Introducing a pelvic floor telephone assessment service
|
|
|
- Annabel Grace Wilson
- 6 years ago
- Views:
Transcription
1 Introducing a pelvic floor telephone assessment service Carlene Igbedioh, Andrew B Williams, Alexis Schizas This article looks at a telephone triage assessment clinic that was set up to improve the bowel, bladder and pelvic floor service in the authors locality. A pelvic floor triage questionnaire was developed to identify patients faecal, urinary and prolapse symptoms then, between April and December 2013, patients were referred to the colorectal pelvic floor clinic via telephone triage assessment. Investigations could also be requested directly from the telephone triage assessment clinic. The need for any investigations and patient responses to the telephone triage assessment clinic questionnaires were reviewed in the pelvic floor multidisciplinary meeting. Previously, the wait for a new pelvic floor appointment was four months and this has been reduced to two weeks (or five weeks for a new consultant appointment). The telephone triage assessment clinic has led to a reduction in waiting times, an improvement in patient experience and more efficient referral. It is also more cost effective as it can replace a new consultant appointment. KEYWORDS: Continence Telephone triage assessment Bowel Bladder Bladder and bowel problems are a common cause of functional and quality of life issues for people in the community and it is imperative that nurses have the knowledge and skills in order to deal with continence issues should they arise. Bowel symptoms are commonly encountered in community settings, with prevalence increasing with age for instance, one-third of women and one-quarter of men aged over the age of 65 report recurrent constipation (Campbell et al, 1993). However; colonic transit can also be affected by comorbidity (e.g. in people who are immobilised Carlene Igbedioh, integrated continence advanced nurse practitioner, pelvic floor unit; Andrew B Williams, consultant colorectal surgeon; Alexis MP Schizas, consultant colorectal surgeon; all at Guy s and St Thomas NHS Foundation Trust, London through illness or medication) rather than ageing alone. Other risk factors include low calorie diets, enteric feeding and dehydration (Bharucha et al, 2013). Diseases such as Parkinson s, diabetes, stroke, renal dialysis, depression and dementia can also affect the functioning of the bowel. Urinary incontinence is also a more common problem than is often realised. In the UK it is estimated that at any one time at least 5% of the total population experience urinary incontinence, while the NHS estimates that between three and six million people in the UK have some degree of urinary incontinence (Royal College of Physicians, 2005). In 2010, the International Continence Society restated the definition of overactive bladder syndrome as a condition characterised by (Marinkovic et al, 2012): THE SCIENCE COMMON BOWEL SYMPTOMS Symptoms of bowel dysfunction are varied, but common problems include: Difficulty having bowel movements or less than three bowel movements per week may indicate constipation, as does straining on the toilet or not feeling empty Passing watery or very loose stools over three times a day Abdominal pain (located in the lower left stomach) and changes in bowel habits, such as constipation or diarrhoea as well as mild fever, nausea and vomiting are symptoms of diverticular disease Diarrhoea, weight loss and abdominal pain are symptoms of Crohn s disease Bloody or mucus-filled diarrhoea as well as a constant urge go to the toilet are symptoms of ulcerative colitis Leaking faeces without being aware of it is a sign of faecal incontinence. Source: Blader and Bowel Foundation: www. bladderandbowelfoundation.org Urinary urgency, usually accompanied by frequency and nocturia, with or without urgency incontinence, in the absence of urinary tract infection or other obvious pathology. Community nurses are ideally placed to advise other clinicians about patients with bladder and bowel symptoms, including the most JCN 2014, Vol 28, No 4 59
2 Table 1: Referral/vetting criteria for telephone triage system Referral sources Internal Colorectal clinics Consultant s clinic (all by letter) Physiotherapist Urogynaecology nurse Consultant nurse Medical, surgical, elderly care out-patient clinics and wards External GPs letter Other hospital/specialist centre Referral guidelines each referral is vetted against the following criteria: Inclusion criteria Patients with the following symptoms: Constipation Evacuation difficulties/outlet obstruction on defecation Bowel leakage/incontinence Exclusion criteria Red flag symptoms (not pelvic floor), such as rectal bleeding; change in bowel habit; weight loss; vaginal bleeding; haematuria; voiding difficulties Inappropriate referrals, poor referral/lack of adequate information on letter Specific tertiary referral/second opinion patient sent straight to pelvic floor clinic Language barrier if interpreter is required, service is not appropriate Multiple/significant comorbidity may impede nurse from collecting all of the patients s history appropriate referral pathways, as they regularly see patients at home or in nursing/residential homes. Recently, there has been an increase in demand for continence services, as incontinence becomes less of a taboo, and patients who have been become used to managing their own symptoms realise that they can access treatment. In the authors experience, GPs are also becoming more aware of pelvic floor