Comparison of Prognosis in Unrecognized Versus Recognized Myocardial Infarction in Men Versus Women >55 Years of Age (from the Rotterdam Study)
|
|
|
- Anissa Gordon
- 5 years ago
- Views:
Transcription
1 Comparison of Prognosis in Unrecognized Versus Recognized Myocardial Infarction in Men Versus Women >55 Years of Age (from the Rotterdam Study) Abbas Dehghan, MD, PhD a, *, Maarten J.G. Leening, MD, MSc a,b, Abbas M. Solouki, MD, MSc a, Eric Boersma, PhD b, Jaap W. Deckers, MD, PhD b, Gerard van Herpen, MD, PhD c, Jan Heeringa, MD, PhD a, Albert Hofman, MD, PhD a, Jan A. Kors, PhD c, Oscar H. Franco, MD, PhD a, M. Arfan Ikram, MD, PhD a,d,e, and Jacqueline C.M. Witteman, PhD a Unrecognized myocardial infarction (MI) is frequent in the general population. Its prognosis is reported to be at least as unpropitious as that of recognized MI, particularly in men. However, contemporary data with long follow-up are lacking. The aims of this study were to investigate the long-term prognosis of unrecognized MI with respect to all-cause and causespecific mortality and to investigate possible differences in prognosis by gender. In the population-based Rotterdam Study (2,672 men and 3,862 women), the presence of unrecognized MI and recognized MI was determined at baseline (1990 to 1993). The cohort was followed for nearly 2 decades for all-cause and cause-specific mortality. During 82,268 patient-years of follow-up (median 15.6 years) 3,412 patients died (1,300 from cardiovascular causes). Men and women with recognized and unrecognized MIs had increased total mortality rates compared with those without MIs. Hazard ratios (HRs) for men and women were 1.57 (95% confidence interval [CI] 1.36 to 1.81) and 1.89 (95% CI 1.56 to 2.30) for recognized MI and 1.72 (95% CI 1.43 to 2.07) and 1.36 (95% CI 1.14 to 1.61) for unrecognized MI. Unrecognized MI was associated with increased risks for cardiovascular mortality (men: HR 2.19, 95% CI 1.66 to 2.91; women: HR 1.36, 95% CI 1.03 to 1.81) and noncardiovascular mortality (men: HR 1.47, 95% CI 1.14 to 1.89; women: HR 1.39, 95% CI 1.10 to 1.75). In conclusion, the long-term prognosis of patients with unrecognized MIs is worse compared with those without MIs and applies not only to cardiovascular mortality but also to noncardiovascular mortality. In men, the prognosis is as unfavorable as that of patients with recognized MIs. Ó 2014 Elsevier Inc. All rights reserved. (Am J Cardiol 2014;113:1e6) According to several reports, 20% to 70% of all myocardial infarctions (MIs) in the general elderly population are asymptomatic or remain clinically unrecognized. 1e8 Because of the absence of typical symptoms, affected subjects may never seek and receive medical care. Consequently, the diagnosis of MI in these subjects is likely to be delayed or never made. This explains why up to 6% of the general elderly population may have had unrecognized Departments of a Epidemiology, b Cardiology, c Medical Informatics, d Radiology, and e Neurology, Erasmus Medical Center, University Medical Center Rotterdam, Rotterdam, The Netherlands. Manuscript received January 21, 2013; revised manuscript received and accepted September 3, The Rotterdam Study is funded by the Erasmus Medical Center and Erasmus University Rotterdam; the Netherlands Organization for the Health Research and Development; the Netherlands Organization for Scientific Research (NWO); the Research Institute for Diseases in the Elderly; the Ministry of Education, Culture and Science; the Ministry for Health, Welfare and Sports; the European Commission (DG XII); and the Municipality of Rotterdam. Dr. Dehghan is supported by Grant VENI from the NWO and an Erasmus University Rotterdam fellowship. Dr. Leening is supported by Grant from the Netherlands Organization for Health Research and Development. Dr. Witteman is supported by Grant VICI from the NWO. See page 5 for disclosure information. *Corresponding author: Tel: þ ; fax: þ address: a.dehghan@erasmusmc.nl (A. Dehghan). MIs. 9,10 Several studies have shown that the prognosis of subjects with unrecognized MIs with respect to future cardiovascular events, such as recurrent MI, is worse than that of healthy individuals. 3e5,7 Similar results have been reported with respect to the risk for death. 5,7 A number of studies have shown that the prognosis of subjects with unrecognized MIs is at least as unfavorable as that of patients with recognized MIs. 4,5,7,8,11 However, advances in primary prevention have been made over the past years, and recent data on the prognosis of unrecognized MI are lacking. In this study, we report results from the Rotterdam Study, a population-based cohort study in subjects aged 55 years ongoing since Our aim was to determine the longterm prognosis of subjects with unrecognized MI with respect to all-cause mortality and cause-specific mortality. We also sought to answer the question of whether the prognosis is different between men and women. Methods The Rotterdam Study is a prospective, population-based cohort study in subjects aged 55 years. A more detailed description of the Rotterdam Study and its data collection has been given elsewhere. 12,13 From 1990 to 1993, all inhabitants of Ommoord, a suburb of the city of Rotterdam, were invited to take part in the study. A total of 7, /13/$ - see front matter Ó 2014 Elsevier Inc. All rights reserved.
2 2 The American Journal of Cardiology ( Table 1 Baseline characteristics of the study population Variable Men Women No MI (n ¼ 2,200) Unrecognized MI (n ¼ 165) Recognized MI (n ¼ 307) No MI (n ¼ 3,527) Unrecognized MI (n ¼ 205) Recognized MI (n ¼ 130) Age (yrs) * * * * Smokers Current 29.9% 39.4% 21.5% 18.1% 18.5%* 16.9%* Former 61.5% 53.3% 73.6%* 27.9% 26.3% 29.2% Body mass index (kg/m 2 ) * * Diabetes mellitus 9.1% 17.0%* 17.3%* 10.2% 15.1% 19.2% Total cholesterol (mmol/l) * Total cholesterol (mg/dl) * HDL cholesterol (mmol/l) *, * * HDL cholesterol (mg/dl) *, * 50 14* Systolic blood pressure (mm Hg) *, * *, Diastolic blood pressure (mm Hg) *, * 69 14*, Hypertension 51.1% 63.0%* 59.9%* 57.0% 67.8% 65.4% Use of blood pressureelowering drugs 22.5% 28.5% 70.7%*, 31.6% 36.6% 82.3%*, Aspirin 11.1% 12.1% 35.5%*, 7.9% 10.2% 32.6%*, Nitrates 4.2% 4.8% 32.6%*, 5.0% 3.9% 52.7%*, Statins 1.4% 1.2% 9.4%*, 1.7% 1.0% 8.5%*, Data are expressed as mean SD or as percentages. HDL ¼ high-density lipoprotein. * Significantly different from subjects without MI (age adjusted if applicable). Significantly different from subjects with recognized MI (age adjusted if applicable). subjects participated (response rate 78%). Once participants entered the Rotterdam Study, they were continuously monitored for mortality and morbidity. The medical ethics committee of Erasmus Medical Center approved the study, and written informed consent was obtained to participate and to permit access to information from treating physicians. At baseline, participants were asked if they had ever experienced a heart attack. Furthermore, a 12-lead electrocardiogram was recorded using an ACTA electrocardiograph (Esaote, Florence, Italy) at a sampling frequency of 500 Hz. All electrocardiograms were digitized and processed using the Modular ECG Analysis System (MEANS) to obtain electrocardiographic (ECG) measurements and interpretations. 14 The MEANS has been extensively evaluated previously. 15e17 The MEANS uses a comprehensive set of criteria, partly derived from the Minnesota codes, to determine MI. 18 The diagnosis of MI is based mainly on measurements on pathologic Q waves and on auxiliary criteria, such as QR ratio and R-wave progression. Subsequently, 2 research physicians, blinded to other clinical information, validated the electrocardiograms that were diagnosed by MEANS as indicating possible, probable, or certain MI. A cardiologist, specializing in ECG methods, ascertained the final diagnosis of MI. A history of recognized MI included subjects with self-reported MIs confirmed by clinical data or ECG evidence of MI. 19,20 A history of unrecognized MI included all participants without documented or self-reported MIs but with ECG characteristics matching an MI. Subjects without indications of MI on electrocardiography and no self-reports of earlier MIs were classified as no MI. At the start of the Rotterdam Study, we did not report the presence of unrecognized MI to participants or general practitioners at baseline (1990 to 1993). The decision was based on the previous perception in The Netherlands that an unrecognized MI was less severe than a recognized MI and was motivated by a lack of evidence for treatment after unrecognized MI to effectively reduce the risk for subsequent cardiovascular events. From the third follow-up visit onward (January 2002), we reported new findings of ECG unrecognized MI to participants and their general practitioners. Participants underwent an extensive interview at home by a trained research assistant using a questionnaire to obtain information on medical history and current health status. Labels of all medications used by participants were copied during this interview. At the research center, blood pressure was measured twice in the right upper arm in a sitting position using a random-zero sphygmomanometer. In the analyses, the average of these 2 measurements was used. Diabetes mellitus was defined as random or postload serum glucose level >11.0 mmol/l or the use of oral blood glucoseelowering drugs or insulin. We calculated body mass index as weight in kilograms divided by the square of height in meters. Serum total cholesterol and high-density lipoprotein cholesterol were determined by means of an automated enzymatic procedure in nonfasting blood samples. Participants vital status was ascertained from the moment of enrollment into the Rotterdam Study until January 1, The information was acquired on a weekly basis from the municipal authorities of Rotterdam. Additionally, the general practitioners in the suburb of Ommoord reported deaths on a continuing basis. Reported deaths were verified by specially trained study personnel who checked the medical records. When an event was reported, additional information was collected (e.g., hospital records, nursing home records). Deaths were classified as cardiovascular or noncardiovascular.
