Increasing Hospital Admission Rates for Urological Complications After Transrectal Ultrasound Guided Prostate Biopsy
|
|
|
- Agnes Butler
- 6 years ago
- Views:
Transcription
1 Increasing Hospital Admission Rates for Urological Complications After Transrectal Ultrasound Guided Prostate Biopsy Robert K. Nam,*, Refik Saskin, Yuna Lee, Ying Liu, Calvin Law, Laurence H. Klotz, D. Andrew Loblaw, John Trachtenberg, Aleksandra Stanimirovic, Andrew E. Simor, Arun Seth, David R. Urbach and Steven A. Narod From the Division of Urology (RKN, LHK, AS), Division of General Surgery (CL), Department of Microbiology and Division of Infectious Diseases (AES), Department of Radiation Oncology (DAL) and Division of Molecular and Cellular Biology (AS), Sunnybrook Research Institute; and Division of General Internal Medicine, St. Michael s Hospital (YL); Institute of Clinical Evaluative Sciences (RS, YL); Division of Urology (JT), Division of General Surgery (DRU), University Health Network; Department of Public Health Sciences (SAN); and Department of Health Policy Management and Evaluation (RKN, CL, DRU), University of Toronto, Toronto, Ontario, Canada Abbreviations and Acronyms CIHI Canadian Institute of Health Information OHIP Ontario Health Insurance Plan SES socioeconomic status TRUS transrectal ultrasound Submitted for publication July 15, Study received research ethics board approval. Supported by National Cancer Institute Grant and the Canadian Institute of Health Research. Supplementary material for this article can be obtained at * Correspondence: Division of Urology, Sunnybrook Health Sciences Centre, 2075 Bayview Ave., Room MG-406, Toronto, Ontario, Canada M4N 3M5 (telephone: ; FAX: ; Robert.nam@utoronto.ca). Nothing to disclose. Financial interest and/or other relationship with Abbott, AstraZeneca, Aventis, Merck and GSK. See Editorial on page 852. Purpose: Transrectal ultrasound guided prostate biopsy is widely used to confirm the diagnosis of prostate cancer. The technique has been associated with significant morbidity in a small proportion of patients. Materials and Methods: We conducted a population based study of 75,190 men who underwent a transrectal ultrasound guided biopsy in Ontario, Canada, between 1996 and We used hospital and cancer registry administrative databases to estimate the rates of hospital admission and mortality due to urological complications associated with the procedure. Results: Of the 75,190 men who underwent transrectal ultrasound biopsy 33,508 (44.6%) were diagnosed with prostate cancer and 41,682 (55.4%) did not have prostate cancer. The hospital admission rate for urological complications within 30 days of the procedure for men without cancer was 1.9% (781/41,482). The 30-day hospital admission rate increased from 1.0% in 1996 to 4.1% in 2005 (p for trend ). The majority of hospital admissions (72%) were for infection related reasons. The probability of being admitted to hospital within 30 days of having the procedure increased 4-fold between 1996 and 2005 (OR 3.7, 95% CI , p ). The overall 30-day mortality rate was 0.09% but did not change during the study period. Conclusions: The hospital admission rates for complications following transrectal ultrasound guided prostate biopsy have increased dramatically during the last 10 years primarily due to an increasing rate of infection related complications. Key Words: mass screening, prostatic neoplasms, biopsy, adverse effects Editor s Note: This article is the fourth of 5 published in this issue for which category 1 CME credits can be earned. Instructions for obtaining credits are given with the questions on pages 1262 and TRANSRECTAL ultrasound guided prostate biopsy is the most common method to determine the presence of prostate cancer. 1 Urological side effects of the procedure include urinary tract infection, hematuria and acute urinary retention. 2 To minimize these effects patients may be offered mechanical bowel preparation and receive prophylactic antibiotics, but standards of care have not been established. Randomized clinical trials comparing prophylactic antibiotics to placebo have shown reduced rates of infection following biopsy. 3,4 Rates of serious complica- S /13/ /0 THE JOURNAL OF UROLOGY Vol. 189, S12-S18, January by AMERICAN UROLOGICAL ASSOCIATION EDUCATION AND RESEARCH, INC. Printed in U.S.A. Please cite this article as J Urol 2013;189: S12-S18. DOI:
2 HOSPITAL ADMISSION FOR UROLOGICAL COMPLICATIONS AFTER PROSTATE BIOPSY S13 tions requiring hospital admission for inpatient treatment have ranged from less than 0.1% to 2.4%. 5 However, previous studies were small 5 7 or were derived from a controlled clinical trial designed to examine a different end point. 8 To our knowledge no study has estimated the morbidity and mortality from a large population based sample. In the last decade we have witnessed increasing rates of bacterial resistance to antibiotics, an increase in the use of antiplatelet agents and a high prevalence of benign prostatic hyperplasia. These trends raise the concern that the rates of serious complications following TRUS guided prostate biopsy might also be increasing. We examined a large, population based data set to establish the incidence of morbidity and mortality associated with TRUS guided prostate biopsy. METHODS Study Subjects and Data Sources We conducted a population based retrospective study of all men who underwent TRUS guided prostate biopsy between January 1, 1996 and December 31, 2005 in Ontario, Canada. All medical procedures are reimbursed by a single, government operated health insurance system (OHIP). Because the sole indication for performing a TRUS guided biopsy is for the detection of prostate cancer, we included all men older than 18 years who underwent this procedure for the first time. To ensure that none of the patients had undergone previous biopsy we excluded anyone who had a biopsy within 5 years before However, in secondary analyses we examined the subset of patients who had repeat prostate biopsy among those with an initial negative biopsy within 2 years of the initial biopsy. OHIP fee codes J138 (transrectal ultrasound) and Z712 (prostate needle biopsy) performed on the same procedure date were used to identify patients. We linked records from the OHIP physician claims database to several other Ontario health databases including the CIHI hospital separation database, the Registered Persons database (a vital statistics registry) and the Ontario Cancer Registry. The CIHI compiles data from 22 databases and registries including all hospital admission data. We used only the Most Responsible Diagnosis designation, which is defined as the most significant contributor to the length of hospital stay or the diagnosis that contributed to the longest length of stay. We electronically searched data from the hospital discharge administrative databases of CIHI using the ICD-9 and ICD-10. From 1996 to 2001 CIHI databases used ICD-9 codes and from 2002 to 2005 they used ICD-10 codes. The study protocol was approved by the research ethics board. Main Outcome Measures The main outcome was hospital admission for 1 of 3 urological conditions within 30 days of TRUS guided prostate biopsy. These included infections, bleeding and obstruction of the urinary tract. Previous studies have shown that these are the most serious urological complications and occur within 30 days from the date of biopsy. 5 8 The 30-day hospital admission rate was based on 3 hospital CIHI discharge diagnoses of 1) urinary infection related, 2) urinary bleeding related and 3) urinary obstruction related. Secondary outcome was 30-day mortality from the date of biopsy. Death information was obtained from the Registered Persons database which tracks all vital status information in the province. The ICD coding scheme changed during the period data were collected from ICD-9 to ICD-10. To validate whether the transition between ICD-9 and ICD-10 codes (2001 to 2002) identified the same group of patients from each coding version we compared for any differences in the frequency of our list of ICD-9 and ICD-10 codes for all patients within Ontario admitted for the same list of chosen codes during the study period, regardless of having prostate biopsy. Exposure Variables We collected information on prostate cancer diagnosis through linkage of the database with the Ontario Cancer Registry. Median annual income was estimated from the neighborhood of residence using 1996 and 2001 census data, and was categorized into community specific quintiles. For each patient we retrieved the number of prostate biopsies performed by the treating physician in the previous year. We also collected information on comorbidity using the Deyo/Charlson comorbidity index. 9 Data Analysis We calculated 30-day hospital admission and mortality rates following the date of biopsy between 1996 and Discharge diagnoses were assigned to 3 categories of 1) infection related, 2) bleeding related and 3) urinary obstruction related. To ensure that hospital admission rates were not due to prostate cancer related treatment, we calculated rates separately for men with and without prostate cancer (based on biopsy result). Age was categorized into 5 groups of 1) younger than 50 years, 2) 50 to 59 years, 3) 60 to 69 years, 4) 70 to 79 years and 5) older than 79 years. Income status was also categorized into quintiles. We conducted multivariate unconditional logistic regression to estimate the odds ratio for 30-day hospital admission based on year of biopsy, age, SES and individual physician volume. Also, to account for other factors of individual physicians who performed the biopsies we adjusted for physician clustering using generalized estimating equations. Because individual physician volume could vary yearly, for every biopsy we assigned the number of biopsies performed by the physician in the last year from the date of biopsy. Statistical analyses were performed using SAS software V9.1. Tests were 2-tailed and significant for p RESULTS TRUS Guided Prostate Biopsy Related Morbidity Between 1996 and 2005, 75,190 men underwent TRUS guided prostate biopsy in the Province of Ontario. Each biopsy was performed by 1 of 437 different physicians. Among the 75,190 men 33,508 (44.6%)
