Urodynamic Patterns of the Idiopathic Overactive Bladder
|
|
|
- Brice Powers
- 6 years ago
- Views:
Transcription
1 Science Journal of Clinical Medicine 2017; 6(5): doi: /j.sjcm ISSN: (Print); ISSN: (Online) Urodynamic Patterns of the Idiopathic Overactive Bladder Yuriy M. Dekhtiar, Fedir I. Kostyev, Oleksandr V. Rudenko, Dmytro O. Kuznietsov Department of Urology and Nephrology, Odessa National Medical University, Odessa, Ukraine address: (D. O. Kuznietsov) To cite this article: Yuriy M. Dekhtiar, Fedir I. Kostyev, Oleksandr V. Rudenko, Dmytro O. Kuznietsov. Urodynamic Patterns of the Idiopathic Overactive Bladder. Science Journal of Clinical Medicine. Vol. 6, No. 5, 2017, pp doi: /j.sjcm Received: August 16, 2017; Accepted: September 4, 2017; Published: October 19, 2017 Abstract: The aim of study was the investigation of frequency and clinical significance of selected stereotypical recurring urodynamic patterns, which are manifested by the results of a complex urodynamic study in patients with idiopathic overactive bladder. The combined urodynamic study (CUS) was conducted in 137 patients with IOAB. The standard cystotonometry allowed to observe the maximum cystometric capacity. It also allowed to determine the bladder sensitivity (BS) and detect the presence of detrusor overactivity (DO). The results of retrograde cystotonometry established three variants of detrusor overactivity: phase DO, terminal DO, and stress-induced DO. The study of the bladder function using methods of UFM and EMG of anal sphincter in the emptying phase, confirmed the association of obstructive urination with incomplete discharge of the urethra from the effects of the sphincter. The coordination of function of the detrusor and external sphincter were assessed according to the results of CUS and sphincteric EMG. The EMG analysis in Work / Rest Assessment mode allowed to reveal the characteristic changes in the biopotential indices of the pelvic sphincter and indicated their correlation with the clinical features of the disease course. The imperative character of urination was established in 137 patients with IOAB during CUS characterized by hyperactivity and hypertensity of bladder, depending on the severity of the violation of the integrative function of LUT. Keywords: Overactive Bladder, Cystotonometry, Uroflowmetry, Detrusor Overactivity 1. Introduction Overactive Bladder (OAB), also known as Overactive Bladder Syndrome, is a condition of frequent feel to urinate which adversely affects the quality of life. Frequent urges for urination may occur at the day, at night, or both, with urinary incontinence (UI) or without it [1]. Although the overall prevalence of OAB is similar between men and women, there are sex-specific differences in the prevalence of various symptoms within the OAB complex [2-4]. Anatomical and physiological differences in the lower urinary tract of males and females may help to explain these variations. Overall, OAB prevalence rates in large population-based studies range from 7-27% in men and 9-43% in women. A proportion of OAB cases (37-39%) has correlated during a given year, but the majority of patients had persistent symptoms [5-6]. Diagnostics of the lower urinary tract symptoms (LUTS) in patients with idiopathic overactive bladder (IOAB) consists of complaints, anamnesis, neurological and urological examinations. It also requires the additional survey methods, among which the urodynamic testing occupies a major place. The discussion about clinical significance of the urodynamic tests in the diagnostics of various forms of urination disorders is still relevant [1, 7]. However, the opinions on this matter are greatly contrasting. Some researchers believe that the urodynamics are mandatory for diagnosis and treatment among patients with OAB symptoms, because diagnosis based on urinary symptoms alone, would lead to under-diagnosis of detrusor overactivity (DO) [8]. The cause of IOAB might be detrusor overactivity, in which the bladder muscle (the detrusor) contracts unexpectedly during bladder filling. Urodynamics can be used to confirm the presence of detrusor overactivity, which may help guide treatment. An overactive detrusor can be associated with urge incontinence [9]. The two main aims in study of the lower urinary tract urodynamics are: to reproduce symptomatic complaints of a patient during urodynamic tests, and to provide a pathophysiological explanation by comparing the patient's symptoms with the results of urodynamic studies. There is an
