Surgical Treatment of LUTS in Men with BPE
|
|
|
- Dustin Nash
- 5 years ago
- Views:
Transcription
1 Patient Information English 35 Surgical Treatment of LUTS in Men with BPE The underlined terms are listed in the glossary. You have been diagnosed with benign prostatic enlargement (BPE) and your doctor recommends surgery. This section describes different treatment options, which you should discuss with your doctor. Together you can decide which approach is best for you. Factors which influence this decision include: Your symptoms and quality of life The size of your prostate Your medical history The kind of treatment available at your hospital and the expertise of your doctor. Ask your urologist about his or her experience with the recommended treatment option. You have the right to know the complication rate of the surgeon who will do the operation Your personal preferences and values. There is no single treatment which is ideal for all patients When should I consider surgery? When your symptoms get worse, even if you already receive drug treatment When you have complications of BPE or if you are at risk of getting them. Complications include: - Kidney failure - Dilatation of your kidneys - Inability to urinate (urinary retention) - Recurring urinary tract infection - Recurring blood in the urine If you do not tolerate drug treatment very well If you prefer surgery over drug treatment During surgical treatment the doctor will remove the enlarged part of your prostate (also known as adenoma). There are different types of surgical procedures, but all of them aim to relieve your symptoms and improve the flow of urine. Page 1 / 15
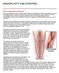
2 The main procedures are: Transurethral resection of the prostate (TURP) Transurethral incision of the prostate (TUIP) Open prostatectomy Laser treatment Prostate stents Transurethral needle ablation (TUNA) Transurethral microwave therapy (TUMT) This section also discusses ethanol and botulinum toxin injections. Research on the effects of these procedures is still on-going and their use is experimental. Each procedure has its own advantages and disadvantages. The choice of treatment depends on your individual situation and preference. This section offers general information about surgical treatment and situations can vary in different countries. Transurethral resection of the prostate (TURP) TURP is the standard surgery for BPE. The aim is to remove the part of the prostate which causes the symptoms. The procedure is done through the urethra without making an incision in your lower abdomen (Fig. 1). This type of surgery is known as minimally invasive treatment. How is TURP performed? For TURP you will receive general or spinal anaesthesia. Once you are under anaesthesia, the doctor uses a resectoscope to enter the through the urethra. This is a type of endoscope with a wire loop which uses a high-frequency electrical current to cut the prostate tissue. The resectoscope also has a camera which allows the doctor to see a high-quality image of the prostate on a video monitor. During the procedure, the doctor removes the adenoma in small parts with the wire loop (Fig. 2). The doctor then flushes the cut tissue out of the and the urethra through the resectoscope. wire loop enlarged prostate urethra resectoscope urethra rectum resectoscope enlarged prostate 2017 patient.uroweb ALL RIGHTS RESERVED 2017 patient.uroweb ALL RIGHTS RESERVED Fig. 1: Surgery through the urethra. Fig. 2: The resectoscope removes parts of the prostate tissue during TURP. Page 2 / 15
3 s Interesting Fact TURP has been performed since the 1930s s Interesting Fact In the early days, the doctor had to look and it has become the standard treatment directly into the endoscope to see the prostate. option in the last 40 years. It has greatly Nowadays, the camera projects a magnified improved in the past decade because of new image onto the video monitor in front of the technologies. doctor. Because of high-definition technology, the doctor can see even the smallest details. After the operation a catheter is placed in your to drain urine. It is also used to continuously flush your and urethra with sterile solution to prevent blood clots. You will need the catheter for 1-3 days until the urethra is healed and you can urinate on your own. When should I consider TURP? Today, TURP is the preferred surgical option for men with moderate to severe symptoms caused by BPE. It is most suited for men with prostates between millilitres. How do I prepare for the procedure? Your doctor will advise you in detail about how to prepare for the procedure. You must not eat, drink, or smoke for 6 hours before surgery to prepare for the anaesthesia. If you are taking any prescribed medication, discuss it with your doctor. You may need to stop taking it several days before surgery. How long will it take me to get back to my daily activities? Usually you can leave the hospital 2 or 3 days after surgery. The length of hospital stay can vary in different countries. There may be some blood in your urine for several days. You may also suffer from urgency and feel pain when you urinate, which can last up to several weeks. For 4-6 weeks after the surgery: Do not take thermal baths or go to the sauna Prevent constipation by adapting your diet Discuss any prescribed medication with your doctor Avoid having sex for 2-3 weeks. After TURP, you may suffer from retrograde ejaculation. This is a chronic condition where semen can no longer leave through the urethra during orgasm. Instead it goes into the and later leaves your body during urination. You need to go to the doctor or go back to the hospital right away if you: Develop a fever Are unable to urinate on your own Have heavy blood loss or pain Advantages of TURP The procedure is safe and widely used Optimal and long-lasting improvement of the symptoms Short hospital stay Disadvantages of TURP Risk of bleeding Risk of retrograde ejaculation Risk of urethral stricture Risk of urinary retention Low risk of urinary tract infection and urgency Very low risk of incontinence Drink 1-2 litres every day, especially water Do not lift anything heavier than 5 kilograms Do not do any heavy exercise and avoid bike riding Page 3 / 15
4 Transurethral incision of the prostate (TUIP) TUIP is effective in men with prostates smaller than 35 millilitres who do not suffer from severe obstruction. This procedure is rarely used for the treatment of BPE because it has the same results as drug treatment. TUIP is recommended if you cannot tolerate drugs for BPE symptoms. During TUIP, the doctor cuts into the prostate through the neck with a resectoscope to improve the flow of urine. After the operation a catheter is placed in your to drain urine. The catheter is also used to continuously flush your and urethra with sterile solution to prevent blood clots. Open prostatectomy Open prostatectomy is an operation which is done by making an incision in the lower part of the abdomen. Because TURP has similar or better results, open prostatectomy is now only done in selected situations. How is open prostatectomy performed? For open prostatectomy you will receive general or spinal anaesthesia. During the operation the surgeon cuts into the lower abdomen to reach the and the prostate. The surgeon then uses his finger to remove the adenoma (Fig. 3). After the operation a catheter will drain the urine. It is also used to continuously flush your and urethra with sterile solution to prevent blood clots. You will need the catheter for several days until the wound is healed and you can urinate on your own. adenoma 2017 patient.uroweb ALL RIGHTS RESERVED Fig. 3: The surgeon removes the adenoma during open prostatectomy. Page 4 / 15
5 s Interesting Fact Open prostatectomy was a major breakthrough in early 1900s when prostate surgery was first pioneered. Although it has been replaced by TURP as the gold standard treatment, open surgery is still recommended for the treatment of very large prostates. When should I consider open prostatectomy? Open prostatectomy is recommended if your prostate is larger than 80 millilitres because other types of surgery would take more time to achieve the same result. Your doctor may also recommend open prostatectomy if you have stones or a condition called diverticulum. How do I prepare for the procedure? Your doctor will advise you in detail about how to prepare for the procedure. You must not eat, drink, or smoke for 6 hours before surgery to prepare for the anaesthesia. If you are taking any prescribed medication, discuss it with your doctor. You may need to stop taking it several days before surgery. How long will it take me to get back to my daily activities? Usually you can leave the hospital 5 to 7 days after surgery. The length of hospital stay can vary in different countries. There may be some blood in your urine for several days. You may also suffer from urgency and feel pain when you urinate. It will take several weeks to completely recover from the surgery. Avoid having sex for 2-3 weeks. After open prostatectomy, you may suffer from retrograde ejaculation. This is a chronic condition where semen can no longer leave through the urethra during orgasm. Instead it goes into the and later leaves your body during urination. Advantages of open prostatectomy Optimal and long-lasting improvement of the symptoms Disadvantages of open prostatectomy Will leave a scar Longer hospital stay Longer use of catheter Significant bleeding may occur Risk of urinary retention, urinary tract infection and urgency Risk of neck stricture Very low risk of urinary incontinence For 4-6 weeks after the surgery: Drink 1-2 litres every day, especially water Do not lift anything heavier than 5 kilograms Do not do any heavy exercise and avoid bike riding Do not take thermal baths or go to the sauna Prevent constipation by adapting your diet Discuss any prescribed medication with your doctor Page 5 / 15
6 Laser treatment Laser treatment is a common treatment option for BPE. The laser uses intensive light to cut or vaporize the prostate tissue. At the same time, the heat from the laser is used to close blood vessels. This is why only a small amount of blood is lost during this type of surgery. There are two main types of laser surgery for BPE: Laser vaporization of the prostate Laser enucleation of the prostate These types of surgery can be done with different laser systems. The choice of the laser depends on the expertise of your doctor and what is available in your hospital. Laser vaporization of the prostate How is laser vaporization performed? For laser vaporization you will receive general or spinal anaesthesia. Once you are under anaesthesia, the doctor uses a resectoscope to enter the through the urethra without making an incision in your lower abdomen (Fig. 1). The resectoscope has a laser for vaporization and a small camera. The camera allows the doctor to see a high-quality image of the prostate on a video monitor. During the procedure, the laser heats up a small part of the prostate. When the tissue reached boiling point it starts to vaporize. In this way, the whole prostate can be treated (Fig. 4). After the operation a urinary catheter will be placed in your to drain urine. It is also used to continuously flush your and urethra with sterile solution to prevent blood clots. You will need the catheter for some days until the urethra is healed and you can urinate on your own. enlarged prostate laser enlarged prostate tissue removed on this side urethra laser resectoscope 2017 patient.uroweb ALL RIGHTS RESERVED Fig. 4: The heat from the laser vaporizes parts of the prostate tissue. Page 6 / 15
7 When should I consider laser vaporization of the prostate? Vaporization may be an option if your prostate is smaller than 80 millilitres. Because vaporization causes very little blood loss, it is recommended for men who need to take blood-thinning medication for other conditions. You need to go to the doctor or go back to the hospital right away if you: Develop fever Are unable to urinate on your own Have heavy blood loss or pain How do I prepare for the procedure? Your doctor will advise you in detail about how to prepare for the procedure. You must not eat, drink, or smoke for 6 hours before surgery to prepare for the anaesthesia. If you are taking any prescribed medication, discuss it with your doctor. You may need to stop taking it before surgery. How long will it take me to get back to my daily activities? Usually you can leave the hospital 1 or 2 days after surgery. The length of hospital stay can vary in different countries. There may be some blood in your urine and you may feel pain when you urinate. This can last up to several weeks. Advantages of laser vaporization Immediate improvement of the urine flow Short hospital stay Shorter period of using a catheter Low risk of complications No need to stop blood-thinning medication Disadvantages of laser vaporization Less effective for very large prostates Painful urination for some time after the surgery May need another surgery after several years because the prostate continues to grow No possibility to analyse the prostate tissue after the surgery Risk of urinary retention, urinary tract infection and urgency Very low risk of urinary incontinence For 4-6 weeks after the surgery: Drink 1-2 litres every day, especially water Do not lift anything heavier than 5 kilograms Do not do any heavy exercise and avoid bike riding Do not take thermal baths or go to the sauna Prevent constipation by adapting your diet Discuss any prescribed medication with your doctor Avoid having sex for 2-3 weeks. Your semen may be stained with blood for a few weeks. After laser vaporization, you may suffer from retrograde ejaculation. This is a chronic condition where semen can no longer leave through the urethra during orgasm. Instead it goes into the and later leaves your body during urination. Page 7 / 15
8 Laser enucleation of the prostate How is laser enucleation performed? For laser enucleation you will receive general, spinal, or intravenous anaesthesia. Once you are under anaesthesia, the doctor uses a resectoscope to enter the through the urethra without making an incision in your lower abdomen (Fig. 1). The resectoscope has a small camera through which the doctor can see the prostate. During laser enucleation the doctor uses the laser to cut prostate tissue and in this way the whole prostate can be treated (Fig. 5). The doctor then uses an instrument known as morcellator to flush the cut tissue out of your body through the and the urethra. enlarged prostate laser enlarged prostate tissue removed on this side urethra laser resectoscope 2017 patient.uroweb ALL RIGHTS RESERVED Fig. 5: The laser cuts out parts of the prostate tissue during laser enucleation. After the operation a a urinary catheter is placed in your to drain urine. It is also used to continuously flush your and urethra with sterile solution to prevent blood clots. You will need the catheter for some days until the urethra is healed and you can urinate on your own. When should I consider laser enucleation of the prostate? If your prostate is over 80 millilitres, laser enucleation may be the best option for you, because it removes the whole adenoma. This type of surgery is also a good option for men with smaller prostates. Laser enucleation is suitable for men who take bloodthinning medication for other conditions. It is important to discuss your individual situation with your doctor. How do I prepare for the procedure? Your doctor will advise you in detail about how to prepare for the procedure. You must not eat, drink, or smoke for 6 hours before surgery to prepare for the anaesthesia. If you are taking any prescribed medication, discuss it with your doctor. You may need to stop taking it before surgery. Page 8 / 15
9 How long will it take me to get back to my daily activities? Usually you can leave the hospital 1 or 2 days after surgery. The length of hospital stay can vary in different countries. There may be some blood in your urine and you may feel pain when you urinate. This can last up to several weeks. For 4-6 weeks after the surgery: Drink 1-2 litres every day, especially water Do not lift anything heavier than 5 kilograms Do not do any heavy exercise and avoid bike riding Do not take thermal baths or go to the sauna Prevent constipation by adapting your diet Discuss any prescribed medication with your doctor Advantages of laser enucleation Immediate improvement of the urine flow Short hospital stay Shorter period of using a catheter Low risk of complications Effective for all prostates, especially for large ones Possibility to analyse the prostate tissue after the surgery Disadvantages of laser enucleation Surgery may take longer for small prostates Painful urination for some time after the surgery Risk of urinary retention, urinary tract infection and urgency Very low risk of urinary incontinence Avoid having sex for 2-3 weeks. Your semen may be stained with blood for a few weeks. After laser enucleation, you may suffer from retrograde ejaculation. This is a chronic condition where semen can no longer leave through the urethra during orgasm. Instead it goes into the and later leaves your body during urination. You need to go to the doctor or go back to the hospital right away if you: Develop a fever Are unable to urinate on your own Have heavy blood loss or pain Page 9 / 15
10 Prostate stents Prostate stents are used to keep the urethra open which improves the flow of urine (Fig. 1). Stents are mainly recommended for men who are not fit for surgery but who are still able to empty the on their own. They are used instead of an indwelling catheter. How is the stent inserted? The stent can be placed in the doctor s office or a clinic under local anaesthesia. It is inserted into the urethra until the tip reaches the (Fig. 6). The correct position is checked with an ultrasound or a cystoscope. When should I consider getting a stent? Today, stents are not recommended as a permanent treatment option. You should consider stents only if you cannot tolerate anaesthesia which is needed for surgery. How do I prepare for the procedure? Your doctor will advise you in detail how to prepare for the procedure. If you are taking any prescribed medication, discuss it with your doctor. You may need to stop taking it before the procedure. How long will it take me to get back to my daily activities? Usually you can go back to your daily activities on the day of the procedure. There may be some blood in your urine and you may feel pain when you urinate. This can last up to several weeks. You need to go to your doctor or the hospital right away if you: Develop a fever Are unable to urinate on your own Have heavy blood loss or pain Advantages of stents Can be used instead of an indwelling catheter No hospital stay Local anaesthesia Disadvantages of stents The stent may shift Pain while urinating for some time after the procedure May fail to improve the flow of urine Low risk of urinary incontinence Risk of stone formation on the stent enlarged prostate stent urethra 2017 patient.uroweb ALL RIGHTS RESERVED Fig. 6: A prostate stent improves the flow of urine. Page 10 / 15
11 Transurethral needle ablation (TUNA) Transurethral needle ablation (TUNA) of the prostate is minimally invasive treatment which uses heat to harden parts of the prostate tissue. This process is called coagulation. The treated part of the prostate is either absorbed by the body or it passes with urine after the procedure. The aim of TUNA is to reduce the prostate volume and to improve the symptoms. How is TUNA performed? For TUNA you will receive intravenous, spinal, or local anaesthesia. Once you are under anaesthesia, the doctor uses a resectoscope to enter the through the urethra. The doctor uses an endoscope which has two needles and a camera. The needles are used to puncture the prostate and to heat up the tissue with radiofrequency energy (Fig. 7). This is done 4 to 8 times to treat the whole adenoma. The camera allows the doctor to see a high-quality image of the prostate on a video monitor. You will need a catheter for some days until the urethra is healed and you can urinate on your own. The catheter is removed by the urologist at the hospital or clinic. treated areas enlarged prostate needle endoscope urethra 2017 patient.uroweb ALL RIGHTS RESERVED Fig. 7: The needle heats up the prostate tissue with radiofrequency energy. Page 11 / 15
12 When should I consider having TUNA? TUNA is advised for men with a prostate between 30 to 80 millilitres, who prefer minimally invasive treatment or who are not fit to have surgery because of other medical conditions. How do I prepare for the procedure? Your doctor will advise you in detail about how to get ready for the procedure. To prepare for the anaesthesia you should not eat, drink, or smoke for 6 hours before the procedure. If you are taking any prescribed medication, discuss it with your doctor. You may need to stop taking it. How long will it take me to get back to my daily activities? Usually you can leave the hospital or clinic a few hours after TUNA. Do not drive a car when leaving the hospital because you may still be drowsy after the anaesthesia. Make sure you get enough rest on the day of the procedure. With the catheter still in your urethra, you can start getting back to your daily activities the next day. Your urine may contain traces of blood which can last up to several weeks. Avoid having sex for 2-3 weeks. Your semen may be stained with blood for a few weeks. You need to go to the doctor or go back to the hospital right away if you: Develop a fever Face problems with the catheter Cannot urinate on your own after the catheter is removed Advantages of TUNA No hospital stay in most cases Low risk of complications No need to stop blood-thinning medication Disadvantages of TUNA Less effective for large prostates and in case of severe obstruction Use of catheter at home for several days after the procedure Slow improvement of symptoms and the flow of urine May need another treatment after several years because the prostate continues to grow For 4-6 weeks after the surgery: Drink 1-2 litres every day, especially water Do not lift anything heavier than 5 kilograms Do not do any heavy exercise and avoid bike riding Do not take thermal baths or go to the sauna Prevent constipation by adapting your diet Discuss any prescribed medication with your doctor Page 12 / 15
13 Transurethral microwave therapy (TUMT) Transurethral microwave therapy (TUMT) of the prostate is minimally invasive treatment which uses microwave energy to harden parts of the prostate tissue. This process is called coagulation. The treated part of the prostate is either absorbed by the body or it passes with urine after the procedure. The aim of TUMT is to reduce the prostate volume and to improve the symptoms. How is TUMT performed? For TUMT you will receive local anaesthesia which is sometimes combined with intravenous anaesthesia. Once you are under anaesthesia, the doctor uses a resectoscope to enter the through the urethra which has a microwave antenna and a balloon. The antenna heats up the prostate tissue with microwave energy and the balloon keeps the antenna in place inside the prostate (Fig. 8). After the procedure a different catheter will be placed in your to help you urinate. You will need this catheter for some days until the urethra is healed and you can urinate on your own. The catheter is removed by the urologist at the hospital or clinic. enlarged prostate balloon catheter heated prostate tissue microwave antenna urethra 2017 patient.uroweb ALL RIGHTS RESERVED Fig. 8: The heat generated by the microwave antenna coagulates parts of the enlarged prostate tissue. Page 13 / 15
14 When should I consider TUMT? TUMT is recommended for men with a prostate between 30 to 100 millilitres who prefer minimally invasive treatment or do not wish to have surgery because of other medical conditions. How do I prepare for the procedure? Your doctor will advise you in detail about how to get ready for the procedure. To prepare for the anaesthesia you should not eat, drink, or smoke for 6 hours before the procedure. If you are taking any prescribed medication, discuss it with your doctor. You may need to stop taking it before TUMT. How long will it take me to get back to my daily activities? In most cases you can leave the hospital a few hours after TUMT. Do not drive a car when leaving the hospital because you may still be drowsy after the anaesthesia. Make sure you get enough rest on the day of the procedure. With the catheter still in your urethra, you can start getting back to your daily activities the next day. Your urine may contain traces of blood which can last up to several weeks. You need to go to the doctor or go back to the hospital right away if you: Develop a fever Face problems with the catheter Are unable to urinate on your own after catheter removal Advantages of TUMT Is performed under local anaesthesia No hospital stay in most cases Low risk of complications No need to stop blood-thinning medication Disadvantages of TUMT Less effective for large prostates and in case of severe obstruction Use of catheter at home for several days after the procedure Slow improvement of symptoms and the flow of urine May need another treatment after several years because the prostate continues to grow For 4-6 weeks after the surgery: Drink 1-2 litres every day, especially water Do not lift anything heavier than 5 kilograms Do not do any heavy exercise and avoid bike riding Do not take thermal baths or go to the sauna Prevent constipation by adapting your diet Discuss any prescribed medication with your doctor Avoid having sex for 2-3 weeks. Your semen may be stained with blood for a few weeks. Page 14 / 15
15 Intra-prostatic ethanol and botulinum toxin injections Today, ethanol and botulinum toxin injections are explored as possible treatment options for BPE. They may become accepted in the future, but today they are still experimental and are usually used in clinical trials. Intra-prostatic ethanol injections Ethanol, which is pure alcohol, is injected through the urethra or the rectum into the prostate tissue. The aim is to reduce the size of the prostate and improve the flow of urine. Intra-prostatic botulinum toxin injections Botulinum toxin is widely known by one of its trade names Botox. It is a strong toxic substance which is used in cosmetic surgery. In BPE treatment it blocks nerve endings and relaxes the smooth muscle in the prostate. Botulinum toxin reduces the size of the prostate and improves the flow of urine. It can be injected through the urethra, the rectum, or the perineum. Recent studies do not support the use of botulinum toxin for the treatment of lower urinary tract symptoms in men with BPE. This information was updated in September This leaflet is part of EAU Patient Information on BPE. It contains general information about benign prostatic enlargement. If you have any specific questions about your individual medical situation you should consult your doctor or other professional healthcare provider. This information was produced by the European Association of Urology (EAU) in collaboration with the EAU Section of Uro-Technology (ESUT), Europa Uomo, and the European Association of Urology Nurses (EAUN). The content of this leaflet is in line with the EAU Guidelines. You can find this and other information on urological diseases at our website: Series contributors: Prof. Thorsten Bach Prof. Alexander Bachmann Prof. Dr. Christopher Chapple Prof. Louis Denis Mr. Günter Feick Prof. Stavros Gravas Dr. Hashim Hashim Prof. Rolf Muschter Dr. Cosimo De Nunzio Mr. Hans Ransdorp Prof. Jens Rassweiler Ms. Maria Russo Dr. Roman Sosnowski Prof. Andrea Tubaro Hamburg, Germany Basel, Switzerland Sheffield, United Kingdom Antwerp, Belgium Gehrden, Germany Larissa, Greece Bristol, United Kingdom Rotenburg, Germany Rome, Italy Bussem, The Netherlands Heilbronn, Germany Orbassano, Turin, Italy Warsaw, Poland Rome, Italy Page 15 / 15
Patient Information. Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE
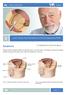 Patient Information English 32 Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE Symptoms The underlined terms are listed in the glossary. Benign prostatic enlargement (BPE) can affect the way you
Patient Information English 32 Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE Symptoms The underlined terms are listed in the glossary. Benign prostatic enlargement (BPE) can affect the way you
Information for Patients. Benign Prostatic Enlargement. English
 Information for Patients Benign Prostatic Enlargement English Table of contents What is the prostate?... 3 What are BPH, BPE, and BPO?... 3 Symptoms... 3 Types of symptoms... 4 Diagnosis... 4 Medical history...
Information for Patients Benign Prostatic Enlargement English Table of contents What is the prostate?... 3 What are BPH, BPE, and BPO?... 3 Symptoms... 3 Types of symptoms... 4 Diagnosis... 4 Medical history...
Second-line Treatment for OAB
 Patient Information English 35 Second-line Treatment for OAB The underlined terms are listed in the glossary. Sometimes the drugs your doctor prescribed do not improve your overactive symptoms (OAB). In
Patient Information English 35 Second-line Treatment for OAB The underlined terms are listed in the glossary. Sometimes the drugs your doctor prescribed do not improve your overactive symptoms (OAB). In
Benign Prostatic Hyperplasia (BPH)
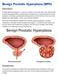 Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Reproduced with the kind permission of Health Press Ltd, Oxford
 Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
Information for Patients. Overactive bladder syndrome (OAB) English
 Information for Patients Overactive bladder syndrome (OAB) English Table of contents What is the bladder?... 3 What are overactive bladder symptoms?... 3 What causes overactive bladder symptoms?... 3 Diagnosis
Information for Patients Overactive bladder syndrome (OAB) English Table of contents What is the bladder?... 3 What are overactive bladder symptoms?... 3 What causes overactive bladder symptoms?... 3 Diagnosis
Transurethral Resection of Prostate (TURP)
 Transurethral Resection of Prostate (TURP) Department of Urology Patient Information What What and and where where is the is prostate? the prostate? The prostate is a small gland, about the size of a walnut,
Transurethral Resection of Prostate (TURP) Department of Urology Patient Information What What and and where where is the is prostate? the prostate? The prostate is a small gland, about the size of a walnut,
What is Benign Prostatic Hyperplasia (BPH)?
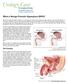 What is Benign Prostatic Hyperplasia (BPH)? Benign prostatic hyperplasia (BPH) is an enlarged prostate. The prostate goes through two main growth periods as a man ages. The first occurs early in puberty,
What is Benign Prostatic Hyperplasia (BPH)? Benign prostatic hyperplasia (BPH) is an enlarged prostate. The prostate goes through two main growth periods as a man ages. The first occurs early in puberty,
Prostate surgery. What is the prostate? What is a TURP? Why is a TURP operation necessary? Deciding to have a TURP operation.
 What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
Diagnosis and Classification of Prostate Cancer
 Patient Information English 32 Diagnosis and Classification of Prostate Cancer The underlined terms are listed in the glossary. prostate biopsy is the only test that can confirm a prostate cancer diagnosis.
Patient Information English 32 Diagnosis and Classification of Prostate Cancer The underlined terms are listed in the glossary. prostate biopsy is the only test that can confirm a prostate cancer diagnosis.
Treatment of Kidney and Ureteral Stones
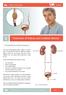 Patient Information English 3 Treatment of Kidney and Ureteral Stones The underlined terms are listed in the glossary. You have been diagnosed with a kidney or ureteral stone. This leaflet describes the
Patient Information English 3 Treatment of Kidney and Ureteral Stones The underlined terms are listed in the glossary. You have been diagnosed with a kidney or ureteral stone. This leaflet describes the
Experience the Innovative Therapy for Benign Prostate Enlargement
 Experience the Innovative Therapy for Benign Prostate Enlargement A Guide to Treatment of Benign Prostatic Hyperplasia 1. 2. The Prostate The prostate gland is a part of the male reproductive system. A
Experience the Innovative Therapy for Benign Prostate Enlargement A Guide to Treatment of Benign Prostatic Hyperplasia 1. 2. The Prostate The prostate gland is a part of the male reproductive system. A
Rezūm procedure for the Prostate
 Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Trans Urethral Resection of Prostate (TURP)
 Trans Urethral Resection of Prostate (TURP) Patient Information Author ID: SF Leaflet Number: Urol 010 Version: 6 Name of Leaflet: Trans Urethral Resection of Prostate (TURP) Date Produced: March 2018
Trans Urethral Resection of Prostate (TURP) Patient Information Author ID: SF Leaflet Number: Urol 010 Version: 6 Name of Leaflet: Trans Urethral Resection of Prostate (TURP) Date Produced: March 2018
Executive Summary. Non-drug local procedures for treatment of benign prostatic hyperplasia 1. IQWiG Reports - Commission No.
 IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
Transurethral Resection of the Prostate (TURP)
 Transurethral Resection of the Prostate (TURP) UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Transurethral Resection of the Prostate (TURP) UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Surgery for an enlarged prostate transurethral resection of the prostate
 Surgery for an enlarged prostate transurethral resection of the prostate Urology Department Patient Information Leaflet Introduction This leaflet is about surgery for an enlarged prostate, known medically
Surgery for an enlarged prostate transurethral resection of the prostate Urology Department Patient Information Leaflet Introduction This leaflet is about surgery for an enlarged prostate, known medically
UW MEDICINE PATIENT EDUCATION. About Your Surgery DRAFT
 UW MEDICINE PATIENT EDUCATION About Your Surgery Transurethral resection of the prostate (TURP) This handout describes a transurethral resection of the prostate. It also gives instructions to follow before
UW MEDICINE PATIENT EDUCATION About Your Surgery Transurethral resection of the prostate (TURP) This handout describes a transurethral resection of the prostate. It also gives instructions to follow before
Treating your enlarged prostate gland using holmium laser enucleation of the prostate (HoLEP)
 Treating your enlarged prostate gland using holmium laser enucleation of the prostate (HoLEP) This leaflet will answer any questions you may have about having holmium laser treatment for your enlarged
Treating your enlarged prostate gland using holmium laser enucleation of the prostate (HoLEP) This leaflet will answer any questions you may have about having holmium laser treatment for your enlarged
Transurethral Resection of Prostate
 Transurethral Resection of Prostate Information for Patients This leaflet explains: What does the procedure involve?...2 What are the alternatives to this procedure?...2 What should I expect before the
Transurethral Resection of Prostate Information for Patients This leaflet explains: What does the procedure involve?...2 What are the alternatives to this procedure?...2 What should I expect before the
Patient Information. Basic Information on Overactive Bladder Symptoms. pubic bone. urethra. scrotum. bladder. vaginal canal
 Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
MODULE 3: BENIGN PROSTATIC HYPERTROPHY
 MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
HOLEP (HOLMIUM LASER ENUCLEATION OF PROSTATE )
 HOLEP (HOLMIUM LASER ENUCLEATION OF PROSTATE ) What does the procedure involve? Removal of obstructing prostate tissue using a telescope and a laser. What are the alternatives to this procedure? Alternatives
HOLEP (HOLMIUM LASER ENUCLEATION OF PROSTATE ) What does the procedure involve? Removal of obstructing prostate tissue using a telescope and a laser. What are the alternatives to this procedure? Alternatives
Trans urethral resection of prostate (TURP)
 Trans urethral resection of prostate (TURP) Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST What is the prostate? Only men have a prostate
Trans urethral resection of prostate (TURP) Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST What is the prostate? Only men have a prostate
THE UROLOGY GROUP
 THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
Laser Trans Urethral Resection of Prostate (TURP)
 Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Transurethral Resection of Prostate (TURP)
 Transurethral Resection of Prostate (TURP) This leaflet explains: What does the procedure involve?... 2 What are the alternatives to this procedure?... 2 What should I expect before the procedure?... 2
Transurethral Resection of Prostate (TURP) This leaflet explains: What does the procedure involve?... 2 What are the alternatives to this procedure?... 2 What should I expect before the procedure?... 2
Having a trans-urethral resection of the prostate (TURP)
 Having a trans-urethral resection of the prostate (TURP) This leaflet gives you information about having a TURP, which is an operation to treat an enlarged prostate gland. It explains the benefits, alternatives
Having a trans-urethral resection of the prostate (TURP) This leaflet gives you information about having a TURP, which is an operation to treat an enlarged prostate gland. It explains the benefits, alternatives
TRANSURETHRAL RESECTION OF THE PROSTATE
 TRANSURETHRAL RESECTION OF THE PROSTATE A discussion of the operation and the pre and post operative care You and your doctor have considered the possibility that you have a transurethral resection of
TRANSURETHRAL RESECTION OF THE PROSTATE A discussion of the operation and the pre and post operative care You and your doctor have considered the possibility that you have a transurethral resection of
Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information
 PATIENT INFORMATION Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information What is the evidence base for this information? This leaflet includes advice from
PATIENT INFORMATION Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information What is the evidence base for this information? This leaflet includes advice from
Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients
 Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i The prostate The prostate is a small gland which is found only in men. It is situated at the base of the bladder
Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i The prostate The prostate is a small gland which is found only in men. It is situated at the base of the bladder
Transurethral Resection of the Prostate (TURP)
 Transurethral Resection of the Prostate (TURP) Information for patients Department of Urology The York Hospital Wigginton Road York YO31 8HE Tel: 01904 631313 Contents Page How is my operation carried
Transurethral Resection of the Prostate (TURP) Information for patients Department of Urology The York Hospital Wigginton Road York YO31 8HE Tel: 01904 631313 Contents Page How is my operation carried
Trans Urethral Resection of Bladder Tumour
 Trans Urethral Resection of Bladder Tumour Department of Urology 2 Patient Information Contents Where is the bladder and what does it do? 3 What is non invasive cancer of the bladder? 4 How is bladder
Trans Urethral Resection of Bladder Tumour Department of Urology 2 Patient Information Contents Where is the bladder and what does it do? 3 What is non invasive cancer of the bladder? 4 How is bladder
Transurethral Resection of the Prostate (TURP) Transurethral Incision of the Prostate (TUIP) PROCEDURE EDUCATION LITERATURE
 Transurethral Resection of the Prostate (TURP) Transurethral Incision of the Prostate (TUIP) PROCEDURE EDUCATION LITERATURE We recommend that you read this handout carefully in order to prepare yourself
Transurethral Resection of the Prostate (TURP) Transurethral Incision of the Prostate (TUIP) PROCEDURE EDUCATION LITERATURE We recommend that you read this handout carefully in order to prepare yourself
Glossary of Terms Primary Urethral Cancer
 Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Bladder neck incision: procedure-specific information
 PATIENT INFORMATION Bladder neck incision: procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British Association of
PATIENT INFORMATION Bladder neck incision: procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British Association of
CYSTOSCOPY & TRANSURETHRAL RESECTION OF THE PROSTATE
 Associates: Dr Kim Pese Dr Kym Horsell Dr Michael Chong Dr Jason Lee The Tennyson Centre Suite 19, First Floor 520 South Road Kurralta Park SA 5037 Appointments: 08 8292 2399 Fax: 08 8292 2388 admin@urologicalsolutions.com.au
Associates: Dr Kim Pese Dr Kym Horsell Dr Michael Chong Dr Jason Lee The Tennyson Centre Suite 19, First Floor 520 South Road Kurralta Park SA 5037 Appointments: 08 8292 2399 Fax: 08 8292 2388 admin@urologicalsolutions.com.au
Transurethral Prostatectomy (TURP) for Benign Disease
 Transurethral Prostatectomy (TURP) for Benign Disease Whiston Hospital Warrington Road, Prescot, Merseyside, L35 5DR Telephone: 0151 426 1600 St Helens Hospital Marshall Cross Road, St Helens, Merseyside,
Transurethral Prostatectomy (TURP) for Benign Disease Whiston Hospital Warrington Road, Prescot, Merseyside, L35 5DR Telephone: 0151 426 1600 St Helens Hospital Marshall Cross Road, St Helens, Merseyside,
You have been booked for a. Flexible Cystoscopy. Under Local Anaesthetic
 You have been booked for a Flexible Cystoscopy Under Local Anaesthetic 1 WHAT IS A FLEXIBLE CYSTOSCOPY A flexible cystoscopy is a test to examine the uretha (waterpipe) and bladder using a thin, lighted
You have been booked for a Flexible Cystoscopy Under Local Anaesthetic 1 WHAT IS A FLEXIBLE CYSTOSCOPY A flexible cystoscopy is a test to examine the uretha (waterpipe) and bladder using a thin, lighted
Uroformation. Prostate Surgery. Robotic Assisted Laparoscopic Prostatectomy (RALP)
 Uroformation Prostate Surgery Robotic Assisted Laparoscopic Prostatectomy (RALP) The Uroformation series is a co-operative venture in patient centered urological information. June 2014 What is the Prostate?
Uroformation Prostate Surgery Robotic Assisted Laparoscopic Prostatectomy (RALP) The Uroformation series is a co-operative venture in patient centered urological information. June 2014 What is the Prostate?
Diagnosis and classification
 Patient Information English 2 Diagnosis and classification The underlined terms are listed in the glossary. Signs and symptoms Blood in the urine is the most common symptom when a bladder tumour is present.
Patient Information English 2 Diagnosis and classification The underlined terms are listed in the glossary. Signs and symptoms Blood in the urine is the most common symptom when a bladder tumour is present.
P ROLIEVE. Thermodilatation System. The Prolieve System Patient Information is Directed to You, the Patient. A Transurethral Microwave Therapy Device
 P ROLIEVE Thermodilatation System A Transurethral Microwave Therapy Device The Prolieve System Patient Information is Directed to You, the Patient. Contents Why am I being treated with the Prolieve Thermodilatation
P ROLIEVE Thermodilatation System A Transurethral Microwave Therapy Device The Prolieve System Patient Information is Directed to You, the Patient. Contents Why am I being treated with the Prolieve Thermodilatation
TURBT (Transurethral Resection of the Bladder Tumour)
 TURBT (Transurethral Resection of the Bladder Tumour) Exceptional healthcare, personally delivered Trans Urethral Resection of Bladder Tumour (TURBT) This leaflet answers some of the questions you may
TURBT (Transurethral Resection of the Bladder Tumour) Exceptional healthcare, personally delivered Trans Urethral Resection of Bladder Tumour (TURBT) This leaflet answers some of the questions you may
Prostate Artery Embolisation (PAE)
 Service: Imaging Prostate Artery Embolisation (PAE) Exceptional healthcare, personally delivered Ask 3 Questions The team delivering your healthcare want to encourage you to become as involved as possible
Service: Imaging Prostate Artery Embolisation (PAE) Exceptional healthcare, personally delivered Ask 3 Questions The team delivering your healthcare want to encourage you to become as involved as possible
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries
 Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH
 Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH The more you know, the better you ll feel. You ve likely had a discussion with your doctor about BPH 1. What follows are some
Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH The more you know, the better you ll feel. You ve likely had a discussion with your doctor about BPH 1. What follows are some
Control & confidence. You deserve both.
 Learn more about BPH and Plasma therapy Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH Your doctor is always happy to offer all the guidance you need so that you feel completely
Learn more about BPH and Plasma therapy Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH Your doctor is always happy to offer all the guidance you need so that you feel completely
Cystoscopy. Information for patients Spinal Injuries
 Cystoscopy Information for patients Spinal Injuries page 2 of 8 What is a cystoscopy? A cystoscopy is a procedure to look inside the bladder using a thin camera called a cystoscope. A cystoscope is inserted
Cystoscopy Information for patients Spinal Injuries page 2 of 8 What is a cystoscopy? A cystoscopy is a procedure to look inside the bladder using a thin camera called a cystoscope. A cystoscope is inserted
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
TURP (Trans Urethral Resection of the Prostate)
 TURP (Trans Urethral Resection of the Prostate) UHN Information for patients You are having your operation at: (please check one) Toronto General Hospital Princess Margaret Cancer Centre Toronto Western
TURP (Trans Urethral Resection of the Prostate) UHN Information for patients You are having your operation at: (please check one) Toronto General Hospital Princess Margaret Cancer Centre Toronto Western
Laser Prostatectomy Urology Patient information Leaflet
 Laser Prostatectomy Urology Patient information Leaflet Page 1 Laser Prostatectomy Your surgeon has recommended that you have laser surgery to your prostate. We hope that this leaflet answers any questions
Laser Prostatectomy Urology Patient information Leaflet Page 1 Laser Prostatectomy Your surgeon has recommended that you have laser surgery to your prostate. We hope that this leaflet answers any questions
Treating BPH: Comparing Rezum UroLift and HoLEP
 Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
Information for Patients. Urinary Incontinence. English
 Information for Patients Urinary Incontinence English Table of contents What is urinary incontinence?... 3 Causes of urinary incontinence... 3 Types of urinary incontinence... 3 Stress urinary incontinence...
Information for Patients Urinary Incontinence English Table of contents What is urinary incontinence?... 3 Causes of urinary incontinence... 3 Types of urinary incontinence... 3 Stress urinary incontinence...
Treatment for ED. Education and couple assessment. Lifestyle advice. Patient Information. Page 1 / 9. Patient Information - Treatment for ED
 Patient Information English 3 Treatment for ED The underlined terms are listed in the glossary. Erectile dysfunction (ED) is a common condition. Although it is not life threatening, it can negatively affect
Patient Information English 3 Treatment for ED The underlined terms are listed in the glossary. Erectile dysfunction (ED) is a common condition. Although it is not life threatening, it can negatively affect
About Your Procedure
 UW MEDICINE PATIENT EDUCATION About Your Procedure UroLift This handout describes a UroLift procedure to treat an enlarged prostate. It also gives instructions to follow before and after your procedure.
UW MEDICINE PATIENT EDUCATION About Your Procedure UroLift This handout describes a UroLift procedure to treat an enlarged prostate. It also gives instructions to follow before and after your procedure.
Frequently Asked Questions about Prostate Cancer. General questions. Patient Information. What is prostate cancer?
 Patient Information English Frequently Asked Questions about Prostate Cancer The underlined terms are listed in the glossary. General questions What is prostate cancer? Prostate cancer is a malignant tumour
Patient Information English Frequently Asked Questions about Prostate Cancer The underlined terms are listed in the glossary. General questions What is prostate cancer? Prostate cancer is a malignant tumour
Cystoscopy and urethroscopy
 Page 1 of 5 Cystoscopy and urethroscopy Introduction This leaflet is provided to give you information about undergoing cystoscopy and/or urethroscopy. What is a cystoscopy? A cystoscopy is a procedure
Page 1 of 5 Cystoscopy and urethroscopy Introduction This leaflet is provided to give you information about undergoing cystoscopy and/or urethroscopy. What is a cystoscopy? A cystoscopy is a procedure
Treatment for bladder tumours (transurethral resection of bladder tumour (TURBT))
 Treatment for bladder tumours (transurethral resection of bladder tumour (TURBT)) Information for patients from the Urology Department You have had a cystoscopy or other examination that has shown that
Treatment for bladder tumours (transurethral resection of bladder tumour (TURBT)) Information for patients from the Urology Department You have had a cystoscopy or other examination that has shown that
Having prostate surgery
 Having prostate surgery Urology department 01935 384 394 yeovilhospital.nhs.uk The most common operation on the prostate is known as a Transurethral Resection of the Prostate (TURP). Sometimes, it is necessary
Having prostate surgery Urology department 01935 384 394 yeovilhospital.nhs.uk The most common operation on the prostate is known as a Transurethral Resection of the Prostate (TURP). Sometimes, it is necessary
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Surgical procedures for benign prostatic hyperplasia: A nationwide survey in Japan
 International Journal of Urology (2011) 18, 166 170 doi: 10.1111/j.1442-2042.2010.02687.x Short Communicationiju_2687 166..170 Surgical procedures for benign prostatic hyperplasia: A nationwide survey
International Journal of Urology (2011) 18, 166 170 doi: 10.1111/j.1442-2042.2010.02687.x Short Communicationiju_2687 166..170 Surgical procedures for benign prostatic hyperplasia: A nationwide survey
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer.
 What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
Radical Cystectomy A Patient s Guide
 Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Ambulatory Emergency Care Pathways. Acute Painful Bladder Outflow Obstruction
 Ambulatory Emergency Care Pathways Acute Painful Bladder Outflow Obstruction Effective Date: November 2011 Content Summary Ref Title Description 1 Condition Details Identifies pathway details and clinical
Ambulatory Emergency Care Pathways Acute Painful Bladder Outflow Obstruction Effective Date: November 2011 Content Summary Ref Title Description 1 Condition Details Identifies pathway details and clinical
TURP - TransUrethral Resection of the Prostate
 TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
w This information leaflet contains basic information Basic Information on Kidney and Ureteral Stones What is a stone? Patient Information Go Online
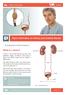 Patient Information English Basic Information on Kidney and Ureteral Stones The underlined terms are listed in the glossary. What is a stone? right kidney left kidney A stone is a hard, solid mass that
Patient Information English Basic Information on Kidney and Ureteral Stones The underlined terms are listed in the glossary. What is a stone? right kidney left kidney A stone is a hard, solid mass that
Transurethral Resection of Bladder Tumours
 2014 Transurethral Resection of Bladder Tumours Transurethral Resection of Bladder Tumours What is the bladder? The bladder is a hollow, muscular organ that stores urine (pee). Urine travels from your
2014 Transurethral Resection of Bladder Tumours Transurethral Resection of Bladder Tumours What is the bladder? The bladder is a hollow, muscular organ that stores urine (pee). Urine travels from your
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients
 Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
Suprapubic Catheter Insertion Clinic
 Suprapubic Catheter Insertion Clinic Exceptional healthcare, personally delivered Suprapubic Catheter Why may I need a suprapubic catheter? A suprapubic catheter enters the bladder through an incision
Suprapubic Catheter Insertion Clinic Exceptional healthcare, personally delivered Suprapubic Catheter Why may I need a suprapubic catheter? A suprapubic catheter enters the bladder through an incision
Glossary of Terms Prostate Cancer
 Patient Information English Glossary of Terms Prostate Cancer Active surveillance A form of treatment in which the doctor actively monitors the tumour or tumours and their growth, based on a strict visiting
Patient Information English Glossary of Terms Prostate Cancer Active surveillance A form of treatment in which the doctor actively monitors the tumour or tumours and their growth, based on a strict visiting
Treating narrowing of the urethra
 Treating narrowing of the urethra Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been recommended to have a procedure to treat narrowing of the urethra.
Treating narrowing of the urethra Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been recommended to have a procedure to treat narrowing of the urethra.
Symptoms, Diagnosis and Classification
 Patient Information English 2 Symptoms, Diagnosis and Classification The underlined terms are listed in the glossary. Signs and symptoms Blood in the urine is the most common symptom when a bladder tumour
Patient Information English 2 Symptoms, Diagnosis and Classification The underlined terms are listed in the glossary. Signs and symptoms Blood in the urine is the most common symptom when a bladder tumour
Benign prostatic hyperplasia (BPH)
 Diseases and Conditions Benign prostatic hyperplasia (BPH) By Mayo Clinic Staff Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate
Diseases and Conditions Benign prostatic hyperplasia (BPH) By Mayo Clinic Staff Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate
Examination of the ureter (ureteroscopy) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Examination of the ureter (ureteroscopy) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Examination of the ureter (ureteroscopy) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Prostate Enlargement: Benign Prostatic Hyperplasia
 Prostate Enlargement: Benign Prostatic Hyperplasia National Kidney and Urologic Diseases Information Clearinghouse What is benign prostatic hyperplasia? Benign prostatic hyperplasiaalso called BPHis a
Prostate Enlargement: Benign Prostatic Hyperplasia National Kidney and Urologic Diseases Information Clearinghouse What is benign prostatic hyperplasia? Benign prostatic hyperplasiaalso called BPHis a
Kaiser Oakland Urology
 Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
HOLMIUM LASER ENUCLEATION OF THE PROSTATE (HoLEP) INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk HOLMIUM
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk HOLMIUM
Retropubic Prostatectomy
 2014 Retropubic Prostatectomy Retropubic Prostatectomy What is the prostate? The prostate is a gland that makes a fluid that helps sperm move. It also gives nourishment for the sperm. It is about the size
2014 Retropubic Prostatectomy Retropubic Prostatectomy What is the prostate? The prostate is a gland that makes a fluid that helps sperm move. It also gives nourishment for the sperm. It is about the size
LDR prostate brachytherapy
 LDR prostate brachytherapy Introduction Low dose rate (LDR) prostate brachytherapy is a modern, effective minimally invasive treatment appropriate for many men with early prostate cancer. I perform this
LDR prostate brachytherapy Introduction Low dose rate (LDR) prostate brachytherapy is a modern, effective minimally invasive treatment appropriate for many men with early prostate cancer. I perform this
BLADDER TUMOUR RESECTION
 BLADDER TUMOUR RESECTION (TRANSURETHRAL RESECTION OF A BLADDER TUMOUR / ) AN INFORMATION LEAFLET Written by: Department of Urology January 2017 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside:
BLADDER TUMOUR RESECTION (TRANSURETHRAL RESECTION OF A BLADDER TUMOUR / ) AN INFORMATION LEAFLET Written by: Department of Urology January 2017 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside:
GUIDELINES ON NON-NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (BPO)
 GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (BPO) (Text update pril 2014) S. Gravas (chair),. Bachmann,. Descazeaud, M. Drake, C. Gratzke, S. Madersbacher, C. Mamoulakis,
GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (BPO) (Text update pril 2014) S. Gravas (chair),. Bachmann,. Descazeaud, M. Drake, C. Gratzke, S. Madersbacher, C. Mamoulakis,
Caring for a Nephrostomy and what is Ureteric Stenting
 Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
ANGIOPLASTY AND STENTING
 ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
Managing your bladder with a Supra-pubic catheter at home
 Managing your bladder with a Supra-pubic catheter at home Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. Managing your bladder with a Supra-pubic catheter at home The purpose
Managing your bladder with a Supra-pubic catheter at home Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. Managing your bladder with a Supra-pubic catheter at home The purpose
Cryotherapy for localised prostate cancer
 Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
Flexible Cystoscopy. Patient Information
 Flexible Cystoscopy Patient Information 05/11/2012 Mehul Pankaj Raithatha 3 rd Year Medical Student Barts and the London - School of Medicine and Dentistry INTRODUCTION The urinary bladder is the organ
Flexible Cystoscopy Patient Information 05/11/2012 Mehul Pankaj Raithatha 3 rd Year Medical Student Barts and the London - School of Medicine and Dentistry INTRODUCTION The urinary bladder is the organ
EAU GUIDELINES POCKET EDITION 3
 EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
What is ureteral reimplantation?
 What is ureteral reimplantation? Ureteral reimplantation is surgery to disconnect the ureter from the bladder and reattach it in a better position. One or both ureters may need to be reimplanted. To understand
What is ureteral reimplantation? Ureteral reimplantation is surgery to disconnect the ureter from the bladder and reattach it in a better position. One or both ureters may need to be reimplanted. To understand
Bladder neck incision
 Bladder neck incision What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content may apply to you. Feel free
Bladder neck incision What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content may apply to you. Feel free
Original Policy Date
 MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
Suprapubic Catheter Insertion Clinic
 Suprapubic Catheter Insertion Clinic Exceptional healthcare, personally delivered Suprapubic Catheter A urinary catheter is a tube used to drain urine from the bladder. The commonest catheters are ones
Suprapubic Catheter Insertion Clinic Exceptional healthcare, personally delivered Suprapubic Catheter A urinary catheter is a tube used to drain urine from the bladder. The commonest catheters are ones
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
3. Urinary Catheters. Indications. Methods of Bladder Catheterization. Hashim Hashim
 3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile)
 Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
CYSTOSCOPY PATIENT INFORMATION
 CYSTOSCOPY PATIENT INFORMATION ADHB Urology Department; Reviewed FEB 2005 Ubix code UPEB3 1 The information contained in this booklet is intended to assist you in understanding your proposed surgery; some
CYSTOSCOPY PATIENT INFORMATION ADHB Urology Department; Reviewed FEB 2005 Ubix code UPEB3 1 The information contained in this booklet is intended to assist you in understanding your proposed surgery; some
A patient information sheet from. What are the alternatives? Before the procedure. page 1 of 5
 A patient information sheet from Transurethral Resection of the Prostate (for Benign Disease) This operation involves the telescopic removal or incision of the obstructing, central part of the prostate
A patient information sheet from Transurethral Resection of the Prostate (for Benign Disease) This operation involves the telescopic removal or incision of the obstructing, central part of the prostate
