Zhishun Liu, 1 Weiming Wang, 1,2 Jiani Wu, 1 Kehua Zhou, 3 and Baoyan Liu Introduction
|
|
|
- Wilfrid Cooper
- 5 years ago
- Views:
Transcription
1 Hindawi Publishing Corporation Evidence-Based Complementary and Alternative Medicine Volume 2013, Article ID , 9 pages Research Article Electroacupuncture Improves Bladder and Bowel Function in Patients with Traumatic Spinal Cord Injury: Results from a Prospective Observational Study Zhishun Liu, 1 Weiming Wang, 1,2 Jiani Wu, 1 Kehua Zhou, 3 and Baoyan Liu 1 1 Department of Acupuncture, Guang An Men Hospital, China Academy of Chinese Medical Sciences, No. 5 Bei Xian Ge Street, Xicheng, Beijing , China 2 Beijing University of Chinese Medicine, No. 11 North Third Ring Road East, Chaoyang, Beijing , China 3 Department of Health Care Studies, Daemen College, 4380 Main Street, Amherst, NY 14226, USA Correspondence should be addressed to Baoyan Liu; cectcm@gmail.com Received 23 June 2013; Accepted 14 November 2013 Academic Editor: Albert Moraska Copyright 2013 Zhishun Liu et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. In order to explore the effect of electroacupuncture (EA) for chronic bowel and dysfunction after traumatic spinal cord injury, 14 patients were treated with electroacupuncture once a day, five times a week for the first four weeks, and once every other day, three times a week for the following four weeks. The patients were then followed up for six months. After treatment, four (4/14, 28.57%) patients resumed normal voiding; six (6/14, 42.86%) resumed normal voiding for no less than half of all micturition behaviors; four (4/14, 28.57%) required supplementary urination methods for higher than half of all micturition behaviors. These effects persisted during followup. Mean postvoid RUV decreased by ± ml (P < 0.01) after treatment and by ± ml (P < 0.01) during followup. Patients weekly urinary incontinence frequency decreased 7.14±46.34 times/week (P = 0.036) after treatment and decreased ± times/week during followup. After treatment, four (4/14, 28.57%) patients resumed normal bowel movements (P = 0.025); five (5/14, 35.71%) reduced the dependence on supplementary defecation methods; five (5/14, 35.71%) had no changes. In patients with chronic bowel and dysfunction after traumatic SCI, EA may provide a valuable alternative tool in improving patients self-controlled bowel and functions with minimal side effects. 1. Introduction Traumatic spinal cord injury (SCI) is an accidental disaster, causing unexpected suffering physically, emotionally, and costly to patients [1]. Traumatic SCI can cause disorders of somatesthesia and locomotion below the level of injury. Neurogenic and bowel dysfunctions which affect the physical and psychological health of patients and severely decrease the quality of life are also prevalent in patients with traumatic SCI. Urological complications of neurogenic caused by traumatic SCI consist of inability to empty the, urinary tract infections (UTIs), incontinence, and upper urinary tract deterioration [2]. A distended may also cause pressure effects on adjacent structures including the left common iliac vein in the pelvis leading to adverse events of other organs [3]. Common bowel dysfunctions in patients with SCI may include poorly localized abdominal pain, difficulty with bowel evacuation, hemorrhoids, abdominal distention, and autonomic hyperreflexia arising from the gastrointestinal tract [4]. In patients with SCI, treatments for dysfunctions may involve conservative treatments (drug treatments,, assisted emptying, rehabilitation, and external appliances), minimally invasive treatments (botulinum toxin A injections in, intravesical vanilloid treatment, sphincterotomy, and ureteral reimplantation), and surgical treatments (autoaugmentation, sacral anterior root stimulation, sacral neuromodulation, and artificial urinary sphincter) [5]; treatments for bowel dysfunctions may include nonpharmacological therapies (, reflex stimulation, abdominal massage, assistive devices, and others), pharmacological agents (prucalopride, metoclopramide, neostigmine, and others), and surgical
2 2 Evidence-Based Complementary and Alternative Medicine interventions (implantation of electrical stimulation systems, colostomy, antegrade continence enema, and enema continence catheter) [6].Although these treatments are effective to some extent, none can help patients regain the self-controlled and bowel function. Furthermore, treatments like, sacral anterior root stimulation, colostomy, and enema will likely cause additional pain and other side effects to patients. Therefore, an effective and safe treatment with few side-effects is warranted for the treatment of and bowel dysfunction in patients with traumatic SCI. Acupuncture is a therapy that is commonly utilized by the Chinese people for the management of bowel and dysfunction. Documentation of acupuncture use for bowel and symptoms dates back to thousands of years ago in the ancient medical monograph Huang Di Nei Jin (Yellow Emperor s Inner Canon). Propositions of therapeutic effects of acupuncture in neurogenic bowel and dysfunctions are supported by modern research studies. Compared with urinary or use of medications, Cheng et al. [7] found that electroacupuncture (EA) could help acute SCI patients with neurogenic achieve balanced (continent, catheter-free) function, and Wong et al. [8]demonstratedthatEAatSI3andBL62inconjugationwith auricular acupoints promoted function recovery in patientswithacutesci.inaddition,wongetal.[8]alsofound thateacoulddecreasetheneedwithbowelcareandepisodes of fecal incontinence due to SCI. Similarly, manual acupuncture was found to induce resolution of urinary incontinence in 15% of patients with SCI-induced detrusor hyperreflexia [9]. In addition, the results of our previous case series study [10] andthestudybyhonjoetal.