Cryobiology is a rapidly evolving field that only. Vitrification of Human ICSI/IVF Spermatozoa Without Cryoprotectants: New Capillary Technology
|
|
|
- Megan Baker
- 5 years ago
- Views:
Transcription
1 Journal of Andrology, Vol. 33, No. 3, May/June 2012 Copyright E American Society of Andrology Vitrification of Human ICSI/IVF Spermatozoa Without Cryoprotectants: New Capillary Technology V. ISACHENKO,*{ R. MAETTNER,{ A. M. PETRUNKINA, 5 K. STERZIK,{ P. MALLMANN,* G. RAHIMI,* R. SANCHEZ," J. RISOPATRON," I. DAMJANOSKI,# AND E. ISACHENKO*{ From the *Department of Obstetrics and Gynecology, Cologne University, Cologne, Germany; the ÀSection of Gynecological Endocrinology and Reproductive Medicine, University of Ulm, Ulm, Germany; the `Private Maternal Hospital, Endokrinologikum Ulm, Ulm, Germany; the Unit of Reproductive Medicine of Clinics, University of Veterinary Medicine of Hannover, Foundation, Clinic for Horses, Hannover, Germany; the 5Cambridge Institute for Medical Research, University of Cambridge, Cambridge, United Kingdom; the "BIOREN-CEBIOR, Department of Preclinical Sciences, Department of Basic Sciences, La Frontera University, Temuco, Chile; and the #Clinic for Urology, University of Ulm, Ulm, Germany. ABSTRACT: The aim of this study was to develop and to test the standardized aseptic technology of permeable cryoprotectant-free vitrification of human spermatozoa in capillaries (for intracytoplasmic sperm injection [ICSI] or in vitro fertilization [IVF]). To test the effect of vitrification on basic sperm parameters, each of 68 swim-up prepared ejaculates from oligo-astheno-terato-zoospermic patients were aliquoted and distributed into 3 groups: 1) nontreated control, 2) 10 ml of spermatozoa cryopreserved by slow conventional freezing with glycerol-contented medium, and 3) 10 ml of spermatozoa vitrified in 50-mL plastic capillaries in culture medium with 0.25 M sucrose. Spermatozoa motility (1, 24, and 48 hours after warming), plasma membrane integrity, acrosomal integrity, and spontaneous capacitation-like changes were determined after warming. Aseptic cryoprotectant-free vitrification showed a significantly stronger cryoprotective effect compared with conventional freezing. One hour after warming, motility, plasma membrane integrity, and acrosomal integrity were significantly higher than is observed for conventionally frozen spermatozoa (28% vs 18%, 56% vs 22%, and 55% vs 21%, respectively; P,.05), although lower than in fresh spermatozoa (35%, 96%, and 84%, respectively; P,.05). Capacitation-like changes did not differ significantly between vitrified and conventionally frozen samples (8% vs 9%, respectively; P..1) (2% in fresh spermatozoa). The newly developed technology of aseptic vitrification of human spermatozoa in capillaries can effectively preserve these cells from cryo-injures. Spermatozoa, vitrified by this technology, are free from seminal plasma owing to swim-up preceding vitrification and are free from permeable cryoprotectants. They are ready for further use immediately after warming without any additional treatment. Therefore, the reported technology has a great potential for use in ICSI/IVF. Key words: Cryoprotectant-free, motility, membrane, acrosome. J Androl 2012;33: Cryobiology is a rapidly evolving field that only relatively recently has found broad applications in reproductive medicine. However, as any emerging technology, it has both a great potential and a need for further developments (Petrunkina, 2007). The use of programmable or nonprogrammable slow (conventional) freezing (McLaughlin et al, 1990; Yin and Seibel, 1999; Stanic et al, 2000) allows preservation of relatively large volumes of diluted ejaculate or sperm preparations, from 0.25 to 1.0 ml, with acceptable rates of motility of spermatozoa after thawing and adequate integrity of acrosomal and cytoplasmic membranes Correspondence to: V. Isachenko, Department of Obstetrics and Gynecology, Cologne University, Kerpener Str. 34, Cologne, Germany ( v.isachenko@yahoo.com). Received for publication April 1, 2011; accepted for publication June 15, Cambridge Institute for Medical Research is in receipt of Wellcome Trust Strategic Award. DOI: /jandrol (Sawetawan et al, 1993; Larson et al, 1997; Hammadeh et al, 1999). It is also instrumental in minimizing cryopreservation-induced cell deterioration, resulting in membrane destabilization processes, such as membrane phosphatidylserine translocation (Glander and Schaller, 2000; Duru et al, 2001; Schuffner et al, 2001). One of relatively recently emerged technologies within the field of reproductive cryobiology is spermatozoa vitrification (cryopreservation by directly plunging into liquid nitrogen). This method is based on rapid cooling of cells by immersion into liquid nitrogen and, thereby, is the key to reducing the chance of forming big ice crystals. In contrast to programmable ( slow ) conventional freezing, vitrification has a series of useful technological advantages: it renders the use of permeable cryoprotectants superfluous and, additionally, is much faster, simpler in application, and more cost effective than conventional freezing. At the same time, vitrification can effectively protect spermatozoa from cryo-injuries associated with cooling and warming (Nawroth et al, 2002; Isachenko 462
2 Isachenko et al N Vitrification of Human Spermatozoa 463 et al, 2003, 2004a,b, 2005, 2008). In particular, the mutagenic effects of permeable cryoprotectants (Fraga et al, 1991) can be avoided. At present, most reported applications of this technology describe vitrification of only very small volumes of spermatozoa suspensions: from 1 to 10 ml with isolation from liquid nitrogen (Isachenko et al, 2005) and from 20 to 30 ml with direct plunging or dropping of the suspension with spermatozoa into liquid nitrogen (Nawroth et al, 2002; Isachenko et al, 2005, 2008). Vitrification of up to 10 ml of a spermatozoon suspension, as it is being used in daily practice (Isachenko et al, 2005), presumes that open pulled straws (Vajta et al, 1998) are used. Current industrial technology does not yet enable the manufacturing of such open pulled straws with a uniform (standard) diameter of the pulled part of the straw. This shortcoming is reflected in nonuniformity of the vitrification regime. On the other hand, industrial suppliers offer plastic capillaries of regular cylinder shape with stable (fixed) diameter for medical applications. The vitrification process can be standardized using these standard capillaries, which would unfold a great potential for assisted reproduction using vitrified spermatozoa. The aim of this study was to develop and test the standardized aseptic technology of permeable cryoprotectant-free vitrification of human spermatozoa in capillaries for intracytoplasmic sperm injection (ICSI) or in vitro fertilization (IVF). Materials and Methods This study was approved by the Review Boards of Cologne and Ulm universities. Except where otherwise stated, all chemicals were obtained from Sigma (Sigma Chemical Co, St Louis, Missouri). Spermatozoa Preparation After informed consent, 68 ejaculates were obtained from 68 patients with oligo-astheno-terato-zoospermia in anamneses who were either patients of an infertility clinic or had donated sperm for research. All specimens used for this study had fulfilled the following quality criteria for spermatozoa concentration, motility, and morphology: less than 20 million spermatozoa/ ml, 35% progressive motile spermatozoa, and a minimum of 3% morphologically normal spermatozoa. Semen analysis was performed according to published guidelines of the World Health Organization (WHO, 1999). All investigations were carried out on swim-up prepared spermatozoa. Human tubal fluid (HTF; Quinn et al, 1985) with 1% human serum albumin (HSA) was the basic medium for spermatozoa preparation. After swim-up, each sample was centrifuged, resuspended with the same medium to achieve a concentration of spermatozoa/ml, and finally aliquoted into 3 equal subsamples. Each of these aliquots was assigned to 1 of 3 groups: Group 1 included fresh, non-cryopreserved swim-up spermatozoa preparations and served as control. Spermatozoa of Group 2 were conventionally frozen, and spermatozoa of Group 3 were vitrified. Vitrification and Warming For preparation of vitrification solution, the basic medium (HTF + 1% HSA) was diluted 1:1 with 0.5 M sucrose. Spermatozoa were centrifuged and resuspended with this vitrification solution (Isachenko et al, 2008). The sucrose stock solution was prepared with bi-distillate water, passed through a 0.22-mm filter, and then stored frozen until use. Diluted suspensions were maintained at room temperature for 5 minutes before the cooling procedure. Spermatozoa were prepared and portioned for aseptic vitrification in the following way. Specifically, for our purposes, 50-mL plastic capillaries were manufactured from hydrophobic material as vehicles for cooling sperm cell suspensions (Gynemed GmbH & Co KG, Lensahn, Germany; Figure 1). The end of the straw was labeled on the top to mark the cut-off position (Figure 1, arrows). The capillary was filled with 10 ml of spermatozoa suspension by aspiration (Figure 1a). It was absolutely crucial that the inner surface of the capillary not become moist during the packaging procedure. Aspirating the volume of sperm cell suspension above the mark and correcting it by lowering the fluid level inside the capillary after aspiration is technologically wrong and would result in an excess volume after thawing. After aspiration was completed, the capillary was inserted into a 0.25-mL straw (Medical Technology GmbH, Bruckberg, Germany). One end of this straw was sealed in advance using a heat-sealer (Cryo Bio System, Paris, France). After sealing the second end of the straw (Figure 1b), the straw was plunged into liquid nitrogen and cooled at 600uC/min. The speed of cooling was determined using a Testo 950 electrical thermometer (Testo AG, Lenzkirch, Germany) using a 0.2-mm electrode located inside the capillary. Hermetical heat sealing of the 0.25-mL straw can be achieved with the flame of an alcohol burner and forceps or any commercial equipment (including ultrasound equipment because of the large distance between the spermatozoa suspension and the focus of the sonographic appliance). Spermatozoa were stored in liquid nitrogen for at least 24 hours before warming. For warming, the capillary was removed from the isolating 0.25-mL straw. The straw was disinfected with ethanol at the marked end of the capillary (Figure 1, arrows). The second end of the capillary was fixed tightly on the inner surface of the straw, and the part of the straw containing spermatozoa was still half submerged in liquid nitrogen (Figure 1c and d). The upper part of the straw was cut off with sterile scissors, as close as possible to the marked end of the capillary, just above the mark, without touching the marked end of the capillary. The capillary was expelled with a conical bolt (Figure 1d). For this purpose, the conical bolt (or, instead, the conical bolt forceps can be used) is inserted into the inner part of the capillary and pulled off the straw. The final warming of spermatozoa is achieved by immersing the capillary without the conical apex (the capillary must be
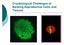
3 464 Journal of Andrology N May ÙJune 2012 using an aspirator (Medical Technology GmbH). These capillaries were placed into 0.25-mL standard insemination straws (Medical Technology GmbH). Then, straws were put horizontally into liquid nitrogen vapor (280uC, 10 cm over the liquid nitrogen surface), kept for 30 minutes, and finally placed into liquid nitrogen, where they were stored a minimum of 24 hours until evaluation. Thawing of spermatozoa was performed in accordance with the technique described above for vitrified spermatozoa. After thawing and expelling 10 ml of spermatozoa from capillaries, 10 ml of basic (HTF-HSA) medium was added to the thawed sample and centrifuged for 5 minutes at g. The supernatant was removed and the pellet resuspended with the same basic medium to obtain a final concentration of spermatozoa/ml. Then, the evaluation of spermatozoa quality was performed. Motility Motility of spermatozoa was assessed 1 hour after liquefaction, swim-up procedure, cryopreservation, and warming of samples and after 24 and 48 hours in vitro in culture for evaluation of long-term spermatozoa survival. The Makler chamber was used for all motility studies. Motility was estimated under light microscope (Zeiss Axiolab epifluorescence microscope) under 6400 magnification. Only spermatozoa with progressive motility (categories a [rapid, regular forward progression] and b [moderate, slow, or sluggish forward progression]) according to WHO (1999) were assessed. Figure 1. Schematic illustration of spermatozoa vitrification using 50- ml capillaries. (Arrows) Marked end of 50-mL capillary; (a) aspiration of spermatozoa suspension in straw, (b) 50-mL capillary sealed in a 0.25-mL straw, (c) cutting of 0.25-mL straw, (d) expelling of 50-mL capillary from 0.25-mL straw, (e) warming of spermatozoa. Color figure available online at open from both sides) with vitrified spermatozoa into a 1.8-mL centrifuge tube with 0.7 ml of vitrification medium prewarmed to 37uC for approximately 20 seconds (Figure 1e). It is important to note that the volume of vitrified suspension after warming is not increased (Figure 1e). Finally, the suspension of spermatozoa was expelled from the capillary for immediate evaluation of spermatozoa quality and use in IVF or ICSI. Conventional Freezing and Thawing After the swim-up procedure, the sperm suspension was diluted 1:2 with freezing medium (12% [v/v] glycerol and 20% [v/v] egg yolk; Freezing Medium TYB, Irvine Scientific, Santa Ana, California) to achieve a concentration of spermatozoa/ml. Subsequently, diluted sperm preparations were equilibrated at room temperature for 10 minutes. Thereafter, 10 ml of spermatozoa suspension was portioned by aspiration into 50-mL plastic capillaries (Gynemed GmbH) Plasma Membrane Integrity Integrity of the plasma membrane was assessed with the LIVE/ DEAD sperm viability kit (Molecular Probes L-7011, Eugene, Oregon). This kit includes SYBR-14 dye and propidium iodide (PI), which stain nucleic acid. With this kit, one can differentiate intact and damaged spermatozoa. Because of its properties, SYBR-14 accumulates inside of living cells and emits green fluorescence; therefore it can be used for identification of live spermatozoa and exclusion of non DNA-containing particles and debris (Garner et al, 1994; Petrunkina and Harrison, 2010). The dead cells membrane will be permeable for PI, which would intercalate DNA and emit red fluorescence. For estimation of cytoplasmic membrane integrity, the 50-mL suspension with spermatozoa/ml were add to 200 ml of phosphate-buffered saline (PBS) with 1.25 ml of SYBR-14 (1:100, Molecular Probes, Grand Island, New York) and exposed for 5 minutes at 37uC. Then, 1 ml of 2.4 mm of PI was added, and this solution with spermatozoa was incubated additionally for 7 minutes at 37uC. Spermatozoa were visualized microscopically using a Zeiss Axiolab epifluorescence microscope. Acrosomal Integrity and Capacitation-like Changes Changes in the membrane status and permeability associated with capacitation are traditionally evaluated by using the double fluorescence chlortetracycline (CTC) Hoechst staining technique (Kay et al, 1994). In short, 100 ml of suspension with spermatozoa/ml were incubated with
4 Isachenko et al N Vitrification of Human Spermatozoa 465 Figure 2. Motility of spermatozoa after conventional freezing and vitrification. All rates in respective groups are significantly different (P,.05). 1 mlof10mg/100ml Hoechst water solution for 5 minutes at room temperature in the dark. After this, the spermatozoa suspension was centrifuged at 340 6g for 5 minutes. The pellet was resuspended in 1 ml of PBS and centrifuged again at g for 5 minutes. After discarding the supernatant, the pellet was gently agitated, and a 5-mL suspension was placed in the center of aslide.next,5ml of 1 mm CTC in 20 mm Tris (ph 7.8) solution was added to the droplet on the slide and incubated for 30 seconds. The cells were fixed with a 1:1 ratio of 25% glutaraldehyde in 1 M Tris buffer. To delay photobleaching during the fluorescence procedure, 0.22 mm 1,4-diazabicyclo[2.2.2]octane was used. The probes were stored in the dark at 4uC until reading (a maximum of 48 hours). At least 200 spermatozoa were observed on each plate, and 3 patterns were identified: a uniform fluorescence on the head of the spermatozoa (classified as noncapacitated ), a band of fluorescence diminished in the postacrosomal region and a relatively shining fluorescence in the acrosomal region (spermatozoa identified as undergoing capacitation-like changes); and a fluorescence of the complete head of the spermatozoa, except for a tenuous band of fluorescence in the equatorial segment (identified as acrosome-reacted spermatozoa). The slides were viewed using a Zeiss Axiolab epifluorescence microscope that was equipped with an excitation/emission filter of 485/520 nm under 6400 magnification. The nonviable spermatozoa were observed with filter set 09 ( nm). The dead spermatozoa displayed a pattern of blue fluorescence in the whole head. Statistical Analysis An ANOVA (Kruskal Wallis test) with a significance of 0.05, for nonparametric statistical analysis, and the Dunn multiple comparison to establish differences between groups were used. Data presented are x + SEM unless otherwise specified. All data refer to 68 observations for each group. Results Motility Motility of small volumes of vitrified spermatozoa (10 ml) in the absence of permeable cryoprotectants displayed statistically higher levels of motility compared Figure 3. Plasma membrane integrity of spermatozoa after conventional freezing and vitrification. All rates in respective groups are significantly different (P,.05). with slow conventional freezing ( % vs %, respectively; P,.05) (in fresh, %). Motility of vitrified spermatozoa in culture after 24 hours in vitro was also statistically different from that of frozen spermatozoa ( % vs %, respectively; P,.05) (in fresh, %) (Figure 2). Motility rates of vitrified spermatozoa in culture after 48 hours in vitro was also statistically different from those of frozen spermatozoa ( % vs %, respectively; P..1) (in fresh, %) (Figure 2). Plasma Membrane Integrity The effect of different modes of cryopreservation on plasma membrane integrity is shown in Figure 3. It was observed that higher rates of membrane integrity were achieved in vitrified spermatozoa compared with slow conventional freezing ( % vs %, respectively; P,.05). However, compared with nontreated control (fresh spermatozoa), spermatozoa viability was significantly diminished in frozen-thawed spermatozoa in both cases (in fresh spermatozoa, %; P,.05). Acrosomal Integrity and Capacitation-like Changes The effect of 2 procedures used for cryopreservation on acrosomal membrane status by CTC staining is shown in Figure 4. There was a statistically significant difference between percentages of spermatozoa with intact acrosome after vitrification compared with conventional freezing ( % vs %, respectively; P,.05) (in fresh, %; P,.05). The presence of capacitation-like changes after different modes of cryopreservation is shown in Figure 5. It was noted that the aseptic vitrification technique provides significantly stronger prevention against cryo-capacitation compared with conventional freezing ( % vs %, respectively; P,.01) (in both cases, the
5 466 Journal of Andrology N May ÙJune 2012 Figure 4. Acrosomal integrity of spermatozoa after conventional freezing and vitrification. All rates in respective groups are significantly different (P,.05). Figure 5. Capacitation-like changes of spermatozoa after conventional freezing and vitrification. Rates in groups after freezing and vitrification are similar (P..5). percentage of cells with capacitation-like changes was higher than in fresh spermatozoa: %; P,.05). Discussion Varied methods of vitrifying spermatozoa have been described previously: cryo-loops, the droplets method, and the open pulled straw method (Nawroth et al, 2002; Isachenko et al, 2004a,b, 2005, 2008). Depending on the vitrification method selected and the quality of the original ejaculate, one can achieve motility levels of up to 60% and 20% after thawing in normospermic and oligo-astheno-terato-zoospermic patients, respectively. Vitrified spermatozoa can be processed for further use immediately after warming. No additional treatment (eg, centrifugation, gradient separation, removal of cryoprotectants, etc) is required. For practical purposes, this simplicity represents one of the most attractive advantages of our technology. It is worth mentioning that the protocol for vitrification does include swim-up treatment; therefore, after swim-up, vitrified and warmed spermatozoa are also free of seminal plasma with potential pathogens. Slow freezing of human spermatozoa traditionally includes the following stages of manipulations: 1) slow, stepwise addition of freezing solution to the ejaculate; 2) cooling for 20 to 45 minutes; 3) warming in a waterbath; and 4) preparation of spermatozoa by density gradient or swim-up for removal of permeable cryoprotectants. The removal of permeable cryoprotectants is the ultimate target of the last manipulation. As a rule, a prerequisite for that step is a dilution of semen suspension with culture medium to reduce toxicity of the permeable cryoprotectant (according to manufacturer s instructions for the cryoprotectant of choice). This step is associated with additional costs and, not the least, with environmental and adaptational challenges for spermatozoa. In fact, the sensitivity of spermatozoa to additional mechanical manipulation increases after freezing-thawing, and the negative effects of cryopreservation on cell viability and functional competence can be aggravated by additional procedures (Petrunkina, 2007). Several protocols of spermatozoa separation are available (eg, swim-up from the ejaculate, single wash of ejaculate and swim-up from the pellet, and double wash of ejaculate and swim-up from the pellet). However, any methodology needs previous centrifugation. Most of the current technologies for sperm vitrification have an obvious shortcoming in terms of standardization of the portion volume. In particular, because the diameter of the pulled part of the straw is not uniform, the volumes of the portions packaged in that way cannot be standardized. Here, we have reported a vitrification methodology that uses standard capillaries supplied by industrial manufacturers. Using the technique described here, exact quantifiable volumes of spermatozoa samples were obtained: 10-mL suspension of spermatozoa were vitrified, 10 ml was thawed, and the same 10 ml was added to the respective volume of medium for ICSI or IVF. Thus, one of the most important features of this novel method of vitrification in capillaries is its potential for standardization, which can be instrumental in clinical practice. The results of the present study suggest that cryopreservation by vitrification helps preserve essential determinants of spermatozoa function, such as motility and plasma membrane integrity. It is well known that spermatozoa cryopreservation is associated with a large decline in spermatozoa viability and other sperm function parameters (Petrunkina, 2007). In the present study, we have compared spermatozoa quality after vitrification by our method with spermato-
6 Isachenko et al N Vitrification of Human Spermatozoa 467 zoa quality after conventional freezing with the addition of permeable cryoprotectant. The outcomes indicated that motility of spermatozoa and membrane integrity were better preserved after vitrification in capillaries than after conventional freezing. Pilot results have been obtained with respect to evaluating capacitation-like changes associated with cryopreservation so called cryo-capacitation (Cormier and Bailey, 2003). A body of evidence suggests that some spermatozoon intracellular signaling pathways can be affected during cryopreservation and cooling, and after warming, spermatozoa display features commonly observed in capacitating or capacitated spermatozoa (Green and Watson, 2001; Petrunkina et al, 2005; Vadnais and Roberts, 2010). It is important, however, to emphasize that the changes induced by cryopreservation are similar to those of capacitation only at the functional level, and they seem to differ at the molecular level and with respect to pathways and signaling mechanisms involved (Cormier and Bailey, 2003). Our observations imply that permeable cryoprotectant free aseptic vitrification is associated with less damage to acrosomes. However, the levels of membrane changes related to cryo-capacitation assessed by CTC in vitrified spermatozoa were comparable to those after conventional freezing. Nevertheless, exposure to low temperatures can affect those crucial signaling mechanisms that cannot be monitored by CTC. Thus, further studies with additional, advanced techniques are needed to investigate the changes induced by vitrification in its complexity (eg, targeting specific pathways and membrane processes such as changes in lipid architecture, protein kinase/phosphatase-regulated pathways, or a combination of processes). Given that the outcome of basic spermatozoon quality was comparable (or even better) than that after conventional freezing, other advantages of the vitrification process must be taken into account. During conventional procedures, the success in applying permeable cryoprotectants for cryopreservation of various cells and tissues is inseparably linked to such cryoprotectant properties as their ability to permeate rapidly through the cellular membrane and their toxicity (Gilmore et al, 1997). These properties are directly connected to osmotic damages of cells during saturation with permeable cryoprotectants before freezing and then at the time of cryoprotectant removal after thawing (Gao et al, 1995; Petrunkina, 2007). It is known that human spermatozoa contain large quantities of proteins, sugars, and other components that may act as natural cryoprotectants. Our technology does not presuppose the use of permeable cryoprotectant. In practical terms, permeable cryoprotectant-free vitrification technology for the cryopreservation of spermatozoa (in straws) instead traditional slow freezing with permeable cryoprotectants is already used in our university s maternity hospital ( IVF Centers in Temuco, Chile (about 200 IUI cycles/y), and in Ulm, Germany ( about 1000 IVF cycles/y). The first successful pregnancies and births of healthy babies have been recently achieved with spermatozoa vitrified without permeable cryoprotectants (Isachenko et al, 2012). The newly developed technology of aseptic vitrification of human spermatozoa in capillaries can effectively preserve these cells from cryo-injures. Spermatozoa vitrified by this technology are free of seminal plasma, owing to swim-up preceding vitrification and are free of permeable cryoprotectants. They are ready for further use immediately after warming without any additional treatment. Therefore, the reported technology has a great potential for use in ICSI/IVF. References Cormier N, Bailey JL. A differential mechanism is involved during heparin- and cryopreservation-induced capacitation of bovine spermatozoa. Biol Reprod. 2003;69: Duru NK, Morshedi M, Schuffner A, Oehninger S. Cryopreservationthawing of fractionated human spermatozoa and plasma membrane translocation of phosphatidylserine. Fertil Steril. 2001;75: Fraga CG, Motchnik PA, Shigenaga MK, Helbock HJ, Jacob RA, Ames BN. Ascorbic acid protects against endogenous oxidative DNA damage in human sperm. Proc Nat Acad Sci U S A. 1991;88: Gao DY, Liu J, Liu C, McGann LE, Watson PF, Kleinhans FW, Mazur P, Critser ES, Critser JK. Prevention of osmotic injury to human spermatozoa during addition and removal of glycerol. Hum Reprod. 1995;10: Garner DL, Johnson LA, Yue ST, Roth BL, Haugland RP. Dual DNA staining assessment of bovine sperm viability using SYBR-14 and propidium iodide. J Androl. 1994;15: Gilmore JA, Liu J, Gao DY, Critser JK. Determination of optimal cryoprotectants and procedures for their addition and removal from human spermatozoa. Hum Reprod. 1997;12: Glander HJ, Schaller J. Hidden effects of cryopreservation on quality of human spermatozoa. Cell Tissue Bank. 2000;1: Green CE, Watson PF. Comparison of the capacitation-like state of cooled boar spermatozoa with true capacitation. Reproduction. 2001;122: Hammadeh ME, Askari AS, Georg T, Rosenbaum P, Schmidt W. Effect of freeze-thawing procedure on chromatin stability, morphological alteration and membrane integrity of human spermatozoa in fertile and subfertile men. Int J Androl. 1999;22: Isachenko E, Isachenko V, Katkov II, Nawroth F. Vitrification of human spermatozoa without cryoprotectants: review of problem and practical success. Reprod Biomed Online. 2003;6: Isachenko E, Isachenko V, Katkov II, Rahimi G, Schondorf T, Mallmann P, Dessole S, Nawroth F. DNA integrity and motility of human spermatozoa after standard slow freezing versus cryoprotectant-free vitrification. Hum Reprod. 2004a;19: Isachenko E, Isachenko V, Weiss JM, Kreienberg R, Katkov II, Schulz M, Lulat AG, Risopatrón MJ, Sánchez R. Acrosomal status
7 468 Journal of Andrology N May ÙJune 2012 and mitochondrial activity of human spermatozoa vitrified with sucrose. Reproduction. 2008;136: Isachenko V, Isachenko E, Katkov II, Montag M, Dessole S, Nawroth F, van der Ven H. Cryoprotectant-free cryopreservation of human spermatozoa by vitrification and freezing in vapor: effect on motility, DNA integrity, and fertilization ability. Biol Reprod. 2004b;71: Isachenko V, Isachenko E, Montag M, Zaeva V, Krivokharchenko A, Nawroth F, Dessole S, Katkov I, van der Ven H. Clean technique for cryoprotectant-free vitrification of human spermatozoa. Reprod Biomed Online. 2005;10: Isachenko V, Isachenko E, Petrunkina AM, Sanchez R. Human spermatozoa vitrified in the absence of permeable cryoprotectants: birth of two healthy babies. Reprod Fertil Dev. 2012; 24: Kay VJ, Coutts JR, Robertson L. Effects of pentoxifylline and progesterone on human sperm capacitation and acrosome reaction. Hum Reprod. 1994;9: Larson JM, McKinney KA, Mixon BA, Burry KA, Wolf DP. An intrauterine insemination-ready cryopreservation method compared with sperm recovery after conventional freezing and postthaw processing. Fertil Steril. 1997;68: McLaughlin EA, Ford WC, Hul MG. A comparison of the freezing of human semen in the uncirculated vapour above liquid nitrogen and in a commercial semi-programmable freezer. Hum Reprod. 1990;5: Nawroth F, Isachenko V, Dessole S, Rahimi G, Farina M, Vargiu N, Mallmann P. Vitrification of human spermatozoa without cryoprotectants. CryoLetters. 2002;23: Petrunkina A. Fundamental aspects of gamete cryobiology. J Reprod Med Endokrinol. 2007;4: Petrunkina AM, Harrison RAP. Systematic misestimation of cell subpopulations by flow cytometry: a mathematical analysis. Theriogenology. 2010;73: Petrunkina AM, Volker G, Weitze KF, Beyerbach M, Töpfen-Petersen E, Waberski D. Detection of cooling-induced membrane changes in the response of boar sperm to capacitating conditions. Theriogenology. 2005;63: Quinn P, Warnes GM, Kerin JF, Kirby C. Culture factors affecting the success rate of in vitro fertilization and embryo transfer. Ann NY Acad Sci. 1985;442: Sawetawan C, Bruns ES, Prins GS. Improvement of post-thaw sperm motility in poor quality human semen. Fertil Steril. 1993;60: Schuffner A, Morshedi M, Oehninger S. Cryopreservation of fractionated, highly motile human spermatozoa: effect on membrane phosphatidylserine externalization and lipid peroxidation. Hum Reprod. 2001;16: Stanic P, Tandara M, Sonicki Z, Simunic V, Radakovic B, Suchanek E. Comparison of protective media and freezing techniques for cryopreservation of human semen. Eur J Obstet Gyn RB. 2000;91: Vadnais ML, Roberts KP. Seminal plasma proteins inhibit in vitroand cooling-induced capacitation in boar spermatozoa. Reprod Fertil Dev. 2010;22: Vajta G, Kuwayama M, Holm P, Booth PJ, Jacobsen H, Greve T, Callesen H. Open pulled straw (OPS) vitrification: a new way to reduce cryoinjuries of bovine ova and embryos. Mol Reprod Dev. 1998;51: World Health Organization (WHO). WHO Laboratory Manual for the Examination of Human Semen Cervical Mucus Interaction. 4th ed. Cambridge, United Kingdom: Cambridge University Press; Yin HZ, Seibel MM. Human sperm cryobanking. Use of modified liquid nitrogen vapor. J Reprod Med. 1999;44:87 90.
Vitrification Technique New Possibilities for Male Gamete Low-Temperature Storage
 Vitrification Technique New Possibilities for Male Gamete Low-Temperature Storage 2 E. Isachenko, P. Mallmann, G. Rahimi, J. Risopatròn, M. Schulz, V. Isachenko and R. Sànchez Woman Hospital, University
Vitrification Technique New Possibilities for Male Gamete Low-Temperature Storage 2 E. Isachenko, P. Mallmann, G. Rahimi, J. Risopatròn, M. Schulz, V. Isachenko and R. Sànchez Woman Hospital, University
Sperm vitrification. Caracteristics of vitrification. Campus Granada Spain With permission from V. Isachenko
 Sperm vitrification Dr. Raúl Sánchez G. Departamento de Ciencias Preclínicas BIOREN-CEBIOR Facultad de Medicina Universidad de La Frontera Temuco-CHILE Campus Granada Spain - 21 With permission from V.
Sperm vitrification Dr. Raúl Sánchez G. Departamento de Ciencias Preclínicas BIOREN-CEBIOR Facultad de Medicina Universidad de La Frontera Temuco-CHILE Campus Granada Spain - 21 With permission from V.
Abstract. Materials and methods. Introduction
 RBMOnline - Vol 10. No 3. 2005 350-354 Reproductive BioMedicine Online; www.rbmonline.com/article/1637 on web 25 January 2005 Article Clean technique for cryoprotectant-free vitrification of human spermatozoa
RBMOnline - Vol 10. No 3. 2005 350-354 Reproductive BioMedicine Online; www.rbmonline.com/article/1637 on web 25 January 2005 Article Clean technique for cryoprotectant-free vitrification of human spermatozoa
Proper steps for bull semen dilution and freezing. IMV Technologies France
 Proper steps for bull semen dilution and freezing IMV Technologies France Introduction Since Polge reported the first successful cryopreservation of spermatozoa in 1949, spermatozoa from many mammalian
Proper steps for bull semen dilution and freezing IMV Technologies France Introduction Since Polge reported the first successful cryopreservation of spermatozoa in 1949, spermatozoa from many mammalian
SPERM PREPARATION, HANDLING & STORAGE
 SPERM PREPARATION, HANDLING & STORAGE Solutions for the andrology laboratory HELP AT EVERY STEP with simpler processes, less stress and better results Multipurpose Handling Medium RETRIEVE AND RINSE OOCYTES
SPERM PREPARATION, HANDLING & STORAGE Solutions for the andrology laboratory HELP AT EVERY STEP with simpler processes, less stress and better results Multipurpose Handling Medium RETRIEVE AND RINSE OOCYTES
XVII Congresso Internazionale SIVE
 SOCIETÀ ITALIANA VETERINARI PER EQUINI SOCIETÀ FEDERATA ANMVI XVII Congresso Internazionale SIVE XVII SIVE International Congress Palacongressi d Abruzzo Montesilvano (PE) - ITALY 4-6 Febbraio 2011 February
SOCIETÀ ITALIANA VETERINARI PER EQUINI SOCIETÀ FEDERATA ANMVI XVII Congresso Internazionale SIVE XVII SIVE International Congress Palacongressi d Abruzzo Montesilvano (PE) - ITALY 4-6 Febbraio 2011 February
OVERVIEW AND FACTS: CRYOPRESERVATION
 OVERVIEW AND FACTS: CRYOPRESERVATION Imprint Published in August, 2013 By Victory A.R.T. Laboratory Phils, Inc. This ebook was created by http://www.ivfvictoryphilippines.com/ in hopes of helping bring
OVERVIEW AND FACTS: CRYOPRESERVATION Imprint Published in August, 2013 By Victory A.R.T. Laboratory Phils, Inc. This ebook was created by http://www.ivfvictoryphilippines.com/ in hopes of helping bring
Comparative Examination of Deep-Frozen Ram Semen after Thawing and Incubating an Different Solution
 International Journal of Applied Science and Technology Vol. 5, No. 6; December 2015 Comparative Examination of Deep-Frozen Ram Semen after Thawing and Incubating an Different Solution A. Csiba E. Gyoker
International Journal of Applied Science and Technology Vol. 5, No. 6; December 2015 Comparative Examination of Deep-Frozen Ram Semen after Thawing and Incubating an Different Solution A. Csiba E. Gyoker
TECHNIQUES AND INSTRUMENTATION
 FERTILITY AND STERILITY VOL. 76, NO. 1, JULY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. TECHNIQUES AND INSTRUMENTATION
FERTILITY AND STERILITY VOL. 76, NO. 1, JULY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. TECHNIQUES AND INSTRUMENTATION
Computerized semen analysis. Product features. Basic system
 AndroVision - more than CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
AndroVision - more than CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
AAB/CRB 2017 Houston, Texas
 AAB/CRB 2017 Houston, Texas Advanced Current & Future Cryogenic Technologies for ART James J. Stachecki Ph.D. Innovative Cryo Enterprises LLC Disclosures Founder of Innovative Cryo Enterprises LLC We focus
AAB/CRB 2017 Houston, Texas Advanced Current & Future Cryogenic Technologies for ART James J. Stachecki Ph.D. Innovative Cryo Enterprises LLC Disclosures Founder of Innovative Cryo Enterprises LLC We focus
ANDROVISION - MORE THAN CASA
 ANDROVISION - MORE THAN CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
ANDROVISION - MORE THAN CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
Sergey I. Moskovtsev and Clifford L. Librach
 Chapter 2 Methods of Sperm Vitality Assessment Sergey I. Moskovtsev and Clifford L. Librach Abstract Sperm vitality is a re fl ection of the proportion of live, membrane-intact spermatozoa determined by
Chapter 2 Methods of Sperm Vitality Assessment Sergey I. Moskovtsev and Clifford L. Librach Abstract Sperm vitality is a re fl ection of the proportion of live, membrane-intact spermatozoa determined by
EFFECT OF THAWING RATE AND POST-THAW TEMPERATURE ON MOTILITY AND ACROSOMAL MAINTENANCE IN BOVINE SEMEN FROZEN IN PLASTIC STRAWS l,2
 EFFECT OF THAWING RATE AND POST-THAW TEMPERATURE ON MOTILITY AND ACROSOMAL MAINTENANCE IN BOVINE SEMEN FROZEN IN PLASTIC STRAWS l,2 P. L. Senger, W. C. Becker and J. K. Hillers Washington State University
EFFECT OF THAWING RATE AND POST-THAW TEMPERATURE ON MOTILITY AND ACROSOMAL MAINTENANCE IN BOVINE SEMEN FROZEN IN PLASTIC STRAWS l,2 P. L. Senger, W. C. Becker and J. K. Hillers Washington State University
Rapid- Vitrification System. Closed system for simple and successful vitrification.
 Rapid- Vitrification System Closed system for simple and successful vitrification. 3 working together for you Media Method Device & accessories Rapid-i Vitrification System puts you in control. The method,
Rapid- Vitrification System Closed system for simple and successful vitrification. 3 working together for you Media Method Device & accessories Rapid-i Vitrification System puts you in control. The method,
Rescue IVF protocol for legacy stock
 Rescue IVF protocol for legacy stock Sperm thawing/ivf protocol for MTG sperm samples (80ul per straw) from straw and conventional CPA from Vial (100ml per vial) This protocol is based on methods developed
Rescue IVF protocol for legacy stock Sperm thawing/ivf protocol for MTG sperm samples (80ul per straw) from straw and conventional CPA from Vial (100ml per vial) This protocol is based on methods developed
Preservation of Liquid Boar Semen: Effect of Genotype, Boar and Sperm Parameters on Motility and Acrosome Integrity
 VETERINARY RESEARCH INTERNATIONAL Journal homepage: www.jakraya.com/journal/vri ORIGINAL ARTICLE Preservation of Liquid Boar Semen: Effect of Genotype, Boar and Sperm Parameters on Motility and Acrosome
VETERINARY RESEARCH INTERNATIONAL Journal homepage: www.jakraya.com/journal/vri ORIGINAL ARTICLE Preservation of Liquid Boar Semen: Effect of Genotype, Boar and Sperm Parameters on Motility and Acrosome
Semen Preservation Dr Hany Lotfi Faculty of veterinary medicine zagazig uinversity
 Semen Preservation Dr Hany Lotfi Faculty of veterinary medicine zagazig uinversity Aim Prolonged the life span of the sperm cell without reducing its fertilizing capacity Idea Induce reversible controllable
Semen Preservation Dr Hany Lotfi Faculty of veterinary medicine zagazig uinversity Aim Prolonged the life span of the sperm cell without reducing its fertilizing capacity Idea Induce reversible controllable
Maximum rates of cooling by three programmable freezers, and the potential relevance to sperm cryopreservation
 Vol. 8, No. 1 69 SHORT NOTE Maximum rates of cooling by three programmable freezers, and the potential relevance to sperm cryopreservation Phillip Matson 1,2,3, Wendy Kappelle 2, Sandra Webb 2 2 Reproductive
Vol. 8, No. 1 69 SHORT NOTE Maximum rates of cooling by three programmable freezers, and the potential relevance to sperm cryopreservation Phillip Matson 1,2,3, Wendy Kappelle 2, Sandra Webb 2 2 Reproductive
I.C.E. Embryo Vitrification Kit
 I.C.E. Embryo Vitrification Kit Vitrification Media V1, V2, V3 ICE Embryo Vitrification Instructions For Use Testing and Cautions Innvative Cryo Enterprises LLC 317 Springfield Road Linden, New Jersey
I.C.E. Embryo Vitrification Kit Vitrification Media V1, V2, V3 ICE Embryo Vitrification Instructions For Use Testing and Cautions Innvative Cryo Enterprises LLC 317 Springfield Road Linden, New Jersey
FERTIUP PM 1 ml / 0.5 ml - CARD MEDIUM Set
 Product manual FERTIUP PM 1 ml / 0.5 ml - CARD MEDIUM Set Cat. No. KYD-004-EX Size: 1 SET KYD-005-EX 1 SET Department of Reproductive Engineering, Center for Animal Resources and Development, Kumamoto
Product manual FERTIUP PM 1 ml / 0.5 ml - CARD MEDIUM Set Cat. No. KYD-004-EX Size: 1 SET KYD-005-EX 1 SET Department of Reproductive Engineering, Center for Animal Resources and Development, Kumamoto
Evaluation of Serial Thawing-Refreezing on Human Spermatozoa Resistance Using Cryovials and Straws
 Original Article Evaluation of Serial Thawing-Refreezing on Human Spermatozoa Resistance Using Cryovials and Straws Fatemeh Ghasemian, M.Sc. 1, 2, Roya Faraji, M.D. 2, Mohaddese Mohammadi Sardoo, M.Sc.
Original Article Evaluation of Serial Thawing-Refreezing on Human Spermatozoa Resistance Using Cryovials and Straws Fatemeh Ghasemian, M.Sc. 1, 2, Roya Faraji, M.D. 2, Mohaddese Mohammadi Sardoo, M.Sc.
Effect of straw size and thawing time on quality of cryopreserved buffalo (Bubalus bubalis) semen
 Vol. 11, No. 1 49 SHORT COMMUNICATION Effect of straw size and thawing time on quality of cryopreserved buffalo (Bubalus bubalis) semen Muhammad S Ansari, Bushra A. Rakha, Syed M. H. Andrabi, Shamim Akhter
Vol. 11, No. 1 49 SHORT COMMUNICATION Effect of straw size and thawing time on quality of cryopreserved buffalo (Bubalus bubalis) semen Muhammad S Ansari, Bushra A. Rakha, Syed M. H. Andrabi, Shamim Akhter
Adoption and Foster Care
 GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
RapiDVIT & rapidwarm oocyte. Specialised media for oocyte vitrification.
 RapiDVIT & rapidwarm oocyte Specialised media for oocyte vitrification. Special media for A unique cell Cryopreservation of oocytes requires care. Some preservation techniques cause premature oocyte activation
RapiDVIT & rapidwarm oocyte Specialised media for oocyte vitrification. Special media for A unique cell Cryopreservation of oocytes requires care. Some preservation techniques cause premature oocyte activation
TECHNICAL REPORT Minitube TurboFreezer A standardised freezing process is crucial for efficient production of cryopreserved bull semen
 TECHNICAL REPORT 02 2016 Minitube TurboFreezer A standardised freezing process is crucial for efficient production of cryopreserved bull semen Dr. Monika Esch, Minitüb GmbH The objective of utilizing nitrogen
TECHNICAL REPORT 02 2016 Minitube TurboFreezer A standardised freezing process is crucial for efficient production of cryopreserved bull semen Dr. Monika Esch, Minitüb GmbH The objective of utilizing nitrogen
Protocol for embryo vitrification using open pulled straws. Introduction. Reagents. Materials
 Protocol for embryo vitrification using open pulled straws Froylan Sosa and Peter J Hansen Department of Animal Sciences, University of Florida Introduction This vitrification protocol is a slight modification
Protocol for embryo vitrification using open pulled straws Froylan Sosa and Peter J Hansen Department of Animal Sciences, University of Florida Introduction This vitrification protocol is a slight modification
INFRAFRONTIER-I3 - Cryopreservation training course. Hosted by the Frozen Embryo and Sperm Archive, MRC - Harwell
 Hosted by the Frozen Embryo and Sperm Archive, MRC - Harwell IVF recovery procedure incorporting methyl-β-cyclodextrin and reduced glutathione This protocol is based on the work published by Takeo et al.,
Hosted by the Frozen Embryo and Sperm Archive, MRC - Harwell IVF recovery procedure incorporting methyl-β-cyclodextrin and reduced glutathione This protocol is based on the work published by Takeo et al.,
Cryopreservation of Porcine Gametes: A Chilly Future in the Swine Industry. EM Walters
 Cryopreservation of Porcine Gametes: A Chilly Future in the Swine Industry EM Walters National Swine Resource and Research Center and Veterinary Pathobiology, University of Missouri, Columbia, MO Corresponding
Cryopreservation of Porcine Gametes: A Chilly Future in the Swine Industry EM Walters National Swine Resource and Research Center and Veterinary Pathobiology, University of Missouri, Columbia, MO Corresponding
Animal Science 434. Semen Collection. Effect of Age on Sperm Output. Age When Semen Can Be Collected. Text: Ch. 10 and 11. Sexual Behavior (cont.
 Animal Science 434 Age When Semen Can Be Collected Sexual Behavior (cont.) B. Applied Reproductive Behavior of the Male: Semen Collection and Processing Text: Ch. 10 and 11 Bull Boar Ram Stallion Dog 12
Animal Science 434 Age When Semen Can Be Collected Sexual Behavior (cont.) B. Applied Reproductive Behavior of the Male: Semen Collection and Processing Text: Ch. 10 and 11 Bull Boar Ram Stallion Dog 12
Basic information on the cryopreservation process
 COST Action FA1205 AQUAGAMETE 5 th AQUAGAMETE Training School Valencia, Spain, 7-11 th March, 2016 Basic information on the cryopreservation process Ákos Horváth Department of Aquaculture, Szent István
COST Action FA1205 AQUAGAMETE 5 th AQUAGAMETE Training School Valencia, Spain, 7-11 th March, 2016 Basic information on the cryopreservation process Ákos Horváth Department of Aquaculture, Szent István
Instructions. Fuse-It-mRNA easy. Shipping and Storage. Overview. Kit Contents. Specifications. Note: Important Guidelines
 Membrane fusion is a highly efficient method for transfecting various molecules and particles into mammalian cells, even into sensitive and primary cells. The Fuse-It reagents are cargo-specific liposomal
Membrane fusion is a highly efficient method for transfecting various molecules and particles into mammalian cells, even into sensitive and primary cells. The Fuse-It reagents are cargo-specific liposomal
Animal Science 434" Semen Collection" Effect of Age on Sperm Output" Age When Semen Can Be Collected" Text: Ch. 10 and 11"
 Animal Science 434" Age When Semen Can Be Collected" Lecture 15b: Sexual Behavior (cont.) B. Applied Reproductive Behavior of the Male: Semen Collection and Processing Text: Ch. 10 and 11" "Bull "Boar
Animal Science 434" Age When Semen Can Be Collected" Lecture 15b: Sexual Behavior (cont.) B. Applied Reproductive Behavior of the Male: Semen Collection and Processing Text: Ch. 10 and 11" "Bull "Boar
Tammie Roy Genea Biomedx Sydney, Australia. Declared to be stakeholder in Genea Biomedx
 Tammie Roy Genea Biomedx Sydney, Australia Declared to be stakeholder in Genea Biomedx 1 24-25 September 2015 Madrid and Alicante, Spain Importance of cryopreservation in Assisted Reproductive Technology
Tammie Roy Genea Biomedx Sydney, Australia Declared to be stakeholder in Genea Biomedx 1 24-25 September 2015 Madrid and Alicante, Spain Importance of cryopreservation in Assisted Reproductive Technology
Welcome to chapter 2. The following chapter is called Sperm preparation for IVF and ICSI and sperm freezing. The author is Bart Desmet.
 Welcome to chapter 2. The following chapter is called Sperm preparation for IVF and ICSI and sperm freezing. The author is Bart Desmet. 1 After this chapter, the student should be able to know the different
Welcome to chapter 2. The following chapter is called Sperm preparation for IVF and ICSI and sperm freezing. The author is Bart Desmet. 1 After this chapter, the student should be able to know the different
Sperm Preparation for Intrauterine Insemination Using Density Gradient Separation
 Sperm Preparation for Intrauterine Insemination Using Density Gradient Separation 14 Ashok Agarwal, Sajal Gupta, and Rakesh Sharma 1 Introduction Sperm washing is performed to remove seminal plasma and
Sperm Preparation for Intrauterine Insemination Using Density Gradient Separation 14 Ashok Agarwal, Sajal Gupta, and Rakesh Sharma 1 Introduction Sperm washing is performed to remove seminal plasma and
Understanding eggs, sperm and embryos. Marta Jansa Perez Wolfson Fertility Centre
 Understanding eggs, sperm and embryos Marta Jansa Perez Wolfson Fertility Centre What does embryology involve? Aims of the embryology laboratory Creation of a large number of embryos and supporting their
Understanding eggs, sperm and embryos Marta Jansa Perez Wolfson Fertility Centre What does embryology involve? Aims of the embryology laboratory Creation of a large number of embryos and supporting their
7-AAD/CFSE Cell-Mediated Cytotoxicity Assay Kit
 7-AAD/CFSE Cell-Mediated Cytotoxicity Assay Kit Catalog Number KA1293 96 assays Version: 02 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 Principle of
7-AAD/CFSE Cell-Mediated Cytotoxicity Assay Kit Catalog Number KA1293 96 assays Version: 02 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 Principle of
Microinsemination (Intracytoplasmic Sperm Injection) Microinsemination schedule. 1. Preparation of mediums
 Microinsemination (Intracytoplasmic Sperm Injection) Masumi Hirabayashi Section of Mammalian Transgenesis, Center for Genetic Analysis of Behavior, National Institute for Physiological Sciences, National
Microinsemination (Intracytoplasmic Sperm Injection) Masumi Hirabayashi Section of Mammalian Transgenesis, Center for Genetic Analysis of Behavior, National Institute for Physiological Sciences, National
Interspecies Challenges
 Cryobiological Challenges of Banking Reproductive Cells, and Tissues Interspecies Challenges Mammals Domestic species Lab animal species Endangered Species Humans (Reproductive Med) Birds Domestic species
Cryobiological Challenges of Banking Reproductive Cells, and Tissues Interspecies Challenges Mammals Domestic species Lab animal species Endangered Species Humans (Reproductive Med) Birds Domestic species
Human Induced Plutipotent Stem Cell (ipsc) Handling Protocols: Matrigel and mtesr/e8 Media
 General Guidelines for Handling Human ipsc cells ipsc are cryopreserved in plastic cryovials and shipped on dry ice. If storing the ipsc before thawing, store in liquid nitrogen vapor. Storage directly
General Guidelines for Handling Human ipsc cells ipsc are cryopreserved in plastic cryovials and shipped on dry ice. If storing the ipsc before thawing, store in liquid nitrogen vapor. Storage directly
COMPARISON OF KAMPONG AND COMMERCIAL CHICKEN EGG-BASED EXTENDERS ON CRYOPRESERVED GOAT SPERM MOVEMENT CHARACTERISTICS
 COMPARISON OF KAMPONG AND COMMERCIAL CHICKEN EGG-BASED EXTENDERS ON CRYOPRESERVED GOAT SPERM MOVEMENT CHARACTERISTICS Janice, C.W.K. 1, Kanwal, K.D.S. 1*, Wan Khadijah, W.E. 2 and Abdullah, R.B. 2 1 School
COMPARISON OF KAMPONG AND COMMERCIAL CHICKEN EGG-BASED EXTENDERS ON CRYOPRESERVED GOAT SPERM MOVEMENT CHARACTERISTICS Janice, C.W.K. 1, Kanwal, K.D.S. 1*, Wan Khadijah, W.E. 2 and Abdullah, R.B. 2 1 School
Vitrification of mouse embryos in straw
 Vitrification of mouse embryos in straw Based on a method originally published by Nakagata et al (1997) 1. Materials 1.1. Media and solutions 1.1.1. PB1 as basic solution 1.1.2. 1M DMSO solution in PB1.
Vitrification of mouse embryos in straw Based on a method originally published by Nakagata et al (1997) 1. Materials 1.1. Media and solutions 1.1.1. PB1 as basic solution 1.1.2. 1M DMSO solution in PB1.
COMPARATIVE STUDY OF DIFFERENT METHODS FOR PLASMA MEMBRANE INTEGRITY ASSESSMENT OF FROZEN-THAWED BOAR SPERMATOZOA
 Bull Vet Inst Pulawy 55, 231-236, 211 COMPARATIVE STUDY OF DIFFERENT METHODS FOR PLASMA MEMBRANE INTEGRITY ASSESSMENT OF FROZEN-THAWED BOAR SPERMATOZOA LEYLAND FRASER, ŁUKASZ ZASIADCZYK, MAREK LECEWICZ,
Bull Vet Inst Pulawy 55, 231-236, 211 COMPARATIVE STUDY OF DIFFERENT METHODS FOR PLASMA MEMBRANE INTEGRITY ASSESSMENT OF FROZEN-THAWED BOAR SPERMATOZOA LEYLAND FRASER, ŁUKASZ ZASIADCZYK, MAREK LECEWICZ,
Human ipsc-derived Ventricular Cardiomyocytes. Protocol version 3.1
 Human ipsc-derived Ventricular Cardiomyocytes Protocol version 3.1 Protocol version 3.1 Table of Contents Product Information 2 Recommendations 2 Preparing Cardiomyocyte Maintenance Medium 3 Cardiomyocyte
Human ipsc-derived Ventricular Cardiomyocytes Protocol version 3.1 Protocol version 3.1 Table of Contents Product Information 2 Recommendations 2 Preparing Cardiomyocyte Maintenance Medium 3 Cardiomyocyte
Improvement of post-thaw sperm motility in poor quality human semen*
 FERTILITY AND STERILITY Vol. 6, No.4, October 1993 Copyright 1993 The American Fertility Society Printed on acid-free paper in U. S. A. Improvement of post-thaw sperm motility in poor quality human semen*
FERTILITY AND STERILITY Vol. 6, No.4, October 1993 Copyright 1993 The American Fertility Society Printed on acid-free paper in U. S. A. Improvement of post-thaw sperm motility in poor quality human semen*
SINGLE UV EXCITATION OF HOECHST AND PROPIDIUM IODIDE FOR VIABILITY ASSESSMENT OF RHESUS MONKEY SPERMATOZOA USING FLOW CYTOMETRY
 Archives of Andrology Journal of Reproductive Systems ISSN: 0148-5016 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iaan19 SINGLE UV EXCITATION OF HOECHST 33342 AND PROPIDIUM IODIDE
Archives of Andrology Journal of Reproductive Systems ISSN: 0148-5016 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iaan19 SINGLE UV EXCITATION OF HOECHST 33342 AND PROPIDIUM IODIDE
CARD HyperOva (Superovulation Reagent for mouse)
 Product manual (Superovulation Reagent for mouse) Cat. No. KYD-010-EX -X5 Size: 5 1 ML Origin Serum of goat, Horse-derived villus gonatropin. Composition 1. Inhibin antiserum (Goat). 2. Equine chorionic
Product manual (Superovulation Reagent for mouse) Cat. No. KYD-010-EX -X5 Size: 5 1 ML Origin Serum of goat, Horse-derived villus gonatropin. Composition 1. Inhibin antiserum (Goat). 2. Equine chorionic
System overview Installation System Description System Default Settings and Loading I-Button Tests Components/Kits /Accessories Maintenance & Cleaning
 SQA-VISION TRAINING Content of Presentation System overview Installation System Description System Default Settings and Loading I-Button Tests Components/Kits /Accessories Maintenance & Cleaning SQA-Vision
SQA-VISION TRAINING Content of Presentation System overview Installation System Description System Default Settings and Loading I-Button Tests Components/Kits /Accessories Maintenance & Cleaning SQA-Vision
Striatal Neuron Medium Kit
 Striatal Neuron Medium Kit Product Information What are included in the Striatal Neuron Medium Kit (ax0333): 2x 250 ml Striatal Neuron Basal Medium (Store at 4 o C upon receipt) 2x 7.5 ml Striatal Neuron
Striatal Neuron Medium Kit Product Information What are included in the Striatal Neuron Medium Kit (ax0333): 2x 250 ml Striatal Neuron Basal Medium (Store at 4 o C upon receipt) 2x 7.5 ml Striatal Neuron
ab65336 Triglyceride Quantification Assay Kit (Colorimetric/ Fluorometric)
 Version 10 Last updated 19 December 2017 ab65336 Triglyceride Quantification Assay Kit (Colorimetric/ Fluorometric) For the measurement of triglycerides in various samples. This product is for research
Version 10 Last updated 19 December 2017 ab65336 Triglyceride Quantification Assay Kit (Colorimetric/ Fluorometric) For the measurement of triglycerides in various samples. This product is for research
The Consequences of Mishandling Cryopreserved Specimens
 The Consequences of Mishandling Cryopreserved Specimens Mexico Embryo Transfer Association 2012 Brad Stroud, DVM Stroud Veterinary Embryo Services Weatherford, Texas Objectives of Presentation Define
The Consequences of Mishandling Cryopreserved Specimens Mexico Embryo Transfer Association 2012 Brad Stroud, DVM Stroud Veterinary Embryo Services Weatherford, Texas Objectives of Presentation Define
EGG BANKS program at clinique ovo
 EGG BANKS program at clinique ovo HISTORY The first pregnancy resulting from egg donation in an IVF cycle was in 1983 Egg donation plays an important role in assisted reproductive technologies since it
EGG BANKS program at clinique ovo HISTORY The first pregnancy resulting from egg donation in an IVF cycle was in 1983 Egg donation plays an important role in assisted reproductive technologies since it
Human Spermatozoa Attach to Trypsin-treated Hamster Zonae Pellucidae but do not Undergo Acrosome Reactions
 Hiroshima J. Med. Sci. Vol.44, No.2, 47~51, June, 1995 HIJM 44-8 47 Human Spermatozoa Attach to Trypsin-treated Hamster Zonae Pellucidae but do not Undergo Acrosome Reactions Masatoshi KUMAGAI, Katsunori
Hiroshima J. Med. Sci. Vol.44, No.2, 47~51, June, 1995 HIJM 44-8 47 Human Spermatozoa Attach to Trypsin-treated Hamster Zonae Pellucidae but do not Undergo Acrosome Reactions Masatoshi KUMAGAI, Katsunori
Effects of Cryopreservation on the Ultrastructure of Human Testicular Sperm
 Journal of Reproduction & Contraception (2005) 16 (4):195-200 ORIGINAL PAPER Effects of Cryopreservation on the Ultrastructure of Human Testicular Sperm Xin-qiang LAI 1, Wei-jie ZHU 2, Jing LI 3, Fu-xing
Journal of Reproduction & Contraception (2005) 16 (4):195-200 ORIGINAL PAPER Effects of Cryopreservation on the Ultrastructure of Human Testicular Sperm Xin-qiang LAI 1, Wei-jie ZHU 2, Jing LI 3, Fu-xing
For research or further manufacturing use only. Not for injection or diagnostic procedures.
 PRIME-XV T cell Expansion XSFM PRIME-XV T Cell Expansion XSFM is a xeno-free, serum-free medium optimized for the activation and expansion of human T lymphocytes. This medium contains gentamicin and requires
PRIME-XV T cell Expansion XSFM PRIME-XV T Cell Expansion XSFM is a xeno-free, serum-free medium optimized for the activation and expansion of human T lymphocytes. This medium contains gentamicin and requires
Multi-Parameter Apoptosis Assay Kit
 Multi-Parameter Apoptosis Assay Kit Catalog Number KA1335 5 x 96 assays Version: 05 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 Principle of the Assay...
Multi-Parameter Apoptosis Assay Kit Catalog Number KA1335 5 x 96 assays Version: 05 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 Principle of the Assay...
ROS Activity Assay Kit
 ROS Activity Assay Kit Catalog Number KA3841 200 assays Version: 03 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 General Information... 4 Materials
ROS Activity Assay Kit Catalog Number KA3841 200 assays Version: 03 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 General Information... 4 Materials
Intracellular (Total) ROS Activity Assay Kit (Red)
 Intracellular (Total) ROS Activity Assay Kit (Red) Catalog Number KA2525 200 assays Version: 04 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 General
Intracellular (Total) ROS Activity Assay Kit (Red) Catalog Number KA2525 200 assays Version: 04 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 General
Product Size Catalog Number. 500,000 proliferating cells. cryopreserved cells that have been thawed and cultured for three days at PromoCell.
 Cardiac Myocytes Instruction Manual Product Size Catalog Number Human Cardiac Myocytes (HCM) 500,000 cryopreserved cells 500,000 proliferating cells C-12810 C-12811 Product Description Cardiac muscle,
Cardiac Myocytes Instruction Manual Product Size Catalog Number Human Cardiac Myocytes (HCM) 500,000 cryopreserved cells 500,000 proliferating cells C-12810 C-12811 Product Description Cardiac muscle,
Use of donor semen in the treatment of
 Use of donor semen in the treatment of male infertility Where is the evidence? Max H.J.M. Curfs Isala clinics Zwolle, The Netherlands Strength of evidence Systematic review Meta-analysis RCT 1A 1A 1B
Use of donor semen in the treatment of male infertility Where is the evidence? Max H.J.M. Curfs Isala clinics Zwolle, The Netherlands Strength of evidence Systematic review Meta-analysis RCT 1A 1A 1B
Fertility Preservation for Trans Women: Sperm Banking
 Fertility Preservation for Trans Women: Sperm Banking A PUBLICATION OF FAIRFAX CRYOBANK About the Author Michelle Ottey, PhD, HCLD is the Director of Operations for Fairfax Cryobank and Cryogenic Laboratories,
Fertility Preservation for Trans Women: Sperm Banking A PUBLICATION OF FAIRFAX CRYOBANK About the Author Michelle Ottey, PhD, HCLD is the Director of Operations for Fairfax Cryobank and Cryogenic Laboratories,
Follicle Dermal Papilla Cells
 Follicle Dermal Papilla Cells Instruction Manual Product Size Catalog Number Human Follicle Dermal Papilla Cells (HFDPC) 500,000 cryopreserved cells 500,000 proliferating cells C-12071 C-12072 Product
Follicle Dermal Papilla Cells Instruction Manual Product Size Catalog Number Human Follicle Dermal Papilla Cells (HFDPC) 500,000 cryopreserved cells 500,000 proliferating cells C-12071 C-12072 Product
EFFECTS OF DIFFERENT TEMPERATURE TREATMENTS APPLIED TO DEEP STORED BULL SEMEN ON POST-THAW COLD SHOCKED SPERMATOZOA
 Bull Vet Inst Pulawy 50, 79-83, 2006 EFFECTS OF DIFFERENT TEMPERATURE TREATMENTS APPLIED TO DEEP STORED BULL SEMEN ON POST-THAW COLD SHOCKED SPERMATOZOA ZEKARIYA NUR, IRFAN KAMURAN ILERI 1 AND KEMAL AK
Bull Vet Inst Pulawy 50, 79-83, 2006 EFFECTS OF DIFFERENT TEMPERATURE TREATMENTS APPLIED TO DEEP STORED BULL SEMEN ON POST-THAW COLD SHOCKED SPERMATOZOA ZEKARIYA NUR, IRFAN KAMURAN ILERI 1 AND KEMAL AK
Cryopreservation of human oocytes with slow freezing techniques
 ESHRE Campus Symposium Cryobiology and cryopreservation of human gametes and embryos Athens, Greece 25-26 September 2009 Cryopreservation of human oocytes with slow freezing techniques Giovanni Coticchio
ESHRE Campus Symposium Cryobiology and cryopreservation of human gametes and embryos Athens, Greece 25-26 September 2009 Cryopreservation of human oocytes with slow freezing techniques Giovanni Coticchio
cryotubes Information from Biochrom AG, May 23, 2011
 Recommendations on how to safely freeze and thaw cell cultures in TPP cryotubes Information from Biochrom AG, May 23, 2011 Cryopreservation can be used to store cell cultures for a virtually indefinite
Recommendations on how to safely freeze and thaw cell cultures in TPP cryotubes Information from Biochrom AG, May 23, 2011 Cryopreservation can be used to store cell cultures for a virtually indefinite
Follicle Dermal Papilla Cell
 Follicle Dermal Papilla Cell Instruction Manual Product Size Catalog Number Human Follicle Dermal Papilla Cells (HFDPC) 500,000 cryopreserved cells 500,000 proliferating cells C-12071 C-12072 Product Description
Follicle Dermal Papilla Cell Instruction Manual Product Size Catalog Number Human Follicle Dermal Papilla Cells (HFDPC) 500,000 cryopreserved cells 500,000 proliferating cells C-12071 C-12072 Product Description
Annexin V-APC/7-AAD Apoptosis Kit
 Annexin V-APC/7-AAD Apoptosis Kit Catalog Number KA3808 100 assays Version: 04 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 General Information... 4
Annexin V-APC/7-AAD Apoptosis Kit Catalog Number KA3808 100 assays Version: 04 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 General Information... 4
SEQUENTIAL CULTURE MEDIA SYSTEM
 SEQUENTIAL CULTURE MEDIA SYSTEM Gamete solutions... 7 Fertilization solutions...15 Cleavage solutions...21 Blastocyst solutions...27 STIC Media Stopper Removal Tool...35 Complete list of order numbers...36
SEQUENTIAL CULTURE MEDIA SYSTEM Gamete solutions... 7 Fertilization solutions...15 Cleavage solutions...21 Blastocyst solutions...27 STIC Media Stopper Removal Tool...35 Complete list of order numbers...36
Bank your future: Insemination and semen cryopreservation. Disclosure. Lecture objectives
 Bank your future: Insemination and semen cryopreservation Roelof Menkveld, PhD Andrology Laboratory, Department of Obstetrics and Gynaecology, Tygerberg Academic Hospital and University of Stellenbosch.
Bank your future: Insemination and semen cryopreservation Roelof Menkveld, PhD Andrology Laboratory, Department of Obstetrics and Gynaecology, Tygerberg Academic Hospital and University of Stellenbosch.
Induction of the human sperm acrosome reaction by human oocytes*
 FERTILITY AND STERILITY Copyright C> 1988 The American Fertility Society Vol. 50, No.6, December 1988 Printed in U.S.A. Induction of the human sperm acrosome reaction by human oocytes* Christopher J. De
FERTILITY AND STERILITY Copyright C> 1988 The American Fertility Society Vol. 50, No.6, December 1988 Printed in U.S.A. Induction of the human sperm acrosome reaction by human oocytes* Christopher J. De
Sandro C. Esteves, M.D. Rakesh K. Sharma, Ph.D. Anthony J. Thomas, Jr., M.D. Ashok Agarwal, Ph.D.
 Int J Fertil, 43 (5), 1998 p. 235-242 1998 U.S. International Foundation for Studies in Reproduction, Inc., the Falloppius International Society, the International Society of Reproductive Medicine, the
Int J Fertil, 43 (5), 1998 p. 235-242 1998 U.S. International Foundation for Studies in Reproduction, Inc., the Falloppius International Society, the International Society of Reproductive Medicine, the
NINDS Repository Human Induced Pluripotent Stem Cell (ipsc) Handling Protocols (Matrigel and mtesr Media)
 General Guidelines for Handling Human ipsc cells ipsc are cryopreserved in plastic cryovials and shipped on dry ice. If storing the ipsc before thawing, store in liquid nitrogen vapor. Storage directly
General Guidelines for Handling Human ipsc cells ipsc are cryopreserved in plastic cryovials and shipped on dry ice. If storing the ipsc before thawing, store in liquid nitrogen vapor. Storage directly
Instructions for Use. APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests
 3URGXFW,QIRUPDWLRQ Sigma TACS Annexin V Apoptosis Detection Kits Instructions for Use APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests For Research Use Only. Not for use in diagnostic procedures.
3URGXFW,QIRUPDWLRQ Sigma TACS Annexin V Apoptosis Detection Kits Instructions for Use APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests For Research Use Only. Not for use in diagnostic procedures.
Microscope Requirements
 SEMEN EVALUATION EQUIPMENT Microscope Requirements Good quality lenses Phase-contrast preferred for % progressive motility evaluations Objectives 10X, 20X*, 40X*, 100X, minimum Heated stage preferred *Preferably
SEMEN EVALUATION EQUIPMENT Microscope Requirements Good quality lenses Phase-contrast preferred for % progressive motility evaluations Objectives 10X, 20X*, 40X*, 100X, minimum Heated stage preferred *Preferably
Instructions. Fuse-It-Color. Overview. Specifications
 Membrane fusion is a novel and highly superior method for incorporating various molecules and particles into mammalian cells. Cargo-specific liposomal carriers are able to attach and rapidly fuse with
Membrane fusion is a novel and highly superior method for incorporating various molecules and particles into mammalian cells. Cargo-specific liposomal carriers are able to attach and rapidly fuse with
Ultrarapid freezing of early cleavage stage human embryos and eight-cell mouse embryos*
 FERTILITY AND STERILITY Copyright 1988 The American Fertility Society Printed in U.S.A. Ultrarapid freezing of early cleavage stage human embryos and eight-cell mouse embryos* Alan Trounson, Ph.D.t:!:
FERTILITY AND STERILITY Copyright 1988 The American Fertility Society Printed in U.S.A. Ultrarapid freezing of early cleavage stage human embryos and eight-cell mouse embryos* Alan Trounson, Ph.D.t:!:
HUMAN TUBAL FLUID MEDIUM (HTF)
 Page 4 Nexus Volume 1 (June 2016) HUMAN TUBAL FLUID MEDIUM (HTF) Figure1a: SAR Healthline India (P) Ltd Figure 1b: Cryo-Genie India (P) Ltd Figure 1c: Cryocell India (P). Ltd. SINGLE DENSITY GRADIENT MEDIUM
Page 4 Nexus Volume 1 (June 2016) HUMAN TUBAL FLUID MEDIUM (HTF) Figure1a: SAR Healthline India (P) Ltd Figure 1b: Cryo-Genie India (P) Ltd Figure 1c: Cryocell India (P). Ltd. SINGLE DENSITY GRADIENT MEDIUM
although work THE TOXICITY OF VARIOUS NON-ELECTROLYTES TO HUMAN SPERMATOZOA AND THEIR PROTECTIVE EFFECTS DURING FREEZING
 THE TOXICITY OF VARIOUS NON-ELECTROLYTES TO HUMAN SPERMATOZOA AND THEIR PROTECTIVE EFFECTS DURING FREEZING D. W. RICHARDSON and R. M. F. S. SADLEIR Endocrine Unit, University College Hospital, London,
THE TOXICITY OF VARIOUS NON-ELECTROLYTES TO HUMAN SPERMATOZOA AND THEIR PROTECTIVE EFFECTS DURING FREEZING D. W. RICHARDSON and R. M. F. S. SADLEIR Endocrine Unit, University College Hospital, London,
Effect of Different Thawing Temperatures on the Motility Recovery of Cryopreserved Human Sperm
 Med. J. Cairo Univ., Vol. 84, No. 1, September: 93-94, 216 www.medicaljournalofcairouniversity.net Effect of Different Thawing Temperatures on the Motility Recovery of Cryopreserved Human Sperm ASHRAF
Med. J. Cairo Univ., Vol. 84, No. 1, September: 93-94, 216 www.medicaljournalofcairouniversity.net Effect of Different Thawing Temperatures on the Motility Recovery of Cryopreserved Human Sperm ASHRAF
Evaluation of Sperm Viability and Acrosomal Integrity by Flow Cytometry Analysis in Jersey Crossbred Bulls
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 10 (2017) pp. 87-93 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.610.010
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 10 (2017) pp. 87-93 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.610.010
TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES
 TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES Approved By: Chief Executive Officer: Ron Josias Accreditation Executive: Mpho Phaloane Revised By: Medical Specialist Technical Committee
TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES Approved By: Chief Executive Officer: Ron Josias Accreditation Executive: Mpho Phaloane Revised By: Medical Specialist Technical Committee
Osmotic Tolerance Limits and Effects of Cryoprotectants on Motility of Bovine Spermatozoa 1
 BIOLOGY OF REPRODUCTION 67, 1811 1816 (2002) Osmotic Tolerance Limits and Effects of Cryoprotectants on Motility of Bovine Spermatozoa 1 H.D. Guthrie, 3 J. Liu, 4 and J.K. Critser 2,4 Germplasm and Gamete
BIOLOGY OF REPRODUCTION 67, 1811 1816 (2002) Osmotic Tolerance Limits and Effects of Cryoprotectants on Motility of Bovine Spermatozoa 1 H.D. Guthrie, 3 J. Liu, 4 and J.K. Critser 2,4 Germplasm and Gamete
Reproductive Medicine, Eastern Virginia Medical School, Norfolk, Virginia
 Mitochondrial membrane potential integrity and plasma membrane translocation of phosphatidylserine as early apoptotic markers: a comparison of two different sperm subpopulations Gerardo Barroso, M.D.,
Mitochondrial membrane potential integrity and plasma membrane translocation of phosphatidylserine as early apoptotic markers: a comparison of two different sperm subpopulations Gerardo Barroso, M.D.,
Effect of sucrose and propylene glycol on the vitrification of sheep oocytes
 Journal of Cell and Animal Biology Vol. 7 (3), pp. 25-30, March 2013 Available online at http://www.academicjournals.org/jcab DOI: 10.5897/JCAB12.033 ISSN 1996-0867 2013 Academic Journals Full Length Research
Journal of Cell and Animal Biology Vol. 7 (3), pp. 25-30, March 2013 Available online at http://www.academicjournals.org/jcab DOI: 10.5897/JCAB12.033 ISSN 1996-0867 2013 Academic Journals Full Length Research
RLI Mouse Vitrification Media Kit
 RLI Mouse Vitrification Media Kit Product Description RLI Vitrification Media Kit (Catalog#: RLI Vitri-Cooling 01, RLI Vitri-Warming 01, RLI Vitri Complete Kit 01) enables ultra-rapid cooling and recovery
RLI Mouse Vitrification Media Kit Product Description RLI Vitrification Media Kit (Catalog#: RLI Vitri-Cooling 01, RLI Vitri-Warming 01, RLI Vitri Complete Kit 01) enables ultra-rapid cooling and recovery
Concentration of glycerol required for optimal survival and in vitro fertilizing capacity of frozen sperm is dependent on cryopreservation medium
 FERTILITY AND STERILITY Copyright e 1988 The American Fertility Society Printed in U.S.A. Concentration of glycerol required for optimal survival and in vitro fertilizing capacity of frozen sperm is dependent
FERTILITY AND STERILITY Copyright e 1988 The American Fertility Society Printed in U.S.A. Concentration of glycerol required for optimal survival and in vitro fertilizing capacity of frozen sperm is dependent
ab Lipid Peroxidation (MDA) Assay kit (Colorimetric/ Fluorometric)
 Version 10b Last updated 19 December 2018 ab118970 Lipid Peroxidation (MDA) Assay kit (Colorimetric/ Fluorometric) For the measurement of Lipid Peroxidation in plasma, cell culture and tissue extracts.
Version 10b Last updated 19 December 2018 ab118970 Lipid Peroxidation (MDA) Assay kit (Colorimetric/ Fluorometric) For the measurement of Lipid Peroxidation in plasma, cell culture and tissue extracts.
Optimize your success
 ANDROLOGY BY ORIGIO Optimize your success by selecting the highest quality sperm QUALITY CONTROL OOCYTE RETRIEVAL ANDROLOGY & IUI FERTILIZATION CULTURE PGD & PGS CRYOPRESERVATION EMBRYO TRANSFER The importance
ANDROLOGY BY ORIGIO Optimize your success by selecting the highest quality sperm QUALITY CONTROL OOCYTE RETRIEVAL ANDROLOGY & IUI FERTILIZATION CULTURE PGD & PGS CRYOPRESERVATION EMBRYO TRANSFER The importance
Comparison between Low/Programmable Freezing and Fast Freezing Protocols of Hungarian Guinea Fowl Semen
 Athens Journal of Natural & Formal Sciences September 2014 Comparison between Low/Programmable Freezing and Fast Freezing Protocols of Hungarian Guinea Fowl Semen By Thieu Ngoc Lan Phuong Eva Varadi Barbara
Athens Journal of Natural & Formal Sciences September 2014 Comparison between Low/Programmable Freezing and Fast Freezing Protocols of Hungarian Guinea Fowl Semen By Thieu Ngoc Lan Phuong Eva Varadi Barbara
FROM GAMETES TO BLASTOCYSTS. Simpler Processes, Less Stress, Better Results.
 FROM GAMETES TO BLASTOCYSTS Simpler Processes, Less Stress, Better Results. HELP AT EVERY STEP with simpler processes, less stress and better results Multipurpose Handling Medium RETRIEVE AND RINSE OOCYTES
FROM GAMETES TO BLASTOCYSTS Simpler Processes, Less Stress, Better Results. HELP AT EVERY STEP with simpler processes, less stress and better results Multipurpose Handling Medium RETRIEVE AND RINSE OOCYTES
Comparison of different hypo-osmotic swelling solutions to select viable immotile spermatozoa for potential use in intracytoplasmic sperm injection
 Human Reproduction Update 1997, Vol. 3, No. 3 pp. 195 203 European Society for Human Reproduction and Embryology Comparison of different hypo-osmotic swelling solutions to select viable immotile spermatozoa
Human Reproduction Update 1997, Vol. 3, No. 3 pp. 195 203 European Society for Human Reproduction and Embryology Comparison of different hypo-osmotic swelling solutions to select viable immotile spermatozoa
IVF: PAST, PRESENT AND FUTURE
 IVF: PAST, PRESENT AND FUTURE Mark Larman Chief Scientific Officer 1 HISTORY OF IVF IVF first achieved with rabbits in 1959 IVF with human gametes - pioneered by Robert Edwards and Patrick Steptoe during
IVF: PAST, PRESENT AND FUTURE Mark Larman Chief Scientific Officer 1 HISTORY OF IVF IVF first achieved with rabbits in 1959 IVF with human gametes - pioneered by Robert Edwards and Patrick Steptoe during
Cryopreservation of Mouse Spermatozoa in
 Cryopreservation of Mouse atozoa in Department of eproductive Engineering, Center for Animal esources and Development, Kumamoto University, Japan Senior Editor: Naomi Nakagata 1. Male mice (12-70 weeks
Cryopreservation of Mouse atozoa in Department of eproductive Engineering, Center for Animal esources and Development, Kumamoto University, Japan Senior Editor: Naomi Nakagata 1. Male mice (12-70 weeks
Effects of frozen diluents on storage of ram sperm
 Available online at http://www.ijabbr.com International journal of Advanced Biological and Biomedical Research Volume, Issue, : 698-74 Effects of frozen diluents on storage of ram sperm Fatemeh Soltanpour,
Available online at http://www.ijabbr.com International journal of Advanced Biological and Biomedical Research Volume, Issue, : 698-74 Effects of frozen diluents on storage of ram sperm Fatemeh Soltanpour,
Cryopreservation of human spermatozoa within human or mouse empty zona pellucidae
 FERTILITY AND STERILITY VOL. 73, NO. 4, APRIL 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Cryopreservation of
FERTILITY AND STERILITY VOL. 73, NO. 4, APRIL 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Cryopreservation of