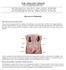
3 S14 HOSPITAL ADMISSION FOR UROLOGICAL COMPLICATIONS AFTER PROSTATE BIOPSY were diagnosed with prostate cancer and 41,682 (55.4%) were not diagnosed with prostate cancer. The hospital admission rate within 30 days from TRUS guided prostate biopsy was 1.4% (1,057/75,190) for all patients. When compared by cancer status the 30-day hospital admission rate was 1.9% for patients without cancer (781/41,482) and 0.8% for patients with cancer (276/33,508, p ). Given this difference in rates by cancer status we examined rates of hospital admission stratified by cancer status. Among the patients without cancer the rate of hospital admission after TRUS guided prostate biopsy increased from 1.0% in 1996 to 4.1% in 2005 (p , chi-square 184.4, 9 df) (see figure and table 1). For patients diagnosed with cancer the rate of hospital admission also increased during the study period. The 30-day hospital admission rate was 0.4% in 1996 and increased to 0.9% in 2005 (p 0.002). The rate was lower for patients with cancer because when those with prostate cancer were admitted to the hospital for biopsy related complications, the coders for the Most Responsible Diagnosis could have assigned it as prostate cancer rather than the complication related diagnoses. In addition, patients were likely to receive treatment for prostate cancer within 30 days of the biopsy, which also affected the accuracy of 30-day hospital admission rates. To dissociate the diagnosis of prostate cancer per se from the biopsy related morbid conditions, these analyses were restricted to the 41,682 men with no diagnosis of prostate cancer. To determine which factors might be associated with the trend in hospital admission, we examined the crude rates of 30-day hospital admission by age and SES, and no differences were found (table 2). To address for potential factors associated with the 437 physicians performing all biopsies we also adjusted for physician clustering and procedural volume within the logistic model. The single most important factor predictive of hospital admission was year of biopsy. The adjusted odds ratio for hospital admission for patients undergoing biopsy in 2005 compared to those biopsied in 1996 was 3.74 (95% CI , p ). For individual physician volume there was a negative correlation with 30-day hospital admission rates. For the patients admitted to hospital mean time to admission from the date of TRUS guided prostate biopsy was 5.0 days (SD 7.9, median 1, range 0 to 30). Mean length of hospital stay was 1.1 days (SD 3.8, median 1, range 1 to 68). No significant differences were found for time to hospital admission or length of hospital stay when comparing by year of biopsy. Causes for 30-Day Hospital Admission The majority of hospital admissions were for infection related diagnoses (71.6%, 556), followed by bleeding related diagnoses (19.4%, 151) and urinary Plots of 30-day hospital admission rate and 30-day mortality rate by year of biopsy and repeat prostate biopsy
4 HOSPITAL ADMISSION FOR UROLOGICAL COMPLICATIONS AFTER PROSTATE BIOPSY S15 Table 1. Baseline patient characteristics No. Study Subjects (%) Yr of biopsy: ,544 (8.7) ,951 (10.6) ,517 (10.0) ,200 (9.6) ,278 (11.0) ,651 (12.8) ,267 (11.0) ,725 (8.9) ,317 (8.4) ,740 (9.0) Age category: Younger than 50 2,307 (3.1) ,948 (21.2) ,286 (41.6) ,084 (29.4) 80 or Older 3,565 (4.7) SES:* 1 10,727 (14.5) 2 13,640 (18.5) 3 14,542 (19.7) 4 15,646 (21.2) 5 19,228 (26.1) * Based on 73,783 subjects because SES could not be ascertained in 1,407. SES based on median annual income estimated from neighborhood of residence using 1996 and 2001 census data, and categorized into community specific quintiles within census regions, from 1 lowest income level to 5 highest income category. Specific income cutoffs cannot be provided because they vary within each community specific region. obstruction related diagnoses (9.0%, 79). The rate of hospital admissions related to infection increased from 0.6% (23) in 1996 to 3.6% (143) in 2005 (see figure, table 3). Rates of obstruction increased to a smaller degree and the rates of bleeding related diagnoses did not change during the study period. The majority of the patients admitted to the hospital without a diagnosis of cancer were considered otherwise healthy. Of the 781 patients 729 (93.3%) had a Charlson index of zero and 21 (2.8%) had a Charlson index of one. TRUS Guided Morbidity for Repeat Prostate Biopsy Of the 41,682 patients who did not have cancer 7,869 (18.9%) underwent repeat prostate biopsy within 2 years from the first prostate biopsy. For these men the 30-day hospital admission rate was 1.3% (99). The 30-day hospital admission rate also increased from 0.9% in 1996 to 3.7% in 2005 (p , chi-square 61.6 with 9 df, see figure). Internal Validity Assessment for ICD-9 and ICD-10 Coding To ensure that there were no variations due to differences in ICD-9 and ICD-10 coding we examined all hospital admissions based on our selected ICD-9 and ICD-10 codes for all patients within the province. In the transition of 2001 to 2002 there was no significant change in the number of hospital admissions. In 2001 there were 73,655 patients admitted for selected ICD-9 codes in Ontario. In 2002, 72,649 patients were admitted for selected ICD-10 codes. From 1996 to 2001 total hospital admissions steadily increased from 58,409 to 73,655. From 2002 to 2005 total hospital admissions remained stable from 72,649 to 72,290. TRUS Guided Prostate Biopsy Mortality For all patients the 30-day mortality rate was 0.09% (64 of 75, 190). The 30-day mortality rates were similar between patients diagnosed with cancer (0.07%, 25 of 33, 508) and those without cancer (0.09%, 39 of 41, 482, p 0.37). Between 1996 and 2005 there was no change in trends of 30-day hospital mortality rates among all patients. In 1996 the 30-day mortality rate was 0.09% and 0.11% in 2005 (range 0.07% to 0.13%). Specific cause of death could not be ascertained through this data linkage. DISCUSSION We observed an increased rate in hospital admissions for urological complications after TRUS guided biopsy from 1996 to 2005 in Ontario, Canada. The increase could be attributed to increasing rates of infection related diagnoses. The majority of hospital admissions occurred within the first week after biopsy. It would be of interest to examine whether these trends continue beyond 2005 and will be forthcoming as data linkages become available. The principal strength of our study is that because our publicly funded health care system consists of a single payer system (OHIP), all biopsy procedures for the population could be identified within the study period. In addition, the transition from ICD-9 to ICD-10 coding versions did not appear to bias our results. We did not perform a medical chart audit of each case to determine the exact cause of hospital admission which is an important limitation in using administrative data. Although we tried to minimize measurement error, coding idiosyncrasies may be present which could bias our results. In the future examination of these records will be conducted to confirm these findings and to identify any key trends, particularly examining the prebiopsy protocols and urinary culture results. Also, our study would have missed patients who were treated on an outpatient basis, or those who presented to an emergency department, and were treated and discharged home. Data on emergency room visits could not be obtained during the same study period. Further study in these areas would be important to conduct. It is unclear why there is an increasing trend of hospital admission rates, particularly for infec-
5 S16 HOSPITAL ADMISSION FOR UROLOGICAL COMPLICATIONS AFTER PROSTATE BIOPSY Table 2. Rates of 30-day hospital admission for complications following TRUS guided biopsy by baseline variables among patients without cancer based on biopsy result No. Pts Admitted (%) No. Pts Not Admitted p Value Adjusted OR* 95% CI p Value Yr of biopsy: (1.0) 3, table (1.1) 4, (1.3) 4, (1.1) 3,893 For trend (1.3) 4, (1.8) 5, (2.3) 4, (1.9) 3, (3.1) 3, (4.1) 3, Age category: Younger than (2.4) 1, table (1.8) 9, (1.9) 16, (1.8) 11,158 For trend or Older 25 (1.5) 1, SES: 1 95 (1.6) 5, table (2.0) 7, (1.5) 7, (2.2) 8,483 For trend (1.9) 10, Physician vol * Multivariate logistic model also adjusted for physician clustering using generalized estimating equations. Chi-square value for 9 2 table 201.8,9 df. Based on logistic regression model using year of biopsy, age and SES variables as ordinal covariates. OR for admission for every 10 biopsies performed per physician per year. Based on 457 physicians performing all biopsies in Ontario. Each biopsy procedure assigned a procedural volume based on the number performed for the previous year from the date of biopsy. tions. Men with underlying prostatitis which would prompt a prostate biopsy due to falsely increased prostate specific antigen may have been predisposed to exacerbated infection requiring hospital admission. This may be a possible etiological source and further medical chart reviews would be helpful in determining this as a possible cause. Antibiotic prophylaxis is often used to prevent infection but the practice is nonstandardized. Lee et al conducted a survey in the United Kingdom of the practice patterns of prostate biopsy. 10 Of the 140 physicians surveyed 48% used a single agent antibiotic and 52% used multiple antibiotics. Only 18% of physicians used a mechanical bowel preparation, 10 although this practice remains controversial. 11 In addition, in a cohort of 30,851 subjects in 2004/5 Laupland et al reported that up to 6% of pathogens causing community onset urinary tract infections were resistant to ciprofloxacin. 12 Feliciano et al reported that of Table 3. Breakdown of 30-day hospital admission rates by underlying diagnosis category Yr of Biopsy Infection Related Complications OR (95% CI, p value) Bleeding Related Complications OR (95% CI, p value) Obstruction Related Complications OR (95% CI, p value) ( , 0.84) 1.21 ( , 0.57) 1.69 ( , 0.56) ( , 0.24) 1.23 ( , 0.54) 2.32 ( , 0.34) ( , 0.37) 0.57 ( , 0.17) 3.51 ( , 0.06) ( , 0.34) 1.28 ( , 0.44) 2.15 ( , 0.38) ( , 0.06) 0.96 ( , 0.91) 4.12 ( , 0.08) ( , 0.007) 0.89 ( , 0.74) 4.98 ( , 0.10) ( , 0.05) 0.70 ( , 0.70) 6.21 ( , 0.02) ( , 0.002) 1.28 ( , 0.48) 4.50 ( , 0.07) ( , ) 0.89 ( , 0.89) 4.33 ( , 0.02) Odds ratios (adjusting for physician clustering) based on all patients undergoing biopsy using infection, bleeding and obstruction as primary outcome variable, and year of biopsy as ordinal variable in the logistic regression model with 1996 as the baseline model. Tests for trend for infection related diagnosis p , chi-square 183.2; for bleeding related diagnosis p 0.48 and for obstruction related diagnosis p
