O (P =.005) in the NDO group and from ± 9.92 cmh 2. O to ± cmh 2
|
|
|
- Philip Ryan
- 6 years ago
- Views:
Transcription
1 MISCELLANEOUS Success Rate and Patients' Satisfaction Following Intradetrusor Dysport Injection in Patients with Detrusor Overactivity: A Comparative Study of Idiopathic and Neurogenic Types of Detrusor Overactivity Saeed Shakeri, 1 Reza Mohammadian, 1 Alireza Aminsharifi, 1 Ali Ariafar, 1 Jalal Vaghedashti, 1 Maryam Yazdani, 2 Mahnza Yadollahi, 3 Vahid Emadmarvasti, 1 Amir Baharikhoob 1 1 Urology and Nephrology Research Center, Shiraz University of Medical Sciences, Shiraz, Iran. 2 Department of Obstetrics and Gynecology, Shiraz University of Medical Sciences, Shiraz, Iran. 3 Trauma Research Center, Shiraz University of Medical Sciences, Shiraz, Iran. Purpose: To evaluate the efficacy of intradetrusor Dysport (a type of botulinum toxin type A) injection in patients with idiopathic or neurogenic detrusor overactivity, who were refractory to antimuscarinic drugs, and to compare the efficacy of Dysport injection in both groups. Materials and Methods: Twelve patients with neurogenic detrusor overactivity (NDO) and 18 patients with idiopathic detrusor overactivity (IDO) participated in this study. All the patients received intravesical injection of 500 units of Dysport. They were followed up for 3 months after injection with maximum cystometric capacity, maximum detrusor filling pressure, and number of catheterization or pad usage. Corresponding Author: Reza Mohammadian, MD Department of Urology, Faghihi Hospital, Shiraz University of Medical Sciences, Shiraz, Iran. Tel: reza_mohammadian@ yahoo.com Received November 2012 Accepted June 2013 Results: After 3 months, the mean maximum cystometric capacity increased from ± ml to ± ml (P =.000) in the NDO group and from ± ml to ± ml (P =.000) in the IDO group. The mean maximum detrusor filling pressure decreased from ± cmh 2 O to ± 9.01 cmh 2 O (P =.005) in the NDO group and from ± 9.92 cmh 2 O to ± cmh 2 O (P =.003) in the IDO group. Conclusion: Intradetrusor Dysport injection improved urodynamic parameters and quality of life (QoL) in both groups significantly. We did not find significant difference in QoL or urodynamic parameters between both groups. Keywords: botulinum toxins, type A; administratin and dosage; urinary bladder, overactive; drug therapy; adverse effects. Vol. 11 No. 01 Jan-Feb
2 INTRODUCTION Overactive bladder (OAB) is a clinical syndrome characterized by urgency with or without urge incontinence, frequency, and nocturia (1) with a prevalence of 11.8% worldwide. (2) OAB has a significant effect on the quality of life in men and women suffering from this syndrome. (3-5) Detrusor overactivity (DO) is one of the main causes of OAB and is classified into idiopathic DO (IDO) and neurogenic DO (NDO) according to the International Continence Society classification. (6) Oral antimuscarinic agents are the first line treatment modality for patients with DO; however, its usage has been limited due to the adverse effects such as dry mouth or headache and their decreased efficacy in long term period as the result of up-regulation phenomenon. (7) More invasive procedures such as bladder augmentation and urinary diversion pose a significant risk of morbidity and complications to the patient. (8) Botulinum toxin type A (BTX-A) which is produced by clostridium botulinum, a gram positive bacteria, inhibits the release of acetylcholine at the neuromuscular junction and subsequently paralyses the muscle. The effects of BTX-A on parasympathetic nervous system was first investigated in the 1920s by Dickson and colleagues. (9) Although several studies also revealed the efficacy of intradetrusor injection of BTX-A in the treatment of both types of DO which were intractable to antimuscarinic therapy, (10,11) the data comparing the efficacy of intradetrusor injection of BTX-A in patients suffering either IDO or NDO are lacking. (12,13) In this study, we evaluated the efficacy of intradetrusor injection of Dysport ((Reloxin/BoNT-A, Ipsen Biopharm Ltd., Wrexham, UK) in patients with IDO and NDO, and the resulting improvement in the quality of life (QoL) in both groups. MATERIALS AND METHODS Study Design Our prospective cohort study was conducted from September 2010 to December Patients with symptoms of OAB and urodynamically proven IDO or NDO who were refractory to oral antimuscarinic medication for at least 3 months or those who had discontinued medical therapy due to drug side effects participated in this experimental study. Being refractory to antimuscarinic treatment was defined as no effect of antimuscarinic drugs available in Iran, i.e. oxybutynin hydrochloride (Iran Darou Co., Tehran-Iran), and Detrusitol (Pharmacia & Upjohn SpA, Milan, Italy) during a trial for at least 3 months. Patients with history of previous bladder surgery or Botox injection, an active urinary tract infection, any anatomical anomaly of the urinary system, urinary stone or urinary tract tumors and any medical disorder such as diabetes mellitus or multiple sclerosis were excluded from the study. Besides, all female patients were examined by a gynecologist to rule out genital infection or pelvic organ prolapse or relaxation which may induce voiding dysfunction. Pretreatment Evaluations All the patients gave their written informed consent and were divided into IDO and NDO groups. The patients were asked to chart a 3 days voiding diary mentioning the number of voids and episodes of urge incontinence per day. In patients with spinal cord injury and associated NDO, the numbers of urethral catheterization, and pad count per day were measured. Urodynamic study was performed in both groups according to International Continence Society s recommendations, (14) measuring parameters such as Maximum Cystometric Capacity (MCC), Maximum Detrusor Pressure on filling cystometry (MDP), and Post Void Residual (PVR) urine volume in the IDO group during urodynamic study or by bladder ultrasonography. QoL was assessed by the Incontinence Impact Questionnaire Short Form 7 (IIQ-7). Oral ciprofloxacin 500 mg (Razak Laboratories, Tehran, Iran) was administered twice daily one day before operation prophylactically in adult patients and cefexime (Zakaria Pharm. Co., Tabriz- Iran) 8 mg/kg/day in children. Patients on antiplatelet drugs were asked to stop their medication 7 days before the operation. Injection Technique The procedure was performed in an outpatient manner under general anesthesia in dorsal lithotomy position with some modifications in those patients with chronic spinal cord injury and limitation of hip joint motion. After cleaning and draping, 20 ml lidocaine gel 2% (Sina Darou, Tehran-Iran) was applied intraurethrally. Dysport was administered with an 11.5 French (F) Wolf rigid pediatric nephroscope (Richard Wolf GmbH, Germany). For each adult patient, 1 vial of Dysport (500 units) was administered, and the dosage for children was 20 units/kg. Each vial was diluted with 20 ml of sterile normal saline solution before injection. The mini Miscellaneous
3 Intradetrusor Dysport Injection in Detrusor Overactivity Shakeri et al Table 1. Comparison of clinical and urodynamic parameters before and after treatment in IDO patients. Variables Before injection After injection P Mean MCC, ml (n = 18) (n = 18) <.001 Mean Maximum Detrusor Pressure, cmh 2 O ± ± Mean Frequency ± ± <.001 Mean FDV ± ± 3.74 <.001 Mean IIQ ± ± <.001 Key: IDO, idiopathic detrusor overactivity; MCC, Maximum Cystometric Capacity; FDV, Mean First Desire to Void; IIQ7, Incontinence Impact Questionnaire Short Form 7. mally invasive technique involved 20 injections at 25 units/ml per injection site into the lateral and posterior walls of the bladder while sparing the trigonal area. Then, the bladder was drained from irrigation solution and checked for any bleeding site. All patients had an indwelling urethral catheter which was removed 24 hour after the operation. The patients were observed for 2 hours after recovery from general anesthesia and then discharged with a 5 day prescription of ciprofloxacin 500 mg twice daily. Followup The patients were followed up 1 week after the injection to evaluate early post-operative complications or complaints. In the 12th week after operation, urodynamic study was performed to measure MCC and MDP. PVR urine volume was measured during urodynamic study or by bladder ultrasonography in IDO group. The participants of both groups were also asked to chart the 3 days voiding diary and QoL was reassessed by the IIQ-7. Statistical Analysis Descriptive data were evaluated by epidemiological parameters such as prevalence, mean, and standard deviation. Normality of quantitative variables (IIQ-7, clinical and urodynamic parameters) was assessed using Kolmogorov-Smirnov test. To compare normal variables between (within) IDO and NDO groups paired t test and for non-normal Mann-Whitney U (Wilcoxon test) were used. To compare categorical variables (sex, effect of drugs and adverse reactions) between groups Chi-Square test was used. P <.05 values was considered as statistically significant. RESULTS Demographic Data Of the 38 initially recruited patients, 8 were excluded from the study considering the exclusion criteria mentioned in the study design. A total of 30 patients (15 males, 15 females) remained in the study who were divided into IDO (18 patients) and NDO (12 patients) groups. The mean age of the participants in the IDO and NDO groups were ± years and ± years, respectively which were comparable. The age range of the patients was 18 to 74 years. In the IDO group, 14 patients (77.77%) were female, and 4 (22.23%) were males. In the NDO group, 1 patient (8.33%) was female, and 11 (91.67%) were males. The mean duration of antimuscarinic consumption was 18.6 ± 14.5 months (4 to 60 months). The drugs were not effective in 14 (77.77%) patients in the IDO group, and in 11 (91.66%) patients of the NDO group. Adverse reactions as the causes of medical treatment cessation were 27.77% (5 patients) and 16.66% (2 patients) in the IDO and NDO groups, respectively. Post-Operation Complications In the IDO group, one (5.55%) case of urinary tract infection was detected who was treated with a course of oral antimicrobial agent according to the result of urine culture. Another patient (5.55%) developed pelvic pain one week after injection which resolved spontaneously in 3 days. In the NDO group, one patient (8.33%) developed a severe febrile urinary tract infection 3 days after injection that was successfully treated with intravenous antibiotics. None of the participants experienced acute urinary retention or significant PVR urine (in the IDO group who void themselves), generalized muscle weakness, or significant gross hematuria. Urodynamic Parameters Vol. 11 No. 01 Jan-Feb
4 Table 2. Comparison of clinical and urodynamic parameters before and after treatment in NDO patients. Before injection After injection P Mean MCC (n = 12) (n = 12) <.001 Mean Maximum Detrusor pressure, cmh 2 O ± ± Mean Pad usage ± ± Mean IIQ ± ± 1.11 <.001 Key: NDO, neurogenic detrusor overactivity; MCC, Maximum Cystometric Capacity; IIQ7, Incontinence Impact Questionnaire Short Form 7. The urodynamic parameters are shown in Tables 1 and 2. Twelve weeks after Dysport treatment, the urodynamic study revealed a significant decrease in the mean MDP and a significant increase in MCC in both groups. Although the mean MCC was significantly different between the two groups before injection (P =.000), the changes in post-injection mean MCC did not differ significantly between the two groups (P =.700) (Figure 1). Although mean MDP before and after Dysport injection decreased significantly in each group, it did not differ significantly between the IDO and NDO groups (P =.200 and.800, respectively) (Figure 2). The mean PVR was significantly increased in IDO patients after Dysport injection from 31 ml to 82.2 ml (P = 0.021). Mean First Desire to Void (FDV) was significantly increased in IDO patients following the treatment from ± ml to ± ml (P =.000) 3-Day Voiding Diary The results were analyzed as a mean of 3 days before treatment and 12 weeks after treatment. In the IDO group before the treatment, 6 patients (33.33%) complained of frequency and 13 of them (72.22%) complained of both frequency and urgency with urge incontinence. The mean frequency rate and mean pad count decreased significantly after treatment in the IDO and NDO patients, respectively (P <.001 and P =.001, respectively) (Tables 1 and 2). Quality of Life Quality of life, as assessed using the IIQ-7, improved in both groups at 12 weeks when comparing the mean IIQ-7 score after the treatment (16.22 ± 1.03) with the mean IIQ-7 score before treatment (21.64 ± 0.48), (P =.000). According to the IIQ-7, 10 patients (33.33%) did not respond to the treatment, and 20 (66.66%) patients responded to the treatment. Of the non-responders, 7 patients (48.88%) were in the IDO group and 3 patients (25%) were in the NDO group; however, the difference between 2 groups was not statistically significant (P =.400) Satisfaction Rate When all patients asked about their satisfaction following the treatments, 76.91% of NDO patients and 57.93% of IDO patients were satisfied with Dysport treatment. Satisfaction rate did not differ significantly between the two groups (P =.600). DISCUSSION OAB is a prevalent condition that affects millions of people in the world. (15) OAB symptoms including frequency and urgency, with or without urge incontinence significantly worsen the patient s QoL. Most patients and practitioners are seeking a therapeutic method which offers appropriate and durable treatment responses in addition to minimal adverse side effects. BTX relaxes the detrusor muscle by inhibiting the release of acetylcholine at the neuromuscular junction. There are seven distinct serotypes of BTX (A, B, C, D, E, F, G) but only two of them, BTX-A and B, are available for clinical use. Several studies have shown the highly beneficial effect of intradetrusor injection of BTX-A in the treatment of DO. (10,11,16,17) BTX-B has more side effects and a shorter duration of action compared with BTX-A; however, the data on BTX-B for the treatment of DO and incontinence are limited (18) and it is too early to determine whether it will have similar results to those with BTX-A. It has been proposed that BTX-A reduces the level of the nerve growth factor in the suburothelium and urine; a factor which can be responsible for induction of inflammatory processes or bladder overactivity. (19) Botox and Dysport are the available products of 1292 Miscellaneous
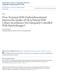
5 Intradetrusor Dysport Injection in Detrusor Overactivity Shakeri et al Figure 1. Comparison of mean maximum cystometric capacity before and after treatment in each group. Key: NDO, neurogenic detrusor overactivity; IDO, idiopathic detrusor overactivity. Figure 2. Comparison of mean maximum detrusor pressure before and after treatment in each group. Key: NDO, neurogenic detrusor overactivity; IDO, idiopathic detrusor overactivity. BTX-A which are now being used and it is suggested that each unit of Botox is equivalent to 3.5 to 5 units of Dysport. (20) To date according to published studies 100 to 400 units of Botox and 500 to 1000 units of Dysport have been used; comparison of the results of these studies shows relatively similar subjective and objective outcomes. (21) In our study, intradetrusor injection of 500 units of Dysport had a significant therapeutic effect on both IDO and NDO patients who were refractory to oral antimuscarinic medications. In each group, a significant increase in MCC and a significant decrease in MDP were observed following treatment with Dysport. Comparing the urinary frequency rate before and after the treatment in IDO patients revealed a significant decrease after the treatment. The mean pad count in NDO patients who used pads within the intervals of urethral catheterizations was significantly decreased after Dysport injection. In IDO patients FDV was significantly increased following the treatment which is probably due to both increase in cystometric capacity and decrease in urgency. According to the IIQ-7, the patients QoLs were significantly improved in both groups following the treatment and in almost all patients; changes in the urodynamic parameters were concomitant with the improvement in patients QoLs and symptoms. Considering the mentioned results, our study confirmed the results of previous studies regarding the beneficial effects of intradetrusor injection of Dysport in patients with DO. A systematic review of the role of Botox and Dysport in the management of lower urinary tract disease was conducted by Mangera and colleagues. (22) They found a high level of evidence for the use of Botox in children and adults with NDO or IDO, but only level 1 evidence for Dysport in adults with NDO. They also concluded that the effective dose of Botox or Dysport was different when managing IDO or NDO patients. Similar results were found in another systematic review done by Chancellor and colleagues. (23) However we used Dysport in both IDO and NDO adult patients with the same dosage and found significant improvements in urodynamic parameters, lower urinary tract symptoms and QoL in both groups. Our results regarding the effectiveness of Dysport in treating both NDO and IDO patients were similar to the Chancellor and colleagues review. (23) While most of the surveys recommend about two fold dose of Dysport to treat patients with NDO than IDO, we managed both groups with the same dose. We should keep in mind that we used 500 units of Dysport for both groups which might be more than what is necessary for treating IDO patients. Although the efficacy of BTX-A injection in the treatment of DO has been proved in different studies, the number of studies comparing the effects of BTX-A injection in the two subdivisions of DO, i.e. NDO and IDO, are lacking. Popat and colleagues followed 24 patients with NDO and 31 patients with IDO 4 weeks and 16 weeks after Botox injection and found no significant differences regarding improvement in clinical and urodynamical parameters Vol. 11 No. 01 Jan-Feb
6 between the mentioned groups. (12) Kalsi and colleagues compared the QoL following intradetrusor Botox injections in IDO and NDO patients and found a similar percent improvement in QoL score for both NDO and IDO groups at 4 and 16 weeks. (13) Evaluating the patients satisfaction rates following the treatment in our study revealed that the patients with NDO were more satisfied with their treatment than those with IDO (76.91% vs %). Although this finding was not statistically significant (P =.600). There are several factors which could be explain the achievement of such results. First, the mean age of the patients with NDO was less than that of IDO patients (43.99 years vs years) which might be an explanation for a better satisfaction rate. Likewise, in a study held by Brian and colleagues evaluating the predictors of response to intradetrusor BTX-A injection in patients with IDO, it was found that younger patients with incontinence were more likely to respond. (24) The second point that should be taken into account is that the patients with NDO in our study had a higher mean MDP and a lesser mean MCC before treatment as compared to the patients with IDO (39.1 cmh 2 O vs cmh 2 O) and (101.3 ml vs ml). It seems that these more abnormal urodynamic parameters in NDO groups responded better to Dysport injection, causing more satisfactory results. Similarly, Sahai and colleagues in their survey found that poor responders to BTX-A injection had significantly higher MDP during DO; (25) however, a confounding factor in their study was that patients participating in that study continued antimuscarinic consumption even after BTX-A injection. With respect to the urodynamic parameters in our study, although the improvements in mean MDP and mean MCC in each group were statistically significant, comparing both groups changes did not differ significantly. Voiding dysfunction and especially urinary retention can be one of the complications after BTX-A injection which is due to the muscle paralysis caused by this substance. In a study by Stephen Jeffery and colleagues a high incidence of voiding dysfunction was reported following injection of 500 units of Dysport in IDO patients which 36% of them required catheterization in 6 weeks and 36 months after injection. (26) The incidence of retention following Dysport injection was 19% in the study held by Popat and colleagues. (12) In our study, the mean PVR urine was significantly increased in IDO patients after Dysport injection from 31 ml to 82.2 ml; however, we did not notice any episodes of urinary retention in our IDO group following the treatment and all the IDO patients voided successfully. Transient muscle weakness is another complication after Dysport injection mentioned in some studies, (26,27,28) but this complication also was not detected in our patients. According to these results, although intradetrusor injection of Dysport was an effective treatment modality for both groups, we did not find any priority for Dysport injection between NDO and IDO patients. Our study is not without limitations. Although neurogenic and idiopathic detrusor overactivity can cause the same clinical symptoms, their pathophysiology and severity of symptoms are different which make the comparison of both groups difficult. In our study the gender and severity of symptoms in both groups were not statistically comparable which can cause a selection bias while comparing both groups. We are also aware that some insignificant findings in our results can be due to small sample which resulted in low study power. CONCLUSION Considering our results and also previous studies, there is no doubt about the valuable effects of BTX-A and especially Dysport in our study in alleviating the signs and symptoms of patients suffering from DO by improving their urodynamic parameters; however, more studies are needed to compare the effects of BTX-A in NDO and IDO patients. ACKNOWLEDGEMENT The authors would like to thank Dr. Abdolreza Haghpanah, for his support, time and consideration. CONFLICT OF INTEREST None declared. REFERENCES 1. Brubaker Linda. Urgency: The cornerstone symptom of overactive bladder. Urology. 2004;64(Suppl 6A): Irwin DE, Milsom I, Hanskaar S, et al. Population-based survey of urinary incontinence, overactive bladder, and other lower urinary tract symptoms in five countries: results of the EPIC study. Eur Urol. 2006;50: Aslan G, Köseoğlu H, Sadik O, Gimen S, Cihan A, Esen A. Sexual function in women with urinary incontinence. Int J Impot Res. 2005;17: Miscellaneous
