In Vitro Fertilization
|
|
|
- Beryl King
- 5 years ago
- Views:
Transcription
1 Patient Education In Vitro Fertilization About the treatment This handout describes how to prepare for and what to expect when you have in vitro fertilization. It provides written information about this treatment process, including risks, benefits, and alternatives. This material is in addition to the discussions you have with your doctors. It is important that you fully understand this information, so please read this information packet thoroughly and ask questions before signing consent forms. There are several steps involved in the in vitro fertilization (IVF) and embryo transfer process: Ovulation Induction: First, you will receive medicines to cause many eggs to grow and mature in your ovaries. Monitoring: You will have blood and ultrasound tests to monitor how you are responding to the medicines by measuring the growth of follicles (egg sacs) and rise in hormones. Triggering: After ovulation induction, another medicine is injected to prepare your follicles to mature and release eggs. Egg Retrieval: You will have an egg retrieval procedure using an ultrasound-guided needle technique, under either intravenous sedation or general anesthesia. Egg Fertilization and Selective Assisted Hatching: Your retrieved eggs will be prepared and fertilized in the laboratory using your partner s (or donor s) sperm. Embryo Transfer: Embryos (fertilized eggs that are beginning to grow but are still microscopic) that result from the fertilization procedure will be transferred back to your body. To do this, a catheter (tube) will be placed through your cervix (uterine, or womb, opening) into your uterus (womb). The embryos will be transferred through this catheter. After-Transfer Management: You may receive medicines to support implantation and early embryo growth.
2 Page 2 Ovulation Induction There are several possible medicines that may be used for developing follicles and maturing your eggs. Your (URC) doctor will discuss these choices with you. These medicines are given by injections that are either intramuscular (into the muscle) or subcutaneous (under the skin). It is important that you stay in close contact with your IVF team during the time you are receiving these medicines and for at least 2 weeks afterward. Monitoring While you are receiving the medicines to stimulate your ovaries, you will be closely monitored by your IVF team. This monitoring may be as often as every day. It will include venipuncture (blood draw) and transvaginal ultrasound exams. In a transvaginal ultrasound, the ultrasound probe (transducer) is placed in your vagina. The probe produces sound waves, which create pictures on a screen. If the monitoring shows that there is likely to be a low chance for successful egg retrieval, the induction cycle may be stopped and no egg retrieval will be done. On the other hand, if you are showing too much response to the induction medicines, they may be stopped and the cycle canceled to prevent the risks of overstimulation. Usually, both partners will be asked to take an oral antibiotic during the first part of the induction cycle. This is to reduce the chance that bacteria may be present in the samples collected during IVF. Triggering During cycle monitoring, your doctor will determine when your follicles are ready for the final steps of maturation. In this step, also called triggering ovulation, you will inject a medicine 36 hours before having the egg retrieval procedure. Egg Retrieval Your IVF team will choose a time they think is best for your egg retrieval procedure. For this procedure, you will go to Northwest Center for Reproductive Sciences, in Kirkland. UWMC has chosen this surgery center and embryology laboratory to provide some services for IVF patients. You will need to fill out separate paperwork to receive care at this center. The egg retrieval procedure is an ambulatory (day surgery) procedure. It is done using a transvaginal ultrasound-guided needle technique to aspirate (draw liquid up from) the egg follicles. You will need sedation and/or anesthesia during this procedure.
3 Page 3 In rare cases, these anesthetic medicines may involve risks to your organs. Your position during anesthesia may cause short-term or permanent nerve damage. You will be closely monitored by an anesthesia team during the egg retrieval procedure to minimize these risks. If your IVF team determines you should not have standard anesthesia, other forms of anesthesia may be used. Guided by ultrasound, your doctor will insert a needle through your vaginal wall and into your ovary. The fluid inside your ovary will be drawn out through the needle. This fluid will be analyzed under the microscope to locate the eggs. The fluid from as many follicles as possible will be drawn out to search for an egg. For a few women, it is not possible to reach the ovaries through their vagina. For these patients, laparoscopy or another abdominal procedure is needed to do the egg retrieval. In laparoscopy, a thin, lighted tube (laparoscope) is used to see inside your body and reach the ovaries from the abdomen. If you need a different procedure, your IVF doctor will talk with you about it before your egg retrieval. During the egg retrieval, other procedures may be done to make the embryo transfer easier. These may include placing a traction suture (stitch) on your cervix to help straighten the canal around the cervix. Your IVF team will decide whether you will need any of these procedures by doing a mock transfer before your IVF cycle begins. In a mock transfer, your doctor will insert a soft catheter into your uterus to mimic the actual embryo transfer. By doing this, potential difficulties can be discovered beforehand. Egg Fertilization Sperm from your male partner (or donor) before the egg retrieval are used to fertilize your retrieved eggs. In some cases, sperm may also be collected before the day of egg retrieval to use as back-up. This sample will be frozen in a process called cryopreservation. After your egg retrieval, your eggs will be evaluated and prepared for the fertilization process by an embryologist. An embryologist specializes in the growth and development of embryos. Fertilization may be tried in 1 of 2 ways: Insemination: The eggs are placed in a culture dish and are exposed to sperm that have been washed and processed. Intra-Cytoplasmic Sperm Injection (ICSI): A single sperm is directly injected into each egg. ICSI is more complicated than insemination and is more costly. It may be used when the chances of normal fertilization by the insemination method appear low. If you need ICSI, you will be given a separate information handout and your IVF doctor will talk with you about it.
4 Page 4 Your IVF team will decide whether you need insemination or ICSI, based on sperm and egg quantity or quality. They can answer your questions about this decision. Selective Assisted Hatching Your IVF team, along with staff from the Northwest Center for Reproductive Sciences, will evaluate your embryos with a microscope to decide whether selective assisted hatching should be done with any of them. This procedure is often done to help the embryo grow. The decision to do this procedure is based on the appearance of each embryo, the age of the female partner, and the female s medical history. You will be given a separate information handout and your IVF doctor will talk with you about it. Embryo Transfer About 3 to 5 days after egg retrieval, several of the embryos that develop will be transferred to the inside of your womb using a catheter passed through your cervix. There is no guarantee that any of the transferred embryos will result in pregnancy. Your IVF team will decide how many embryos to transfer, based on guidelines that take into account your age, embryo quality, and other medical factors. The number they choose will allow for both the best chance of pregnancy and the lowest chance of multiple gestation (being pregnant with more than 1 baby at the same time). You will be given a separate information handout from the American Society for Reproductive Medicine titled, Guidelines on number of embryos transferred. Your IVF doctor will also talk with you about it. Some embryos may be cryopreserved as cleavage-stage embryos (day 2 to 4) or blastocysts (day 5 to 7) for possible use in a later IVF cycle. There are more steps and costs that are needed for embryo cryopreservation. You will be given a separate information handout about this if it is being considered, and your IVF team will talk with you about it. After-Transfer Management To increase the chances of successful implantation (attachment of the embryo(s) to the wall of the uterus to achieve pregnancy), you may be given the hormone progesterone. This will be given either by intramuscular injection, vaginal suppository, or vaginal pills. Usually, the progesterone is continued until pregnancy is confirmed by ultrasound, and it may even be continued for several weeks in early pregnancy. During that time, you may need to have hormonal evaluations as instructed by your IVF team.
5 Page 5 Discarded Material After the IVF treatment, there may be unused biological material (tissue), including sperm, immature or unfertilized eggs, and abnormal or arrested preembryos (embryos that have stopped developing). These unused materials will be: Discarded OR Used for training purposes or in research for the advancement of medical science If the material is used for training or research, no new embryos or pregnancies will be created. To protect patient privacy, all information that links you and your partner or donor to the biological material will be removed before the materials are used for training or research. Please tell us if at any time you decide that you do not want to have unused tissues used in this way. Your decision will not have any effect on your participation in IVF treatment. What are the options for extra embryos created from IVF? If your IVF procedure results in too many embryos (more than the number selected for transfer), the extra ones may be cryopreserved, depending on their quality. To lower the risk of damaging these embryos during transport, they will be cryopreserved and stored at the embryology lab for the first few months after your IVF. For long-term storage, the embryos will be moved to a commercial cryobank facility. That facility will assume and handle all responsibilities related to maintaining your embryos. You will be given a separate information handout about this if it is being considered, and your IVF team will talk with you about it. What are the benefits of IVF? You might receive the following benefits from this treatment: Pregnancy Additional embryos may be cryopreserved for your future familybuilding URC doctors and staff cannot guarantee that any of the steps in the process will succeed, that the treatment process will result in pregnancy, or that the pregnancy will result in delivery of a healthy full-term newborn. Only you can decide if the possible benefits of having IVF are worth the risks.
6 Page 6 What are the possible risks and complications from this treatment? Ovulation induction medicines are given by intramuscular or subcutaneous injections. This may cause bruising and discomfort at the injection site. Ovulation induction medicines have some common side effects: - Lupron: fatigue, muscle and joint pain, and short-term menopause-like symptoms (headaches, hot flashes, mood swings, sweats, insomnia, fatigue, etc.). - Clomiphene citrate: hot flashes, abdominal distention, bloating, headache, and changes in vision. - Letrozole: hot flashes, dizziness, headaches, mild fluid retention, nausea and changes in bowel habits, joint and muscle pain, and fatigue. (Using this medicine for ovulation induction is called off-label use, which means this drug was not originally approved for this purpose, but it is legal to prescribe it for this use.) - Gonadotropins (such as Repronex, Menopur, Gonal-f, Follistim, Bravelle, Luveris): headache, breast pain, nausea and changes in bowel habits, abdominal pain, injection site reactions, and overstimulated ovaries that can lead to ovarian hyperstimulation syndrome or OHSS, a condition that causes the ovaries to become swollen, which may result in fluid shifts in your body. (Please see the separate information handout on OHSS.) - Human chorionic gonadotropin (Novarel, Ovidrel): injection site reactions and OHSS. - Progesterone: injection site reactions, breast pain, nausea, bloating, constipation. - Antibiotics: vaginal yeast infections, nausea, or abdominal pain. - Oral steroids: long-term use may lead to osteoporosis and greater risk of getting infections; in short-term use (as for IVF), very few side effects are expected. Also, some studies suggest that fertility medicines may increase the risk of developing ovarian cancer. While you are receiving the ovulation induction medicines described above, you may need to have blood drawn as often as every day. There is a risk of mild discomfort and bruising at the venipuncture site. Transvaginal ultrasound exams also may cause some discomfort, but there is no known medical risk from these.
7 Page 7 Questions? Call Your questions are important. Call your doctor or other UWMC health care provider if you have questions or concerns. University Reproductive Care: Website: edu/obgyn/urc/index. shtm Box Roosevelt Way N.E. 3rd Floor, Women s Health Care Center Seattle, WA Risks related to the egg retrieval procedure include: - Infection - Bleeding - Rarely, injury to other abdominal and pelvic organs If you develop an infection, you may need to be admitted to the hospital to receive IV antibiotics. If you develop vaginal bleeding, your doctor may need to stitch the site where the ultrasound-guided needle entered. In rare cases, if the bleeding is internal (in your ovary, uterus, or a blood vessel in your pelvis), or if your doctor suspects other organs have been injured, you may need to be admitted to the hospital. In the hospital, you will be monitored and may need a blood transfusion, and/or a laparoscopy or laparotomy (abdominal surgery) to stop the bleeding and repair the injury. The embryo transfer procedure may cause some cramping, discomfort, and possibly a small amount of bleeding. Rarely, infection occurs where the catheter was inserted. This may require antibiotic treatment. A higher number and quality of embryos transferred to the womb may lead to a higher chance of success with IVF. But, IVF in general puts you at higher risk for multiple gestation, and this risk is higher when more embryos are transferred. The risks of multiple gestation include: - Premature labor - The delivery of premature infants who need intensive care and could have long-term complications from being born prematurely Premature labor and delivery may also place the mother at greater risk for Cesarean section, bleeding, and infection. Sometimes, the IVF team may decide to cancel egg collection shortly before it is to take place. This is done when it looks like too few eggs will be recovered, when there are no live sperm found, or for other medical reasons. What are the alternatives to this treatment? You may decide not to have IVF treatment. You may decide to continue other fertility treatments, such as ovulation induction and intrauterine insemination. Other options include adoption or remaining childless. University of Washington Medical Center 07/2010 Reprints on Health Online:
In Vitro Fertilization What to expect
 Patient Education In Vitro Fertilization What to expect This handout describes how to prepare for and what to expect when you have in vitro fertilization. It provides written information about this process,
Patient Education In Vitro Fertilization What to expect This handout describes how to prepare for and what to expect when you have in vitro fertilization. It provides written information about this process,
UW MEDICINE PATIENT EDUCATION. In Vitro Fertilization How to prepare and what to expect DRAFT
 UW MEDICINE PATIENT EDUCATION In Vitro Fertilization How to prepare and what to expect This handout tells how to prepare for and what to expect when you go through a cycle of in vitro fertilization. It
UW MEDICINE PATIENT EDUCATION In Vitro Fertilization How to prepare and what to expect This handout tells how to prepare for and what to expect when you go through a cycle of in vitro fertilization. It
Patient Information: Patient Name: Date of Birth:
 Weill Cornell Medicine Ronald O. Perelman and Claudia Cohen Center for Reproductive Medicine Informed Consent for Oocyte (Egg) Cryopreservation Patient Information: Part 1: I have requested to be treated
Weill Cornell Medicine Ronald O. Perelman and Claudia Cohen Center for Reproductive Medicine Informed Consent for Oocyte (Egg) Cryopreservation Patient Information: Part 1: I have requested to be treated
A new set of consent documents is required for each IVF attempt. CRM staff is available to answer your questions related to the consent documents.
 Informed Consent Packet - In Vitro Fertilization (IVF) This packet contains the required IVF treatment consent documents. Please read, consider and, if you agree, sign and return the attached documents.
Informed Consent Packet - In Vitro Fertilization (IVF) This packet contains the required IVF treatment consent documents. Please read, consider and, if you agree, sign and return the attached documents.
WOMEN & INFANTS HOSPITAL Providence, RI CONSENT FOR IVF WITH EMBRYO TRANSFER
 *40639* 40639 WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR IVF WITH EMBRYO TRANSFER I have requested treatment by the physicians and (Print Patient s name) staff of the Women & Infants Fertility
*40639* 40639 WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR IVF WITH EMBRYO TRANSFER I have requested treatment by the physicians and (Print Patient s name) staff of the Women & Infants Fertility
WOMEN & INFANTS HOSPITAL Providence, RI CONSENT FOR IN VITRO FERTILIZATION USING A GESTATIONAL CARRIER (PATIENT/INTENDED PARENTS) 1.
 *40675* 40675 MR-838 (9-2017) WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR IN VITRO FERTILIZATION USING A GESTATIONAL CARRIER (PATIENT/INTENDED PARENTS) 1. I, and (Print Patient s name) (Print
*40675* 40675 MR-838 (9-2017) WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR IN VITRO FERTILIZATION USING A GESTATIONAL CARRIER (PATIENT/INTENDED PARENTS) 1. I, and (Print Patient s name) (Print
WOMEN & INFANTS HOSPITAL Providence, RI CONSENT FOR THAWING AND TRANSFER OF CRYOPRESERVED EMBRYOS. I and
 *40668* 40668 WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR THAWING AND TRANSFER OF CRYOPRESERVED EMBRYOS FOR inpatients: affix patient label OR I and (Print Patient s name) (Print Partner
*40668* 40668 WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR THAWING AND TRANSFER OF CRYOPRESERVED EMBRYOS FOR inpatients: affix patient label OR I and (Print Patient s name) (Print Partner
I. ART PROCEDURES. A. In Vitro Fertilization (IVF)
 DFW Fertility Associates ASSISTED REPRODUCTIVE TECHNOLOGY (ART) Welcome to DFW Fertility Associates/ Presbyterian-Harris Methodist Hospital ARTS program. This document provides an overview of treatment
DFW Fertility Associates ASSISTED REPRODUCTIVE TECHNOLOGY (ART) Welcome to DFW Fertility Associates/ Presbyterian-Harris Methodist Hospital ARTS program. This document provides an overview of treatment
IVF Patient Information
 What is IVF? IVF (In Vitro Fertilisation) is a treatment by which fertilisation of eggs by sperm takes place outside the body in a dish in an IVF laboratory. An ovary has a pool of immature eggs. In a
What is IVF? IVF (In Vitro Fertilisation) is a treatment by which fertilisation of eggs by sperm takes place outside the body in a dish in an IVF laboratory. An ovary has a pool of immature eggs. In a
Information Booklet. Exploring the causes of infertility and treatment options.
 Information Booklet Exploring the causes of infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Faith is taking the first step even if you don t see the whole
Information Booklet Exploring the causes of infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Faith is taking the first step even if you don t see the whole
Treating Infertility
 Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
Puerto Rico Fertility Center
 Puerto Rico Fertility Center General Information of the In-Vitro Fertilization Program Dr. Pedro J. Beauchamp First test-tube baby IN PUERTO RICO Dr. Pedro Beauchamp with Adlin Román in his arms. Paseo
Puerto Rico Fertility Center General Information of the In-Vitro Fertilization Program Dr. Pedro J. Beauchamp First test-tube baby IN PUERTO RICO Dr. Pedro Beauchamp with Adlin Román in his arms. Paseo
Egg Freezing. Information for Patients and Partners. Date of Issue:28/08/15 Doc 327 Issue 08 1 of 11 Approved by Jane Blower
 Egg Freezing Information for Patients and Partners Date of Issue:28/08/15 Doc 327 Issue 08 1 of 11 What is this service and who is it for? This treatment is for two groups of patients. You may be about
Egg Freezing Information for Patients and Partners Date of Issue:28/08/15 Doc 327 Issue 08 1 of 11 What is this service and who is it for? This treatment is for two groups of patients. You may be about
Informed Consent for Transfer of Embryos from Thawed Oocytes (FOT) Patient Information: Patient Name: Date of Birth:
 Informed Consent for Transfer of Embryos from Thawed Oocytes (FOT) I/We have requested treatment from the (CRM) to use my frozen oocytes (eggs) for the purposes of achieving a pregnancy. I/We understand
Informed Consent for Transfer of Embryos from Thawed Oocytes (FOT) I/We have requested treatment from the (CRM) to use my frozen oocytes (eggs) for the purposes of achieving a pregnancy. I/We understand
Embryo Selection after IVF
 Embryo Selection after IVF Embryo Selection after IVF Many of human embryos produced after in vitro fertilization carry abnormal chromosomes. Placing a chromosomally normal embryo (s) into a normal uterus
Embryo Selection after IVF Embryo Selection after IVF Many of human embryos produced after in vitro fertilization carry abnormal chromosomes. Placing a chromosomally normal embryo (s) into a normal uterus
Fertility care for women diagnosed with cancer
 Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Fertility care for women diagnosed with cancer Contents Page Overview... 2 Our service... 2 Effects of cancer treatment
Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Fertility care for women diagnosed with cancer Contents Page Overview... 2 Our service... 2 Effects of cancer treatment
Produce Eggs. Fertility Preservation for Trans People who. LGBTQ Reproductive Options
 for Trans People who Produce Eggs LGBTQ Reproductive Options Many trans people are interested in being parents and want to know their options. While many trans people may conceive on their own, this info
for Trans People who Produce Eggs LGBTQ Reproductive Options Many trans people are interested in being parents and want to know their options. While many trans people may conceive on their own, this info
A guide to In Vitro Fertilisation (IVF)
 A guide to In Vitro Fertilisation (IVF) Introducing Fertility Plus What is IVF? Fertility Plus is a leading fertility clinic based in Harley Street, dedicated to offering couples and individuals the best
A guide to In Vitro Fertilisation (IVF) Introducing Fertility Plus What is IVF? Fertility Plus is a leading fertility clinic based in Harley Street, dedicated to offering couples and individuals the best
CONSENT FORM FOR TREATMENT WITH OVULATION INDUCTION MEDICATIONS AND INTRAUTERINE INSEMINATIONS
 CONSENT FORM FOR TREATMENT WITH OVULATION INDUCTION MEDICATIONS AND INTRAUTERINE INSEMINATIONS INSTRUCTIONS: This consent form provides a description of the treatment that you are undertaking. Read the
CONSENT FORM FOR TREATMENT WITH OVULATION INDUCTION MEDICATIONS AND INTRAUTERINE INSEMINATIONS INSTRUCTIONS: This consent form provides a description of the treatment that you are undertaking. Read the
Adoption and Foster Care
 GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
Genetics Review and Reproductive Options in Kennedy Disease
 + Alice Schindler, MS, CGC Genetic Counselor, NIH/NINDS/Neurogenetics Branch Heather Montie, PhD, Assistant Professor Department of Bio-Medical Sciences Philadelphia College of Osteopathic Medicine Annual
+ Alice Schindler, MS, CGC Genetic Counselor, NIH/NINDS/Neurogenetics Branch Heather Montie, PhD, Assistant Professor Department of Bio-Medical Sciences Philadelphia College of Osteopathic Medicine Annual
INDICATIONS OF IVF/ICSI
 PROCESS OF IVF/ICSI INDICATIONS OF IVF/ICSI IVF is most clearly indicated when infertility results from one or more causes having no other effective treatment; Tubal disease. In women with blocked fallopian
PROCESS OF IVF/ICSI INDICATIONS OF IVF/ICSI IVF is most clearly indicated when infertility results from one or more causes having no other effective treatment; Tubal disease. In women with blocked fallopian
Welcome. Fertility treatment can be complicated. What s included. Your fertility treatment journey begins here. Fertility treatment basics 2
 Welcome Your fertility treatment journey begins here Fertility treatment can be complicated Managing expectations, keeping track of medications and appointments, remembering all the information your physician
Welcome Your fertility treatment journey begins here Fertility treatment can be complicated Managing expectations, keeping track of medications and appointments, remembering all the information your physician
Infertility F REQUENTLY A SKED Q UESTIONS. Q: Is infertility a common problem?
 Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Information for Patients and Partners
 In Vitro Fertilisation (IVF) & Intra-Cytoplasmic Sperm Injection (ICSI) Information for Patients and Partners Date of Issue:14.09.15 Doc 389 Issue 10 1 of 14 What is this leaflet about and who is it for?
In Vitro Fertilisation (IVF) & Intra-Cytoplasmic Sperm Injection (ICSI) Information for Patients and Partners Date of Issue:14.09.15 Doc 389 Issue 10 1 of 14 What is this leaflet about and who is it for?
Arizona Reproductive Medicine Specialists. Assisted Reproductive Technology. Patient Guide
 Arizona Reproductive Medicine Specialists Assisted Reproductive Technology Patient Guide Welcome All of us at Arizona Reproductive Medicine Specialists are pleased to welcome you to our program. We know
Arizona Reproductive Medicine Specialists Assisted Reproductive Technology Patient Guide Welcome All of us at Arizona Reproductive Medicine Specialists are pleased to welcome you to our program. We know
Intra uterine insemination (IUI) Information for Patients and Partners
 Intra uterine insemination (IUI) Information for Patients and Partners What is this leaflet about and who is it for? This leaflet is produced to inform couples undergoing IUI (intrauterine insemination)
Intra uterine insemination (IUI) Information for Patients and Partners What is this leaflet about and who is it for? This leaflet is produced to inform couples undergoing IUI (intrauterine insemination)
H. Christina Lee, M.D., J.D., H.C.L.D., F.A.C.O.G. 95 Highland Avenue, #100 Telephone (610) Bethlehem, PA Fax (610)
 Overview CONSENT TO TREATMENT WITH ASSISTED REPRODUCTIVE TECHNOLOGIES Assisted reproductive technology (ART) The Centers for Disease Control and Prevention (CDC) defines ART to include "all fertility treatments
Overview CONSENT TO TREATMENT WITH ASSISTED REPRODUCTIVE TECHNOLOGIES Assisted reproductive technology (ART) The Centers for Disease Control and Prevention (CDC) defines ART to include "all fertility treatments
Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur?
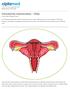 Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Patient Overview: Invitro Fertilisation
 Patient Overview: Overview IVF stands for in-vitro fertilisation i.e. literally fertilisation in a glass dish. You may also hear the term ART used which stands for Assisted Reproductive Technologies. IVF
Patient Overview: Overview IVF stands for in-vitro fertilisation i.e. literally fertilisation in a glass dish. You may also hear the term ART used which stands for Assisted Reproductive Technologies. IVF
CONSENT TO TREATMENT WITH ASSISTED REPRODUCTIVE TECHNOLOGIES
 Overview Assisted reproductive technology (ART) The Centers for Disease Control and Prevention (CDC) defines ART to include "all fertility treatments in which both eggs and sperm are handled. In general,
Overview Assisted reproductive technology (ART) The Centers for Disease Control and Prevention (CDC) defines ART to include "all fertility treatments in which both eggs and sperm are handled. In general,
Fertility, Egg Freezing, and You. If you have questions, we can help you get answers.
 Fertility, Egg Freezing, and You If you have questions, we can help you get answers. Let s talk about fertility If you re thinking about having a baby someday but aren t ready now, you should learn all
Fertility, Egg Freezing, and You If you have questions, we can help you get answers. Let s talk about fertility If you re thinking about having a baby someday but aren t ready now, you should learn all
CONSENT TO TREATMENT WITH ASSISTED REPRODUCTIVE TECHNOLOGIES
 Overview Assisted reproductive technology (ART) The Centers for Disease Control and Prevention (CDC) defines ART to include "all fertility treatments in which eggs or embryos are handled. In general, ART
Overview Assisted reproductive technology (ART) The Centers for Disease Control and Prevention (CDC) defines ART to include "all fertility treatments in which eggs or embryos are handled. In general, ART
Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition
 Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition Patient Name (please print) Patient DOB (MM/DD/YYYY) Patient eivf number Partner
Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition Patient Name (please print) Patient DOB (MM/DD/YYYY) Patient eivf number Partner
Infertility treatment
 In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
CONSENT FORM FOR A COUPLE USING A GESTATIONAL CARRIER
 CONSENT FORM FOR A COUPLE USING A GESTATIONAL CARRIER INSTRUCTIONS: This consent form provides a description of the treatment that you are undertaking. Read the consent completely. If you have any questions
CONSENT FORM FOR A COUPLE USING A GESTATIONAL CARRIER INSTRUCTIONS: This consent form provides a description of the treatment that you are undertaking. Read the consent completely. If you have any questions
Oocyte Cryopreservation Process, Risk, and Consent
 Oocyte Cryopreservation Process, Risk, and Consent While embryos and sperm have been frozen and thawed with good results for many years, eggs have proved much more difficult to manage. Newer egg freezing
Oocyte Cryopreservation Process, Risk, and Consent While embryos and sperm have been frozen and thawed with good results for many years, eggs have proved much more difficult to manage. Newer egg freezing
Brighton & Hove CCG PLS CONFERENCE Dr Carole Gilling-Smith Medical Director
 Brighton & Hove CCG PLS CONFERENCE 2016 Dr Carole Gilling-Smith Medical Director FERTILITY CHALLENGES IN THE NHS A TERTIARY CARE PERSPECTIVE LEARNING OBJECTIVES Understand the pathways through assisted
Brighton & Hove CCG PLS CONFERENCE 2016 Dr Carole Gilling-Smith Medical Director FERTILITY CHALLENGES IN THE NHS A TERTIARY CARE PERSPECTIVE LEARNING OBJECTIVES Understand the pathways through assisted
Acute Salpingitis. Fallopian Tubes. Uterus
 Acute Salpingitis Introduction Acute salpingitis is a type of infection that affects the Fallopian tubes. The Fallopian tubes carry eggs from the ovaries to the uterus. Acute salpingitis is one of the
Acute Salpingitis Introduction Acute salpingitis is a type of infection that affects the Fallopian tubes. The Fallopian tubes carry eggs from the ovaries to the uterus. Acute salpingitis is one of the
Palm Beach Obstetrics & Gynecology, PA
 Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Endometriosis The lining of the uterus is
Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Endometriosis The lining of the uterus is
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Planning for Parenthood After a Cancer Diagnosis
 Cancer and Fertility Planning for Parenthood After a Cancer Diagnosis If you or someone you love is facing cancer, preserving fertility may be the last thing on your mind. But if you re a woman of childbearing
Cancer and Fertility Planning for Parenthood After a Cancer Diagnosis If you or someone you love is facing cancer, preserving fertility may be the last thing on your mind. But if you re a woman of childbearing
Introduction to CRM. Ronald O. Perelman and Claudia Cohen Center for Reproductive Medicine - CRM
 Introduction to CRM Ronald O. Perelman and Claudia Cohen Center for Reproductive Medicine - CRM 1 CRM Locations Upper East Side (Main Office) 1305 York Avenue, 6 th Floor New York, NY 10021 *open 7 days
Introduction to CRM Ronald O. Perelman and Claudia Cohen Center for Reproductive Medicine - CRM 1 CRM Locations Upper East Side (Main Office) 1305 York Avenue, 6 th Floor New York, NY 10021 *open 7 days
CHR CENTER FOR HUMAN REPRODUCTION Informed Consent for the Performance of In Vitro Fertilization (IVF) and Related Procedures
 Patient Name:. Social Security #: Partner Name: Social Security #: CHR CENTER FOR HUMAN REPRODUCTION Informed Consent for the Performance of In Vitro Fertilization (IVF) and Related Procedures We have
Patient Name:. Social Security #: Partner Name: Social Security #: CHR CENTER FOR HUMAN REPRODUCTION Informed Consent for the Performance of In Vitro Fertilization (IVF) and Related Procedures We have
Informed Consent for Assisted Reproduction: In Vitro Fertilization, Intracytoplasmic Sperm Injection (ICSI), Assisted Hatching, and Embryo Freezing
 Patient: Print Name Partner: Account #: Print Name Informed Consent for Assisted Reproduction: In Vitro Fertilization, Intracytoplasmic Sperm Injection (ICSI), Assisted Hatching, and Embryo Freezing OVERVIEW
Patient: Print Name Partner: Account #: Print Name Informed Consent for Assisted Reproduction: In Vitro Fertilization, Intracytoplasmic Sperm Injection (ICSI), Assisted Hatching, and Embryo Freezing OVERVIEW
IVF Treatment Plan & Consents
 Seth Levrant MD PC, Partners in Reproductive Health. www.myivfbaby.com Page 1 of 24 IVF Treatment Plan & Consents Patient name: Date: Spouse / partner name: for IVF when? Provider of Eggs (oocytes) and
Seth Levrant MD PC, Partners in Reproductive Health. www.myivfbaby.com Page 1 of 24 IVF Treatment Plan & Consents Patient name: Date: Spouse / partner name: for IVF when? Provider of Eggs (oocytes) and
Fact Sheet. Quick guide to infertility and treatment options
 Fact Sheet Quick guide to infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Ovarian Hyper stimulation syndrome OHSS is a potentially life threatening complication
Fact Sheet Quick guide to infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Ovarian Hyper stimulation syndrome OHSS is a potentially life threatening complication
Informed Consent for Assisted Reproduction: In Vitro Fertilization,
 Informed Consent for Assisted Reproduction: In Vitro Fertilization, Intracytoplasmic Sperm Injection, Assisted Hatching, Sperm and Embryo Cryopreservation Please place your initials below to acknowledge
Informed Consent for Assisted Reproduction: In Vitro Fertilization, Intracytoplasmic Sperm Injection, Assisted Hatching, Sperm and Embryo Cryopreservation Please place your initials below to acknowledge
The facts about egg freezing
 The facts about egg freezing 1800 111 483 qfg.com.au Who might benefit from egg freezing? Age-related infertility in women is one of the most common issues presented to fertility specialists each day when
The facts about egg freezing 1800 111 483 qfg.com.au Who might benefit from egg freezing? Age-related infertility in women is one of the most common issues presented to fertility specialists each day when
Cycle Plan Page1 CYCLE PLAN TYPE CYCLE TYPE: Initial Plan Updated Plan Management Team Review Monitoring Review
 Cycle Plan Page1 CYCLE PLAN TYPE Initial Plan Updated Plan Management Team Review Monitoring Review CYCLE TYPE: Undecided - diagnostic testing only Natural Cycle Coitus with IUI Ovulation Induction CC
Cycle Plan Page1 CYCLE PLAN TYPE Initial Plan Updated Plan Management Team Review Monitoring Review CYCLE TYPE: Undecided - diagnostic testing only Natural Cycle Coitus with IUI Ovulation Induction CC
THE WONDERFUL WORLD OF IVF-
 THE WONDERFUL WORLD OF IVF- What is IVF? A. In-Vitro Fertilization & Embryo Transfer IVF is a process by which one of more eggs (oocytes) are removed from the ovaries by a Non-surgical needle aspiration
THE WONDERFUL WORLD OF IVF- What is IVF? A. In-Vitro Fertilization & Embryo Transfer IVF is a process by which one of more eggs (oocytes) are removed from the ovaries by a Non-surgical needle aspiration
Informed Consent for Assisted Reproduction: In Vitro Fertilization, Intracytoplasmic Sperm Injection, Assisted Hatching, Embryo Cryopreservation
 Page 1 of 24 Informed Consent for ART, Seth Levrant MD PC, Partners in Reproductive Health, version may2013 Informed Consent for Assisted Reproduction: In Vitro Fertilization, Intracytoplasmic Sperm Injection,
Page 1 of 24 Informed Consent for ART, Seth Levrant MD PC, Partners in Reproductive Health, version may2013 Informed Consent for Assisted Reproduction: In Vitro Fertilization, Intracytoplasmic Sperm Injection,
Introduction to Intrauterine Insemination (IUI) Service
 Introduction to Intrauterine Insemination (IUI) Service Assisted Reproductive Technology Unit The Chinese University of Hong Kong Prince of Wales Hospital 2017 Treatment Procedures IUI involves six main
Introduction to Intrauterine Insemination (IUI) Service Assisted Reproductive Technology Unit The Chinese University of Hong Kong Prince of Wales Hospital 2017 Treatment Procedures IUI involves six main
Infertility. F r e q u e n t l y A s k e d Q u e s t i o n s. Q: What causes infertility in men? A: Infertility in men is most often caused by:
 Infertility Q: What is infertility? A: Infertility means not being able to get pregnant after one year of trying. Or, six months, if a woman is 35 or older. Women who can get pregnant but are unable to
Infertility Q: What is infertility? A: Infertility means not being able to get pregnant after one year of trying. Or, six months, if a woman is 35 or older. Women who can get pregnant but are unable to
Partner Name: Patient Signature Partner Signature (If applicable) Date (COS/IUI) Witness Name Witness Signature Date
 1. Please place your initials below to indicate which components of controlled ovarian Stimulation (COS) and intrauterine insemination (IUI) treatment you agree to undertake in your upcoming treatment
1. Please place your initials below to indicate which components of controlled ovarian Stimulation (COS) and intrauterine insemination (IUI) treatment you agree to undertake in your upcoming treatment
This Booklet is provided by The New Hope Center for Reproductive Medicine. TSPoe
 This Booklet is provided by The New Hope Center for Reproductive Medicine TSPoe Page 1 of 20 Booklet-ART Procedures Jan-2017 Assisted Reproductive Techniques: In Vitro Fertilization, Intracytoplasmic Sperm
This Booklet is provided by The New Hope Center for Reproductive Medicine TSPoe Page 1 of 20 Booklet-ART Procedures Jan-2017 Assisted Reproductive Techniques: In Vitro Fertilization, Intracytoplasmic Sperm
Assisted Reproduction. By Dr. Afraa Mahjoob Al-Naddawi
 Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
PROCEDURES LAPAROSCOPY
 PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
Schedule of Fees for Private Treatment
 Schedule of Fees for Private Treatment Fertility Treatment is personalized to each individual and couple, based on diagnosis and best treatment options. At Fertility Plus, we are mindful of the costs involved
Schedule of Fees for Private Treatment Fertility Treatment is personalized to each individual and couple, based on diagnosis and best treatment options. At Fertility Plus, we are mindful of the costs involved
Realizing dreams booklet.indd 1 5/20/ :26:52 AM
 Realizing dreams. 18891booklet.indd 1 5/20/2010 11:26:52 AM The Journey To Parenthood The first Gator Baby was born in 1988 through the in vitro fertilization program at the University of Florida. Since
Realizing dreams. 18891booklet.indd 1 5/20/2010 11:26:52 AM The Journey To Parenthood The first Gator Baby was born in 1988 through the in vitro fertilization program at the University of Florida. Since
UTERINE LEIOMYOSARCOMA. About Uterine leiomyosarcoma
 UTERINE LEIOMYOSARCOMA Uterine Lms, Ulms Or Just Lms Rare uterine malignant tumour that arises from the smooth muscular part of the uterine wall. Diagnosis Female About Uterine leiomyosarcoma Uterine LMS
UTERINE LEIOMYOSARCOMA Uterine Lms, Ulms Or Just Lms Rare uterine malignant tumour that arises from the smooth muscular part of the uterine wall. Diagnosis Female About Uterine leiomyosarcoma Uterine LMS
Fertility 101. About SCRC. A Primary Care Approach to Diagnosing and Treating Infertility. Definition of Infertility. Dr.
 Dr. Shahin Ghadir A Primary Care Approach to Diagnosing and Treating Infertility St. Charles Bend Grand Rounds November 30, 2018 I have no conflicts of interest to disclose. + About SCRC State-of-the-art
Dr. Shahin Ghadir A Primary Care Approach to Diagnosing and Treating Infertility St. Charles Bend Grand Rounds November 30, 2018 I have no conflicts of interest to disclose. + About SCRC State-of-the-art
X-Plain Ovarian Cancer Reference Summary
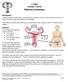 X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
Consent for In Vitro Fertilization/Assisted Reproduction
 Consent for In Vitro Fertilization/Assisted Reproduction I / we, and, desire to participate in the Assisted Reproduction Program at The A.R.T. Institute of Washington, Inc. at Walter Reed National Military
Consent for In Vitro Fertilization/Assisted Reproduction I / we, and, desire to participate in the Assisted Reproduction Program at The A.R.T. Institute of Washington, Inc. at Walter Reed National Military
THE CENTER FOR HUMAN REPRODUCTION (CHR)
 PATIENT NAME: RECORD #: THE CENTER FOR HUMAN REPRODUCTION (CHR) 21 East 69 th Street, New York, NY 10021 T: 212-994-4400; F: 212-994-4499 Informed Consent for Assisted Reproduction: In Vitro Fertilization,
PATIENT NAME: RECORD #: THE CENTER FOR HUMAN REPRODUCTION (CHR) 21 East 69 th Street, New York, NY 10021 T: 212-994-4400; F: 212-994-4499 Informed Consent for Assisted Reproduction: In Vitro Fertilization,
F REQUENTLY A SKED Q UESTIONS
 Polycystic heart, blood vessels, and appearance. Women with PCOS have these characteristics: Ovarian high levels of male hormones, also called androgens an irregular or no menstrual cycle Syndrome may
Polycystic heart, blood vessels, and appearance. Women with PCOS have these characteristics: Ovarian high levels of male hormones, also called androgens an irregular or no menstrual cycle Syndrome may
Section III Consent Forms
 Section III Consent Forms Please read the consents prior to your IVF consultation appointment. Most people have questions regarding the consent forms. Your questions will be addressed during the appointment.
Section III Consent Forms Please read the consents prior to your IVF consultation appointment. Most people have questions regarding the consent forms. Your questions will be addressed during the appointment.
In Vitro Fertilization, Intracytoplasmic Sperm Injection Assisted Hatching Embryo Freezing
 NAME (Patient): NAME (Partner): DOB: DOB: MEDICAL RECORD NUMBER: MEDICAL RECORD NUMBER: Informed Consent for Assisted Reproduction: In Vitro Fertilization, Intracytoplasmic Sperm Injection Assisted Hatching
NAME (Patient): NAME (Partner): DOB: DOB: MEDICAL RECORD NUMBER: MEDICAL RECORD NUMBER: Informed Consent for Assisted Reproduction: In Vitro Fertilization, Intracytoplasmic Sperm Injection Assisted Hatching
INSEMINATION IUI. Engelsk Info IUI ~ 1 ~
 Engelsk Info IUI ~ 1 ~ INSEMINATION IUI Engelsk Info IUI ~ 2 ~ In cases of unexplained infertility, irregular periods, ovulatory dysfunction or poor sperm quality, insemination of sperm cells directly
Engelsk Info IUI ~ 1 ~ INSEMINATION IUI Engelsk Info IUI ~ 2 ~ In cases of unexplained infertility, irregular periods, ovulatory dysfunction or poor sperm quality, insemination of sperm cells directly
Another great resource for information is from the American Society for Reproductive Medicine.
 Thank you for choosing the Center for Women's Reproductive Care at Columbia University (CWRC) as your fertility care provider. In our ongoing attempt to make the fertility treatment process as stress free
Thank you for choosing the Center for Women's Reproductive Care at Columbia University (CWRC) as your fertility care provider. In our ongoing attempt to make the fertility treatment process as stress free
Information and Risks Associated with In Vitro Fertilization
 1 of 14 INTRODUCTION The following information offers a description for potential adverse effects and risks of In Vitro Fertilization (IVF) offered at the Regional Fertility Program. Our staff will educate
1 of 14 INTRODUCTION The following information offers a description for potential adverse effects and risks of In Vitro Fertilization (IVF) offered at the Regional Fertility Program. Our staff will educate
Laboratoires Genevirer Menotrophin IU 1.8.2
 Important missing information VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Infertility is when a woman cannot get pregnant (conceive) despite having regular unprotected sexual
Important missing information VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Infertility is when a woman cannot get pregnant (conceive) despite having regular unprotected sexual
Laparoscopy and Hysteroscopy
 AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
Biology of fertility control. Higher Human Biology
 Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
Package leaflet: Information for the patient. Orgalutran 0.25 mg/0.5 ml solution for injection Ganirelix
 Package leaflet: Information for the patient Orgalutran 0.25 mg/0.5 ml solution for injection Ganirelix Read all of this leaflet carefully before you start using this medicine because it contains important
Package leaflet: Information for the patient Orgalutran 0.25 mg/0.5 ml solution for injection Ganirelix Read all of this leaflet carefully before you start using this medicine because it contains important
Initials: Patient: Partner (if applicable): 5 Columbus Circle New York, NY (646)
 In Vitro Fertilization Intracytoplasmic Sperm Injection Assisted Hatching Embryo Freezing Please place your initials below to indicate which components of IVF treatment you agree to undertake in your upcoming
In Vitro Fertilization Intracytoplasmic Sperm Injection Assisted Hatching Embryo Freezing Please place your initials below to indicate which components of IVF treatment you agree to undertake in your upcoming
South Jersey Fertility Center (SJFC) Informed Consent for Assisted Reproduction: In Vitro Fertilization and Embryo Freezing
 South Jersey Fertility Center (SJFC) Informed Consent for Assisted Reproduction: In Vitro Fertilization and Embryo Freezing Please sign your name(s) below to indicate which components of IVF treatment
South Jersey Fertility Center (SJFC) Informed Consent for Assisted Reproduction: In Vitro Fertilization and Embryo Freezing Please sign your name(s) below to indicate which components of IVF treatment
GENA2. Source Booklet. General Studies (Specification A) General Certificate of Education Advanced Subsidiary Examination June 2011
 General Certificate of Education Advanced Subsidiary Examination June 2011 General Studies (Specification A) GENA2 Unit 2 AS Science and Society Source Booklet Source for use with Questions 1.1 to 1.30.
General Certificate of Education Advanced Subsidiary Examination June 2011 General Studies (Specification A) GENA2 Unit 2 AS Science and Society Source Booklet Source for use with Questions 1.1 to 1.30.
FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system)
 FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system) Mirena does not protect against HIV infection (AIDS) and other sexually transmitted infections
FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system) Mirena does not protect against HIV infection (AIDS) and other sexually transmitted infections
Introduction to CRM. Ronald O. Perelman and Claudia Cohen Center for Reproductive Medicine - CRM
 Introduction to CRM Ronald O. Perelman and Claudia Cohen Center for Reproductive Medicine - CRM 1 CRM Locations Upper East Side (Main Office) 1305 York Avenue, 6 th Floor New York, NY 10021 *open 7 days
Introduction to CRM Ronald O. Perelman and Claudia Cohen Center for Reproductive Medicine - CRM 1 CRM Locations Upper East Side (Main Office) 1305 York Avenue, 6 th Floor New York, NY 10021 *open 7 days
Age Related Fertility Preservation: Should you Consider Multiple Egg Freezing Cycles?
 Age Related Fertility Preservation: Should you Consider Multiple Egg Freezing Cycles? Age Related fertility Preservation: Should you Consider Multiple Egg Freezing Cycles? All what we really know for sure
Age Related Fertility Preservation: Should you Consider Multiple Egg Freezing Cycles? Age Related fertility Preservation: Should you Consider Multiple Egg Freezing Cycles? All what we really know for sure
Dr Manuela Toledo - Procedures in ART -
 Dr Manuela Toledo - Procedures in ART - Fertility Specialist MBBS FRANZCOG MMed CREI Specialities: IVF & infertility Fertility preservation Consulting Locations East Melbourne Planning a pregnancy - Folic
Dr Manuela Toledo - Procedures in ART - Fertility Specialist MBBS FRANZCOG MMed CREI Specialities: IVF & infertility Fertility preservation Consulting Locations East Melbourne Planning a pregnancy - Folic
Assisted Reproductive Technology (ART) Process, Risk, and Consent
 Page 1 of 21 Informed Consent for Assisted Reproductive Technology (ART) version 2018 Assisted Reproductive Technology (ART) Process, Risk, and Consent Date: Patient Last Name: ID# Partner Last Name: ID
Page 1 of 21 Informed Consent for Assisted Reproductive Technology (ART) version 2018 Assisted Reproductive Technology (ART) Process, Risk, and Consent Date: Patient Last Name: ID# Partner Last Name: ID
Package leaflet: Information for the user
 Package leaflet: Information for the user Bemfola 75 IU/0.125 ml solution for injection in a pre-filled pen Bemfola 150 IU/0.25 ml solution for injection in a pre-filled pen Bemfola 225 IU/0.375 ml solution
Package leaflet: Information for the user Bemfola 75 IU/0.125 ml solution for injection in a pre-filled pen Bemfola 150 IU/0.25 ml solution for injection in a pre-filled pen Bemfola 225 IU/0.375 ml solution
ANU. the ultimate guide. becoming an egg donor. Cally ANU Fertility Egg Donor
 ANU F E R T I L I T Y becoming an egg donor Cally ANU Fertility Egg Donor the ultimate guide We are so happy that you have expressed an interest in becoming an Egg Donor and genuinely appreciate you considering
ANU F E R T I L I T Y becoming an egg donor Cally ANU Fertility Egg Donor the ultimate guide We are so happy that you have expressed an interest in becoming an Egg Donor and genuinely appreciate you considering
Age and Fertility. A Guide for Patients Revised 2012 Copyright 2012 by the American Society for Reproductive Medicine
 1 Age and Fertility A Guide for Patients Revised 2012 Copyright 2012 by the American Society for Reproductive Medicine INTRODUCTION Fertility changes with age. Both males and females become fertile in
1 Age and Fertility A Guide for Patients Revised 2012 Copyright 2012 by the American Society for Reproductive Medicine INTRODUCTION Fertility changes with age. Both males and females become fertile in
Fertility assessment and assisted conception
 Fertility assessment and assisted conception Dr Geetha Venkat MD FRCOG Director Pulse Learning Women s health 14 September 2016 Disclosure statement Dr Venkat is a director of Harley Street Fertility Clinic.
Fertility assessment and assisted conception Dr Geetha Venkat MD FRCOG Director Pulse Learning Women s health 14 September 2016 Disclosure statement Dr Venkat is a director of Harley Street Fertility Clinic.
Agonist (Lupron) Injection Protocol
 Agonist (Lupron) Injection Protocol DO s and DON Ts DO Avoid high impact exercise (spinning, running, Zumba etc.) Low impact exercise okay (swimming, walking, etc.) Okay to have sex while on stimulation
Agonist (Lupron) Injection Protocol DO s and DON Ts DO Avoid high impact exercise (spinning, running, Zumba etc.) Low impact exercise okay (swimming, walking, etc.) Okay to have sex while on stimulation
treatments to become a mom last fall.
 September Newsletter 2018 IVF Medications and Protocols Most common fertility treatments: how they work and how much they cost - Patricia Kozicka Most common fertility treatments: how they work and how
September Newsletter 2018 IVF Medications and Protocols Most common fertility treatments: how they work and how much they cost - Patricia Kozicka Most common fertility treatments: how they work and how
Causes of Infertility and Treatment Options
 Causes of Infertility and Treatment Options Dr Mrs.Kiran D. Sekhar Former vice President-FOGSI Former Chairperson- Genetics and Foetal medicine-fogsi Founder and Medical Director-Kiran Infertility centre
Causes of Infertility and Treatment Options Dr Mrs.Kiran D. Sekhar Former vice President-FOGSI Former Chairperson- Genetics and Foetal medicine-fogsi Founder and Medical Director-Kiran Infertility centre
Consent for In Vitro Fertilization with Donor Oocyte: Donor - Patient/Husband
 with Donor Oocyte: Donor - Patient/Husband Name of Patient: Name of Partner: I, the Patient, and my husband (if applicable) named above, are each over the age of twenty-one (21) years. I am a healthy female
with Donor Oocyte: Donor - Patient/Husband Name of Patient: Name of Partner: I, the Patient, and my husband (if applicable) named above, are each over the age of twenty-one (21) years. I am a healthy female
GENERAL INFORMATION FOR OVULATION INDUCTION PATIENTS USING INJECTABLE MEDICATIONS
 GENERAL INFORMATION FOR OVULATION INDUCTION PATIENTS USING INJECTABLE MEDICATIONS What follows is some information concerning normal reproductive physiology, the use of these injectable medications and
GENERAL INFORMATION FOR OVULATION INDUCTION PATIENTS USING INJECTABLE MEDICATIONS What follows is some information concerning normal reproductive physiology, the use of these injectable medications and
WHAT IS A PATIENT CARE ADVOCATE?
 WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
Melanoma-What Every Woman Need to Know about Fertility and Pregnancy
 Melanoma-What Every Woman Need to Know about Fertility and Pregnancy Women diagnosed with melanoma may require counseling for fertility preservation, fertility treatment and safety of pregnancy after treatment.
Melanoma-What Every Woman Need to Know about Fertility and Pregnancy Women diagnosed with melanoma may require counseling for fertility preservation, fertility treatment and safety of pregnancy after treatment.
Older. Freezing your eggs? Information about the procedure of retrieving and freezing eggs or a section of an ovary.
 Older Freezing your eggs? Information about the procedure of retrieving and freezing eggs or a section of an ovary. Good to know. This information is for younger people who, due to cancer treatment, may
Older Freezing your eggs? Information about the procedure of retrieving and freezing eggs or a section of an ovary. Good to know. This information is for younger people who, due to cancer treatment, may
Female Consultation Questionnaire
 Female Consultation Questionnaire In order to schedule a consultation with the doctor, an overview of your medical history along with a copy of your medical records are requested. Dr. Zouves will review
Female Consultation Questionnaire In order to schedule a consultation with the doctor, an overview of your medical history along with a copy of your medical records are requested. Dr. Zouves will review
Laparoscopy-Hysteroscopy
 Laparoscopy-Hysteroscopy Patient Information Laparoscopy The laparoscope, a surgical instrument similar to a telescope, is inserted through a small incision (cut) in the belly button during laparoscopy.
Laparoscopy-Hysteroscopy Patient Information Laparoscopy The laparoscope, a surgical instrument similar to a telescope, is inserted through a small incision (cut) in the belly button during laparoscopy.
(A) In-Vitro Fertilization (per cycle) HKD Payable to (1) Standard Drug Package (IVF) $11,000 CUHK. (5) Laboratory Fee for Embryo Transfer $1,800 CUHK
 The services provided by this Unit are funded by both the Chinese University of Hong Kong () and the Hospital Authority (). You will therefore receive bills from both and. Payment to the Chinese University
The services provided by this Unit are funded by both the Chinese University of Hong Kong () and the Hospital Authority (). You will therefore receive bills from both and. Payment to the Chinese University
Reproductive Endocrinology & Infertility Glossary
 Reproductive Endocrinology & Infertility Glossary The following is a glossary of terms you may hear during your association with the University of Mississippi Health Care's reproductive endocrinology and
Reproductive Endocrinology & Infertility Glossary The following is a glossary of terms you may hear during your association with the University of Mississippi Health Care's reproductive endocrinology and
In Vitro Fertilization Process, Risk, and Consent
 Department of Obstetrics and Gynecology Strong Fertility Center Kathleen Hoeger, MD, MPH Director Bala Bhagavath, MD Vivian Lewis, MD John T. Queenan, Jr., MD Wendy Vitek, MD In Vitro Fertilization Process,
Department of Obstetrics and Gynecology Strong Fertility Center Kathleen Hoeger, MD, MPH Director Bala Bhagavath, MD Vivian Lewis, MD John T. Queenan, Jr., MD Wendy Vitek, MD In Vitro Fertilization Process,
