Spermatogonial proliferation and apoptosis in hypospermatogenesis associated with nonobstructive azoospermia
|
|
|
- Leon Jasper Mason
- 6 years ago
- Views:
Transcription
1 FERTILITY AND STERILITY VOL. 76, NO. 5, NOVEMBER 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Spermatogonial proliferation and apoptosis in hypospermatogenesis associated with nonobstructive azoospermia Seiji Takagi, M.D., Naoki Itoh, M.D., Makoto Kimura, M.D., Takumi Sasao, M.D., and Taiji Tsukamoto, M.D. Department of Urology, Sapporo Medical University School of Medicine, Sapporo, Japan Objective: To provide evidence that a pathological process in spermatogonial proliferation and apoptosis may participate in developing hypospermatogenesis of infertile men. Design: Case-controlled retrospective analysis. Setting: University-based male infertility clinic. Patient(s): Thirty-four patients with idiopathic hypospermatogenesis. Intervention(s): Collecting blood samples for measurement of hormones and performing testicular biopsy for assessment of spermatogenesis. Main Outcome Measure(s): The expression of proliferating cell nuclear antigen (PCNA) of spermatogonia and the frequency of apoptosis of spermatogonia demonstrated by the in situ DNA 3 -end labeling method were investigated to determine the degree of cell degeneration. Result(s): We could classify 34 infertile patients into four subgroups according to spermatogonial proliferation and differentiation. No significant difference in the expression of PCNA was demonstrated between these four groups and the control group. In all groups, the balance of spermatogonial proliferation (PCNApositive rate) to apoptosis was significantly lower than that of the control group. Conclusion(s): It was demonstrated that accelerated apoptosis, rather than proliferative dysfunction in the mitotic phase, may induce the decreased number of spermatogonia in hypospermatogenesis. These findings suggest that disorders of the control and regulation of apoptosis may participate in the pathogenesis of idiopathic hypospermatogenesis. (Fertil Steril 2001;76: by American Society for Reproductive Medicine.) Key Words: Spermatogonia, cell proliferation, apoptosis, hypospermatogenesis Received January 23, 2001; revised and accepted May 4, Reprint requests: Naoki Itoh, M.D., Department of Urology, Sapporo Medical University School of Medicine, S-1, W-16, Chuo-ku, Sapporo , Japan (FAX: ; nitoh@sapmed.ac.jp) /01/$20.00 PII S (01) The etiology of idiopathic hypospermatogenesis has not been fully clarified. Many factors may affect this disorder so that clinically effective treatments are limited for infertile males with idiopathic hypospermatogenesis. Elucidating the causes and pathogenesis of hypospermatogenesis may be helpful in improving the outcome of the treatment for these patients. Spermatogenesis is one of the most elaborate processes of cell differentiation. The first process of spermatogenesis is spermatogonial proliferation for the maintenance of the cells as stem cells that can enter the cycle of the spermatogenetic process resulting in the production of spermatozoa. Throughout adult life, spermatogonial stem cells furnish cells for maturation in a cyclic pattern, at the same time renewing them to maintain a constant reservoir so as to produce spermatozoa continuously. The second process of spermatogenesis is differentiation of spermatogonia to spermatozoa with a meiotic phase and spermiogenesis. The role of spermatogonial proliferation in spermatogenesis has been extensively studied in a variety of experimental conditions, including during chemotherapy and irradiation therapy (1 3). These studies demonstrated that the recovery of spermatogenesis depends on the degree of stem cell killing. For the recovery of spermatogenesis from these conditions, a selfrenewing capacity of spermatogenesis is required to restore the cell populations and differentiating divisions to produce cells developing 901
2 into spermatozoa (1). However, the role of spermatogonial proliferation in infertile men has not yet been studied. The histological findings of testicular biopsy specimens of patients with idiopathic hypospermatogenesis demonstrate various patterns. It was suspected that some of the patients had a decrease of the spermatogonial population, suggested by a proliferative disorder during the first period of spermatogenesis. Therefore, in the current study, we hypothesized that a disorder of spermatogonial proliferation might be one of the causes of hypospermatogenesis in infertile males. To clarify this hypothesis, we investigated spermatogonial apoptosis as one of the causes of the decreased number of spermatogonia in patients with idiopathic hypospermatogenesis. Generally, a balance between cell proliferation and cell death determines the cell number (4). Not only an increment of spermatogonial death but also a decline of their proliferative activity may be involved in disturbance of their balance, resulting in hypospermatogenesis. Therefore, we investigated the expression of proliferating cell nuclear antigen (PCNA) of spermatogonia as an index of the proliferative activity (5), as well as the frequency of apoptosis of spermatogonia by in situ DNA 3 -end labeling to determine the degree of cell degeneration (6). By analyzing both proliferation and apoptosis of spermatogonia in infertile men, we found that an imbalance between cell proliferation and apoptosis of spermatogonia may partly cause impaired spermatogenesis. MATERIALS AND METHODS Subjects The subjects consisted of 61 Japanese patients with either azoospermia or severe oligozoospermia. Patients who had a medical history that included mumps orchitis, cryptorchism, receiving chemotherapy or irradiation therapy, genital tract infections, childhood inguinal herniorrhaphy, or pelvic surgery were excluded from this study. Patients with varicocele testis and hypogonadotropic hypogonadism were also excluded. All patients underwent testicular biopsies for assessment of spermatogenesis at our hospital after being informed of the benefits and risks of the procedure. These biopsies were performed from 1990 to At that time, we did not have an institutional review board in our hospital. We fully informed patients of all possibilities of the use of a part of these specimens for research. In addition, an initial overall histological evaluation allowed us to exclude from the study those specimens of 27 patients featuring seminiferous tubules with Sertoli cells only and maturation arrest, leaving 34 infertile men evaluable. Twenty-one additional patients who underwent a vasoreconstruction operation and testicular biopsy for obstructive azoospermia served as a control group in this study. Physical examination, semen analysis, and hormonal examination were performed in all patients. Seminal parameters of each subject were examined on two different occasions. Sperm concentration was estimated by using a Makler counting chamber (7). Serum was collected for the analyses of LH, FSH, and total T. Plasma LH and FSH levels were determined with an immunoradiometric assay system (LH: normal, 1.8 to 5.2 miu/ml; FSH: normal, 2.9 to 8.2 miu/ ml) (8). Intra-assay and interassay coefficients of variation in LH and FSH measurements were as follows: LH (intraassay), 1.54%; LH (interassay), 3.29%; FSH (intra-assay), 1.03%; FSH (interassay), 0.37%. The plasma total T concentration was determined by radioimmunoassay (normal, ng/ml). Intra-assay and interassay coefficients of variation in T were 3.2% and 5.5%, respectively. Blood was sampled on two different occasions between 10:00 and 12:00 AM. Mean values were used. Histological Examination of Spermatogenesis The biopsy specimens were fixed in Bouin s solution for 2 hours and in 10% neutral buffered formalin for 2 4 hours, embedded in paraffin, and stained with hematoxylin and eosin. We quantitatively analyzed 20 seminiferous tubules of a round cross-section selected at random per specimen by light microscopy. All germ cells and Sertoli cells were counted in each cross-section of the tubules. Germ cells were classified as spermatogonia (dark type A, pale type A, type B), primary spermatocytes (preleptotene, leptotene, zygotene, pachytene), round spermatids (secondary spermatocyte, Sa and Sb1 spermatid) and elongated spermatids (Sb2, Sc, and Sd spermatid). Immunohistochemical Staining of PCNA and In Situ TUNEL Staining Sections (5 m) were immunostained with an anti-pcna antibody (DAKO, Copenhagen, Denmark) by using the avidin-biotin method, followed by counterstaining with hematoxylin (5). The numbers of PCNA-positive spermatogonia and all spermatogonia were counted in 20 seminiferous tubules per specimen. The number of PCNA-positive spermatogonia per the total number of total spermatogonia was defined as the PCNA-positive rate. Terminal deoxy-nucleotidyl transferase-mediated digoxigenin-dutp nick-end labeling (TUNEL) was performed on formalin-fixed 5- m sections of specimens using an ApopTag Plus kit (Oncor, Gaithersburg, MD). In brief, digoxigenin-dutp end-labeled DNA was detected with an anti-digoxigenin-peroxidase antibody followed by peroxidase detection with 0.05% diaminobenzidine (DAB) and 0.02% H 2 O 2 (6). The numbers of apoptotic spermatogonia and all spermatogonia were counted in 20 seminiferous tubules per specimen. The number of apoptotic spermatogonia per weaning the total number spermatogonia was defined as the apoptotic rate. As the positive control for TUNEL assay, rat mammary glands obtained at the 4th day after weaning were used. Coefficients of variation of intra-assay and interassay for TUNEL assay were 6.3% and 11.9%, respectively. 902 Takagi et al. Spermatogonial proliferation and apoptosis Vol. 76, No. 5, November 2001
3 FIGURE 1 Four groups of infertile males classified by two criteria with quantitative analyses of spermatogenesis. The criteria consisted of the ratio of spermatogonia per Sertoli cell, used as an index of capability of spermatogonial proliferation, and the ratio of the number of spermatids to the number of spermatogonia, used as an index of capability of spermatogonial differentiation into spermatids. Statistical Analysis The StatView statistical analysis program (Abacus Concept, Inc., Berkeley, CA) was used to analyze all data. The Mann-Whitney U test and one-way analysis of variance (ANOVA) were used for statistical analyses. Statistically significant differences were confirmed when the P value was.05. For ANOVA, significant differences were evaluated by using the Turkey-Kramer honestly significant difference test for multiple comparisons. RESULTS Classifying Infertile Patients into Four Groups by Quantitative Analyses of Spermatogenesis We tried to classify infertile patients into four groups by quantitative analyses of spermatogenesis based on cell proliferation and differentiation. First, to determine which patients suffered from a disorder of proliferation of spermatogonia, we divided infertile patients into two major groups, depending on the ratio of spermatogonia per Sertoli cell (spermatogonia/sertoli cells/tubules) that was used as an index of capability for spermatogonial proliferation. In the control group, the mean 2SD of the ratio of spermatogonia to each Sertoli cell was 0.92, so that a ratio of 0.92 was defined as normal. Of 34 infertile patients, 17 patients had a decreased ratio of spermatogonia per Sertoli cell, compared with the control. Second, to distinguish which patients had a differentiation disturbance from spermatogonia to elongated spermatids, the two major groups were further classified into two groups each by the ratio of the number of elongated spermatids to the number of spermatogonia. The mean 2SD of this ratio was 0.61 in the control group, so that a ratio of 0.61 was defined as normal. Consequently, infertile males were classified into four groups using two parameters, the ratio of spermatogonia per Sertoli cell (cell proliferation) and the ratio of elongated spermatids to spermatogonia (cell differentiation; Fig. 1). Group A consisted of 9 patients with reduction in both the ratio of spermatogonia per Sertoli cell and the spermatid/ spermatogonia ratio. Group B included 8 patients, who had only a decreased ratio of spermatogonia per Sertoli cell. In group C, 7 patients had only a decreased spermatid/sper- FERTILITY & STERILITY 903
4 TABLE 1 The ratios of each germ cell number to Sertoli cell number in seminiferous tubules in the four groups and control. Group (No.) Spermatogonia Primary spermatocytes Round spermatids Elongated spermatids A (9) * * * * B (8) * * * C (7) * D (10) * * Control (21) * Note: All values are expressed as mean SD. Statistical analyses were performed by the Turkey-Kramer honestly significant difference test for multiple comparison. Statistical difference is indicated by different superscripts and was determined when the P value was.05. matogonia ratio. Group D consisted of 10 patients who had both a normal ratio of spermatogonia per Sertoli cell and spermatid/spermatogonium ratio. In brief, patients of group A had disorders in both spermatogonial proliferation and differentiation. Groups B and C had impairment in either spermatogonial differentiation (group B) or differentiation (group C). In patients of group D, spermatogonial proliferation and differentiation potential were maintained. The Degree of Spermatogenesis and Clinical Features of Infertile Men The ratios of each type of germ cell per Sertoli cell in the four groups are shown in Table 1. Infertile males were mostly classified equally into four groups according to our definitions. This finding indicated that the causes of hypospermatogenesis were heterogenous. Some patients had a disorder of spermatogonial proliferation or deterioration of spermatogonial differentiation, but others had both. For instance, in the patients of group B, the ratio of spermatogonia per Sertoli cell was significantly decreased according to this classification. However, both those of elongated and round spermatids were significantly higher in this group than in groups A and C (Table 1). In group C, numbers of spermatogonia were in the normal range; however, all germ cells after spermatogonia were significantly diminished, suggesting the impairment of spermatogonial differentiation. To compare clinical backgrounds among the four groups, several clinical findings, such as age, testicular size, parameters of semen analysis, and hormonal analysis are represented in Table 2. There was no significant difference in age distribution between any group and the control group. Testicular size of patients of group A was significantly smaller than that of the control group. Serum LH and FSH levels were elevated in the patients of group A. There was no significant difference in the hormonal analysis between group B and the control group. A significant elevation (P.05) of the serum FSH level was found in group C. In group D, serum LH and FSH levels were normal; however, the serum T level was significantly elevated compared with that of the control. Proliferating Cell Nuclear Antigen-Positive Rate and Apoptotic Rate in Hypospermatogenesis Spermatogonia and primary spermatocytes were stained positively with the anti-pcna antibody. The label was confined to the nucleus (Fig. 2). There was no significant difference in the PCNA-positive rate among infertile males and normal controls (Table 3). TABLE 2 Comparison of clinical characteristics of the four groups of infertile men. Group Age Testis volume (ml) Sperm density (per ml 10 6 ) Sperm motility (%) LH (IU/L) FSH (IU/L) T (ng/ml) A b b b B C a D a Control (azoospermia) Note: All values are expressed as mean SD. a P.05 vs. control group. b P.01 vs. control group. 904 Takagi et al. Spermatogonial proliferation and apoptosis Vol. 76, No. 5, November 2001
5 FIGURE 2 Immunostaining of PCNA in testicular biopsy specimens obtained from infertile patients. (Original magnification, 400). Spermatogonia and a few primary spermatocytes were stained positively. FIGURE 3 TUNEL-stained testicular biopsy specimens. (Original magnification, 400). A few spermatogonia within the basal compartment were stained positively. FERTILITY & STERILITY 905
6 TABLE 3 Comparison of PCNA-positive rate, apoptotic rate, and PCNA-positive rate per apoptotic rate in four infertile groups. Group PCNA-positive rate (%) Apoptotic rate (%) PCNA-positive rate/apoptotic rate A * * B C D * * Control * * Note: All values are expressed as mean SD. Statistical analyses were performed by the Turkey-Kramer honestly significant difference test for multiple comparison. Statistical difference is indicated by different superscripts and was determined when the P value was.05. The in situ end-labeling method detected apoptotic cells. The cells were identified as spermatogonia and, rarely, as primary spermatocytes (Fig. 3). The apoptotic rate was significantly elevated in group A compared with the cases of group D and the control (Table 2). The ratios of the PCNApositive rate to the apoptotic rate were analyzed as an index of the balance between cell proliferation and apoptosis of spermatogonia. The ratios in all four groups of infertile males were significantly higher than in normal controls. Group A had a significantly higher rate compared with group D. However, no other significant difference among groups was recognized (Table 3). DISCUSSION The causes of idiopathic hypospermatogenesis seem to be heterogeneous. The constant maintenance of the proliferation of spermatogonial stem cells during the first step of spermatogenesis is indispensable for maintaining the constant production of spermatozoa. However, the clinical implications of spermatogonial proliferation have not been fully studied in infertile men. Our study revealed that among 34 infertile patients with idiopathic hypospermatogenesis, there were 8 (23.5%) unique patients (group B) who had a decreased spermatogonial population suggesting a disorder of spermatogonial proliferation but who had almost normal differentiation in spermatogenesis subsequent to spermatogonial proliferation. The normal differentiation of spermatogenesis in those 8 was supported by evidence that they did not show any elevation of the serum FSH level. In contrast, 17 patients (groups A and C) who had a disturbance of differentiation as determined by their elongated spermatid/spermatogonium ratio showed abnormal elevation of serum FSH, indicating severe Sertoli cell dysfunction. Therefore, we investigated the cause of the decreased number of spermatogonia in patients with idiopathic hypospermatogenesis. Generally, a balance between cell proliferation and cell death determines the control of cell number (4). In patients with a decreased number of spermatogonia, this balance might be relatively inclined toward cell death. We speculated that proliferative dysfunction in the mitotic phase or accelerated germ-cell death might be one of the causes of this decrease. Therefore, we tried to assess both proliferative activity and the frequency of apoptosis of