3 Coronary Artery Disease/Prognosis of Unrecognized Myocardial Infarction 3 Table 2 All-cause mortality in patients with recognized and unrecognized myocardial infarctions Group Number (Deaths) Mortality Rate* Hazard Ratio (95% Confidence Interval) Age and Gender Adjusted Multivariate Adjusted Men No MI 2,200 (1,179) (reference) 1.00 (reference) Unrecognized MI 165 (126) (1.43e2.07) 1.57 (1.30e1.89) Recognized MI 307 (230) (1.36e1.81) 1.67 (1.45e1.94) Women No MI 3,527 (1,630) (reference) 1.00 (reference) Unrecognized MI 205 (137) (1.14e1.61) 1.33 (1.11e1.58) Recognized MI 130 (110) (1.56e2.30) 1.87 (1.54e2.28) * Per 1,000 patient-years. Further adjusted for systolic and diastolic blood pressure, indication for antihypertensive medication, total cholesterol, high-density lipoprotein cholesterol, smoking, body mass index, and type 2 diabetes. center at baseline. ECG data were missing for 619 subjects, mainly for logistic reasons. The population for analysis consisted of 6,534 subjects. The 1,449 excluded subjects were older (8.7 years) and more likely to be men (14% of women and 21% of men were excluded). Because previous reports suggested a difference in prognosis of unrecognized MI between men and women, 3,22 analysis was done separately in men and women. All analyses were adjusted for age. Differences in baseline characteristics between subjects without MI, those with recognized MI, and those with unrecognized MI were evaluated using linear and logistic regression models adjusted for age. We used Cox proportional-hazards models to calculate the hazard ratios for total mortality and cause-specific mortality associated with unrecognized MI and recognized MI at baseline. Subjects without MIs were used as the reference group. To examine whether the association was significantly different in men and women, we introduced an interaction term to the model. We first investigated all-cause mortality and subsequently cardiovascular and noncardiovascular mortality separately. Kaplan-Meier plots were generated to illustrate the survival differences over time among different groups. Missing values were imputed using an expectation maximization algorithm. 23 Figure 1. Kaplan-Meier curves for cumulative survival in men (A) and women (B) with unrecognized, recognized, and no MIs. The methods of adjudication and the underlying definition of cardiovascular mortality have been described previously. 21 This classification focuses on the underlying cause rather than on mode of death. In short, a research physician weighed all available clinical information in each potentially cardiovascular death according to predefined criteria to adjudicate the underlying cause of death as being cardiovascular or noncardiovascular. All cases were verified by a physician specializing in cardiology, whose judgment was considered final. We excluded 830 subjects who did not visit the research Results Table 1 lists the baseline characteristics of the study population, stratified by gender. Men with unrecognized MIs had significantly higher body mass indexes and were more often diagnosed as hypertensive. Women had significantly higher body mass indexes, had higher systolic and diastolic blood pressure, had lower high-density lipoprotein cholesterol, and more often reported being current smokers. The comparisons were adjusted for age and gender. During 82,268 patient-years of follow-up (median 15.6 years) a total of 3,412 patients died. Of these deaths, 1,300 were due to cardiovascular diseases, 1,956 were due to noncardiovascular diseases, and 156 were due to uncertain causes because of limited information. Table 2 lists the association of recognized and unrecognized MI with all-cause mortality. Recognized MI and unrecognized MI were associated with an increased risk for all-cause mortality. In men, unrecognized MI showed a somewhat stronger association with all-cause
4 4 The American Journal of Cardiology ( Table 3 Cause-specific mortality in patients with recognized and unrecognized myocardial infarctions Group Number Cardiovascular Mortality Noncardiovascular Mortality Deaths Mortality Rate* HR (95% CI) Deaths Mortality Rate* HR (95% CI) Men No MI 2, (reference) (reference) Unrecognized MI (1.66e2.91) (1.14e1.89) Recognized MI (2.02e3.02) (0.85e1.31) Women No MI 3, (reference) (reference) Unrecognized MI (1.03e1.81) (1.10e1.75) Recognized MI (1.93e3.32) (1.13e2.02) CI ¼ confidence interval; HR ¼ hazard ratio. * Per 1,000 patient-years. Adjusted for age and gender. mortality compared with recognized MI. In women, however, recognized MI was more strongly associated with all-cause mortality than unrecognized MI. The gender difference in the strength of associations was not statistically significant for unrecognized MI (p for interaction ¼ 0.053), or recognized MI (p for interaction ¼ 0.080). Additional adjustment for cardiovascular risk factors did not materially change the results. Figure 1 shows the Kaplan-Meier curves for all-cause mortality in men and women. Table 3 lists the associations of recognized and unrecognized MI with cardiovascular and noncardiovascular mortality. Unrecognized MI was associated with cardiovascular mortality in men and women. The association was significantly stronger in men than in women (p for interaction ¼ 0.024). Conversely, recognized MI increased the risk for noncardiovascular mortality in women but not in men (p for interaction ¼ 0.054). Discussion This population-based cohort study confirms that unrecognized MI is associated with high all-cause mortality in men and women. In men, the increased risk is even larger than that associated with recognized MI. Furthermore, unrecognized MI was associated with higher risk for cardiovascular as well as noncardiovascular mortality in men and women. Thus far, several studies have investigated the prognosis of unrecognized MI pertaining to mortality and recurrent ischemic heart disease. 4,5,7,11,24 These studies, which were conducted mainly in the 1990s, showed that unrecognized MI is not a benign condition and that patients with unrecognized MIs had increased risk for mortality compared with those without MIs. Recently, we have reported on the prognosis of unrecognized MI with respect to risk for stroke, 22 dementia, 25 heart failure, 20 and atrial fibrillation. 26 In the present study, we report on contemporary data regarding the prognosis of unrecognized MI with respect to all-cause mortality and cause-specific mortality. We hypothesized that changes in lifestyle, better self-awareness of health, and widespread introduction of primary prevention of cardiovascular disease could have changed the prognosis of unrecognized MI over the years. However, our results show that the prognosis of unrecognized MI is still as unfavorable as of recognized MI. We found that men and women with unrecognized MI had an increased risk for all-cause mortality compared with subjects without MI. This is in accordance with previous studies reporting similar results. 4,5,7,11,24 A likely explanation for this finding is that lack of preventive cardiovascular treatment and lifestyle advice may have contributed to a poorer prognosis after unrecognized MI compared with the prognosis after recognized MI. Support for this hypothesis comes from the observation in our study that subjects with recognized MIs considerably more often used aspirin, nitrates, statins, and b blockers than those with unrecognized MIs (Table 1). However, it should be noted that the lipid profiles of patients with recognized MIs were slightly worse than the profiles of those with unrecognized MIs. To take such baseline differences into account, we further adjusted the association for major cardiovascular risk factors. However, the prognosis of unrecognized MI remained as unfavorable as of recognized MI. This may indicate that unrecognized MI gives a more comprehensive image of an patient s cardiovascular risk profile than individual cardiovascular risk factors measured only once at baseline. Although unrecognized MI was followed by an increase in all-cause mortality in men and women, the increase was not to the same extent in men (72%) and women (36%). Although men with unrecognized MIs had >10% increased risk compared with men with recognized MI, women with unrecognized MI had a better prognosis compared with women with recognized MI. This gender difference was observed in former studies 24 and was reported by us with other end points, such as stroke and brain infarct, 22,27 dementia, 25 heart failure, 20 and atrial fibrillation. 26 An explanation for this difference between men and women might be the misclassification of unrecognized MI in women. ECG abnormalities that are not caused by coronary artery disease, but can be mistaken for MI, are more often present in women than in men. These abnormalities are possibly caused by difficulties in correctly placing the electrodes because of breast tissue. 28 In agreement with this explanation, we found that the prevalence of unrecognized MI was similar in men and women (6.2% vs 5.3%), while the percentages were far from each other concerning recognized MI (11.5% vs 3.4%). Because of this possible nondifferential misclassification of our unrecognized MI, dilution of the effect might have occurred, and therefore the
