The overactive bladder and the role of the pelvic floor muscles
|
|
|
- Jeffry Haynes
- 5 years ago
- Views:
Transcription
1 BJU International (1999), 83, Suppl. 2, The overactive bladder and the role of the pelvic floor muscles E.J. MESSELINK Department of Urology, Academic Medical Centre Amsterdam, The Netherlands Keywords Pelvic floor muscle, overactive bladder, therapy, biofeedback, neurology, psychology, bladder dysfunction Introduction bladder with pelvic floor rehabilitation, both under the supervision of a physiotherapist. In this article, the relationship between PFM function and bladder function is discussed. The overactive pelvic floor seems to play an important role in relation to the symptoms of the over- active bladder. There are few reports on the relationship between the overactive bladder and overactive pelvic floor. Hence, some of the views in this article are based on clinical experience. The overactive bladder is a common disorder of the lower urinary tract; in the Netherlands, a recent survey showed that 10% of the Dutch population 18 years of age (about 1 million people) report symptoms of an overactive bladder [1]. The symptoms of bladder overactivity are urinary frequency (>8 times/24 h), urgency and urge incontinence. According to the ICS definitions, an overactive bladder is diagnosed by urodynamic investigation, i.e. filling cystometry [2]. The disorder is characterized by involuntary detrusor contractions while the patient is trying to suppress them (Fig. 1). If a known neurological disorder is the cause, the condition is classified as hyper-reflexia, and otherwise it is termed detrusor instability. There is still much debate about the classification and value of the cystometric findings [3]. In the treatment of bladder control problems, the pelvic floor muscles (PFMs) play an important role. In the past this therapy was used only for patients with stress incontinence. Recently there has also been a tendency to treat patients with urinary symptoms including an overactive Neurological control In the physiological situation the pelvic floor and the bladder co-operate to fulfil the demands of a normal lower urinary tract cycle. This cycle is primarily under the involuntary control of centres in the spinal and central nervous system. The desire to void is a warning signal that facilitates voiding at a convenient place and time. The neuronal circuitry of the lower urinary tract is still debated; a recent description was provided from the study by Blok et al. [4], using positron emission tomography to image central activity during voiding. Fig. 1. Urodynamic investigation of a 20- year-old women with dysfunctional voiding. Note the pelvic floor muscle action during coughing (red bars at the top of the recording) and during voiding BJU International 31
2 32 E.J. MESSELINK The neuronal circuitry has several elements in common, lems [12]. Respondent conditioning means that anxiety, i.e. the musculature of the lower urinary tract, and the expectations and other external signals are associated sympathetic, parasympathetic and somatic connections. with the feelings of the desire to void. Operantconditioning These elements regulate the storage and voiding phase, mechanisms (see below) can train a person and the end of voiding. To illustrate the role of the pelvic to postpone voiding because they are rewarded for this floor in the lower urinary tract cycle, the scheme by their social environment. Generalization causes more described by Holstege et al. is used (cited in [5]). and unspecific signals to acquire the same emotional The PFMs and the urinary bladder transmit acerent burden as the original signals, and thus influence both information to the lumbosacral cord and the periaquad- the lower urinary tract cycle and the process of voiding. uctal grey matter (PAG), the latter being part of the Another mechanism is trained helplessness, whereby emotional motor system [6]. The pontine micturition patients are convinced of their own inability to manage centre (PMC) receives excitatory information from the their bladder behaviour. For some patients the bladder PAG. In the PMC there are two regions of interest, the problems function as a method to avoid specific situations, m and the l region (medial and lateral region of the e.g. sexual intercourse [13]. Other patients try to pons). An important mechanism is the reciprocal inhibi- obtain special privileges because of their complaints and tory ecect of the m-region and the l-region on each symptoms [14]. other. The m-region is the centre of synergetic micturition, with projections via the sacral intermediolateral cell groups to the bladder and the urethral sphincter. Pelvic floor control The l-region has direct projections on the nucleus of The pelvic floor is a complex of muscular and fascial Onuf and in this way initiates contraction of the PFMs structures forming a structural unit. First, the PFMs and striated sphincter of urethra and anus [7]. provide support for the pelvic organs; second, the pelvic In the normal situation, the PFMs and bladder are coordinated floor plays a role in the process of continence and at the level of the PMC under control of the excretion (both urinary and faecal); and third, it is PAG region. Voluntary control of the lower urinary tract important in sexual functioning. Thus disorders of the cycle can be assessed by contracting the pelvic floor PFMs may lead to bladder control problems, retention, when longer storage is needed. The superomedial part prolapse or sexual dysfunction. Because the pelvic floor of the precentral gyrus projects onto the l-region, is a functional unit it gives rise to symptoms in dicerent resulting in a contraction of the PFMs [8]. The ecect of tracts; thus it is important to take a detailed history and a contraction of the PFMs on the bladder is inhibition of to have a multidisciplinary approach if more than one the detrusor contraction [9]. This reflex mechanism may organ system is involved. The pelvic floor may play a be of sacral origin, but the role of the PMC in this role in the development of bladder symptoms in the child mechanism has been described as inhibition of the l- and the adult. During normal development the child has region on the m-region [10]. During voiding there should learned to manage the bladder by using central control be maximal relaxation of the PFMs. This co-ordinated mechanisms. Some children learn to use other tech- action is also controlled by the PMC. Activation of the niques to prevent bladder control problems or to cope m-region initiates a detrusor contraction and simultaneously inhibits the l-region, relaxing the PFMs. Psychological control The desire to void is a sensation which, in the developing child, is incorporated into daily life so that voiding takes place at an appropriate time and place. Interpreting the desire and taking the right actions are the goal of training during childhood. Problems with training or general physical or psychological problems during training can have a great impact on the results of training, e.g. some women patients report that, when a child, they were taken to the toilet many times because their parents thought they had to void [11]. When children receive a negative sensual input related to voiding they may develop an abnormal voiding pattern. Conditioning is an important psychological mechanism for these prob- with urgency, e.g. some sit on their heel to compress the urethra. Other children use their pelvic floor to diminish the detrusor contraction or to prevent urine loss. Using the PFMs as a primary voluntary mechanism to regulate the lower urinary tract cycle can lead to bladder dysfunction and signs of an overactive bladder; this finally results in an overactive pelvic floor. In the western world, voiding in adults is probably no longer as natural as it was before modern civilization; for many people, the lower urinary tract cycle is dictated by their work or social activities. Many professions have dibculty coping with their lower urinary tract cycle, e.g. cab-drivers, salesmen and waiters. During their work there is little time for voiding so they train themselves to postpone micturition for a long time. The interval between consecutive voids increases, with some voiding only two or three times a day. Their functional bladder capacity can exceed 500 ml and there is often a
