BJUI. TURP and sex: patient and partner prospective 12 years follow-up study
|
|
|
- Milton May
- 5 years ago
- Views:
Transcription
1 BJUI TURP and sex: patient and partner prospective 12 years follow-up study Said F. Mishriki, Samuel J.S. Grimsley, Thomas Lam, Ghulam Nabi * and Nicholas P. Cohen Urology Department, Aberdeen Royal Infirmary, Grampian NHS Trust, Aberdeen, and *Academic Clinical Practice, Department of Urology, Ninewells Hospital and Medical School, Dundee, UK Accepted for publication 16 March 2011 Study Type Symptom prevalence (prospective cohort) Level of Evidence 1b OBJECTIVE To evaluate the effect of transurethral resection of the prostate (TURP) on sexual function in the short (6 months), medium (6 years) and long (12 years) term and assess the conformity between patient and partner regarding sexual function. What s known on the subject? and What does the study add? Evidence that transurethral resection of the prostate (TURP) leads to erectile dysfunction () is conflicting. Several studies claimed significant risk of after TURP for benign prostatic hyperplasia with some reporting complete loss of erection. Several studies have been retrospective or have not considered levels of pre-operative. associated with lower urinary tract symptoms frequently precedes TURP. TURP did not adversely affect erectile function. Pre-operative can be improved by TURP and long-term erectile function is maintained following TURP. The improvement was corroborated by the partners in the short, medium and long-term and was statistically significant. RESULTS CONCLUSIONS PATIENTS AND METHODS A prospective cohort study set at the Aberdeen Royal Infirmary University Hospital. A total of 280 men referred with lower urinary tract symptoms (LUTS) to a university hospital underwent TURP between January 1993 and September 1994; 145 of their partners (partner or spouse) participated. Assessment included American Urological Association symptom score, flow rates and validated self-reported sexual questionnaires (SQ). Data were collected at baseline, 3 months, 6 months, 6 years and 12 years of follow-up. In all, 120 (43%) men were sexually active preoperatively. At 6 months, 73 (61%) of these 120 men completed the SQ and all were sexually active. No sexually active patient became impotent after the procedure. Moreover, 27 (15%) with pre-existing erectile dysfunction reported improved sexual activity and erection quality. At 6 years 101 men completed the SQ and 31 (30.7%) were sexually active. At 12 years, 36 (31.9%) of 113 who completed the SQ were sexually active. Partners agreed with the men s self assessment at all visits. Limitations include possible attrition bias and lack of information from non-responders. Erectile dysfunction associated with LUTS frequently precedes TURP. The TURP did not adversely affect sexual function. Pre-operative erectile dysfunction can be improved by TURP and long-term sexual function is maintained after TURP. These findings, corroborated by the partners, were statistically significant. KEYWORDS benign prostatic enlargement, benign prostatic hyperplasia, erectile dysfunction, lower urinary tract symptoms, sex, transurethral resection of the prostate INTRODUCTION Erectile dysfunction () is defined as the consistent inability to attain or maintain an erection of sufficient quality to permit satisfactory sexual intercourse [1 ]. Evidence that transurethral resection of the prostate (TURP) leads to is conflicting. Studies claiming significant risk of from TURP include 31% experiencing after prostatectomy for benign prostatic hyperplasia (BPH) [2 ], 27% reporting complete loss of erection and 8.3% becoming impotent on objective testing [3,4 ]. In one study significant sexual function improvement after TURP was reported [5 ]. A randomized study showed non-significant improvement in sexual function associated with TURP when compared with watchful waiting [6 ]. One important clinical question remains unanswered. Is the long-held idea that TURP is detrimental to sexual function correct or could TURP improve sex life? , doi: /j x x 745
2 MISHRIKI ET AL. There are several reasons for the confusing picture. Severity of urinary symptoms was correlated with measures of [7,8 ]. That the improvement in after TURP is associated with an improvement in lower urinary tract symptoms (LUTS), is supported by a similar observation of the improvement produced by alpha-blockers [9,10 ]. Few studies highlighted the fact that significant numbers of patients with LUTS have before TURP [7,11 ]. Several studies have been retrospective or have not considered levels of preoperative [2 ]. Studies of sexual function after TURP have been limited when compared with other outcomes. Long-term randomized trials are awaited. Sexual function is an important outcome measure to consider before TURP (still regarded by many as the standard for the treatment of BPH). Hence the determination of its true long-term influence on sexual function is essential. The patient characteristics, functional results and complications of TURP for this study have been published previously [12 ]. Long-term improvement in quality of life and bother scores noted by patients and corroborated by partners in this study was also reported previously [13 ]. The objectives of this study were to evaluate the effect of TURP on sexual function in the short (6 months), medium (6 years) and long (12 years) term and to assess the conformity between patient and partner regarding sexual function. PATIENTS AND METHODS In all, 280 men with LUTS referred to Aberdeen Royal Infirmary University Hospital between January 1993 and September 1994 underwent TURP as a definitive treatment in this prospective-protocol-based study. Treatment decision was based on combined assessment of symptoms, AUA symptom score, flow rates and residual urine. Of their partners (partners and spouses), 145 agreed to participate. Personal details, DRE, PSA, flow studies, post-micturition residuals and TRUS for prostate size were recorded. Patients and partners completed the Sex Questionnaire (Appendices 1 and 2). Possible minimum and maximum individual scores were 0 and 8. Men diagnosed with carcinoma of the prostate after TURP and patients presenting with urinary retention or requiring open prostatectomy were excluded from the study. Patients and partners have been followed up for 12 years after TURP. Partners were asked to complete the questionnaire independently. This took place when accompanying the patient to the clinic, at home in the presence of a research nurse or questionnaires were returned by post. Patients and partners completed these questionnaires preoperatively and at 3 months, 6 months, 6 years and 12 years. During the 12 years, some of the men who were single or widowed at the start of the study have married and some married men have divorced or been widowed. Ethical approval was granted for the initial study and all follow-up stages and all participants provided written informed consent. A questionnaire suitable for selfadministration designed to assess sexual desire, sexual activity and erection quality was based on early non-validated questionnaires used in The international index of erectile function was not available till February 1997 [14 ]. Reliability of the questionnaires and stability of responses over time were internally validated by a test retest analysis, achieved by conducting the questionnaires twice in the same group with a 3-month interval between tests during which no change in therapy was instituted. This method has been used in at least one similar study [15 ]. The test retest analysis compared with Spearmann s rank analysis, to assess consistency in scoring, showed strong correlation (patients: r = 0.753, P = 0.001; partners: r = 1.0, P = 0.01). Inter-rater reliability is a measure used to examine the agreement between two raters/ observers on the assignment of categories of a categorical variable. Cohen s Kappa coefficient was used to determine the consistency of responses between patients and their partners who had responded at the various time-points (pre-turp, 6 months, 6 years and 12 years). Patients without partners or whose partners had not responded were excluded from the analysis FIG. 1. Patient and partner flow chart. Number of patients and partners attending at each stage throughout the study Preoperative 6 months 6 years 12 years because the patients and partners responses were considered in pairs. There were four possible paired outcomes: Yes Yes, No No, Yes No, No Yes, with the Yes Yes and No No groups reflecting agreement between patients and partners. RESULTS n = 280 n = 145 n = 168 n = 67 n = 101 n = 58 n = 113 n = 60 The number of patients and partners at each stage of follow-up is shown in Fig. 1. Mean age of patients at the time of TURP was 68 years (range years). Table 1 shows patient and partner numbers and percentage of partners agreeing/ differing with the patients sexual status. At baseline, 217 men were married, 10 were single, 31 were widowed and 22 did not declare a marital status. Preoperatively 120 (43%) men (mean age 65 years) were sexually active with 81.8% of 66 partners in agreement. A total of 160 (57%) men (mean age 70 years) had with 96.2% of 79 partners in agreement. At the 6 months follow-up, 168 men were followed up. One hundred men (mean age 69 years) were sexually active with 86% of 36 partners in agreement and 68 men (mean age 70 years) had with 96.8% of 31 partners in agreement. Of the 180 men who were sexually inactive
3 TURP AND SEX TABLE 1 Partner agreeing or differing regarding sexual status Point in time Sex status Conformity Pre-TURP n = 12 0 /partner participating n = 66 (55%) No partner or no response n = 54 (45%) Partner agrees n = 54 (81.8%) Partner differs n = 12 (18.2%) Pre-TURP n = months n = months n = 68 6 years n = 31 6 years n = years n = years n = 77 /partner participating n = 79 (49.4%) No partner or no response n = 81 (50.6%) /partner participating n = 36 (36%) No partner or no response n = 64 (64%) /partner participating n = 31 (45.6%) No partner or no response n = 37 (54.4%) /partner participating n = 22 (71%) No partner or no response n = 9 (29%) /partner participating n = 36 (51.4%) No partner or no response n = 34 (48.6%) /partner participating n = 24 (66.7%) No partner or no response n = 12 (33.3%) /partner participating n = 36 (46.8%) No partner or no response n = 41 (53.2%), erectile dysfunction; TURP, transurethral resection of the prostate. TABLE 2 Inter-rater reliability analysis using Cohen s kappa coefficient Partner agrees n = 76 (96.2%) Partner differs n = 3 (3.8%) Partner agrees n = 31 (86%) Partner differs n = 5 (14%) Partner agrees n = 30 (96.8%) Partner differs n = 1 (3.2%) Partner agrees n = 17 (77.3%) Partner differs n = 5 (22.7%) Partner agrees n = 34 (94.4%) Partner differs n = 2 (5.6%) Partner agrees n = 22 (91.7%) Partner differs n = 2 (8.3%) Partner agrees n = 35 (97.2%) Partner differs n = 1 (2.8%) Time-point Kappa coefficient P valuese 95% confidence interval Pre-TURP < ( ) 6 months < ( ) 6 years < ( ) 12 years < ( ) Interpretation of Kappa coefficient values: , moderate; , good; 0.80, excellent. TURP, transurethral resection of the prostate. preoperatively, 27 (15%) men with preexisting reported improved sexual activity. Of the 120 men who were sexually active preoperatively, 73 (61%) completed the 6 months follow-up. All (100%) were still sexually active after TURP. No patient who was fully sexually active preoperatively reported developing. At the 6 years follow-up, 215 of the original 280 patients were still alive and 101 men (mean age 72 years) completed the SQ. Thirty-one (mean age 69 years) were sexually active with 77.3% of 22 partners in agreement and 70 men (mean age 73 years) had with 94.4% of 36 partners in agreement. Of the 73 sexually active patients who completed the 6 months follow-up, 47 (mean age 64 years) completed the 6 years follow-up. Of these, 30 (64%) were still sexually active. At the 12 years follow-up 164 of the original 280 patients were still alive. In all, 113 (mean age 77 years) completed the SQ and 60 partners completed the questionnaires. This response, considering the significant number of single or widowed men, reflected the zeal in tracing patients and partners for the final follow-up. Of the 113, 36 (mean age 73 years) were still sexually active with 91.7% of 24 partners in agreement and 77 (mean age 79 years) had with 97.2% of 36 partners in agreement. Inter-rater reliability scores (kappa coefficient) for patients and their partners are shown in Table 2, which shows a high level of agreement between patients and partners regarding the patients sexual activity status. DISCUSSION To our knowledge, no such data involving partners have been published, although one-shot sexual activity assessment by both man and partner showed good correlation [ 16 ]. In this study TURP was not associated with postoperatively. The long-term follow-up and corroboration by the partners are the main strong points of this study. These findings have several important implications for clinical practice. First, TURP was traditionally thought to be associated with so counselling was advocated during consent for the procedure. Erectile dysfunction has been reported in % [2 4 ] with one study noting postoperative as high as 81% [17 ]. The large variation is the result of differing definitions of /impotence, use of varied outcome measures (subjective and objective), varying follow-up duration and inclusion of procedures other than TURP (bladder neck incision/open prostatectomy) [ 2 ]. In the light of this study, counselling may need to be revisited. Second, this study has highlighted a crucial point; is common in patients with LUTS before treatment with 57% reporting preoperatively. A study of patients with BPH found a significant difference in sexual function between those with severe LUTS (44.2% unsuccessful coitus) and mild LUTS (13.1%) [7 ]. Reports of post-turp should be contextualized with the preoperative condition; reporting 81% postoperative is qualified by a preoperative figure of 86% [ 17 ]. A 12% after TURP when compared with 3% for equivalent general surgical procedures was noted [18 ] and was reported in 11.8% of 158 patients undergoing TURP or suprapubic/transvesical prostatectomy [19 ]
4 MISHRIKI ET AL. The importance of age in relation to is apparent in this study. men were younger preoperatively and at all follow-up stages although this was not significant. The Multinational Survey of the Aging Male involving over men linked to age and LUTS severity. correlated with age and the BPH impact index and with individual components of the International Prostatic Symptom Score (IPSS) notably nocturia and urgency [8 ]. Third, this study contradicts the concept that TURP damages sexual function. In one previous study, 56% of 168 men with BPH had poor sexual function and 46% were functionally impotent [11 ]. Objective assessment showed that patients who were fully potent preoperatively had 34.7% at 4 days but this had decreased to 8.3% at 3 months [ 4 ]. Rigiscan of nocturnal tumescence in addition to International Index of Erectile Function-15 reported 14% in 63 preoperatively potent men [20 ]. Fourth, this study has confirmed that TURP is associated with a 15% improvement in pre-existing contradicting several previous studies. Some studies are in agreement, noting postoperative improvement [5 ]. One previous study using the International Prostatic Symptom Score, BPH impact index and a sexual function questionnaire for four surgical options including TURP reported that none of the procedures caused although 48.6% in the TURP subcohort experienced reduction in ejaculation [17 ]. Another reported no significant change in postoperative (24%) vs preoperative (22%) impotence in 388 men undergoing TURP [21 ]. No change in sexual satisfaction and libido was found between preoperative and 12 months values after TURP in 155 men [ 18 ] and no difference was found between men undergoing TURP and inguinal hernia repair except for retrograde ejaculation [22 ]. Another study reported a significant increase in morning erections after TURP [17 ]. In the present study, patients were adequately counselled regarding postoperative retrograde ejaculation. This may account for the fact that none confused retrograde ejaculation with. There are no guidelines regarding retrograde ejaculation. It should be noted that even those studies showing no recorded absence or reduction of ejaculate [17,23 ]. Post-TURP retrograde ejaculation may explain the continued perception by patients that TURP is detrimental to sexual function. Studies comparing TURP and alternative surgical modalities show similar outcomes in all areas except retrograde ejaculation [17,23 ]. Details regarding ejaculation were not collected in this study and it would have been impossible for the partners to comment on or verify ejaculatory findings. Could TURP be actually beneficial in terms of sexual function outcome? The pathophysiology of after TURP remains unknown. Psychological factors such as loss of sexual self-confidence after TURP play a role [24 ]. Various treatments can both increase and decrease post-treatment sexual activity [25 ]. Few studies identified factors that may increase the risk of. These include age [4 ], diabetes mellitus [20 ], cardiovascular disease [26 ], relatively poor International Index of Erectile Function-15 and nocturnal tumescence scores [20 ], small adenoma size [3,4 ], intraoperative capsular perforation [3 ], and damage to penile small nerve fibres [27 ]. Some have shown mixed outcomes in the same study [28 ]. The US Food and Drug Administration approved sildenafil citrate, the first phosphodiesterase 5 inhibitor in March 1998 [29 ]. Active Viagra prescribing started in the UK in 1999, which is when the 6 years follow-up took place so it could not have affected the results. The 12 years follow-up may have been affected. The improvement in in this study is related to the improvement in LUTS after TURP, which was also corroborated by the partners and the results were published previously [12,13 ]. This is akin to the improvement in produced by alphablockers [9,10 ]. Surgical alternatives to TURP show a mixed picture. Transurethral microwave thermotherapy, interstitial laser coagulation, transurethral needle ablation and Holmium laser enucleation gave similar results to TURP regarding sexual function [24,30 ]. Laser therapy had a beneficial effect on pre-existing [7 ]. There was consistent agreement between patient and partner scores before and after TURP. The same SQ was completed by the patient and partner preoperatively, at 6 months, 6 years and 12 years. In this respect this study is unique. It is interesting to note that the partner had no difficulty commenting on specific topics in the SQ. This may provide an independent sexual function assessment source worthy of note during counselling. Statistically significant conformity was maintained throughout. In less than 3% of cases, at various follow-up stages, a man s test score was 8 whereas his partner s score was 0. Data analysis failed to find a reason for the variation and there is no plausible explanation. Readers can draw their own conclusions. Potential limitations include the design, conduct and reporting by a single group on a single site and no age-matched men not undergoing TURP. Attrition bias and lack of information from non-responders are also factors. It is possible to consider the non-responders as sexually inactive and therefore not interested in the questionnaire or as sexually active and simply not attending. The percentage of partners responding throughout the study was between 36% and 71%. Other limitations include the lack of an internationally accepted questionnaire at the time of the study initiation. The 12 years follow-up may have been biased by the presence of phosphodiesterase 5 inhibitors. In conclusion, this long-term prospective study in which partners actively participated confirms that is associated with LUTS and frequently precedes TURP. Improvement in was associated with improvement in LUTS. TURP probably does not adversely affect sexual function and in some cases preoperative can be improved by TURP. Furthermore, long-term sexual function continued to be maintained after TURP. These findings, corroborated by the partners, were significant. ACKNOWLGEMENTS The authors wish to thank Mrs Barbara Gibbons for encouraging partner involvement during the initial period, Mrs Edna Ledingham for patient and partner long-term follow-up and Mrs Penny Vale for proofreading the manuscript. CONFLICT OF INTEREST None declared
5 TURP AND SEX REFERENCES 1 NIH Consensus Development Panel on Impotence. Impotence. JAMA 1993 ; 270 : Emberton M, Neal DE, Black N et al. The effect of prostatectomy on symptom severity and quality of life. Br J Urol 1996 ; 77 : Bieri S, Iselin CE, Rohner S. Capsular perforation localization and adenoma size as prognostic indicators of erectile dysfunctional after transurethral prostatectomy. Scand J Urol Nephrol 1997 ; 3 : Tscholl R, Largo M, Poppinghaus E, Recker F, Subotic B. Incidence of erectile impotence secondary to transurethral resection of benign prostatic hyperplasia, assessed by preoperative and postoperative Snap Gauge tests. J Urol 1995 ; 153 : Brookes ST, Donovan JL, Peters TJ, Abrams P, Neal DE. Sexual dysfunction in men after treatment for lower urinary tract symptoms: evidence from randomised controlled trial. BMJ 2002 ; 324 : Wasson JH, Reda DJ, Bruskewitz RC, Elinson J, Keller AM, Henderson WG. A comparison of transurethral surgery with watchful waiting for moderate symptoms of benign prostatic hyperplasia. The Veterans Affairs Cooperative Study Group on Transurethral Resection of the Prostate. N Engl J Med 1995 ; 332 : Baniel J, Israilov S, Shmueli J, Segenreich E, Livne PM. Sexual function in 131 patients with benign prostatic hyperplasia before prostatectomy. Eur Urol 2000 ; 38 : Rosen R, Altwein J, Boyle P et al. Lower urinary tract symptoms and male sexual dysfunction: the multinational survey of the aging male (MSAM-7). Eur Urol 2003 ; 44 : H ö fner K, Claes H, De Reijke TM, Folkestad B, Speakman MJ. Tamulosin 0.4 mg once dailly: effect on sexual function in patients with lower urinary tract symptoms suggestive of benign prostatic obstruction. Eur Urol 1999 ; 36 : Vallancien G, Emberton M, Harving N, van Moorselaar RJ, Alf-One Study Group. Sexual dysfunction in 1,274 European men suffering from lower urinary tract symptoms. J Urol 2003 ; 169 : Namasivayam S, Minhas S, Brooke J, Joyce AD, Prescott S, Eardley I. The evaluation of sexual function in men presenting with symptomatic benign prostatic hyperplasia. Br J Urol 1998 ; 82 : Mishriki SF, Grimsley SJ, Nabi G, Cohen NP. Partners agree that the treatment of LUTS reduces patients bother and improves their quality of life. Prospective 12 years follow-up study. World J Urol 2010 ; 28 : Mishriki SF, Grimsley SJ, Nabi G, Cohen NP. Improved quality of life and enhanced satisfaction after TURP: prospective 12-year follow-up study. Urology 2008 ; 72 : Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A. The international index of erectile function (IIEF): a multidimensional scale for assessment of erectile dysfunction. Urology 1997 ; 49 : Boyle P, Robertson C, Mazzetta C et al. The prevalence of male urinary incontinence in four centres: the UREPIK study. BJU Int 2003 ; 92 : Boyle P, Robertson C, Mazzetta C et al. The association between lower urinary tract symptoms and erectile dysfunction in four centres: the UrEpik study. BJU Int 2003 ; 92 : Tuhkanen K, Heino A, Aaltomo S, Ala-Opas M. Sexual function of LUTS Patients before and after Neodymium Laser Prostatectomy and Transurethral Resection of Prostate. Urol Int 2004 ; 73 : Bolt JW, Evans C, Marshal VR. Sexual dysfunction after prostatectomy. Br J Urol 1987 ; 58 : Lindner A, Golomb J, Korzcak D, Keller T, Siegal Y. Effects of prostatectomy on sexual function. Urology 1991 ; 38 : Taher A. Erectile dysfunction after transurethral resection of the prostate: incidence and risk factors. World J Urol 2004 ; 22 : Doll HA, Black NA, McPherson K, Flood AB, Williams GB, Smith JC. Mortality, morbidity and complications following transurethral resection of the prostate for benign prostatic hypertrophy. J Urol 1992 ; 147 : Libman E, Fichten CS, Rothenberg P et al. Prostatectomy and inguinal hernia repair: a comparison of the sexual consequences. J Sex Marital Ther 1991 ; 17 : Arai Y, Aoki Y, Okubo K et al. Impact of interventional therapy for benign prostatic hyperplasia on quality of life and sexual function: a prospective study. J Urol 2000 ; 164 : Libman E, Fichten CS, Creti L, Weinstein N, Amsel R, Brender W. Transurethral prostatectomy: differential effects of age category and presurgery sexual functioning on postprostatectomy sexual adjustment. J Behav Med 1989 ; 12 : Leliefeld HH, Stoevelaar HJ, McDonnell J. Sexual function before and after various treatments for symptomatic benign prostatic hyperplasia. BJU Int 2002 ; 89 : De Giorgi G, Luciani LG, Valotto C, Isola M, Zattoni F. Role of risk factors for erectile dysfunction in patients undergoing transurethral resection of the prostate: early impact on sexual function. Arch Ital Urol Androl 2005 ; 77 : Lefaucheur JP, Yiou R, Salomon L, Chopin DK, Abbou CC. Assessment of penile small nerve fiber damage after transurethral resection of the prostate by measurement of penile thermal sensation. J Urol 2000 ; 164 : De Baker E, Lauwerijns A, Willem C. Sexual behaviour after prostatectomy. Eur Urol 1977 ; 3 : Goldenberg MM. Safety and efficacy of sildenafil citrate in the treatment of male erectile dysfunction. Clin Ther 1998 ; 20 : Briganti A, Naspro R, Gallina A et al. Impact on sexual function of holmium laser enucleation versus transurethral resection of the prostate: results of a prospective, 2-center, randomized trial. J Urol 2006 ; 175 : Correspondence: Said Fadel Mishriki, Department of Urology, Aberdeen Royal Infirmary Hospital, Aberdeen AB25 2ZN, Scotland, UK. smishriki@nhs.net Abbreviations : BPH, benign prostatic hyperplasia ;, erectile dysfunction ; TURP, transurethral resection of the prostate
6 MISHRIKI ET AL. APPENDIX 1. SEX QUESTIONNAIRE FOR PATIENT SEXUAL QUESTIONNAIRE Sex questionnaire Patient of Study number Sex score 1. Over the past month or so have you had any interest in sex? No 0 2. Over the past month or so, have you had any kind of sexual activity (intercourse, masturbation etc.)? No 0 3. Over the past month or so, how often have you been able to have sexual erections when you were sexually stimulated? Not at all 0 Less than 1 time in 5 1 Less than half the time 2 About half the time 3 More than half the time 4 Almost always 5 4. Over the past month or so, how would you rate your erections? Not firm enough to have intercourse 0 Firm enough to have intercourse 1 APPENDIX 2. SEX QUESTIONNAIRE FOR PARTNER Sex questionnaire partner Partner of Patient Study Number Sex score SEXUAL QUESTIONNAIRE 1. Over the past month or so has your partner had any interest in sex? No 0 (if no, ignore questions 3 and 4) 2. Over the past month or so, has your partner had any kind of sexual activity (intercourse, masturbation etc.)? No 0 (if no, ignore questions 3 and 4) 3. Over the past month or so, how often has your partner been able to have sexual erections when sexually stimulated? Not at all 0 Less than 1 time in 5 1 Less than half the time 2 About half the time 3 More than half the time 4 Almost always 5 4. Over the past month or so, how would you rate the erections? Not firm enough to have intercourse 0 Firm enough to have intercourse
Evaluation of Sexual Dysfunction in Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Patients
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/10 Evaluation of Sexual Dysfunction in Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Patients N. Narayanamoorthy,
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/10 Evaluation of Sexual Dysfunction in Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Patients N. Narayanamoorthy,
Erectile dysfunction after transurethral prostatectomy for lower urinary tract symptoms: results from a center with over 500 patients
 Asian J Androl 2006; 8 (1): 69 74 DOI: 10.1111/j.1745-7262.2006.00088.x. Original Article. Erectile dysfunction after transurethral prostatectomy for lower urinary tract symptoms: results from a center
Asian J Androl 2006; 8 (1): 69 74 DOI: 10.1111/j.1745-7262.2006.00088.x. Original Article. Erectile dysfunction after transurethral prostatectomy for lower urinary tract symptoms: results from a center
ORIGINAL ARTICLE Effect of transurethral resection of the prostate on erectile function: a prospective comparative study
 (2010) 22, 146 151 & 2010 Nature Publishing Group All rights reserved 0955-9930/10 $32.00 www.nature.com/ijir ORIGINAL ARTICLE Effect of transurethral resection of the prostate on erectile function: a
(2010) 22, 146 151 & 2010 Nature Publishing Group All rights reserved 0955-9930/10 $32.00 www.nature.com/ijir ORIGINAL ARTICLE Effect of transurethral resection of the prostate on erectile function: a
Overview. Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia. Iain McAuley September 15, 2014
 Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
NOTE: This policy is not effective until April 1, Transurethral Water Vapor Thermal Therapy of the Prostate
 NOTE: This policy is not effective until April 1, 2019. Medical Policy Manual Surgery, Policy No. 210 Transurethral Water Vapor Thermal Therapy of the Prostate Next Review: December 2019 Last Review: December
NOTE: This policy is not effective until April 1, 2019. Medical Policy Manual Surgery, Policy No. 210 Transurethral Water Vapor Thermal Therapy of the Prostate Next Review: December 2019 Last Review: December
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Sexual Function after Transurethral Resection of the Prostate (TURP): Results of an Independent Prospective Multicentre Assessment of Outcome
 european urology 52 (2007) 510 516 available at www.sciencedirect.com journal homepage: www.europeanurology.com Benign Prostatic Enlargement Bladder Outlet Obstruction Sexual Function after Transurethral
european urology 52 (2007) 510 516 available at www.sciencedirect.com journal homepage: www.europeanurology.com Benign Prostatic Enlargement Bladder Outlet Obstruction Sexual Function after Transurethral
BPH: a present and future perspective on health impact
 BPH: a present and future perspective on health impact Burden of disease in men with moderate LUTS Dalibor Pacík This presentation is financially supported by GlaxoSmithKline. CZ/DUTT/0019/12 Men with
BPH: a present and future perspective on health impact Burden of disease in men with moderate LUTS Dalibor Pacík This presentation is financially supported by GlaxoSmithKline. CZ/DUTT/0019/12 Men with
50% of men. 90% of men PATIENT FACTSHEET: BPH CONDITION AND TREATMENTS. Want more information? What are the symptoms?
 PATIENT FACTSHEET: BPH CONDITION AND TREATMENTS What is Benign Prostatic Hyperplasia (enlarged prostate)? Benign prostatic hyperplasia (BPH) is a noncancerous enlargement of the prostate, the gland that
PATIENT FACTSHEET: BPH CONDITION AND TREATMENTS What is Benign Prostatic Hyperplasia (enlarged prostate)? Benign prostatic hyperplasia (BPH) is a noncancerous enlargement of the prostate, the gland that
Change in intraoperative rectal temperature influencing erectile dysfunction following transurethral resection of the prostate
 Journal of the Formosan Medical Association (2012) 111, 320e324 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Change in intraoperative rectal temperature
Journal of the Formosan Medical Association (2012) 111, 320e324 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Change in intraoperative rectal temperature
Assessment of Erectile and Ejaculatory Function after Penile Prosthesis Implantation
 www.kjurology.org DOI:.4/kju.2.5.3.22 Sexual Dysfunction/Infertility Assessment of Erectile and Ejaculatory Function after Penile Prosthesis Implantation Jang Ho Bae, Phil Hyun Song, Hyun Tae Kim, Ki Hak
www.kjurology.org DOI:.4/kju.2.5.3.22 Sexual Dysfunction/Infertility Assessment of Erectile and Ejaculatory Function after Penile Prosthesis Implantation Jang Ho Bae, Phil Hyun Song, Hyun Tae Kim, Ki Hak
EAU GUIDELINES POCKET EDITION 3
 EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
Treating BPH: Comparing Rezum UroLift and HoLEP
 Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
Original Policy Date
 MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA
 St. Louis Hospital PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA INITIAL CLINICAL RESULTS Faculty of Medical Sciences New University of Lisbon JOÃO PISCO LUÍS CAMPOS PINHEIRO TIAGO BILHIM HUGO RIO TINTO
St. Louis Hospital PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA INITIAL CLINICAL RESULTS Faculty of Medical Sciences New University of Lisbon JOÃO PISCO LUÍS CAMPOS PINHEIRO TIAGO BILHIM HUGO RIO TINTO
A prospective study of sexual dysfunction in patients with benign prostatic hyperplasia
 International Surgery Journal Leelakrishna P et al. Int Surg J. 218 Mar;5(3):82-89 http://www.ijsurgery.com pissn 2349-335 eissn 2349-292 Original Research Article DOI: http://dx.doi.org/1.1823/2349-292.isj2185
International Surgery Journal Leelakrishna P et al. Int Surg J. 218 Mar;5(3):82-89 http://www.ijsurgery.com pissn 2349-335 eissn 2349-292 Original Research Article DOI: http://dx.doi.org/1.1823/2349-292.isj2185
The Journal of International Medical Research 2012; 40:
 The Journal of International Medical Research 2012; 40: 899 908 Comparison of α-blocker Monotherapy and α-blocker Plus 5α-Reductase Inhibitor Combination Therapy Based on Prostate Volume for Treatment
The Journal of International Medical Research 2012; 40: 899 908 Comparison of α-blocker Monotherapy and α-blocker Plus 5α-Reductase Inhibitor Combination Therapy Based on Prostate Volume for Treatment
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
Trans Urethral Resection of Prostate (TURP)
 Trans Urethral Resection of Prostate (TURP) Patient Information Author ID: SF Leaflet Number: Urol 010 Version: 6 Name of Leaflet: Trans Urethral Resection of Prostate (TURP) Date Produced: March 2018
Trans Urethral Resection of Prostate (TURP) Patient Information Author ID: SF Leaflet Number: Urol 010 Version: 6 Name of Leaflet: Trans Urethral Resection of Prostate (TURP) Date Produced: March 2018
European Urology 48 (2005)
 European Urology European Urology 48 (2005) 269 276 BPH/Prostatic Diseases Evaluation of Male Sexual Function in Patients with Lower UrinaryTract Symptoms (LUTS) Associated with Benign Prostatic Hyperplasia
European Urology European Urology 48 (2005) 269 276 BPH/Prostatic Diseases Evaluation of Male Sexual Function in Patients with Lower UrinaryTract Symptoms (LUTS) Associated with Benign Prostatic Hyperplasia
for ED and LUTS/BPH Pierre Sarkis, M.D. Assistant Professor Fellow of the European Board of Urology
 Tadalafil 5 mg once daily for ED and LUTS/BPH Pierre Sarkis, M.D. Assistant Professor Fellow of the European Board of Urology Why this conference? Not promotional but educational The pharmacist regularly
Tadalafil 5 mg once daily for ED and LUTS/BPH Pierre Sarkis, M.D. Assistant Professor Fellow of the European Board of Urology Why this conference? Not promotional but educational The pharmacist regularly
All about the Prostate
 MEN S HEALTH Dr Nick Pendleton January 16 th 2018 All about the Prostate 1 What does it do? Functions of the Prostate 1. Secretes Prostatic Fluid slightly alkaline fluid, 30% of volume of seminal fluid,
MEN S HEALTH Dr Nick Pendleton January 16 th 2018 All about the Prostate 1 What does it do? Functions of the Prostate 1. Secretes Prostatic Fluid slightly alkaline fluid, 30% of volume of seminal fluid,
Benign Prostatic Hyperplasia (BPH):
 Benign Prostatic Hyperplasia (BPH): Evidence Based Guidelines for Primary Care Providers Jeanne Martin, DNP, ANP-BC Objectives 1. Understand the pathophysiology and prevalence of BPH 2. Select the appropriate
Benign Prostatic Hyperplasia (BPH): Evidence Based Guidelines for Primary Care Providers Jeanne Martin, DNP, ANP-BC Objectives 1. Understand the pathophysiology and prevalence of BPH 2. Select the appropriate
Rezūm procedure for the Prostate
 Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Benign Prostatic Hyperplasia (BPH)
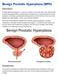 Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP)
 JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
REPORTS. Clinical and Economic Outcomes in Patients Treated for Enlarged Prostate
 Clinical and Economic Outcomes in Patients Treated for Enlarged Prostate Michael James Naslund, MD, MBA; Muta M. Issa, MD, MBA; Amy L. Grogg, PharmD; Michael T. Eaddy, PharmD, PhD; and Libby Black, PharmD
Clinical and Economic Outcomes in Patients Treated for Enlarged Prostate Michael James Naslund, MD, MBA; Muta M. Issa, MD, MBA; Amy L. Grogg, PharmD; Michael T. Eaddy, PharmD, PhD; and Libby Black, PharmD
Effect of Transurethral Resection of the Prostate Based on the Degree of Obstruction Seen in Urodynamic Study
 www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.12.840 Voiding Dysfunction/Female Urology Effect of Transurethral Resection of the Prostate Based on the Degree of Obstruction Seen in Urodynamic
www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.12.840 Voiding Dysfunction/Female Urology Effect of Transurethral Resection of the Prostate Based on the Degree of Obstruction Seen in Urodynamic
Original Article - Lasers in Urology. Min Ho Lee, Hee Jo Yang, Doo Sang Kim, Chang Ho Lee, Youn Soo Jeon
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
ISSN: (Print) (Online) Journal homepage:
 Archives of Andrology Journal of Reproductive Systems ISSN: 0148-5016 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iaan19 CHANGE IN INTERNATIONAL PROSTATE SYMPTOM SCORE AFTER TRANSURETHRAL
Archives of Andrology Journal of Reproductive Systems ISSN: 0148-5016 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iaan19 CHANGE IN INTERNATIONAL PROSTATE SYMPTOM SCORE AFTER TRANSURETHRAL
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Limited text update March 2016) S. Gravas (Chair), T. Bach, A. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher,
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Limited text update March 2016) S. Gravas (Chair), T. Bach, A. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher,
Wednesday 25 June Poster Session 9: BPH 1 Chairmen: M. Speakman and D. Rosario
 Wednesday 25 June 14.30 15.30 Poster Session 9: BPH 1 Chairmen: M. Speakman and D. Rosario P080 Unreliable residual volume measurement after increased water load diuresis G. ALIVIZATOS, A. SKOLARIKOS,
Wednesday 25 June 14.30 15.30 Poster Session 9: BPH 1 Chairmen: M. Speakman and D. Rosario P080 Unreliable residual volume measurement after increased water load diuresis G. ALIVIZATOS, A. SKOLARIKOS,
Benign Prostatic Hyperplasia: Update on Innovative Current Treatments
 Benign Prostatic Hyperplasia: Update on Innovative Current Treatments Michael Ferrandino, MD As.soc Professor Director of Minimally Invasive Urologic Surgery Division of Urologic Surgery Duke University
Benign Prostatic Hyperplasia: Update on Innovative Current Treatments Michael Ferrandino, MD As.soc Professor Director of Minimally Invasive Urologic Surgery Division of Urologic Surgery Duke University
Sexual Dysfunction in Aging Men With Lower Urinary Tract Symptoms
 Sexual Dysfunction and Infertility Sexual Dysfunction in Aging Men With Lower Urinary Tract Symptoms Darab Mehraban, Gholam Hossein Naderi, Seyed Reza Yahyazadeh, Mahdi Amirchaghmaghi Introduction: Our
Sexual Dysfunction and Infertility Sexual Dysfunction in Aging Men With Lower Urinary Tract Symptoms Darab Mehraban, Gholam Hossein Naderi, Seyed Reza Yahyazadeh, Mahdi Amirchaghmaghi Introduction: Our
GUIDELINES ON NON-NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (BPO)
 GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (BPO) (Text update pril 2014) S. Gravas (chair),. Bachmann,. Descazeaud, M. Drake, C. Gratzke, S. Madersbacher, C. Mamoulakis,
GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (BPO) (Text update pril 2014) S. Gravas (chair),. Bachmann,. Descazeaud, M. Drake, C. Gratzke, S. Madersbacher, C. Mamoulakis,
Benign enlargement of prostate (BEP), which is. Early Experiences with HoLEP. Original Article ABSTRACT INTRODUCTION. Bhandari BB*
 Original Article Early Experiences with HoLEP Bhandari BB* * Consultant Urologist, Shree Birendra Army Hospital, Norvic International Hospital, Alka Hospital ABSTRACT introduction: Holmium Laser Enucleation
Original Article Early Experiences with HoLEP Bhandari BB* * Consultant Urologist, Shree Birendra Army Hospital, Norvic International Hospital, Alka Hospital ABSTRACT introduction: Holmium Laser Enucleation
Name of Policy: Transurethral Microwave Thermotherapy
 Name of Policy: Transurethral Microwave Thermotherapy Policy #: 449 Latest Review Date: September 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable
Name of Policy: Transurethral Microwave Thermotherapy Policy #: 449 Latest Review Date: September 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
MMM. Topic The use of Tadalafil 5mg daily for the treatment of BPH-LUTS
 Dr Tan & Partners MMM Vol. 1 No. 1 Morbidity & Mortality Meeting 14 th November 2014 Introduction Topic The use of Tadalafil 5mg daily for the treatment of BPH-LUTS Tadalafil 5mg daily is a well established
Dr Tan & Partners MMM Vol. 1 No. 1 Morbidity & Mortality Meeting 14 th November 2014 Introduction Topic The use of Tadalafil 5mg daily for the treatment of BPH-LUTS Tadalafil 5mg daily is a well established
Can men with prostates sized 80 ml or larger be managed conservatively?
 Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Text update March 2017) S. Gravas (Chair), T. Bach, M. Drake, M. Gacci, C. Gratzke, T.R.W. Herrmann, S. Madersbacher,
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Text update March 2017) S. Gravas (Chair), T. Bach, M. Drake, M. Gacci, C. Gratzke, T.R.W. Herrmann, S. Madersbacher,
VOIDING DYSFUNCTION IN ELDERLY MALE CURRENT STATUS
 VOIDING DYSFUNCTION IN ELDERLY MALE CURRENT STATUS DR. FRANCIS LEE Voiding dysfunction Storage Emptying Common voiding dysfunction in elderly male Emptying BPH Storage Incontinence Overactive bladder Post-prostatectomy
VOIDING DYSFUNCTION IN ELDERLY MALE CURRENT STATUS DR. FRANCIS LEE Voiding dysfunction Storage Emptying Common voiding dysfunction in elderly male Emptying BPH Storage Incontinence Overactive bladder Post-prostatectomy
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
MODULE 3: BENIGN PROSTATIC HYPERTROPHY
 MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of prostatic urethral lift implants to treat lower urinary tract symptoms
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of prostatic urethral lift implants to treat lower urinary tract symptoms
This is the author version of an article originally published in. World Journal of Urology 2010;28(1):23-32.
 This is the author version of an article originally published in World Journal of Urology 2010;28(1):23-32. http://www.springerlink.com/content/l5042x96550407m5/?p=aa95561773704ad99add75 87e77e7450&pi=4
This is the author version of an article originally published in World Journal of Urology 2010;28(1):23-32. http://www.springerlink.com/content/l5042x96550407m5/?p=aa95561773704ad99add75 87e77e7450&pi=4
A Comparative Study of Trans Urethral Resection Versus Trans Urethral Incision for Small Size Obstructing Prostate
 ORIGINAL ARTICLE A Comparative Study of Trans Urethral Resection Versus Trans Urethral Incision for Small Size Obstructing Prostate ABSTRACT Rafique Ahmed Sahito, Abdul Jabbar Pirzada, Masood Ahmed Qureshi,
ORIGINAL ARTICLE A Comparative Study of Trans Urethral Resection Versus Trans Urethral Incision for Small Size Obstructing Prostate ABSTRACT Rafique Ahmed Sahito, Abdul Jabbar Pirzada, Masood Ahmed Qureshi,
GUIDELINES ON NON-NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (Text update March 2015) S. Gravas (Chair), T. Bach,. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher, C. Mamoulakis,
GUIDELINES ON NON-NEUROGENIC MLE LUTS INCLUDING BENIGN PROSTTIC OBSTRUCTION (Text update March 2015) S. Gravas (Chair), T. Bach,. Bachmann, M. Drake, M. Gacci, C. Gratzke, S. Madersbacher, C. Mamoulakis,
Will Medical Management of Benign Prostatic Hyperplasia Result in Better or Worse Sexual Function in Men?
 Urol Sci 2011;22(1):14 18 MINI REVIEW Will Medical Management of Benign Prostatic Hyperplasia Result in Better or Worse Sexual Function in Men? Thomas I.S. Hwang 1,2,3 * 1 Shin Kong WHS Hospital, Taipei,
Urol Sci 2011;22(1):14 18 MINI REVIEW Will Medical Management of Benign Prostatic Hyperplasia Result in Better or Worse Sexual Function in Men? Thomas I.S. Hwang 1,2,3 * 1 Shin Kong WHS Hospital, Taipei,
Impact of Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Treatment with Tamsulosin and Solifenacin Combination Therapy on Erectile Function
 www.kjurology.org DOI:10.4111/kju.2011.52.1.49 Sexual Dysfunction Impact of Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Treatment with Tamsulosin and Solifenacin Combination Therapy on Erectile
www.kjurology.org DOI:10.4111/kju.2011.52.1.49 Sexual Dysfunction Impact of Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Treatment with Tamsulosin and Solifenacin Combination Therapy on Erectile
JMSCR Vol 04 Issue 10 Page October 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i10.40 Combined Bladder Stones Removal: In
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i10.40 Combined Bladder Stones Removal: In
Prostate Artery Embolization
 Prostate Artery Embolization in the office interventional suite Robert J. Kennedy, M.D. Interventional & Vascular Center Melbourne, Florida The speaker has no financial conflicts of interest to disclose.
Prostate Artery Embolization in the office interventional suite Robert J. Kennedy, M.D. Interventional & Vascular Center Melbourne, Florida The speaker has no financial conflicts of interest to disclose.
Diagnosis and Mangement of Nocturia in Adults
 Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Male Lower Urinary Tract Symptoms: Management in primary care and beyond. Daniel Cohen PhD FRCS(Urol) Consultant Urological Surgeon
 Male Lower Urinary Tract Symptoms: Management in primary care and beyond Daniel Cohen PhD FRCS(Urol) Consultant Urological Surgeon 1 LUTS Very common: 1/3 men over age of 50 have moderate to severe LUTS
Male Lower Urinary Tract Symptoms: Management in primary care and beyond Daniel Cohen PhD FRCS(Urol) Consultant Urological Surgeon 1 LUTS Very common: 1/3 men over age of 50 have moderate to severe LUTS
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of transurethral water vapour ablation for lower urinary tract symptoms caused by
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of transurethral water vapour ablation for lower urinary tract symptoms caused by
Management of Voiding Problems in Older Men. Dr. John Fenn Consultant, QEH 10 th October, 2005
 Management of Voiding Problems in Older Men Dr. John Fenn Consultant, QEH 10 th October, 2005 Voiding Problems Poor stream Hesitancy Straining Incomplete emptying Intermittent micturition Terminal dribbling
Management of Voiding Problems in Older Men Dr. John Fenn Consultant, QEH 10 th October, 2005 Voiding Problems Poor stream Hesitancy Straining Incomplete emptying Intermittent micturition Terminal dribbling
The Evolution of Combination Therapy. US men eligible for BPH treatment * with projected population changes
 The Management of BPH & The Impact of Combination Therapy Results Combination of Avodart and Tamsulosin (CombAT) Medical Therapy of Prostate Symptoms (MTOPS) Dr. Jack Barkin, md, fics, facs, dabu, Mcert
The Management of BPH & The Impact of Combination Therapy Results Combination of Avodart and Tamsulosin (CombAT) Medical Therapy of Prostate Symptoms (MTOPS) Dr. Jack Barkin, md, fics, facs, dabu, Mcert
Abstract. Key words Trial without catheter, Acute urinary retention, Benign prostatic hyperplasia, Introduction
 The role of sustained-released alfuzosin in the treatment of acute urinary retention Mohamed Fawzi Ahmed. Department of Surgery, Ninevah College of Medicine, University of Mosul. Abstract To see whether
The role of sustained-released alfuzosin in the treatment of acute urinary retention Mohamed Fawzi Ahmed. Department of Surgery, Ninevah College of Medicine, University of Mosul. Abstract To see whether
Evidence based urology in practice: heterogeneity in a systematic review meta-analysis. Health Services Research Unit, University of Aberdeen, UK
 Version 6, 12/10/2009 Evidence based urology in practice: heterogeneity in a systematic review meta-analysis Mari Imamura 1, Jonathan Cook 2, Sara MacLennan 1, James N Dow 1 and Philipp Dahm 3 for the
Version 6, 12/10/2009 Evidence based urology in practice: heterogeneity in a systematic review meta-analysis Mari Imamura 1, Jonathan Cook 2, Sara MacLennan 1, James N Dow 1 and Philipp Dahm 3 for the
Prostate Overview Quiz
 Prostate Overview Quiz 1. The path report reads: Gleason 3 + 4 = 7. The Gleason s score is a. 3 b. 4 c. 7 d. None of the above 2. The path report reads: Moderately differentiated adenocarcinoma of the
Prostate Overview Quiz 1. The path report reads: Gleason 3 + 4 = 7. The Gleason s score is a. 3 b. 4 c. 7 d. None of the above 2. The path report reads: Moderately differentiated adenocarcinoma of the
Effects of Low-Dose Tamsulosin on Sexual Function in Patients With Lower Urinary Tract Symptoms Suggestive of Benign Prostatic Hyperplasia
 www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.10.697 Sexual Dysfunction/Male Infertility Effects of Low-Dose Tamsulosin on Sexual Function in Patients With Lower Urinary Tract Symptoms Suggestive
www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.10.697 Sexual Dysfunction/Male Infertility Effects of Low-Dose Tamsulosin on Sexual Function in Patients With Lower Urinary Tract Symptoms Suggestive
Transurethral Prostatic Resection for Acute Urinary Retention in Patients with Prostate Cancer
 ORIGINAL ARTICLE Transurethral Prostatic Resection for Acute Urinary Retention in Patients with Prostate Cancer Chang-Chi Chang, Junne-Yih Kuo*, Kuang-Kuo Chen, Alex Tong-Long Lin, Yen-Hwa Chang, Howard
ORIGINAL ARTICLE Transurethral Prostatic Resection for Acute Urinary Retention in Patients with Prostate Cancer Chang-Chi Chang, Junne-Yih Kuo*, Kuang-Kuo Chen, Alex Tong-Long Lin, Yen-Hwa Chang, Howard
INVESTIGATION OF LOWER URINARY TRACT SYMPTOMS IN UROLOGICAL OUTPATIENTS USING ORIGINAL IPSS PLUS POST MICTURITION DRIBBLE QUESTIONNAIRE
 INVESTIGATION OF LOWER URINARY TRACT SYMPTOMS IN UROLOGICAL OUTPATIENTS USING ORIGINAL IPSS PLUS POST MICTURITION DRIBBLE QUESTIONNAIRE Tadashi Hanail*, Seiji Matsumotol*, Nobutaka Shimizu, Hirotsugu Uemural
INVESTIGATION OF LOWER URINARY TRACT SYMPTOMS IN UROLOGICAL OUTPATIENTS USING ORIGINAL IPSS PLUS POST MICTURITION DRIBBLE QUESTIONNAIRE Tadashi Hanail*, Seiji Matsumotol*, Nobutaka Shimizu, Hirotsugu Uemural
Increasing Awareness, Diagnosis, and Treatment of BPH, LUTS, and EP
 Introduction to Enlarged Prostate E. David Crawford, MD Professor of Surgery (Urology) and Radiation Oncology Head, Urologic Oncology E. David Crawford Endowed Chair in Urologic Oncology University of
Introduction to Enlarged Prostate E. David Crawford, MD Professor of Surgery (Urology) and Radiation Oncology Head, Urologic Oncology E. David Crawford Endowed Chair in Urologic Oncology University of
Korean Urologist s View of Practice Patterns in Diagnosis and Management of Benign Prostatic Hyperplasia: A Nationwide Survey
 Original Article DOI 10.3349/ymj.2010.51.2.248 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(2):248-252, 2010 Korean Urologist s View of Practice Patterns in Diagnosis and Management of Benign Prostatic
Original Article DOI 10.3349/ymj.2010.51.2.248 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(2):248-252, 2010 Korean Urologist s View of Practice Patterns in Diagnosis and Management of Benign Prostatic
Measurement Properties of the Malay Version of the Golombok-Rust Inventory of Marital State (GRIMS) Among Urological Patients.
 ORIGINAL PAPER Measurement Properties of the Malay Version of the Golombok-Rust Inventory of Marital State (GRIMS) Among Urological Patients. Quek Kia Fatt, Low Wah Yun, And Hassan Razack, Loh Chit Sin,
ORIGINAL PAPER Measurement Properties of the Malay Version of the Golombok-Rust Inventory of Marital State (GRIMS) Among Urological Patients. Quek Kia Fatt, Low Wah Yun, And Hassan Razack, Loh Chit Sin,
Executive Summary. Non-drug local procedures for treatment of benign prostatic hyperplasia 1. IQWiG Reports - Commission No.
 IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
Clinical evaluation of Tentex forte and Himcolin cream in the treatment of functional erectile dysfunction
 Medicine Update (2004): 11(9), 47-51 Clinical evaluation of Tentex forte and Himcolin cream in the treatment of functional erectile dysfunction Dr. Roumen Bostandjiev, Ph.D. Founder and Director of Sexology
Medicine Update (2004): 11(9), 47-51 Clinical evaluation of Tentex forte and Himcolin cream in the treatment of functional erectile dysfunction Dr. Roumen Bostandjiev, Ph.D. Founder and Director of Sexology
Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj
 Original Article Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj Abstract Objectives: Prospective evaluation
Original Article Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj Abstract Objectives: Prospective evaluation
Long-term Follow-up of Transurethral Enucleation Resection of the Prostate for Symptomatic Benign Prostatic Hyperplasia
 Journal of Surgery 2016; 4(2): 40-44 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160402.18 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Long-term Follow-up of Transurethral Enucleation
Journal of Surgery 2016; 4(2): 40-44 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160402.18 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Long-term Follow-up of Transurethral Enucleation
100% Effective Natural Hormone Treatment Menopause, Andropause And Other Hormone Imbalances Impair Healthy Healing In People Over The Age Of 30!
 This Free E Book is brought to you by Natural Aging.com. 100% Effective Natural Hormone Treatment Menopause, Andropause And Other Hormone Imbalances Impair Healthy Healing In People Over The Age Of 30!
This Free E Book is brought to you by Natural Aging.com. 100% Effective Natural Hormone Treatment Menopause, Andropause And Other Hormone Imbalances Impair Healthy Healing In People Over The Age Of 30!
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
Last Review Status/Date: December Summary
 Section: Surgery Effective Date: January 15, 2016 Subject: Prostatic Urethral Lift Page: 1 of 9 Last Review Status/Date: December 2015 Summary Benign prostatic hyperplasia (BPH) is a common condition in
Section: Surgery Effective Date: January 15, 2016 Subject: Prostatic Urethral Lift Page: 1 of 9 Last Review Status/Date: December 2015 Summary Benign prostatic hyperplasia (BPH) is a common condition in
Transurethral Prostatectomy: Differential Effects of Age Category and Presurgery Sexual Functioning on Postprostatectomy Sexual Adjustment
 Journal of Behavioral Medicine, VoL 12, No. 5, 1989 Transurethral Prostatectomy: Differential Effects of Age Category and Presurgery Sexual Functioning on Postprostatectomy Sexual Adjustment Eva Libman,
Journal of Behavioral Medicine, VoL 12, No. 5, 1989 Transurethral Prostatectomy: Differential Effects of Age Category and Presurgery Sexual Functioning on Postprostatectomy Sexual Adjustment Eva Libman,
Consensus Meeting for Asian-Pacific BPH Guideline
 Consensus Meeting for Asian-Pacific BPH Guideline Byung Ha Chung Yonsei University Health System S a t e l l i t e S y m p o s i u m I Contents Diagnosis and Treatment Guidelines for BPH Prostate Volume
Consensus Meeting for Asian-Pacific BPH Guideline Byung Ha Chung Yonsei University Health System S a t e l l i t e S y m p o s i u m I Contents Diagnosis and Treatment Guidelines for BPH Prostate Volume
What is Benign Prostatic Hyperplasia (BPH)?
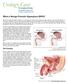 What is Benign Prostatic Hyperplasia (BPH)? Benign prostatic hyperplasia (BPH) is an enlarged prostate. The prostate goes through two main growth periods as a man ages. The first occurs early in puberty,
What is Benign Prostatic Hyperplasia (BPH)? Benign prostatic hyperplasia (BPH) is an enlarged prostate. The prostate goes through two main growth periods as a man ages. The first occurs early in puberty,
REVIEW Validated questionnaires for assessing sexual dysfunction and BPH/LUTS: solidifying the common pathophysiologic link
 (2008) 20, S27 S32 & 2008 Nature Publishing Group All rights reserved 0955-9930/08 $30.00 www.nature.com/ijir REVIEW Validated questionnaires for assessing sexual dysfunction and BPH/LUTS: solidifying
(2008) 20, S27 S32 & 2008 Nature Publishing Group All rights reserved 0955-9930/08 $30.00 www.nature.com/ijir REVIEW Validated questionnaires for assessing sexual dysfunction and BPH/LUTS: solidifying
Current drug management of BPH in primary care Claire Taylor MRCS, Charlotte Foley MRCS and Roger Kirby MA, MD, FRCS Urol
 Drug review BPH Current drug management of BPH in primary care Claire Taylor MRCS, Charlotte Foley MRCS and Roger Kirby MA, MD, FRCS Urol Skyline Imaging Ltd The range of drug treatments for BPH, alone
Drug review BPH Current drug management of BPH in primary care Claire Taylor MRCS, Charlotte Foley MRCS and Roger Kirby MA, MD, FRCS Urol Skyline Imaging Ltd The range of drug treatments for BPH, alone
Peter T. Chin, Damien M. Bolton, Greg Jack, Prem Rashid, Jeffrey Thavaseelan, R. James Yu, Claus G. Roehrborn, and Henry H. Woo
 Rapid Communication Prostatic Urethral Lift: Two-year Results After Treatment for Lower Urinary Tract Symptoms Secondary to Benign Prostatic Hyperplasia Peter T. Chin, Damien M. Bolton, Greg Jack, Prem
Rapid Communication Prostatic Urethral Lift: Two-year Results After Treatment for Lower Urinary Tract Symptoms Secondary to Benign Prostatic Hyperplasia Peter T. Chin, Damien M. Bolton, Greg Jack, Prem
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA. A Minimally Invasive Innovative Treatment
 PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
The Global Online Sexuality Survey (GOSS) 2015: Erectile Dysfunction Among English-Speaking Internet Users in the United States
 Original Article The Global Online Sexuality Survey (GOSS) 2015: Erectile Dysfunction Among English-Speaking Internet Users in the United States Osama Shaeer 1, Kamal Shaeer 2, Mikkel 3, Fode, Ege Serefoglu
Original Article The Global Online Sexuality Survey (GOSS) 2015: Erectile Dysfunction Among English-Speaking Internet Users in the United States Osama Shaeer 1, Kamal Shaeer 2, Mikkel 3, Fode, Ege Serefoglu
Ambulatory Try off Catheter (ATOC) Program for the Patient with Acute Retention of Urine Outpatient Service
 Ambulatory Try off Catheter (ATOC) Program for the Patient with Acute Retention of Urine Outpatient Service Mr. Tang, Chi Chiu Kevin (APN) Urology Center Department of Surgery Kwong Wah Hospital Redevelopment
Ambulatory Try off Catheter (ATOC) Program for the Patient with Acute Retention of Urine Outpatient Service Mr. Tang, Chi Chiu Kevin (APN) Urology Center Department of Surgery Kwong Wah Hospital Redevelopment
EVALUATION OF THE EFFICACY OF TADALAFIL IN IMPROVING LOWER URINARY TRACT SYMPTOMS IN PATIENTS WITH SYMPTOMATIC BENIGN PROSTATIC ENLARGEMENT
 Basrah Journal Of Surgery EVALUATION OF THE EFFICACY OF TADALAFIL IN IMPROVING LOWER URINARY TRACT SYMPTOMS IN PATIENTS WITH SYMPTOMATIC BENIGN PROSTATIC ENLARGEMENT MB, ChB, FIBMS, Assistant Professor
Basrah Journal Of Surgery EVALUATION OF THE EFFICACY OF TADALAFIL IN IMPROVING LOWER URINARY TRACT SYMPTOMS IN PATIENTS WITH SYMPTOMATIC BENIGN PROSTATIC ENLARGEMENT MB, ChB, FIBMS, Assistant Professor
APPENDIX CLINICAL INPUT RESPONSES
 CLINICAL INPUT RESPONSES AUA: American Urological Association; UCSF Med Ctr: University of California San Francisco Medical Center; PUL: prostatic urethral lift. * Indicates that information on conflicts
CLINICAL INPUT RESPONSES AUA: American Urological Association; UCSF Med Ctr: University of California San Francisco Medical Center; PUL: prostatic urethral lift. * Indicates that information on conflicts
PHOTOSELECTIVE POTASSIUM-TITANYL-PHOSPHATE LASER VAPORIZATION OF THE BENIGN OBSTRUCTIVE PROSTATE: OBSERVATIONS ON LONG-TERM OUTCOMES
 0022-5347/05/1744-1344/0 Vol. 174, 1344 1348, October 2005 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2005 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000173913.41401.67 PHOTOSELECTIVE
0022-5347/05/1744-1344/0 Vol. 174, 1344 1348, October 2005 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2005 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000173913.41401.67 PHOTOSELECTIVE
/04/ /0 Reprinted from Vol. 172, , August 2004 THE JOURNAL OF UROLOGY
 0022-5347/04/1722-0658/0 Reprinted from Vol. 172, 658 663, August 2004 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2004 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000132389.97804.d7
0022-5347/04/1722-0658/0 Reprinted from Vol. 172, 658 663, August 2004 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2004 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000132389.97804.d7
The impact of minimally invasive surgeries for the treatment of symptomatic benign prostatic hyperplasia on male sexual function: a systematic review
 500 Review Asian Journal of Andrology (2010) 12: 500 508 2010 AJA, SIMM & SJTU All rights reserved 1008-682X/10 $ 32.00 www.nature.com/aja The impact of minimally invasive surgeries for the treatment of
500 Review Asian Journal of Andrology (2010) 12: 500 508 2010 AJA, SIMM & SJTU All rights reserved 1008-682X/10 $ 32.00 www.nature.com/aja The impact of minimally invasive surgeries for the treatment of
Development of Feedback Microwave Thermotherapy in Symptomatic Benign Prostatic Hyperplasia.
 Development of Feedback Microwave Thermotherapy in Symptomatic Benign Prostatic Hyperplasia. Schelin, Sonny 2006 Link to publication Citation for published version (APA): Schelin, S. (2006). Development
Development of Feedback Microwave Thermotherapy in Symptomatic Benign Prostatic Hyperplasia. Schelin, Sonny 2006 Link to publication Citation for published version (APA): Schelin, S. (2006). Development
Clinical guideline Published: 23 May 2010 nice.org.uk/guidance/cg97
 Lower urinary tract symptoms in men: management Clinical guideline Published: 23 May 2010 nice.org.uk/guidance/cg97 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Lower urinary tract symptoms in men: management Clinical guideline Published: 23 May 2010 nice.org.uk/guidance/cg97 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Authors KC Cheng, LF Lee, KW Wong, HC Chan, CL Cho, H Chau, KM Lam, HS So. Division of Urology, Department of Surgery, United Christian Hospital
 Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
Ejaculation. Emission. Ejection. Orgasm
 Ejaculation Emission Ejection Orgasm Ejaculation sc T10-L2 S2-4 Emission: vas deferens, prostate, bladder neck Post. Urethra distention Ejection: Pelvic Floor / bulbocavernous muscle contraction Orgasm:
Ejaculation Emission Ejection Orgasm Ejaculation sc T10-L2 S2-4 Emission: vas deferens, prostate, bladder neck Post. Urethra distention Ejection: Pelvic Floor / bulbocavernous muscle contraction Orgasm:
Submitted: December 1, Accepted: Dec 24, Published: January 14, 2019.
 Case Study DOI:10.22374/jeleu.v2i1.31 UROLIFT FOR THE TREATMENT OF LOWER URINARY TRACT SYMPTOMS IN A PATIENT WITH AMS 700 PENILE PROSTHESIS: THE FIRST REPORTED CASE Adam Jones, YC Phan, Wasim Mahmalji
Case Study DOI:10.22374/jeleu.v2i1.31 UROLIFT FOR THE TREATMENT OF LOWER URINARY TRACT SYMPTOMS IN A PATIENT WITH AMS 700 PENILE PROSTHESIS: THE FIRST REPORTED CASE Adam Jones, YC Phan, Wasim Mahmalji
김준철 가톨릭대학교의과대학비뇨기과학교실
 비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
Transurethral resection of the prostate (TURP)
 This information tells you about an operation on the prostate called a transurethral resection of the prostate (TURP). It explains how the operation is done, how it can help, what the risks are and what
This information tells you about an operation on the prostate called a transurethral resection of the prostate (TURP). It explains how the operation is done, how it can help, what the risks are and what
An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms
 Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