[9] indicatethateacould improve voiding abilities in patients with SCI. Among the aforementioned research studies, effects of EA on both bowel and functions were only reported in the study by Wong et al. [8]. Nonetheless, due to that the main purpose was patients general functional recovery after SCI, Wong et al. [8] did not provide sufficient information (such baseline values of patients voiding abilities) regarding patients bowel and function. As quality of these acupuncture studies is of dispute, conclusive evidence regarding acupuncture effects in patients with simultaneous neurogenic bowel and dysfunction after traumatic SCI is still lacking [11]. Consequently, in the present study, we aimed to explore the effects of EA for chronic bowel and dysfunction after traumatic SCI. 2. Materials and Methods 2.1. Study Design. This was a prospective consecutive case series study performed at the Acupuncture Department of Guang An Men Hospital, China Academy of Chinese Medical Sciences. The hospital ethics committee approved this treatment protocol, and all patients signed informed consent before study participation. Acupuncture procedures were implemented by senior acupuncturists at the department with more than 20 years clinical experiences. Data management and analysis were performed by graduates who were blinded to the treatment procedures Participants. For inclusion, the participants had to fulfill the following criteria: (1) simultaneous and bowel dysfunctions caused by traumatic SCI of or above Level L1; (2) no history of sphincter injury or surgery of the urinary tract, gastrointestinal tract, or anus; (3) SCI history for no less than six months and onset of bowel and symptoms after SCI;(4)theymustbeatleast18yearsold;(5)cardiac,hepatic, and renal functions as well as coagulative functions are normal or near normal; (6) no cognitive or mental disorders Acupuncture Protocol. Huatuo brand needles (size 0.45 mm 125 mm and 0.30 mm 75 mm, manufactured by Suzhou Medical Appliance, Suzhou, Jiangsu, China) together with GB Electro-Acu Stimulators (Medical Supply & Equipment Co., Ltd., Shanghai, China) were used. The parameters of electric stimulation were set as the follows: continuous wave with electric current frequency of 20 Hz and intensity between 3 and 10 ma according to patients tolerance. Based on the clinical experiences and anatomical knowledge (direct stimulation of S2-S3) of the acupuncturists, bilateral BL32, BL33, and BL35 were used. Acupoints were selected and localized according to the WHO Standardized Acupuncture Points Location [12]. Needlesofthesizeof0.30mm 75 mm were inserted into bilateral BL35 vertically with a depth of mm; 0.45 mm 125 mm size needles were inserted inwardly and downwardly into bilateral BL32 and BL33 (S2 and S3 foramina) at an angle of with a depth of mm. Paired alligator clips with negative and positive electrodes of the EA apparatus were attached to the needle holders at each pair of the same acupoints on each side during treatment. The positive electrodes were attached on the left, and the negative electrodes were attached on the right. Each EA treatment lasted for 50 minutes. All patients received EA treatment once a day, five times a week for the first four weeks, and once every other day, three times a week for the following four weeks. The patients were then followed up for 6 months Outcome Measurement. Bladder functions including postvoid residual urine volume (RUV), weekly urinary incontinence frequency, and additional conservative interventions (if any) were measured and documented at baseline, after treatment, and during followup. With reference to the International Lower Urinary Tract Function Basic Spinal Cord Injury Data Set [13], normal voiding in the present study is defined as voluntary initiation of micturition without reflex stimulation or compression of. Based on patients voiding abilities during the past 24 hours, they were divided into three groups after treatment: patients who had normal voiding all the time were categorized into Group A; patients with normal voiding frequency no less than half of all micturition behaviors were categorized into Group B; all the remaining patients who require assistive urination help with afrequencyforhigherthanhalfofallmicturitionbehaviors werecategorizedintogroupc. With reference to the International Bowel Function Basic SpinalCordInjury DataSet [14], patients bowel movements were divided into normal, partially normal, and complete
3 Evidence-Based Complementary and Alternative Medicine 3 constipation. In the present study, normal bowel movement is defined as self-initiated bowel movements without any help ofsupplementarymethodsduringthepast48hours;partially normal bowel movement is defined as more than half of the times that patient have self-initiated bowel movements with occasional supplementary defecation method use during the past 48 hours; complete constipation is defined as more than half of the times that patient require supplementary defecation method use for bowel movements during the past 48 hours. Postvoid RUV was measured using a cylinder via self-urethral after urination. The frequencies of normal voiding and urinary incontinence, postvoid RUV, and bowel movement conditions, as well a supplementary urination and defecation methods were recorded by our research staff in a and bowel diary each time during patients visit. Assessed for eligibility (n =69) Excluded (n =55) Did not have simultaneous and bowel dysfunction (n =44) History less than 6 months (n =6) Younger than 18 years old (n =3) Received EA treatment less than 5 times and dropped out (n =2) 2.5. Safety Measurement. Adverse events which may include hematoma, fainting, and unbearable pain and others were documented during study Statistical Analysis. Statistical analysis was performed with the SPSS software package (Version 17.0) for Windows XP. Quantitative data of postvoid RUV and weekly urinary incontinence frequency were expressed with mean ± standard deviations (SD). Paired samples t-test was used to measure the difference among values at baseline, after treatment, and during followup. A significance level of P < 0.05 and twotailed tests were used for all analyses. 3. Results As presented in Figure 1, from December 12, 2007, to October 31, 2011, a total of 69 patients with SCI visited the Outpatient Department of Acupuncture at Guang An Men Hospital. Among these patients, 25 had and bowel dysfunctions; however, 11 of them were excluded from the present study for the following reasons: six patients had SCI injury less than six months ago; three patients were younger than 18 years old; two patients received EA treatment less than 5 times and dropped out during treatment. Consequently, 14 patients were included in the final analysis. Ofthese14patients,nineweremaleandfivewerefemale; eight had motor vehicle accident, five were injured from falling, and one was injured by gun shot. The mean age of these participants was 34 years old with a range from 21 to 57 years old. The mean disease course was 16.3 months with a range from six months to nine years. In these 14 patients, two patients injuries were at the cervical level, two at the upper thoracic level, four at the lower thoracic level, and six at thelumbarlevel.accordingtoamericanspinalcordinjury Association (ASIA) Impairment Scale (AIS) classification [15], impairments of the included patients were classified as follows: five had Grade A (complete) impairment, six had Grade B (sensory incomplete) impairment, and three had Grade C (motor incomplete) impairment (Table 1). Patients accepted acupuncture treatment (n =14) Gender: female (n =5), male (n =9) Causes: motor vehicle accident (n =8) Falling injury (n =5) Gunshot injury (n =1) Age: years old History: 6 months 9 years Figure 1: Flow chart of study participation Assessments of Bladder Function. Before treatment, all 14 