5 Coronary Artery Disease/Prognosis of Unrecognized Myocardial Infarction 5 poor prognosis may have been underestimated in women. Such misclassification is less likely to have occurred for recognized MI, because this diagnosis is also confirmed by clinical information. We reported that recognized MI was associated with higher cardiovascular mortality in men and women compared with unrecognized MI. It is likely that extensive MIs less often remained unrecognized. In agreement with this conjecture, it has been shown that the infarct size is smaller in unrecognized MI compared with recognized MI. 29 Therefore, higher cardiovascular mortality in recognized MI may be due to more sever and extensive MI. Another speculation is suboptimal treatment of recognized MI, which can be seen in Table 1. Most of these subjects might have experienced MIs well before the start of this study (1990 to 1993), when coronary revascularization during acute MI was not part of everyday clinical practice. Therefore, the current anticipated improvements in outcomes for recognized MI should not be fully expected in our population. We report that subjects with unrecognized MIs had significantly higher noncardiovascular mortality. This finding is consistent with those of former studies. 5 An explanation for the increase in noncardiovascular mortality might be the presence of noncardiovascular morbidities. Such morbidities might lead patients to mistake their infarcts atypical symptoms for morbidity (e.g., dyspnea in chronic obstructive pulmonary disease) or affect their ability to sense their infarcts ( silent MI ). We did not report the presence of unrecognized MIs to participants and practitioners until Therefore, our results reflect in part the situation in the general population, in which a large proportion of MIs remain unrecognized and hence untreated. Since 2002, however, medication use and lifestyles may have changed in those who were still alive as a result of the their awareness about their unrecognized MIs. This may have caused an underestimation of the prognosis of silent MI. The strengths of our study lie in its large population and long follow-up period. We examined the association separately in men and women and identified gender differences in the prognosis of unrecognized MI. A number of limitations should be acknowledged. First, >500 subjects were excluded from our analysis because of missing electrocardiograms. Given that the missing electrocardiograms were randomly distributed and due mainly to temporary logistic reasons, our results are not likely to have been affected by this problem. Second, MI on electrocardiography was diagnosed using the MEANS computer program. However, this program has been formerly validated, and diagnoses agree very well with diagnoses made by an experienced cardiologist. 14,15 Moreover, any potential misclassification is likely to be nondifferential because MEANS diagnoses were made independent from the prognosis. Finally, as in a classic cohort study design, we based our analysis only on the status of individuals (recognized or unrecognized MI) at baseline. Given that the follow-up period was rather long (median 15.6 years), this may have caused a nondifferential misclassification of exposure, leading to an underestimation of the effect estimates. Unrecognized MI remains a problem in clinical practice. It would be worthwhile to search for factors related to the recognition of MI. Such risk factors could help identify those who are more at risk for unrecognized MI and will help more timely recognition of MI cases. In parallel, its diagnosis needs to be improved, especially in the elderly. Given the high prevalence of unrecognized MI in the elderly population and its poor prognosis, studies should investigate to what extent screening for unrecognized MI is feasible, whether it will help reducing mortality rates, and whether it is cost effective or not. Acknowledgment: We are very grateful to the participants and staff members of the Rotterdam Study, as well as the participating general practitioners and the pharmacists of the Ommoord district, Rotterdam, for help with data collection and validation. Disclosures The authors have no conflicts of interest to disclose. 1. Aronow WS. Silent MI. Prevalence and prognosis in older patients diagnosed by routine electrocardiograms. Geriatrics 2003;58:24e de Torbal A, Boersma E, Kors JA, van Herpen G, Deckers JW, van der Kuip DAM, Stricker BH, Hofman A, Witteman JCM. Incidence of recognized and unrecognized myocardial infarction in men and women aged 55 and older: the Rotterdam Study. Eur Heart J 2006;27:729e Kannel WB, Abbott RD. Incidence and prognosis of unrecognized myocardial infarction. An update on the Framingham study. N Engl J Med 1984;311:1144e Sigurdsson E, Thorgeirsson G, Sigvaldason H, Sigfusson N. Unrecognized myocardial infarction: epidemiology, clinical characteristics, and the prognostic role of angina pectoris. The Reykjavik Study. Ann Intern Med 1995;122:96e Sheifer SE, Gersh BJ, Yanez ND III, Ades PA, Burke GL, Manolio TA. Prevalence, predisposing factors, and prognosis of clinically unrecognized myocardial infarction in the elderly. J Am Coll Cardiol 2000;35: 119e Ammar KA, Yawn BP, Urban L, Mahoney DW, Kors JA, Jacobsen S, Rodeheffer RJ. Identification of optimal electrocardiographic criteria for the diagnosis of unrecognized myocardial infarction: a populationbased study. Ann Noninvasive Electrocardiol 2005;10:197e Nadelmann J, Frishman WH, Ooi WL, Tepper D, Greenberg S, Guzik H, Lazar EJ, Heiman M, Aronson M. Prevalence, incidence and prognosis of recognized and unrecognized myocardial infarction in persons aged 75 years or older: the Bronx Aging Study. Am J Cardiol 1990;66:533e Schelbert EB, Cao JJ, Sigurdsson S, Aspelund T, Kellman P, Aletras AH, Dyke CK, Thorgeirsson G, Eiriksdottir G, Launer LJ, Gudnason V, Harris TB, Arai AE. Prevalence and prognosis of unrecognized myocardial infarction determined by cardiac magnetic resonance in older adults. JAMA 2012;308:890e Sheifer SE, Manolio TA, Gersh BJ. Unrecognized myocardial infarction. Ann Intern Med 2001;135:801e Boland LL, Folsom AR, Sorlie PD, Taylor HA, Rosamond WD, Chambless LE, Cooper LS. Occurrence of unrecognized myocardial infarction in subjects aged 45 to 65 years (the ARIC study). Am J Cardiol 2002;90:927e Yano K, MacLean CJ. The incidence and prognosis of unrecognized myocardial infarction in the Honolulu, Hawaii, Heart Program. Arch Intern Med 1989;149:1528e Hofman A, Grobbee DE, de Jong PT, van den Ouweland FA. Determinants of disease and disability in the elderly: the Rotterdam Elderly Study. Eur J Epidemiol 1991;7:403e Hofman A, van Duijn CM, Franco OH, Ikram MA, Janssen HLA, Klaver CCW, Kuipers EJ, Nijsten TEC, Stricker BH, Tiemeier H,
6 6 The American Journal of Cardiology ( Uitterlinden AG, Vernooij MW, Witteman JCM. The Rotterdam Study: 2012 objectives and design update. Eur J Epidemiol 2011;26: 657e van Bemmel JH, Kors JA, van Herpen G. Methodology of the modular ECG analysis system MEANS. Methods Inf Med 1990;29:346e de Bruyne MC, Kors JA, Hoes AW, Kruijssen DA, Deckers JW, Grosfeld M, van Herpen G, Grobbee DE, van Bemmel JH. Diagnostic interpretation of electrocardiograms in population-based research: computer program research physicians, or cardiologists? J Clin Epidemiol 1997;50:947e Willems JL, Abreu-Lima C, Arnaud P, van Bemmel JH, Brohet C, Degani R, Denis B, Gehring J, Graham I, van Herpen G, Machado H, Macfarlane PW, Michaelis J, Moulopoulos SD, Rubel P, Zywietz C. The diagnostic performance of computer programs for the interpretation of electrocardiograms. N Engl J Med 1991;325:1767e Kors JA, van Herpen G, Wu J, Zhang Z, Prineas RJ, van Bemmel JH. Validation of a new computer program for Minnesota coding. J Electrocardiol 1996;29:83e Prineas RJ, Crow RS, Blackburn H. The Minnesota code manual of electrocardiographic findings. Boston, Massachusetts: John Wright PSB; de Bruyne MC, Mosterd A, Hoes AW, Kors JA, Kruijssen DA, van Bemmel JH, Hofman A, Grobbee DE. Prevalence, determinants, and misclassification of myocardial infarction in the elderly. Epidemiology 1997;8:495e Leening MJG, Elias-Smale SE, Felix JF, Kors JA, Deckers JW, Hofman A, Stricker BH, Witteman JC. Unrecognised myocardial infarction and long-term risk of heart failure in the elderly: the Rotterdam Study. Heart 2010;96:1458e Leening MJG, Kavousi M, Heeringa J, van Rooij FJA, Verkroost-van Heemst J, Deckers JW, Mattace-Raso FUS, Ziere G, Hofman A, Stricker BHC, Witteman JCM. Methods of data collection and definitions of cardiac outcomes in the Rotterdam Study. Eur J Epidemiol 2012;27: 173e Ikram MA, Hollander M, Bos MJ, Kors JA, Koudstaal PJ, Hofman A, Witteman JCM, Breteler MMB. Unrecognized myocardial infarction and the risk of stroke: the Rotterdam Study. Neurology 2006;67: 1635e Dempster A, Laird NM, Laird NM. Maximum likelihood from incomplete data via the EM algorithm. J Stat Soc B 1977;39:1e Kannel WB, Cupples LA, Gagnon DR. Incidence, precursors and prognosis of unrecognized myocardial infarction. Adv Cardiol 1990;37:202e Ikram MA, van Oijen M, de Jong FJ, Kors JA, Koudstaal PJ, Hofman A, Witteman JCM, Breteler MMB. Unrecognized myocardial infarction in relation to risk of dementia and cerebral small vessel disease. Stroke 2008;39:1421e Krijthe BP, Leening MJG, Heeringa J, Kors JA, Hofman A, Franco OH, Witteman JCM, Stricker BH. Unrecognized myocardial infarction and risk of atrial fibrillation: the Rotterdam Study. Int J Cardiol 2013;168: 1453e Jonsdottir LS, Sigfusson N, Sigvaldason H, Thorgeirsson G. Incidence and prevalence of recognised and unrecognised myocardial infarction in women. The Reykjavik Study. Eur Heart J 1998;19:1011e Murabito JM, Evans JC, Larson MG, Levy D. Prognosis after the onset of coronary heart disease. An investigation of differences in outcome between the sexes according to initial coronary disease presentation. Circulation 1993;88:2548e Cabin HS, Roberts WC. Quantitative comparison of extent of coronary narrowing and size of healed myocardial infarct in 33 necropsy patients with clinically recognized and in 28 with clinically unrecognized ( silent ) previous acute myocardial infarction. Am J Cardiol 1982;50: 677e681.
