Variability in testis biopsy interpretation: implications for male infertility care in the era of intracytoplasmic sperm injection
|
|
|
- Austin Gary Hood
- 6 years ago
- Views:
Transcription
1 Variability in testis biopsy interpretation: implications for male infertility care in the era of intracytoplasmic sperm injection Matthew R. Cooperberg, M.D., a Thomas Chi, B.A., a Amir Jad, M.D., a Imok Cha, M.D., b and Paul J. Turek, M.D. a a Department of Urology and b Department of Pathology, University of California San Francisco, San Francisco, California Objective: To determine whether center to center discrepancies in the ability to locate sperm in infertile testes with abnormal histology stems in part from inconsistencies in pathologists readings of testis biopsies. Design: Prospective cohort study. Setting: Academic male infertility practice. Patient(s): Consecutive series of azoospermic men referred with testis biopsy slides between 1998 and Intervention(s): Testis biopsy histologies on azoospermic patients referred for infertility care were re-reviewed by a single pathologist blinded to the original reading. Subsequent infertility care was guided by the findings from the second histologic reading. Main Outcome Measure(s): Agreement between the outside and in-house review of testis biopsy readings was assessed with the kappa statistic. Pregnancy outcomes that resulted from clinical decisions informed by the second histologic readings were also assessed. Result(s): Among 113 histologic specimens, re-review was complicated by fixation artifacts in 18 cases (16%) and insufficient biopsy sample size in 13 cases (12%). The kappa score for interobserver agreement in readings was 0.43 (95% CI ). Mixed histology patterns in particular were underappreciated by outside pathologists (13% of cases on original reading, 36% of cases on review). In 27% of all cases, the differences in biopsy readings had a significant impact on clinical management. Conclusion(s): A correlation between independent testis histology readings in azoospermic men demonstrates frequent inconsistencies. These differences contribute to inaccurate phenotyping of male infertility and can significantly impact the direction of infertility care. These findings highlight the need for a standardized approach to testis histologic review. (Fertil Steril 2005;84: by American Society for Reproductive Medicine.) Key Words: Testis biopsy, azoospermia, male infertility, spermatogenesis In infertility due to azoospermia, paternity can be achieved with spermatozoa retrieved from the testis in combination with in vitro fertilization (IVF) and intracytoplasmic sperm injection (ICSI) (1). In men with excurrent duct obstruction, sperm retrieval is not difficult; however, among men with severe testis failure or nonobstructive azoospermia, sperm for ICSI are not successfully retrieved in 25% to 50% of cases (2). In men with nonobstructive azoospermia, clinical features including testicular size, history of ejaculated sperm, serum follicle stimulating hormone level, or testis biopsy histology do not accurately predict whether sperm will be recovered during testicular exploration (2). However, among these variables, successful testicular sperm retrieval is most closely related to the type or pattern of spermatogenic defect observed on testicular biopsy (3). A close examination of the literature suggests that there is a wide variation in clinicians ability to locate sperm in testes that share commonly recognized histologic patterns. For example, in cases of Sertoli cell-only (germ cell aplasia) pathology, successful sperm retrieval occurs in 5% to 60% of cases (3 6). Although this may reflect differences in surgical technique among individuals and centers that specialize in male infertility care, we hypothesize this variation may also stem from inconsistent interpretation of biopsy histology by pathologists. To address the issue of interobserver variability in testis biopsy interpretation, we prospectively compared the findings from two independent testis histology readings performed on a cohort of patients with azoospermia. Our goal was to assess how uniformly pathologists read testis biopsy histology and delineate biopsy patterns that exhibit the widest variability in interpretation. Received September 21, 2004; revised and accepted May 13, Presented at the American Society for Reproductive Medicine, San Antonio, Texas, October 11 15, Reprint requests: Paul J. Turek, M.D., Department of Urology, 1600 Divisadero Street, A633, San Francisco, California (FAX: ; mrvas@itsa.ucsf.edu). MATERIALS AND METHODS As part of the evaluation of azoospermic patients referred to the Male Reproductive Health Center at the University of California at San Francisco, testis biopsy slides prepared at the referring institution are routinely procured and re-reviewed by a 672 Fertility and Sterility Vol. 84, No. 3, September /05/$30.00 Copyright 2005 American Society for Reproductive Medicine, Published by Elsevier Inc. doi: /j.fertnstert
2 single pathologist (I.C.). Histology re-reviews were performed prospectively, and were blinded to the original pathologic diagnosis. For the study, a third independent review summarized the written findings from the two readings and assessed each of the following: [1] specimen adequacy ( 25 seminiferous tubule cross-sections) (7), [2] presence or absence of fixation artifact (vacuole formation due to air-drying or fixation in formalin, or specimen overstaining or understaining), and [3] biopsy pattern. As described by Levin (8), biopsy patterns were categorized as normal spermatogenesis, hypoplasia or hypospermatogenesis (HYP), complete or early maturation arrest (EMA), Sertoli cell only (SCO), incomplete or late maturation arrest (LMA), or other (including sclerosis). When referral reports did not use this terminology, they were assigned to the category best fitting the recorded narrative description. If a biopsy contained a single histologic pattern throughout the specimen, it was deemed a pure pattern. If biopsies exhibited two or more patterns, then a mixed pattern was assigned. Mixed readings were further characterized in terms of the primary, or predominant, pattern and the secondary pattern. The frequency of each histologic pattern on paired readings was determined, and the concordance rate was calculated for each pattern. Overall agreement between original and second readings was assessed using the simple kappa statistic for interobserver agreement. Additionally, in each case, a determination was made whether the difference in histologic diagnosis between the two readings was clinically significant, defined as a difference that would confer a change in clinical management of the patient. The criteria for a clinically significant change include the following: [1] a change from normal to any abnormal pattern (i.e., change in presumed etiology from obstructive to nonobstructive azoospermia); [2] a change from any abnormal pattern to a normal pattern (i.e., change in presumed etiology from nonobstructive to obstructive azoospermia); [3] any pure pattern diagnosis without mature sperm (i.e., EMA, SCO) changed to a pure or mixed pattern that suggests presence of mature sperm (i.e., HYP or normal); and [4] any mixed pattern diagnosis without mature sperm (i.e., EMA, SCO) changed to a pure or mixed pattern that suggests mature sperm is present (i.e., HYP or normal). Finally, fertility pathways and outcomes for patients who met the criteria for a clinically significant change in management were examined to better understand the ultimate impact of these clinical decisions. RESULTS Over a 5-year period, 132 testis biopsies were evaluated. Of these, a formal histologic diagnosis from a referring institution was available for 113 (86%) cases. The median interval between the date of the biopsy procedure and the date of re-review was 5.5 months. Fixation artifact was noted in 18 cases (16%), making re-review difficult, and in 13 cases (12%) testis biopsy sample size was considered suboptimal for interpretation. Concordance Between Readings The concordance between histologic patterns assigned in the two readings original and review is outlined in Table 1. Several observations are evident from this comparison. The general frequency distribution of histologic patterns is similar between biopsy readings (except for mixed pattern readings). There is a 23% reduction in the diagnosis of normal spermat- TABLE 1 Concordance in testis histologic patterns between two readings. Review diagnosis Normal Hypo EMA LMA SCO Mixed Other Total Agree (%) Original diagnosis Normal Hypo EMA LMA SCO Mixed Other Total Agree (%) Note: Hypo hypoplasia or hypospermatogenesis; EMA early maturation arrest; LMA late maturation arrest; SCO Sertoli cell only. Cooperberg. Variability in testis biopsy analysis for infertility. Fertil Steril Fertility and Sterility 673
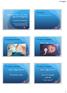
3 FIGURE 1 Examples of mixed testicular histology that resulted in changes in clinical care. (A) An area of normal spermatogenesis (arrow) is identified in a large biopsy sample originally read as pure sclerosis. (B) An area of late maturation arrest is identified (arrow) in a biopsy sample originally read as pure early maturation arrest. Cooperberg. Variability in testis biopsy analysis for infertility. Fertil Steril ogenesis when original (n 39, 35%) and review (n 30, 27%) readings are compared. The best concordance is observed with the SCO pattern, identified in 11 cases on both original and review examination, and in agreement in 91% (10/11) of cases. The overall simple kappa score for agreement between the original and review diagnoses is 0.43 (95% CI ). Discordance Between Readings There are also interesting observations in the patterns of discordance among biopsy-sample readings. Among biopsy samples originally read as normal (n 39), almost half (49%, n 19) were confirmed as normal on re-review, whereas 12% (n 5) demonstrated HYP and 39% (n 15) 674 Cooperberg et al. Variability in testis biopsy analysis for infertility Vol. 84, No. 3, September 2005
4 mixed histology. Clinically, this represents a significant shift in diagnosis, as many men considered normal (i.e., obstructed ) on the original review were not obstructed on re-review. However, the greatest source of discordance between the biopsy readings was the underappreciation of mixed histology by the original pathologist: 15 cases (13%) were felt to demonstrate mixed histology on the original reading whereas 41 cases (36%) were interpreted as mixed pattern on re-review, representing an almost threefold difference in detection rate. In addition, although most biopsies originally read as mixed pattern were re-reviewed as mixed pattern (80%), three others (20%) had pure pattern interpretations that included normal. Readings With Mixed Histologic Patterns Of the 41 cases read as mixed on review, 10 (24%) had a normal primary pattern, and an additional 10 (24%) had a normal secondary pattern. The primary pattern was HYP in 11 cases (27%), EMA in 7 (17%), LMA in 3 (7%), and SCO in 10 (24%). Of the 29 cases read as mixed on review but not on original reading, in 15 cases (52%) the review diagnosis correlated with the primary pattern of the mixed histology. Primary and secondary patterns in the mixed cases existed in virtually every potential combination, with the exception that EMA never coexisted with normal histology in the same testis. In 3 cases, three or four discrete histologic patterns were identified on review; only 1 of these cases was originally read as mixed. Significance of Differences in Readings Concerning the significance of the differences in biopsy readings, in 27% of the cases the differences in histology readings had significant impact on clinical management. In 14 cases (12%), an original reading of normal was reread as abnormal, suggesting nonobstructive azoospermia. In 11 cases (10%) an initial reading of abnormal was re-read as normal, suggesting obstructive azoospermia amenable to reconstructive surgery. In 5 cases (5%), a biopsy read as pure EMA, SCO, or other was reread as containing at least some normal, hypospermatogenic, or LMA spermatogenic elements, thus raising the potential for sperm retrieval. Figure 1 illustrates a case for which reinterpretation significantly changed the treatment plan. Fertility Follow-up Among Patients With Significantly Different Readings To determine whether altered clinical decisions among these 30 patients were accurate and actually resulted in improved clinical outcomes, information regarding subsequent fertility procedures was available for 26 couples (86%), and birth outcomes for 23 (77%). The mean partner age in this cohort was 33 years, and the overall birth rate was 63% in couples with known pregnancy outcomes. Among 10 patients with a change in diagnosis from nonobstructive to obstructive etiology, 3 underwent bilateral vasoepididymostomy, and all 3 achieved successful singleton pregnancies. Six patients elected microsurgical epididymal sperm aspiration (MESA) with IVF, after which 3 had successful pregnancies, 2 were unsuccessful, and 1 had an unknown outcome. One patient, whose spouse was 41 years of age, opted for testicular sperm aspiration (TESA) and did not achieve pregnancy. Of the 14 patients whose diagnoses changed from obstructive to nonobstructive azoospermia, one underwent vasoepididymostomy with a diagnosis of hypospermatogenesis and did not achieve a pregnancy. Two underwent varicocelectomy, resulting in one pregnancy and one adoption. Two opted for MESA, with one successfully conceiving after IVF. The remainder (n 9) elected testis mapping with fine-needle aspiration followed by TESA or testicular sperm extraction (TESE). Among 6 patients with known birth outcomes, 4 had successful pregnancies. Finally, 2 patients harbored mixed patterns on both original and review readings, but mature sperm were found only on re-review. Both patients proceeded to sperm retrieval with IVF/ICSI, and both had successful pregnancies (Table 2). DISCUSSION Although no clinical parameter correlates perfectly with the potential for sperm retrieval for ICSI, testis histology serves as one of the better surrogate markers. Testis histology as represented by a single biopsy site certainly does not accurately reflect overall testis biology, as significant spermatogenic variation has been shown to exist in infertile testes (9). Despite this limitation, an accurate assessment of testicular histology has been important for planning infertility treatment; the suggestion of even small areas of complete spermatogenesis makes successful sperm retrieval very likely. Despite the routine role of the testis biopsy in the diagnosis of azoospermia, the relationship between sperm retrieval success and histologic pattern on diagnostic biopsy varies widely from center to center. We hypothesized that some of this variation may be because of inconsistencies in histologic interpretation by pathologists. Indeed, this study confirms that there is wide interobserver discrepancy in the interpretation of samples from routine testis biopsies performed for azoospermia. One reason for the large interobserver discrepancy observed in testis biopsy interpretation could stem from the review of poorly prepared or insufficiently sized biopsy samples. We noted that over 25% of specimens showed such features, constituting a significant variable in reporting quality. Another explanation for interobserver discrepancy is that no particular method of testis biopsy evaluation is uniformly applied and serves as standard procedure for pathologists. Several testis biopsy interpretation algorithms have been reported in the last 3 decades. In general, they show large variations in the quantitative and qualitative assessment of spermatogenesis (7, 8, 10 12). The three most commonly Fertility and Sterility 675
5 TABLE 2 Changes in diagnosis affecting clinical management. Original diagnosis Review diagnosis Procedures Fertility outcome Partner age (y) Change in diagnosis from nonobstructive to obstructive Mixed (LMA EMA) Normal MESA Unknown 42 Hypo Normal VE, MESA Singleton-natural 32 Hypo Normal VE, MESA Singleton 31 Hypo Normal TESA No pregnancy 41 Hypo Normal MESA Twins 29 Hypo Normal MESA No pregnancy 39 Hypo Normal MESA No pregnancy 29 Hypo Normal MESA Singleton 29 Hypo Normal MESA Singleton 27 Hypo Normal VE, MESA Singleton-natural Unknown Change in diagnosis from obstructive to nonobstructive Normal Mixed (Normal Hypo) Varicocelectomy, IVF Singleton 35 Normal Mixed (Normal Hypo) TESE Unknown 32 Normal Mixed (Normal LMA) MESA Twins 28 Normal Mixed (Normal LMA) TESE No pregnancy 31 Normal Mixed (Hypo Normal) TESE Singleton 36 Normal Mixed (Hypo Normal) VE No pregnancy Unknown Normal Mixed (Hypo Normal) TESE Singleton 28 Normal Mixed (Hypo LMA) TESE Twins 26 Normal Mixed (Hypo LMA) TESA Unknown 30 Normal Mixed (Hypo LMA) TESA Singleton 35 Normal Mixed (LMA Normal) TESE Singleton 35 Normal Hypo TESA No pregnancy 30 Normal Hypo MESA No pregnancy 37 Normal Hypo Varicocelectomy No pregnancy Unknown No change in assumed etiology, but mature elements found on review only EMA Hypo TESE Singleton 40 EMA LMA Varicocelectomy Twins 30 Note: Hypo hypospermatogenesis; LMA late maturation arrest; EMA early maturation arrest; SCO Sertoli cell only; VE vasoepididymostomy; MESA microsurgical epididymal sperm aspiration; TESA testicular sperm aspiration; TESE testicular sperm extraction. Cooperberg. Variability in testis biopsy analysis for infertility. Fertil Steril cited scoring systems are those by Johnsen (11), Levin (8), and Silber and Rodriquez-Rigau (12). The Johnsen system is based on the idea that testis damage causes the successive disappearance of the most mature cell type (11); therefore, the scoring system involves a detailed, quantitative assessment of germ cell types and is considered too laborious for routine clinical use by most practicing pathologists. Based on an assessment of 21 patients, Silber and Rodriquez-Rigau (12) proposed a simpler quantitative scoring system that counts only mature spermatids. Finally, the scoring system proposed by Levin (8) is the most qualitative scoring system, involving the recognition of certain spermatogenic patterns that occur quite typically in infertility cases. No method is considered the standard, despite a great need for a uniform approach to testis biopsy sample interpretation. The issue of interobserver variability in testis biopsy interpretation is of increased importance in the era of ICSI. Indeed, we observed that clinical management was altered in 27% of patients when biopsy histology was re-reviewed by a single in-house pathologist. Such changes in clinical care treatment decisions vary from whether certain genetic risks are discussed with the patient, to the level of difficulty required for testis sperm retrieval or the ability to provide surgical reconstruction for obstructive azoospermia in cases previously deemed nonobstructive in nature. The validity of this analysis is supported by the comprehensive assessment of pregnancy outcomes in couples in whom fertility care was altered by histologic re-review, which demonstrated excellent overall success rates. 676 Cooperberg et al. Variability in testis biopsy analysis for infertility Vol. 84, No. 3, September 2005
6 Study limitations include the fact that that biopsy rereview was subject to similar, though albeit better controlled, restrictions defined earlier for any biopsy scoring system used in the analysis. However, the spirit of the study is to encourage clinicians to develop and partake in a uniformly acceptable method of assessing fertility potential in male infertility. The lack of a standard approach to testis biopsy sample histologic examination by pathologists may contribute to inaccurate phenotyping of male infertility. Such inaccuracy may significantly impact on the clinical care of patients. One area of variability in testis biopsy readings is the accurate identification of mixed spermatogenic patterns, as even a small number of tubules with complete spermatogenesis may yield viable spermatozoa for ICSI. Another concern is that the definition of normal spermatogenesis varies widely depending on the scoring system, a fact that can significantly alter the care of infertile men. We recommend that the clinical care of male infertility involve an experienced pathologist, working in close association with infertility clinicians. REFERENCES 1. Schlegel PN, Palermo GD, Goldstein M, Menendez S, Zaninovic N, Veeck LL, et al. Testicular sperm extraction with intracytoplasmic sperm injection for nonobstructive azoospermia. Urology 1997;49: Tournaye H, Verheyen G, Nagy P, Ubaldi F, Goossens A, Silber S, et al. Are there any predictive factors for successful testicular sperm recovery in azoospermic patients? Hum Reprod 1997;12: Su LM, Palermo GD, Goldstein M, Veeck LL, Rosenwaks Z, Schlegel PN. Testicular sperm extraction with intracytoplasmic sperm injection for nonobstructive azoospermia: testicular histology can predict success of sperm retrieval. J Urol 1999;161: Tournaye H, Liu J, Nagy PZ, Camus M, Goossens A, Silber S, et al. Correlation between testicular histology and outcome after intracytoplasmic sperm injection using testicular spermatozoa. Hum Reprod 1996;11: Seo JT, Ko WJ. Predictive factors of successful testicular sperm recovery in non-obstructive azoospermia patients. Int J Androl 2001;24: Meng MV, Cha I, Ljung BM, Turek PJ. Relationship between classic histological pattern and sperm findings on fine needle aspiration map in infertile men. Hum Reprod 2000;15: Steinberger E, Tijoe D. A method for quantitative analysis of human seminiferous epithelium. Fertil Steril 1968;19: Levin HS. Testicular biopsy in the study of male infertility: its current usefulness, histologic techniques, and prospects for the future. Hum Pathol 1979;10: Turek PJ, Ljung BM, Cha I, Conaghan J. Diagnostic findings from testis fine needle aspiration mapping in obstructed and nonobstructed azoospermic men. J Urol 2000;163: Meinhard E, McRae CU, Chisholm GD. Testicular biopsy in evaluation of male infertility. BMJ 1973;3: Johnsen SG. Testicular biopsy score count a method for registration of spermatogenesis in human testes: normal values and results in 335 hypogonadal males. Hormones 1970;1: Silber SJ, Rodriguez-Rigau LJ. Quantitative analysis of testicle biopsy: determination of partial obstruction and prediction of sperm count after surgery for obstruction. Fertil Steril 1981;36: Fertility and Sterility 677
Male factors determining the outcome of intracytoplasmic sperm injection with epididymal and testicular spermatozoa
 andrologia 35, 220 226 (2003) Accepted: April 25, 2003 Male factors determining the outcome of intracytoplasmic sperm injection with epididymal and testicular spermatozoa J. U. Schwarzer, K. Fiedler, I.
andrologia 35, 220 226 (2003) Accepted: April 25, 2003 Male factors determining the outcome of intracytoplasmic sperm injection with epididymal and testicular spermatozoa J. U. Schwarzer, K. Fiedler, I.
Testicular Biopsy in Males With Infertility: A Longitudinal Study
 Short Communication Iran J Pathol. 2017; 12(2): 177-182 Iranian Journal of Pathology ISSN: 2345-3656 Testicular Biopsy in Males With Infertility: A Longitudinal Study Sepideh Siadati 1*, Hamid Shafi 2,
Short Communication Iran J Pathol. 2017; 12(2): 177-182 Iranian Journal of Pathology ISSN: 2345-3656 Testicular Biopsy in Males With Infertility: A Longitudinal Study Sepideh Siadati 1*, Hamid Shafi 2,
With advances in assisted reproduction techniques,
 Journal of Andrology, Vol. 26, No. 6, November/December 2005 Copyright American Society of Andrology Clomiphene Administration for Cases of Nonobstructive Azoospermia: A Multicenter Study ALAYMAN HUSSEIN,*
Journal of Andrology, Vol. 26, No. 6, November/December 2005 Copyright American Society of Andrology Clomiphene Administration for Cases of Nonobstructive Azoospermia: A Multicenter Study ALAYMAN HUSSEIN,*
Predictive Factors of Successful Microdissection Testicular Sperm Extraction in Patients with Presumed Sertoli Cell-Only Syndrome
 Original Article Predictive Factors of Successful Microdissection Testicular Sperm Extraction in Patients with Presumed Sertoli Cell-Only Syndrome Tahereh Modarresi, M.Sc. 1, Hani Hosseinifar, M.Sc. 1,
Original Article Predictive Factors of Successful Microdissection Testicular Sperm Extraction in Patients with Presumed Sertoli Cell-Only Syndrome Tahereh Modarresi, M.Sc. 1, Hani Hosseinifar, M.Sc. 1,
Testicular fine needle aspiration as a diagnostic tool in nonobstructive
 Asian J Androl 2005; 7 (3): 289 294 DOI: 10.1111/j.1745-7262.2005.00043.x. Original Article. Testicular fine needle aspiration as a diagnostic tool in nonobstructive azoospermia A. Bettella 1, A. Ferlin
Asian J Androl 2005; 7 (3): 289 294 DOI: 10.1111/j.1745-7262.2005.00043.x. Original Article. Testicular fine needle aspiration as a diagnostic tool in nonobstructive azoospermia A. Bettella 1, A. Ferlin
Outcome of repeated micro-surgical testicular sperm extraction in patients with non-obstructive azoospermia
 Repeated micro-surgical testicular sperm extraction DOI: 10.1111/j.1745-7262.2007.00273.x www.asiaandro.com. Original Article. Outcome of repeated micro-surgical testicular sperm extraction in patients
Repeated micro-surgical testicular sperm extraction DOI: 10.1111/j.1745-7262.2007.00273.x www.asiaandro.com. Original Article. Outcome of repeated micro-surgical testicular sperm extraction in patients
Outcome of first and repeated testicular sperm extraction and ICSI in patients with non-obstructive azoospermia
 Human Reproduction Vol.17, No.9 pp. 2356 2361, 2002 Outcome of first and repeated testicular sperm extraction and ICSI in patients with non-obstructive azoospermia S.Friedler 1, A.Raziel, M.Schachter,
Human Reproduction Vol.17, No.9 pp. 2356 2361, 2002 Outcome of first and repeated testicular sperm extraction and ICSI in patients with non-obstructive azoospermia S.Friedler 1, A.Raziel, M.Schachter,
MALE FACTOR. Gerald J. Matthews, M.D.,* Ellen Dakin Matthews, R.N., and Marc Goldstein, M.D.*
 FERTILITY AND STERILITY VOL. 70, NO. 1, JULY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Induction
FERTILITY AND STERILITY VOL. 70, NO. 1, JULY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Induction
Effect of female partner age on pregnancy rates after vasectomy reversal
 MALE FACTOR Effect of female partner age on pregnancy rates after vasectomy reversal Edward R. Gerrard, Jr., M.D., a Jay I. Sandlow, b Robert A. Oster, Ph.D., c John R. Burns, M.D., a Lyndon C. Box, M.D.,
MALE FACTOR Effect of female partner age on pregnancy rates after vasectomy reversal Edward R. Gerrard, Jr., M.D., a Jay I. Sandlow, b Robert A. Oster, Ph.D., c John R. Burns, M.D., a Lyndon C. Box, M.D.,
Multiple testicular sampling in non-obstructive azoospermia is it necessary?
 Human Reproduction vol.13 no.11 pp.3081 3085, 1998 Multiple testicular sampling in non-obstructive azoospermia is it necessary? R.Hauser 1,3, A.Botchan 1, A.Amit 2, D.Ben Yosef 2, R.Gamzu 1, G.Paz 1, J.B.Lessing
Human Reproduction vol.13 no.11 pp.3081 3085, 1998 Multiple testicular sampling in non-obstructive azoospermia is it necessary? R.Hauser 1,3, A.Botchan 1, A.Amit 2, D.Ben Yosef 2, R.Gamzu 1, G.Paz 1, J.B.Lessing
Intracytoplasmic Sperm Injection Outcome Using Ejaculated Sperm and Retrieved Sperm in Azoospermic Men
 Sexual Dysfunction and Infertility Intracytoplasmic Sperm Injection Outcome Using Ejaculated Sperm and Retrieved Sperm in Azoospermic Men Tahira Naru, 1 M Nasir Sulaiman, 2 Atiya Kidwai, 3 M Hammad Ather,
Sexual Dysfunction and Infertility Intracytoplasmic Sperm Injection Outcome Using Ejaculated Sperm and Retrieved Sperm in Azoospermic Men Tahira Naru, 1 M Nasir Sulaiman, 2 Atiya Kidwai, 3 M Hammad Ather,
Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia
 Urology Journal UNRC/IUA Vol. 3, No. 2, 92-96 Spring 2006 Printed in IRAN Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia Seyed Amirmohsen Ziaee, 1 * Mohammadreza Ezzatnegad,
Urology Journal UNRC/IUA Vol. 3, No. 2, 92-96 Spring 2006 Printed in IRAN Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia Seyed Amirmohsen Ziaee, 1 * Mohammadreza Ezzatnegad,
Tomomoto ISHIKAWA and Masato FUJISAWA
 Microdissection testicular sperm extraction micro- TESE has become a recognized procedure for men with nonobstructive azoospermia NOA. Micro-TESE and intracytoplasmic sperm injection ICSI cycles expose
Microdissection testicular sperm extraction micro- TESE has become a recognized procedure for men with nonobstructive azoospermia NOA. Micro-TESE and intracytoplasmic sperm injection ICSI cycles expose
UroToday International Journal. Volume 2 - February 2009
 UroToday International Journal www.urotodayinternationaljournal.com Volume 2 - February 2009 Azoospermic Patients: Mosaic Pattern in Testicular Sperm Extraction Mai Ahmed Banakhar, Hassan A. Farsi, Suha
UroToday International Journal www.urotodayinternationaljournal.com Volume 2 - February 2009 Azoospermic Patients: Mosaic Pattern in Testicular Sperm Extraction Mai Ahmed Banakhar, Hassan A. Farsi, Suha
Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update
 Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update Fábio Firmbach Pasqualotto, M.D., Ph.D., Bernardo Passos Sobreiro, M.D., Jorge Hallak, M.D., Ph.D., Eleonora Bedin
Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update Fábio Firmbach Pasqualotto, M.D., Ph.D., Bernardo Passos Sobreiro, M.D., Jorge Hallak, M.D., Ph.D., Eleonora Bedin
Fertility with testicular sperm extraction and intracytoplasmic sperm injection in non-obstructive azoospermic men
 Human Reproduction vol. no.4 pp.75-70, 199 Fertility with testicular sperm extraction and intracytoplasmic sperm injection in non-obstructive azoospermic men Semra Kahraman 1-4, Suat Ozgur 2, Cengiz Alatas.
Human Reproduction vol. no.4 pp.75-70, 199 Fertility with testicular sperm extraction and intracytoplasmic sperm injection in non-obstructive azoospermic men Semra Kahraman 1-4, Suat Ozgur 2, Cengiz Alatas.
Patterns of Testicular Histopathology in Egyptian Azoospermic Men
 ISPUB.COM The Internet Journal of Urology Volume 13 Number 1 Patterns of Testicular Histopathology in Egyptian Azoospermic Men M K Khalifa, A M Issa, M O El Hamshary, K Z Shaeer Citation M K Khalifa, A
ISPUB.COM The Internet Journal of Urology Volume 13 Number 1 Patterns of Testicular Histopathology in Egyptian Azoospermic Men M K Khalifa, A M Issa, M O El Hamshary, K Z Shaeer Citation M K Khalifa, A
Enzymatic digestion of testicular tissue may rescue the intracytoplasmic sperm injection cycle in some patients with non-obstructive azoospermia
 Human Reproduction vol.13 no.10 pp.2791 2796, 1998 Enzymatic digestion of testicular tissue may rescue the intracytoplasmic sperm injection cycle in some patients with non-obstructive azoospermia E.Crabbé
Human Reproduction vol.13 no.10 pp.2791 2796, 1998 Enzymatic digestion of testicular tissue may rescue the intracytoplasmic sperm injection cycle in some patients with non-obstructive azoospermia E.Crabbé
Evaluation and Treatment of the Subfertile Male. Karen Baker, MD Associate Professor Duke University, Division of Urology
 Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Assisted reproduction for the treatment of azoospermia
 Assisted reproduction for the treatment of azoospermia Anat Safran 1, Benjamin E.Reubinoff, Anat Porat-Katz, Joseph G.Schenker and Aby Lewin IVF Unit, Department of Obstetrics and Gynecology, Hadassah
Assisted reproduction for the treatment of azoospermia Anat Safran 1, Benjamin E.Reubinoff, Anat Porat-Katz, Joseph G.Schenker and Aby Lewin IVF Unit, Department of Obstetrics and Gynecology, Hadassah
How successful is TESE-ICSI in couples with non-obstructive azoospermia?
 Human Reproduction, Vol.30, No.8 pp. 1790 1796, 2015 Advanced Access publication on June 16, 2015 doi:10.1093/humrep/dev139 ORIGINAL ARTICLE Andrology How successful is TESE-ICSI in couples with non-obstructive
Human Reproduction, Vol.30, No.8 pp. 1790 1796, 2015 Advanced Access publication on June 16, 2015 doi:10.1093/humrep/dev139 ORIGINAL ARTICLE Andrology How successful is TESE-ICSI in couples with non-obstructive
Abstract. Introduction. RBMOnline - Vol 19. No Reproductive BioMedicine Online; on web 12 October 2009
 RBMOnline - Vol 19. No 6. 2009 778 783 Reproductive BioMedicine Online; www.rbmonline.com/article/4178 on web 12 October 2009 Article Does age at orchidopexy impact on the results of testicular sperm extraction?
RBMOnline - Vol 19. No 6. 2009 778 783 Reproductive BioMedicine Online; www.rbmonline.com/article/4178 on web 12 October 2009 Article Does age at orchidopexy impact on the results of testicular sperm extraction?
Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients
 Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients Basim Sh. Ahmed F.I.C.M.S Department of Pathology, College of Medicine, Al-Mustansiriya University, Baghdad,
Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients Basim Sh. Ahmed F.I.C.M.S Department of Pathology, College of Medicine, Al-Mustansiriya University, Baghdad,
Use of Testicular Sperm for ICSI in Non-Azoospermic Men: How Far Should we Go?
 Use of Testicular Sperm for ICSI in Non-Azoospermic Men: How Far Should we Go? Armand Zini, MD, FRCSC McGill University Disclosure: Shareholder in YAD Tech Neutraceuticals Co. Sperm Retrieval: Overview
Use of Testicular Sperm for ICSI in Non-Azoospermic Men: How Far Should we Go? Armand Zini, MD, FRCSC McGill University Disclosure: Shareholder in YAD Tech Neutraceuticals Co. Sperm Retrieval: Overview
Fine-Needle Aspiration Cytology of the Testis: Can It Be a Single Diagnostic Modality in Azoospermia?
 Urologia Internationalis Original Paper Urol Int 2004;73:23 27 DOI: 10.1159/000078799 Received: July 16, 2003 Accepted after revision: October 29, 2003 Fine-Needle Aspiration Cytology of the Testis: Can
Urologia Internationalis Original Paper Urol Int 2004;73:23 27 DOI: 10.1159/000078799 Received: July 16, 2003 Accepted after revision: October 29, 2003 Fine-Needle Aspiration Cytology of the Testis: Can
A comparison between open and percutaneous needle biopsies in men with azoospermia
 Human Reproduction vol.13 no.5 pp.1266 1271, 1998 A comparison between open and percutaneous needle biopsies in men with azoospermia B.Rosenlund 1,6, U.Kvist 3, L.Plöen 4, B.Lundh Rozell 2, P.Sjöblom 1
Human Reproduction vol.13 no.5 pp.1266 1271, 1998 A comparison between open and percutaneous needle biopsies in men with azoospermia B.Rosenlund 1,6, U.Kvist 3, L.Plöen 4, B.Lundh Rozell 2, P.Sjöblom 1
Surgical Sperm Retrieval
 Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
MATERIALS AND METHODS
 www.kjurology.org http://dx.doi.org/1.4111/kju.213.54.2.111 Male Infertility Detection of Y Chromosome Microdeletion is Valuable in the Treatment of Patients With Nonobstructive Azoospermia and Oligoasthenoteratozoospermia:
www.kjurology.org http://dx.doi.org/1.4111/kju.213.54.2.111 Male Infertility Detection of Y Chromosome Microdeletion is Valuable in the Treatment of Patients With Nonobstructive Azoospermia and Oligoasthenoteratozoospermia:
Sherman J.Silber 1,3, Zsolt Nagy 2, Paul Devroey 2, Michel Camus 2 and André C.Van Steirteghem 2
 Human Reproduction vol.12 no.12 pp.2693 2700, 1997 The effect of female age and ovarian reserve on pregnancy rate in male infertility: treatment of azoospermia with sperm retrieval and intracytoplasmic
Human Reproduction vol.12 no.12 pp.2693 2700, 1997 The effect of female age and ovarian reserve on pregnancy rate in male infertility: treatment of azoospermia with sperm retrieval and intracytoplasmic
Infertility is not an uncommon problem in Western
 Review Article A Practical Approach to Testicular Biopsy Interpretation for Male Infertility Lisa A. Cerilli, MD; Wayne Kuang, MD; David Rogers, MD Infertility is not an uncommon problem in Western societies
Review Article A Practical Approach to Testicular Biopsy Interpretation for Male Infertility Lisa A. Cerilli, MD; Wayne Kuang, MD; David Rogers, MD Infertility is not an uncommon problem in Western societies
MICROSCOPIC TESTICULAR SPERM EXTRACTION; IN PATIENTS OF NON-OBSTRUCTIVE AZOOSPERMIA WITH HISTPATHOLOGIC, CYTOGENETIC AND HORMONAL VARIATIONS.
 The Professional Medical Journal DOI: 10.29309/TPMJ/18.4055 ORIGINAL PROF-4055 1. MD, FRCSC, FEBU,. 2. FACS, FCPS, FRCSEd Ex. Assistant Assistant Prof. Urology, University Medical & Dental College, Madina
The Professional Medical Journal DOI: 10.29309/TPMJ/18.4055 ORIGINAL PROF-4055 1. MD, FRCSC, FEBU,. 2. FACS, FCPS, FRCSEd Ex. Assistant Assistant Prof. Urology, University Medical & Dental College, Madina
Extended sperm preparation: an alternative to testicular sperm extraction in non-obstructive azoospermia
 Human Reproduction vol.12 no.6 pp.1222 1226, 1997 Extended sperm preparation: an alternative to testicular sperm extraction in non-obstructive azoospermia R.Ron-El 1, D.Strassburger, S.Friedler, D.Komarovski,
Human Reproduction vol.12 no.6 pp.1222 1226, 1997 Extended sperm preparation: an alternative to testicular sperm extraction in non-obstructive azoospermia R.Ron-El 1, D.Strassburger, S.Friedler, D.Komarovski,
Male Fertility: Your Questions Answered
 Male Fertility: Your Questions Answered Michael S. Neal Scientific Director, ONE Fertility, 3210 Harvester Rd. Burlington, Ontario www.onefertility.com mneal@onefertility.com Outline Assisted Conception
Male Fertility: Your Questions Answered Michael S. Neal Scientific Director, ONE Fertility, 3210 Harvester Rd. Burlington, Ontario www.onefertility.com mneal@onefertility.com Outline Assisted Conception
Male Factor Infertility and Health. Karen Baker, MD Associate Professor Duke University, Division of Urology
 Male Factor Infertility and Health Karen Baker, MD Associate Professor Duke University, Division of Urology Fertility and Cancer Heart disease Metabolic syndrome Diabetes Early death Goals: Review literature
Male Factor Infertility and Health Karen Baker, MD Associate Professor Duke University, Division of Urology Fertility and Cancer Heart disease Metabolic syndrome Diabetes Early death Goals: Review literature
Cryptorchidism and its impact on male fertility: a state of art review of current literature. Case 1
 CASE REPORT Cryptorchidism and its impact on male fertility: a state of art review of current literature Eric Chung, MBBS, FRACS; Gerald B. Brock, MD, FRCSC Division of Urology, University of Western Ontario,
CASE REPORT Cryptorchidism and its impact on male fertility: a state of art review of current literature Eric Chung, MBBS, FRACS; Gerald B. Brock, MD, FRCSC Division of Urology, University of Western Ontario,
Effects of Cryopreservation on the Ultrastructure of Human Testicular Sperm
 Journal of Reproduction & Contraception (2005) 16 (4):195-200 ORIGINAL PAPER Effects of Cryopreservation on the Ultrastructure of Human Testicular Sperm Xin-qiang LAI 1, Wei-jie ZHU 2, Jing LI 3, Fu-xing
Journal of Reproduction & Contraception (2005) 16 (4):195-200 ORIGINAL PAPER Effects of Cryopreservation on the Ultrastructure of Human Testicular Sperm Xin-qiang LAI 1, Wei-jie ZHU 2, Jing LI 3, Fu-xing
Microsurgical Management of the Infertile Male
 Microsurgical Management of the Infertile Male a report by Jonathan D Schiff, MD and Natan Bar-Chama, MD Assistant Clinical Professor of Urology and Associate Professor of Urology, Obstetrics/Gynecology
Microsurgical Management of the Infertile Male a report by Jonathan D Schiff, MD and Natan Bar-Chama, MD Assistant Clinical Professor of Urology and Associate Professor of Urology, Obstetrics/Gynecology
REAPPRAISAL OF THE VALUE OF TESTICULAR BIOPSY IN THE INVESTIGATION OF INFERTILITY
 FERTWTY AND STEIuLlTY Copyright 1980 The American Fertility Society Vol., No.1 January 1980 Prinwl in U.S.A. REAPPRAISAL OF THE VALUE OF TESTICULAR BIOPSY IN THE INVESTIGATION OF INFERTILITY TERENCE
FERTWTY AND STEIuLlTY Copyright 1980 The American Fertility Society Vol., No.1 January 1980 Prinwl in U.S.A. REAPPRAISAL OF THE VALUE OF TESTICULAR BIOPSY IN THE INVESTIGATION OF INFERTILITY TERENCE
A new power Doppler ultrasound guiding technique for improved testicular sperm extraction
 FERTILITY AND STERILITY VOL. 81, NO. 2, FEBRUARY 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. A new power Doppler ultrasound
FERTILITY AND STERILITY VOL. 81, NO. 2, FEBRUARY 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. A new power Doppler ultrasound
Surgical management of nonobstructive azoospermia
 Asian Journal of Urology (2015) 2, 85e91 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur REVIEW Surgical management of nonobstructive azoospermia
Asian Journal of Urology (2015) 2, 85e91 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur REVIEW Surgical management of nonobstructive azoospermia
Getting Help for Obstructive Azoospermia A BASIC GUIDE TO MALE. A doctor s guide for patients developed by the American Urological Association, Inc.
 A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
Cryopreservation of human spermatozoa within human or mouse empty zona pellucidae
 FERTILITY AND STERILITY VOL. 73, NO. 4, APRIL 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Cryopreservation of
FERTILITY AND STERILITY VOL. 73, NO. 4, APRIL 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Cryopreservation of
Sperm retrieval techniques
 Chapter5 Sperm retrieval techniques Sandro C. Esteves and Ashok Agarwal Introduction Two major breakthroughs occurred in the area of male infertility only 2 to 3 years apart [1 3]. The first was the development
Chapter5 Sperm retrieval techniques Sandro C. Esteves and Ashok Agarwal Introduction Two major breakthroughs occurred in the area of male infertility only 2 to 3 years apart [1 3]. The first was the development
Aspiration flow cytometry of the testes in the evaluation of spermatogenesis in the infertile male*t
 FERTILITY AND STERILITY Copyright e 1987 The American Fertility Society Printed in U.S.A. Aspiration flow cytometry of the testes in the evaluation of spermatogenesis in the infertile male*t David G. Kaufman,
FERTILITY AND STERILITY Copyright e 1987 The American Fertility Society Printed in U.S.A. Aspiration flow cytometry of the testes in the evaluation of spermatogenesis in the infertile male*t David G. Kaufman,
Induction of spermatogenesis in azoospermic men after varicocele repair
 Human Reproduction Vol.18, No.1 pp. 108±112, 2003 DOI: 10.1093/humrep/deg032 Induction of spermatogenesis in azoospermic men after varicocele repair FaÂbio F.Pasqualotto 1, AntoÃnio M.Lucon, Jorge Hallak,
Human Reproduction Vol.18, No.1 pp. 108±112, 2003 DOI: 10.1093/humrep/deg032 Induction of spermatogenesis in azoospermic men after varicocele repair FaÂbio F.Pasqualotto 1, AntoÃnio M.Lucon, Jorge Hallak,
U.I.O.Ezeh 1, H.D.M.Moore 1,2,3 and I.D.Cooke 1
 Human Reproduction vol.13 no.11 pp.3066 3074, 1998 Correlation of testicular sperm extraction with morphological, biophysical and endocrine profiles in men with azoospermia due to primary gonadal failure
Human Reproduction vol.13 no.11 pp.3066 3074, 1998 Correlation of testicular sperm extraction with morphological, biophysical and endocrine profiles in men with azoospermia due to primary gonadal failure
Outline. History of sperm freezing. Testicular tissue: When and how should it be cryopreserved?
 Testicular tissue: When and how should it be cryopreserved? Greta Verheyen Centre for Reproductive Medicine UZ Brussel, Belgium ESHRE Campus Granada 25-26 March 2010 Outline History of sperm freezing Indications
Testicular tissue: When and how should it be cryopreserved? Greta Verheyen Centre for Reproductive Medicine UZ Brussel, Belgium ESHRE Campus Granada 25-26 March 2010 Outline History of sperm freezing Indications
INTRACYTOPLASMIC SPERM INJECTION
 1 Background... 2 2 Male Factor Infertility... 2 3 ICSI... 3 4 Surgical sperm aspiration... 4 5 What is the chance of success?... 6 6 What are the risks?... 7 M Rajkhowa, October 2004 Authorised by V Kay
1 Background... 2 2 Male Factor Infertility... 2 3 ICSI... 3 4 Surgical sperm aspiration... 4 5 What is the chance of success?... 6 6 What are the risks?... 7 M Rajkhowa, October 2004 Authorised by V Kay
CUA Guideline: The workup of azoospermic males
 CUA GUIDELINE CUA Guideline: The workup of azoospermic males Keith Jarvi, MD, FRCSC; Kirk Lo, MD, FRCSC; Anthony Fischer, MD, FRCSC; John Grantmyre, MD, FRCSC; Armand Zini, MD, FRCSC; Victor Chow, MD,
CUA GUIDELINE CUA Guideline: The workup of azoospermic males Keith Jarvi, MD, FRCSC; Kirk Lo, MD, FRCSC; Anthony Fischer, MD, FRCSC; John Grantmyre, MD, FRCSC; Armand Zini, MD, FRCSC; Victor Chow, MD,
Fertility options after vasectomy: a cost-effectiveness analysis
 FERTILITY AND STERILITY '~v Vol. 67, No. 1, January. 1997 Ct~pyright ' 1997 American Sf)eiety tbr Rep,'~Jductive Medicine Printed on acid-free paper in U. S. A. Fertility options after vasectomy: a cost-effectiveness
FERTILITY AND STERILITY '~v Vol. 67, No. 1, January. 1997 Ct~pyright ' 1997 American Sf)eiety tbr Rep,'~Jductive Medicine Printed on acid-free paper in U. S. A. Fertility options after vasectomy: a cost-effectiveness
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia
 Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Article Computational models for prediction of IVF/ICSI outcomes with surgically retrieved spermatozoa
 RBMOnline - Vol 11. No 3. 2005 325-331 Reproductive BioMedicine Online; www.rbmonline.com/article/1800 on web 11 July 2005 Article Computational models for prediction of IVF/ICSI outcomes with surgically
RBMOnline - Vol 11. No 3. 2005 325-331 Reproductive BioMedicine Online; www.rbmonline.com/article/1800 on web 11 July 2005 Article Computational models for prediction of IVF/ICSI outcomes with surgically
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Male infertility too often ignored & forgotten
 Male infertility too often ignored & forgotten The journey 1. of the men A review of the guidelines Joo Teoh FRANZCOG MRCP(Ire) MRCOG MBBCh MSc(Lon) MD(Glasgow) SubspecialtyRepromed(UK) Consultant Obstetrician
Male infertility too often ignored & forgotten The journey 1. of the men A review of the guidelines Joo Teoh FRANZCOG MRCP(Ire) MRCOG MBBCh MSc(Lon) MD(Glasgow) SubspecialtyRepromed(UK) Consultant Obstetrician
Sperm recovery and IVF outcome after surgical sperm retrieval in azoospermia: our experience
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Rai S et al. Int J Reprod Contracept Obstet Gynecol. 2018 Feb;7(2):xxx-xxx www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20180019
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Rai S et al. Int J Reprod Contracept Obstet Gynecol. 2018 Feb;7(2):xxx-xxx www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20180019
The effect of testicular nongerm cell tumors on local spermatogenesis
 FERTILITY AND STERILITY Vol. 62, No.1, July 1994 Copyright" 1994 The American Fertility Society Printed on acid-free paper in U. S. A. The effect of testicular nongerm cell tumors on local spermatogenesis
FERTILITY AND STERILITY Vol. 62, No.1, July 1994 Copyright" 1994 The American Fertility Society Printed on acid-free paper in U. S. A. The effect of testicular nongerm cell tumors on local spermatogenesis
COMMISSIONING POLICY. Tertiary treatment for assisted conception services
 Final Version COMMISSIONING POLICY Tertiary treatment for assisted conception services Designated providers for patients registered with a Worcestershire GP BMI The Priory Hospital, Birmingham - 1 - Commissioning
Final Version COMMISSIONING POLICY Tertiary treatment for assisted conception services Designated providers for patients registered with a Worcestershire GP BMI The Priory Hospital, Birmingham - 1 - Commissioning
Clinical Study Predictive Factors for Natural Pregnancy after Microsurgical Reconstruction in Patients with Primary Epididymal Obstructive Azoospermia
 International Endocrinology, Article ID 873527, 6 pages http://dx.doi.org/10.1155/2014/873527 Clinical Study Predictive Factors for Natural Pregnancy after Microsurgical Reconstruction in Patients with
International Endocrinology, Article ID 873527, 6 pages http://dx.doi.org/10.1155/2014/873527 Clinical Study Predictive Factors for Natural Pregnancy after Microsurgical Reconstruction in Patients with
MALE FACTOR. Liverpool Women s Hospital, Liverpool, England
 MALE FACTOR FERTILITY AND STERILITY VOL. 77, NO. 6, JUNE 2002 Copyright 2002 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Reproductive
MALE FACTOR FERTILITY AND STERILITY VOL. 77, NO. 6, JUNE 2002 Copyright 2002 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Reproductive
Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy
 Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy Wayland Hsiao, James S. Rosoff, Joseph R. Pale, Eleni A. Greenwood
Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy Wayland Hsiao, James S. Rosoff, Joseph R. Pale, Eleni A. Greenwood
I would be happy to discuss all of these options for fertility after vasectomy with you at the time of our consultation or over the phone.
 F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
PERCUTANEOUS EPIDIDYMAL SPERM ASPIRATION (PESA) IN MEN WITH OBSTRUCTIVE AZOOSPERMIA
 Clinical Urology PESA IN OBSTRUCTIVE AZOOSPERMIA International Braz J Urol Vol. 29 (2): 4-46, March - April, 2003 Official Journal of the Brazilian Society of Urology PERCUTANEOUS EPIDIDYMAL SPERM ASPIRATION
Clinical Urology PESA IN OBSTRUCTIVE AZOOSPERMIA International Braz J Urol Vol. 29 (2): 4-46, March - April, 2003 Official Journal of the Brazilian Society of Urology PERCUTANEOUS EPIDIDYMAL SPERM ASPIRATION
PROCEDURES LAPAROSCOPY
 PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
Sperm retrieval from patients with nonmosaic Klinefelter s syndrome by semen cytology examination
 Sperm retrieval from patients with nonmosaic Klinefelter s syndrome by semen cytology examination Y.-T. Jiang 1, Y. Dong 1, X.-W. Yu 1, R.-C. Du 1,2, L.-L. Li 1,2, H.-G. Zhang 1 and R.-Z. Liu 1 1 Center
Sperm retrieval from patients with nonmosaic Klinefelter s syndrome by semen cytology examination Y.-T. Jiang 1, Y. Dong 1, X.-W. Yu 1, R.-C. Du 1,2, L.-L. Li 1,2, H.-G. Zhang 1 and R.-Z. Liu 1 1 Center
MALE FACTOR. Use of frozen-thawed testicular sperm for intracytoplasmic sperm injection
 FERTILITY AND STERILITY VOL. 73, NO. 3, MARCH 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Use of frozen-thawed
FERTILITY AND STERILITY VOL. 73, NO. 3, MARCH 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Use of frozen-thawed
Clinical Policy Committee
 Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Microdissection testicular sperm extraction: an update
 (2013) 15, 35 39 ß 2013 AJA, SIMM & SJTU. All rights reserved 1008-682X/13 $32.00 www.nature.com/aja REVIEW Microdissection testicular sperm extraction: an update Ali A Dabaja and Peter N Schlegel Patients
(2013) 15, 35 39 ß 2013 AJA, SIMM & SJTU. All rights reserved 1008-682X/13 $32.00 www.nature.com/aja REVIEW Microdissection testicular sperm extraction: an update Ali A Dabaja and Peter N Schlegel Patients
MALE FACTOR. Preoperative semen analysis as a predictor of seminal improvement following varicocelectomy
 FERTILITY AND STERILITY VOL. 75, NO. 1, JANUARY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Preoperative
FERTILITY AND STERILITY VOL. 75, NO. 1, JANUARY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Preoperative
Azoospermia, which is the complete absence of
 SEXUAL DYSFUNCTION AND INFERTILITY Evaluation of Microdissection Testicular Sperm Extraction Results in Patients with Non-Obstructive Azoospermia: Independent Predictive Factors and Best Cutoff Values
SEXUAL DYSFUNCTION AND INFERTILITY Evaluation of Microdissection Testicular Sperm Extraction Results in Patients with Non-Obstructive Azoospermia: Independent Predictive Factors and Best Cutoff Values
Abstract. Introduction. RBMOnline - Vol 18. No Reproductive BioMedicine Online; on web 8 January 2009
 RBMOnline - Vol 18. No 3. 2009 315-319 Reproductive BioMedicine Online; www.rbmonline.com/article/3549 on web 8 January 2009 Article Microsurgical TESE versus conventional TESE for ICSI in non-obstructive
RBMOnline - Vol 18. No 3. 2009 315-319 Reproductive BioMedicine Online; www.rbmonline.com/article/3549 on web 8 January 2009 Article Microsurgical TESE versus conventional TESE for ICSI in non-obstructive
ASSISTED REPRODUCTIVE TECHNOLOGIES (ART)
 ASSISTED REPRODUCTIVE TECHNOLOGIES (ART) Dr. Herve Lucas, MD, PhD, Biologist, Andrologist Dr. Taher Elbarbary, MD Gynecologist-Obstetrician Geneva Foundation for Medical Education and research Definitions
ASSISTED REPRODUCTIVE TECHNOLOGIES (ART) Dr. Herve Lucas, MD, PhD, Biologist, Andrologist Dr. Taher Elbarbary, MD Gynecologist-Obstetrician Geneva Foundation for Medical Education and research Definitions
Yang Yu, Qun Wang, Hongguo Zhang, Linlin Li, Dongliang Zhu, Ruizhi Liu
 Int J Clin Exp Med 2017;10(3):5338-5343 www.ijcem.com /ISSN:1940-5901/IJCEM0041408 Original Article Relationship of paternal age with outcome of percutaneous epididymal sperm aspiration and testicular
Int J Clin Exp Med 2017;10(3):5338-5343 www.ijcem.com /ISSN:1940-5901/IJCEM0041408 Original Article Relationship of paternal age with outcome of percutaneous epididymal sperm aspiration and testicular
TESE: Testis Sperm Extraction
 TESE: Testis Sperm Extraction Robert D. Oates, M.D., F.A.C.S. Department of Urology Boston University School of Medicine When is Microsurgical TESE indicated? Cases of Non-obstructive Azoospermia (NOA)
TESE: Testis Sperm Extraction Robert D. Oates, M.D., F.A.C.S. Department of Urology Boston University School of Medicine When is Microsurgical TESE indicated? Cases of Non-obstructive Azoospermia (NOA)
Effect Of Obstruction To Sperm Egress On The Male Testis And Epididymis
 ISPUB.COM The Internet Journal of Urology Volume 8 Number 1 Effect Of Obstruction To Sperm Egress On The Male Testis And Epididymis A Sarda, D Pandey, S Bhalla, S Gupta, N Khurana Citation A Sarda, D Pandey,
ISPUB.COM The Internet Journal of Urology Volume 8 Number 1 Effect Of Obstruction To Sperm Egress On The Male Testis And Epididymis A Sarda, D Pandey, S Bhalla, S Gupta, N Khurana Citation A Sarda, D Pandey,
A decision analysis of treatments for obstructive azoospermia
 Human Reproduction Vol.23, No.9 pp. 2043 2049, 2008 Advance Access publication on June 13, 2008 doi:10.1093/humrep/den200 A decision analysis of treatments for obstructive azoospermia R. Lee 1,2, P.S.
Human Reproduction Vol.23, No.9 pp. 2043 2049, 2008 Advance Access publication on June 13, 2008 doi:10.1093/humrep/den200 A decision analysis of treatments for obstructive azoospermia R. Lee 1,2, P.S.
Microdissection testicular sperm extraction causes spermatogenic alterations in the contralateral testis
 causes spermatogenic alterations in the contralateral testis A.B. Oliveira Filho 1, R.S. Souza 2, M.T.V. Azeredo-Oliveira 2, R.L. Peruquetti 2 and A.P. Cedenho 1 1 Departamento de Cirurgia, Divisão de
causes spermatogenic alterations in the contralateral testis A.B. Oliveira Filho 1, R.S. Souza 2, M.T.V. Azeredo-Oliveira 2, R.L. Peruquetti 2 and A.P. Cedenho 1 1 Departamento de Cirurgia, Divisão de
Microscopic varicocelectomy as a treatment option for patients with severe oligospermia
 Original Article - Sexual Dysfunction/Infertility pissn 2466-0493 eissn 2466-054X Microscopic varicocelectomy as a treatment option for patients with severe oligospermia Chirag Gupta 1, Arun Chinchole
Original Article - Sexual Dysfunction/Infertility pissn 2466-0493 eissn 2466-054X Microscopic varicocelectomy as a treatment option for patients with severe oligospermia Chirag Gupta 1, Arun Chinchole
ORIGINAL ARTICLE. V. Mitchell,* G. Robin, à F. Boitrelle, P. Massart, C. Marchetti, F. Marcelli and J.-M. Rigot. Summary
 international journal of andrology ISSN 0105-6263 ORIGINAL ARTICLE Correlation between testicular sperm extraction outcomes and clinical, endocrine and testicular histology parameters in 120 azoospermic
international journal of andrology ISSN 0105-6263 ORIGINAL ARTICLE Correlation between testicular sperm extraction outcomes and clinical, endocrine and testicular histology parameters in 120 azoospermic
Histological findings of testicular biopsy in North Indian population
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Mahajan A et al. Int J Reprod Contracept Obstet Gynecol. 2015 Apr;4(2):432-438 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Mahajan A et al. Int J Reprod Contracept Obstet Gynecol. 2015 Apr;4(2):432-438 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
Male Factor Infertility
 Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Immune response in obstructive male infertility. Prof. A.K.Sarda Department of Surgery Maulana Azad Medical College New Delhi
 Immune response in obstructive male infertility Prof. A.K.Sarda Department of Surgery Maulana Azad Medical College New Delhi Sperm transport from the testicle Seminiferous tubule contractions of the myoid
Immune response in obstructive male infertility Prof. A.K.Sarda Department of Surgery Maulana Azad Medical College New Delhi Sperm transport from the testicle Seminiferous tubule contractions of the myoid
CUA Guideline: The workup and management of azoospermic males
 Original cua guideline research CUA Guideline: The workup and management of azoospermic males Keith Jarvi, MD, FRCSC; * Kirk Lo, MD, FRCSC; * Ethan Grober, MD; * Victor Mak, MD, FRCSC; * Anthony Fischer,
Original cua guideline research CUA Guideline: The workup and management of azoospermic males Keith Jarvi, MD, FRCSC; * Kirk Lo, MD, FRCSC; * Ethan Grober, MD; * Victor Mak, MD, FRCSC; * Anthony Fischer,
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
HHS Public Access Author manuscript Basic Clin Androl. Author manuscript; available in PMC 2015 March 09.
 Predictive factors of successful microdissection testicular sperm extraction Aaron M. Bernie, Ranjith Ramasamy, and Peter N. Schlegel * Department of Urology, Weill Cornell Medical College, New York-Presbyterian
Predictive factors of successful microdissection testicular sperm extraction Aaron M. Bernie, Ranjith Ramasamy, and Peter N. Schlegel * Department of Urology, Weill Cornell Medical College, New York-Presbyterian
Comparative studies of spermatogenesis in fertile and
 J Clin Pathol 1981 ;34:145-150 Comparative studies of spermatogenesis in fertile and subfertile men MA LAMONT,* MJW FAED,* AND K BAXBYt From the *Cytogenetics Laboratory, Ninewells Hospital and Medical
J Clin Pathol 1981 ;34:145-150 Comparative studies of spermatogenesis in fertile and subfertile men MA LAMONT,* MJW FAED,* AND K BAXBYt From the *Cytogenetics Laboratory, Ninewells Hospital and Medical
Spermatogenesis Following Experimental Testicular Ischemia
 Spermatogenesis Following Experimental Testicular Ischemia Frank Hinman, Jr, MD, and Gilbert I Smith, MD REGENERATION of the spermatogenic elements of the testis after depression by testosterone and by
Spermatogenesis Following Experimental Testicular Ischemia Frank Hinman, Jr, MD, and Gilbert I Smith, MD REGENERATION of the spermatogenic elements of the testis after depression by testosterone and by
Postgraduate Training in Reproductive Health
 SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients
 Urol Sci 2010;21(1):30 37 ORIGINAL ARTICLE Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients Chia-Feng Lee 1, Pei-Yu Lin 1,2, I-Hung Chen 1,2, Yu-Sheng Cheng 1,2,
Urol Sci 2010;21(1):30 37 ORIGINAL ARTICLE Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients Chia-Feng Lee 1, Pei-Yu Lin 1,2, I-Hung Chen 1,2, Yu-Sheng Cheng 1,2,
Intratubular Germ Cell Neoplasia of the Testis
 Intratubular Germ Cell Neoplasia of the Testis KS Ngoo Department of Urology Hospital Selayang Advanced Urology Course 15 Aug 2014 MUA Office Clinical scenario A 33 years old man has bilateral testicular
Intratubular Germ Cell Neoplasia of the Testis KS Ngoo Department of Urology Hospital Selayang Advanced Urology Course 15 Aug 2014 MUA Office Clinical scenario A 33 years old man has bilateral testicular
WHAT IS A PATIENT CARE ADVOCATE?
 WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
ANDROLOGY. Introduction. Original Article. Serkan Karamazak, Fuat Kızılay, Tuncer Bahçeci, Bülent Semerci ABSTRACT
 202 Turk J Urol 2018; 44(3): 202-7 DOI: 10.5152/tud.2017.80000 ANDROLOGY Original Article Do body mass index, hormone profile and testicular volume effect sperm retrieval rates of microsurgical sperm extraction
202 Turk J Urol 2018; 44(3): 202-7 DOI: 10.5152/tud.2017.80000 ANDROLOGY Original Article Do body mass index, hormone profile and testicular volume effect sperm retrieval rates of microsurgical sperm extraction
ICSI Cycle with a Sperm from TESE versus From Ejaculate in Oligospermic Men
 ICSI Cycle with a Sperm from TESE versus From Ejaculate in Oligospermic Men Hassan S.O. Abduljabbar Ohoud Al-Shamrani Osama Bajouh King Abdulaziz University, P.O.Box 8215 Jeddah 21452, Kingdom of Saudi
ICSI Cycle with a Sperm from TESE versus From Ejaculate in Oligospermic Men Hassan S.O. Abduljabbar Ohoud Al-Shamrani Osama Bajouh King Abdulaziz University, P.O.Box 8215 Jeddah 21452, Kingdom of Saudi
Outcome of varicocele repair in men with nonobstructive azoospermia: systematic review and meta analysis
 (2016) 18, 246 253 2016 AJA, SIMM & SJTU. All rights reserved 1008-682X www.asiaandro.com; www.ajandrology.com Male Fertility Open Access INVITED REVIEW Outcome of varicocele repair in men with nonobstructive
(2016) 18, 246 253 2016 AJA, SIMM & SJTU. All rights reserved 1008-682X www.asiaandro.com; www.ajandrology.com Male Fertility Open Access INVITED REVIEW Outcome of varicocele repair in men with nonobstructive
Reversible Conditions Organising More Information semen analysis Male Infertility at Melbourne IVF Fertility Preservation
 Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
Comparison of Intracytoplasmic Sperm Injection Outcomes between Oligozoospermic, Obstructive Azoospermic and Non-Obstructive Azoospermic Patients
 Original Article Comparison of Intracytoplasmic Sperm Injection Outcomes between Oligozoospermic, Obstructive Azoospermic and Non-Obstructive Azoospermic Patients Ensieh Shahrokh Tehraninejad, M.D. 1,
Original Article Comparison of Intracytoplasmic Sperm Injection Outcomes between Oligozoospermic, Obstructive Azoospermic and Non-Obstructive Azoospermic Patients Ensieh Shahrokh Tehraninejad, M.D. 1,
Rejuvenation of Gamete Cells; Past, Present and Future
 Rejuvenation of Gamete Cells; Past, Present and Future Denny Sakkas PhD Scientific Director, Boston IVF Waltham, MA, USA Conflict of Interest I have no conflict of interest related to this presentation.
Rejuvenation of Gamete Cells; Past, Present and Future Denny Sakkas PhD Scientific Director, Boston IVF Waltham, MA, USA Conflict of Interest I have no conflict of interest related to this presentation.
MALE INFERTILITY & SEMEN ANALYSIS
 MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
GUIDELINES ON MALE INFERTILITY
 European Association of Urology GUIDELINES ON MALE INFERTILITY G.R. Dohle, W. Weidner, A. Jungwirth, G. Colpi, G. Papp, J. Pomerol, T.B. Hargreave UPDATE MARCH 2004 TABLE OF CONTENTS PAGE 1 INTRODUCTION
European Association of Urology GUIDELINES ON MALE INFERTILITY G.R. Dohle, W. Weidner, A. Jungwirth, G. Colpi, G. Papp, J. Pomerol, T.B. Hargreave UPDATE MARCH 2004 TABLE OF CONTENTS PAGE 1 INTRODUCTION
ORIGINAL ARTICLE TESTICULAR VERSUS EPIDIDYMAL SPERMATOZOA IN INTRACYTOPLASMIC SPERM INJECTION TREATMENT CYCLES
 ORIGINAL ARTICLE TESTICULAR VERSUS EPIDIDYMAL SPERMATOZOA IN INTRACYTOPLASMIC SPERM INJECTION TREATMENT CYCLES Hameed N, Ozturk O* PAF Hospital, Munir Road, Lahore, Pakistan, *University College Hospital,
ORIGINAL ARTICLE TESTICULAR VERSUS EPIDIDYMAL SPERMATOZOA IN INTRACYTOPLASMIC SPERM INJECTION TREATMENT CYCLES Hameed N, Ozturk O* PAF Hospital, Munir Road, Lahore, Pakistan, *University College Hospital,
CONTROVERSIAL PROBLEMS INVOLVING MALE INFERTILITY
 CONTROVERSIAL PROBLEMS INVOLVING MALE INFERTILITY Sherman J. Silber, M.D. Infertility Center of St. Louis St. Luke s Hospital 224 South Woods Mill Road, Suite 730 St. Louis, MO 63017 Telephone: 314-576-1400
CONTROVERSIAL PROBLEMS INVOLVING MALE INFERTILITY Sherman J. Silber, M.D. Infertility Center of St. Louis St. Luke s Hospital 224 South Woods Mill Road, Suite 730 St. Louis, MO 63017 Telephone: 314-576-1400
