Getting Help for Obstructive Azoospermia A BASIC GUIDE TO MALE. A doctor s guide for patients developed by the American Urological Association, Inc.
|
|
|
- Avis Morton
- 6 years ago
- Views:
Transcription
1 A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice Committee Report
2 2 An AUA Doctor s Guide for Patients Glossary Aspermia: the complete absence of semen. Azoospermia: the complete absence of sperm from the semen. Ejaculatory duct: paired ducts in males that are located behind the bladder and within the prostate. The end of the vas deferens continues into the ejaculatory duct which transports sperm into the urethra. Epididymis: a tightly coiled tubule located behind the testes. Sperm mature as they travel through the epididymis. Non-obstructive azoospermia: azoospermia that is due to absence or marked reduction of sperm production by the testes. Obstructive azoospermia: azoospermia that is due to a blockage in the sperm duct system. Prostate: a small gland about the size of a walnut, located below the bladder. It produces some of the sperm-carrying fluid for the semen. Scrotum: the pouch of skin that hangs from the lower abdominal region below the penis. Semen: fluid that comes out during ejaculation and orgasm. It contains sperm and secretions from glands of the male reproductive tract. Seminiferous tubules: specialized microscopic ducts located within the testes. Immature sperm begin to mature in these tubules. Testes (testicles): the organs that produce sperm. They are paired ovalshaped glands located in the scrotum. Urethra: the tube that carries the urine from the bladder and the semen from the prostate and ejaculatory ducts out through the tip of the penis. It is the final passageway for both urine and sperm to leave the body. Urologist: a doctor who specializes in diseases of the urinary tract and male reproductive system. Vas deferens (also called the vas): a muscular tube through which the sperm flow. It begins at the epididymis and ends behind the bladder.
3 Getting Help for Obstructive Azoospermia 3 What Is Azoospermia and How Common Is It? Definition: The term azoospermia refers to the complete absence of sperm from the semen. About 10-15% of cases of male infertility are due to azoospermia. Azoospermia, or the complete absence of sperm from the semen (also called the seminal fluid or the ejaculate), is different from the complete absence of semen, which is called aspermia. Azoospermia is more common than aspermia. Azoospermia has many causes. Some of the causes are called obstructive, meaning that there is a blockage in the sperm delivery system. Other causes of azoospermia are non-obstructive, meaning that there is absence or very marked reduction of sperm production in the testicles. This booklet is only about the obstructive causes of azoospermia. Even if your doctor has already told you that you have obstructive azoospermia, it is important to remember that the inability to conceive a child often results from problems contributed by both partners. Doctors now know that a male factor for infertility may be involved in as many as half of all infertile couples. Successful outcomes very often depend on both partners being treated. Because this is a time when key decisions must be made, couples should seek help together. They should try to avoid placing blame on one another. This booklet is designed to provide answers to your questions on obstructive azoospermia so that you and your partner, together with your physicians, can choose the best treatment options for you.
4 4 An AUA Doctor s Guide for Patients Overview of the Male Reproductive System: How Are Sperm Produced? The functions of the male reproductive system are to produce sperm and store sperm. The system also transports the sperm to the outside of the body. These 3 steps occur throughout the reproductive life of a male. This process is regulated by a number of hormones. The following diagrams will help you to understand how the male reproductive system works. Ureter Bladder Ampulla Vas Deferens Seminal Vesicle Ejaculatory Duct Prostate Urethra Scrotum Epididymis Testis Glans Meatus
5 Getting Help for Obstructive Azoospermia 5 Epididymis Vas Deferens Seminiferous Tubules Tubule Wall Testis Lumen Mature Sperm Developing Sperm Cells The organs that produce sperm are called the testes. There are 2 testes. They are located in the scrotum, the pouch of skin that hangs from the lower abdomen below the penis. In addition to producing sperm, the testes produce the male hormone testosterone. Sperm production begins with immature sperm cells that grow and develop within the seminiferous tubules. These are very tiny tubules located within the testes. In the seminiferous tubules, the sperm in the testes are not yet fully mature. As a result, they are unable to move on their own.
6 6 An AUA Doctor s Guide for Patients With the help of other accessory organs the sperm mature and become functional. The main organ in this process is called the epididymis. The epididymis is a coiled tubule located behind the testis. Sperm mature as they travel through the epididymis. During the climax (orgasm), the semen, the fluid that contains the sperm, is ejaculated. Semen is composed of fluid from the epididymis, vas deferens, seminal vesicles, and prostate. The sperm must travel through a series of ducts, including the epididymis, vas deferens, ampulla of the vas and ejaculatory ducts. Once the semen is ejaculated, the sperm live about 2 days in the female reproductive tract. The development and transportation of mature, functional sperm depend on a specific sequence of events. As described next, obstructions to the movement of sperm through the male reproductive tract can occur in a number of places along the pathway. Such obstructions prevent sperm from getting to their destination. What Are the Causes of Obstructive Azoospermia? Obstructive azoospermia accounts for about 40% of azoospermia cases. Obstructions may result from defects in any of the ducts (passageways) involved in the sperm delivery system. As seen in the diagrams, the main ducts through which sperm must pass are called the 1) epididymis, 2) vas deferens, 3) ampulla of the vas and 4) ejaculatory duct. Ductal obstruction may be either congenital (you were born with it) or acquired (you were not born with it). Vasectomy is a common form of male contraception. In it, the vas deferens is cut and sealed on each side, forming an acquired obstruction. It is the most common cause of obstruction in the vas. Another common cause is infection. Infection can make a scar form in the epididymis. Congenital obstruction can be due to either a malformation or the absence of a ductal structure.
7 Getting Help for Obstructive Azoospermia 7 What Is the Purpose of an Evaluation for Obstructive Azoospermia? Obstruction of the male reproductive tract can often be corrected by an operation. But in some men, surgical correction is not possible. In this situation it may still be possible for the man to father children by removing a few sperm from his reproductive system and using the sperm for in vitro fertilization (IVF) with intracytoplasmic sperm injection (ICSI). Some of the more common treatment options will be discussed further. Finding the cause of your obstructive azoospermia is helpful for several reasons. First, it allows your physician to decide whether you are a candidate for surgical treatment. Second, if your obstruction is not surgically treatable, your doctor might be able to suggest other treatment options for you and your partner. Third, if there is a major medical or genetic disorder underlying the azoospermia, it may be important to identify these disorders. It is also important to know whether the genetic problem might be passed on to your children. What Is the Best Treatment Option for Me? How to Decide. The options available to couples in whom the male partner has obstructive azoospermia are: surgical correction of the obstruction removal (retrieval) of sperm from the male reproductive system combined with IVF/ICSI artificial insemination with sperm from a donor adoption deciding not to have children The best treatment option for you depends on the cause of the obstruction as well as a number of personal factors. The reproductive health status of your partner, social, marital, religious, cultural and financial
8 8 An AUA Doctor s Guide for Patients factors, and genetic factors are other important considerations. Before you choose the best treatment for you, an evaluation of both you and your partner is recommended. This evaluation will determine whether your obstruction is surgically correctable, and what are the approximate chances for having a baby with each option. It will also tell you what the costs are for each option, and whether there are any genetic abnormalities that might be passed on to your children. The genetic abnormality that may be associated with obstructive azoospermia occurs in some men who are born without the vas deferens. This condition is called congenital bilateral absence of the vasa deferentia (CBAVD). About two-thirds of men who have CBAVD have a genetic mutation that can cause cystic fibrosis if they initiate a pregnancy with a woman who has the same genetic mutation. Fortunately, there is only a 4% chance that a woman will have the cystic fibrosis gene abnormality. Therefore, if you have CBAVD, genetic testing and counseling should be sought to help you and your partner understand the risks of passing this defect to your children. If there is a significant risk of having children with cystic fibrosis, you may want to consider alternatives such as donor insemination or adoption. Am I a Good Candidate for Surgical Treatment? Microsurgical Reconstruction Reconstruction of the reproductive tract is often a successful treatment for obstructive azoospermia. It can be used, for example, to reverse a vasectomy. The doctor s skill at microsurgery can affect the results of the procedure. If you are thinking about this type of treatment, it is important to keep in mind that best results are obtained by surgeons with specialized training and experience in reproductive microsurgery. After vasectomy reversal, sperm return to the semen in about 70-95% of men. Pregnancy without assisted reproductive technology occurs in 30-75% of couples. The chance for pregnancy depends on many factors, most importantly, the age and fertility status of the female partner and the number of years between the vasectomy and its reversal. The longer you wait to reverse a vasectomy, the less the chances are
9 Getting Help for Obstructive Azoospermia 9 for a successful reversal. Still, there is no magic number of years beyond which a reversal is certain to fail. Contrary to what is commonly believed, the chance for success with a vasectomy reversal does not suddenly decline after 10 years or after any other specific number of years. Microsurgical reconstruction is a 2-4 hour operation but it is often performed as an outpatient procedure. It is usually done under general anesthesia although it can be done with local anesthesia and intravenous sedation. This surgery causes only mild postoperative pain. Patients should expect to be out of work for 4-7 days. Transurethral Resection of the Ejaculatory Duct (TURED) This procedure can be used to treat ejaculatory duct obstruction. It involves passing a scope into the urethra and cutting into the ejaculatory ducts. Transurethral resection of the ejaculatory duct results in the appearance of sperm in the ejaculate in about 50-75% of men. Pregnancy rates following this surgery are about 25%. Transurethral resection of the ejaculatory duct requires general or spinal anesthesia. It can be done as an outpatient procedure or with just one night in the hospital. Postoperative pain is minimal. Some surgeons place a urinary catheter (drainage tube) in the bladder for a short time after this surgery. Patients should expect to be out of work for 1-3 days.
10 10 An AUA Doctor s Guide for Patients Should I Consider Sperm Retrieval With In Vitro Fertilization Rather Than Surgical Reconstruction? Intracytoplasmic sperm injection: advanced female age is present Intracytoplasmic sperm injection (ICSI) is the injection of a single sperm into a mature oocyte (egg). It is the form of in vitro fertilization (IVF) that must be used in almost all cases of obstructive azoospermia when sperm are removed from the testicle or epididymis. This is because the number of motile (active) sperm that can be obtained is small and only enough to do the ICSI technique rather than standard IVF. Using the ICSI technique, it is reasonable to expect that the chance to have a baby will be about 30% for each menstrual cycle in which ICSI is attempted. Sperm retrieval followed by ICSI is preferable to surgical treatment when: female factors requiring IVF are present sperm retrieval/icsi is the financially preferable option Sperm Retrieval: There are several methods of sperm retrieval. The choice of method depends mainly on the urologist who will perform the procedure and the laboratory performing the ICSI. Sperm retrieval may be performed prior to or simultaneously with the female partner s egg retrieval. Many reproductive centers prefer to use fresh sperm obtained on the same day as the egg retrieval, but others prefer to use sperm that have been previously harvested and frozen. Your doctor should explain the different techniques to you before you start.
11 Getting Help for Obstructive Azoospermia 11 For those whose azoospermia is due to obstruction, sperm retrieval can be accomplished by either a needle aspiration or microsurgical technique. Details of each procedure should be discussed with your physician. Are There Any Risks Associated With IVF/ICSI? There are some risks associated with this type of treatment for infertility. These risks include: Ovarian hyperstimulation. This is a risk to the female partner of the couple. It is due to the hormone stimulation in the IVF/ICSI process. In some women, the ovaries become over-stimulated by the hormones, causing high blood pressure, fluid accumulation (edema), malaise, weakness, and other symptoms. Mild ovarian hyperstimulation, which is easily tolerated, can occur in up to 20% of patients. Moderate ovarian hyperstimulation occurs in up to 5% of women undergoing IVF. Severe ovarian hyperstimulation, which can cause severe medical problems in addition to the failure of the ICSI, occurs in 1% of women undergoing IVF. Multiple gestations (births). In the U.S., there is a 30-35% risk for twin gestations and 5-10% for triplets (or higher) gestations. Multiple gestation births are associated with increased infant morbidity and mortality rates due primarily to prematurity. You and your partner may want to discuss the advantages and disadvantages of IVF/ICSI with your physician. Knowing as much as you can about these procedures can help you make the right choice.
12 12 An AUA Doctor s Guide for Patients Some Final Considerations Identifying and treating reversible conditions may improve the male partner s fertility and allow for conception through intercourse. Detection of conditions for which there is no cure will spare couples the distress of attempting ineffective therapies. Finding genetic causes of male infertility allows couples to be informed about the potential to transmit genetic problems to their offspring. Many complex factors go into the decision to use microsurgical reconstruction of the male reproductive system versus sperm retrieval with ICSI. Microsurgical reconstruction of the male reproductive system often is more cost-effective than sperm retrieval with IVF/ICSI. IVF/ICSI requires intervention in both male and female partners and is more expensive than microsurgical reconstruction in most centers. Microsurgical reconstruction allows couples to have subsequent children without additional medical treatment. On the other hand, there are situations in which sperm retrieval with IVF/ICSI is a better choice for you. For example, couples in whom there is both male and female factor infertility are usually better treated by sperm retrieval and ICSI. The fertility status of the female partner is another important consideration. For example, the woman s age is important. Although individuals vary greatly, a woman s fertility begins to decline after the age of about 35. This means that the chance for success with both microsurgical reconstruction and sperm retrieval with ICSI decreases with increasing female partner age, especially beyond age 37. It is important to understand that after a successful microsurgical vasectomy reversal, the average interval until pregnancy is about one year, while a successful ICSI cycle pregnancy occurs within 1-2 months of starting hormonal therapy. The choice of either sperm retrieval with IVF/ICSI or microsurgical reconstruction should also be influenced by the pregnancy rates achieved with ICSI by the IVF team with which you are working. The pregnancy rates of the surgeon who would perform reconstructive microsurgery should also influence your choice. In addition, the choice of treatment for obstructive azoospermia is impacted by the preferences of the couple, cost considerations, and the availability of specific medical expertise in the local community.
13 Getting Help for Obstructive Azoospermia 13
14 14 An AUA Doctor s Guide for Patients
15 For More Information The following list of organizations is intended as a resource for couples who would like more information. If you still have unanswered questions, need help finding a specialist, or need some emotional support, there are groups you can contact. Remember, there are many couples experiencing similar difficulties. Getting the support and education you need can save you both time and frustration. The more you know, the better decision you can make. American Society for Reproductive Medicine 1209 Montgomery Highway Birmingham, Alabama Phone: (205) Web: Reproductive Health Council c/o American Foundation for Urologic Disease 1128 North Charles Street Baltimore, MD Phone: (410) Fax: (410) Web: RESOLVE 1310 Broadway Somerville, MA National HelpLine: (617) Business Office: (617) Web: Society for the Study of Male Reproduction Executive Director: Wendy J. Weiser 1111 N. Plaza Dr. Suite 550 Schaumburg, IL Phone: (847) Fax: (847) Web:
16 16 An AUA Doctor s Guide for Patients This doctor s guide for patients is intended to stimulate and facilitate discussion between the patient and doctor regarding the types of evaluation and treatment described in summary fashion in this brochure. The brochure was developed by the Male Infertility Best Practice Policy Committee of the American Urological Association. It is based on the Report on Management of Obstructive Azoospermia, a document jointly developed by the American Urological Association and the American Society for Reproductive Medicine. Other Doctor Guides for Patients in this series include: A Basic Guide to Male Infertility: How to Find Out What s Wrong and A Basic Guide to Male Infertility: Answers to Your Questions About Varicoceles. This material may not be reproduced in electronic or other format without written permission of the AUA. For additional copies of this brochure physicians may contact: American Urological Association, Inc North Charles Street Baltimore, MD Phone: (410)
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
Male Reproductive System
 Male Reproductive System The male reproductive system consists of a number of sex organs that are part of the reproductive process. The following sections describe the function of each part of the male
Male Reproductive System The male reproductive system consists of a number of sex organs that are part of the reproductive process. The following sections describe the function of each part of the male
Treating Infertility
 Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
Chris Davies & Greg Handley
 Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Reversible Conditions Organising More Information semen analysis Male Infertility at Melbourne IVF Fertility Preservation
 Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
INTRACYTOPLASMIC SPERM INJECTION
 1 Background... 2 2 Male Factor Infertility... 2 3 ICSI... 3 4 Surgical sperm aspiration... 4 5 What is the chance of success?... 6 6 What are the risks?... 7 M Rajkhowa, October 2004 Authorised by V Kay
1 Background... 2 2 Male Factor Infertility... 2 3 ICSI... 3 4 Surgical sperm aspiration... 4 5 What is the chance of success?... 6 6 What are the risks?... 7 M Rajkhowa, October 2004 Authorised by V Kay
Information Sheet. Male Infertility
 Infertility National Public Awareness Campaign Information Sheet Male Infertility In approximately half of couples complaining of infertility part of the problem lies with the male. Male infertility has
Infertility National Public Awareness Campaign Information Sheet Male Infertility In approximately half of couples complaining of infertility part of the problem lies with the male. Male infertility has
Testicular Biopsy and Sperm Extraction for Fertility Preservation
 Testicular Biopsy and Sperm Extraction for Fertility Preservation This fact sheet aims to provide information about why and when a testicular biopsy or aspiration might be offered, what it involves and
Testicular Biopsy and Sperm Extraction for Fertility Preservation This fact sheet aims to provide information about why and when a testicular biopsy or aspiration might be offered, what it involves and
Reproductive system Presented by: Ms. Priya
 Reproductive system Presented by: Ms. Priya Reproductive system Female reproductive system has two functions: produce egg cells to protect and nourish the offspring (baby) until birth. Male reproductive
Reproductive system Presented by: Ms. Priya Reproductive system Female reproductive system has two functions: produce egg cells to protect and nourish the offspring (baby) until birth. Male reproductive
Male and Female Reproduction
 Male and Female Reproduction Similarities / Differences Develop very similar structures of sex glands Two genital tubes Manufacture the hormones of the other sex. Hormones of one sex are often used to
Male and Female Reproduction Similarities / Differences Develop very similar structures of sex glands Two genital tubes Manufacture the hormones of the other sex. Hormones of one sex are often used to
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Surgical Sperm Retrieval
 Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Reproductive System: Male
 Reproductive System Reproductive System: Male Produces new life Same types of organs for males and females Gonads, or sex glands Male organs located mainly outside of body Testes The male gonads Located
Reproductive System Reproductive System: Male Produces new life Same types of organs for males and females Gonads, or sex glands Male organs located mainly outside of body Testes The male gonads Located
Science and Health THE HUMAN REPRODUCTIVE SYSTEM
 5 Module 1 Science and Health THE HUMAN REPRODUCTIVE SYSTEM Male Female A DepEd-BEAM Distance Learning Program supported by the Australian Agency for International Development NOTICE Section 9 of the Presidential
5 Module 1 Science and Health THE HUMAN REPRODUCTIVE SYSTEM Male Female A DepEd-BEAM Distance Learning Program supported by the Australian Agency for International Development NOTICE Section 9 of the Presidential
UNDERSTANDING. Permanent Birth Control for Men
 UNDERSTANDING VASECTOMY Permanent Birth Control for Men Is Vasectomy for You? Vasectomy is a simple, safe procedure that makes a man sterile (unable to father a child). It s the most effective birth control
UNDERSTANDING VASECTOMY Permanent Birth Control for Men Is Vasectomy for You? Vasectomy is a simple, safe procedure that makes a man sterile (unable to father a child). It s the most effective birth control
A USER S GUIDE WHAT EVERY MAN NEEDS TO KNOW
 A USER S GUIDE WHAT EVERY MAN NEEDS TO KNOW 1. Why men need to know more Good health is vital for a happy and full life. But, with work and family responsibilities, men often overlook their own health
A USER S GUIDE WHAT EVERY MAN NEEDS TO KNOW 1. Why men need to know more Good health is vital for a happy and full life. But, with work and family responsibilities, men often overlook their own health
Infertility F REQUENTLY A SKED Q UESTIONS. Q: Is infertility a common problem?
 Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Information for Patients. Male infertility. English
 Information for Patients Male infertility English Table of contents What is male infertility?... 3 Diagnosis... 3 Medical history... 3 Physical examination... 3 Hormone blood tests... 3 Semen analysis...
Information for Patients Male infertility English Table of contents What is male infertility?... 3 Diagnosis... 3 Medical history... 3 Physical examination... 3 Hormone blood tests... 3 Semen analysis...
Chapter 16 Endocrine and Reproductive Health
 Note Taking Lesson 2 The Male Reproductive System Directions: Use the following outline to help organize your notes as you read through the lesson. Key Concept Consider and Reconsider Before reading the
Note Taking Lesson 2 The Male Reproductive System Directions: Use the following outline to help organize your notes as you read through the lesson. Key Concept Consider and Reconsider Before reading the
Topic 18- Human Reproductive System. Day 2-Female (and review of) Male Reproductive Systems
 Topic 18- Human Reproductive System Day 2-Female (and review of) Male Reproductive Systems Bell Ringer (5 minutes) Bioblitz WHAT ARE WE LEARNING TODAY? Date: 12/14-12/15 Topic: Human Reproductive System
Topic 18- Human Reproductive System Day 2-Female (and review of) Male Reproductive Systems Bell Ringer (5 minutes) Bioblitz WHAT ARE WE LEARNING TODAY? Date: 12/14-12/15 Topic: Human Reproductive System
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Human Growth and Development
 Human Growth and Development 6th Grade Male Click here for teacher notes Ground Rules Use proper terminology. (Do not use slang.) Participate seriously. Share today s information with your parents. (Do
Human Growth and Development 6th Grade Male Click here for teacher notes Ground Rules Use proper terminology. (Do not use slang.) Participate seriously. Share today s information with your parents. (Do
Adoption and Foster Care
 GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
How Long To Heal After Vasectomy Reversal Can You Have Intercourse
 How Long To Heal After Vasectomy Reversal Can You Have Intercourse The recovery after vasectomy reversal is very important. If you can have help for a week, so that other person can do all the lifting,
How Long To Heal After Vasectomy Reversal Can You Have Intercourse The recovery after vasectomy reversal is very important. If you can have help for a week, so that other person can do all the lifting,
When should I ask my doctor about my fertility?
 Preserving Fertility for Men with Cancer Some cancers and their treatments can affect a man s ability to father a child (his fertility). These changes can last for a short time, or may be permanent. This
Preserving Fertility for Men with Cancer Some cancers and their treatments can affect a man s ability to father a child (his fertility). These changes can last for a short time, or may be permanent. This
I would be happy to discuss all of these options for fertility after vasectomy with you at the time of our consultation or over the phone.
 F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
The Reproductive System
 16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
Chapter 14 The Reproductive System
 Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM
 Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Clinical Policy Committee
 Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
The Reproductive System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
THE PATIENT S GUIDE TO VASECTOMY REVERSAL
 The Basics of Vasectomy Reversal What is a Vasectomy? A vasectomy is a safe, simple, quick and effective method of contraception. As shown in Figure 1a, the testicles are continually producing sperm even
The Basics of Vasectomy Reversal What is a Vasectomy? A vasectomy is a safe, simple, quick and effective method of contraception. As shown in Figure 1a, the testicles are continually producing sperm even
Level I - Lesson 8: Know Your Body
 Level I - Lesson 8: Synopsis: This computer session will allow students to learn more about the human reproductive system and the changes their body will go through during puberty. Objectives: Students
Level I - Lesson 8: Synopsis: This computer session will allow students to learn more about the human reproductive system and the changes their body will go through during puberty. Objectives: Students
1. Both asexual and sexual reproduction occur in the animal kingdom
 1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur?
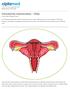 Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Outline OVERVIEW PUBERTY PRE-TESTS PUBERTY WITH SAM AND SALLY MENSTRUATION: HOW DOES IT WORK? SPERMATOGENESIS: HOW DOES IT WORK?
 UNIT FIVE: PUBERTY HiTOPS, Inc./Princeton Center for Leadership Training OVERVIEW PUBERTY PRE-TESTS Outline PUBERTY WITH SAM AND SALLY MENSTRUATION: HOW DOES IT WORK? SPERMATOGENESIS: HOW DOES IT WORK?
UNIT FIVE: PUBERTY HiTOPS, Inc./Princeton Center for Leadership Training OVERVIEW PUBERTY PRE-TESTS Outline PUBERTY WITH SAM AND SALLY MENSTRUATION: HOW DOES IT WORK? SPERMATOGENESIS: HOW DOES IT WORK?
Male Reproductive System
 21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
Human Growth and Development
 Human Growth and Development 5th Grade Male Click here for teacher notes Ground Rules Use proper terminology. (Do not use slang.) Participate seriously. Share today s information with your parents. (Do
Human Growth and Development 5th Grade Male Click here for teacher notes Ground Rules Use proper terminology. (Do not use slang.) Participate seriously. Share today s information with your parents. (Do
Female and Male Reproductive Systems
 Female and Male Reproductive Systems Reproductive System: Organs that make possible the production of offspring. Female Reproductive System Female Reproductive System: Words to be familiar with ESTROGEN
Female and Male Reproductive Systems Reproductive System: Organs that make possible the production of offspring. Female Reproductive System Female Reproductive System: Words to be familiar with ESTROGEN
Male Reproductive System. Anatomy
 Male Reproductive System Medical Terminology Chapter Seven HIT # 141 Anatomy Testis or testicle = main male sex organs, paired, oval shaped, enclosed in a sac called the scrotum. Seminiferous tubules =
Male Reproductive System Medical Terminology Chapter Seven HIT # 141 Anatomy Testis or testicle = main male sex organs, paired, oval shaped, enclosed in a sac called the scrotum. Seminiferous tubules =
Evaluation and Treatment of the Subfertile Male. Karen Baker, MD Associate Professor Duke University, Division of Urology
 Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Assisted Reproduction. By Dr. Afraa Mahjoob Al-Naddawi
 Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
INTRODUCTION TABLE OF CONTENTS. If you want to become a parent after cancer, we would like to give you the information you need to make that happen.
 TABLE OF CONTENTS INTRODUCTION INTRODUCTION 1 MEN Fertility Risks 2 Fertility Preservation Options 3 Possible Fertility Outcomes 4 Parenthood After Cancer Options 5 Important Tips for Men 6 WOMEN Fertility
TABLE OF CONTENTS INTRODUCTION INTRODUCTION 1 MEN Fertility Risks 2 Fertility Preservation Options 3 Possible Fertility Outcomes 4 Parenthood After Cancer Options 5 Important Tips for Men 6 WOMEN Fertility
PROCEDURES LAPAROSCOPY
 PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
Human Sexuality - Ch. 2 Sexual Anatomy (Hock)
 Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Fertility care for women diagnosed with cancer
 Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Fertility care for women diagnosed with cancer Contents Page Overview... 2 Our service... 2 Effects of cancer treatment
Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Fertility care for women diagnosed with cancer Contents Page Overview... 2 Our service... 2 Effects of cancer treatment
Growth and Development 6 th Grade
 Growth and Development 6 th Grade All living things reproduce. Our bodies change during puberty to make reproduction possible. This is not always fun But it is pretty amazing! PUBERTY is the process of
Growth and Development 6 th Grade All living things reproduce. Our bodies change during puberty to make reproduction possible. This is not always fun But it is pretty amazing! PUBERTY is the process of
Infertility treatment
 In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
Reproductive Technology, Genetic Testing, and Gene Therapy
 Michael Cummings Chapter 16 Reproductive Technology, Genetic Testing, and Gene Therapy David Reisman University of South Carolina 16.1 Infertility Is a Common Problem In the US, about 13% of all couples
Michael Cummings Chapter 16 Reproductive Technology, Genetic Testing, and Gene Therapy David Reisman University of South Carolina 16.1 Infertility Is a Common Problem In the US, about 13% of all couples
Clinical Policy Committee
 Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Cancer & Fertility: Patient Education Booklet. information suppor t hope
 Cancer & Fertility: Patient Education Booklet information suppor t hope 1 table of contents introduction 1 men Fertility Risks 2 Fertility Preservation Options 3 Possible Fertility Outcomes 4 Parenthood
Cancer & Fertility: Patient Education Booklet information suppor t hope 1 table of contents introduction 1 men Fertility Risks 2 Fertility Preservation Options 3 Possible Fertility Outcomes 4 Parenthood
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Committee Paper SCAAC(05/09)01. ICSI guidance. Hannah Darby and Rachel Fowler
 Committee Paper Committee: Scientific and Clinical Advances Advisory Committee Meeting Date: 12 May 2009 Agenda Item: 4 Paper Number: SCAAC(05/09)01 Paper Title: ICSI guidance Author: Hannah Darby and
Committee Paper Committee: Scientific and Clinical Advances Advisory Committee Meeting Date: 12 May 2009 Agenda Item: 4 Paper Number: SCAAC(05/09)01 Paper Title: ICSI guidance Author: Hannah Darby and
Lecture Series: Pregnancy
 Lecture Series: Pregnancy Stephanie Mitelman, MA, CSE Certified Sexuality Educator Teacher's Notes Information Slides Review Quiz 1 Teacher's Notes Welcome! These slides will help you teach your class
Lecture Series: Pregnancy Stephanie Mitelman, MA, CSE Certified Sexuality Educator Teacher's Notes Information Slides Review Quiz 1 Teacher's Notes Welcome! These slides will help you teach your class
The Repr duct ve System. Function: producing offspring
 The Repr duct ve System Function: producing offspring Anatomy of male reproductive system Location: The reproductive organs are classified as external and internal genitalia. The external genitalia are
The Repr duct ve System Function: producing offspring Anatomy of male reproductive system Location: The reproductive organs are classified as external and internal genitalia. The external genitalia are
What are Varicoceles?
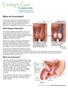 What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
Male Fertility: Your Questions Answered
 Male Fertility: Your Questions Answered Michael S. Neal Scientific Director, ONE Fertility, 3210 Harvester Rd. Burlington, Ontario www.onefertility.com mneal@onefertility.com Outline Assisted Conception
Male Fertility: Your Questions Answered Michael S. Neal Scientific Director, ONE Fertility, 3210 Harvester Rd. Burlington, Ontario www.onefertility.com mneal@onefertility.com Outline Assisted Conception
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproduction. Male & Female Systems & Menstration
 Human Reproduction Male & Female Systems & Menstration Make a Sperm & Ovum Female Mons Pubis Labia Urethra Perineum Vagina Cervix Uterus Endometrium Fallopian tubes Ovaries Ovum Male Scrotrum Testicle
Human Reproduction Male & Female Systems & Menstration Make a Sperm & Ovum Female Mons Pubis Labia Urethra Perineum Vagina Cervix Uterus Endometrium Fallopian tubes Ovaries Ovum Male Scrotrum Testicle
Chapter 7. Male Reproductive System
 Chapter 7 Male Reproductive System 1 Sexual Reproduction Sexual reproduction two individuals produce offspring that have genetic characteristics from both parents Sexual reproduction introduces new gene
Chapter 7 Male Reproductive System 1 Sexual Reproduction Sexual reproduction two individuals produce offspring that have genetic characteristics from both parents Sexual reproduction introduces new gene
FEMALE REPRODUCTIVE SYSTEM
 FEMALE REPRODUCTIVE SYSTEM UTERUS (made up of muscular walls, a lining called the endometrium, and a cervix. The uterus is also called womb ) houses and protects embryo/fetus/baby allows nutrient & waste
FEMALE REPRODUCTIVE SYSTEM UTERUS (made up of muscular walls, a lining called the endometrium, and a cervix. The uterus is also called womb ) houses and protects embryo/fetus/baby allows nutrient & waste
Male Reproductive System Dr. Gary Mumaugh
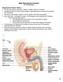 Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
SpermComet DNA Test your results and what they mean
 SpermComet DNA Test your results and what they mean Sperm DNA damage and why it is important for your fertility. You and your partner are each going to give some of your DNA to your baby, so the health
SpermComet DNA Test your results and what they mean Sperm DNA damage and why it is important for your fertility. You and your partner are each going to give some of your DNA to your baby, so the health
The beginning of puberty is marked by the progressive increase in the production of sex hormones.
 Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Planning for Parenthood After a Cancer Diagnosis
 Cancer and Fertility Planning for Parenthood After a Cancer Diagnosis If you or someone you love is facing cancer, preserving fertility may be the last thing on your mind. But if you re a woman of childbearing
Cancer and Fertility Planning for Parenthood After a Cancer Diagnosis If you or someone you love is facing cancer, preserving fertility may be the last thing on your mind. But if you re a woman of childbearing
6.7 IN. Continuity through Reproduction. What are the differences between male and female gametes? Discuss their formation and physical attributes.
 6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
describe the parts and function of semen and the glands that contribute to it
 You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
Student Academic Learning Services Page 1 of 5 Reproductive System Practice
 Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
INFERTILITY. Services - Part 2
 INFERTILITY Services - Part 2 1 Imprint Published in January, 2013 By Victory A.R.T. Laboratory Phils, Inc. These articles were compiled by in hopes of helping bring into light infertility questions and
INFERTILITY Services - Part 2 1 Imprint Published in January, 2013 By Victory A.R.T. Laboratory Phils, Inc. These articles were compiled by in hopes of helping bring into light infertility questions and
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal
 What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
Appendix D Answers to the KAP Survey
 From Trainer s Resource Book to accompany Management of Men s Reproductive Health Problems 2003 EngenderHealth Appendix D Answers to the KAP Survey In the answer key that follows: The answers appear in
From Trainer s Resource Book to accompany Management of Men s Reproductive Health Problems 2003 EngenderHealth Appendix D Answers to the KAP Survey In the answer key that follows: The answers appear in
INDICATIONS OF IVF/ICSI
 PROCESS OF IVF/ICSI INDICATIONS OF IVF/ICSI IVF is most clearly indicated when infertility results from one or more causes having no other effective treatment; Tubal disease. In women with blocked fallopian
PROCESS OF IVF/ICSI INDICATIONS OF IVF/ICSI IVF is most clearly indicated when infertility results from one or more causes having no other effective treatment; Tubal disease. In women with blocked fallopian
Why Reproduce? In order to ensure the continuation of the species and the continuation of life in general by producing offspring
 HUMAN REPRODUCTION Why Reproduce? In order to ensure the continuation of the species and the continuation of life in general by producing offspring Asexual vs Sexual Reproduction Remember: Asexual reproduction:
HUMAN REPRODUCTION Why Reproduce? In order to ensure the continuation of the species and the continuation of life in general by producing offspring Asexual vs Sexual Reproduction Remember: Asexual reproduction:
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Chapter 22 Reproductive Systems. Male Reproductive Organs. Male Reproductive Organs. Specialized to produce, maintain the male sex cells (sperm)
 Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
Grade 9 Science - Human Reproduction
 Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Assisted Reproductive Technologies
 Assisted Reproductive Technologies Textbook pages 224 231 Section 6.3 Summary Before You Read What do you think the phrase test-tube baby refers to? Write your ideas on the lines below. Mark the Text Check
Assisted Reproductive Technologies Textbook pages 224 231 Section 6.3 Summary Before You Read What do you think the phrase test-tube baby refers to? Write your ideas on the lines below. Mark the Text Check
Female and Male Reproductive Systems
 Female and Male Reproductive Systems Reproductive System: Organs that make possible the production of offspring. Female Reproductive System: Produces the female sex hormones Provides female reproductive
Female and Male Reproductive Systems Reproductive System: Organs that make possible the production of offspring. Female Reproductive System: Produces the female sex hormones Provides female reproductive
Health Science: the structures & functions of the reproductive system
 Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Sperm Donation - Information for Donors
 Sperm Donation - Information for Donors The donation of sperm to help someone to have a child is one of the most generous gifts anyone can give. Many donors feel a sense of pride, knowing the joy they
Sperm Donation - Information for Donors The donation of sperm to help someone to have a child is one of the most generous gifts anyone can give. Many donors feel a sense of pride, knowing the joy they
 Page 1 of 5 Official reprint from UpToDate www.uptodate.com 2012 UpToDate Patient information: Infertility in men (The Basics) Written by the doctors and editors at UpToDate What is male infertility? Male
Page 1 of 5 Official reprint from UpToDate www.uptodate.com 2012 UpToDate Patient information: Infertility in men (The Basics) Written by the doctors and editors at UpToDate What is male infertility? Male
Biology of fertility control. Higher Human Biology
 Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
Body Wise. Living, Growing, Learning Boys Only
 Body Wise Living, Growing, Learning Boys Only So what have we learned so far? Remember the rules This may be embarrassing and cause you to laugh but compose yourself quickly Female Reproductive System
Body Wise Living, Growing, Learning Boys Only So what have we learned so far? Remember the rules This may be embarrassing and cause you to laugh but compose yourself quickly Female Reproductive System
Transformation Information elearning Kit Combined Program Lesson Plan Page 1. LESSON TITLE: Combined Program
 Page 1 LESSON TITLE: LESSON DESCRIPTION: In this animated activity, students will go more in depth about changes that happen to both males and females during puberty. The Coach re-introduces Ted Testosterone,
Page 1 LESSON TITLE: LESSON DESCRIPTION: In this animated activity, students will go more in depth about changes that happen to both males and females during puberty. The Coach re-introduces Ted Testosterone,
Unit 8: Human Sexuality
 Unit 8: Human Sexuality Adolescence is the time when young people go through the, emotional, and social changes that end in adulthood. refers to the physical changes that occur during adolescence. During
Unit 8: Human Sexuality Adolescence is the time when young people go through the, emotional, and social changes that end in adulthood. refers to the physical changes that occur during adolescence. During
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition
 Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition Patient Name (please print) Patient DOB (MM/DD/YYYY) Patient eivf number Partner
Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition Patient Name (please print) Patient DOB (MM/DD/YYYY) Patient eivf number Partner
TESE: Testis Sperm Extraction
 TESE: Testis Sperm Extraction Robert D. Oates, M.D., F.A.C.S. Department of Urology Boston University School of Medicine When is Microsurgical TESE indicated? Cases of Non-obstructive Azoospermia (NOA)
TESE: Testis Sperm Extraction Robert D. Oates, M.D., F.A.C.S. Department of Urology Boston University School of Medicine When is Microsurgical TESE indicated? Cases of Non-obstructive Azoospermia (NOA)
Female Reproduction. Ova- Female reproduction cells stored in the ovaries
 Reproduction Puberty stage of growth and development where males and females become capable of producing offspring. Time of physical and emotional changes. Female *occurs between ages 8 -- 15 *estrogen
Reproduction Puberty stage of growth and development where males and females become capable of producing offspring. Time of physical and emotional changes. Female *occurs between ages 8 -- 15 *estrogen
Produce Eggs. Fertility Preservation for Trans People who. LGBTQ Reproductive Options
 for Trans People who Produce Eggs LGBTQ Reproductive Options Many trans people are interested in being parents and want to know their options. While many trans people may conceive on their own, this info
for Trans People who Produce Eggs LGBTQ Reproductive Options Many trans people are interested in being parents and want to know their options. While many trans people may conceive on their own, this info
Reproductive System. Where it all begins
 Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
Preoperative Consultation
 Easy Vasectomy Reversal A vasectomy reversal is a microsurgical procedure that reconnects the vas deferens where it was interrupted by a vasectomy. Although vasectomy has historically been considered a
Easy Vasectomy Reversal A vasectomy reversal is a microsurgical procedure that reconnects the vas deferens where it was interrupted by a vasectomy. Although vasectomy has historically been considered a
Structure and Function
 Section 2 Objectives ~ Describe three functions of the male reproductive system. ~ Identify five ways to keep the male reproductive system healthy. Vocabulary sperm fertilization testes testosterone scrotum
Section 2 Objectives ~ Describe three functions of the male reproductive system. ~ Identify five ways to keep the male reproductive system healthy. Vocabulary sperm fertilization testes testosterone scrotum
FERTILITY & TCM. On line course provided by. Taught by Clara Cohen
 FERTILITY & TCM On line course provided by Taught by Clara Cohen FERTILITY & TCM FERTILITY AND TCM THE PRACTITIONER S ROLE CAUSES OF INFERTILITY RISK FACTORS OBJECTIVES UNDERSTANDING TESTS Conception in
FERTILITY & TCM On line course provided by Taught by Clara Cohen FERTILITY & TCM FERTILITY AND TCM THE PRACTITIONER S ROLE CAUSES OF INFERTILITY RISK FACTORS OBJECTIVES UNDERSTANDING TESTS Conception in
European IVF Monitoring (EIM) Year: 2012
 European IVF Monitoring (EIM) Year: 2012 Name of the country Poland Name and full address of the contact person. Professor Rafal Kurzawa, MD PhD Wojska Polskiego 103 Street 70-483 Szczecin Poland Telephone
European IVF Monitoring (EIM) Year: 2012 Name of the country Poland Name and full address of the contact person. Professor Rafal Kurzawa, MD PhD Wojska Polskiego 103 Street 70-483 Szczecin Poland Telephone
MALE SEXUAL SYSTEM ~::> bladder penis prostate gland scrotum seminal vesicle testicle urethra vas deferens ;:; . l0\ OJ IQ) I"- ...
 MALE SEXUAL SYSTEM 8 7 7 8. l0\... OJ '" ~ IQ) I"- cr su::> >. ~::> "0 ~
MALE SEXUAL SYSTEM 8 7 7 8. l0\... OJ '" ~ IQ) I"- cr su::> >. ~::> "0 ~
WHAT IS A PATIENT CARE ADVOCATE?
 WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