services and are now referring patients for treatment. To implement an integrated plan, modern continence services need to be continually updated. However, an efficient continence service depends upon organisational reform rather than large-scale financial investment (Abram 2002a; 2002b) The importance of promoting best practice through an integrated continence service was established by the Department of Health (DH, 2000), which stated that an integrated continence service should provide expert advice and be available to people whose condition does not respond to initial treatment, as well as including designated medical and surgical specialists to provide a clear pathway of care. BACKGROUND Historically, referrals to the authors pelvic floor service were vetted through a consultant clinic. Patients attended hospital for a consultant consultation, after which they might have been sent to the pelvic floor service for a series of tests. Consultations took place in busy clinics and patients were asked a series of intimate and often embarrassing questions in what was often an unfamiliar environment. After the series of tests, patients might have been referred for conservative treatment in the bowel function clinic (such as biofeedback), or back to the consultant clinic for a discussion about surgery. Biofeedback uses symptom assessment, bowel and muscle retraining, behavioural therapy, visual education and psychological support to help people regulate their bowel function (Schwartz et al, 1995). For instance, by using a combination of internal sensors, electrodes placed on the abdomen and a computer screen, biofeedback training can help the patient to coordinate the sphincter muscles and improve his or her ability to sense the presence of faeces in the rectum. If conservative measures failed, patients were also referred back to the consultant to discuss surgical intervention, which includes transvaginal rectocoele repair, ventral mesh rectopexy, anal sphincter repair, the use of bulking agents and neuromodulation. Due to the number of diagnostic stages in the pathway, the specialist THE SCIENCE COMMON BLADDER SYMPTOMS Symptoms of bladder dysfunction include: A sudden urge to go to urinate or difficulty holding on is a symptom of urgency or urge incontinence Needing to urinate more than eight times in a single day can be a sign of urinary frequency Nocturia is signaled by repeated urination through the night; nocturnal enuresis is wetting the bed at night Mixed urinary continence is signaled by a mixture of the above symptoms Urination upon laughing, coughing, sneezing or exercise is a symptom stress urinary incontinence (SUI) Overflow incontinence is signaled by small leakages of urine that are not noticed by the individual. Source: Bladder and Bowel Foundation: 60 JCN 2014, Vol 28, No 4
3 Introducing GB Soft Skin Medical Adhesive Remover Spray... GREAT BEAR HEALTHCARE GB Soft Skin is a non-sting Medical Adhesive Remover Spray for quick and painless removal of Medical Adhesives as found on Sheaths and Stoma pouches. Aerosol spray for application can be sprayed upside down Aesthetically pleasing and discreet design Easy to use nozzle for those with poor dexterity Prevents against build up of sticky residue on the skin after removal of Sheath or Stoma Pouch The spray is non-chill and dries quickly Great Bear a brand you can trust GB Soft Skin is non-sting and moisturising on the skin Clearly identifiable re-order code Soft, Gentle & Kind to Skin For more information please contact: FREEPHONE: mail@gbhl.co.uk Great Bear Healthcare Ltd JCNAUG/2014
4 Colorectal letter or choose and book Referral centre (EVS) Five-minute test Answer the following questions about this topic, either to test the new knowledge you have gained or to form part of your ongoing practice development portfolio. 1 What are the common causes of colorectal problems? 2 Can you name some of the signs of bowel problems? 3 Do you understand what telephone triage is? 4 What are the main benefits of phone triage? 5 Can you explain how integrated referrals might benefit your area? nature of pelvic floor problems and increasing demand, patients requiring both conservative and surgical treatment were having to wait an increasing amount of time to be seen. THE NEW MODEL In response to increasing demands on the service and the need to reduce waiting times, the authors introduced a telephone triage assessment clinic. This involved patients being interviewed in their home so that they could discuss delicate pelvic floor issues in a familiar environment, without having to travel what were sometimes long distances for an assessment. Under the new system, patients are initially vetted using an assessment protocol (Table 1; Figure 1), before being given a telephone triage appointment. Patients are sent a detailed patient information sheet along with a date and time to wait by their phone. A healthcare professional with significant expertise in pelvic floor pathology then calls the patient and talks through a continence-specific questionnaire, which has been Assessment of referrals. Consultants surgeon and consultant nurse vets referral letter on a rota, from the referral box/electronic EVS system in the genitourinary department Letter sent to patient and GP Results to patient and GP Telephone clinic appointment made and letter to patient sent Bowel function clinic Combined clinic Consultant clinic Figure 1. Colorectal telephone assessment clinic referral pathway. developed to assess the patient s symptoms and identify those