Histological findings of testicular biopsy in North Indian population
|
|
|
- Amberly Williamson
- 6 years ago
- Views:
Transcription
1 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Mahajan A et al. Int J Reprod Contracept Obstet Gynecol Apr;4(2): pissn eissn DOI: / ijrcog Research Article Histological findings of testicular biopsy in North Indian population Arpita Mahajan*, Smita Kakar, J. M. Kaul, Sabita Mishra Department of Anatomy, Maulana Azad Medical College, Delhi University, New Delhi , India Received: 09 February 2015 Revised: 17 February 2015 Accepted: 01 March 2015 *Correspondence: Dr. Arpita Mahajan, arpitamahajan27@gmail.com Copyright: the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Background: Infertility is defined as the inability to achieve pregnancy after one year of unprotected intercourse. To interpret these testicular causes, biopsy of testis and its classification becomes an important tool for diagnoses. Biopsy is mostly done in severe oligozoospermic or azoospermic patients. Biopsies are also important in recent times due to introduction of Assisted Reproductive Techniques (ART) because they determine the level of spermatogenesis. In the present study the testicular biopsy has been classified into seven categories. One of the classification is that of the highly homogenous mass, which is an addition to the studies done previously. The increase in connective tissue has been demonstrated by Masson s trichrome stain not cited in the literature. This study will help relook into the way of categorising the testicular biopsy which will benefit those seeking treatment of male infertility. Methods: The study was carried out on 30 infertile patients who were either azoospermic (nil to <2 x10 6 sperms/ml) or severe oligozoospermic (<5 x10 6 sperms/ml). Testicular biopsy of these patients was taken after obtaining ethical clearance and written consent of the patients. The biopsy was processed, stained and assessed using haematoxylin and eosin and Masson s trichrome. They were classified into different histological types. They were also categorised by modified Johnsen scoring. Results: The biopsies were classified histologically into obstructive azoospermia in 4 cases (13.33%). Hypospermatogenesis in 5 cases (16.66%), maturation arrest in 3 cases (10%), sertoli cell only syndrome in 3 cases (10%), seminiferous tubule hyalinization in 7 cases (23.33%), mixed patterns in 6 cases (20%) and highly cellular homogenous tissue in 2 cases (6.66%). The last condition has not been classified in the literature cited. Conclusions: By the present study we can determine the level of spermatogenesis and by studying the nature of different germ cells we can use it for ART. Consideration of the biopsy being taken from a particular part of the testis must be kept in mind, and there might be the possibility of spermatogenesis occurring in some other quadrant. The patient needs to be explained this. Keywords: Testicular biopsy, Male infertility, Histological classification INTRODUCTION The investigation of male infertility includes history, physical examination, biochemical investigations, semen analysis and testicular biopsy. 1 The first investigation as an infertile patient approaches for treatment is semen analysis. Some patients with low semen count need to get a testicular biopsy done. The combination of testicular biopsy and clinical evaluation for male infertility is becoming progressively more important because new technologies allow men previously considered infertile to father a child. 2 Earlier studies have categorized biopsies into different conditions. In men with azoospermia (sperm count nil), testicular biopsy determines if a blockage is present in the sperm pathway as there is presence of germ cells on histological examination of the testicular tissue. If there is primary testicular failure no germ cells are seen in the biopsy. 3 For obstructive azoospermic patients with Volume 4 Issue 2 Page 432
2 normal spermatogenesis, biopsy can be used to identify spermatozoa or spermatids, which can be therapeutically used in assisted reproductive techniques. 4-6 To understand testicular biopsy, knowledge of spermatogenesis and detailed information about the organization of the germinal epithelium its structure and function of different types of germ cells is necessary. Normally all stages of differentiation are not present simultaneously and hence normal spermatogenesis does not yield mature spermatids in every tubular cross section in a testicular biopsy. Various immature stages are normally observed and do not necessarily mean a maturation abnormality. Histologically each tubule has a basement membrane composed of a basal lamina and laminated connective tissue containing numerous fibres covered externally by flat epitheloid cells. Internal to it, the seminiferous epithelium consists of spermatogenic and supportive cells. The former when active include an array of types ranging from spermatogonia through their derived forms, spermatocytes and spermatids to mature spermatozoa. In the fully differentiated testis they appear along the basal laminae of the seminiferous tubules. 5,6 Primary spermatocytes at first resemble in size and cytological characteristics the spermatogonia from which they arise but as they move away from basal lamina of the germinal epithelium, they accumulate more cytoplasm and become distinctly larger. After completion of meiosis I there is formation of secondary spermatocytes carrying only half the number of chromosomes originally present. The secondary spermatocytes quickly complete the second phase of meiotic division and spermatids are formed that have a haploid set of chromosomes. 7 Sertoli cells or sustentacular cells abut on the basal lamina of the tubules. In tangential sections, these are polygonal and in transverse section the same are columnar. 5,8,9 Leydig cells lie in the interstitial tissue in small and sometimes large groups. The intertubular tissue contains fibroblasts, collagen and blood vessels. 10,11 Spermatogenesis is the series of changes by which spermatogonia are transformed into spermatozoa. It may be divided into three phases, spermatocytogenesis, in which spermatogonia proliferate by mitotic division to produce primary spermatocytes. In the second phase (meiosis) successive maturation divisions produce secondary spermatocytes and spermatids, all with haploid number of chromosomes. The third phase is spermiogenesis when the spermatids become spermatozoa. 5,12,13 The spermatogenic cycle is defined as a series of changes in a given region of seminiferous epithelium between two appearances of the same developmental stages. Using spermiation as reference, the cycle is composed of all the events that occur in a given region of the tubule between two consecutive spermiations. In humans the 27 days of spematocytogenesis, 24 days of meiosis, and 23 days of spermiogenesis compose the 74-day duration of spermatogenesis. 10,14 The biopsies studied by various scientists have been categorized into different conditions and each of these needs to be dealt clinically at an individual level. The present study highlights the various conditions in the north Indian population. METHODS The study was carried out on 30 patients who had presented to Surgery OPD with complaint of infertility. Semen analysis was carried out to categorize them, cases of azoospermia or severe oligozoospermia were taken as subjects for study. Testicular biopsy of these patients were taken in department of surgery after obtaining ethical clearance and written consent. The biopsy was processed, stained and assessed. Collection and processing of biopsy The testicular biopsy of one side was obtained by removal of a small piece of tissue while the patient was under light anesthesia (conscious sedation) and tissue was preserved in 10% buffered formalin for 1 week. Tissue was labeled and embedded in paraffin and sections were cut at 5µ with rotary microtome. The testicular morphology was analyzed after staining with haematoxylin & eosin and Masson s trichrome. Testicular tissue was also obtained from fresh male cadavers in department of anatomy and the one that showed normal spermatogenesis was used as a control for the study. The testicular biopsies were first analyzed qualitatively under low power and study of cells was done at high power. The control showed seminiferous tubules which had germ cells and sertoli cells confined to the basement membrane. Spermatogonia were close to the basement membrane and had clumped nuclear chromatin. Primary spermatocytes were largest cells, displaying a scattered chromatin and secondary spermatocytes formed an inner layer of smaller cells. Spermatids were 2 to 3 layers of small round cells with oval nuclei and late spermatids were more flattened. Sertoli cells were pyramidal in shape and stood at intervals on basement membrane. Leydig cells occurred in intertubular tissue, were large and polyhedral, with an eccentric nucleus and a scanty and poorly stained cytoplasm. Leydig cells, connective tissue and blood vessels were in the interstitial tissue. Myoid cells with flattened nuclei were just external to the basement membrane. RESULTS The thirty testicular biopsies obtained from Department of surgery were studied after processing and staining, a normal testis was used as control (Figure 1) to compare. The morphology of biopsied tissues studied International Journal of Reproduction, Contraception, Obstetrics and Gynecology Volume 4 Issue 2 Page 433