Unrecognized Myocardial Infarction in Relation to Risk of Dementia and Cerebral Small Vessel Disease
 Unrecognized Myocardial Infarction in Relation to Risk of Dementia and Cerebral Small Vessel Disease M. Arfan Ikram, MD; Marieke van Oijen, MD, PhD; Frank Jan de Jong, MD; Jan A. Kors, PhD; Peter J. Koudstaal,
Unrecognized Myocardial Infarction in Relation to Risk of Dementia and Cerebral Small Vessel Disease M. Arfan Ikram, MD; Marieke van Oijen, MD, PhD; Frank Jan de Jong, MD; Jan A. Kors, PhD; Peter J. Koudstaal,
Supplementary Online Content
 Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
Non-steroidal anti-inflammatory drugs and the risk of atrial fibrillation: a population-based follow-up study
 Research Non-steroidal anti-inflammatory drugs and the risk of atrial fibrillation: a population-based follow-up study Bouwe P Krijthe, 1,2 Jan Heeringa, 1 Albert Hofman, 1 Oscar H Franco, 1 Bruno H Stricker
Research Non-steroidal anti-inflammatory drugs and the risk of atrial fibrillation: a population-based follow-up study Bouwe P Krijthe, 1,2 Jan Heeringa, 1 Albert Hofman, 1 Oscar H Franco, 1 Bruno H Stricker
Orthostatic hypotension is common in elderly people 1 4
 CLINICAL INVESTIGATIONS Orthostatic Hypotension and Risk of Cardiovascular Disease in Elderly People: The Rotterdam Study Germaine C. Verwoert, w Francesco U. S. Mattace-Raso, MD, PhD, w Albert Hofman,
CLINICAL INVESTIGATIONS Orthostatic Hypotension and Risk of Cardiovascular Disease in Elderly People: The Rotterdam Study Germaine C. Verwoert, w Francesco U. S. Mattace-Raso, MD, PhD, w Albert Hofman,
Heart failure and the risk of stroke: the Rotterdam Study
 Eur J Epidemiol (2010) 25:807 812 DOI 10.1007/s10654-010-9520-y NEURO-EPIDEMIOLOGY Heart failure and the risk of stroke: the Rotterdam Study V. P. Alberts M. J. Bos P. J. Koudstaal A. Hofman J. C. M. Witteman
Eur J Epidemiol (2010) 25:807 812 DOI 10.1007/s10654-010-9520-y NEURO-EPIDEMIOLOGY Heart failure and the risk of stroke: the Rotterdam Study V. P. Alberts M. J. Bos P. J. Koudstaal A. Hofman J. C. M. Witteman
A: Epidemiology update. Evidence that LDL-C and CRP identify different high-risk groups
 A: Epidemiology update Evidence that LDL-C and CRP identify different high-risk groups Women (n = 27,939; mean age 54.7 years) who were free of symptomatic cardiovascular (CV) disease at baseline were
A: Epidemiology update Evidence that LDL-C and CRP identify different high-risk groups Women (n = 27,939; mean age 54.7 years) who were free of symptomatic cardiovascular (CV) disease at baseline were
Clinical Investigation and Reports. Predictive Value of Noninvasive Measures of Atherosclerosis for Incident Myocardial Infarction
 Clinical Investigation and Reports Predictive Value of Noninvasive Measures of Atherosclerosis for Incident Myocardial Infarction The Rotterdam Study Irene M. van der Meer, MD, PhD; Michiel L. Bots, MD,
Clinical Investigation and Reports Predictive Value of Noninvasive Measures of Atherosclerosis for Incident Myocardial Infarction The Rotterdam Study Irene M. van der Meer, MD, PhD; Michiel L. Bots, MD,
Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts Future Cardiovascular Events
 Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
Selecting subjects for ultrasonographic screening for aneurysms of the abdominal aorta: four different strategies
 International Epidemiological Association 1999 Printed in Great Britain International Journal of Epidemiology 1999;28:682 686 Selecting subjects for ultrasonographic screening for aneurysms of the abdominal
International Epidemiological Association 1999 Printed in Great Britain International Journal of Epidemiology 1999;28:682 686 Selecting subjects for ultrasonographic screening for aneurysms of the abdominal
Risk Factors for Ischemic Stroke: Electrocardiographic Findings
 Original Articles 232 Risk Factors for Ischemic Stroke: Electrocardiographic Findings Elley H.H. Chiu 1,2, Teng-Yeow Tan 1,3, Ku-Chou Chang 1,3, and Chia-Wei Liou 1,3 Abstract- Background: Standard 12-lead
Original Articles 232 Risk Factors for Ischemic Stroke: Electrocardiographic Findings Elley H.H. Chiu 1,2, Teng-Yeow Tan 1,3, Ku-Chou Chang 1,3, and Chia-Wei Liou 1,3 Abstract- Background: Standard 12-lead
Effect of intravenous atropine on treadmill stress test results in patients with poor exercise capacity or chronotropic incompetence ABSTRACT
 Effect of intravenous atropine on treadmill stress test results in patients with poor exercise capacity or chronotropic incompetence Samad Ghaffari, MD, Bahram Sohrabi, MD. ABSTRACT Objective: Exercise
Effect of intravenous atropine on treadmill stress test results in patients with poor exercise capacity or chronotropic incompetence Samad Ghaffari, MD, Bahram Sohrabi, MD. ABSTRACT Objective: Exercise
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION Subclinical Atherosclerosis and Risk of Atrial Fibrillation The Rotterdam Study Jan Heeringa, MD; Deirdre A. M. van der Kuip, MD, PhD; Albert Hofman, MD, PhD; Jan A. Kors, PhD; Frank
ORIGINAL INVESTIGATION Subclinical Atherosclerosis and Risk of Atrial Fibrillation The Rotterdam Study Jan Heeringa, MD; Deirdre A. M. van der Kuip, MD, PhD; Albert Hofman, MD, PhD; Jan A. Kors, PhD; Frank
Is Carotid Intima-Media Thickness Useful in Cardiovascular Disease Risk Assessment? The Rotterdam Study
 Is Carotid Intima-Media Thickness Useful in Cardiovascular Disease Risk Assessment? The Rotterdam Study Antonio Iglesias del Sol, MD; Karel G.M. Moons, MD, PhD; Monika Hollander, MD; Albert Hofman, MD,
Is Carotid Intima-Media Thickness Useful in Cardiovascular Disease Risk Assessment? The Rotterdam Study Antonio Iglesias del Sol, MD; Karel G.M. Moons, MD, PhD; Monika Hollander, MD; Albert Hofman, MD,
Panel III (ATP-III), and the European Society of Cardiology (ESC) guidelines using a cohort of Dutch individuals aged 55 years or older.