spermatogonia in infertile men, using immunohistochemistry. To our knowledge, there is no report on investigation of both proliferative activity and the frequency of apoptosis for spermatogenesis in humans. When we studied the proliferative dysfunction or accelerated apoptosis as a cause of the decreased number of spermatogonia, the results demonstrated a significant difference for the apoptotic index only between group A and the control group. Moreover, when we focused on the balance between cell proliferation and apoptosis of spermatogonia, this balance in all four groups was strongly inclined toward apoptosis. On the basis of these observations, it was suggested that an elevated apoptotic rate of spermatogonia may have a more crucial role than a decrease of spermatogonial proliferation as one of causes of hypospermatogenesis. Of course, not only spermatogonial apoptosis but also other factors may be involved in defective spermatogenesis. Moreover, the accelerated spermatogonial apoptosis might be a result, not a cause, of defective testicular tissue. Recently, using molecular cell biology techniques, many genes and proteins were found to be expressed in each process of spermatogenesis. Among them, the c-kit protoncogene that encodes for transmembrane protein receptors has been demonstrated to be important for germ cell migration, development, and maturation (9). Yoshinaga et al. (10) demonstrated that blocking the c-kit receptor in mice would cause sterility by preventing the proliferation of the stem cells necessary for spermatogenesis. Although group B patients in this study had normal expression of PCNA as assessed for proliferative activity, other factors such as c-kit and stem cell factor, which may participate in the regulation 906 Takagi et al. Spermatogonial proliferation and apoptosis Vol. 76, No. 5, November 2001
7 of proliferation of spermatogonia themselves, may affect the number of spermatogonia. Recent evidence suggests that alterations in apoptosis contribute to the pathogenesis of a number of human diseases, including cancer, viral infections, autoimmune diseases, and neurodegenerative disorders (11). In the testis, germ cell apoptosis occurs during normal spermatogenesis and continuously throughout life (12). The regulation of apoptosis appears to play an important role during normal spermatogenesis. Accelerated germ cell apoptosis has been observed in a variety of experimental conditions, such as those after irradiation (13), toxicant exposures (14), gonadotropin-releasing hormone antagonist treatment (15), heat stress (16), and mild hypothermia (17). More recently, Lin et al. (18) demonstrated that increased apoptosis occurred in maturation arrest and hypospermatogenesis in infertile men. These histological findings resemble those of group A in our study. These results suggested that accelerated apoptosis may participate in the pathogenesis of idiopathic hypospermatogenesis in some infertile patients. However, the control and mechanisms of apoptosis in spermatogenesis have not been elucidated. Experimental models of disorders of regulation of apoptosis have been reported. Several of them used transgenic mice overexpressing bcl-2 and others that were bax-deficient and which developed male infertility as a result of disordered seminiferous tubules with an accumulation of atypical premeiotic germ cells but no mature spermatozoa (19, 20). To investigate whether these genes and proteins associated with apoptosis participate in spermatogenesis may help to elucidate the pathogenesis of idiopathic hypospermatogenesis. Although clinically effective treatments for males with idiopathic hypospermatogenesis are limited, Foresta et al. (21) reported that FSH treatment increases the spermatogonial population in men who have normal FSH levels and a testicular histology characterized by hypospermatogenesis without maturational disturbance. The responders to FSH treatment in their report appear to resemble group B patients in our study, who had normal FSH levels and a decreased spermatogonial population without maturational disturbance. Experimentally, the number of pale type A spermatogonia could be increased by FSH treatment in the monkey (22). Appropriate patient selection may lead to a satisfactory outcome with FSH treatment. In conclusion, we demonstrated for the first time that some infertile males have a disorder of differentiation of spermatogonial stem cells. Accelerated apoptosis, rather than proliferative dysfunction in the mitotic phase, may induce the decreased number of spermatogonia in these patients. These findings suggest that disorders of the control and regulation of apoptosis may participate in the pathogenesis of idiopathic hypospermatogenesis. Elucidating the mechanism and regulation of apoptosis in spermatogenesis may help to resolve at least some problems in the pathogenesis of male infertility. References 1. Meistrich ML. Effects of chemotherapy and radiotherapy on spermatogenesis. Eur Urol 1993;23: Bustos-Obregon E, Rodriguez H. Testicular x-ray irradiation in adult mice as a model to study spermatogonial proliferation. Andrologia 1991;23: Judas L, Bentzen SM, Hansen PV, Overgaard J. Proliferative response of mouse spermatogonial stem cells after irradiation: a quantitative model analysis of experimental data. Cell Prolif 1996;29: Raff MC. Social controls on cell survival and cell death. Nature 1992;356: Hall PA, Levison DA. Review: assessment of cell proliferation in histological material. J Clin Pathol 1990;43: Gavrieli Y, Sherman Y, Ben-Sasson SA. Identification of programmed cell death in situ via specific labeling of nuclear DNA fragmentation. J Cell Biol 1992;119: Makler A. A new chamber for rapid sperm count and motility estimation. Fertil Steril 1978;30: Itoh N, Kumamoto Y, Maruta H, Takagi Y, Mikuma N, Nanbu A, et al. Determination of the normal range of serum LH and FSH levels in normal adult males comparison with IRMA and RIA. Folia Endocrinol 1990;66: Manova K, Huang EJ, Angeles M, De Leon V, Sanchez S, Pronovost SM, et al. The expression pattern of the c-kit ligand in gonads of mice supports a role for the c-kit receptor in oocyte growth and in proliferation of spermatogonia. Dev Biol 1993;157: Yoshinaga K, Nishikawa S, Ogawa M, Hayashi SI, Kunisada T, Fujimoto T, et al. Role of c-kit in mouse spermatogenesis: identification of spermatogonia as a specific site of c-kit expression and function. Development 1991;113: Thompson CB. Apoptosis in the pathogenesis and treatment of disease. Science 1995;267: Rodriguez JB, Garcia CM. Spontaneous germ cell death in the testis of the adult rat takes the form of apoptosis: re-evaluation of cell types that exhibit the ability to die during spermatogenesis. Cell Prolif 1996;29: Henriksen K, Kulmala J, Toppari J, Mehrotra K, Parvinen M. Stagespecific apoptosis in the rat seminiferous epithelium: quantification of irradiation effects. J Androl 1996;17: Richburg JH, Boekelheide K. Mono-(2-ethylhexyl) phthalate rapidly alters both Sertoli cell vimentin filaments and germ cell apoptosis in young rat testes. Toxicol Appl Pharmacol 1996;137: Hikim APS, Wang C, Leung A, Swerdloff RS. Involvement of apoptosis in the induction of germ cell degeneration in adult rats after gonadotropin-releasing hormone antagonist treatment. Endocrinology 1995; 136: Yin Y, Hawkins KL, Dewolf WC, Morgentaler A. Heat stress causes testicular germ cell apoptosis in adult mice. J Androl 1997;18: Rodriguez JB, Garcia CM. Mild hypothermia induces apoptosis in rat testis at specific stages of the seminiferous epithelium. J Androl 1997; 18: Lin WW, Lipshultz LI, Lamb DJ, Kim ED, Wheeler TM. In situ end-labeling of human testicular tissue demonstrates increased apoptosis in conditions of abnormal spermatogenesis. Fertil Steril 1997;68: Furuchi T, Masuko K, Nishimune Y, Obinata M, Matsui Y. Inhibition of testicular germ cell apoptosis and differentiation in mice misexpressing bcl-2 in spermatogonia. Development 1996;122: Knudson CM, Tung KSK, Tourtellotte WG, Brown GAJ, Korsmeyer SJ. Bax-deficient mice with lymphoid hyperplasia and male germ cell death. Science 1995;270: Foresta C, Bettella A, Ferlin A, Garolla A, Rossato M. Evidence for a stimulatory role of follicle-stimulating hormone on the spermatogonial population in adult males. Fertil Steril 1997;69: De Rooij DG, Van Dissel-Emiliani FMF, Van Pelt AMM. Regulation of spermatogonial proliferation. Ann NY Acad Sci 1989;564: FERTILITY & STERILITY 907
Testicular stem cells
 Testicular stem cells Dirk G. de Rooij Department of Endocrinology Faculty of Biology, Utrecht University 1. Knowledge on the development of the spermatogenic stem cell lineage 2. Principals of the nature
Testicular stem cells Dirk G. de Rooij Department of Endocrinology Faculty of Biology, Utrecht University 1. Knowledge on the development of the spermatogenic stem cell lineage 2. Principals of the nature
Inhibin B plasma concentrations in oligozoospermic subjects before and after therapy with follicle stimulating hormone
 Human Reproduction vol.14 no.4 pp.906 912, 1999 Inhibin B plasma concentrations in oligozoospermic subjects before and after therapy with follicle stimulating hormone Carlo Foresta 1,4, Andrea Bettella
Human Reproduction vol.14 no.4 pp.906 912, 1999 Inhibin B plasma concentrations in oligozoospermic subjects before and after therapy with follicle stimulating hormone Carlo Foresta 1,4, Andrea Bettella
Spermatogenesis. What is it and what does it look like? How do hormones regulate spermatogenesis?
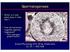 Spermatogenesis What is it and what does it look like? How do hormones regulate spermatogenesis? FSH, androgens, growth factors Animal Physiology (Hill, Wise, Anderson): Ch. 15 435-438 1 Spermatogenesis:
Spermatogenesis What is it and what does it look like? How do hormones regulate spermatogenesis? FSH, androgens, growth factors Animal Physiology (Hill, Wise, Anderson): Ch. 15 435-438 1 Spermatogenesis:
Testicular fine needle aspiration as a diagnostic tool in nonobstructive
 Asian J Androl 2005; 7 (3): 289 294 DOI: 10.1111/j.1745-7262.2005.00043.x. Original Article. Testicular fine needle aspiration as a diagnostic tool in nonobstructive azoospermia A. Bettella 1, A. Ferlin
Asian J Androl 2005; 7 (3): 289 294 DOI: 10.1111/j.1745-7262.2005.00043.x. Original Article. Testicular fine needle aspiration as a diagnostic tool in nonobstructive azoospermia A. Bettella 1, A. Ferlin
Adapted from Preg. & Part., Senger
 MALE ENDOCRINOLOGY AND SPERMATOGENESIS (Chapter 10) AVS 222 (Instructor: Dr. Amin Ahmadzadeh) I. MALE ENDOCRINOLOGY (Figure10-1 to 10-3) A. Glands and their respective hormones 1) Hypothalamic hormone:
MALE ENDOCRINOLOGY AND SPERMATOGENESIS (Chapter 10) AVS 222 (Instructor: Dr. Amin Ahmadzadeh) I. MALE ENDOCRINOLOGY (Figure10-1 to 10-3) A. Glands and their respective hormones 1) Hypothalamic hormone:
Article Abnormal spermatozoa in the ejaculate: abortive apoptosis and faulty nuclear remodelling during spermatogenesis
 RBMOnline - Vol 7. No 4. 428 432 Reproductive BioMedicine Online; www.rbmonline.com/article/1019 on web 16 July 2003 Article Abnormal spermatozoa in the ejaculate: abortive apoptosis and faulty nuclear
RBMOnline - Vol 7. No 4. 428 432 Reproductive BioMedicine Online; www.rbmonline.com/article/1019 on web 16 July 2003 Article Abnormal spermatozoa in the ejaculate: abortive apoptosis and faulty nuclear
MALE INFERTILITY & SEMEN ANALYSIS
 MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
DAX1, testes development role 7, 8 DFFRY, spermatogenesis role 49 DMRT genes, male sex differentiation role 15
 Subject Index N-Acetylcysteine, sperm quality effects 71 Ambiguous genitalia, origins 1, 2 Anti-Müllerian hormone function 13 receptors 13 Sertoli cell secretion 10, 38 Apoptosis assays in testes 73, 74
Subject Index N-Acetylcysteine, sperm quality effects 71 Ambiguous genitalia, origins 1, 2 Anti-Müllerian hormone function 13 receptors 13 Sertoli cell secretion 10, 38 Apoptosis assays in testes 73, 74
AZOOSPERMIA CYTOLOGICAL MANIFESTATIONS
 ý Comptes rendus de l Académie bulgare des Sciences ÌÓÑ ÆÓ ¾¼½½ BIOLOGIE Morphologie AZOOSPERMIA CYTOLOGICAL MANIFESTATIONS Stefka Ivanova, Petia Tzvetkova (Submitted by Corresponding Member J. Jordanov
ý Comptes rendus de l Académie bulgare des Sciences ÌÓÑ ÆÓ ¾¼½½ BIOLOGIE Morphologie AZOOSPERMIA CYTOLOGICAL MANIFESTATIONS Stefka Ivanova, Petia Tzvetkova (Submitted by Corresponding Member J. Jordanov
The effect of testicular nongerm cell tumors on local spermatogenesis
 FERTILITY AND STERILITY Vol. 62, No.1, July 1994 Copyright" 1994 The American Fertility Society Printed on acid-free paper in U. S. A. The effect of testicular nongerm cell tumors on local spermatogenesis
FERTILITY AND STERILITY Vol. 62, No.1, July 1994 Copyright" 1994 The American Fertility Society Printed on acid-free paper in U. S. A. The effect of testicular nongerm cell tumors on local spermatogenesis
Spermatogonial Cell Proliferation in Organ Culture of Immature Rat Testis'
 BIOLOGY OF REPRODUCTION 48, 761-767 (1993) Spermatogonial Cell Proliferation in Organ Culture of Immature Rat Testis' CARLA BOITANI, 2 MARIA GIUDITTA POLITI, and TIZIANA MENNA Institute of Histology and
BIOLOGY OF REPRODUCTION 48, 761-767 (1993) Spermatogonial Cell Proliferation in Organ Culture of Immature Rat Testis' CARLA BOITANI, 2 MARIA GIUDITTA POLITI, and TIZIANA MENNA Institute of Histology and
Decreased expression of the c-kit receptor is associated with increased apoptosis in subfertile human testes
 FERTILITY AND STERILITY VOL. 71, NO. 1, JANUARY 1999 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Decreased expression
FERTILITY AND STERILITY VOL. 71, NO. 1, JANUARY 1999 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Decreased expression
Functional and cytologic features of the contralateral testis in cryptorchidism
 FERTILITY AND STERILITY@ Copyright Ci') 1996 American Society for Reproductive Medicine Printed on acid-free paper in U. S. A. Functional and cytologic features of the contralateral testis in cryptorchidism
FERTILITY AND STERILITY@ Copyright Ci') 1996 American Society for Reproductive Medicine Printed on acid-free paper in U. S. A. Functional and cytologic features of the contralateral testis in cryptorchidism
Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients
 Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients Basim Sh. Ahmed F.I.C.M.S Department of Pathology, College of Medicine, Al-Mustansiriya University, Baghdad,
Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients Basim Sh. Ahmed F.I.C.M.S Department of Pathology, College of Medicine, Al-Mustansiriya University, Baghdad,
Infertility is not an uncommon problem in Western
 Review Article A Practical Approach to Testicular Biopsy Interpretation for Male Infertility Lisa A. Cerilli, MD; Wayne Kuang, MD; David Rogers, MD Infertility is not an uncommon problem in Western societies
Review Article A Practical Approach to Testicular Biopsy Interpretation for Male Infertility Lisa A. Cerilli, MD; Wayne Kuang, MD; David Rogers, MD Infertility is not an uncommon problem in Western societies
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility
 Article ID: WMC001510 ISSN 2046-1690 Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility Author(s):Dr. Geetika, Dr. Sunita
Article ID: WMC001510 ISSN 2046-1690 Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility Author(s):Dr. Geetika, Dr. Sunita
Reproductive Toxicology
 Reproductive Toxicology 32 (2011) 395 406 Contents lists available at SciVerse ScienceDirect Reproductive Toxicology jo u r n al hom epa ge: ww w.elsevier.com/locate/reprotox Effects of multiple doses
Reproductive Toxicology 32 (2011) 395 406 Contents lists available at SciVerse ScienceDirect Reproductive Toxicology jo u r n al hom epa ge: ww w.elsevier.com/locate/reprotox Effects of multiple doses
Cell Divisions. The autosomes represent the whole body. * Male Sex Chromosomes: XY * Female Sex Chromosomes: XX
 Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
Spermatogenesis in Man
 Spermatogenesis in Man I. Nuclear Morphology During Spermatogenesis in Man BRUNETTO CHIARELLI, PH.D., ARTHUR FALEK, PH.D., KAREN J. BACK, B.S., and C. THOMAS COWART, M.D. THE SEQUENCE of transformations
Spermatogenesis in Man I. Nuclear Morphology During Spermatogenesis in Man BRUNETTO CHIARELLI, PH.D., ARTHUR FALEK, PH.D., KAREN J. BACK, B.S., and C. THOMAS COWART, M.D. THE SEQUENCE of transformations
The Use of Rabbits in Male Reproductive Toxicology
 Environmental Health Perspectives Vol. 77, pp. 5-9, 1988 The Use of Rabbits in Male Reproductive Toxicology by Daniel Morton* The rabbit is the smallest and least expensive laboratory animal in which serial
Environmental Health Perspectives Vol. 77, pp. 5-9, 1988 The Use of Rabbits in Male Reproductive Toxicology by Daniel Morton* The rabbit is the smallest and least expensive laboratory animal in which serial
SPERMATOGENESIS IN VITRO
 SPERMATOGENESIS IN VITRO INDUCTION OF PROLIFERATION, MEIOSIS AND DIFFERENTIATION Mário Sousa Lab Cell Biology Institute of Biomedical Sciences (ICBAS) University of Porto msousa@icbas.up.pt Spermatogonia
SPERMATOGENESIS IN VITRO INDUCTION OF PROLIFERATION, MEIOSIS AND DIFFERENTIATION Mário Sousa Lab Cell Biology Institute of Biomedical Sciences (ICBAS) University of Porto msousa@icbas.up.pt Spermatogonia
5 15/3/2012. Malik Al-Momani
 5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
REAPPRAISAL OF THE VALUE OF TESTICULAR BIOPSY IN THE INVESTIGATION OF INFERTILITY
 FERTWTY AND STEIuLlTY Copyright 1980 The American Fertility Society Vol., No.1 January 1980 Prinwl in U.S.A. REAPPRAISAL OF THE VALUE OF TESTICULAR BIOPSY IN THE INVESTIGATION OF INFERTILITY TERENCE
FERTWTY AND STEIuLlTY Copyright 1980 The American Fertility Society Vol., No.1 January 1980 Prinwl in U.S.A. REAPPRAISAL OF THE VALUE OF TESTICULAR BIOPSY IN THE INVESTIGATION OF INFERTILITY TERENCE
available at
 NAOSITE: Nagasaki University's Ac Title Hybrid male sterility is caused by Author(s) Hayashida, Kenji; Kohno, Shigeru Citation Molecular biology reports, (), p Issue Date 00-0 URL Right http://hdl.handle.net/0/01
NAOSITE: Nagasaki University's Ac Title Hybrid male sterility is caused by Author(s) Hayashida, Kenji; Kohno, Shigeru Citation Molecular biology reports, (), p Issue Date 00-0 URL Right http://hdl.handle.net/0/01
Male Reproductive System
 Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
MicroRNA and Male Infertility: A Potential for Diagnosis
 Review Article MicroRNA and Male Infertility: A Potential for Diagnosis * Abstract MicroRNAs (mirnas) are small non-coding single stranded RNA molecules that are physiologically produced in eukaryotic
Review Article MicroRNA and Male Infertility: A Potential for Diagnosis * Abstract MicroRNAs (mirnas) are small non-coding single stranded RNA molecules that are physiologically produced in eukaryotic
Production of Fertile Sperm. Animal Science 434. Hormonal Regulation of the Testis. hormonal regulation of the testis
 roduction of Fertile Sperm hormonal regulation of the testis nimal Science 434 Lecture 12: Spermatogenesis mitotic division of spermatogonia meiotic divisions of spermatocytes morphologic transformation
roduction of Fertile Sperm hormonal regulation of the testis nimal Science 434 Lecture 12: Spermatogenesis mitotic division of spermatogonia meiotic divisions of spermatocytes morphologic transformation
Treatment of male idiopathic infertility with recombinant human follicle-stimulating hormone: a prospective, controlled, randomized clinical study
 Treatment of male idiopathic infertility with recombinant human follicle-stimulating hormone: a prospective, controlled, randomized clinical study Carlo Foresta, M.D., Ph.D., a Andrea Bettella, M.D., Ph.D.,
Treatment of male idiopathic infertility with recombinant human follicle-stimulating hormone: a prospective, controlled, randomized clinical study Carlo Foresta, M.D., Ph.D., a Andrea Bettella, M.D., Ph.D.,
Treatment of Defective Spermatogenesis tvith Human Gonadotropins
 Treatment of Defective Spermatogenesis tvith Human Gonadotropins W. Z. POLISHUK, M.D., Z. PALTI, M.D., and A. LAUFER, M.D. TREATMENT of male sterility due to defective spermatogenesis is not satisfactory.
Treatment of Defective Spermatogenesis tvith Human Gonadotropins W. Z. POLISHUK, M.D., Z. PALTI, M.D., and A. LAUFER, M.D. TREATMENT of male sterility due to defective spermatogenesis is not satisfactory.
Intratubular Germ Cell Neoplasia of the Testis
 Intratubular Germ Cell Neoplasia of the Testis KS Ngoo Department of Urology Hospital Selayang Advanced Urology Course 15 Aug 2014 MUA Office Clinical scenario A 33 years old man has bilateral testicular
Intratubular Germ Cell Neoplasia of the Testis KS Ngoo Department of Urology Hospital Selayang Advanced Urology Course 15 Aug 2014 MUA Office Clinical scenario A 33 years old man has bilateral testicular
Failure to Launch. Impairment of Primary Spermatogenesis & Optimization of Reproductive Techniques
 Failure to Launch. Impairment of Primary Spermatogenesis & Optimization of Reproductive Techniques October 16, 2013 Ryan Flannigan PGY3 UBC Urology http://www.chinahearsay.com/china-lethargic-sperm-economic-development/
Failure to Launch. Impairment of Primary Spermatogenesis & Optimization of Reproductive Techniques October 16, 2013 Ryan Flannigan PGY3 UBC Urology http://www.chinahearsay.com/china-lethargic-sperm-economic-development/
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
A COMPARATIVE STUDY OF GERM CELL KINETICS IN THE TESTES OF CHILDREN WITH UNILATERAL CRYPTORCHIDISM: A PRELIMINARY REPORT*
 FERTILITY AND STERILITY Copyright 1970 by the Williams & Wilkins Co. Vol. 21, No. 11, November 1970 Printed in U.S.A. A COMPARATIVE STUDY OF GERM CELL KINETICS IN THE TESTES OF CHILDREN WITH UNILATERAL
FERTILITY AND STERILITY Copyright 1970 by the Williams & Wilkins Co. Vol. 21, No. 11, November 1970 Printed in U.S.A. A COMPARATIVE STUDY OF GERM CELL KINETICS IN THE TESTES OF CHILDREN WITH UNILATERAL
Variability in testis biopsy interpretation: implications for male infertility care in the era of intracytoplasmic sperm injection
 Variability in testis biopsy interpretation: implications for male infertility care in the era of intracytoplasmic sperm injection Matthew R. Cooperberg, M.D., a Thomas Chi, B.A., a Amir Jad, M.D., a Imok
Variability in testis biopsy interpretation: implications for male infertility care in the era of intracytoplasmic sperm injection Matthew R. Cooperberg, M.D., a Thomas Chi, B.A., a Amir Jad, M.D., a Imok
Immunocytochemical localization of epidermal growth factor receptors in human testis from infertile subjects*
 FERTILITY AND STERILITY Copyright 1994 The American Fertility Society Vol. 61. No.5, May 1994 Printed on acid-free paper in U. S. A. Immunocytochemical localization of epidermal growth factor receptors
FERTILITY AND STERILITY Copyright 1994 The American Fertility Society Vol. 61. No.5, May 1994 Printed on acid-free paper in U. S. A. Immunocytochemical localization of epidermal growth factor receptors
Original Article Morphometrical Evaluation of Germ Cell Apoptosis in Infertile Men
 Original Article Morphometrical Evaluation of Germ Cell Apoptosis in Infertile Men (apoptosis / germ cells / infertile men / morphometry) D. ŠTIBLAR-MARTINČIČ Department of Histology and Embryology, Faculty
Original Article Morphometrical Evaluation of Germ Cell Apoptosis in Infertile Men (apoptosis / germ cells / infertile men / morphometry) D. ŠTIBLAR-MARTINČIČ Department of Histology and Embryology, Faculty
Male reproduction. Cross section of Human Testis ผศ.ดร.พญ.ส ว ฒณ ค ปต ว ฒ ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล 1. Aims
 Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
With advances in assisted reproduction techniques,
 Journal of Andrology, Vol. 26, No. 6, November/December 2005 Copyright American Society of Andrology Clomiphene Administration for Cases of Nonobstructive Azoospermia: A Multicenter Study ALAYMAN HUSSEIN,*
Journal of Andrology, Vol. 26, No. 6, November/December 2005 Copyright American Society of Andrology Clomiphene Administration for Cases of Nonobstructive Azoospermia: A Multicenter Study ALAYMAN HUSSEIN,*
Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia
 Urology Journal UNRC/IUA Vol. 3, No. 2, 92-96 Spring 2006 Printed in IRAN Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia Seyed Amirmohsen Ziaee, 1 * Mohammadreza Ezzatnegad,
Urology Journal UNRC/IUA Vol. 3, No. 2, 92-96 Spring 2006 Printed in IRAN Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia Seyed Amirmohsen Ziaee, 1 * Mohammadreza Ezzatnegad,
ABNORMAL SPERMATOGENESIS IN XYY MALES: A REPORT ON 4 CASES ASCERTAINED THROUGH A POPULATION STUDY*
 FERTILITY AND STERILITY Copyright 1973 by The Williams & Wilkins Co. Vol. 24, No.5, May 1973 Printed in U.S.A. ABNORMAL SPERMATOGENESIS IN XYY MALES: A REPORT ON 4 CASES ASCERTAINED THROUGH A POPULATION
FERTILITY AND STERILITY Copyright 1973 by The Williams & Wilkins Co. Vol. 24, No.5, May 1973 Printed in U.S.A. ABNORMAL SPERMATOGENESIS IN XYY MALES: A REPORT ON 4 CASES ASCERTAINED THROUGH A POPULATION
Histology of Male Reproductive system (1)
 Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