3 qualitatively\with respect to the tubules, basement membrane and interstitium. The haematoxylin and eosin staining was used to identify the germ cells, leydig cells and interstitial tissue. To study the increased connective tissue Masson s trichrome staining was used. On the basis of above description the biopsies were classified histologically into seven types in Table 1. commonly in our study (Figure 7a, 7b). Two of the biopsies showed haphazardly scattered cells which could not be defined, no tubules were seen. Figure 1: Normal testis: Haematoxylin and Eosin (H&E) staining in normal testis at 40x (magnification) showing seminiferous tubules with normal spermatogenesis, intertubular connective tissue (ITT), spermatogonia (Sg), spermatocyte (Sp), sertoli cell (Sc), spermatids (St), leydig cells (L). Figure 2a: Obstructive azoospermia: H&E staining in obstructive azoospermia at 40x. Increased connective tissue (CT), spermatogonia (Sg), sertoli cell (Sc), spermatids (St) and myoid cell (M). Table 1: Histopathological classification of male infertility. Clinical condition No. of cases % Obstructive azoospermia % Hypospermatogenesis % Maturation arrest 3 10% Sertoli cell only syndrome 3 10% Seminiferous tubule hyalinization % Mixed pattern 6 20% Highly homogenous mass % Obstructive azoospermia (Figure 2a, 2b) showed essentially normal spermatogenesis with a high density of germ cells in the tubules, azoospermia on semen analysis implied obstruction of some part of the duct system. In Hypospermatogenesis (Figure 3), tissue showed a decrease in the total number of germ cell types though all stages of the spermatogenesis were seen, the sperm count was severe oligozoospermic or azoospermic. Maturation Arrest (Figure 4) presented the germ cells upto the spermatocytic stage, the semen mostly showed azoospermia. Sertoli cell only syndrome (Figure 5) had only sertoli cells with no or very few germ cells in the seminiferous tubules, the semen analysis mostly showed azoospermia. Seminiferous tubule hyalinization (Figure 6a, 6b, 6c, 6d) showed no tubules but increased connective tissue with azoospermia. In Mixed patterns hypospermatogenesis with maturation arrest was seen Figure 2b: Obstructive azoospermia: Masson s trichrome staining in obstructive azoospermia at 40x showing connective tissue (CT). Seminiferous tubules (T) seen. Basement membrane shown with the arrow. Figure 3: Hypospermatogenesis: H&E staining in hypospermatogenesis at 40x. Stippled arrow showing spermatogonia, small bold arrow showing spermatids, big bold arrow showing sertoli cell. Arrow head showing leydig cells. International Journal of Reproduction, Contraception, Obstetrics and Gynecology Volume 4 Issue 2 Page 434
4 Figure 4: Maturation arrest: H&E staining in maturation arrest at 40x. Stippled arrows showing spermatogonia and big bold arrow showing sertoli cell showing sertoli cell. Bold arrow heads showing leydig cells. Figure 6a: Seminiferous tubule hyalinization: H&E staining in seminiferous tubule hyalinization at 10x. The tubular outline cannot be seen. Figure 6b: Seminiferous tubule hyalinization: H&E staining in seminiferous tubule hyalinizationat 40x. Hyalinization (H) seen. Figure 5: Sertoli cell only syndrome: H&E staining in sertoli cell only syndrome at 40x. Big bold arrow showing sertoli cell, stippled arrow showing myoid cells and bold arrow showing blood vessel. Figure 6c: Seminiferous tubule hyalinization: Masson s trichrome staining in seminiferous tubule hyalinization at 10x. Hyalinization seen. Blood vessel (BV) seen. International Journal of Reproduction, Contraception, Obstetrics and Gynecology Volume 4 Issue 2 Page 435
5 Figure 6d: Seminiferous tubule hyalinization: Masson s trichrome staining in seminiferous tubule hyalinization at 40x. Hyalinization (H) seen. Figure 8a: Highly cellular homogenous mass: H&E staining in highly cellular homogenous mass at 40x. Figure 7a: Mixed patterns: H&E staining in mixed pattern at 40x. Hypospermatogenesis shown by (H) and maturation arrest by (M). Figure 7b: Mixed patterns: H&E staining in mixed pattern at 40x. Hypospermatogenesis shown by (H) and maturation arrest by (M). Figure 8b: Highly cellular homogenous mass: H&E staining in highly cellular homogenous mass at 40x. DISCUSSION Testicular biopsy is an important tool in the investigation and the assessment of male infertility. It may shed some light on the etiology as well as providing essential prognostic information. The histological patterns in the testicular biopsies are classified according to the presence and amount of spermatogenesis, maturation of germinal cells and presence of associated tubular atrophy, interstitial fibrosis. It is not the only parameter for determining the testicular histopathology pattern but apparently the strongest indicator to foresee the possibility of finding sperms in the testis for therapeutic sperm retrieval in assisted reproductive techniques. The introduction of intracytoplasmic sperm injection revolutionized the treatment of male infertility by requiring a minimal number of sperm to achieve pregnancy. The surgical testicular biopsy techniques followed by morphologic examination, permits many patients with infertility to receive a favorable prognosis and therapeutic trial. 6 In addition, testicular biopsy is important in the evaluation of men at risk for testicular International Journal of Reproduction, Contraception, Obstetrics and Gynecology Volume 4 Issue 2 Page 436
6 cancer. 2 The testicular biopsy for infertility requires understanding of a different set of diagnostic categories not otherwise commonly encountered. 3 Studying human spermatogenesis will benefit clinicians, toxicologists, and epidemiologists by direct evaluation of testis or indirectly via evaluations of quantity and quality of sperm ejaculated. It also will benefit scientists interested in renewal and proliferation of spermatogonia as a prototype stem cell. 14 Since classification of biopsies is important to determine treatment of the infertile patient they were categorised into obstructive azoospermia with normal spermatogenesis, hypospermatogenesis, maturation arrest, sertoli cell only syndrome (Germinal cell aplasia), seminiferous tubular hyalinization, mixed pattern and highly cellular homogenous mass. The above classification, has been used by many authors in their studies, 4,15-18 There are a few authors who have added a mixed pattern, showing more than one type of pattern in a particular biopsy. 2,19,20 The homogenous mass has not been described in any of the studies cited. In our study tubular hyalinization was the most common cause of male infertility followed by hypospermatogenesis, which is the most common cause according to some studies. 1 A comparison has been worked out with the work of other authors and has been described in Table 2. To describe each of the above conditions the biopsies were studied systematically according to previous studies. Obsrtructive azoospermia was reported when the tubules showed all stages of spermatogenesis but with increase in number as compared to a normal control. Cases of maturation arrest were classified by evaluating whether spermatogenesis proceeds to full spermatid differentiation across the tubules. It was done by working backwards for the presence of elongated spermatids across tubules, if they were absent, then working backward through spermatocytes to spermatogonia allowed us to note at which level differentiation was arrested. Germ cell arrest was diagnosed only if there was no maturation beyond an immature stage in all tubules present within the biopsy. When there was heterogeneous i.e. some tubules showed a particular condition and others showed another pattern a mixed pattern was reported. The term sertoli-cell-only syndrome was reserved for those cases in which all the tubules in the biopsy showed absence of germ cells with presence of sertoli cells. If the tubular basement membranes were thickened, along with absence of germ cell development and shrunken lumens, the diagnosis was tubular hyalinization. We saw a few cases which showed haphazard arrangement of cells which could not be classified into above groups and were put under highly homogenous tissue. A comparison of our study with the other authors has been done in table II. The distinction between obstructive and non-obstructive azoospermia is important. Testicular biopsy helps to differentiate between them. Men with obstructive azoospermia may have options for treatment, such as surgical reconstruction of the reproductive tract. Table 2: Comparison of the present study with other studies. Condition Abdullah L Wong TW Rosai J Brannen GE Present et al. et al. et al. et al. study Obstructive azoospermia 13% - 27% % Hypospermatogenesis 29% 22.9% - 23% 16.66% Maturation arrest 12% 32.1% 26% 4% 10% Sertoli-cell-only syndrome 16% - 29% 12.5% 10% Seminiferous tubular hyalinization 16% 18% 12.5% 23.3% Mixed patterns 9% % Highly cellular homogenous mass % Non-obstructive azoospermia may be caused by many causes but most are idiopathic. Testicular biopsy may show scattered foci of spermatogenesis in some cases with potential for surgical sperm retrieval and intracytoplasmic sperm injection but a real risk of failure to retrieve spermatozoa exists in men with nonobstructive azoospermia and couples must be informed of this risk before attempting assisted reproduction as the area from where the biopsy is obtained may or may not be having spermatogenesis. Men with non-obstructive azoospermia should have genetic testing as 15-30% of them have sex chromosome aneuploidy or Y chromosome deletions On starting the TESE-ICSI programme a preliminary explorative testicular biopsy is done to ascertain that complete spermatogenesis is present in at least some seminiferous tubules in order to guarantee sperm retrieval for the planned TESE-ICSI attempt. If the sperms are not available some studies suggest use of spermatids which is under study. 23 Male infertility study requires systematization of clinical and paraclinical diagnostic procedures and the knowledge of techniques to analyze functional capacity of human spermatozoon. The application of the various methods of assisted reproduction in male infertility treatment, should be judged with a good criterion in order to offer maximal benefit and least risk. The present study will help in International Journal of Reproduction, Contraception, Obstetrics and Gynecology Volume 4 Issue 2 Page 437
7 determining the nature of germ cells in the testicular biopsy which will benefit in above procedures. Consideration of the biopsy being taken from a particular part of the testis must be kept in mind, and there might be the possibility of spermatogenesis occurring in some other quadrant. The patient needs to be explained this. Patients in whom ICSI is not possible, need to go for surrogacy or adoption. Funding: No funding sources Conflict of interest: None declared Ethical approval: The study was approved by the institutional ethics committee REFERENCES 1. Shefi S, Turek PJ. Definition and current evaluation of subfertile men. Int Braz J Urol Jul;32(4): Abdullah L, Bondagji N. Histopathological patterns of testicular biopsy in male infertility: a retrospective study from a tertiary care centre in the western part of Saudi Arabia. Urol Ann Jan-Apr;3(1): Brugh VM, Lipshultz LI. Male factor infertility: Evaluation and management. Med Clin North Am Mar;88(2): Wong TW, Strauss FH, Warner NE. Testicular biopsy in the study of male infertility. Arch Pathol. 1973;95: Williams PL, Bannister LH, Berry MM, Collins P, Dyson M, Dussek JE. Reproductive organs of the male. In: Williams PL, Bannister LH, Berry MM, Collins P, Dyson M, Dussek JE, eds. Gray s Anatomy, 38th ed. London: Elsevier Churchill Livingstone; 2000: Ross MH, Pawlina W. Male reproductive system: spermatogenesis. In: Ross MH, Pawlina W, eds. Histology. A Text and Atlas. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2011: Bloom W, Fawcett DW. Male reproductive system. In: Bloom W, Fawcett DW, eds. A Textbook of Histology. 11th ed. Philadelphia: W.B. Saunders; 1986: Ronald CS. The testis: the normal testis. Arch Pathol Sep;50(3): Kobil E, Neill JD. Cytology of testis and intrinsic control mechanisms. In: Kobil E, Neill JD, eds. Physiology of Reproduction, 3rd ed. US: Elsevier; 2006: Wallace RL. Testis overview. In: Wallace RL, eds. Encyclopedia of Reproduction. 4th ed. US: Academic Press; 1998: Kerr JB. Functional cytology of the human testis. Baillieres Clin Endocrinol Metab Apr;6(2): Johnson L. Efficiency of spermatogenesis. Microsc Res Tech Dec;32(5): Miething A. The establishment of spermatogenesis in the seminiferous epithelium of the pubertal golden hamster (Mesocricetus auratus). Adv Anat Embryol Cell Biol. 1998;140: Clermont Y. Dynamics of human spermatogenesis. In: Clermont Y, eds. Proceedings of the Workshop Conference on the Human Testis in Positano. Italy: Plenum Press; 1970: Rosai J. Male reproductive system: normal embryology and anatomy. In: Rosai J, eds. Surgical Pathology. 9th ed. US: Elsevier; 2004: Brannen GE, Roth RR. Testicular abnormalities of the subfertile male. J Urol Dec;122: Anthony S, Leong Y, Mathews CD. The role of testicular biopsy in the investigation of male infertility. Pathology Apr;14(2): Ronald CS, Howard RP, Simmons FA. The Testis: abnormalities of spermatogenesis. Arch Pathol Sep;50(3): Mills SE. Urinary tract and male genital system. In: Mills SE, eds. Diagnostic Surgical Pathology. 4th ed. Philadelphia: Lippincott Williams & Wilkins; 2004: Cerilli LA, Kuang W, Rogers D. A practical approach to testicular biopsy interpretation for male infertility. Arch Pathol Lab Med Aug;134: Hung AJ, King P, Schlegel PN. Uniform testicular maturation arrest: a unique subset of men with nonobstructive azoospermia. J Urol Aug;178(2): Maymon BB, Yogev L, Paz G, Kleiman SE, Schreiber L, Botchan A, et al. Sertoli cell maturation in men with azoospermia of different etiologies. Fertil Steril May;77(5): Vanderzwalmen P, Zech H, Birkenfeld A, Yemini M, Bertin G, Lejeune B, et al. Intracytoplasmic injection of spermatids retrieved from testicular tissue: influence of testicular pathology, type of selected spermatids and oocyte activation. Hum Reprod. 1997;12(6): DOI: / ijrcog Cite this article as: Mahajan A, Kakar S, Kaul JM, Mishra S. Histological findings of testicular biopsy in North Indian population. Int J Reprod Contracept Obstet Gynecol 2015;4: International Journal of Reproduction, Contraception, Obstetrics and Gynecology Volume 4 Issue 2 Page 438
Infertility is not an uncommon problem in Western
 Review Article A Practical Approach to Testicular Biopsy Interpretation for Male Infertility Lisa A. Cerilli, MD; Wayne Kuang, MD; David Rogers, MD Infertility is not an uncommon problem in Western societies
Review Article A Practical Approach to Testicular Biopsy Interpretation for Male Infertility Lisa A. Cerilli, MD; Wayne Kuang, MD; David Rogers, MD Infertility is not an uncommon problem in Western societies
Male Reproductive System
 Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
Variability in testis biopsy interpretation: implications for male infertility care in the era of intracytoplasmic sperm injection
 Variability in testis biopsy interpretation: implications for male infertility care in the era of intracytoplasmic sperm injection Matthew R. Cooperberg, M.D., a Thomas Chi, B.A., a Amir Jad, M.D., a Imok
Variability in testis biopsy interpretation: implications for male infertility care in the era of intracytoplasmic sperm injection Matthew R. Cooperberg, M.D., a Thomas Chi, B.A., a Amir Jad, M.D., a Imok
REAPPRAISAL OF THE VALUE OF TESTICULAR BIOPSY IN THE INVESTIGATION OF INFERTILITY
 FERTWTY AND STEIuLlTY Copyright 1980 The American Fertility Society Vol., No.1 January 1980 Prinwl in U.S.A. REAPPRAISAL OF THE VALUE OF TESTICULAR BIOPSY IN THE INVESTIGATION OF INFERTILITY TERENCE
FERTWTY AND STEIuLlTY Copyright 1980 The American Fertility Society Vol., No.1 January 1980 Prinwl in U.S.A. REAPPRAISAL OF THE VALUE OF TESTICULAR BIOPSY IN THE INVESTIGATION OF INFERTILITY TERENCE
Histology of Male Reproductive system (1)
 Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Patterns of Testicular Histopathology in Egyptian Azoospermic Men
 ISPUB.COM The Internet Journal of Urology Volume 13 Number 1 Patterns of Testicular Histopathology in Egyptian Azoospermic Men M K Khalifa, A M Issa, M O El Hamshary, K Z Shaeer Citation M K Khalifa, A
ISPUB.COM The Internet Journal of Urology Volume 13 Number 1 Patterns of Testicular Histopathology in Egyptian Azoospermic Men M K Khalifa, A M Issa, M O El Hamshary, K Z Shaeer Citation M K Khalifa, A
Adapted from Preg. & Part., Senger
 MALE ENDOCRINOLOGY AND SPERMATOGENESIS (Chapter 10) AVS 222 (Instructor: Dr. Amin Ahmadzadeh) I. MALE ENDOCRINOLOGY (Figure10-1 to 10-3) A. Glands and their respective hormones 1) Hypothalamic hormone:
MALE ENDOCRINOLOGY AND SPERMATOGENESIS (Chapter 10) AVS 222 (Instructor: Dr. Amin Ahmadzadeh) I. MALE ENDOCRINOLOGY (Figure10-1 to 10-3) A. Glands and their respective hormones 1) Hypothalamic hormone:
Spermatogenesis. What is it and what does it look like? How do hormones regulate spermatogenesis?
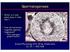 Spermatogenesis What is it and what does it look like? How do hormones regulate spermatogenesis? FSH, androgens, growth factors Animal Physiology (Hill, Wise, Anderson): Ch. 15 435-438 1 Spermatogenesis:
Spermatogenesis What is it and what does it look like? How do hormones regulate spermatogenesis? FSH, androgens, growth factors Animal Physiology (Hill, Wise, Anderson): Ch. 15 435-438 1 Spermatogenesis:
The spermatogenesis CHARACTERISTICS OF THE SPERMATOZOON 26/04/2017. Reproductive Biotechnologies Andrology I. Prof. Alberto Contri
 Reproductive Biotechnologies Andrology I The spermatogenesis Prof. Alberto Contri CHARACTERISTICS OF THE SPERMATOZOON 1) Aploid cell with high condensed DNA 2) Forward motility - flagellum 3) Enzymes for
Reproductive Biotechnologies Andrology I The spermatogenesis Prof. Alberto Contri CHARACTERISTICS OF THE SPERMATOZOON 1) Aploid cell with high condensed DNA 2) Forward motility - flagellum 3) Enzymes for
Male Reproductive System
 Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Medical School Histology Basics Male Reproductive System. VIBS 289 lab
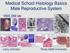 Medical School Histology Basics Male Reproductive System VIBS 289 lab Larry Johnson Texas A&M University OBJECTIVE To conduct a histologic examination of the testis (which produce spermatozoa), excretory
Medical School Histology Basics Male Reproductive System VIBS 289 lab Larry Johnson Texas A&M University OBJECTIVE To conduct a histologic examination of the testis (which produce spermatozoa), excretory
MALE INFERTILITY & SEMEN ANALYSIS
 MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
5 15/3/2012. Malik Al-Momani
 5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
The Use of Rabbits in Male Reproductive Toxicology
 Environmental Health Perspectives Vol. 77, pp. 5-9, 1988 The Use of Rabbits in Male Reproductive Toxicology by Daniel Morton* The rabbit is the smallest and least expensive laboratory animal in which serial
Environmental Health Perspectives Vol. 77, pp. 5-9, 1988 The Use of Rabbits in Male Reproductive Toxicology by Daniel Morton* The rabbit is the smallest and least expensive laboratory animal in which serial
Spermatogenesis Following Experimental Testicular Ischemia
 Spermatogenesis Following Experimental Testicular Ischemia Frank Hinman, Jr, MD, and Gilbert I Smith, MD REGENERATION of the spermatogenic elements of the testis after depression by testosterone and by
Spermatogenesis Following Experimental Testicular Ischemia Frank Hinman, Jr, MD, and Gilbert I Smith, MD REGENERATION of the spermatogenic elements of the testis after depression by testosterone and by
Testicular fine needle aspiration as a diagnostic tool in nonobstructive
 Asian J Androl 2005; 7 (3): 289 294 DOI: 10.1111/j.1745-7262.2005.00043.x. Original Article. Testicular fine needle aspiration as a diagnostic tool in nonobstructive azoospermia A. Bettella 1, A. Ferlin
Asian J Androl 2005; 7 (3): 289 294 DOI: 10.1111/j.1745-7262.2005.00043.x. Original Article. Testicular fine needle aspiration as a diagnostic tool in nonobstructive azoospermia A. Bettella 1, A. Ferlin
Outcome of repeated micro-surgical testicular sperm extraction in patients with non-obstructive azoospermia
 Repeated micro-surgical testicular sperm extraction DOI: 10.1111/j.1745-7262.2007.00273.x www.asiaandro.com. Original Article. Outcome of repeated micro-surgical testicular sperm extraction in patients
Repeated micro-surgical testicular sperm extraction DOI: 10.1111/j.1745-7262.2007.00273.x www.asiaandro.com. Original Article. Outcome of repeated micro-surgical testicular sperm extraction in patients
Gametogenesis. Omne vivum ex ovo All living things come from eggs.
 Omne vivum ex ovo All living things come from eggs. William Harvery, 1651 Gametogenesis This lecture is the preface, so to speak, to embryology; that is, it introduces the development of the specialized
Omne vivum ex ovo All living things come from eggs. William Harvery, 1651 Gametogenesis This lecture is the preface, so to speak, to embryology; that is, it introduces the development of the specialized
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Spermatogenesis in Man
 Spermatogenesis in Man I. Nuclear Morphology During Spermatogenesis in Man BRUNETTO CHIARELLI, PH.D., ARTHUR FALEK, PH.D., KAREN J. BACK, B.S., and C. THOMAS COWART, M.D. THE SEQUENCE of transformations
Spermatogenesis in Man I. Nuclear Morphology During Spermatogenesis in Man BRUNETTO CHIARELLI, PH.D., ARTHUR FALEK, PH.D., KAREN J. BACK, B.S., and C. THOMAS COWART, M.D. THE SEQUENCE of transformations
Identification of the spermatogenic stages in living seminiferous tubules of man
 Identification of the spermatogenic stages in living seminiferous tubules of man V. Nikkanen, K.-O. S\l=o"\derstr\l=o"\m and M. Parvinen Department of Obstetrics and Gynecology, Turku University Central
Identification of the spermatogenic stages in living seminiferous tubules of man V. Nikkanen, K.-O. S\l=o"\derstr\l=o"\m and M. Parvinen Department of Obstetrics and Gynecology, Turku University Central
IN normal male fowls, four developmental stages of spermatogenetic activity
 Development of the Testis Tubule in the Fowl By GAMAL A. R. KAMAR (From the Animal Production Department, Faculty of Agriculture, Cairo University, Giza, Egypt) With three plates (figs. 1-3) SUMMARY Three
Development of the Testis Tubule in the Fowl By GAMAL A. R. KAMAR (From the Animal Production Department, Faculty of Agriculture, Cairo University, Giza, Egypt) With three plates (figs. 1-3) SUMMARY Three
Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients
 Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients Basim Sh. Ahmed F.I.C.M.S Department of Pathology, College of Medicine, Al-Mustansiriya University, Baghdad,
Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients Basim Sh. Ahmed F.I.C.M.S Department of Pathology, College of Medicine, Al-Mustansiriya University, Baghdad,
Basic histology 5/4/2015
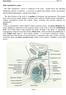 Male reproductive system The male reproductive system is composed of the testes, genital ducts (the adjoining epididymis, and the vas deferens, a accessory sex glands (the seminal vesicles, the prostrate
Male reproductive system The male reproductive system is composed of the testes, genital ducts (the adjoining epididymis, and the vas deferens, a accessory sex glands (the seminal vesicles, the prostrate
Chapter1 Introduction
 Chapter1 Introduction Male subfertility is a very significant global problem. Epidemiological data show that approximately 1-in-7 couples are classed as subfertile [1]. Sperm dysfunction is the single
Chapter1 Introduction Male subfertility is a very significant global problem. Epidemiological data show that approximately 1-in-7 couples are classed as subfertile [1]. Sperm dysfunction is the single
Comparative studies of spermatogenesis in fertile and
 J Clin Pathol 1981 ;34:145-150 Comparative studies of spermatogenesis in fertile and subfertile men MA LAMONT,* MJW FAED,* AND K BAXBYt From the *Cytogenetics Laboratory, Ninewells Hospital and Medical
J Clin Pathol 1981 ;34:145-150 Comparative studies of spermatogenesis in fertile and subfertile men MA LAMONT,* MJW FAED,* AND K BAXBYt From the *Cytogenetics Laboratory, Ninewells Hospital and Medical
The Male Reproductive System
 The Male Reproductive System YONG-MEI CHEN ( 陈咏梅 ) Dept. of Anatomy, Histology & Embryology Peking Union Medical College Tel:69156461 E-mail address: pumc_he@126.com Content Spermatogenesis Spermiogenesis
The Male Reproductive System YONG-MEI CHEN ( 陈咏梅 ) Dept. of Anatomy, Histology & Embryology Peking Union Medical College Tel:69156461 E-mail address: pumc_he@126.com Content Spermatogenesis Spermiogenesis
Production of Fertile Sperm. Animal Science 434. Hormonal Regulation of the Testis. hormonal regulation of the testis
 roduction of Fertile Sperm hormonal regulation of the testis nimal Science 434 Lecture 12: Spermatogenesis mitotic division of spermatogonia meiotic divisions of spermatocytes morphologic transformation
roduction of Fertile Sperm hormonal regulation of the testis nimal Science 434 Lecture 12: Spermatogenesis mitotic division of spermatogonia meiotic divisions of spermatocytes morphologic transformation
Seminiferous Tubules
 Testes The testes are compound tubular glands that lie within a scrotal sac, suspended from the body by a spermatic cord. The testes are dual organs that act as exocrine glands producing a holocrine secretion,
Testes The testes are compound tubular glands that lie within a scrotal sac, suspended from the body by a spermatic cord. The testes are dual organs that act as exocrine glands producing a holocrine secretion,
MALE REPRODUCTIVE SYSTEM
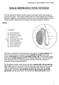 MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
Embryology 3. Spermatogenesis:
 Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Treatment of Defective Spermatogenesis tvith Human Gonadotropins
 Treatment of Defective Spermatogenesis tvith Human Gonadotropins W. Z. POLISHUK, M.D., Z. PALTI, M.D., and A. LAUFER, M.D. TREATMENT of male sterility due to defective spermatogenesis is not satisfactory.