 Research Original Investigation Comparison of Application of the ACC/AHA Guidelines, Adult Treatment Panel III Guidelines, and European Society of Cardiology Guidelines for Cardiovascular Disease Prevention
Research Original Investigation Comparison of Application of the ACC/AHA Guidelines, Adult Treatment Panel III Guidelines, and European Society of Cardiology Guidelines for Cardiovascular Disease Prevention
Coronary calcification detected by electron-beam computed tomography and myocardial infarction
 European Heart Journal (2002) 23, 1596 1603 doi:10.1053/euhj.2002.3240, available online at http://www.idealibrary.com on Coronary calcification detected by electron-beam computed tomography and myocardial
European Heart Journal (2002) 23, 1596 1603 doi:10.1053/euhj.2002.3240, available online at http://www.idealibrary.com on Coronary calcification detected by electron-beam computed tomography and myocardial
Baldness and Coronary Heart Disease Rates in Men from the Framingham Study
 A BRIEF ORIGINAL CONTRIBUTION Baldness and Coronary Heart Disease Rates in Men from the Framingham Study The authors assessed the relation between the extent and progression of baldness and coronary heart
A BRIEF ORIGINAL CONTRIBUTION Baldness and Coronary Heart Disease Rates in Men from the Framingham Study The authors assessed the relation between the extent and progression of baldness and coronary heart
Prevalence, incidence and lifetime risk of atrial fibrillation: the Rotterdam study
 European Heart Journal (2006) 27, 949 953 doi:10.1093/eurheartj/ehi825 Clinical research Arrhythmia/electrophysiology Prevalence, incidence and lifetime risk of atrial fibrillation: the Rotterdam study
European Heart Journal (2006) 27, 949 953 doi:10.1093/eurheartj/ehi825 Clinical research Arrhythmia/electrophysiology Prevalence, incidence and lifetime risk of atrial fibrillation: the Rotterdam study
Comparison of Probability of Stroke Between the Copenhagen City Heart Study and the Framingham Study
 80 Comparison of Probability of Stroke Between the Copenhagen City Heart Study and the Framingham Study Thomas Truelsen, MB; Ewa Lindenstrtfm, MD; Gudrun Boysen, DMSc Background and Purpose We wished to
80 Comparison of Probability of Stroke Between the Copenhagen City Heart Study and the Framingham Study Thomas Truelsen, MB; Ewa Lindenstrtfm, MD; Gudrun Boysen, DMSc Background and Purpose We wished to
Donald M. Lloyd-Jones, MD, ScM a,b, *, Alan R. Dyer, PhD a, Renwei Wang, MS a, Martha L. Daviglus, MD, PhD a, and Philip Greenland, MD a,b
 Risk Factor Burden in Middle Age and Lifetime Risks for Cardiovascular and Non-Cardiovascular Death (Chicago Heart Association Detection Project in Industry) Donald M. Lloyd-Jones, MD, ScM a,b, *, Alan
Risk Factor Burden in Middle Age and Lifetime Risks for Cardiovascular and Non-Cardiovascular Death (Chicago Heart Association Detection Project in Industry) Donald M. Lloyd-Jones, MD, ScM a,b, *, Alan
YOUNG ADULT MEN AND MIDDLEaged
 BRIEF REPORT Favorable Cardiovascular Profile in Young Women and Long-term of Cardiovascular and All-Cause Mortality Martha L. Daviglus, MD, PhD Jeremiah Stamler, MD Amber Pirzada, MD Lijing L. Yan, PhD,
BRIEF REPORT Favorable Cardiovascular Profile in Young Women and Long-term of Cardiovascular and All-Cause Mortality Martha L. Daviglus, MD, PhD Jeremiah Stamler, MD Amber Pirzada, MD Lijing L. Yan, PhD,
Journal of the American College of Cardiology Vol. 50, No. 11, by the American College of Cardiology Foundation ISSN /07/$32.
 Journal of the American College of Cardiology Vol. 50, No. 11, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.05.035
Journal of the American College of Cardiology Vol. 50, No. 11, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.05.035
Hospital and 1-year outcome after acute myocardial infarction in patients with diabetes mellitus and hypertension
 (2003) 17, 665 670 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Hospital and 1-year outcome after acute myocardial infarction in patients with
(2003) 17, 665 670 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Hospital and 1-year outcome after acute myocardial infarction in patients with
High-Normal Blood Pressure Progression to Hypertension in the Framingham Heart Study
 22 High- Blood Pressure Progression to Hypertension in the Framingham Heart Study Mark Leitschuh, L. Adrienne Cupples, William Kannel, David Gagnon, and Aram Chobanian This study sought to determine if
22 High- Blood Pressure Progression to Hypertension in the Framingham Heart Study Mark Leitschuh, L. Adrienne Cupples, William Kannel, David Gagnon, and Aram Chobanian This study sought to determine if
Antihypertensive Trial Design ALLHAT
 1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
Original Article. Resting Heart Rate and the Risk of Heart Failure in Healthy Adults The Rotterdam Study
 Original Article Resting Heart Rate and the Risk of Heart Failure in Healthy Adults The Rotterdam Study David Nanchen, MD, MSc; Maarten J.G. Leening, MD, MSc; Isabella Locatelli, PhD; Jacques Cornuz, MD,
Original Article Resting Heart Rate and the Risk of Heart Failure in Healthy Adults The Rotterdam Study David Nanchen, MD, MSc; Maarten J.G. Leening, MD, MSc; Isabella Locatelli, PhD; Jacques Cornuz, MD,
ARIC Manuscript Proposal # PC Reviewed: 05/12/09 Status: A Priority: 2 SC Reviewed: Status: Priority:
 ARIC Manuscript Proposal # 1508 PC Reviewed: 05/12/09 Status: A Priority: 2 SC Reviewed: Status: Priority: 1.a. Full Title: Hemostatic markers and risk of atrial fibrillation: the Atherosclerosis Risk
ARIC Manuscript Proposal # 1508 PC Reviewed: 05/12/09 Status: A Priority: 2 SC Reviewed: Status: Priority: 1.a. Full Title: Hemostatic markers and risk of atrial fibrillation: the Atherosclerosis Risk
ARIC Manuscript Proposal # PC Reviewed: 2/10/09 Status: A Priority: 2 SC Reviewed: Status: Priority:
 ARIC Manuscript Proposal # 1475 PC Reviewed: 2/10/09 Status: A Priority: 2 SC Reviewed: Status: Priority: 1.a. Full Title: Hypertension, left ventricular hypertrophy, and risk of incident hospitalized
ARIC Manuscript Proposal # 1475 PC Reviewed: 2/10/09 Status: A Priority: 2 SC Reviewed: Status: Priority: 1.a. Full Title: Hypertension, left ventricular hypertrophy, and risk of incident hospitalized
Does quality of life predict morbidity or mortality in patients with atrial fibrillation (AF)?
 Does quality of life predict morbidity or mortality in patients with atrial fibrillation (AF)? Erika Friedmann a, Eleanor Schron, b Sue A. Thomas a a University of Maryland School of Nursing; b NEI, National
Does quality of life predict morbidity or mortality in patients with atrial fibrillation (AF)? Erika Friedmann a, Eleanor Schron, b Sue A. Thomas a a University of Maryland School of Nursing; b NEI, National
Central pressures and prediction of cardiovascular events in erectile dysfunction patients
 Central pressures and prediction of cardiovascular events in erectile dysfunction patients N. Ioakeimidis, K. Rokkas, A. Angelis, Z. Kratiras, M. Abdelrasoul, C. Georgakopoulos, D. Terentes-Printzios,
Central pressures and prediction of cardiovascular events in erectile dysfunction patients N. Ioakeimidis, K. Rokkas, A. Angelis, Z. Kratiras, M. Abdelrasoul, C. Georgakopoulos, D. Terentes-Printzios,
The Whitehall II study originally comprised 10,308 (3413 women) individuals who, at
 Supplementary notes on Methods The study originally comprised 10,308 (3413 women) individuals who, at recruitment in 1985/8, were London-based government employees (civil servants) aged 35 to 55 years.
Supplementary notes on Methods The study originally comprised 10,308 (3413 women) individuals who, at recruitment in 1985/8, were London-based government employees (civil servants) aged 35 to 55 years.
Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden
 Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden Cardiovascular Disease Prevention (CVD) Three Strategies for CVD
Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden Cardiovascular Disease Prevention (CVD) Three Strategies for CVD
Long-term prognosis of unrecognized myocardial infarction detected with cardiovascular magnetic resonance in an elderly population
 Barbier et al. Journal of Cardiovascular Magnetic Resonance (2016) 18:43 DOI 10.1186/s12968-016-0264-z RESEARCH Long-term prognosis of unrecognized myocardial infarction detected with cardiovascular magnetic
Barbier et al. Journal of Cardiovascular Magnetic Resonance (2016) 18:43 DOI 10.1186/s12968-016-0264-z RESEARCH Long-term prognosis of unrecognized myocardial infarction detected with cardiovascular magnetic
CVD risk assessment using risk scores in primary and secondary prevention
 CVD risk assessment using risk scores in primary and secondary prevention Raul D. Santos MD, PhD Heart Institute-InCor University of Sao Paulo Brazil Disclosure Honoraria for consulting and speaker activities
CVD risk assessment using risk scores in primary and secondary prevention Raul D. Santos MD, PhD Heart Institute-InCor University of Sao Paulo Brazil Disclosure Honoraria for consulting and speaker activities
GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS
 GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS Table of Contents List of authors pag 2 Supplemental figure I pag 3 Supplemental figure II pag 4 Supplemental
GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS Table of Contents List of authors pag 2 Supplemental figure I pag 3 Supplemental figure II pag 4 Supplemental
Serum glucose and insulin are associated with QTc and RR intervals in nondiabetic elderly
 European Journal of Endocrinology (2010) 162 241 248 ISSN 0804-4643 CLINICAL STUDY Serum glucose and insulin are associated with QTc and RR intervals in nondiabetic elderly Charlotte van Noord 1,4, Miriam
European Journal of Endocrinology (2010) 162 241 248 ISSN 0804-4643 CLINICAL STUDY Serum glucose and insulin are associated with QTc and RR intervals in nondiabetic elderly Charlotte van Noord 1,4, Miriam
The Framingham Coronary Heart Disease Risk Score
 Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
Supplementary Online Content
 Supplementary Online Content Åsvold BO, Vatten LJ, Bjøro T, et al; Thyroid Studies Collaboration. Thyroid function within the normal range and risk of coronary heart disease: an individual participant
Supplementary Online Content Åsvold BO, Vatten LJ, Bjøro T, et al; Thyroid Studies Collaboration. Thyroid function within the normal range and risk of coronary heart disease: an individual participant
Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient
 Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient Dr. Peersab.M. Pinjar 1, Dr Praveenkumar Devarbahvi 1 and Dr Vasudeva Murthy.C.R 2, Dr.S.S.Bhat 1, Dr.Jayaraj S G 1
Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient Dr. Peersab.M. Pinjar 1, Dr Praveenkumar Devarbahvi 1 and Dr Vasudeva Murthy.C.R 2, Dr.S.S.Bhat 1, Dr.Jayaraj S G 1
Risk factors for coronary calcification in older subjects
 European Heart Journal (2004) 25, 48 55 Clinical research Risk factors for coronary calcification in older subjects The Rotterdam Coronary Calcification Study Hok-Hay S. Oei a,b, Rozemarijn Vliegenthart
European Heart Journal (2004) 25, 48 55 Clinical research Risk factors for coronary calcification in older subjects The Rotterdam Coronary Calcification Study Hok-Hay S. Oei a,b, Rozemarijn Vliegenthart
Coronary Calcification Improves Cardiovascular Risk Prediction in the Elderly
 Coronary Calcification Improves Cardiovascular Risk Prediction in the Elderly Rozemarijn Vliegenthart, PhD; Matthijs Oudkerk, MD, PhD; Albert Hofman, MD, PhD; Hok-Hay S. Oei, MD, PhD; Wim van Dijck, MSc;
Coronary Calcification Improves Cardiovascular Risk Prediction in the Elderly Rozemarijn Vliegenthart, PhD; Matthijs Oudkerk, MD, PhD; Albert Hofman, MD, PhD; Hok-Hay S. Oei, MD, PhD; Wim van Dijck, MSc;
Inflammation, as Measured by the Erythrocyte Sedimentation Rate, Is an Independent Predictor for the Development of Heart Failure
 Journal of the American College of Cardiology Vol. 45, No. 11, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.02.066
Journal of the American College of Cardiology Vol. 45, No. 11, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.02.066
The Framingham Risk Score (FRS) is widely recommended
 C-Reactive Protein Modulates Risk Prediction Based on the Framingham Score Implications for Future Risk Assessment: Results From a Large Cohort Study in Southern Germany Wolfgang Koenig, MD; Hannelore
C-Reactive Protein Modulates Risk Prediction Based on the Framingham Score Implications for Future Risk Assessment: Results From a Large Cohort Study in Southern Germany Wolfgang Koenig, MD; Hannelore
Silent brain infarcts are frequently seen on MRIs in healthy
 Incidence and Risk Factors of Silent Brain Infarcts in the Population-Based Rotterdam Scan Study Sarah E. Vermeer, MD, PhD; Tom den Heijer, MD; Peter J. Koudstaal, MD, PhD; Matthijs Oudkerk, MD, PhD; Albert
Incidence and Risk Factors of Silent Brain Infarcts in the Population-Based Rotterdam Scan Study Sarah E. Vermeer, MD, PhD; Tom den Heijer, MD; Peter J. Koudstaal, MD, PhD; Matthijs Oudkerk, MD, PhD; Albert
Prevalence and Positive Predictive Value of Poor R-Wave Progression and Impact of the Cardiothoracic Ratio
 ORIGINAL ARTICLE DOI 1070 / kcj.2009.39.118 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Open Access Prevalence and Positive Predictive Value of Poor
ORIGINAL ARTICLE DOI 1070 / kcj.2009.39.118 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Open Access Prevalence and Positive Predictive Value of Poor
Title for Paragraph Format Slide
 Title for Paragraph Format Slide Presentation Title: Month Date, Year Atherosclerosis A Spectrum of Disease: February 12, 2015 Richard Cameron Padgett, MD Executive Medical Director, OHVI Pt RB Age 38
Title for Paragraph Format Slide Presentation Title: Month Date, Year Atherosclerosis A Spectrum of Disease: February 12, 2015 Richard Cameron Padgett, MD Executive Medical Director, OHVI Pt RB Age 38
Elevated blood pressure (BP) is a major modifiable risk factor
 Blood Pressure in Adulthood and Life Expectancy With Cardiovascular Disease in Men and Women Life Course Analysis Oscar H. Franco, Anna Peeters, Luc Bonneux, Chris de Laet Abstract Limited information
Blood Pressure in Adulthood and Life Expectancy With Cardiovascular Disease in Men and Women Life Course Analysis Oscar H. Franco, Anna Peeters, Luc Bonneux, Chris de Laet Abstract Limited information
The MAIN-COMPARE Study
 Long-Term Outcomes of Coronary Stent Implantation versus Bypass Surgery for the Treatment of Unprotected Left Main Coronary Artery Disease Revascularization for Unprotected Left MAIN Coronary Artery Stenosis:
Long-Term Outcomes of Coronary Stent Implantation versus Bypass Surgery for the Treatment of Unprotected Left Main Coronary Artery Disease Revascularization for Unprotected Left MAIN Coronary Artery Stenosis:
4/4/17 HYPERTENSION TARGETS: WHAT DO WE DO NOW? SET THE STAGE BP IN CLINICAL TRIALS?
 HYPERTENSION TARGETS: WHAT DO WE DO NOW? MICHAEL LEFEVRE, MD, MSPH PROFESSOR AND VICE CHAIR DEPARTMENT OF FAMILY AND COMMUNITY MEDICINE UNIVERSITY OF MISSOURI 4/4/17 DISCLOSURE: MEMBER OF THE JNC 8 PANEL
HYPERTENSION TARGETS: WHAT DO WE DO NOW? MICHAEL LEFEVRE, MD, MSPH PROFESSOR AND VICE CHAIR DEPARTMENT OF FAMILY AND COMMUNITY MEDICINE UNIVERSITY OF MISSOURI 4/4/17 DISCLOSURE: MEMBER OF THE JNC 8 PANEL
Supplementary Online Content
 Supplementary Online Content Schnabel RB, Aspelund T, Li G, et al. Validation of an atrial fibrillation risk algorithm in whites and African Americans. Arch Intern Med. 2010;170(21):1909-1917. eappendix.
Supplementary Online Content Schnabel RB, Aspelund T, Li G, et al. Validation of an atrial fibrillation risk algorithm in whites and African Americans. Arch Intern Med. 2010;170(21):1909-1917. eappendix.
The Impact of Diabetes Mellitus and Prior Myocardial Infarction on Mortality From All Causes and From Coronary Heart Disease in Men
 Journal of the American College of Cardiology Vol. 40, No. 5, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)02044-2
Journal of the American College of Cardiology Vol. 40, No. 5, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)02044-2
/13/$ - see front matter Ó 2013 Elsevier Inc. All rights reserved.
 Prognostic Value of Frontal QRS-T Angle in Patients Without Clinical Evidence of Cardiovascular Disease (from the Multi-Ethnic Study of Atherosclerosis) Joseph A. Walsh III, MD, MS a,b, Elsayed Z. Soliman,
Prognostic Value of Frontal QRS-T Angle in Patients Without Clinical Evidence of Cardiovascular Disease (from the Multi-Ethnic Study of Atherosclerosis) Joseph A. Walsh III, MD, MS a,b, Elsayed Z. Soliman,
the U.S. population, have some form of cardiovascular disease. Each year, approximately 6 million hospitalizations
 Cardioprotection: What is it? Who needs it? William B. Kannel, MD, MPH From the Department of Preventive Medicine and Epidemiology, Evans Department of Clinical Research, Boston University School of Medicine,
Cardioprotection: What is it? Who needs it? William B. Kannel, MD, MPH From the Department of Preventive Medicine and Epidemiology, Evans Department of Clinical Research, Boston University School of Medicine,
Supplementary Online Content
 Supplementary Online Content Pedersen SB, Langsted A, Nordestgaard BG. Nonfasting mild-to-moderate hypertriglyceridemia and risk of acute pancreatitis. JAMA Intern Med. Published online November 7, 2016.
Supplementary Online Content Pedersen SB, Langsted A, Nordestgaard BG. Nonfasting mild-to-moderate hypertriglyceridemia and risk of acute pancreatitis. JAMA Intern Med. Published online November 7, 2016.