3 THE OVERACTIVE BLADDER AND PELVIC FLOOR MUSCLES 33 significant postvoid residual urine volume. Not only do the results are better and achieved earlier [19]. In a they postpone voiding, but they also wish to void whenever long-term study, the initial success rate was 88% but it is convenient. In this situation, voiding may declined to 38% after 6 months [20], and when reviewed, change from an involuntary regulated reflex action to a the proportion responding completely was 10 15%. In voluntarily initiated and most often uncoordinated those patients (50%) who had fewer symptoms, there action of the bladder and PFMs. During voiding the was a 50 75% improvement when compared with their PFMs are not relaxed but instead reflexively contract condition before treatment [21]. through abdominal straining; hence, a dysfunctional voiding pattern develops. As expected, this is a vicious circle, resulting in an overactive pelvic floor with dysfunctional Pelvic floor muscle training voiding and residual urine. PFM training may be important in treating the overactive Theoretically, the development of an overactive pelvic bladder. To determine whether such therapy is ecective floor may induce peripheral and central changes leading and to apply the right form of therapy, it is necessary to to a new system managing and controlling the lower know the status of the PFMs. Three types of pelvic floor urinary tract cycle. This system could be more vulnerable dysfunction can be identified on physical examination, to loss of co-ordination between the detrusor and PFMs, i.e. no voluntary control, voluntary control but impaired and loss of inhibitory signals to the detrusor, leading to strength and/or relaxation, and voluntary control with detrusor overactivity. On the other hand, there may be normal strength and/or relaxation. The dicerent treat- an important role for the central regulation of the lower ment modalities are shown in Table 1. urinary tract cycle. The m-region and the PAG are part When there is no voluntary control, biofeedback (BFB) of the emotional motor system; the ecect of emotional alone or combined with electrotherapy may be a good trauma on the lower urinary tract is well known [15]. therapeutic strategy. When there is voluntary control Psychological, emotional or sexual trauma are frequently but strength or relaxation is impaired, pelvic floor reeducation, seen in patients with symptoms of an overactive bladder including exercises to improve strength or in combination with an overactive pelvic floor [16]. relaxation, is the therapy of choice. If there is voluntary control and good strength/relaxation, conditioning will teach the patient to use the pelvic floor correctly. The Bladder training ability to relax the pelvic floor during a physical examination The overactive bladder can be treated pharmacologically does not exclude an overactive pelvic floor. During with antimuscarinics, oestrogen, and other drugs. It can voiding these patients may be contracting the pelvic also be treated by bladder training programmes and the floor instead of relaxing. In these situations, the history psychological mechanism described for the development can provide clues about the activity pattern of the pelvic of the overactive bladder can be used in such a training floor. The most important feature of PFM rehabilitation programme. One of the earliest training schemes was is training the co-ordination between bladder and pelvic devised by JeCcoate and Frewen [17], who described the floor. Initially, the patient should become aware of the method of postponing voiding in case of urgency and PFMs and incorporate this group of muscles into their frequency by progressively delaying micturition. By body scheme. The patient should be taught the normal observing the interval between separate voids it was function of the PFMs and their interaction with the possible to learn that voiding could be postponed with bladder. In the final stage, the patient should learn how no significant problems (operant conditioning). Because the results of bladder training soon diminish, concomitant cognitive behavioural therapy is advocated. Patients Table 1 Methods of pelvic floor therapy should have more knowledge about their symptoms and Method Components about their urinary tract function [18]. Concomitant psychological counselling may be important when anxi- Pelvic floor rehabilitation Muscle training ety is excessive. The help of a trained psychologist, Bladder training interested in patients with bladder problems, can then Co-ordination training be vital to therapeutic success. Depending on whether Biofeedback Digital Perineometer the psychological factors are related to sexual problems, Pelvic floor EMG a sexologist may be an optional first choice for the Urethral pressure psychological part of the therapy. Urinary flow recording The reported results of bladder training vary greatly; Neuromuscular electrical Pelvic floor muscles Hz they depend on whether detrusor overactivity was present (motor urge) or not (sensory urge). With the latter, stimulation Detrusor muscle 5 10 Hz
4 34 E.J. MESSELINK with an overactive pelvic floor, only improving muscle strength will aggravate the symptoms. Another import- ant precaution is to recognize any association of an overactive pelvic floor and psychological trauma in the history. In our clinical experience, patients with an overactive pelvic floor more often have psychological and especially sexual trauma in their past. This can be unclear at the start of therapy because it may be impossible for the patient to discuss it with the specialist; some patients only recount these experiences after a long time. One opportunity to initiate discussion may be during PFM therapy sessions; when relaxation appears to be a problem, the specialist can then inform the patient that negative experiences in the past may be a factor in the present symptoms. Where such experiences are reported it is obvious that psychological counselling should be ocered to the patient. Based on this knowledge, it seems wise to be careful when performing invasive investigations (e.g. cystoscopy) and using intravaginal or intra-anal treatment devices in such patients. In these situations, this should be discussed with the patient and with the psychologist if appropriate. to manage the pelvic floor and practise this in dicerent daily situations. Biofeedback is important for showing the patients the ecect of their ecorts; patients showing no or poor voluntary control over the pelvic floor can be assisted using BFB. Comparing those using or not using BFB showed that the results were no better but were achieved more quickly in the former. The simplest form of BFB is the provision of information on the action of the pelvic floor as measured digitally by the instructing physiotherapist. This combination of training and feedback is important at the start of training. Neuromuscular electrical stimulation (NMES) can be used to stimulate nerve fibres and muscles, the optimal stimulus frequency being based on the conduction velocity of the targeted nerve fibre type. NMES at Hz can stimulate the PFM through a pudendal nerve reflex loop, which improves re-innervation and converts fastinto slow-twitch fibres. At 5 10 Hz, NMES can also acect the detrusor muscle by reflex inhibition; at this frequency, a pudendal to pelvic nerve reflex is activated. As a result of PFM training, problems were completely resolved in 20% of patients; most patients reported a reduction in urinary symptoms of 50 75% [22]. The results of BFB are reported only in a few studies; in children, the results were classified as good in 68%, improved in 13% and not improved in 29% [23]. In a study on adults, 43% were rendered continent and there was a significant decrease in daytime frequency and nocturia [24]. The results of NMES, reported in a review [25], were 20% dry and 37% significantly improved; other studies report comparable results [26]. Complications of PFM training The future There remains much work in the field of PFMs and the overactive bladder. First, there needs to be a consensus on the classification of pelvic floor disorders. Second, the instruments for measuring pelvic floor function should be more objective and reproducible. Outcome measures should be stated, and clinical, sham-controlled trials of the ebcacy of dicerent treatment options and combinations should be constructed. Another important field of research is the neurological basis for the interaction between the bladder and pelvic floor. The recent results with positron emission tomography should encourage investigators to conduct further trials on these aspects. Combined with this area, more attention must be given to the psychological and sexual aspects of the overactive pelvic floor and bladder. Using the term overactive bladder syndrome rather than overactive bladder may provide a broader view of the complex relations of the bladder, the pelvic floor and the brain in patients with urge, urgency, frequency and urge incontinence. Further investigations are needed and these should be multi- disciplinary. The indications for PFM therapy have increased over recent years; currently, physiotherapy of the PFMs may be applied not only to women