Treatment of Defective Spermatogenesis tvith Human Gonadotropins W. Z. POLISHUK, M.D., Z. PALTI, M.D., and A. LAUFER, M.D. TREATMENT of male sterility due to defective spermatogenesis is not satisfactory.
Male factors determining the outcome of intracytoplasmic sperm injection with epididymal and testicular spermatozoa
 andrologia 35, 220 226 (2003) Accepted: April 25, 2003 Male factors determining the outcome of intracytoplasmic sperm injection with epididymal and testicular spermatozoa J. U. Schwarzer, K. Fiedler, I.
andrologia 35, 220 226 (2003) Accepted: April 25, 2003 Male factors determining the outcome of intracytoplasmic sperm injection with epididymal and testicular spermatozoa J. U. Schwarzer, K. Fiedler, I.
Novel Technologies for Selecting the Best Sperm for IVF and ICSI
 Novel Technologies for Selecting the Best Sperm for IVF and ICSI Denny Sakkas, Ph.D. Scientific Director, Boston IVF Waltham, MA, USA Testing The Sperm Population NOW Sperm DNA testing Although we are
Novel Technologies for Selecting the Best Sperm for IVF and ICSI Denny Sakkas, Ph.D. Scientific Director, Boston IVF Waltham, MA, USA Testing The Sperm Population NOW Sperm DNA testing Although we are
LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM
 LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM Slide #101 (1096). Testis, rat. sustentacular ( Sertoli ) cells Nuclei of Sustentacular cells Leydig cells Spermatogonia Spermatocytes Spermatids pale
LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM Slide #101 (1096). Testis, rat. sustentacular ( Sertoli ) cells Nuclei of Sustentacular cells Leydig cells Spermatogonia Spermatocytes Spermatids pale
Morphogenesis of the residual body of the mouse testis
 93 Morphogenesis of the residual body of the mouse testis By CASIMIR F. FIRLIT and JOSEPH R. DAVIS (From the Department of Pharmacology and Therapeutics, Stritch School of Medicine, and Graduate School,
93 Morphogenesis of the residual body of the mouse testis By CASIMIR F. FIRLIT and JOSEPH R. DAVIS (From the Department of Pharmacology and Therapeutics, Stritch School of Medicine, and Graduate School,
Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility
 Article ID: WMC001510 ISSN 2046-1690 Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility Author(s):Dr. Geetika, Dr. Sunita
Article ID: WMC001510 ISSN 2046-1690 Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility Author(s):Dr. Geetika, Dr. Sunita
A comparison between open and percutaneous needle biopsies in men with azoospermia
 Human Reproduction vol.13 no.5 pp.1266 1271, 1998 A comparison between open and percutaneous needle biopsies in men with azoospermia B.Rosenlund 1,6, U.Kvist 3, L.Plöen 4, B.Lundh Rozell 2, P.Sjöblom 1
Human Reproduction vol.13 no.5 pp.1266 1271, 1998 A comparison between open and percutaneous needle biopsies in men with azoospermia B.Rosenlund 1,6, U.Kvist 3, L.Plöen 4, B.Lundh Rozell 2, P.Sjöblom 1
DAX1, testes development role 7, 8 DFFRY, spermatogenesis role 49 DMRT genes, male sex differentiation role 15
 Subject Index N-Acetylcysteine, sperm quality effects 71 Ambiguous genitalia, origins 1, 2 Anti-Müllerian hormone function 13 receptors 13 Sertoli cell secretion 10, 38 Apoptosis assays in testes 73, 74
Subject Index N-Acetylcysteine, sperm quality effects 71 Ambiguous genitalia, origins 1, 2 Anti-Müllerian hormone function 13 receptors 13 Sertoli cell secretion 10, 38 Apoptosis assays in testes 73, 74
AZOOSPERMIA CYTOLOGICAL MANIFESTATIONS
 ý Comptes rendus de l Académie bulgare des Sciences ÌÓÑ ÆÓ ¾¼½½ BIOLOGIE Morphologie AZOOSPERMIA CYTOLOGICAL MANIFESTATIONS Stefka Ivanova, Petia Tzvetkova (Submitted by Corresponding Member J. Jordanov
ý Comptes rendus de l Académie bulgare des Sciences ÌÓÑ ÆÓ ¾¼½½ BIOLOGIE Morphologie AZOOSPERMIA CYTOLOGICAL MANIFESTATIONS Stefka Ivanova, Petia Tzvetkova (Submitted by Corresponding Member J. Jordanov
UroToday International Journal. Volume 2 - February 2009
 UroToday International Journal www.urotodayinternationaljournal.com Volume 2 - February 2009 Azoospermic Patients: Mosaic Pattern in Testicular Sperm Extraction Mai Ahmed Banakhar, Hassan A. Farsi, Suha
UroToday International Journal www.urotodayinternationaljournal.com Volume 2 - February 2009 Azoospermic Patients: Mosaic Pattern in Testicular Sperm Extraction Mai Ahmed Banakhar, Hassan A. Farsi, Suha
THE EFFECTS OF LIGATION OF CAUDA EPIDIDYMIDIS ON THE DOG TESTIS
 Copyright 1974 The American Fertility Society FERTILITY AND STERILITY Vol. 25, No.3, March, 1974 Printed in U.S.A. THE EFFECTS OF LIGATION OF CAUDA EPIDIDYMIDIS ON THE DOG TESTIS A. M. VARE, M.B.B.S.,
Copyright 1974 The American Fertility Society FERTILITY AND STERILITY Vol. 25, No.3, March, 1974 Printed in U.S.A. THE EFFECTS OF LIGATION OF CAUDA EPIDIDYMIDIS ON THE DOG TESTIS A. M. VARE, M.B.B.S.,
Pathology of Male Reproductive System 1
 Pathology of Male Reproductive System 1 Professor dr Ali Hassan Altimimi Professor of Pathology& Histology MSc, PHD, MD(UK) MALE REPRODUCTIVE SYSTEM The internal male genitalia consist of the testes with
Pathology of Male Reproductive System 1 Professor dr Ali Hassan Altimimi Professor of Pathology& Histology MSc, PHD, MD(UK) MALE REPRODUCTIVE SYSTEM The internal male genitalia consist of the testes with
A COMPARATIVE STUDY OF GERM CELL KINETICS IN THE TESTES OF CHILDREN WITH UNILATERAL CRYPTORCHIDISM: A PRELIMINARY REPORT*
 FERTILITY AND STERILITY Copyright 1970 by the Williams & Wilkins Co. Vol. 21, No. 11, November 1970 Printed in U.S.A. A COMPARATIVE STUDY OF GERM CELL KINETICS IN THE TESTES OF CHILDREN WITH UNILATERAL
FERTILITY AND STERILITY Copyright 1970 by the Williams & Wilkins Co. Vol. 21, No. 11, November 1970 Printed in U.S.A. A COMPARATIVE STUDY OF GERM CELL KINETICS IN THE TESTES OF CHILDREN WITH UNILATERAL
Predictive Factors of Successful Microdissection Testicular Sperm Extraction in Patients with Presumed Sertoli Cell-Only Syndrome
 Original Article Predictive Factors of Successful Microdissection Testicular Sperm Extraction in Patients with Presumed Sertoli Cell-Only Syndrome Tahereh Modarresi, M.Sc. 1, Hani Hosseinifar, M.Sc. 1,
Original Article Predictive Factors of Successful Microdissection Testicular Sperm Extraction in Patients with Presumed Sertoli Cell-Only Syndrome Tahereh Modarresi, M.Sc. 1, Hani Hosseinifar, M.Sc. 1,
Cell Divisions. The autosomes represent the whole body. * Male Sex Chromosomes: XY * Female Sex Chromosomes: XX
 Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
MALE REPRODUCTIVE SYSTEM
 1 MALE REPRODUCTIVE SYSTEM SCPA 602 Anatomical Basis for Pathological Study Updated: 20.09.2018 Lect. Nisamanee Charoenchon, PhD nisamanee.cha@mahidol.ac.th Department of Pathobiology, Mahidol University
1 MALE REPRODUCTIVE SYSTEM SCPA 602 Anatomical Basis for Pathological Study Updated: 20.09.2018 Lect. Nisamanee Charoenchon, PhD nisamanee.cha@mahidol.ac.th Department of Pathobiology, Mahidol University
U.I.O.Ezeh 1, H.D.M.Moore 1,2,3 and I.D.Cooke 1
 Human Reproduction vol.13 no.11 pp.3066 3074, 1998 Correlation of testicular sperm extraction with morphological, biophysical and endocrine profiles in men with azoospermia due to primary gonadal failure
Human Reproduction vol.13 no.11 pp.3066 3074, 1998 Correlation of testicular sperm extraction with morphological, biophysical and endocrine profiles in men with azoospermia due to primary gonadal failure
THE EFFECTS OF REPEATED INJECTIONS OF CHORIONIC GONADOTROPIN ON THE TESTES OF THE LEOPARD FROG (RANA PIPIENS SCHREBER)
 THE EFFECTS OF REPEATED INJECTIONS OF CHORIONIC GONADOTROPIN ON THE TESTES OF THE LEOPARD FROG (RANA PIPIENS SCHREBER) ROBERT P. McCOURT Department of Zoology and Entomology, The Ohio State University,
THE EFFECTS OF REPEATED INJECTIONS OF CHORIONIC GONADOTROPIN ON THE TESTES OF THE LEOPARD FROG (RANA PIPIENS SCHREBER) ROBERT P. McCOURT Department of Zoology and Entomology, The Ohio State University,
Evaluation of antifertility efficacy of Carica papaya seed extract through histological indices in Male Albino Rats
 International Journal of Chemical and Pharmaceutical Sciences 2013, Sep., Vol. 4 (3) ISSN: 0976-9390 IJCPS Evaluation of antifertility efficacy of Carica papaya seed extract through histological indices
International Journal of Chemical and Pharmaceutical Sciences 2013, Sep., Vol. 4 (3) ISSN: 0976-9390 IJCPS Evaluation of antifertility efficacy of Carica papaya seed extract through histological indices
ABNORMAL SPERMATOGENESIS IN XYY MALES: A REPORT ON 4 CASES ASCERTAINED THROUGH A POPULATION STUDY*
 FERTILITY AND STERILITY Copyright 1973 by The Williams & Wilkins Co. Vol. 24, No.5, May 1973 Printed in U.S.A. ABNORMAL SPERMATOGENESIS IN XYY MALES: A REPORT ON 4 CASES ASCERTAINED THROUGH A POPULATION
FERTILITY AND STERILITY Copyright 1973 by The Williams & Wilkins Co. Vol. 24, No.5, May 1973 Printed in U.S.A. ABNORMAL SPERMATOGENESIS IN XYY MALES: A REPORT ON 4 CASES ASCERTAINED THROUGH A POPULATION
Microscopic Anatomy of Inferior Medullary Velum Of Cerebellum
 32 J Anat. Soc. India 51(1) 32-34 (2002) Microscopic Anatomy of Of Cerebellum Arora, N.K. Department of Anatomy, Government Medical College, Chandigarh INDIA. Abstract. A study of the inferior medullary
32 J Anat. Soc. India 51(1) 32-34 (2002) Microscopic Anatomy of Of Cerebellum Arora, N.K. Department of Anatomy, Government Medical College, Chandigarh INDIA. Abstract. A study of the inferior medullary
Cycle of the Seminiferous Epithelium of the Guinea Pig
 Cycle of the Seminiferous Epithelium of the Guinea Pig A Method for Identification of the Stages Yves Clermont, Ph.D. IN THE GUINEA PIG, the cells of the seminiferous epithelium are arranged in definite
Cycle of the Seminiferous Epithelium of the Guinea Pig A Method for Identification of the Stages Yves Clermont, Ph.D. IN THE GUINEA PIG, the cells of the seminiferous epithelium are arranged in definite
Male reproduction. Cross section of Human Testis ผศ.ดร.พญ.ส ว ฒณ ค ปต ว ฒ ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล 1. Aims
 Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE
 ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
With advances in assisted reproduction techniques,
 Journal of Andrology, Vol. 26, No. 6, November/December 2005 Copyright American Society of Andrology Clomiphene Administration for Cases of Nonobstructive Azoospermia: A Multicenter Study ALAYMAN HUSSEIN,*
Journal of Andrology, Vol. 26, No. 6, November/December 2005 Copyright American Society of Andrology Clomiphene Administration for Cases of Nonobstructive Azoospermia: A Multicenter Study ALAYMAN HUSSEIN,*
Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia
 Urology Journal UNRC/IUA Vol. 3, No. 2, 92-96 Spring 2006 Printed in IRAN Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia Seyed Amirmohsen Ziaee, 1 * Mohammadreza Ezzatnegad,
Urology Journal UNRC/IUA Vol. 3, No. 2, 92-96 Spring 2006 Printed in IRAN Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia Seyed Amirmohsen Ziaee, 1 * Mohammadreza Ezzatnegad,
Microdissection testicular sperm extraction causes spermatogenic alterations in the contralateral testis
 causes spermatogenic alterations in the contralateral testis A.B. Oliveira Filho 1, R.S. Souza 2, M.T.V. Azeredo-Oliveira 2, R.L. Peruquetti 2 and A.P. Cedenho 1 1 Departamento de Cirurgia, Divisão de
causes spermatogenic alterations in the contralateral testis A.B. Oliveira Filho 1, R.S. Souza 2, M.T.V. Azeredo-Oliveira 2, R.L. Peruquetti 2 and A.P. Cedenho 1 1 Departamento de Cirurgia, Divisão de
TESTICULAR FINE NEEDLE ASPIRATION CYTOLOGY AND HISTOPATHOLOGY CORRELATION IN MALE INFERTILITY
 TESTICULAR FINE NEEDLE ASPIRATION CYTOLOGY AND HISTOPATHOLOGY CORRELATION IN MALE INFERTILITY Dissertation submitted in partial fulfillment of the requirements for the degree of M.D. (Pathology) Branch
TESTICULAR FINE NEEDLE ASPIRATION CYTOLOGY AND HISTOPATHOLOGY CORRELATION IN MALE INFERTILITY Dissertation submitted in partial fulfillment of the requirements for the degree of M.D. (Pathology) Branch
Histological evaluation of the human testis approaches to optimizing the clinical value of the assessment: Mini Review
 Human Reproduction Vol.22, No.1 pp. 2 16, 2007 Advance Access publication August 3, 2006. doi:10.1093/humrep/del279 Histological evaluation of the human testis approaches to optimizing the clinical value
Human Reproduction Vol.22, No.1 pp. 2 16, 2007 Advance Access publication August 3, 2006. doi:10.1093/humrep/del279 Histological evaluation of the human testis approaches to optimizing the clinical value
Immune response in obstructive male infertility. Prof. A.K.Sarda Department of Surgery Maulana Azad Medical College New Delhi
 Immune response in obstructive male infertility Prof. A.K.Sarda Department of Surgery Maulana Azad Medical College New Delhi Sperm transport from the testicle Seminiferous tubule contractions of the myoid
Immune response in obstructive male infertility Prof. A.K.Sarda Department of Surgery Maulana Azad Medical College New Delhi Sperm transport from the testicle Seminiferous tubule contractions of the myoid
Outcome of first and repeated testicular sperm extraction and ICSI in patients with non-obstructive azoospermia
 Human Reproduction Vol.17, No.9 pp. 2356 2361, 2002 Outcome of first and repeated testicular sperm extraction and ICSI in patients with non-obstructive azoospermia S.Friedler 1, A.Raziel, M.Schachter,
Human Reproduction Vol.17, No.9 pp. 2356 2361, 2002 Outcome of first and repeated testicular sperm extraction and ICSI in patients with non-obstructive azoospermia S.Friedler 1, A.Raziel, M.Schachter,
Differentiation of Renal Tubular Epithelium in Renal Transplantation Cytology
 Differentiation of Renal Tubular Epithelium in Renal Transplantation Cytology G. BERRY SCHUMANN, M.D., LAWRENCE J. PALMIERI, B.S., C.T.(ASCP), AND DAVID B. JONES, M.D. Schumann, G. Berry, Palmieri, Lawrence
Differentiation of Renal Tubular Epithelium in Renal Transplantation Cytology G. BERRY SCHUMANN, M.D., LAWRENCE J. PALMIERI, B.S., C.T.(ASCP), AND DAVID B. JONES, M.D. Schumann, G. Berry, Palmieri, Lawrence
Testicular Biopsy in Males With Infertility: A Longitudinal Study
 Short Communication Iran J Pathol. 2017; 12(2): 177-182 Iranian Journal of Pathology ISSN: 2345-3656 Testicular Biopsy in Males With Infertility: A Longitudinal Study Sepideh Siadati 1*, Hamid Shafi 2,
Short Communication Iran J Pathol. 2017; 12(2): 177-182 Iranian Journal of Pathology ISSN: 2345-3656 Testicular Biopsy in Males With Infertility: A Longitudinal Study Sepideh Siadati 1*, Hamid Shafi 2,
BIOL 2402 Reproductive Systems
 Collin College Dr. Chris Doumen BIOL 2402 Reproductive Systems 1 Reproductive System Most systems between males and females in the human body are similar in structure. The exception of course are the organs
Collin College Dr. Chris Doumen BIOL 2402 Reproductive Systems 1 Reproductive System Most systems between males and females in the human body are similar in structure. The exception of course are the organs
Testicular histology and gonadotropin levels in infertile men with non-obstructive oligo-/azoospermia
 1 THE NATIONAL MEDICAL JOURNAL OF INDIA VOL., NO.5 Testicular histology and gonadotropin levels in infertile men with non-obstructive oligo-/azoospermia ARUN KUMAR, B. JAYAKUMAR, M. L. KHURANA, VED PRAKASH,
1 THE NATIONAL MEDICAL JOURNAL OF INDIA VOL., NO.5 Testicular histology and gonadotropin levels in infertile men with non-obstructive oligo-/azoospermia ARUN KUMAR, B. JAYAKUMAR, M. L. KHURANA, VED PRAKASH,
Bank your future: Insemination and semen cryopreservation. Disclosure. Lecture objectives
 Bank your future: Insemination and semen cryopreservation Roelof Menkveld, PhD Andrology Laboratory, Department of Obstetrics and Gynaecology, Tygerberg Academic Hospital and University of Stellenbosch.
Bank your future: Insemination and semen cryopreservation Roelof Menkveld, PhD Andrology Laboratory, Department of Obstetrics and Gynaecology, Tygerberg Academic Hospital and University of Stellenbosch.
Animal Development. Lecture 3. Germ Cells and Sex
 Animal Development Lecture 3 Germ Cells and Sex 1 The ovary of sow. The ovary of mare. The ovary of cow. The ovary of ewe. 2 3 The ovary. A generalized vertebrate ovary. (Wilt and Hake, Ch 2, 2004) 4 The
Animal Development Lecture 3 Germ Cells and Sex 1 The ovary of sow. The ovary of mare. The ovary of cow. The ovary of ewe. 2 3 The ovary. A generalized vertebrate ovary. (Wilt and Hake, Ch 2, 2004) 4 The
For more information about how to cite these materials visit
 Author: A. Kent Christensen, Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike 3.0 License: http://creativecommons.org/licenses/by-sa/3.0/
Author: A. Kent Christensen, Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike 3.0 License: http://creativecommons.org/licenses/by-sa/3.0/
Physiologic Anatomy of the Male Sexual Organs
 Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin
 Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin A Preliminary Report S. J. GLASS, M.D., and H. M. HOLLAND, M.D. BEFORE discussing gonadotropic therapy of oligospermia, it is
Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin A Preliminary Report S. J. GLASS, M.D., and H. M. HOLLAND, M.D. BEFORE discussing gonadotropic therapy of oligospermia, it is
Occurrence of polyovular follicles and its possible significance in the ovary of the bat, Scotophilus heathi
 Biol Res 31: 75-80 (1998) Occurrence of polyovular follicles and its possible significance in the ovary of the bat, Scotophilus heathi UP SINGH, J DOVAL and A KRISHNA* Department of Zoology, Bañaras Hindu
Biol Res 31: 75-80 (1998) Occurrence of polyovular follicles and its possible significance in the ovary of the bat, Scotophilus heathi UP SINGH, J DOVAL and A KRISHNA* Department of Zoology, Bañaras Hindu
The Male Reproductive System
 The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
Microscopic Anatomy of Sertoli and Leydig Cells During Fetal Development in Baladi Rabbit
 International Journal of Animal Science and Technology 2018; 2(1): 1-5 http://www.sciencepublishinggroup.com/j/ijast doi: 10.11648/j.ijast.20180201.11 Microscopic Anatomy of Sertoli and Leydig Cells During
International Journal of Animal Science and Technology 2018; 2(1): 1-5 http://www.sciencepublishinggroup.com/j/ijast doi: 10.11648/j.ijast.20180201.11 Microscopic Anatomy of Sertoli and Leydig Cells During
ROLE OF SOME ANTIOXIDANTS ON MERCURY CHLORIDE INDUCED SPERMATOGENESIS IN SWISS ALBINO MICE DURING PRE PUBERTAL PHASE OF LIFE
 Indian J.Sci.Res.1(2) : 19-25, 2010 ROLE OF SOME ANTIOXIDANTS ON MERCURY CHLORIDE INDUCED SPERMATOGENESIS IN SWISS ALBINO MICE DURING PRE PUBERTAL PHASE OF LIFE a1 DUGESH NANDINI SHARMA AND LATA BHATTACHARYA
Indian J.Sci.Res.1(2) : 19-25, 2010 ROLE OF SOME ANTIOXIDANTS ON MERCURY CHLORIDE INDUCED SPERMATOGENESIS IN SWISS ALBINO MICE DURING PRE PUBERTAL PHASE OF LIFE a1 DUGESH NANDINI SHARMA AND LATA BHATTACHARYA
Sperm recovery and IVF outcome after surgical sperm retrieval in azoospermia: our experience
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Rai S et al. Int J Reprod Contracept Obstet Gynecol. 2018 Feb;7(2):xxx-xxx www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20180019
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Rai S et al. Int J Reprod Contracept Obstet Gynecol. 2018 Feb;7(2):xxx-xxx www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20180019
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Multiple testicular sampling in non-obstructive azoospermia is it necessary?
 Human Reproduction vol.13 no.11 pp.3081 3085, 1998 Multiple testicular sampling in non-obstructive azoospermia is it necessary? R.Hauser 1,3, A.Botchan 1, A.Amit 2, D.Ben Yosef 2, R.Gamzu 1, G.Paz 1, J.B.Lessing
Human Reproduction vol.13 no.11 pp.3081 3085, 1998 Multiple testicular sampling in non-obstructive azoospermia is it necessary? R.Hauser 1,3, A.Botchan 1, A.Amit 2, D.Ben Yosef 2, R.Gamzu 1, G.Paz 1, J.B.Lessing
Genetics Aspects of Male infertility
 Genetics Aspects of Male infertility A. Ebrahimi, Molecular Genetic SM Kalantar, Prof. Molecular Cytogenetic Research & Clinical Centre for Infertility, Reproductive & Genetic Unit, Yazd Medical Sciences
Genetics Aspects of Male infertility A. Ebrahimi, Molecular Genetic SM Kalantar, Prof. Molecular Cytogenetic Research & Clinical Centre for Infertility, Reproductive & Genetic Unit, Yazd Medical Sciences
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Male Anatomy. testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics
 Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
IN THE STUDY of male fertility and infertility there are several criteria which
 Cytologic Examination of Semen Irwin N. Frank, A.B., John A. Benjamin, M.D., and James E. Segerson, M.D. IN THE STUDY of male fertility and infertility there are several criteria which have been established
Cytologic Examination of Semen Irwin N. Frank, A.B., John A. Benjamin, M.D., and James E. Segerson, M.D. IN THE STUDY of male fertility and infertility there are several criteria which have been established
川北医学院讲稿. Under low power note the testis is enclosed by a strong fibrous. layer of serous epithelium. These fibrous tissue
 川北医学院讲稿 Experiment 5: Male and Female Reproductive System Hello, everybody, class is begin,keep quiet, please. And this is the last experimental class. Today we will learn 5 slices and review all structures
川北医学院讲稿 Experiment 5: Male and Female Reproductive System Hello, everybody, class is begin,keep quiet, please. And this is the last experimental class. Today we will learn 5 slices and review all structures
II.3.9 Evaluation of Testicular Biopsy Samples from the Clinical Perspective
 454 Diagnostic Tools.9 Evaluation of Testicular Biopsy Samples from the Clinical Perspective M. Bergmann Summary Testicular biopsy is indicated therapeutically in cases of obstructive azoospermia, and
454 Diagnostic Tools.9 Evaluation of Testicular Biopsy Samples from the Clinical Perspective M. Bergmann Summary Testicular biopsy is indicated therapeutically in cases of obstructive azoospermia, and
Primary sex organs (gonads): testes and ovaries. Accessory reproductive organs: ducts, glands, and external genitalia
 Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Sperm retrieval from patients with nonmosaic Klinefelter s syndrome by semen cytology examination
 Sperm retrieval from patients with nonmosaic Klinefelter s syndrome by semen cytology examination Y.-T. Jiang 1, Y. Dong 1, X.-W. Yu 1, R.-C. Du 1,2, L.-L. Li 1,2, H.-G. Zhang 1 and R.-Z. Liu 1 1 Center
Sperm retrieval from patients with nonmosaic Klinefelter s syndrome by semen cytology examination Y.-T. Jiang 1, Y. Dong 1, X.-W. Yu 1, R.-C. Du 1,2, L.-L. Li 1,2, H.-G. Zhang 1 and R.-Z. Liu 1 1 Center
Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update
 Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update Fábio Firmbach Pasqualotto, M.D., Ph.D., Bernardo Passos Sobreiro, M.D., Jorge Hallak, M.D., Ph.D., Eleonora Bedin
Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update Fábio Firmbach Pasqualotto, M.D., Ph.D., Bernardo Passos Sobreiro, M.D., Jorge Hallak, M.D., Ph.D., Eleonora Bedin
Postgraduate Training in Reproductive Health
 SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
18 Urinary system. 19 Male reproductive system. Female reproductive system. Blok 11: Genital and Urinary Tract Diseases
 Blok 11: Genital and Urinary Tract Diseases 18 Urinary System 19 Male Genital System 20 Female Genital System 18 Urinary system You should be able to: 1. Describe the structures and associated functions
Blok 11: Genital and Urinary Tract Diseases 18 Urinary System 19 Male Genital System 20 Female Genital System 18 Urinary system You should be able to: 1. Describe the structures and associated functions
Inhibin B plasma concentrations in oligozoospermic subjects before and after therapy with follicle stimulating hormone
 Human Reproduction vol.14 no.4 pp.906 912, 1999 Inhibin B plasma concentrations in oligozoospermic subjects before and after therapy with follicle stimulating hormone Carlo Foresta 1,4, Andrea Bettella
Human Reproduction vol.14 no.4 pp.906 912, 1999 Inhibin B plasma concentrations in oligozoospermic subjects before and after therapy with follicle stimulating hormone Carlo Foresta 1,4, Andrea Bettella
A study on correlation between bleeding pattern and histopathological findings of endometrium among perimenopausal women
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Nair R et al. Int J Reprod Contracept Obstet Gynecol. 25 Dec;4(6):1758-1762 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Nair R et al. Int J Reprod Contracept Obstet Gynecol. 25 Dec;4(6):1758-1762 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
15% ART accounts for ~4% of Australian births
 The General Practice Education Day HealthEd / Generation Next 20 th February Sydney Declarations Male Infertility & Assisted Reproduction Prof Robert I McLachlan FRACP, Ph.D. Consultant Andrologist, Monash
The General Practice Education Day HealthEd / Generation Next 20 th February Sydney Declarations Male Infertility & Assisted Reproduction Prof Robert I McLachlan FRACP, Ph.D. Consultant Andrologist, Monash
15% ART accounts for ~4% of Australian births
 The General Practice Education Day HealthEd / Generation Next 5 th March Melbourne Declarations Male Infertility & Assisted Reproduction Prof Robert I McLachlan FRACP, Ph.D. Consultant Andrologist, Monash
The General Practice Education Day HealthEd / Generation Next 5 th March Melbourne Declarations Male Infertility & Assisted Reproduction Prof Robert I McLachlan FRACP, Ph.D. Consultant Andrologist, Monash
describe the parts and function of semen and the glands that contribute to it
 You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
Intratubular Germ Cell Neoplasia of the Testis
 Intratubular Germ Cell Neoplasia of the Testis KS Ngoo Department of Urology Hospital Selayang Advanced Urology Course 15 Aug 2014 MUA Office Clinical scenario A 33 years old man has bilateral testicular
Intratubular Germ Cell Neoplasia of the Testis KS Ngoo Department of Urology Hospital Selayang Advanced Urology Course 15 Aug 2014 MUA Office Clinical scenario A 33 years old man has bilateral testicular
ANATOMY. lecture # : 2 1 Date : Lecturer : Maher Hadidi
 ANATOMY lecture # : 2 1 Date : Lecturer : Maher Hadidi Spermatogenesis Transformation of Spermatogonia into mature sperm that begins at puberty into old age. Provide motility of the sperm...-c:tail to
ANATOMY lecture # : 2 1 Date : Lecturer : Maher Hadidi Spermatogenesis Transformation of Spermatogonia into mature sperm that begins at puberty into old age. Provide motility of the sperm...-c:tail to
Lab #9: Kidney: Gross Anatomy & Histology
 Name Date Lab #9: Kidney: Gross Anatomy & Histology Lab #10: Male Reproductive System: Human Models & Histology Lab #11: Female Reproductive System: Human Models & Histology Stuff to Know Dr. L. Bacha
Name Date Lab #9: Kidney: Gross Anatomy & Histology Lab #10: Male Reproductive System: Human Models & Histology Lab #11: Female Reproductive System: Human Models & Histology Stuff to Know Dr. L. Bacha
Gametogenesis. Dr Corinne de Vantéry Arrighi Dr Hervé Lucas
 WHO Collaborating Center for Research in Human Reproduction Clinic for Infertility and Gynecological Endocrinology University Hospital, Geneva, Switzerland Gametogenesis Dr Corinne de Vantéry Arrighi Dr
WHO Collaborating Center for Research in Human Reproduction Clinic for Infertility and Gynecological Endocrinology University Hospital, Geneva, Switzerland Gametogenesis Dr Corinne de Vantéry Arrighi Dr
HISTOLOGY OF THE MALE REPRODUCTIVE SYSTEM
 HISTOLOGY OF THE MALE REPRODUCTIVE SYSTEM Learning Objectives: 1. Describe the histology of and identify, in order, the passageways through which sperm pass as they exit from the body. 2. Describe the
HISTOLOGY OF THE MALE REPRODUCTIVE SYSTEM Learning Objectives: 1. Describe the histology of and identify, in order, the passageways through which sperm pass as they exit from the body. 2. Describe the
