Effects of Infertility Insurance Mandates on Fertility
|
|
|
- Godfrey Fletcher
- 5 years ago
- Views:
Transcription
1 Preliminary & Incomplete Do Not Cite Comments Appreciated Effects of Infertility Insurance Mandates on Fertility Lucie Schmidt Department of Economics Williams College June 2004 Alex Bal, Julia Brown, and Katherine McGrath provided excellent research assistance. I am grateful to Purvi Sevak and Lara Shore-Sheppard for useful conversations and comments. All errors or omissions are my own. Contact information: Department of Economics, Fernald House, Williams College, Williamstown, MA 01267, lschmidt@williams.edu.
2 I. Introduction Infertility is a disease that imposes health-related and financial costs on women and families. It currently affects over 6 million individuals, and one in ten couples cannot conceive without medical assistance. However, only 25 percent of all health plan sponsors provide any coverage for infertility services. In response to the perceived need for coverage, legislation was introduced at the federal level in 2003 that would require health plans to provide infertility benefits. 1 As the fraction of the population affected by infertility continues to rise, there are likely to be continued efforts to legislate mandated coverage. Understanding the implications of coverage expansion thus becomes increasingly important. As of 2003, fifteen states have enacted some form of infertility insurance mandate. The experiences of these states provide useful information on how expanding coverage affects access to services and birthrates, as well as on how the costs of coverage are distributed across individuals and society. My goal in this paper is to improve our understanding of the benefit of mandated infertility insurance coverage by examining the impact of state mandates on birth rates. I use fertility rates by age cohort, race and state generated from Vital Statistics Detail Natality Data and Census Population estimates to examine whether these mandates were successful in increasing fertility rates among those women most likely to be affected. Using a difference-indifferences approach, I exploit variation in the enactment of mandates both across states and over time, and identify control groups that should not have been affected by infertility coverage. My results suggest that the mandates have been successful in increasing the number of women who are able to give birth. 1 The Family Building Act of 2003 (HR 3014) would require insurance coverage of infertility treatment (including up to four IVF attempts) by all group health plans that also require obstetrical benefits. 1
3 II. Background Information Infertility is considered by medical organizations to be a disease of the reproductive system (American Society of Reproductive Medicine (ASRM), 2003). As such, it imposes costs on women and families that are both health-related and economic. In this section, I discuss the incidence of infertility, the costs associated with it, and insurance coverage of treatment. A. Incidence of Infertility/Impaired Fecundity There are a variety of problems associated with defining infertility as well as with obtaining standardized measures of its incidence that can be followed over time. (Chandra et al, 2003). Demographers using the National Survey of Family Growth have used two criteria to classify whether women are having difficulties in childbearing. Infertility only applies to married or cohabiting women, and is defined as the condition of being unable to conceive after 12 or more consecutive months of unprotected intercourse. Impaired fecundity (IF), however, applies to women of any marital or cohabiting status, and is defined as having problems with conceiving or carrying a pregnancy to term, as well as being unable to conceive after 3 years of unprotected intercourse (Chandra and Stephen, 1998). 2 However, the ASRM does not, in official documents, make this distinction. For simplicity, I refer to impaired fecundity and infertility interchangeably. Overall, the proportion of women reporting IF has risen only 2 percentage points between 1982 and 1995, from 8% to 10%. However, due to increasing numbers of women between the ages of 15-44, there has actually been a fairly dramatic increase in the number of women reporting infecundity, from 4.6 million to 6.2 million. This increase has occurred across almost all subgroups of women, including along the dimensions of marital status, income, education, 2 Both conditions only apply to those women who are not surgically sterile. 2
4 race, and ethnicity (Chandra and Stephen, 1998). Because of this, the population of fertility impaired women is similar to the general population of women, except that they are older -- 43% are aged 35-44, as compared with 36% of the general population (Stephen and Chandra, 2000) Like other diseases, infertility imposes large physical and psychological costs on individuals and families. The psychological effects of infertility have been compared to the effects of other diseases such as cancer and heart disease (Fidler and Bernstein, 1999). In addition to the physical nature of the disease of infertility, and the psychological costs of the disease, there are also nonnegligable financial costs. Most instances of impaired fecundity are treated by conventional methods, such as drug treatment or surgical repair of reproductive organs. Some of the less invasive therapies such as hormone therapy can range from $200- $3,000 per cycle. Tubal surgery can range from $10,000-$15,000, requires a hospital stay and poses a high risk of complication (Resolve, 2003). Assisted Reproductive Technology (ART) refers to all fertility treatments in which both eggs and sperm are handled. The most common type of ART is in vitro fertilization (IVF), which comprises approximately five percent of all infertility treatments, and the average cost of an IVF cycle in the United States is $12,400 (ASRM, 2003). Despite the large and growing share of the population that faces infertility problems, and despite the large financial costs of treatment, health care coverage of treatment is limited. Nationwide, only 25% of health care plans cover infertility treatment, and coverage varies significantly by state. 3 Of the 6.2 million women with impaired fecundity in 1995, 2.7 million (44%) had ever sought treatment. Of that group, 700,000 women had sought treatment within the past year. However, as a result of the high (and often uninsured) costs associated with 3 As a comparison, in % of covered workers had coverage for oral contraceptives (Kaiser Foundation, 2002), and a study of health plans found that 57% covered colonoscopy (Klabunde et al, 2004). 3
5 treatment, medical assistance for infertility is sought primarily by women and couples that are white, college-educated, and affluent. Women with private health insurance coverage were 50% more likely to have received services, as were women with income more than 300% of the poverty line (Stephen and Chandra, 2000). This is the case even though increases in infertility over time have occurred across all race, ethnicity, income, and education groups (see Chandra and Stephen (1998) and Stephen and Chandra (2000)). It is widely believed that there is an unmet need for infertility services, especially among those with lower incomes and lower levels of education (Chandra & Mosher 1994). B. State Mandates The first state-level infertility insurance mandate was enacted by West Virginia in Since that time, fourteen other states have passed mandates, and additional states have ongoing legislative advocacy efforts in this area. State mandates fall into one of two categories. A mandate to cover requires that health insurance companies provide coverage of infertility treatment as a benefit included in every policy. A mandate to offer requires that health insurance companies make available for purchase a policy which offers coverage of infertility treatment. In addition, some mandates exclude coverage of IVF, which is one of the most expensive treatments available for infertility. Table 1 provides a list of the states with mandates currently in place, the date the mandates were enacted, whether the provisions are mandates to offer or mandates to cover, and whether the mandates cover IVF. Detailed information on these mandates, including any further restrictions placed on coverage, can be found in Appendix A. Many mandates restrict treatment to individuals on the basis of marital status. In addition, several states also restrict treatment on the basis of age. As of 2000, these mandates only 4
6 affected thirteen states. However, as is illustrated in Table 2, a number of large states are affected. In 1985, less than one percent of all live births in the US occurred in mandate states. By 1990, 30% of births were in mandate states, and this percentage rose to 46% by Despite the increasing prevalence of infertility, the significant disparities in access to treatment, and the ongoing efforts to legislate coverage expansions, to date only a few studies have looked at the effects of these mandates. Jain et al. (2002) use clinic data from 1998 and find that states with required coverage for IVF have the highest rates of IVF utilization, and the lowest number of embryos transferred per cycle. 4 Reynolds et al. (2003) find that the states with mandated insurance coverage of IVF have lower numbers of embryos transferred than states without coverage, as well as a lower proportion of multiple births resulting from IVF. Hamilton and McManus (2004) develop a model of the market for ART and use data from clinics at the Metropolitan Statistical Area level to test the model s predictions. Using data from , they confirm the findings of Jain et al. (2002) and Reynolds et al. (2003) that a mandate increases IVF utilization rates and reduces the number of embryos transferred. They also find that clinics are attracted to areas where women are more educated and wealthier, but find no evidence that clinics are attracted to places where mandates are in effect. These three studies focus exclusively on IVF and ignore other types of fertility treatments that may be covered by the mandates. In addition, the studies are generally cross-sectional analyses that cannot control for unobservable differences in patients or clinics that may be state-specific. Finally, they all 4 Individuals with insurance coverage for IVF are thought to be likely to transplant fewer embryos in a given cycle, since the pressure for a successful procedure on the first try is lower. Fewer embryos leads to lower incidence of multiple births, which is important from a public health standpoint. 5
7 look at a period of time during which no changes in mandated coverage were legislated, so they cannot exploit variation within a state over time as the mandate is enacted. 5 In this paper, I use a difference-in-differences approach where I exploit variation in the enactment of mandates both across states and over time to determine whether these mandates have been successful in increasing birth rates for those women most likely to need infertility treatment. III. Data Information on births comes from Vital Statistics Detail Natality Data, gathered by the National Center for Health Statistics. This information is based on birth certificate data, and includes specific information about the timing, parity (whether it was a first or subsequent birth), and plurality (whether it was a single, twin, triplet, or higher order birth) of each birth. These data also include demographic information on the mother, including age, race, ethnicity, marital status, and educational attainment, and limited demographic information on the father. Geographic information about the mother's state of residence is also provided. Beginning in 1985 the data cover every birth in the United States. The count of births by state, year, race, and five-year age cohort are used to generate birth rates. 6 The denominators for birth rates must come from another data source, since the birth certificates only provide information on those women who actually give birth. Population estimates are available for black and non-black women by age and state from through 5 Bitler (2004) does not analyze the effects of the state mandates, but instead uses variation generated by those mandates between 1981 and 2000 to examine the effects of ART on infant health outcomes. She finds evidence that living in a state with a mandate, which is likely to improve access to ART, leads to a small but significant decrease in gestation, with larger effects for older women. 6 Five year cohorts are used up to the age of 44 (15-19, 20-24, 25-29, 30-34, 35-39, 40-44). Due to smaller numbers of births in older ages, births to women are grouped together. 6
