Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate
|
|
|
- Katherine Reed
- 5 years ago
- Views:
Transcription
1 Singapore Med J 2016; 57(12): doi: /smedj Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate Sundaram Palaniappan 1, MBBS, Tricia Li Chuen Kuo 1, MBBS, FAMS, Christopher Wai Sam Cheng 1, FRCS, FAMS, Keong Tatt Foo 1, FRCS, FAMS INTRODUCTION Recurrent prostate adenoma is a long-term complication following transurethral resection of the prostate (TURP). Transurethral enucleation and resection of the prostate (TUERP) is more appealing, since the nodular adenoma can be completely removed through endoscopy. TUERP is also hypothesised to result in a lower frequency of recurrent adenoma. This study aimed to compare the early outcomes of TUERP and TURP, and assess the feasibility and safety of TUERP. METHODS We compared the outcome of 81 patients who underwent TUERP with that of 85 patients who underwent TURP. International prostate symptom score, quality of life score, prostate volume, degree of intravesical prostatic protrusion, maximum flow rate, post-void residual volume and prostate-specific antigen (PSA) level were obtained pre- and postoperatively. Complications (e.g. transfusion rate, incontinence, infection and urethral stricture) were analysed. RESULTS Operative time was significantly longer in the TUERP group compared to the TURP group (85.3 minutes vs minutes). After TUERP, the maximum flow rate was significantly higher (21.1 ml/s vs ml/s) and PSA level was significantly lower (1.2 ng/ml vs. 1.9 ng/ml) than after TURP. The rates of infection, transfusion and urethral stricture were similar for both groups, but the TUERP group had a higher rate of temporary incontinence (13.6% vs. 4.7%). CONCLUSION The lower PSA level and better maximum flow rate achieved following TUERP suggest that prostate adenoma removal was more complete with TUERP. Long-term follow-up is required to establish whether TUERP results in fewer resections for recurrent adenoma. Keywords: benign prostatic hyperplasia, transurethral enucleation and resection of prostate, transurethral resection of prostate INTRODUCTION Transurethral resection of the prostate (TURP) is the established gold standard surgical treatment for benign prostatic hyperplasia (BPH). In the last few years, we have seen a growing number of minimally invasive procedures being developed to treat BPH; these procedures, which are based on different technologies, aim to minimise morbidity while still maintaining the efficacy of TURP. Rassweiler et al reported that the number of complications associated with TURP (e.g. clot retention, urinary tract infection and the need for blood transfusion) has declined over the years, and that transurethral resection syndrome is rare in clinical practice these days due to the advent of bipolar TURP, which allows for resection of the prostate with normal saline irrigation. (1) However, the authors also highlighted that 3% 15% of patients required intervention five years after TURP for recurrence of BPH. (1) This is likely due to inadequate resection of the large prostate adenoma during initial surgery. In addition, TURP for large glands results in significantly more bleeding and clot retention as compared to open prostatectomy. It also requires a longer resection time, which leads to a higher risk of transurethral resection syndrome and substantial morbidity. (2,3) For the aforementioned reasons, the guidelines published by the European Association of Urology recommend open prostatectomy over TURP in managing symptomatic large prostates (i.e. > g). (4) However, as open prostatectomy necessitates a lower abdominal incision, this may result in greater morbidity, a longer hospital stay and an extended recovery period. This problem led to the development of a new technique, in which the practice of enucleation is adapted from open prostatectomy and incorporated into transurethral resection. This technique was first described in 1989 by Hiraoka and Akimoto, who used the tip of the resectoscope and a prostate-detaching blade to enucleate the prostate prior to its resection. (5) This was then followed by a study by Liu et al in 2006, in which the authors performed a similar procedure using a bipolar resectoscope and no other additional equipment. (6) The aim of the present study was to assess whether this new technique, termed transurethral enucleation and resection of the prostate (TUERP), was feasible, as well as to compare the early outcome of TUERP versus TURP. METHODS We retrospectively reviewed 81 consecutive patients who underwent TUERP (i.e. TUERP group) at the Department of Urology, Singapore General Hospital, Singapore, between March 2008 and January This cohort of patients was compared with 85 consecutive patients who underwent TURP (i.e. TURP group) in the same hospital between January 2006 and February Department of Urology, Singapore General Hospital, Singapore Correspondence: Dr Sundaram Palaniappan, Registrar, Department of Urology, Singapore General Hospital, 20 College Road, Academia Level 5, Singapore palaniappan.sundaram@sgh.com.sg 676
2 Patients who had prostate cancer, neurogenic bladder and/or previous urethral or prostate surgery were excluded. The use of the BPH registry was approved by the Institutional Review Board of Singapore General Hospital. All 166 patients had voiding symptoms that were attributed to BPH. The diagnosis was confirmed after detailed history was taken and physical examinations, which included a digital rectal examination and transabdominal ultrasonography (TAUS), were performed. International prostate symptom score (IPSS) was used to grade the severity of the patient s voiding symptoms and assess the impact of the symptoms on the patient s quality of life (QOL). Uroflowmetry was done to measure the maximum flow rate (Qmax), and TAUS was performed to measure the prostate volume (PV), degree of intravesical prostatic protrusion (IPP) and post-void residual urine volume (PVR). Pre- and postoperative (six weeks after surgery) assessment of the PV was conducted by the same surgeon. PV was calculated using the ellipsoid formula (i.e. volume was calculated after the anteroposterior distance, transverse width and cephalocaudal height had been multiplied by 0.52). PV measurement was performed when the bladder was reasonably filled (i.e ml), as this has been shown to correlate well with transrectal PV measurement in a previous study. (7) Indications for surgery included acute retention of urine, chronic retention, recurrent haematuria due to BPH, urinary tract infection and bladder stones secondary to BPH, failure of medical treatment, and significant obstruction. A patient was deemed to have significant obstruction if the PVR was persistently > 100 ml, (8) usually with a reduced Qmax (i.e. < 10 ml/s). The following outcomes were measured in both groups of patients: time taken for resection of the prostate; weight of the resected prostate; number of days on bladder irrigation; number of days with indwelling catheter; and length of hospital stay. Postoperative IPSS, QOL score, Qmax, PVR, PV and serum prostate-specific antigen (PSA) level were measured during the patient s first follow-up visit to the clinic (six weeks after surgery). Patients were followed up for a variable length of time, depending on their symptoms, but the majority had at least six months of follow-up after discharge. Adverse events, such as the need for blood transfusion, sepsis following surgery, urethral stricture and urinary incontinence, were recorded. Further need for prostate surgery was also recorded if the patient re-presented to the surgeon with recurrent voiding symptoms suggestive of prostate adenoma regrowth. Both TURP and TUERP were performed using the plasmakinetic bipolar system with normal saline irrigation, under spinal or general anaesthesia. All surgeries were performed or closely supervised by the same surgeon. Preprogrammed power settings for cutting (180 W) and coagulation (80 W) were used. Preliminary cystoscopy was done using a 20-F-sized sheath, to assess both prostate size and shape, and visualise landmarks (including the two ureteric orifices and the verumontanum). A 26-F-sized resectoscope was then introduced, and the TUERP procedure was performed as described in the following paragraph. The distal margin of the prostate lobes was marked with a cutting loop. Starting with the median lobe, the mark between Table I. Baseline characteristics of the patients who underwent TURP or TUERP. Variable Mean (range) p value TURP group (n = 85) TUERP group (n = 81) Age (yr) 68.3 (50 94) 70.3 (48 92) 0.28 PV (ml) 53.7 (13 152) 53.0 (11 158) 0.87 PSA level (ng/ml) 6.7 ( ) 10.7 ( ) 0.06 IPSS 16.3 (4 35) 13.3 (2 29) 0.05 QOL score 3.6 (1 6) 3.1 (0 6) 0.05 Qmax (ml/s) 9.6 ( ) 7.9 ( ) 0.17 PRV (ml) 91.3 (0 300) (0 300) 0.18 IPSS: international prostate symptom score; PRV: post void residual urine volume; PSA: prostate specific antigen; PV: prostate volume; Qmax: maximum flow rate; QOL: quality of life; TUERP: transurethral enucleation and resection of the prostate; TURP: transurethral resection of the prostate the 5 o clock and 7 o clock positions was deepened, down to the surgical capsule. Next, the incision just proximal to the verumontanum was deepened so that the plane between the adenoma and false capsule (i.e. the compressed normal prostatic tissue) could be identified with a thick resectoscope loop. The tip of the resectoscope was then inserted to further develop this plane. The adenoma was gradually dissected away from the capsule in the avascular plane, toward the bladder neck, until the circular fibres of the bladder neck were seen. The perforating vessels were diathermied at the source and cut. Bleeding points noted during this mechanical dissection were easily controlled with coagulation. The median lobe, which was still attached to the bladder neck, was then resected. The plane between the lateral lobe and false capsule was developed in a similar manner and resected. No morcellator was used. The chips were then evacuated using a bladder evacuator. On completion, a three-way Foley catheter was inserted and continuous bladder irrigation was initiated. Bladder irrigation was kept overnight or until the effluent was clear. Once the irrigation was stopped, the catheter was removed after two days, or when the urine was clear or had only a light pink colouration. The baseline characteristics and perioperative data of the two groups were compared using Student s t-test, while the incidence of postoperative adverse events was compared using chi-square test. A p-value < 0.05 was considered to be statistically significant in all analyses. RESULTS The baseline characteristics of all the patients are shown in Table I. No significant differences were found between the patients in the TURP and TUERP groups in terms of age, PV, PSA level, IPSS, QOL score, Qmax and PVR. Table II shows the perioperative data of the patients. The duration of bladder irrigation was significantly higher for the patients who underwent TURP compared to those who underwent TUERP (1.17 days vs days, p = 0.03); this is likely related to the better haemostasis achieved with the TUERP procedure. However, the duration of indwelling catheter and length of hospital stay were not lower in the TUERP group. Although the weights of 677
3 Table II. Perioperative data of the patients who underwent TURP or TUERP. Variable Mean (range) p value TURP group (n = 85) TUERP group (n = 81) Weight of resected prostate chips (g) 32.2 (2 145) 29.7 (3 73) 0.12 Resection time (min) 51.6 (9 150) 85.3 (20 190) < 0.01* Duration of bladder irrigation (day) 1.17 (0 3) 1.00 (1) 0.03* Duration of indwelling catheter (day) 2.07 (1 7) 2.26 (1 8) 0.27 Length of hospital stay (day) 3.8 (2 11) 3.65 (3 8) 0.15 Postoperative PV (ml) 14.7 (5 41) 14.9 (5 39) 0.67 Postoperative PSA level (ng/ml) 1.9 ( ) 1.2 ( ) 0.01* IPSS 7.1 (1 29) 6.9 (0 25) 0.80 QOL score 1.8 (0 6) 1.5 (0 6) 0.48 Qmax (ml/s) 17.1 ( ) 21.1 ( ) < 0.01* PRV (ml) 27.2 (0 167) 32.5 (0 100) 0.13 *Statistically significant at p < IPSS: international prostate symptom score; PRV: post void residual urine volume; PSA: prostate specific antigen; PV: prostate volume; Qmax: maximum flow rate; QOL: quality of life; TUERP: transurethral enucleation and resection of the prostate; TURP: transurethral resection of the prostate Table III. Complications observed among the patients during the follow up period, according to the type of surgery. Variable No. (%) p value TURP (n = 85) TUERP (n = 81) Blood transfusion 2 (2.4) 3 (3.7) 0.68 Urinary sepsis 2 (2.4) 1 (1.2) 1.00 Urethral stricture 5 (5.9) 2 (2.5) 0.44 Incontinence 4 (4.7) 11 (13.6) 0.06 TUERP: transurethral enucleation and resection of the prostate; TURP: transurethral resection of the prostate prostate chips resected from the patients in the TUERP and TURP groups were similar (29.7 g vs g, p = 0.12), the resection time was found to be significantly longer for the TUERP group (85.3 minutes vs minutes, p < 0.01). The longer resection time may be due to the steep learning curve associated with any new surgical procedure. No statistical difference was noted between the two groups in terms of the patients postoperative IPSS, QOL score, PVR and PV. The postoperative serum PSA level was significantly higher in the TURP group than in the TUERP group (1.9 ng/ml vs. 1.2 ng/ml, p = 0.01) and improvement in Qmax was significantly better for the TUERP group (21.1 ml/s vs ml/s, p < 0.01). The median duration of follow-up for the patients in the TURP group was 8 (range 2 108) months, while the corresponding duration for the patients in the TUERP group was 11 (range 2 85) months. The complications observed during the follow-up period are shown in Table III. No significant difference was found between the two groups in terms of the rates of transfusion, urethral stricture and urinary sepsis. Even though the number of patients with urinary incontinence was higher in the TUERP group than in the TURP group (11 vs. four), this difference was not statistically significant. The incontinence was commonly urge-related and transient in all cases, with all of the patients showing gradual improvement over six months. In addition, the urge incontinence could have been secondary to preoperative benign prostatic obstruction; storage symptoms arising from this cause have been known to improve gradually after surgery. DISCUSSION The evolution of TURP to include enucleation was deemed necessary, as TURP had a higher re-operation rate than open prostatectomy. Between 12% and 15.5% of patients who underwent TURP required a second operation, while only 1.8% 4.5% of patients who underwent open prostatectomy required a second one. (9) This difference could be related to the inadequate excision of the prostate adenoma in TURP as compared to open prostatectomy. Transurethral enucleation of the prostate was first developed by Hiraoka and Akimoto; in their described method, a prostate-detaching blade was used to assist in the detachment of the adenoma from the surgical capsule. (5) Neill et al later proposed the use of bipolar plasmakinetic energy as an alternative energy source to enucleate the prostate; this method is similar to holmium laser enucleation of the prostate (HoLEP), (10) a procedure that is becoming established as the endoscopic alternative to open prostatectomy. After enucleation of the adenoma with the holmium laser, the cavity in the prostate is comparable to that achieved after open prostatectomy. According to a meta-analysis, HoLEP is the only minimally invasive procedure that is more efficacious than TURP; recent long-term follow-up data also proved that HoLEP is a durable procedure. (11,12) In a similar manner to holmium energy in enucleation of the prostate adenoma, plasmakinetic energy could be used. The technique used in the present study has been described by Liu et al. In this technique, a plasmakinetic device is exclusively used to perform the procedure from enucleation of the adenoma and coagulation of the bleeding vessels during dissection to resection of the adenoma tissue that is still partially attached to the bladder neck. (6) Liu et al s review of 1,100 patients who underwent this procedure showed improvements in Qmax (to 24.3 ml/s), reduction in PVR and improvement in symptom scores over 4.3 years of follow-up. (6) Recently, another study compared the results of TUERP with TURP and found that patients from both groups had smaller PV (10.5 g vs g) after the procedures; it also found that the postoperative PSA level of patients who underwent TUERP was significantly lower than that of patients who underwent TURP (0.8 ng/ml vs. 2.8 ng/ml); (13) however, 678
4 the patients in the two groups were operated on at different institutions, by different surgeons. In our cohort of patients who underwent surgical management of BPH, there were no significant differences in PV, symptom scores, PSA level, Qmax and PVR. Our results showed that symptomatic improvement (measured using IPSS and QOL score) following TUERP was equivalent to that following TURP. In addition, postoperative PV and PVR (measured during follow-up at the clinic) did not differ significantly between the two groups. This suggests that no significant obstruction was present after TUERP (subjectively, based on the symptom scores, and objectively, based on postoperative PV and PVR). Ultrasonographic assessments of prostate size, intravesical prostatic protrusion and PVR (14,15) are considered to be a surrogate for the degree of bladder outlet obstruction. Postoperative PV is difficult to interpret, as it does not correspond well to the actual residual PV since there is a cavity after prostate resection. This may explain the lack of difference in postoperative PV. Although we did not observe any significant difference in the mean resected volume, this may have been due to the small number of patients in the present study. Moreover, the volume of resected prostate is not as important as the volume of adenoma left behind. In contrast, Qmax was found to be significantly higher in the TUERP group compared to the TURP group (21.1 ml/s vs ml/s, p < 0.01). Uroflowmetry is a more objective way of assessing postoperative obstruction than PVR measurement; this is because PVR may vary significantly due to premicturition volume and the timing of the measurement. Hence, the greater Qmax seen among the patients who underwent TUERP suggests that TUERP was more effective in removing the obstructing adenoma than TURP. The postoperative PSA level of the patients in the TUERP group was significantly lower than that of the patients in the TURP group (1.2 ng/ml vs. 1.9 ng/ml, p = 0.01). Furthermore, the reduction in mean PSA level for the TUERP group was 88.8%, while it was only 71.6% for the TURP group. The raised PSA level seen in BPH is proposed to be due to hyperplasia of the transition zone. Hence, if there was complete resection of the adenoma, the PSA level should return to the normal range (i.e. below 4 ng/ml). (16) Thus, the greater reduction in mean PSA level in the TUERP group indicated that adenoma resection was more complete with TUERP than with TURP. (17) The lower PSA level and higher peak urinary flow can be considered as surrogate markers of complete adenoma removal. However, the most important assessment is whether these patients eventually developed recurrence of the prostate adenoma. This data, however, was not available in the present study due to its short follow-up period. A longer follow-up period (i.e. > 5 years) may be necessary to find out whether there is a difference in the recurrence rates of prostate adenoma between patients who underwent TUERP and those who underwent conventional TURP. In the present study, the time taken for resection was notably longer in TUERP than in TURP. This is not surprising, as TUERP requires time for both enucleation and resection. Furthermore, the patients who underwent TUERP were part of our early experience in this procedure and, hence, there was a relatively steep learning curve associated with the acquisition of the technique for enucleation. The main hurdles include identification of the cleavage plane between the false capsule and adenoma, as well as performing blunt detachment of the adenoma in a retrograde manner (i.e. the crucial steps in TUERP). (18) With experience, the resection time for TUERP should improve. We did not observe any significant increase in the incidence of complications (e.g. blood transfusion, urinary sepsis and urethral stricture) among both groups of patients. However, there was a significantly higher percentage of patients who developed urinary incontinence following TUERP. This could be explained by the need for more extensive dissection around the external sphincter region during the identification of the cleavage plane in TUERP. Both the complete removal of the prostate adenoma and disuse of the external sphincter could have led to the weakening of the external sphincter, leading to incontinence. (19) However, the incontinence was temporary and resolved in all the patients after six months. In terms of adenoma recurrence, both the TUERP and TURP groups had a similar number of patients who presented with recurrence, although the adenoma was not significant enough to warrant a repeat resection. Based on our early experience with TUERP, the ideal or index patient for this procedure would be one whose preoperative assessment showed a prostate size of g on ultrasonography. This is because the plane between the adenoma and false capsule is better defined in a large prostate than in a small one (i.e. < 40 g). A small prostate may have a less well-defined plane, possibly due to chronic inflammation. Large prostates that weigh > 80 g can be challenging, as during enucleation, potential spaces are created, which may cause a beginner to be disorientated. To overcome this problem, the surgeon can resort to enucleation and resection at the same time. There is no real necessity to complete enucleation before resection of the adenoma. In the present study, there were too few patients with a prostate size > 80 g in both groups to make a meaningful comparison. With bipolar resection using normal saline, transurethral resection syndrome is no longer a problem. Even though resection time may be prolonged for large prostates, they can still be operated on. The more immediate advantage of TUERP is that haemostasis can be better achieved, as the perforating vessels are diathermied at the source instead of repeatedly resected (as in conventional TURP). There are limitations to the present study. First, we used a retrospective study design and the analysis was done using a relatively small sample size. Additionally, as the period of follow-up was short, we were unable to comment on the longterm outcomes of TUERP, particularly its effects on prostate adenoma recurrence. Long-term follow-up data was not available for all the patients, as most of the patients who underwent transurethral surgery were discharged from follow-up about six months after surgery. Nevertheless, the present study provides evidence that TUERP is a safe and efficacious treatment option for larger prostates. Undoubtedly, a randomised prospective trial with a longer follow-up period would be useful in determining 679
5 whether patients who undergo TUERP have fewer re-operations than patients who undergo TURP. In the present study, we showed that TUERP has equivalent early outcomes as TURP in terms of symptom improvement and PVR. Patients who underwent TUERP achieved better peak urinary flow and lower postoperative PSA level, suggesting that TUERP results in more complete adenoma removal than TURP. While any attempt to remove a prostate adenoma via endoscopic means such as open simple prostatectomy is fundamentally possible, it remains to be seen whether the procedure results in less adenoma recurrence. Further studies with long-term follow-up are needed to ascertain this. REFERENCES 1. Rassweiler J, Teber D, Kuntz R, Hofmann R. Complications of transurethral resection of the prostate (TURP)--incidence, management, and prevention. Eur Urol 2006; 50:969-79; discussion Persu C, Georgescu D, Arabagiu I, et al. TURP for BPH. How large is too large? J Med Life 2010; 3: Simforoosh N, Abdi H, Kashi AH, et al. Open prostatectomy versus transurethral resection of the prostate, where are we standing in the new era? A randomized controlled trial. Urol J 2010; 7: Gravas S, Bach T, Bachmann A, et al. Guidelines on the management of non-neurogenic male lower urinary tract symptoms (LUTS), incl. benign prostatic obstruction (BPO). In: European Association of Urology [online]. Available at: Non-Neurogenic-Male-LUTS-Guidelines-2015-v2.pdf. Accessed February 1, Hiraoka Y, Akimoto M. Transurethral enucleation of benign prostatic hyperplasia. J Urol 1989; 142: Liu C, Zheng S, Li H, Xu K. Transurethral enucleation and resection of prostate in patients with benign prostatic hyperplasia by plasma kinetics. J Urol 2010; 184: Yuen JS, Ngiap JT, Cheng CW, Foo KT. Effects of bladder volume on transabdominal ultrasound measurements of intravesical prostatic protrusion and volume. Int J Urol 2002; 9: Wang D, Foo KT. Staging of benign prostate hyperplasia is helpful in patients with lower urinary tract symptoms suggestive of benign prostate hyperplasia. Ann Acad Med Singapore 2010; 39: Roos NP, Wennberg JE, Malenka DJ, et al. Mortality and reoperation after open and transurethral resection of the prostate for benign prostatic hyperplasia. N Engl J Med 1989; 320: Neill MG, Gilling PJ, Kennett KM, et al. Randomized trial comparing holmium laser enucleation of prostate with plasmakinetic enucleation of prostate for treatment of benign prostatic hyperplasia. Urology 2006; 68: Tan AH, Gilling PJ, Kennett KM, et al. A randomized trial comparing holmium laser enucleation of the prostate with transurethral resection of the prostate for the treatment of bladder outlet obstruction secondary to benign prostatic hyperplasia in large glands (40 to 200 grams). J Urol 2003; 170: Ahyai SA, Gilling P, Kaplan SA, et al. Meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic enlargement. Eur Urol 2010; 58: Zhang KY, Xing JC, Chen BS, et al. Bipolar plasmakinetic transurethral resection of the prostate vs. transurethral enucleation and resection of the prostate: pre-and postoperative comparisons of parameters used in assessing benign prostatic enlargement. Singapore Med J 2011; 52: Chia SJ, Heng CT, Chan SP, Foo KT. Correlation of intravesical prostatic protrusion with bladder outlet obstruction. BJU Int 2009; 91: Foo KT. Decision making in the management of benign prostatic enlargement and the role of transabdominal ultrasound. Int J Urol 2010; 17: Furuya Y, Akakura K, Tobe T, et al. Changes in serum prostate-specific antigen following prostatectomy in patients with benign prostate hyperplasia. Int J Urol 2000; 7: Tinmouth WW, Habib E, Kim SC, et al. Change in serum prostate specific antigen concentration after holmium laser enucleation of the prostate: a marker for completeness of adenoma resection? J Endourol 2005; 19: Xiong W, Sun M, Ran Q, et al. Learning curve for bipolar transurethral enucleation and resection of the prostate in saline for symptomatic benign prostatic hyperplasia: experience in the first 100 consecutive patients. Urol Int 2013; 90: Shah HN, Mahajan AP, Hegde SS, Bansal MB. Peri-operative complications of holmium laser enucleation of the prostate: experience in the first 280 patients, and a review of literature. BJU Int 2007; 100:
Original Article - Lasers in Urology. Min Ho Lee, Hee Jo Yang, Doo Sang Kim, Chang Ho Lee, Youn Soo Jeon
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
Long-term Follow-up of Transurethral Enucleation Resection of the Prostate for Symptomatic Benign Prostatic Hyperplasia
 Journal of Surgery 2016; 4(2): 40-44 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160402.18 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Long-term Follow-up of Transurethral Enucleation
Journal of Surgery 2016; 4(2): 40-44 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160402.18 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Long-term Follow-up of Transurethral Enucleation
Can men with prostates sized 80 ml or larger be managed conservatively?
 Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP)
 JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
= 0.62, P <0.001) with important clinical exceptions. There was negative correlation between the PV and Qmax (r s
 Original Article 60 Relationships between Prostatic Volume and Intravesical Prostatic Protrusion on Transabdominal Ultrasound and Benign Prostatic Obstruction in Patients with Lower Urinary Tract Symptoms
Original Article 60 Relationships between Prostatic Volume and Intravesical Prostatic Protrusion on Transabdominal Ultrasound and Benign Prostatic Obstruction in Patients with Lower Urinary Tract Symptoms
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
1 Department of Urology, the First Affiliated Hospital of Fujian Medical University, Fuzhou, China
 ORIGINAL ARTICLE Vol. 42 (4): 747-756, July - August, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0225 Bipolar transurethral enucleation and resection of the prostate versus bipolar resection of the prostate
ORIGINAL ARTICLE Vol. 42 (4): 747-756, July - August, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0225 Bipolar transurethral enucleation and resection of the prostate versus bipolar resection of the prostate
Combination of Thulium Laser Incision and Bipolar Resection Offers Higher Resection. Velocity than Bipolar Resection Alone in Large Prostates
 Running Head: combination of thulium laser and bipolar in endoscopic prostatectomy-huang et al. Combination of Thulium Laser Incision and Bipolar Resection Offers Higher Resection Velocity than Bipolar
Running Head: combination of thulium laser and bipolar in endoscopic prostatectomy-huang et al. Combination of Thulium Laser Incision and Bipolar Resection Offers Higher Resection Velocity than Bipolar
Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj
 Original Article Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj Abstract Objectives: Prospective evaluation
Original Article Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj Abstract Objectives: Prospective evaluation
Holmium Laser Enucleation of the Prostate: Modified Morcellation Technique and Results
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.11.779 Voiding Dysfunction Holmium Laser Enucleation of the Prostate: Modified Morcellation Technique and Results Su Hyung Lee, Jong In Choi, Kyung
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.11.779 Voiding Dysfunction Holmium Laser Enucleation of the Prostate: Modified Morcellation Technique and Results Su Hyung Lee, Jong In Choi, Kyung
Benign prostatic hyperplasia (BPH) is one of the
 MISCELLANEOUS Safety and Efficacy of Bipolar Versus Monopolar Transurethral Resection of the Prostate: A Comparative Study Erkan Hirik, 1 Aliseydi Bozkurt, 1 Mehmet Karabakan, 1 * Huseyin Aydemir, 2 Binhan
MISCELLANEOUS Safety and Efficacy of Bipolar Versus Monopolar Transurethral Resection of the Prostate: A Comparative Study Erkan Hirik, 1 Aliseydi Bozkurt, 1 Mehmet Karabakan, 1 * Huseyin Aydemir, 2 Binhan
Biomedical Research 2017; 28 (12):
 Biomedical Research 2017; 28 (12): 5432-5437 ISSN 0970-938X www.biomedres.info A prospective, randomised trial comparing transurethral enucleation with bipolar system (TUEB) to monopolar resectoscope enucleation
Biomedical Research 2017; 28 (12): 5432-5437 ISSN 0970-938X www.biomedres.info A prospective, randomised trial comparing transurethral enucleation with bipolar system (TUEB) to monopolar resectoscope enucleation
Int J Clin Exp Med 2016;9(4): /ISSN: /IJCEM
 Int J Clin Exp Med 2016;9(4):7328-7333 www.ijcem.com /ISSN:1940-5901/IJCEM0021226 Original Article Comparison of plasmakinetic enucleation of the prostate with holmium laser enucleation of the prostate
Int J Clin Exp Med 2016;9(4):7328-7333 www.ijcem.com /ISSN:1940-5901/IJCEM0021226 Original Article Comparison of plasmakinetic enucleation of the prostate with holmium laser enucleation of the prostate
Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size
 Author's response to reviews Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size Authors: Aihua Li (Li121288@aliyun.com) Chengdong
Author's response to reviews Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size Authors: Aihua Li (Li121288@aliyun.com) Chengdong
Holmium laser enucleation of the prostate can be taught: the first learning experience
 Blackwell Science, LtdOxford, UK BJUBJU International1464-4096BJU International 909December 2002 3071 LEARNING HoLEP A. EL-HAKIM and M.M. ELHILALI 10.1046/j.1464-4096.2002.03071.x Original Article863869BEES
Blackwell Science, LtdOxford, UK BJUBJU International1464-4096BJU International 909December 2002 3071 LEARNING HoLEP A. EL-HAKIM and M.M. ELHILALI 10.1046/j.1464-4096.2002.03071.x Original Article863869BEES
Benign enlargement of prostate (BEP), which is. Early Experiences with HoLEP. Original Article ABSTRACT INTRODUCTION. Bhandari BB*
 Original Article Early Experiences with HoLEP Bhandari BB* * Consultant Urologist, Shree Birendra Army Hospital, Norvic International Hospital, Alka Hospital ABSTRACT introduction: Holmium Laser Enucleation
Original Article Early Experiences with HoLEP Bhandari BB* * Consultant Urologist, Shree Birendra Army Hospital, Norvic International Hospital, Alka Hospital ABSTRACT introduction: Holmium Laser Enucleation
PREDICTORS OF ENUCLEATION AND MORCELLATION TIME DURING HOLMIUM LASER ENUCLEATION OF THE PROSTATE
 PREDICTORS OF ENUCLEATION AND MORCELLATION TIME DURING HOLMIUM LASER ENUCLEATION OF THE PROSTATE M Francesca Monn, Marawan El Tayeb, Naeem Bhojani, Matthew J. Mellon, James C. Sloan, Ronald S. Boris, James
PREDICTORS OF ENUCLEATION AND MORCELLATION TIME DURING HOLMIUM LASER ENUCLEATION OF THE PROSTATE M Francesca Monn, Marawan El Tayeb, Naeem Bhojani, Matthew J. Mellon, James C. Sloan, Ronald S. Boris, James
Original Article Holmium laser enucleation of the prostate prevents postoperative stress incontinence in patients with benign prostate hyperplasia
 Int J Clin Exp Med 2018;11(3):2572-2576 www.ijcem.com /ISSN:1940-5901/IJCEM0054035 Original Article Holmium laser enucleation of the prostate prevents postoperative stress incontinence in patients with
Int J Clin Exp Med 2018;11(3):2572-2576 www.ijcem.com /ISSN:1940-5901/IJCEM0054035 Original Article Holmium laser enucleation of the prostate prevents postoperative stress incontinence in patients with
EFFECT OF INTRAVESICAL PROSTATIC PROTRUSION (IVPP) ON LOWER URINARY TRACT FUNCTION AND MANAGEMENT
 EFFECT OF INTRAVESICAL PROSTATIC PROTRUSION (IVPP) ON LOWER URINARY TRACT FUNCTION AND MANAGEMENT Rajaraman T 1, Balaji A. R 2, Vetrichandar S 3, Shekar M. G 4, Bhat K. R. S 5, Muthurathinam R 6, Ashokkumar
EFFECT OF INTRAVESICAL PROSTATIC PROTRUSION (IVPP) ON LOWER URINARY TRACT FUNCTION AND MANAGEMENT Rajaraman T 1, Balaji A. R 2, Vetrichandar S 3, Shekar M. G 4, Bhat K. R. S 5, Muthurathinam R 6, Ashokkumar
Treating BPH: Comparing Rezum UroLift and HoLEP
 Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
Outcomes of the Holmium Laser Enucleation of the Prostate for Patients With Prior Benign Prostatic Hyperplasia Surgery
 Original Article J Korean Geriatr Soc 2014;18(4):199-204 http://dx.doi.org/10.4235/jkgs.2014.18.4.199 Print ISSN 1229-2397 On-line ISSN 2288-1239 Outcomes of the Holmium Laser Enucleation of the Prostate
Original Article J Korean Geriatr Soc 2014;18(4):199-204 http://dx.doi.org/10.4235/jkgs.2014.18.4.199 Print ISSN 1229-2397 On-line ISSN 2288-1239 Outcomes of the Holmium Laser Enucleation of the Prostate
Wednesday 25 June Poster Session 9: BPH 1 Chairmen: M. Speakman and D. Rosario
 Wednesday 25 June 14.30 15.30 Poster Session 9: BPH 1 Chairmen: M. Speakman and D. Rosario P080 Unreliable residual volume measurement after increased water load diuresis G. ALIVIZATOS, A. SKOLARIKOS,
Wednesday 25 June 14.30 15.30 Poster Session 9: BPH 1 Chairmen: M. Speakman and D. Rosario P080 Unreliable residual volume measurement after increased water load diuresis G. ALIVIZATOS, A. SKOLARIKOS,
Original Policy Date
 MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
BENIGN PROSTATIC HYPERPLASIA (BPH) affects 70%
 JOURNAL OF ENDOUROLOGY Volume 14, Number 2, March 2000 Mary Ann Liebert, Inc. Holmium Laser Enucleation of the Prostate With Tissue Morcellation: Initial United States Experience JEFFREY A. MOODY, M.D.,
JOURNAL OF ENDOUROLOGY Volume 14, Number 2, March 2000 Mary Ann Liebert, Inc. Holmium Laser Enucleation of the Prostate With Tissue Morcellation: Initial United States Experience JEFFREY A. MOODY, M.D.,
Overview. Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia. Iain McAuley September 15, 2014
 Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
Preliminary experience with Monopolar Transurethral Resection of Prostate (TURP)
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 8 Ver. VI (Aug. 2017), PP 16-21 www.iosrjournals.org Preliminary experience with Monopolar
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 8 Ver. VI (Aug. 2017), PP 16-21 www.iosrjournals.org Preliminary experience with Monopolar
Shrestha A, Chalise PR, Sharma UK, Gyawali PR, Shrestha GK, Joshi BR. Department of Surgery, TU Teaching Hospital, Maharajgunj, Kathmandu, Nepal
 Original Article Intravesical Prostatic Protrusion is better than Prostate Volume in Predicting Symptom Severity in Benign Prostatic Hyperplasia: A Prospective Clinical Study Shrestha A, Chalise PR, Sharma
Original Article Intravesical Prostatic Protrusion is better than Prostate Volume in Predicting Symptom Severity in Benign Prostatic Hyperplasia: A Prospective Clinical Study Shrestha A, Chalise PR, Sharma
Comparison of outpatient versus inpatient transurethral prostate resection for benign prostatic hyperplasia: Comparative, prospective bi-centre study
 original research Comparison of outpatient versus inpatient transurethral prostate resection for benign prostatic hyperplasia: Comparative, prospective bi-centre study Jae Heon Kim, MD; * Jae Young Park,
original research Comparison of outpatient versus inpatient transurethral prostate resection for benign prostatic hyperplasia: Comparative, prospective bi-centre study Jae Heon Kim, MD; * Jae Young Park,
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
GUIDELINES ON NON-NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (Text update March 2015) S. Gravas (Chair), T. Bach,. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher, C. Mamoulakis,
GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (Text update March 2015) S. Gravas (Chair), T. Bach,. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher, C. Mamoulakis,
Thulium Laser versus Standard Transurethral Resection of the Prostate: A Randomized Prospective Trial
 european urology 53 (2008) 382 390 available at www.sciencedirect.com journal homepage: www.europeanurology.com Benign Prostatic Obstruction Thulium Laser versus Standard Transurethral Resection of the
european urology 53 (2008) 382 390 available at www.sciencedirect.com journal homepage: www.europeanurology.com Benign Prostatic Obstruction Thulium Laser versus Standard Transurethral Resection of the
Introduction. Original Article: Clinical Investigation. Yosuke Hirasawa, 1 Yuji Kato 2 and Kiichiro Fujita 2
 International Journal of Urology (2018) 25, 76--80 doi: 10.1111/iju.13472 Original Article: Clinical Investigation Age and prostate volume are risk factors for transient urinary incontinence after transurethral
International Journal of Urology (2018) 25, 76--80 doi: 10.1111/iju.13472 Original Article: Clinical Investigation Age and prostate volume are risk factors for transient urinary incontinence after transurethral
EAU GUIDELINES POCKET EDITION 3
 EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
INJINTERNATIONAL. Original Article INTRODUCTION. Int Neurourol J 2017;21: pissn eissn
 Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
OUTCOMES OF HoLEP IN THE RETREATMENT SETTING
 OUTCOMES OF HoLEP IN THE RETREATMENT SETTING Tracy Marien 1 MD, Mustafa Kadihasanoglu 1 MD, Teerayut Tangpaitoon 1 MD, Nadya York 2 MD, Andrew T. Blackburne 3 MD, Haidar Abdul-Muhsin 4 MD, Michael S. Borofsky
OUTCOMES OF HoLEP IN THE RETREATMENT SETTING Tracy Marien 1 MD, Mustafa Kadihasanoglu 1 MD, Teerayut Tangpaitoon 1 MD, Nadya York 2 MD, Andrew T. Blackburne 3 MD, Haidar Abdul-Muhsin 4 MD, Michael S. Borofsky
Xin Li 1, Jin-hong Pan 1, Qi-gui Liu 2, Peng He 1, Si-ji Song 1, Tao Jiang 1, Zhan-song Zhou 1 * Abstract. Introduction
 Combined with Transurethral Incision of the Bladder Neck for Bladder Outlet Obstruction in Patients with Small Volume Benign Prostate Hyperplasia (BPH): A Prospective Randomized Study Xin Li 1, Jin-hong
Combined with Transurethral Incision of the Bladder Neck for Bladder Outlet Obstruction in Patients with Small Volume Benign Prostate Hyperplasia (BPH): A Prospective Randomized Study Xin Li 1, Jin-hong
Voiding Dysfunction. Joon Seok Kwon, Jung Woo Lee 1, Seung Wook Lee, Hong Yong Choi, Hong Sang Moon. DOI: /kju
 www.kjurology.org DOI:10.4111/kju.2011.52.4.269 Voiding Dysfunction Comparison of Effectiveness of Monopolar and Bipolar Transurethral Resection of the Prostate and Open Prostatectomy in Large Benign Prostatic
www.kjurology.org DOI:10.4111/kju.2011.52.4.269 Voiding Dysfunction Comparison of Effectiveness of Monopolar and Bipolar Transurethral Resection of the Prostate and Open Prostatectomy in Large Benign Prostatic
Safety and efficacy of photoselective vaporization of the prostate using the 180-W GreenLight XPS laser system in patients taking oral anticoagulants
 Clinical Report Safety and efficacy of photoselective vaporization of the prostate using the 180-W GreenLight XPS laser system in patients taking oral anticoagulants Journal of International Medical Research
Clinical Report Safety and efficacy of photoselective vaporization of the prostate using the 180-W GreenLight XPS laser system in patients taking oral anticoagulants Journal of International Medical Research
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of transurethral water jet ablation for lower urinary tract symptoms caused by benign
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of transurethral water jet ablation for lower urinary tract symptoms caused by benign
IS IRRIGATION NECESSARY AFTER MONOPOLAR TURP? OUR 11 YEARS EXPERIENCE
 IS IRRIGATION NECESSARY AFTER MONOPOLAR TURP? OUR 11 YEARS EXPERIENCE Prasannakumar K, Venkatesh Krishnamoorthy, Maneesh Sinha, Krishna Prasad T, Pradeepa MG Abstract Objective: This study was conducted
IS IRRIGATION NECESSARY AFTER MONOPOLAR TURP? OUR 11 YEARS EXPERIENCE Prasannakumar K, Venkatesh Krishnamoorthy, Maneesh Sinha, Krishna Prasad T, Pradeepa MG Abstract Objective: This study was conducted
GREENLIGHT XPS LASER THERAPY SYSTEM: A SYSTEMATIC APPROACH TO VAPORIZATION
 TM GREENLIGHT XPS LASER THERAPY SYSTEM: A SYSTEMATIC APPROACH TO VAPORIZATION Gregg R. Eure, MD, FACS Urology of Virginia Virginia Beach, Virginia GREENLIGHT XPS TM A SYSTEMATIC APPROACH TO VAPORIZATION
TM GREENLIGHT XPS LASER THERAPY SYSTEM: A SYSTEMATIC APPROACH TO VAPORIZATION Gregg R. Eure, MD, FACS Urology of Virginia Virginia Beach, Virginia GREENLIGHT XPS TM A SYSTEMATIC APPROACH TO VAPORIZATION
GUIDELINES ON NON-NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (BPO)
 GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (BPO) (Text update pril 2014) S. Gravas (chair),. Bachmann,. Descazeaud, M. Drake, C. Gratzke, S. Madersbacher, C. Mamoulakis,
GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (BPO) (Text update pril 2014) S. Gravas (chair),. Bachmann,. Descazeaud, M. Drake, C. Gratzke, S. Madersbacher, C. Mamoulakis,
Lasers in Urology. Myung Soo Kim, Kyung Kgi Park 1, Byung Ha Chung, Seung Hwan Lee.
 www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.1.36 Lasers in Urology Effect of Photoselective Vaporization Prostatectomy on Lower Urinary Tract Symptoms in Benign Prostatic Hyperplasia With or
www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.1.36 Lasers in Urology Effect of Photoselective Vaporization Prostatectomy on Lower Urinary Tract Symptoms in Benign Prostatic Hyperplasia With or
An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms
 Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Transurethral incision versus transurethral resection of the prostate in small prostatic adenoma: Long-term follow-up
 African Journal of Urology (2012) 18, 29 33 Pan African Urological Surgeons Association African Journal of Urology www.ees.elsevier.com/afju www.sciencedirect.com Transurethral incision versus transurethral
African Journal of Urology (2012) 18, 29 33 Pan African Urological Surgeons Association African Journal of Urology www.ees.elsevier.com/afju www.sciencedirect.com Transurethral incision versus transurethral
Lasers in Urology. Ju Hyun Park 1, Hwancheol Son 1,2, Jae-Seung Paick 1. DOI: /kju
 www.kjurology.org DOI:10.4111/kju.2010.51.2.115 Lasers in Urology Comparative Analysis of the Efficacy and Safety of Photoselective Vaporization of the Prostate for Treatment of Benign Prostatic Hyperplasia
www.kjurology.org DOI:10.4111/kju.2010.51.2.115 Lasers in Urology Comparative Analysis of the Efficacy and Safety of Photoselective Vaporization of the Prostate for Treatment of Benign Prostatic Hyperplasia
Yong Taec Lee, Young Woo Ryu, Dong Min Lee, Sang Wook Park, Seung Hee Yum, June Hyun Han
 www.kjurology.org http://dx.doi.org/10.4111/kju.2011.52.11.763 Voiding Dysfunction Comparative Analysis of the Efficacy and Safety of Conventional Transurethral Resection of the Prostate, Transurethral
www.kjurology.org http://dx.doi.org/10.4111/kju.2011.52.11.763 Voiding Dysfunction Comparative Analysis of the Efficacy and Safety of Conventional Transurethral Resection of the Prostate, Transurethral
TRANSURETHRAL RESECTION
 TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
Lasers in Urology. Sae Woong Choi, Yong Sun Choi, Woong Jin Bae, Su Jin Kim, Hyuk Jin Cho, Sung Hoo Hong, Ji Youl Lee, Tae Kon Hwang, Sae Woong Kim
 www.kjurology.org http://dx.doi.org/10.4111/kju.2011.52.12.824 Lasers in Urology 120 W Greenlight HPS Laser Photoselective Vaporization of the Prostate for Treatment of Benign Prostatic Hyperplasia in
www.kjurology.org http://dx.doi.org/10.4111/kju.2011.52.12.824 Lasers in Urology 120 W Greenlight HPS Laser Photoselective Vaporization of the Prostate for Treatment of Benign Prostatic Hyperplasia in
Holmium laser enucleation of the prostate: surgical, functional, and quality-of-life outcomes upon extended follow-up
 ORIGINAL ARTICLE Vol. 42 (2): 293-301, March - April, 2016 doi: 10.1590/S1677-5538.IBJU.2014.0561 Holmium laser enucleation of the prostate: surgical, functional, and quality-of-life outcomes upon extended
ORIGINAL ARTICLE Vol. 42 (2): 293-301, March - April, 2016 doi: 10.1590/S1677-5538.IBJU.2014.0561 Holmium laser enucleation of the prostate: surgical, functional, and quality-of-life outcomes upon extended
Executive Summary. Non-drug local procedures for treatment of benign prostatic hyperplasia 1. IQWiG Reports - Commission No.
 IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Limited text update March 2016) S. Gravas (Chair), T. Bach, A. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher,
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Limited text update March 2016) S. Gravas (Chair), T. Bach, A. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher,
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Text update March 2017) S. Gravas (Chair), T. Bach, M. Drake, M. Gacci, C. Gratzke, T.R.W. Herrmann, S. Madersbacher,
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Text update March 2017) S. Gravas (Chair), T. Bach, M. Drake, M. Gacci, C. Gratzke, T.R.W. Herrmann, S. Madersbacher,
Submitted: August 15, Accepted: September 10, Published: October 15, 2018.
 Original Article doi: 10.22374/jeleu.v1i2.21 THULIUM LASER ENUCLEATION OF THE PROSTATE (THULEP) AS A TECHNIQUE FOR TREATMENT OF BPH: EVALUATION OF A SIX-YEAR EXPERIENCE AT A SINGLE INSTITUTION Mahmood
Original Article doi: 10.22374/jeleu.v1i2.21 THULIUM LASER ENUCLEATION OF THE PROSTATE (THULEP) AS A TECHNIQUE FOR TREATMENT OF BPH: EVALUATION OF A SIX-YEAR EXPERIENCE AT A SINGLE INSTITUTION Mahmood
Benign Prostatic Hyperplasia (BPH)
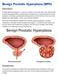 Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
ISPUB.COM. Photoselective Vaporisation of the Prostate - Independent Surgical Experience Following Comprehensive Resident Training in the Technique.
 ISPUB.COM The Internet Journal of Urology Volume 9 Number 4 Photoselective Vaporisation of the Prostate - Independent Surgical Experience Following Comprehensive Resident Training in the Technique. R Eapen,
ISPUB.COM The Internet Journal of Urology Volume 9 Number 4 Photoselective Vaporisation of the Prostate - Independent Surgical Experience Following Comprehensive Resident Training in the Technique. R Eapen,
Name of Policy: Transurethral Microwave Thermotherapy
 Name of Policy: Transurethral Microwave Thermotherapy Policy #: 449 Latest Review Date: September 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable
Name of Policy: Transurethral Microwave Thermotherapy Policy #: 449 Latest Review Date: September 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable
Surgical Treatment of LUTS in Men with BPE
 Patient Information English 35 Surgical Treatment of LUTS in Men with BPE The underlined terms are listed in the glossary. You have been diagnosed with benign prostatic enlargement (BPE) and your doctor
Patient Information English 35 Surgical Treatment of LUTS in Men with BPE The underlined terms are listed in the glossary. You have been diagnosed with benign prostatic enlargement (BPE) and your doctor
TURP: How Much Should Be Resected? International Braz J Urol Vol. 35 (6): , November - December, 2009 doi: /S
 Clinical Urology TURP: How Much Should Be Resected? International Braz J Urol Vol. 35 (6): 683-691, November - December, 2009 doi: 10.1590/S1677-55382009000600007 Transurethral Resection of the Prostate
Clinical Urology TURP: How Much Should Be Resected? International Braz J Urol Vol. 35 (6): 683-691, November - December, 2009 doi: 10.1590/S1677-55382009000600007 Transurethral Resection of the Prostate
Transurethral Laser Technology: Treatments for BPH
 Transurethral Laser Technology: Treatments for BPH Richard Lee, MD Departments of Urology and Public Health The New York Presbyterian Hospital Weill Medical College of Cornell University Background Traditional
Transurethral Laser Technology: Treatments for BPH Richard Lee, MD Departments of Urology and Public Health The New York Presbyterian Hospital Weill Medical College of Cornell University Background Traditional
Elective Hemi Transurethral Resection of Prostate: A Safe and Effective Method of Treating Huge Benign Prostatic Hyperplasia
 ORIGINAL ARTICLE Elective Hemi Transurethral Resection of Prostate: A Safe and Effective Method of Treating Huge Benign Prostatic Hyperplasia Syed Saeed Abidi 1, Irfan Feroz 1, Mohammad Aslam 1 and Ahmed
ORIGINAL ARTICLE Elective Hemi Transurethral Resection of Prostate: A Safe and Effective Method of Treating Huge Benign Prostatic Hyperplasia Syed Saeed Abidi 1, Irfan Feroz 1, Mohammad Aslam 1 and Ahmed
Can 80 W KTP Laser Vaporization Effectively Relieve the Obstruction in Benign Prostatic Hyperplasia?: A Nonrandomized Trial
 pissn: 2287-428 / eissn: 2287-469 World J Mens Health 212 December 3(3): 16-165 http://dx.doi.org/1.5534/wjmh.212.3.3.16 Original Article Can 8 W KTP Laser Vaporization Effectively Relieve the Obstruction
pissn: 2287-428 / eissn: 2287-469 World J Mens Health 212 December 3(3): 16-165 http://dx.doi.org/1.5534/wjmh.212.3.3.16 Original Article Can 8 W KTP Laser Vaporization Effectively Relieve the Obstruction
(2018) The Clinical Effect of Bipolar Transurethral Resection in Saline of Benign. Hyperplasia with Long Term Follow-Up
 Open Journal of Urology, 2018, 8, 108-117 http://www.scirp.org/journal/oju ISSN Online: 2160-5629 ISSN Print: 2160-5440 The Clinical Effect of Bipolar Transurethral Resection in Saline of Benign Prostate
Open Journal of Urology, 2018, 8, 108-117 http://www.scirp.org/journal/oju ISSN Online: 2160-5629 ISSN Print: 2160-5440 The Clinical Effect of Bipolar Transurethral Resection in Saline of Benign Prostate
Technique and Short-Term Outcome of Green Light Laser (KTP, 80 W) Vaporisation of the Prostate
 european urology 52 (2007) 1632 1637 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Technique and Short-Term Outcome of Green Light Laser (KTP, 80 W) Vaporisation
european urology 52 (2007) 1632 1637 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Technique and Short-Term Outcome of Green Light Laser (KTP, 80 W) Vaporisation
Prostatic Diseases and Male Voiding Dysfunction
 Prostatic Diseases and Male Voiding Dysfunction Prostatic-specific Antigen Velocity After Holmium Laser Enucleation of the Prostate: Possible Predictor for the Assessment of Treatment Effect Durability
Prostatic Diseases and Male Voiding Dysfunction Prostatic-specific Antigen Velocity After Holmium Laser Enucleation of the Prostate: Possible Predictor for the Assessment of Treatment Effect Durability
Lasers in Urology. Hyeon Jun Kim, Han Yi Lee, Sang Hun Song 1, Jae-Seung Paick.
 www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.2.89 Lasers in Urology Relationship of Postoperative Recatheterization and Intraoperative Bladder Distention Volume in Holmium Laser Enucleation
www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.2.89 Lasers in Urology Relationship of Postoperative Recatheterization and Intraoperative Bladder Distention Volume in Holmium Laser Enucleation
Peri-operative complications of holmium laser enucleation of the prostate: experience in the first 280 patients, and a review of literature
 Lower Urinary Tract PERI-OPERATIVE COMPLICATIONS OF HoLEP SHAH et al. Peri-operative complications of holmium laser enucleation of the prostate: experience in the first 280 patients, and a review of literature
Lower Urinary Tract PERI-OPERATIVE COMPLICATIONS OF HoLEP SHAH et al. Peri-operative complications of holmium laser enucleation of the prostate: experience in the first 280 patients, and a review of literature
JMSCR Vol 04 Issue 10 Page October 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i10.40 Combined Bladder Stones Removal: In
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i10.40 Combined Bladder Stones Removal: In
NIH Public Access Author Manuscript J Urol. Author manuscript; available in PMC 2010 May 4.
 NIH Public Access Author Manuscript Published in final edited form as: J Urol. 2009 December ; 182(6): 2819 2824. doi:10.1016/j.juro.2009.08.086. Intravesical Prostatic Protrusion in Men in Olmsted County,
NIH Public Access Author Manuscript Published in final edited form as: J Urol. 2009 December ; 182(6): 2819 2824. doi:10.1016/j.juro.2009.08.086. Intravesical Prostatic Protrusion in Men in Olmsted County,
Transurethral Resection of Prostate (TURP) Through The Decades A Comparison of Results Over the Last Thirty Years in a Single Institution in Asia
 Original Article 775 Transurethral Resection of Prostate (TURP) Through The Decades A Comparison of Results Over the Last Thirty Years in a Single Institution in Asia KB Lim, 1 FRCS (Edin), MYC Wong, 1
Original Article 775 Transurethral Resection of Prostate (TURP) Through The Decades A Comparison of Results Over the Last Thirty Years in a Single Institution in Asia KB Lim, 1 FRCS (Edin), MYC Wong, 1
Roberto Giulianelli, Barbara Gentile, Luca Albanesi, Paola Tariciotti, and Gabriella Mirabile
 Surgical Techniques in Urology Bipolar Button Transurethral Enucleation of Prostate in Benign Prostate Hypertrophy Treatment: A New Surgical Technique Roberto Giulianelli, Barbara Gentile, Luca Albanesi,
Surgical Techniques in Urology Bipolar Button Transurethral Enucleation of Prostate in Benign Prostate Hypertrophy Treatment: A New Surgical Technique Roberto Giulianelli, Barbara Gentile, Luca Albanesi,
Original Article Retrospective comparison of the modified and traditional holmium laser transurethral prostatectomy based on a 1-year follow-up
 Int J Clin Exp Med 2016;9(2):4009-4015 www.ijcem.com /ISSN:1940-5901/IJCEM0017779 Original Article Retrospective comparison of the modified and traditional holmium laser transurethral prostatectomy based
Int J Clin Exp Med 2016;9(2):4009-4015 www.ijcem.com /ISSN:1940-5901/IJCEM0017779 Original Article Retrospective comparison of the modified and traditional holmium laser transurethral prostatectomy based
Hee Young Park, Joo Yong Lee, Sung Yul Park, Seung Wook Lee, Yong Tae Kim, Hong Yong Choi, Hong Sang Moon
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.2.92 Voiding Dysfunction Efficacy of Alpha Blocker Treatment According to the Degree of Intravesical Prostatic Protrusion Detected by Transrectal
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.2.92 Voiding Dysfunction Efficacy of Alpha Blocker Treatment According to the Degree of Intravesical Prostatic Protrusion Detected by Transrectal
Rezūm procedure for the Prostate
 Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Clinical Study Long-Term Followup after Electrocautery Transurethral Resection of the Prostate for Benign Prostatic Hyperplasia
 Advances in Urology Volume 2011, Article ID 359478, 6 pages doi:10.1155/2011/359478 Clinical Study Long-Term Followup after Electrocautery Transurethral Resection of the Prostate for Benign Prostatic Hyperplasia
Advances in Urology Volume 2011, Article ID 359478, 6 pages doi:10.1155/2011/359478 Clinical Study Long-Term Followup after Electrocautery Transurethral Resection of the Prostate for Benign Prostatic Hyperplasia
Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH
 Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH The more you know, the better you ll feel. You ve likely had a discussion with your doctor about BPH 1. What follows are some
Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH The more you know, the better you ll feel. You ve likely had a discussion with your doctor about BPH 1. What follows are some
Control & confidence. You deserve both.
 Learn more about BPH and Plasma therapy Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH Your doctor is always happy to offer all the guidance you need so that you feel completely
Learn more about BPH and Plasma therapy Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH Your doctor is always happy to offer all the guidance you need so that you feel completely
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
Katsumi Shigemura, Kazushi Tanaka, Fukashi Yamamichi, Koji Chiba, Masato Fujisawa
 Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
Review Article A Personal Reflection of Greenlight 532 nm Laser for BPH Treatment
 Advances in Andrology, Article ID 207901, 6 pages http://dx.doi.org/10.1155/2014/207901 Review Article A Personal Reflection of Greenlight 532 nm Laser for BPH Treatment Bilal Chughtai, Claire Dunphy,
Advances in Andrology, Article ID 207901, 6 pages http://dx.doi.org/10.1155/2014/207901 Review Article A Personal Reflection of Greenlight 532 nm Laser for BPH Treatment Bilal Chughtai, Claire Dunphy,
Author's Accepted Manuscript
 Author's Accepted Manuscript Direct comparison of Green Light Laser XPS Photoselective Vaporization of the Prostate (PVP) and Green Laser En Bloc enucleation of the prostate (GreenLEP) in enlarged glands
Author's Accepted Manuscript Direct comparison of Green Light Laser XPS Photoselective Vaporization of the Prostate (PVP) and Green Laser En Bloc enucleation of the prostate (GreenLEP) in enlarged glands
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA. A Minimally Invasive Innovative Treatment
 PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
INJINTERNATIONAL. Efficacy of Holmium Laser Enucleation of the Prostate Based on Patient Preoperative Characteristics. Original Article INTRODUCTION
 Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
MODULE 3: BENIGN PROSTATIC HYPERTROPHY
 MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
TITLE: Plasma Vaporization of the Prostate for Treatment of Benign Prostatic Hypertrophy: A Review of Clinical and Cost-Effectiveness, and Safety
 TITLE: Plasma Vaporization of the Prostate for Treatment of Benign Prostatic Hypertrophy: A Review of Clinical and Cost-Effectiveness, and Safety DATE: 05 March 2014 CONTEXT AND POLICY ISSUES Benign prostatic
TITLE: Plasma Vaporization of the Prostate for Treatment of Benign Prostatic Hypertrophy: A Review of Clinical and Cost-Effectiveness, and Safety DATE: 05 March 2014 CONTEXT AND POLICY ISSUES Benign prostatic
CYSTOSCOPY & TRANSURETHRAL RESECTION OF THE PROSTATE
 Associates: Dr Kim Pese Dr Kym Horsell Dr Michael Chong Dr Jason Lee The Tennyson Centre Suite 19, First Floor 520 South Road Kurralta Park SA 5037 Appointments: 08 8292 2399 Fax: 08 8292 2388 admin@urologicalsolutions.com.au
Associates: Dr Kim Pese Dr Kym Horsell Dr Michael Chong Dr Jason Lee The Tennyson Centre Suite 19, First Floor 520 South Road Kurralta Park SA 5037 Appointments: 08 8292 2399 Fax: 08 8292 2388 admin@urologicalsolutions.com.au
Cheng Liu, Xuejun Liu, Duo Liu, Jiagui Mu, Dongsheng Zhu, Li Fan, Qun Song, Dongwei Yao *
 Biomedical Research 2017; 28 (5): 2278-2283 ISSN 0970-938X www.biomedres.info Effect of dual-band semiconductor laser transurethral resection of prostate on efficacy, stress response and quality of life
Biomedical Research 2017; 28 (5): 2278-2283 ISSN 0970-938X www.biomedres.info Effect of dual-band semiconductor laser transurethral resection of prostate on efficacy, stress response and quality of life
ABSTRACT KEY WORDS. Original Article. Page 163. Background
 Outcomes of Transurethral Resection of the Prostate in Benign Prostatic Hyperplasia Comparing Prostate Size of more than 80 Grams to Prostate Size less than 80 Grams. Joshi HN, 1 de Jong IJ, 2 Karmacharya
Outcomes of Transurethral Resection of the Prostate in Benign Prostatic Hyperplasia Comparing Prostate Size of more than 80 Grams to Prostate Size less than 80 Grams. Joshi HN, 1 de Jong IJ, 2 Karmacharya
Management of Voiding Problems in Older Men. Dr. John Fenn Consultant, QEH 10 th October, 2005
 Management of Voiding Problems in Older Men Dr. John Fenn Consultant, QEH 10 th October, 2005 Voiding Problems Poor stream Hesitancy Straining Incomplete emptying Intermittent micturition Terminal dribbling
Management of Voiding Problems in Older Men Dr. John Fenn Consultant, QEH 10 th October, 2005 Voiding Problems Poor stream Hesitancy Straining Incomplete emptying Intermittent micturition Terminal dribbling
Authors KC Cheng, LF Lee, KW Wong, HC Chan, CL Cho, H Chau, KM Lam, HS So. Division of Urology, Department of Surgery, United Christian Hospital
 Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
EUROPEAN UROLOGY 58 (2010)
 EUROPEAN UROLOGY 58 (2010) 349 355 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Benign Prostatic Hyperplasia Editorial by Petrisor Geavlete on pp. 356
EUROPEAN UROLOGY 58 (2010) 349 355 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Benign Prostatic Hyperplasia Editorial by Petrisor Geavlete on pp. 356
Transurethral Resection of Prostate (TURP)
 Transurethral Resection of Prostate (TURP) Department of Urology Patient Information What What and and where where is the is prostate? the prostate? The prostate is a small gland, about the size of a walnut,
Transurethral Resection of Prostate (TURP) Department of Urology Patient Information What What and and where where is the is prostate? the prostate? The prostate is a small gland, about the size of a walnut,
TURP Complications & Treatments. G. Testa
 TURP Complications & Treatments G. Testa Statistics Operative mortality 0.2 per cent Most common cause of death was sepsis which occurred >1 month after surgery 77% of patients had significant pre-existing
TURP Complications & Treatments G. Testa Statistics Operative mortality 0.2 per cent Most common cause of death was sepsis which occurred >1 month after surgery 77% of patients had significant pre-existing
Aquablation therapy for symptomatic benign prostatic hyperplasia: a single-centre experience in 47 patients
 Aquablation therapy for symptomatic benign prostatic hyperplasia: a single-centre experience in 47 patients Mihir M. Desai*, Abhishek Singh, Shashank Abhishek, Abhishek Laddha, Harshad Pandya, Akbar N.
Aquablation therapy for symptomatic benign prostatic hyperplasia: a single-centre experience in 47 patients Mihir M. Desai*, Abhishek Singh, Shashank Abhishek, Abhishek Laddha, Harshad Pandya, Akbar N.
The One Year Outcome after KTP Laser Vaporization of the Prostate According to the Calculated Vaporized Volume
 J Korean Med Sci 9; 24: 1187-91 ISSN 111-8934 DOI: 1.3346/jkms.9.24.6.1187 Copyright The Korean Academy of Medical Sciences The One Year Outcome after KTP Laser Vaporization of the Prostate According to
J Korean Med Sci 9; 24: 1187-91 ISSN 111-8934 DOI: 1.3346/jkms.9.24.6.1187 Copyright The Korean Academy of Medical Sciences The One Year Outcome after KTP Laser Vaporization of the Prostate According to
Factors Affecting De Novo Urinary Retention after Holmium Laser Enucleation of the Prostate
 Florida International University FIU Digital Commons Environmental & Occupational Health Robert Stempel College of Public Health & Social Work 1-21-2014 Factors Affecting De Novo Urinary Retention after
Florida International University FIU Digital Commons Environmental & Occupational Health Robert Stempel College of Public Health & Social Work 1-21-2014 Factors Affecting De Novo Urinary Retention after
Holmium:YAG Transurethral Incision Versus Laser Photoselective Vaporization for Benign Prostatic Hyperplasia in a Small Prostate
 Holmium:YAG Transurethral Incision Versus Laser Photoselective Vaporization for Benign Prostatic Hyperplasia in a Small Prostate Ahmed M. Elshal, Mohamed A. Elkoushy, Hazem M. Elmansy, John Sampalis and
Holmium:YAG Transurethral Incision Versus Laser Photoselective Vaporization for Benign Prostatic Hyperplasia in a Small Prostate Ahmed M. Elshal, Mohamed A. Elkoushy, Hazem M. Elmansy, John Sampalis and