Atrial fibrillation (AF), the most common sustained cardiac
 Atrial Fibrillation and the Prothrombotic State in the Elderly The Rotterdam Study Dwayne S.G. Conway, MRCP; Jan Heeringa, MD; Deirdre A.M. Van Der Kuip, MD, PhD; Bernard S.P. Chin, MRCP; Albert Hofman,
Atrial Fibrillation and the Prothrombotic State in the Elderly The Rotterdam Study Dwayne S.G. Conway, MRCP; Jan Heeringa, MD; Deirdre A.M. Van Der Kuip, MD, PhD; Bernard S.P. Chin, MRCP; Albert Hofman,
Antihypertensive Drug Therapy and Survival by Treatment Status in a National Survey
 1-28 Antihypertensive Drug Therapy and Survival by Treatment Status in a National Survey Richard J. Havlik, Andrea Z. LaCroix, Joel C. Kleinman, Deborah D. Ingram, Tamara Harris, and Joan Cornoni-Huntley
1-28 Antihypertensive Drug Therapy and Survival by Treatment Status in a National Survey Richard J. Havlik, Andrea Z. LaCroix, Joel C. Kleinman, Deborah D. Ingram, Tamara Harris, and Joan Cornoni-Huntley
LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC
![LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC](/thumbs/88/116891773.jpg) Am J Cardiol (2004);94:729-32 Relation of degree of physical activity to coronary artery calcium score in asymptomatic individuals with multiple metabolic risk factors M. Y. Desai, et al. Ciccarone Preventive
Am J Cardiol (2004);94:729-32 Relation of degree of physical activity to coronary artery calcium score in asymptomatic individuals with multiple metabolic risk factors M. Y. Desai, et al. Ciccarone Preventive
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Berry JD, Dyer A, Cai X, et al. Lifetime risks of cardiovascular
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Berry JD, Dyer A, Cai X, et al. Lifetime risks of cardiovascular
Andrew Cohen, MD and Neil S. Skolnik, MD INTRODUCTION
 2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
Prevalence (%) Table S4 Prevalence of AF in women and men, age- specific Study name/country Study population Study period Age group
 Table S4 Prevalence of AF in and men, age- specific Study name/country Yunnan Province, China Random sample of government Guo (2015) 1 medical insurance plan Age 20 years Spain Gomez- Doblas (2014) 2 The
Table S4 Prevalence of AF in and men, age- specific Study name/country Yunnan Province, China Random sample of government Guo (2015) 1 medical insurance plan Age 20 years Spain Gomez- Doblas (2014) 2 The
(n=6279). Continuous variables are reported as mean with 95% confidence interval and T1 T2 T3. Number of subjects
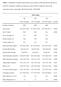 Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Low fractional diastolic pressure in the ascending aorta increased the risk of coronary heart disease
 (2002) 16, 837 841 & 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Low fractional diastolic pressure in the ascending aorta increased the risk
(2002) 16, 837 841 & 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Low fractional diastolic pressure in the ascending aorta increased the risk
Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors.
 Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Appendix to: Banks E, Crouch SR, Korda RJ, et al. Absolute risk of cardiovascular
Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Appendix to: Banks E, Crouch SR, Korda RJ, et al. Absolute risk of cardiovascular
ORIGINAL INVESTIGATION. Corticosteroids and the Risk of Atrial Fibrillation
 ORIGINAL INVESTIGATION Corticosteroids and the Risk of Atrial Fibrillation Cornelis S. van der Hooft, MD; Jan Heeringa, MD; Guy G. Brusselle, MD, PhD; Albert Hofman, MD, PhD; Jacqueline C. M. Witteman,
ORIGINAL INVESTIGATION Corticosteroids and the Risk of Atrial Fibrillation Cornelis S. van der Hooft, MD; Jan Heeringa, MD; Guy G. Brusselle, MD, PhD; Albert Hofman, MD, PhD; Jacqueline C. M. Witteman,
The MAIN-COMPARE Registry
 Long-Term Outcomes of Coronary Stent Implantation versus Bypass Surgery for the Treatment of Unprotected Left Main Coronary Artery Disease Revascularization for Unprotected Left MAIN Coronary Artery Stenosis:
Long-Term Outcomes of Coronary Stent Implantation versus Bypass Surgery for the Treatment of Unprotected Left Main Coronary Artery Disease Revascularization for Unprotected Left MAIN Coronary Artery Stenosis:
Predicting cardiovascular risk in the elderly in different European countries
 European Heart Journal (2002) 23, 294 300 doi:10.1053/euhj.2001.2898, available online at http://www.idealibrary.com on Predicting cardiovascular risk in the elderly in different European countries S.
European Heart Journal (2002) 23, 294 300 doi:10.1053/euhj.2001.2898, available online at http://www.idealibrary.com on Predicting cardiovascular risk in the elderly in different European countries S.
Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial
 Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial Sripal Bangalore, MD, MHA, Chuan-Chuan Wun, PhD, David A DeMicco, PharmD,
Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial Sripal Bangalore, MD, MHA, Chuan-Chuan Wun, PhD, David A DeMicco, PharmD,
ORIGINAL INVESTIGATION. The Long-term Prognostic Value of the Resting and Postexercise Ankle-Brachial Index
 ORIGINAL INVESTIGATION The Long-term Prognostic Value of the Resting and Postexercise Ankle-Brachial Index Harm H. H. Feringa, MD; Jeroen J. J. Bax, MD, PhD; Virginie H. van Waning, MD; Eric Boersma, PhD;
ORIGINAL INVESTIGATION The Long-term Prognostic Value of the Resting and Postexercise Ankle-Brachial Index Harm H. H. Feringa, MD; Jeroen J. J. Bax, MD, PhD; Virginie H. van Waning, MD; Eric Boersma, PhD;
Clinical and Economic Value of Rivaroxaban in Coronary Artery Disease
 CHRISTOPHER B. GRANGER, MD Professor of Medicine Division of Cardiology, Department of Medicine; Director, Cardiac Care Unit Duke University Medical Center, Durham, NC Clinical and Economic Value of Rivaroxaban
CHRISTOPHER B. GRANGER, MD Professor of Medicine Division of Cardiology, Department of Medicine; Director, Cardiac Care Unit Duke University Medical Center, Durham, NC Clinical and Economic Value of Rivaroxaban
/HE. Both Decreased and Increased Heart Rate Variability on the Standard 10-Second Electrocardiogram Predict Cardiac Mortality In the Elderly
 /HE American Journal of Epidemiology Copyright 0999 by The Johns Hopkins University School or Hygiene and PubOc Health All rights reserved Vol. 50, No. 2 Printed in U.S.A. Both Decreased and Increased
/HE American Journal of Epidemiology Copyright 0999 by The Johns Hopkins University School or Hygiene and PubOc Health All rights reserved Vol. 50, No. 2 Printed in U.S.A. Both Decreased and Increased
Serum cholesterol and long-term prognosis in middle-aged men with myocardial infarction and angina pectoris
 European Heart Journal (1997) 18, 754-761 Serum cholesterol and long-term prognosis in middle-aged men with myocardial and angina pectoris A 16-year follow-up of the Primary Prevention Study in Goteborg,
European Heart Journal (1997) 18, 754-761 Serum cholesterol and long-term prognosis in middle-aged men with myocardial and angina pectoris A 16-year follow-up of the Primary Prevention Study in Goteborg,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/25009 holds various files of this Leiden University dissertation. Author: Sabayan, Behnam Title: Cardiovascular and hemodynamic contribution to brain aging
Cover Page The handle http://hdl.handle.net/1887/25009 holds various files of this Leiden University dissertation. Author: Sabayan, Behnam Title: Cardiovascular and hemodynamic contribution to brain aging
10-Year Mortality of Older Acute Myocardial Infarction Patients Treated in U.S. Community Practice
 10-Year Mortality of Older Acute Myocardial Infarction Patients Treated in U.S. Community Practice Ajar Kochar, MD on behalf of: Anita Y. Chen, Puza P. Sharma, Neha J. Pagidipati, Gregg C. Fonarow, Patricia
10-Year Mortality of Older Acute Myocardial Infarction Patients Treated in U.S. Community Practice Ajar Kochar, MD on behalf of: Anita Y. Chen, Puza P. Sharma, Neha J. Pagidipati, Gregg C. Fonarow, Patricia
Diabetologia 9 Springer-Verlag 1991
 Diabetologia (1991) 34:590-594 0012186X91001685 Diabetologia 9 Springer-Verlag 1991 Risk factors for macrovascular disease in mellitus: the London follow-up to the WHO Multinational Study of Vascular Disease
Diabetologia (1991) 34:590-594 0012186X91001685 Diabetologia 9 Springer-Verlag 1991 Risk factors for macrovascular disease in mellitus: the London follow-up to the WHO Multinational Study of Vascular Disease
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Setting The setting was the Walter Reed Army Medical Center. The economic study was carried out in the USA.
 Coronary calcium independently predicts incident premature coronary heart disease over measured cardiovascular risk factors: mean three-year outcomes in the Prospective Army Coronary Calcium (PACC) project
Coronary calcium independently predicts incident premature coronary heart disease over measured cardiovascular risk factors: mean three-year outcomes in the Prospective Army Coronary Calcium (PACC) project
I t is well established that non-insulin dependent diabetes is
 1398 CARDIOVASCULAR MEDICINE Cardiovascular disease incidence and mortality in older men with diabetes and in men with coronary heart disease S G Wannamethee, A G Shaper, L Lennon... See end of article
1398 CARDIOVASCULAR MEDICINE Cardiovascular disease incidence and mortality in older men with diabetes and in men with coronary heart disease S G Wannamethee, A G Shaper, L Lennon... See end of article
Prognostic Significance of Coronary Collaterals in Patients With Coronary Heart Disease Having Percutaneous Transluminal Coronary Angioplasty
 Prognostic Significance of Coronary Collaterals in Patients With Coronary Heart Disease Having Percutaneous Transluminal Coronary Angioplasty Jeroen Koerselman, MD, PhD a, Peter P.T. de Jaegere, MD, PhD
Prognostic Significance of Coronary Collaterals in Patients With Coronary Heart Disease Having Percutaneous Transluminal Coronary Angioplasty Jeroen Koerselman, MD, PhD a, Peter P.T. de Jaegere, MD, PhD
Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes
 Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes Seung-Jae Joo and other KAMIR-NIH investigators Department of Cardiology, Jeju National
Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes Seung-Jae Joo and other KAMIR-NIH investigators Department of Cardiology, Jeju National
Usefulness of Exercise Testing in the Prediction of Coronary Disease Risk Among Asymptomatic Persons as a Function of the Framingham Risk Score
 Usefulness of Exercise Testing in the Prediction of Coronary Disease Risk Among Asymptomatic Persons as a Function of the Framingham Risk Score Gary J. Balady, MD; Martin G. Larson, SD; Ramachandran S.
Usefulness of Exercise Testing in the Prediction of Coronary Disease Risk Among Asymptomatic Persons as a Function of the Framingham Risk Score Gary J. Balady, MD; Martin G. Larson, SD; Ramachandran S.
John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam
 Latest Insights from the JUPITER Study John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam Inflammation, hscrp, and Vascular Prevention
Latest Insights from the JUPITER Study John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam Inflammation, hscrp, and Vascular Prevention
Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis
 CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
Fatality of Future Coronary Events Is Related to Inflammation-Sensitive Plasma Proteins
 Fatality of Future Coronary Events Is Related to Inflammation-Sensitive Plasma Proteins A Population-Based Prospective Cohort Study Gunnar Engström, MD; Bo Hedblad, MD; Lars Stavenow, MD; Patrik Tydén,
Fatality of Future Coronary Events Is Related to Inflammation-Sensitive Plasma Proteins A Population-Based Prospective Cohort Study Gunnar Engström, MD; Bo Hedblad, MD; Lars Stavenow, MD; Patrik Tydén,
Subclinical AF: Implications of device based episodes
 Subclinical AF: Implications of device based episodes Michael R Gold, MD, PhD Medical University of South Carolina Charleston, SC Disclosures: Clinical Trials and Consulting: Medtronic, Boston Scientific
Subclinical AF: Implications of device based episodes Michael R Gold, MD, PhD Medical University of South Carolina Charleston, SC Disclosures: Clinical Trials and Consulting: Medtronic, Boston Scientific
ORIGINAL INVESTIGATION. C-Reactive Protein Concentration and Incident Hypertension in Young Adults
 ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
Effects of Statins on Endothelial Function in Patients with Coronary Artery Disease
 Effects of Statins on Endothelial Function in Patients with Coronary Artery Disease Iana I. Simova, MD; Stefan V. Denchev, PhD; Simeon I. Dimitrov, PhD Clinic of Cardiology, University Hospital Alexandrovska,
Effects of Statins on Endothelial Function in Patients with Coronary Artery Disease Iana I. Simova, MD; Stefan V. Denchev, PhD; Simeon I. Dimitrov, PhD Clinic of Cardiology, University Hospital Alexandrovska,
ATTENTION-DEFICIT/HYPERACTIVITY DISORDER, PHYSICAL HEALTH, AND LIFESTYLE IN OLDER ADULTS
 CHAPTER 5 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER, PHYSICAL HEALTH, AND LIFESTYLE IN OLDER ADULTS J. AM. GERIATR. SOC. 2013;61(6):882 887 DOI: 10.1111/JGS.12261 61 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER,
CHAPTER 5 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER, PHYSICAL HEALTH, AND LIFESTYLE IN OLDER ADULTS J. AM. GERIATR. SOC. 2013;61(6):882 887 DOI: 10.1111/JGS.12261 61 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER,
Diabetes and Decline in Heart Disease Mortality in US Adults JAMA. 1999;281:
 ORIGINAL CONTRIBUTION and Decline in Mortality in US Adults Ken Gu, PhD Catherine C. Cowie, PhD, MPH Maureen I. Harris, PhD, MPH MORTALITY FROM HEART disease has declined substantially in the United States
ORIGINAL CONTRIBUTION and Decline in Mortality in US Adults Ken Gu, PhD Catherine C. Cowie, PhD, MPH Maureen I. Harris, PhD, MPH MORTALITY FROM HEART disease has declined substantially in the United States
Population prevalence, incidence, and predictors of atrial fibrillation in the Renfrew/Paisley study
 516 Clinical Research Initiative in Heart Failure, Wolfson Building (Level 3), University of Glasgow, Glasgow G12 8QQ, UK S Stewart J J V McMurray Department of Public Health, University of Glasgow C L
516 Clinical Research Initiative in Heart Failure, Wolfson Building (Level 3), University of Glasgow, Glasgow G12 8QQ, UK S Stewart J J V McMurray Department of Public Health, University of Glasgow C L
The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009
 The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009 Learning Objectives 1. Understand the role of statin therapy in the primary and secondary prevention of stroke 2. Explain
The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009 Learning Objectives 1. Understand the role of statin therapy in the primary and secondary prevention of stroke 2. Explain
Transient Ischemic Attacks and Risk of Stroke in an Elderly Poor Population
 Transient Ischemic Attacks and Risk of Stroke in an Elderly Poor Population BY A. M. OSTFELD, M.D., R. B. SHEKELLE, Ph.D., AND H. L. KLAWANS, M.D. Abstract: Transient Ischemic A t tacks and Risk of Stroke
Transient Ischemic Attacks and Risk of Stroke in an Elderly Poor Population BY A. M. OSTFELD, M.D., R. B. SHEKELLE, Ph.D., AND H. L. KLAWANS, M.D. Abstract: Transient Ischemic A t tacks and Risk of Stroke
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Bhakta N, Liu Q, Yeo F, et al. Cumulative burden
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Bhakta N, Liu Q, Yeo F, et al. Cumulative burden
Magnetic resonance imaging, image analysis:visual scoring of white matter
 Supplemental method ULSAM Magnetic resonance imaging, image analysis:visual scoring of white matter hyperintensities (WMHI) was performed by a neuroradiologist using a PACS system blinded of baseline data.
Supplemental method ULSAM Magnetic resonance imaging, image analysis:visual scoring of white matter hyperintensities (WMHI) was performed by a neuroradiologist using a PACS system blinded of baseline data.
Blood Pressure Targets: Where are We Now?
 Blood Pressure Targets: Where are We Now? Diana Cao, PharmD, BCPS-AQ Cardiology Assistant Professor Department of Clinical & Administrative Sciences California Northstate University College of Pharmacy
Blood Pressure Targets: Where are We Now? Diana Cao, PharmD, BCPS-AQ Cardiology Assistant Professor Department of Clinical & Administrative Sciences California Northstate University College of Pharmacy
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
Mortality Trends in Patients Diagnosed With First Atrial Fibrillation
 Journal of the American College of Cardiology Vol. 49, No. 9, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.10.062
Journal of the American College of Cardiology Vol. 49, No. 9, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.10.062
Evaluation of Anthropometric Indices of Patients with Left Ventricle Dysfunction Fallowing First Acute Anterior Myocardial Infarction
 Journal of Cardiovascular and Thoracic Research, 2012, 4(1), 11-15 doi: 10.5681/jcvtr.2012.003 http://jcvtr.tbzmed.ac.ir Evaluation of Anthropometric Indices of Patients with Left Ventricle Dysfunction
Journal of Cardiovascular and Thoracic Research, 2012, 4(1), 11-15 doi: 10.5681/jcvtr.2012.003 http://jcvtr.tbzmed.ac.ir Evaluation of Anthropometric Indices of Patients with Left Ventricle Dysfunction
What have We Learned in Dyslipidemia Management Since the Publication of the 2013 ACC/AHA Guideline?
 What have We Learned in Dyslipidemia Management Since the Publication of the 2013 ACC/AHA Guideline? Salim S. Virani, MD, PhD, FACC, FAHA Associate Professor, Section of Cardiovascular Research Baylor
What have We Learned in Dyslipidemia Management Since the Publication of the 2013 ACC/AHA Guideline? Salim S. Virani, MD, PhD, FACC, FAHA Associate Professor, Section of Cardiovascular Research Baylor