7 Intradetrusor Dysport Injection in Detrusor Overactivity Shakeri et al 4. Kim YH, Seo JT, Yoon H. The effect of overactive bladder syndrome on the sexual quality of life in Korean young and middle aged women. Int J Impo Res. 2005;17: Liberman JN, Hunt TL, Stewart WF, et al. Health-related quality of life among adults with symptoms of overactive bladder: results from a US community-based survey. Urology. 2001;57: Sand PK, Dmochowski R. Analysis of the standardisation of terminology of lower urinary tract dysfunction: Report from the standardisation sub-committee of the international continence society. Neurourol Urodynam. 2002;21: Andersson KE. Antimuscarinics for treatment of over active bladder. Lancet Neurol. 2004;3: Flood HD, Malhotra SJ, O'Connell HE, Ritchey MJ, Bloom DA, McGuire EJ. Long term results and complications using augmentation cystoplasty and reconstruction urology. Neurourol Urodyn. 1995;14: Dickson EC, Shevky R. Studies on manner in which the toxin of clostridium botulinum acts upon the body. The effect upon the autonomic nervous system. J Exp Med. 1923;37: Sahai A, Shamim Khan M, Dasgupta P. Efficacy of botulinium toxin- A for treating idiopathic detrusor overactivity: Results from a single center, randomized, double blind, placebo controlled trial. J Urol. 2007;177: Patki PS, Hamid R, Arumugam K, Shah PJ, Craggs M. Botulinum toxin-type A in the treatment of drug resistant neurogenic detrusor overactivity secondary to traumatic spinal cord injury. BJU Int. 2006;98: Popat R, Apostolidis A, Kalsi V, Gonzales G, Fowler CJ, Dasgupta P. A comparison between the response of patients with idiopathic detrusor overactivity and neurogenic detrusor overactivity to the first intradetrusor injection of botulinum-a toxin. J Urol. 2005;174: Kalsi V, Apostolidis A, Popat R, Gonzales G, Fowler CJ, Dasgupta P. Quality of life changes in patients with neurogenic versus idiopathic detrusor overactivity after intradetrusor injection of butolinum neurotoxin type A and correlations with lower urinary tract symptoms and urodynamic changes. Eur Urol. 2006;49: Schäfer W, Abrams P, Liao L, et al. Good urodynamic practices: uroflowmetry, filling cystometry, and pressure-flow studies. Neurourol Urodyn. 2002;21: Milsom I, Abrams P, Cardozo L, Roberts RG, Thüroff J, Wein AJ. How widespread are the symptoms of an overactive bladder and how are they managed? A population-based prevalence study. BJU Int. 2001;87: Schurch B, de Sèze M, Denys P, et al. Botulinum toxin type A is a safe and effective treatment for neurogenic urinary incontinence: results of a single treatment, randomized, placebo controlled 6-month study. J Urol. 2005;174: Ghei M, Maraj BH, Miller R, et al. Effects of botulinum toxin B on refractory detrusor overactivity: A randomized, double-blind, placebo controlled, crossover trial. J Urol. 2005;174: Liu HT, Chancellor MB, Kuo H. Urinary nerve growth factor levels are elevated in patients with detrusor overactivity and decreased in responders to detrusor botulinum toxin-a injection. Eur Urol. 2009;56: Grosse J, Kramer G, Tong TQT, Stohrer M, Jakse G. Efficacy, dosage and safety of Dysport English botulinum toxin A in severe neurogenic detrusor overactivity. Eur Urol. 2005; suppl. 4:Abst # Rapp DE, Lucioni A, Bales GT. Botulinum toxin injection: a review of injection principles and protocols. Int Braz J Urol. 2007;33: Magnera A, Andesson KE, Apostolidis A, et al. Contemporary management of lower urinary tract disease with botulinum toxin A: a systematic review of botox (onabotulinumtoxina) and dysport (abobotulinumtoxina). Eur Urol. 2011;60: Chancellor MB, Elovic E, Esquenazi A, et al. Evidence-Based Review and Assessment of Butolinum Neurotoxin for the Treatment of Urologic Conditions. Toxicon. 2013;67: Cohen BL, Caruso DJ, Kanagarajah P, Gousse AE. Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive Bladder. Adv Urol. 2009: Sahai A, Khan MS, Le Gall N, Dasgupta P; GKT Botulinum Study Group. Urodynamic Assessment of Poor Responders After Botulinum Toxin-A Treatment for Overactive Bladder. Urology. 2008;71: Jeffery S, Fynes M, Lee F, Wang K, Williams L, Morley R. Efficacy and complications of intradetrusor injection with botulinum toxin A in patients with refractory idiopathic detrusor overactivity. BJU Int. 2007;100: Ruffion A, Capelle O, Paparel P, Leriche B, Leriche A, Grise P. What is the optimum dose of type A botulinum toxin for treating neurogenic bladder overactivity? BJU Int. 2006;97: Grosse J, Kramer G, Stohrer M. Success of repeat detrusor injections of botulinum A toxin in patients with severe neurogenic detrusor overactivity and incontinence. Eur Urol. 2005;47: Patel AK, Patterson JM, Chapple CR. Botulinum Toxin Injections for Neurogenic and Idiopathic Detrusor Overactivity: A Critical Analysis of Results. Eur Urol. 2006;50: Vol. 11 No. 01 Jan-Feb
2/9/2008. Men Women. Prevalence of OAB. Men: 16.0% Women: 16.9% Prevalence (%) < Age (years)
 Definition Botox for Overactive Bladder Donna Y. Deng Assistant Professor UCSF Department of Urology Urinary urgency With or without urge incontinence Usually with frequency & nocturia International Continence
Definition Botox for Overactive Bladder Donna Y. Deng Assistant Professor UCSF Department of Urology Urinary urgency With or without urge incontinence Usually with frequency & nocturia International Continence
Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive Bladder
 Advances in Urology Volume 2009, Article ID 328364, 4 pages doi:10.1155/2009/328364 Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive
Advances in Urology Volume 2009, Article ID 328364, 4 pages doi:10.1155/2009/328364 Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive
Hospital and Tzu Chi University, Hualien, Taiwan
 LUTS (2012) 4, 29 34 ORIGINAL ARTICLE Difficult Urination Does Not Affect the Successful Outcome after 100U OnabotulinumtoxinA Intravesical Injection in Patients with Idiopathic Detrusor Overactivity Yih-Chou
LUTS (2012) 4, 29 34 ORIGINAL ARTICLE Difficult Urination Does Not Affect the Successful Outcome after 100U OnabotulinumtoxinA Intravesical Injection in Patients with Idiopathic Detrusor Overactivity Yih-Chou
Hasheminejad Kidney Center (HKC), Iran University of Medical Sciences (IUMS), Tehran, Iran
 ORIGINAL ARTICLE Vol. 43 (6): 1122-1128, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0622 Abobotulinum - a toxin injection in patients with refractory idiopathic detrusor overactivity:
ORIGINAL ARTICLE Vol. 43 (6): 1122-1128, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0622 Abobotulinum - a toxin injection in patients with refractory idiopathic detrusor overactivity:
Adverse Events of Intravesical Botulinum Toxin A Injections for Idiopathic Detrusor Overactivity: Risk Factors and Influence on Treatment Outcome
 EUROPEAN UROLOGY 58 (2010) 919 926 available at www.sciencedirect.com journal homepage: www.europeanurology.com Incontinence Adverse Events of Intravesical Botulinum Toxin A Injections for Idiopathic Detrusor
EUROPEAN UROLOGY 58 (2010) 919 926 available at www.sciencedirect.com journal homepage: www.europeanurology.com Incontinence Adverse Events of Intravesical Botulinum Toxin A Injections for Idiopathic Detrusor
Botulinum toxin-a for the treatment of overactive bladder: UK contributions
 473096URO6210.1177/2051415812473096Journal of Clinical UrologySeth et al. 2013 Original Article Botulinum toxin-a for the treatment of overactive bladder: UK contributions Journal of Clinical Urology 6(2)
473096URO6210.1177/2051415812473096Journal of Clinical UrologySeth et al. 2013 Original Article Botulinum toxin-a for the treatment of overactive bladder: UK contributions Journal of Clinical Urology 6(2)
Prospective randomized trial of 100u vs 200u botox in the treatment of idiopathic overactive bladder
 Original Article Prospective randomized trial of vs botox in the treatment of idiopathic overactive bladder Waleed AlTaweel, Alaa Mokhtar, Danny M. Rabah 1 King Faisal Specialist Hospital and Research
Original Article Prospective randomized trial of vs botox in the treatment of idiopathic overactive bladder Waleed AlTaweel, Alaa Mokhtar, Danny M. Rabah 1 King Faisal Specialist Hospital and Research
GOVINDARAJ N. RAJKUMAR, DOUGLAS R. SMALL, ABDUL W. MUSTAFA and GRAEME CONN Department of Urology, Southern General Hospital, Glasgow, UK
 Original Article BTXA IN DETRUSOR FOR REFRACTORY IDIOPATHIC DOA RAJKUMAR et al. A prospective study to evaluate the safety, tolerability, efficacy and durability of response of intravesical injection of
Original Article BTXA IN DETRUSOR FOR REFRACTORY IDIOPATHIC DOA RAJKUMAR et al. A prospective study to evaluate the safety, tolerability, efficacy and durability of response of intravesical injection of
Botulinum Toxin: Applications in Urology
 Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
Overactive Bladder (OAB) and Quality of Life
 Overactive Bladder (OAB) and Quality of Life Dr. Byron Wong MBBS (Sydney), FRCSEd, FRCSEd (Urol), FCSHK, FHKAM (Surgery) Specialist in Urology Central Urology Clinic Hong Kong Continence Society Annual
Overactive Bladder (OAB) and Quality of Life Dr. Byron Wong MBBS (Sydney), FRCSEd, FRCSEd (Urol), FCSHK, FHKAM (Surgery) Specialist in Urology Central Urology Clinic Hong Kong Continence Society Annual
Use of the Botulinum Toxin A in the Treatment of the Neurogenic Detrusor Overactivity
 Use of the Botulinum Toxin A in the Treatment of the Neurogenic Detrusor Overactivity Editorial Raluca Borcăiaș 1,2, A. Manu-Marin 3, S. Nedelea 1,2, S. Rascu 1,2, V. Jinga 1,2 1 Prof. Dr. Th. Burghele
Use of the Botulinum Toxin A in the Treatment of the Neurogenic Detrusor Overactivity Editorial Raluca Borcăiaș 1,2, A. Manu-Marin 3, S. Nedelea 1,2, S. Rascu 1,2, V. Jinga 1,2 1 Prof. Dr. Th. Burghele
REVIEW ARTICLE. Botulinum-A Toxin s efficacy in the treatment of idiopathic overactive bladder
 76 REVIEW ARTICLE Botulinum-A Toxin s efficacy in the treatment of idiopathic overactive bladder Marius Alexandru Moga, 1 Simona Banciu, 2 Oana Dimienescu, 3 Nicusor-Florin Bigiu, 4 Ioan Scarneciu 5 Abstract
76 REVIEW ARTICLE Botulinum-A Toxin s efficacy in the treatment of idiopathic overactive bladder Marius Alexandru Moga, 1 Simona Banciu, 2 Oana Dimienescu, 3 Nicusor-Florin Bigiu, 4 Ioan Scarneciu 5 Abstract
Philadelphia College of Osteopathic Medicine. Victoria J. Kopec Philadelphia College of Osteopathic Medicine,
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 Does Treatment With OnabotulinumtoxinA
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 Does Treatment With OnabotulinumtoxinA
EUROPEAN UROLOGY 57 (2010)
 EUROPEAN UROLOGY 57 (2010) 891 896 available at www.sciencedirect.com journal homepage: www.europeanurology.com Incontinence Complete Continence after Botulinum Neurotoxin Type A Injections for Refractory
EUROPEAN UROLOGY 57 (2010) 891 896 available at www.sciencedirect.com journal homepage: www.europeanurology.com Incontinence Complete Continence after Botulinum Neurotoxin Type A Injections for Refractory
How to assess and predict success or failure of intra-detrusor injections with onabotulinumtoxina
 Reviews How to assess and predict success or failure of intra-detrusor injections with onabotulinumtoxina Mikolaj Przydacz A F, Tomasz Golabek A,E,F, Piotr Chlosta A,E,F Department of Urology, Jagiellonian
Reviews How to assess and predict success or failure of intra-detrusor injections with onabotulinumtoxina Mikolaj Przydacz A F, Tomasz Golabek A,E,F, Piotr Chlosta A,E,F Department of Urology, Jagiellonian
OnabotulinumtoxinA for the treatment of overactive bladder
 OnabotulinumtoxinA for the treatment of overactive bladder Clin. Invest. (2014) 4(3), 281 286 OnabotulinumtoxinA has recently been granted a license for use in overactive bladder (OAB). This review assesses
OnabotulinumtoxinA for the treatment of overactive bladder Clin. Invest. (2014) 4(3), 281 286 OnabotulinumtoxinA has recently been granted a license for use in overactive bladder (OAB). This review assesses
Managing urinary morbidity after brachytherapy. Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester
 Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
Tuesday 24 June Poster Session 1: Voiding Dysfunction Chairmen: C. Chapple and L. Stewart
 Tuesday 24 June 10.30 11.30 Poster Session 1: Voiding Dysfunction Chairmen: C. Chapple and L. Stewart P001 Can oral antibiotic prophylaxis reduce the rate of infection after conventional urodynamic studies?
Tuesday 24 June 10.30 11.30 Poster Session 1: Voiding Dysfunction Chairmen: C. Chapple and L. Stewart P001 Can oral antibiotic prophylaxis reduce the rate of infection after conventional urodynamic studies?
Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies. Dr. Boris Friedman May 2, 2012 OBJECTIVES
 Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies Dr. Boris Friedman May 2, 2012 OBJECTIVES 1) Definition and classification of MS 2) Interventional radiology
Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies Dr. Boris Friedman May 2, 2012 OBJECTIVES 1) Definition and classification of MS 2) Interventional radiology
Botulinum Toxin Injection for OAB: Indications & Technique
 Classification of LUTS Botulinum Toxin Injection for OAB: Indications & Technique Sherif Mourad, MD Professor of Urology, Ain Shams University General Secretary of International Continence President of
Classification of LUTS Botulinum Toxin Injection for OAB: Indications & Technique Sherif Mourad, MD Professor of Urology, Ain Shams University General Secretary of International Continence President of
european urology 52 (2007)
 european urology 52 (2007) 1729 1735 available at www.sciencedirect.com journal homepage: www.europeanurology.com Neuro-urology Do Repeat Intradetrusor Botulinum Toxin Type A Injections Yield Valuable
european urology 52 (2007) 1729 1735 available at www.sciencedirect.com journal homepage: www.europeanurology.com Neuro-urology Do Repeat Intradetrusor Botulinum Toxin Type A Injections Yield Valuable
Botulinum Toxin Injection: A Review of Injection Principles and Protocols
 Review Article Botulinum Toxin Injection International Braz J Urol Vol. 33 (2): 132-141, March - April, 2007 Botulinum Toxin Injection: A Review of Injection Principles and Protocols David E. Rapp, Alvaro
Review Article Botulinum Toxin Injection International Braz J Urol Vol. 33 (2): 132-141, March - April, 2007 Botulinum Toxin Injection: A Review of Injection Principles and Protocols David E. Rapp, Alvaro
Onabotulinumtoxin - A Injections for the Treatment of Neurogenic Detrusor Overactivity
 Onabotulinumtoxin - A Injections for the Treatment of Neurogenic Detrusor Overactivity Raluca Borcăiaș 1, S. Rașcu 1,2, V. Jinga 1,2, D. Mischianu 1,3, A. Manu-Marin 4 1 Carol Davila University of Medicine
Onabotulinumtoxin - A Injections for the Treatment of Neurogenic Detrusor Overactivity Raluca Borcăiaș 1, S. Rașcu 1,2, V. Jinga 1,2, D. Mischianu 1,3, A. Manu-Marin 4 1 Carol Davila University of Medicine
An Effective Day Case Treatment Combination for Refractory Neuropathic Mixed Incontinence
 Neurourology A Day Case Treatment for Neuropathic Mixed Incontinence International Braz J Urol Vol. 34(1): 63-72, January - February, 2008 An Effective Day Case Treatment Combination for Refractory Neuropathic
Neurourology A Day Case Treatment for Neuropathic Mixed Incontinence International Braz J Urol Vol. 34(1): 63-72, January - February, 2008 An Effective Day Case Treatment Combination for Refractory Neuropathic
The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence
 european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
Botulinum-AToxin Detrusor and Sphincter Injection in Treatment of Overactive Bladder Syndrome: Objective Outcome and Patient Satisfaction
 European Urology European Urology 48 (2005) 984 990 Botulinum-AToxin Detrusor and Sphincter Injection in Treatment of Overactive Bladder Syndrome: Objective Outcome and Patient Satisfaction Heinrich Schulte-Baukloh
European Urology European Urology 48 (2005) 984 990 Botulinum-AToxin Detrusor and Sphincter Injection in Treatment of Overactive Bladder Syndrome: Objective Outcome and Patient Satisfaction Heinrich Schulte-Baukloh
SELECTED POSTER PRESENTATIONS
 SELECTED POSTER PRESENTATIONS The following summaries are based on posters presented at the American Urogynecological Society 2004 Scientific Meeting, held July 29-31, 2004, in San Diego, California. CENTRAL
SELECTED POSTER PRESENTATIONS The following summaries are based on posters presented at the American Urogynecological Society 2004 Scientific Meeting, held July 29-31, 2004, in San Diego, California. CENTRAL
BOTULINUM TOXIN IN LOWER URINARY TRACT
 BOTULINUM TOXIN IN LOWER URINARY TRACT Selcuk Yucel, MD Professor in Urology and Pediatric Urology Acibadem University School of Medicine Department of Uroloy and Pediatric Urology Acibadem University
BOTULINUM TOXIN IN LOWER URINARY TRACT Selcuk Yucel, MD Professor in Urology and Pediatric Urology Acibadem University School of Medicine Department of Uroloy and Pediatric Urology Acibadem University
Efficacy of botulinum-a toxin in the treatment of detrusor overactivity incontinence: A prospective nonrandomized study
 American Journal of Obstetrics and Gynecology (2005) 192, 1735 40 www.ajog.org Efficacy of botulinum-a toxin in the treatment of detrusor overactivity incontinence: A prospective nonrandomized study Matthias
American Journal of Obstetrics and Gynecology (2005) 192, 1735 40 www.ajog.org Efficacy of botulinum-a toxin in the treatment of detrusor overactivity incontinence: A prospective nonrandomized study Matthias
Botulinum Toxin Treatment for Overactive Bladder: Efficacy, Mechanism of Action, Techniques and Practical Tips W16, 15 October :00-17:00
 Botulinum Toxin Treatment for Overactive Bladder: Efficacy, Mechanism of Action, Techniques and Practical Tips W16, 15 October 2012 14:00-17:00 Start End Topic Speakers 14:00 14:15 Introduction Mohammad
Botulinum Toxin Treatment for Overactive Bladder: Efficacy, Mechanism of Action, Techniques and Practical Tips W16, 15 October 2012 14:00-17:00 Start End Topic Speakers 14:00 14:15 Introduction Mohammad
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
ABSTRACT ORIGINAL RESEARCH
 Adv Ther (2013) 30:819 833 DOI 10.1007/s25-013-0054-z ORIGINAL RESEARCH OnabotulinumtoxinA is Effective in Patients with Urinary Incontinence due to Neurogenic Detrusor Activity Regardless of Concomitant
Adv Ther (2013) 30:819 833 DOI 10.1007/s25-013-0054-z ORIGINAL RESEARCH OnabotulinumtoxinA is Effective in Patients with Urinary Incontinence due to Neurogenic Detrusor Activity Regardless of Concomitant
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH
 TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH CONTENTS Overactive bladder (OAB) Treatment of OAB Beta-3 adrenoceptor agonist (Betmiga ) - Panacea? LASER treatment - a flash in the pan or the
TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH CONTENTS Overactive bladder (OAB) Treatment of OAB Beta-3 adrenoceptor agonist (Betmiga ) - Panacea? LASER treatment - a flash in the pan or the
Outcome of a Randomized, Double-Blind, Placebo Controlled Trial of Botulinum A Toxin for Refractory Overactive Bladder
 Outcome of a Randomized, Double-Blind, Placebo Controlled Trial of Botulinum A Toxin for Refractory Overactive Bladder Michael K. Flynn,* Cindy L. Amundsen, MaryAnn Perevich, Fan Liu and George D. Webster
Outcome of a Randomized, Double-Blind, Placebo Controlled Trial of Botulinum A Toxin for Refractory Overactive Bladder Michael K. Flynn,* Cindy L. Amundsen, MaryAnn Perevich, Fan Liu and George D. Webster
Multiple Sclerosis. Véronique Phé, MD, PhD Pitié-Salpêtrière Academic Hospital Department of Urology Paris 6 University Paris, FRANCE
 Queen Square Uro-neurology course, London, UK 20 th -21 st October 2016 Multiple Sclerosis Véronique Phé, MD, PhD Pitié-Salpêtrière Academic Hospital Department of Urology Paris 6 University Paris, FRANCE
Queen Square Uro-neurology course, London, UK 20 th -21 st October 2016 Multiple Sclerosis Véronique Phé, MD, PhD Pitié-Salpêtrière Academic Hospital Department of Urology Paris 6 University Paris, FRANCE
UK Consensus on Bladder Management in MS
 Continence Care Forum Annual Conference UK Consensus on Bladder Management in MS Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Association of British Neurologists
Continence Care Forum Annual Conference UK Consensus on Bladder Management in MS Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Association of British Neurologists
A Simplified Technique for Botulinum Toxin Injections in Children With Neurogenic Bladder
 A Simplified Technique for Botulinum Toxin Injections in Children With Neurogenic Bladder Maria Paola Pascali, Giovanni Mosiello,* Armando Marciano, Maria Luisa Capitanucci, Antonio Maria Zaccara and Mario
A Simplified Technique for Botulinum Toxin Injections in Children With Neurogenic Bladder Maria Paola Pascali, Giovanni Mosiello,* Armando Marciano, Maria Luisa Capitanucci, Antonio Maria Zaccara and Mario
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
Validation of a simple patient questionnaire to assist self-detection of overactive bladder
 æoriginal PAPER Validation of a simple patient questionnaire to assist self-detection of overactive bladder A study in general practice Arnfinn Seim 1, Trygve Talseth 2, Harriet Haukeland 3, Kjetil Høye
æoriginal PAPER Validation of a simple patient questionnaire to assist self-detection of overactive bladder A study in general practice Arnfinn Seim 1, Trygve Talseth 2, Harriet Haukeland 3, Kjetil Høye
Management, Evaluation, and Treatment of Overactive Bladder and Urinary Incontinence
 Management, Evaluation, and Treatment of Overactive Bladder and Urinary Incontinence Arthur Mourtzinos, MD, MBA Co-Vice Chair, Institute of Urology Director, Continence Center Assistant Professor of Urology,
Management, Evaluation, and Treatment of Overactive Bladder and Urinary Incontinence Arthur Mourtzinos, MD, MBA Co-Vice Chair, Institute of Urology Director, Continence Center Assistant Professor of Urology,
Effect of Desmopressin with Anticholinergics in Female Patients with Overactive Bladder
 www.kjurology.org DOI:10.4111/kju.2011.52.6.396 Voiding Dysfunction Effect of Desmopressin with Anticholinergics in Female Patients with Overactive Bladder Young Kook Han, Won Ki Lee, Seong Ho Lee, Dae
www.kjurology.org DOI:10.4111/kju.2011.52.6.396 Voiding Dysfunction Effect of Desmopressin with Anticholinergics in Female Patients with Overactive Bladder Young Kook Han, Won Ki Lee, Seong Ho Lee, Dae
Urodynamic findings in women with insensible incontinence
 bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
3/20/10. Prevalence of OAB Men: 16.0% Women: 16.9% Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Dry. Population (millions) Wet
 1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Overactive Bladder; OAB. Aδ silent C. Adenosine triphosphate; ATP SD g n Key words
 25-32 2009 SD 200-270g n 28 4 1 2 3 4 PE-50 4-5 0.25 60 C Key words acupuncture stimulation overactive bladder rat bladder irritation C C fiber Received November 17, 2008; Accepted January 9, 2009 I Overactive
25-32 2009 SD 200-270g n 28 4 1 2 3 4 PE-50 4-5 0.25 60 C Key words acupuncture stimulation overactive bladder rat bladder irritation C C fiber Received November 17, 2008; Accepted January 9, 2009 I Overactive
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
The International Continence Society
 REPORTS Safety and Tolerability of Tolterodine for the Treatment of Overactive Bladder in Adults Richard G. Roberts, MD, JD; Alan D. Garely, MD; and Tamara Bavendam, MD Abstract This article evaluates
REPORTS Safety and Tolerability of Tolterodine for the Treatment of Overactive Bladder in Adults Richard G. Roberts, MD, JD; Alan D. Garely, MD; and Tamara Bavendam, MD Abstract This article evaluates
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline.
 Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder
 European Urology European Urology 48 (2005) 110 115 Female UrologyöIncontinence Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder Martin
European Urology European Urology 48 (2005) 110 115 Female UrologyöIncontinence Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder Martin
Experience with Different Botulinum Toxins for the Treatment of Refractory Neurogenic Detrusor Overactivity
 Neurourology Botulinum Toxins for Refractory Detrusor Overactivity International Braz J Urol Vol. 36 (1): 66-74, January - February, 2010 doi: 10.1590/S1677-55382010000100011 Experience with Different
Neurourology Botulinum Toxins for Refractory Detrusor Overactivity International Braz J Urol Vol. 36 (1): 66-74, January - February, 2010 doi: 10.1590/S1677-55382010000100011 Experience with Different
INTRAVESICAL INJECTION OF BOTULINUM TOXIN TYPE A: MANAGEMENT OF NEUROPATHIC BLADDER AND BOWEL DYSFUNCTION IN CHILDREN WITH MYELOMENINGOCELE
 PEDIATRIC UROLOGY INTRAVESICAL INJECTION OF BOTULINUM TOXIN TYPE A: MANAGEMENT OF NEUROPATHIC BLADDER AND BOWEL DYSFUNCTION IN CHILDREN WITH MYELOMENINGOCELE ABDOL-MOHAMMAD KAJBAFZADEH, SHAHRAM MOOSAVI,
PEDIATRIC UROLOGY INTRAVESICAL INJECTION OF BOTULINUM TOXIN TYPE A: MANAGEMENT OF NEUROPATHIC BLADDER AND BOWEL DYSFUNCTION IN CHILDREN WITH MYELOMENINGOCELE ABDOL-MOHAMMAD KAJBAFZADEH, SHAHRAM MOOSAVI,
Urinary incontinence (UI), a prevalent condition affecting
 JOURNAL OF GYNECOLOGIC SURGERY Volume 29, Number 5, 2013 ª Mary Ann Liebert, Inc. DOI: 10.1089/gyn.2012.0134 Tension-Free Vaginal Tape Plus Intradetrusor BOTOX â Injection Versus Tension-Free Vaginal Tape
JOURNAL OF GYNECOLOGIC SURGERY Volume 29, Number 5, 2013 ª Mary Ann Liebert, Inc. DOI: 10.1089/gyn.2012.0134 Tension-Free Vaginal Tape Plus Intradetrusor BOTOX â Injection Versus Tension-Free Vaginal Tape
EMR template and postprocedure notes
 EMR template and postprocedure notes Sample autopopulated text to create a BOTOX injection procedure report Information gathered from market research. These considerations are for reference only and should
EMR template and postprocedure notes Sample autopopulated text to create a BOTOX injection procedure report Information gathered from market research. These considerations are for reference only and should
Diagnosis and Mangement of Nocturia in Adults
 Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
PRE-OPERATIVE URODYNAMIC
 PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder
 Urol Sci 21;21(1):38 43 ORIGINAL ARTICLE Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder Yih-Chou Chen, Chia-Yen Chen, Hann-Chorng
Urol Sci 21;21(1):38 43 ORIGINAL ARTICLE Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder Yih-Chou Chen, Chia-Yen Chen, Hann-Chorng
BOTOX (onabotulinumtoxina) for Therapeutic Use
 BOTOX (onabotulinumtoxina) for Therapeutic Use BOTOX (onabotulinumtoxina) & BOTOX Cosmetic (onabotulinumtoxina) Important Information IMPORTANT SAFETY INFORMATION BOTOX and BOTOX Cosmetic may cause serious
BOTOX (onabotulinumtoxina) for Therapeutic Use BOTOX (onabotulinumtoxina) & BOTOX Cosmetic (onabotulinumtoxina) Important Information IMPORTANT SAFETY INFORMATION BOTOX and BOTOX Cosmetic may cause serious
Introduction. Spinal Cord Injury (SCI) Is it necessary to perform surveillance investigations for long term follow up of spinal cord injury patients?
 Is it necessary to perform surveillance investigations for long term follow up of spinal cord injury patients? Rizwan Hamid MBBS, FRCSEd, FRCS(Urol), MD(Res) Honorary Senior Lecturer & Consultant Urologist
Is it necessary to perform surveillance investigations for long term follow up of spinal cord injury patients? Rizwan Hamid MBBS, FRCSEd, FRCS(Urol), MD(Res) Honorary Senior Lecturer & Consultant Urologist
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
GUIDELINES ON URINARY INCONTINENCE
 12 GUIDELINES ON URINARY INCONTINENCE (Text updated March 2005) J. Thüroff, (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck Introduction The condition
12 GUIDELINES ON URINARY INCONTINENCE (Text updated March 2005) J. Thüroff, (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck Introduction The condition
Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions?
 Review Article SENSORY ACTIONS OF ANTIMUSCARINICS FINNEY et al. Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions? STEVEN M. FINNEY, KARL-ERIK
Review Article SENSORY ACTIONS OF ANTIMUSCARINICS FINNEY et al. Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions? STEVEN M. FINNEY, KARL-ERIK
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
Use of botulinum toxin for voiding dysfunction
 Review Article Use of botulinum toxin for voiding dysfunction David Eldred-Evans, Prokar Dasgupta Department of Urology, Medical Research Council (MRC) Centre for Transplantation, King s College London,
Review Article Use of botulinum toxin for voiding dysfunction David Eldred-Evans, Prokar Dasgupta Department of Urology, Medical Research Council (MRC) Centre for Transplantation, King s College London,
Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity
 ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Comparison of Side Effects of Tolterodine and Solifenacinsucinate in Patients with Urinary Incontinence
 ORIGINAL ARTICLE Comparison of Side Effects of Tolterodine and Solifenacinsucinate in Patients with Urinary Incontinence MARYAM RANA, IRAM MOBUSHER ABSTRACT Background: Overactive bladder syndrome is a
ORIGINAL ARTICLE Comparison of Side Effects of Tolterodine and Solifenacinsucinate in Patients with Urinary Incontinence MARYAM RANA, IRAM MOBUSHER ABSTRACT Background: Overactive bladder syndrome is a
BJUI. Validity and reliability of the patient s perception of intensity of urgency scale in overactive bladder
 ; 2010 Lower Urinary Tract PATIENT S PERCEPTION OF INTENSITY OF URGENCY SCALE IN OAB CARTWRIGHT ET AL. BJUI Validity and reliability of the patient s perception of intensity of urgency scale in overactive
; 2010 Lower Urinary Tract PATIENT S PERCEPTION OF INTENSITY OF URGENCY SCALE IN OAB CARTWRIGHT ET AL. BJUI Validity and reliability of the patient s perception of intensity of urgency scale in overactive
Anticholinergic medication use for female overactive bladder in the ambulatory setting in the United States.
 Página 1 de 6 PubMed darifenacin vs solifenacin Display Settings:, Sorted by Recently Added Results: 5 1. Int Urogynecol J. 2013 Oct 25. [Epub ahead of print] Anticholinergic medication use for female
Página 1 de 6 PubMed darifenacin vs solifenacin Display Settings:, Sorted by Recently Added Results: 5 1. Int Urogynecol J. 2013 Oct 25. [Epub ahead of print] Anticholinergic medication use for female
GUIDELINES ON URINARY INCONTINENCE
 GUIDELINES ON URINARY INCONTINENCE 9 J. Thüroff, (chairman), P. Abrams, J-T. Andersen, W. Artibani, E. Chartier-Kastler, C. Hampel, M. Hohenfellner, T. Tammela, Ph. van Kerrebroeck Introduction The condition
GUIDELINES ON URINARY INCONTINENCE 9 J. Thüroff, (chairman), P. Abrams, J-T. Andersen, W. Artibani, E. Chartier-Kastler, C. Hampel, M. Hohenfellner, T. Tammela, Ph. van Kerrebroeck Introduction The condition
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging
 Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Urinary Incontinence for the Primary Care Provider
 Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Possible Effect of Carbamazepine A Sodium Channel Blocker on Urinary Bladder Dysfunction in Type-1 Diabetic Patients
 Med. J. Cairo Univ., Vol. 84, No. 1, March: 85-90, 2016 www.medicaljournalofcairouniversity.net Possible Effect of Carbamazepine A Sodium Channel Blocker on Urinary Bladder Dysfunction in Type-1 Diabetic
Med. J. Cairo Univ., Vol. 84, No. 1, March: 85-90, 2016 www.medicaljournalofcairouniversity.net Possible Effect of Carbamazepine A Sodium Channel Blocker on Urinary Bladder Dysfunction in Type-1 Diabetic
Urodynamic Results of Sacral Neuromodulation Correlate with Subjective Improvement in Patients with an Overactive Bladder
 European Urology European Urology 43 (2003) 282±287 Urodynamic Results of Sacral Neuromodulation Correlate with Subjective Improvement in Patients with an Overactive Bladder W.A. Scheepens a, G.A. van
European Urology European Urology 43 (2003) 282±287 Urodynamic Results of Sacral Neuromodulation Correlate with Subjective Improvement in Patients with an Overactive Bladder W.A. Scheepens a, G.A. van
Voiding Dysfunction. Yao-Chi Chuang,* Jonathan H. Kaufmann, David D. Chancellor, Michael B. Chancellor and Hann-Chorng Kuo,k
 Voiding Dysfunction Bladder Instillation of Liposome Encapsulated OnabotulinumtoxinA Improves Overactive Bladder Symptoms: A Prospective, Multicenter, Double-Blind, Randomized Trial Yao-Chi Chuang,* Jonathan
Voiding Dysfunction Bladder Instillation of Liposome Encapsulated OnabotulinumtoxinA Improves Overactive Bladder Symptoms: A Prospective, Multicenter, Double-Blind, Randomized Trial Yao-Chi Chuang,* Jonathan
european urology 53 (2008)
 european urology 53 (2008) 275 287 available at www.sciencedirect.com journal homepage: www.europeanurology.com Review Neuro-urology Botulinum Toxin A (Botox W ) Intradetrusor Injections in Adults with
european urology 53 (2008) 275 287 available at www.sciencedirect.com journal homepage: www.europeanurology.com Review Neuro-urology Botulinum Toxin A (Botox W ) Intradetrusor Injections in Adults with
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
The Successful and Novel Treatment of Non-Neurogenic Detrusor- External Sphincter Dyssynergia (DESD) with Botulinum Toxin A
 original article The Successful and Novel Treatment of Non-Neurogenic - External Sphincter Dyssynergia (DESD) with Botulinum Toxin A Tricia LC Kuo, MBBS, MRCSEd, M Med (Surg), FAMS, Lay Guat Ng, MBBS,
original article The Successful and Novel Treatment of Non-Neurogenic - External Sphincter Dyssynergia (DESD) with Botulinum Toxin A Tricia LC Kuo, MBBS, MRCSEd, M Med (Surg), FAMS, Lay Guat Ng, MBBS,
Additional low-dose antimuscarinics can improve overactive bladder symptoms in patients with suboptimal response to beta 3 agonist monotherapy
 Original Article - Female Urology Investig Clin Urol Posted online 217.6.27 Posted online 217.6.27 pissn 2466-493 eissn 2466-54X Additional low-dose antimuscarinics can improve overactive bladder symptoms
Original Article - Female Urology Investig Clin Urol Posted online 217.6.27 Posted online 217.6.27 pissn 2466-493 eissn 2466-54X Additional low-dose antimuscarinics can improve overactive bladder symptoms
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA
 Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
/05/ /0 Vol. 174, , July 2005 THE JOURNAL OF UROLOGY. Printed in U.S.A. Copyright 2005 by AMERICAN UROLOGICAL ASSOCIATION
 0022-5347/05/1741-0196/0 Vol. 174, 196 200, July 2005 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2005 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000162035.73977.1c BOTULINUM TOXIN TYPE
0022-5347/05/1741-0196/0 Vol. 174, 196 200, July 2005 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2005 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000162035.73977.1c BOTULINUM TOXIN TYPE
Urogynecology Office. Can You Hold? An Update on the Treatment of OAB. Can You Hold? Urogynecology Office
 Urogynecology Office Urogynecology Office Can You Hold? An Update on the Treatment of OAB Can You Hold? Karen Noblett, MD Professor and Chair Department of OB/GYN University of California, Riverside Disclosures
Urogynecology Office Urogynecology Office Can You Hold? An Update on the Treatment of OAB Can You Hold? Karen Noblett, MD Professor and Chair Department of OB/GYN University of California, Riverside Disclosures
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
Urinary nerve growth factor levels could be a biomarker for overactive bladder symptom: a meta-analysis
 Urinary nerve growth factor levels could be a biomarker for overactive bladder symptom: a meta-analysis H.C. Qu, S. Yan, X.L. Zhang, X.W. Zhu, Y.L. Liu and P. Wang Department of Urological Surgery, The
Urinary nerve growth factor levels could be a biomarker for overactive bladder symptom: a meta-analysis H.C. Qu, S. Yan, X.L. Zhang, X.W. Zhu, Y.L. Liu and P. Wang Department of Urological Surgery, The
Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in children
 ORIGINAL ARTICLE Vol. 41 (4): 739-743, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0303 Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in
ORIGINAL ARTICLE Vol. 41 (4): 739-743, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0303 Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in
EFFECTS OF BOTULINUM TOXIN A INJECTIONS IN SPINAL CORD INJURY PATIENTS WITH DETRUSOR OVERACTIVITY AND DETRUSOR SPHINCTER DYSSYNERGIA
 J Rehabil Med 2016; 48: 683 687 ORIGINAL REPORT EFFECTS OF BOTULINUM TOXIN A INJECTIONS IN SPINAL CORD INJURY PATIENTS WITH DETRUSOR OVERACTIVITY AND DETRUSOR SPHINCTER DYSSYNERGIA Maping Huang, PhD 1,
J Rehabil Med 2016; 48: 683 687 ORIGINAL REPORT EFFECTS OF BOTULINUM TOXIN A INJECTIONS IN SPINAL CORD INJURY PATIENTS WITH DETRUSOR OVERACTIVITY AND DETRUSOR SPHINCTER DYSSYNERGIA Maping Huang, PhD 1,
EUROPEAN UROLOGY 60 (2011)
 EUROPEAN UROLOGY 60 (2011) 784 795 available at www.sciencedirect.com journal homepage: www.europeanurology.com Collaborative Review Neuro-urology Contemporary Management of Lower Urinary Tract Disease
EUROPEAN UROLOGY 60 (2011) 784 795 available at www.sciencedirect.com journal homepage: www.europeanurology.com Collaborative Review Neuro-urology Contemporary Management of Lower Urinary Tract Disease
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
Solifenacin significantly improves all symptoms of overactive bladder syndrome
 REVIEW doi: 10.1111/j.1742-1241.2006.01067.x Solifenacin significantly improves all symptoms of overactive bladder syndrome C. R. CHAPPLE, 1 L. CARDOZO, 2 W. D. STEERS, 3 F. E. GOVIER 4 1 Department of
REVIEW doi: 10.1111/j.1742-1241.2006.01067.x Solifenacin significantly improves all symptoms of overactive bladder syndrome C. R. CHAPPLE, 1 L. CARDOZO, 2 W. D. STEERS, 3 F. E. GOVIER 4 1 Department of
EAU GUIDELINES ON NEURO-UROLOGY
 EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2016) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler. Guidelines Associates:
EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2016) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler. Guidelines Associates:
