Assessment and management of male androgen disorders: an update
|
|
|
- Sherman Sanders
- 5 years ago
- Views:
Transcription
1 Irene Chan Mark Ng Tang Fui Jeffrey D Zajac Mathis Grossmann Assessment and management of male androgen disorders: an update Background Male hypogonadism, caused by intrinsic pathology of the hypothalamic pituitary testicular (HPT) axis, is an under-diagnosed condition not to be missed. By contrast, late onset hypogonadism (LOH), due to functional suppression of the HPT axis from age-related comorbidities, may be less common than previously believed. Objective This article outlines the aetiology, clinical features, investigation and management of male hypogonadism and discusses the more controversial area of LOH. Discussion Pathologically based hypogonadism is, after a thorough diagnostic work-up, treated with testosterone replacement therapy, unless fertility is desired. LOH with modest reductions in testosterone levels should primarily be managed by attention to lifestyle measures, especially weight loss, and optimisation of comorbidities. Clear treatment goals should be identified, and efficacy and safety should be monitored according to published clinical practice guidelines. Keywords men s health; endocrine system diseases; obesity; diabetes mellitus Male hypogonadism is a clinical syndrome that results from failure to produce physiological levels of testosterone (androgen deficiency) and a normal number of spermatozoa due to organic pathology that disrupts one or more levels of the hypothalamic pituitary testicular (HPT) axis. 1 It therefore includes androgen deficiency and infertility, although both components can be present in isolation. The prevalence of organic hypogonadism in Australia is about 1 in 500 men 2 and general practitioners (GPs) will see several such men in their practice. There is evidence that male hypogonadism is under-diagnosed and late diagnosis of, for example, Klinefelter s syndrome, which is easily diagnosed by testicular examination, is not uncommon. 3 Organic hypogonadism needs to be distinguished from the less well-defined entity called late onset hypogonadism (LOH), which is caused by functional (and hence potentially reversible) suppression of the HPT axis due to accumulation of agerelated comorbidities, especially obesity. Recent data suggest that LOH is less common than previously believed and has a prevalence of about 2%. 4 In contrast to women who experience a sudden drop in oestradiol levels around the time that menses ceases, the age-related drop in testosterone in men is more gradual at % per year from early adulthood onwards. As levels of sex hormone binding globulin (SHBG) rise with age by 1 2% per year, the decline in free testosterone level is greater and is 2 3% per year. Most older men have testosterone levels within the reference range and there is recent evidence from Australia that healthy ageing alone may not be associated with marked decreases in testosterone levels. 5 However, the age-dependent decrease in testosterone levels is accelerated by accumulation of comorbidities, especially obesity. 6 Indeed, a normal testosterone level can be considered to be a sensitive biomarker of good health. Diagnosis of hypogonadism The diagnosis of androgen deficiency should be made only in men with consistent symptoms and signs, and unequivocally and repeatedly low serum testosterone levels. 1 In practice this diagnosis is often difficult, especially in older obese men with chronic disease, as symptoms REPRINTED FROM AUSTRALIAN FAMILY PHYSICIAN VOL. 43, NO. 5, MAY
2 Assessment and management of male androgen disorders: an update and signs are often non-specific and because there is no evidence-based, universally agreed pathological testosterone cut-off level. 1,7 Clinical diagnosis Given that hypogonadism is primarily a clinical diagnosis supported by consistent biochemical findings, a thorough history and examination are essential. Clinical assessment should be focused on eliciting symptoms and signs of androgen deficiency and on identifying clues to the underlying aetiology (Table 1 8 ). Signs and symptoms include incomplete or delayed sexual development (if hypogonadism occurs before or during puberty), reduced libido, decreased spontaneous erections, breast discomfort, loss of body hair, reduced shaving, very small (especially <5 ml) or shrinking testes, infertility, height loss, low trauma fracture, low bone mineral density, hot flushes. It should be kept in mind that clinical features can be non-specific and Table 1. Causes of androgen deficiency 8 Partial/transient Acute illness Chronic disease ESRF COPD HIV T2DM Androgen deprivation therapy (GnRH agonists) Anabolic steroids Primary (elevated FSH/ LH) ACQUIRED Testicular damage Trauma Orchitis CTX/RTX/toxins Drugs Spironolactone Ketoconazole CONGENITAL Klinefelter syndrome Cryptorchidism Mutations in androgen biosynthesis enzymes LH/FSH-receptor mutations Myotonic dystrophy related to other medical conditions. In men aged over 50 years, digital rectal examination must be performed to exclude palpable prostate pathology before commencing testosterone replacement therapy. In addition, although controversial in the general population, regular testing for prostate-specific antigen (PSA) is recommended during testosterone therapy and a baseline PSA of >4 ng/ml without urological evaluation is a contraindication to testosterone treatment. 1 Biochemical diagnosis Of the total circulating testosterone, 60% is tightly bound to SHBG, 38% is loosely bound to albumin and only 2% is free. Bioavailable testosterone refers to albumin-bound and free testosterone. Total testosterone is the mainstay of biochemical diagnosis of androgen deficiency. The initial diagnostic test in suspected androgen deficiency is measurement of fasting morning total testosterone in men with consistent Secondary (low/normal FSH/LH) STRUCTURAL Tumour Surgery Radiation Trauma Infiltration Iron overload Sarcoid Histiocytosis GENETIC Kallmann syndrome 'Idiopathic' HH LH/FSH beta subunit mutations FUNCTIONAL Hyperprolactinaemia Morbid obesity Cushing s syndrome Alcohol excess* COPD, chronic obstructive pulmonary disease; CTX, chemotherapy; ESRF, end stage renal disease; RTX, radiotherapy; HH, hypogonadotropic hypogonadism; T2DM, type 2 diabetes mellitus *Alcohol excess typically causes mixed (combined primary and secondary) hypogonadism. symptoms and signs. Patients should be well or medically stable, without acute decompensation of any underlying comorbidity. As testosterone release is diurnal, with the highest levels in the early morning, blood samples should be taken close to 8 am. Food intake can reduce total testosterone acutely by as much as 25%, explaining the importance of a fasting blood sample. There is marked variability in testosterone levels not only between individuals but also within an individual. Therefore, repeated measurements are necessary to confirm a low testosterone level and a diagnosis of hypogonadism should never be based on a single testosterone level. There is no general agreement on the acceptable normal range of testosterone. Reference intervals also vary between laboratories because of differences in assay methods and/ or reference population of men. In practice, if the total testosterone level is 12 nmol/l or above, the patient is usually eugonadal and further testing is generally not required. If the total testosterone level in a man with consistent symptoms and signs is less than 12 nmol/l, a repeat measurement of fasting morning testosterone level is suggested. Levels of 8 12 nmol/l may be considered borderline and <8 nmol/l low. If a testosterone level is borderline, requesting measurement of free testosterone may be helpful because the levels of total testosterone can be affected by alterations in levels of SHBG and albumin. Men with obesity and diabetes commonly have a low SHBG and here a normal free testosterone can be reassuring that such men are not, in fact, hypogonadal. In general, a repeatedly low testosterone level is more indicative of hypogonadism in younger, healthier and leaner men but more difficult to interpret in older obese men with chronic disease and non-specific symptoms. 6,7 Aetiology of hypogonadism Once the low testosterone value has been confirmed on repeated morning measurements in patients with consistent symptoms and signs, luteinizing hormone (LH) and follicle stimulating hormone (FSH) values should be obtained to further distinguish between primary or secondary hypogonadism (Table 1). Elevated LH and FSH values indicate primary (testicular) 278 REPRINTED FROM AUSTRALIAN FAMILY PHYSICIAN VOL. 43, NO. 5, MAY 2014
3 Assessment and management of male androgen disorders: an update CLINICAL hypogonadism, whereas low or importantly even inappropriately normal LH and FSH values may indicate secondary (pituitary hypothalamic) hypogonadism. Combined primary and secondary hypogonadism have variable gonadotropin levels, depending on whether primary or secondary hypogonadism predominates. Primary hypogonadism It is important to ask the patient about the age of onset of his problems, about congenital defects such as cryptorchidism, pubertal development, fertility, previous testicular trauma or infection, radiotherapy, chemotherapy, use of medications that inhibit androgen biosynthesis, and medical conditions that can cause both primary and secondary hypogonadism. A karyotype analysis should be obtained in men with primary testicular failure to exclude Klinefelter s syndrome (47XXY), which occurs in about 1 in 500 men. 3 for example due to a microprolactinoma, the hypogonadism will respond to, and should be treated by, normalising the prolactin level rather than by testosterone therapy. In the work-up for secondary hypogonadism, it is very important not to miss pituitary or hypothalamic pathology, which can damage gonadotroph production, resulting in hypogonadism. A careful clinical assessment for a pituitary mass effect (headache, visual field defect, eye movement disturbance), as well as for features of hypopituitarism or of a hormone producing pituitary tumour (eg. Cushing s syndrome) must be undertaken. Clinical suspicion of hypogonadism, clinically stable no intercurrent illness Haemochromatosis can be ruled out by measuring iron levels and determining the fasting transferrin saturation. Biochemical assessment of pituitary (dys-)function may be necessary, and pituitary imaging may need to be considered. Given that functional hypogonadism due to comorbidities presents with secondary hypogonadism, the yield of organic pathology is low in older obese men with comorbidities and only modest reductions in testosterone levels. The practitioner needs to be aware that men with prior or current anabolic steroid use may present with low testosterone and LH levels and use may be denied even with specific questioning. Secondary hypogonadism TT <8 12 nmol/l TT 8 12 nmol/l* Organic congenital causes of secondary hypogonadism are rare and include Kallmann syndrome, GnRH receptor mutation and deficiency, or genetic mutations associated with other pituitary hormone deficiencies. These congenital disorders are usually diagnosed in childhood or adolescence when patients present with pubertal delay. Acquired causes of secondary hypogonadism are summarised in Table 1. Androgen deprivation therapy given to men with prostate cancer is an increasingly important cause of severe androgen deficiency. Many chronic diseases are associated with low testosterone levels via suppression of gonadotropin production. levels are commonly lowered in men with metabolic syndrome, type 2 diabetes mellitus, obesity, depression, obstructive sleep apnoea, chronic kidney disease or anorexia nervosa. 7 In addition, certain medications, in particular glucocorticoids or opioids, reduce gonadotropins and testosterone levels. Hyperprolactinaemia can lead to secondary hypogonadism through suppression of the pulsatile release of gonadotropin-releasing hormone (GnRH) from the hypothalamus. Hence, measurement of prolactin levels is essential and, if elevated, its cause should be investigated. If there is pathological hyperprolactinaemia, Repeat, add free T T <8 12 nmol/l Free T low LH Normal or low Hypogonadotrophic hypogonadism Check medications that may lower T Anabolic steroids Opiates Glucocorticoids Measure: Prolactin Iron studies Consider pituitary imaging Review medical history Obesity, type 2 diabetes (very common) Severe chronic illness Figure 1. Work-up of androgen deficiency Consider other causes for clinical presentation eg. chronic illness, psycho-social issues Primary testicular failure: consider karyotype for Klinefelter s High LH, luteinizing hormone TT, testosterone trough T, testosterone REPRINTED FROM AUSTRALIAN FAMILY PHYSICIAN VOL. 43, NO. 5, MAY
4 Assessment and management of male androgen disorders: an update Clues to androgen abuse are muscular build, a low HDL level or a higher than expected haematocrit; organic androgen deficiency is often associated with mild anaemia due to the erythropoietic actions of testosterone. The diagnostic approach to hypogonadism is summarised in Figure 1. treatment It is very important to remember that an underlying aetiology should always be sought before testosterone therapy is considered. This is not only because hypogonadism can be due to underlying pathologies such as a pituitary tumour or haemochromatosis, important diagnoses not to be missed, but also because gonadotropin treatment of secondary hypogonadism may restore fertility. Importantly, if testosterone therapy is commenced before the diagnosis is confirmed, the diagnostic work-up can be obscured and fertility compromised. replacement is recommended for symptomatic classical androgen deficiency syndromes after excluding contraindications in the initial work up (Table 2). Men with organic hypogonadism respond very well to testosterone replacement therapy and show a marked improvement in sexual function, sense of well being and energy levels, and maintenance of secondary sexual characteristics. However, testosterone therapy does not improve fertility; in fact, because of gonadotropin suppression, testosterone therapy may supress spermatogenesis. Indeed, testosterone therapy is being evaluated in trials of male contraception. By contrast, in men with LOH, the distinction between replacement and pharmacological testosterone therapy becomes more difficult to define. Moreover, there is overlap between classical androgen deficiency and LOH. Certain Table 2. Contraindications to testosterone therapy 1 men who have functional hypogonadism have profound androgen deficiency similar to men with organic hypogonadism due to intrinsic HPT axis pathology. The risk benefit ratio of testosterone therapy in men with LOH is not well established because there are no large long-term randomised controlled clinical trials (RCT) that provide information about benefits for patients (eg. fracture reduction, improved functional morbidity or mortality) or therapy-associated risks. In men with functional hypogonadism resulting from chronic illness, especially obesity, the focus of therapy should be on lifestyle measures (especially weight loss) and optimisation of comorbidities. Although difficult to achieve and sustain, moderate weight loss (<10%) can increase testosterone levels by 2 3 nmol/l. Substantially larger increases (up to >10 nmol/) may be achieved in severely obese men who have successful bariatric surgery. 6,7 treatment in men with only modest reductions in circulating testosterone levels should be considered only if such measures fail, and is only recommended in the presence of symptoms. Symptoms of hypogonadism are non-specific and may be consequent to underlying comorbidities; men with symptomatic LOH are less likely to respond to testosterone therapy, compared with younger men with organic hypogonadism in whom such comorbidities are absent. 7 There are no restrictions regarding testosterone replacement in men with organic hypogonadism due to established pathology of the HPT axis. By contrast, in men without classical androgen deficiency, testosterone therapy is subsidised by the Pharmaceutical Benefit Scheme (PBS) only if the testosterone level is <8 nmol/l or 8 15 nmol/l with high LH levels, defined as >1.5 Breast or prostate cancer A palpable prostate nodule or induration without further urological evaluation PSA >4 ng/ml (or >3 ng/ml in men at high risk of prostate cancer) without further urological evaluation Severe lower urinary tract symptoms (International prostate symptom score >19) Haematocrit >50% Untreated severe obstructive sleep apnoea Uncontrolled or poorly controlled heart failure When fertility is desired times the upper limit of the eugonadal reference range for young men. However, the primary intent of this PBS cut-off of 8 nmol/l was to restrict unproven overuse of testosterone therapy, and even in men with repeated total testosterone levels of <8 nmol/l, treatment should be individualised. It may be reasonable to consider a trial of testosterone therapy in selected men with LOH, in the absence of contraindications. As symptoms of androgen deficiency should improve within 1 3 months, a therapy trial of 3 6 months is usually of sufficient duration. It is important to inform the patient that this approach is not backed by highlevel evidence of efficacy and safety. In addition, the patient should be informed at the outset that testosterone therapy will be stopped should there be no benefit, according to defined treatment goals agreed by the patient and practitioner. In such men, the therapeutic target should be to raise serum testosterone levels to the low-to-mid-normal range of healthy young men. The risk of iatrogenic suppression of the HPT axis with a short course of testosterone therapy is low, but longer acting testosterone preparations should be avoided initially. In men suitable for long-term testosterone therapy, different options are available (Table 3) and choice depends on patient and physician preference. Androgen deficiency and erectile dysfunction are two overlapping conditions with distinct pathophysiology. A randomised, placebo-controlled trial studied the effect of testosterone therapy added to sildenafil in erectile dysfunction. The results showed that sildenafil plus testosterone was not superior to sildenafil plus placebo, although pre-treatment testosterone levels in such men were not unequivocally low. 9 treatment: potential risks and monitoring for adverse events Young men with organic hypogonadism generally have a favourable risk benefit ratio with testosterone therapy, provided they are monitored for side effects (Table 4) and men with contraindications (Table 2) have been excluded. By contrast, there may be increased risks in older, obese men because of comorbidities, such as prostate disease and undiagnosed obstructive sleep apnoea. 1 RCTs in older men receiving testosterone therapy and meta-analyses to date 280 REPRINTED FROM AUSTRALIAN FAMILY PHYSICIAN VOL. 43, NO. 5, MAY 2014
5 Assessment and management of male androgen disorders: an update CLINICAL Table 3. therapy: formulations 1 Preparation/ administration gel 1%, daily Advantages Disadvantages monitoring Short half-life in case of side effects Chance for inadvertent transfer to close contacts (spouse, children, nurses) Imprecise dose adjustment Marked variation in blood levels Skin irritation Morning, before application, after use for 7 days patch, daily Short half-life in case of side effects Skin irritation Limited scope for dose variation Morning after evening application transdermal solution, daily Short half-life in case of side-effects Low chance of inadvertent transfer to others Pump applicator required Must be administered in the axilla Skin irritation May not wash, shower or swim within 2 hours of application Monitor after 2 weeks, trough level taken 2 8 hours after application undecanoate 40 mg capsule, 2 3 times per day Short half-life in case of side effects Frequent dosing required (2 3 times daily) Marked variation in blood levels Gastrointestinal intolerance Monitor after 2 weeks undecanoate 1 g. IM injection 3-monthly Convenience Compliance Stable testosterone (T) levels Injection site pain Contraindicated in men with coagulopathies Cannot be self-administered Morning, before fourth injection. Aim for trough level nmol/l. Allow a further 2 3 injections after dose adjustment before rechecking implant 100 mg 6 monthly Convenience Compliance Stable T levels Invasive procedure required Extrusion, infection, bleeding 6-monthly after a mg dose Table 4. Adverse effects of testosterone therapy 1 More common Erythrocytosis Acne and oily skin Detection of subclinical prostate cancer Growth of metastatic prostate cancer Reduced sperm production and fertility Uncommon Gynaecomastia Male pattern balding (familial) Growth of breast cancer Induction or worsening of obstructive sleep apnoea have been underpowered to provide definitive outcome data regarding cardiovascular and prostate events. The main areas of concern relate to prostate and cardiovascular events. While there is no evidence that testosterone causes prostate cancer, the main practical issue is that because of prostate monitoring during testosterone therapy, there may be an increased risk of over-diagnosing pre-existing, clinically insignificant prostate cancer. One recent RCT has shown an increase in cardiovascular events with testosterone treatment in relatively frail older men, 10 but numbers were small and may have been due to chance. Another RCT in a similar population has not confirmed this finding. 11 Hence, monitoring patients according to a standardised monitoring plan is important. 1 Key points Organic androgen deficiency due to intrinsic HPT axis pathology can be missed, and there is indeed evidence that classical androgen deficiency is underdiagnosed. Such men usually benefit markedly from testosterone replacement (except fertility), with a generally low risk of adverse events. therapy should not be started without a thorough work-up to delineate the underlying aetiology and identify associated pathologies. Older obese men with chronic comorbidities commonly present with non-specific symptoms and modestly low testosterone. In such men emphasis should be on weight loss and optimisation of comorbidities. The risk benefit ratio of testosterone therapy in such men is less favourable than in men with organic androgen deficiency. therapy should include: a discussion about the uncertainties REPRINTED FROM AUSTRALIAN FAMILY PHYSICIAN VOL. 43, NO. 5, MAY
6 Assessment and management of male androgen disorders: an update regarding risks/benefits (especially in men without organic androgen deficiency) patient-centred goals implementation of a standardised monitoring program ongoing evaluation for benefit/ adverse events. Large, well-conducted clinical trials are needed to provide more evidence to guide clinicians and patients regarding the benefits, and risks, of testosterone therapy. Authors Irene Chan MBBS, BMedSc, Endocrinology Advanced Trainee, Department of Endocrinology, Austin Health, Melbourne, VIC. KaIan.Chan@ austin.org.au Mark Ng Tang Fui MBBS, BMedSC, FRACP, Consultant Endocrinologist, Department of Endocrinology, Austin Health, Melbourne, VIC Jeffrey D. Zajac MBBS, PhD, FRACP, Professor of Medicine and Head of Department of Medicine, Austin Health, University of Melbourne, and Director, Department of Endocrinology, Austin Health, Melbourne, VIC Mathis Grossmann MD, PhD, FRACP, Principal Research Fellow, Department of Medicine Austin Health, University of Melbourne, and Head of Men s Health, Department of Endocrinology, Austin Health, Melbourne, VIC Competing interests: None. Provenance and peer review: Not commissioned; externally peer reviewed. References 1. Bhasin S, Cunningham GR, Hayes FJ, et al. therapy in men with androgen deficiency syndromes: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 2010;95: Handelsman DJ, Zajac JD. Androgen deficiency and replacement therapy in men. Med J Aust 2014;180: Herlihy AS, Halliday JL, Cock ML, McLachlan RI. The prevalence and diagnosis rates of Klinefelter syndrome: an Australian comparison. Med J Aust 2011;194: Wu FC, Tajar A, Beynon JM, et al. Identification of late-onset hypogonadism in middle-aged and elderly men. N Engl J Med 2010;363: Sartorius G, Spasevska S, Idan A, et al. Serum testosterone, dihydrotestosterone and estradiol concentrations in older men self-reporting very good health: the healthy man study. Clin Endocrinol (Oxf) 2012;77: Ng Tan Fui M, Dupuis P, Grosssmann M. Lowered in Male Obesity: Mechanisms, Morbidity and Management. Asian J Androl. In press. 7. Grossmann M. Low testosterone in men with type 2 diabetes: significance and treatment. J Clin Endocrinol Metab 2011;96: Snyder P. Causes of secondary hypogonadism in males. In: Matsumoto AM, Geffner M, editors. UpToDate. Waltham: Wolters Kluwer Spitzer M, Basaria S, Travison TG, et al. Effect of testosterone replacement on response to sildenafil citrate in men with erectile dysfunction: a parallel, randomized trial. Ann Intern Med 2012;157: Basaria S, Coviello AD, Travison TG, et al. Adverse events associated with testosterone administration. N Engl J Med 2010;363: Srinivas-Shankar U, Roberts SA, Connolly MJ, et al. Effects of testosterone on muscle strength, physical function, body composition, and quality of life in intermediate-frail and frail elderly men: a randomized, double-blind, placebo-controlled study. J Clin Endocrinol Metab 2010;95: REPRINTED FROM AUSTRALIAN FAMILY PHYSICIAN VOL. 43, NO. 5, MAY 2014
Hypogonadism 4/27/2018. Male Hypogonadism -- Definition. Epidemiology. Objectives HYPOGONADISM. Men with Hypogonadism. 95% untreated.
 Male Hypogonadism -- Definition - Low T, Low Testosterone Hypogonadism -...a clinical syndrome that results from failure of the testes to produce physiological concentrations of testosterone due to pathology
Male Hypogonadism -- Definition - Low T, Low Testosterone Hypogonadism -...a clinical syndrome that results from failure of the testes to produce physiological concentrations of testosterone due to pathology
GUIDELINES ON. Introduction. G.R. Dohle, S. Arver, C. Bettocchi, S. Kliesch, M. Punab, W. de Ronde
 GUIDELINES ON Male Hypogonadism G.R. Dohle, S. Arver,. Bettocchi, S. Kliesch, M. Punab, W. de Ronde Introduction Male hypogonadism is a clinical syndrome caused by androgen deficiency. It may adversely
GUIDELINES ON Male Hypogonadism G.R. Dohle, S. Arver,. Bettocchi, S. Kliesch, M. Punab, W. de Ronde Introduction Male hypogonadism is a clinical syndrome caused by androgen deficiency. It may adversely
EAU GUIDELINES ON MALE HYPOGONADISM
 EAU GUIDELINES ON MALE HYPOGONADISM (Limited text update March 2017) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch Introduction Male hypogonadism is a clinical syndrome caused by androgen
EAU GUIDELINES ON MALE HYPOGONADISM (Limited text update March 2017) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch Introduction Male hypogonadism is a clinical syndrome caused by androgen
EAU GUIDELINES ON MALE HYPOGONADISM
 EAU GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by
EAU GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by
GUIDELINES ON MALE HYPOGONADISM
 GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by androgen
GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by androgen
BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE
 Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
Testosterone Treatment: Myths Vs Reality. Fadi Al-Khayer, M.D, F.A.C.E
 Testosterone Treatment: Myths Vs Reality Fadi Al-Khayer, M.D, F.A.C.E The Biological Functions of Testosterone in Men Testosterone is essential to the musculoskeletal and metabolic systems throughout a
Testosterone Treatment: Myths Vs Reality Fadi Al-Khayer, M.D, F.A.C.E The Biological Functions of Testosterone in Men Testosterone is essential to the musculoskeletal and metabolic systems throughout a
Testosterone Therapy in Men with Hypogonadism
 Testosterone Therapy in Men with Hypogonadism (Endocrine Society 2018 Guideline) Ngwe Yin, MD Assistant Clinical Professor of Medicine, UCSF Fresno Medical Education Program Disclosures None Objective
Testosterone Therapy in Men with Hypogonadism (Endocrine Society 2018 Guideline) Ngwe Yin, MD Assistant Clinical Professor of Medicine, UCSF Fresno Medical Education Program Disclosures None Objective
Corporate Medical Policy Testosterone Pellet Implantation for Androgen Deficiency
 Corporate Medical Policy Testosterone Pellet Implantation for Androgen Deficiency File Name: Origination: Last CAP Review: Next CAP Review: Last Review: testosterone_pellet_implantation_for_androgen_deficiency
Corporate Medical Policy Testosterone Pellet Implantation for Androgen Deficiency File Name: Origination: Last CAP Review: Next CAP Review: Last Review: testosterone_pellet_implantation_for_androgen_deficiency
Androgen deficiency. Dr Rakesh Iyer Staff Specialist in Endocrinology Calvary hospital
 Androgen deficiency Dr Rakesh Iyer Staff Specialist in Endocrinology Calvary hospital Outline Pathological androgen deficiency - Background, causes, interpretation - Indications for treatment Androgen
Androgen deficiency Dr Rakesh Iyer Staff Specialist in Endocrinology Calvary hospital Outline Pathological androgen deficiency - Background, causes, interpretation - Indications for treatment Androgen
Evaluation and Treatment of Primary Androgen Deficiency Syndrome in Male Patients
 Evaluation and Treatment of Primary Androgen Deficiency Syndrome in Male Patients Jeff Unger, MD Director Chino Medical Group Diabetes and Headache Intervention Center Chino, California January 16, 2008
Evaluation and Treatment of Primary Androgen Deficiency Syndrome in Male Patients Jeff Unger, MD Director Chino Medical Group Diabetes and Headache Intervention Center Chino, California January 16, 2008
TESTOSTERONE DEFINITION
 DEFINITION A hormone that is a hydroxyl steroid ketone (C19H28O2) produced especially by the testes or made synthetically and that is responsible for inducing and maintaining male secondary sex characteristics.
DEFINITION A hormone that is a hydroxyl steroid ketone (C19H28O2) produced especially by the testes or made synthetically and that is responsible for inducing and maintaining male secondary sex characteristics.
ISSM QUICK REFERENCE GUIDE ON TESTOSTERONE DEFICIENCY FOR MEN
 International Society for Sexual Medicine - www.issm.info ISSM QUICK REFERENCE GUIDE ON TESTOSTERONE DEFICIENCY FOR MEN Version: September 2015 What is testosterone deficiency? Testosterone deficiency
International Society for Sexual Medicine - www.issm.info ISSM QUICK REFERENCE GUIDE ON TESTOSTERONE DEFICIENCY FOR MEN Version: September 2015 What is testosterone deficiency? Testosterone deficiency
ANDROGEN DEFICIENCY/MALE HYPOGONADISM
 ANDROGEN DEFICIENCY/MALE HYPOGONADISM 1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of testosterone (androgen deficiency)
ANDROGEN DEFICIENCY/MALE HYPOGONADISM 1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of testosterone (androgen deficiency)
Male Hypogonadism. Types and causes of hypogonadism. What is male hypogonadism? Symptoms. Testosterone production. Patient Information.
 Patient Information English 31 Male Hypogonadism The underlined terms are listed in the glossary. What is male hypogonadism? Male hypogonadism means the testicles do not produce enough of the male sex
Patient Information English 31 Male Hypogonadism The underlined terms are listed in the glossary. What is male hypogonadism? Male hypogonadism means the testicles do not produce enough of the male sex
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acquired hypogonadism, prevalence of, 165 167 primary, 165 secondary, 167 Adipose tissue, as an organ, 240 241 Adrenal hyperplasia, congenital,
Note: Page numbers of article titles are in boldface type. A Acquired hypogonadism, prevalence of, 165 167 primary, 165 secondary, 167 Adipose tissue, as an organ, 240 241 Adrenal hyperplasia, congenital,
6/14/2010. GnRH=Gonadotropin-Releasing Hormone.
 Male Androgen Replacement Mitchell Sorsby, MD June 19, 2010. QUESTION # 1 Which of the following is not a symptom associated with low T levels? a) decreased libido b) erectile dysfunction c) depression
Male Androgen Replacement Mitchell Sorsby, MD June 19, 2010. QUESTION # 1 Which of the following is not a symptom associated with low T levels? a) decreased libido b) erectile dysfunction c) depression
How to treat: TRT modalities and formulations
 How to treat: TRT modalities and formulations Paul PIETTE, PharmD Senior Research Fellow Clinique Antoine Depage - Belgium ppiette@besins-healthcare.com Bruges 2014, May 15 th Testosterone-replacement
How to treat: TRT modalities and formulations Paul PIETTE, PharmD Senior Research Fellow Clinique Antoine Depage - Belgium ppiette@besins-healthcare.com Bruges 2014, May 15 th Testosterone-replacement
Pharmacy Coverage Guidelines are subject to change as new information becomes available.
 TESTOSTERONE REPLACEMENT THERAPY: ANDRODERM transdermal patch ANDROGEL pump transdermal gel and transdermal gel AXIRON transdermal solution FORTESTA transdermal gel NATESTO nasal gel STRIANT buccal mucoadhesive
TESTOSTERONE REPLACEMENT THERAPY: ANDRODERM transdermal patch ANDROGEL pump transdermal gel and transdermal gel AXIRON transdermal solution FORTESTA transdermal gel NATESTO nasal gel STRIANT buccal mucoadhesive
What Is the Low T Syndrome? Is Testosterone Supplementation Safe?
 What Is the Low T Syndrome? Is Testosterone Supplementation Safe? UCSF Osher Mini Medical School March 7, 2018 Dolores Shoback, MD Staff Physician SF-VAMC Professor of Medicine, UCSF No disclosures or
What Is the Low T Syndrome? Is Testosterone Supplementation Safe? UCSF Osher Mini Medical School March 7, 2018 Dolores Shoback, MD Staff Physician SF-VAMC Professor of Medicine, UCSF No disclosures or
ANDROGEN DEFICIENCY/MALE HYPOGONADISM
 Medical Information to Support the Decisions of TUE Committees 1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of
Medical Information to Support the Decisions of TUE Committees 1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of
Laboratory Investigation of Male Gonadal Function. Dr N Oosthuizen Dept of Chemical Pathology UP 2010
 Laboratory Investigation of Male Gonadal Function Dr N Oosthuizen Dept of Chemical Pathology UP 2010 1 Figure 1. Hypothalamic-pituitary pituitary-testicular testicular axis 2 Testosterone (T) measurement
Laboratory Investigation of Male Gonadal Function Dr N Oosthuizen Dept of Chemical Pathology UP 2010 1 Figure 1. Hypothalamic-pituitary pituitary-testicular testicular axis 2 Testosterone (T) measurement
Managing Testosterone Deficiency: A Practical Guide. John Grantmyre MD Professor of Urology Dalhousie University
 Managing Testosterone Deficiency: A Practical Guide John Grantmyre MD Professor of Urology Dalhousie University 1 2 Case Study #1 A 59-Year-Old Man with Erectile Dysfunction 3 Case History Robert is a
Managing Testosterone Deficiency: A Practical Guide John Grantmyre MD Professor of Urology Dalhousie University 1 2 Case Study #1 A 59-Year-Old Man with Erectile Dysfunction 3 Case History Robert is a
Prior Authorization Criteria Update: Androgens, Topical and Parenteral
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Testosterone Injection / Implant
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Testosterone Injection / Implant Page: 1 of 9 Last Review Date: December 5, 2014 Testosterone
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Testosterone Injection / Implant Page: 1 of 9 Last Review Date: December 5, 2014 Testosterone
Androderm patch, AndroGel packets and pump, Axiron solution, First- Testosterone, First-Testosterone MC, Fortesta gel, Testim gel, Vogelxo
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.31 Subject: Testosterone Topical Page: 1 of 9 Last Review Date: September 23, 2016 Testosterone topical
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.31 Subject: Testosterone Topical Page: 1 of 9 Last Review Date: September 23, 2016 Testosterone topical
Testosterone Oral Buccal Nasal. Android, Androxy, Methitest, Natesto, Striant, Testred. Description
 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.32 Subject: Testosterone Oral Buccal Nasal Page: 1 of 10 Last Review Date: March 17, 2017 Testosterone Oral Buccal Nasal Description
1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.32 Subject: Testosterone Oral Buccal Nasal Page: 1 of 10 Last Review Date: March 17, 2017 Testosterone Oral Buccal Nasal Description
Implantable Hormone Pellets
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Testosterone Therapy in Men An update
 Testosterone Therapy in Men An update SANDEEP DHINDSA Associate Professor of Medicine Director, Division of Endocrinology and Metabolism, Saint Louis University, St. Louis, MO Presenter Disclosure None
Testosterone Therapy in Men An update SANDEEP DHINDSA Associate Professor of Medicine Director, Division of Endocrinology and Metabolism, Saint Louis University, St. Louis, MO Presenter Disclosure None
Testosterone Oral Buccal Nasal. Android, Androxy, Methitest, Natesto, Striant, Testred. Description
 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.32 Subject: Testosterone Oral Buccal Nasal Page: 1 of 10 Last Review Date: June 24, 2016 Testosterone Oral Buccal Nasal Description
1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.32 Subject: Testosterone Oral Buccal Nasal Page: 1 of 10 Last Review Date: June 24, 2016 Testosterone Oral Buccal Nasal Description
Androgens. Medication Strengths Quantity Limit Comments Androderm (testosterone patch) 1% pump 2 pump bottles per Non-Preferred
 Market DC Androgens Override(s) Prior Authorization Quantity Limit Approval Duration Varies upon diagnosis Medication Strengths Quantity Limit Comments Androderm (testosterone patch) AndroGel (testosterone
Market DC Androgens Override(s) Prior Authorization Quantity Limit Approval Duration Varies upon diagnosis Medication Strengths Quantity Limit Comments Androderm (testosterone patch) AndroGel (testosterone
Testosterone Therapy in Men With Hypogonadism: An Endocrine Society* Clinical Practice Guideline
 CLINICAL PRACTICE GUIDELINE Testosterone Therapy in Men With Hypogonadism: An Endocrine Society* Clinical Practice Guideline Shalender Bhasin, 1 Juan P. Brito, 2 Glenn R. Cunningham, 3 Frances J. Hayes,
CLINICAL PRACTICE GUIDELINE Testosterone Therapy in Men With Hypogonadism: An Endocrine Society* Clinical Practice Guideline Shalender Bhasin, 1 Juan P. Brito, 2 Glenn R. Cunningham, 3 Frances J. Hayes,
Late onset Hypogonadism. Dr KhooSay Chuan Department of Urology Penang General Hospital
 Late onset Hypogonadism Dr KhooSay Chuan Department of Urology Penang General Hospital Late onset hypogonadism(loh) Definition LOH age associated testoteronedeficiency syndrome (TDS) Male menopause, andropause,
Late onset Hypogonadism Dr KhooSay Chuan Department of Urology Penang General Hospital Late onset hypogonadism(loh) Definition LOH age associated testoteronedeficiency syndrome (TDS) Male menopause, andropause,
ANDROGEN DEFICIENCY A GUIDE TO MALE HORMONES A BOOKLET IN THE SERIES OF CONSUMER GUIDES ON MALE REPRODUCTIVE HEALTH FROM
 ANDROGEN DEFICIENCY A GUIDE TO MALE HORMONES A BOOKLET IN THE SERIES OF CONSUMER GUIDES ON MALE REPRODUCTIVE HEALTH FROM First published in July 2003 by Andrology Australia 5th Edition, December 2015 Copyright
ANDROGEN DEFICIENCY A GUIDE TO MALE HORMONES A BOOKLET IN THE SERIES OF CONSUMER GUIDES ON MALE REPRODUCTIVE HEALTH FROM First published in July 2003 by Andrology Australia 5th Edition, December 2015 Copyright
Testosterone Therapy in Men with Androgen Deficiency Syndromes: An Endocrine Society Clinical Practice Guideline
 SPECIAL FEATURE Clinical Practice Guideline Testosterone Therapy in Men with Androgen Deficiency Syndromes: An Endocrine Society Clinical Practice Guideline Shalender Bhasin, Glenn R. Cunningham, Frances
SPECIAL FEATURE Clinical Practice Guideline Testosterone Therapy in Men with Androgen Deficiency Syndromes: An Endocrine Society Clinical Practice Guideline Shalender Bhasin, Glenn R. Cunningham, Frances
Testosterone Oral Buccal Nasal. Android, Androxy, Methitest, Natesto, Striant, Testred. Description
 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.32 Subject: Testosterone Oral Buccal Nasal Page: 1 of 10 Last Review Date: November 30, 2018 Testosterone Oral Buccal Nasal
1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.32 Subject: Testosterone Oral Buccal Nasal Page: 1 of 10 Last Review Date: November 30, 2018 Testosterone Oral Buccal Nasal
Clinical Policy: Testosterone Pellet (Testopel) Reference Number: CP.CPA.## [Pre-P&T approval] Effective Date:
![Clinical Policy: Testosterone Pellet (Testopel) Reference Number: CP.CPA.## [Pre-P&T approval] Effective Date: Clinical Policy: Testosterone Pellet (Testopel) Reference Number: CP.CPA.## [Pre-P&T approval] Effective Date:](/thumbs/75/72057018.jpg) Clinical Policy: (Testopel) Reference Number: CP.CPA.## [Pre-P&T approval] Effective Date: 07.25.17 Last Review Date: 11.17 Line of Business: Commercial Coding Implications Revision Log See Important Reminder
Clinical Policy: (Testopel) Reference Number: CP.CPA.## [Pre-P&T approval] Effective Date: 07.25.17 Last Review Date: 11.17 Line of Business: Commercial Coding Implications Revision Log See Important Reminder
Testosterone Injection and Implant
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.33 Subject: Testosterone Injection Implant Page: 1 of 10 Last Review Date: December 8, 2017 Testosterone
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.33 Subject: Testosterone Injection Implant Page: 1 of 10 Last Review Date: December 8, 2017 Testosterone
GA KS KY LA MD NJ NV NY TN TX WA Applicable X X N/A N/A X N/A X X X X X X N/A N/A NA *FHK- Florida Healthy Kids. Androgens
 Androgens Override(s) Prior Authorization Quantity Limit Approval Duration Varies upon diagnosis Medication Strengths Quantity Limit Comments Generic Androgel 1% (2.5 g) packet 2 packets per day (testosterone
Androgens Override(s) Prior Authorization Quantity Limit Approval Duration Varies upon diagnosis Medication Strengths Quantity Limit Comments Generic Androgel 1% (2.5 g) packet 2 packets per day (testosterone
Implantable Hormone Pellets
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Testosterone Therapy in Adult Men with Androgen Deficiency Syndromes:
 The Endocrine Society s CLINICAL GUIDELINES Testosterone Therapy in Adult Men with Androgen Deficiency Syndromes: An Endocrine Society Clinical Practice Guideline Authors: Shalender Bhasin, Glenn R. Cunningham,
The Endocrine Society s CLINICAL GUIDELINES Testosterone Therapy in Adult Men with Androgen Deficiency Syndromes: An Endocrine Society Clinical Practice Guideline Authors: Shalender Bhasin, Glenn R. Cunningham,
Men Getting Older Will Testosterone Keep Him Young?
 Men Getting Older Will Testosterone Keep Him Young? Alvin M. Matsumoto, M.D. Associate Director, GRECC V.A. Puget Sound Health Care System Professor, Department of Medicine Division of Gerontology and
Men Getting Older Will Testosterone Keep Him Young? Alvin M. Matsumoto, M.D. Associate Director, GRECC V.A. Puget Sound Health Care System Professor, Department of Medicine Division of Gerontology and
Outline. Classic Androgen deficiency. Cardiovascular Risk and Testosterone Fact vs Fiction. Professor Robert I McLachlan AM, FRACP, PhD
 Health Ed Brisbane Saturday 27 th October 2018 Cardiovascular Risk and Testosterone Fact vs Fiction Professor Robert I McLachlan AM, FRACP, PhD Hudson Institute of Medical Research, Monash University Department
Health Ed Brisbane Saturday 27 th October 2018 Cardiovascular Risk and Testosterone Fact vs Fiction Professor Robert I McLachlan AM, FRACP, PhD Hudson Institute of Medical Research, Monash University Department
Prof. Dr. Michael Zitzmann Internal Medicine Endocrinology, Diabetology, Andrology University of Muenster, Germany
 Induction of fertility in hypogonadal men Prof. Dr. Michael Zitzmann Internal Medicine Endocrinology, Diabetology, Andrology University of Muenster, Germany Induction of fertility in hypogonadal men Prof.
Induction of fertility in hypogonadal men Prof. Dr. Michael Zitzmann Internal Medicine Endocrinology, Diabetology, Andrology University of Muenster, Germany Induction of fertility in hypogonadal men Prof.
Contents. At A Glance 04. Male Hormones 06. Androgen Deficiency 10. Symptoms 11. Causes 14. Staying Healthy 20. Diagnosis 22. Treatment 29.
 Androgen Deficiency Contents At A Glance 04 Male Hormones 06 Androgen Deficiency 10 Symptoms 11 - DATE REVIEWED: JANUARY 2019 (6TH EDITION) Healthy Male (Andrology Australia) 2003 Causes 14 Staying Healthy
Androgen Deficiency Contents At A Glance 04 Male Hormones 06 Androgen Deficiency 10 Symptoms 11 - DATE REVIEWED: JANUARY 2019 (6TH EDITION) Healthy Male (Andrology Australia) 2003 Causes 14 Staying Healthy
OVERVIEW OF PRESENTATION
 Thanh D. Hoang, DO, FACP, FACE Division of Endocrinology Department of Internal Medicine WRNMMC 13 Aug 2018 OVERVIEW OF PRESENTATION Take Home Points Definition of Hypogonadism Clinical Manifestations
Thanh D. Hoang, DO, FACP, FACE Division of Endocrinology Department of Internal Medicine WRNMMC 13 Aug 2018 OVERVIEW OF PRESENTATION Take Home Points Definition of Hypogonadism Clinical Manifestations
Pharmacy Coverage Guidelines are subject to change as new information becomes available.
 TESTOSTERONE REPLACEMENT THERAPY: ANDRODERM transdermal patch ANDROGEL pump transdermal gel and transdermal gel ANDROID (methyltestosterone) oral capsule ANDROXY (fluoxymesterone) oral tablet AXIRON transdermal
TESTOSTERONE REPLACEMENT THERAPY: ANDRODERM transdermal patch ANDROGEL pump transdermal gel and transdermal gel ANDROID (methyltestosterone) oral capsule ANDROXY (fluoxymesterone) oral tablet AXIRON transdermal
Late Onset Hypogonadism. Toh Charng Chee Hospital Selayang
 Late Onset Hypogonadism Toh Charng Chee Hospital Selayang Introduction Although suppressed serum testosterone (T) is common in ageing men, only a small proportion of them develop the genuine syndrome of
Late Onset Hypogonadism Toh Charng Chee Hospital Selayang Introduction Although suppressed serum testosterone (T) is common in ageing men, only a small proportion of them develop the genuine syndrome of
MALE HYPOGONADISM: CHOOSING THE APPROPRIATE THERAPY. Michael S. Irwig, M.D. Director, Center for Andrology Division of Endocrinology & Metabolism
 MALE HYPOGONADISM: CHOOSING THE APPROPRIATE THERAPY Michael S. Irwig, M.D. Director, Center for Andrology Division of Endocrinology & Metabolism Disclosures Aromatase inhibitors & clomiphene citrate are
MALE HYPOGONADISM: CHOOSING THE APPROPRIATE THERAPY Michael S. Irwig, M.D. Director, Center for Andrology Division of Endocrinology & Metabolism Disclosures Aromatase inhibitors & clomiphene citrate are
Late onset hypogonadism
 Late onset hypogonadism Farrukh Javid Male Menopause Clinical AND biochemical syndrome Testosterone levels decline by 0.4-3% per year after the age of 30, as opposed to the more rapid decline that occurs
Late onset hypogonadism Farrukh Javid Male Menopause Clinical AND biochemical syndrome Testosterone levels decline by 0.4-3% per year after the age of 30, as opposed to the more rapid decline that occurs
Testosterone Injection and Implant
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.33 Subject: Testosterone Injection Implant Page: 1 of 10 Last Review Date: March 17, 2017 Testosterone
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.33 Subject: Testosterone Injection Implant Page: 1 of 10 Last Review Date: March 17, 2017 Testosterone
Testosterone Injection and Implant
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.33 Subject: Testosterone Injection Implant Page: 1 of 10 Last Review Date: November 30, 2018 Testosterone
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.33 Subject: Testosterone Injection Implant Page: 1 of 10 Last Review Date: November 30, 2018 Testosterone
Prof Dato Dr TAN Hui Meng University of Malaya, Kuala Lumpur University of Pennsylvania, USA
 Prof Dato Dr TAN Hui Meng University of Malaya, Kuala Lumpur University of Pennsylvania, USA Prevailing context Increase number of men who are potential candidates for Testosterone Replacement Therapy
Prof Dato Dr TAN Hui Meng University of Malaya, Kuala Lumpur University of Pennsylvania, USA Prevailing context Increase number of men who are potential candidates for Testosterone Replacement Therapy
GONADAL FUNCTION: An Overview
 GONADAL FUNCTION: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences Clinical Biochemistry BMLS III & BDS IV VJ Temple 1 What are the Steroid hormones?
GONADAL FUNCTION: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences Clinical Biochemistry BMLS III & BDS IV VJ Temple 1 What are the Steroid hormones?
Reproductive Health and Pituitary Disease
 Reproductive Health and Pituitary Disease Janet F. McLaren, MD Assistant Professor Division of Reproductive Endocrinology and Infertility Department of Obstetrics and Gynecology jmclaren@uabmc.edu Objectives
Reproductive Health and Pituitary Disease Janet F. McLaren, MD Assistant Professor Division of Reproductive Endocrinology and Infertility Department of Obstetrics and Gynecology jmclaren@uabmc.edu Objectives
TUE Physician Guidelines Medical Information to Support the Decisions of TUE Committees MALE HYPOGONADISM MALE HYPOGONADISM
 1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of testosterone (testosterone deficiency) and in some instances normal
1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of testosterone (testosterone deficiency) and in some instances normal
Didactic Series. Hypogonadism and HIV. Daniel Lee, MD UCSD Medical Center, Owen Clinic July 28, 2016
 Didactic Series Hypogonadism and HIV Daniel Lee, MD UCSD Medical Center, Owen Clinic July 28, 2016 This project is supported by the Health Resources and Services Administration (HRSA) of the U.S. Department
Didactic Series Hypogonadism and HIV Daniel Lee, MD UCSD Medical Center, Owen Clinic July 28, 2016 This project is supported by the Health Resources and Services Administration (HRSA) of the U.S. Department
ANDROGEN DEFICIENCY Update on Evaluation and Management
 ANDROGEN DEFICIENCY Update on Evaluation and Management Kristen Gill Hairston, MD, MPH Associate Professor of Internal Medicine Section of Endocrinology and Metabolism Wake Forest University School of
ANDROGEN DEFICIENCY Update on Evaluation and Management Kristen Gill Hairston, MD, MPH Associate Professor of Internal Medicine Section of Endocrinology and Metabolism Wake Forest University School of
in Primary Care (Part 2) Jonathan R. Anolik, MD, FACP, FACE Lewis Katz School of Medicine at Temple University
 Common Endocrine Problems Seen in Primary Care (Part 2) Lecture #34 Jonathan R. Anolik, MD, FACP, FACE Lewis Katz School of Medicine at Temple University None Conflict of Interest Topics to be Covered
Common Endocrine Problems Seen in Primary Care (Part 2) Lecture #34 Jonathan R. Anolik, MD, FACP, FACE Lewis Katz School of Medicine at Temple University None Conflict of Interest Topics to be Covered
Male History, Clinical Examination and Testing
 Male History, Clinical Examination and Testing Dirk Vanderschueren, MD, PhD Case Jan is 29 years old and consults for 1 year primary subfertility partner 28 years old and normal gynaecological investigation
Male History, Clinical Examination and Testing Dirk Vanderschueren, MD, PhD Case Jan is 29 years old and consults for 1 year primary subfertility partner 28 years old and normal gynaecological investigation
IOWA MEDICAID DRUG UTILIZATION REVIEW COMMISSION 100 Army Post Road 5)
 IOWA MEDICAID DRUG UTILIZATION REVIEW COMMISSION 100 Army Post Road 5) 974-3131 -866-626-0216 Brett Faine, Pharm.D. Larry Ambroson, R.Ph. Brian Couse, M.D. Date: February 10, 2015 Mark Graber, M.D., FACEP,
IOWA MEDICAID DRUG UTILIZATION REVIEW COMMISSION 100 Army Post Road 5) 974-3131 -866-626-0216 Brett Faine, Pharm.D. Larry Ambroson, R.Ph. Brian Couse, M.D. Date: February 10, 2015 Mark Graber, M.D., FACEP,
M0BCore Safety Profile. Active substance: Triptorelin Pharmaceutical form(s)/strength: 0,1 mg P-RMS: DE/H/PSUR/0038/002 Date of FAR:
 M0BCore Safety Profile Active substance: Triptorelin Pharmaceutical form(s)/strength: 0,1 mg P-RMS: DE/H/PSUR/0038/002 Date of FAR: 26.05.2014 4.3 Contraindications Hypersensitivity to GnRH, its analogues
M0BCore Safety Profile Active substance: Triptorelin Pharmaceutical form(s)/strength: 0,1 mg P-RMS: DE/H/PSUR/0038/002 Date of FAR: 26.05.2014 4.3 Contraindications Hypersensitivity to GnRH, its analogues
Update on Androgen Deficiency. Acknowledgments. Curatio PowerPoint TemplateControversies in Male Hypogonadism Bradley D.
 The General Practice Education Day Healthed / Generation Next August 22 nd Sydney Update on Androgen Deficiency Robert I. McLachlan, FRACP, PhD Director, Andrology Australia Principal Research Fellow,
The General Practice Education Day Healthed / Generation Next August 22 nd Sydney Update on Androgen Deficiency Robert I. McLachlan, FRACP, PhD Director, Andrology Australia Principal Research Fellow,
PRISM Bruges June Herman Leliefeld Urologist. The Netherlands
 PRISM Bruges 25-26 June 2015 Herman Leliefeld Urologist The Netherlands Guidelines EAU 2015: a rich source of Knowledge! Epidemiology/ Aetiology / Pathology Diagnostic evaluation Disease management Follow-Up
PRISM Bruges 25-26 June 2015 Herman Leliefeld Urologist The Netherlands Guidelines EAU 2015: a rich source of Knowledge! Epidemiology/ Aetiology / Pathology Diagnostic evaluation Disease management Follow-Up
TUE Application for Testosterone Physician Worksheet
 TUE Application for Testosterone Physician Worksheet Attention Physicians - USADA will not process Therapeutic Use Exemptions (TUE) for the use of testosterone unless all of the requirements for documentation
TUE Application for Testosterone Physician Worksheet Attention Physicians - USADA will not process Therapeutic Use Exemptions (TUE) for the use of testosterone unless all of the requirements for documentation
Clinical Policy: Implantable Hormone Pellets Reference Number: CA.CP.MP.507
 Clinical Policy: Reference Number: CA.CP.MP.507 Effective Date: 1/12 Last Review Date: 7/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CA.CP.MP.507 Effective Date: 1/12 Last Review Date: 7/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Over the past decade, androgen replacement
 J. Andrew Hoover, MD; Jeffrey T. Kirchner, DO, FAAFP Department of Family and Community Medicine, Lancaster General Hospital, Pa jhoover4@lghealth.org The authors reported no potential conflict of interest
J. Andrew Hoover, MD; Jeffrey T. Kirchner, DO, FAAFP Department of Family and Community Medicine, Lancaster General Hospital, Pa jhoover4@lghealth.org The authors reported no potential conflict of interest
Testosterone (cypionate, enanthate, and propionate) powder, Fluoxymesterone powder, Methyltestosterone powder
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.37 Subject: Testosterone Powder Page: 1 of 12 Last Review Date: November 30, 2018 Testosterone powder
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.37 Subject: Testosterone Powder Page: 1 of 12 Last Review Date: November 30, 2018 Testosterone powder
Sexual dysfunction of chronic kidney disease. Razieh salehian.md psychiatrist
 Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
Diagnosis and Clinical Evaluation of Hypogonadism in Adult Patients with Obesity and Diabetes
 Diagnosis and Clinical Evaluation of Hypogonadism in Adult Patients with Obesity and Diabetes Adrian Dobs, M.D., M.H.S. Professor of Medicine and Oncology The Johns Hopkins University School of Medicine
Diagnosis and Clinical Evaluation of Hypogonadism in Adult Patients with Obesity and Diabetes Adrian Dobs, M.D., M.H.S. Professor of Medicine and Oncology The Johns Hopkins University School of Medicine
GP guide to testosterone replacement therapy in men
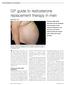 GP guide to testosterone replacement therapy in men SPL Mike Kirby FRCP Professor Mike Kirby describes how the diagnosis and treatment of test - osterone deficiency in primary care can lead to improved
GP guide to testosterone replacement therapy in men SPL Mike Kirby FRCP Professor Mike Kirby describes how the diagnosis and treatment of test - osterone deficiency in primary care can lead to improved
11: Androgen deficiency and replacement therapy in men
 11: Androgen deficiency and replacement therapy in men While androgen replacement therapy is essential and effective in overt deficiency, it is no anti-ageing elixir David J Handelsman and Jeffrey D Zajac
11: Androgen deficiency and replacement therapy in men While androgen replacement therapy is essential and effective in overt deficiency, it is no anti-ageing elixir David J Handelsman and Jeffrey D Zajac
Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234)
 Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland.
Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland.
Update on diagnosis and complications of adult and elderly male hypogonadism
 Hypoandrogenism in the elderly: to treat or not to treat? 12 th Italian AME Meeting; 6 th joint Meeting with AAC Bari november 10th Update on diagnosis and complications of adult and elderly male hypogonadism
Hypoandrogenism in the elderly: to treat or not to treat? 12 th Italian AME Meeting; 6 th joint Meeting with AAC Bari november 10th Update on diagnosis and complications of adult and elderly male hypogonadism
Testosterone (cypionate, enanthate, and propionate) powder, Fluoxymesterone powder, Methyltestosterone powder
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.08.37 Subject: Testosterone Powder Page: 1 of 11 Last Review Date: September 18, 2015 Testosterone powder
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.08.37 Subject: Testosterone Powder Page: 1 of 11 Last Review Date: September 18, 2015 Testosterone powder
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 2: Precocious Puberty. These podcasts are designed to give medical students an overview
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 2: Precocious Puberty. These podcasts are designed to give medical students an overview
Pulsatile gonadotrophin releasing hormone versus gonadotrophin treatment of hypothalamic hypogonadism in males
 Human Reproduction vol.8 Suppl.2 pp. 175-179, 1993 Pulsatile gonadotrophin releasing hormone versus gonadotrophin treatment of hypothalamic hypogonadism in males Jochen Schopohl Medizinische Klinik, Klinikum
Human Reproduction vol.8 Suppl.2 pp. 175-179, 1993 Pulsatile gonadotrophin releasing hormone versus gonadotrophin treatment of hypothalamic hypogonadism in males Jochen Schopohl Medizinische Klinik, Klinikum
Recognizing and Managing Testosterone Deficiency
 Recognizing and Managing Testosterone Deficiency J. Bruce Redmon, M.D. Professor Division of Endocrinology Departments of Medicine and Urologic Surgery Disclosure Information I have no financial relationships
Recognizing and Managing Testosterone Deficiency J. Bruce Redmon, M.D. Professor Division of Endocrinology Departments of Medicine and Urologic Surgery Disclosure Information I have no financial relationships
Recommendations on the diagnosis, treatment and monitoring of Testosterone deficiency (TD) in adult men
 Recommendations on the diagnosis, treatment and monitoring of Testosterone deficiency (TD) in adult men Bruno Lunenfeld, George Mskhalaya, Svetlana Kalinchenko, Yulia Tishova, Michael Zitzmann, Stefan
Recommendations on the diagnosis, treatment and monitoring of Testosterone deficiency (TD) in adult men Bruno Lunenfeld, George Mskhalaya, Svetlana Kalinchenko, Yulia Tishova, Michael Zitzmann, Stefan
Hypogonadism in Men. CME Away India & Sri Lanka March 23 - April 7, 2018
 Hypogonadism in Men CME Away India & Sri Lanka March 23 - April 7, 2018 Richard A. Bebb MD, ABIM, FRCPC Consultant Endocrinologist Medical Subspecialty Institute Cleveland Clinic Abu Dhabi Copyright 2017
Hypogonadism in Men CME Away India & Sri Lanka March 23 - April 7, 2018 Richard A. Bebb MD, ABIM, FRCPC Consultant Endocrinologist Medical Subspecialty Institute Cleveland Clinic Abu Dhabi Copyright 2017
Disclosures. Learning Objectives. Effects of Hormone Therapy on the Metabolic Syndrome and Cardiovascular Disease. None
 Effects of Hormone Therapy on the Metabolic Syndrome and Cardiovascular Disease Micol S. Rothman, MD Associate Professor of Medicine Endocrinology, Diabetes and Metabolism Clinical Director Metabolic Bone
Effects of Hormone Therapy on the Metabolic Syndrome and Cardiovascular Disease Micol S. Rothman, MD Associate Professor of Medicine Endocrinology, Diabetes and Metabolism Clinical Director Metabolic Bone
SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY
 1 SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL SEMINAR: SEX HORMONES PART 1 An Overview What are steroid hormones? Steroid
1 SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL SEMINAR: SEX HORMONES PART 1 An Overview What are steroid hormones? Steroid
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: Pellet (Testopel) Reference Number: CP.PHAR.354 Effective Date: 08.01.17 Last Review Date: 11.18 Line of Business: Medicaid Coding Implications Revision Log See Important Reminder at the
Clinical Policy: Pellet (Testopel) Reference Number: CP.PHAR.354 Effective Date: 08.01.17 Last Review Date: 11.18 Line of Business: Medicaid Coding Implications Revision Log See Important Reminder at the
Point-Counterpoint: Late Onset Hypogonadism (LOH)
 Point-Counterpoint: Late Onset Hypogonadism (LOH) We are Under-diagnosing and Treating Men with LOH LOH is a Non-existent Disease ~ Robert E. Donohue, MD Late Onset Hypogonadism LOH: underdx. & undertx
Point-Counterpoint: Late Onset Hypogonadism (LOH) We are Under-diagnosing and Treating Men with LOH LOH is a Non-existent Disease ~ Robert E. Donohue, MD Late Onset Hypogonadism LOH: underdx. & undertx
North of Tyne and Gateshead Area Prescribing Committee GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA
 North of Tyne and Gateshead Area Prescribing Committee GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA Information for Primary Care July 2014 (Minor update November 2014) (Review
North of Tyne and Gateshead Area Prescribing Committee GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA Information for Primary Care July 2014 (Minor update November 2014) (Review
MEN S HEALTH. Selected topics in. Erectile dysfunction Gynaecomastia Late-onset hypogonadism Delayed puberty in males
 Selected topics in MEN S HEALTH www.bpac.org.nz keyword: menshealth Erectile dysfunction Gynaecomastia Late-onset hypogonadism Delayed puberty in males 2 September 2010 best tests Erectile dysfunction
Selected topics in MEN S HEALTH www.bpac.org.nz keyword: menshealth Erectile dysfunction Gynaecomastia Late-onset hypogonadism Delayed puberty in males 2 September 2010 best tests Erectile dysfunction
An Idea Whose Time Has Come-Male Health Programs: An Opportunity For Clinical Expansion and Better Health
 An Idea Whose Time Has Come-Male Health Programs: An Opportunity For Clinical Expansion and Better Health KEVIN R. LOUGHLIN MD,MBA Harvard Medical School Boston, MA THE WEAKER SEX-MALES LIFE EXPECTANCY
An Idea Whose Time Has Come-Male Health Programs: An Opportunity For Clinical Expansion and Better Health KEVIN R. LOUGHLIN MD,MBA Harvard Medical School Boston, MA THE WEAKER SEX-MALES LIFE EXPECTANCY
Why is my body not changing? Conflicts of interest. Overview 11/9/2015. None
 Why is my body not changing? Murthy Korada Pediatrician, Pediatric Endocrinologist Ridge Meadows Hospital Surrey Memorial Hospital None Conflicts of interest Overview Overview of normal pubertal timing
Why is my body not changing? Murthy Korada Pediatrician, Pediatric Endocrinologist Ridge Meadows Hospital Surrey Memorial Hospital None Conflicts of interest Overview Overview of normal pubertal timing
Consent for Testosterone Therapy-Men Revised 4/10/18
 Consent for Testosterone Therapy in Men You have been diagnosed with or have an increased risk of having a hormone deficiency and your provider has recommended treatment with bio-identical hormone replacement
Consent for Testosterone Therapy in Men You have been diagnosed with or have an increased risk of having a hormone deficiency and your provider has recommended treatment with bio-identical hormone replacement
OBJECTIVES. Rebecca McEachern, MD. Puberty: Too early, Too Late or Just Right? Special Acknowledgements. Maryann Johnson M.Ed.
 1 Puberty: Too early, Too Late or Just Right? Maryann Johnson M.Ed., BSN, RN Special Acknowledgements Rebecca McEachern, MD OBJECTIVES Illustrate basic endocrine system and hormonal pathways Define the
1 Puberty: Too early, Too Late or Just Right? Maryann Johnson M.Ed., BSN, RN Special Acknowledgements Rebecca McEachern, MD OBJECTIVES Illustrate basic endocrine system and hormonal pathways Define the
Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018
 Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018 Learning Objectives At the conclusion of this lecture, learners should: 1) Know the various diagnostic
Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018 Learning Objectives At the conclusion of this lecture, learners should: 1) Know the various diagnostic
GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA. Information for Primary Care December 2015 (Review Date June 2016)
 GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA Information for Primary Care December 2015 (Review Date June 2016) Further information on this guideline can be obtained from: Claire
GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA Information for Primary Care December 2015 (Review Date June 2016) Further information on this guideline can be obtained from: Claire
Degarelix Subcutaneous Injection (Firmagon ) Treatment Guideline
 Mid Essex Locality Degarelix Subcutaneous Injection (Firmagon ) Treatment Guideline Contents FlowChart 2 Summary... 3 Key points... 3 Introduction... 3 Pharmacology... 3 Product information... 4 Place
Mid Essex Locality Degarelix Subcutaneous Injection (Firmagon ) Treatment Guideline Contents FlowChart 2 Summary... 3 Key points... 3 Introduction... 3 Pharmacology... 3 Product information... 4 Place
MALE INFERTILITY & SEMEN ANALYSIS
 MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
Puberty and Pubertal Disorders Part 3: Delayed Puberty
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 3: Delayed Puberty These podcasts are designed to give medical students an overview
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 3: Delayed Puberty These podcasts are designed to give medical students an overview
EAU Guidelines on Male Hypogonadism
 EAU Guidelines on Male Hypogonadism G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab European Association of Urology 2016 TABLE OF CONTENTS PAGE 1. INTRODUCTION 4 1.1 Aim 4
EAU Guidelines on Male Hypogonadism G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab European Association of Urology 2016 TABLE OF CONTENTS PAGE 1. INTRODUCTION 4 1.1 Aim 4
Low Testosterone Consultation Information
 T Low Testosterone Consultation Information www.urologyaustin.com Andropause or Male Menopause This syndrome has been nicknamed ADAM, which stands for androgen deficiency of the aging male. It differs
T Low Testosterone Consultation Information www.urologyaustin.com Andropause or Male Menopause This syndrome has been nicknamed ADAM, which stands for androgen deficiency of the aging male. It differs
 www.iffs-reproduction.org @IntFertilitySoc Int@FedFertilitySoc Conflict of interest none Outline Causes of ovulatory dysfunction Assessment of women with ovulatory dysfunction Management First line Second
www.iffs-reproduction.org @IntFertilitySoc Int@FedFertilitySoc Conflict of interest none Outline Causes of ovulatory dysfunction Assessment of women with ovulatory dysfunction Management First line Second
Western Locality Shared care information ~ Gonadorelin Analogues (Gnrh)
 Western Locality Shared care information ~ Gonadorelin Analogues (Gnrh) Specialist: Please complete the Shared Care letter sending a request to GP (see bottom of the page) April 2013 GP: Please indicate
Western Locality Shared care information ~ Gonadorelin Analogues (Gnrh) Specialist: Please complete the Shared Care letter sending a request to GP (see bottom of the page) April 2013 GP: Please indicate