6 HOSPITAL ADMISSION FOR UROLOGICAL COMPLICATIONS AFTER PROSTATE BIOPSY S17 1,273 patients undergoing prostate biopsy in whom an infection developed the prevalence of resistant organisms increased. 7 Another possibility is that there may have been an increase in the average number of needle core samples obtained over time. Currently up to 21 needle core samples are examined (extended pattern). 13 We did not have detailed information on how the biopsy was performed in terms of the needle core number and pattern, or the type of anesthesia used. However, when we examined the hospital admission rates for patients who underwent repeat prostate biopsy, the admission rates were not higher and also showed a similar increasing trend. Generally patients undergoing repeat prostate biopsy have more needle cores obtained. Thus, increasing number of needle cores may not be the sole reason for the increase in hospital admission rates. Also, studies that compare the sextant pattern and the extended pattern of biopsies showed no significant increase in morbidity rates. 13,14 However, these studies had small sample sizes and were underpowered to examine for differences. Further medical audits of our subjects will be required to examine these details. It is also important to note that mortality rates did not increase during the same study period and that specific medical chart audits will be required to examine the specific causes of death. It is unclear why mortality rates did not increase similarly, but treatment methods for sepsis in hospital may have averted this. It is also important to consider noninfectious complications. We saw a small increase in complications related to urinary obstruction, although the number of patients was small. This may be a result of a higher prevalence of benign prostatic hyperplasia due to the aging population. 15 A steady rate of bleeding related complications is consistent with previous findings that showed men taking low dose aspirin did not have increased rates of bleeding. 16 Patients of physicians who performed a high number of biopsy procedures experienced relatively low 30-day hospital admission rates. This has not been seen for TRUS biopsies before, but physician volume has been associated with patient outcome for other urological procedures such as radical prostatectomy. 17 REFERENCES 1. Hodge KK, McNeal JE and Stamey TA: Ultrasound guided transrectal core biopsies of the palpably abnormal prostate. J Urol 1989; 142: Terris MK: Ultrasonography and biopsy of the prostate. In: Campbell s Urology, 8th ed. Edited by PC Walsh, AB Retik, ED Vaughan et al: Philadelphia: Saunders 2002; vol. 4, pp Kapoor DA, Klimberg IW, Malek GH et al: Single-dose oral ciprofloxacin versus placebo for prophylaxis during transrectal prostate biopsy. Urology 1998; 52: Aron M, Rajeev TP and Gupta NP: Antibiotic prophylaxis for transrectal needle biopsy of the prostate: a randomized controlled study. BJU Int 2000; 85: Ghani KR, Dundas D and Patel U: Bleeding after transrectal ultrasonography-guided prostate biopsy: a study of 7-day morbidity after a six-, eight- and 12-core biopsy protocol. BJU Int 2004; 94: Sieber PR, Rommel FM, Theodoran CG et al: Contemporary prostate biopsy complication rates in community-based urology practice. Urology 2007; 70: 498. EDITORIAL COMMENTS 7. Feliciano J, Teper E, Ferrandino M et al: The incidence of fluoroquinolone resistant infections after prostate biopsy are fluoroquinolones still effective prophylaxis? J Urol 2008; 179: Raaijmakers R, Kirkels WJ, Roobol MJ et al: Complication rates and risk factors of 5802 transrectal ultrasound-guided sextant biopsies of the prostate within a population-based screening program. Urology 2002; 60: Deyo RA, Cherkin DC and Ciol MA: Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 1992; 45: Lee G, Attar K, Laniado M et al: Trans-rectal ultrasound guided biopsy of the prostate: nationwide diversity in practice and training in the United Kingdom. Int Urol Nephrol 2007; 39: Jeon SS, Woo SH, Hyun JH et al: Bisacodyl rectal preparation can decrease infectious complications of transrectal ultrasound-guided prostate biopsy. Urology 2003; 62: Laupland KB, Ross T, Pitout JD et al: Communityonset urinary tract infections: a population-based assessment. Infection 2007; 35: de la Taille A, Antiphon P, Salomon L et al: Prospective evaluation of a 21-sample needle biopsy procedure designed to improve the prostate cancer detection rate. Urology 2003; 61: Presti JC Jr, Chang JJ, Bhargava V et al: The optimal systematic prostate biopsy scheme should include 8 rather than 6 biopsies: results of a prospective clinical trial. J Urol 2000; 163: Roehrborn CG, Nuckolls JG, Wei JT et al: The benign prostatic hyperplasia registry and patient survey: study design, methods and patient baseline characteristics. BJU Int 2007; 100: Giannarini G, Mogorovich A, Valent F et al: Continuing or discontinuing low-dose aspirin before transrectal prostate biopsy: results of a prospective randomized trial. Urology 2007; 70: Begg CB, Riedel ER, Bach PB et al: Variations in morbidity after radical prostatectomy. N Engl J Med 2002; 346: This population based study conducted on more than 75,000 men in Canada analyzed hospitalization due to prostate biopsy complications between 1996 and The Canadian health care system is nationally run and has the advantage of compiling data on all patients into 1 file. Interestingly the study demonstrated that patients with prostate cancer had a lower incidence of complications than those without prostate cancer. The majority of complications were for infections. Preexisting infection (eg prostatitis) may explain higher rates in patients without prostate cancer.
7 S18 HOSPITAL ADMISSION FOR UROLOGICAL COMPLICATIONS AFTER PROSTATE BIOPSY The study also demonstrated that complication rates increased from 1% to 4% during the 10-year period. In addition, it would be valuable to know if outpatient complications also increased. This study adds to the growing body of evidence supporting the need for the development of standardized prostate biopsy prophylaxis protocols, with overall goals of decreasing post-biopsy infectious complications (reference 3 in article). Moreover this reinforces the need for urologists to treat urinary tract infections before performing prostate biopsy (reference 8 in article). 1 Janet Colli Department of Urology University of Alabama Birmingham, Alabama REFERENCE 1. Djavan B, Waldert M, Zlotta A et al: Safety and morbidity of first and repeat transrectal ultrasound guided prostate needle biopsies: results of a prospective European prostate cancer detection study. J Urol 2001; 166: 856. Nam et al present an insightful and careful assessment of complications related to transrectal ultrasound guided prostate biopsies. During a study period of 1 decade postoperative (30-day) hospital admission rates and admission diagnoses were determined from ICD-9 and ICD-10 codes as applied to a data set of more than 75,000 men from a single, government operated health insurance system in Ontario, Canada. The authors found a statistically significant yet concerning trend toward increasing infection related admissions within 30 days of the biopsy, increasing from 1.0% in 1996 to 4.1% in All cause mortality rates within 30 days from the date of biopsy and admission rates for urinary obstruction or bleeding complications remained steady, or did not change significantly during the study period. Why did infection related admissions increase over time? Hopefully the answer to this important question is forthcoming. The authors acknowledge potential study biases that medical records were not reviewed, emergency room visits were not evaluated, outpatient management of complications (infections, episodes of obstruction requiring catheterization) was undetermined and the number of cores obtained per biopsy session was unknown. Essentially the prostate biopsy practice patterns of urologists in the Ontario province (ie bowel/rectal cleansing preparations, antibiotic use and duration, and number of biopsy cores) and arguably the practice patterns of urologists across the world vary greatly (reference 10 in article). During the last decade there has been a general decrease in antibiotic use and rectal cleansing (ie enemas or other forms of bowel preparation) simultaneous with the recognition that extended biopsy schemes increase the diagnostic yield of the procedure for detecting prostate cancer. 1 The ongoing work by this collaborative group of physicians should facilitate the establishment of best practice statements related to the performance of prostate biopsies. Wade J. Sexton Genitourinary Oncology Program H. Lee Moffitt Cancer Center Tampa, Florida REFERENCE 1. Eskew LA, Bare RL and McCullough DL: Systematic 5 region prostate biopsy is superior to sextant method for diagnosing carcinoma of the prostate. J Urol 1997; 157: 199.
Key Words: prostatic neoplasms, biopsy, infection, sepsis, treatment outcome
 Infection/Inflammation The Impact of Repeat Biopsies on Infectious Complications in Men with Prostate Cancer on Active Surveillance Behfar Ehdaie,* Emily Vertosick,* Massimiliano Spaliviero,* Anna Giallo-Uvino,*
Infection/Inflammation The Impact of Repeat Biopsies on Infectious Complications in Men with Prostate Cancer on Active Surveillance Behfar Ehdaie,* Emily Vertosick,* Massimiliano Spaliviero,* Anna Giallo-Uvino,*
Major Complications and Associated Risk Factors of Transrectal Ultrasound Guided Prostate Needle Biopsy: A Retrospective Study of 1875 Cases in Taiwan
 ORIGINAL ARTICLE Major Complications and Associated Risk Factors of Transrectal Ultrasound Guided Prostate Needle Biopsy: A Retrospective Study of 1875 Cases in Taiwan I-Ni Chiang, 1 Shang-Jen Chang, 2
ORIGINAL ARTICLE Major Complications and Associated Risk Factors of Transrectal Ultrasound Guided Prostate Needle Biopsy: A Retrospective Study of 1875 Cases in Taiwan I-Ni Chiang, 1 Shang-Jen Chang, 2
Thuchchai Pipitpanpipit, M.D.
 ARC Journal of Urology Volume 1, Issue 2, 2016, PP 15-19 www.arcjournals.org Prospective Randomized Controlled Study of the Results of Medication with Oral versus Oralcefixime to Prevent Transient Bacteraemia
ARC Journal of Urology Volume 1, Issue 2, 2016, PP 15-19 www.arcjournals.org Prospective Randomized Controlled Study of the Results of Medication with Oral versus Oralcefixime to Prevent Transient Bacteraemia
THE SIGNIFICANCE OF HYPOECHOIC LESION DIRECTED AND TRANSITION ZONE BIOPSIES IN IMPROVING THE DIAGNOSTIC ABILITY IN PROSTATE CANCER
 Clinical Urology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 222-226, May - June, 2001 THE SIGNIFICANCE OF HYPOECHOIC LESION DIRECTED AND TRANSITION ZONE
Clinical Urology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 222-226, May - June, 2001 THE SIGNIFICANCE OF HYPOECHOIC LESION DIRECTED AND TRANSITION ZONE
Are extended biopsies really necessary to improve prostate cancer detection?
 (2003) 6, 250 255 & 2003 Nature Publishing Group All rights reserved 1365-7852/03 $25.00 www.nature.com/pcan Are extended biopsies really necessary to improve prostate cancer detection? R Damiano*,1, R
(2003) 6, 250 255 & 2003 Nature Publishing Group All rights reserved 1365-7852/03 $25.00 www.nature.com/pcan Are extended biopsies really necessary to improve prostate cancer detection? R Damiano*,1, R
Prostate Cancer Screening Guidelines in 2017
 Prostate Cancer Screening Guidelines in 2017 Pocharapong Jenjitranant, M.D. Division of Urology, Department of Surgery, Faculty of Medicine, Ramathibodi Hospital Prostate Specific Antigen (PSA) Prostate
Prostate Cancer Screening Guidelines in 2017 Pocharapong Jenjitranant, M.D. Division of Urology, Department of Surgery, Faculty of Medicine, Ramathibodi Hospital Prostate Specific Antigen (PSA) Prostate
Since the beginning of the prostate-specific antigen (PSA) era in the. Characteristics of Insignificant Clinical T1c Prostate Tumors
 2001 Characteristics of Insignificant Clinical T1c Prostate Tumors A Contemporary Analysis Patrick J. Bastian, M.D. 1 Leslie A. Mangold, B.A., M.S. 1 Jonathan I. Epstein, M.D. 2 Alan W. Partin, M.D., Ph.D.
2001 Characteristics of Insignificant Clinical T1c Prostate Tumors A Contemporary Analysis Patrick J. Bastian, M.D. 1 Leslie A. Mangold, B.A., M.S. 1 Jonathan I. Epstein, M.D. 2 Alan W. Partin, M.D., Ph.D.
Finland and Sweden and UK GP-HOSP datasets
 Web appendix: Supplementary material Table 1 Specific diagnosis codes used to identify bladder cancer cases in each dataset Finland and Sweden and UK GP-HOSP datasets Netherlands hospital and cancer registry
Web appendix: Supplementary material Table 1 Specific diagnosis codes used to identify bladder cancer cases in each dataset Finland and Sweden and UK GP-HOSP datasets Netherlands hospital and cancer registry
Supplementary Online Content
 Supplementary Online Content Pincus D, Ravi B, Wasserstein D. Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. JAMA. doi: 10.1001/jama.2017.17606 eappendix
Supplementary Online Content Pincus D, Ravi B, Wasserstein D. Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. JAMA. doi: 10.1001/jama.2017.17606 eappendix
Prostate gold seed fiducial implantation by radiation oncologists: A report on feasibility
 Prostate gold seed fiducial implantation by radiation oncologists: A report on feasibility Poster No.: R-0006 Congress: Type: Authors: Keywords: DOI: 2014 CSM Scientific Exhibit C. Jayaratne, A. Brown,
Prostate gold seed fiducial implantation by radiation oncologists: A report on feasibility Poster No.: R-0006 Congress: Type: Authors: Keywords: DOI: 2014 CSM Scientific Exhibit C. Jayaratne, A. Brown,
Cancer. Description. Section: Surgery Effective Date: October 15, 2016 Subsection: Original Policy Date: September 9, 2011 Subject:
 Subject: Saturation Biopsy for Diagnosis, Last Review Status/Date: September 2016 Page: 1 of 9 Saturation Biopsy for Diagnosis, Description Saturation biopsy of the prostate, in which more cores are obtained
Subject: Saturation Biopsy for Diagnosis, Last Review Status/Date: September 2016 Page: 1 of 9 Saturation Biopsy for Diagnosis, Description Saturation biopsy of the prostate, in which more cores are obtained
J Clin Oncol 28: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 28 NUMBER 1 JANUARY 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Clinical Results of Long-Term Follow-Up of a Large, Active Surveillance Cohort With Localized Prostate Cancer
VOLUME 28 NUMBER 1 JANUARY 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Clinical Results of Long-Term Follow-Up of a Large, Active Surveillance Cohort With Localized Prostate Cancer
Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer
 Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Transrectal ultrasound-guided biopsy for the diagnosis of prostate cancer
 Transrectal ultrasound-guided for the diagnosis of prostate cancer Adrian Haşegan Clinica de Urologie, Spitalul Clinic Judeţean de Urgenţă Sibiu Facultatea de Medicină Sibiu Abstract Transrectal ultrasound-guided
Transrectal ultrasound-guided for the diagnosis of prostate cancer Adrian Haşegan Clinica de Urologie, Spitalul Clinic Judeţean de Urgenţă Sibiu Facultatea de Medicină Sibiu Abstract Transrectal ultrasound-guided
Controversies in Prostate Cancer Screening
 Controversies in Prostate Cancer Screening William J Catalona, MD Northwestern University Chicago Disclosure: Beckman Coulter, a manufacturer of PSA assays, provides research support PSA Screening Recommendations
Controversies in Prostate Cancer Screening William J Catalona, MD Northwestern University Chicago Disclosure: Beckman Coulter, a manufacturer of PSA assays, provides research support PSA Screening Recommendations
The efficacy of duration of prophylactic antibiotics in transrectal ultrasound guided prostate biopsy
 ORIGINAL ARTICLE Vol. 41 (5): 906-910, September - October, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0419 The efficacy of duration of prophylactic antibiotics in transrectal ultrasound guided prostate biopsy
ORIGINAL ARTICLE Vol. 41 (5): 906-910, September - October, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0419 The efficacy of duration of prophylactic antibiotics in transrectal ultrasound guided prostate biopsy
ONCOLOGY LETTERS 8: , 2014
 1834 Systematic 12 and 13 core transrectal ultrasound or magnetic resonance imaging guided biopsies significantly improve prostate cancer detection rate: A single center 13 year experience GONG CHENG *,
1834 Systematic 12 and 13 core transrectal ultrasound or magnetic resonance imaging guided biopsies significantly improve prostate cancer detection rate: A single center 13 year experience GONG CHENG *,
The effect of surgeon volume on procedure selection in non-small cell lung cancer surgeries. Dr. Christian Finley MD MPH FRCSC McMaster University
 The effect of surgeon volume on procedure selection in non-small cell lung cancer surgeries Dr. Christian Finley MD MPH FRCSC McMaster University Disclosures I have no conflict of interest disclosures
The effect of surgeon volume on procedure selection in non-small cell lung cancer surgeries Dr. Christian Finley MD MPH FRCSC McMaster University Disclosures I have no conflict of interest disclosures
Preoperative Gleason score, percent of positive prostate biopsies and PSA in predicting biochemical recurrence after radical prostatectomy
 JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
Ultrasound-guided transrectal extended prostate biopsy: a prospective study
 DOI: 10.1111/j.1745-7262.2005.00019.x. Original Article. Ultrasound-guided transrectal extended prostate biopsy: a prospective study Mohammed Ahmed Al-Ghazo, Ibrahim Fathi Ghalayini, Ismail Ibrahim Matalka
DOI: 10.1111/j.1745-7262.2005.00019.x. Original Article. Ultrasound-guided transrectal extended prostate biopsy: a prospective study Mohammed Ahmed Al-Ghazo, Ibrahim Fathi Ghalayini, Ismail Ibrahim Matalka
INTEROBSERVER VARIATION OF PROSTATIC VOLUME ESTIMATION WITH DIGITAL RECTAL EXAMINATION BY UROLOGICAL STAFFS WITH DIFFERENT EXPERIENCES
 Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology DIGITAL RECTAL EXAMINATION BY UROLOGICAL STAFFS Vol. 30 (6): 466-471, November - December, 2004 INTEROBSERVER
Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology DIGITAL RECTAL EXAMINATION BY UROLOGICAL STAFFS Vol. 30 (6): 466-471, November - December, 2004 INTEROBSERVER
Questions and Answers about Prostate Cancer Screening with the Prostate-Specific Antigen Test
 Questions and Answers about Prostate Cancer Screening with the Prostate-Specific Antigen Test About Cancer Care Ontario s recommendations for prostate-specific antigen (PSA) screening 1. What does Cancer
Questions and Answers about Prostate Cancer Screening with the Prostate-Specific Antigen Test About Cancer Care Ontario s recommendations for prostate-specific antigen (PSA) screening 1. What does Cancer
Clinical Study Single Dose of Levofloxacin versus Three Dosages for Prophylaxis in Prostate Biopsy
 International Scholarly Research Notices, Article ID 875670, 4 pages http://dx.doi.org/10.1155/2014/875670 Clinical Study Single Dose of Levofloxacin versus Three Dosages for Prophylaxis in Prostate Biopsy
International Scholarly Research Notices, Article ID 875670, 4 pages http://dx.doi.org/10.1155/2014/875670 Clinical Study Single Dose of Levofloxacin versus Three Dosages for Prophylaxis in Prostate Biopsy
Contribution of prostate-specific antigen density in the prediction of prostate cancer: Does prostate volume matter?
 ORIGINAL ARTICLE Gulhane Med J 2018;60: 14-18 Gülhane Faculty of Medicine 2018 doi: 10.26657/gulhane.00010 Contribution of prostate-specific antigen density in the prediction of prostate cancer: Does prostate
ORIGINAL ARTICLE Gulhane Med J 2018;60: 14-18 Gülhane Faculty of Medicine 2018 doi: 10.26657/gulhane.00010 Contribution of prostate-specific antigen density in the prediction of prostate cancer: Does prostate
Ultrasound Reimbursement Guide 2015: BioJet Fusion
 Ultrasound Reimbursement Guide 2015: BioJet Fusion Diagnosis codes explain the rationale for a given service and are a key factor in a payer s evaluation of medical necessity and coverage determination
Ultrasound Reimbursement Guide 2015: BioJet Fusion Diagnosis codes explain the rationale for a given service and are a key factor in a payer s evaluation of medical necessity and coverage determination
PREVALENCE OF PROSTATE CANCER AMONG HYPOGONADAL MEN WITH PROSTATE-SPECIFIC ANTIGEN LEVELS OF 4.0 ng/ml OR LESS
 ADULT UROLOGY PREVALENCE OF PROSTATE CANCER AMONG HYPOGONADAL MEN WITH PROSTATE-SPECIFIC ANTIGEN LEVELS OF 4.0 ng/ml OR LESS ABRAHAM MORGENTALER AND ERNANI LUIS RHODEN ABSTRACT Objectives. To determine
ADULT UROLOGY PREVALENCE OF PROSTATE CANCER AMONG HYPOGONADAL MEN WITH PROSTATE-SPECIFIC ANTIGEN LEVELS OF 4.0 ng/ml OR LESS ABRAHAM MORGENTALER AND ERNANI LUIS RHODEN ABSTRACT Objectives. To determine
Increasing Awareness, Diagnosis, and Treatment of BPH, LUTS, and EP
 Introduction to Enlarged Prostate E. David Crawford, MD Professor of Surgery (Urology) and Radiation Oncology Head, Urologic Oncology E. David Crawford Endowed Chair in Urologic Oncology University of
Introduction to Enlarged Prostate E. David Crawford, MD Professor of Surgery (Urology) and Radiation Oncology Head, Urologic Oncology E. David Crawford Endowed Chair in Urologic Oncology University of
THE UROLOGY GROUP
 THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
Health Quality Ontario
 Health Quality Ontario The provincial advisor on the quality of health care in Ontario Indicator Technical Specifications for the Quality Standard Major Depression: Care for Adults and Adolescents Technical
Health Quality Ontario The provincial advisor on the quality of health care in Ontario Indicator Technical Specifications for the Quality Standard Major Depression: Care for Adults and Adolescents Technical
Introduction. Key Words: high-grade prostatic intraepithelial neoplasia, HGPIN, radical prostatectomy, prostate biopsy, insignificant prostate cancer
 Prostate cancer after initial high-grade prostatic intraepithelial neoplasia and benign prostate biopsy Premal Patel, MD, 1 Jasmir G. Nayak, MD, 1,2 Zlatica Biljetina, MD, 4 Bryan Donnelly, MD 3, Kiril
Prostate cancer after initial high-grade prostatic intraepithelial neoplasia and benign prostate biopsy Premal Patel, MD, 1 Jasmir G. Nayak, MD, 1,2 Zlatica Biljetina, MD, 4 Bryan Donnelly, MD 3, Kiril
Computer simulated additional deep apical biopsy enhances cancer detection in palpably benign prostate gland
 Blackwell Publishing AsiaMelbourne, AustraliaIJUInternational Journal of Urology0919-81722006 Blackwell Publishing Asia Pty Ltd? 200613?12901295Original ArticleAdditional apical biopsy in prostatic gland
Blackwell Publishing AsiaMelbourne, AustraliaIJUInternational Journal of Urology0919-81722006 Blackwell Publishing Asia Pty Ltd? 200613?12901295Original ArticleAdditional apical biopsy in prostatic gland
Extended 12-Core Prostate Biopsy Increases Both the Detection of Prostate Cancer and the Accuracy of Gleason Score
 european urology xxx (2005) xxx xxx available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Extended 12-Core Prostate Biopsy Increases Both the Detection of Prostate
european urology xxx (2005) xxx xxx available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Extended 12-Core Prostate Biopsy Increases Both the Detection of Prostate
Ambulatory Try off Catheter (ATOC) Program for the Patient with Acute Retention of Urine Outpatient Service
 Ambulatory Try off Catheter (ATOC) Program for the Patient with Acute Retention of Urine Outpatient Service Mr. Tang, Chi Chiu Kevin (APN) Urology Center Department of Surgery Kwong Wah Hospital Redevelopment
Ambulatory Try off Catheter (ATOC) Program for the Patient with Acute Retention of Urine Outpatient Service Mr. Tang, Chi Chiu Kevin (APN) Urology Center Department of Surgery Kwong Wah Hospital Redevelopment
REPORTS. Clinical and Economic Outcomes in Patients Treated for Enlarged Prostate
 Clinical and Economic Outcomes in Patients Treated for Enlarged Prostate Michael James Naslund, MD, MBA; Muta M. Issa, MD, MBA; Amy L. Grogg, PharmD; Michael T. Eaddy, PharmD, PhD; and Libby Black, PharmD
Clinical and Economic Outcomes in Patients Treated for Enlarged Prostate Michael James Naslund, MD, MBA; Muta M. Issa, MD, MBA; Amy L. Grogg, PharmD; Michael T. Eaddy, PharmD, PhD; and Libby Black, PharmD
The Impact of MRI-TRUS Cognitively Targeted Biopsy on the Incidence of Pathologic Upgrading After Radical Prostatectomy
 Original Article World J Nephrol Urol. 2018;7(1):12-16 The Impact of MRI-TRUS Cognitively Targeted Biopsy on the Incidence of Pathologic Upgrading After Radical Prostatectomy Ragheed Saoud a, Albert El-Haj
Original Article World J Nephrol Urol. 2018;7(1):12-16 The Impact of MRI-TRUS Cognitively Targeted Biopsy on the Incidence of Pathologic Upgrading After Radical Prostatectomy Ragheed Saoud a, Albert El-Haj
Owing to the widespread use of prostate specific antigen (PSA)
 ORIGINAL RESEARCH Subsequent prostate cancer detection in patients with prostatic intraepithelial neoplasia or atypical small acinar proliferation Moamen M. Amin, MD; Suganthiny Jeyaganth, MSc; Nader Fahmy,
ORIGINAL RESEARCH Subsequent prostate cancer detection in patients with prostatic intraepithelial neoplasia or atypical small acinar proliferation Moamen M. Amin, MD; Suganthiny Jeyaganth, MSc; Nader Fahmy,
Date Modified: May 29, Clinical Quality Measures for PQRS
 Date Modified: May 29, 2014 Clinical Quality s for PQRS # Domain Type Denominator Numerator Denominator Exclusions/Exceptions Rationale QCDR-1 QCDR-2 Patient Safety 102 Efficiency and Cost Reduction QCDR-3
Date Modified: May 29, 2014 Clinical Quality s for PQRS # Domain Type Denominator Numerator Denominator Exclusions/Exceptions Rationale QCDR-1 QCDR-2 Patient Safety 102 Efficiency and Cost Reduction QCDR-3
Estimates and predictors of health care costs of esophageal adenocarcinoma: a population-based cohort study
 Thein et al. BMC Cancer (2018) 18:694 https://doi.org/10.1186/s12885-018-4620-2 RESEARCH ARTICLE Estimates and predictors of health care costs of esophageal adenocarcinoma: a population-based cohort study
Thein et al. BMC Cancer (2018) 18:694 https://doi.org/10.1186/s12885-018-4620-2 RESEARCH ARTICLE Estimates and predictors of health care costs of esophageal adenocarcinoma: a population-based cohort study
Supplementary Online Content
 Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Supplementary Online Content
 Supplementary Online Content Pham B, Stern A, Chen W, et al. Preventing pressure ulcers in long-term care: a costeffectiveness analysis. Arch Intern Med. Published online September 26, 2011. doi:10.1001/archinternmed.2011.473
Supplementary Online Content Pham B, Stern A, Chen W, et al. Preventing pressure ulcers in long-term care: a costeffectiveness analysis. Arch Intern Med. Published online September 26, 2011. doi:10.1001/archinternmed.2011.473
The Chances of Subsequent Cancer Detection in Patients with a PSA > 20 ng/ml and an Initial Negative Biopsy
 Research Article TheScientificWorldJOURNAL (2009) 9, 343 348 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.47 The Chances of Subsequent Cancer Detection in Patients with a PSA > 20 ng/ml and an Initial
Research Article TheScientificWorldJOURNAL (2009) 9, 343 348 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.47 The Chances of Subsequent Cancer Detection in Patients with a PSA > 20 ng/ml and an Initial
α-blocker Monotherapy and α-blocker Plus 5-Alpha-Reductase Inhibitor Combination Treatment in Benign Prostatic Hyperplasia; 10 Years Long-Term Results
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.4.248 Voiding Dysfunction α-blocker Monotherapy and α-blocker Plus 5-Alpha-Reductase Inhibitor Combination Treatment in Benign Prostatic Hyperplasia;
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.4.248 Voiding Dysfunction α-blocker Monotherapy and α-blocker Plus 5-Alpha-Reductase Inhibitor Combination Treatment in Benign Prostatic Hyperplasia;
Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer
 Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer Policy Number: 7.01.121 Last Review: 2/2018 Origination: 8/2006 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas
Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer Policy Number: 7.01.121 Last Review: 2/2018 Origination: 8/2006 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas
Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009
 Western University Scholarship@Western Electronic Thesis and Dissertation Repository June 2015 Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009 Ngan Lam The University
Western University Scholarship@Western Electronic Thesis and Dissertation Repository June 2015 Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009 Ngan Lam The University
A Competing Risk Analysis of Men Age Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer
 A Competing Risk Analysis of Men Age 55-74 Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer Peter C. Albertsen, MD 1 James A. Hanley, PhD 2 Donald F.Gleason, MD, PhD 3
A Competing Risk Analysis of Men Age 55-74 Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer Peter C. Albertsen, MD 1 James A. Hanley, PhD 2 Donald F.Gleason, MD, PhD 3
Data Sources, Methods and Limitations
 Data Sources, Methods and Limitations The main data sources, methods and limitations of the data used in this report are described below: Local Surveys Rapid Risk Factor Surveillance System Survey The
Data Sources, Methods and Limitations The main data sources, methods and limitations of the data used in this report are described below: Local Surveys Rapid Risk Factor Surveillance System Survey The
The In uence of Prostate Volume on Prostate Cancer Detection
 European Urology Supplements European Urology Supplements 1 (2002) 35±39 The In uence of Prostate Volume on Prostate Cancer Detection Michael K. Brawer * Northwest Prostate Institute, Seattle, USA Abstract
European Urology Supplements European Urology Supplements 1 (2002) 35±39 The In uence of Prostate Volume on Prostate Cancer Detection Michael K. Brawer * Northwest Prostate Institute, Seattle, USA Abstract
Utility of Incorporating Genetic Variants for the Early Detection of Prostate Cancer
 Utility of Incorporating Genetic Variants for the Early Detection of Prostate Cancer Robert K. Nam, 1,9 William W. Zhang, 1 John Trachtenberg, 6 Arun Seth, 2 Laurence H. Klotz, 1 Aleksandra Stanimirovic,
Utility of Incorporating Genetic Variants for the Early Detection of Prostate Cancer Robert K. Nam, 1,9 William W. Zhang, 1 John Trachtenberg, 6 Arun Seth, 2 Laurence H. Klotz, 1 Aleksandra Stanimirovic,
Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer
 Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer Policy Number: 7.01.121 Last Review: 2/2019 Origination: 8/2006 Next Review: 8/2019 Policy Blue Cross and Blue Shield of Kansas
Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer Policy Number: 7.01.121 Last Review: 2/2019 Origination: 8/2006 Next Review: 8/2019 Policy Blue Cross and Blue Shield of Kansas
Outcomes of Patients with Preoperative Weight Loss following Colorectal Surgery
 Outcomes of Patients with Preoperative Weight Loss following Colorectal Surgery Zhobin Moghadamyeghaneh MD 1, Michael J. Stamos MD 1 1 Department of Surgery, University of California, Irvine Nothing to
Outcomes of Patients with Preoperative Weight Loss following Colorectal Surgery Zhobin Moghadamyeghaneh MD 1, Michael J. Stamos MD 1 1 Department of Surgery, University of California, Irvine Nothing to
Single-Dose Antibiotic Prophylaxis in Core Prostate Biopsy: Impact of Timing and Identification of Risk Factors
 european urology 50 (2006) 832 837 available at www.sciencedirect.com journal homepage: www.europeanurology.com Infections Single-Dose Antibiotic Prophylaxis in Core Prostate Biopsy: Impact of Timing and
european urology 50 (2006) 832 837 available at www.sciencedirect.com journal homepage: www.europeanurology.com Infections Single-Dose Antibiotic Prophylaxis in Core Prostate Biopsy: Impact of Timing and
or more transrectal ultrasonography (TRUS)-guided ng/ml and 39% if it was 20.0 ng/ml. of >10 ng/ml have prostate cancer [3], many other
![or more transrectal ultrasonography (TRUS)-guided ng/ml and 39% if it was 20.0 ng/ml. of >10 ng/ml have prostate cancer [3], many other or more transrectal ultrasonography (TRUS)-guided ng/ml and 39% if it was 20.0 ng/ml. of >10 ng/ml have prostate cancer [3], many other](/thumbs/92/108155308.jpg) BJU International (1999), 83, 34 38 Elevated serum prostate specific antigen levels in conjunction with an initial prostatic biopsy negative for carcinoma: who should undergo a repeat biopsy? G.C. DURKAN
BJU International (1999), 83, 34 38 Elevated serum prostate specific antigen levels in conjunction with an initial prostatic biopsy negative for carcinoma: who should undergo a repeat biopsy? G.C. DURKAN
Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer
 Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer Preliminary Results from the National Program of Cancer Registries Patterns of Care Study (PoC1) NAACCR Annual Meeting
Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer Preliminary Results from the National Program of Cancer Registries Patterns of Care Study (PoC1) NAACCR Annual Meeting
ABSTRACT. KEY WORDS antibiotics; prophylaxis; hysterectomy
 Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
Statin Use and Risk of Prostate Cancer in a Population of Men Who Underwent Biopsy
 Statin Use and Risk of Prostate Cancer in a Population of Men Who Underwent Biopsy Nelly Tan,* Eric A. Klein, Jianbo Li, Ayman S. Moussa and J. Stephen Jones From the Glickman Urological and Kidney Institute,
Statin Use and Risk of Prostate Cancer in a Population of Men Who Underwent Biopsy Nelly Tan,* Eric A. Klein, Jianbo Li, Ayman S. Moussa and J. Stephen Jones From the Glickman Urological and Kidney Institute,
The Risk of Fracture with Taking Alpha Blockers for Treating Benign Prostatic Hyperplasia
 J Prev Med Public Health 2009;42(3):165-170 DOI: 103961/jpmph2009423165 The Risk of Fracture with Taking Alpha Blockers for Treating Benign Prostatic Hyperplasia Joongyub Lee 1) Nam-Kyoung Choi 13) Sun-Young
J Prev Med Public Health 2009;42(3):165-170 DOI: 103961/jpmph2009423165 The Risk of Fracture with Taking Alpha Blockers for Treating Benign Prostatic Hyperplasia Joongyub Lee 1) Nam-Kyoung Choi 13) Sun-Young
NIH Public Access Author Manuscript World J Urol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
National Bowel Cancer Audit Supplementary Report 2011
 National Bowel Cancer Audit Supplementary Report 2011 This Supplementary Report contains data from the 2009/2010 reporting period which covers patients in England with a diagnosis date from 1 August 2009
National Bowel Cancer Audit Supplementary Report 2011 This Supplementary Report contains data from the 2009/2010 reporting period which covers patients in England with a diagnosis date from 1 August 2009
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project
 Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
The Pennsylvania State University. The Graduate School. College of Medicine. The Department of Public Health Sciences
 The Pennsylvania State University The Graduate School College of Medicine The Department of Public Health Sciences EVALUATION OF TWO PROCEDURES FOR TREATMENT OF KNEE PROSTHETIC JOINT INFECTION (PJI) A
The Pennsylvania State University The Graduate School College of Medicine The Department of Public Health Sciences EVALUATION OF TWO PROCEDURES FOR TREATMENT OF KNEE PROSTHETIC JOINT INFECTION (PJI) A
Zhao Y Y et al. Ann Intern Med 2012;156:
 Zhao Y Y et al. Ann Intern Med 2012;156:560-569 Introduction Fibrates are commonly prescribed to treat dyslipidemia An increase in serum creatinine level after use has been observed in randomized, placebocontrolled
Zhao Y Y et al. Ann Intern Med 2012;156:560-569 Introduction Fibrates are commonly prescribed to treat dyslipidemia An increase in serum creatinine level after use has been observed in randomized, placebocontrolled
Nomogram using transrectal ultrasound-derived information predicting the detection of high grade prostate cancer on initial biopsy
 Original Article Prostate Int 2013;1(2):69-75 P R O S T A T E INTERNATIONAL Nomogram using transrectal ultrasound-derived information predicting the detection of high grade prostate cancer on initial biopsy
Original Article Prostate Int 2013;1(2):69-75 P R O S T A T E INTERNATIONAL Nomogram using transrectal ultrasound-derived information predicting the detection of high grade prostate cancer on initial biopsy
Best Papers. F. Fusco
 Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Active surveillance for low-risk Prostate Cancer Compared with Immediate Treatment: A Canadian cost evaluation
 Active surveillance for low-risk Prostate Cancer Compared with Immediate Treatment: A Canadian cost evaluation Alice Dragomir, PhD Fabio Cury, MD Armen Aprikian, MD Introduction Clinical and economic burden
Active surveillance for low-risk Prostate Cancer Compared with Immediate Treatment: A Canadian cost evaluation Alice Dragomir, PhD Fabio Cury, MD Armen Aprikian, MD Introduction Clinical and economic burden
Getting to Diagnosis. Debbie Victor Uro-Oncology CNS Royal Cornwall Hospitals Trust
 Getting to Diagnosis Debbie Victor Uro-Oncology CNS Royal Cornwall Hospitals Trust GP Visit Symptoms Reduced urinary flow Difficulty starting/stopping Urgency Frequency Nocturia Because a friend/relative
Getting to Diagnosis Debbie Victor Uro-Oncology CNS Royal Cornwall Hospitals Trust GP Visit Symptoms Reduced urinary flow Difficulty starting/stopping Urgency Frequency Nocturia Because a friend/relative
Fisher s exact test for contingency tables. A two-tailed p-value <0.05 was accepted as statistically significant.
 BJUI A prospective, randomized trial comparing the Vienna nomogram to an eight-core prostate biopsy protocol Angus Lecuona and Chris F. Heyns Department of Urology, Tygerberg Hospital and University of
BJUI A prospective, randomized trial comparing the Vienna nomogram to an eight-core prostate biopsy protocol Angus Lecuona and Chris F. Heyns Department of Urology, Tygerberg Hospital and University of
Screening for Prostate Cancer
 Screening for Prostate Cancer Review against programme appraisal criteria for the UK National Screening Committee (UK NSC) Version 1: This document summarises the work of ScHARR 1 2 and places it against
Screening for Prostate Cancer Review against programme appraisal criteria for the UK National Screening Committee (UK NSC) Version 1: This document summarises the work of ScHARR 1 2 and places it against
Saturation Biopsy for Diagnosis, Staging, and Management of Prostate Cancer
 Saturation Biopsy for Diagnosis, Staging, and Management of Prostate Cancer Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Saturation Biopsy for Diagnosis, Staging, and Management of Prostate Cancer Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
One Stop Prostate Biopsy Protocol Author Consultation Date Approved
 One Stop Prostate Biopsy Protocol Author Consultation Date Approved Urology Nurse Practioner PROTOCOL FOR MEN ATTENDING A ONE STOP PROSTATE BIOPSY CLINIC RATIONALE Prostate cancer is the most common cancer
One Stop Prostate Biopsy Protocol Author Consultation Date Approved Urology Nurse Practioner PROTOCOL FOR MEN ATTENDING A ONE STOP PROSTATE BIOPSY CLINIC RATIONALE Prostate cancer is the most common cancer
Rates and patterns of participation in cardiac rehabilitation in Victoria
 Rates and patterns of participation in cardiac rehabilitation in Victoria Vijaya Sundararajan, MD, MPH, Stephen Begg, MS, Michael Ackland, MBBS, MPH, FAPHM, Ric Marshall, PhD Victorian Department of Human
Rates and patterns of participation in cardiac rehabilitation in Victoria Vijaya Sundararajan, MD, MPH, Stephen Begg, MS, Michael Ackland, MBBS, MPH, FAPHM, Ric Marshall, PhD Victorian Department of Human
Incidence of Surgically Treated Benign Prostatic Hypertrophy and of Prostate Cancer among Blacks and Whites in a Prepaid Health Care Plan
 American Journal of EpKtermotogy Vo! 134, No 8 Copyright C 1991 by The Johns Hopkrts Uruversfty School of Hygiene and Put*: Health Printed in US A AS rights reserved A BRIEF ORIGINAL CONTRIBUTION Incidence
American Journal of EpKtermotogy Vo! 134, No 8 Copyright C 1991 by The Johns Hopkrts Uruversfty School of Hygiene and Put*: Health Printed in US A AS rights reserved A BRIEF ORIGINAL CONTRIBUTION Incidence
Prostate cancer diagnosis: should patients with prostate specific antigen >10 ng/ml have stratified prostate biopsy protocols?
 Cancer Detection and Prevention 32 (2009) 34 38 www.elsevier.com/locate/cdp Prostate cancer diagnosis: should patients with prostate specific antigen >0 ng/ml have stratified prostate biopsy protocols?
Cancer Detection and Prevention 32 (2009) 34 38 www.elsevier.com/locate/cdp Prostate cancer diagnosis: should patients with prostate specific antigen >0 ng/ml have stratified prostate biopsy protocols?
Ankle fractures are one of
 Elevated Risks of Ankle Fracture Surgery in Patients With Diabetes Nelson F. SooHoo, MD, Lucie Krenek, MD, Michael Eagan, MD, and David S. Zingmond, MD, PhD Ankle fractures are one of the most common types
Elevated Risks of Ankle Fracture Surgery in Patients With Diabetes Nelson F. SooHoo, MD, Lucie Krenek, MD, Michael Eagan, MD, and David S. Zingmond, MD, PhD Ankle fractures are one of the most common types
Supplementary Online Content
 Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
EUROPEAN UROLOGY 58 (2010)
 EUROPEAN UROLOGY 58 (2010) 551 558 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Prostate Cancer Prevention Trial and European Randomized Study of Screening
EUROPEAN UROLOGY 58 (2010) 551 558 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Prostate Cancer Prevention Trial and European Randomized Study of Screening
Correlation of Gleason Scores Between Needle-Core Biopsy and Radical Prostatectomy Specimens in Patients with Prostate Cancer
 ORIGINAL ARTICLE Correlation of Gleason Scores Between Needle-Core Biopsy and Radical Prostatectomy Specimens in Patients with Prostate Cancer Teng-Fu Hsieh, Chao-Hsian Chang, Wen-Chi Chen, Chien-Lung
ORIGINAL ARTICLE Correlation of Gleason Scores Between Needle-Core Biopsy and Radical Prostatectomy Specimens in Patients with Prostate Cancer Teng-Fu Hsieh, Chao-Hsian Chang, Wen-Chi Chen, Chien-Lung
Transurethral Prostatic Resection for Acute Urinary Retention in Patients with Prostate Cancer
 ORIGINAL ARTICLE Transurethral Prostatic Resection for Acute Urinary Retention in Patients with Prostate Cancer Chang-Chi Chang, Junne-Yih Kuo*, Kuang-Kuo Chen, Alex Tong-Long Lin, Yen-Hwa Chang, Howard
ORIGINAL ARTICLE Transurethral Prostatic Resection for Acute Urinary Retention in Patients with Prostate Cancer Chang-Chi Chang, Junne-Yih Kuo*, Kuang-Kuo Chen, Alex Tong-Long Lin, Yen-Hwa Chang, Howard
Annual surveillance mammography after early-stage breast cancer and breast cancer mortality
 ORIGINAL ARTICLE Annual surveillance mammography after early-stage breast cancer and breast cancer mortality L.F. Paszat md ms,* R. Sutradhar phd,* S. Gu msc,* and E. Rakovitch md msc* ABSTRACT Background
ORIGINAL ARTICLE Annual surveillance mammography after early-stage breast cancer and breast cancer mortality L.F. Paszat md ms,* R. Sutradhar phd,* S. Gu msc,* and E. Rakovitch md msc* ABSTRACT Background
Meeting the Guidelines for End-of-Life Care
 Advances in Peritoneal Dialysis, Vol. 22, 2006 Gillian Brunier, David M.J. Naimark, Michelle A. Hladunewich Meeting the Guidelines for End-of-Life Care The number of patients initiating dialysis in most
Advances in Peritoneal Dialysis, Vol. 22, 2006 Gillian Brunier, David M.J. Naimark, Michelle A. Hladunewich Meeting the Guidelines for End-of-Life Care The number of patients initiating dialysis in most
Role of Prostate-Specific Antigen Change Ratio at Initial Biopsy as a Novel Decision-Making Marker for Repeat Prostate Biopsy
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53..46 Urological Oncology Role of Prostate-Specific Antigen Change Ratio at Initial Biopsy as a Novel Decision-Making Marker for Repeat Prostate Biopsy
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53..46 Urological Oncology Role of Prostate-Specific Antigen Change Ratio at Initial Biopsy as a Novel Decision-Making Marker for Repeat Prostate Biopsy
Central European Journal of Urology
 192 O R I G I N A L P A P E R urinary tract infections Fluoroquinolone-resistant Escherichia coli in intestinal flora of patients undergoing transrectal ultrasound-guided prostate biopsy possible shift
192 O R I G I N A L P A P E R urinary tract infections Fluoroquinolone-resistant Escherichia coli in intestinal flora of patients undergoing transrectal ultrasound-guided prostate biopsy possible shift
Attending for your Prostate Scan
 Attending for your Prostate Scan Patient Information The aim of this booklet is to give you enough information: To help you prepare for your hospital visit To give properly informed consent for the procedure
Attending for your Prostate Scan Patient Information The aim of this booklet is to give you enough information: To help you prepare for your hospital visit To give properly informed consent for the procedure
Elsevier Editorial System(tm) for European Urology Manuscript Draft
 Elsevier Editorial System(tm) for European Urology Manuscript Draft Manuscript Number: EURUROL-D-13-00306 Title: Post-Prostatectomy Incontinence and Pelvic Floor Muscle Training: A Defining Problem Article
Elsevier Editorial System(tm) for European Urology Manuscript Draft Manuscript Number: EURUROL-D-13-00306 Title: Post-Prostatectomy Incontinence and Pelvic Floor Muscle Training: A Defining Problem Article
Linkage of Indiana State Cancer Registry and Indiana Network for Patient Care
 Linkage of Indiana State Cancer Registry and Indiana Network for Patient Care A collaboration between Regenstrief Institute, Indiana University, and the Indiana State Cancer Registry Objectives Understand
Linkage of Indiana State Cancer Registry and Indiana Network for Patient Care A collaboration between Regenstrief Institute, Indiana University, and the Indiana State Cancer Registry Objectives Understand
Long-Term Follow-Up of a Large Active Surveillance Cohort of Patients With Prostate Cancer
 Published Ahead of Print on December 15, 1 as 1.1/JCO.1.55.119 The latest version is at http://jco.ascopubs.org/cgi/doi/1.1/jco.1.55.119 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Long-Term
Published Ahead of Print on December 15, 1 as 1.1/JCO.1.55.119 The latest version is at http://jco.ascopubs.org/cgi/doi/1.1/jco.1.55.119 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Long-Term
On-going and planned colorectal cancer clinical outcome analyses
 On-going and planned colorectal cancer clinical outcome analyses Eva Morris Cancer Research UK Bobby Moore Career Development Fellow National Cancer Data Repository Numerous routine health data sources
On-going and planned colorectal cancer clinical outcome analyses Eva Morris Cancer Research UK Bobby Moore Career Development Fellow National Cancer Data Repository Numerous routine health data sources
Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis A. Herran, Peter T. Scardino, James A. Eastham and Farhang Rabbani
 Age, Obesity, Medical Comorbidities and Surgical Technique are Predictive of Symptomatic Anastomotic Strictures After Contemporary Radical Prostatectomy Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis
Age, Obesity, Medical Comorbidities and Surgical Technique are Predictive of Symptomatic Anastomotic Strictures After Contemporary Radical Prostatectomy Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis
The Prevalence and Characteristic Differences in Prostatic Calcification between Health Promotion Center and Urology Department Outpatients
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.5.330 Voiding Dysfunction The Prevalence and Characteristic Differences in Prostatic Calcification between Health Promotion Center and Urology Department
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.5.330 Voiding Dysfunction The Prevalence and Characteristic Differences in Prostatic Calcification between Health Promotion Center and Urology Department
AHA Clinical Science Special Report: November 10, 2015
 www.canheart.ca High-density lipoprotein cholesterol and cause-specific mortality: A population-based study of more than 630,000 individuals without prior cardiovascular conditions Dennis T. Ko, MD, MSc;
www.canheart.ca High-density lipoprotein cholesterol and cause-specific mortality: A population-based study of more than 630,000 individuals without prior cardiovascular conditions Dennis T. Ko, MD, MSc;
Ambulatory and Office Urology Optimal Measure of PSA Kinetics to Identify Prostate Cancer
 Ambulatory and Office Urology Optimal Measure of PSA Kinetics to Identify Prostate Cancer Luigi Benecchi, Anna Maria Pieri, Carmelo Destro Pastizzaro, and Michele Potenzoni OBJECTIVES METHODS RESULTS CONCLUSIONS
Ambulatory and Office Urology Optimal Measure of PSA Kinetics to Identify Prostate Cancer Luigi Benecchi, Anna Maria Pieri, Carmelo Destro Pastizzaro, and Michele Potenzoni OBJECTIVES METHODS RESULTS CONCLUSIONS
Date Modified: March 31, Clinical Quality Measures for PQRS
 Date Modified: March 31, 2015 2015 Clinical Quality s for PQRS # Domain Title Description Type Denominator Numerator Denominator Exclusions/Exceptions 1 Patient Safety Prostate Biopsy Antibiotic Process
Date Modified: March 31, 2015 2015 Clinical Quality s for PQRS # Domain Title Description Type Denominator Numerator Denominator Exclusions/Exceptions 1 Patient Safety Prostate Biopsy Antibiotic Process
Racial and Socioeconomic Disparities in Appendicitis
 Racial and Socioeconomic Disparities in Appendicitis Steven L. Lee, MD Chief of Pediatric Surgery, Harbor-UCLA Associate Clinical Professor of Surgery and Pediatrics David Geffen School of Medicine at
Racial and Socioeconomic Disparities in Appendicitis Steven L. Lee, MD Chief of Pediatric Surgery, Harbor-UCLA Associate Clinical Professor of Surgery and Pediatrics David Geffen School of Medicine at
MRI in the Enhanced Detection of Prostate Cancer: What Urologists Need to Know
 MRI in the Enhanced Detection of Prostate Cancer: What Urologists Need to Know Michael S. Cookson, MD, FACS Professor and Chair Department of Urology Director of Prostate and Urologic Oncology University
MRI in the Enhanced Detection of Prostate Cancer: What Urologists Need to Know Michael S. Cookson, MD, FACS Professor and Chair Department of Urology Director of Prostate and Urologic Oncology University
RESEARCH. Katrina Wilcox Hagberg, 1 Hozefa A Divan, 2 Rebecca Persson, 1 J Curtis Nickel, 3 Susan S Jick 1. open access
 open access Risk of erectile dysfunction associated with use of 5-α reductase inhibitors for benign prostatic hyperplasia or alopecia: population based studies using the Clinical Practice Research Datalink
open access Risk of erectile dysfunction associated with use of 5-α reductase inhibitors for benign prostatic hyperplasia or alopecia: population based studies using the Clinical Practice Research Datalink
Use of early PSA velocity to predict eventual abnormal PSA values in men at risk for prostate cancer {
 Use of early PSA velocity to predict eventual abnormal PSA values in men at risk for prostate cancer { (2003) 6, 39 44 ß 2003 Nature Publishing Group All rights reserved 1365 7852/03 $25.00 www.nature.com/pcan
Use of early PSA velocity to predict eventual abnormal PSA values in men at risk for prostate cancer { (2003) 6, 39 44 ß 2003 Nature Publishing Group All rights reserved 1365 7852/03 $25.00 www.nature.com/pcan
Untreated Gleason Grade Progression on Serial Biopsies during Prostate Cancer Active Surveillance: Clinical Course and Pathological Outcomes
 Untreated Gleason Grade Progression on Serial Biopsies during Prostate Cancer Active Surveillance: Clinical Course and Pathological Outcomes A. A. Hussein,* C. J. Welty,* N. Ameli,* J. E. Cowan, M. Leapman,*
Untreated Gleason Grade Progression on Serial Biopsies during Prostate Cancer Active Surveillance: Clinical Course and Pathological Outcomes A. A. Hussein,* C. J. Welty,* N. Ameli,* J. E. Cowan, M. Leapman,*
The Pennsylvania State University. The Graduate School. Department of Public Health Sciences
 The Pennsylvania State University The Graduate School Department of Public Health Sciences THE LENGTH OF STAY AND READMISSIONS IN MASTECTOMY PATIENTS A Thesis in Public Health Sciences by Susie Sun 2015
The Pennsylvania State University The Graduate School Department of Public Health Sciences THE LENGTH OF STAY AND READMISSIONS IN MASTECTOMY PATIENTS A Thesis in Public Health Sciences by Susie Sun 2015
Authors KC Cheng, LF Lee, KW Wong, HC Chan, CL Cho, H Chau, KM Lam, HS So. Division of Urology, Department of Surgery, United Christian Hospital
 Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
Dichotomous Estimation of Prostate Volume: A Diagnostic Study of the Accuracy of the Digital Rectal Examination
 pissn: 2287-4208 / eissn: 2287-4690 World J Mens Health 2013 December 31(3): 220-225 http://dx.doi.org/10.5534/wjmh.2013.31.3.220 Original Article Dichotomous Estimation of Prostate Volume: A Diagnostic
pissn: 2287-4208 / eissn: 2287-4690 World J Mens Health 2013 December 31(3): 220-225 http://dx.doi.org/10.5534/wjmh.2013.31.3.220 Original Article Dichotomous Estimation of Prostate Volume: A Diagnostic