2 75 Yuriy M. Dekhtiar et al.: Urodynamic Patterns of the Idiopathic Overactive Bladder opinion that LUTS is important because it leads the patient to a doctor, but it also complicates the treatment tactics for the doctor [10]. 2. Purpose of the Study The purpose of the study was to determine the frequency and clinical significance of selected stereotypical recurring urodynamic patterns, which are manifested by the results of urodynamic studies in patients with idiopathic overactive bladder. 3. Method The combined urodynamic studies (CUS) (uroflowmetry, urethral profilometry, filling and emptying cystotonometry in the "pressure-flow study") was conducted in 137 patients (105 women, 32 males) with IOAB. The study was conducted on the urodynamic device "Pico Compact" (Menfis Bio Medica, Italy) and Delphis KT (Laborie, Canada), according to the recommendations of the International Committee for the Prevention of Urinary Incontinence (UI). The study of the pelvic floor muscle system bioelectric activity with computer electromyography (EMG) of the sphincter pelvic apparatus was conducted on a 2-channel electromyograph "Neuro Trac Myo Plus 4" in the Work / Rest Assessment mode. 4. Result The standard cystotonometry allowed to observe the maximum cystometric capacity. It also allowed to determine the bladder sensitivity (BS) and detect the presence of detrusor overactivity (DO) (Table 1). Bladder sensitivity is the only subjective parameter whose assessment only depends on the patient. The bladder sensitivity is determined during retrograde cystotonometry and closely related to the volume and rate of fluid intake during the study. The increased sensitivity of bladder (hypersensitivity) was defined as urge to urinate, which arised early and persisted until the end of the study. Table 1. Frequency of urodynamic symptoms in patients with IOAB (n = 137). Symptoms Number of patients (%) Hypersensitivity 97 (70,8%) Decrease of compliance 59 (43,1%) Detrusor overactivity 49 (35,8%) Urinary incontinence during the study 31(22,6%) Functional intravesical obstruction 47 (34,3%) Sphincter insufficiency 61 (44,5%) Reduction of the functional urethral length 55 (40,1%) Dysfunctional urination (pseudodysynergia) 10 (7,3%) Instability of urethra 34 (24,8%) Cystalgias during the study 37 (27%) Reduction of maximum cystometric capacity 118 (86,1%) The results of retrograde cystotonometry established three variants of detrusor overactivity: phase DO, terminal DO, and stress-induced DO. The phase DO was defined as the presence of phase waves with urine leakage or without it. The terminal DO was defined as the uninhibited reduction of detrusor. Phase DO was the most frequently observed in younger patients, regardless of gender. The average age of women with phase DO was 41.5 years. The average age of women with terminal DO was 62.3 years. The average age of males with phase DO was 43.3 years and 58.1 years in males with terminal DO. The volume of bladder with one uninhibited reduction of the detrusor was greater in phase DO (117.3 ± 11.7 ml versus 83.8 ± 9.1 ml). Other parameters did not differ significantly in both genders. The amplitude of one uninhibited reduction of the detrusor during the phase DO was significantly lower than terminal DO in both genders. Phase detrusor overactivity is a wave-like involuntary reduction of the detrusor, which often leads to the urgency (Figure 1). Figure 1. Retrograde cystotomometry of the patient E., 36 years old. Phase DO, wavy involuntary reduction of detrusor.
