Urinary Retention in Women
|
|
|
- Roxanne Campbell
- 6 years ago
- Views:
Transcription
1 REVIEW Urinary Retention in Women 1 2 K. Stamatiou, M. Elnagar 1 Urology Department, Tzaneio, General Hospital. Piraeus, Greece, 2 Gynecology Department, Hera General Hospital, Makkah, Saudi Arabia Corresponding Author: Dr. Konstantinos Stamatiou 2, Salepoula street Piraeus, PC 18536, Greece stamatiouk@gmail.com Tel: Summary The pathophysiology and epidemiology of urinary retention in women is not well documented. According to the current knowledge the aetiology of this condition appears to be multifactorial. Implicating factors vary and often coexist. They are mainly distinguished in infective, neoplastic, pharmacological, neurological, anatomical, myopathic, functional and psychogenic. Initial management includes bladder drainage if urinary retention is acute or if it is chronic accompanied by obstructive uropathy, infection or pain. Investigations should be initially focused on identifying actual complications and secondly the underlying aetiology. Keywords Urinary retention, womenintroduction Urinary retention (UR) is defined as the inability to achieve full bladder drainage by voluntary micturition and is classified into acute (complete inability to drain) and chronic (incomplete with post-void residual volume). The clinical features of Acute Urinary Retention (AUR) are clearly contrary to those of Chronic Urinary Retention (CUR). Moreover, the absence of a well-defined normal range for the clinical post-void residual volume, the diagnostic setting (ultrasound) and the bladder capacity 1 differentiations make CUR difficult to identify. While UR commonly affects men and especially in older ages, it is relatively unusual in women. In fact, the epidemiology of female UR is not welldocumented and its pathophysiology remains unclarified. Indeed, for male patients and especially the elderly, UR is mainly caused by Bladder Outlet Obstruction (BOO) induced by Prostatic 2 Hyperplasia (PH). Women on the contrary, especially in older ages, present a number o various pathological conditions that may contribute to the development of UR such as decreased bladder contractility, poorly sustained detrusor contraction, lack of adequate anatomical outlet or neurological disorder impairing the coordination of the urination process. Thusly, a considerable rate of older women present cysteoscopic findings of urinary obstruction like trabeculitis and bladder diverticulitis nonaccompanied by a considerable amount of post-void residual volume; a smaller rate of patients manifest post-void residual volume non-accompanied by obstructive indications. In particular, the presence of a clear anatomical impediment does not constitute a common finding though obstruction symptoms, such as poor or intermittent urinary flow, terminal dribbling or post-micturition dribbling, are comm- 24 Hellenic UROLOGY
2 Urinary Retention in Women only reported by female patients with UR. Materials and Methods Studies published in 1980 onwards were examined via search on MEDLINE, National Library of Medicine and Iatrotek databases. Our initial keywords were: urine retention, woman in combination with: epidemiology, risk factor, treatment. The references in the selected articles were investigated for publications not included in the initial search on the databases. Results 1. Epidemiological data The impact of female UR is not well-documented and most information comes from a small case 3 series or case reports. Indicatively and for AUR only, Klarskov et al. conducted a very small prospective study and estimated the annual impact at 7/ whereas its ratio compared to male AUR 4 was estimated at 1:13. García-Fadrique et al. performed a urodynamic study on 202 female subjects exhibiting AUR. Only 28.7% reported uri - nation disorders; the rest 71.3 % had no symptoms. However, only 31.7% had normal urodynamic fin - dings contrary to 32.2% exhibiting decreased detru - sor contractility. Complete absence of detrusor con - tractility was manifested in 18.3%, BOO in 10.4% and decreased pelvic floor relaxation in 7.4% of the cases. Notably, in almost half of all-cause cases (52.4%), normal urination was completely restored 5 and no treatment plan was applied. The retention was finally attributed to neurological causes in 37.1% (10.9% of which was associated to diabetes mellitus), gynecological causes in 9.4% and uro - logical causes in 7.9%. 