8 the Census Bureau, and can be used to calculate birth rates. However, they do not allow for further breakouts. For example, birth counts by parity or by marital status of the mother can be calculated, but denominators with counts of women by the number of children they have already borne cannot be generated. Other control variables, collected by state and by year, come from a variety of publicly available sources. State level unemployment rates and female labor force participation rates are published by the Bureau of Labor Statistics. Data on the distribution of usual weekly earnings (median and tenth percentile) have been generated from the CPS Outgoing Rotation Group Data. Data on abortion policies (e.g. whether Medicaid funds abortions in the state; whether parental involvement is required for minors to obtain an abortion) have been collected from a variety of public sources. The maximum level of state welfare benefits available to a family of three come from various editions of the U.S. House of Representatives Green Book. 7 IV. Model Specification and Empirical Results As shown in Table 1, the mandates were enacted in different states in different years. I use a difference-in-differences approach where I am able to exploit variation in mandates both across states and over time, as well as identify control groups that should not have been affected by infertility coverage. Using birth rates generated from Vital Statistics Detail Natality data and Census population counts, I estimate the following model: 2 2 ln( fstbthrt) = α + βz + γmand + θ( Mand Over35) + ajt jt j( t k ) j( t k ) k= 1 k= 1 δ S + δt + ε j j j t t t i (1) 7 Summary statistics for the data set can be found in Appendix B, and a full description of the data used in the analysis can be found in Appendix C. 7
9 where the dependent variable is the log first birth rate for a given age cohort in state j and year t. The first birth rate is equal to the number of first births within an age cohort-race-state-year cell, divided by the number of women in that same age cohort-race-state-year cell. I focus on first birth rates, because treatments are more likely to be sought by women who have not already borne children. The Z vector controls for variables that will vary across states and over time that might also affect birth rates. 8 These include variables that reflect economic conditions, including the state unemployment rate, log median usual weekly earnings, log tenth percentile weekly usual earnings, and female labor force participation rates. Variables describing state-level abortion policies are also included, such as whether Medicaid funds abortions in the state, and whether parental involvement is required for minors to obtain an abortion. These policies have been found in previous research to affect birth rates (e.g. Blank, London, and George (1996); Levine, Trainor, and Zimmerman (1996); and Klerman (1999)). Finally, the Z vector also includes the log maximum level of state welfare benefits available to a family of three. 9 The specification also includes state fixed effects (S j ) to control for any time-invariant unobserved state characteristics that may influence age-specific birth rates, year fixed effects (T t ) to control for national trends in birth rates over time, and age effects. The error term is represented by ε. I calculate White robust standard errors clustered by state, as suggested by Bertrand et al (2002). 10 Regressions are weighted by the population counts in each cell. 11 The independent variable of interest is the policy variable Mand. This variable equals one if a state had either a mandate to cover or a mandate to offer infertility insurance. Mandates 8 I am grateful to Rebecca Blank for providing much of the state-level data. 9 These values are for the Aid to Families with Dependent Children program through 1996, and for the Temporary Assistance for Needy Families program from 1997 through Difference-in-differences estimation can lead to artifically low standard error estimates if the outcomes and the policy changes of interest are serially correlated. This approach corrects for this potential problem. 11 The results are robust to running unweighted regressions. 8
10 are allowed to affect fertility rates with a two-year lag structure, such that mandates in year t-1 and in year t-2 are allowed to affect fertility rates in year t. This is to account for two factors: 1) infertility treatments often do not result in an immediate conception; and 2) even if a conception occurs immediately, there is still a necessary nine-month waiting period before those new conceptions can affect fertility rates. If the mandates have been successful at increasing access to infertility treatments, and if these treatments have been successful, then the estimated coefficient on this variable is expected to be positive. However, it is possible that there exist systematic differences in first birth rates across states that are correlated with, but not caused by the state-level mandates. If this unobserved heterogeneity exists, one way to estimate the effects of the mandates accurately is to identify a treatment group for whom the mandates should have a direct effect, and a control group for whom they should not. This approach allows for estimation of the parameter of interest without bias. To this end, I use age cohort as a way of distinguishing a treatment group and a control group. The probability that a woman experiences infertility is extremely low for young women, and increases with age. Those women most likely to be affected by the mandates are those who have delayed childbearing, and specifically those women 35 and older. 12 As such, I interact the mandate with an identifier for whether the birth rates are for age cohorts 35 and older. The estimated coefficient γ will pick up any unobserved heterogeneity in birth rates that is correlated with the state mandates. The effect of the mandates on the treatment group of older women, θ, will then be estimated without bias. The use of the log first birth rate as the dependent variable 12 The age of 35 appears to be an important turning point in the risk of infertility problems. The government publication Infertility: Medical and Social Choices states that the probability of infertility increases somewhat after age 30 and significantly more after age 35. In addition, the American Society for Reproductive Medicine identifies 35 as a turning point. Their Patient s Fact Sheet on the Prediction of Fertility Potential in Older Female Patients states that approximately one-third of couples in which the female partner is age 35 or older will have problems with fertility. Finally, Resolve (the national support group for those faced with infertility) says Most physicians advise you not to be concerned unless you have been trying to conceive for at least one year and are under 35. If you are over 35 and have been trying for six months, you should consult a physician. 9
11 means that the estimated coefficient θ can be interpreted as the percentage change in the first birth rate of older women with respect to the implementation of a mandate. One potential concern with this approach is the possibility that women under 35 may be a contaminated control group. This could happen for two reasons that would affect results in opposing directions. First, the younger women might also be receiving infertility treatments. Alternatively, it is possible that younger women may be more likely to delay childbearing if they know infertility treatment is covered by their insurance. An alternative way to think of the methodological approach is to interpret γ as the estimated effect of the mandates on all women, and θ as the additional effect on older women. The estimate of γ would be positive if the first effect dominated, and negative if the second effect was larger. As another robustness check, I estimate all regressions omitting the portion of the control group most likely to be receiving infertility treatment those women All results presented below are robust to this alternate specification. Results from the estimation of equation (1) can be found in Column 1 of Table 3. The age pattern of births is nonlinear. Compared to the omitted category of women ages 15-19, women in their early twenties are the most likely to bear children. After age 25, first birth rates decline with age. The coefficient on black is negative and significant, suggesting that after controlling for a variety of other factors that affect birth rates, black women are less likely to have a first birth. The one year lag mandate variable has no significant effects. The two year lag, however, is significant at the one-percent level. The estimate of γ shows that in fact there is some correlation between birth rates and the mandates, as overall first birth rates in states with mandates are lower than those without. However, the interaction between the mandate and the 10
12 indicator for Over 35 is positive and strongly significant, suggesting that the presence of a mandate is associated with fertility rates for women over the age of 35 that are 42 percent higher than in states without mandates. One potential concern with these results is that first birth rates for older women have been increasing over time, as an increasing number of women delay their first births until older ages. 13 Since the mandates are also positively correlated with time, it is possible that the effect of the mandates on the treatment group may simply be picking up increases in birth rates among older women. To allow for this possibility, I re-estimate equation (1) controlling for a set of interactions between age cohort and year. The results from this regression are presented in Column 2 of Table 3. It is clear that the original estimates of the effects of mandates in Column 1 were spuriously picking up changes in age-specific trends. The estimate of γ becomes much smaller and is no longer statistically different from zero. The estimate of θ, the effect of the mandate on older women, falls in magnitude. However, there is still a positive significant effect of the mandates, suggesting that the mandates increased birth rates for women over the age of 35 by 18 percent. As an additional sensitivity test, I re-estimate the specification in Column 2 with additional controls for state-specific linear time trends. These do not change the magnitude nor the statistical significance of the mandate variables, suggesting that once age-year interactions are added, there are no additional state-specific trends over time that are correlated with the mandates. 14 It is possible that the effect of the mandates on first birth rates varies depending on the type of mandate enacted. In particular, one might expect a mandate to cover to affect births differently than a mandate to offer, or a mandate including IVF to affect births differently than a 13 The mean age at first birth for women in the United States has risen from 21.4 years in 1970 to almost 25 years in 2000 (Mathews and Hamilton, 2002). 14 These results are available from the author. 11
13 mandate excluding IVF coverage. In Table 4, I break out the mandates by type. Panel A shows results from a specification separating mandates to cover from mandates to offer. The estimated coefficients on the control variables in the regression are similar to those presented in Column 2 of Table 3, so only the estimates of the mandate coefficients are presented here. The two year lags on both types of mandates are positive and significant for women over 35, and there is no statistical evidence that a mandate to cover affects first birth rates differently than a mandate to offer. Panel B of Table 4 shows results separating mandates with and without required IVF coverage. For the mandates with IVF, the pattern of coefficients is similar to that of the single mandate variable. The two year lag is positive and significant for women over 35, and no other mandate variables are statistically different from zero. For mandates without IVF coverage, the coefficient on the two year lag is positive and statistically significant, and is not statistically different from the coefficient on the corresponding variable with IVF coverage. However, there is also a positive and statistically significant effect of the one-year lag on women over 35. These differential lag effects of mandates with and without IVF are worth further exploration One argument from a policy standpoint for expanding coverage for infertility treatment is that there are currently large differentials in terms of who has access to treatment. White, married women with higher levels of income are most likely to seek and to receive treatment for infertility (e.g. Stephen and Chandra, 2000). To test whether the mandates are having differential effects on birth rates by race, I re-estimate the main specification (including age-year interactions) separately by the race of the mother (separating black women from white and other). These results are presented in Table 5. The two year lag on the mandate variable is positive and significant for women over the age of 35. It suggests that a mandate increases first 12