with combined symptoms as these are not always apparent in an initial referral (this phone call is usually made by a senior nurse but can also be delivered by a specialist physiotherapist or a medical consultant). The questionnaire poses a range of questions, for example: On average how many times do you open your bowels in a 24-hour period? Do you have to rush to the toilet Telephone Investigations Ultrasound and physiology Transit studies Colonoscopy Proctogram Other Multidisciplinary meeting when you need to open your bowels? Are you able to control accidental loss of formed, watery or loose stool leaking from your back passage? Do you have bowel accidents when you have no need to open your bowels? Is it difficult to hold urine when you get the urge to go Do you leak urine? This questionnaire has been designed to identify where input from other specialities, particularly 62 JCN 2014, Vol 28, No 4
5 Confused about wound care?? Then you need Wound Care Today, a brand new journal for everyone managing wounds For details on how to obtain your copy, go to: In association with:
6 urology and/or urogynaecology may be required. At the start of the telephone assessment, patients are asked about specific red flag symptoms for colorectal, urological and vaginal pathology, such as rectal bleeding; changes in bowel habit; weight loss; vaginal bleeding; haematuria; and voiding difficulties. If there are any red flag symptoms, the appropriate diagnostic test/s are requested (if they have not already been requested before referral). Following analysis of the questionnaire, the patient may be referred directly for appropriate conservative management or further investigations if necessary. The telephone interview will also identify those patients who require surgical review before treatment of any incontinence issues. Where it is clear from the original referral letter that a direct clinic appointment is required, this will be made for the patient. The results of the investigations are discussed in the colorectal multidisciplinary team meeting, then patients are referred for biofeedback or consultant clinic. Those patients with combined symptoms are discussed in the new joint pelvic floor multidisciplinary team meeting with the urology and urogynaecology teams. Following this, the patient is referred for biofeedback or new joint consultant clinic. The telephone triage assessment clinic runs three times per week and has both morning and afternoon clinics to provide a flexible approach. AUDIT The authors performed an audit to assess the suitability of the telephone triage assessment clinic and whether it: Adequately streamlined the patient pathway Offered an integrated service Reduced waiting times Offered a better patient experience Provided a cost-effective service. From March to November 2013, all data from the telephone clinic questionnaires was collected and then retrospectively reviewed by the authors. Results The telephone triage assessment clinic led to a reduction in waiting times, an improvement in patient experience and efficient referral to appropriate treatment. It also proved more cost effective, as the telephone assessment replaced the old system where the patient would require a new consultant appointment. Overall, the authors findings were: In total, 201 patient were reviewed Fifty-four percent of patients had combined symptoms Seventy-seven percent went on to receive biofeedback Twenty-three percent went on to a consultant clinic following review in the multidisciplinary meeting Seventeen percent subsequently underwent surgery, including ventral mesh rectopexy and transvaginal rectocoele repair In 13% of patients, conservative measures failed and they were referred back to the consultant clinic to discuss further options, i.e. surgery Three percent of those referred from biofeedback underwent an operation Three patients (1%) did not attend their appointment with the telephone triage assessment clinic On average, the time taken from telephone triage assessment clinic to biofeedback was seven weeks All patients were satisfied with the telephone triage assessment clinic (patients were asked if they were satisfied with the service at the end of the phone call) The wait for a new pelvic floor appointment before introduction of the telephone triage assessment clinic was four months this was reduced to two weeks. There is now a fiveweek wait for a new consultant appointment. Red Flag DISCUSSION Rectal bleeding Rectal bleeding can be caused simply by swollen blood vessels or small tears in the tissue of the anus (bright red blood), but can be more serious and should never be ignored. If the blood is darker in colour (melaena black or plum-coloured blood), it may come from the digestive system and is potentially more serious. Although rectal bleeding can signify early bowel cancer, there are many other symptoms that need to be verified and the patient should always seek medical advice. Source: rectal-bleeding This telephone triage assessment clinic replaced the old system where patients were given a new appointment with a consultant, irrespective of their symptoms. The continence questionnaire that forms part of the telephone assessment allows patients to be directed to the appropriate clinic, thereby reducing the number of unnecessary patient visits to hospital. As the continence questionnaire also identifies urology and urogynaecological symptoms, multidisciplinary meetings with colorectal, urology and urogynaecology departments were set up and joint colorectal, urology and urogynaecology clinics were established. This further reduced the number of new consultant appointments across a range of specialities and has led to a reduction in waiting and fewer hospital visits. The integration of referrals has aided integration of the continence service. Patients assessed by the integrated referral service now have access to individual clinics (biofeedback, physiotherapy or surgery), whereas those with combined incontinence symptoms have access to combined (urogynaecology) clinics. 64 JCN 2014, Vol 28, No 4