22.8% of the cases sustained a mixed aetiology and in the rest 22.8% no cause 5 was determined. A respective ratio of neurological and non-urological UR is examined in another small study but a considerable rate of the latter was 6 attributed to psychological causes. Interestingly, studies before , when Fowler's syndrome was established, regard urethral and bladder cervix deformities as the main causes of female UR. On the contrary, younger females encounter Fowler's syndrome. For approximately one third of the cases, 7 the cause remains undetected. 2. Aetiology 2.1 Neurological causes Neurogenic lower urinary tract dysfunction (NLUTD) is exhibited in individuals with neurological diseases (Cerebral Vascular Accident-CVA, Parkinson disease, Multiple Sclerosis-MS), lumbar injuries and peripheral neuropathies (like diabetes mellitus and tabes dorsalis). Other conditions associated with NLUTD are spinal lesions (congenital like spina bifida and secondary like cervical myelopathy and lumbar disk herniation) as well as some neoplasms of the Central Nervous System (CNS) (primary or metastatic). Regional anaesthesia and major surgical procedures on the pelvis are also related to NLUTD yet, they can also be classified as iatro- 8 genic. The most common neurological problems associated with female UR are MS, lumbar injury and Hellenic UROLOGY 25
3 K. Stamatiou, M. Elnagar 6 diabetes mellitus. However, the exact rate of MS (and Parkinson's disease) inducing UR cannot be precisely defined given that the onset of symptoms in the urinary tract may precede for a mean period of 5 years prior to the disease diagnosis and 2 years prior to the encounter of more specific neurological 9 symptoms. In addition, certain patients, apart from the detrusor hyperreflexia, are referred with a significant post-micturition residual which is usually 10 disregarded. The mechanism of NLUTD in patients identified with Parkinson's disease or MS has not been fully elucidated. Nevertheless, basal ganglia lesions and neurons demyelination realized in these conditions, possibly affect the CNS at several different locations important for the bladder control. This explains the variety of manifestations in the urinary tract system and their early onset. For example, the detrusor hyperreflexia is attributed to cell loss in the brainstem region, whereas incomplete bladder voiding is due to cell atrophy of the 11 Intermediolateral Nucleus (IML). Furthermore, cell loss in the anterior horn in Onuf's nucleus causes 12 urethral sphincter dysfunction. Consequently, it is possible for the patient to present a combination of bladder hyperactivity and sphincter deficiency along with incomplete voiding. In Parkinsonism, outflow obstruction may also be manifested due to impaired relaxation or bradykinaesia of the urethral 13 sphincter ; dopaminergeric medication is also responsible for directly impacting the detrusor 14 muscle. Likewise, in diabetes mellitus, the mechanism of urethrovesical dysfunction is not clearly understood. However, peripheral neuropathy, changes in the Autonomic Nervous System (ANS) receptors, change in the micturition reflex at the sacral neurotomes of the spinal cord and detrusor muscle injury have been identified. Main neuropathic changes include nerve loss, axon degeneration and gradual demyelination. These changes are induced by Schwann cell metabolic disorders and changes resulting from chronic glucohemia. Early signs include increased water intake followed by increased micturition frequency and urine volume and are accompanied by detrusor overactivity (DO) (early urodynamic finding). Given the gradual decrease in the bladder's sensation, the progressive decrease in frequency follows together with a parallel increase in the urine volume. The combination of these two along with the decrease in the bladder's contractility encountered much later, cause incomplete bladder outflow and UR. Symptoms commonly appear ten years after the 15 onset of diabetes mellitus. In a large pool of females with UR, none of the aforementioned causes is detected. However, they exhibit detrusor hyperactivity with impaired contractility (DHIC). Some investigators attribute these 15 cases to age-related changes. The same females - especially the elderly whom symptoms at the LUT are more often - do not exhibit CUR frequently. Valentini et al. performed a urodynamic study on 100 symptomatic female subjects aged years and found an impact of 15%. Notably, the population study exhibited all-cause detrusor hypoflexia 16 significantly rarely compared to hyperflexia. 26 Hellenic UROLOGY
4 Urinary Retention in Women 2.2 Psychogenic causes UR may occur single or concomitant to micturition difficulty and perineal pain in terms of somatoform 17 disorders. These mental disorders are exhibited as somatoform disorders. Their main characteristic is the presence of physical symptoms that can neither be fully explained on the basis of a disease nor can they be interpreted as a substance's action or even be attributed to some other form of mental disorder (eg panic attack). Contrary to the factitious disorders 17 and faking, physical symptoms are not intentional. Psychosocial problems may contribute to urinary retention, single or concomitant to some diseases (e.g. urinary tract infection-uti). To a great extent, demonstration of UR is associated with a previous incident such as a spouse argument, the death of a 6 loved one etc. 2.3 Medication Prospective studies data suggest that up to 10% of AUR cases can be attributed to use of medication. Occasionally, UR has been reported following the intake of anticholinergic medication (eg antipsychotics, antidepressants and respiratory anticholinergic agents) and after the intake of opioids and other anaesthetics, benzodiazepines, alpha adrenergic receptors, nonsteroidal antiinflammatory analgesics (NSAIA), muscle 18 relaxants and calcium channel blockers (CCB). It is not clear whether the aforementioned medication causes the UR and the conditions for CUR, single or concomitant to the presence of another agent. However, bladder is susceptible to side-effects of medication like antidepressants, opioids, antipsychotics, antimuskarins and alpha adrenergic receptors, due to the complex neurological control and the frequent excretion of the metabolites of this medication via urine. A further trial suggests the following: CUR is rarely caused by antidepressants as it shown in case reports available in literature. Though this type of medication has many pharmacological actions, its exact role in the urinary tract is not fully known, however, it is supposed to have an alpha-adrenergic action on the smooth muscles of the urethra and thusly it increases the 18 outflow resistance via the urethra. Indeed, the bladder neck and the proximal urethra have alpha adrenergic receptors, which when stimulated, cause smooth muscle fibers contraction. Tricyclic antidepressants (TCAs) like imipramine and doxepin increase urethral resistance but may decrease bladder contractility. It is still under investigation whether UR develops when some other pathological condition acts as a background or whether antidepressants impair detrusor contractility in the long-term. In this case, retention is chronic and possibly realized in various stages associated with serotonin reuptake. The following are indications of the above: 1) long-standing antidepressants administration leads to a decrease 19 in 5-HT2 receptors' number and sensitivity, 2) serotonergic neurons engage in controlling the 12 lower urinary tract, 3) older (tricyclic) as well as recent (selective serotonin reuptake inhibitors SSRI) antidepressants have been associated with 20 UR insidents and 4) norepinephrine reuptake Hellenic UROLOGY 27
5 K. Stamatiou, M. Elnagar inhibitors (NRI) (thionisoxetine) do not affect bladder capacity or sphincter activity. Yet, the fact that in all cases recorded micturition was restored upon medication interruption limits the above possibility. Anticholinergic drugs have occasionally been 22 associated with AUR. A randomized, placebocontrolled study investigated, among others, the safety of the antimuscarinic agent oxybutynin, in 65 aged female subjects with intellectual disability (ID) suffering from urge urinary incontinence (UUI). Only one patient (1.5%) complained of UR, which 23 resolved without treatment. This medication competes the muscarinic acetylcholine receptors effect and does not induce Ca2+ release and consequent muscle contraction at the detrusor. It is not established whether detrusor contractility becomes resistant to medication over time, however, the observed URs are more likely to develop due to another condition. The case of increased urethral resistance and/or obstruction is possibly not included in them. Actually, in another randomized controlled trial comparing antimuscarinic tolterodine to tamsulosin, an alpha1 adrenoceptor blocking agent for the treatment of male subjects with lower urinary tract symptoms (LUTS) and overactive bladder (OAB), did not reveal statistically significant differences in the development frequency of UR (tolterodine & tamsulosin 0.4%, tolterodine 0.5%, tamsulosin 0% and placebo 0%). In addition, the development of UR was similar for both men with small and men with 24 large cell prostate cancer. Interestingly, a retrospective study by Roehrborn et al. revealed that the relative risk for AUR in patients receiving antimuscarinics dose independent was higher during the early treatment (first 30 days) and in patients with genitourinary system conditions. This shows that in fact, URs do develop caused by 25 another pathological mechanism. In most cases though, micturition resolves upon medication interruption and this implicates antimuscarinics to a 26 great extent. Opioids have been associated with UR in case reports and in clinical trials. In their majority, opioids were administered for operative analgesia. The post-operative UR impact was estimated at 5% whereas predisposing factors were diabetes mellitus, intraoperative atropine administration and 27 prolonged hospitalization. Given that UR patients sustain more than one risk factors, the exact impact of opioids on UR is hard to be assessed but is 27, 28 estimated between 3.8 and 18.1%. Nonetheless, Panicke et al. found that a high percentage (39%) of females manifesting all-cause URs had been 29 administered opioids the previous period. The mechanism is yet unknown and their urinary tract impact is not fully apprehended. Based on up to date knowledge, it seems that they reduce detrusor tone, contraction strength, sense of fullness and at the same time suspend micturiotion reflex. They do 30 not however increase sphincter tone. Experimental studies have found that these effects, irreversible when naloxone is administered, are realized centrally in the brain and the spinal cord with 31 recorded peripheral impacts on the bladder. Rosow et al. proved that some of the above changes 28 Hellenic UROLOGY
6 Urinary Retention in Women in the bladder activity are partially induced by opioids' peripheral action that can be reversed by methylnaltrexone, a peripherally-acting ì-opioid receptor antagonist. Post-operative UR surgery independent is more likely to develop following epidural morphine and less likely after intravenous 32 or intramuscular administration. Prolonged peripheral nerve blockade (PNB) shows the smallest frequency of post-operative UR (15.8); epidural 33 anaelgesia shows the highest (48.1%). Generally, UR resolves spontaneously hours after uri- 34 nary catheterization removal Anatomical causes Pure urethral obstructions have been established in females exhibiting UR. Though their mechanism is shared, these vary according to aetiology and origin. The most common cause is primary bladder neck obstruction (PBNO) identified in 9-16% of females with obstructive micturition. Malignant neoplasias in the female reproductive system, colon and bladder as well as benign bladder neck masses 35, 36 induce BOO. Female neoplasia-induced UR frequency is not known but is estimated to less than 5 10% of the total. Anterior vaginal wall or uterus prolapse-induced UR frequency is not reported. In the first case, possible bladder neck displacement causes dysouria and incomplete bladder voiding whereas the second may induce acute as well as 37 chronic UR. UR induced by gallstones, female bladder anatomical anomalies and haematocolpos is likewise unsual. 2.5 Surgical procedures Vaginal vault suspension may lead to overcorrection as well as to urethral compression or deformation especially when one of the sutures is placed close to the urethra. Dysuria develops commonly; UR is very rare. Symptoms may last for up to a month. The Marshall-Marchetti-Krantz technique produced 42 higher rates of overcorrection and UR. In less than 10% of the cases, dysfunctional micturition and UR are observed in the initial post-operative period for the restoration of stress urinary incontinence (SUI) by applying tension-free vaginal tapes (TVT). That said, AUR is quite uncommon and complete bladder voiding usually resolves quickly (median period 9 43 days). In these cases, the technique is not as much implicated as in anaesthesia, discomfort, localized oedema, haematoma formation and outlet realignment procedure. Overcorrection is mainly implicated when AUR is observed or when symptoms and post-void residual volume remission 42 do not resolve within a month. Augmentation cystoplasties (AC) aim to increase bladder capacity by reducing bladder contractions during filling but they affect bladder contraction and so, some patients present with a considerable post- 43 void residual volume and may manifest UR. Intravesical botulinum toxin (BT) injection for the treatment of OAB bears a significant risk of UR which 44 increases by repetition of injections. 2.6 Fowler's syndrome Fowler's syndrome is defined as UR with large postvoid residual volume in young females following menarche. It is detected in UTI screening tests or it Hellenic UROLOGY 29
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Disclosures. Geriatric Incontinence and Voiding Dysfunction. Agenda. Agenda. UI: a Geriatric Syndrome. Geriatric Syndromes 9/7/2018.
 Disclosures Geriatric Incontinence and Voiding Dysfunction None Shachi Tyagi MD, MS Assistant Professor Division of Geriatric Medicine University of Pittsburgh Medical Center UI: a Geriatric Syndrome Geriatric
Disclosures Geriatric Incontinence and Voiding Dysfunction None Shachi Tyagi MD, MS Assistant Professor Division of Geriatric Medicine University of Pittsburgh Medical Center UI: a Geriatric Syndrome Geriatric
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Voiding Dysfunction Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU.
 Voiding Dysfunction 2009 Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU. Objectives Understand and explain physiologic function and dysfunction of lower urinary tract.
Voiding Dysfunction 2009 Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU. Objectives Understand and explain physiologic function and dysfunction of lower urinary tract.
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
INCONTINENCE What can Wee do about it?
 Prevalence INCONTINENCE What can Wee do about it? High risk groups Myths Aetiology Assessment-History Assessment-Drugs Assessment- Examination & Tests INCONTINENCE What can wee do about it? Treatment-First
Prevalence INCONTINENCE What can Wee do about it? High risk groups Myths Aetiology Assessment-History Assessment-Drugs Assessment- Examination & Tests INCONTINENCE What can wee do about it? Treatment-First
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Dr Jonathan Evans Paediatric Nephrologist
 How do I manage a patient with intractable daytime wetting: Dr Jonathan Evans Paediatric Nephrologist Of 107 children aged 11-12 with day-wetting 91 (85%) were dry at 15-16 yr Swithinbank et al BJU 1998
How do I manage a patient with intractable daytime wetting: Dr Jonathan Evans Paediatric Nephrologist Of 107 children aged 11-12 with day-wetting 91 (85%) were dry at 15-16 yr Swithinbank et al BJU 1998
Table 1. International Consultation on Incontinence recommendations for frail older adults
 Table 1. International Consultation on Incontinence recommendations for frail older adults Clinicians need to assess and manage co-existing co morbid conditions which are known to have an impact on continence
Table 1. International Consultation on Incontinence recommendations for frail older adults Clinicians need to assess and manage co-existing co morbid conditions which are known to have an impact on continence
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
NON-Neurogenic Chronic Urinary Retention AUA White Paper
 NON-Neurogenic Chronic Urinary Retention AUA White Paper Great Lakes SUNA Inside Urology March 16, 2018 Michelle J. Lajiness FNP-BC Nurse Practitioner DMC Urology Incidence Really unknown Lack consensus
NON-Neurogenic Chronic Urinary Retention AUA White Paper Great Lakes SUNA Inside Urology March 16, 2018 Michelle J. Lajiness FNP-BC Nurse Practitioner DMC Urology Incidence Really unknown Lack consensus
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Urinary incontinence (UI) affects as many
 EXPLORING NEW HORIZONS IN STRESS INCONTINENCE: THE NEUROUROLOGY CONNECTION W. Glenn Hurt, MD* ABSTRACT As many as one-third of women are affected by urinary incontinence, the most common of which being
EXPLORING NEW HORIZONS IN STRESS INCONTINENCE: THE NEUROUROLOGY CONNECTION W. Glenn Hurt, MD* ABSTRACT As many as one-third of women are affected by urinary incontinence, the most common of which being
URGE MOTOR INCONTINENCE
 URGE MOTOR INCONTINENCE URGE INCONTINENCE COMMONEST TYPE IN ELDERLY WOMEN Causes: 1 - Defects in CNS regulation Stroke Parkinson s disease Dementia (Alzheimer s and other types) Normopressure hydrocephalus
URGE MOTOR INCONTINENCE URGE INCONTINENCE COMMONEST TYPE IN ELDERLY WOMEN Causes: 1 - Defects in CNS regulation Stroke Parkinson s disease Dementia (Alzheimer s and other types) Normopressure hydrocephalus
Recommandations de prise en charge des vessies neurogènes EAU 2006
 Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Alpha antagonists from initial concept to routine clinical practice
 european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
Neurourology, especially the video urodynamic
 NEUROUROLOGIC FINDINGS WITH APPLICABILITY TO INCONTINENCE AND URETHRAL FUNCTION * Edward J. McGuire, MD ABSTRACT Neurourology is applicable to urinary incontinence and obstructive uropathy in the general
NEUROUROLOGIC FINDINGS WITH APPLICABILITY TO INCONTINENCE AND URETHRAL FUNCTION * Edward J. McGuire, MD ABSTRACT Neurourology is applicable to urinary incontinence and obstructive uropathy in the general
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
April Clinical Focus Topic URINARY FREQUENCY
 April Clinical Focus Topic URINARY FREQUENCY This month I am focusing on a topic that may seem a little boring. But I would like to look at it from a less common perspective.urinary Frequency and its relationship
April Clinical Focus Topic URINARY FREQUENCY This month I am focusing on a topic that may seem a little boring. But I would like to look at it from a less common perspective.urinary Frequency and its relationship
Incontinence. When I was given this topic in urology to discuss with you today I
 Incontinence When I was given this topic in urology to discuss with you today I was slightly disappointed. I personally see mostly men for problems such as stones, benign prostatic hyperplasia, prostate
Incontinence When I was given this topic in urology to discuss with you today I was slightly disappointed. I personally see mostly men for problems such as stones, benign prostatic hyperplasia, prostate
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies. Dr. Boris Friedman May 2, 2012 OBJECTIVES
 Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies Dr. Boris Friedman May 2, 2012 OBJECTIVES 1) Definition and classification of MS 2) Interventional radiology
Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies Dr. Boris Friedman May 2, 2012 OBJECTIVES 1) Definition and classification of MS 2) Interventional radiology
POSTOPERATIVE URINARY RETENTION IN ABDOMINAL SURGERY. Marta Alves Servicio de Urología
 POSTOPERATIVE URINARY RETENTION IN ABDOMINAL SURGERY Marta Alves Servicio de Urología Introduction Incidence Mechanism of micturition Risk factors Prevention Diagnosis Complications/Adverse effects associated
POSTOPERATIVE URINARY RETENTION IN ABDOMINAL SURGERY Marta Alves Servicio de Urología Introduction Incidence Mechanism of micturition Risk factors Prevention Diagnosis Complications/Adverse effects associated
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Parkinson s Disease and Multiple System Atrophy
 Parkinson s Disease and Multiple System Atrophy Jalesh N. Panicker MD, FRCP Department of Uro-Neurology National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen Square, London
Parkinson s Disease and Multiple System Atrophy Jalesh N. Panicker MD, FRCP Department of Uro-Neurology National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen Square, London
Guidelines on Urinary Incontinence
 Guidelines on Urinary Incontinence J. Thüroff (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck European Association of Urology 2006 TABLE OF CONTENTS
Guidelines on Urinary Incontinence J. Thüroff (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck European Association of Urology 2006 TABLE OF CONTENTS
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
NEUROPATHIC BLADDER DISORDERS
 NEUROPATHIC BLADDER DISORDERS ANATOMY & PHYSIOLOGY The Bladder Unit The functional features of the bladder include (1) a normal capacity of 400 500 ml, (2) a sensation of fullness, (3) the ability to accommodate
NEUROPATHIC BLADDER DISORDERS ANATOMY & PHYSIOLOGY The Bladder Unit The functional features of the bladder include (1) a normal capacity of 400 500 ml, (2) a sensation of fullness, (3) the ability to accommodate
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
What should we consider before surgery? BPH with bladder dysfunction. Inje University Sanggye Paik Hospital Sung Luck Hee
 What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
Urogynecology ICD-9 to ICD-10 Crosswalks
 1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
We have heard a great deal about "overactive" bladder recently. But what
 BLADDER DYSFUNCTION Differential Diagnosis and Treatment of Impaired Bladder Emptying Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh School of Medicine,
BLADDER DYSFUNCTION Differential Diagnosis and Treatment of Impaired Bladder Emptying Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh School of Medicine,
Spinal Cord Injury. R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH
 Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline.
 Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT
 UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT Yunizaf, MD Division of Urogynecology Department of Obstetrics and Gynecology School of Medicine, University of Indonesia/ Dr. Cipto Mangunkusumo Hospital
UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT Yunizaf, MD Division of Urogynecology Department of Obstetrics and Gynecology School of Medicine, University of Indonesia/ Dr. Cipto Mangunkusumo Hospital
Bladder Dysfunction in Multiple Sclerosis. by Nancy J. Holland, EdD, RN and Nancy C. Reitman, MA, RN
 Clinical Bulletin Information for Health Professionals Bladder Dysfunction in Multiple Sclerosis by Nancy J. Holland, EdD, RN and Nancy C. Reitman, MA, RN Effective bladder management strategies make it
Clinical Bulletin Information for Health Professionals Bladder Dysfunction in Multiple Sclerosis by Nancy J. Holland, EdD, RN and Nancy C. Reitman, MA, RN Effective bladder management strategies make it
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Video-urodynamics. P J R Shah Institute of Urology and UCH
 Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence
 Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY
 PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
Policy for Prostatism/Lower Urinary Tract Symptoms in men
 NHS Halton Clinical Commissioning Group NHS Liverpool Clinical Commissioning Group NHS St Helens Clinical Commissioning Group NHS South Sefton Clinical Commissioning Group NHS Southport and Formby Clinical
NHS Halton Clinical Commissioning Group NHS Liverpool Clinical Commissioning Group NHS St Helens Clinical Commissioning Group NHS South Sefton Clinical Commissioning Group NHS Southport and Formby Clinical
Management of Urinary Incontinence in Older Women. Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital
 Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Urine a Mess: Micturition Disorders Joe Bartges, DVM, PhD, DACVIM, DACVN Cornell University Veterinary Specialists Stamford, CT
 Urine a Mess: Micturition Disorders Joe Bartges, DVM, PhD, DACVIM, DACVN Cornell University Veterinary Specialists Stamford, CT 1. Micturition refers to the process of storing and periodically voiding
Urine a Mess: Micturition Disorders Joe Bartges, DVM, PhD, DACVIM, DACVN Cornell University Veterinary Specialists Stamford, CT 1. Micturition refers to the process of storing and periodically voiding
Neural control of the lower urinary tract
 Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Morphine causing urinary retention
 Morphine causing urinary retention Search 27-2-2018. Postoperative Urinary Retention: causing severe complications. Bonnet F: Spinal clonidine produces less urinary retention than spinal morphine. 1-3-2008
Morphine causing urinary retention Search 27-2-2018. Postoperative Urinary Retention: causing severe complications. Bonnet F: Spinal clonidine produces less urinary retention than spinal morphine. 1-3-2008
Causes of Transient Incontinence. Geriatrics: Urinary Incontinence, Dementia, and Delirium. Classification of Established Incontinence
 Causes of Transient Geriatrics: Urinary, Dementia, and Delirium Carla Zeilmann, PharmD, BCPS St. Louis College of Pharmacy Therapeutics 3 Fall 2003 D delirium I infection A atrophic urethritis and vaginitis
Causes of Transient Geriatrics: Urinary, Dementia, and Delirium Carla Zeilmann, PharmD, BCPS St. Louis College of Pharmacy Therapeutics 3 Fall 2003 D delirium I infection A atrophic urethritis and vaginitis
Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach)
 Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach) Andrew Combs, PA-C Director, Pediatric Urodynamics Division of Pediatric Urology New York Presbyterian-Weill Cornell
Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach) Andrew Combs, PA-C Director, Pediatric Urodynamics Division of Pediatric Urology New York Presbyterian-Weill Cornell
Neural control of the lower urinary tract in health and disease
 Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
THE vesical dysfunction which follows injury or disease of the spinal cord
 VESICAL NECK RESECTION FOR NEUROGENIC BLADDER WILLIAM J. ENGEL, M.D. Department of Urology THE vesical dysfunction which follows injury or disease of the spinal cord or cauda equina has always presented
VESICAL NECK RESECTION FOR NEUROGENIC BLADDER WILLIAM J. ENGEL, M.D. Department of Urology THE vesical dysfunction which follows injury or disease of the spinal cord or cauda equina has always presented
NEUROUROLOGY BACKGROUND
 NEUROUROLOGY BACKGROUND Lower urinary tract dysfunction is common among patients with underlying neurologic conditions. Also known as neurogenic bladder, this occurs as a result of the disruption of the
NEUROUROLOGY BACKGROUND Lower urinary tract dysfunction is common among patients with underlying neurologic conditions. Also known as neurogenic bladder, this occurs as a result of the disruption of the
Practical urodynamics What PA s need to know. Gary E. Lemack, MD Professor of Urology and Neurology
 Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
2/9/2008. Men Women. Prevalence of OAB. Men: 16.0% Women: 16.9% Prevalence (%) < Age (years)
 Definition Botox for Overactive Bladder Donna Y. Deng Assistant Professor UCSF Department of Urology Urinary urgency With or without urge incontinence Usually with frequency & nocturia International Continence
Definition Botox for Overactive Bladder Donna Y. Deng Assistant Professor UCSF Department of Urology Urinary urgency With or without urge incontinence Usually with frequency & nocturia International Continence
Physiologic Anatomy and Nervous Connections of the Bladder
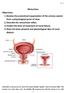 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
2. Surgeons considering invasive therapy in patients with SUI should assess postvoid residual (PVR) urine volume. (Expert Opinion)
 1 ADULT URODYNAMICS: AUA/SUFU GUIDELINE Approved by the AUA Board of Directors April 2012 Authors disclosure of potential conflicts of interest and author/staff contributions appear at the end of the article.
1 ADULT URODYNAMICS: AUA/SUFU GUIDELINE Approved by the AUA Board of Directors April 2012 Authors disclosure of potential conflicts of interest and author/staff contributions appear at the end of the article.
Dr. Melissa Kagarise, PA C
 Dr. Melissa Kagarise, PA C This program has been supported by an educational grant from Pfizer Pharmaceuticals PharmCon is accredited by the Accreditation Council for Pharmacy Education as a provider of
Dr. Melissa Kagarise, PA C This program has been supported by an educational grant from Pfizer Pharmaceuticals PharmCon is accredited by the Accreditation Council for Pharmacy Education as a provider of
Overactive Bladder in Clinical Practice
 Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
Urinary Incontinence. Lee A. Jennings, MD, MSHS. Assistant Professor Reynolds Department of Geriatrics University of Oklahoma Health Sciences Center
 Urinary Incontinence Lee A. Jennings, MD, MSHS Assistant Professor Reynolds Department of Geriatrics University of Oklahoma Health Sciences Center Slides adapted from Alison Moore, MD, MPH University of
Urinary Incontinence Lee A. Jennings, MD, MSHS Assistant Professor Reynolds Department of Geriatrics University of Oklahoma Health Sciences Center Slides adapted from Alison Moore, MD, MPH University of
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital
 LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital LUTS- Classification Men LUTS can be divided into: Storage Voiding Frequency Nocturia Urgency
LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital LUTS- Classification Men LUTS can be divided into: Storage Voiding Frequency Nocturia Urgency
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
What is on the Horizon in Drug Therapy for OAB?
 What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
Prolapse and Urogynae. By Sarah Rangan & Daniel Warrell
 Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA. A Minimally Invasive Innovative Treatment
 PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
MP A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction. Gaines W. Hammond Jr.
 MP73-06 - A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction Gaines W. Hammond Jr. MD FACS M3 Mini Catheter M3 Segmented M3 Plus Dynamic Wings M3
MP73-06 - A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction Gaines W. Hammond Jr. MD FACS M3 Mini Catheter M3 Segmented M3 Plus Dynamic Wings M3
