Urinary incontinence is defined (since
|
|
|
- Melvyn Simpson
- 6 years ago
- Views:
Transcription
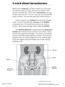
1 THE EPIDEMIOLOGY AND EVALUATION OF URINARY INCONTINENCE * David H. Thom, MD, PhD ABSTRACT The prevalence of urinary incontinence varies by definition, age, and sex. Urinary incontinence defined as leakage during 6 days in the past 12 months occurs in a mean of 41% (range, 12% to 53%) of women. For those with leakage twice per month, the prevalence is a mean of 14% (range, 5% to 37%), and for those with any frequency that the patient views as a problem, mean prevalence is 24% (range, 12% to 44%). In middle age, incontinence is much more frequent in women, but in older adults, it also becomes a health problem for men. In the 35- to 44-year-old age group, the ratio of women to men who have urinary incontinence is approximately 10:1. This ratio decreases to 1:1 in patients older than 85 years. Urine leakage usually occurs under 2 circumstances: with physical exertion, sneezing, or coughing (stress incontinence) or preceded by a strong and urgent desire to void (urge incontinence). Age, obesity, and vaginal delivery are risk factors; age appears to be the strongest predictor of incidence. Urinary incontinence often leads to social isolation, physical limitation of activities, avoidance of sexual activity, decreased work productivity, and depression. Careful patient history and physical examination constitute the basic evaluation for the condition. Because of the impact of urinary incontinence on quality of life, identification and treatment are essential. (Adv Stud Med. 2004;4(2A):S81-S87) *Based on a presentation given by Dr Thom at a symposium held in conjunction with the Pri-Med West annual meeting. Associate Professor, Department of Family and Community Medicine, University of California, San Francisco. Address correspondence to: David H. Thom, MD, PhD, 1001 Potrero, San Francisco, CA dthom@itsa.ucsf.edu. Urinary incontinence is defined (since 2002) by the International Continence Society as the complaint of any involuntary leakage of urine. 1 This definition includes any complaint from the patient of urine leakage. Of note, this definition represents the first time that objective urodynamic testing has not been required for diagnosis, thus supporting the way for urinary incontinence to be diagnosed and treated by primary care physicians. Urine leakage principally occurs under 2 conditions: with physical exertion or upon sneezing or coughing (stress incontinence) or with a strong and urgent desire to void (urge incontinence). Mixed incontinence (a combination of stress and urge incontinence) is also observed. To understand the primary underlying causes of incontinence, it is worthwhile to review the micturition cycle, which includes filling and emptying phases (reviewed in more detail by Dr Ostergard, page S88). As urine fills the bladder, the detrusor muscle relaxes, allowing the bladder to expand at low pressure, while the urethral sphincter and pelvic floor contract. A normal sensation of the desire to void is felt when approximately 400 ml to 500 ml of urine is stored. During voiding, the detrusor muscle of the bladder contracts (increasing bladder pressure) to expel the urine, and the urethral sphincter and pelvic floor relax, allowing urine passage. Urge incontinence is caused by instability of the detrusor muscle (ie, involuntary bladder contractions). Stress incontinence is caused by diminished urethral sphincter function and/or urethral hypermobility. Diminished sphincter function refers to smooth muscle dysfunction of the sphincter in the lower part of the bladder trigone and the proximal urethra (Figure 1). Urethral hypermobility refers to the loss of pelvic floor Advanced Studies in Medicine S81
2 support that maintains the anatomic position of the urethra. Both of these types of malfunctions can cause stress incontinence and can occur in the same person. Complicating diagnosis further, not every case of clinical urge incontinence is diagnosed as detrusor overactivity on examination, just as not all stress incontinence is due to a poor response to increased bladder pressure. It is possible, however, to differentiate urge from stress incontinence. As shown in Table 1, a marker of urge incontinence is nighttime wakening with urge. However, the absence of this symptom does not rule out urge incontinence. Leaking during physical activity is a diagnostic marker for stress incontinence. Urgency and leakage due to urgency are the 2 most important signs of urge incontinence. However, physical exertion, such as a Valsalva maneuver, may sometimes trigger involuntary detrusor contraction (usually associated with urge incontinence), confusing the identification of the underlying etiology. In patients with urge incontinence, a brief delay should occur between the execution of the Valsalva technique and urine loss. The amount of urine loss is also frequently higher in patients with urge incontinence compared with stress incontinence, but that detail may be obscured: sometimes the amount of urine loss with urge incontinence is small because of good sphincter control. In practice, there may be overlap among symptoms between stress, urge, and other types of incontinence. Also, urge incontinence is part of the general condition of overactive bladder, which includes urge incontinence as well as sudden, strong urges to urinate or frequent urination. Two other types of incontinence that may be encountered in primary care are overflow and functional incontinence. Overflow incontinence is due to outflow obstruction (eg, in men with enlarged prostates) or a weak detrusor contraction. It is seen rarely in women, although it occurs occasionally with severe pelvic prolapse or in women who have urethral scarring resulting from instrumentation. It is most commonly seen in people with neurologic damage from long-standing diabetes or spinal cord injury. Functional incontinence refers to incontinence not due primarily to a physiologic problem in the urogenital system but may be due to dementia or reduced mobility. DEMOGRAPHICS OF URINARY INCONTINENCE The prevalence of urinary incontinence varies by definition, age, and sex. Urinary incontinence defined as leakage during 6 days in the past 12 months occurs in a mean of 41% (range, 12% to 53%) of women. For those with leakage twice per month, the mean prevalence is 14% (range, 5% to 37%), and for those with any frequency that the patient views as a problem, mean prevalence is 24% (range, 12% to 44%). 2 Figure 1. Primary Underlying Causes of Incontinence Urge incontinence is caused by detrusor instability. Stress incontinence is caused by diminished urethral sphincter function and/or urethral hypermobility. Table 1. Symptoms Differentiating Stress from Urge Incontinence Stress Urge Symptoms Incontinence Incontinence Leaking during physical activity (coughing, sneezing, lifting) Yes Sometimes Inability to reach the toilet in time following an urge to void No Yes Urgency accompanies incontinence (strong, sudden desire to void) Seldom Often Waking at night to urinate No Yes S82 Vol. 4 (2A) February 2004
3 The prevalence of incontinence increases with age for both men and women, although the peak prevalence occurs at different ages according to sex (Figure 2). 3 The discrepancy between the sexes begins in the teen years, when urinary incontinence is more common in females than males. By middle age, incontinence is a much more frequent health condition for women, but in older adults, it also becomes a health problem for men. In the 35- to 44-year-old age group, the ratio of women to men who have incontinence is approximately 10:1. This ratio decreases to 1:1 in patients older than 85 years. 3 Type of incontinence also varies with age in women. In women younger than 60 years of age, stress incontinence accounts for 55% of cases, followed by mixed (25%) and urge incontinence (20%). These percentages change for urge (35%), mixed (35%), and stress incontinence (30%) in those older than 60 years. 4 The predominant risk factors for urinary incontinence are female sex, parity, and obesity. Vaginal delivery is the primary risk factor in women who have had 1 or more vaginal births compared with women who have had none. The prevalence of urinary incontinence up to 5 years after delivery is 30% among all women but can be as high as 92% in those who are incontinent during pregnancy or puerperium and remain incontinent 3 months after delivery. 5 The risk increases most with 1 vaginal birth and generally increases modestly with subsequent births. 6 Obesity has been found to be another factor related to the development and recurrence of incontinence. 7-9 Resolution of incontinence has been reported (albeit more subjectively) in morbidly obese women who have lost weight after bariatric surgery. 10,11 A few studies have also shown that stress incontinence may be more common in white women compared with African American women, although the studies have typically been small due to medications) or established. Established incontinence is usually refractory to medical treatment and is often caused by neurologic damage or intrinsic urinary tract dysfunction. 22 Annual direct costs of incontinence range from $16 million to $26 million (in 1995 dollars), expenditures that reflect about the same costs as those for osteoporosis or breast cancer Costs for women older than 65 years of age were more than twice the costs for those younger than 65 years ($7.6 and $3.6 billion, respectively). In those older than 60 years, the largest cost category was routine care (70% of costs for women), followed by nursing home admissions (14%), treatment (9%), complications (6%), and diagnosis and evaluation (1%). 24 The most important aspect of incontinence is its impact on quality of life. Incontinence inflicts a heavy emotional toll on patients sense of well-being, affecting several quality-of-life indicators, such as social, physical, sexual, psychological, occupational, and domestic indicators. About 25% of women report some bother from incontinence, and only a slightly smaller percentage say they are severely bothered by the symptoms. As a patient population, this represents a substantial number of women, most of whom are not being treated for the condition. Individuals with incontinence suffer from isolation, reporting that they are less likely to travel or to attend social events or visit family. For women in mid- Figure 2. Prevalence of Urinary Incontinence by Age and Sex THE BURDEN OF DISEASE Urinary incontinence is more prevalent than many of the more common chronic diseases in women, such as hypertension, depression, and diabetes (Figure 3). 2,17-19 In institutionalized patients, the prevalence is about 50%. 20,21 These patients are elderly, and their incontinence is either transient (often Adapted with permission from Thomas et al. Br Med J. 1980;281(6250): Advanced Studies in Medicine S83