7 CONCLUSION The authors of this study set out to devise a new way of arranging referrals in the locality s busy bowel, bladder and pelvic floor service. In response to increasing demands on the service and the need to reduce waiting times, the authors introduced a telephone triage assessment clinic, which involved patients being interviewed in their home so that they could discuss delicate pelvic floor issues in a familiar environment without having to travel what were sometimes long distances for an assessment. An audit of the new service showed that patient s in the authors locality who require an integrated referral service now have a shorter wait for appointments. Also, the number of patient visits to outpatients has been reduced. JCN REFERENCES Abrams P (2002a) Our South West Vision for Integrated Services. Continence Foundation, London Abrams P (2002b) Our West Midlands Vision for Integrated Services. Continence Foundation, London Bharucha AE, Pemberton JH, Locke GR (2013) American Gastroenterological Association technical review on constipation. Gastroenterology 144(1): Campbell AJ, Busby WJ, Horwath CC (1993) Factors associated with constipation in a community based sample of people aged 70 years and over. J Epidemiol Comm Health 47: 23 6 DH (2000) Good Practice in Continence Services. DH, London Marinkovic SP, Rovner ES, Moldwin RM, Stanton SL, Gillen LM, Marinkovic CM (2012) The management of overactive bladder syndrome. Br Med J 344: 236 Royal College of Physicians (2005) Inadequate and incomplete continence care in the UK. Press release Available at: inadequate-and-incomplete-continencecare-uk (accessed 16 July, 2014) Schwartz MS, Andrasik F (1995) Biofeedback: a practitioner s guide. 2nd edition. Guilford, New York, USA Welcome to JCN s learning zone... JCN s online resource, which, together with the learning zone in the Journal of Community Nursing, helps you to develop your knowledge in vital areas of care, to keep up-to-date with clinical practice. Read the article Reflect on what you have learnt Review your knowledge with the online test... Then, download your certificate to show that you have completed this e-learning unit and gained competency in this area of clinical practice. JCN s learning zone an essential educational resource for all busy nurses working in the community. KEY POINTS This article looks at a telephone triage assessment clinic that was set up to improve the bowel, bladder and pelvic floor service in the authors locality. Overall, 201 patients were reviewed by the telephone triage clinic and 54% of these were found to have combined faecal and urinary symptoms. One hundred and twentyseven patients were referred to the biofeedback clinic and 29 to a consultant clinic following review in the multidisciplinary meeting. The telephone triage assessment clinic has led to a reduction in waiting times, an improvement in patient experience, and more efficient referral. It is also more cost-effective, as it can replace a new consultant appointment. JOURNAL OF COMMUNITY NURSING JCN 2014, Vol 28, No 4 65
Tertiary, regional and local pelvic floor service providers: the future. model? Andrew Williams
 Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Urinary dysfunction assessment tool (community)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Urinary dysfunction assessment tool (care home)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Faecal Incontinence Information Leaflet THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
Integrated Continence Service Policy. January SafeCare Council January Carol Giffin, Continence Advisor
 Policy No: OP51 Version: 1.0 Name of Policy: Integrated Continence Service Policy Effective From: January 2008 Approved by: SafeCare Council January 2008 Next Review Date: January 2010 Reviewed by: Carol
Policy No: OP51 Version: 1.0 Name of Policy: Integrated Continence Service Policy Effective From: January 2008 Approved by: SafeCare Council January 2008 Next Review Date: January 2010 Reviewed by: Carol
Keeping control What you should expect from your NHS bladder and bowel service
 Keeping control What you should expect from your NHS bladder and bowel service Based on findings from the national audit of continence care 2010 National audit funded by: Report authors Dr Danielle Harari
Keeping control What you should expect from your NHS bladder and bowel service Based on findings from the national audit of continence care 2010 National audit funded by: Report authors Dr Danielle Harari
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Drinking fluids and how they affect your bladder
 www.olarts.com Drinking fluids and how they affect your bladder Contact us Patient Advice and Liaison Service (PALS) To make comments or raise concerns about the Trust s services, please contact PALS.
www.olarts.com Drinking fluids and how they affect your bladder Contact us Patient Advice and Liaison Service (PALS) To make comments or raise concerns about the Trust s services, please contact PALS.