with stress incontinence but also in both sexes with symptoms of dysfunctional voiding and an overactive bladder. PFM therapy is a functional approach and is therefore a reasonable option for functional disorders of the lower urinary tract. Restoring normal function is the main goal of PFM therapy. By broadening the indications for PFM therapy, it will become increasingly important that specialists and physiotherapists who treat this type of patient are familiar with the nature of PFM problems and the characteristics of the dicerent treatment modalities. The overactive pelvic floor is a relatively References new indication for PFM therapy and some precautions 1 De overactive blaas. OBce Report Veldkamp 1998 are necessary. The diagnosis of PFM overactivity may 2 Abrams PH, Blaivas JG, Stanton SL, Andersen JT. be dibcult and therefore missed. When applying PFM Standardisation of terminology of lower urinary tract therapy it is important to realize that, in all cases, function. Neurourol Urodynam 1988; 7: control of the PFMs and co-ordination are the primary 3 Artibani W. Diagnosis and significance of idiopathic goals and muscle strengthening the second. In those overactive bladder. Urology 1997; 50: 25 32
5 THE OVERACTIVE BLADDER AND PELVIC FLOOR MUSCLES 35 4 Blok BFM, Willemsen ATM, Holstege G. A PET study on another causative factor in dysfunctional voiding. J Urol brain control of micturition in humans. Brain 1997; 1995; 153: : Frewen WK. Role of bladder training in the treatment of 5 Kinder MV, Bastiaanssen EHC, Janknegt RA, Marani E. the unstable bladder in the female. Urol Clin North Am Neuronal circuitry of the lower urinary tract; central and 1979; 6: peripheral neuronal control of the micturition cycle. Anat 18 Bitzer J. Harninkontinenz integrativ angehen. Ein psychoso- Embryol 1995; 192: matisch orientiertes Therapiekonzept. Sexualmedizin 1990; 6 Vanderhorst VG, Mouton LJ, Blok BF, Holstege G. Distinct 19: cell groups in the lumbosacral cord of the cat project to 19 Holmes DM, Stone AR, Bary PR, Richards CJ, Stephenson dicerent areas in the periaqueductal gray. J Comp Neurol TP. Bladder training 3 years on. Br J Urol 1983; 1996; 376: : Holstege G, GriBths D, de Wall H, Dalm E. Anatomical and 20 Ferrie BG, Smith JS, Logan D, Lyle R, Paterson PJ. physiological observations on supraspinal control of bladder Experience with bladder training in 65 patients. Br J Urol and urethral sphincter muscles in the cat. J Comp Neurol 1984; 56: ; 250: Fantl JA, Wyman JF, McClish DK et al. EBcacy of bladder 8 Blok BFM, Sturms LM, Holstege G. A PET study on cortical training in older women with urinary incontinence. JAMA and subcortical control of pelvic floor musculature in the 1991; 265: women. J Comp Neurol 1997; 389: Fantl JA. Behavioral intervention for community-dwelling 9 Vodusek DB, Plevnik S, Vrtacnik P, Janez J. Detrusor individuals with urinary incontinence. Urology 1998; inhibition on selective pudendal nerve stimulation in the (Suppl): 30 4 perineum. Neurourol Urodynam 1988; 6: Vijverberg MA, Elzinga-Plomp A, Messer AP, van Gool JD, 10 Holstege G. Neuronal organisation of micturition. In Lower de Jong TP. Bladder rehabilitation, the ecect of a cognitive Urinary Tract Dysfunction: from All to Clinical Approach. training programme on urge incontinence. Eur Urol 1997; MicroSymposium, Erasmus University Rotterdam, 31: Rotterdam. 24 Stein M, Discippio W, Davia M, Taub H. Biofeedback for 11 JeCcoate TNA, Francis WJA. Urgency incontinence in the the treatment of stress and urge incontinence. J Urol 1995; female. Am J Obst Gyn 1966; 94: : Straub LR, Ripley HS, Wolf S. Disturbances of bladder 25 Payne CK. Electrostimulation. In O Donnell PD, ed. Urinary function associated with emotional states. JAMA 1949; Incontinence. St Louis: Mosby 1977: : Sand PK. Pelvic floor stimulation in the treatment of mixed 13 Hafner RJ, Stanton SL, Guy J. A psychiatric study of incontinence complicated by a low-pressure urethra. Obst women with urgency and urgency incontinence. Br J Urol Gyn 1996; 88: ; 49: Debus-Thiede G, Dimpfl Th. Die psychische Situation der harninkontinenten Frau. Z Gynäkol 1993; 115: Author 15 Wheeler JS. Functional voiding disorders. Med Aspects E.J. Messelink, MD, Academic Medical Centre G4 105, Human Sexuality 1985; 19: University of Amsterdam, Meibergdreef 9, 1105 AZ, 16 Ellsworth PI, Merguerian PA, Copening ME. Sexual abuse: Amsterdam, The Netherlands.
Neural control of the lower urinary tract in health and disease
 Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
The central control of micturition and continence: implications for urology
 BJU International (1999), 83, Suppl. 2, 1 6 The central control of micturition and continence: implications for urology B.F.M. BLOK and G. HOLSTEGE Department of Anatomy and Embryology, Faculty of Medical
BJU International (1999), 83, Suppl. 2, 1 6 The central control of micturition and continence: implications for urology B.F.M. BLOK and G. HOLSTEGE Department of Anatomy and Embryology, Faculty of Medical
Neural control of the lower urinary tract
 Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
University of Groningen. Neuronal control of micturition Kuipers, Rutger
 University of Groningen Neuronal control of micturition Kuipers, Rutger IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Neuronal control of micturition Kuipers, Rutger IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Neural Control of Lower Urinary Tract Function. William C. de Groat University of Pittsburgh Medical School
 Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Updates in the nonpharmacological. treatment on overactive bladder
 Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Physiologic Anatomy and Nervous Connections of the Bladder
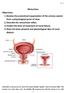 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
The new ICCS terminology J Urol 176, , 2006
 The new ICCS terminology J Urol 176, 314-324, 2006 The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Report from the Standardisation Committee of the International
The new ICCS terminology J Urol 176, 314-324, 2006 The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Report from the Standardisation Committee of the International
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome
 Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome Karl-Erik Andersson SUMMARY The pathophysiology of overactive bladder syndrome (OABS) and detrusor overactivity
Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome Karl-Erik Andersson SUMMARY The pathophysiology of overactive bladder syndrome (OABS) and detrusor overactivity
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY
 PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
Spinal Cord Injury. R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH
 Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E.
 UvA-DARE (Digital Academic Repository) Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E. Link to publication Citation for published version (APA): Puspitoayu,
UvA-DARE (Digital Academic Repository) Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E. Link to publication Citation for published version (APA): Puspitoayu,
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories
 Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY IN CHILDREN
 0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
Regulation of the Urinary Bladder Chapter 26
 Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Chapter 23. Micturition and Renal Insufficiency
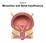 Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
Module 3 Causes Of Urinary Incontinence
 Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
Training a Wayward Bladder
 D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Pelvic Floor Exercise. Brigi0e Fung Physiotherapist
 Pelvic Floor Exercise Brigi0e Fung Physiotherapist Treatment for urinary incontinence Pelvic floor muscle exercise (Kegel, 1948) Bladder retraining Behaviour modification Treatment for urinary incontinence
Pelvic Floor Exercise Brigi0e Fung Physiotherapist Treatment for urinary incontinence Pelvic floor muscle exercise (Kegel, 1948) Bladder retraining Behaviour modification Treatment for urinary incontinence
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Paediatric Urotherapy Training
 Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Prolapse & Urogynaecology. Hester Mannion and Fabi Sica
 Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
排尿障礙治療中心版權所有. Physiotherapy of Lower Urinary Tract Dysfunction.
 Physiotherapy of Lower Urinary Tract Dysfunction www.fisiokinesiterapia.biz Lower Urinary Tract Dysfunction Urinary Incontinence Stress, urge, or mixed incontinence Frequency urgency syndrome Spastic urethral
Physiotherapy of Lower Urinary Tract Dysfunction www.fisiokinesiterapia.biz Lower Urinary Tract Dysfunction Urinary Incontinence Stress, urge, or mixed incontinence Frequency urgency syndrome Spastic urethral
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
HOW PHYSICAL THERAPY CAN MAKE A DIFFERENCE AFTER PROSTATE SURGERY
 HOW PHYSICAL THERAPY CAN MAKE A DIFFERENCE AFTER PROSTATE SURGERY JANE FRAHM, BS,PT,BCIA PMDB 7/7/2010 jdf,pt 1 REHABILITATION INSTITUTE OF MICHIGAN RIM PART OF COMPREHENSIVE TREATMENT PROGRAM. 7/7/2010
HOW PHYSICAL THERAPY CAN MAKE A DIFFERENCE AFTER PROSTATE SURGERY JANE FRAHM, BS,PT,BCIA PMDB 7/7/2010 jdf,pt 1 REHABILITATION INSTITUTE OF MICHIGAN RIM PART OF COMPREHENSIVE TREATMENT PROGRAM. 7/7/2010
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE
 PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Recommandations de prise en charge des vessies neurogènes EAU 2006
 Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Dysfunctional voiding
 Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
URINARY INCONTINENCE FOR FALLS PREVENTION. by Susan Elms P.T. Elms Physiotherapy
 URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
Sexual Function in Women with Urinary Incontinence Treated by Pelvic Floor Transvaginal Electrical Stimulation
 Blackwell Publishing IncMalden, USAJSMJournal of Sexual Medicine1743-6095 2006 International Society for Sexual Medicine200743702707Original ArticleWomen Affected by UI and WSD Treated by TESGiuseppe et
Blackwell Publishing IncMalden, USAJSMJournal of Sexual Medicine1743-6095 2006 International Society for Sexual Medicine200743702707Original ArticleWomen Affected by UI and WSD Treated by TESGiuseppe et
GUIDELINES ON URINARY INCONTINENCE
 GUIDELINES ON URINARY INCONTINENCE 9 J. Thüroff, (chairman), P. Abrams, J-T. Andersen, W. Artibani, E. Chartier-Kastler, C. Hampel, M. Hohenfellner, T. Tammela, Ph. van Kerrebroeck Introduction The condition
GUIDELINES ON URINARY INCONTINENCE 9 J. Thüroff, (chairman), P. Abrams, J-T. Andersen, W. Artibani, E. Chartier-Kastler, C. Hampel, M. Hohenfellner, T. Tammela, Ph. van Kerrebroeck Introduction The condition
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging
 Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain
 Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
The new International Continence Society
 ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
Technologies and architectures" Stimulator, electrodes, system flexibility, reliability, security, etc."
 March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
How to manage a patient with bladder dysfunction
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 13 How to manage a patient with autonomic dysfunction - Level 2 How to manage a patient with
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 13 How to manage a patient with autonomic dysfunction - Level 2 How to manage a patient with
URINARY INCONTINENCE IN THE. Summary
 Age and Ageing (984) 3, 23-234 H. D. H. EASTWOOD Consultant in Geriatric Medicine R WARRELL' Senior Registrar in Geriatric Medicine URNARY NCONTNENCE N THE ELDERLY FEMALE: PREDCTON, N D AG NOSS AND OUTCOME
Age and Ageing (984) 3, 23-234 H. D. H. EASTWOOD Consultant in Geriatric Medicine R WARRELL' Senior Registrar in Geriatric Medicine URNARY NCONTNENCE N THE ELDERLY FEMALE: PREDCTON, N D AG NOSS AND OUTCOME
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Perineal Electrophysiologic Tests
 Perineal disorders and emg! Perineal Electrophysiologic Tests Voiding dysfunction Stress Urinary Incontinence urgency OAB Urge Incontinence nocturia Pr. Gerard Amarenco Mixed Incontinence frequency Service
Perineal disorders and emg! Perineal Electrophysiologic Tests Voiding dysfunction Stress Urinary Incontinence urgency OAB Urge Incontinence nocturia Pr. Gerard Amarenco Mixed Incontinence frequency Service
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in children
 ORIGINAL ARTICLE Vol. 41 (4): 739-743, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0303 Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in
ORIGINAL ARTICLE Vol. 41 (4): 739-743, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0303 Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
Diagnosis and Mangement of Nocturia in Adults
 Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Urinary incontinence: the management of urinary incontinence in women
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence: the management of urinary incontinence in women 1.1 Short title Urinary incontinence 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence: the management of urinary incontinence in women 1.1 Short title Urinary incontinence 2 Background a) The National
URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS- SECTIONAL STUDY
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Aisha et al. SJIF Impact Factor 6.647 Volume 6, Issue 9, 1384-1391 Research Article ISSN 2278 4357 URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS-
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Aisha et al. SJIF Impact Factor 6.647 Volume 6, Issue 9, 1384-1391 Research Article ISSN 2278 4357 URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS-
A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes
 Neurourology and Urodynamics 19:127 135 (2000) A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes Asnat Groutz, Jerry G. Blaivas,* and Jarrod E. Rosenthal Weill Medical College,
Neurourology and Urodynamics 19:127 135 (2000) A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes Asnat Groutz, Jerry G. Blaivas,* and Jarrod E. Rosenthal Weill Medical College,
Retrospective Analysis of Efficacy and Tolerability of Tolterodine in Children with Overactive Bladder
 European Urology European Urology 45 (2004) 240 244 Retrospective Analysis of Efficacy and Tolerability of Tolterodine in Children with Overactive Bladder A. Raes a,, P. Hoebeke b, I. Segaert a, E. Van
European Urology European Urology 45 (2004) 240 244 Retrospective Analysis of Efficacy and Tolerability of Tolterodine in Children with Overactive Bladder A. Raes a,, P. Hoebeke b, I. Segaert a, E. Van
Overactive Bladder. When to see a doctor. Normal bladder function
 Overactive Bladder Overactive bladder is a problem with bladder-storage function that causes a sudden urge to urinate. The urge may be difficult to stop, and overactive bladder may lead to the involuntary
Overactive Bladder Overactive bladder is a problem with bladder-storage function that causes a sudden urge to urinate. The urge may be difficult to stop, and overactive bladder may lead to the involuntary
Module 5 Management Of Urinary Incontinence
 Management Of Urinary Incontinence V3: Last Reviewed September 2017 Learning Outcomes Outline conservative management options Discover the options available to manage the different types of incontinence
Management Of Urinary Incontinence V3: Last Reviewed September 2017 Learning Outcomes Outline conservative management options Discover the options available to manage the different types of incontinence
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Urodynamic findings in women with insensible incontinence
 bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
17 th European congress of Physical Rehabilitation Medicine. 38th SIMFER congress
 17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
Pelvic Floor and More.. Urinary Continence. Urinary Incontinence. Normal Bladder Function
 Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Managing Female Urinary Incontinence Within Primary Care
 Managing Female Urinary Incontinence Within Primary Care Angela Patterson Lead Clinical Nurse Specialist in Bladder and Bowel Dysfunction. South Eastern HSCT Background More than 14 million in the UK affected
Managing Female Urinary Incontinence Within Primary Care Angela Patterson Lead Clinical Nurse Specialist in Bladder and Bowel Dysfunction. South Eastern HSCT Background More than 14 million in the UK affected
THE OVER-ACTIVE BLADDER (OAB)
 THE OVER-ACTIVE BLADDER (OAB) Passage of urine is caused by the bladder muscle contracting coordinated with the relaxation of the sphincter muscles, which is controlled by higher centers in the central
THE OVER-ACTIVE BLADDER (OAB) Passage of urine is caused by the bladder muscle contracting coordinated with the relaxation of the sphincter muscles, which is controlled by higher centers in the central
3/20/10. Prevalence of OAB Men: 16.0% Women: 16.9% Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Dry. Population (millions) Wet
 1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
Refractory Lower Urinary Tract Symptoms
 Sacral Neuromodulation for Treatment of Refractory Lower Urinary Tract Symptoms Alex Kavanagh, PGY3 Mar 30/2011 Goals 1. Define sacral neuromodulation (SNM) and review the clinical implementation 2. Provide
Sacral Neuromodulation for Treatment of Refractory Lower Urinary Tract Symptoms Alex Kavanagh, PGY3 Mar 30/2011 Goals 1. Define sacral neuromodulation (SNM) and review the clinical implementation 2. Provide
Video-urodynamics. P J R Shah Institute of Urology and UCH
 Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
5/29/2015. Objectives. Functions of the PFM. Various phases of PFM. Evaluation of the PFM
 The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
Half-Day Urotherapy Improves Voiding Parameters in Children with Dysfunctional Emptying
 european urology 49 (2006) 570 574 available at www.sciencedirect.com journal homepage: www.europeanurology.com Pediatric Urology Half-Day Urotherapy Improves Voiding Parameters in Children with Dysfunctional
european urology 49 (2006) 570 574 available at www.sciencedirect.com journal homepage: www.europeanurology.com Pediatric Urology Half-Day Urotherapy Improves Voiding Parameters in Children with Dysfunctional