14 birth rates for older white women by 17%, and for older black women by 32%. However, these percentage changes are on different bases, as first birth rates for women over 35 differ by race. In 1999, the average first birth rate across states for white/other women 35 and older was , while the corresponding rate for black women was lower at V. Conclusions and Directions for Future Work For a woman or couple faced with fertility problems, a healthy birth is the ultimate goal. From this perspective, it appears as if the state-level infertility insurance mandates have been a success, as I find that the mandates increase first birth rates among women over 35 by 18% percent. The effects are similar for the different types of mandates (mandates to cover vs. mandates to offer and mandates including or excluding IVF coverage), and the effects are larger in percentage terms for black women (albeit from a smaller base rate). However, this analysis leaves several important questions unanswered. In ongoing work, I am working on addressing the following questions. First, have the mandates been successful at increasing births for those groups who have traditionally had less access to treatment? This requires individual data that allows breakdowns along dimensions of race, ethnicity, education, and income. Second, what is the intermediate mechanism through which the mandates are increasing birth rates? Are they increasing particular types of treatments? This is essential for determining the costs of the mandates. Finally, who bears the cost of these state mandates? How do they affect the labor market? Do they reduce labor demand like a tax, leading to a reduction in employment? Or do they also increase labor supply, offsetting the negative effects of reduced labor demand on employment through reduced wages? 13
15 As infertility becomes an increasingly common medical problem, advocacy groups are likely to continue to pressure policymakers to enact mandated benefits at both the state and federal levels. Insurance providers are likely to continue to resist these pressures. A full evaluation of the effects of mandated benefits is essential to informing this policy debate. 14
16 References Bertrand, Marianne, Esther Duflo, and Sendhil Mullainathan How Much Should We Trust Differences-in-Differences Estimates? National Bureau of Economic Research Working Paper #8841. Bitler, Marianne P Effects of Increased Access to Infertility Treatment on Infant Health Outcomes: Evidence from Twin Births. RAND Unpublished Manuscript. Blank, Rebecca M., Christine C. George, and Rebecca A. London State Abortion Rates: The Impact of Policies, Providers, Politics, Demographics, and Economic Environment. Journal of Health Economics 15: Chandra, Anjani, Elizabeth Hervey Stephen, Dik Habbema, and Egbert R. te Velde How Long Can You Wait? Measurement Challenges and Health Concerns Related to Infertility and Delayed Childbearing. Draft. Chandra, Anjani and Mosher, W.D The Demography of Infertility and the Use of Medical Care for Infertility Infertility and Reproductive Medicine Clinics of North America 5(2): Chandra, Anjani and Elizabeth Hervey Stephen Impaired Fecundity in the United States: Family Planning Perspectives 30(1): Fidler, A.T. and J. Bernstein Infertility: From a Personal to a Public Health Problem. Public Health Reports 114: Gruber, Jonathan The Incidence of Mandated Maternity Benefits. American Economic Review 84(3): Hamilton, Barton H. and Brian McManus Competition, Insurance, and Quality in the Market for Advanced Infertility Treatment. Manuscript. Jain, Tarun, Bernard L. Harlow, and Mark D. Hornstein Insurance Coverage and Outcomes of In Vitro Fertilization. New England Journal of Medicine 347(9): Kaiser Foundation Latest Findings on Employer Based Coverage of Contraception. Memo. Klabunde, Carrie, Gerald F. Riley, Margaret T. Mandelson, Paul S. Frame, and Martin L. Brown Health Care Policies and Programs for Colorectal Cancer Screening: A National Profile. American Journal of Managed Care 10(4): Klerman, Jacob Alex U.S. Abortion Policy and Fertility. American Economic Review 89(2): Levine, Phillip B., Amy B. Trainor, and David J. Zimmerman The Effect of Medicaid Abortion Funding Restrictions on Abortions, Pregnancies and Births. Journal of Health Economics 15(5): Mathews, T.J. and Brady E. Hamilton Mean Age of Mother: National Vital Statistics Reports 51(1). Hyattsville, Maryland: National Center for Health Statistics. Reynolds, Meredith A., Laura A. Schieve, Gary Jeng, and Herbert B. Peterson Does Insurance Coverage Decrease the Risk for Multiple Births Associated with Reproductive Tehcnology? Fertility and Sterility 80(1): Ruhm, C.J The Economic Consequences of Parental Leave Mandates: Lessons from Europe. Quarterly Journal of Economics 113(1). Stephen, Elizabeth Hervey and Anjani Chandra Use of Infertility Services in the United States: Family Planning Perspectives 32(3):
17 Summers, Lawrence H Some Simple Economics of Mandated Benefits. AEA Papers and Proceedings 79(2): U.S. House of Representatives th Congress, 1st Session. H.R. 3014, Family Building Act of
18 State Table 1 State Mandated Infertility Insurance Year Enacted Mandate to Cover/Mandate to Offer In Vitro Fertilization Coverage? Arkansas 1987* Cover Yes California 1989* Offer No Connecticut 1989 Offer Yes Hawaii 1987 Cover Yes Illinois 1991 Cover Yes Louisiana 2001 Cover No Maryland 1985 Cover Yes Massachusetts 1987 Cover Yes Montana 1987 Cover No New Jersey 2001 Cover Yes New York 1990* Cover No Ohio 1991 Cover No Rhode Island 1989 Cover Yes Texas 1987 Offer Yes West Virginia 1977* Cover No Sources: Resolve ( and state laws (see Appendix A). *Arkansas, California, New York, and West Virginia first passed mandates in the years shown. These mandates were subsequently revised, but remained in place. 17
19 Table 2 Live Births in Mandate States Live births in mandate states 25,259 1,258,990 1,782,930 Live births in US 3,765,064 4,162,917 3,903,012 Births in mandate states as a percentage of total births 0.67% 30.24% 45.68% Source: National Center for Health Statistics, Vital Statistics of the United States, Volume I (Natality), various years. Births are considered to be in mandate states if a mandate was in place in the previous calendar year. 18
20 Table 3 Effects of Mandates on First Birth Rates Column 1 Column 2 Black (0.0378) ** (0.0375) Age (0.0232) (0.0272) Age (0.0576) (0.0651) Age (0.0732) (0.0833) Age (0.0733) (0.1082) Age (0.0828) (0.1416) Age (0.0862) (0.1918) Log median weekly earnings (0.1950) (0.1967) Log 10 th percentile weekly earnings (0.1037) (0.1026) Unemployment rate ** (0.0084) (0.0083) Female labor force participation rate (0.0047) (0.0048) Log maximum AFDC/TANF benefit (0.0901) (0.0887) State in compliance with Hyde amendment (0.0220) (0.0218) State funds abortions beyond Hyde requirements Parental involvement abortion restrictions (0.0254) (0.0257) (0.0255) (0.0254) ** * Mandate (t-1) γ t (0.0445) Mandate(t-1)*Over35 θt (0.1057) Mandate (t-2) γ t (0.0344) Mandate(t-2)*Over35 θt (0.0355) (0.0460) (0.1082) (0.0422) (0.0529) State fixed effects Yes Yes Year fixed effects Yes Yes Age*year interactions No Yes Notes: Dependent variable is the log of the first birth rate in a state-year-race-age cohort cell. White robust standard errors clustered by state in parentheses. Regressions are weighted by cell-level population counts. Levels of statistical significance: denotes significance at the one-percent level; ** at the five-percent level; and * at the ten-percent level. 19
21 Table 4 Effects of Mandates on First Birth Rates, by Type of Mandate A. Mandate to cover vs. mandate to offer Mandate to cover (t-1) (0.0815) Mandate to cover (t-1)*over (0.1399) Mandate to cover (t-2) (0.0203) Mandate to cover (t-2)*over (0.0404) Mandate to offer (t-1) (0.0502) Mandate to offer (t-1)*over (0.2054) Mandate to offer (t-2) (0.0621) Mandate to offer (t-2)*over (0.0716) ** Test equality of coefficients: mandate to cover and to offer (2 year lag interacted with Over 35) F(1, 31958) 0.20 B. Mandate covering IVF vs. mandate not covering IVF Mandate with IVF (t-1) (0.0505) Mandate with IVF (t-1)*over (0.1382) Mandate with IVF (t-2) (0.0332) Mandate with IVF (t-2)*over (0.0636) Mandate without IVF (t-1) (0.0672) Mandate without IVF (t-1)*over (0.1242) Mandate without IVF (t-2) (0.0311) Mandate without IVF (t-2)*over (0.0496) ** ** Test equality of coefficients: mandate with IVF and without IVF (2 year lag interacted with Over 35) F(1, 31958) 0.03 Notes: Dependent variable is the log of the first birth rate in a state-year-race-age cohort cell. White robust standard errors clustered by state in parentheses. Regressions include state and year fixed effects, as well as age*year interactions. Regressions are weighted by cell-level population counts. Levels of statistical significance: denotes significance at the one-percent level; ** at the five-percent level; and * at the ten-percent level. 20
22 Table 5: Effects of Mandates on First Birth Rates, By Race White and Other Black Age (0.0286) (0.0383) Age (0.0713) (0.0663) Age (0.0867) (0.0864) Age (0.1099) (0.1152) Age (0.1426) (0.1571) Age (0.2165) (0.1867) Log median weekly earnings (0.2164) (0.3014) Log 10 th percentile weekly earnings (0.1278) (0.1610) Unemployment rate ** (0.0099) (0.0076) Female labor force participation rate (0.0057) (0.0075) Log maximum AFDC/TANF benefit (0.1023) (0.1568) State in compliance with Hyde amendment (0.0280) (0.0190) State funds abortions beyond Hyde requirements (0.0321) (0.0320) Parental involvement abortion restrictions (0.0279) (0.0320) * ** * Mandate (t-1) γ t (0.0494) Mandate(t-1)*Over35 θt (0.1187) Mandate (t-2) γ t (0.0389) Mandate(t-2)*Over35 θt (0.0593) (0.0377) (0.1042) (0.0219) (0.0576) State fixed effects Yes Yes Year fixed effects Yes Yes Age*year interactions Yes Yes Notes: Dependent variable is the log of the first birth rate in a state-year-race-age cohort cell. White robust standard errors clustered by state in parentheses. Levels of statistical significance: denotes significance at the onepercent level; ** at the five-percent level; and * at the ten-percent level. 21
23 Arkansas Appendix A: State Laws Regarding Insurance Coverage of Infertility Treatment The current law, enacted in 1991, requires all insurance policies which provide pregnancyrelated benefits to provide coverage for in vitro fertilization. To qualify: The patient must be the policyholder or the spouse of the policyholder and must be a covered dependent under that policy. The patient must have her oocytes fertilized by her spouse s sperm. The patient and her spouse must have a history of unexplained infertility for at least two years, or must have one or more of the following medical conditions: 1. Endometriosis 2. Exposure in utero to Diethylstillbestrol (DES) 3. Blockage or removal of one or both fallopian tubes, not as a result of voluntary sterilization. 4. Abnormal male factors. The patient must have been unable to obtain successful pregnancy through other less costly infertility treatments for which coverage is available under the policy. The in vitro procedure must be performed at a medical facility licensed by the Arkansas Department of Health and meeting the standards set by either the American College of Obstetricians and Gynecologists or the American Fertility Society These qualifications indicate that the woman must be married to receive coverage; however, no other restrictions exist regarding the age of the patient, the maximum firm size that may omit coverage, or exceptions for religious organizations. The law has existed in this form since 1991, but some coverage for in vitro fertilization was first required of health insurance companies in The 1991 law revised the 1987 one by setting maximum and minimum benefit levels and establishing the above standards for determining whether a policy or certificate must include coverage. ( California California s 1989 law mandates that all insurers covering hospital, medical or surgical expenses on a group basis offer coverage of infertility treatment, excluding in vitro fertilization. Infertility is defined as either the presence of a demonstrated medical condition recognized by a licensed physician, or as the inability to conceive a pregnancy or carry a pregnancy to term after at least a year of regular unprotected sexual intercourse. Covered treatment includes diagnosis, medication, surgery, and gamete intrafallopian transfer (GIFT). No restrictions exist as to the age or marital status of the patient, or the size of the firm or group offering the policy. Religious organizations whose religious or ethical principles disagree with this policy are exempt from having to offer coverage. (California Insurance Code section ) 22
24 Connecticut According to 1989 law, all group insurers must offer an insurance plan that covers the medically necessary expenses of the diagnosis and treatment of infertility, including in vitro fertilization procedures. Infertility is defined as the inability to conceive or to retain a pregnancy during a one year period. Medically necessary is not defined, nor are there any other restrictions or exemptions. (Connecticut General Statutes Annotated, section 38a-536) Hawaii In 1987, Hawaii passed a law requiring all individual and group health insurance policies which provide pregnancy-related benefits to provide a one-time only benefit for all outpatient expenses arising from in vitro fertilization. To qualify: The patient must be the policyholder or the spouse of the policyholder and must be a covered dependent under that policy. The patient must have her oocytes fertilized by her spouse s sperm, where spouse is defined as the person who is lawfully married to the patient under the laws of the state. The patient and her spouse must have a history of unexplained infertility for at least five years, or must have one or more of the following medical conditions: 1. Endometriosis 2. Exposure in utero to Diethylstillbestrol (DES) 3. Blockage or removal of one or both fallopian tubes, not as a result of voluntary sterilization. 4. Abnormal male factors. The patient must have been unable to obtain successful pregnancy through other less costly infertility treatments for which coverage is available under the policy. The in vitro procedure must be performed at a medical facility meeting the standards set by either the American College of Obstetricians and Gynecologists or the American Fertility Society. No restrictions exist for age of the patient or firm size, and no exemptions are made for religious organizations. (Hawaii Revised Statutes, 431:10A-116.5) Illinois Illinois law requires that all group insurers providing coverage for more than 25 employees after 1991 must cover the diagnosis and treatment of infertility, including in vitro fertilization, uterine embryo lavage, embryo transfer, artificial insemination, gamete intrafallopian tube transfer, zygote intrafallopian tube transfer, and low ovum tube transfer. To qualify: 23
25 The patient must be unable to conceive or sustain a pregnancy after one year of unprotected sexual intercourse. The patient must be unable to obtain successful pregnancy through other less costly infertility treatments for which coverage is available under the policy. The patient must have undergone fewer than four oocyte retrievals, unless a live birth has resulted from a completed oocyte retrieval, in which case she is entitled to two more covered retrievals. The procedure must be performed at a medical facility meeting the standards set by either the American College of Obstetricians and Gynecologists or the American Fertility Society. No other restrictions exist; however, the insurer does not have to pay for: The reversal of voluntary sterilization. Costs rendered to a surrogate for purposes of childbirth The cryopreservation and storage of sperm, eggs, and embryos. Non-medical costs of a sperm or egg donor, including travel costs. Experimental treatments. Furthermore, religious organizations which find these policies to be at odds with their moral and ethical teachings are exempt from providing coverage. ( Maryland As of 1985, Maryland requires that insurers of individuals and groups, including HMO s, must provide coverage of in vitro fertilization to the same extent as pregnancy-related services are provided. To qualify: The patient must be the policyholder or the spouse of the policyholder and must be a covered dependent under that policy. The patient must have her oocytes fertilized by her spouse s sperm. The patient and her spouse must have a history of unexplained infertility for at least two years, or must have one or more of the following medical conditions: 1. Endometriosis 2. Exposure in utero to Diethylstillbestrol (DES) 3. Blockage or removal of one or both fallopian tubes, not as a result of voluntary sterilization. 4. Abnormal male factors. The patient must have been unable to obtain successful pregnancy through other less costly infertility treatments for which coverage is available under the policy. The in vitro procedure must be performed at a medical facility meeting the standards set by either the American College of Obstetricians and Gynecologists or the American Fertility Society. 24
26 Benefits may not exceed a maximum lifetime benefit of $100,100. Women must be married, but no further restrictions apply. Religious organizations are exempt from providing coverage if it conflicts with their moral beliefs. Firms with 50 or fewer employees are also exempt as of (Maryland Insurance Article ) Massachusetts 1987 Massachusetts law requires all insurers and HMO s to cover benefits for required infertility procedures, including artificial insemination, in vitro fertilization, gamete intrafallopian transfer, sperm or egg procurement, processing, and storage, intracytoplasmic sperm injection, and zygote intrafallopian transfer. The insurer must also cover prescription drugs relating to infertility. Insurers are not required to cover experimental procedures, surrogacy, reversal of voluntary sterilization, or cryopreservation of eggs. Patients must hold the insurance policy themselves, or must be the spouse or dependent of the insured person. Infertility is defined as the inability to conceive or carry a pregnancy to term during the period of one year. No other requirements or exemptions apply. (Annotated Laws of Massachusetts 211 CMR: Division of Insurance 37.00) Montana Montana s laws require HMO s to cover infertility treatment, but specifically excludes artificial insemination and infertility treatment from coverage mandated for other insurance companies. No mention is made of what infertility is, nor what is covered by the HMO s. No other requirements or exemptions apply. (Montana Code Annotated, , ) New Jersey New Jersey s law was not enacted until However, it mandates that all insurers covering groups of 50 or more must cover the diagnosis and treatment of infertility. This includes artificial insemination, assisted hatching, diagnostic tests, fresh and frozen embryo transfer, up to four completed egg retrievals, GIFT and ZIFT, in vitro fertilization, medications, ovulation induction, and surgery. Insurers do not have to pay for reversal of voluntary sterilization, surrogacy cryopreservation of eggs, sperm, or embryos, non-medical costs of the egg or sperm donor, experimental treatments, or ovulation or sperm testing kits. They also do not have to pay for IVF, GIFT, or ZIFT for women who are 46 years of age or older. Employers with religious objections are exempt from offering coverage. A patient is considered infertile if she a) is under age 35 and is unable to conceive after two years of unprotected sexual intercourse; b)is over age 35 and is unable to conceive after one year of unprotected sexual intercourse; or c) is medically sterile. Patients must use all reasonable, less expensive treatments before turning to IVF, GIFT, or ZIFT, and all such procedures must be performed in a medical facility meeting the standards 25
27 set by either the American College of Obstetricians and Gynecologists or the American Fertility Society. No other requirements or exemptions apply. ( New Jersey P.L. 2001, c :4-54) New York As of 1990, group insurers in New York are required to provide coverage of infertility treatments, including diagnostic tests and pharmaceuticals, for all infertile women between ages 21 and 44 who have been covered under the policy for at least a year. Insurers are not required to cover in vitro fertilization, gamete intrafallopian transfer, zygote intrafallopian transfer, reversal of voluntary sterilization, sex change procedures, cloning, or experimental procedures. Infertility must be determined in accordance with the standards of the American College of Obstetrics and Gynecologists and the American Society for Reproductive Medicine. No other requirements or exemptions apply. In 2002 the state of NY passed a revised law, which clarified the 1990 law and appropriated $10 million to a pilot project to help pay for in vitro procedures for a small number of people who received care from those facilities that were to be the beneficiaries of grants awarded through the program. (New York Consolidated Laws, Insurance, Section 3221(k)(6), Section 4303(s).) Ohio Under a 1991 law, Ohio includes coverage for infertility services as part of its basic health care services, and, as such, covers the medically necessary diagnosis and correction of problems causing infertility. There is no specific law covering in vitro fertilization, gamete intrafallopian transfer, or zygote intrafallopian transfer; however, the Superintendent of Insurance stated in 1997 that IVF, GIFT and ZIFT were not essential for the protection of an individual s health and were therefore not subject to mandated insurance coverage. Ohio has no definition of infertility, nor does it detail any other specific requirements or exemptions. ( Rhode Island Rhode Island (1989) requires that all insurers which cover pregnancy-related benefits also cover the diagnosis and treatment of infertility, where infertility is defined as the condition of an otherwise healthy married individual who is unable to conceive or produce conception during a period of one year. It further stipulates that the patient co-payment may not exceed 20%. There are no other requirements or exemptions. (Rhode Island General Laws, ) 26
28 Texas 1987 Texas law requires group and private insurers to offer coverage for outpatient expenses arising from in vitro fertilization procedures. To qualify: The patient must be the policyholder or the spouse of the policyholder and must be a covered dependent under that policy. The patient must have her oocytes fertilized by her spouse s sperm. The patient and her spouse must have a history of unexplained infertility for at least five years, or must have one or more of the following medical conditions: 1. Endometriosis 2. Exposure in utero to Diethylstillbestrol (DES) 3. Blockage or removal of one or both fallopian tubes, not as a result of voluntary sterilization. 4. Abnormal male factors. The patient must have been unable to obtain successful pregnancy through other less costly infertility treatments for which coverage is available under the policy. The in vitro procedure must be performed at a medical facility that meets the standards set by either the American College of Obstetricians and Gynecologists or the American Fertility Society Religious organizations whose moral code conflicts with this policy are exempt from offering coverage. No other restrictions or exemptions exist. (Texas Insurance Statutes, Art , Section 3A) West Virginia Since 1977, West Virginia has required HMO s to cover infertility services as part of Basic Health Care Services. The 1977 law did not specify which services were covered, which women were covered, or whether any organizations were exempt from providing coverage. That 1977 law was amended in 2001, and mandated HMO s to cover infertility treatment only as a preventative service benefit (thus excluding in vitro fertilization). (West Virginia Code 33-25A-2). 27
Of Competitive Pressures and Care Quality: Infertility Treatment Case
 Of Competitive Pressures and Care Quality: Infertility Treatment Case Helen Schneider Department of Economics, University of Texas at Austin Importance of the Study About 11 percent of American women 15
Of Competitive Pressures and Care Quality: Infertility Treatment Case Helen Schneider Department of Economics, University of Texas at Austin Importance of the Study About 11 percent of American women 15
Department of Legislative Services Maryland General Assembly 2010 Session
 Department of Legislative Services Maryland General Assembly 2010 Session SB 27 Senate Bill 27 Finance FISCAL AND POLICY NOTE Revised (Senator Conway) Health and Government Operations Health Insurance
Department of Legislative Services Maryland General Assembly 2010 Session SB 27 Senate Bill 27 Finance FISCAL AND POLICY NOTE Revised (Senator Conway) Health and Government Operations Health Insurance
WHAT YOU DIDN T KNOW, BUT NEED TO
 WHAT YOU DIDN T KNOW, BUT NEED TO In 2016, 7 million people will try to conceive through natural pregnancy, but only 5 million will be successful 20% of women are born with low ovarian reserve 200,000
WHAT YOU DIDN T KNOW, BUT NEED TO In 2016, 7 million people will try to conceive through natural pregnancy, but only 5 million will be successful 20% of women are born with low ovarian reserve 200,000
LISI CARRIERS INFERTILITY COMPARISON
 AETNA Diagnostic services for the diagnosis and treatment of the underlying medical condition, and: Infertility Treatment - AI/OI Advanced Reproductive Technology including but not limited to GIFT, ZIFT,
AETNA Diagnostic services for the diagnosis and treatment of the underlying medical condition, and: Infertility Treatment - AI/OI Advanced Reproductive Technology including but not limited to GIFT, ZIFT,
Infertility Treatment, ART and IUI Procedures and Delivery. Outcomes: How Important is Selection? 1
 Infertility Treatment, ART and IUI Procedures and Delivery Outcomes: How Important is Selection? 1 Pooja G. Mookim 2, Randall P. Ellis 3, Ariella Kahn-Lang 4 May 1, 2008 Abstract: High infertility levels
Infertility Treatment, ART and IUI Procedures and Delivery Outcomes: How Important is Selection? 1 Pooja G. Mookim 2, Randall P. Ellis 3, Ariella Kahn-Lang 4 May 1, 2008 Abstract: High infertility levels
RESOLVE: The National Infertility Association. 21 st Century Infertility Treatment & Access to Care
 RESOLVE: The National Infertility Association 21 st Century Infertility Treatment & Access to Care What is Infertility? Infertility is a disease impacting 7.3 million Americans. 1 in 8 individuals or couples
RESOLVE: The National Infertility Association 21 st Century Infertility Treatment & Access to Care What is Infertility? Infertility is a disease impacting 7.3 million Americans. 1 in 8 individuals or couples
Utilization with High Out-of-Pocket Costs: Evidence from In-Vitro-Fertilization Treatment
 Utilization with High Out-of-Pocket Costs: Evidence from In-Vitro-Fertilization Treatment Lucie Schmidt, Lindsay Tedds, Arezou Zaresani September 2017 (Download the latest draft from http://azaresani.com/work-in-progress)
Utilization with High Out-of-Pocket Costs: Evidence from In-Vitro-Fertilization Treatment Lucie Schmidt, Lindsay Tedds, Arezou Zaresani September 2017 (Download the latest draft from http://azaresani.com/work-in-progress)
INFERTILITY SERVICES
 INFERTILITY SERVICES Protocol: OBG036 Effective Date: August 1, 2018 Table of Contents Page COMMERCIAL COVERAGE RATIONALE... 1 DEFINITIONS... 4 MEDICARE AND MEDICAID COVERAGE RATIONALE... 5 REFERENCES...