Lets talk about Faecal incontinence (FI) in Scleroderma
 Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Bladder retraining - treatment for urgency and urge incontinence
 Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS. A08/S/d Colorectal: Faecal Incontinence (Adult)
 A08/S/d 2013/14 NHS STANDARD CONTRACT FOR COLORECTAL: FAECAL INCONTINENCE (ADULT) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
A08/S/d 2013/14 NHS STANDARD CONTRACT FOR COLORECTAL: FAECAL INCONTINENCE (ADULT) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider.
 Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Disease Management. Incontinence Care. Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09
 Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
Treatments for Fecal Incontinence A Review of the Research for Adults
 Treatments for Fecal Incontinence A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional* said you or your loved one
Treatments for Fecal Incontinence A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional* said you or your loved one
Constipation Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.uk
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Tension-free Vaginal Tape (TVT)
 Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Constipation. What is constipation? What is the criteria for having constipation? What are the different types of constipation?
 What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
Pelvic floor exercises for women. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic floor exercises for women This leaflet will provide you with information about
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic floor exercises for women This leaflet will provide you with information about
Pelvic Floor Disorders. Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon
 Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Women s & Children s Directorate The TVT Operation - a guide for patients
 Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Pelvic floor exercises for women. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic Floor Exercises for Women This leaflet will provide you with information about
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic Floor Exercises for Women This leaflet will provide you with information about
Oxford Pelvic Floor Services A guide to the pelvic floor muscles. Information for men
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Rectal Bleeding. Exceptional healthcare, personally delivered
 Rectal Bleeding Exceptional healthcare, personally delivered Content n The surgical team has assessed you because you have had bleeding from the back passage (rectal bleeding). n But your condition needs
Rectal Bleeding Exceptional healthcare, personally delivered Content n The surgical team has assessed you because you have had bleeding from the back passage (rectal bleeding). n But your condition needs
TRANSURETHRAL BULKING AGENT PATIENT INFORMATION
 TRANSURETHRAL BULKING AGENT PATIENT INFORMATION ADHB Urology Department; Reviewed FEB 2005 Ubix code UPEB23 1 The information contained in this booklet is intended to assist you in understanding your proposed
TRANSURETHRAL BULKING AGENT PATIENT INFORMATION ADHB Urology Department; Reviewed FEB 2005 Ubix code UPEB23 1 The information contained in this booklet is intended to assist you in understanding your proposed
15. Prevention of UTI and lifestyle modifications
 15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
Continence Promotion in
 Everybody s Business- Continence Promotion in Aged Care Melissa O Grady Clinical Nurse Consultant Continence Warning Some graphic images are contained in this presentation Objectives What is Old Age? What
Everybody s Business- Continence Promotion in Aged Care Melissa O Grady Clinical Nurse Consultant Continence Warning Some graphic images are contained in this presentation Objectives What is Old Age? What
Leaving Hospital with a Stoma
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Leaving Hospital with a Stoma General Surgery Contents What is this leaflet all about? 3 What stoma equipment am I using? 3-4
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Leaving Hospital with a Stoma General Surgery Contents What is this leaflet all about? 3 What stoma equipment am I using? 3-4
Sphincter exercises for people with bowel control problems. Information for patients. Physiotherapy Department
 Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
A guide to Anoplasty (anal surgery)
 Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Pelvic Floor Exercises
 Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Laparoscopic Ventral. Mesh Rectopexy (LVMR)
 Laparoscopic Ventral Mesh Rectopexy (LVMR) Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard
Laparoscopic Ventral Mesh Rectopexy (LVMR) Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard
ONE IN THREE WOMEN WHO EVER HAD A BABY WET THEMSELVES EVERY WOMAN WHO HAS HAD A BABY SHOULD DO PELVIC FLOOR MUSCLE TRAINING.