patients had no normal voiding ability and required assisted therapies ( or abdominal push) to empty. After eight-week treatment, four (4/14, 28.57%) patients resumed normal voiding (Group A); six (6/14, 42.86%) resumed normal voiding for no less than half of all micturition behaviors (Group B); four (4/14, 28.57%) required assistive urination therapies for higher than half of all micturition behaviors (Group C). In the six patients of Group B, three patients required emptying via abdominal push, two required, and one required both. Similar results were found during followup (Table 1). Mean postvoid RUV for these 14 patients decreased by ± ml after treatment, from ± ml at baseline to ± ml (P = 0.000). Compared with baseline, the mean postvoid RUV was decreased by ± ml during followup, from ± ml at baseline to ± ml (P = 0.000). Compared with baseline, the mean postvoid RUV of patients was decreased by 190 ± ml after eight-week treatment and by 192 ± ml during followup in Group A; the decreases were ± ml after treatment and ± ml during followup in Group B, and ± ml after treatment and ± ml during followup in Group C(see Figure2 and Table 2). Of these 14 patients, seven patients (7/14, 50.00%) had various degrees of urinary incontinence. Five out of these seven patients were diagnosed as detrusor hyperreflexia
4 4 Evidence-Based Complementary and Alternative Medicine The whole sample Group A Group B Group C Baseline After treatment Followup Figure2:HistogramofmeanpostvoidRUV.GroupArefersto patients who had normal voiding all the time; Group B refers to patients with normal voiding frequency no less than half of all micturition; Group C refers to patients who require assistive urination help with a frequency higher than half of all micturition. through urodynamic study (UDS) before treatment; the remaining two patients lacked relevant examination. After treatment, the weekly urinary incontinence frequency for these seven patients reduced from ± times/week at baseline to ± times/week (P = 0.036); during followup, the weekly urinary incontinence frequency reduced to ± times/week (P = 0.025). Among the remaining seven patients who had urinary retention before treatment, four patients were diagnosed as detrusor areflexia through UDS, and the other three patients did not provide UDS information. During treatment, five (all four patients with detrusor areflexia and one with insufficient UDS information) out of these seven patients with urinary retention developed urinary incontinence. Two patients developed urinary incontinence during the 2nd week; however, the urinary incontinence symptoms were completely gone by the end of the 4th week. The remaining three patients developed urinary incontinence during the 8th week with a frequency of three times per week, 10 times per week, and five times per week, respectively; however, two out of these three had no incontinence during followup; the remaining one continued to present with urinary incontinence which was 5 times per week during followup Assessment of Bowel Function. Before treatment, all 14 patients had constipation and required supplementary methods for defecation, and thus their symptoms were considered as complete constipation. After treatment, four (4/14, 28.57%) resumed normal bowel movements; five (5/14, 35.71%) regained partially normal bowel movements and reduced the dependence on supplementary defecation methods;five(5/14,35.71%)hadnochange.inthefivepatientswho regained partially normal bowel movements, one resumed the desire to defecate, one resumed anal reflex, and three regained the soft and smooth stool which was made of nutslike hard lumps before. The effects of EA were maintained during followup (Table 1) Adverse Effects. No adverse effects were found. Five patients with residual sensory functions reported pain, sourness, numbness, and/or distension upon acupuncture procedures, which were well tolerated during treatment and disappeared after needle removal. Based on traditional Chinese medicine theories, these sensations are likely to be categorized into the De Qi sensations and are thus considered normal during acupuncture treatment [16]. 4. Discussion 4.1. EA and Function Recovery in SCI Patients. Under physiological conditions, neurons are considered as permanent cells which remain in the G0 phase and lack proliferation. With spinal cord injury, sprouting and regeneration of the CNS tracts depend on the functions of glia cells due to the poor regenerative capacity of axons [17]. The development of a glial scar and the accumulation of extracellular matrix (ECM) proteoglycans generate an impermeable barrier that further hinders axons from regenerating across the site of injury [18, 19]. Thus, neurological dysfunctions caused by SCI are generally considered extremely difficult to recover [11]. Patients with SCI who have no perianal pinprick sensation at initial evaluation never regain volitional voiding and bowel function recovery following SCI is not favorable [20]. Therefore, therapies that enhance more natural patient control of voiding and defecation are appealing. In the present study, adult patients with a history of chronic neurogenic bowel and symptoms were included. Improvements in bowel and functions in these patients are more likely to be related to the therapeutic effects of EA rather than spontaneous recovery. 4.2.BowelandBladderFunctionswithEA.Improvements of bowel and functions will reinforce patients confidence in recovery, encourage patient s social interaction, andincreasethequalityoflifeandthusgreatlydecrease the incidence of SCI-associated complications and the development of other comorbidities [11]. Recently, sacral neuromodulation which employs implants of electric stimulator in the pelvic region and surgical reinnervation with nerve anastomosis were found effective in the treatment of bowel and dysfunctions caused by TSCI [21 23]. However, these interventions require surgical procedures which may be only applicable to a limited number of patients and may be accompanied with unfavorable side effects [5]. EA at S2-3 provides a combinational stimulation of acupuncture and electric therapy; therefore, EA therapy in the present study can be considered as minimal invasive type of sacral neuromodulation which has minimal side effects. Results of the present study indicate that EA at S2-3 and perianal region could improve patients voiding abilities. The results were consistent with our previous findings in which 10 outof15patientswithcaudaequinainjuryresumedvoiding
