attempted but failed and both atrial flutter and inappropriate discharge of the ICD recurred, the patient was eventually referred to another hospital to attempt atrial flutter ablation with a thermocool catheter and 3D mapping, and in the last patient it was for over-sensing noise caused by ICD pocket manipulation, in this patient the right ventricular lead was unscrewed and re-inserted at the ICD pocket. One patient received an appropriate discharge which was for VF properly sensed and terminated. Other therapies administered were anti-tachycardia pacing which successfully terminated sustained VT in two patients. Lead related complications occurred in five patients; coronary sinus lead needed to be repositioned in one patient because of diaphragmatic stimulation on the 22 nd post-implantation day, right ventricular lead had to be repositioned into right ventricular apex in one patient on the 5 th post-implantation day as was under-sensing, atrial lead had to be removed on the 0 th post-implantation day in one patient as it was not in place and the patient developed atrial fibrillation which persisted after a trial of electric cardio-version, right ventricular lead had to be repositioned in one patient because of high threshold on the 29 th post-implantation day and lastly one patient needed a special right ventricular lead to replace the original lead which was done in a different hospital because of VT un-detection leading to a syncopal event which happened on day 44 post-implantation. 44 of readmission days directly related to ICD problems happened because of these complications, and a total of 4 patients had to be referred to another institute to deal with these complications as outlined above as our institute lacked the technology or the personnel to deal with those complications. For a summary of device complication refer to (table-5). Discussion ICD/BVPs are very effective life-saving devices that are also very costly which is an important limitation to their use; device only cost in our registry was Australian Dollars. In addition their use can be associated 24
4 Australasian Medical Journal 200,,, with a lot of complications that can affect patients quality of life quite adversely; these complications make the second important limitation to the expansion in their use. The incidence of ICD complications is difficult to determine due to inconsistent definitions and the lack of mandatory reporting. Information comes from annual reports filed with the United States Food and Drug Administration, by companies that make devices and from voluntary registries (2). Approximately 50% of patients experience an adverse event within the first year after ICD implantation (2, 3). The rate of freedom from any adverse event at, 3, and 2 months was 79, 68, and 5 percent, respectively as was illustrated in a prospective study of 778 patients receiving a trans-venous ICD (2,3). Among the complications that occurred, 60 % were due to the ICD system, 29 % were related to the implantation procedure and % were not device-related (2). As far as procedural complications are concerned, a peri-procedural mortality of % has been reported (2), incidence of severe bleeding was.5%, and infection of the generator pocket or leads has been reported in up to 7%. ICD system problems included lead failure; the estimated lead survival rates at 5 and 8 years are 85% and 60% respectively. The annual defect rate increases with time and reaches 20% in 0-year-old leads (5) mainly due to lead dislodgement, fracture, and insulation defects (2, 5). The other common complication is inappropriate shocks which occurred in 20-25% of ICD patients the main cause being supra-ventricular tachy-arrhythmias including sinus tachycardia, atrial fibrillation, and the other important cause is non-sustained VT (2). In conclusion, we believe that ICDs are very effective lifesaving devices but unfortunately they still are very expensive and their use can be associated with significant morbidities especially during the learning curve. We appreciate the limitation of our data and that generalisation is difficult because our sample size is quite small, and it early experience in a single public hospital with a relatively low volume of device implantation basically led by one cardiologist. But we believe that it represents the experience of many programs on a learning curve and we present our experience to help those planning to start a similar program. Reference ) Guidelines for the prevention, detection and management of chronic heart failure in Australia, 2006 (National Heart Foundation of Australia and the Cardiac Society of Australia and New Zealand) 2) Morton F Arnsdorf, MD, MACCLeonard I Ganz, MD, UpToDate.com : article on (Implantable cardioverterdefibrillators: Complications). 3) Rosenqvist, M, Beyer, T, Block, M, et al on behalf of the European 729 Jewel ICD Investigators. Adverse events with transvenous implantable cardioverter-defibrillators: A prospective multicenter study. Circulation 998; 98:663. cardioverter-defibrillators over a period of>0 years. Circulation 2007; 5: ) Eckstein, J, Koller, MT, Zabel, M, et al. Necessity for surgical revision of defibrillator leads implanted long-term: causes and management. Circulation 2008; 7: ) DiMarco, JP. Implantable cardioverter-defibrillators. New England Journal of Medicine 2003; 349:836. 7) The Antiarrhythmic versus Implantable Defibrillators (AVID) Investigators. A Comparison of antiarrhythmic-drug therapy with implantable defibrillators in patients resuscitated from near-fatal ventricular arrhythmias. New England Journal of Medicine 997;337: ) Connolly SJ, Gent M, Roberts RS, et al.canadian Implantable Defibrillator Study (CIDS): a randomized trial of the implantable cardioverter defibrillator against amiodarone. Circulation 2000;0: ) Kuck KH, Cappato R, Siebels J, Ruppel R. Randomized comparison of Antiarrhythmic drug therapy with implantable defibrillators in patients resuscitated from cardiac arrest: the Cardiac Arrest Study Hamburg (CASH). Circulation 2000;02: ) Moss AJ, Hall WJ, Cannom DS, et al. Improved survival with an implantable defibrillator in patients with coronary disease at high risk for ventricular arrhythmia. New England Journal of Medicine 996;335: ) Moss AJ, Zareba W, Hall WJ, et al. Prophylactic implantation of a defibrillator in patients with myocardial infarction and reduced ejection fraction. New England Journal of Medicine 2002;346: ) Bigger JT Jr. Prophylactic use of implanted cardiac defibrillators in patients at high risk for ventricular arrhythmias after coronary-artery bypass graft surgery. New England Journal of Medicine997; 337: ) Bänsch D, Antz M, Boczor S, et al. Primary prevention of sudden death in Idiopathic dilated cardiomyopathy: the Cardiomyopathy Trial (CAT). Circulation 2002; 05: ) Gervais R, Leclercq C, Shankar A, Jacobs S, Eiskjær H, Johannessen A, Freemantle N, Cleland JG, Tavazzi L, Daubert C; on behalf of the CARE-HF investigators. European Journal of Heart Failure Jul; (7): Epub 2009 Jun 7. 4) Kleemann, T, Becker, T, Doenges, K, et al. Annual rate of transvenous defibrillation lead defects in implantable 25
5 Australasian Medical Journal 200,,, PEER REVIEW Not commissioned; externally peer reviewed CONFLICT OF INTEREST The authors declare that they have no competing interests. TABLES Table () Number of patients for each device indication Device indication Number of Primary prevention of SCD 2 (67%) Ischemic DCM 3 (0%) Non-ischemic DCM (35%) Conscious VT (LV scar tissue) 4 (3%) LQTS CPVT (3%) Secondary prevention of SCD Out-of-hospital cardiac arrest Ischemic DCM IHD ( LV scar tissue) IHD ( LV aneurysm) LQTS In-hospital cardiac arrest Ischemic DCM IHD (LV aneurysm) 0 (33%) 8 (26%) 3 (0%) 3 (0%) (3%) (3%) (3%) (3%) Table key words: SCD (sudden cardiac death), LV (left ventricle), LQTS (long QT syndrome), CPVT (catechol-related polymorphic VT), DCM (dilated cardiomyopathy), IHD (ischemic heart disease). Table (2) Patient characteristics Patient s characteristics Number of Echocardiography: Left ventricular dilatation 22 (70%) Significant left ventricular 3 (60%) dilatation (LVEDD > 60 mm) 26 (83%) Reduced Left Ventricular EF (< 6 (23%) 50%) 5 (9%) Mild LVSD (EF 40-49%) 5 (58%) Moderate LVSD ( EF 30-39%) 5 (50%) Severe LVSD ( EF < 30%) 3 (42%) Regional wall motion abnormality (hypo/akinesia) Global left ventricular hypokinesis Coronary angiography: Normal coronaries Stable coronary artery disease (no intervention) Coronary artery disease requiring intervention (stent) Electrocardiography: Rhythm Sinus Atrial Fibrillation/ Flutter Pathological Q- waves Wide QRS complex LBBB pattern RBBB pattern NIVCD pattern Non-specific T wave changes 22 (7%) (50%) 0 (32%) (3%) 27 (87%) 4 (3%) 2 (38%) 3 (42%) 0 (32%) (3%) 5 (48%) Table key word: LVEDD (left ventricle end-diastolic dimension), EF (ejection fraction), LVSD (left ventricular systolic dysfunction), LBBB (left bundle branch block), RBBB (right bundle branch block), NIVCD (non-specific intra-ventricular conduction delay). 26
6 Australasian Medical Journal 200,,, Table (3) Patients co-morbidities Co-morbidities: Number of Ischemic heart disease: 7(55%) Acute myocardial (33%) infarction history CABG surgery PCI/ stents Heart failure: NYHA class -2 NYHA class 3-4 Atrial Fibrillation/ Flutter: Diabetes Mellitus: Hypertension: Aortic valve replacement: Alcohol abuse: Dys-lipidemia: Cerebro-vascular accidents/ Transient ischemic attacks: Chronic obstructive airway disease: Thyroid disorders: Hyperthyroidism Hypothyroidism 27 (78%) 2 (77%) 6 (23%) 5 (6%) 6 (5%) 9 (29%) 4 (3%) 4 (3%) 3 (0%) Table (4) Medications taken by patients Medication Number of Beta- blockers 30 (96%) Carvedilol 3 (42%) Bisoprolol Metoprolol 5 (6%) Atenolol 4 (3%) Sotalol (3%) Angiotensin Converting Enzyme Inhibitors /Angiotensin 2 Antagonists Statins Aldosterone antagonists Spironolactone Epleronone anti-platelets/ anti-coagulants Aspirin Clopidogrel Warfarin Amiodarone Diuretics Frusemide Thiazide Digoxine 24 (77%) 8 (58%) 2 (38%) (35%) (3%) 23 (74%) 8 (58%) 6 (9%) 8 (25%) 6 (52%) 4 (45%) Chronic liver disease: Chronic renal failure: Table key words: CABG (coronary artery bypass graft), PCI (percutaneous coronary intervention), NYHA (New York Heart Association). Table (5) Device Complications Complication Procedure related Pain Bleeding Haematoma Lung contusion Haemothorax Subclavian vein thrombosis Failed coronary sinus lead positioning Persistent shoulder and ICD pocket pain Device/ lead related Inappropriate discharges Coronary sinus lead repositioning Right ventricular lead repositioning Atrial lead removal Right ventricular lead replacement Number of patients
Arrhythmias Focused Review. Who Needs An ICD?
 Who Needs An ICD? Cesar Alberte, MD, Douglas P. Zipes, MD, Krannert Institute of Cardiology, Indiana University School of Medicine, Indianapolis, IN Sudden cardiac arrest is one of the most common causes
Who Needs An ICD? Cesar Alberte, MD, Douglas P. Zipes, MD, Krannert Institute of Cardiology, Indiana University School of Medicine, Indianapolis, IN Sudden cardiac arrest is one of the most common causes
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
Primary prevention ICD recipients: the need for defibrillator back-up after an event-free first battery service-life
 Chapter 3 Primary prevention ICD recipients: the need for defibrillator back-up after an event-free first battery service-life Guido H. van Welsenes, MS, Johannes B. van Rees, MD, Joep Thijssen, MD, Serge
Chapter 3 Primary prevention ICD recipients: the need for defibrillator back-up after an event-free first battery service-life Guido H. van Welsenes, MS, Johannes B. van Rees, MD, Joep Thijssen, MD, Serge
Antiarrhythmic Drugs and Ablation in Patients with ICD and Shocks
 Antiarrhythmic Drugs and Ablation in Patients with ICD and Shocks Alireza Ghorbani Sharif, MD Interventional Electrophysiologist Tehran Arrhythmia Clinic January 2016 Recurrent ICD shocks are associated
Antiarrhythmic Drugs and Ablation in Patients with ICD and Shocks Alireza Ghorbani Sharif, MD Interventional Electrophysiologist Tehran Arrhythmia Clinic January 2016 Recurrent ICD shocks are associated
Implantable Cardioverter Defibrillator Therapy in MADIT II Patients with Signs and Symptoms of Heart Failure
 Implantable Cardioverter Defibrillator Therapy in MADIT II Patients with Signs and Symptoms of Heart Failure Wojciech Zareba Postinfarction patients with left ventricular dysfunction are at increased risk
Implantable Cardioverter Defibrillator Therapy in MADIT II Patients with Signs and Symptoms of Heart Failure Wojciech Zareba Postinfarction patients with left ventricular dysfunction are at increased risk
Secondary prevention of sudden cardiac death
 Secondary prevention of sudden cardiac death Balbir Singh, MD, DM; Lakshmi N. Kottu, MBBS, Dip Card, PGPCard Department of Cardiology, Medanta Medcity Hospital, Gurgaon, India Abstract All randomised secondary
Secondary prevention of sudden cardiac death Balbir Singh, MD, DM; Lakshmi N. Kottu, MBBS, Dip Card, PGPCard Department of Cardiology, Medanta Medcity Hospital, Gurgaon, India Abstract All randomised secondary
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT JANUARY 24, 2012
 IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201203 JANUARY 24, 2012 The IHCP to reimburse implantable cardioverter defibrillators separately from outpatient implantation Effective March 1, 2012, the
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201203 JANUARY 24, 2012 The IHCP to reimburse implantable cardioverter defibrillators separately from outpatient implantation Effective March 1, 2012, the
Tachycardia Devices Indications and Basic Trouble Shooting
 Tachycardia Devices Indications and Basic Trouble Shooting Peter A. Brady, MD., FRCP Cardiology Review Course London, March 6 th, 2014 2011 MFMER 3134946-1 Tachycardia Devices ICD Indications Primary and
Tachycardia Devices Indications and Basic Trouble Shooting Peter A. Brady, MD., FRCP Cardiology Review Course London, March 6 th, 2014 2011 MFMER 3134946-1 Tachycardia Devices ICD Indications Primary and
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm
 Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm Guy Amit, MD, MPH Soroka University Medical Center Ben-Gurion University of the Negev Beer-Sheva, Israel Disclosures Consultant:
Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm Guy Amit, MD, MPH Soroka University Medical Center Ben-Gurion University of the Negev Beer-Sheva, Israel Disclosures Consultant:
Heart Failure Treatments
 Heart Failure Treatments Past & Present www.philippelefevre.com Background Background Chronic heart failure Drugs Mechanical Electrical Background Chronic heart failure Drugs Mechanical Electrical Sudden
Heart Failure Treatments Past & Present www.philippelefevre.com Background Background Chronic heart failure Drugs Mechanical Electrical Background Chronic heart failure Drugs Mechanical Electrical Sudden
ESC Stockholm Arrhythmias & pacing
 ESC Stockholm 2010 Take Home Messages for Practitioners Arrhythmias & pacing Prof. Panos E. Vardas Professor of Cardiology Heraklion University Hospital Crete, Greece Disclosures Small teaching fees from
ESC Stockholm 2010 Take Home Messages for Practitioners Arrhythmias & pacing Prof. Panos E. Vardas Professor of Cardiology Heraklion University Hospital Crete, Greece Disclosures Small teaching fees from
PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS. HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate
 PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate Measure Title Description Measure Type Data Source Level of Analysis Numerator HRS-3:
PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate Measure Title Description Measure Type Data Source Level of Analysis Numerator HRS-3:
Comparison of clinical trials evaluating cardiac resynchronization therapy in mild to moderate heart failure
 HOT TOPIC Cardiology Journal 2010, Vol. 17, No. 6, pp. 543 548 Copyright 2010 Via Medica ISSN 1897 5593 Comparison of clinical trials evaluating cardiac resynchronization therapy in mild to moderate heart
HOT TOPIC Cardiology Journal 2010, Vol. 17, No. 6, pp. 543 548 Copyright 2010 Via Medica ISSN 1897 5593 Comparison of clinical trials evaluating cardiac resynchronization therapy in mild to moderate heart
Program Metrics. New Unique ID. Old Unique ID. Metric Set Metric Name Description. Old Metric Name
 Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
CRT-D or CRT-P: HOW TO CHOOSE THE RIGHT PATIENT?
 CRT-D or CRT-P: HOW TO CHOOSE THE RIGHT PATIENT? Alessandro Lipari, MD Chair and Department of Cardiology University of Study and Spedali Civili Brescia -Italy The birth of CRT in Europe, 20 years ago
CRT-D or CRT-P: HOW TO CHOOSE THE RIGHT PATIENT? Alessandro Lipari, MD Chair and Department of Cardiology University of Study and Spedali Civili Brescia -Italy The birth of CRT in Europe, 20 years ago
Cardiac Resynchronisation Therapy Patient Information
 Melbourne Heart Rhythm Cardiac Resynchronisation Therapy Patient Information Normal Heart Function The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two
Melbourne Heart Rhythm Cardiac Resynchronisation Therapy Patient Information Normal Heart Function The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two
that number is extremely high. It s 16 episodes, or in other words, it s 14, one-four, ICD shocks per patient per day.
 Doctor Karlsner, Doctor Schumosky, ladies and gentlemen. It s my real pleasure to participate in this session on controversial issues in the management of ventricular tachycardia and I m sure that will
Doctor Karlsner, Doctor Schumosky, ladies and gentlemen. It s my real pleasure to participate in this session on controversial issues in the management of ventricular tachycardia and I m sure that will
Prophylactic ablation
 Ventricular tachycardia in ischaemic heart disease. Update on electrical therapy 29 august 2010 Prophylactic ablation Pasquale Notarstefano Cardiovacular Department S. Donato Hospital, Arezzo (IT) Prophylactic
Ventricular tachycardia in ischaemic heart disease. Update on electrical therapy 29 august 2010 Prophylactic ablation Pasquale Notarstefano Cardiovacular Department S. Donato Hospital, Arezzo (IT) Prophylactic
Make you feel better Make you live longer
 Drugs and Devices for Women with Heart Disease Sharonne N. Hayes MD, FACC Director, Women s Heart Clinic Mayo Clinic Rochester, MN CP986192-1 CP1045209-2 Goals of Medical Treatments for Heart Disease Make
Drugs and Devices for Women with Heart Disease Sharonne N. Hayes MD, FACC Director, Women s Heart Clinic Mayo Clinic Rochester, MN CP986192-1 CP1045209-2 Goals of Medical Treatments for Heart Disease Make
Silvia G Priori MD PhD
 The approach to the cardiac arrest survivor Silvia G Priori MD PhD Molecular Cardiology, IRCCS Fondazione Salvatore Maugeri Pavia, Italy AND Leon Charney Division of Cardiology, Cardiovascular Genetics
The approach to the cardiac arrest survivor Silvia G Priori MD PhD Molecular Cardiology, IRCCS Fondazione Salvatore Maugeri Pavia, Italy AND Leon Charney Division of Cardiology, Cardiovascular Genetics
What Every Physician Should Know:
 What Every Physician Should Know: The Canadian Heart Rhythm Society estimates that, in Canada, sudden cardiac death (SCD) is responsible for about 40,000 deaths annually; more than AIDS, breast cancer
What Every Physician Should Know: The Canadian Heart Rhythm Society estimates that, in Canada, sudden cardiac death (SCD) is responsible for about 40,000 deaths annually; more than AIDS, breast cancer
The Therapeutic Role of the Implantable Cardioverter Defibrillator in Arrhythmogenic Right Ventricular Dysplasia
 The Therapeutic Role of the Implantable Cardioverter Defibrillator in Arrhythmogenic Right Ventricular Dysplasia By Sandeep Joshi, MD and Jonathan S. Steinberg, MD Arrhythmia Service, Division of Cardiology
The Therapeutic Role of the Implantable Cardioverter Defibrillator in Arrhythmogenic Right Ventricular Dysplasia By Sandeep Joshi, MD and Jonathan S. Steinberg, MD Arrhythmia Service, Division of Cardiology
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh
 Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
Do All Patients With An ICD Indication Need A BiV Pacing Device?
 Do All Patients With An ICD Indication Need A BiV Pacing Device? Muhammad A. Hammouda, MD Electrophysiology Laboratory Department of Critical Care Medicine Cairo University Etiology and Pathophysiology
Do All Patients With An ICD Indication Need A BiV Pacing Device? Muhammad A. Hammouda, MD Electrophysiology Laboratory Department of Critical Care Medicine Cairo University Etiology and Pathophysiology
Implantation-Related Complications of Implantable Cardioverter-Defibrillators and Cardiac Resynchronization Therapy Devices
 Journal of the American College of Cardiology Vol. 58, No. 10, 2011 2011 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2011.06.007
Journal of the American College of Cardiology Vol. 58, No. 10, 2011 2011 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2011.06.007
MEDICAL POLICY Cardioverter Defibrillators
 POLICY........ PG-0224 EFFECTIVE......06/01/09 LAST REVIEW... 01/27/17 MEDICAL POLICY Cardioverter Defibrillators GUIDELINES This policy does not certify benefits or authorization of benefits, which is
POLICY........ PG-0224 EFFECTIVE......06/01/09 LAST REVIEW... 01/27/17 MEDICAL POLICY Cardioverter Defibrillators GUIDELINES This policy does not certify benefits or authorization of benefits, which is
Ventricular tachycardia Ventricular fibrillation and ICD
 EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
Quality Measures MIPS CV Specific
 Quality Measures MIPS CV Specific MEASURE NAME Atrial Fibrillation and Atrial Flutter: Chronic Anticoagulation Therapy CAHPS for MIPS Clinician/Group Survey Cardiac Rehabilitation Patient Referral from
Quality Measures MIPS CV Specific MEASURE NAME Atrial Fibrillation and Atrial Flutter: Chronic Anticoagulation Therapy CAHPS for MIPS Clinician/Group Survey Cardiac Rehabilitation Patient Referral from
Synopsis of Management on Ventricular arrhythmias. M. Soni MD Interventional Cardiologist
 Synopsis of Management on Ventricular arrhythmias M. Soni MD Interventional Cardiologist No financial disclosure Premature Ventricular Contraction (PVC) Ventricular Bigeminy Ventricular Trigeminy Multifocal
Synopsis of Management on Ventricular arrhythmias M. Soni MD Interventional Cardiologist No financial disclosure Premature Ventricular Contraction (PVC) Ventricular Bigeminy Ventricular Trigeminy Multifocal
Chapter 3. Eur Heart J 2009; 30:
 Recurrence of Ventricular Arrhythmias in Ischemic Secondary Prevention ICD Recipients: Long-term Followup of the Leiden Out-of- Hospital Cardiac Arrest Study (LOHCAT) C. Jan Willem Borleffs, MD 1, Lieselot
Recurrence of Ventricular Arrhythmias in Ischemic Secondary Prevention ICD Recipients: Long-term Followup of the Leiden Out-of- Hospital Cardiac Arrest Study (LOHCAT) C. Jan Willem Borleffs, MD 1, Lieselot
Atrial fibrillation (AF) is a disorder seen
 This Just In... An Update on Arrhythmia What do recent studies reveal about arrhythmia? In this article, the authors provide an update on atrial fibrillation and ventricular arrhythmia. Beth L. Abramson,
This Just In... An Update on Arrhythmia What do recent studies reveal about arrhythmia? In this article, the authors provide an update on atrial fibrillation and ventricular arrhythmia. Beth L. Abramson,
ICD Therapy. Disclaimers
 ICD Therapy Rodney Horton, MD Texas Cardiac Arrhythmia Institute Texas Cardiovascular, PA Austin, TX Speaker s Bureau St. Jude Medical Medtronic Boston Scientific Disclaimers Clinical Advisory Panel St.
ICD Therapy Rodney Horton, MD Texas Cardiac Arrhythmia Institute Texas Cardiovascular, PA Austin, TX Speaker s Bureau St. Jude Medical Medtronic Boston Scientific Disclaimers Clinical Advisory Panel St.
Clinical Policy: Holter Monitors Reference Number: CP.MP.113
 Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Ventricular Tachycardia in Structurally Normal Hearts (Idiopathic VT) Patient Information
 Melbourne Heart Rhythm Ventricular Tachycardia in Structurally Normal Hearts (Idiopathic VT) Patient Information What is Ventricular Tachycardia? Ventricular tachycardia (VT) is an abnormal rapid heart
Melbourne Heart Rhythm Ventricular Tachycardia in Structurally Normal Hearts (Idiopathic VT) Patient Information What is Ventricular Tachycardia? Ventricular tachycardia (VT) is an abnormal rapid heart
Supplemental Material
 Supplemental Material 1 Table S1. Codes for Patient Selection Cohort Codes Primary PM CPT: 33206 or 33207 or 33208 (without 33225) ICD-9 proc: 37.81, 37.82, 37.83 Primary ICD Replacement PM Replacement
Supplemental Material 1 Table S1. Codes for Patient Selection Cohort Codes Primary PM CPT: 33206 or 33207 or 33208 (without 33225) ICD-9 proc: 37.81, 37.82, 37.83 Primary ICD Replacement PM Replacement
Meta-analysis of the implantable cardioverter defibrillator secondary prevention trials
 European Heart Journal (2000) 21, 2071 2078 doi.10.1053/euhj.2000.2476, available online at http://www.idealibrary.com on Meta-analysis of the implantable cardioverter defibrillator secondary prevention
European Heart Journal (2000) 21, 2071 2078 doi.10.1053/euhj.2000.2476, available online at http://www.idealibrary.com on Meta-analysis of the implantable cardioverter defibrillator secondary prevention
Device Update Implantable Cardioverter Defibrillator (ICD) 박상원
 2012 년춘계학술대회 Device Update Implantable Cardioverter Defibrillator (ICD) 박상원 Arrhythmia Center, KUMC www.korea-heartrhythm.com Korea University Medical Center Seoul, Korea The Development of ICD by a team
2012 년춘계학술대회 Device Update Implantable Cardioverter Defibrillator (ICD) 박상원 Arrhythmia Center, KUMC www.korea-heartrhythm.com Korea University Medical Center Seoul, Korea The Development of ICD by a team
Different indications for pacemaker implantation are the following:
 Patient Resources: ICD/Pacemaker Overview ICD/Pacemaker Overview What is a pacemaker? A pacemaker is a device that uses low energy electrical pulses to prompt the heart to beat whenever a pause in the
Patient Resources: ICD/Pacemaker Overview ICD/Pacemaker Overview What is a pacemaker? A pacemaker is a device that uses low energy electrical pulses to prompt the heart to beat whenever a pause in the
G Lin, R F Rea, S C Hammill, D L Hayes, P A Brady
 Division of Cardiovascular Diseases, Mayo Clinic, Rochester, MN, USA Correspondence to: Dr Peter A Brady, MD, FRCP, Mayo Clinic, 200 First Street SW, Rochester, MN, 55905, USA; brady.peter@mayo.edu Accepted
Division of Cardiovascular Diseases, Mayo Clinic, Rochester, MN, USA Correspondence to: Dr Peter A Brady, MD, FRCP, Mayo Clinic, 200 First Street SW, Rochester, MN, 55905, USA; brady.peter@mayo.edu Accepted
Mission Statement for our Arrhythmia Care
 Mission Statement for our Arrhythmia Care We are dedicated to provide a compassionate and an outstanding care for patients with cardiac arrhythmias. We will be utilizing the cutting edge and the most advanced
Mission Statement for our Arrhythmia Care We are dedicated to provide a compassionate and an outstanding care for patients with cardiac arrhythmias. We will be utilizing the cutting edge and the most advanced
Risk Stratification and Benefit of ICD-Therapy in Congestive Heart Failure Patients
 120 April 2001 Risk Stratification and Benefit of ICD-Therapy in Congestive Heart Failure Patients P. SCHIRDEWAHN, G. HINDRICKS, H. KOTTKAMP Department of Cardiology, University of Leipzig Heart Center,
120 April 2001 Risk Stratification and Benefit of ICD-Therapy in Congestive Heart Failure Patients P. SCHIRDEWAHN, G. HINDRICKS, H. KOTTKAMP Department of Cardiology, University of Leipzig Heart Center,
Where Does the Wearable Cardioverter Defibrillator (WCD) Fit In?
 Where Does the Wearable Cardioverter Defibrillator (WCD) Fit In? 24 th Annual San Diego Heart Failure Symposium June 1-2, 2018 La Jolla, CA Barry Greenberg, MD Distinguished Professor of Medicine Director,
Where Does the Wearable Cardioverter Defibrillator (WCD) Fit In? 24 th Annual San Diego Heart Failure Symposium June 1-2, 2018 La Jolla, CA Barry Greenberg, MD Distinguished Professor of Medicine Director,
Dos and Don t in Cardiac Arrhythmia. Case 1 -ECG. Case 1. Management. Emergency Admissions. Reduction of TE risk -CHADS 2 score. Hospital Admissions
 Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
Re: National Coverage Analysis (NCA) for Implantable Cardioverter Defibrillators (CAG R4)
 December 20, 2017 Ms. Tamara Syrek-Jensen Director, Coverage & Analysis Group Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, MD 21244 Re: National Coverage Analysis (NCA) for
December 20, 2017 Ms. Tamara Syrek-Jensen Director, Coverage & Analysis Group Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, MD 21244 Re: National Coverage Analysis (NCA) for
PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART II
 1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART II 2012 Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 ADDITIVES IN DEVICE THERAPY Key Choice / CNEA 1 Adaptive Rate
1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART II 2012 Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 ADDITIVES IN DEVICE THERAPY Key Choice / CNEA 1 Adaptive Rate
Ventricular tachycardia and ischemia. Martin Jan Schalij Department of Cardiology Leiden University Medical Center
 Ventricular tachycardia and ischemia Martin Jan Schalij Department of Cardiology Leiden University Medical Center Disclosure: Research grants from: Boston Scientific Medtronic Biotronik Sudden Cardiac
Ventricular tachycardia and ischemia Martin Jan Schalij Department of Cardiology Leiden University Medical Center Disclosure: Research grants from: Boston Scientific Medtronic Biotronik Sudden Cardiac
THE ROLE OF ICD THERAPY FOR PRIMARY PREVENTION Leonard Ganz, M.D. Pittsburgh, PA
 THE ROLE OF ICD THERAPY FOR PRIMARY PREVENTION Leonard Ganz, M.D. Pittsburgh, PA Speakers Bureau: Zoll / Lifecore, Sanofi Aventis, Cardionet Consultant: Boston Scientific, St. Jude Medical, Biotronik,
THE ROLE OF ICD THERAPY FOR PRIMARY PREVENTION Leonard Ganz, M.D. Pittsburgh, PA Speakers Bureau: Zoll / Lifecore, Sanofi Aventis, Cardionet Consultant: Boston Scientific, St. Jude Medical, Biotronik,
NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS
 NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS OBJECTIVES Discuss history of ICDs Review the indications for ICD and CRT therapy Describe basic lead and device technology Discuss different therapies
NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS OBJECTIVES Discuss history of ICDs Review the indications for ICD and CRT therapy Describe basic lead and device technology Discuss different therapies
3/17/2014. NCDR-14 ICD Registry WS # 24 Case Scenarios Including Syndromes w/ Risk of Sudden Death. Objectives
 NCDR-14 ICD Registry WS # 24 Case Scenarios Including Syndromes w/ Risk of Sudden Death Denise Pond BSN, RN The following relationships exist related to this presentation: No Disclosures Objectives Discuss
NCDR-14 ICD Registry WS # 24 Case Scenarios Including Syndromes w/ Risk of Sudden Death Denise Pond BSN, RN The following relationships exist related to this presentation: No Disclosures Objectives Discuss
Effectiveness of Implantable Cardioverter-Defibrillator Therapy for Heart Failure Patients according to Ischemic or Non-Ischemic Etiology in Korea
 Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Effectiveness of Implantable Cardioverter-Defibrillator Therapy for Heart Failure Patients according to Ischemic
Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Effectiveness of Implantable Cardioverter-Defibrillator Therapy for Heart Failure Patients according to Ischemic
Implantable cardioverter defibrillator, Inappropriate shock, Lead failure
 Inappropriate Discharges of Intravenous Implantable Cardioverter Defibrillators Owing to Lead Failure Takashi WASHIZUKA, 1 MD, Masaomi CHINUSHI, 1 MD, Ryu KAZAMA, 1 MD, Takashi HIRONO, 1 MD, Hiroshi WATANABE,
Inappropriate Discharges of Intravenous Implantable Cardioverter Defibrillators Owing to Lead Failure Takashi WASHIZUKA, 1 MD, Masaomi CHINUSHI, 1 MD, Ryu KAZAMA, 1 MD, Takashi HIRONO, 1 MD, Hiroshi WATANABE,
8:30-10:30 WS #4: Cardiology :00-13:00 WS #11: Cardiology 101 (Repeated)
 Professor Ralph Stewart Cardiologist Auckland City Hospital Green Lane Cardiovascular Research Unit Auckland Heart Group Fiona Stewart Cardiologist Green Lane Hospital National Women's Hospital Professor
Professor Ralph Stewart Cardiologist Auckland City Hospital Green Lane Cardiovascular Research Unit Auckland Heart Group Fiona Stewart Cardiologist Green Lane Hospital National Women's Hospital Professor
SPORTS AND EXERCISE ADVICE IN PATIENTS WITH ICD AND PPM
 SPORTS AND EXERCISE ADVICE IN PATIENTS WITH ICD AND PPM Rio De Janeiro 2016 Sport and Exercise Cardiology Symposium SBC/SOCERJ ACC Sharlene M. Day, MD Associate Professor, Cardiovascular Medicine Director,
SPORTS AND EXERCISE ADVICE IN PATIENTS WITH ICD AND PPM Rio De Janeiro 2016 Sport and Exercise Cardiology Symposium SBC/SOCERJ ACC Sharlene M. Day, MD Associate Professor, Cardiovascular Medicine Director,
VT Ablation in Structural Heart Disease Patient Information
 Melbourne Heart Rhythm VT Ablation in Structural Heart Disease Patient Information Ventricular Tachycardia in Structural Heart Disease (VT-SHD) Ventricular tachycardia (VT) is an abnormal rapid heart rhythm
Melbourne Heart Rhythm VT Ablation in Structural Heart Disease Patient Information Ventricular Tachycardia in Structural Heart Disease (VT-SHD) Ventricular tachycardia (VT) is an abnormal rapid heart rhythm
UnitedHealthcare Medicare Advantage Cardiology Prior Authorization Program
 Electrophysiology Implant Classification Table The table below contains the codes that apply to our UnitedHealthcare Medicare Advantage cardiology prior Description Includes Generator Placement Includes
Electrophysiology Implant Classification Table The table below contains the codes that apply to our UnitedHealthcare Medicare Advantage cardiology prior Description Includes Generator Placement Includes
Need to Know: Implantable Devices. Carolyn Brown RN, MN, CCRN Education Coordinator Emory Healthcare Atlanta, Georgia
 Need to Know: Implantable Devices Carolyn Brown RN, MN, CCRN Education Coordinator Emory Healthcare Atlanta, Georgia Disclosure Statement I have no relationships to disclose. Objectives Discuss the most
Need to Know: Implantable Devices Carolyn Brown RN, MN, CCRN Education Coordinator Emory Healthcare Atlanta, Georgia Disclosure Statement I have no relationships to disclose. Objectives Discuss the most
Title: Automatic External Defibrillators Division: Medical Management Department: Utilization Management
 Retired Date: Page 1 of 7 1. POLICY DESCRIPTION: Automatic External Defibrillators 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management, Pharmacy,
Retired Date: Page 1 of 7 1. POLICY DESCRIPTION: Automatic External Defibrillators 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management, Pharmacy,
Automatic External Defibrillators
 Last Review Date: April 21, 2017 Number: MG.MM.DM.10dC3v4 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: April 21, 2017 Number: MG.MM.DM.10dC3v4 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Cardiac resynchronisation therapy (biventricular pacing) for the treatment of heart failure
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal for the treatment of heart failure Final scope Appraisal objective To appraise the clinical and cost effectiveness of cardiac
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal for the treatment of heart failure Final scope Appraisal objective To appraise the clinical and cost effectiveness of cardiac
Revisions to the BC Guide for Physicians in Determining Fitness to Drive a Motor Vehicle
 Revisions to the BC Guide for Physicians in Determining Fitness to Drive a Motor Vehicle Thank you for taking the time to review the draft Cardiovascular Diseases and Disorders chapter. Please provide
Revisions to the BC Guide for Physicians in Determining Fitness to Drive a Motor Vehicle Thank you for taking the time to review the draft Cardiovascular Diseases and Disorders chapter. Please provide
InterQual Care Planning SIM plus Criteria 2014 Clinical Revisions
 InterQual Care Planning SIM plus Criteria 2014 Clinical Revisions The Clinical Revisions provide details of changes to InterQual Clinical Criteria. They do not provide information on changes made to CareEnhance
InterQual Care Planning SIM plus Criteria 2014 Clinical Revisions The Clinical Revisions provide details of changes to InterQual Clinical Criteria. They do not provide information on changes made to CareEnhance
Congestive Heart Failure or Heart Failure
 Congestive Heart Failure or Heart Failure Dr Hitesh Patel Ascot Cardiology Group Heart Failure Workshop April, 2014 Question One What is the difference between congestive heart failure and heart failure?
Congestive Heart Failure or Heart Failure Dr Hitesh Patel Ascot Cardiology Group Heart Failure Workshop April, 2014 Question One What is the difference between congestive heart failure and heart failure?
Experience with pectoral versus abdominal implantation of a small defibrillator
 European Heart Journal (1998) 19, 185 198 Article No. hj9816 Experience with pectoral versus abdominal implantation of a small defibrillator A multicenter comparison in 778 patients E. Hoffmann, G. Steinbeck,
European Heart Journal (1998) 19, 185 198 Article No. hj9816 Experience with pectoral versus abdominal implantation of a small defibrillator A multicenter comparison in 778 patients E. Hoffmann, G. Steinbeck,
Cardiac implantable electronic devices (CIEDs) in children include pacemakers and implantable cardioverter defibrillators (ICDs).
 Management of Children with Cardiac Devices Guideline originally developed by Leann Miles, APRN; Lindsey Pumphrey, RN; Srikant Das, MD, and the ANGELS Team. Last reviewed by Lindsey Pumphrey, RN, Srikant
Management of Children with Cardiac Devices Guideline originally developed by Leann Miles, APRN; Lindsey Pumphrey, RN; Srikant Das, MD, and the ANGELS Team. Last reviewed by Lindsey Pumphrey, RN, Srikant
A Square Peg in a Round Hole: CRT IN PAEDIATRICS AND CONGENITAL HEART DISEASE
 A Square Peg in a Round Hole: CRT IN PAEDIATRICS AND CONGENITAL HEART DISEASE Adele Greyling Dora Nginza Hospital, Port Elizabeth SA Heart November 2017 What are the guidelines based on? MADIT-II Size:
A Square Peg in a Round Hole: CRT IN PAEDIATRICS AND CONGENITAL HEART DISEASE Adele Greyling Dora Nginza Hospital, Port Elizabeth SA Heart November 2017 What are the guidelines based on? MADIT-II Size:
Chapter 2. Long-term follow-up of primary and secondary prevention implantable cardioverter defibrillator patients
 Chapter 2 Long-term follow-up of primary and secondary prevention implantable cardioverter defibrillator patients Guido H. van Welsenes, MS, Johannes B. van Rees, MD, C. Jan Willem Borleffs, MD, PhD, Suzanne
Chapter 2 Long-term follow-up of primary and secondary prevention implantable cardioverter defibrillator patients Guido H. van Welsenes, MS, Johannes B. van Rees, MD, C. Jan Willem Borleffs, MD, PhD, Suzanne
Dialysis-Dependent Cardiomyopathy Patients Demonstrate Poor Survival Despite Reverse Remodeling With Cardiac Resynchronization Therapy
 Dialysis-Dependent Cardiomyopathy Patients Demonstrate Poor Survival Despite Reverse Remodeling With Cardiac Resynchronization Therapy Evan Adelstein, MD, FHRS John Gorcsan III, MD Samir Saba, MD, FHRS
Dialysis-Dependent Cardiomyopathy Patients Demonstrate Poor Survival Despite Reverse Remodeling With Cardiac Resynchronization Therapy Evan Adelstein, MD, FHRS John Gorcsan III, MD Samir Saba, MD, FHRS
NHS. Implantable cardioverter defibrillators (ICDs) for arrhythmias. National Institute for Health and Clinical Excellence. Issue date: January 2006
 NHS National Institute for Health and Clinical Excellence Issue date: January 2006 Implantable cardioverter defibrillators (ICDs) for arrhythmias Understanding NICE guidance information for people with
NHS National Institute for Health and Clinical Excellence Issue date: January 2006 Implantable cardioverter defibrillators (ICDs) for arrhythmias Understanding NICE guidance information for people with
Cardiovascular Disease
 Cardiovascular Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars on the 3 rd Wednesday of each month to address topics related to risk adjustment
Cardiovascular Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars on the 3 rd Wednesday of each month to address topics related to risk adjustment
Pediatric pacemakers & ICDs:
 Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
National Imaging Associates, Inc. Clinical guidelines CARDIAC CATHETERIZATION -LEFT HEART CATHETERIZATION. Original Date: October 2015 Page 1 of 5
 National Imaging Associates, Inc. Clinical guidelines CARDIAC CATHETERIZATION -LEFT HEART CATHETERIZATION CPT Codes: 93451, 93452, 93453, 93454, 93455, 93456, 93457, 93458, 93459, 93460, 93461 LCD ID Number:
National Imaging Associates, Inc. Clinical guidelines CARDIAC CATHETERIZATION -LEFT HEART CATHETERIZATION CPT Codes: 93451, 93452, 93453, 93454, 93455, 93456, 93457, 93458, 93459, 93460, 93461 LCD ID Number:
ESSA HEART AND VASCULAR INSTITUTE APR/MAY/JUNE 2009 CLINICAL LETTER
 CLINICAL LETTER Exciting things are happening at the ESSA Heart and Vascular Institute and the Pocono Medical Center! We are all proud of the stellar team of professionals who are working very hard to
CLINICAL LETTER Exciting things are happening at the ESSA Heart and Vascular Institute and the Pocono Medical Center! We are all proud of the stellar team of professionals who are working very hard to
Cardiac Resynchronization Therapy. Michelle Khoo, MD
 Cardiac Resynchronization Therapy Michelle Khoo, MD 10.7.08 HuiKuri HV NEJM 2001 Sudden Death (SD) in Subset Populations HuiKuri HV NEJM 2001 Sudden Death (SD) in Subset Populations SD in Competitive Athletes
Cardiac Resynchronization Therapy Michelle Khoo, MD 10.7.08 HuiKuri HV NEJM 2001 Sudden Death (SD) in Subset Populations HuiKuri HV NEJM 2001 Sudden Death (SD) in Subset Populations SD in Competitive Athletes
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Implantable Cardioverter Defibrillators Page 1 of 44 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See also: Implantable Cardioverter Defibrillators Wearable Cardioverter
Implantable Cardioverter Defibrillators Page 1 of 44 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See also: Implantable Cardioverter Defibrillators Wearable Cardioverter
The patient with (without) an ICD and heart failure: Management of electrical storm
 ISHNE Heart Failure Virtual Symposium April 2008 The patient with (without) an ICD and heart failure: Management of electrical storm Westfälische Wilhelms-Universität Münster Günter Breithardt, MD, FESC,
ISHNE Heart Failure Virtual Symposium April 2008 The patient with (without) an ICD and heart failure: Management of electrical storm Westfälische Wilhelms-Universität Münster Günter Breithardt, MD, FESC,
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
ICD Guidelines: who benefits from an ICD?
 ICD Guidelines: who benefits from an ICD? Matthew Bennett Cardiac Electrophysiologist Vancouver Coastal Health, Device Lead Associate Professor, UBC Matthew.bennett@vch.ca Disclosures I have research collaborations
ICD Guidelines: who benefits from an ICD? Matthew Bennett Cardiac Electrophysiologist Vancouver Coastal Health, Device Lead Associate Professor, UBC Matthew.bennett@vch.ca Disclosures I have research collaborations
Quality Payment Program: Cardiology Specialty Measure Set
 Quality Payment Program: Cardiology Specialty Set Title Number CMS Reporting Method(s) Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor or Angiotensin Receptor Blocker (ARB) Therapy for
Quality Payment Program: Cardiology Specialty Set Title Number CMS Reporting Method(s) Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor or Angiotensin Receptor Blocker (ARB) Therapy for
Resynchronization/Defibrillation
 Resynchronization/Defibrillation for Ambulatory Heart Failure Trial Cardiac Resynchronization Therapy for Mild to Moderate Heart Failure George Wells University of Ottawa Heart Institute Department of
Resynchronization/Defibrillation for Ambulatory Heart Failure Trial Cardiac Resynchronization Therapy for Mild to Moderate Heart Failure George Wells University of Ottawa Heart Institute Department of
(For items 1-12, each question specifies mark one or mark all that apply.)
 Form 121 - Report of Cardiovascular Outcome Ver. 9.2 COMMENTS -Affix label here- Member ID: - - To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: - Central Case No.:
Form 121 - Report of Cardiovascular Outcome Ver. 9.2 COMMENTS -Affix label here- Member ID: - - To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: - Central Case No.:
Supplementary Online Content
 Supplementary Online Content Inohara T, Manandhar P, Kosinski A, et al. Association of renin-angiotensin inhibitor treatment with mortality and heart failure readmission in patients with transcatheter
Supplementary Online Content Inohara T, Manandhar P, Kosinski A, et al. Association of renin-angiotensin inhibitor treatment with mortality and heart failure readmission in patients with transcatheter
Sudden cardiac death: Primary and secondary prevention
 Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Performance and Quality Measures 1. NQF Measure Number. Coronary Artery Disease Measure Set
 Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
2
 1 2 Although the term "cardiomyopathy" could theoretically apply to almost any disease affecting the heart, it is usually reserved for "severe myocardial disease leading to heart failure".cardiomyopathy
1 2 Although the term "cardiomyopathy" could theoretically apply to almost any disease affecting the heart, it is usually reserved for "severe myocardial disease leading to heart failure".cardiomyopathy
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
Implantable Cardioverter Defibrillator (ICD)
 Medical Coverage Policy Effective Date... 3/15/2018 Next Review Date... 3/15/2019 Coverage Policy Number... 0181 Implantable Cardioverter Defibrillator (ICD) Table of Contents Related Coverage Resources
Medical Coverage Policy Effective Date... 3/15/2018 Next Review Date... 3/15/2019 Coverage Policy Number... 0181 Implantable Cardioverter Defibrillator (ICD) Table of Contents Related Coverage Resources
Tachycardias II. Štěpán Havránek
 Tachycardias II Štěpán Havránek Summary 1) Supraventricular (supraventricular rhythms) Atrial fibrillation and flutter Atrial ectopic tachycardia / extrabeats AV nodal reentrant a AV reentrant tachycardia
Tachycardias II Štěpán Havránek Summary 1) Supraventricular (supraventricular rhythms) Atrial fibrillation and flutter Atrial ectopic tachycardia / extrabeats AV nodal reentrant a AV reentrant tachycardia
Michel Mirowski and colleagues ABSTRACT CARDIOLOGY. ICD Update: New Evidence and Emerging Clinical Roles in Primary Prevention of Sudden Cardiac Death
 ICD Update: New Evidence and Emerging Clinical Roles in Primary Prevention of Sudden Cardiac Death Ronald D. Berger, MD, PhD, FACC ABSTRACT PURPOSE: To review recent major randomized trials of implantable
ICD Update: New Evidence and Emerging Clinical Roles in Primary Prevention of Sudden Cardiac Death Ronald D. Berger, MD, PhD, FACC ABSTRACT PURPOSE: To review recent major randomized trials of implantable
Heart failure hospitalizations with preserved or reduced ejection fraction
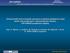 Clinical profile and in-hospital outcomes in patients admitted for heart failure with preserved or reduced ejection fraction. EPI-CARDIO prospective registry Tajer, C; Mariani, J; de Abreu, M; Charask,
Clinical profile and in-hospital outcomes in patients admitted for heart failure with preserved or reduced ejection fraction. EPI-CARDIO prospective registry Tajer, C; Mariani, J; de Abreu, M; Charask,
Cardiac Devices CRT,ICD: Who is and is not a Candidate? Who Decides
 Cardiac Devices CRT,ICD: Who is and is not a Candidate? Who Decides Colette Seifer MB(Hons) FRCP(UK) Associate Professor, University of Manitoba, Cardiologist, Cardiac Sciences Program, St Boniface Hospital
Cardiac Devices CRT,ICD: Who is and is not a Candidate? Who Decides Colette Seifer MB(Hons) FRCP(UK) Associate Professor, University of Manitoba, Cardiologist, Cardiac Sciences Program, St Boniface Hospital
Chapter 8: Cardiovascular Disease in Patients with ESRD
 Chapter 8: Cardiovascular Disease in Patients with ESRD Cardiovascular disease (CVD) is common in adult end-stage renal disease (ESRD) patients, with coronary artery disease (CAD) and heart failure (HF)
Chapter 8: Cardiovascular Disease in Patients with ESRD Cardiovascular disease (CVD) is common in adult end-stage renal disease (ESRD) patients, with coronary artery disease (CAD) and heart failure (HF)
UnitedHealthcare, UnitedHealthcare of the River Valley and Neighborhood Health Partnership Cardiology Notification and Prior Authorization Program:
 Notification and Prior Authorization Program: Electrophysiology Implant Classification Table The following chart contains the codes that require notification or prior authorization as part of UnitedHealthcare
Notification and Prior Authorization Program: Electrophysiology Implant Classification Table The following chart contains the codes that require notification or prior authorization as part of UnitedHealthcare
Implantable cardioverter-defibrillators (ICD) terminate
 Primary Prevention of Sudden Cardiac Death in Idiopathic Dilated Cardiomyopathy The Cardiomyopathy Trial (CAT) Dietmar Bänsch, MD; Matthias Antz, MD; Sigrid Boczor; Marius Volkmer, MD; Jürgen Tebbenjohanns,
Primary Prevention of Sudden Cardiac Death in Idiopathic Dilated Cardiomyopathy The Cardiomyopathy Trial (CAT) Dietmar Bänsch, MD; Matthias Antz, MD; Sigrid Boczor; Marius Volkmer, MD; Jürgen Tebbenjohanns,
State-of-the-Art Management of Chronic Systolic Heart Failure
 State-of-the-Art Management of Chronic Systolic Heart Failure Michael McCulloch, MD 17 th Annual Cardiovascular Update Intermountain Medical Center December 16, 2017 Disclosures: I have no financial disclosures
State-of-the-Art Management of Chronic Systolic Heart Failure Michael McCulloch, MD 17 th Annual Cardiovascular Update Intermountain Medical Center December 16, 2017 Disclosures: I have no financial disclosures
QRS Duration Does Not Predict Occurrence of Ventricular Tachyarrhythmias in Patients With Implanted Cardioverter-Defibrillators
 Journal of the American College of Cardiology Vol. 46, No. 2, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.03.060
Journal of the American College of Cardiology Vol. 46, No. 2, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.03.060
Subcutaneous Implantable Cardioverter Defibrillator (ICD) System
 Subcutaneous Implantable Cardioverter Defibrillator (ICD) System Policy Number: Original Effective Date: MM.06.025 07/01/2015 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 3/24/201701/01/2019
Subcutaneous Implantable Cardioverter Defibrillator (ICD) System Policy Number: Original Effective Date: MM.06.025 07/01/2015 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 3/24/201701/01/2019
Abbreviation List: 2017 by the American Heart Association, Inc. and the American College of Cardiology Foundation. 1
 2017 AHA/ACC/HRS Systematic Review for the Guideline for Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death Data Supplement Table of Contents Part 1. For Asymptomatic
2017 AHA/ACC/HRS Systematic Review for the Guideline for Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death Data Supplement Table of Contents Part 1. For Asymptomatic
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Table S1. Patient Selection Codes, CIED Generator Procedures Code Type Code Description ICD9 Proc 00.51 Implantation of cardiac resynchronization defibrillator, total system [CRT-D]
SUPPLEMENTAL MATERIAL Table S1. Patient Selection Codes, CIED Generator Procedures Code Type Code Description ICD9 Proc 00.51 Implantation of cardiac resynchronization defibrillator, total system [CRT-D]
Dual-Chamber Implantable Cardioverter-Defibrillator
 February 1998 9 Dual-Chamber Implantable Cardioverter-Defibrillator A.SH. REVISHVILI A.N. Bakoulev Research Center for Cardiovascular Surgery, Russian Academy of Medical Sciences, Moscow, Russia Summary
February 1998 9 Dual-Chamber Implantable Cardioverter-Defibrillator A.SH. REVISHVILI A.N. Bakoulev Research Center for Cardiovascular Surgery, Russian Academy of Medical Sciences, Moscow, Russia Summary