 08 EVERY WOMAN WHO HAS HAD A BABY SHOULD Women who have even just one baby are nearly three times more likely to leak urine and wet themselves, than women who have not had a baby. The more babies you have,
08 EVERY WOMAN WHO HAS HAD A BABY SHOULD Women who have even just one baby are nearly three times more likely to leak urine and wet themselves, than women who have not had a baby. The more babies you have,
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Surgical treatment of urinary stress incontinence with tension free vaginal tape
 Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
Pelvic Floor Muscle Exercises
 INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
Module 5 Management Of Urinary Incontinence
 Management Of Urinary Incontinence V3: Last Reviewed September 2017 Learning Outcomes Outline conservative management options Discover the options available to manage the different types of incontinence
Management Of Urinary Incontinence V3: Last Reviewed September 2017 Learning Outcomes Outline conservative management options Discover the options available to manage the different types of incontinence
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men Why are my pelvic floor muscles important? Your pelvic floor muscles are important for bladder and bowel control. These muscles help to keep the bladder
Pelvic Floor Muscle Exercises and Advice for Men Why are my pelvic floor muscles important? Your pelvic floor muscles are important for bladder and bowel control. These muscles help to keep the bladder
Anorectal physiology test
 Anorectal physiology test We hope this factsheet will help to answer some of your questions about having an anorectal physiology test. If you have any further questions or concerns, please don t hesitate
Anorectal physiology test We hope this factsheet will help to answer some of your questions about having an anorectal physiology test. If you have any further questions or concerns, please don t hesitate
Prostate surgery. What is the prostate? What is a TURP? Why is a TURP operation necessary? Deciding to have a TURP operation.
 What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
Haldimand Physiotherapy Centre. Welcome Letter
 Haldimand Physiotherapy Centre 41 Caithness Street West, Caledonia, ON, N3W 2J2 Phone: (905)765-5449 email: ifeelgood@haldimandphysio.ca Website: www.haldimandphysio.ca Welcome Letter Welcome! Thank you
Haldimand Physiotherapy Centre 41 Caithness Street West, Caledonia, ON, N3W 2J2 Phone: (905)765-5449 email: ifeelgood@haldimandphysio.ca Website: www.haldimandphysio.ca Welcome Letter Welcome! Thank you
from Bowel Control Problems twitter.com/voicesforpfd
 BREAK FREE from Bowel Control Problems POP Quiz THE NUMBER OF PEOPLE IN THE UNITED STATES WITH BOWEL CONTROL PROBLEMS: A. 6 million B. 12 million C. 18 million BOWEL CONTROL PROBLEMS Nearly 18 million
BREAK FREE from Bowel Control Problems POP Quiz THE NUMBER OF PEOPLE IN THE UNITED STATES WITH BOWEL CONTROL PROBLEMS: A. 6 million B. 12 million C. 18 million BOWEL CONTROL PROBLEMS Nearly 18 million
Transanal irrigation. Toolbox for neurogenic bowel management. Information for patients Spinal Injuries
 Transanal irrigation Toolbox for neurogenic bowel management Information for patients Spinal Injuries Neurogenic bowel dysfunction A number of people with a spinal injury experience faecal incontinence
Transanal irrigation Toolbox for neurogenic bowel management Information for patients Spinal Injuries Neurogenic bowel dysfunction A number of people with a spinal injury experience faecal incontinence
Motility Disorders. Pelvic Floor. Colorectal Center for Functional Bowel Disorders (N = 701) January 2010 November 2011
 Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
To help you understand your operation, it is helpful to have a basic knowledge of how the body works (see Figure 1).
 Page 1 of 11 Anterior resection Introduction This leaflet tells you about the procedure known as an anterior resection. It explains what the procedure involves and also some of the common complications
Page 1 of 11 Anterior resection Introduction This leaflet tells you about the procedure known as an anterior resection. It explains what the procedure involves and also some of the common complications
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
Patient Information Leaflet
 Patient Information Leaflet MID-URETHRAL SLING OPERATION TENSION-FREE VAGINAL TAPE (TVT) TRANSOBTURATOR TAPE (TOT, TVT-O) This information leaflet has been developed to help your understanding of what
Patient Information Leaflet MID-URETHRAL SLING OPERATION TENSION-FREE VAGINAL TAPE (TVT) TRANSOBTURATOR TAPE (TOT, TVT-O) This information leaflet has been developed to help your understanding of what
University College Hospital at Westmoreland Street. Percutaneous Tibial Nerve Stimulation (PTNS)
 University College Hospital at Westmoreland Street Percutaneous Tibial Nerve Stimulation (PTNS) Urology Directorate If you need a large print, audio or translated copy of this document, please contact
University College Hospital at Westmoreland Street Percutaneous Tibial Nerve Stimulation (PTNS) Urology Directorate If you need a large print, audio or translated copy of this document, please contact
Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications
 Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications Consultation guide: Specialised gynaecology surgery and complex urogynaecology conditions
Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications Consultation guide: Specialised gynaecology surgery and complex urogynaecology conditions
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
encathopedia Volume 7 PARKINSON S AND THE BLADDER
 encathopedia Volume 7 PARKINSON S AND THE BLADDER Parkinson s disease Parkinson s is a progressive neurological condition. In people with Parkinson s, some of the brain cells that create the chemical dopamine
encathopedia Volume 7 PARKINSON S AND THE BLADDER Parkinson s disease Parkinson s is a progressive neurological condition. In people with Parkinson s, some of the brain cells that create the chemical dopamine
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
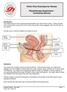 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Saint Mary s Hospital. The Warrell Unit. Perineal Clinic
 Saint Mary s Hospital The Warrell Unit Perineal Clinic 2 What is the Perineal Clinic? The Perineal Clinical is a clinic for women who have had a tear of the anal sphincter during the delivery of their
Saint Mary s Hospital The Warrell Unit Perineal Clinic 2 What is the Perineal Clinic? The Perineal Clinical is a clinic for women who have had a tear of the anal sphincter during the delivery of their
COLORECTAL RESECTIONS
 COLORECTAL RESECTIONS What is a colorectal (bowel) resection? Surgery to remove a part of the large bowel is called a resection. Different parts of the colon require different operations and have different
COLORECTAL RESECTIONS What is a colorectal (bowel) resection? Surgery to remove a part of the large bowel is called a resection. Different parts of the colon require different operations and have different
Stapled transanal rectal resection for obstructed defaecation syndrome
 Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
International Urogynecological Association (IUGA) Observership Grant. Final Report
 International Urogynecological Association (IUGA) 2009-10 Observership Grant Final Report Observership Grant Recipient: Renato Silva Martins 5 th Year Obstetrics and Gynaecology Resident at Coimbra s University
International Urogynecological Association (IUGA) 2009-10 Observership Grant Final Report Observership Grant Recipient: Renato Silva Martins 5 th Year Obstetrics and Gynaecology Resident at Coimbra s University
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE The management of faecal incontinence in adults 1.1 Short title Faecal incontinence 2 Background (a) (b) (c) The National Institute
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE The management of faecal incontinence in adults 1.1 Short title Faecal incontinence 2 Background (a) (b) (c) The National Institute
Urinary Incontinence for the Primary Care Provider
 Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Pelvic floor exercises for women. Information for patients Continence Service
 Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Bulkamid. Patient Information. Obstetrics & Gynaecology Department
 Bulkamid Patient Information Obstetrics & Gynaecology Department Author ID: JD Leaflet Number: Gyn 050 Version: 5 Name of Leaflet: Bulkamid Date Produced: November 2017 Review Date: November 2019 Bulkamid
Bulkamid Patient Information Obstetrics & Gynaecology Department Author ID: JD Leaflet Number: Gyn 050 Version: 5 Name of Leaflet: Bulkamid Date Produced: November 2017 Review Date: November 2019 Bulkamid
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Pelvic floor muscle exercises
 Lifestyle Helpline 0800 074 8383 prostatecanceruk.org 31 Pelvic floor muscle exercises In this fact sheet: How do pelvic floor muscle exercises help with urinary problems? How do I do the exercises? More
Lifestyle Helpline 0800 074 8383 prostatecanceruk.org 31 Pelvic floor muscle exercises In this fact sheet: How do pelvic floor muscle exercises help with urinary problems? How do I do the exercises? More
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
opyright 2017 SAMPLE COPY Property of Hayward Bell Ltd Copyright 2017 Bladder and bowel conditions can affect anyone
 Bladder and bowel conditions can affect anyone This booklet could be your first positive step to a full and active life Contents 1. Introduction 2. A bladder 3. The most common problems 5. A bowel 6. Functional
Bladder and bowel conditions can affect anyone This booklet could be your first positive step to a full and active life Contents 1. Introduction 2. A bladder 3. The most common problems 5. A bowel 6. Functional
EXPECTING A BABY? SOME PREGNANT WOMEN CAN HAVE BLADDER AND BOWEL CONTROL PROBLEMS. YOU CAN GET HELP. HOW DO I KNOW IF I HAVE A PROBLEM?