5 Evidence-Based Complementary and Alternative Medicine 5 Table 1: Demographic information and changes of urination and defecation after electroacupuncture treatment. No. Gender (F/M) Age (years) Courses (months) Injured level AISA classification 1 F 21 8 T11 A Urination form Defecation form Baseline after treatment After followup Baseline after treatment After followup Normal voiding Normal voiding 2 F 36 6 L1 A Normal voiding Normal voiding perianal stimulation perianal stimulation perianal stimulation 3 M 48 6 L1 B Normal voiding Normal voiding Normal defecation Normal defecation 4 M L1 B assisted by hands 5 F C5 C 6 M 27 6 L1 C Normal defecation Normal defecation 7 M 27 9 L1 B + pushing the
6 6 Evidence-Based Complementary and Alternative Medicine No. Gender (F/M) Age (years) Courses (months) Injured level AISA classification 8 M 48 6 T10 B 9 F T9 A 10 M C5 B 11 M T3 C 12 F 26 7 T6 A 13 M L1 B 14 M 26 6 T12 A Table 1: Continued. Urination form Defecation form Baseline after treatment After followup Baseline after treatment After followup Normal voiding Normal voiding Normal defecation Normal defecation (dosage reduced 50%) (dosage reduced 50%) (dosage reduced 50%) (dosage reduced 50%) Normal defecation Normal defecation
7 Evidence-Based Complementary and Alternative Medicine 7 Table 2: Mean postvoid RUV. n Baseline (A) After treatment (B) Followup (C) Difference x±s tvalue P value AB AC BC AB AC BC AB AC BC 14 (total) ± ± ± ± ± ± >0.05 4(groupA) ± ± ± ± ± ± >0.05 6(groupB) ± ± ± ± ± ± >0.05 4(groupC) ± ± ± ± ± ± >0.05 >0.05
8 8 Evidence-Based Complementary and Alternative Medicine abilities and were urinary catheter-free after a similar EA treatment protocol [10]. Honjo et al. [9] found that EA at S2 was found to be effective in improving control decreasing incontinence frequencies in patients with detrusor hyperreflexia. The present study demonstrated a similar response of EA via decreasing patients incontinence frequencies. In the present study, detrusor hyperreflexia in nine patients (five patients with previous detrusor hyperreflexia and four patients with transient detrusor hyperreflexia) was successfully treated by EA and had no urinary incontinence at the end of treatment. Furthermore, Wong et al. [8] found that EA could decrease incontinence frequencies or assistance for bowel care in patients with SCI; the results of the present study indicate that EA could increase patients abilities to self-initiate bowel movements and decrease the need of supplementary defection methods. Thus, the results of the present study add further credence to the therapeutic effects of EA on neurogenic bowel. Bladder functions can also be reflected by postvoid RUV. In the present study, postvoid RUV was measured using a cylinder via self-urethral after full urination. This technique theoretically provides reliable information regarding residue urine volume and thus the first impression of patients voiding function [24]. In the present study, EA was found to significantly decrease postvoid RUV both after treatment and during followup. These results echo with our previous findings in patients with cauda equina injury patients [10]. The decrease in postvoid RUV reflects the improvement of voiding ability with EA in patients with neurogenic. In addition, findings of heaven amount of postvoid RUV in patients with urinary incontinence or detrusor hyperreflexia in the present study indicate that involuntary contraction in urinary incontinence is ineffective which concurs with other urinary incontinence studies [25, 26] Possible Therapeutic Mechanism of EA in Bowel and Bladder Dysfunctions. In conjuncture with evidence from the aforementioned research studies, we hypothesize that EA sacral nerve stimulation could modulate urinary functions in patients with SCI. Pelvic splanchnic nerves do not only provide parasympathetic innervations to the detrusor muscle responsible for involuntary emptying, but also parasympathetic innervations to the sigmoid colon and rectum responsible for involuntary bowel movements. Somatic components of the pudendal nerve directly innervate the external urethral sphincter and the external anal sphincter via its branches of inferior anal nerves; normal functions of these sphincters serve as the foundation for normal bowel and control. Both the pelvic splanchnic nerves and pudendal nerve arise from S2 S4; therefore, EA at S2-3 provides direct electric and mechanical stimulation to these nerves. Nonetheless, EA stimulation at S2-3 is nonselective which indicates two extremely opposite conditions. This could at least partially contribute to the interesting opposite phenomena (effects on neurogenic urinary retention and urinary incontinence) discovered with EA treatment at S2-3[9, 10]. To better utilize this minimal invasive direct nerve stimulation, more studies are warranted to develop selective EA treatment on the parasympathetic nerves or the pudendal nerve Limitations. Nonetheless, the present study is a case seriesstudywitharelativesmallsamplesizewhichindicates that results of the present study may not well represent the general response of patients with chronic bowel and dysfunction caused by SCI. For example, in the present study, standard deviations of some quantitative measurements (such as postvoid RUV and the change of weekly urinary incontinence frequency after treatment) were bigger than its corresponding mean which indicates relative wide dispersions of values in the small sample and is unfavorable for the statistical analyses. Assessments of acupuncture effects in the present study mainly depend on patients reports which may be interfered with recall bias and patients believes and emotional status upon visits. To objectively evaluate EA effects on neurogenic bowel and dysfunction, we may need to incorporate urodynamic measurements in future studies. Furthermore, assessment of bowel functions is limited to patient-reported bowel movement frequencies and supplementary defecation methods, information like average time required for defecation, frequency of defecation, and frequency of fecal incontinence is lacking. 5. Conclusion In patients with chronic bowel and dysfunction after SCI, EA may provide a valuable alternative tool in improving patients self-controlled bowel and functions. Conflict of Interests No competing financial interests exist. Acknowledgments This study was funded by 12th National Key Technology Support Program in China (no. 2012BAI24B01). References [1] B.B.Lee,R.A.Cripps,M.Fitzharris,andP.C.Wing, Theglobal map for traumatic spinal cord injury epidemiology: update 2011, global incidence rate, Spinal Cord, pp. 1 7, [2] W. Al Taweel and A. Abdullah, Neurogenic evaluation and management after spinal cord injury: current practice among urologists working in Saudi Arabia, Urology Annals,vol. 3, no. 1, pp , [3] S.Vaidyanathan,P.Hughes,B.M.Sonietal., Occlusionofleft common iliac vein by a distended urinary in a male with paraplegia due to spinal cord injury, Spinal Cord, vol. 39, no. 7, pp , [4]J.M.Stone,M.Nino-Murcia,V.A.Wolfe,andI.Perkash, Chronic gastrointestinal problems in spinal cord injury patients: a prospective analysis, American Journal of Gastroenterology,vol.85,no.9,pp ,1990.