INFERTILITY SERVICES Protocol: OBG036 Effective Date: August 1, 2018 Table of Contents Page COMMERCIAL COVERAGE RATIONALE... 1 DEFINITIONS... 4 MEDICARE AND MEDICAID COVERAGE RATIONALE... 5 REFERENCES...
INSURANCE COVERAGE AND IN VITRO FERTILIZATION. Special Article INSURANCE COVERAGE AND OUTCOMES OF IN VITRO FERTILIZATION
 INSURANCE AND IN VITRO FERTILIZATION Special Article INSURANCE AND OUTCOMES OF IN VITRO FERTILIZATION TARUN JAIN, M.D., BERNARD L. HARLOW, PH.D., AND MARK D. HORNSTEIN, M.D. ABSTRACT Background Although
INSURANCE AND IN VITRO FERTILIZATION Special Article INSURANCE AND OUTCOMES OF IN VITRO FERTILIZATION TARUN JAIN, M.D., BERNARD L. HARLOW, PH.D., AND MARK D. HORNSTEIN, M.D. ABSTRACT Background Although
Clinical Policy Committee
 Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Group Hospitalization and Medical Services, Inc., doing business as CareFirst BlueCross BlueShield
 Group Hospitalization and Medical Services, Inc. doing business as CareFirst BlueCross BlueShield 840 First Street, NE Washington, DC 20065 202-479-8000 An independent licensee of the Blue Cross and Blue
Group Hospitalization and Medical Services, Inc. doing business as CareFirst BlueCross BlueShield 840 First Street, NE Washington, DC 20065 202-479-8000 An independent licensee of the Blue Cross and Blue
Why Insurance Coverage Fails To Close The Access Gap To Artificial Reproductive Technology. Andrew Fisher, BSE, MS4.
 Why Insurance Coverage Fails To Close The Access Gap To Artificial Reproductive Technology Andrew Fisher, BSE, MS4 February 10, 2014 Submitted here for consideration for the Perelman School of Medicine
Why Insurance Coverage Fails To Close The Access Gap To Artificial Reproductive Technology Andrew Fisher, BSE, MS4 February 10, 2014 Submitted here for consideration for the Perelman School of Medicine
Clinical Policy Committee
 Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Policy statement. Commissioning of Fertility treatments
 Policy statement Commissioning of Fertility treatments NB: The policy relating to commissioning of fertility treatments is unchanged from the version approved by the CCG in March 2017. The clinical thresholds
Policy statement Commissioning of Fertility treatments NB: The policy relating to commissioning of fertility treatments is unchanged from the version approved by the CCG in March 2017. The clinical thresholds
Contents. Introduction. Acknowledgments. 1 Assisted Reproduction and the Diversity of the Modern Family 1. 2 Intrauterine Insemination 31.
 Introduction Acknowledgments xvii xix 1 Assisted Reproduction and the Diversity of the Modern Family 1 1.1 Assisted Reproduction Technology Today....1 1.2 ART and Marriage...5 1.3 Evolution of the Family...8
Introduction Acknowledgments xvii xix 1 Assisted Reproduction and the Diversity of the Modern Family 1 1.1 Assisted Reproduction Technology Today....1 1.2 ART and Marriage...5 1.3 Evolution of the Family...8
Reproductive Technology, Genetic Testing, and Gene Therapy
 Michael Cummings Chapter 16 Reproductive Technology, Genetic Testing, and Gene Therapy David Reisman University of South Carolina 16.1 Infertility Is a Common Problem In the US, about 13% of all couples
Michael Cummings Chapter 16 Reproductive Technology, Genetic Testing, and Gene Therapy David Reisman University of South Carolina 16.1 Infertility Is a Common Problem In the US, about 13% of all couples
NHS FUNDED TREATMENT FOR SUBFERTILITY. ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs
 NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO
NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO
Commissioning Policy For In Vitro Fertilisation (IVF) / Intracytoplasmic Sperm Injection (ICSI) within Tertiary Infertility Services
 Commissioning Policy For In Vitro Fertilisation (IVF) / Intracytoplasmic Sperm Injection (ICSI) within Tertiary Infertility Services Reference No: Version: 2 Ratified by: EMSCGP006V2 EMSCG Date ratified:
Commissioning Policy For In Vitro Fertilisation (IVF) / Intracytoplasmic Sperm Injection (ICSI) within Tertiary Infertility Services Reference No: Version: 2 Ratified by: EMSCGP006V2 EMSCG Date ratified:
ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE
 ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE Version 1.0 Page 1 of 11 MARCH 2014 POLICY DOCUMENT VERSION CONTROL CERTIFICATE TITLE Title: Assisted Conception
ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE Version 1.0 Page 1 of 11 MARCH 2014 POLICY DOCUMENT VERSION CONTROL CERTIFICATE TITLE Title: Assisted Conception
Treating Infertility
 Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
Blackpool CCG. Policies for the Commissioning of Healthcare. Assisted Conception
 1 Introduction Blackpool CCG Policies for the Commissioning of Healthcare Assisted Conception 1.1 This policy describes circumstances in which NHS Blackpool Clinical Commissioning Group (CCG) will fund
1 Introduction Blackpool CCG Policies for the Commissioning of Healthcare Assisted Conception 1.1 This policy describes circumstances in which NHS Blackpool Clinical Commissioning Group (CCG) will fund
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL Policy Number: PA.018.MH Last Review Date: 08/04/2016 Effective Date: 01/01/2017
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL PA.018.MH Infertility- Treatment This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP (Not Covered) MedStar
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL PA.018.MH Infertility- Treatment This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP (Not Covered) MedStar
Director of Commissioning, Telford and Wrekin CCG and Shropshire CCG. Version No. Approval Date August 2015 Review Date August 2017
 Commissioning Policy for In Vitro Fertilisation (IVF)/ Intracytoplasmic Sperm Injection (ICSI) within tertiary Infertility Services, in Shropshire and Telford and Wrekin Owner(s) Version No. Director of
Commissioning Policy for In Vitro Fertilisation (IVF)/ Intracytoplasmic Sperm Injection (ICSI) within tertiary Infertility Services, in Shropshire and Telford and Wrekin Owner(s) Version No. Director of
Infertility services reported by men in the United States: national survey data
 MALE FACTOR Infertility services reported by men in the United States: national survey data John E. Anderson, Ph.D., Sherry L. Farr, Ph.D., M.S.P.H., Denise J. Jamieson, M.D., M.P.H., Lee Warner, Ph.D.,
MALE FACTOR Infertility services reported by men in the United States: national survey data John E. Anderson, Ph.D., Sherry L. Farr, Ph.D., M.S.P.H., Denise J. Jamieson, M.D., M.P.H., Lee Warner, Ph.D.,
HALTON CLINICAL COMMISSIONING GROUP NHS FUNDED TREATMENT FOR SUBFERTILITY. CONTENTS Page
 HALTON CLINICAL COMMISSIONING GROUP NHS FUNDED TREATMENT FOR SUBFERTILITY CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO TREATMENT 3 4. DEFINITION
HALTON CLINICAL COMMISSIONING GROUP NHS FUNDED TREATMENT FOR SUBFERTILITY CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO TREATMENT 3 4. DEFINITION
Infertility Service Use among Fertility-Impaired Women in the United States:
 Infertility Service Use among Fertility-Impaired Women in the United States: 1995-2010 Anjani Chandra, Ph.D., CDC/National Center for Health Statistics Elizabeth Hervey Stephen, Ph.D., Georgetown University
Infertility Service Use among Fertility-Impaired Women in the United States: 1995-2010 Anjani Chandra, Ph.D., CDC/National Center for Health Statistics Elizabeth Hervey Stephen, Ph.D., Georgetown University
Health Service System City & County of San Francisco
 Health Service System City & County of San Francisco Health Service Board Meeting Infertility Coverage January 12, 2017 Prepared by: Infertility Infertility is defined as not being able to get pregnant
Health Service System City & County of San Francisco Health Service Board Meeting Infertility Coverage January 12, 2017 Prepared by: Infertility Infertility is defined as not being able to get pregnant
St Helens CCG NHS Funded Treatment for Subfertility Policy 2015/16
 St Helens CCG NHS Funded Treatment for Subfertility Policy 2015/16 1 Standard Operating Procedure St Helens CCG NHS Funded Treatment for Sub Fertility Policy Version 1 Implementation Date May 2015 Review
St Helens CCG NHS Funded Treatment for Subfertility Policy 2015/16 1 Standard Operating Procedure St Helens CCG NHS Funded Treatment for Sub Fertility Policy Version 1 Implementation Date May 2015 Review
Infertility F REQUENTLY A SKED Q UESTIONS. Q: Is infertility a common problem?
 Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
CONTROVERSY: INSURANCE COVERAGE
 CONTROVERSY: INSURANCE COVERAGE FERTILITY AND STERILITY VOL. 80, NO. 1, JULY 2003 Copyright 2003 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A.
CONTROVERSY: INSURANCE COVERAGE FERTILITY AND STERILITY VOL. 80, NO. 1, JULY 2003 Copyright 2003 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A.
MATERNAL AND CHILD HEALTH AND DISPARITIES FOR ASIAN AMERICANS, NATIVE HAWAIIANS, AND PACIFIC ISLANDERS
 MATERNAL AND CHILD HEALTH AND DISPARITIES FOR ASIAN AMERICANS, NATIVE HAWAIIANS, AND PACIFIC ISLANDERS Why does maternal and child health matter for realizing health justice in AA and NHPI communities?
MATERNAL AND CHILD HEALTH AND DISPARITIES FOR ASIAN AMERICANS, NATIVE HAWAIIANS, AND PACIFIC ISLANDERS Why does maternal and child health matter for realizing health justice in AA and NHPI communities?
Increased Length of Awareness of Assisted Reproductive Technologies Fosters Positive Attitudes and Acceptance among Women
 www.ijfs.ir Supplementary Information for Increased Length of Awareness of Assisted Reproductive Technologies Fosters Positive Attitudes and Acceptance among Women Chelsea Fortin, M.D. 1, 2 *, Susanne
www.ijfs.ir Supplementary Information for Increased Length of Awareness of Assisted Reproductive Technologies Fosters Positive Attitudes and Acceptance among Women Chelsea Fortin, M.D. 1, 2 *, Susanne
Rabson, Mia. (2012, April 14). Fertile ground for controversy. Winnipeg Free Press. Retrieved
 Rabson, Mia. (2012, April 14). Fertile ground for controversy. Winnipeg Free Press. Retrieved from http://www.winnipegfreepress.com/local/fertile-ground-for-controversy- 147422385.html Key Questions 1)
Rabson, Mia. (2012, April 14). Fertile ground for controversy. Winnipeg Free Press. Retrieved from http://www.winnipegfreepress.com/local/fertile-ground-for-controversy- 147422385.html Key Questions 1)
T39: Fertility Policy Checklist
 Patient Name: Address: Date of Birth: NHS Number: Consultant/Service to whom referral will be made: Institution Lifestyle Information Latest BMI: Latest BP: Smoking Status: Has the patient been referred
Patient Name: Address: Date of Birth: NHS Number: Consultant/Service to whom referral will be made: Institution Lifestyle Information Latest BMI: Latest BP: Smoking Status: Has the patient been referred
Bonnie Steinbock University at Albany (emerita) Distinguished Visiting Professor, CUHK Centre for Bioethics 12th December, 2015
 Bonnie Steinbock University at Albany (emerita) Distinguished Visiting Professor, CUHK Centre for Bioethics 12th December, 2015 Defined as inability to get pregnant after a year of regular sexual intercourse
Bonnie Steinbock University at Albany (emerita) Distinguished Visiting Professor, CUHK Centre for Bioethics 12th December, 2015 Defined as inability to get pregnant after a year of regular sexual intercourse
Assisted Reproductive Technologies
 Assisted Reproductive Technologies Textbook pages 224 231 Section 6.3 Summary Before You Read What do you think the phrase test-tube baby refers to? Write your ideas on the lines below. Mark the Text Check
Assisted Reproductive Technologies Textbook pages 224 231 Section 6.3 Summary Before You Read What do you think the phrase test-tube baby refers to? Write your ideas on the lines below. Mark the Text Check
[Act on Artificial Fertilisation and use of Human Gametes and Embryos for Stem-Cell Research] 1) No. 55/1996 1) Act No. 27/2008, Article 9
![[Act on Artificial Fertilisation and use of Human Gametes and Embryos for Stem-Cell Research] 1) No. 55/1996 1) Act No. 27/2008, Article 9 [Act on Artificial Fertilisation and use of Human Gametes and Embryos for Stem-Cell Research] 1) No. 55/1996 1) Act No. 27/2008, Article 9](/thumbs/83/87125205.jpg) [Act on Artificial Fertilisation and use of Human Gametes and Embryos for Stem-Cell Research] 1) No. 55/1996 1) Act No. 27/2008, Article 9 as amended by Act No. 65/2006, Act No. 27/2008, Act No. 54/2008,
[Act on Artificial Fertilisation and use of Human Gametes and Embryos for Stem-Cell Research] 1) No. 55/1996 1) Act No. 27/2008, Article 9 as amended by Act No. 65/2006, Act No. 27/2008, Act No. 54/2008,
NICE fertility guidelines. Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic
 NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
Fertility treatment and referral criteria for tertiary level assisted conception
 Fertility treatment and referral criteria for tertiary level assisted conception Version Number Name of Originator/Author Cross Reference V2 East of England Consortium Commissioning Policy for Fertility
Fertility treatment and referral criteria for tertiary level assisted conception Version Number Name of Originator/Author Cross Reference V2 East of England Consortium Commissioning Policy for Fertility
The Healthy Indiana Plan
 The Healthy Indiana Plan House Enrolled Act 1678 A Pragmatic Approach Governor Mitch Daniels July 16, 2007 Indiana s Fiscal Health is Good First Back-to-Back Balanced Budget in Eight Years $1,000.0 Revenue
The Healthy Indiana Plan House Enrolled Act 1678 A Pragmatic Approach Governor Mitch Daniels July 16, 2007 Indiana s Fiscal Health is Good First Back-to-Back Balanced Budget in Eight Years $1,000.0 Revenue
Submission to the Commission on Assisted Human Reproduction December 2001
 Submission to the Commission on Assisted Human Reproduction December 2001 We believe that the following core principles should govern public policy related to Assisted Human Reproduction: 1. Assisted human
Submission to the Commission on Assisted Human Reproduction December 2001 We believe that the following core principles should govern public policy related to Assisted Human Reproduction: 1. Assisted human
Assisted Conception Policy
 Assisted Conception Policy NHS Eligibility Criteria for assisted conception services (excluding In vitro fertilisation (IVF) Intracytoplasmic sperm injection (ICSI) treatment) for people with infertility
Assisted Conception Policy NHS Eligibility Criteria for assisted conception services (excluding In vitro fertilisation (IVF) Intracytoplasmic sperm injection (ICSI) treatment) for people with infertility
Haringey CCG Fertility Policy April 2014
 Haringey CCG Fertility Policy April 2014 1 SUMMARY This policy describes the clinical pathways and entry criteria for Haringey patients wishing to access NHS funded fertility treatment. 2 RESPONSIBLE PERSON:
Haringey CCG Fertility Policy April 2014 1 SUMMARY This policy describes the clinical pathways and entry criteria for Haringey patients wishing to access NHS funded fertility treatment. 2 RESPONSIBLE PERSON:
GROUND. Fertile. On rare occasions, self-insured programs carry
 Fertile GROUND Infertility benefits help prevent multiple births and manage costly treatments, but also elevate recruitment and retention On rare occasions, self-insured programs carry almost equal weight
Fertile GROUND Infertility benefits help prevent multiple births and manage costly treatments, but also elevate recruitment and retention On rare occasions, self-insured programs carry almost equal weight
Did the US infertility insurance mandates affect the time of firs
 Did the US infertility insurance mandates affect the time of first birth? Department of Economics University of Warwick January 13, 2010 Motivation and Research Summary Impaired fecundity affects 7.3 million
Did the US infertility insurance mandates affect the time of first birth? Department of Economics University of Warwick January 13, 2010 Motivation and Research Summary Impaired fecundity affects 7.3 million
WHO ARE THE DONORS? - An HFEA Analysis of donor registrations and use of donor gametes over the last 10 years
 WHO ARE THE DONORS? - An HFEA Analysis of donor registrations and use of donor gametes over the last 10 years Page 1 of 9 05/29501 Trends in the use of donor gametes (sperm and eggs) Donor assisted conception
WHO ARE THE DONORS? - An HFEA Analysis of donor registrations and use of donor gametes over the last 10 years Page 1 of 9 05/29501 Trends in the use of donor gametes (sperm and eggs) Donor assisted conception
LEGAL CONSIDERATIONS
 LEGAL CONSIDERATIONS As part of the egg donation process, you will be required to sign an agreement between yourself and the prospective parents. If you are doing an anonymous donation, we will keep your
LEGAL CONSIDERATIONS As part of the egg donation process, you will be required to sign an agreement between yourself and the prospective parents. If you are doing an anonymous donation, we will keep your
Intrauterine (IUI) and Donor Insemination (DI) Policy (excluding In vitro fertilisation (IVF) & Intracytoplasmic sperm injection (ICSI) treatment)
 Leicester City Clinical Commissioning Group West Leicestershire Clinical Commissioning Group East Leicestershire and Rutland Clinical Commissioning Group POLICY DOCUMENT Intrauterine (IUI) and Donor Insemination
Leicester City Clinical Commissioning Group West Leicestershire Clinical Commissioning Group East Leicestershire and Rutland Clinical Commissioning Group POLICY DOCUMENT Intrauterine (IUI) and Donor Insemination
Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur?
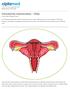 Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
East and North Hertfordshire CCG. Fertility treatment and referral criteria for tertiary level assisted conception
 East and North Hertfordshire CCG Fertility treatment and referral criteria for tertiary level assisted conception December 2015 1 1. Introduction This policy sets out the entitlement and service that will
East and North Hertfordshire CCG Fertility treatment and referral criteria for tertiary level assisted conception December 2015 1 1. Introduction This policy sets out the entitlement and service that will
Fertility Policy. December Introduction
 Fertility Policy December 2015 Introduction Camden Clinical Commissioning Group (CCG) is responsible for commissioning a range of health services including hospital, mental health and community services
Fertility Policy December 2015 Introduction Camden Clinical Commissioning Group (CCG) is responsible for commissioning a range of health services including hospital, mental health and community services
The indicators studied in this report are shaped by a broad range of factors, many of which are determined by
 Health Care Payments and Workforce The indicators studied in this report are shaped by a broad range of factors, many of which are determined by policies made at the state level. State-level policies help
Health Care Payments and Workforce The indicators studied in this report are shaped by a broad range of factors, many of which are determined by policies made at the state level. State-level policies help
WHAT IS A PATIENT CARE ADVOCATE?
 WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
Policy statement. Fertility treatments. This policy is unchanged from the version approved by the CCG in July 2014.
 Policy statement Fertility treatments This policy is unchanged from the version approved by the CCG in July 2014. Title Policy statement: Fertility treatments v2.0 Author Jacky Walters Approved by Kingston
Policy statement Fertility treatments This policy is unchanged from the version approved by the CCG in July 2014. Title Policy statement: Fertility treatments v2.0 Author Jacky Walters Approved by Kingston
The Science and Psychology of Infertility
 University of Massachusetts Medical School escholarship@umms Women s Health Research Faculty Publications Women's Faculty Committee 6-25-2014 The Science and Psychology of Infertility Julia V. Johnson
University of Massachusetts Medical School escholarship@umms Women s Health Research Faculty Publications Women's Faculty Committee 6-25-2014 The Science and Psychology of Infertility Julia V. Johnson
DRAFT: PLEASE DO NOT CITE OR QUOTE WITHOUT PERMISSION OF AUTHORS
 The Supply of and Demand for Assisted Reproductive Technologies in the United States: Clinic and Population Based Data, 1995-2010 *Elizabeth Hervey Stephen, Ph.D., Georgetown University Anjani Chandra,
The Supply of and Demand for Assisted Reproductive Technologies in the United States: Clinic and Population Based Data, 1995-2010 *Elizabeth Hervey Stephen, Ph.D., Georgetown University Anjani Chandra,
Policy updated: November 2018 (approved by Haringey and Islington s Executive Management Team on 5 December 2018)
 Islington CCG Fertility Policy First approved: 29 January 2015 Policy updated: November 2018 (approved by Haringey and Islington s Executive Management Team on 5 December 2018) Introduction Islington CCG
Islington CCG Fertility Policy First approved: 29 January 2015 Policy updated: November 2018 (approved by Haringey and Islington s Executive Management Team on 5 December 2018) Introduction Islington CCG
HIP Year 2020 Health Objectives related to Perinatal Health:
 PERINATAL HEALTH Perinatal health is the health and wellbeing of mothers and babies before, during, and after child birth. As described by Healthy People 2020, Pregnancy can provide an opportunity to identify
PERINATAL HEALTH Perinatal health is the health and wellbeing of mothers and babies before, during, and after child birth. As described by Healthy People 2020, Pregnancy can provide an opportunity to identify
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES V2.
 COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES V2.3 2017 Agreed at Cannock Chase CCG Signature: Designation: Chair of
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES V2.3 2017 Agreed at Cannock Chase CCG Signature: Designation: Chair of
Approved January Waltham Forest CCG Fertility policy
 Approved January 2015 Waltham Forest CCG Fertility policy Contents 1 Introduction 1 2 Individual Funding Requests 1 2.1 Eligibility criteria 1 2.2 Number of cycles funded 2 2.3 Treatment Pathway 3 Page
Approved January 2015 Waltham Forest CCG Fertility policy Contents 1 Introduction 1 2 Individual Funding Requests 1 2.1 Eligibility criteria 1 2.2 Number of cycles funded 2 2.3 Treatment Pathway 3 Page
Motherhood and Female Labor Force Participation: Evidence from Infertility Shocks
 Motherhood and Female Labor Force Participation: Evidence from Infertility Shocks Jorge M. Agüero Univ. of California, Riverside jorge.aguero@ucr.edu Mindy S. Marks Univ. of California, Riverside mindy.marks@ucr.edu
Motherhood and Female Labor Force Participation: Evidence from Infertility Shocks Jorge M. Agüero Univ. of California, Riverside jorge.aguero@ucr.edu Mindy S. Marks Univ. of California, Riverside mindy.marks@ucr.edu
Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition
 Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition Patient Name (please print) Patient DOB (MM/DD/YYYY) Patient eivf number Partner
Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition Patient Name (please print) Patient DOB (MM/DD/YYYY) Patient eivf number Partner
SUBFERTILITY. (Defined as involuntary failure to conceive within 12 months with regular coitus)
 SUBFERTILITY (Defined as involuntary failure to conceive within 12 months with regular coitus) Clients attending with fertility concerns should have a medical, drug, menstrual, contraception, social and
SUBFERTILITY (Defined as involuntary failure to conceive within 12 months with regular coitus) Clients attending with fertility concerns should have a medical, drug, menstrual, contraception, social and
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES
 COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES Version number V2.3 Responsible individual Author(s) Barry Weaver Trish
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES Version number V2.3 Responsible individual Author(s) Barry Weaver Trish
NBER WORKING PAPER SERIES DO MARKETS RESPOND TO QUALITY INFORMATION? THE CASE OF FERTILITY CLINICS
 NBER WORKING PAPER SERIES DO MARKETS RESPOND TO QUALITY INFORMATION? THE CASE OF FERTILITY CLINICS M. Kate Bundorf Natalie Chun Gopi Shah Goda Daniel P. Kessler Working Paper 13888 http://www.nber.org/papers/w13888
NBER WORKING PAPER SERIES DO MARKETS RESPOND TO QUALITY INFORMATION? THE CASE OF FERTILITY CLINICS M. Kate Bundorf Natalie Chun Gopi Shah Goda Daniel P. Kessler Working Paper 13888 http://www.nber.org/papers/w13888
DESTINATION :FAMILY. Reproductive Services TABLE OF CONTENTS
 DESTINATION :FAMILY Reproductive Services TABLE OF CONTENTS Which doctor should I choose? What resources are available to help me? What is covered? How will I afford treatment? What can I do to help prepare
DESTINATION :FAMILY Reproductive Services TABLE OF CONTENTS Which doctor should I choose? What resources are available to help me? What is covered? How will I afford treatment? What can I do to help prepare
Minnesota Journal of Law, Science & Technology. Valarie Blake. Volume 12 Issue 2 Article 9
 Minnesota Journal of Law, Science & Technology Volume 12 Issue 2 Article 9 2011 It's an ART not a Science: State-Mandated Insurance Coverage of Assisted Reproductive Technologies and Legal Implications
Minnesota Journal of Law, Science & Technology Volume 12 Issue 2 Article 9 2011 It's an ART not a Science: State-Mandated Insurance Coverage of Assisted Reproductive Technologies and Legal Implications
College of Physicians and Surgeons of Saskatchewan STANDARDS. Assisted Reproductive Technology PREAMBLE
 College of Physicians and Surgeons of Saskatchewan STANDARDS Assisted Reproductive Technology STATUS: UNDER REVIEW Approved by Council: September 2012 Amended: November 2015 To be reviewed: November 2020
College of Physicians and Surgeons of Saskatchewan STANDARDS Assisted Reproductive Technology STATUS: UNDER REVIEW Approved by Council: September 2012 Amended: November 2015 To be reviewed: November 2020
Family Planning and the LGBTQ Community
 Family Planning and the LGBTQ Community Adarsh E. Krishen, MD, MMM, FAAFP Chief Medical Officer Brian W. Lutz Community Health Educator Andrew E. Kohn, JD Copywriter, Marketing and Communications Conflict
Family Planning and the LGBTQ Community Adarsh E. Krishen, MD, MMM, FAAFP Chief Medical Officer Brian W. Lutz Community Health Educator Andrew E. Kohn, JD Copywriter, Marketing and Communications Conflict
Society for Assisted Reproductive Technology and American Society for Reproductive Medicine
 FERTILITY AND STERILITY VOL. 74, NO. 4, OCTOBER 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. ASRM/SART REGISTRY
FERTILITY AND STERILITY VOL. 74, NO. 4, OCTOBER 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. ASRM/SART REGISTRY
Does Male Education Affect Fertility? Evidence from Mali
 Does Male Education Affect Fertility? Evidence from Mali Raphael Godefroy (University of Montreal) Joshua Lewis (University of Montreal) April 6, 2018 Abstract This paper studies how school access affects
Does Male Education Affect Fertility? Evidence from Mali Raphael Godefroy (University of Montreal) Joshua Lewis (University of Montreal) April 6, 2018 Abstract This paper studies how school access affects
Fertility Services Commissioning Policy
 Fertility Services Commissioning Policy Author: Commissioning Team Version No: Two Policy Effective From: 29 September 2016 Review Date: September 2017 Policy Amendment: 02 August 2017 Document Reader
Fertility Services Commissioning Policy Author: Commissioning Team Version No: Two Policy Effective From: 29 September 2016 Review Date: September 2017 Policy Amendment: 02 August 2017 Document Reader
What are the various Motives for Patients to Travel? -Dr Samit Sekhar Executive Director
 What are the various Motives for Patients to Travel? -Dr Samit Sekhar Executive Director Reproductive Tourism Assisted reproductive technology (ART) lures people across borders. The willingness to travel
What are the various Motives for Patients to Travel? -Dr Samit Sekhar Executive Director Reproductive Tourism Assisted reproductive technology (ART) lures people across borders. The willingness to travel
THE CENTER FOR ADVANCED REPRODUCTIVE SERVICES (CARS) (The Center) CONSENT TO PERFORM THERAPEUTIC DONOR INSEMINATION WITH IDENTIFIED DONOR SPERM
 THE CENTER FOR ADVANCED REPRODUCTIVE SERVICES (CARS) (The Center) CONSENT TO PERFORM THERAPEUTIC DONOR INSEMINATION WITH IDENTIFIED DONOR SPERM Partner #1 Last Name (Surname): Partner #1 First Name: Partner
THE CENTER FOR ADVANCED REPRODUCTIVE SERVICES (CARS) (The Center) CONSENT TO PERFORM THERAPEUTIC DONOR INSEMINATION WITH IDENTIFIED DONOR SPERM Partner #1 Last Name (Surname): Partner #1 First Name: Partner
Incomplete working draft, please do not quote without authors permission
 Will fertility of Danish women remain stable due to assisted reproduction? Assessing the role of assisted reproduction in sustaining cohort fertility rates Incomplete working draft, please do not quote
Will fertility of Danish women remain stable due to assisted reproduction? Assessing the role of assisted reproduction in sustaining cohort fertility rates Incomplete working draft, please do not quote
North Staffordshire Clinical Commissioning Group. Infertility and Assisted Reproduction Commissioning Policy and Eligibility Criteria
 North Staffordshire Clinical Commissioning Group Infertility and Assisted Reproduction Commissioning Policy and Eligibility Criteria Policy Infertility and Assisted Reproduction Commissioning Policy and
North Staffordshire Clinical Commissioning Group Infertility and Assisted Reproduction Commissioning Policy and Eligibility Criteria Policy Infertility and Assisted Reproduction Commissioning Policy and
Wiltshire CCG Fertility Policy
 Wiltshire CCG Fertility Policy Introduction This policy sets out the limits within which WCCG will fund treatment with either Intrauterine Insemination [IUI], ovulation induction medication or donor insemination
Wiltshire CCG Fertility Policy Introduction This policy sets out the limits within which WCCG will fund treatment with either Intrauterine Insemination [IUI], ovulation induction medication or donor insemination
Bromley CCG Assisted Conception Funding Form Checklist for Eligibility Criteria for NHS funding of Assisted Conception
 Bromley CCG Assisted Conception Funding Form Checklist for Eligibility Criteria for NHS funding of Assisted Conception This form is for the use of administrators of Assisted Conception Units to notify
Bromley CCG Assisted Conception Funding Form Checklist for Eligibility Criteria for NHS funding of Assisted Conception This form is for the use of administrators of Assisted Conception Units to notify
REFERENCE TITLE: health insurance; infertility coverage SB 1149
 REFERENCE TITLE: health insurance; infertility coverage State of Arizona Senate Fifty-third Legislature Second Regular Session SB Introduced by Senators Bradley: Cajero Bedford, Dalessandro, Hobbs, Miranda,
REFERENCE TITLE: health insurance; infertility coverage State of Arizona Senate Fifty-third Legislature Second Regular Session SB Introduced by Senators Bradley: Cajero Bedford, Dalessandro, Hobbs, Miranda,
Perinatal Health in the Rural United States, 2005
 Perinatal Health in the Rural United States, 2005 Policy Brief Series #138: LOW BIRTH WEIGHT RATES IN THE RURAL UNITED STATES, 2005 #139: LOW BIRTH WEIGHT RATES AMONG RACIAL AND ETHNIC GROUPS IN THE RURAL
Perinatal Health in the Rural United States, 2005 Policy Brief Series #138: LOW BIRTH WEIGHT RATES IN THE RURAL UNITED STATES, 2005 #139: LOW BIRTH WEIGHT RATES AMONG RACIAL AND ETHNIC GROUPS IN THE RURAL
THE CENTER FOR ADVANCED REPRODUCTIVE SERVICES (CARS) (The Center) CONSENT TO PERFORM THERAPEUTIC DONOR INSEMINATION WITH ANONYMOUS DONOR SPERM
 THE CENTER FOR ADVANCED REPRODUCTIVE SERVICES (CARS) (The Center) CONSENT TO PERFORM THERAPEUTIC DONOR INSEMINATION WITH ANONYMOUS DONOR SPERM Partner #1 Last Name (Surname): Partner #1 First Name: Partner
THE CENTER FOR ADVANCED REPRODUCTIVE SERVICES (CARS) (The Center) CONSENT TO PERFORM THERAPEUTIC DONOR INSEMINATION WITH ANONYMOUS DONOR SPERM Partner #1 Last Name (Surname): Partner #1 First Name: Partner
Fertility treatment and referral criteria for tertiary level assisted conception
 Fertility treatment and referral criteria for tertiary level assisted conception Version Number 2.0 Ratified by HVCCG Exec Team Date Ratified 9 th November 2017 Name of Originator/Author Dr Raj Nagaraj
Fertility treatment and referral criteria for tertiary level assisted conception Version Number 2.0 Ratified by HVCCG Exec Team Date Ratified 9 th November 2017 Name of Originator/Author Dr Raj Nagaraj
PLAN DESIGN. Customer Name: High Desert & Inland Employee-Employer Trust. Effective Date: Plan: HMO Plan. Location(s): California
 PLAN DESIGN Customer Name: High Desert & Inland Employee-Employer Trust Plan: HMO Plan Location(s): California Organization Name: Aetna PLAN FEATURES Deductible (per calendar year) Out-of-Pocket Maximum
PLAN DESIGN Customer Name: High Desert & Inland Employee-Employer Trust Plan: HMO Plan Location(s): California Organization Name: Aetna PLAN FEATURES Deductible (per calendar year) Out-of-Pocket Maximum
HEALTH & WELL-BEING TOP LINE FINDINGS
 Health & Well-Being Reproductive Rights Violence & Safety KEY FINDINGS HEALTH & WELL-BEING TOP LINE FINDINGS Nationally, women s health status has improved in four areas and worsened in five: o Improved:
Health & Well-Being Reproductive Rights Violence & Safety KEY FINDINGS HEALTH & WELL-BEING TOP LINE FINDINGS Nationally, women s health status has improved in four areas and worsened in five: o Improved:
JAWDA Quarterly & Yearly Guidelines for Assisted Reproductive Technology Treatment (ART) Providers January 2019
 JAWDA Quarterly & Yearly Guidelines for Assisted Reproductive Technology Treatment (ART) Providers January 2019 Page 1 Table of Contents Executive Summary... 3 About this Guidance... 4 Glossary:... 5 ART
JAWDA Quarterly & Yearly Guidelines for Assisted Reproductive Technology Treatment (ART) Providers January 2019 Page 1 Table of Contents Executive Summary... 3 About this Guidance... 4 Glossary:... 5 ART
Possibilities Plan. Access to the care you need.
 Possibilities Plan If you do not have insurance or have insurance but lack coverage for infertility services and are concerned about the cost of infertility services, The Center for Advanced Reproductive
Possibilities Plan If you do not have insurance or have insurance but lack coverage for infertility services and are concerned about the cost of infertility services, The Center for Advanced Reproductive
Access to IVF. Help us decide Discussion paper. South Central Specialised Commissioning Group C - 1
 Access to IVF Help us decide Discussion paper South Central Specialised Commissioning Group 1 C - 1 Access to IVF treatment Contents 1. Background 3 2. Developing a single policy for NHS South Central..4
Access to IVF Help us decide Discussion paper South Central Specialised Commissioning Group 1 C - 1 Access to IVF treatment Contents 1. Background 3 2. Developing a single policy for NHS South Central..4
50-STATE REPORT CARD
 JANUARY 2014 The State of Reproductive Health and Rights: 50-STATE REPORT CARD U.S. REPRODUCTIVE HEALTH AND RIGHTS AT A CROSSROADS The status of reproductive health and rights in the U.S. is at an historic
JANUARY 2014 The State of Reproductive Health and Rights: 50-STATE REPORT CARD U.S. REPRODUCTIVE HEALTH AND RIGHTS AT A CROSSROADS The status of reproductive health and rights in the U.S. is at an historic
Subject to Routine Physical Exam benefit. Same as applicable participating provider office visit member cost sharing Allergy Testing
 PLAN FEATURES Deductible (per calendar year) Out-of-Pocket Maximum (per calendar year) None Individual None Family $2,000 Individual $4,000 Family Member cost sharing for certain services may not apply
PLAN FEATURES Deductible (per calendar year) Out-of-Pocket Maximum (per calendar year) None Individual None Family $2,000 Individual $4,000 Family Member cost sharing for certain services may not apply
Guide to Good Practice in fertility cases
 2018 Guide to Good Practice in fertility cases This Guidance was reviewed in March 2018. The law or procedure may have changed since that time and members should check the up-to-date position. Resolution
2018 Guide to Good Practice in fertility cases This Guidance was reviewed in March 2018. The law or procedure may have changed since that time and members should check the up-to-date position. Resolution
DIABLO VALLEY ESTATE PLANNING COUNCIL THE NEW BIOLOGY: WHAT DO ESTATE PLANNERS NEED TO KNOW ABOUT ASSISTED REPRODUCTION OCTOBER 15, 2014
 DIABLO VALLEY ESTATE PLANNING COUNCIL THE NEW BIOLOGY: WHAT DO ESTATE PLANNERS NEED TO KNOW ABOUT ASSISTED REPRODUCTION OCTOBER 15, 2014 Lisa C. Ikemoto Professor U.C. Davis School of Law APPROACH Assisted
DIABLO VALLEY ESTATE PLANNING COUNCIL THE NEW BIOLOGY: WHAT DO ESTATE PLANNERS NEED TO KNOW ABOUT ASSISTED REPRODUCTION OCTOBER 15, 2014 Lisa C. Ikemoto Professor U.C. Davis School of Law APPROACH Assisted
Health Care Reform: Colorectal Cancer Screening Disparities, Before and After the Affordable Care Act (ACA)
 University of Arkansas for Medical Sciences From the SelectedWorks of Michael Preston June 7, 2014 Health Care Reform: Colorectal Cancer Screening Disparities, Before and After the Affordable Care Act
University of Arkansas for Medical Sciences From the SelectedWorks of Michael Preston June 7, 2014 Health Care Reform: Colorectal Cancer Screening Disparities, Before and After the Affordable Care Act
Health Care Reform: Colorectal Cancer Screening Expansion, Before and After the Affordable Care Act (ACA)
 University of Arkansas for Medical Sciences From the SelectedWorks of Michael Preston April 9, 2014 Health Care Reform: Colorectal Cancer Screening Expansion, Before and After the Affordable Care Act (ACA)
University of Arkansas for Medical Sciences From the SelectedWorks of Michael Preston April 9, 2014 Health Care Reform: Colorectal Cancer Screening Expansion, Before and After the Affordable Care Act (ACA)
Recent Developments in Infertility Treatment
 Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Chapter 7 Infertility, Contraception, and Abortion
 Chapter 7 Infertility, Contraception, and Abortion Infertility Incidence Affects about 10% to 15% of reproductive-age population Subfertility: prolonged time to conceive Sterility: inability to conceive
Chapter 7 Infertility, Contraception, and Abortion Infertility Incidence Affects about 10% to 15% of reproductive-age population Subfertility: prolonged time to conceive Sterility: inability to conceive
Fertility Services Commissioning Policy (Level 3)
 Fertility Services Commissioning Policy (Level 3) Author: Karin Bryant (Norwich CCG) has coordinated the refresh of policy Version No: V54 Policy Effective from: TBC Review Date: TBC This policy replaces
Fertility Services Commissioning Policy (Level 3) Author: Karin Bryant (Norwich CCG) has coordinated the refresh of policy Version No: V54 Policy Effective from: TBC Review Date: TBC This policy replaces
FERTILITY SERVICE POLICY
 FERTILITY SERVICE POLICY Page 1 of 8 FERTILITY SERVICE POLICY Please note that all Clinical Commissioning policies are currently under review and elements within the individual policies may have been replaced
FERTILITY SERVICE POLICY Page 1 of 8 FERTILITY SERVICE POLICY Please note that all Clinical Commissioning policies are currently under review and elements within the individual policies may have been replaced
Note: This updated policy supersedes all previous fertility policies and reflects changes agreed by BHR CCGs governing bodies in June 2017.
 Fertility Policy 10 July 2017 Note: This updated policy supersedes all previous fertility policies and reflects changes agreed by BHR CCGs governing bodies in June 2017. Introduction BHR CCGs are responsible
Fertility Policy 10 July 2017 Note: This updated policy supersedes all previous fertility policies and reflects changes agreed by BHR CCGs governing bodies in June 2017. Introduction BHR CCGs are responsible
The Gay Woman s Guide to Becoming a Mom PATH2PARENTHOOD. path2parenthood.org
 The Gay Woman s Guide to Becoming a Mom PATH2PARENTHOOD path2parenthood.org For lesbians, there are a number of viable routes that can be considered when achieving motherhood is the goal. Whether you are
The Gay Woman s Guide to Becoming a Mom PATH2PARENTHOOD path2parenthood.org For lesbians, there are a number of viable routes that can be considered when achieving motherhood is the goal. Whether you are
Infertility. F r e q u e n t l y A s k e d Q u e s t i o n s. Q: What causes infertility in men? A: Infertility in men is most often caused by:
 Infertility Q: What is infertility? A: Infertility means not being able to get pregnant after one year of trying. Or, six months, if a woman is 35 or older. Women who can get pregnant but are unable to
Infertility Q: What is infertility? A: Infertility means not being able to get pregnant after one year of trying. Or, six months, if a woman is 35 or older. Women who can get pregnant but are unable to