3 Science Journal of Clinical Medicine 2017; 6(5): The phase reduction of the detrusor may not be accompanied by certain feelings of the patient. It can be perceived as the first sensation of bladder filling, or standard urge to urinate. Terminal DO was characterized by the presence of a single involuntary reduction of the detrusor, which occurred when the bladder filled to the maximum cystometric capacity (Figure 2, Figure 3). Stress-induced DO is a significant increase in intravesical pressure, occurred due to physical effort, coughing, sneezing, or change in body position (Figure 4). Figure 2. Retrograde cystotomometry of patient S., 34 years. Terminal DO. Figure 3. Investigation of "pressure-flow". Patient L., 67 years old. The phase of the terminal DO with urine loss (urgent incontinence). One of the most important functional lower urinary tract indicators is the extensiveness (compliance) of the bladder. Bladder compliance states the communication between the change in volume of bladder filling and the increase of detrusor pressure during the CUS. Bladder compliance is the ability to maintain stable indices of intravesical pressure during its filling. Its parameter is > ml / cm H 2 O in normal. It is important to remember that the pathological values of compliance can be an artifact when the bladder is filled to fast. The test of the filling speed changing was
4 77 Yuriy M. Dekhtiar et al.: Urodynamic Patterns of the Idiopathic Overactive Bladder performed to prove it. This phenomenon was considered as an artifact, in the case of compliance normalization. Reduction of the bladder compliance during CUS can be also considered as urodynamic pattern of the IOAB. Figure 4. Retrograde cystotomometry of patient V., 41 years. Stress-induced DO detected after cough test. Indicators of CUS may not show the true anatomical capacity of bladder, but such urodynamic indicator exceeded the volume of urinations, captured by patients in urination diaries. Normal indices of cystotomometry in our study were found in 22 (15.3%) patients. At the same time, we did not exclude these patients from the treatment group of IOAB. The function of the sphincter apparatus was suffered also. The maximum urethral pressure did not exceed 30 cm of water column, according to the results of urethral profilometry in 61 (44.5%) patient with IOAB, testifying to the presence of urethral sphincter deficiency. A decrease in the functional length of the urethra was detected in 55 (40.1%) patients. The fluctuations of maximum intravesical pressure, with a static position of the sensor for 5-10 minutes and the amplitude of cm of water column was defined as the instability of the urethra in 34 (24.8%) patients. Fluctuations in maximum urethral pressure may lead to urgency and also to obstructive urination. The instability of the urethra was registered in combination with the DO and without it. Urethral instability was characterized by significant, spontaneous, non-induced deviations of urethral pressure, provided by a critical reduction in the value of closure pressure, which may cause the involuntary loss of urine due to a negative urethral-bladder pressure gradient. The 3 probable variants of bladder excretion were observed according to the results of uroflowmetry (UFM). The normal urination was observed in 56 (40.1%) patients, rapid urination in 34 (24.8%) patients and obstructive urination in 47 (34.3%) patients. The intermittent urination was observed in 24 (17.5%) patients. An increase in the tone of the detrusor before the urination, according to results of CUS, was observed in most of patients with IOAB. The hope for "rapid" urination was observed in the case of a proportional tone of an increase in the effective diameter of the urethra. However, it was only in 47 patients. The absence of it in other patients was due to the disproportionate opening of the sphincter apparatus. The normal micturition was observed in case of the minimal incomplete relaxation of sphincter during the urination. The obstructive urination with functional disorders is the one of manifestations in disorders of urine evacuation detected in patients with OAB. The instability of the urethra, incomplete relaxation of the bladder neck or sphincter during micturation, pseudodyssynergia of the detrusor-sphincter segment, are the main causes of obstructive urination development in patients with OAB. Difficulty urinating in patients with OAB may be a consequence of a violation of bladder contractile ability, through the DO. Difficulty urinating in women with OAB may be also due to omission of the vaginal walls, the formation of cystocele and violation of the angle of the urethrovesical segment. 5. Discussion The study of the bladder function using methods of UFM and EMG of anal sphincter in the emptying phase, confirmed the association of obstructive urination with incomplete discharge of the urethra from the effects of the sphincter. The excretion of bladder proceeds against a background of its high electrical activity. It was manifested by the registration of "outbreaks" in contractile activity of the transversalstriated sphincter of urethra and muscles of the pelvic floor,
5 Science Journal of Clinical Medicine 2017; 6(5): making it difficult to urinate or completely stopped the urinary flow. The detailed assessment of urination in "pressure-flow" regime was found the decrease of urethral pressure during urination, which caused intravesical obstruction in patients with signs of obstructive urination and instability of the urethra. The spontaneous increase and decrease of detrusor pressure during micturation were recorded in patients with DO. It could also cause a combination of pollakiuria, urge UI and obstructive urination. The coordination of function of the detrusor and external sphincter were assessed according to the results of CUS and sphincteric EMG. The symptoms of muscle dysfunction of the perineum and sphincter apparatus were not detected by EMG in 17.8% of patients with IOAB. The increased EMG activity of the LUT sphincter with the maximum increase of EMG signals at the time of the first urge to urinate was observed in these patients during the phase of urinary accumulation in the bladder. The arbitrary reduction of the detrusor and relaxation of the periurethral striated muscle were observed during the evacuation phase of urination. It was manifested in the sphincter EMG curve by the disappearance of electrical signals. The EMG analysis in Work / Rest Assessment mode allowed to reveal the characteristic changes in the biopotential indices of the pelvic sphincter and indicated their correlation with the clinical features of the disease course. The symptoms of dysfunction of the perineal striated muscles and sphincter apparatus of pelvic organs were detected by the EMG study in 78.2% of women with an urgent form UI. The dysfunction of perineal muscles and sphincter apparatus was detected in 36.8% women with "sensory" symptoms of IOAB, without urinary incontinence. The same dysfunction was detected in 53.4% of patients with IOAB with pain syndrome. Symptoms of dysfunction are manifested by the contraction of the external sphincter of bladder with a cystometric determined reflex of the detrusor reduction, which is characterized by loss of ability to reduce or relax the external sphincter during the period of detrusor reduction. The characteristic feature of EMG in the Work / Rest Assessment (62%) mode, conducted in patients with urodynamically proven DO, was the decrease in the amplitude of biopotentials of perineal striated muscles and the increase of the biopotentials of the sphincter apparatus of the pelvic organs. The spontaneous activity of the biopotentials in striated muscles of the bladder external sphincter and the sphincter of the anus was detected in 6 (12.2%) patients with DO in the state of relative physiological rest, during the course of CUS. It was observed on EMG curve by increasing the amplitude of the signals up to 100 µv during the period of urine accumulation with imperative urges, coughing and sneezing. Meanwhile, the urinary disorders are not primarily associated with dysfunction of the bladder external sphincter in the IOAB. It is confirmed by the absence of reliable differences in the characteristics of the EMG-curves, which analyzed in the Work / Rest Assessment mode, including the amplitude, duration of one EMG signal and the number of waves per unit time. Thus, sphincter EMG in the Work / Rest Assessment mode with sphincter EMG during urodynamic tests allows study the complete information about the functional state of LUT. The sphincter EMG acquires special significance in patients with IOAB and intravesical obstruction with dysfunction of the bladder sphincter apparatus. The EMG study, conducted on two channels of biofeedback with the study of the intravesical pressure dynamics, was established the distinct functional state of bladder external and anal sphincter in 35 patients with IOAB. It was manifested by a significant difference in the levels of electrical activity of these sphincters. This form of dysfunction was noted in 12 patients (24.5%) with DO and 23 patients (26.1%) without DO. 6. Conclusion 1. The imperative character of urination was established in 137 patients with IOAB during CUS characterized by overactivity and hypertensity of bladder, depending on the severity of the violation of the integrative function of LUT. It leads to decrease of the maximum cystometric capacity in 86.1% of patients, decrease of the bladder sensitivity in 70,8% of patients, detrusor overactivity in 35,8% of patients, decrease of complicacy in 43,1% of patients and instability of urethra in 24,8% of patients. 2. The sphincter EMG in the Work / Rest Assessment mode during CUS allows to get more complete information about the functional state of LUT and plays an important role in the diagnosis of electro neurophysiological disorders of the pelvic floor muscle and pelvic sphincter function, changes in intravesical pressure, which is accompanied by significant differences in characteristics of EMG - curves analyzed in the Work / Rest Assessment mode and a significant reduction in the time keeping maximum muscular effort (reduction). The sphincter EMG takes significant part in observation of patients with IOAB and intravesical obstruction due to dysfunction of the bladder sphincter apparatus. 3. Reduction of the bladder ability to accumulate and retain urine at normal or low intravesical pressure and frequent combination of bladder instability with signs of obstructive urination are the main features of urodynamic violations of the lower urinary tract in patients with IOAB. Abbreviation IOAB BS DO UFM EMG CUS LUTS idiopathic overactive bladder bladder sensitivity detrusor overactivity uroflowmetry electromyography combined urodynamic study lower urinary tract symptoms
6 79 Yuriy M. Dekhtiar et al.: Urodynamic Patterns of the Idiopathic Overactive Bladder References [1] Gormley EA, Lightner DJ, Burgio KL, Chai TC, Clemens JQ, Culkin DJ, Das AK, Foster Jr HE, Scarpero HM, Tessier CD, Vasavada SP. Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. J Urol. 2012; 188(6): [2] Vaughan CP, Johnson TM, 2nd, Ala-Lipasti MA, Cartwright R, Tammela TL, Taari K, et al. The Prevalence of Clinically Meaningful Overactive Bladder: Bother and Quality of Life Results from the Population-Based FINNO Study. Eur Urol 2011; Jan 25. [3] Link CL, Steers WD, Kusek JW, et al. The association of adiposity and overactive bladder appears to differ by gender: Results from the Boston Area Community Health survey. J Urol 2011; 185: ; [4] Patra PB, Patra S. Sex differences in the physiology and pharmacology of the lower urinary tract. Curr Urol 2013; 6: [5] Choo MS, Ku JH, Lee JB, et al. Cross-cultural differences for adapting overactive bladder symptoms: Results of an epidemiologic survey in Korea. World J Uro 2007; 25: [6] Coyne KS, Sexton CC, Vats V, et al. National community prevalence of overactive bladder in the United States stratified by sex and age. Urology 2011; 77: [7] Gammie A, Clarkson B, Constantinou C, et al. International continence society guidelines on urodynamic equipment performance. Neurourol. Urodyn. 2014; 33: [8] Digesu GA, Khullar V, Cardozo L, Salvatore S. Overactive bladder symptoms: do we need urodynamics? Neurourol Urodyn. 2003; 22: Erratum in: Neurourol Urodyn. 2003; 22: 356. [9] Gormley, EA; Lightner, DJ; Faraday, M; Vasavada, SP (May 2015). "Diagnosis and Treatment of Overactive Bladder (Non- Neurogenic) in Adults: AUA/SUFU Guideline Amendment." The Journal of Urology. 193 (5): [10] Farzeen Firoozi. Interpretation of Basic and Advanced Urodynamics. Springer International Publishing Switzerland; p. 134.
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Video-urodynamics. P J R Shah Institute of Urology and UCH
 Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME?
 URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME? Andrea Tubaro, MD, FEBU Chairman Department of Urology Sant Andrea Hospital Sapienza University of Rome, Italy Disclosures Consultant, paid speaker,
URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME? Andrea Tubaro, MD, FEBU Chairman Department of Urology Sant Andrea Hospital Sapienza University of Rome, Italy Disclosures Consultant, paid speaker,
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Practical urodynamics What PA s need to know. Gary E. Lemack, MD Professor of Urology and Neurology
 Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY
 PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
The new International Continence Society
 ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
National Kidney and Urologic Diseases Information Clearinghouse
 Urodynamic Testing National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is the urinary tract? The urinary tract
Urodynamic Testing National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is the urinary tract? The urinary tract
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA
 Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Recommandations de prise en charge des vessies neurogènes EAU 2006
 Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories
 Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
What should we consider before surgery? BPH with bladder dysfunction. Inje University Sanggye Paik Hospital Sung Luck Hee
 What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity
 ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우
 Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
Development of mathematical model for lower urinary tract dysfunctions
 Development of mathematical model for lower urinary tract dysfunctions Mohanad A.Deaf 1, Mohamed A.A.Eldosoky 1, Ahmed M. El-Garhy 2, Hesham W.Gomma 2, Ahmed S.El-Azab 3 Dept. of Biomedical Engineering,
Development of mathematical model for lower urinary tract dysfunctions Mohanad A.Deaf 1, Mohamed A.A.Eldosoky 1, Ahmed M. El-Garhy 2, Hesham W.Gomma 2, Ahmed S.El-Azab 3 Dept. of Biomedical Engineering,
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Training a Wayward Bladder
 D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Urodynamic findings in women with insensible incontinence
 bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY IN CHILDREN
 0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
PRE-OPERATIVE URODYNAMIC
 PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT
 UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT Yunizaf, MD Division of Urogynecology Department of Obstetrics and Gynecology School of Medicine, University of Indonesia/ Dr. Cipto Mangunkusumo Hospital
UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT Yunizaf, MD Division of Urogynecology Department of Obstetrics and Gynecology School of Medicine, University of Indonesia/ Dr. Cipto Mangunkusumo Hospital
April Clinical Focus Topic URINARY FREQUENCY
 April Clinical Focus Topic URINARY FREQUENCY This month I am focusing on a topic that may seem a little boring. But I would like to look at it from a less common perspective.urinary Frequency and its relationship
April Clinical Focus Topic URINARY FREQUENCY This month I am focusing on a topic that may seem a little boring. But I would like to look at it from a less common perspective.urinary Frequency and its relationship
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
MP A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction. Gaines W. Hammond Jr.
 MP73-06 - A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction Gaines W. Hammond Jr. MD FACS M3 Mini Catheter M3 Segmented M3 Plus Dynamic Wings M3
MP73-06 - A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction Gaines W. Hammond Jr. MD FACS M3 Mini Catheter M3 Segmented M3 Plus Dynamic Wings M3
 giovanni.montini@aosp.bo.it VD: definition Voiding dysfunction refers to daytime voiding disorders in children who do not have neurologic, anatomic, obstructive, or infectious abnormalities of the urinary
giovanni.montini@aosp.bo.it VD: definition Voiding dysfunction refers to daytime voiding disorders in children who do not have neurologic, anatomic, obstructive, or infectious abnormalities of the urinary
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Diagnosis and Mangement of Nocturia in Adults
 Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
This report presents definitions of the symptoms,
 UPDATE THE STANDARDISATION OF TERMINOLOGY IN LOWER URINARY TRACT FUNCTION: REPORT FROM THE STANDARDISATION SUB-COMMITTEE OF THE INTERNATIONAL CONTINENCE SOCIETY PAUL ABRAMS, LINDA CARDOZO, MAGNUS FALL,
UPDATE THE STANDARDISATION OF TERMINOLOGY IN LOWER URINARY TRACT FUNCTION: REPORT FROM THE STANDARDISATION SUB-COMMITTEE OF THE INTERNATIONAL CONTINENCE SOCIETY PAUL ABRAMS, LINDA CARDOZO, MAGNUS FALL,
Treatment Outcomes of Tension-free Vaginal Tape Insertion
 Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Module 3 Causes Of Urinary Incontinence
 Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Paediatric Urotherapy Training
 Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Report from the Standardisation Sub-committee of the International Continence Society
 THE STANDARDISATION OF TERMINOLOGY IN LOWER URINARY TRACT FUNCTION Report from the Standardisation Sub-committee of the International Continence Society Committee: Paul Abrams, Linda Cardozo, Magnus Fall,
THE STANDARDISATION OF TERMINOLOGY IN LOWER URINARY TRACT FUNCTION Report from the Standardisation Sub-committee of the International Continence Society Committee: Paul Abrams, Linda Cardozo, Magnus Fall,
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach)
 Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach) Andrew Combs, PA-C Director, Pediatric Urodynamics Division of Pediatric Urology New York Presbyterian-Weill Cornell
Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach) Andrew Combs, PA-C Director, Pediatric Urodynamics Division of Pediatric Urology New York Presbyterian-Weill Cornell
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
Managing Female Urinary Incontinence Within Primary Care
 Managing Female Urinary Incontinence Within Primary Care Angela Patterson Lead Clinical Nurse Specialist in Bladder and Bowel Dysfunction. South Eastern HSCT Background More than 14 million in the UK affected
Managing Female Urinary Incontinence Within Primary Care Angela Patterson Lead Clinical Nurse Specialist in Bladder and Bowel Dysfunction. South Eastern HSCT Background More than 14 million in the UK affected
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Updates in the nonpharmacological. treatment on overactive bladder
 Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
FACTORS AFFECTING VOIDING FUNCTION IN UROGYNECOLOGY PATIENTS
 ORIGINAL ARTICLE FACTORS AFFECTING VOIDING FUNCTION IN UROGYNECOLOGY PATIENTS Ling-Hong Tseng*, Ching-Chung Liang, Pei-Kwei Tsay 1, Alex C. Wang, Tsia-Shu Lo, Yi-Hao Lin Department of Obstetrics and Gynecology,
ORIGINAL ARTICLE FACTORS AFFECTING VOIDING FUNCTION IN UROGYNECOLOGY PATIENTS Ling-Hong Tseng*, Ching-Chung Liang, Pei-Kwei Tsay 1, Alex C. Wang, Tsia-Shu Lo, Yi-Hao Lin Department of Obstetrics and Gynecology,
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Incontinence: Risks, Causes and Care
 Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Urogynecology Associates of Philadelphia URODYNAMIC TESTING
 URODYNAMIC TESTING Urogynecology Associates of Philadelphia Most women with urinary incontinence will need to complete a few simple tests, performed in the office, to help your doctor assess your symptoms
URODYNAMIC TESTING Urogynecology Associates of Philadelphia Most women with urinary incontinence will need to complete a few simple tests, performed in the office, to help your doctor assess your symptoms
Urodynamics in women. Aims of Urodynamics in women. Why do Urodynamics?
 Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Overactive Bladder in Clinical Practice
 Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
3/20/10. Prevalence of OAB Men: 16.0% Women: 16.9% Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Dry. Population (millions) Wet
 1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
Brief Reports. Cystometric Evaluation of Voiding Dysfunctions
 Brief Reports Cystometric Evaluation of Voiding Dysfunctions Pawanindra Lal Navneet Kaur Anurag Krishna Not infrequently, in pediatric practice one is confronted by anxious parents of children with voiding
Brief Reports Cystometric Evaluation of Voiding Dysfunctions Pawanindra Lal Navneet Kaur Anurag Krishna Not infrequently, in pediatric practice one is confronted by anxious parents of children with voiding
Peter K. Sand, M.D. Roger Dmochowski, M.D.
 ANALYSIS OF THE STANDARDISATION OF TERMINOLOGY OF LOWER URINARY TRACT DYSFUNCTION: REPORT FROM THE STANDARDISATION SUB-COMMITTEE OF THE INTERNATIONAL CONTINENCE SOCIETY Neurourol Urodynam 21: 167-78, 2002
ANALYSIS OF THE STANDARDISATION OF TERMINOLOGY OF LOWER URINARY TRACT DYSFUNCTION: REPORT FROM THE STANDARDISATION SUB-COMMITTEE OF THE INTERNATIONAL CONTINENCE SOCIETY Neurourol Urodynam 21: 167-78, 2002
Physiologic Anatomy and Nervous Connections of the Bladder
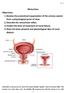 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Urodynamics Mismatch - Should We Listen to the Study, or the Patient?
 Urodynamics Mismatch - Should We Listen to the Study, or the Patient? A Practical Approach to the Diagnosis and Treatment of Lower Urinary Tract Dysfunction Victor W. Nitti MD Professor of Urology and
Urodynamics Mismatch - Should We Listen to the Study, or the Patient? A Practical Approach to the Diagnosis and Treatment of Lower Urinary Tract Dysfunction Victor W. Nitti MD Professor of Urology and
Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in children
 ORIGINAL ARTICLE Vol. 41 (4): 739-743, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0303 Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in
ORIGINAL ARTICLE Vol. 41 (4): 739-743, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0303 Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in
Appendix F: Continence Care and Bowel Management Program Training Presentation. Audience: For Front-line Staff Release Date: December 22, 2010
 Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
The Management of Male Incontinence
 The Management of Male Incontinence P J R Shah Institute of Urology UCLH LONDON And Victoria Muir Specialist Pelvic Health Physio Bedford Hospital NHS Trust Anatomy of the Prostate What does the prostate
The Management of Male Incontinence P J R Shah Institute of Urology UCLH LONDON And Victoria Muir Specialist Pelvic Health Physio Bedford Hospital NHS Trust Anatomy of the Prostate What does the prostate
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
EXPERIMENTAL AND THERAPEUTIC MEDICINE 4: , 2012
 1112 Usefulness of total bladder capacity and post void residual urine volume as a predictor of detrusor overactivity with impaired contractility in stroke patients SANG HYUB LEE, JOONG GEUN LEE, GYEONG
1112 Usefulness of total bladder capacity and post void residual urine volume as a predictor of detrusor overactivity with impaired contractility in stroke patients SANG HYUB LEE, JOONG GEUN LEE, GYEONG
4. Know how to examine and name relevant test performed on patients
 Chapter 18 Female Urinary lncontinence Dr Zeelha Abdool Ed ucational Objectives : After completion of this chapter you should be able to: 1. Understand the pathophysiology of incontinence 2. Define and
Chapter 18 Female Urinary lncontinence Dr Zeelha Abdool Ed ucational Objectives : After completion of this chapter you should be able to: 1. Understand the pathophysiology of incontinence 2. Define and
Outcomes of Midurethral Slings in Women with Concomitant Preoperative Severe Lower Urinary Tract Voiding Symptoms
 ORIGINAL RESEARCH The Ochsner Journal 15:223 227, 2015 Ó Academic Division of Ochsner Clinic Foundation Outcomes of Midurethral Slings in Women with Concomitant Preoperative Severe Lower Urinary Tract
ORIGINAL RESEARCH The Ochsner Journal 15:223 227, 2015 Ó Academic Division of Ochsner Clinic Foundation Outcomes of Midurethral Slings in Women with Concomitant Preoperative Severe Lower Urinary Tract
LUTS after TURP: How come and how to manage? Matthias Oelke
 LUTS after TURP: How come and how to manage? Matthias Oelke Department of Urology Global Congress on LUTD, Rome, 26 th June 2015 Disclosures Consultant, speaker, trial participant and/or research grants
LUTS after TURP: How come and how to manage? Matthias Oelke Department of Urology Global Congress on LUTD, Rome, 26 th June 2015 Disclosures Consultant, speaker, trial participant and/or research grants
The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence
 european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
排尿障礙治療中心版權所有. Physiotherapy of Lower Urinary Tract Dysfunction.
 Physiotherapy of Lower Urinary Tract Dysfunction www.fisiokinesiterapia.biz Lower Urinary Tract Dysfunction Urinary Incontinence Stress, urge, or mixed incontinence Frequency urgency syndrome Spastic urethral
Physiotherapy of Lower Urinary Tract Dysfunction www.fisiokinesiterapia.biz Lower Urinary Tract Dysfunction Urinary Incontinence Stress, urge, or mixed incontinence Frequency urgency syndrome Spastic urethral
ORIGINAL ARTICLE. Carlo Vecchioli Scaldazza 1, Carolina Morosetti 2, Rosita Giampieretti 3, Rossana Lorenzetti 3, Marinella Baroni 3
 ORIGINAL ARTICLE Vol. 43 (1): 121-126, January - February, 2017 doi: 10.1590/S1677-5538.IBJU.2015.0719 Percutaneous tibial nerve stimulation versus electrical stimulation with pelvic floor muscle training
ORIGINAL ARTICLE Vol. 43 (1): 121-126, January - February, 2017 doi: 10.1590/S1677-5538.IBJU.2015.0719 Percutaneous tibial nerve stimulation versus electrical stimulation with pelvic floor muscle training
2. Surgeons considering invasive therapy in patients with SUI should assess postvoid residual (PVR) urine volume. (Expert Opinion)
 1 ADULT URODYNAMICS: AUA/SUFU GUIDELINE Approved by the AUA Board of Directors April 2012 Authors disclosure of potential conflicts of interest and author/staff contributions appear at the end of the article.
1 ADULT URODYNAMICS: AUA/SUFU GUIDELINE Approved by the AUA Board of Directors April 2012 Authors disclosure of potential conflicts of interest and author/staff contributions appear at the end of the article.
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Urinary incontinence: the management of urinary incontinence in women
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence: the management of urinary incontinence in women 1.1 Short title Urinary incontinence 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence: the management of urinary incontinence in women 1.1 Short title Urinary incontinence 2 Background a) The National
Impact of urethral catheterization on uroflow during pressure-flow study
 Research Report Impact of urethral catheterization on uroflow during pressure-flow study Journal of International Medical Research 2016, Vol. 44(5) 1034 1039! The Author(s) 2016 Reprints and permissions:
Research Report Impact of urethral catheterization on uroflow during pressure-flow study Journal of International Medical Research 2016, Vol. 44(5) 1034 1039! The Author(s) 2016 Reprints and permissions:
