Da Vinci Robotic Hysterectomy and removal of ovaries (oophorectomy) with discharge advice
|
|
|
- Claire Byrd
- 5 years ago
- Views:
Transcription
1 Da Vinci Robotic Hysterectomy and removal of ovaries (oophorectomy) with discharge advice Patient information leaflet Royal Surrey County Hospital Frimley Park Hospital Ashford and St. Peters Hospital Surrey and Sussex Hospitals
2 This leaflet has been written for women who have a diagnosis or possible diagnosis of a gynaecological cancer and have been advised to have a robotic hysterectomy. Are there any alternative procedures? If it is decided that the robot is not suitable, a traditional abdominal hysterectomy could be performed. If you are unable, or do not wish, to have an operation, hormonal or radiotherapy treatment may be offered. What is a Da Vinci robotic hysterectomy and removal of ovaries? The Da Vinci robotic system is designed to provide your surgeon with a clearer view and more precision during the procedure. Your surgeon controls the robot, which converts their hand movements into smaller, more precise movements of tiny instruments inside your body. Though it is called a robot, your surgeon controls all the movements during your operation. The robot allows your surgeon to perform complex procedures through five small cuts in your abdomen. Traditional abdominal hysterectomies for gynaecological cancers are performed by a long vertical incision (from the pubic bone to just above the navel). This can be painful for patients, with a longer stay in hospital and longer recovery. A robotic hysterectomy is a less invasive procedure leaving the patient with five small cuts on the abdomen which will be stitched following your surgery. For most women, it offers numerous benefits over the more traditional hysterectomy. Less pain Less blood loss and need for transfusion Less risk of infection Shorter stay in hospital Quicker recovery and return to normal activities Small incisions and minimal scaring As with any surgery, these benefits cannot be guaranteed. 2
3 Factors that may increase the risk of complications: Pre-existing heart or lung problems/condition Previous abdominal/pelvic surgery Smoking Obesity What happens during the procedure? Five small cuts are made in your abdomen through which the arms of the robot are positioned. A small amount of carbon dioxide gas will be used to expand your abdomen to make it easier for the surgeon to view the organs. The surgeon removes the lymph glands in the pelvis through the small abdominal cuts. The fallopian tubes and ovaries are initially freed from their attachments and will be removed with the uterus and cervix through the vagina. If the uterus is too big (bulky), removal through the vagina might not be appropriate and a little cut will be made along the bikini line, to enable your surgeon to remove your ovaries, uterus and cervix safely. It may not be necessary to remove your ovaries. If applicable, that would be discussed with you during your consultation in a clinic and during your consenting for the surgery. If your surgeon has consented you for a Radical Hysterectomy. This will involve the removal of the uterus and cervix as well as the removal of the tissue on the sides of the uterus and the cervix (parametrium), and the top part of the vagina. Nearby lymphatic nodes are removed either during this procedure or as a separate procedure beforehand. What will happen prior to your admission for surgery? Your operation will be discussed with you in detail with your surgeon prior to consent for surgery. To enable you to make an informed decision, the surgery will be fully explained to you by the surgical team. You will also have the opportunity to ask questions and voice your concerns prior to signing the consent form. 3
4 The clinical nurse specialist will be available for support and information. You will be asked to attend a pre-assessment clinic to ensure that all the necessary investigations are undertaken to assess your fitness for anaesthetic and surgery. It will also give you a further opportunity to ask questions related to the surgery. On request we can arrange for you to visit the surgical ward. Your partner, a close relative or friend is welcome to attend any of these appointments. Please inform your surgical team as well as pre-operative assessment nurse about all the medications you are taking as some might need to be stopped prior to your surgery (e.g warfarin, aspirin). Please bring your medicine list with you and ask your doctor if you can take them prior to the surgery. You will be admitted to either a surgical ward the day before surgery, or the Elective Surgical Unit (ESU) on the day of surgery. Following your operation, you will be transferred to the Surgical Short Stay Unit (SSSU) or surgical ward. On the morning of your surgery, the anaesthetist looking after you will discuss pain relief following your operation. You will also see your surgical team. What are the risks and side effects of the surgery? As with any surgery, there are risks of bleeding, bruising damage to neighbouring structures and infection. You may require a blood transfusion during your admission however the risk is low. Main side effects following surgery: Deep vein thrombosis and pulmonary emboli: anti-emboli (T.E.D) stockings, Fragmin /Dalteparin, (sub-cutaneous blood thinning injection) good hydration and early movement following surgery will help reduce the risk. Changes in bladder function Changes in feeling during intercourse 4
5 Changes in bowel function Lymphoedema Numbness around scar and tops of legs What happens following the operation? Following your robotic surgery the plan would be for you to be discharged the following day. Your catheter may either be removed the same evening of the operation or the following morning. Nurses on the ward will be monitoring your urination function prior to your discharge from the ward. After urinary catheter removal, some patients experience urination difficulties; that could be caused by postsurgical inflammation, pain and damage to nerve endings. This may require going home with the catheter. The ward staff will show you how to look after it and your surgical team will arrange a trial without catheter (TWOC) at your local hospital or back at the Royal Surrey County Hospital a week later. If you have had a radical hysterectomy, you will be going home with a catheter, usually for a week. Drinking plenty of fluids of between 6 to 8 glasses a day are important to prevent bladder infection while the catheter is in place. Following the removal, it is important for us to ensure your bladder is emptying properly. The nurse looking after you will check this. If you are discharged with a bladder catheter, it relieves pressure on the surgical site and allows greater healing of the tiny nerves to the bladder. These nerves help to sense when your bladder is full. They also help you empty your bladder when it is full. The catheter also prevents your bladder from becoming too full until you can pass water on your own. You may experience some wind pains in the abdomen which may also cause shoulder pain. This is caused by the carbon dioxide gas used during surgery. This settles eventually and is helped by eating small, regular meals. Some patients find peppermint tea, cordial and plenty of walking around helpful to shift the gas. It is common to feel low in mood following surgery, especially when you may have a diagnosis of cancer. You might find it helpful to talk to the ward nurses or clinical nurse specialist to ease these anxieties. 5
6 Wound care Your dressings will be checked prior to your discharge. You will have five small dressings covering the incisions; these can be removed two to three days following your surgery. The wound can stay exposed. When having a shower or washing, ensure you dry your wounds completely to prevent wound break down or infection. If there is any sign of redness or soreness at the wound site, contact yourgp or Clinical Nurse Specialist for advice. If your ovaries were removed, you may experience hot flushes. These may start within a week following surgery. If you have a diagnosis of cervical cancer, hormone replacement can be prescribed. Your team will prescribe regular painkillers to take home with you. Your doctor or GP can provide a sick certificate on request for two to four weeks following a robotic hysterectomy. You will commence fragmin injections daily to prevent blood clots for four weeks following your surgery. The nurses will teach you how to administer them prior to discharge. Recovery can differ between patients this is only a guide Day two to three following your operation: You should be able to walk up and down stairs, take a shower, make drinks and prepare snacks. You may continue to need occasional painkillers. It is common to feel tired and sometime feel irritable, so ask other people to continue to support you and help with household chores. If you have severe increasing pain, constipation, oozing wound or feel feverish, contact the Clinical Nurse Specialist, your GP or Compton ward at the Royal Surrey as soon as possible. You may be experiencing some bleeding which will become darker and less heavy. If you have a fresh heavy blood loss, contact your ward, Clinical Nurse Specialist, GP or come straight to A&E as soon as possible. Do not use tampons for at least six weeks following surgery as they can cause infection in the vagina. The area around the incision 6
7 site (cut) will be numb because the nerves have been disturbed. It may take up to six months for the skin sensation to return. Drink a normal amount (not more than you feel you want). Eat plenty of fruit and vegetables to help your bowel get back to normal. Stay active and take plenty of rest periods as you feel necessary. One week following your operation: You will be able to make meals, although you may still feel quite tired and need to have rests. You will feel well enough to go to the shops but do not burden yourself with heavy shopping bags. You may still have periods of feeling low especially if you are tired. Listen to what your body is telling you and continue ask for support from others. If you were discharged with a urinary catheter, your TWOC will take place this week. Two weeks following your operation: Most women feel they are feeling better. You can take on light housework such as dusting, ironing small amounts and vacuum cleaning only carpets you see. Do not lift heavy furniture. When lifting anything from a low position, remember to bend your knees, keep your back straight and pull in your abdomen. Avoid standing for a long time. Any internal stitches begin to dissolve. You may notice an increased vaginal discharge which may be bloodstained. Discharge and spotting can continue for up to two months. Four weeks following your operation: You should feel quite well, and without any symptoms you had before the operation. You can take part in activities such as gentle walking, provided the five cuts have healed well. You may be able to return to work depending on what your job involves. You may drive if you feel safe to perform an emergency stop, but check with your insurance company. You need to be able to do an emergency stop and reverse safely. 7
8 Bowel function: After abdominal surgery bowel function normally is slow due to the anaesthetic and surgery. Analgesia used post-surgery might cause constipation in some patients. Dietary management (daily prune juice, high fibre or high bulk diets) or stool softeners medication or mild laxatives may help to prevent difficulties. Increased fluid intake also helps improve bowel function. Once your normal diet and activity are resumed, bowel function usually returns to normal. Bladder function: Following your surgery you may find you need to go to the toilet more frequently. Sometimes the sensation of bladder fullness is reduced and you may be less aware of a full bladder. If this happens, it is important to get into the habit of going to the toilet at regular intervals. Your Clinical Nurse Specialist will be able to give you advice. Pelvic floor exercises How does the pelvic floor work? The pelvic floor consist of layers of muscles which stretch from the pubic bone in front to the bottom of the back bone. The pelvic floor muscles are kept firm and slightly tense to stop urine leakage from the bladder and faeces from the bowel. When you pass urine or have a bowel motion the pelvic floor muscles relax, afterwards they tighten again to restore control. Why do pelvic floor exercises? Pelvic floor muscles can become weak and sag because of child birth, lack of exercise, pelvic surgery and the menopause. 8
9 Basic exercises These can be done in sitting, standing or lying position. Imagine you are trying to stop yourself passing wind and at the same time trying to stop your flow of urine mid-stream. The feeling is one of squeeze and lift, closing and drawing-up the back and front passages. This should be done without-pulling in your tummy, squeezing your legs together, tightening your buttocks, or holding your breath. When can I resume sexual activity? We would recommend no intercourse for six weeks whilst healing occurs. Some women worry about intercourse being painful and are concerned about resuming sex. In the beginning, gentle penetration in a position which is comfortable for you, is recommended. You may find your feeling during intercourse is a little numb. This should improve with time. Sometimes lubrication jelly can be used such as REPLENSE or SYLK both can be prescribed by your GP Your Clinical Nurse Specialist is available to help with advice with any of these issues. Menopause A leaflet is available for advice on treatment induced menopause. Please contact your clinical Nurse Specialist for a copy and further advice. Who do I contact following discharge? If you have any concerns when you are discharged, you can contact: Your Clinical Nurse Specialist Tel: ext 2038 Compton Ward Tel: ext 4941 or 6372 Gynae Oncology surgical team secretaries Tel: ext: 2176 / 2720 Nearest A&E department 9
10 Results All surgical specimens results will be discussed at the Multi-Disciplinary Team Meeting (MDT) by the histopathology team between two to three weeks post your surgery. Rarely in complex cases, your histology could be sent away for a second opinion for further review. The MDT meets weekly to review results and decide treatment accordingly. The Gynaecological Oncology Clinic Your next appointment after surgery will usually be between 2-3 weeks. All results, further treatment options and follow up will be discussed with you at this appointment by the Consultant Gynaecologist. The Clinical Nurse Specialist is available to discuss any concerns you may have. What happens for my follow up care? This depends on your diagnosis and if you have had previous treatment or will require any further treatment following your surgery. Most patients that receive a cancer diagnosis will be followed up for five years following completion of all your treatment. References Blake, Lambert and Crawford (1998) Gynaecological Oncology A Guide to Clinical Management pp162-4 Oxford University press (accessed ) Local support groups Gynaecological Cancer Support Group Location: Fountain Centre, St. Luke s Cancer Centre held on alternate months. Contact: Gynaecological Oncology CNS Telephone: ext
11 The Fountain Centre This is a centre which provides supportive and complimentary therapies such as reflexology and counselling services. Based in the Royal Surrey County Hospital. Telephone: / 19 Website: The Olive Centre Crawley Cancer Support Sussex Annexe, Crawley Hospital Telephone: Website: East Surrey Macmillan Cancer Support Centre East Surrey Hospital, Redhill, Surrey, RH1 5RH Telephone: informationcentre.sash@nhs.net National support information Macmillan Cancerbackup Freephone: Website: Cancer Research UK Website: Citizen Advice Bureau Telephone: Cancer Counselling Trust Telephone: Website: 11
12 PALS and Advocacy contact details Contact details of independent advocacy services can be provided by our Patient Advice and Liaison Service (PALS) who are located on the right hand side as you enter the main reception area. PALS are also your first point of contact for health related issues, questions or concerns surrounding RSCH patient services. Telephone: Opening hours: 9.00am 3.00pm, Monday to Friday If you would like information documents in large print, on tape or in another language or form please contact PALS. Past review date: June 2018 Future review date: June 2021 Author: Fiona Thompson PIN Royal Surrey County Hospital NHS Foundation Trust 2018
Total Abdominal Hysterectomy and removal of ovaries and fallopian tubes (salpingooophorectomy)
 Total Abdominal Hysterectomy and removal of ovaries and fallopian tubes (salpingooophorectomy) for Gynaecological Cancers with discharge information Gynaecology Department Patient information leaflet This
Total Abdominal Hysterectomy and removal of ovaries and fallopian tubes (salpingooophorectomy) for Gynaecological Cancers with discharge information Gynaecology Department Patient information leaflet This
Going home after major gynaecological surgery. Information for patients Gynaecology
 Going home after major gynaecological surgery Information for patients Gynaecology page 2 of 16 Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice
Going home after major gynaecological surgery Information for patients Gynaecology page 2 of 16 Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice
Going home after major gynaecological surgery. Information for patients Gynaecology
 Going home after major gynaecological surgery Information for patients Gynaecology Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice about what
Going home after major gynaecological surgery Information for patients Gynaecology Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice about what
Post-operative advice for women following gynaecological surgery
 Post-operative advice for women following gynaecological surgery Information for patients from Women s Health This information leaflet has been compiled to help aid a good recovery after your surgery.
Post-operative advice for women following gynaecological surgery Information for patients from Women s Health This information leaflet has been compiled to help aid a good recovery after your surgery.
Pelvic Floor Exercises
 Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Hysterectomy. Will my ovaries be removed at the same time?
 Hysterectomy What is a hysterectomy? This is a major operation which removes the uterus (womb) and cervix (neck of the womb) from your body. Why is hysterectomy performed? Some hysterectomies are performed
Hysterectomy What is a hysterectomy? This is a major operation which removes the uterus (womb) and cervix (neck of the womb) from your body. Why is hysterectomy performed? Some hysterectomies are performed
Endovenous Laser Treatment (EVLT)
 Endovenous Laser Treatment (EVLT) Day Surgery Unit Patient information leaflet What is Endovenous Laser Treatment (EVLT)? Endovenous laser therapy is a treatment for varicose veins which seals the vein
Endovenous Laser Treatment (EVLT) Day Surgery Unit Patient information leaflet What is Endovenous Laser Treatment (EVLT)? Endovenous laser therapy is a treatment for varicose veins which seals the vein
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Gynaecology Department Patient Information Leaflet
 Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Burch Colposuspension
 Burch Colposuspension Department of Gynaecology Patient Information What is is botulinum Burch colposuspension? toxin A? The operation is intended to support the bladder neck, which is the area between
Burch Colposuspension Department of Gynaecology Patient Information What is is botulinum Burch colposuspension? toxin A? The operation is intended to support the bladder neck, which is the area between
Laparoscopy. Patient information leaflet
 Laparoscopy Division of Adhesions Dye Test Treatment of Endometriosis Cystectomy Oophorectomy, Salpingectomy Salpingostomy Sterilisation Gynaecology Department Patient information leaflet What is a Laparoscopy?
Laparoscopy Division of Adhesions Dye Test Treatment of Endometriosis Cystectomy Oophorectomy, Salpingectomy Salpingostomy Sterilisation Gynaecology Department Patient information leaflet What is a Laparoscopy?
Sacrocolpopexy. Department of Gynaecology. Patient Information
 Sacrocolpopexy Department of Gynaecology 2 Patient Information What What is is a a sacrocolpopexy? This is an operation carried out to correct prolapse of the vaginal vault in patients who had a hysterectomy.
Sacrocolpopexy Department of Gynaecology 2 Patient Information What What is is a a sacrocolpopexy? This is an operation carried out to correct prolapse of the vaginal vault in patients who had a hysterectomy.
OG24 Posterior Repair
 www.rcseng.ac.uk www.rcsed.ac.uk www.pre-op.org OG24 Posterior Repair Expires end of February 2018 Issued May 2017 What is a posterior prolapse? A posterior prolapse is a bulge in the back wall of your
www.rcseng.ac.uk www.rcsed.ac.uk www.pre-op.org OG24 Posterior Repair Expires end of February 2018 Issued May 2017 What is a posterior prolapse? A posterior prolapse is a bulge in the back wall of your
There are many types of pelvic floor repair that may have been called:
 Pelvic floor repair This information explains: Overview... 1 Your admission Date... 2 The Anaesthetic... 2 The Repair Operation... 2 After the Operation... 2 Going home... 3 Getting back to Normal... 3
Pelvic floor repair This information explains: Overview... 1 Your admission Date... 2 The Anaesthetic... 2 The Repair Operation... 2 After the Operation... 2 Going home... 3 Getting back to Normal... 3
Repair of Epigastric, Umbilical or Incisional Hernia
 Repair of Epigastric, Umbilical or Incisional Hernia Day Surgery Unit Surgical Short Stay Unit Patient information leaflet 2 What is an epigastric, umbilical or incisional hernia? A hernia is a defect
Repair of Epigastric, Umbilical or Incisional Hernia Day Surgery Unit Surgical Short Stay Unit Patient information leaflet 2 What is an epigastric, umbilical or incisional hernia? A hernia is a defect
Open repair of Inguinal Hernia
 Open repair of Inguinal Hernia Day Surgery Unit Surgical Short Stay Unit Patient information leaflet What is an Inguinal Hernia? A hernia is a defect in the abdominal wall (stomach muscles). When there
Open repair of Inguinal Hernia Day Surgery Unit Surgical Short Stay Unit Patient information leaflet What is an Inguinal Hernia? A hernia is a defect in the abdominal wall (stomach muscles). When there
Laparoscopy. Department of Gynaecology. Patient information
 Laparoscopy Department of Gynaecology Patient information What is is a a laparoscopy? A laparoscopy is an operation performed under general anaesthetic to help your gynaecologist make a diagnosis by looking
Laparoscopy Department of Gynaecology Patient information What is is a a laparoscopy? A laparoscopy is an operation performed under general anaesthetic to help your gynaecologist make a diagnosis by looking
Leaving Hospital with a Stoma
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Leaving Hospital with a Stoma General Surgery Contents What is this leaflet all about? 3 What stoma equipment am I using? 3-4
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Leaving Hospital with a Stoma General Surgery Contents What is this leaflet all about? 3 What stoma equipment am I using? 3-4
Professor Christian Phillips BSc Hons BM DM FRCOG Consultant Gynaecologist and Urogynaecologist
 Professor Christian Phillips BSc Hons BM DM FRCOG Consultant Gynaecologist and Urogynaecologist Laparoscopic Hysterectomy What is a laparoscopic hysterectomy? Laparoscopic hysterectomy is an operation
Professor Christian Phillips BSc Hons BM DM FRCOG Consultant Gynaecologist and Urogynaecologist Laparoscopic Hysterectomy What is a laparoscopic hysterectomy? Laparoscopic hysterectomy is an operation
If you have any further questions, please speak to a doctor or nurse caring for you.
 Having a laparoscopy This leaflet aims to answer your questions about having a laparoscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital. If
Having a laparoscopy This leaflet aims to answer your questions about having a laparoscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital. If
Spinal anaesthesia for pain relief after surgery
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Spinal anaesthesia for pain relief after surgery Anaesthetics Department This leaflet explains how and what to expect from
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Spinal anaesthesia for pain relief after surgery Anaesthetics Department This leaflet explains how and what to expect from
REVERSAL OF ILEOSTOMY. Patient information Leaflet
 REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
In-patient brachytherapy for gynaecological cancer. Cancer Services Information for patients
 In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Exercises and advice following gynaecological surgery
 Exercises and advice following gynaecological surgery Bed mobility Immediately after your surgery, especially if you have had a general anaesthetic, you may not be able to move around as much as normal.
Exercises and advice following gynaecological surgery Bed mobility Immediately after your surgery, especially if you have had a general anaesthetic, you may not be able to move around as much as normal.
Colposuspension operation
 Colposuspension operation This information explains: Overview... 1 Your admission date... 1 The operation... 2 The anaesthetic... 2 After the operation... 3 Problems... 3 Going home... 4 Getting back to
Colposuspension operation This information explains: Overview... 1 Your admission date... 1 The operation... 2 The anaesthetic... 2 After the operation... 3 Problems... 3 Going home... 4 Getting back to
Having a hysterectomy
 Having a hysterectomy Gynaecology Oncology Information for patients Gynaecology It is expected that you will have discussed other methods of treatment for your health concern with your doctor and have
Having a hysterectomy Gynaecology Oncology Information for patients Gynaecology It is expected that you will have discussed other methods of treatment for your health concern with your doctor and have
Excision of Morton s Neuroma
 Excision of Morton s Neuroma Day Surgery Unit Patient information leaflet This leaflet outlines the risks, general advice and information about foot surgery called an excision of a Morton s Neuroma. If
Excision of Morton s Neuroma Day Surgery Unit Patient information leaflet This leaflet outlines the risks, general advice and information about foot surgery called an excision of a Morton s Neuroma. If
Antegrade Ureteric Stent
 Antegrade Ureteric Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains what is involved and the possible
Antegrade Ureteric Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains what is involved and the possible
ABDOMINAL PERINEAL RESECTION. Patient information Leaflet
 ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
Physiotherapy advice following your third or fourth degree perineal tear
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Vaginal Repair and Vaginal Hysterectomy
 Vaginal Repair and Vaginal Hysterectomy Patient Information Obstetrics & Gynaecology Department Author ID: JD/MC Leaflet Number: Gyn 027 Version: 5.1 Name of Leaflet: Vaginal Repairs Date Produced: February
Vaginal Repair and Vaginal Hysterectomy Patient Information Obstetrics & Gynaecology Department Author ID: JD/MC Leaflet Number: Gyn 027 Version: 5.1 Name of Leaflet: Vaginal Repairs Date Produced: February
Laparoscopy. Patient Information. Womens Health
 Laparoscopy Patient Information Womens Health What is a Laparoscopy Laparoscopy is a minimally invasive or key hole surgical procedure performed under general anaesthetic. It enables the surgeon to look
Laparoscopy Patient Information Womens Health What is a Laparoscopy Laparoscopy is a minimally invasive or key hole surgical procedure performed under general anaesthetic. It enables the surgeon to look
Knee arthroscopy. Physiotherapy Department. Patient information leaflet
 Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
HARTMANNS PROCEDURE. Patient information Leaflet
 HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
AN INFORMATION LEAFLET
 LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients
 Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Nephrostomy. Radiology Department. Patient information leaflet
 Nephrostomy Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a nephrostomy. It explains what is involved and the possible risks. The benefits and risks
Nephrostomy Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a nephrostomy. It explains what is involved and the possible risks. The benefits and risks
Gynaecology Department Patient Information Leaflet
 Laparoscopy Gynaecology Department Patient Information Leaflet Introduction This leaflet is for people who are having a procedure called a laparoscopy. It explains what the operation involves, why it is
Laparoscopy Gynaecology Department Patient Information Leaflet Introduction This leaflet is for people who are having a procedure called a laparoscopy. It explains what the operation involves, why it is
Keep high, stay dry. Pelvic floor exercises for men
 Keep high, stay dry Pelvic floor exercises for men What is the pelvic floor? Layers of muscle stretch like a hammock from your pubic bone in the front to the bottom of your backbone (see diagram). These
Keep high, stay dry Pelvic floor exercises for men What is the pelvic floor? Layers of muscle stretch like a hammock from your pubic bone in the front to the bottom of your backbone (see diagram). These
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Maternity Information Leaflet
 Maternity Information Leaflet Recovery following your Caesarean Section This leaflet provides information to help you recover following a Caesarean Section (CS) birth. Recovery after a CS may take a little
Maternity Information Leaflet Recovery following your Caesarean Section This leaflet provides information to help you recover following a Caesarean Section (CS) birth. Recovery after a CS may take a little
Kent Oncology Centre
 Kent Oncology Centre High Dose Rate Intracavitary Gynaecological Brachytherapy Information for patients We hope this leaflet will help you to understand about brachytherapy (internal radiotherapy) to the
Kent Oncology Centre High Dose Rate Intracavitary Gynaecological Brachytherapy Information for patients We hope this leaflet will help you to understand about brachytherapy (internal radiotherapy) to the
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft
 Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Roboticassisted. laparoscopic nephrectomy
 Roboticassisted laparoscopic nephrectomy This leaflet is designed to give you information on why this procedure may be suitable for you, and what you can expect from it. It outlines the advantages and
Roboticassisted laparoscopic nephrectomy This leaflet is designed to give you information on why this procedure may be suitable for you, and what you can expect from it. It outlines the advantages and
Laparoscopic repair of Inguinal Hernia
 Laparoscopic repair of Inguinal Hernia Day Surgery Unit Surgical Short Stay Unit Patient information leaflet 2 What is an inguinal hernia? A hernia is a defect in the abdominal wall (stomach muscles).
Laparoscopic repair of Inguinal Hernia Day Surgery Unit Surgical Short Stay Unit Patient information leaflet 2 What is an inguinal hernia? A hernia is a defect in the abdominal wall (stomach muscles).
Arthroscopic subacromial decompression of the shoulder
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Arthroscopic subacromial decompression of the shoulder Physiotherapy Department Information booklet for Name of Patient: Date:
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Arthroscopic subacromial decompression of the shoulder Physiotherapy Department Information booklet for Name of Patient: Date:
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Laparoscopic Ventral Mesh Rectopexy
 Laparoscopic Ventral Mesh Rectopexy (LVMR) Information for patients General Surgery What is a LVMR? A laparoscopic ventral mesh rectopexy (LVMR) is an operation in which the rectum (last part of the bowel)
Laparoscopic Ventral Mesh Rectopexy (LVMR) Information for patients General Surgery What is a LVMR? A laparoscopic ventral mesh rectopexy (LVMR) is an operation in which the rectum (last part of the bowel)
Delorme s Operation For Rectal Prolapse
 Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Laparoscopic Sacrohysteropexy
 Professor Christian Phillips BSc Hons BM DM FRCOG Consultant Gynaecologist and Urogynaecologist Laparoscopic Sacrohysteropexy What is a prolapse? Uterine prolapse is a bulge or lump in the vagina caused
Professor Christian Phillips BSc Hons BM DM FRCOG Consultant Gynaecologist and Urogynaecologist Laparoscopic Sacrohysteropexy What is a prolapse? Uterine prolapse is a bulge or lump in the vagina caused
Non weight bearing advice (post operative)
 Non weight bearing advice (post operative) Physiotherapy Department Patient information leaflet Who is this booklet for? This booklet is for post-operative patients who have been told that they will have
Non weight bearing advice (post operative) Physiotherapy Department Patient information leaflet Who is this booklet for? This booklet is for post-operative patients who have been told that they will have
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
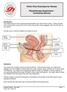 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Department of Urology Patient Information What What is Laparoscopic is Laparoscopic Nephrectomy? Nephrectomy? Laparoscopic Nephrectomy is a minimal invasive procedure or key-hole
Laparoscopic Nephrectomy Department of Urology Patient Information What What is Laparoscopic is Laparoscopic Nephrectomy? Nephrectomy? Laparoscopic Nephrectomy is a minimal invasive procedure or key-hole
Posterior Lumbar Spinal Fusion
 Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Laparoscopic Sacrohysteropexy
 Laparoscopic Sacrohysteropexy Department of Gynaecology Patient Information What is is a a laparoscopic sacrohysteropexy? This is an operation carried out to correct uterine prolapse, in patients who do
Laparoscopic Sacrohysteropexy Department of Gynaecology Patient Information What is is a a laparoscopic sacrohysteropexy? This is an operation carried out to correct uterine prolapse, in patients who do
Department of Gynaecology Services Whiston Hospital, Warrington Road, Prescot L35 5DR Sacrocolpopexy
 Patient information leaflet Department of Gynaecology Services Whiston Hospital, Warrington Road, Prescot L35 5DR 0151 426 1600 Sacrocolpopexy What is a Sacrocolpopexy? A sacrocolpopexy is a procedure
Patient information leaflet Department of Gynaecology Services Whiston Hospital, Warrington Road, Prescot L35 5DR 0151 426 1600 Sacrocolpopexy What is a Sacrocolpopexy? A sacrocolpopexy is a procedure
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients
 Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
The Leeds Teaching Hospitals NHS Trust Glansectomy and Glans Resurfacing
 n The Leeds Teaching Hospitals NHS Trust Glansectomy and Glans Resurfacing Information for patients This leaflet is to give you information about having a glansectomy or a glans resurfacing procedure.
n The Leeds Teaching Hospitals NHS Trust Glansectomy and Glans Resurfacing Information for patients This leaflet is to give you information about having a glansectomy or a glans resurfacing procedure.
Pelvic Floor Exercises
 Pelvic Floor Exercises Physiotherapy - Woman s Health Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. 2 Introduction Physiotherapists, doctors and nurses know that exercising
Pelvic Floor Exercises Physiotherapy - Woman s Health Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. 2 Introduction Physiotherapists, doctors and nurses know that exercising
Physiotherapy advice following your vaginal birth
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Stabilisation of the shoulder joint
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Stabilisation of the shoulder joint Physiotherapy Department Information leaflet for Name of Patient: Date: Name of Physiotherapist:
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Stabilisation of the shoulder joint Physiotherapy Department Information leaflet for Name of Patient: Date: Name of Physiotherapist:
Laparoscopic Cholecystectomy
 Treatment Centre Laparoscopic Cholecystectomy What is a laparoscopic cholecystectomy? You need this operation because stones have collected in your gallbladder (the area where a small amount of bile is
Treatment Centre Laparoscopic Cholecystectomy What is a laparoscopic cholecystectomy? You need this operation because stones have collected in your gallbladder (the area where a small amount of bile is
Patient information leaflet. Royal Surrey County Hospital. NHS Foundation Trust. Haemorrhoids. Day Surgery Unit
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Haemorrhoids Day Surgery Unit What are haemorrhoids? The anal canal (back passage) contains cushions of tissue at the top of
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Haemorrhoids Day Surgery Unit What are haemorrhoids? The anal canal (back passage) contains cushions of tissue at the top of
UROLOGY SYDNEY Level 1, St George Medical Centre 1 South Street Kogarah NSW 2217 Ph: Fax:
 Pre Operative care: Preop investigations: Radical Prostatectomy Pre and Post Operative Care Once your surgery date has been decided you will be sent for routine blood and urine tests, an ECG will also
Pre Operative care: Preop investigations: Radical Prostatectomy Pre and Post Operative Care Once your surgery date has been decided you will be sent for routine blood and urine tests, an ECG will also
Transurethral Resection of the Prostate (TURP)
 Transurethral Resection of the Prostate (TURP) UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Transurethral Resection of the Prostate (TURP) UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
information The Enhanced Recovery Programme for Total Hip Replacement (1 of 6) What will happen before I come into hospital?
 information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
EXERCISE and ADVICE. after pregnancy
 EXERCISE and ADVICE after pregnancy Contents Introduction...1 Comfort...2 Activity in the early days...3 Caesarean section operation...3 Exercises...4 Regaining your physical well-being...7 Contact information...ibc
EXERCISE and ADVICE after pregnancy Contents Introduction...1 Comfort...2 Activity in the early days...3 Caesarean section operation...3 Exercises...4 Regaining your physical well-being...7 Contact information...ibc
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Laparoscopic (keyhole) colorectal (bowel) resection
 Laparoscopic (keyhole) colorectal (bowel) resection Your operation explained Information for patients Colorectal Surgery Introduction This leaflet should be read together with a booklet which explains
Laparoscopic (keyhole) colorectal (bowel) resection Your operation explained Information for patients Colorectal Surgery Introduction This leaflet should be read together with a booklet which explains
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
A Guide to your Bowel Surgery
 A Guide to your Bowel Surgery Colorectal Department Patient information leaflet Contents page Introduction 3 What is colorectal cancer? 3 What is the function of the large bowel? 3 How is the diagnosis
A Guide to your Bowel Surgery Colorectal Department Patient information leaflet Contents page Introduction 3 What is colorectal cancer? 3 What is the function of the large bowel? 3 How is the diagnosis
Sacrospinous Fixation Operation
 Sacrospinous Fixation Operation Information for patients Gynaecology Department Phone no: 01625 661161 East Cheshire NHS Trust www.eastcheshire.nhs.uk @eastcheshirenhs Ref: 11485 Review: 10/2015 Revised
Sacrospinous Fixation Operation Information for patients Gynaecology Department Phone no: 01625 661161 East Cheshire NHS Trust www.eastcheshire.nhs.uk @eastcheshirenhs Ref: 11485 Review: 10/2015 Revised
Squint surgery in adults
 Squint surgery in adults Eye Department Patient information leaflet What is the aim of surgery? The main aim of squint surgery is to improve the alignment of the eyes so that the squint is less noticeable.
Squint surgery in adults Eye Department Patient information leaflet What is the aim of surgery? The main aim of squint surgery is to improve the alignment of the eyes so that the squint is less noticeable.
Ultrasound scan of abdomen and pelvis followed by transvaginal scan
 Ultrasound scan of abdomen and pelvis followed by transvaginal scan Radiology Department Patient information leaflet This leaflet has been produced in order to let you know what to expect and how to prepare
Ultrasound scan of abdomen and pelvis followed by transvaginal scan Radiology Department Patient information leaflet This leaflet has been produced in order to let you know what to expect and how to prepare
The Leeds Teaching Hospitals NHS Trust Feminine care after pelvic radiotherapy
 n The Leeds Teaching Hospitals NHS Trust Feminine care after pelvic radiotherapy Information for patients This leaflet is designed to give you information about the late side-effects following radiotherapy
n The Leeds Teaching Hospitals NHS Trust Feminine care after pelvic radiotherapy Information for patients This leaflet is designed to give you information about the late side-effects following radiotherapy
Pain injections Discharge advice
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Pain injections Discharge advice Day Surgery Department This leaflet will give you a better understanding of what to expect
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Pain injections Discharge advice Day Surgery Department This leaflet will give you a better understanding of what to expect
Trans Urethral Resection of Bladder Tumour
 Trans Urethral Resection of Bladder Tumour Department of Urology 2 Patient Information Contents Where is the bladder and what does it do? 3 What is non invasive cancer of the bladder? 4 How is bladder
Trans Urethral Resection of Bladder Tumour Department of Urology 2 Patient Information Contents Where is the bladder and what does it do? 3 What is non invasive cancer of the bladder? 4 How is bladder
Patient information leaflet. Royal Surrey County Hospital. NHS Foundation Trust. Lower back pain. Physiotherapy Department
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Lower back pain Physiotherapy Department Lower back pain This leaflet is intended for people who have been diagnosed with generalised
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Lower back pain Physiotherapy Department Lower back pain This leaflet is intended for people who have been diagnosed with generalised
Vertebroplasty. Radiology Department. Patient information leaflet
 Vertebroplasty Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a vertebroplasty. It explains what is involved and the possible risks. The benefits
Vertebroplasty Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a vertebroplasty. It explains what is involved and the possible risks. The benefits
Cholecystectomy (removal of the gallbladder) Patient Information
 Cholecystectomy (removal of the gallbladder) Patient Information Author ID: MP Leaflet Number: Surg 060 Name of Leaflet: Cholecystectomy (removal of the gallbladder) Version: 1 Date Produced: October 2017
Cholecystectomy (removal of the gallbladder) Patient Information Author ID: MP Leaflet Number: Surg 060 Name of Leaflet: Cholecystectomy (removal of the gallbladder) Version: 1 Date Produced: October 2017
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients
 Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
Treating your prolapse
 Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
Sentinel Lymph Node Biopsy and Wide Local Excision. Gynae-oncology
 Sentinel Lymph Node Biopsy and Wide Local Excision Gynae-oncology We put our patients first by working as one team; leading and listening, and striving for the best. Together, we make the difference. Patient
Sentinel Lymph Node Biopsy and Wide Local Excision Gynae-oncology We put our patients first by working as one team; leading and listening, and striving for the best. Together, we make the difference. Patient
Treatment for Bladder Tumours transurethral resection of bladder tumour (TURBT)
 Treatment for Bladder Tumours transurethral resection of bladder tumour (TURBT) Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high
Treatment for Bladder Tumours transurethral resection of bladder tumour (TURBT) Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high
Wedge incision of an ingrowing toenail
 Wedge incision of an ingrowing toenail Children and young people Paediatrics Department Patient information leaflet What is an ingrowing toenail? This problem occurs when the toenail grows into the skin
Wedge incision of an ingrowing toenail Children and young people Paediatrics Department Patient information leaflet What is an ingrowing toenail? This problem occurs when the toenail grows into the skin
TURP - TransUrethral Resection of the Prostate
 TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
University Hospitals Bristol NHS Foundation Trust NHS. Catheterisation using a Mitrofanoff
 University Hospitals Bristol NHS Foundation Trust NHS Tel: 0117 342 8840 DEPARTMENT OF PAEDIATRIC UROLOGY Fax 0117 342 8845 Bristol Royal Hospital for Children Paul O Gorman Building Family information
University Hospitals Bristol NHS Foundation Trust NHS Tel: 0117 342 8840 DEPARTMENT OF PAEDIATRIC UROLOGY Fax 0117 342 8845 Bristol Royal Hospital for Children Paul O Gorman Building Family information
Robot Assisted Total Laparoscopic Hysterectomy
 Robot Assisted Total Laparoscopic Hysterectomy What is a robot assisted total laparoscopic hysterectomy? It is the removal of the uterus, including the cervix, through four small (1/2-1 ) abdominal incisions
Robot Assisted Total Laparoscopic Hysterectomy What is a robot assisted total laparoscopic hysterectomy? It is the removal of the uterus, including the cervix, through four small (1/2-1 ) abdominal incisions
Laparoscopic Sacrocolpopexy
 Laparoscopic Sacrocolpopexy Department of Gynaecology Patient Information What is is a a laparoscopic sacrocolpopexy? This is an operation carried out using key hole surgery under general anaesthesia to
Laparoscopic Sacrocolpopexy Department of Gynaecology Patient Information What is is a a laparoscopic sacrocolpopexy? This is an operation carried out using key hole surgery under general anaesthesia to
Vacuum-Assisted Stereotactic core biopsy of the breast
 Vacuum-Assisted Stereotactic core biopsy of the breast Radiology Department Patient information leaflet This leaflet provides you with information about our vacuum assisted stereotactic core biopsy service.
Vacuum-Assisted Stereotactic core biopsy of the breast Radiology Department Patient information leaflet This leaflet provides you with information about our vacuum assisted stereotactic core biopsy service.
Hernia repair. Paediatric Day Surgery Unit. Patient information leaflet
 Hernia repair Paediatric Day Surgery Unit Patient information leaflet 2 What is a Hernia? A hernia is where part of the bowel is pushing through the muscle wall, resulting in a swelling. This can occur
Hernia repair Paediatric Day Surgery Unit Patient information leaflet 2 What is a Hernia? A hernia is where part of the bowel is pushing through the muscle wall, resulting in a swelling. This can occur
Squint surgery in children
 Squint surgery in children Eye Department Patient information leaflet What is the aim of surgery? The main aim of squint surgery is to improve the alignment of the eyes so that the squint is less noticeable.
Squint surgery in children Eye Department Patient information leaflet What is the aim of surgery? The main aim of squint surgery is to improve the alignment of the eyes so that the squint is less noticeable.
Pelvic Girdle Pain in Pregnancy
 CHFT If you have any comments about this leaflet or the service you have received you can contact : Assistant Therapy Services Co-ordinator Rehabilitation Department Calderdale Royal Hospital Salterhebble
CHFT If you have any comments about this leaflet or the service you have received you can contact : Assistant Therapy Services Co-ordinator Rehabilitation Department Calderdale Royal Hospital Salterhebble
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Antegrade Ureteric Stent
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Antegrade Ureteric Stent Radiology This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Antegrade Ureteric Stent Radiology This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains
B11 Breast Reconstruction with Abdominal Tissue Flap
 B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
Tension-free Vaginal Tape (TVT)
 Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