9 Evidence-Based Complementary and Alternative Medicine 9 [5] M. Stöhrer, B. Blok, D. Castro-Diaz et al., EAU guidelines on neurogenic lower urinary tract dysfunction, European Urology, vol.56,no.1,pp.81 88,2009. [6] A.Krassioukov,J.J.Eng,G.Claxton,B.M.Sakakibara,andS. Shum, Neurogenic bowel management after spinal cord injury: a systematic review of the evidence, Spinal Cord,vol.48,no.10, pp ,2010. [7] P.-T. Cheng, M.-K. Wong, and P.-L. Chang, A therapeutic trial of acupuncture in neurogenic of spinal cord injured patients: a preliminary report, Spinal Cord, vol.36,no.7,pp , [8] A. M. K. Wong, C. P. Leong, T. Y. Su et al., Clinical trial of acupuncture for patients with spinal cord injuries, The AmericanJournalofPhysicalMedicineandRehabilitation,vol. 82, pp , [9] H. Honjo, Y. Naya, O. Ukimura, M. Kojima, and T. Miki, Acupuncture on clinical symptoms and urodynamic measurements in spinal-cord-injured patients with detrusor hyperreflexia, Urologia Internationalis, vol.65,no.4,pp , [10] Z. Liu, K. Zhou, Y. Wang, and Y. Pan, Electroacupuncture improves voiding function inpatients with neurogenic urinary retention secondaryto caudaequina injury: results from a prospectiveobservational study, Acupuncture in Medicine, vol. 29, pp , [11] P. T. Dorsher and P. M. McIntosh, Acupuncture s effects in treating the sequelae of acute and chronic spinal cord injuries: a review of allopathic and traditional Chinese medicine literature, Evidence-Based Complementary and Alternative Medicine, vol. 2011, Article ID , 9 pages, [12] WHO Regional Office for the Western Pacific, WHO Standard Acupuncture Point Locations in the Western Pacific Region, World Health Organization, Manila, Philippines, [13] F. Biering-Sørensen, M. Craggs, M. Kennelly, E. Schick, and J.- J. Wyndaele, International lower urinary tract function basic spinal cord injury data set, Spinal Cord,vol.46,no.5,pp , [14] K. Krogh, I. Perkash, S. A. Stiens, and F. Biering-Sørensen, International bowel function basic spinal cord injury data set, Spinal Cord,vol.47,no.3,pp ,2009. [15] S. C. Kirshblum, S. P. Burns, F. Biering-Sorensen et al., International standards for neurological classification of spinal cord injury (Revised 2011), JournalofSpinalCordMedicine,vol.34, no. 6, pp , [16] K. Zhou, J. Fang, X. Wang et al., Characterization of de qi with electroacupuncture at acupoints with different properties, Journal of Alternative and Complementary Medicine,vol.17,no. 11, pp , [17] A. P. Pego, S. Kubinova, D. Cizkova et al., Regenerative medicine for the treatment of spinal cord injury:more than just promises? Journal of Cellular and Molecular Medicine, vol. 16, no. 11, pp , [18] M. T. Fitch and J. Silver, CNS injury, glial scars, and inflammation: inhibitory extracellular matrices and regeneration failure, Experimental Neurology,vol.209,no.2,pp ,2008. [19] M. Ronaghi, S. Erceg, V. Moreno-Manzano, and M. Stojkovic, Challenges of stem cell therapy for spinal cord injury: human embryonic stem cells, endogenous neural stem cells, or induced pluripotent stem cells? Stem Cells, vol. 28, no. 1, pp , [20] D. J. Weiss, G. W. Fried, M. B. Chancellor, G. J. Herbison, J. F. Ditunno Jr., and W. E. Staas Jr., Spinal cord injury and recovery, Archives of Physical Medicine and Rehabilitation,vol. 77, no. 11, pp , [21] K.-D. Sievert, B. Amend, G. Gakis et al., Early sacral neuromodulation prevents urinary incontinence after complete spinal cord injury, Annals of Neurology, vol. 67, no. 1, pp , [22] M. Vallès, A. Rodríguez, A. Borau, and F. Mearin, Effect of sacral anterior root stimulator on bowel dysfunction in patients with spinal cord injury, Diseases of the Colon and Rectum,vol. 52,no.5,pp ,2009. [23] G. H. Creasey, C. H. Ho, R. J. Triolo et al., Clinical applications of electrical stimulation after spinal cord injury, Journal of Spinal Cord Medicine,vol.27,no.4,pp ,2004. [24] M. Stohrer, M. Goepel, A. Kondo et al., The standardization of terminology in neurogenic lower urinary tract dysfunction: with suggestions for diagnostic procedures. International Continence Society Standardization Committee, Neurourology and Urodynamics,vol.18,pp ,1999. [25]J.R.Vignes,L.Bauchet,andF.Ohanna, Dorsalrhizotomy combined with anterior sacral root stimulation for neurogenic, Acta Neurochirurgica, no. 97, pp , [26] M. K. Shirvan, D. H. Alamdari, M. D. Mahboub, A. Ghanadi, H. R. Rahimi, and A. M. Seifalian, A novel cell therapy for stress urinary incontinence, short-term outcome, Neurourology and Urodynamics,vol.32,no.4,pp ,2013.