 11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
Management of Incontinence and Pelvic Floor Disorders
 Management of Incontinence and Pelvic Floor Disorders Dear Colleague: Multiple studies demonstrate that pelvic floor disorders urinary or fecal leakage occurring at an inappropriate time or place has a
Management of Incontinence and Pelvic Floor Disorders Dear Colleague: Multiple studies demonstrate that pelvic floor disorders urinary or fecal leakage occurring at an inappropriate time or place has a
Incontinence in neurological disease
 nice bulletin Incontinence in neurological disease NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin - Incontinence in neurological disease.indd
nice bulletin Incontinence in neurological disease NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin - Incontinence in neurological disease.indd
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Pelvic Floor Exercises: a guide for women
 Approvals: Gynae Guidelines Group: Jul 2018 O&G SDU: Jul 2018 Clinical Guidelines Subgroup: not required BMV: Sep 2018 Equality Impact Assessment: Oct 2018 Patient Experience Group: February 2019 Division
Approvals: Gynae Guidelines Group: Jul 2018 O&G SDU: Jul 2018 Clinical Guidelines Subgroup: not required BMV: Sep 2018 Equality Impact Assessment: Oct 2018 Patient Experience Group: February 2019 Division
Stoma Care Policy and Procedures
 Stoma Care Policy and Procedures Policy number 19.09 Approved by :CEO Version 1 Scheduled review date 28/3/2018 Created on 28/3/2017 POLICY STATEMENT Clients requiring management with the stoma will be
Stoma Care Policy and Procedures Policy number 19.09 Approved by :CEO Version 1 Scheduled review date 28/3/2018 Created on 28/3/2017 POLICY STATEMENT Clients requiring management with the stoma will be
The Urology One-Stop Clinic
 The Urology One-Stop Clinic Exceptional healthcare, personally delivered The aim of this leaflet is to answer any questions you may have about the Urology One-Stop Clinic. What is the Urology One-Stop
The Urology One-Stop Clinic Exceptional healthcare, personally delivered The aim of this leaflet is to answer any questions you may have about the Urology One-Stop Clinic. What is the Urology One-Stop
Cryotherapy for localised prostate cancer
 Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
MEDICAL QUESTIONNAIRE
 Center for Restorative Pelvic Medicine MEDICAL QUESTIONNAIRE Dear Patient: Please take a few minutes to complete this form. This will help assure you of the best possible care and will be held in confidence
Center for Restorative Pelvic Medicine MEDICAL QUESTIONNAIRE Dear Patient: Please take a few minutes to complete this form. This will help assure you of the best possible care and will be held in confidence
Cancer Screening Programmes BOWEL CANCER SCREENING. The Facts
 Cancer Screening Programmes BOWEL CANCER SCREENING The Facts What is the aim of this leaflet? This leaflet gives you information about bowel cancer, and the benefits and risks of bowel cancer screening.
Cancer Screening Programmes BOWEL CANCER SCREENING The Facts What is the aim of this leaflet? This leaflet gives you information about bowel cancer, and the benefits and risks of bowel cancer screening.
Advanced Practice in Women s Health and Continence Physiotherapy Project. Robyn Brennen Grade 4 Physiotherapist, Monash Health
 Advanced Practice in Women s Health and Continence Physiotherapy Project Robyn Brennen Grade 4 Physiotherapist, Monash Health Acknowledgements Desiree Terrill, Wendy Davis, Duncan Baulch Sarah Cleaver,
Advanced Practice in Women s Health and Continence Physiotherapy Project Robyn Brennen Grade 4 Physiotherapist, Monash Health Acknowledgements Desiree Terrill, Wendy Davis, Duncan Baulch Sarah Cleaver,
Bowel cancer risk in the under 50s. Greg Rubin Professor of General Practice and Primary Care
 Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
Pelvic organ prolapse
 Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Name: Date: Referring Provider: What is the nature of your current gynecologic or urologic medical problem (use the other side if necessary).
 Name: Date: Referring Provider: Age: D.O.B. Race/ ethnicity: What is the nature of your current gynecologic or urologic medical problem (use the other side if necessary). We are interested in learning
Name: Date: Referring Provider: Age: D.O.B. Race/ ethnicity: What is the nature of your current gynecologic or urologic medical problem (use the other side if necessary). We are interested in learning
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Stricture guide. Urology department. yeovilhospital.nhs.uk
 Stricture guide Urology department 01935 384 394 yeovilhospital.nhs.uk What is a urethral stricture? A urethral stricture is a narrowing or restriction of the urethra (the tube from your bladder through
Stricture guide Urology department 01935 384 394 yeovilhospital.nhs.uk What is a urethral stricture? A urethral stricture is a narrowing or restriction of the urethra (the tube from your bladder through
Appendix F: Continence Care and Bowel Management Program Training Presentation. Audience: For Front-line Staff Release Date: December 22, 2010
 Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
REVERSAL OF ILEOSTOMY. Patient information Leaflet
 REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