4 dle age, stress incontinence specifically limits leisure activities that would be of most health benefit, such as physical exercise and sports participation. Incontinence also leads to avoidance of sexual activity, and its association with depression and loss of selfesteem is fairly strong. Decreased productivity has been linked to stress urinary incontinence. For some women, certain jobs are prohibitive because of inadequate access to bathrooms or allowance for the requisite number of bathroom breaks. Urinary incontinence has become such a pervasive influence on quality of life that it has been proposed as a basis for outcomes measures among patients in nursing homes. 26 EVALUATION The basic evaluation for incontinence is based on a thorough history (including a voiding diary) and physical examination with urinalysis. HISTORY Obtaining patient history involves asking medical, neurologic, and genitourinary questions to rule out diabetes, congestive heart failure, stroke, neurologic disorders, and pelvic organ prolapse. A surgical history is also important, regarding surgery in the abdomen or pelvic area. 27,28 A complete list of medications particularly diuretics, central nervous system depressants, cholinergics, and alpha antagonists, all of which can affect bladder function is necessary. Diet is also important to determine because of evidence albeit limited that spicy foods, caffeine, and alcohol can be bladder irritants, especially for women with more urge incontinence symptoms. There are several methods to screen for incontinence. The most successful way to determine the presence of incontinence involves direct questioning under circumstances that are comfortable for the patient. 29 Queries that may aid in identifying incontinence include, Many women sometimes experience a problem with leaking urine accidentally. Has that ever happened to you? If the patient concurs, follow-up questions can be used to differentiate between stress and urge incontinence. Positive responses to, How many times have you actually leaked urine with a physical activity like coughing, sneezing, lifting, or exercising? suggest a stress component. In contrast, urge incontinence can often be detected by inquiring, Did you have a feeling of a strong, sudden need to pass your urine that did not allow you to get to the toilet fast enough? The corresponding pathology associated with urge incontinence detrusor instability often is recognized by a patient, who feels the involuntary muscle changes that proceed unwanted voiding. Conversely, in stress incontinence, such triggers include laughter, coughing, sneezing, or some physical exertion. A large majority of patients who report stress incontinence are women and are generally middle-aged or older. A voiding diary may be helpful in several ways. Diaries can help with diagnostic confirmation of type of incontinence or, if the patient has mixed incontinence, can assist in determining which type predominates. In general, patients are adept at recording both storage and expulsion of urine accurately during the day, even though the voiding diary for incontinence can be complex. From such patient-rendered recordings, patterns will emerge. Diary recordings also actively engage patients in the care of their condition. A sample voiding diary is shown in Figure 4. Columns 1, 3, and 5 are most important, and the diary can be simplified to only those 3 columns for some patients, depending on Figure 3. Urinary Incontinence Is More Prevalent than Other Chronic Diseases in Women* *All types of urinary incontinence combined. Data from: Hampel et al 2 ; American Heart Association 17 ; American Academy of Family Physicians 18 ; National Institute of Diabetes and Digestive and Kidney Diseases. 19 S84 Vol. 4 (2A) February 2004
5 the symptoms and the patient s circumstances. In some patients, the incontinence will improve by just keeping the diary. Figure 4. Sample Urine Voiding Diary PHYSICAL EXAMINATION Abdominal Examination. An abdominal examination is important to detect masses, organomegaly, ascites, and other physical causes that can increase abdominal pressure and lead to incontinence. The bladder examination is less important because even when there is significant residual urine, it is often difficult to palpate the bladder, particularly in heavier women. Vaginal Examination. The vaginal examination is essential, and the key areas of assessment are outlined in Table 2. In general, the physician looks for the possibility of prolapse and the occurrence of masses and assesses pelvic floor strength. One method that aids in such assessment is to have the woman contract the vagina around the physician s fingers during a manual examination (ie, Kegel exercises) to establish voluntary control and assess the strength of the pelvic floor. The degree of estrogenization of the vagina is also important to assess by looking at the quality of the skin based on tone, thickness, and dryness. Fecal impaction is an important reversible cause of incontinence, especially in the elderly, and should always be determined in incontinent patients. Neurologic Examination. The sacral neurologic examination is a component of the pelvic examination. It is performed to test perineal sensation, anal sphincter strength (through voluntary contraction of the anal sphincter), and lower extremity function and muscle strength. In a woman without neurologic symptoms, this examination can be done by testing the bulbocavernosus and anal wink reflexes. Urinalysis. Urinalysis is recommended in all women with incontinence. Urinary tract infections will more frequently cause urgency symptoms rather than stress incontinence, so performing the test is worthwhile. Testing