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury
 The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
Recommandations de prise en charge des vessies neurogènes EAU 2006
 Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Physiologic Anatomy and Nervous Connections of the Bladder
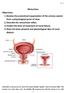 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Regulation of the Urinary Bladder Chapter 26
 Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Technologies and architectures" Stimulator, electrodes, system flexibility, reliability, security, etc."
 March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
Anorectal Diagnostic Overview
 Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
Electrostimulation Part 3: Bladder dysfunctions
 GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
GBM8320 Dispositifs Médicaux Intelligents. Electrostimulation. Part 3: Bladder dysfunctions
 GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
OHTAC Recommendation
 OHTAC Recommendation Sacral Nerve Stimulation for the Management of Urge Incontinence, Urgency-Frequency, Urinary Retention and Fecal Incontinence March 2, 2005 1 The Ontario Health Technology Advisory
OHTAC Recommendation Sacral Nerve Stimulation for the Management of Urge Incontinence, Urgency-Frequency, Urinary Retention and Fecal Incontinence March 2, 2005 1 The Ontario Health Technology Advisory
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
ORIGINAL ARTICLE Sacral anterior root stimulation improves bowel function in subjects with spinal cord injury
 (2015) 53, 297 301 & 2015 International Society All rights reserved 1362-4393/15 www.nature.com/sc ORIGINAL ARTICLE Sacral anterior root stimulation improves bowel function in subjects with spinal cord
(2015) 53, 297 301 & 2015 International Society All rights reserved 1362-4393/15 www.nature.com/sc ORIGINAL ARTICLE Sacral anterior root stimulation improves bowel function in subjects with spinal cord
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
University College Hospital at Westmoreland Street. Percutaneous Tibial Nerve Stimulation (PTNS)
 University College Hospital at Westmoreland Street Percutaneous Tibial Nerve Stimulation (PTNS) Urology Directorate If you need a large print, audio or translated copy of this document, please contact
University College Hospital at Westmoreland Street Percutaneous Tibial Nerve Stimulation (PTNS) Urology Directorate If you need a large print, audio or translated copy of this document, please contact
Spinal Cord Injury. R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH
 Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
INTERNATIONAL SPINAL CORD INJURY DATA SETS URINARY TRACT IMAGING BASIC DATA SET - COMMENTS
 1 INTERNATIONAL SPINAL CORD INJURY DATA SETS URINARY TRACT IMAGING BASIC DATA SET - COMMENTS The working-group consists of: Fin Biering-Sørensen representing the Executive Committee of The International
1 INTERNATIONAL SPINAL CORD INJURY DATA SETS URINARY TRACT IMAGING BASIC DATA SET - COMMENTS The working-group consists of: Fin Biering-Sørensen representing the Executive Committee of The International
What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction?
 London, 2016 What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction? David B. Vodušek Medical Faculty, University of Ljubljana, Slovenia vodusek.david.b@gmail.com
London, 2016 What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction? David B. Vodušek Medical Faculty, University of Ljubljana, Slovenia vodusek.david.b@gmail.com
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Research Article Acupuncture for Chronic Urinary Retention due to Spinal Cord Injury: A Systematic Review
 Evidence-Based Complementary and Alternative Medicine Volume 2016, Article ID 9245186, 9 pages http://dx.doi.org/10.1155/2016/9245186 Research Article Acupuncture for Chronic Urinary Retention due to Spinal
Evidence-Based Complementary and Alternative Medicine Volume 2016, Article ID 9245186, 9 pages http://dx.doi.org/10.1155/2016/9245186 Research Article Acupuncture for Chronic Urinary Retention due to Spinal
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
Management of Neurogenic Bowel Dysfunction. Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders
 Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
MCOMPASS ANAL MANOMETRY AN OVERVIEW
 MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW
 MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
EAU GUIDELINES ON NEURO-UROLOGY
 EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2017) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler Guidelines Associates:
EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2017) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler Guidelines Associates:
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Neuromodulation and the pudendal nerve
 Neuromodulation and the pudendal nerve Stefan De Wachter, MD, PhD, FEBU Professor of Urology University of Antwerpen, Belgium Chairman dept of Urology, UZA Disclosures Consultant speaker: Astellas, Medtronic,
Neuromodulation and the pudendal nerve Stefan De Wachter, MD, PhD, FEBU Professor of Urology University of Antwerpen, Belgium Chairman dept of Urology, UZA Disclosures Consultant speaker: Astellas, Medtronic,
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER
 SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
Chapter 23. Micturition and Renal Insufficiency
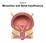 Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
SACRAL NERVE STIMULATION FOR EXPERIENCE IN CHILDREN
 SACRAL NERVE STIMULATION FOR COLORECTAL DISEASES: EXPERIENCE IN CHILDREN C. LOUIS-BORRIONE - JM. GUYS TIMONE-ENFANTS MARSEILLE SACRAL NEUROMODULATION IN CHILDREN 26 : Humphreys et al - 23 children with
SACRAL NERVE STIMULATION FOR COLORECTAL DISEASES: EXPERIENCE IN CHILDREN C. LOUIS-BORRIONE - JM. GUYS TIMONE-ENFANTS MARSEILLE SACRAL NEUROMODULATION IN CHILDREN 26 : Humphreys et al - 23 children with
Posterior Tibial Nerve Stimulation
 Posterior Tibial Nerve Stimulation Policy Number: Original Effective Date: MM.02.025 01/01/2015 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2015 Section: Medicine Place(s)
Posterior Tibial Nerve Stimulation Policy Number: Original Effective Date: MM.02.025 01/01/2015 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2015 Section: Medicine Place(s)
Dysfunctional voiding
 Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Neural control of the lower urinary tract
 Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
EAU GUIDELINES ON NEURO-UROLOGY
 EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2016) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler. Guidelines Associates:
EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2016) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler. Guidelines Associates:
Paediatric Urotherapy Training
 Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Application of Anorectal Dynamics in the Treatment of Colon Disease Packing
 Application of Anorectal Dynamics in the Treatment of Colon Disease Packing Zongyue Gao 1, 2, a, Yuyan Liu 1, 2, b, Chunxia Wan 1, 2, c 3, d* and Xiaoli Zhou 1 Henan Province Hospital of TCM, 450000, Henan,
Application of Anorectal Dynamics in the Treatment of Colon Disease Packing Zongyue Gao 1, 2, a, Yuyan Liu 1, 2, b, Chunxia Wan 1, 2, c 3, d* and Xiaoli Zhou 1 Henan Province Hospital of TCM, 450000, Henan,
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Research Article Deqi Sensations of Transcutaneous Electrical Nerve Stimulation on Auricular Points
 Evidence-Based Complementary and Alternative Medicine Volume 213, Article ID 371543, 5 pages http://dx.doi.org/1.1155/213/371543 Research Article Deqi Sensations of Transcutaneous Electrical Nerve Stimulation
Evidence-Based Complementary and Alternative Medicine Volume 213, Article ID 371543, 5 pages http://dx.doi.org/1.1155/213/371543 Research Article Deqi Sensations of Transcutaneous Electrical Nerve Stimulation
Elimination Patterns: Bladder
 Elimination Patterns: Bladder CRRN Review Material Christa Carter, RN, BSN, CRRN Objectives Identify different types of neurogenic bladder Identify different types of incontinence Identify at least three
Elimination Patterns: Bladder CRRN Review Material Christa Carter, RN, BSN, CRRN Objectives Identify different types of neurogenic bladder Identify different types of incontinence Identify at least three
Updates in the nonpharmacological. treatment on overactive bladder
 Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
Human Anatomy. Autonomic Nervous System
 Human Anatomy Autonomic Nervous System 1 Autonomic Nervous System ANS complex system of nerves controls involuntary actions. Works with the somatic nervous system (SNS) regulates body organs maintains
Human Anatomy Autonomic Nervous System 1 Autonomic Nervous System ANS complex system of nerves controls involuntary actions. Works with the somatic nervous system (SNS) regulates body organs maintains
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? How does the implant work?
 information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National
 Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National What is Bowel and Bladder Dysfunction? Lower urinary tract symptoms (LUTS) and bowel movement disorders Majority
Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National What is Bowel and Bladder Dysfunction? Lower urinary tract symptoms (LUTS) and bowel movement disorders Majority
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
Neural Control of Lower Urinary Tract Function. William C. de Groat University of Pittsburgh Medical School
 Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive Bladder
 Advances in Urology Volume 2009, Article ID 328364, 4 pages doi:10.1155/2009/328364 Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive
Advances in Urology Volume 2009, Article ID 328364, 4 pages doi:10.1155/2009/328364 Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive
Neural control of the lower urinary tract in health and disease
 Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Disclosures. Background. Expanding the Xiao Concept to Spina Bifida
 Lumbar to Sacral Nerve Rerouting to Restore Voiding and Bowel Function in Spina Bifida Kenneth M. Peters, MD Professor and Chairman of Urology Oakland University William Beaumont School of Medicine Royal
Lumbar to Sacral Nerve Rerouting to Restore Voiding and Bowel Function in Spina Bifida Kenneth M. Peters, MD Professor and Chairman of Urology Oakland University William Beaumont School of Medicine Royal
Fecal Incontinence. Inability to retain feces or bowel movements, resulting in involuntary passage of feces or bowel movements
 Fecal Incontinence (Involuntary Passage of Feces or Bowel Movements) Basics OVERVIEW Inability to retain feces or bowel movements, resulting in involuntary passage of feces or bowel movements GENETICS
Fecal Incontinence (Involuntary Passage of Feces or Bowel Movements) Basics OVERVIEW Inability to retain feces or bowel movements, resulting in involuntary passage of feces or bowel movements GENETICS
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
15. Prevention of UTI and lifestyle modifications
 15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
Complications Audit of Urological Issues in Spinal Cord Injury Evaluation Study (CAUSES)
 Complications Audit of Urological Issues in Spinal Cord Injury Evaluation Study (CAUSES) Dr Andrew Nunn Ms Melinda Millard Ms Janette Alexander Ms Louise MacLellan Ms Catherine Byrne 23 rd September 2015
Complications Audit of Urological Issues in Spinal Cord Injury Evaluation Study (CAUSES) Dr Andrew Nunn Ms Melinda Millard Ms Janette Alexander Ms Louise MacLellan Ms Catherine Byrne 23 rd September 2015
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Objectives. Key Outlines:
 Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
ParasymPathetic Nervous system. Done by : Zaid Al-Ghnaneem
 ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
Corporate Medical Policy
 Corporate Medical Policy Percutaneous Tibial Nerve Stimulation for Voiding Dysfunction File Name: Origination: Last CAP Review: Next CAP Review: Last Review: percutaneous_tibial_nerve_stimulation_for_voiding_dysfunction
Corporate Medical Policy Percutaneous Tibial Nerve Stimulation for Voiding Dysfunction File Name: Origination: Last CAP Review: Next CAP Review: Last Review: percutaneous_tibial_nerve_stimulation_for_voiding_dysfunction
We have heard a great deal about "overactive" bladder recently. But what
 BLADDER DYSFUNCTION Differential Diagnosis and Treatment of Impaired Bladder Emptying Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh School of Medicine,
BLADDER DYSFUNCTION Differential Diagnosis and Treatment of Impaired Bladder Emptying Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh School of Medicine,
The Effect ofverapamil on the Treatment of Detrusor Hyperreflexia in the Spinal Cord Injured Population
 Paraplegia 27 (1989) 364-369 0031-1758/89/0027-0364$10.00 ([j 1989 International Medical Society of Paraplegia The Effect ofverapamil on the Treatment of Detrusor Hyperreflexia in the Spinal Cord Injured
Paraplegia 27 (1989) 364-369 0031-1758/89/0027-0364$10.00 ([j 1989 International Medical Society of Paraplegia The Effect ofverapamil on the Treatment of Detrusor Hyperreflexia in the Spinal Cord Injured
What should we consider before surgery? BPH with bladder dysfunction. Inje University Sanggye Paik Hospital Sung Luck Hee
 What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
How to manage a patient with bladder dysfunction
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 13 How to manage a patient with autonomic dysfunction - Level 2 How to manage a patient with
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 13 How to manage a patient with autonomic dysfunction - Level 2 How to manage a patient with
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Bladder Management. A guide for patients. Key points
 Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET (version 2.0)
 1 INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET (version 2.0) The first version of the International Spinal Cord Injury Lower Urinary Tract Function Basic Data Set (Biering-Sørensen
1 INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET (version 2.0) The first version of the International Spinal Cord Injury Lower Urinary Tract Function Basic Data Set (Biering-Sørensen
Accidental Bowel Leakage (Fecal Incontinence)
 Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Sacral Nerve Neuromodulation / Stimulation
 Sacral Nerve Neuromodulation / Stimulation Policy Number: 7.01.69 Last Review: 2/2018 Origination: 2/2001 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Sacral Nerve Neuromodulation / Stimulation Policy Number: 7.01.69 Last Review: 2/2018 Origination: 2/2001 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Continence Promotion in
 Everybody s Business- Continence Promotion in Aged Care Melissa O Grady Clinical Nurse Consultant Continence Warning Some graphic images are contained in this presentation Objectives What is Old Age? What
Everybody s Business- Continence Promotion in Aged Care Melissa O Grady Clinical Nurse Consultant Continence Warning Some graphic images are contained in this presentation Objectives What is Old Age? What
Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E.
 UvA-DARE (Digital Academic Repository) Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E. Link to publication Citation for published version (APA): Puspitoayu,
UvA-DARE (Digital Academic Repository) Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E. Link to publication Citation for published version (APA): Puspitoayu,
Bowel and Bladder Management Following Transverse Myeli5s
 Bowel and Bladder Management Following Transverse Myeli5s Janet Dean, MS, RN, CRRN, CRNP Pediatric Nurse Prac55oner Interna5onal Center for Spinal Cord Injury Department of Physical Medicine and Rehabilita5on
Bowel and Bladder Management Following Transverse Myeli5s Janet Dean, MS, RN, CRRN, CRNP Pediatric Nurse Prac55oner Interna5onal Center for Spinal Cord Injury Department of Physical Medicine and Rehabilita5on
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Sacral Nerve Neuromodulation/Stimulation for Pelvic Floor Dysfunction
 Medical Policy Manual Surgery, Policy No. 134 Sacral Nerve Neuromodulation/Stimulation for Pelvic Floor Dysfunction Next Review: December 2018 Last Review: June 2018 Effective: July 1, 2018 IMPORTANT REMINDER
Medical Policy Manual Surgery, Policy No. 134 Sacral Nerve Neuromodulation/Stimulation for Pelvic Floor Dysfunction Next Review: December 2018 Last Review: June 2018 Effective: July 1, 2018 IMPORTANT REMINDER
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Urinary Bladder. Prof. Imran Qureshi
 Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
3/3/2016. International Standards for the Neurologic Classification of Spinal Cord Injury (ISNCSCI)
 International Standards for the Neurologic Classification of Spinal Cord Injury (ISNCSCI) American Spinal Injury Association International Spinal Cord Society Presented by Adam Stein, MD Chairman and Professor
International Standards for the Neurologic Classification of Spinal Cord Injury (ISNCSCI) American Spinal Injury Association International Spinal Cord Society Presented by Adam Stein, MD Chairman and Professor
Pelvic Floor Therapy for the Oncology Patient
 Therapy for the Oncology Patient CARINA SIRACUSA, PT, DPT, WCS OHIOHEALTH PELVIC FLOOR PHYSICAL THERAPIST ONCOLOGY REHABILITATION PROGRAM COORDINATOR What does a pelvic floor therapist treat? Muscles Muscles
Therapy for the Oncology Patient CARINA SIRACUSA, PT, DPT, WCS OHIOHEALTH PELVIC FLOOR PHYSICAL THERAPIST ONCOLOGY REHABILITATION PROGRAM COORDINATOR What does a pelvic floor therapist treat? Muscles Muscles
Physiology and Management of Bladder and Bowel Continence following Spinal Cord Injury
 STUDENT FEATURE Physiology and Management of Bladder and Bowel Continence following Spinal Cord Injury Kathleen Francis, RN, MSN Patients with spinal cord injury commonly develop bladder and bowel symptoms
STUDENT FEATURE Physiology and Management of Bladder and Bowel Continence following Spinal Cord Injury Kathleen Francis, RN, MSN Patients with spinal cord injury commonly develop bladder and bowel symptoms
Incontinence; Lets talk about it. Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery
 Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
