Treating your enlarged prostate gland using holmium laser enucleation of the prostate (HoLEP)
|
|
|
- Lilian Carter
- 6 years ago
- Views:
Transcription
1 Treating your enlarged prostate gland using holmium laser enucleation of the prostate (HoLEP) This leaflet will answer any questions you may have about having holmium laser treatment for your enlarged prostate. It explains why this treatment may be suitable for you, its risks and benefits and what you can expect if you decide to have this treatment. If you have any questions, please ask your prostate nurse specialist who will be happy to help. What is the prostate? Your prostate is part of your reproductive system. It is a plum-sized gland and is only found in men. It lies at the base of your bladder and surrounds your urethra (tube that takes urine from the bladder, along the penis and out of your body). Your prostate produces nutrients for your sperm, which makes up part of the milky fluid (semen) when you ejaculate. bladder pelvic floor muscle prostate gland penis anus urethra 1 of 6
2 Why has my prostate enlarged? As men get older, the cells of the prostate begin to swell, which increases the size of the prostate. This is called benign prostatic hyperplasia (BPH), which means extra growth of normal (non-cancerous) cells. This isn t usually serious, but sometimes the prostate grows so large that it puts pressure on your urethra (the tube you pass urine through). This can make it difficult for you to pass urine and may cause other urinary symptoms such as not being able to empty your bladder completely, so you may need to go to the toilet more often (referred to as frequency) having a weak urine flow having to strain to pass urine. Because of the squeeze on your urethra, you may have to use a lot of pressure to pass urine. In the long term, this can damage your bladder and kidneys. Why do I need this treatment? Not everyone who develops an enlarged prostate will need treatment. However, your consultant has recommended holmium laser treatment as the best option to relieve your symptoms. It will make it easier for you to pass urine and may relieve your other symptoms, although it may not resolve all of them. If you do not have treatment, your prostate will continue to grow. This may make your symptoms worse and increases the possibility of problems with your bladder and/or kidneys. What does holmium laser treatment involve? A thin telescope-like instrument is inserted into your urethra. The high-powered laser is then inserted through this instrument and used to carefully remove the excess prostate tissue that is causing obstruction of the urethra. The residual pieces (or lobes) of the prostate are removed by the surgeon. This tissue can be examined to check for cancerous cells. This differs from some other laser procedures which work by completely destroying the prostate tissue that is removed. When the surgeon has finished lasering your excess prostate tissue, a catheter will be inserted. Depending on the time of your surgery, the catheter will be removed on the evening of surgery (before you go to sleep) or early in the morning. The operation can be carried out either under a general anaesthetic, which means you will be asleep for the entire procedure, or under a spinal anaesthetic where you remain awake, but your body is numb from the waist downwards and you do not feel pain. What are the benefits of this treatment? The holmium laser seals the blood vessels of the prostate tissue. This means there is very little blood loss in comparison to the other surgical options outlined below. The catheter that is inserted after the procedure can usually be removed between hours of the surgery. This allows you to leave hospital more quickly than the other surgical options below and reduces your recovery time.
3 Are there any alternatives? There are several alternative treatment options outlined below, although they may not all be appropriate for you. Your consultant or nurse specialist will discuss these with you if they are suitable for your situation: Observation of your symptoms. Some men may want time to think about surgery, or to wait and see if their symptoms become any worse before opting for treatment. Medicines. There are two types of medicine available. They either shrink your prostate, or relax the muscles in your prostate and bladder to improve the flow of urine. However, the effects only last as long as you take the medicine. You may have already tried this option without success. Transurethral resection of the prostate (TURP). This is an operation to remove the parts of your prostate that are pressing on your urethra, to make it easier for you to pass urine. It involves a surgeon inserting a special telescope-like instrument into your urethra, which has a heated wire at one end. This is then used to destroy the prostate tissue or cut it into pieces. Open (traditional) surgery (Millin s prostatectomy). This is considered if your prostate is too large to be removed via a TURP. laser prostatectomy surgery. This is an operation to remove the parts of your prostate that are pressing on your urethra, to make it easier for you to pass urine. It involves a surgeon inserting a special tube into your urethra then using a laser to destroy the prostate tissue or cut it into pieces. Prostatic stent. This is where an expandable tube is inserted into your urethra, to push back the prostatic tissue and widen your urethra. Use of a permanent catheter. This is an option for men who do not want, or who are not suitable for any of the treatments above. Prostate arterial embolisation. This is a minimally invasive procedure that blocks the arteries that supply blood to the prostate, and is performed under local anaesthetic. A radiologist uses an x-ray camera to guide the delivery of small particles to block about 90% of the prostate arteries, they are injected through a catheter (thin tube). What are the risks? Urinary frequency and urgency. It is not uncommon to experience this after the procedure. These symptoms should go within six to 12 weeks. If they persist you may need further treatment which you will receive at your follow-up appointment, but it could also be the result of an infection. Please contact your GP to check that you do not have a urinary infection. Urinary infection. This can cause symptoms such as pain, blood in the urine, or a burning feeling when passing urine, but can be treated with antibiotics. This happens to about five in 100 patients. Retrograde ejaculation. This is where your semen travels to your bladder when you ejaculate, rather than out through your penis. This is not harmful the semen will leave your bladder the next time you pass urine and may make your urine appear cloudy. This occurs in about seven in 10 men having this treatment and is a long-term side effect. You will still be able to have an erection and orgasm, but your fertility may be affected. Do not rely on this as a form of contraception. Erectile dysfunction. The nerves that control your erections are very close to the prostate gland. About 15 in 100 patients may notice a slight deterioration in the quality of their erections, which will usually respond to medication. However, about three in 10 men will notice that their erectile function improves significantly because their quality of life has improved after surgery.
4 Bleeding. There is much less bleeding with holmium laser treatment compared with other surgical procedures for an enlarged prostate. If the bleeding is severe you may need a blood transfusion, but this is extremely rare. Self-catheterisation. Occasionally, if your bladder is weak as a long term result of your enlarged prostate gland, you may need to use a catheter to empty your bladder. If this risk applies to you, your consultant will discuss this with you in more detail. Prostate re-growth. Your prostate continues to enlarge even after surgery and if your symptoms return you may need another operation in the future. About three in 100 men need further surgery within a year of this treatment. Deep vein thrombosis (DVT). Any surgery carries the risk of DVT. This is where a blood clot forms in your veins or arteries, most commonly in the legs. This happens to less than one in 100 people). Injury to the urethra, causing delayed scar formation. This does not delay your recovery, but can lead to urethral stricture, which is where a section of the urethra narrows, reducing the flow of your urine. This happens to about two in 100 men who have this procedure. Preparing for surgery You will be offered a choice of dates for your surgery. You will need to attend the preassessment clinic where we will assess your suitability for surgery under anaesthetic. You will either attend this appointment straight from clinic, or we will send an appointment date by post. Your surgery will not go ahead until you have been passed as fit at the pre-assessment clinic. If you smoke, you may be asked to stop smoking, as it increases the risk of developing a chest infection or DVT. Smoking can also delay wound healing because it reduces the amount of oxygen that reaches the tissues in your body. If you would like to give up smoking, please telephone the NHS Smoking Helpline (details at the end of this leaflet). Please do not eat or drink anything (except non-fizzy water) for six hours before your appointment. This means that you cannot suck on sweets or chew gum. You are allowed to drink water up to two hours before your appointment. If you continue to eat or drink after this, your surgery will be cancelled. Please continue to take all your medicines unless you are told otherwise and remember to bring them into hospital with you. What should I expect when I come to hospital? If you arrive on the ward the day before your surgery, you will be seen by a nurse who will ask you some questions, show you around the ward and prepare you for theatre. If you arrive at the surgical admissions lounge, usually at 7am or 11am, the nurses there will prepare your for your surgery. You will be advised of your arrival time. Consent asking for your consent We want to involve you in all the decisions about your care and treatment. If you decide to go ahead, you will be asked to sign a consent form by your consultant or one of his team to confirm that you agree to have the procedure and understand what it involves If you would like more information about our consent process, please speak to a member of staff caring for you.
5 The anaesthetist will visit you to discuss your anaesthetic. You should have been given a copy of the leaflet Having an anaesthetic please ask the staff for a copy if you have not received this. If you have any further questions or concerns, your specialist nurse will be available to answer them. After your surgery You should not have any pain from the operation, but you may have some discomfort from the catheter. Some men experience bladder spasms (contractions) caused by the catheter rubbing against the trigone (muscle) inside your bladder. The spasms result in urine passing down the sides of the catheter which may leak into your underwear. The spasms may also make you have the urge to pass urine, which can be uncomfortable. If you experience these spasms or have a sudden urge to pass urine, please tell a member of staff, as these symptoms can often be relieved. What problems might I experience after the surgery? You may experience a mild burning feeling or find it a little uncomfortable to pass urine at first. This is because your urethra will be swollen and sore from the surgery and having the catheter in place. This is normal and should not last long (usually between days). Some men find that they cannot pass urine when the catheter has been removed. If this happens, a new catheter will be inserted into your urethra and you may need to keep this in for several weeks to allow your bladder to rest. If this happens to you, you will be taught how to look after the catheter and we will arrange for a district nurse to visit you at home, if necessary. It is common to have less control passing urine for a short time after surgery. If you experience this, please tell your nurse, who will explain how to perform pelvic floor exercises to improve your control. For more information, please ask for the leaflet, Pelvic floor exercises for men. Once you can pass urine comfortably, you will be allowed home. When you are home please make sure you drink regularly (about one-and-a-half to two litres per day), as poor drinking habits may make it more difficult to regain control of your bladder, and may increase your chances of getting a urine infection. You may notice blood in your urine for about a week after your treatment, although this is much less common with this treatment than other surgical options. Leaving hospital Patients can usually go home within 24 hours of the procedure. It may be possible for some patients to go home on the same day as the procedure. If you still have a catheter in your bladder, we will arrange for a district nurse to visit you at home. We will give you specific instructions on when and where the catheter is removed. When will I have a follow-up appointment? You will be seen in clinic eight to 12 weeks after your surgery, by the surgeon who operated on you. You will be asked to pass urine into a special machine (flow rate machine) to assess your urinary flow after your treatment, so you will need to attend the clinic with a full bladder. You will have a scan of your bladder to make sure you are emptying your bladder when you pass urine. You may also have to fill out a symptom questionnaire, to see if your symptoms have improved since the surgery. If staff are satisfied with the results of these tests, you will be discharged from the clinic.
6 You will also be given any histology (examination of tissue and cells) results then, which will show whether the tissue removed was cancerous or not. When can I go back to my normal activities? Heavy lifting. Do not lift anything heavy, such as a bag of shopping or a vacuum cleaner until one week after your surgery. Sex. You should be able to have sexual intercourse soon after surgery, as long as there is no bleeding and you and your partner both feel ready. Driving. If you are discharged from hospital on the same day as your operation, you must ask someone to take you home as you are not allowed to drive within 24 hours of having an anaesthetic. You should only drive again when you are free of pain and able to perform an emergency stop comfortably. You should check with your insurance company to make sure you are covered to start driving again as they may refuse to meet a claim if they feel you have driven too soon. Drinking alcohol. Your clinical nurse specialist can give you advice about when you can start drinking alcohol. Contact us If you have any questions or concerns about holmium laser treatment, please contact one of the prostate nurse specialists t: , Monday to Friday, 8am to 5pm. Out of these hours contact Florence Ward t: or Aston Key Ward t: Alternatively you can call the nurse specialists t: (to leave a message) or t: or , or to bleep a prostate nurse specialist, call t: and ask for the bleep desk. Ask for bleep 1596 and wait for a response. For more information leaflets on conditions, procedures, treatments and services offered at our hospitals, please visit Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: am to 5pm, Monday to Friday Your comments and concerns For advice, support or to raise a concern, contact our Patient Advice and Liaison Service (PALS). To make a complaint, contact the complaints department. t: (PALS) e: pals@gstt.nhs.uk t: (complaints) e: complaints2@gstt.nhs.uk Language and accessible support services If you need an interpreter or information about your care in a different language or format, please get in touch: t: e: languagesupport@gstt.nhs.uk NHS Choices Provides online information and guidance on all aspects of health and healthcare, to help you make choices about your health. w: Leaflet number: 2354/VER5 Date published: December 2017 Review date: December Guy s and St Thomas NHS Foundation Trust A list of sources is available on request
Having a trans-urethral resection of the prostate (TURP)
 Having a trans-urethral resection of the prostate (TURP) This leaflet gives you information about having a TURP, which is an operation to treat an enlarged prostate gland. It explains the benefits, alternatives
Having a trans-urethral resection of the prostate (TURP) This leaflet gives you information about having a TURP, which is an operation to treat an enlarged prostate gland. It explains the benefits, alternatives
Having a ureteric stent inserted
 Having a ureteric stent inserted This leaflet explains more about having a ureteric stent inserted. It describes the benefits, risks, alternatives and what you can expect when you come to hospital. If
Having a ureteric stent inserted This leaflet explains more about having a ureteric stent inserted. It describes the benefits, risks, alternatives and what you can expect when you come to hospital. If
Transurethral Resection of the Prostate (TURP)
 Transurethral Resection of the Prostate (TURP) UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Transurethral Resection of the Prostate (TURP) UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Trans urethral resection of prostate (TURP)
 Trans urethral resection of prostate (TURP) Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST What is the prostate? Only men have a prostate
Trans urethral resection of prostate (TURP) Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST What is the prostate? Only men have a prostate
HOLEP (HOLMIUM LASER ENUCLEATION OF PROSTATE )
 HOLEP (HOLMIUM LASER ENUCLEATION OF PROSTATE ) What does the procedure involve? Removal of obstructing prostate tissue using a telescope and a laser. What are the alternatives to this procedure? Alternatives
HOLEP (HOLMIUM LASER ENUCLEATION OF PROSTATE ) What does the procedure involve? Removal of obstructing prostate tissue using a telescope and a laser. What are the alternatives to this procedure? Alternatives
Transurethral Resection of Prostate
 Transurethral Resection of Prostate Information for Patients This leaflet explains: What does the procedure involve?...2 What are the alternatives to this procedure?...2 What should I expect before the
Transurethral Resection of Prostate Information for Patients This leaflet explains: What does the procedure involve?...2 What are the alternatives to this procedure?...2 What should I expect before the
Surgery to remove your kidney stones
 Surgery to remove your kidney stones a percutaneous nephrolithotomy (PCNL) This leaflet explains more about percutaneous nephrolithotomy, a surgery to remove your kidney stones. It describes the benefits,
Surgery to remove your kidney stones a percutaneous nephrolithotomy (PCNL) This leaflet explains more about percutaneous nephrolithotomy, a surgery to remove your kidney stones. It describes the benefits,
Transurethral Resection of Prostate (TURP)
 Transurethral Resection of Prostate (TURP) This leaflet explains: What does the procedure involve?... 2 What are the alternatives to this procedure?... 2 What should I expect before the procedure?... 2
Transurethral Resection of Prostate (TURP) This leaflet explains: What does the procedure involve?... 2 What are the alternatives to this procedure?... 2 What should I expect before the procedure?... 2
Transurethral Resection of Prostate (TURP)
 Transurethral Resection of Prostate (TURP) Department of Urology Patient Information What What and and where where is the is prostate? the prostate? The prostate is a small gland, about the size of a walnut,
Transurethral Resection of Prostate (TURP) Department of Urology Patient Information What What and and where where is the is prostate? the prostate? The prostate is a small gland, about the size of a walnut,
Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information
 PATIENT INFORMATION Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information What is the evidence base for this information? This leaflet includes advice from
PATIENT INFORMATION Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information What is the evidence base for this information? This leaflet includes advice from
Surgery for an enlarged prostate transurethral resection of the prostate
 Surgery for an enlarged prostate transurethral resection of the prostate Urology Department Patient Information Leaflet Introduction This leaflet is about surgery for an enlarged prostate, known medically
Surgery for an enlarged prostate transurethral resection of the prostate Urology Department Patient Information Leaflet Introduction This leaflet is about surgery for an enlarged prostate, known medically
Prostate surgery. What is the prostate? What is a TURP? Why is a TURP operation necessary? Deciding to have a TURP operation.
 What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
Treatment for bladder tumours - transurethral resection of a bladder tumour
 Treatment for bladder tumours - transurethral resection of a bladder tumour (TURBT) You have had a cystoscopy or other examination that has shown that you have an abnormal area (tumour) in your bladder.
Treatment for bladder tumours - transurethral resection of a bladder tumour (TURBT) You have had a cystoscopy or other examination that has shown that you have an abnormal area (tumour) in your bladder.
Reproduced with the kind permission of Health Press Ltd, Oxford
 Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
Transurethral Prostatectomy (TURP) for Benign Disease
 Transurethral Prostatectomy (TURP) for Benign Disease Whiston Hospital Warrington Road, Prescot, Merseyside, L35 5DR Telephone: 0151 426 1600 St Helens Hospital Marshall Cross Road, St Helens, Merseyside,
Transurethral Prostatectomy (TURP) for Benign Disease Whiston Hospital Warrington Road, Prescot, Merseyside, L35 5DR Telephone: 0151 426 1600 St Helens Hospital Marshall Cross Road, St Helens, Merseyside,
Ankle arthroscopy. If you have any further questions, please speak to a doctor or nurse caring for you
 Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Laser Trans Urethral Resection of Prostate (TURP)
 Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Treatment for Bladder Tumours transurethral resection of bladder tumour (TURBT)
 Treatment for Bladder Tumours transurethral resection of bladder tumour (TURBT) Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high
Treatment for Bladder Tumours transurethral resection of bladder tumour (TURBT) Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high
Trans Urethral Resection of Prostate (TURP)
 Trans Urethral Resection of Prostate (TURP) Patient Information Author ID: SF Leaflet Number: Urol 010 Version: 6 Name of Leaflet: Trans Urethral Resection of Prostate (TURP) Date Produced: March 2018
Trans Urethral Resection of Prostate (TURP) Patient Information Author ID: SF Leaflet Number: Urol 010 Version: 6 Name of Leaflet: Trans Urethral Resection of Prostate (TURP) Date Produced: March 2018
Deflux for the treatment of vesico-ureteric reflux (VUR)
 Deflux for the treatment of vesico-ureteric reflux (VUR) This information sheet explains more about the use of Deflux to treat your VUR (sometimes referred to as STING procedure). If you have any questions
Deflux for the treatment of vesico-ureteric reflux (VUR) This information sheet explains more about the use of Deflux to treat your VUR (sometimes referred to as STING procedure). If you have any questions
Bladder neck incision: procedure-specific information
 PATIENT INFORMATION Bladder neck incision: procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British Association of
PATIENT INFORMATION Bladder neck incision: procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British Association of
Rezūm procedure for the Prostate
 Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
HOLMIUM LASER ENUCLEATION OF THE PROSTATE (HoLEP) INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk HOLMIUM
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk HOLMIUM
Having a diagnostic catheter angiogram
 Having a diagnostic catheter angiogram This information leaflet will explain what an angiogram is and why you have been sent for one. Please read this leaflet carefully. If you have any questions or concerns
Having a diagnostic catheter angiogram This information leaflet will explain what an angiogram is and why you have been sent for one. Please read this leaflet carefully. If you have any questions or concerns
Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients
 Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i The prostate The prostate is a small gland which is found only in men. It is situated at the base of the bladder
Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i The prostate The prostate is a small gland which is found only in men. It is situated at the base of the bladder
Bladder retraining - treatment for urgency and urge incontinence
 Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Robotic-assisted laparoscopic partial nephrectomy
 Robotic-assisted laparoscopic partial nephrectomy This leaflet is designed to give you information on why this procedure may be suitable for you, and what you can expect from it. It outlines the advantages
Robotic-assisted laparoscopic partial nephrectomy This leaflet is designed to give you information on why this procedure may be suitable for you, and what you can expect from it. It outlines the advantages
Sphenopalatine ganglion (SPG) stimulation for the treatment of cluster headaches
 Headache Centre Sphenopalatine ganglion (SPG) stimulation for the treatment of cluster headaches This leaflet is for patients, family and carers. It explains about the benefits, risks and any alternatives
Headache Centre Sphenopalatine ganglion (SPG) stimulation for the treatment of cluster headaches This leaflet is for patients, family and carers. It explains about the benefits, risks and any alternatives
Laser Prostatectomy Urology Patient information Leaflet
 Laser Prostatectomy Urology Patient information Leaflet Page 1 Laser Prostatectomy Your surgeon has recommended that you have laser surgery to your prostate. We hope that this leaflet answers any questions
Laser Prostatectomy Urology Patient information Leaflet Page 1 Laser Prostatectomy Your surgeon has recommended that you have laser surgery to your prostate. We hope that this leaflet answers any questions
If you have any further questions, please speak to a doctor or nurse caring for you.
 Having a laparoscopy This leaflet aims to answer your questions about having a laparoscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital. If
Having a laparoscopy This leaflet aims to answer your questions about having a laparoscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital. If
Having an open retroperitoneal lymph node dissection (RPLND)
 Having an open retroperitoneal lymph node dissection (RPLND) This leaflet explains more about retroperitoneal lymph node dissection (RPLND), including the benefits, risks and any alternatives and what
Having an open retroperitoneal lymph node dissection (RPLND) This leaflet explains more about retroperitoneal lymph node dissection (RPLND), including the benefits, risks and any alternatives and what
Prostate Artery Embolisation (PAE)
 Service: Imaging Prostate Artery Embolisation (PAE) Exceptional healthcare, personally delivered Ask 3 Questions The team delivering your healthcare want to encourage you to become as involved as possible
Service: Imaging Prostate Artery Embolisation (PAE) Exceptional healthcare, personally delivered Ask 3 Questions The team delivering your healthcare want to encourage you to become as involved as possible
Surgery for carpal tunnel syndrome
 Surgery for carpal tunnel syndrome This leaflet will help answer some of the questions you may have about having surgery to treat carpal tunnel syndrome. It should accompany the leaflet, Surgical Admissions
Surgery for carpal tunnel syndrome This leaflet will help answer some of the questions you may have about having surgery to treat carpal tunnel syndrome. It should accompany the leaflet, Surgical Admissions
Robot-assisted kidney transplantation pilot study
 Robot-assisted kidney transplantation pilot study This leaflet explains more about a new technique called robot-assisted kidney transplantation. This is a pilot study - this means that we are offering
Robot-assisted kidney transplantation pilot study This leaflet explains more about a new technique called robot-assisted kidney transplantation. This is a pilot study - this means that we are offering
Treating narrowing of the urethra
 Treating narrowing of the urethra Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been recommended to have a procedure to treat narrowing of the urethra.
Treating narrowing of the urethra Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been recommended to have a procedure to treat narrowing of the urethra.
Percutaneous nephrolithotomy (PCNL)
 Percutaneous nephrolithotomy (PCNL) Department of Urology Patient Information What What is a is percutaneous a percutaneous nephrolithotomy nephrolithotomy (PCNL)? (PCNL)? A percutaneous nephrolithotomy
Percutaneous nephrolithotomy (PCNL) Department of Urology Patient Information What What is a is percutaneous a percutaneous nephrolithotomy nephrolithotomy (PCNL)? (PCNL)? A percutaneous nephrolithotomy
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients
 Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
Foot and ankle injections
 Foot and ankle injections Contents 3 What is a foot or ankle injection? 4 What are the benefits? 4 What are the risks? 6 Are there any alternatives? 6 How can I prepare for a foot or ankle injection? 7
Foot and ankle injections Contents 3 What is a foot or ankle injection? 4 What are the benefits? 4 What are the risks? 6 Are there any alternatives? 6 How can I prepare for a foot or ankle injection? 7
Having a pancreas transplant alone (PTA)
 Having a pancreas transplant alone (PTA) This leaflet explains more about having a pancreas transplant alone (PTA), including the benefits, risks, alternatives, and what you can expect at the time of the
Having a pancreas transplant alone (PTA) This leaflet explains more about having a pancreas transplant alone (PTA), including the benefits, risks, alternatives, and what you can expect at the time of the
Having inhalation sedation for your dental treatment
 Having inhalation sedation for your dental treatment This aim of this information sheet is to help answer some of the questions you may have about having inhalation sedation for your dental treatment.
Having inhalation sedation for your dental treatment This aim of this information sheet is to help answer some of the questions you may have about having inhalation sedation for your dental treatment.
Forefoot deformity correction
 Forefoot deformity correction This leaflet aims to answer your questions about having forefoot deformity correction surgery. It explains the benefits, risks and alternatives, as well as what you can expect
Forefoot deformity correction This leaflet aims to answer your questions about having forefoot deformity correction surgery. It explains the benefits, risks and alternatives, as well as what you can expect
TRANSURETHRAL RESECTION OF THE PROSTATE
 TRANSURETHRAL RESECTION OF THE PROSTATE A discussion of the operation and the pre and post operative care You and your doctor have considered the possibility that you have a transurethral resection of
TRANSURETHRAL RESECTION OF THE PROSTATE A discussion of the operation and the pre and post operative care You and your doctor have considered the possibility that you have a transurethral resection of
CYSTOSCOPY & TRANSURETHRAL RESECTION OF THE PROSTATE
 Associates: Dr Kim Pese Dr Kym Horsell Dr Michael Chong Dr Jason Lee The Tennyson Centre Suite 19, First Floor 520 South Road Kurralta Park SA 5037 Appointments: 08 8292 2399 Fax: 08 8292 2388 admin@urologicalsolutions.com.au
Associates: Dr Kim Pese Dr Kym Horsell Dr Michael Chong Dr Jason Lee The Tennyson Centre Suite 19, First Floor 520 South Road Kurralta Park SA 5037 Appointments: 08 8292 2399 Fax: 08 8292 2388 admin@urologicalsolutions.com.au
Treating your prolapse
 Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
Rapid access prostate imaging and diagnosis pathway Information for patients, relatives and carers
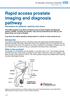 Rapid access prostate imaging and diagnosis pathway Information for patients, relatives and carers This leaflet explains more about the Rapid access prostate imaging and diagnosis pathway (RAPID), including
Rapid access prostate imaging and diagnosis pathway Information for patients, relatives and carers This leaflet explains more about the Rapid access prostate imaging and diagnosis pathway (RAPID), including
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Robotic-assisted lingual tonsillectomy for sleep apnoea
 Robotic-assisted lingual tonsillectomy for sleep apnoea You have been given this leaflet because you have been referred for a robotic-assisted lingual tonsillectomy for sleep apnoea. This leaflet offers
Robotic-assisted lingual tonsillectomy for sleep apnoea You have been given this leaflet because you have been referred for a robotic-assisted lingual tonsillectomy for sleep apnoea. This leaflet offers
Bladder neck incision
 Bladder neck incision What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content may apply to you. Feel free
Bladder neck incision What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content may apply to you. Feel free
Patient Information Leaflet
 Patient Information Leaflet MID-URETHRAL SLING OPERATION TENSION-FREE VAGINAL TAPE (TVT) TRANSOBTURATOR TAPE (TOT, TVT-O) This information leaflet has been developed to help your understanding of what
Patient Information Leaflet MID-URETHRAL SLING OPERATION TENSION-FREE VAGINAL TAPE (TVT) TRANSOBTURATOR TAPE (TOT, TVT-O) This information leaflet has been developed to help your understanding of what
Having a transperineal prostate biopsy
 Having a transperineal prostate biopsy This leaflet should help to answer some of your questions about having a transperineal prostate biopsy. If you have any further questions, please speak to a doctor
Having a transperineal prostate biopsy This leaflet should help to answer some of your questions about having a transperineal prostate biopsy. If you have any further questions, please speak to a doctor
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients
 Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Big toe fusion. If you have any further questions, please speak to a doctor or nurse caring for you.
 Big toe fusion This leaflet aims to answer your questions about having big toe fusion surgery. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Big toe fusion This leaflet aims to answer your questions about having big toe fusion surgery. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Having a vitrectomy surgery to repair your retinal detachment
 Having a vitrectomy surgery to repair your retinal detachment If you need information on audiotape about having a vitrectomy or your hospital visit, please call 020 7188 8815. You have been given this
Having a vitrectomy surgery to repair your retinal detachment If you need information on audiotape about having a vitrectomy or your hospital visit, please call 020 7188 8815. You have been given this
Laparoscopic Sacrohysteropexy
 Professor Christian Phillips BSc Hons BM DM FRCOG Consultant Gynaecologist and Urogynaecologist Laparoscopic Sacrohysteropexy What is a prolapse? Uterine prolapse is a bulge or lump in the vagina caused
Professor Christian Phillips BSc Hons BM DM FRCOG Consultant Gynaecologist and Urogynaecologist Laparoscopic Sacrohysteropexy What is a prolapse? Uterine prolapse is a bulge or lump in the vagina caused
In-patient brachytherapy for gynaecological cancer. Cancer Services Information for patients
 In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
Ankle, sub-talar or mid-foot joint fusion
 Ankle, sub-talar or mid-foot joint fusion This leaflet aims to answer your questions about having an ankle, sub-talar or mid-foot joint fusion. It explains the benefits, risks and alternatives, as well
Ankle, sub-talar or mid-foot joint fusion This leaflet aims to answer your questions about having an ankle, sub-talar or mid-foot joint fusion. It explains the benefits, risks and alternatives, as well
Cystoscopy and hydrostatic bladder distension
 Cystoscopy and hydrostatic bladder distension Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been recommended to have a procedure called cystoscopy and
Cystoscopy and hydrostatic bladder distension Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been recommended to have a procedure called cystoscopy and
Having prostate surgery
 Having prostate surgery Urology department 01935 384 394 yeovilhospital.nhs.uk The most common operation on the prostate is known as a Transurethral Resection of the Prostate (TURP). Sometimes, it is necessary
Having prostate surgery Urology department 01935 384 394 yeovilhospital.nhs.uk The most common operation on the prostate is known as a Transurethral Resection of the Prostate (TURP). Sometimes, it is necessary
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer.
 What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft
 Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Cystoscopy and insertion of a ureteric stent
 Cystoscopy and insertion of a ureteric stent Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been recommended to have a procedure called cystoscopy and insertion
Cystoscopy and insertion of a ureteric stent Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been recommended to have a procedure called cystoscopy and insertion
A patient information sheet from. What are the alternatives? Before the procedure. page 1 of 5
 A patient information sheet from Transurethral Resection of the Prostate (for Benign Disease) This operation involves the telescopic removal or incision of the obstructing, central part of the prostate
A patient information sheet from Transurethral Resection of the Prostate (for Benign Disease) This operation involves the telescopic removal or incision of the obstructing, central part of the prostate
Third molar (wisdom) teeth
 Third molar (wisdom) teeth This information leaflet is for patients who may need to have their third molar (wisdom) teeth removed. It explains why they may need to be removed, what is involved and any
Third molar (wisdom) teeth This information leaflet is for patients who may need to have their third molar (wisdom) teeth removed. It explains why they may need to be removed, what is involved and any
Removing your prostate to treat your prostate cancer Robotic-assisted laparoscopic prostatectomy
 Removing your prostate to treat your prostate cancer Robotic-assisted laparoscopic prostatectomy This leaflet gives you information about having robotic-assisted surgery to treat your prostate cancer,
Removing your prostate to treat your prostate cancer Robotic-assisted laparoscopic prostatectomy This leaflet gives you information about having robotic-assisted surgery to treat your prostate cancer,
UW MEDICINE PATIENT EDUCATION. About Your Surgery DRAFT
 UW MEDICINE PATIENT EDUCATION About Your Surgery Transurethral resection of the prostate (TURP) This handout describes a transurethral resection of the prostate. It also gives instructions to follow before
UW MEDICINE PATIENT EDUCATION About Your Surgery Transurethral resection of the prostate (TURP) This handout describes a transurethral resection of the prostate. It also gives instructions to follow before
Trans Urethral Resection of Bladder Tumour
 Trans Urethral Resection of Bladder Tumour Department of Urology 2 Patient Information Contents Where is the bladder and what does it do? 3 What is non invasive cancer of the bladder? 4 How is bladder
Trans Urethral Resection of Bladder Tumour Department of Urology 2 Patient Information Contents Where is the bladder and what does it do? 3 What is non invasive cancer of the bladder? 4 How is bladder
Varicoceles can cause various problems, including subfertility.
 This leaflet has been provided to help answer some of the questions you or those who care for you may have about percutaneous abscess drainage. It is not meant to replace the consultation between you and
This leaflet has been provided to help answer some of the questions you or those who care for you may have about percutaneous abscess drainage. It is not meant to replace the consultation between you and
Urology Department Percutaneous Nephrolithotomy (PCNL)
 Urology Department Percutaneous Nephrolithotomy (PCNL) Your consultant has diagnosed that you have a problem with kidney stones and has recommended that you have an operation called a percutaneous nephrolithotomy
Urology Department Percutaneous Nephrolithotomy (PCNL) Your consultant has diagnosed that you have a problem with kidney stones and has recommended that you have an operation called a percutaneous nephrolithotomy
CYSTOSCOPY PATIENT INFORMATION
 CYSTOSCOPY PATIENT INFORMATION ADHB Urology Department; Reviewed FEB 2005 Ubix code UPEB3 1 The information contained in this booklet is intended to assist you in understanding your proposed surgery; some
CYSTOSCOPY PATIENT INFORMATION ADHB Urology Department; Reviewed FEB 2005 Ubix code UPEB3 1 The information contained in this booklet is intended to assist you in understanding your proposed surgery; some
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients
 Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
Tension Free vaginal tape. Mrs Ami Shukla, Consultant Urogynaecologist Northampton General Hospital Northampton NN1 5BD
 Tension Free vaginal tape Mrs Ami Shukla, Consultant Urogynaecologist Northampton General Hospital Northampton NN1 5BD What is a TVT procedure? A TVT (Tension Free Vaginal Tape) procedure is an operation
Tension Free vaginal tape Mrs Ami Shukla, Consultant Urogynaecologist Northampton General Hospital Northampton NN1 5BD What is a TVT procedure? A TVT (Tension Free Vaginal Tape) procedure is an operation
Nephrostomy. Radiology Department. Patient information leaflet
 Nephrostomy Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a nephrostomy. It explains what is involved and the possible risks. The benefits and risks
Nephrostomy Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a nephrostomy. It explains what is involved and the possible risks. The benefits and risks
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE)
 PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
What is an aneurysm? Arteries carry blood away from your heart to the rest of your body. An aneurysm occurs when the walls of an artery weaken.
 Endovascular aneurysm repair (EVAR) This leaflet aims to answer some of the questions you may have about having an endovascular aneurysm repair. It explains the benefits, risks and alternatives of the
Endovascular aneurysm repair (EVAR) This leaflet aims to answer some of the questions you may have about having an endovascular aneurysm repair. It explains the benefits, risks and alternatives of the
Tension-free Vaginal Tape (TVT)
 Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Percutaneous nephrolithotomy (PCNL)
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What does this procedure involve? The breakdown and removal of kidney stones using
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What does this procedure involve? The breakdown and removal of kidney stones using
Benign Prostatic Hyperplasia (BPH)
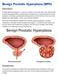 Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Laparoscopic partial removal of the kidney
 Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
Caring for a Nephrostomy and what is Ureteric Stenting
 Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Gynaecology Department Patient Information Leaflet
 Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Laparoscopic Cholecystectomy
 Treatment Centre Laparoscopic Cholecystectomy What is a laparoscopic cholecystectomy? You need this operation because stones have collected in your gallbladder (the area where a small amount of bile is
Treatment Centre Laparoscopic Cholecystectomy What is a laparoscopic cholecystectomy? You need this operation because stones have collected in your gallbladder (the area where a small amount of bile is
Uroformation. Prostate Surgery. Robotic Assisted Laparoscopic Prostatectomy (RALP)
 Uroformation Prostate Surgery Robotic Assisted Laparoscopic Prostatectomy (RALP) The Uroformation series is a co-operative venture in patient centered urological information. June 2014 What is the Prostate?
Uroformation Prostate Surgery Robotic Assisted Laparoscopic Prostatectomy (RALP) The Uroformation series is a co-operative venture in patient centered urological information. June 2014 What is the Prostate?
CYSTOSCOPY AND URETHRAL BULKING INJECTIONS INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk CYSTOSCOPY
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk CYSTOSCOPY
Femoral endarterectomy
 Femoral endarterectomy The femoral arteries run from the groin to the thigh delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Femoral endarterectomy The femoral arteries run from the groin to the thigh delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Penile Straightening Nesbit tuck, Lue vein patch or synthetic graft operation): procedure-specific information
 PATIENT INFORMATION Penile Straightening Nesbit tuck, Lue vein patch or synthetic graft operation): procedure-specific information This information is intended to supplement any advice you may already
PATIENT INFORMATION Penile Straightening Nesbit tuck, Lue vein patch or synthetic graft operation): procedure-specific information This information is intended to supplement any advice you may already
Treatment for bladder tumours (transurethral resection of bladder tumour (TURBT))
 Treatment for bladder tumours (transurethral resection of bladder tumour (TURBT)) Information for patients from the Urology Department You have had a cystoscopy or other examination that has shown that
Treatment for bladder tumours (transurethral resection of bladder tumour (TURBT)) Information for patients from the Urology Department You have had a cystoscopy or other examination that has shown that
Transurethral resection of a bladder tumour (TURBT)
 Transurethral resection of a bladder tumour (TURBT) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Transurethral resection of a bladder tumour (TURBT) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
What you need to know about having a vasectomy
 University Teaching Trust What you need to know about having a vasectomy Urology Hope Building 0161 206 5380 All Rights Reserved 2017. Document for issue as handout. What is a vasectomy? A vasectomy is
University Teaching Trust What you need to know about having a vasectomy Urology Hope Building 0161 206 5380 All Rights Reserved 2017. Document for issue as handout. What is a vasectomy? A vasectomy is
EVOLVE LASER PROSTATECTOMY
 Associates: Dr Kim Pese Dr Kym Horsell Dr Michael Chong Dr Jason Lee The Tennyson Centre Suite 19, First Floor 520 South Road Kurralta Park SA 5037 Appointments: 08 8292 2399 Fax: 08 8292 2388 admin@urologicalsolutions.com.au
Associates: Dr Kim Pese Dr Kym Horsell Dr Michael Chong Dr Jason Lee The Tennyson Centre Suite 19, First Floor 520 South Road Kurralta Park SA 5037 Appointments: 08 8292 2399 Fax: 08 8292 2388 admin@urologicalsolutions.com.au
Antegrade Ureteric Stent
 Antegrade Ureteric Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains what is involved and the possible
Antegrade Ureteric Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains what is involved and the possible
Simple removal of the kidney (simple nephrectomy): procedure-specific information
 PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
SUPRA PUBIC CATHETER(SPC)
 Suprapubic versus urethral catheter? When a long-term catheter to drain the bladder is advised, it can be placed in the urethra (water pipe) or suprapubically (directly into the bladder through the skin
Suprapubic versus urethral catheter? When a long-term catheter to drain the bladder is advised, it can be placed in the urethra (water pipe) or suprapubically (directly into the bladder through the skin
Cystoscopy and Hydrostatic Bladder Distension Urology Patient information Leaflet
 Cystoscopy and Hydrostatic Bladder Distension Urology Patient information Leaflet Page 1 Why do I need this procedure? Bladder distension (stretching the bladder) has shown some success in reducing urinary
Cystoscopy and Hydrostatic Bladder Distension Urology Patient information Leaflet Page 1 Why do I need this procedure? Bladder distension (stretching the bladder) has shown some success in reducing urinary
WEB device for treating brain (intracranial) aneurysms
 WEB device for treating brain (intracranial) aneurysms This leaflet explains more about the WEB device, including the benefits, risks and any alternatives and what you can expect when you come to hospital.
WEB device for treating brain (intracranial) aneurysms This leaflet explains more about the WEB device, including the benefits, risks and any alternatives and what you can expect when you come to hospital.
Restorative dentistry new patient clinic
 Restorative dentistry new patient clinic You have been referred to the Restorative Dentistry Service for an assessment regarding a specific dental problem, and this leaflet provides information about your
Restorative dentistry new patient clinic You have been referred to the Restorative Dentistry Service for an assessment regarding a specific dental problem, and this leaflet provides information about your
Radical removal of the kidney (radical nephrectomy): procedure-specific information
 PATIENT INFORMATION Radical removal of the kidney (radical nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATIENT INFORMATION Radical removal of the kidney (radical nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
Laparoscopic radical nephrectomy
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is a laparoscopic radical nephrectomy? This is a procedure which involves removal
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is a laparoscopic radical nephrectomy? This is a procedure which involves removal
LAPAROSCOPIC RADICAL REMOVAL OF THE KIDNEY INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk LAPAROSCOPIC
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk LAPAROSCOPIC
Arthroscopic rotator cuff repair
 Arthroscopic rotator cuff repair This leaflet aims to answer some of the questions you may have about having an arthroscopic rotator cuff repair. It explains the benefits, risks and alternatives to the
Arthroscopic rotator cuff repair This leaflet aims to answer some of the questions you may have about having an arthroscopic rotator cuff repair. It explains the benefits, risks and alternatives to the