for hematuria, pyuria, glycosuria, and proteinuria should also be completed. Pad Test. Several other tests are helpful in confirming diagnosis and in making treatment decisions for women with urinary incontinence. The pad test is not often done in a primary care setting because it is Amount Urge Present Fluid Intake Time Voided Activity Leakage* (Yes/No) Amount/Type 6:50 AM 425 ml Getting up/ 0 Yes 16 oz coffee Breakfast 6 oz orange juice 7:45 AM 150 ml Leaving for 0 Slight work 8:20 AM 350 ml At work 0 Yes 8 oz coffee 9:10 AM Cough 2 Yes 9:15 AM 300 ml Working 0 Yes 10 oz water 12:25 PM 275 ml Working/ 0 Yes 8 oz water at lunch 2:45 PM 400 ml Bending 1 Yes 4 oz water 5:30 PM 250 ml Leaving work 0 Yes 6:30 PM 125 ml Exercise class 2 Slight 12 oz water 7:45 PM Dinner 0 No 4 oz wine 8 oz water 8:20 PM 375 ml At home 0 Yes 4 oz water 10:50 PM 250 ml Getting ready 0 Yes for bed *0 = no leakage; 1 = drops; 2 = wet underwear or light pad; 3 = soaked pad or clothing. Table 2. Rectal and Vaginal Examination for Incontinence Prolapse Mass Voluntary pelvic floor contraction Perineal skin condition Pelvic floor muscle tone Palpation of anterior vaginal wall and urethra Assess strength and voluntary control of levator muscles Determine degree of estrogenization Cotton-swab test Fecal impaction Advanced Studies in Medicine S85
6 more of a research tool used to quantify urine loss. Patients are given a pad of predetermined weight and asked to wear it for 24 hours, at which time the pad is weighed again. Stress or Cough Test. The stress or cough test is simple to perform and provides objective assessment of stress urinary incontinence. A woman with a full bladder is asked to cough or undergo a Valsalva maneuver, in lying, standing, and seated positions. By holding a pad at the urethra, urine leakage can be detected. Cotton-Swab Test. The cotton-swab test is especially useful if the woman is being considered for surgery, but it is also used to gauge the general degree of urethral support. A moistened cotton swab is placed in the urethra, and the woman is asked to bear down in a Valsalva maneuver. Normally, an exertion of the distal part of the cotton swab of 10 degrees or less will occur as a result of pressure being applied to the proximal end of the urethra. This technique reflects a normal amount of movement of the pelvic floor. In women with a hypermobile urethra, the movement will be much greater usually 30 degrees or more. This larger movement does not rule out intrinsic sphincter deficiency, but if the movement is not detected and the patient has stress incontinence, it implies intrinsic sphincter dysfunction rather than a pelvic floor support or hypermobility problem. The cotton-swab test is more an anatomical test than a diagnostic test for stress incontinence. Postvoid Residual Test. The postvoid residual test measures the amount of urine remaining in the bladder after voiding to determine if voiding is incomplete. Catheterization of the bladder is required after the woman has voided. Although this test can be performed in the office setting, it needs to be performed only in women with symptoms of retention or obstruction, which are relatively uncommon. Urodynamic Testing. Urodynamic testing is achieved with either eyeball cystometry or multichannel urodynamic studies. Neither of these methods is usually performed in primary care; however, it is useful to be familiar with them. Eyeball cystometry involves filling the bladder through a catheter. The bladder is first filled to the point where the patient feels a sensation to void, then to the point where she feels unable to avoid elimination. The syringe is held approximately 15 mm above the synthesis pubis, and the physician watches for rises and falls in the meniscus, which indicate detrusor contraction. At that point, the catheter is removed, and the patient performs a cough test for stress incontinence. The patient is then asked to void, and the time required to begin voiding and the size, force, and continuity of the urinary stream is recorded. The amount of urine, duration of voiding, and presence of straining, hesitancy, and dribbling are also recorded. Multichannel urodynamic studies include cystometry to assess bladder filling, pressure flow studies and uroflowmetry to assess voiding function, and leakpoint pressures or urethral pressure profiles to assess urethral function. Cystometry assesses bladder pressure-volume relationships within the bladder. After voiding, the patient lies down, and a catheter is positioned in the bladder; any urine left in the bladder is measured and recorded. Next, thermal sensation is evaluated. Room temperature saline solution is placed into the bladder, followed by warm water. The patient is asked to indicate any sensations, and the water is drained from the bladder. Finally, pressure within the bladder is measured during filling. A cystometer is connected to the catheter, and water or saline is slowly introduced into the bladder at a controlled rate. As with eyeball cystometry, the patient will indicate when the need to void is first felt. The pressures and volumes are recorded. When the bladder is full, voiding studies are performed. The patient voids, and the pressure of the voiding is recorded. The bladder is again drained of any residual urine, and the catheter is then removed. Electromyographic activity of the pelvic floor in response to bladder capacity, first and filling sensations, bladder compliance, and leak-point pressures may also be measured. CONCLUSION Urinary incontinence is a common problem, particularly for women of childbearing age and all older adults. It has significant negative impact on numerous aspects of quality of life. Because it is an embarrassing condition, many patients do not discuss their incontinence with their physicians; the condition therefore remains untreated or undertreated. Increasingly, the treatment of incontinence occurs in a primary care setting rather than a specialty practice. This form of care lends itself to longterm patient-physician relationships, in which trust builds with time. S86 Vol. 4 (2A) February 2004
7 REFERENCES 1. Abrams P, Cardozo L, Fall M, et al. The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Neurourol Urodyn. 2002;21(2): Hampel C, Wienhold D, Benken N, Eggersmann C, Thuroff JW. Definiton of overactive bladder and epidemology of urinary incontinence. Urology. 1997;50(suppl 6A): Thomas TM, Plymat KR, Blannin J, Meade TW. Prevalence of urinary incontinence. Br Med J. 1980;281(6250): Thom D. Variation in estimates of urinary incontinence prevalence in the community: effects of differences in definition, population characteristics, and study type. J Am Geriatr Soc. 1998;46(4): Viktrup L, Lose G. The risk of stress incontinence 5 years after first delivery. Am J Obstet Gynecol. 2001;185(1): Thom DH, van den Eeden SK, Brown JS. Evaluation of parturition and other reproductive variables as risk factors for urinary incontinence in later life. Obstet Gynecol. 1997;90(6): Dwyer PL, Lee ET, Hay DM. Obesity and urinary incontinence in women. Br J Obstet Gynaecol. 1988;95(1): Yarnell JW, Voyle GJ, Sweetnam PM, Milbank J, Richards CJ, Stephenson TP. Factors associated with urinary incontinence in women. J Epidemiol Community Health. 1982;36(1): Bai SW, Kang JY, Rha KH, Lee MS, Kim JY, Park KH. Relationship of urodynamic parameters and obesity in women with stress urinary incontinence. J Reprod Med. 2002;47(7): Deitel M, Stone E, Kassam HA, Wilk EJ, Sutherland DJ. Gynecologic-obstetric changes after loss of massive excess weight following bariatric surgery. J Am Coll Nutr. 1988;7(2): Bump RC, Sugerman HJ, Fantl JA, McClish DK. Obesity and lower urinary tract function in women: effect of surgically induced weight loss. Am J Obstet Gynecol. 1992;167(2): Graham CA, Mallett VT. Race as a predictor of urinary incontinence and pelvic organ prolapse. Am J Obstet Gynecol. 2001;185(1): Duong TH, Korn AP. A comparison of urinary incontinence among African American, Asian, Hispanic, and white women. Am J Obstet Gynecol. 2001;184(6): Burgio KL, Matthews KA, Engel BT. Prevalence, incidence and correlates of urinary incontinence in healthy, middleaged women. J Urol. 1991;146(5): Bump RC. Racial comparisons and contrasts in urinary incontinence and pelvic organ prolapse. Obstet Gynecol. 1993;81(3): Brown JS, Grady D, Ouslander JG, Herzog AR, Varner RE, Posner SF. Prevalence of urinary incontinence and associated risk factors in postmenopausal women. Heart & Estrogen/Progestin Replacement Study (HERS) Research Group. Obstet Gynecol. 1999;94(1): American Heart Association. Heart Disease and Stroke Statistics 2003 Update. Dallas, Tex: American Heart Association; Depression in women fact sheet. American Academy of Family Physicians Web site. Available at: org/handouts/443.html. Accessed December 1, National diabetes statistics. National Institute of Diabetes and Digestive and Kidney Diseases Web site. Available at: htm#7. Accessed December 1, Cheater FM, Castleden CM. Epidemiology and classification of urinary incontinence. Baillieres Best Pract Res Clin Obstet Gynaecol. 2000;14(2): Brandeis GH, Baumann MM, Hossain M, Morris JN, Resnick NM. The prevalence of potentially remediable urinary incontinence in frail older people: a study using the Minimum Data Set. J Am Geriatr Soc. 1997;45(2): Nihira MA, Henderson N. Epidemiology of urinary incontinence in women. Curr Womens Health Rep. 2003;3(4): Wagner TH, Hu TW. Economic costs of urinary incontinence in Urology. 1998;51(3): Wilson L, Brown JS, Shin GP, Luc KO, Subak LL. Annual direct cost of urinary incontinence. Obstet Gynecol. 2001;98(3): Bladder awareness campaign urges women to seek treatment [press release]. Bethesda, Md: National Institute of Diabetes and Digestive and Kidney Diseases; January 10, Available at: gov/welcome/releases/1_10_97.htm. Accessed December 1, Abrams P, Kelleher CJ, Kerr LA, Rogers RG. Overactive bladder significantly affects quality of life. Am J Manag Care. 2000;6(11 suppl):s580-s Brown JS, Waetjen LE, Subak LL, Thom DH, Van den Eeden S, Vittinghoff E. Pelvic organ prolapse surgery in the United States, Am J Obstet Gynecol. 2002;186(4): Brown JS, Sawaya G, Thom DH, Grady D. Hysterectomy and urinary incontinence: a systematic review. Lancet. 2000;356: Kravitz RL, Bell RA, Azari R, Krupat E, Kelly-Reif S, Thom D. Request fulfillment in office practice antecedents and relationship to outcomes. Med Care. 2002;40(1): Advanced Studies in Medicine S87
Incontinence: Risks, Causes and Care
 Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
743 Jefferson Avenue Suite 203 Scranton, Pennsylvania VOIDING DIARY. Column #3 LEAK
 743 Jefferson Avenue Suite 203 Scranton, Pennsylvania 18510 570.344.9997 VOIDING DIARY This paperwork MUST be completed prior to your appointment. If not, your appointment will need to be rescheduled.
743 Jefferson Avenue Suite 203 Scranton, Pennsylvania 18510 570.344.9997 VOIDING DIARY This paperwork MUST be completed prior to your appointment. If not, your appointment will need to be rescheduled.
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider.
 Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Incontinence Patient Information Form
 Incontinence Patient Information Form (To be completed by patient) Before talking with you, the doctor would like some information about your urine leakage. These questions are important for finding out
Incontinence Patient Information Form (To be completed by patient) Before talking with you, the doctor would like some information about your urine leakage. These questions are important for finding out
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS- SECTIONAL STUDY
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Aisha et al. SJIF Impact Factor 6.647 Volume 6, Issue 9, 1384-1391 Research Article ISSN 2278 4357 URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS-
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Aisha et al. SJIF Impact Factor 6.647 Volume 6, Issue 9, 1384-1391 Research Article ISSN 2278 4357 URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS-
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
A word about incontinence
 A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Information on Physical Therapy For Urogynecologic Problems
 Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
Urogynecology Associates of Philadelphia URODYNAMIC TESTING
 URODYNAMIC TESTING Urogynecology Associates of Philadelphia Most women with urinary incontinence will need to complete a few simple tests, performed in the office, to help your doctor assess your symptoms
URODYNAMIC TESTING Urogynecology Associates of Philadelphia Most women with urinary incontinence will need to complete a few simple tests, performed in the office, to help your doctor assess your symptoms
Module 3 Causes Of Urinary Incontinence
 Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Incontinence: The silent scourge of the young and old. The International Continence Society has. In this article:
 Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Table 1. International Consultation on Incontinence recommendations for frail older adults
 Table 1. International Consultation on Incontinence recommendations for frail older adults Clinicians need to assess and manage co-existing co morbid conditions which are known to have an impact on continence
Table 1. International Consultation on Incontinence recommendations for frail older adults Clinicians need to assess and manage co-existing co morbid conditions which are known to have an impact on continence
Stress incontinence -- occurs during certain activities like coughing, sneezing, laughing, or exercise.
 Urinary incontinence Definition Incontinence is the inability to control the passage of urine. This can range from an occasional leakage of urine, to a complete inability to hold any urine. The three main
Urinary incontinence Definition Incontinence is the inability to control the passage of urine. This can range from an occasional leakage of urine, to a complete inability to hold any urine. The three main
When Laughing is No Longer Funny Managing Transient Urinary Incontinence in Hospitalized Elderly Women
 When Laughing is No Longer Funny Managing Transient Urinary Incontinence in Hospitalized Elderly Women Grace Umejei, BSN, RN, CWOC. Texas Health Presbyterian Hospital Dallas NICHE Online Connect Webinars
When Laughing is No Longer Funny Managing Transient Urinary Incontinence in Hospitalized Elderly Women Grace Umejei, BSN, RN, CWOC. Texas Health Presbyterian Hospital Dallas NICHE Online Connect Webinars
743 Jefferson Avenue Suite 203 Scranton, Pennsylvania
 743 Jefferson Avenue Suite 203 Scranton, Pennsylvania 18510 570.344.9997 Name: DOB: / / Age: Address: City: State: Zip: Home Phone: Work Phone: Cell Phone: Reason for your visit today: Who referred you
743 Jefferson Avenue Suite 203 Scranton, Pennsylvania 18510 570.344.9997 Name: DOB: / / Age: Address: City: State: Zip: Home Phone: Work Phone: Cell Phone: Reason for your visit today: Who referred you
Appendix F: Continence Care and Bowel Management Program Training Presentation. Audience: For Front-line Staff Release Date: December 22, 2010
 Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Continence Promotion in
 Everybody s Business- Continence Promotion in Aged Care Melissa O Grady Clinical Nurse Consultant Continence Warning Some graphic images are contained in this presentation Objectives What is Old Age? What
Everybody s Business- Continence Promotion in Aged Care Melissa O Grady Clinical Nurse Consultant Continence Warning Some graphic images are contained in this presentation Objectives What is Old Age? What
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Diagnosis and Treatment of Urinary Incontinence. Urinary Incontinence
 Diagnosis and Treatment of Urinary Incontinence Leslee L. Subak, MD Professor Obstetrics, Gynecology & RS Epidemiology, Urology University of California, San Francisco Urinary Incontinence Common - 25%
Diagnosis and Treatment of Urinary Incontinence Leslee L. Subak, MD Professor Obstetrics, Gynecology & RS Epidemiology, Urology University of California, San Francisco Urinary Incontinence Common - 25%
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Women s and Men s Health Intake Form Comprehensive Physical Therapy Center
 Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Information to Help You Live Life to the Fullest
 Information to Help You Live Life to the Fullest For more information and to join the conversation visit: Prevail.com/LOBC 800-227-3551 CONSUMER EDUCATION 2015 First Quality Products, Inc. All rights reserved.
Information to Help You Live Life to the Fullest For more information and to join the conversation visit: Prevail.com/LOBC 800-227-3551 CONSUMER EDUCATION 2015 First Quality Products, Inc. All rights reserved.
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Urogynecology History Questionnaire. Name: Date: Date of Birth: Age:
 Urogynecology History Questionnaire Name: Date: Date of Birth: Age: 1. Have you had treatment for urinary tract diseases such as (please check): stones, kidney disease, infections, tumors, injuries? 2.
Urogynecology History Questionnaire Name: Date: Date of Birth: Age: 1. Have you had treatment for urinary tract diseases such as (please check): stones, kidney disease, infections, tumors, injuries? 2.
Incontinence. Urinary. In Adults. THIS PUBLICATION IS OUT OF DATE. For most current information:
 Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
Disease Management. Incontinence Care. Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09
 Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors
 DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors D Delirium Acute confusion alters one s ability to anticipate and meet own needs. Delirium may occur from drugs, surgery,
DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors D Delirium Acute confusion alters one s ability to anticipate and meet own needs. Delirium may occur from drugs, surgery,
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Urodynamic findings in women with insensible incontinence
 bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Training a Wayward Bladder
 D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT
 UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT Yunizaf, MD Division of Urogynecology Department of Obstetrics and Gynecology School of Medicine, University of Indonesia/ Dr. Cipto Mangunkusumo Hospital
UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT Yunizaf, MD Division of Urogynecology Department of Obstetrics and Gynecology School of Medicine, University of Indonesia/ Dr. Cipto Mangunkusumo Hospital
Clean Intermittent Self-Catheterisation (CISC)
 Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
AgePage. Urinary Incontinence
 National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Urinary Incontinence for the Primary Care Provider
 Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Todd Martin, PT Jared Bailey, PT Samantha Stollberg, PT, PRPC Karen Bailey, PT John Hollinshead, PT Sarada Bird, DPT Adrian Asencio, OTR/L, CHT
 Adrian Asencio, OTR/L, CHT Please fill out the enclosed forms and bring them with you to your first appointment. At that time, we will do a brief examination of your pelvic floor muscles, and you are welcome
Adrian Asencio, OTR/L, CHT Please fill out the enclosed forms and bring them with you to your first appointment. At that time, we will do a brief examination of your pelvic floor muscles, and you are welcome
Urinary Incontinence. a problem for many
 Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
AgePage. Urinary Incontinence
 National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
Incontinence; Lets talk about it. Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery
 Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Overactive Bladder. When to see a doctor. Normal bladder function
 Overactive Bladder Overactive bladder is a problem with bladder-storage function that causes a sudden urge to urinate. The urge may be difficult to stop, and overactive bladder may lead to the involuntary
Overactive Bladder Overactive bladder is a problem with bladder-storage function that causes a sudden urge to urinate. The urge may be difficult to stop, and overactive bladder may lead to the involuntary
Urogyn Initial Visit Packet
 Urogyn Initial Visit Packet Please complete the questions. If they do not apply you can skip to the next question or the next section whichever is appropriate. Thanks so much for your time. This will help
Urogyn Initial Visit Packet Please complete the questions. If they do not apply you can skip to the next question or the next section whichever is appropriate. Thanks so much for your time. This will help
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS.
 IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
Urinary incontinence (UI) affects as many
 EXPLORING NEW HORIZONS IN STRESS INCONTINENCE: THE NEUROUROLOGY CONNECTION W. Glenn Hurt, MD* ABSTRACT As many as one-third of women are affected by urinary incontinence, the most common of which being
EXPLORING NEW HORIZONS IN STRESS INCONTINENCE: THE NEUROUROLOGY CONNECTION W. Glenn Hurt, MD* ABSTRACT As many as one-third of women are affected by urinary incontinence, the most common of which being
Appendix E: Continence Care and Bowel Management Program Training Presentation. Audience: For Registered Staff Release Date: December 22, 2010
 Appendix E: Continence Care and Bowel Management Program Training Presentation Audience: For Registered Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Appendix E: Continence Care and Bowel Management Program Training Presentation Audience: For Registered Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Coping with urges and leaks?
 OAB AND YOU Coping with urges and leaks? Let me help you learn more about overactive bladder (OAB) symptoms and ways to help manage them 1 HOW DOES THE BLADDER WORK? Within the urinary tract, the kidneys
OAB AND YOU Coping with urges and leaks? Let me help you learn more about overactive bladder (OAB) symptoms and ways to help manage them 1 HOW DOES THE BLADDER WORK? Within the urinary tract, the kidneys
UROGYNECOLOGY. In your own words, please write the nature of your medical problem for which you are being seen today.
 Thank you for taking the time to fill out this questionnaire. A detailed and accurate health history will enable us to give you the best care and treatment. NAME AGE DATE In your own words, please write
Thank you for taking the time to fill out this questionnaire. A detailed and accurate health history will enable us to give you the best care and treatment. NAME AGE DATE In your own words, please write
Urinary Continence & Management Post Stroke
 Urinary Continence & Management Post Stroke Incontinence and Stroke occurs in greater than 50% of acute stroke patients despite the personal, economic and psychosocial impact treatment evidence specific
Urinary Continence & Management Post Stroke Incontinence and Stroke occurs in greater than 50% of acute stroke patients despite the personal, economic and psychosocial impact treatment evidence specific
Y0028_2726_0 File&Use Bladder Control Does Matter
 Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
Management, Evaluation, and Treatment of Overactive Bladder and Urinary Incontinence
 Management, Evaluation, and Treatment of Overactive Bladder and Urinary Incontinence Arthur Mourtzinos, MD, MBA Co-Vice Chair, Institute of Urology Director, Continence Center Assistant Professor of Urology,
Management, Evaluation, and Treatment of Overactive Bladder and Urinary Incontinence Arthur Mourtzinos, MD, MBA Co-Vice Chair, Institute of Urology Director, Continence Center Assistant Professor of Urology,
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Patient Information. Basic Information on Overactive Bladder Symptoms. pubic bone. urethra. scrotum. bladder. vaginal canal
 Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Urodynamics in women. Aims of Urodynamics in women. Why do Urodynamics?
 Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Research. Estrogen receptors have been identified
 Research UROGYNECOLOGY Postmenopausal hormone therapy and incident urinary incontinence in middle-aged women Mary K. Townsend, ScD; Gary C. Curhan, MD, ScD; Neil M. Resnick, MD; Francine Grodstein, ScD
Research UROGYNECOLOGY Postmenopausal hormone therapy and incident urinary incontinence in middle-aged women Mary K. Townsend, ScD; Gary C. Curhan, MD, ScD; Neil M. Resnick, MD; Francine Grodstein, ScD
FEMALE SYMPTOM MONITOR
 FEMALE SYMPTOM MONITOR Name: Occupation: Date: Age: Complaints: 1. 2. 3. GYNECOLOGICAL HISTORY: # pregnancies: # live births: Wt. heaviest baby: lbs oz Length pushing stage: hours Forceps? Yes No Episiotomies?
FEMALE SYMPTOM MONITOR Name: Occupation: Date: Age: Complaints: 1. 2. 3. GYNECOLOGICAL HISTORY: # pregnancies: # live births: Wt. heaviest baby: lbs oz Length pushing stage: hours Forceps? Yes No Episiotomies?
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
2 Voiding Dysfunction
 2 Voiding Dysfunction Diagnostic Evaluation Victor W. Nitti, MD and Michael Ficazzola, MD Contents Introduction Classification of Voiding Dysfunction History Physical Examination Laboratory Testing Simple
2 Voiding Dysfunction Diagnostic Evaluation Victor W. Nitti, MD and Michael Ficazzola, MD Contents Introduction Classification of Voiding Dysfunction History Physical Examination Laboratory Testing Simple
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
Prostate surgery. What is the prostate? What is a TURP? Why is a TURP operation necessary? Deciding to have a TURP operation.
 What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
Compassionate and effective management
 IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
The relationship between urinary symptom questionnaires and urodynamic diagnoses: an analysis of two methods of questionnaire administration
 BJOG: an International Journal of Obstetrics and Gynaecology May 2004, Vol. 111, pp. 468 474 DOI: 1 0. 1111/j.1471-0528.2004.00126.x The relationship between urinary symptom questionnaires and urodynamic
BJOG: an International Journal of Obstetrics and Gynaecology May 2004, Vol. 111, pp. 468 474 DOI: 1 0. 1111/j.1471-0528.2004.00126.x The relationship between urinary symptom questionnaires and urodynamic
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
Date: Initial Visit: am/pm 1st Return: am/pm
 DEMOGRAPHICS RECORDS Patient Code: MDK / LK / KH / KC-H / JS Date: Initial Visit: am/pm 1st Return: am/pm Patient Aware: Yes No FAX WALK-IN PATIENT CALLED Rx Date: DTA: PATIENT INFORMATION: Injury/Diagnosis:
DEMOGRAPHICS RECORDS Patient Code: MDK / LK / KH / KC-H / JS Date: Initial Visit: am/pm 1st Return: am/pm Patient Aware: Yes No FAX WALK-IN PATIENT CALLED Rx Date: DTA: PATIENT INFORMATION: Injury/Diagnosis:
Differences in Prevalence of Urinary Incontinence by Race /Ethnicity
 Differences in Prevalence of Urinary Incontinence by Race /Ethnicity David H. Thom, MD, PhD, 1 Stephen K. Van Den Eeden, PhD, 2 Arona I. Ragins, MA, 2 Christina Wassel-Fyr, MS, 1 Eric Vittinghof, PhD,
Differences in Prevalence of Urinary Incontinence by Race /Ethnicity David H. Thom, MD, PhD, 1 Stephen K. Van Den Eeden, PhD, 2 Arona I. Ragins, MA, 2 Christina Wassel-Fyr, MS, 1 Eric Vittinghof, PhD,
The development of a questionnaire to measure the severity of symptoms and the quality of life before and after surgery for stress incontinence
 BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
Female Symptom Monitor
 Occupation Female Symptom Monitor Presenting problems When did this start? Please fill out each section that is relevant to your problem Gynecological History What age did your period start? Is your cycle
Occupation Female Symptom Monitor Presenting problems When did this start? Please fill out each section that is relevant to your problem Gynecological History What age did your period start? Is your cycle
Female Pelvic Medicine & Reconstructive Surgery Beth Israel Deaconess Medical Center (BIDMC)
 Female Pelvic Medicine & Reconstructive Surgery Beth Israel Deaconess Medical Center (BIDMC) Name: Age: Reason for visit/referral: Are you referred for or interested in surgery? Yes No Maybe Referring
Female Pelvic Medicine & Reconstructive Surgery Beth Israel Deaconess Medical Center (BIDMC) Name: Age: Reason for visit/referral: Are you referred for or interested in surgery? Yes No Maybe Referring
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
