Probability of pregnancy after sterilization: a comparison of hysteroscopic versus laparoscopic sterilization,
|
|
|
- Brent Perkins
- 6 years ago
- Views:
Transcription
1 Contraception xx (2014) xxx xxx Original research article Probability of pregnancy after sterilization: a comparison of hysteroscopic versus laparoscopic sterilization, Aileen M. Gariepy a,, Mitchell D. Creinin b, Kenneth J. Smith c, Xiao Xu a a Department of Obstetrics, Gynecology, and Reproductive Sciences, Yale School of Medicine, New Haven, CT 06510, USA b Department of Obstetrics and Gynecology, University of California, Davis, Sacramento, CA 95817, USA c Department of Medicine, Division of General Internal Medicine, University of Pittsburgh School of Medicine, Pittsburgh, PA 15261, USA Received 9 October 2013; revised 11 March 2014; accepted 16 March 2014 Abstract Objective: To compare the expected probability of pregnancy after hysteroscopic versus laparoscopic sterilization based on available data using decision analysis. Study design: We developed an evidence-based Markov model to estimate the probability of pregnancy over 10 years after three different female sterilization procedures: hysteroscopic, laparoscopic silicone rubber band application and laparoscopic bipolar coagulation. Parameter estimates for procedure success, probability of completing follow-up testing and risk of pregnancy after different sterilization procedures were obtained from published sources. Results: In the base case analysis at all points in time after the sterilization procedure, the initial and cumulative risk of pregnancy after sterilization is higher in women opting for hysteroscopic than either laparoscopic band or bipolar sterilization. The expected pregnancy rates per 1000 women at 1 year are 57, 7 and 3 for hysteroscopic sterilization, laparoscopic silicone rubber band application and laparoscopic bipolar coagulation, respectively. At 10 years, the cumulative pregnancy rates per 1000 women are 96, 24 and 30, respectively. Sensitivity analyses suggest that the three procedures would have an equivalent pregnancy risk of approximately 80 per 1000 women at 10 years if the probability of successful laparoscopic (band or bipolar) sterilization drops below 90% and successful coil placement on first hysteroscopic attempt increases to 98% or if the probability of undergoing a hysterosalpingogram increases to 100%. Conclusion: Based on available data, the expected population risk of pregnancy is higher after hysteroscopic than laparoscopic sterilization. Consistent with existing contraceptive classification, future characterization of hysteroscopic sterilization should distinguish perfect and typical use failure rates. Implications: Pregnancy probability at 1 year and over 10 years is expected to be higher in women having hysteroscopic as compared to laparoscopic sterilization Elsevier Inc. All rights reserved. Keywords: Female sterilization; Hysteroscopic sterilization; Laparoscopic sterilization; Tubal ligation; Pregnancy after sterilization; Sterilization failure 1. Introduction Female surgical sterilization is the most popular method of pregnancy prevention worldwide and is the most commonly used method of contraception among women age 35 years and older in the United States (U.S.) [1,2]. Each year, 345,000 U.S. women undergo sterilization procedures Funding: A grant from the Society of Family Planning. Disclosure: The authors report no conflict of interest. Corresponding author. Tel.: ; fax: address: aileen.gariepy@yale.edu (A.M. Gariepy). and a total of 10.3 million U.S. women rely on female sterilization for pregnancy prevention [3,4]. Since the introduction of a hysteroscopic approach in 2001, an increasing number of women are undergoing hysteroscopic sterilization instead of laparoscopic sterilization [5 7]. Hysteroscopic sterilization has several advantages over laparoscopic sterilization: it avoids abdominal entry, can be performed as an office procedure and may avoid general anesthesia [5]. More than 650,000 hysteroscopic sterilization procedures have been performed worldwide [5]. One U.S. academic center reported that the proportion of interval sterilization performed laparoscopically from 2002 to 2006 decreased by 50% with a / 2014 Elsevier Inc. All rights reserved.
2 2 A.M. Gariepy et al. / Contraception xx (2014) xxx xxx corresponding increase in the proportion of procedures performed by hysteroscopic sterilization by 50% [6]. However, hysteroscopic sterilization has limitations as well. The likelihood of achieving successful bilateral coil placement on first attempt varies from 76% to 96% [8 22].In addition, unlike laparoscopic sterilization, hysteroscopic sterilization is not immediately effective; at least 3 months is required for tubal fibrosis and occlusion to occur for the procedure to be effective. During these 3 months, women need to use alternative contraception until they can undergo a post-procedure hysterosalpingogram (HSG) to confirm bilateral tubal blockage [23]. Prior research has shown that some (6 87%) women never return for their HSGs [8,10,12 14,16 19,24] and that blockage does not occur in 5 16% of HSG evaluations 3 months post-procedure [8,12 14,16 19]. The multiple steps involved in hysteroscopic sterilization, including the 3-month delay in possibly achieving sterilization, can increase the risk of patient non-compliance with this clinical care protocol and subject women to contraceptive failures (unintended pregnancies) during the process [23]. For any new method of contraception or sterilization, the most important variable to scrutinize is effectiveness. Unfortunately, the literature on hysteroscopic sterilization is limited by lack of such data [2,25 27]. Most studies of its efficacy have excluded women who failed initial microinsert placement did not return for HSG or who became pregnant before their HSG [23]. Furthermore, there are no prospective studies comparing the effectiveness of hysteroscopic and laparoscopic sterilizations. Most studies that do retrospectively report pregnancies after hysteroscopic sterilization are limited by small study numbers, short follow-up duration, lack of reporting follow-up duration and high loss to follow-up [27,28]. We sought to gain a more objective and comprehensive understanding of hysteroscopic sterilization outcomes, based on the published literature. In the absence of a prospective study directly comparing short- and long-term probability of pregnancy after hysteroscopic and laparoscopic sterilization procedures, the best way to understand the consequences of the two contraceptive approaches is through a decision analytic model. Decision analysis can account for the complexity of the multi-step process for coil placement and follow-up, can incorporate the variability in clinical outcomes reported in the literature and can compare the expected probability of pregnancy after hysteroscopic and laparoscopic sterilization. Also, by mapping out the clinical pathway of these procedures, it provides a unique opportunity to identify knowledge gaps in the current literature and help set priorities for future research. 2. Materials and methods 2.1. Study design We developed a Markov state-transition model (Fig. 1)to estimate the probability of pregnancy following three sterilization strategies: hysteroscopic, laparoscopic with silicone rubber band application (falope rings) and laparoscopic with bipolar coagulation. Laparoscopic sterilization was chosen as the comparator for the newer hysteroscopic sterilization procedure, since it is the standard of care for interval (not related to pregnancy) female sterilization [2]. Using yearly cycles, the Markov model mapped health states (major clinical events) and clinical pathways between those states following each strategy. These health states and pathways included successful or failed sterilization attempts, follow-up procedures and their outcomes and progression to alternative procedures if prior procedures were unsuccessful and their outcomes. Fig. 1 depicts this complex model that incorporates the probabilities of the health states and pathways (Table 1) to estimate the risk of pregnancy. We estimated the expected probability of pregnancy in hypothetical cohorts of women based on available data. Sterilization success was defined in accordance with standard clinical practice. A successful hysteroscopic sterilization was defined as having bilateral blockage of fallopian tubes on follow-up HSG. A successful laparoscopic sterilization was defined as physical fallopian tube obstruction at surgery. Procedure characteristics and follow-up testing probabilities were estimated from published sources (Table 1). Resultant sterilizations and pregnancies within each cohort were attributed to the initial procedure. Thus, women undergoing hysteroscopic sterilization who ultimately received laparoscopic sterilization were counted as hysteroscopic successes. Cohorts were followed in the model for 10 years. In the absence of published data, assumptions from a previous and similar model [25], where relevant, were carried over to this analysis. Data not obtainable from published literature were acquired from our practice s active database, initiated in July Standard decision analysis software (TreeAge Pro Suite 2012) was used Data sources for hysteroscopic sterilization For hysteroscopic sterilization, we used data on Essure hysteroscopic sterilization, as it is the only method available. Base case values and reported ranges of the relevant parameters (Table 1) came from a comprehensive literature search of all pertinent studies in English in PubMed and Ovid last searched September 20, 2013, and by reviewing the bibliographies of identified references. All published studies that reported more than 50 subjects were included. Base case values are weighted by study sample size averages from those studies. Data from studies not using HSG to evaluate hysteroscopic sterilization success as required by the U.S. Food and Drug Administration (FDA) were not included. Scant data are available regarding pregnancy risk after hysteroscopic sterilization [2,25 27]; the most recent available data are from the Essure package insert, updated between April and August From 2001 to 2010, 748 pregnancies following an Essure procedure were reported to the manufacturer, the FDA, or in published reports; the company also reported sales of 497,306 Essure kits during that time period [30]. To calculate the risk of pregnancy after a confirmatory HSG shows bilateral occlusion, we excluded
3 A.M. Gariepy et al. / Contraception xx (2014) xxx xxx 3 Fig. 1. Decision model for estimating the probability of pregnancy after female sterilization a. Schematic decision tree for the overall model. b. Illustrated details about the branch for hysteroscopic sterilization. HS: Hysteroscopic sterilization. LS: Laparoscopic sterilization. indicates that the branch continues as illustrated in the other figures. indicates Markov cycles with follow-up during the remainder of the first year and up to 9 more years thereafter. Each Markov cycle represents 1 year and reflects whether women became pregnant or not during that year. If pregnancy occurs, the model ends. Women who are not pregnant continue to cycle through clinical scenarios of the Markov cycles until they become pregnant or 10 years of cycles are completed.
4 4 A.M. Gariepy et al. / Contraception xx (2014) xxx xxx Table 1 Parameter values for model Probability of Baseline value (%) Range (%) Reference or assumption Laparoscopic sterilization Successful LS , 29 Choosing HS if LS failed Author consensus Hysteroscopic sterilization Successful coil placement on first attempt Returning for HSG at 3 months , 10, 12 14, 16 HSG: coils present at 3 months , HSG: blockage at 3 months , 12 14, Returning for HSG at 6 months Assume same as for 3 months HSG: blockage at 6 months , 14, Assumed sterile if do not return for HSG 91 (95% of 96%) Assume same as women returning at 3 and 6 months Additional sterilization attempts Choosing another procedure (HS or LS) after , 14, 16, 21 one failed HS attempt (unable to place coils) Choosing LS after one failed HS attempt , 14, 16, 21 Choosing LS after two failed HS attempts , Practice database Successful coil placement on second HS attempt , 9, 11, 16, 18, 21, 22 If HSG at 3 months shows no coils or HSG at 6 months shows non-occlusion Choosing another procedure 30 Practice database Choosing second HS 50 Practice database Occlusion with second HS , Practice database Pregnancy after hysteroscopic sterilization Among women using contraception (after HS and before HSG) During 3 months waiting period after HS , 32 Incremental pregnancy months During 6 months waiting period after HS , 32 Incremental pregnancy months During 9 months waiting period after HS Incremental pregnancy months Annually, years , 31, 32 Among women not using contraception (after HS and before HSG) During 3 months of no contraception Incremental pregnancy months 3 6 no contraception 22 During 6 months of no contraception Incremental pregnancy months 6 9 no contraception 21 During 9 months of no contraception Incremental pregnancy months 9 12 no contraception 21 Annually, years After HSG Annually if bilateral occlusion not confirmed , 31, 32 Annually if bilateral occlusion confirmed a Monthly risk after occlusion confirmed Calculation from above Pregnancy after laparoscopic sterilization b Pregnancy after silicone band application Year Year Year Year Year Year Year Year Year Year
5 A.M. Gariepy et al. / Contraception xx (2014) xxx xxx 5 Table 1 (continued) Probability of Baseline value (%) Range (%) Reference or assumption Pregnancy after bipolar coagulation Year Year Year Year Year Year Year Year Year Year Abbreviations: LS, laparoscopic sterilization; HS, hysteroscopic sterilization. a The manufacturer reports 748 pregnancies following an Essure procedure and sales of 497,306 HS kits during the same time period [30].Toestimatetherateof pregnancy after confirmatory HSG, we excluded the following pregnancies: (1) 32 luteal phase pregnancies that should not differ between laparoscopic and hysteroscopic sterilization, (2) 229 pregnancies due to patient non-compliance, (3) 95 pregnancies due to perforation, (4) 45 pregnancies due to unsatisfactory placement and (5) 35 pregnancies due to physician non-compliance. The latter four categories were excluded because they more likely occurred prior to HSG confirmation of tubal blockage. An additional 240 pregnancies were reported as insufficient information. We assumed half of these pregnancies occurred before HSG testing. This resulted in a total of 192 pregnancies (748 total pregnancies minus 556 pregnancies before HSG) occurring after HSG testing among 496,750 sterilizations over 10 years, i.e., 0.4 pregnancies per 1000 sterilizations over 10 years [or 0.004% annual pregnancy rate, which was calculated as 1 ( ) (1/10) ]. b To calculate the annual rate of pregnancy after LS, we used the cumulative pregnancy rate reported in CREST [33] to denote the point estimate of the cumulative pregnancy rate for year t as P(t), upper bound of the 95% confidence interval of the cumulative pregnancy rate in year t as P u (t) and the lower bound of the 95% confidence interval of the cumulative pregnancy rate in year t as P l (t). For year t after LS, we calculated the annual pregnancy rate as P(t) P(t 1), the upper bound of the annual pregnancy rate as P u (t) P l (t 1) and the lower bound of the annual pregnancy rate as P l (t) P u (t 1) (but restricted to 0). 32 luteal phase pregnancies, which should not differ between laparoscopic and hysteroscopic sterilization, and 524 pregnancies that occurred prior to HSG (e.g., patient noncompliance, perforation, unsatisfactory placement, physician non-compliance). This provided a conservative estimate of pregnancy risk after HSG of 192 per 496,750 over 10 years (0.4 per 1000 sterilizations) and an annual pregnancy rate of 0.004% after HSG testing (Table 1) Data sources for laparoscopic sterilization Data from the U.S. Collaborative Review of Sterilization (CREST), the largest prospective study (n= 12,138) of laparoscopic sterilization, were used for base case values and ranges of pregnancy risk after laparoscopic sterilization [33]. The study, which enrolled women during , included all procedures currently used in practice today except for the Filshie clip. Because of a lack of long-term Filshie clip followup data, this method was not included in the current model. We modeled pregnancy risk after laparoscopic sterilization using silicone rubber band application and bipolar coagulation Interventions and measures Sterilizations via hysteroscopy, laparoscopy with silicone rubber band application and laparoscopy with bipolar coagulation were tested in identical hypothetical cohorts. The model used estimated probabilities of women undergoing a second or third sterilization attempt after one failed attempt from the published literature (Table 1). Pregnancy following hysteroscopic sterilization may occur at four different time points: (1) during the 3- or 6-month waiting period when patients rely on alternative contraception before confirmatory HSG testing, (2) after HSG fails to confirm bilateral occlusion, (3) after HSG confirms bilateral occlusion and (4) after a failed hysteroscopic sterilization attempt when no further sterilization attempts occur. While the probability of hysteroscopic sterilization success was assumed to be identical whether or not women completed follow-up HSG testing, the risk of pregnancy differs. This is because women who did not have a follow-up HSG would not know if they were still at risk for pregnancy and may not be using additional necessary contraception, hence resulting in a higher risk of pregnancy (Table 1). Cohorts were followed for 10 years, consistent with the analysis of pregnancy risk in the CREST study [33]. Finally, to simulate real patient experiences, we also used published data on contraceptive use and pregnancies from Cycle 6 of the U.S. National Survey of Family Growth and calculated weighted average pregnancy risk over time among U.S. women using reversible contraception [31]. These calculations for contraceptive failure were used to determine pregnancy risk for women awaiting a confirmatory HSG and for women who stop pursuing sterilization and rely on routine contraception instead [32] (Table 1). We conducted both one-way and twoway sensitivity analyses to assess the impact on findings when varying the value of a single parameter (one-way sensitivity analysis) and the values of two parameters simultaneously (two-way sensitivity analysis) in the model. The plausible range for each parameter is listed in Table Results In the base case analysis at all points in time after the sterilization procedure (ranging from 1 year to 10 years after procedure initiation), the expected cumulative risk of
6 6 A.M. Gariepy et al. / Contraception xx (2014) xxx xxx pregnancy after sterilization is higher in women opting for hysteroscopic than laparoscopic sterilization using silicone band application or bipolar coagulation. Pregnancy risk after hysteroscopic sterilization is primarily accrued in the first year after initiating the process. The expected pregnancy rates per 1000 women at 1 year are 57, 7 and 3 for hysteroscopic sterilization, laparoscopic silicone rubber band application and laparoscopic bipolar coagulation, respectively. At 10 years, the cumulative pregnancy rates per 1000 women are 96, 24 and 30, respectively (Fig. 2). One-way sensitivity analyses suggest that pregnancy risk after hysteroscopic or laparoscopic sterilization is most influenced by the probability of the following events: pregnancy during 3 months of routine contraception use after successfully performed hysteroscopic sterilization, choosing a second procedure after one failed hysteroscopic sterilization attempt, returning for mandated HSG, the assumption of sterility among women who do not return for HSG, pregnancy after confirmed bilateral occlusion in hysteroscopic sterilization, probability of successful coil placement on first hysteroscopic sterilization attempt and successful laparoscopic sterilization procedure. Results from our two-way sensitivity analyses also informed us of which variables would need to change and by how much they would need to change to create equal effectiveness between hysteroscopic and laparoscopic sterilization. To reach equivalency, the probability of successful band or bipolar laparoscopic sterilization would need to decrease below 90% (base case, 99%) and one of three improvements in hysteroscopic outcomes would need to occur: (1) the probability of successful bilateral coil placement on first hysteroscopic sterilization attempt would need to increase to 98% (base case, 92%), (2) the probability of choosing a second procedure after one failed hysteroscopic sterilization would need to increase to 93% (base case, 63%) or (3) the probability of returning for the mandated HSG would need to increase to 100% (base case, 79%). Under these circumstances, the three procedures would have an equivalent pregnancy risk of approximately 80 per 1000 women at 10 years. Fig. 2. Cumulative pregnancy risk after sterilization for women of all ages. Hysteroscopic sterilization. Bipolar laparoscopic sterilization. Band laparoscopic sterilization 4. Discussion Based on best data currently available, our model suggests that hysteroscopic sterilization is not as effective as laparoscopic sterilization in preventing pregnancy when the complete clinical pathways of the procedures are considered. Our analysis improves upon prior studies of hysteroscopic sterilization by taking into account uncertainties in successful placement of coils, return for HSG and successful blockage of tubes. Reflecting these real-life circumstances, our base case estimates showed that a woman undergoing hysteroscopic sterilization is expected to have a pregnancy risk of 96 per 1000 women after 10 years, compared to 24 and 30 per 1000 women for laparoscopic sterilization with silicone rubber band and bipolar cautery, respectively. This analysis expands upon our previous study that compared the likelihood of successful bilateral tubal occlusion after hysteroscopic versus laparoscopic sterilization procedures [25]. By estimating the risk of pregnancy after both sterilization procedures over a 10-year period, our current study provides important new data on expected long-term outcomes. This information is essential for patients and clinicians. Our findings have important implications for future development of hysteroscopic sterilization products. The higher pregnancy rate over 10 years with hysteroscopic compared to laparoscopic sterilization is primarily driven by first-year failures because the subsequent failure per year is similar between hysteroscopic and laparoscopic methods. Future efforts to improve hysteroscopic sterilization need to focus on its higher first-year failure risk, which is primarily influenced by the rate of successful placement of both coils on first attempt, lack of immediate effectiveness and need for follow-up evaluations. Even if certain steps of the hysteroscopic sterilization procedure are optimized (e.g., 98% bilateral coil placement), laparoscopic sterilization remains superior unless the probability of successfully performing a laparoscopic sterilization procedure also drops below 90%, which is not clinically probable. Thus, the expected higher failure rate of hysteroscopic sterilization needs to be considered and communicated to patients, in conjunction with its benefits when counseling patients about female sterilization options. Unintended pregnancy resulting from sterilization failure can have serious consequences for both women s quality of life and maternal and neonatal health outcomes and should be considered a significant adverse event. We recognize that although we have used the best evidence available, our analysis is limited by the quality of the data used in the model. There are no prospective studies on pregnancy risk after hysteroscopic sterilization [2,25 27], let alone studies directly comparing the effectiveness of hysteroscopic and laparoscopic sterilizations [2,25 27]. Of the retrospective studies of pregnancy after hysteroscopic sterilization, most are limited by small study numbers, short follow-up duration, lack of reporting follow-up duration, high loss to follow-up, reliance on X-ray instead of HSG for
7 A.M. Gariepy et al. / Contraception xx (2014) xxx xxx 7 confirmation, passive reporting of pregnancy or estimates of the number of procedures performed [25 27,30,34]. For example, one large retrospective study of 4306 women from Spain reported 7 (0.16%) pregnancies over 7 years, but only 20% of the original cohort had follow-up for 7 years, and abdominal X-ray was used primarily instead of HSG [28]. Hence we estimated the pregnancy rate after hysteroscopic sterilization based on passive (not mandatory) pregnancy reporting data to FDA and the manufacturer and the manufacturer s estimates of the number of Essure kits sold (rather than the number of devices actually implanted). The inability to account for unused kits, failed procedures or multiple attempts could have resulted in an underestimated pregnancy rate for hysteroscopic sterilization [30]. Similarly, the CREST data, which provided the pregnancy rates after laparoscopic sterilization for our analysis, have limitations too. The CREST was a longitudinal prospective study of laparoscopic sterilization procedures performed years ago, early in the learning curve of laparoscopic surgery [2,35]. Consequently, our estimated pregnancy outcome may be biased in favor of hysteroscopic sterilization. Nevertheless, our analysis is a useful first step to understand the full impact of hysteroscopic sterilization on pregnancy risk, based on currently available data. The finding that laparoscopic is superior to hysteroscopic sterilization occurred despite a bias in favor of hysteroscopic sterilization in the analysis. That is, the study assessed outcome by initial method of sterilization attempted, including 6% of women starting with hysteroscopic sterilization that are ultimately sterilized laparoscopically [25]. Thus, women undergoing hysteroscopic sterilization who ultimately received laparoscopic sterilization, which had a higher success rate, were counted as hysteroscopic successes. Future research from a prospective cohort of women undergoing hysteroscopic and laparoscopic sterilization procedures with high long-term follow-up rates would enhance our understanding of hysteroscopic sterilization effectiveness. Contraceptive methods are ranked by effectiveness and characterized by perfect and typical use failure rates. Methods requiring multiple steps (i.e., frequent compliance) like combined hormonal contraceptive pills have higher typical use failure rates than the corresponding perfect use failure rates and are significantly less effective than one-step methods such as intrauterine devices and contraceptive implants [32,33]. This difference in perfect and typical use failure rates is also important to consider when assessing the effectiveness of multi-step hysteroscopic sterilization. However, most rankings do not differentiate hysteroscopic from laparoscopic sterilization and do not ascribe different failure rates for perfect and typical sterilization use. Our findings suggest that it is time to rethink this characterization. Acknowledgment The authors thank Lisbet Lundsberg, PhD, for her assistance with the literature review. References [1] EngenderHealth. Contraceptive sterilization: global issues and trends. New York, NY: EngenderHealth; 2002, pp [2] Peterson HB. Sterilization. Obstet Gynecol 2008;111: [3] Jones J, Mosher W, Daniels K. Current contraceptive use in the United States, , and changes in patterns of use since Natl Health Stat Rep 2012;60:1 5. [4] Mosher WD, Jones J. Use of contraception in the United States: Vital Health Stat :1 4. [5] Conceptus. Essure permanent birth control. Available at:, essuremd.com/about-essure Retrieved March 25, [6] Shavell VI, Abdallah ME, Shade Jr GH, Diamond MP, Berman JM. Trends in sterilization since the introduction of Essure hysteroscopic sterilization. J Minim Invasive Gynecol 2009;16:22 7. [7] Connor VF. Essure: a review six years later. J Minim Invasive Gynecol 2009;16(3): [8] Duffy S, Marsh F, Rogerson L, Hudson H, Cooper K, Jack S, et al. Female sterilisation: a cohort controlled comparative study of ESSURE versus laparoscopic sterilisation. BJOG 2005;112: [9] Ubeda A, Labastida R, Dexeus S. Essure: a new device for hysteroscopic tubal sterilization in an outpatient setting. Fertil Steril 2004;82: [10] Shavell VI, Abdallah ME, Diamond MP, Kmak DC, Berman JM. Post- Essure hysterosalpingography compliance in a clinic population. J Minim Invasive Gynecol 2008;15: [11] Shavell VI, Abdallah ME, Diamond MP, Berman JM. Placement of a permanent birth control device at a university medical center. J Reprod Med 2009;54: [12] Savage UK, Masters SJ, Smid MC, Hung YY, Jacobson GF. Hysteroscopic sterilization in a large group practice: experience and effectiveness. Obstet Gynecol 2009;114: [13] Levie M, Chudnoff SG. Prospective analysis of office-based hysteroscopic sterilization. J Minim Invasive Gynecol 2006;13: [14] Sinha D, Kalathy V, Gupta JK, Clark TJ. The feasibility, success and patient satisfaction associated with outpatient hysteroscopic sterilisation. BJOG 2007;114: [15] Levie M, Chudnoff SG. A comparison of novice and experienced physicians performing hysteroscopic sterilization: an analysis of an FDA-mandated trial. Fertil Steril 2011;96:643e1 8e1. [16] Chen BA, Hayes JL, Reeves MF, Creinin MD. Outcomes of transcervical hysteroscopic sterilization in an urban academic medical center. Contraception 2009;80:205. [17] Kerin JF, Carignan CS, Cher D. The safety and effectiveness of a new hysteroscopic method for permanent birth control: results of the first Essure pbc clinical study. Aust N Z J Obstet Gynaecol 2001; 41: [18] Kerin JF, Cooper JM, Price T, Herendael BJ, Cayuela-Font E, Cher D, et al. Hysteroscopic sterilization using a micro-insert device: results of a multicentre Phase II study. Hum Reprod 2003;18: [19] Cooper JM, Carignan CS, Cher D, Kerin JF, Selective Tubal Occlusion Procedure 2000 Investigators Group. Microinsert nonincisional hysteroscopic sterilization. Obstet Gynecol 2003;102: [20] Nichols M, Carter JF, Fylstra DL, Childers M, Essure System U.S. Post-Approval Study Group. A comparative study of hysteroscopic sterilization performed in-office versus a hospital operating room. J Minim Invasive Gynecol 2006;13: [21] Andersson S, Eriksson S, Mints M. Hysteroscopic female sterilization with Essure in an outpatient setting. Acta Obstet Gynecol Scand 2009; 88: [22] Miño M, Arjona JE, Cordón J, Pelegrin B, Povedano B, Chacon E. Success rate and patient satisfaction with the Essure sterilisation in an outpatient setting: a prospective study of 857 women. BJOG 2007;114 (6): [23] ACOG Committee on Gynecologic Practice. ACOG Committee Opinion No. 458: hysterosalpingography after tubal sterilization. Obstet Gynecol 2010;115:
8 8 A.M. Gariepy et al. / Contraception xx (2014) xxx xxx [24] Thiel JA, Carson GD. Cost-effectiveness analysis comparing the essure tubal sterilization procedure and laparoscopic tubal sterilization. J Obstet Gynaecol Can 2008;30: [25] Gariepy AM, Creinin MD, Schwarz EB, Smith KJ. Reliability of laparoscopic compared with hysteroscopic sterilization at 1 year: a decision analysis. Obstet Gynecol 2011;118: [26] Hurskainen R, Hovi SL, Gissler M, Grahn R, Kukkonen-Harjula K, Nord-Saari M, et al. Hysteroscopic tubal sterilization: a systematic review of the Essure system. Fertil Steril 2010;94:16 9. [27] Cleary TP, Tepper NK, Cwiak C, Whiteman MK, Jamieson DJ, Marchbanks PA, et al. Pregnancies after hysteroscopic sterilization: a systematic review. Contraception 2013;87(5): [28] Povedano B, Arjona JE, Velasco E, Monserrat JA, Lorente J, Castelo- Branco C. Complications of hysteroscopic Essure( ) sterilisation: report on 4306 procedures performed in a single centre. BJOG 2012; 119(7): [29] Destefano F, Greenspan JR, Dicker RC, Peterson HB, Strauss LT, Rubin GL. Complications of interval laparoscopic tubal sterilization. Obstet Gynecol 1983;61: [30] Conceptus. Essure permanent birth control. Available at:, Retrieved March 25, [31] Kost K, Singh S, Vaughan B, Trussell J, Bankole A. Estimates of contraceptive failure from the 2002 National Survey of Family Growth. Contraception 2008;77: [32] Trussell J. Contraceptive failure in the United States. Contraception 2011;83: [33] Peterson HB, Xia Z, Hughes JM, Wilcox LS, Tylor LR, Trussell J. The risk of pregnancy after tubal sterilization: findings from the U.S. Collaborative Review of Sterilization. Am J Obstet Gynecol 1996; 174: [34] Levy B, Levie MD, Childers ME. A summary of reported pregnancies after hysteroscopic sterilization. J Minim Invasive Gynecol 2007;14: [35] Peterson HB, Xia Z, Wilcox LS, Tylor LR, Trussell J. Pregnancy after tubal sterilization with bipolar electrocoagulation. U.S. Collaborative Review of Sterilization Working Group. Obstet Gynecol 1999;94:
Aileen M. CON-08309; No of Pages 8. Contraception xx (2014) xxx xxx
 CON-08309; No of Pages 8 1 Original research article 2 Probability of pregnancy after sterilization: a comparison of hysteroscopic 3 versus laparoscopic sterilization, 4Q1 Aileen M. 5 6 7 Contraception
CON-08309; No of Pages 8 1 Original research article 2 Probability of pregnancy after sterilization: a comparison of hysteroscopic 3 versus laparoscopic sterilization, 4Q1 Aileen M. 5 6 7 Contraception
Complications of hysteroscopic Essure â sterilisation: report on 4306 procedures performed in a single centre
 DOI: 10.1111/j.1471-0528.2012.03292.x www.bjog.org Fertility control Complications of hysteroscopic Essure â sterilisation: report on 4306 procedures performed in a single centre B Povedano, a JE Arjona,
DOI: 10.1111/j.1471-0528.2012.03292.x www.bjog.org Fertility control Complications of hysteroscopic Essure â sterilisation: report on 4306 procedures performed in a single centre B Povedano, a JE Arjona,
Female sterilisation: a cohort controlled comparative study of ESSURE versus laparoscopic sterilisation
 BJOG: an International Journal of Obstetrics and Gynaecology November 2005, Vol. 112, pp. 1522 1528 DOI: 10.1111/j.1471-0528.2005.00726.x Female sterilisation: a cohort controlled comparative study of
BJOG: an International Journal of Obstetrics and Gynaecology November 2005, Vol. 112, pp. 1522 1528 DOI: 10.1111/j.1471-0528.2005.00726.x Female sterilisation: a cohort controlled comparative study of
Permanent Sterilization: When you are really sure!
 Permanent Sterilization: When you are really sure! Tony Ogburn MD Department of Ob/Gyn 2006-8 National Survey of Family Growth 6.1% of women had a sterilized male partner The History of Female Sterilization
Permanent Sterilization: When you are really sure! Tony Ogburn MD Department of Ob/Gyn 2006-8 National Survey of Family Growth 6.1% of women had a sterilized male partner The History of Female Sterilization
Satisfaction and tolerance with office hysteroscopic tubal sterilization
 TECHNIQUES AND INSTRUMENTATION Satisfaction and tolerance with office hysteroscopic tubal sterilization Jose E. Arjona, M.D., Ph.D., a Monica Mi~no, M.D., Ph.D., a Javier Cordon, M.D., Ph.D., a Balbino
TECHNIQUES AND INSTRUMENTATION Satisfaction and tolerance with office hysteroscopic tubal sterilization Jose E. Arjona, M.D., Ph.D., a Monica Mi~no, M.D., Ph.D., a Javier Cordon, M.D., Ph.D., a Balbino
MEDICAL POLICY SUBJECT: FEMALE STERILIZATION. POLICY NUMBER: CATEGORY: Contract Clarification
 MEDICAL POLICY SUBJECT: FEMALE STERILIZATION PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: FEMALE STERILIZATION PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
National Institute for Health and Clinical Excellence
 National Institute for Health and Clinical Excellence 218_2 Hysteroscopic sterilisation by tubal cannulation and placement of intrafallopian implants Consultation Comments table IPAC date: Thursday 16
National Institute for Health and Clinical Excellence 218_2 Hysteroscopic sterilisation by tubal cannulation and placement of intrafallopian implants Consultation Comments table IPAC date: Thursday 16
Unintended pregnancies after Essure sterilization in the Netherlands
 Unintended pregnancies after Essure sterilization in the Netherlands S. Veersema M.P.H. Vleugels L.M. Moolenaar C.A.H. Janssen H.A.M. Brölmann Fertil Steril. 2010;93:35-8. 13 Hysteroscopic Sterilization
Unintended pregnancies after Essure sterilization in the Netherlands S. Veersema M.P.H. Vleugels L.M. Moolenaar C.A.H. Janssen H.A.M. Brölmann Fertil Steril. 2010;93:35-8. 13 Hysteroscopic Sterilization
Clinical Experience With Contrast Infusion Sonography as an Essure Confirmation Test
 ORIGINAL RESEARCH Clinical Experience With Contrast Infusion Sonography as an Essure Confirmation Test Viviane F. Connor, MD Received November 3, 2010, from the Department of Gynecology, Section of Minimally
ORIGINAL RESEARCH Clinical Experience With Contrast Infusion Sonography as an Essure Confirmation Test Viviane F. Connor, MD Received November 3, 2010, from the Department of Gynecology, Section of Minimally
Permanent contraception for women
 For reprint orders, please contact: reprints@futuremedicine.com Permanent methods of contraception are used by an estimated 220 million couples worldwide, and are often selected due to convenience, ease
For reprint orders, please contact: reprints@futuremedicine.com Permanent methods of contraception are used by an estimated 220 million couples worldwide, and are often selected due to convenience, ease
Hysteroscopic Tubal Occlusion for Contraception
 Hysteroscopic Tubal Occlusion for Contraception (Essure and Adiana Systems) Policy Number: 2014M0056A Effective Date: June 1, 2014 Table of Contents: Page: Cross Reference Policy: POLICY DESCRIPTION 2
Hysteroscopic Tubal Occlusion for Contraception (Essure and Adiana Systems) Policy Number: 2014M0056A Effective Date: June 1, 2014 Table of Contents: Page: Cross Reference Policy: POLICY DESCRIPTION 2
Transcervical Sterilization
 Q UESTIONS & ANSWERS A BOUT Transcervical Sterilization A New Choice in Permanent Birth Control Choosing a Birth Control Method Women and their partners now have more birth control choices than ever. How
Q UESTIONS & ANSWERS A BOUT Transcervical Sterilization A New Choice in Permanent Birth Control Choosing a Birth Control Method Women and their partners now have more birth control choices than ever. How
Hysteroscopic Essure Inserts for Permanent Contraception Extended Follow-up Results of a Phase III, Multicenter, International Study
 Accepted Manuscript Hysteroscopic Essure Inserts for Permanent Contraception Extended Follow-up Results of a Phase III, Multicenter, International Study Scott G. Chudnoff, MD, MS, John E. Nichols, Jr.,
Accepted Manuscript Hysteroscopic Essure Inserts for Permanent Contraception Extended Follow-up Results of a Phase III, Multicenter, International Study Scott G. Chudnoff, MD, MS, John E. Nichols, Jr.,
CLINICAL GUIDELINES ID TAG Female Sterilisation (tubal occlusion) at Caesarean Section- Guideline for counselling and consent
 Title: Author: Designation: Speciality / Division: Directorate: CLINICAL GUIDELINES ID TAG Female Sterilisation (tubal occlusion) at Caesarean Section- Guideline for counselling and consent Dr Meeta Kamath
Title: Author: Designation: Speciality / Division: Directorate: CLINICAL GUIDELINES ID TAG Female Sterilisation (tubal occlusion) at Caesarean Section- Guideline for counselling and consent Dr Meeta Kamath
Labeling for Permanent Hysteroscopically-Placed Tubal Implants Intended for Sterilization
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 Labeling for Permanent Hysteroscopically-Placed Tubal Implants Intended for Sterilization Draft Guidance for Industry and Food and Drug
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 Labeling for Permanent Hysteroscopically-Placed Tubal Implants Intended for Sterilization Draft Guidance for Industry and Food and Drug
Female sterilization by the natural pathways
 info-canada@conceptus.com www.essure.com Female sterilization by the natural pathways magazine 1.Hatcher R et al. Contraceptive Technology, 17 th Edition. New York : Ardent Media, 1998. 2. Bhiwandiwala
info-canada@conceptus.com www.essure.com Female sterilization by the natural pathways magazine 1.Hatcher R et al. Contraceptive Technology, 17 th Edition. New York : Ardent Media, 1998. 2. Bhiwandiwala
Hysteroscopic Tubal Sterilization: An Evidence-Based Analysis
 Hysteroscopic Tubal Sterilization: An Evidence-Based Analysis K McMartin October 2013 Ontario Health Technology Assessment Series; Vol.13: No. 21, pp. 1 35, October 2013 Suggested Citation This report
Hysteroscopic Tubal Sterilization: An Evidence-Based Analysis K McMartin October 2013 Ontario Health Technology Assessment Series; Vol.13: No. 21, pp. 1 35, October 2013 Suggested Citation This report
Case Report Essure Surgical Removal and Subsequent Resolution of Chronic Pelvic Pain: A Case Report and Review of the Literature
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 6961202, 5 pages http://dx.doi.org/10.1155/2016/6961202 Case Report Essure Surgical Removal and Subsequent Resolution of Chronic Pelvic
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 6961202, 5 pages http://dx.doi.org/10.1155/2016/6961202 Case Report Essure Surgical Removal and Subsequent Resolution of Chronic Pelvic
Clinical Policy: Essure Removal Reference Number: CP.MP.131
 Clinical Policy: Reference Number: CP.MP.131 Effective Date: 11/16 Last Review Date: 11/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.131 Effective Date: 11/16 Last Review Date: 11/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Essure By Mayo Clinic staff
 Page 1 of 5 Reprints A single copy of this article may be reprinted for personal, noncommercial use only. Essure By Mayo Clinic staff Original Article: http://www.mayoclinic.com/health/essure/my00999 Definition
Page 1 of 5 Reprints A single copy of this article may be reprinted for personal, noncommercial use only. Essure By Mayo Clinic staff Original Article: http://www.mayoclinic.com/health/essure/my00999 Definition
Female Sterilization. Kavita Nanda, MD, MHS FHI 360 Expanding Contraceptive Choice December 6, 2018
 Female Sterilization Kavita Nanda, MD, MHS FHI 360 Expanding Contraceptive Choice December 6, 2018 What is female sterilization? Family planning method that provides permanent contraception to women and
Female Sterilization Kavita Nanda, MD, MHS FHI 360 Expanding Contraceptive Choice December 6, 2018 What is female sterilization? Family planning method that provides permanent contraception to women and
ESSURE A RESOURCE FOR CODING
 ESSURE REIMBURSEMENT GUIDE A RESOURCE FOR CODING INDICATION Essure is indicated for women who desire permanent birth control (female sterilization) by bilateral occlusion of fallopian tubes. IMPORTANT
ESSURE REIMBURSEMENT GUIDE A RESOURCE FOR CODING INDICATION Essure is indicated for women who desire permanent birth control (female sterilization) by bilateral occlusion of fallopian tubes. IMPORTANT
Consider what is best for you...
 Consider what is best for you... PERMANENT CONTRACEPTION A HIGHLY EFFECTIVE AND COMPLICATION FREE BIRTH CONTROL DEVICE Effective. Safe. Proven. FILSHIE - THE CLIP, EASY TO CORRECTLY APPLY Quick laparoscopic
Consider what is best for you... PERMANENT CONTRACEPTION A HIGHLY EFFECTIVE AND COMPLICATION FREE BIRTH CONTROL DEVICE Effective. Safe. Proven. FILSHIE - THE CLIP, EASY TO CORRECTLY APPLY Quick laparoscopic
Sterilisation for women at the RD&E: what you need to know Reference Number: CW
 Sterilisation for women at the RD&E: what you need to know Royal Devon and Exeter NHS Foundation Trust Patient Information Sterilisation for Women at The Royal Devon and Exeter Hospital What you need to
Sterilisation for women at the RD&E: what you need to know Royal Devon and Exeter NHS Foundation Trust Patient Information Sterilisation for Women at The Royal Devon and Exeter Hospital What you need to
Microinsert Nonincisional Hysteroscopic Sterilization
 Microinsert Nonincisional Hysteroscopic Sterilization Jay M. Cooper, MD, Charles S. Carignan, MD, Daniel Cher, MD, and John F. Kerin, MD, for the Selective Tubal Occlusion Procedure 2000 Investigators
Microinsert Nonincisional Hysteroscopic Sterilization Jay M. Cooper, MD, Charles S. Carignan, MD, Daniel Cher, MD, and John F. Kerin, MD, for the Selective Tubal Occlusion Procedure 2000 Investigators
Instruction for the patient
 Instruction for the patient Your situation You are a 38-year-old, woman who is pregnant with her third child You and your partner agree that with this child your family is complete In the past, you used
Instruction for the patient Your situation You are a 38-year-old, woman who is pregnant with her third child You and your partner agree that with this child your family is complete In the past, you used
Update on the Essure System for Permanent Birth Control
 Update on the Essure System for Permanent Birth Control Heidi Collins Fantasia IIn 2002, the U.S. Food and Drug Administration (FDA) approved Essure (Bayer, Whippany, NJ), a minimally invasive procedure
Update on the Essure System for Permanent Birth Control Heidi Collins Fantasia IIn 2002, the U.S. Food and Drug Administration (FDA) approved Essure (Bayer, Whippany, NJ), a minimally invasive procedure
Disclosures. Contraceptive Method Use, U.S. Best Practices in Contraception: Advances, Tips, and Tricks
 Best Practices in Contraception: Advances, Tips, and Tricks Disclosures I have no disclosures I may discuss off-label use of some contraceptives Biftu Mengesha MD MAS Department of Obstetrics, Gynecology
Best Practices in Contraception: Advances, Tips, and Tricks Disclosures I have no disclosures I may discuss off-label use of some contraceptives Biftu Mengesha MD MAS Department of Obstetrics, Gynecology
Myometrial Insertion of Essure Mirco-Insert
 Case Report http://www.alliedacademies.org/research-and-reports-in-gynecology-and-obstetrics Myometrial Insertion of Essure Mirco-Insert Jeffrey J Woo 1*, Barbara E Simpson 1, Dale W Stovall 2 1 Department
Case Report http://www.alliedacademies.org/research-and-reports-in-gynecology-and-obstetrics Myometrial Insertion of Essure Mirco-Insert Jeffrey J Woo 1*, Barbara E Simpson 1, Dale W Stovall 2 1 Department
Women spend about 5 years of their
 CONTRACEPTION Why we have not yet reduced the unintended pregnancy rate Melody Y. Hou, MD, MPH Dr. Hou is Assistant Professor of Obstetrics and Gynecology at the University of California, Davis, in Sacramento.
CONTRACEPTION Why we have not yet reduced the unintended pregnancy rate Melody Y. Hou, MD, MPH Dr. Hou is Assistant Professor of Obstetrics and Gynecology at the University of California, Davis, in Sacramento.
Family Planning Eligibility Program
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Family Planning Eligibility Program L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 5 3 P U B L I S H E D : N O V E M B E R 2
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Family Planning Eligibility Program L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 5 3 P U B L I S H E D : N O V E M B E R 2
Essure Permanent Birth Control Device: Radiological followup results at our center
 Essure Permanent Birth Control Device: Radiological followup results at our center Poster No.: C-0212 Congress: ECR 2013 Type: Scientific Exhibit Authors: R. Díaz Aguilera, A. M. Higuera Higuera, V. Palomo
Essure Permanent Birth Control Device: Radiological followup results at our center Poster No.: C-0212 Congress: ECR 2013 Type: Scientific Exhibit Authors: R. Díaz Aguilera, A. M. Higuera Higuera, V. Palomo
SIMPLE PERMANENT CONTRACEPTION A HIGHLY EFFECTIVE AND COMPLICATION FREE BIRTH CONTROL DEVICE
 CONSIDER WHAT IS BEST FOR YOU... SIMPLE PERMANENT CONTRACEPTION A HIGHLY EFFECTIVE AND COMPLICATION FREE BIRTH CONTROL DEVICE Effective. Safe. Proven. FILSHIE - THE CLIP, A HIGHLY EFFECTIVE CHOICE FOR
CONSIDER WHAT IS BEST FOR YOU... SIMPLE PERMANENT CONTRACEPTION A HIGHLY EFFECTIVE AND COMPLICATION FREE BIRTH CONTROL DEVICE Effective. Safe. Proven. FILSHIE - THE CLIP, A HIGHLY EFFECTIVE CHOICE FOR
CLINICAL ASSISTED REPRODUCTION
 CLINICAL ASSISTED REPRODUCTION IVF Births and Pregnancies: An Exploration of Two Methods of Assessment Using Life-Table Analysis R. DEONANDAN, 1,4 M. K. CAMPBELL, 1 T. OSTBYE, 2 I. TUMMON, 3 and J. ROBERTSON
CLINICAL ASSISTED REPRODUCTION IVF Births and Pregnancies: An Exploration of Two Methods of Assessment Using Life-Table Analysis R. DEONANDAN, 1,4 M. K. CAMPBELL, 1 T. OSTBYE, 2 I. TUMMON, 3 and J. ROBERTSON
V. Mijatovic S. Veersema M.H. Emanuel R. Schats P.G. Hompes. Fertil Steril. 2010;93:
 Essure hysteroscopic tubal occlusion device for the treatment of hydrosalpinx prior to in vitro fertilization-embryo transfer in patients with a contraindication for laparoscopy. V. Mijatovic S. Veersema
Essure hysteroscopic tubal occlusion device for the treatment of hydrosalpinx prior to in vitro fertilization-embryo transfer in patients with a contraindication for laparoscopy. V. Mijatovic S. Veersema
Commissioning Policy Individual Funding Request
 Commissioning Policy Individual Funding Request Female Sterilisation Prior Approval Policy Date Adopted: 6 th February 2017 Version: 1617.1 Individual Funding Request Team - A partnership between Bristol,
Commissioning Policy Individual Funding Request Female Sterilisation Prior Approval Policy Date Adopted: 6 th February 2017 Version: 1617.1 Individual Funding Request Team - A partnership between Bristol,
Robot-Assisted Gynecologic Surgery. Gynecologic Surgery
 Robot-Assisted Gynecologic Surgery Alison F. Jacoby, MD Department of Obstetrics, Gynecology and Reproductive Sciences University of California, San Francisco Robot-Assisted Gynecologic Surgery Clinical
Robot-Assisted Gynecologic Surgery Alison F. Jacoby, MD Department of Obstetrics, Gynecology and Reproductive Sciences University of California, San Francisco Robot-Assisted Gynecologic Surgery Clinical
Regret following female sterilization at a young age: a systematic review B
 Contraception 73 (2006) 205 210 Review article Regret following female at a young age: a systematic review B Kathryn M. Curtis a, T, Anshu P. Mohllajee a, Herbert B. Peterson b,c a WHO Collaborating Center
Contraception 73 (2006) 205 210 Review article Regret following female at a young age: a systematic review B Kathryn M. Curtis a, T, Anshu P. Mohllajee a, Herbert B. Peterson b,c a WHO Collaborating Center
The Pennsylvania State University. The Graduate School. Department of Public Health Sciences
 The Pennsylvania State University The Graduate School Department of Public Health Sciences THE IMPACT OF THE AFFORDABLE CARE ACT ON CONTRACEPTIVE USE AND COSTS AMONG PRIVATELY INSURED WOMEN A Thesis in
The Pennsylvania State University The Graduate School Department of Public Health Sciences THE IMPACT OF THE AFFORDABLE CARE ACT ON CONTRACEPTIVE USE AND COSTS AMONG PRIVATELY INSURED WOMEN A Thesis in
One-step transvaginal three-dimensional hysterosalpingofoam sonography (3D-HyFoSy) confirmation test for Essure follow-up: a multicenter study
 Ultrasound Obstet Gynecol 2018; 51: 134 141 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.17398 One-step transvaginal three-dimensional hysterosalpingofoam sonography
Ultrasound Obstet Gynecol 2018; 51: 134 141 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.17398 One-step transvaginal three-dimensional hysterosalpingofoam sonography
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of sterilisation by insertion of intrafallopian implants Sterilisation is sometimes
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of sterilisation by insertion of intrafallopian implants Sterilisation is sometimes
BRIEF REPORTS. Providing Long-Acting Reversible Contraception in an Academic Family Medicine Center Jennifer Amico, MD, MPH; Justine Wu, MD, MPH
 Providing Long-Acting Reversible Contraception in an Academic Family Medicine Center Jennifer Amico, MD, MPH; Justine Wu, MD, MPH BACKGROUND AND OBJECTIVES: Providing long-acting reversible contraception
Providing Long-Acting Reversible Contraception in an Academic Family Medicine Center Jennifer Amico, MD, MPH; Justine Wu, MD, MPH BACKGROUND AND OBJECTIVES: Providing long-acting reversible contraception
MENSTRUAL PATTERNS AND WOMEN'S ATTITUDES FOLLOWING STERILIZATION BY FA LOPE RINGS*
 FERTILITY AND STERILITY Copyright 1979 The American Fertility Society Vol. 31, No.6, June 1979 Printed in U.s.A. MENSTRUAL PATTERNS AND WOMEN'S ATTITUDES FOLLOWING STERILIZATION BY FA LOPE RINGS* LIDIA
FERTILITY AND STERILITY Copyright 1979 The American Fertility Society Vol. 31, No.6, June 1979 Printed in U.s.A. MENSTRUAL PATTERNS AND WOMEN'S ATTITUDES FOLLOWING STERILIZATION BY FA LOPE RINGS* LIDIA
Lindsey Tingen, MD Department of Obstetrics and Gynecology, Greenville Health System Greenville, SC
 Postpartum IUD Insertion: Continued Usage at Six Months Based on Expulsion and Removal Rates at Greenville Memorial Hospital in the First Year After Adoption of the Practice Lindsey Tingen, MD Department
Postpartum IUD Insertion: Continued Usage at Six Months Based on Expulsion and Removal Rates at Greenville Memorial Hospital in the First Year After Adoption of the Practice Lindsey Tingen, MD Department
ACCESS LARC INCREASING ACCESS TO IMMEDIATE POSTPARTUM LONG-ACTING REVERSIBLE CONTRACEPTION
 ACCESS LARC INCREASING ACCESS TO IMMEDIATE POSTPARTUM LONG-ACTING REVERSIBLE CONTRACEPTION Chapter Four: Policies and Procedures Overview This procedure outline is a pre-cursor to detailed procedures related
ACCESS LARC INCREASING ACCESS TO IMMEDIATE POSTPARTUM LONG-ACTING REVERSIBLE CONTRACEPTION Chapter Four: Policies and Procedures Overview This procedure outline is a pre-cursor to detailed procedures related
Clinics in diagnostic imaging (110)
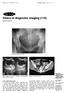 M e d i c a l E d u c a t i o n Singapore Med Med J 2006; J 2006; 47(7) 47(7) : 642 : 1 Clinics in diagnostic imaging (110) Lim S Y, Lam S L Fig. 1 Radiograph of the pelvis. Fig. 2 Sagittal and coronal
M e d i c a l E d u c a t i o n Singapore Med Med J 2006; J 2006; 47(7) 47(7) : 642 : 1 Clinics in diagnostic imaging (110) Lim S Y, Lam S L Fig. 1 Radiograph of the pelvis. Fig. 2 Sagittal and coronal
Chapter 1. Chapter 2. Chapter 3
 Summary To perform IUI some conditions are required. This includes 1) a certain amount of progressively motile spermatozoa, 2) the presence of ovulation, 3) the presence of functional fallopian tubes,
Summary To perform IUI some conditions are required. This includes 1) a certain amount of progressively motile spermatozoa, 2) the presence of ovulation, 3) the presence of functional fallopian tubes,
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics THE ROLE OF POST- ABORTION CONTRACEPTION IN PREVENTION OF UNSAFE ABORTION THE ROLE OF POST- ABORTION CONTRACEPTION IN PREVENTION OF UNSAFE ABORTION
International Federation of Gynecology and Obstetrics THE ROLE OF POST- ABORTION CONTRACEPTION IN PREVENTION OF UNSAFE ABORTION THE ROLE OF POST- ABORTION CONTRACEPTION IN PREVENTION OF UNSAFE ABORTION
Same-Day Access to Highly Effective Reversible Contraception: Moving from Plan B to Happily Ever After
 Same-Day Access to Highly Effective Reversible Contraception: Moving from Plan B to Happily Ever After Eleanor Bimla Schwarz, MD, MS Director, Women s Health Services Research Unit Center for Research
Same-Day Access to Highly Effective Reversible Contraception: Moving from Plan B to Happily Ever After Eleanor Bimla Schwarz, MD, MS Director, Women s Health Services Research Unit Center for Research
Male and female sterilization
 Male and female sterilization Catriona Melville Alison Bigrigg Abstract Male and female sterilization is used in many countries worldwide as a permanent method of contraception. Failure rates for female
Male and female sterilization Catriona Melville Alison Bigrigg Abstract Male and female sterilization is used in many countries worldwide as a permanent method of contraception. Failure rates for female
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea
 Page: 1 of 7 Last Review Status/Date: June 2015 for Primary and Secondary Dysmenorrhea Description Two laparoscopic surgical approaches are proposed as adjuncts to conservative surgical therapy for the
Page: 1 of 7 Last Review Status/Date: June 2015 for Primary and Secondary Dysmenorrhea Description Two laparoscopic surgical approaches are proposed as adjuncts to conservative surgical therapy for the
female steri e sterilisation female sterilisation male and female sterilisation male sterilisation emale sterilisation female male sterilisati
 your guide to male and female sterilisation Helping you choose the method of contraception that is best for you female sterilisati le sterilisation male sterilisation e sterilisation female female ster
your guide to male and female sterilisation Helping you choose the method of contraception that is best for you female sterilisati le sterilisation male sterilisation e sterilisation female female ster
According to the most recent data (2011
 CONTRACEPTION Adopting the opportunistic salpingectomy philosophy for benign hysterectomies has been fairly easy for ObGyns, but what about for permanent? Is it time to advocate for this global practice?
CONTRACEPTION Adopting the opportunistic salpingectomy philosophy for benign hysterectomies has been fairly easy for ObGyns, but what about for permanent? Is it time to advocate for this global practice?
The development of new medical technology invariably
 Cost-Effectiveness Analysis Comparing the Essure Tubal Sterilization Procedure and Laparoscopic Tubal Sterilization John A. Thiel, MD, George D. Carson, MD Department of Obstetrics and Gynecology, Regina
Cost-Effectiveness Analysis Comparing the Essure Tubal Sterilization Procedure and Laparoscopic Tubal Sterilization John A. Thiel, MD, George D. Carson, MD Department of Obstetrics and Gynecology, Regina
Carolyn Westhoff, M.D., and Anne Davis, M.D. INCIDENCE AND PREVALENCE
 FERTILITY AND STERILITY VOL. 73, NO. 5, MAY 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. CONTRACEPTION Tubal sterilization:
FERTILITY AND STERILITY VOL. 73, NO. 5, MAY 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. CONTRACEPTION Tubal sterilization:
Contraceptive. Ready Lessons II. What Can a Contraceptive Security Champion Do?
 Contraceptive Lesson Security Ready Lessons II Expand client choice and contraceptive security by supporting access to underutilized family planning methods. What Can a Contraceptive Security Champion
Contraceptive Lesson Security Ready Lessons II Expand client choice and contraceptive security by supporting access to underutilized family planning methods. What Can a Contraceptive Security Champion
Compare and contrast laparoscopic surgery verses methotrexate in a woman with the diagnosis of ectopic pregnancy
 Compare and contrast laparoscopic surgery verses methotrexate in a woman with the diagnosis of ectopic pregnancy Ectopic pregnancy is defined as the implantation of a conceptus outside of the uterine cavity.
Compare and contrast laparoscopic surgery verses methotrexate in a woman with the diagnosis of ectopic pregnancy Ectopic pregnancy is defined as the implantation of a conceptus outside of the uterine cavity.
CODING GUIDELINES FOR CONTRACEPTIVES. Effective June 1, 2017 Version 1.40
 CODING GUIDELINES FOR CONTRACEPTIVES Effective June 1, 2017 Version 1.40 TABLE OF CONTENTS ICD-10 CM Diagnosis Codes: Encounter for Contraception page 2 Coding for IUD Insertion and Removal Procedures
CODING GUIDELINES FOR CONTRACEPTIVES Effective June 1, 2017 Version 1.40 TABLE OF CONTENTS ICD-10 CM Diagnosis Codes: Encounter for Contraception page 2 Coding for IUD Insertion and Removal Procedures
Medicaid Family Planning Waiver Services CPT Codes and ICD-10 Diagnosis Codes
 CPT Code Description of Covered Codes Evaluation and Management 99384FP 99385FP Family planning new visit 99386FP 99394FP 99395FP Family planning established visit 99396FP 99401FP HIV counseling (pre-test)
CPT Code Description of Covered Codes Evaluation and Management 99384FP 99385FP Family planning new visit 99386FP 99394FP 99395FP Family planning established visit 99396FP 99401FP HIV counseling (pre-test)
REPRODUCTIVE ENDOCRINOLOGY
 REPRODUCTIVE ENDOCRINOLOGY FERTILITY AND STERILITY VOL. 82, NO. 1, JULY 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. Treatment
REPRODUCTIVE ENDOCRINOLOGY FERTILITY AND STERILITY VOL. 82, NO. 1, JULY 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. Treatment
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea. Original Policy Date
 MP 4.01.10 Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 4.01.10 Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
Infertility services reported by men in the United States: national survey data
 MALE FACTOR Infertility services reported by men in the United States: national survey data John E. Anderson, Ph.D., Sherry L. Farr, Ph.D., M.S.P.H., Denise J. Jamieson, M.D., M.P.H., Lee Warner, Ph.D.,
MALE FACTOR Infertility services reported by men in the United States: national survey data John E. Anderson, Ph.D., Sherry L. Farr, Ph.D., M.S.P.H., Denise J. Jamieson, M.D., M.P.H., Lee Warner, Ph.D.,
Patient Awareness and Understanding of Intrauterine Devices
 University of Vermont ScholarWorks @ UVM Family Medicine Block Clerkship, Student Projects College of Medicine 2016 Patient Awareness and Understanding of Intrauterine Devices Lindsey Marie Eastman University
University of Vermont ScholarWorks @ UVM Family Medicine Block Clerkship, Student Projects College of Medicine 2016 Patient Awareness and Understanding of Intrauterine Devices Lindsey Marie Eastman University
Family Planning and Infertility
 Family Planning and Infertility Chapter 20 Objectives Discuss types of reversible contraception Natural methods Mechanical barrier methods Hormonal contraceptives Discuss types of permanent contraception
Family Planning and Infertility Chapter 20 Objectives Discuss types of reversible contraception Natural methods Mechanical barrier methods Hormonal contraceptives Discuss types of permanent contraception
FEMALE MEDICAL HISTORY
 Name: Surname: Date of birth: Dear patient, filling out this questionnaire correctly and completely is very important, because this allows us to assess your situation faster during the consultation and
Name: Surname: Date of birth: Dear patient, filling out this questionnaire correctly and completely is very important, because this allows us to assess your situation faster during the consultation and
A Study on Tubal Recanalization
 DOI 10.1007/s13224-012-0165-5 ORIGINAL ARTICLE Ramalingappa A. Yashoda Received: 23 May 2009 / Accepted: 9 March 2012 / Published online: 8 June 2012 Ó Federation of Obstetric & Gynecological Societies
DOI 10.1007/s13224-012-0165-5 ORIGINAL ARTICLE Ramalingappa A. Yashoda Received: 23 May 2009 / Accepted: 9 March 2012 / Published online: 8 June 2012 Ó Federation of Obstetric & Gynecological Societies
Simplifying Vide Contraception. University of Utah Department of Ob/Gyn Post Grad Course February 13, 2017 David Turok
 Simplifying Vide Contraception University of Utah Department of Ob/Gyn Post Grad Course February 13, 2017 David Turok Background Objectives At the conclusion of this presentation participants will be able
Simplifying Vide Contraception University of Utah Department of Ob/Gyn Post Grad Course February 13, 2017 David Turok Background Objectives At the conclusion of this presentation participants will be able
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/57234 holds various files of this Leiden University dissertation. Author: Chapelle, C.F. la Title: Evidence-based implementation of minimally invasive surgery
Cover Page The handle http://hdl.handle.net/1887/57234 holds various files of this Leiden University dissertation. Author: Chapelle, C.F. la Title: Evidence-based implementation of minimally invasive surgery
Hysteroscopy - current trends and challenges
 J Obstet Gynecol India Vol. 58, No. 1 : January/February 2008 pg 57-62 Original Article Hysteroscopy - current trends and challenges Gour A, Zawiejska A, Mettler L Department of Obstetrics and Gynaecology,
J Obstet Gynecol India Vol. 58, No. 1 : January/February 2008 pg 57-62 Original Article Hysteroscopy - current trends and challenges Gour A, Zawiejska A, Mettler L Department of Obstetrics and Gynaecology,
Case Report. Introduction. E. Scott Sills 1-3, Gianpiero D. Palermo 4
 Case Report Obstet Gynecol Sci 2016;59(4):337-341 http://dx.doi.org/10.5468/ogs.2016.59.4.337 pissn 2287-8572 eissn 2287-8580 Combined hysteroscopy-laparoscopy approach for excision of pelvic nitinol fragment
Case Report Obstet Gynecol Sci 2016;59(4):337-341 http://dx.doi.org/10.5468/ogs.2016.59.4.337 pissn 2287-8572 eissn 2287-8580 Combined hysteroscopy-laparoscopy approach for excision of pelvic nitinol fragment
Sterilization: Introduction. Female Sterilization. Puerperal Tubal Sterilization
 Print Close Window Note: Large images and tables on this page may necessitate printing in landscape mode. Copyright The McGraw-Hill Companies. All rights reserved. Williams Obstetrics > Section VI. The
Print Close Window Note: Large images and tables on this page may necessitate printing in landscape mode. Copyright The McGraw-Hill Companies. All rights reserved. Williams Obstetrics > Section VI. The
Dr. P. M. Gopinath. Director & Senior Consultant Institute of OBG & IVF SRM Institute for Medical Sciences Chennai
 Dr. P. M. Gopinath PRESENT DESIGNATI ON: PRESENT AFFILIATIO NS: MAJOR ACHIEVEM ENTS: Director & Senior Consultant Institute of OBG & IVF SRM Institute for Medical Sciences Chennai Vice President of FERTILITY
Dr. P. M. Gopinath PRESENT DESIGNATI ON: PRESENT AFFILIATIO NS: MAJOR ACHIEVEM ENTS: Director & Senior Consultant Institute of OBG & IVF SRM Institute for Medical Sciences Chennai Vice President of FERTILITY
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea
 Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Policy Number: 4.01.17 Last Review: 11/2013 Origination: 11/2007 Next Review: 11/2014 Policy Blue Cross and Blue Shield
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Policy Number: 4.01.17 Last Review: 11/2013 Origination: 11/2007 Next Review: 11/2014 Policy Blue Cross and Blue Shield
Role of diagnostic hysteroscopy in evaluation of abnormal uterine bleeding and its histopathological correlation
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Chaudhari KR et al. Int J Reprod Contracept Obstet Gynecol. 2014 Sep;3(3):666-670 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Chaudhari KR et al. Int J Reprod Contracept Obstet Gynecol. 2014 Sep;3(3):666-670 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
The Value of Hysterosalpingography Before Reversal of Sterilization Procedures Involving the Fallopian Tubes
 1247 0361-803X/89/1 536-1 247 C American Aoentgen Ray SOCiety Stephen Karasick1 Saundra Ehrlich Received May 30, 1989; accepted after revision July 13, 1989 I Both authors: Department of Radiology, Thomas
1247 0361-803X/89/1 536-1 247 C American Aoentgen Ray SOCiety Stephen Karasick1 Saundra Ehrlich Received May 30, 1989; accepted after revision July 13, 1989 I Both authors: Department of Radiology, Thomas
Information for Informed Consent for Insertion of a Mirena IUD
 Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
Hysteroscopic sterilization using a micro-insert device: results of a multicentre Phase II study*
 Human Reproduction Vol.18, No.6 pp. 1223±1230, 2003 DOI: 10.1093/humrep/deg256 Hysteroscopic sterilization using a micro-insert device: results of a multicentre Phase II study* John F.Kerin 1,8, Jay M.Cooper
Human Reproduction Vol.18, No.6 pp. 1223±1230, 2003 DOI: 10.1093/humrep/deg256 Hysteroscopic sterilization using a micro-insert device: results of a multicentre Phase II study* John F.Kerin 1,8, Jay M.Cooper
According to data from the 2006 to 2008 National Survey
 ORIGINAL RESEARCH Modeled Cost Differences Associated With Use of Levonorgestrel Intrauterine Devices Amy Law, PharmD; Mark McCoy, PharmD, MBA; Melissa Lingohr-Smith, PhD; Jay Lin, PhD, MBA; and Richard
ORIGINAL RESEARCH Modeled Cost Differences Associated With Use of Levonorgestrel Intrauterine Devices Amy Law, PharmD; Mark McCoy, PharmD, MBA; Melissa Lingohr-Smith, PhD; Jay Lin, PhD, MBA; and Richard
TUBAL PLASTIC SURGERY is an accepted form of therapy in the treatment
 Tubal Plastic Surgery ADNAN MROUEH, M.D., ROBERT H. GLASS, M.D., and C. LEE BUXTON, M.D. TUBAL PLASTIC SURGERY is an accepted form of therapy in the treatment of infertility. However, reports have differed
Tubal Plastic Surgery ADNAN MROUEH, M.D., ROBERT H. GLASS, M.D., and C. LEE BUXTON, M.D. TUBAL PLASTIC SURGERY is an accepted form of therapy in the treatment of infertility. However, reports have differed
TUBAL INTRAMURAL POLYPS AND THEIR RELATIONSHIP TO INFERTILITY
 FERTHJTY AND STERILITY Copyright c 98 The American Fertility Society Vol. 36, No.6. May 98 Printed. in U.SA. TUBAL INTRAMURAL POLYPS AND THEIR RELATIONSHIP TO INFERTILITY MENACHEM P; DAVID, M.D.* DAVIDBEN-ZWI,
FERTHJTY AND STERILITY Copyright c 98 The American Fertility Society Vol. 36, No.6. May 98 Printed. in U.SA. TUBAL INTRAMURAL POLYPS AND THEIR RELATIONSHIP TO INFERTILITY MENACHEM P; DAVID, M.D.* DAVIDBEN-ZWI,
Contraception Choices: An Evidence Based Approach Case Study Approach. Susan Hellier PhD, DNP, FNP-BC, CNE
 Contraception Choices: An Evidence Based Approach Case Study Approach Susan Hellier PhD, DNP, FNP-BC, CNE Objectives Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC)
Contraception Choices: An Evidence Based Approach Case Study Approach Susan Hellier PhD, DNP, FNP-BC, CNE Objectives Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC)
Product Information. Confidence that lasts
 Confidence that lasts What is Mirena? Inhibition of sperm motility and function inside the uterus and the fallopian tubes, preventing fertilization (Videla-Rivero et al. 1987). Section of system Levonorgestrel
Confidence that lasts What is Mirena? Inhibition of sperm motility and function inside the uterus and the fallopian tubes, preventing fertilization (Videla-Rivero et al. 1987). Section of system Levonorgestrel
Our Moment of Truth TM
 Our Moment of Truth TM Report on Women s Health Care Experiences & Perceptions: Spotlight on Family Planning & Contraception Media Webinar Wednesday, October 9, 2013 10:30-11:30 a.m. Today s Agenda Welcome
Our Moment of Truth TM Report on Women s Health Care Experiences & Perceptions: Spotlight on Family Planning & Contraception Media Webinar Wednesday, October 9, 2013 10:30-11:30 a.m. Today s Agenda Welcome
Diagnostic L/S: Is it ever indicated? Prof. Dr. Nilgün Turhan Fatih University Medical School
 Diagnostic L/S: Is it ever indicated? Prof. Dr. Nilgün Turhan Fatih University Medical School Diagnostic Laparoscopy (DLS) DLS is the gold standard in diagnosing tubal pathology and other intraabdominal
Diagnostic L/S: Is it ever indicated? Prof. Dr. Nilgün Turhan Fatih University Medical School Diagnostic Laparoscopy (DLS) DLS is the gold standard in diagnosing tubal pathology and other intraabdominal
Trends in use of and complications from intrauterine contraceptive devices and tubal ligation or occlusion
 Howard et al. Reproductive Health (27) 4:7 DOI.86/s2978-7-334- RESEARCH Open Access Trends in use of and complications from intrauterine contraceptive devices and tubal ligation or occlusion Brandon Howard
Howard et al. Reproductive Health (27) 4:7 DOI.86/s2978-7-334- RESEARCH Open Access Trends in use of and complications from intrauterine contraceptive devices and tubal ligation or occlusion Brandon Howard
Fertility Assessment and Treatment Pathway
 Rejected referrals sent back to GP Fertility Assessment and Treatment Pathway Patients with fertility problems go to the GP GP Advice and Assessment GP to inform patient of access criteria for NHS-funded
Rejected referrals sent back to GP Fertility Assessment and Treatment Pathway Patients with fertility problems go to the GP GP Advice and Assessment GP to inform patient of access criteria for NHS-funded
Contraception: The Pill Needs to Share (or Move Over) Frankly Speaking EP 17
 Contraception: The Pill Needs to Share (or Move Over) Frankly Speaking EP 17 Transcript Details This is a transcript of an episode from the podcast series Frankly Speaking accessible at Pri- Med.com. Additional
Contraception: The Pill Needs to Share (or Move Over) Frankly Speaking EP 17 Transcript Details This is a transcript of an episode from the podcast series Frankly Speaking accessible at Pri- Med.com. Additional
KUALA LUMPUR SUMMARY MATERIALS AND METHODS INTRODUCTION
 Med. J. Malaysia Vol. 37 No. 3 September 1982. WITH HULKA CLIPS AT THE UNIVERSITY KUALA LUMPUR ASARI ABDUL RAHMAN V. SIVANESARATNAM A. ADLAN NURUDDIN SUMMARY An analysis of 86 patients sterilized laparoscopically
Med. J. Malaysia Vol. 37 No. 3 September 1982. WITH HULKA CLIPS AT THE UNIVERSITY KUALA LUMPUR ASARI ABDUL RAHMAN V. SIVANESARATNAM A. ADLAN NURUDDIN SUMMARY An analysis of 86 patients sterilized laparoscopically
Clinical Policy: Robotic Surgery Reference Number: CP.MP. 207
 Clinical Policy: Robotic Surgery Reference Number: CP.MP. 207 Effective Date: 03/05 Last Review Date: 10/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: Robotic Surgery Reference Number: CP.MP. 207 Effective Date: 03/05 Last Review Date: 10/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important
Coding for the Contraceptive Implant and IUDs
 LARC Quick Coding Guide 2018 UPDATE Coding for the Contraceptive Implant and IUDs CORRECT CODING can result in more appropriate compensation for services and devices. To help practices receive appropriate
LARC Quick Coding Guide 2018 UPDATE Coding for the Contraceptive Implant and IUDs CORRECT CODING can result in more appropriate compensation for services and devices. To help practices receive appropriate
Techniques for the interruption of tubal patency for female sterilisation (Review)
 Techniques for the interruption of tubal patency for female sterilisation (Review) Lawrie TA, Kulier R, Nardin JM This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Techniques for the interruption of tubal patency for female sterilisation (Review) Lawrie TA, Kulier R, Nardin JM This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Global Contraception
 Video Companion Guide Global Contraception Learning Objectives: By the end of the session, learners will be able to: Describe of all contraceptive methods. Develop a basic understanding of patient-centered
Video Companion Guide Global Contraception Learning Objectives: By the end of the session, learners will be able to: Describe of all contraceptive methods. Develop a basic understanding of patient-centered
REPRODUCTIVE ENDOCRINOLOGY
 FERTILITY AND STERILITY VOL. 74, NO. 2, AUGUST 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. REPRODUCTIVE ENDOCRINOLOGY
FERTILITY AND STERILITY VOL. 74, NO. 2, AUGUST 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. REPRODUCTIVE ENDOCRINOLOGY
Endometrial Cancer Biopsy of the endometrium Evaluation of women of all ages
 Endometrial Cancer Biopsy of the endometrium Evaluation of women of all ages Barbara S. Apgar, MD, MS Professor of Family Medicine University of Michigan Health System Ann Arbor, Michigan Cancer of the
Endometrial Cancer Biopsy of the endometrium Evaluation of women of all ages Barbara S. Apgar, MD, MS Professor of Family Medicine University of Michigan Health System Ann Arbor, Michigan Cancer of the
LEARNING OBJECTIVES. Beyond the Pill: Long Acting Contraception. Distribution Of Contraception Use By Women In The Us. Unintended Pregnancy is Common
 4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
Impact of Sterilization on Fertility in Southern India
 Impact of Sterilization on Fertility in Southern India Background The first two international conferences on population were mainly focused on the need for curtailing rapid population growth by placing
Impact of Sterilization on Fertility in Southern India Background The first two international conferences on population were mainly focused on the need for curtailing rapid population growth by placing
Surgery and Infertility
 Surgery and Infertility Dr Phill McChesney BHB MBChB FRANZCOG MRMed CREI Laparoscopy Prior to Considering IVF Diagnostic Tubal Surgery Treatment of peritubal adhesions Reconstructive surgery Sterilization
Surgery and Infertility Dr Phill McChesney BHB MBChB FRANZCOG MRMed CREI Laparoscopy Prior to Considering IVF Diagnostic Tubal Surgery Treatment of peritubal adhesions Reconstructive surgery Sterilization
RESOLUTION NO. 301 (Co-Sponsored G) SUBSTITUTE ADOPTED See Below
 RESOLUTION NO. 301 (Co-Sponsored G) SUBSTITUTE ADOPTED See Below Support Placement and Coverage of Long-Acting Reversible Contraceptives (LARC) in the Early Postpartum Period Introduced by the California
RESOLUTION NO. 301 (Co-Sponsored G) SUBSTITUTE ADOPTED See Below Support Placement and Coverage of Long-Acting Reversible Contraceptives (LARC) in the Early Postpartum Period Introduced by the California
ENDOMETRIAL ABLATION: TRENDS AND CHALLENGES IN 2017
 ENDOMETRIAL ABLATION: TRENDS AND CHALLENGES IN 2017 Philippe Laberge MD FRCSC ACGE Professor Obstetrics and Gynecology Laval University Quebec, Canada Disclosures I have used products or done clinical
ENDOMETRIAL ABLATION: TRENDS AND CHALLENGES IN 2017 Philippe Laberge MD FRCSC ACGE Professor Obstetrics and Gynecology Laval University Quebec, Canada Disclosures I have used products or done clinical
Ex Post-Evaluation Brief Yemen: Family Planning and Family Health
 Ex Post-Evaluation Brief Yemen: Family Planning and Family Health Programme/Client 13030/ - Family Planning Programme executing agency Family Planning and Family Health BMZ No. 1998 65 288 Year of sample/ex
Ex Post-Evaluation Brief Yemen: Family Planning and Family Health Programme/Client 13030/ - Family Planning Programme executing agency Family Planning and Family Health BMZ No. 1998 65 288 Year of sample/ex