The spermatogenesis CHARACTERISTICS OF THE SPERMATOZOON 26/04/2017. Reproductive Biotechnologies Andrology I. Prof. Alberto Contri
 Reproductive Biotechnologies Andrology I The spermatogenesis Prof. Alberto Contri CHARACTERISTICS OF THE SPERMATOZOON 1) Aploid cell with high condensed DNA 2) Forward motility - flagellum 3) Enzymes for
Reproductive Biotechnologies Andrology I The spermatogenesis Prof. Alberto Contri CHARACTERISTICS OF THE SPERMATOZOON 1) Aploid cell with high condensed DNA 2) Forward motility - flagellum 3) Enzymes for
IN normal male fowls, four developmental stages of spermatogenetic activity
 Development of the Testis Tubule in the Fowl By GAMAL A. R. KAMAR (From the Animal Production Department, Faculty of Agriculture, Cairo University, Giza, Egypt) With three plates (figs. 1-3) SUMMARY Three
Development of the Testis Tubule in the Fowl By GAMAL A. R. KAMAR (From the Animal Production Department, Faculty of Agriculture, Cairo University, Giza, Egypt) With three plates (figs. 1-3) SUMMARY Three
Mohammad Sha ban. Basheq Jehad. Hamzah Nakhleh
 11 Mohammad Sha ban Basheq Jehad Hamzah Nakhleh Physiology of the reproductive system In physiology, we are concerned with the mechanisms in which the system functions, and how the system responds to different
11 Mohammad Sha ban Basheq Jehad Hamzah Nakhleh Physiology of the reproductive system In physiology, we are concerned with the mechanisms in which the system functions, and how the system responds to different
DISORDERS OF MALE GENITALS
 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
Male Factor Infertility and Health. Karen Baker, MD Associate Professor Duke University, Division of Urology
 Male Factor Infertility and Health Karen Baker, MD Associate Professor Duke University, Division of Urology Fertility and Cancer Heart disease Metabolic syndrome Diabetes Early death Goals: Review literature
Male Factor Infertility and Health Karen Baker, MD Associate Professor Duke University, Division of Urology Fertility and Cancer Heart disease Metabolic syndrome Diabetes Early death Goals: Review literature
Outcome of repeated micro-surgical testicular sperm extraction in patients with non-obstructive azoospermia
 Repeated micro-surgical testicular sperm extraction DOI: 10.1111/j.1745-7262.2007.00273.x www.asiaandro.com. Original Article. Outcome of repeated micro-surgical testicular sperm extraction in patients
Repeated micro-surgical testicular sperm extraction DOI: 10.1111/j.1745-7262.2007.00273.x www.asiaandro.com. Original Article. Outcome of repeated micro-surgical testicular sperm extraction in patients
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Assessment of Sperm DNA Fragmentation for Patients Suffering from Varicocele
 Assessment of Sperm DNA Fragmentation for Patients Suffering from Varicocele Saif H. Mohammed 1, Adib M. Al-Kazzaz 2, Usama S.Al- Nasiri 3 1-Department of Urology- College of Medicine- Al-Nahrain University-
Assessment of Sperm DNA Fragmentation for Patients Suffering from Varicocele Saif H. Mohammed 1, Adib M. Al-Kazzaz 2, Usama S.Al- Nasiri 3 1-Department of Urology- College of Medicine- Al-Nahrain University-
The Comet and TUNEL Assays
 Sperm DNA: organization, protection and vulnerability from basic science to clinical application Methods to assess the status of the sperm DNA: The Comet and TUNEL Assays Lars Björndahl Centre for Andrology
Sperm DNA: organization, protection and vulnerability from basic science to clinical application Methods to assess the status of the sperm DNA: The Comet and TUNEL Assays Lars Björndahl Centre for Andrology
Comparative studies of spermatogenesis in fertile and
 J Clin Pathol 1981 ;34:145-150 Comparative studies of spermatogenesis in fertile and subfertile men MA LAMONT,* MJW FAED,* AND K BAXBYt From the *Cytogenetics Laboratory, Ninewells Hospital and Medical
J Clin Pathol 1981 ;34:145-150 Comparative studies of spermatogenesis in fertile and subfertile men MA LAMONT,* MJW FAED,* AND K BAXBYt From the *Cytogenetics Laboratory, Ninewells Hospital and Medical
Minireview. Telomerase Activity and Telomere Length in Male Germ Cells. Downloaded from Saffet Ozturk 1
 BIOLOGY OF REPRODUCTION (2015) 92(2):53, 1 11 Published online before print 7 January 2015. DOI 10.1095/biolreprod.114.124008 Minireview Telomerase Activity and Telomere Length in Male Germ Cells Saffet
BIOLOGY OF REPRODUCTION (2015) 92(2):53, 1 11 Published online before print 7 January 2015. DOI 10.1095/biolreprod.114.124008 Minireview Telomerase Activity and Telomere Length in Male Germ Cells Saffet
Identification of the spermatogenic stages in living seminiferous tubules of man
 Identification of the spermatogenic stages in living seminiferous tubules of man V. Nikkanen, K.-O. S\l=o"\derstr\l=o"\m and M. Parvinen Department of Obstetrics and Gynecology, Turku University Central
Identification of the spermatogenic stages in living seminiferous tubules of man V. Nikkanen, K.-O. S\l=o"\derstr\l=o"\m and M. Parvinen Department of Obstetrics and Gynecology, Turku University Central
Aspiration flow cytometry of the testes in the evaluation of spermatogenesis in the infertile male*t
 FERTILITY AND STERILITY Copyright e 1987 The American Fertility Society Printed in U.S.A. Aspiration flow cytometry of the testes in the evaluation of spermatogenesis in the infertile male*t David G. Kaufman,
FERTILITY AND STERILITY Copyright e 1987 The American Fertility Society Printed in U.S.A. Aspiration flow cytometry of the testes in the evaluation of spermatogenesis in the infertile male*t David G. Kaufman,
Spermatogenesis Following Experimental Testicular Ischemia
 Spermatogenesis Following Experimental Testicular Ischemia Frank Hinman, Jr, MD, and Gilbert I Smith, MD REGENERATION of the spermatogenic elements of the testis after depression by testosterone and by
Spermatogenesis Following Experimental Testicular Ischemia Frank Hinman, Jr, MD, and Gilbert I Smith, MD REGENERATION of the spermatogenic elements of the testis after depression by testosterone and by
EXPRESSION PROFILING OF CREM GENE IN TESTIS WITH NORMAL AND IMPAIRED SPERMATOGENESIS IN EGYPTIAN MALES
 EXPRESSION PROFILING OF CREM GENE IN TESTIS WITH NORMAL AND IMPAIRED SPERMATOGENESIS IN EGYPTIAN MALES MANAL O. EL HAMSHARY 1, ALIAA M. ISSA 2, M. K. KHALIFA 3, K. Z. SHAEER 4 1. 2. 3. Genetic Engineering
EXPRESSION PROFILING OF CREM GENE IN TESTIS WITH NORMAL AND IMPAIRED SPERMATOGENESIS IN EGYPTIAN MALES MANAL O. EL HAMSHARY 1, ALIAA M. ISSA 2, M. K. KHALIFA 3, K. Z. SHAEER 4 1. 2. 3. Genetic Engineering
Sami Ventelä, 1,2 Hiroshi Ohta, 3 Martti Parvinen, 2 and Yoshitake Nishimune 3
 BIOLOGY OF REPRODUCTION 66, 1422 1429 (2002) Development of the Stages of the Cycle in Mouse Seminiferous Epithelium after Transplantation of Green Fluorescent Protein-Labeled Spermatogonial Stem Cells
BIOLOGY OF REPRODUCTION 66, 1422 1429 (2002) Development of the Stages of the Cycle in Mouse Seminiferous Epithelium after Transplantation of Green Fluorescent Protein-Labeled Spermatogonial Stem Cells
Male Anatomy. testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics
 Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
Physiology of Male Reproductive System
 Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Inhibition of testicular germ cell apoptosis and differentiation in mice misexpressing Bcl-2 in spermatogonia
 Development 122, 1703-1709 (1996) Printed in Great Britain The Company of Biologists Limited 1996 DEV4674 1703 Inhibition of testicular germ cell apoptosis and differentiation in mice misexpressing Bcl-2
Development 122, 1703-1709 (1996) Printed in Great Britain The Company of Biologists Limited 1996 DEV4674 1703 Inhibition of testicular germ cell apoptosis and differentiation in mice misexpressing Bcl-2
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
Hormones of brain-testicular axis
 (Hormone Function) Hormones of brain-testicular axis anterior pituitary drives changes during puberty controlled by GnRH from hypothalamus begins to secrete FSH, LH LH targets interstitial endocrinocytes
(Hormone Function) Hormones of brain-testicular axis anterior pituitary drives changes during puberty controlled by GnRH from hypothalamus begins to secrete FSH, LH LH targets interstitial endocrinocytes
Inhibin B plasma concentrations in infertile patients with DAZ gene deletions treated with FSH
 European Journal of Endocrinology (2002) 146 801 806 ISSN 0804-4643 CLINICAL STUDY Inhibin B plasma concentrations in infertile patients with DAZ gene deletions treated with FSH Carlo Foresta, Andrea Bettella,
European Journal of Endocrinology (2002) 146 801 806 ISSN 0804-4643 CLINICAL STUDY Inhibin B plasma concentrations in infertile patients with DAZ gene deletions treated with FSH Carlo Foresta, Andrea Bettella,
II.3.9 Evaluation of Testicular Biopsy Samples from the Clinical Perspective
 454 Diagnostic Tools.9 Evaluation of Testicular Biopsy Samples from the Clinical Perspective M. Bergmann Summary Testicular biopsy is indicated therapeutically in cases of obstructive azoospermia, and
454 Diagnostic Tools.9 Evaluation of Testicular Biopsy Samples from the Clinical Perspective M. Bergmann Summary Testicular biopsy is indicated therapeutically in cases of obstructive azoospermia, and
Sperm retrieval from patients with nonmosaic Klinefelter s syndrome by semen cytology examination
 Sperm retrieval from patients with nonmosaic Klinefelter s syndrome by semen cytology examination Y.-T. Jiang 1, Y. Dong 1, X.-W. Yu 1, R.-C. Du 1,2, L.-L. Li 1,2, H.-G. Zhang 1 and R.-Z. Liu 1 1 Center
Sperm retrieval from patients with nonmosaic Klinefelter s syndrome by semen cytology examination Y.-T. Jiang 1, Y. Dong 1, X.-W. Yu 1, R.-C. Du 1,2, L.-L. Li 1,2, H.-G. Zhang 1 and R.-Z. Liu 1 1 Center
Knockout TM SR : ; ; ; : R ; R : A : X(2013) , ,, B. , (Knockout TM
 33 1 Vol.33 No.1 013 1 Dec. 013 Reproduction & Contraception doi: 10.7669/j.issn.03-37X.013.1.0804 E-mail: randc_journal@163.com Knockout TM SR ; ; ; 400014 : FBS Knockout TM SRKSR : FBS KSR HE TUNEL RT-PCR
33 1 Vol.33 No.1 013 1 Dec. 013 Reproduction & Contraception doi: 10.7669/j.issn.03-37X.013.1.0804 E-mail: randc_journal@163.com Knockout TM SR ; ; ; 400014 : FBS Knockout TM SRKSR : FBS KSR HE TUNEL RT-PCR
Changes of androgen receptor expression in stages VII-VIII seminiferous tubules of rat testis after exposure to methamphetamine
 Songklanakarin J. Sci. Technol. 38 (3), 275-279, May - Jun. 2016 http://www.sjst.psu.ac.th Original Article Changes of androgen receptor expression in stages VII-VIII seminiferous tubules of rat testis
Songklanakarin J. Sci. Technol. 38 (3), 275-279, May - Jun. 2016 http://www.sjst.psu.ac.th Original Article Changes of androgen receptor expression in stages VII-VIII seminiferous tubules of rat testis
The effects of cancer treatment on male infertility
 The effects of cancer treatment on male infertility Kirsi Jahnukainen Children s Hospital, Helsinki Karolinska Institutet, Stockholm Department of Pediatrics 21.11.2017 1 Disclosure statement I declare
The effects of cancer treatment on male infertility Kirsi Jahnukainen Children s Hospital, Helsinki Karolinska Institutet, Stockholm Department of Pediatrics 21.11.2017 1 Disclosure statement I declare
Germ Cell Degeneration During Postprophase of Meiosis and Serum Concentrations of Gonadotropins in Young Adult and Older Adult Men
 BIOLOGY OF REPRODUCTION 31, 779-784 (1984) Germ Cell Degeneration During Postprophase of Meiosis and Serum Concentrations of Gonadotropins in Young Adult and Older Adult Men LARRY JOHNSON,2 CHARLES S.
BIOLOGY OF REPRODUCTION 31, 779-784 (1984) Germ Cell Degeneration During Postprophase of Meiosis and Serum Concentrations of Gonadotropins in Young Adult and Older Adult Men LARRY JOHNSON,2 CHARLES S.
Effect of Cigarette Smoke on Spermatogenesis in Rats
 Sexual Dysfunction and Infertility Effect of Cigarette Smoke on Spermatogenesis in Rats Hassan Ahmadnia, 1 Mohsen Ghanbari, 1 Mohammad Reza Moradi, 2 Mohammad Khaje-Dalouee 3 Keywords: smoking, spermatogenesis,
Sexual Dysfunction and Infertility Effect of Cigarette Smoke on Spermatogenesis in Rats Hassan Ahmadnia, 1 Mohsen Ghanbari, 1 Mohammad Reza Moradi, 2 Mohammad Khaje-Dalouee 3 Keywords: smoking, spermatogenesis,
Male Reproductive System
 Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
Stem cells in the testis
 Int. J. Exp. Path. (1998), 79, 67 80 Stem Cell Review Stem cells in the testis DIRK G. DE ROOIJ Department of Cell Biology, Utrecht University, Utrecht, The Netherlands Received for publication 5 January
Int. J. Exp. Path. (1998), 79, 67 80 Stem Cell Review Stem cells in the testis DIRK G. DE ROOIJ Department of Cell Biology, Utrecht University, Utrecht, The Netherlands Received for publication 5 January
Morphogenesis of the residual body of the mouse testis
 93 Morphogenesis of the residual body of the mouse testis By CASIMIR F. FIRLIT and JOSEPH R. DAVIS (From the Department of Pharmacology and Therapeutics, Stritch School of Medicine, and Graduate School,
93 Morphogenesis of the residual body of the mouse testis By CASIMIR F. FIRLIT and JOSEPH R. DAVIS (From the Department of Pharmacology and Therapeutics, Stritch School of Medicine, and Graduate School,
Cycle of the Seminiferous Epithelium of the Guinea Pig
 Cycle of the Seminiferous Epithelium of the Guinea Pig A Method for Identification of the Stages Yves Clermont, Ph.D. IN THE GUINEA PIG, the cells of the seminiferous epithelium are arranged in definite
Cycle of the Seminiferous Epithelium of the Guinea Pig A Method for Identification of the Stages Yves Clermont, Ph.D. IN THE GUINEA PIG, the cells of the seminiferous epithelium are arranged in definite
Predictive Factors of Successful Microdissection Testicular Sperm Extraction in Patients with Presumed Sertoli Cell-Only Syndrome
 Original Article Predictive Factors of Successful Microdissection Testicular Sperm Extraction in Patients with Presumed Sertoli Cell-Only Syndrome Tahereh Modarresi, M.Sc. 1, Hani Hosseinifar, M.Sc. 1,
Original Article Predictive Factors of Successful Microdissection Testicular Sperm Extraction in Patients with Presumed Sertoli Cell-Only Syndrome Tahereh Modarresi, M.Sc. 1, Hani Hosseinifar, M.Sc. 1,
SUPPLEMENTAL INFORMATION FOR. PAX7 expression defines germline stem cells in the adult testis
 SUPPLEMENTAL INFORMATION FOR PAX7 expression defines germline stem cells in the adult testis Gina M. Aloisio, Yuji Nakada, Hatice D. Saatcioglu, Christopher G. Peña, Michael D. Baker, Edward D. Tarnawa,
SUPPLEMENTAL INFORMATION FOR PAX7 expression defines germline stem cells in the adult testis Gina M. Aloisio, Yuji Nakada, Hatice D. Saatcioglu, Christopher G. Peña, Michael D. Baker, Edward D. Tarnawa,
Embryology 3. Spermatogenesis:
 Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Harbor-UCLA Medical Center Division of Endocrinology and Metabolism
 LABioMed Harbor-UCLA Medical Center Division of Endocrinology and Metabolism Reversible Contraceptive Method for Men Niloufar Ilani, M.D. Endocrine Fellow Introduction Unintended pregnancy remains a major
LABioMed Harbor-UCLA Medical Center Division of Endocrinology and Metabolism Reversible Contraceptive Method for Men Niloufar Ilani, M.D. Endocrine Fellow Introduction Unintended pregnancy remains a major
12/3/12. Managing Bull Development to Optimize Fertility Rearing bulls for fertility
 Managing Bull Development to Optimize Fertility Rearing bulls for fertility Effect of post weaning nutrition (after normal calf hood nutrition) - testis size - age at puberty - semen quality Effect of
Managing Bull Development to Optimize Fertility Rearing bulls for fertility Effect of post weaning nutrition (after normal calf hood nutrition) - testis size - age at puberty - semen quality Effect of
Gametogenesis. Omne vivum ex ovo All living things come from eggs.
 Omne vivum ex ovo All living things come from eggs. William Harvery, 1651 Gametogenesis This lecture is the preface, so to speak, to embryology; that is, it introduces the development of the specialized
Omne vivum ex ovo All living things come from eggs. William Harvery, 1651 Gametogenesis This lecture is the preface, so to speak, to embryology; that is, it introduces the development of the specialized
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Repression of hspa2 messenger RNA in human testes with abnormal spermatogenesis
 FERTILITY AND STERILITY VOL. 73, NO. 6, JUNE 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Repression of hspa2 messenger
FERTILITY AND STERILITY VOL. 73, NO. 6, JUNE 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Repression of hspa2 messenger
Glucocorticoid hormone can suppress apoptosis of rat testicular germ cells induced by testicular ischemia
 FERTILITY AND STERILITY VOL. 75, NO. 5, MAY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Glucocorticoid hormone
FERTILITY AND STERILITY VOL. 75, NO. 5, MAY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Glucocorticoid hormone
Yamagata University School of Medicine, Yamagata, Japan
 FERTILITY AND STERILITY VOL. 77, NO. 4, APRIL 2002 Copyright 2002 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. REPRODUCTIVE BIOLOGY
FERTILITY AND STERILITY VOL. 77, NO. 4, APRIL 2002 Copyright 2002 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. REPRODUCTIVE BIOLOGY
Physiologic Anatomy of the Male Sexual Organs
 Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin
 Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin A Preliminary Report S. J. GLASS, M.D., and H. M. HOLLAND, M.D. BEFORE discussing gonadotropic therapy of oligospermia, it is
Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin A Preliminary Report S. J. GLASS, M.D., and H. M. HOLLAND, M.D. BEFORE discussing gonadotropic therapy of oligospermia, it is
Medical School Histology Basics Male Reproductive System. VIBS 289 lab
 Medical School Histology Basics Male Reproductive System VIBS 289 lab Larry Johnson Texas A&M University OBJECTIVE To conduct a histologic examination of the testis (which produce spermatozoa), excretory
Medical School Histology Basics Male Reproductive System VIBS 289 lab Larry Johnson Texas A&M University OBJECTIVE To conduct a histologic examination of the testis (which produce spermatozoa), excretory
All You Wanted to Know About Spermatogonia but Were Afraid to Ask
 All You Wanted to Know About Spermatogonia but Were Afraid to Ask Review DIRK G. DE ROOIJ* AND LONNIE D. RUSSELL From the *Department of Cell Biology, University Medical Center Utrecht, Utrecht, The Netherlands;
All You Wanted to Know About Spermatogonia but Were Afraid to Ask Review DIRK G. DE ROOIJ* AND LONNIE D. RUSSELL From the *Department of Cell Biology, University Medical Center Utrecht, Utrecht, The Netherlands;
THE EFFECTS OF REPEATED INJECTIONS OF CHORIONIC GONADOTROPIN ON THE TESTES OF THE LEOPARD FROG (RANA PIPIENS SCHREBER)
 THE EFFECTS OF REPEATED INJECTIONS OF CHORIONIC GONADOTROPIN ON THE TESTES OF THE LEOPARD FROG (RANA PIPIENS SCHREBER) ROBERT P. McCOURT Department of Zoology and Entomology, The Ohio State University,
THE EFFECTS OF REPEATED INJECTIONS OF CHORIONIC GONADOTROPIN ON THE TESTES OF THE LEOPARD FROG (RANA PIPIENS SCHREBER) ROBERT P. McCOURT Department of Zoology and Entomology, The Ohio State University,
Effect of methotrexate (mtx) administration on spermatogenesis: an experimental on animal model
 Effect of methotrexate (mtx) administration on spermatogenesis: an experimental on animal model S Shrestha, 1 S Dhungel, 1 AK Saxena, 2 S Bhattacharya 1 and D Maskey 1 1 Department of Anatomy, B. P. Koirala
Effect of methotrexate (mtx) administration on spermatogenesis: an experimental on animal model S Shrestha, 1 S Dhungel, 1 AK Saxena, 2 S Bhattacharya 1 and D Maskey 1 1 Department of Anatomy, B. P. Koirala
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
Patterns of Testicular Histopathology in Egyptian Azoospermic Men
 ISPUB.COM The Internet Journal of Urology Volume 13 Number 1 Patterns of Testicular Histopathology in Egyptian Azoospermic Men M K Khalifa, A M Issa, M O El Hamshary, K Z Shaeer Citation M K Khalifa, A
ISPUB.COM The Internet Journal of Urology Volume 13 Number 1 Patterns of Testicular Histopathology in Egyptian Azoospermic Men M K Khalifa, A M Issa, M O El Hamshary, K Z Shaeer Citation M K Khalifa, A
MALE FACTOR. Gerald J. Matthews, M.D.,* Ellen Dakin Matthews, R.N., and Marc Goldstein, M.D.*
 FERTILITY AND STERILITY VOL. 70, NO. 1, JULY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Induction
FERTILITY AND STERILITY VOL. 70, NO. 1, JULY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Induction
CURRICULUM VITAE. Suite 1835 Chicago, Illinois Phone: Fax:
 CURRICULUM VITAE NAME OFFICE ADDRESS CITIZENSHIP BIRTH DATE EDUCATION William Wei Lin, M.D. 2233 North Seminary Avenue 60614 676 N. St. Clair Suite 1835 60611 Phone: 312-926-3535 Fax: 312-926-3585 Email:
CURRICULUM VITAE NAME OFFICE ADDRESS CITIZENSHIP BIRTH DATE EDUCATION William Wei Lin, M.D. 2233 North Seminary Avenue 60614 676 N. St. Clair Suite 1835 60611 Phone: 312-926-3535 Fax: 312-926-3585 Email:
Downloaded From: on 07 Mar 2019 Terms of Use:
 The First and The Second Mitotic Phases of Spermatogonial Stage in Xenopus laevis: Secondary Spermatogonia Which Have Differentiated after Completion of The First Mitotic Phase Acquire an Ability of Mitosis
The First and The Second Mitotic Phases of Spermatogonial Stage in Xenopus laevis: Secondary Spermatogonia Which Have Differentiated after Completion of The First Mitotic Phase Acquire an Ability of Mitosis
THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS
 Nagoya J. Med. Sci. 59. 25-29,1996 THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS MASANORI YAMAMOTO, HATSUKI HIBI, and KOJI MIYAKE Department of Urology, Nagoya University
Nagoya J. Med. Sci. 59. 25-29,1996 THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS MASANORI YAMAMOTO, HATSUKI HIBI, and KOJI MIYAKE Department of Urology, Nagoya University
MALE REPRODUCTIVE SYSTEM
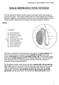 MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
Induction of spermatogenic synchrony by retinoic acid in neonatal mice
 EDITOR'S Letter to CORNER the Editor Spermatogenesis 3:1, e23180; January/February/March 2013 2013; 2013 Landes Bioscience EDITOR'S CORNER Induction of spermatogenic synchrony by retinoic acid in neonatal
EDITOR'S Letter to CORNER the Editor Spermatogenesis 3:1, e23180; January/February/March 2013 2013; 2013 Landes Bioscience EDITOR'S CORNER Induction of spermatogenic synchrony by retinoic acid in neonatal
/00/$03.00/0 Vol. 141, No. 4
 0013-7227/00/$03.00/0 Vol. 141, No. 4 Endocrinology Printed in U.S.A. Copyright 2000 by The Endocrine Society Testicular Heat Exposure Enhances the Suppression of Spermatogenesis by Testosterone in Rats:
0013-7227/00/$03.00/0 Vol. 141, No. 4 Endocrinology Printed in U.S.A. Copyright 2000 by The Endocrine Society Testicular Heat Exposure Enhances the Suppression of Spermatogenesis by Testosterone in Rats:
