Inflammatory Atrophy on Prostate Needle Biopsies: Is There Topographic Relationship to Cancer?
|
|
|
- Derek Fitzgerald
- 6 years ago
- Views:
Transcription
1 Clinical Urology Inflammatory Atrophy on Prostate Biopsies and Cancer International Braz J Urol Vol. 33 (3): , May - June, 2007 Inflammatory Atrophy on Prostate Needle Biopsies: Is There Topographic Relationship to Cancer? Athanase Billis, Leandro L. L. Freitas, Luis A. Magna, Ubirajara Ferreira Departments of Anatomic Pathology (AB, LLLF), Genetics and Biostatistics (LAM), and Urology (UF), School of Medicine, State University of Campinas (Unicamp), Campinas, Sao Paulo, Brazil ABSTRACT Introduction: Chronic inflammation of longstanding duration has been linked to the development of carcinoma in several organ systems. It is controversial whether there is any relationship of inflammatory atrophy to prostate cancer. It has been suggested that the proliferative epithelium in inflammatory atrophy may progress to high-grade prostatic intraepithelial neoplasia and/or adenocarcinoma. The objective of our study is to compare on needle prostate biopsies of patients showing cancer the topographical relation of inflammatory atrophy and atrophy with no inflammation to adenocarcinoma. Materials and Methods: The frequency and extent of the lesions were studied on 172 needle biopsies of patients with prostate cancer. In cores showing both lesions, the foci of atrophy were counted. Clinicopathological features were compared according to presence or absence of inflammation. Results: Considering only cores showing adenocarcinoma, atrophy was seen in 116/172 (67.44%) biopsies; 70/116 (60.34%) biopsies showed atrophy and no inflammation and 46/116 (39.66%) biopsies showed inflammatory atrophy. From a total of 481 cores in 72 biopsies with inflammatory atrophy 184/481 (38.25%) cores showed no atrophy; 166/481 (34.51%) cores showed atrophy and no inflammation; 111/481 (23.08%) cores showed both lesions; and 20/481 (4.16%) showed only inflammatory atrophy. There was no statistically significant difference for the clinicopathological features studied. Conclusion: The result of our study seems not to favor the model of prostatic carcinogenesis in which there is a topographical relation of inflammatory atrophy to adenocarcinoma. Key words: prostate; inflammation; atrophy; carcinoma; needle biopsy Int Braz J Urol. 2007; 33: INTRODUCTION Chronic inflammation of longstanding duration has been linked to the development of carcinoma in several organ systems (1-3). In the prostate, it is controversial whether there is any relationship of atrophy with inflammation (or inflammatory atrophy) to prostate cancer (4-10). De Marzo et al. (5) propose that there is a topographical relation with morphological transitions within the same acinar/duct unit, between high-grade prostatic intraepithelial neoplasia (HGPIN) and inflammatory atrophy which occur frequently (7). This finding supports a model whereby the proliferative epithelium in inflammatory atrophy may progress to HGPIN and subsequently to adenocarcinoma. The aim of this study is to compare in cores of needle biopsies of patients showing prostate cancer the topographic relation of inflammatory atro- 355
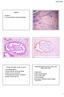
2 phy and atrophy with no inflammation to adenocarcinoma. MATERIALS AND METHODS The material of this retrospective study was obtained from 172 consecutive men with cancer on needle prostate biopsies and subsequently submitted to radical retropubic prostatectomy. Both partial and complete prostatic atrophy were considered. Partial prostatic atrophy was diagnosed according to criteria described by Oppenheimer et al. (11) and complete atrophy by criteria described by Billis (4). Three histological subtypes were identified: simple atrophy, hyperplastic atrophy (or postatrophic hyperplasia) (Figure-1), and sclerotic atrophy. Elastosis of the stroma was a useful microscopic feature for the identification of prostatic atrophy of any subtype (12). Inflammatory atrophy (prostatic atrophy with inflammation) - Both inactive and active inflammation were considered. Inflammatory infiltrate with lymphocytes, plasmacytes or macrophages was considered inactive. The infiltrate was considered active whenever neutrophils were seen in the stroma. All grades of inflammation were considered according to a modified consensus development of a histopathological classification system for chronic prostatic inflammation (13): mild (scattered individual inflammatory cells), moderate (clusters of inflammatory cells) and severe (confluent sheets of inflammatory cells) in areas of prostatic atrophy of any kind: simple, hyperplastic (Figure-2) or sclerotic. According to the pathologic findings, patients were stratified into group A (biopsies with atrophy and no inflammation), and group B (biopsies with inflammatory atrophy). The frequency of atrophy was evaluated considering all cores of the biopsy as well as only the cores showing adenocarcinoma. Extent of inflammatory atrophy and atrophy with no inflammation was evaluated according to the number of cores showing the lesion. In group B, we counted the cores showing only inflammatory atrophy, cores showing atrophy and no inflammation, and cores showing both lesions. In cores showing both inflammatory atrophy and atrophy with no inflammation, the foci of each lesion were counted using an image analyzer (ImageLab-2000). The clinicopathological features included age of the patients, preoperative PSA, and biopsy Gleason score. The data were analyzed using the Mann- Whitney test for comparison of continuous variables Figure 1 Atrophy with no inflammation, hyperplastic subtype (HE, X100). Figure 2 Inflammatory atrophy, hyperplastic subtype (HE, X200). 356
3 with P < 0.05 being considered statistically significant. All statistical analyses were performed using Statistica 5.5 (StatSoft, Inc., Tulsa, OK, USA). RESULTS A total of 1,088 cores (mean, median and range 6.32, 6 and 1-13, respectively) were obtained from 172 needle biopsies of patients with prostate cancer. Considering all cores of the biopsy, atrophy was seen in 144/172 (83.72%) biopsies; 72/144 (50%) biopsies showed atrophy with no inflammation and 72/ 144 (50%) biopsies showed inflammatory atrophy. In 57/72 (79.16%) biopsies with inflammatory atrophy inflammation was inactive, and in 15/72 (20.83%) biopsies inflammation was active. Considering only cores showing adenocarcinoma, atrophy was seen in 116/172 (67.44%) biopsies; 70/116 (60.34%) biopsies showed atrophy with no inflammation and 46/116 (39.66%) biopsies showed inflammatory atrophy (Table-1). There was a total of 481 cores in the 72 biopsies with inflammatory atrophy; 184/481 (38.25%) cores showed no atrophy; 166/481 (34.51%) cores showed atrophy and no inflammation; 111/481 (23.08%) cores showed both lesions; and, 20/481 (4.16%) cores showed only inflammatory atrophy (Table-2). In the cores showing both lesions, inflammatory atrophy was seen in 193/398 (48.49%) foci, and atrophy with no inflammation was seen in 205/ 398 (51.51%) foci. Table-3 shows the clinicopathologic features by groups A and B according to age, preoperative PSA and biopsy Gleason score. There was no statistically significant difference between patients showing atrophy and no inflammation (group A) and patients showing inflammatory atrophy (group B). COMMENTS Prostatic atrophy is one of the most frequent mimics of prostatic adenocarcinoma (14). It occurs most frequently in the posterior lobe or peripheral zone (15) and gained importance with the increasing use of needle biopsies for the detection of prostatic carcinoma (16). The frequency of the lesion in autopsies is 85% and increases with age (4). The etiopathogenesis of prostatic atrophy is unknown. Compression due to hyperplastic nodules, inflammation, hormones, nutritional deficiency, systemic or local ischemia, are all factors that may play a role in the pathogenesis of atrophy (4,14,15,17,18). The histologic subtypes of Table 1 Frequency of atrophy in 172 biopsies considering only cores showing adenocarcinoma. Findings N % Biopsies with atrophy (groups A + B) 116/ Biopsies with atrophy and no inflammation (group A) 070/ Biopsies with inflammatory atrophy (group B) 046/ Table 2 Findings in 481 cores from 72 biopsies showing inflammatory atrophy. Findings N % Cores without atrophy 184/ Cores showing atrophy and no inflammation 166/ Cores showing both lesions 111/ Cores showing only inflammatory atrophy 020/
4 Table 3 Clinicopathologic features of 172 patients with prostate cancer in the biopsy by groups A (with atrophy and no inflammation) and B (inflammatory atrophy). Characteristic Group A Group B p Value Age (years) Mean ± SD Median Preoperative PSA (ng/ml) Mean ± SD Median Gleason score Mean ± SD Median ± ± ± ± ± ± ( ) ( ) ( ) SD = standard deviation, = Mann-Whitney test. prostatic atrophy do not represent distinct entities but a morphologic continuum of acinar atrophy. Subtyping atrophy is useful not only for its recognition, and for distinguishing it from prostate cancer (4,16). Chronic inflammation of longstanding duration has been linked to the development of carcinoma in several organ systems (1-3). In the prostate, it is controversial whether there is any relationship of inflammatory atrophy to prostate cancer (4-10). The term proliferative inflammatory atrophy was proposed by De Marzo et al. (5) to designate discrete foci of proliferative glandular epithelium with the morphological appearance of simple atrophy or postatrophic hyperplasia occurring in association with inflammation. According to these authors the morphology of proliferative inflammatory atrophy is consistent with McNeal s description of postinflammatory atrophy (19), with that of chronic prostatitis described by Bennett et al. (20), and with the lesion referred to previously as lymphocytic prostatitis by Blumenfeld et al. (21). De Marzo et al. (5) and Putzi and De Marzo (7) suggest that proliferative atrophy may indeed give rise to carcinoma directly or that proliferative atrophy may lead to carcinoma indirectly via development into HGPIN. This hypothesis by the authors is based on three separate findings providing supportive evidence: 1) A topographical relation with morphologic merging between proliferative inflammatory atrophy and HGPIN in 34% of the inflammatory atrophy lesions; 2) The phenotype of many of the cells in inflammatory atrophy is most consistent with that of an immature secretory-type cell, similar to that for the cells of HGPIN; and 3) proliferative inflammatory atrophy, HGPIN, and carcinoma all occur with high prevalence in the peripheral zone and low prevalence in the central zone of the human prostate. Favoring a link of inflammation to prostate adenocarcinoma, Cohen et al. (22) found a positive association between Propionibacterium acnes and prostatic inflammation, which may be implicated in the development of prostate cancer. However, the authors comment that it is possible that prostatic inflammation may also be caused by other microorganisms which could not be identified by the study, for example obligate anerobes or species which are difficult to culture under laboratory conditions. They also comment on a second important limitation of the study related to the lack of appropriate negative controls such as prostate tissue from patients without inflammation, atrophy and cancer. Other studies are at odds with the findings of De Marzo et al. (5) and Putzi and De Marzo (7). In 100 consecutively autopsied men more than 40 years of age, Billis (4) studied the etiopathogenesis of atrophy and its possible potential as a precancerous lesion. There was no statistically significant relation of atrophy to histologic (incidental) carcinoma or HGPIN. The author concluded that prostatic atrophy probably is not a premalignant lesion. In this autopsy study, prevalence of atrophy increased with age and chronic 358
5 ischemia caused by local intense arteriosclerosis seemed to be a potential factor for its pathogenesis. In a subsequent study, Billis and Magna (9) stratified the 100 prostates into group A (atrophy without inflammation) and group B (inflammatory atrophy). The groups were correlated to age, race, histologic (incidental) carcinoma, HGPIN, and extent of both these latter lesions. There was no statistically significant difference between groups A and B for all the variables studied. Neither a topographical relation nor a morphologic transition was seen between prostatic atrophy and histologic carcinoma or HGPIN. The authors concluded that inflammatory atrophy does not appear to be associated with cancer or HGPIN. Anton et al. (6) studying 272 radical prostatectomies and 44 cystoprostatectomies concluded that postatrophic hyperplasia is a relatively common lesion present in about one-third of prostates, either with or without prostate carcinoma. The authors found no association between the presence of postatrophic hyperplasia and the likelihood of cancer and no topographic association between postatrophic hyperplasia and prostate carcinoma foci. Bakshi et al. (8) studied 79 consecutive prostate biopsies: 54% of initial biopsies were benign, 42% of the cases showed cancer, and 4% HGPIN or atypia. Postatrophic hyperplasia was seen in 17% of benign initial biopsies with available follow-up. Of these, 75% had associated inflammation. There was no significant difference in the subsequent diagnosis of prostate cancer for groups with postatrophic hyperplasia, partial atrophy, atrophy, or no specific abnormality. The authors concluded that the subcategories of atrophy do not appear to be associated with a significant increase in the risk of diagnosis of prostate cancer subsequently. Postma et al. (10) evaluated whether the incidence of atrophy reported on sextant biopsies is associated with subsequent prostate cancer detection. The authors concluded that atrophy is a very common lesion in prostate biopsy cores (94%). Atrophy in an asymptomatic population undergoing screening was not associated with a greater prostate cancer or HGPIN incidence during subsequent screening rounds. In the present study, from a total of 172 needle biopsies of men with prostate cancer, 144/172 showed atrophy; 72/144 (50%) biopsies showed atrophy and no inflammation and 72/144 (50%) biopsies showed inflammatory atrophy. However, considering only cores with cancer, atrophy was seen in 116/172 (67.44%) biopsies; 70/116 (60.34%) biopsies showed atrophy and no inflammation and 46/116 (39.66%) biopsies showed inflammatory atrophy. This finding seems to contradict the topographical model by De Marzo et al. (5) whereby inflammatory atrophy may progress directly to adenocarcinoma or indirectly via development to HGPIN. In cores with adenocarcinoma it would be expected a higher frequency of inflammatory atrophy. Another relevant finding in our study was the evaluation of the extension of inflammatory atrophy in the 481 cores of the 72 biopsies showing this lesion. In only 20/481 (4.16%) cores inflammatory atrophy was the only lesion present. Most frequently cores showed either atrophy with no inflammation (166/481, 34.51%) or both lesions (111/ 481, 23.08%). A criticism to our findings is that a thin prostate needle biopsy may not represent a real topographic relation between lesions if compared to findings in large specimens such as radical prostatectomy or autopsy prostates. In the study on autopsies with step-sectioning of the prostate, a topographic relation of inflammatory atrophy and HGPIN and/or histologic adenocarcinoma was also not found (9). There was no statistically significant difference for age (P = ), preoperative PSA (P = ), and Gleason score in the biopsy (P = ) between patients with atrophy and no inflammation and patients with inflammatory atrophy probably indicating no difference in temporal onset and aggressiveness of the tumor in this two groups. CONCLUSION The result of our study seems not to favor the model of prostatic carcinogenesis in which there is a topographical relation of inflammatory atrophy to adenocarcinoma. In cores with adenocarcinoma, atrophy with no inflammation was more frequently seen than inflammatory atrophy, and in biopsies with inflammatory atrophy, only 4.16% of the cores showed this lesion as the only finding. 359
6 CONFLICT OF INTEREST REFERENCES None declared. 1. Ames BN: Mutagenesis and carcinogenesis: endogenous and exogenous factors. Environ Mol Mutagen. 1989; 14: Weitzman SA, Gordon LI: Inflammation and cancer: role of phagocyte-generated oxidants in carcinogenesis. Blood. 1990; 76: Bartsch H, Frank N: Blocking the endogenous formation of N-nitroso compounds and related carcinogens. IARC Sci Publ. 1996; 139: Billis A: Prostatic atrophy: an autopsy study of a histologic mimic of adenocarcinoma. Mod Pathol. 1998; 11: De Marzo AM, Marchi VL, Epstein JI, Nelson WG: Proliferative inflammatory atrophy of the prostate: implications for prostatic carcinogenesis. Am J Pathol. 1999; 155: Anton RC, Kattan MW, Chakraborty S, Wheeler TM: Postatrophic hyperplasia of the prostate: lack of association with prostate cancer. Am J Surg Pathol. 1999; 23: Putzi MJ, De Marzo AM: Morphologic transitions between proliferative inflammatory atrophy and highgrade prostatic intraepithelial neoplasia. Urology. 2000; 56: Bakshi NA, Pandya S, Schervish EW, Wojno KJ: Morphologic features and clinical significance of post-atrophic hyperplasia in biopsy specimens of prostate. Mod Pathol. 2002; 15: 154A. 9. Billis A, Magna LA: Inflammatory atrophy of the prostate. Prevalence and significance. Arch Pathol Lab Med. 2003; 127: Postma R, Schroder FH, van der Kwast TH: Atrophy in prostate needle biopsy cores and its relationship to prostate cancer incidence in screened men. Urology. 2005; 65: Oppenheimer JR, Wills ML, Epstein JI: Partial atrophy in prostate needle cores: another diagnostic pitfall for the surgical pathologist. Am J Surg Pathol. 1998; 22: Billis A, Magna LA: Prostate elastosis: a microscopic feature useful for the diagnosis of postatrophic hyperplasia. Arch Pathol Lab Med. 2000; 124: Nickel JC, True LD, Krieger JN, Berger RE, Boag AH, Young ID: Consensus development of a histopathological classification system for chronic prostatic inflammation. BJU Int. 2001; 87: Srigley JR: Benign mimickers of prostatic adenocarcinoma. Mod Pathol. 2004; 17: Liavag I: Atrophy and regeneration in the pathogenesis of prostatic carcinoma. Acta Pathol Microbiol Scand. 1968; 73: Cheville JC, Bostwick DG: Postatrophic hyperplasia of the prostate. A histologic mimic of prostatic adenocarcinoma. Am J Surg Pathol. 1995; 19: Rich AR: On the frequency of occurrence of occult carcinoma of the prostate. J Urol.1935; 33: Ro JY, Sahin AA, Ayala AG. Tumors and tumorous conditions of the male genital tract. In: Fletcher CDM (eds.), Diagnostic Histopathology of Tumors. New York, Churchill Livingstone. 1995; pp McNeal JE: Prostate. In: Sternberg SS (ed.), Histology for Pathologists. second edition. Philadelphia, Lippincott-Raven. 1997; pp Bennett BD, Richardson PH, Gardner WA Jr. Histopathology and cytology of prostatitis. In: Lepor H, Lawson RK (eds.), Prostate Diseases. Philadelphia, WB Saunders Co. 1993; pp Blumenfeld W, Tucci S, Narayan P: Incidental lymphocytic prostatitis. Selective involvement with nonmalignant glands. Am J Surg Pathol. 1992; 16: Cohen RJ, Shannon BA, McNeal JE, Shannon T, Garrett KL: Propionibacterium acnes associated with inflammation in radical prostatectomy specimens: a possible link to cancer evolution? J Urol. 2005; 173: Correspondence address: Dr. Athanase Billis Dep. de Anatomia Patologica Fac. de Ciências Médicas - UNICAMP Caixa Postal 6111 Campinas, SP, , Brazil athanase@fcm.unicamp.br Accepted after revision: December 30,
7 EDITORIAL COMMENT High-grade prostatic intraepithelial neoplasia (HGPIN) is the most likely precursor of prostatic adenocarcinoma, according to virtually all available evidence. There are other possible findings in the prostate that may be premalignant (Low-grade PIN, inflammatory atrophy, malignancy-associated foci, and atypical adenomatous hyperplasia), but the data for them are much less convincing than that for HGPIN (1). The paper by Athanase Billis and collaborators entitled Inflammatory Atrophy on Prostate Needle Biopsies: Is There Topographic Relationship to Cancer? deals with the interesting topic of preneoplastic lesions and conditions of the prostate, in particular with proliferative inflammatory atrophy (2). The objective of their study was to compare on needle prostate biopsies of patients showing cancer the topographical relation of inflammatory atrophy and atrophy with no inflammation to adenocarcinoma. The result of their study did not favor the model of prostatic carcinogenesis in which there is a topographical relation of inflammatory atrophy to adenocarcinoma. Dr Billis study does not exclude that inflammatory atrophy could be an early step in the development of prostate cancer and one of the possible preneoplastic conditions and lesions that precede the appearance of cancer. Low-grade PIN (LGPIN) - Earlier morphometric and immunohistochemical studies showed that LGPIN has features that are intermediate between normal tissue and HGPIN (1). Little information on LGPIN has been accumulated in recent times. This is probably due to the fact, while HGPIN in needle biopsy tissue is a risk factor for the subsequent detection of carcinoma, LGPIN is not. Currently, LGPIN is not documented in pathology reports due a relatively low risk of cancer following re-biopsy. In Bostwick s progression model of PIN to carcinoma, the transition between normal, low-grade PIN, high-grade PIN, and then carcinoma is continuous (3). Few epidemiologic, morphologic, or molecular genetic studies have examined the relation between low and high-grade PIN development. In part, this relates to the difficulty in distinguishing low-grade PIN from normal tissue on the one hand and high-grade PIN on the other. Nevertheless, Putzi and De Marzo (4) found that lesions that could be considered lowgrade PIN often coexisted with high-grade PIN, suggesting either that high-grade PIN is derived from lowgrade PIN or that high and low grade PIN arise concomitantly. Focal Prostate Atrophy as a Morphological Manifestation of a Field Effect and a Potential Prostate Cancer Precursor - Pathologists have long recognized focal areas of epithelial atrophy in the prostate that appear more commonly in the peripheral zone of the prostate. These lesions may be associated with chronic inflammation, and less commonly with acute inflammation (5). The term proliferative inflammatory atrophy (PIA) has been proposed (5). Many of the atrophic cells are not quiescent and possess a phenotype that is intermediate between basal and luminal cells. Intermediate epithelial cells have been postulated to be the targets of neoplastic transformation in the prostate (6). Additionally, PIA cells show elevated levels of GSTP1, glutathione S transferase alpha (GSTA1) and COX-2 in many cells, suggesting that these cells are responding to increased oxidant/nitrosative/electrophilic stress. Many of the molecular and genetic changes seen in HGPIN and cancer have also been documented in PIA (7). In morphological studies, it has been observed frequent merging of areas of focal atrophy directly with high grade PIN (7). It has been observed these atrophic lesions near early carcinoma lesions, at times with direct merging between atrophic epithelium in PIA and adenocarcinoma (7). Some of such changes could be called atrophic HGPIN. Malignancy-associated changes (Putative preneoplastic markers with minimal or no morphological changes) - Malignancy-associated changes refer to molecular abnormalities in the epithelial cells that are not usually distinguishable by routine light microscopic examination. Scant data are available in the prostate. Normal-looking epithelium in prostates with adenocarcinoma may show some molecular abnormalities in GSTP- I and telomerase that are similar to those in cancer (2). These observations are related to the so- 361
8 called enzyme-altered foci as putative preneoplastic markers (8,9). According to Dr TG Pretlow and coworkers, the most abundant of these lesions with molecular alterations show minimal or no morphological changes (8). Changes occur also in the stroma. Montironi et al (10) have shown that the degree of vascularization in normal-looking prostate tissue from total prostatectomies performed because of a preoperative diagnosis of PCa is close to that of LGPIN. The transition from normal-looking epithelium to prostate cancer without an intermediate morphological stage identifiable as HGPIN was considered possible (8). This raises the question of the existence of PIN without morphological changes as a precursor of some well-differentiated adenocarcinomas of the transition zone. Atypical adenomatous hyperplasia AAH (Adenosis) - Is characterized by a circumscribed proliferation of closely packed small glands that tends to merge with the surrounding, histologically benign glands (11). AAH has been considered a premalignant lesion of the transition zone. A direct transition from AAH to cancer, as it has been observed between HGPIN and cancer, has not been documented. The link between cancer and AAH is probably an epiphenomenon and that the data are insufficient to conclude that AAH is a premalignant lesion. REFERENCES 1. Montironi R, Mazzucchelli R, Algaba F, Lopez-Beltran A: Morphological identification of the patterns of prostatic intraepithelial neoplasia and their significance. J Clin Pathol. 2000; 53: Billis A, Freitas LLL, Magna LA, Ferreira U: Inflammatory Atrophy on Prostate Needle Biopsies: Is There Topographic Relationship to Cancer? Int Braz J Urol (present work). 3. Bostwick DG, Brawer MK: Prostatic intra-epithelial neoplasia and early invasion in prostate cancer. Cancer. 1987; 59: Putzi MJ, De Marzo AM: Morphologic transitions between proliferative inflammatory atrophy and highgrade prostatic intraepithelial neoplasia. Urology, 2000; 56: De Marzo AM, Marchi VL, Epstein JI, Nelson WG: Proliferative inflammatory atrophy of the prostate: implications for prostatic carcinogenesis. Am J Pathol. 1999; 155: van Leenders G, Dijkman H, Hulsbergen-van de Kaa C, Ruiter D, Schalken J: Demonstration of intermediate cells during human prostate epithelial differentiation in situ and in vitro using triple-staining confocal scanning microscopy. Lab Invest. 2000; 80: De Marzo AM, DeWeese TL, Platz EA, Meeker AK, Nakayama M, Epstein JI, Isaacs WB, Nelson WG: Pathological and molecular mechanisms of prostate carcinogenesis: implications for diagnosis, detection, prevention, and treatment. J Cell Biochem. 2004; 91: Montironi R, Thompson D, Bartels PH (1999) Premalignant Lesions of the Prostate. In: Lowe DG, Underwood JCE (Eds), Recent Advances in Histopathology. Orlando, Elsevier, 1999; pp Pretlow TG, Nagabhushan M, Pretlow TP: Prostatic intraepithelial neoplasia and other changes during promotion and progression. Path Res Pract. 1995; 191: Montironi R, Galluzzi CM, Diamanti L, Taborro R, Scarpelli M, Pisani E: Prostatic intra-epithelial neoplasia. Qualitative and quantitative analyses of the blood capillary architecture thin tissue sections. Path Res Pract. 1993; 189: Cheng L, Shan A, Cheville JC, Qian J, Bostwick DG: Atypical adenomatous hyperplasia of the prostate: a premalignant lesion? Cancer Res. 1998; 58: Dr. Rodolfo Montironi Polytechnic University of the Marche Region Institute of Pathological Anatomy School of Medicine, United Hospitals Ancona, Italy r.montironi@univpm.it Dr. Liang Cheng Dept of Pathology & Lab Medicine Indiana University School of Medicine Indianapolis, IN, 46202, USA liang_cheng@yahoo.com 362
9 EDITORIAL COMMENT A hypothesis for prostate carcinogenesis proposes that injury to the prostate from a variety of causes leads to chronic inflammation and proliferative inflammatory atrophy (PIA) which may be a risk factor for prostate cancer. Prostatic glandular atrophy can be diffuse or focal with diffuse atrophy resulting from androgen deprivation. PIA is a type of focal atrophy that occurs in the absence of androgen deprivation and occurs in small or large foci, most commonly in the peripheral zone. Recognized morphological types of PIA include simple atrophy and postatrophic hyperplasia in which chronic inflammation as well as increased proliferative activity has been demonstrated. It is unknown whether the other types of focal atrophy, including simple atrophy with cyst formation and partial atrophy have increased cellular proliferation. Therefore, these lesions are currently not considered PIA. A variety of other carcinomas including those in the liver, stomach, large bowel and urinary bladder appear to be related to long-standing chronic inflammation and proliferation. Prostate cancer and its precursor, high-grade prostatic intraepithelial neoplasia (HGPIN) have has been linked with PIA lesions through topographical and morphological associations. De Marzo et al. (1) have shown frequent morphological transitions between HGPIN and PIA suggesting that PIA may be a highrisk lesion for prostate cancer through HGPIN. Although topographical and morphological associations alone are not proofs of a cancer-causing role for PIA lesions, these support a model of prostatic carcinogenesis in proliferative epithelium in chronic inflammation. The authors studied needle core biopsies of patients with prostate cancer and did not show a topographical relationship of inflammatory atrophy to adenocarcinoma. Other studies have shown similar results with inflammatory atrophy found to be a very common lesion. These findings, while not supporting this model of prostate carcinogenesis, do not rule out this association and ultimately experimental animal studies, epidemiological studies and molecular pathological approaches are needed to clarify this hypothesis. REFERENCE 1. Putzi MJ, De Marzo AM: Morphologic transitions between proliferative inflammatory atrophy and highgrade prostatic intraepithelial neoplasia. Urology. 2000; 56: Dr. H. Samaratunga Department of Anatomical Pathology Sullivan Nicolaides Pathology Royal Brisbane Hospital University of Queensland Brisbane, Queensland, Australia hema_samaratunga@snp.com.au 363
Chronic inflammation of long-standing duration has
 Inflammatory Atrophy of the Prostate Prevalence and Significance Athanase Billis, MD; Luis A. Magna, MD Context. Recently, prostatic atrophy associated with chronic inflammation has been linked to carcinoma
Inflammatory Atrophy of the Prostate Prevalence and Significance Athanase Billis, MD; Luis A. Magna, MD Context. Recently, prostatic atrophy associated with chronic inflammation has been linked to carcinoma
University of Zagreb Medical School Repository
 Središnja medicinska knjižnica Tomas, D., Krušlin, B., Rogatsch, H., Schäfer, G., Belicza, M., Mikuz, G. (00) Different Types of Atrophy in the Prostate With and Without Adenocarcinoma. European Urology,
Središnja medicinska knjižnica Tomas, D., Krušlin, B., Rogatsch, H., Schäfer, G., Belicza, M., Mikuz, G. (00) Different Types of Atrophy in the Prostate With and Without Adenocarcinoma. European Urology,
MORPHOLOGIC TRANSITIONS BETWEEN PROLIFERATIVE INFLAMMATORY ATROPHY AND HIGH-GRADE PROSTATIC INTRAEPITHELIAL NEOPLASIA
 ADULT UROLOGY MORPHOLOGIC TRANSITIONS BETWEEN PROLIFERATIVE INFLAMMATORY ATROPHY AND HIGH-GRADE PROSTATIC INTRAEPITHELIAL NEOPLASIA MATHEW J. PUTZI AND ANGELO M. DE MARZO ABSTRACT Objectives. To validate
ADULT UROLOGY MORPHOLOGIC TRANSITIONS BETWEEN PROLIFERATIVE INFLAMMATORY ATROPHY AND HIGH-GRADE PROSTATIC INTRAEPITHELIAL NEOPLASIA MATHEW J. PUTZI AND ANGELO M. DE MARZO ABSTRACT Objectives. To validate
Are Prostate Carcinoma Clinical Stages T1c and T2 Similar?
 Clinical Urology Are Clinical Stages T1c and T2 Similar? International Braz J Urol Vol. 32 (2): 165-171, March - April, 2006 Are Prostate Carcinoma Clinical Stages T1c and T2 Similar? Athanase Billis,
Clinical Urology Are Clinical Stages T1c and T2 Similar? International Braz J Urol Vol. 32 (2): 165-171, March - April, 2006 Are Prostate Carcinoma Clinical Stages T1c and T2 Similar? Athanase Billis,
Hyperplastic, Premalignant and Malignant Lesions of the Prostate Gland
 Jehoram Tei Anim, md, FRCPath; Sitara Abdul Sathar, MB; Mohammed Ejaz Bhatti, MSc From the Department of Pathology, Faculty of Medicine, Kuwait University, Kuwait. Address reprint requests and correspondence
Jehoram Tei Anim, md, FRCPath; Sitara Abdul Sathar, MB; Mohammed Ejaz Bhatti, MSc From the Department of Pathology, Faculty of Medicine, Kuwait University, Kuwait. Address reprint requests and correspondence
ACCME/Disclosures. Cribriform Lesions of the Prostate. Case
 Cribriform Lesions of the Prostate Ming Zhou, MD, PhD Departments of Pathology and Urology New York University Langone Medical Center New York, NY Ming.Zhou@NYUMC.ORG ACCME/Disclosures The USCAP requires
Cribriform Lesions of the Prostate Ming Zhou, MD, PhD Departments of Pathology and Urology New York University Langone Medical Center New York, NY Ming.Zhou@NYUMC.ORG ACCME/Disclosures The USCAP requires
5/21/2018. Difficulty in Underdiagnosing Prostate Cancer. Diagnosis of Prostate Cancer. Evaluation of Prostate Cancer and Atypical on Needle Biopsy
 Evaluation of Prostate Cancer and Atypical on Needle Biopsy Jonathan I. Epstein Difficulty in Underdiagnosing Prostate Cancer Limited tissue on needle biopsy (1 cm. x
Evaluation of Prostate Cancer and Atypical on Needle Biopsy Jonathan I. Epstein Difficulty in Underdiagnosing Prostate Cancer Limited tissue on needle biopsy (1 cm. x
ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY. Jonathan I. Epstein.
 1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
3/28/2017. Disclosure of Relevant Financial Relationships. GU Evening Subspecialty Case Conference. Differential Diagnosis:
 GU Evening Subspecialty Case Conference Rajal B. Shah, M.D. VP, Medical Director, Urologic Pathology Miraca Life Sciences, Irving, Texas Clinical Associate Professor of Pathology Baylor College of Medicine,
GU Evening Subspecialty Case Conference Rajal B. Shah, M.D. VP, Medical Director, Urologic Pathology Miraca Life Sciences, Irving, Texas Clinical Associate Professor of Pathology Baylor College of Medicine,
STUDY OF PROSTATIC LESION FOR A PERIOD OF FIVE YEARS
 Page222 IJPBS Volume 4 Issue 2 APR-JUN 2014 222-226 Research Article Biological Sciences STUDY OF PROSTATIC LESION FOR A PERIOD OF FIVE YEARS B. Rajashekar Reddy 1, Rameswarapu Suman Babu 1 and Sujatha.P*
Page222 IJPBS Volume 4 Issue 2 APR-JUN 2014 222-226 Research Article Biological Sciences STUDY OF PROSTATIC LESION FOR A PERIOD OF FIVE YEARS B. Rajashekar Reddy 1, Rameswarapu Suman Babu 1 and Sujatha.P*
Although current American Cancer Society guidelines
 ORIGINAL ARTICLE Diffuse Adenosis of the Peripheral Zone in Prostate Needle Biopsy and Prostatectomy Specimens Tamara L. Lotan, MD* and Jonathan I. Epstein, MD*w z Abstract: We have observed a group of
ORIGINAL ARTICLE Diffuse Adenosis of the Peripheral Zone in Prostate Needle Biopsy and Prostatectomy Specimens Tamara L. Lotan, MD* and Jonathan I. Epstein, MD*w z Abstract: We have observed a group of
Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance
 & 2006 USCAP, Inc All rights reserved 0893-3952/06 $30.00 www.modernpathology.org Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance Charles C Guo 1 and
& 2006 USCAP, Inc All rights reserved 0893-3952/06 $30.00 www.modernpathology.org Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance Charles C Guo 1 and
Diagnosis, pathology and prognosis including variant pathology
 PROSTATE CANCER Diagnosis, pathology and prognosis including variant pathology No Conflict of Interest Universitat Autónoma de Barcelona F.Algaba Section of Pathology PROSTATE CANCER Diagnosis, pathology
PROSTATE CANCER Diagnosis, pathology and prognosis including variant pathology No Conflict of Interest Universitat Autónoma de Barcelona F.Algaba Section of Pathology PROSTATE CANCER Diagnosis, pathology
2016 WHO CLASSIFICATION OF TUMOURS OF THE PROSTATE. Peter A. Humphrey, MD, PhD Yale University School of Medicine New Haven, CT
 2016 WHO CLASSIFICATION OF TUMOURS OF THE PROSTATE Peter A. Humphrey, MD, PhD Yale University School of Medicine New Haven, CT 2016 WHO CLASSIFICATION OF TUMOURS OF THE PROSTATE AUTHORS : PROSTATE CHAPTER
2016 WHO CLASSIFICATION OF TUMOURS OF THE PROSTATE Peter A. Humphrey, MD, PhD Yale University School of Medicine New Haven, CT 2016 WHO CLASSIFICATION OF TUMOURS OF THE PROSTATE AUTHORS : PROSTATE CHAPTER
Although partial atrophy is one of the most common
 ORIGINAL ARTICLE Partial Atrophy on Prostate Needle Biopsy Cores: A Morphologic and Immunohistochemical Study Wenle Wang, MD, PhD,* Xinlai Sun, MD,w and Jonathan I. Epstein, MD*zy Abstract: Partial atrophy
ORIGINAL ARTICLE Partial Atrophy on Prostate Needle Biopsy Cores: A Morphologic and Immunohistochemical Study Wenle Wang, MD, PhD,* Xinlai Sun, MD,w and Jonathan I. Epstein, MD*zy Abstract: Partial atrophy
PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA AND IMPORTANT MIMICKERS PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA
 PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA AND IMPORTANT MIMICKERS PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA 1 A good H & E helps! ADENOCARCINOMA DIAGNOSTIC CRITERIA Relatively uniform proliferation
PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA AND IMPORTANT MIMICKERS PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA 1 A good H & E helps! ADENOCARCINOMA DIAGNOSTIC CRITERIA Relatively uniform proliferation
Study of High Grade Prostatic Intraepithelial Neoplasia for a Period of Five Years B. Rajashekar Reddy 1, Rameswarapu Suman Babu 2 and P.
 Indian Journal of Mednodent and Allied Sciences Vol. 2, No. 2, June-July, 2014, pp- 149-154 DOI : 10.5958/2347-6206.2014.00004.1 Original Research Study of High Grade Prostatic Intraepithelial Neoplasia
Indian Journal of Mednodent and Allied Sciences Vol. 2, No. 2, June-July, 2014, pp- 149-154 DOI : 10.5958/2347-6206.2014.00004.1 Original Research Study of High Grade Prostatic Intraepithelial Neoplasia
Pathology of the Prostate. PathoBasic Tatjana Vlajnic
 Pathology of the Prostate PathoBasic 24.01.17 Tatjana Vlajnic Overview Adenocarcinoma of the prostate Grading Special variants Mimickers of prostate adenocarcinoma Atrophy Inflammatory conditions Granulomatous
Pathology of the Prostate PathoBasic 24.01.17 Tatjana Vlajnic Overview Adenocarcinoma of the prostate Grading Special variants Mimickers of prostate adenocarcinoma Atrophy Inflammatory conditions Granulomatous
Prostate Pathology: Prostate Carcinoma, variants and Gleason Grading (Part 1)
 Prostate Pathology: Prostate Carcinoma, variants and Gleason Grading (Part 1) Jae Y. Ro, MD, PhD June 7, 2012 Ten Leading Cancer Types for the Estimated New Cancer Cases and Deaths By Sex, United States,
Prostate Pathology: Prostate Carcinoma, variants and Gleason Grading (Part 1) Jae Y. Ro, MD, PhD June 7, 2012 Ten Leading Cancer Types for the Estimated New Cancer Cases and Deaths By Sex, United States,
Macro- and microacinar proliferations of the prostate
 Macro- and microacinar proliferations of the prostate (with emphasis on cancer mimics) Rodolfo Montironi, MD (IT), FRCPath (UK), IFCAP (USA) Polytechnic University of Marche Region (Ancona) School of Medicine,
Macro- and microacinar proliferations of the prostate (with emphasis on cancer mimics) Rodolfo Montironi, MD (IT), FRCPath (UK), IFCAP (USA) Polytechnic University of Marche Region (Ancona) School of Medicine,
Division of Oncology, S Orsola-Malpighi Hospital, Bologna, Italy. Department of Surgery, Cordoba University Medical School, Cordoba, Spain
 Prostate cancer glands with cribriform architecture and with glomeruloid features should be considered as Gleason pattern 4 and not pattern 3 Daniele Minardi,1, Roberta Mazzucchelli,, Marina Scarpelli,
Prostate cancer glands with cribriform architecture and with glomeruloid features should be considered as Gleason pattern 4 and not pattern 3 Daniele Minardi,1, Roberta Mazzucchelli,, Marina Scarpelli,
ROLE OF PROSTATIC BASAL CELL MARKER IN DIAGNOSIS OF PROSTATIC LESIONS
 Original Research Article Pathology International Journal of Pharma and Bio Sciences ISSN 0975-6299 ROLE OF PROSTATIC BASAL CELL MARKER IN DIAGNOSIS OF PROSTATIC LESIONS SUBATHRA K* Department of pathology,
Original Research Article Pathology International Journal of Pharma and Bio Sciences ISSN 0975-6299 ROLE OF PROSTATIC BASAL CELL MARKER IN DIAGNOSIS OF PROSTATIC LESIONS SUBATHRA K* Department of pathology,
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017
 Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
INTRADUCTAL LESIONS OF THE PROSTATE. Jonathan I. Epstein
 INTRADUCTAL LESIONS OF THE PROSTATE Jonathan I. Epstein Topics Prostatic intraepithelial neoplasia (PIN) Intraductal adenocarcinoma (IDC-P) Intraductal urothelial carcinoma Ductal adenocarcinoma High Prostatic
INTRADUCTAL LESIONS OF THE PROSTATE Jonathan I. Epstein Topics Prostatic intraepithelial neoplasia (PIN) Intraductal adenocarcinoma (IDC-P) Intraductal urothelial carcinoma Ductal adenocarcinoma High Prostatic
According to the original drawing of D. F. Gleason,
 ORIGINAL ARTICLE Grading of Invasive Cribriform Carcinoma on Prostate Needle Biopsy An Interobserver Study among Experts in Genitourinary Pathology Mathieu Latour, MD,* Mahul B. Amin, MD,y Athanase Billis
ORIGINAL ARTICLE Grading of Invasive Cribriform Carcinoma on Prostate Needle Biopsy An Interobserver Study among Experts in Genitourinary Pathology Mathieu Latour, MD,* Mahul B. Amin, MD,y Athanase Billis
Introduction. Key Words: high-grade prostatic intraepithelial neoplasia, HGPIN, radical prostatectomy, prostate biopsy, insignificant prostate cancer
 Prostate cancer after initial high-grade prostatic intraepithelial neoplasia and benign prostate biopsy Premal Patel, MD, 1 Jasmir G. Nayak, MD, 1,2 Zlatica Biljetina, MD, 4 Bryan Donnelly, MD 3, Kiril
Prostate cancer after initial high-grade prostatic intraepithelial neoplasia and benign prostate biopsy Premal Patel, MD, 1 Jasmir G. Nayak, MD, 1,2 Zlatica Biljetina, MD, 4 Bryan Donnelly, MD 3, Kiril
Prostatic ductal adenocarcinoma is a subtype of
 ORIGINAL ARTICLE High-grade Prostatic Intraepithelial Neoplasialike Ductal Adenocarcinoma of the Prostate: A Clinicopathologic Study of 28 Cases Fabio Tavora, MD* and Jonathan I. Epstein, MD*w z Abstract:
ORIGINAL ARTICLE High-grade Prostatic Intraepithelial Neoplasialike Ductal Adenocarcinoma of the Prostate: A Clinicopathologic Study of 28 Cases Fabio Tavora, MD* and Jonathan I. Epstein, MD*w z Abstract:
Internationally indexed journal
 www.ijpbs.net Internationally indexed journal Indexed in Chemical Abstract Services (USA), Index coppernicus, Ulrichs Directory of Periodicals, Google scholar, CABI,DOAJ, PSOAR, EBSCO, Open J gate, Proquest,
www.ijpbs.net Internationally indexed journal Indexed in Chemical Abstract Services (USA), Index coppernicus, Ulrichs Directory of Periodicals, Google scholar, CABI,DOAJ, PSOAR, EBSCO, Open J gate, Proquest,
ISPUB.COM. Interpretation Of Prostatic Biopsies: A Review. A Chitale, S Khubchandani INTRODUCTION NON-NEOPLASTIC LESIONS GRADING: GLEASON'S SCORE
 ISPUB.COM The Internet Journal of Urology Volume 3 Number 1 A Chitale, S Khubchandani Citation A Chitale, S Khubchandani.. The Internet Journal of Urology. 2004 Volume 3 Number 1. Abstract The incidence
ISPUB.COM The Internet Journal of Urology Volume 3 Number 1 A Chitale, S Khubchandani Citation A Chitale, S Khubchandani.. The Internet Journal of Urology. 2004 Volume 3 Number 1. Abstract The incidence
Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of
 Tiền liệt tuyến Tiền liệt tuyến Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of solid and microcystic areas.
Tiền liệt tuyến Tiền liệt tuyến Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of solid and microcystic areas.
They Do Look Alike : Mimics of Prostate Cancer in Biopsy Samples
 They Do Look Alike : in Biopsy Samples Gladell P. Paner, MD Departments of Pathology and Surgery (Urology) University of Chicago, IL USA Gladell.paner@uchospitals.edu Benign in Needle Biopsy 1. Benign
They Do Look Alike : in Biopsy Samples Gladell P. Paner, MD Departments of Pathology and Surgery (Urology) University of Chicago, IL USA Gladell.paner@uchospitals.edu Benign in Needle Biopsy 1. Benign
Original Article. Premalignant Lesions of Prostate and Its Association with Nodular Hyperplasia and Carcinoma of Prostate: A Histomorphological Study
 Original Article Premalignant Lesions of Prostate and Its Association with Nodular Hyperplasia and Carcinoma of Prostate: A Histomorphological Study Rajeshwari K 1 *, Karibasappa GN 2, N. V. Dravid 1,
Original Article Premalignant Lesions of Prostate and Its Association with Nodular Hyperplasia and Carcinoma of Prostate: A Histomorphological Study Rajeshwari K 1 *, Karibasappa GN 2, N. V. Dravid 1,
Influence of Focal and Diffuse Extraprostatic Extension and Positive Surgical Margins on Biochemical Progression Following Radical Prostatectomy
 ORIGINAL ARTICLE Vol. 38 (2): 175-184; March - April, 2012 Influence of Focal and Diffuse Extraprostatic Extension and Positive Surgical Margins on Biochemical Progression Following Radical Prostatectomy
ORIGINAL ARTICLE Vol. 38 (2): 175-184; March - April, 2012 Influence of Focal and Diffuse Extraprostatic Extension and Positive Surgical Margins on Biochemical Progression Following Radical Prostatectomy
Prostate Overview Quiz
 Prostate Overview Quiz 1. The path report reads: Gleason 3 + 4 = 7. The Gleason s score is a. 3 b. 4 c. 7 d. None of the above 2. The path report reads: Moderately differentiated adenocarcinoma of the
Prostate Overview Quiz 1. The path report reads: Gleason 3 + 4 = 7. The Gleason s score is a. 3 b. 4 c. 7 d. None of the above 2. The path report reads: Moderately differentiated adenocarcinoma of the
PSA. HMCK, p63, Racemase. HMCK, p63, Racemase
 Case 1 67 year old male presented with gross hematuria H/o acute prostatitis & BPH Urethroscopy: small, polypoid growth with a broad base emanating from the left side of the verumontanum Serum PSA :7 ng/ml
Case 1 67 year old male presented with gross hematuria H/o acute prostatitis & BPH Urethroscopy: small, polypoid growth with a broad base emanating from the left side of the verumontanum Serum PSA :7 ng/ml
Grading Prostate Cancer: Recent Changes and Refinements
 USPSTF: 2012 Report on serum PSA Screening Recommendation rating of D Reduced screening, Reduced biopsies, reduced incidence Refinements currently occurring in 2017. WHY? Grading Prostate Cancer: Recent
USPSTF: 2012 Report on serum PSA Screening Recommendation rating of D Reduced screening, Reduced biopsies, reduced incidence Refinements currently occurring in 2017. WHY? Grading Prostate Cancer: Recent
Morphological identification of the patterns of prostatic intraepithelial neoplasia and their importance
 J Clin Pathol 2000;53:655 665 655 Institute of Pathological Anatomy and Histopathology, University of Ancona, Ospedale Regionale, I-60020 Torrette, Ancona, Italy R Montironi R Mazzucchelli Institute of
J Clin Pathol 2000;53:655 665 655 Institute of Pathological Anatomy and Histopathology, University of Ancona, Ospedale Regionale, I-60020 Torrette, Ancona, Italy R Montironi R Mazzucchelli Institute of
Original Article INTRODUCTION. Abstract
 Original Article DOI: 10.17354/ijss/2016/72 Prevalence of Prostatic Intraepithelial Neoplasia in Patients Diagnosed as Benign Prostatic Hyperplasia Underwent Transurethral Resection of the Prostate at
Original Article DOI: 10.17354/ijss/2016/72 Prevalence of Prostatic Intraepithelial Neoplasia in Patients Diagnosed as Benign Prostatic Hyperplasia Underwent Transurethral Resection of the Prostate at
OMPRN Pathology Matters Meeting 2017
 OMPRN Pathology Matters Meeting 2017 Pathology of Aggressive Prostate Cancer Intraductal Carcinoma and Cribriform Carcinoma Dr. Michelle Downes, Staff Urologic Pathologist Sunnybrook Health Sciences Centre,
OMPRN Pathology Matters Meeting 2017 Pathology of Aggressive Prostate Cancer Intraductal Carcinoma and Cribriform Carcinoma Dr. Michelle Downes, Staff Urologic Pathologist Sunnybrook Health Sciences Centre,
European Urology 43 (2003) 164±175
 European Urology European Urology 43 (2003) 164±175 Distribution of Inflammation, Pre-Malignant Lesions, Incidental Carcinoma in Histologically Confirmed Benign Prostatic Hyperplasia: A Retrospective Analysis
European Urology European Urology 43 (2003) 164±175 Distribution of Inflammation, Pre-Malignant Lesions, Incidental Carcinoma in Histologically Confirmed Benign Prostatic Hyperplasia: A Retrospective Analysis
Clinicopathological Study of Associated Lesions in Benign Prostatic Hyperplasia and Prostatic Adenocarcinoma in Surgical Biopsy Specimens
 Original Article DOI: 10.21276/APALM.1608 Clinicopathological Study of Associated Lesions in Benign Prostatic Hyperplasia and Prostatic Adenocarcinoma in Surgical Biopsy Specimens Esakki Muthuvel, Vimal
Original Article DOI: 10.21276/APALM.1608 Clinicopathological Study of Associated Lesions in Benign Prostatic Hyperplasia and Prostatic Adenocarcinoma in Surgical Biopsy Specimens Esakki Muthuvel, Vimal
Coordinate Expression of Cytokeratins 7 and 20 in Prostate Adenocarcinoma and Bladder Urothelial Carcinoma
 Anatomic Pathology / CYTOKERATINS 7 AND 20 IN PROSTATE AND BLADDER CARCINOMAS Coordinate Expression of Cytokeratins 7 and 20 in Prostate Adenocarcinoma and Bladder Urothelial Carcinoma Nader H. Bassily,
Anatomic Pathology / CYTOKERATINS 7 AND 20 IN PROSTATE AND BLADDER CARCINOMAS Coordinate Expression of Cytokeratins 7 and 20 in Prostate Adenocarcinoma and Bladder Urothelial Carcinoma Nader H. Bassily,
, De La Taille Alexandre * INSERM : U955, Universit é Paris XII Val de Marne, IFR10, FR. , Universit é Paris XII Val de Marne, Créteil,FR
 High-grade prostatic intraepithelial neoplasia and atypical small acinar proliferation on initial 21-core extended biopsy scheme: incidence and implications for patient care and surveillance Ploussard
High-grade prostatic intraepithelial neoplasia and atypical small acinar proliferation on initial 21-core extended biopsy scheme: incidence and implications for patient care and surveillance Ploussard
Patient identifiers Date of request Accession/Laboratory number. CLINICAL STAGE (Note 3)
 Prostate Core Needle Biopsy Histopathology Reporting Guide Part 1 - Clinical Information/Specimen Receipt Family/Last name Given name(s) Date of birth DD MM YYYY Patient identifiers Date of request Accession/Laboratory
Prostate Core Needle Biopsy Histopathology Reporting Guide Part 1 - Clinical Information/Specimen Receipt Family/Last name Given name(s) Date of birth DD MM YYYY Patient identifiers Date of request Accession/Laboratory
Some prostatic diseases
 Some prostatic diseases Benign Prostatic Hyperplasia (Nodular Hyperplasia) Extremely common Present in a significant number of men by the age of 40 & its frequency rises progressively with age, reaching
Some prostatic diseases Benign Prostatic Hyperplasia (Nodular Hyperplasia) Extremely common Present in a significant number of men by the age of 40 & its frequency rises progressively with age, reaching
Prostate Immunohistochemistry. Literature Interpretation: Caveats. Must be aware of staining pattern of antibody in the relevant tissue
 IHC Interpretation: General Principles (1) Prostate Immunohistochemistry Murali Varma Cardiff, UK wptmv@cf.ac.uk Sarajevo Nov 2013 Must be aware of staining pattern of antibody in the relevant tissue Nuclear/cytoplasmic/membranous
IHC Interpretation: General Principles (1) Prostate Immunohistochemistry Murali Varma Cardiff, UK wptmv@cf.ac.uk Sarajevo Nov 2013 Must be aware of staining pattern of antibody in the relevant tissue Nuclear/cytoplasmic/membranous
Cairo University. Journal of the Egyptian National Cancer Institute.
 Journal of the Egyptian National Cancer Institute (2014) 26, 15 22 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com Full Length Article Basal cell
Journal of the Egyptian National Cancer Institute (2014) 26, 15 22 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com Full Length Article Basal cell
Original Article - Urological Oncology. Ho Gyun Park 1, Oh Seok Ko 1, Young Gon Kim 1, Jong Kwan Park 1-4
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.4.249 Original Article - Urological Oncology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.4.249&domain=pdf&date_stamp=2014-04-17
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.4.249 Original Article - Urological Oncology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.4.249&domain=pdf&date_stamp=2014-04-17
Anatomic distribution and pathologic characterization of small-volume prostate cancer (o0.5 ml) in whole-mount prostatectomy specimens
 & 2005 USCAP, Inc All rights reserved 0893-3952/05 $30.00 www.modernpathology.org Anatomic distribution and pathologic characterization of small-volume prostate cancer (o0.5 ml) in whole-mount prostatectomy
& 2005 USCAP, Inc All rights reserved 0893-3952/05 $30.00 www.modernpathology.org Anatomic distribution and pathologic characterization of small-volume prostate cancer (o0.5 ml) in whole-mount prostatectomy
Premalignant Lesions of Prostate and their Association with Nodular Hyperplasia and Carcinoma Prostate
 Original Article Premalignant Lesions of Prostate and their Association with Nodular Hyperplasia and Carcinoma Prostate Rekhi B, Jaswal TS,* Arora B* Institute of Pathology-ICMR, Safdarjung Hospital, New
Original Article Premalignant Lesions of Prostate and their Association with Nodular Hyperplasia and Carcinoma Prostate Rekhi B, Jaswal TS,* Arora B* Institute of Pathology-ICMR, Safdarjung Hospital, New
Predictive criteria of insignificant prostate cancer: what is the correspondence of linear extent to percentage of cancer in a single core?
 ORIGINAL ARTICLE Vol. 41 (2): 367-372, March - April, 2015 doi: 10.1590/S1677-5538.IBJU.2015.02.26 Predictive criteria of insignificant prostate cancer: what is the correspondence of linear extent to percentage
ORIGINAL ARTICLE Vol. 41 (2): 367-372, March - April, 2015 doi: 10.1590/S1677-5538.IBJU.2015.02.26 Predictive criteria of insignificant prostate cancer: what is the correspondence of linear extent to percentage
1 NORMAL HISTOLOGY AND METAPLASIAS
 1 NORMAL HISTOLOGY AND METAPLASIAS, MD Anatomy and Histology 1 Metaplasias 2 ANATOMY AND HISTOLOGY The female breast is composed of a branching duct system, which begins at the nipple with the major lactiferous
1 NORMAL HISTOLOGY AND METAPLASIAS, MD Anatomy and Histology 1 Metaplasias 2 ANATOMY AND HISTOLOGY The female breast is composed of a branching duct system, which begins at the nipple with the major lactiferous
High-grade prostatic intraepithelial neoplasia is an independent predictor of outcome after radical prostatectomy
 Urological Oncology HGPIN AS AN INDEPENDENT PREDICTOR OF OUTCOME AFTER RP PIERORAZIO et al. High-grade prostatic intraepithelial neoplasia is an independent predictor of outcome after radical prostatectomy
Urological Oncology HGPIN AS AN INDEPENDENT PREDICTOR OF OUTCOME AFTER RP PIERORAZIO et al. High-grade prostatic intraepithelial neoplasia is an independent predictor of outcome after radical prostatectomy
Percentage of Gleason Pattern 4 and 5 Predicts Survival After Radical Prostatectomy
 1967 Percentage of Gleason Pattern 4 and 5 Predicts Survival After Radical Prostatectomy Liang Cheng, MD 1,2 Darrell D. Davidson, MD, PhD 1 Haiqun Lin, MD, PhD 3 Michael O. Koch, MD 2 1 Department of Pathology
1967 Percentage of Gleason Pattern 4 and 5 Predicts Survival After Radical Prostatectomy Liang Cheng, MD 1,2 Darrell D. Davidson, MD, PhD 1 Haiqun Lin, MD, PhD 3 Michael O. Koch, MD 2 1 Department of Pathology
2004 World Health Organization Classification of the Noninvasive Urothelial Neoplasms: Inherent Problems and Clinical Reflections
 european urology supplements 8 (2009) 453 457 available at www.sciencedirect.com journal homepage: www.europeanurology.com 2004 World Health Organization Classification of the Noninvasive Urothelial Neoplasms:
european urology supplements 8 (2009) 453 457 available at www.sciencedirect.com journal homepage: www.europeanurology.com 2004 World Health Organization Classification of the Noninvasive Urothelial Neoplasms:
Prostatic epithelial and luminal area in the transition zone acini: morphometric analysis in normal and hyperplastic human prostate
 Original Article MORPHOMETRY OF TRANSITION ZONE ACINI IN NORMAL PROSTATE and IN BPH M.A. BABINSKI et al. Prostatic epithelial and luminal area in the transition zone acini: morphometric analysis in normal
Original Article MORPHOMETRY OF TRANSITION ZONE ACINI IN NORMAL PROSTATE and IN BPH M.A. BABINSKI et al. Prostatic epithelial and luminal area in the transition zone acini: morphometric analysis in normal
Normal Morphology. Anatomic Considerations. Normal Urothelial Histology and Cytology
 1 Normal Morphology Anatomic Considerations The urinary tract can be divided into three regions: the kidney; the calyces, pelves and ureters (upper collecting system or upper tract); and the bladder and
1 Normal Morphology Anatomic Considerations The urinary tract can be divided into three regions: the kidney; the calyces, pelves and ureters (upper collecting system or upper tract); and the bladder and
Synonyms. Nephrogenic metaplasia Mesonephric adenoma
 Nephrogenic Adenoma Synonyms Nephrogenic metaplasia Mesonephric adenoma Definition Benign epithelial lesion of urinary tract with tubular, glandular, papillary growth pattern Most frequently in the urinary
Nephrogenic Adenoma Synonyms Nephrogenic metaplasia Mesonephric adenoma Definition Benign epithelial lesion of urinary tract with tubular, glandular, papillary growth pattern Most frequently in the urinary
Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ).
 SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
Prostatic stromal hyperplasia with atypia (PSHA) is a
 Prostatic Stromal Hyperplasia With Atypia Follow-up Study of 18 Cases Deloar Hossain, MD, FRCPC; Isabelle Meiers, MD; Junqi Qian, MD; Gregory T. MacLennan, MD; David G. Bostwick, MD, MBA Context. Prostatic
Prostatic Stromal Hyperplasia With Atypia Follow-up Study of 18 Cases Deloar Hossain, MD, FRCPC; Isabelle Meiers, MD; Junqi Qian, MD; Gregory T. MacLennan, MD; David G. Bostwick, MD, MBA Context. Prostatic
Signet-Ring Cell Change in Benign Prostatic Hyperplasia - A Rare Case Report
 Article ID: WMC00688 ISSN 2046-1690 Signet-Ring Cell Change in Benign Prostatic Hyperplasia - A Rare Case Report Author(s):Dr. Pallavi Bhuyan, Dr. Smita Mahapatra, Dr. Sujata Pujari, Dr. Jayasree Rath
Article ID: WMC00688 ISSN 2046-1690 Signet-Ring Cell Change in Benign Prostatic Hyperplasia - A Rare Case Report Author(s):Dr. Pallavi Bhuyan, Dr. Smita Mahapatra, Dr. Sujata Pujari, Dr. Jayasree Rath
Minimal Adenocarcinoma in Prostate Needle Biopsy Tissue
 Anatomic Pathology / MINIMAL PROSTATE CANCER Minimal Adenocarcinoma in Prostate Needle Biopsy Tissue Phataraporn Thorson, MD, and Peter A. Humphrey, MD, PhD Key Words: Prostate; Cancer; Biopsy; Minimal
Anatomic Pathology / MINIMAL PROSTATE CANCER Minimal Adenocarcinoma in Prostate Needle Biopsy Tissue Phataraporn Thorson, MD, and Peter A. Humphrey, MD, PhD Key Words: Prostate; Cancer; Biopsy; Minimal
THE SIGNIFICANCE OF HYPOECHOIC LESION DIRECTED AND TRANSITION ZONE BIOPSIES IN IMPROVING THE DIAGNOSTIC ABILITY IN PROSTATE CANCER
 Clinical Urology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 222-226, May - June, 2001 THE SIGNIFICANCE OF HYPOECHOIC LESION DIRECTED AND TRANSITION ZONE
Clinical Urology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 222-226, May - June, 2001 THE SIGNIFICANCE OF HYPOECHOIC LESION DIRECTED AND TRANSITION ZONE
Prostate Cancer Grading, Staging and Reporting: An Update Cristina Magi-Galluzzi, MD, PhD
 Prostate Cancer Grading, Staging and Reporting: An Update Cristina Magi-Galluzzi, MD, PhD Director, Genitourinary Pathology R.J. Tomsich Pathology & Laboratory Medicine Institute Professor of Pathology,
Prostate Cancer Grading, Staging and Reporting: An Update Cristina Magi-Galluzzi, MD, PhD Director, Genitourinary Pathology R.J. Tomsich Pathology & Laboratory Medicine Institute Professor of Pathology,
Procedures Needle Biopsy Transurethral Prostatic Resection Suprapubic or Retropubic Enucleation (Subtotal Prostatectomy) Radical Prostatectomy
 Prostate Gland Protocol applies to invasive carcinomas of the prostate gland. Protocol web posting date: July 2006 Protocol effective date: April 2007 Based on AJCC/UICC TNM, 6 th edition Procedures Needle
Prostate Gland Protocol applies to invasive carcinomas of the prostate gland. Protocol web posting date: July 2006 Protocol effective date: April 2007 Based on AJCC/UICC TNM, 6 th edition Procedures Needle
Low grade urothelial carcinoma mimicking basal cell hyperplasia and transitional metaplasia in needle prostate biopsy
 ORIGINAL ARTICLE Vol. 42 (2): 247-252, March - April, 2016 doi: 10.1590/S1677-5538.IBJU.2014.0512 Low grade urothelial carcinoma mimicking basal cell hyperplasia and transitional metaplasia in needle prostate
ORIGINAL ARTICLE Vol. 42 (2): 247-252, March - April, 2016 doi: 10.1590/S1677-5538.IBJU.2014.0512 Low grade urothelial carcinoma mimicking basal cell hyperplasia and transitional metaplasia in needle prostate
CASE 4 21/07/2017. Ectopic Prostatic Tissue in Cervix. Female 31. LLETZ for borderline nuclear abnormalities
 Female 31 CASE 4 LLETZ for borderline nuclear abnormalities PSA Ectopic Prostatic Tissue in Cervix AJSP 2006;30;209-215 usually incidental microscopic finding usually in ectocervical stroma? developmental
Female 31 CASE 4 LLETZ for borderline nuclear abnormalities PSA Ectopic Prostatic Tissue in Cervix AJSP 2006;30;209-215 usually incidental microscopic finding usually in ectocervical stroma? developmental
Metachronous anterior urethral metastasis of prostatic ductal adenocarcinoma
 http://dx.doi.org/10.7180/kmj.2016.31.1.66 KMJ Case Report Metachronous anterior urethral metastasis of prostatic ductal adenocarcinoma Jeong Hyun Oh 1, Taek Sang Kim 1, Hyun Yul Rhew 1, Bong Kwon Chun
http://dx.doi.org/10.7180/kmj.2016.31.1.66 KMJ Case Report Metachronous anterior urethral metastasis of prostatic ductal adenocarcinoma Jeong Hyun Oh 1, Taek Sang Kim 1, Hyun Yul Rhew 1, Bong Kwon Chun
Kidney, Bladder and Prostate Neoplasia. David Bingham MD
 Kidney, Bladder and Prostate Neoplasia David Bingham MD typical malignant cytology of bladder washings 1 benign 2 malignant typical malignant cytology of bladder washings b Bladder tumor Non invasive papillary
Kidney, Bladder and Prostate Neoplasia David Bingham MD typical malignant cytology of bladder washings 1 benign 2 malignant typical malignant cytology of bladder washings b Bladder tumor Non invasive papillary
Are extended biopsies really necessary to improve prostate cancer detection?
 (2003) 6, 250 255 & 2003 Nature Publishing Group All rights reserved 1365-7852/03 $25.00 www.nature.com/pcan Are extended biopsies really necessary to improve prostate cancer detection? R Damiano*,1, R
(2003) 6, 250 255 & 2003 Nature Publishing Group All rights reserved 1365-7852/03 $25.00 www.nature.com/pcan Are extended biopsies really necessary to improve prostate cancer detection? R Damiano*,1, R
Gleason Scoring System 2017 JASREMAN DHILLON, MD ASSOCIATE PROFESSOR, DEPARTMENT OF ANATOMIC PATHOLOGY, MOFFITT CANCER CENTER, TAMPA, FLORIDA
 Gleason Scoring System 2017 JASREMAN DHILLON, MD ASSOCIATE PROFESSOR, DEPARTMENT OF ANATOMIC PATHOLOGY, MOFFITT CANCER CENTER, TAMPA, FLORIDA Learners Objectives u Latest changes per ISUP 2014 that impact
Gleason Scoring System 2017 JASREMAN DHILLON, MD ASSOCIATE PROFESSOR, DEPARTMENT OF ANATOMIC PATHOLOGY, MOFFITT CANCER CENTER, TAMPA, FLORIDA Learners Objectives u Latest changes per ISUP 2014 that impact
Mucin-producing urothelial-type adenocarcinoma of prostate: report of two cases of a rare and diagnostically challenging entity
 & 2005 USCAP, Inc All rights reserved 0893-3952/05 $30.00 www.modernpathology.org Mucin-producing urothelial-type adenocarcinoma of prostate: report of two cases of a rare and diagnostically challenging
& 2005 USCAP, Inc All rights reserved 0893-3952/05 $30.00 www.modernpathology.org Mucin-producing urothelial-type adenocarcinoma of prostate: report of two cases of a rare and diagnostically challenging
Flat Epithelial Atypia
 Flat Epithelial Atypia Richard Owings, M.D. University of Arkansas for Medical Sciences Department of Pathology Flat epithelial atypia can be a difficult lesion May be a subtle diagnosis Lots of changes
Flat Epithelial Atypia Richard Owings, M.D. University of Arkansas for Medical Sciences Department of Pathology Flat epithelial atypia can be a difficult lesion May be a subtle diagnosis Lots of changes
ASSESSMENT OF GLEASON SYSTEM USE ON DIFFERENT TYPES OF PROSTATIC TISSUE SAMPLES
 ASSESSMENT OF GLEASON SYSTEM USE ON DIFFERENT TYPES OF PROSTATIC TISSUE SAMPLES I. E. PLEŞEA*, B. ZAHARIA*, S. D. ENACHE**, G. MITROI***, P. TOMESCU***, O. T. POP*, P. BADEA****, A. KOŻOKIĆ***** *Department
ASSESSMENT OF GLEASON SYSTEM USE ON DIFFERENT TYPES OF PROSTATIC TISSUE SAMPLES I. E. PLEŞEA*, B. ZAHARIA*, S. D. ENACHE**, G. MITROI***, P. TOMESCU***, O. T. POP*, P. BADEA****, A. KOŻOKIĆ***** *Department
A re-audit of Prostate biopsies from January to December 2010 and 2013.
 A re-audit of Prostate biopsies from January to December 2010 and 2013. Dr. M S Siddiqui Consultant Histopathologist University Hospital of North Tees Stockton on Tees. Objectives To assess and compare
A re-audit of Prostate biopsies from January to December 2010 and 2013. Dr. M S Siddiqui Consultant Histopathologist University Hospital of North Tees Stockton on Tees. Objectives To assess and compare
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Update on 2015 WHO Classification of Lung Adenocarcinoma 1/3/ Mayo Foundation for Medical Education and Research. All rights reserved.
 1 Our speaker for this program is Dr. Anja Roden, an associate professor of Laboratory Medicine and Pathology at Mayo Clinic as well as consultant in the Anatomic Pathology Laboratory and co-director of
1 Our speaker for this program is Dr. Anja Roden, an associate professor of Laboratory Medicine and Pathology at Mayo Clinic as well as consultant in the Anatomic Pathology Laboratory and co-director of
Uropathology January Jon Oxley
 Uropathology January 2012 Jon Oxley Background to seminar These slides were available to view via the web from scanned slides The junior pathologists answered questions on them via the web The answers
Uropathology January 2012 Jon Oxley Background to seminar These slides were available to view via the web from scanned slides The junior pathologists answered questions on them via the web The answers
PDF of Trial CTRI Website URL -
 Clinical Trial Details (PDF Generation Date :- Sun, 25 Nov 2018 12:22:24 GMT) CTRI Number Last Modified On 06/07/2013 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Clinical Trial Details (PDF Generation Date :- Sun, 25 Nov 2018 12:22:24 GMT) CTRI Number Last Modified On 06/07/2013 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Inverted (hobnail) high grade prostatic intraepithelial neoplasia and invasive inverted pattern
 ONCOLOGY LETTERS 10: 2395-2399, 2015 Inverted (hobnail) high grade prostatic intraepithelial neoplasia and invasive inverted pattern MELTEM ÖZNUR 1, SEVIM BAYKAL KOCA 2, PELIN YILDIZ 3, BURAK BAHADIR 4
ONCOLOGY LETTERS 10: 2395-2399, 2015 Inverted (hobnail) high grade prostatic intraepithelial neoplasia and invasive inverted pattern MELTEM ÖZNUR 1, SEVIM BAYKAL KOCA 2, PELIN YILDIZ 3, BURAK BAHADIR 4
Signet-Ring Cell Change in Benign Prostatic Hyperplasia - A Rare Case Report
 Article ID: WMC00688 ISSN 2046-1690 Signet-Ring Cell Change in Benign Prostatic Hyperplasia - A Rare Case Report Author(s):Dr. Pallavi Bhuyan, Dr. Smita Mahapatra, Dr. Sujata Pujari, Dr. Jayasree Rath
Article ID: WMC00688 ISSN 2046-1690 Signet-Ring Cell Change in Benign Prostatic Hyperplasia - A Rare Case Report Author(s):Dr. Pallavi Bhuyan, Dr. Smita Mahapatra, Dr. Sujata Pujari, Dr. Jayasree Rath
Atypical Foci Suspicious but not Diagnostic of Malignancy in Prostate Needle Biopsies (Also Referred to as Atypical Small Acinar Proliferation
 european urology 50 (2006) 666 674 available at www.sciencedirect.com journal homepage: www.europeanurology.com Review Prostate Cancer Atypical Foci Suspicious but not Diagnostic of Malignancy in Prostate
european urology 50 (2006) 666 674 available at www.sciencedirect.com journal homepage: www.europeanurology.com Review Prostate Cancer Atypical Foci Suspicious but not Diagnostic of Malignancy in Prostate
Prostatic ductal adenocarcinoma: An aggressive variant that is underdiagnosed and undersampled on transrectal ultrasound (TRUS)-guided needle biopsy
 Original research Prostatic ductal adenocarcinoma: An aggressive variant that is underdiagnosed and undersampled on transrectal ultrasound (TRUS)-guided needle biopsy Previn Gulavita, MD; * Shaheed W.
Original research Prostatic ductal adenocarcinoma: An aggressive variant that is underdiagnosed and undersampled on transrectal ultrasound (TRUS)-guided needle biopsy Previn Gulavita, MD; * Shaheed W.
International Society of Gynecological Pathologists Symposium 2007
 International Society of Gynecological Pathologists Symposium 2007 Anais Malpica, M.D. Department of Pathology The University of Texas M.D. Anderson Cancer Center Grading of Ovarian Cancer Histologic grade
International Society of Gynecological Pathologists Symposium 2007 Anais Malpica, M.D. Department of Pathology The University of Texas M.D. Anderson Cancer Center Grading of Ovarian Cancer Histologic grade
An Official Periodical of The International Academy of Cytology and the Italian Society of Urologic Pathology
 ANALYTICAL AND QUANTITATIVE CYTOLOGY AND HISTOLOGY ARTICLES An Official Periodical of The International Academy of Cytology and the Italian Society of Urologic Pathology Cell Proliferation and Apoptosis
ANALYTICAL AND QUANTITATIVE CYTOLOGY AND HISTOLOGY ARTICLES An Official Periodical of The International Academy of Cytology and the Italian Society of Urologic Pathology Cell Proliferation and Apoptosis
Urinary Bladder: WHO Classification and AJCC Staging Update 2017
 Urinary Bladder: WHO Classification and AJCC Staging Update 2017 Houston Society of Clinical Pathologists 58 th Annual Spring Symposium Houston, TX April 8, 2017 Jesse K. McKenney, MD Classification
Urinary Bladder: WHO Classification and AJCC Staging Update 2017 Houston Society of Clinical Pathologists 58 th Annual Spring Symposium Houston, TX April 8, 2017 Jesse K. McKenney, MD Classification
Since the beginning of the prostate-specific antigen (PSA) era in the. Characteristics of Insignificant Clinical T1c Prostate Tumors
 2001 Characteristics of Insignificant Clinical T1c Prostate Tumors A Contemporary Analysis Patrick J. Bastian, M.D. 1 Leslie A. Mangold, B.A., M.S. 1 Jonathan I. Epstein, M.D. 2 Alan W. Partin, M.D., Ph.D.
2001 Characteristics of Insignificant Clinical T1c Prostate Tumors A Contemporary Analysis Patrick J. Bastian, M.D. 1 Leslie A. Mangold, B.A., M.S. 1 Jonathan I. Epstein, M.D. 2 Alan W. Partin, M.D., Ph.D.
chapter 4. The effect of oncogenic HPV on transformation zone epithelium
 chapter 4. The effect of oncogenic HPV on transformation zone epithelium CHAPTER 1 All squamous cervical cancer (and probably all cervical adenocarcinoma) is associated with oncogenic HPV, and the absence
chapter 4. The effect of oncogenic HPV on transformation zone epithelium CHAPTER 1 All squamous cervical cancer (and probably all cervical adenocarcinoma) is associated with oncogenic HPV, and the absence
Case: The patient is a 62 year old woman with a history of renal cell carcinoma that was removed years ago. A 2.4 cm liver mass was found on CT
 Case: The patient is a 62 year old woman with a history of renal cell carcinoma that was removed years ago. A 2.4 cm liver mass was found on CT during follow- up. ALT, AST, Alk Phos and bilirubin were
Case: The patient is a 62 year old woman with a history of renal cell carcinoma that was removed years ago. A 2.4 cm liver mass was found on CT during follow- up. ALT, AST, Alk Phos and bilirubin were
Pathologic Results of Radical Prostatectomies in Patients with Simultaneous Atypical Small Acinar Proliferation and Prostate Cancer
 www.kjurology.org DOI:10.4111/kju.2010.51.6.398 Urological Oncology Pathologic Results of Radical Prostatectomies in Patients with Simultaneous Atypical Small Acinar Proliferation and Prostate Cancer Kwang
www.kjurology.org DOI:10.4111/kju.2010.51.6.398 Urological Oncology Pathologic Results of Radical Prostatectomies in Patients with Simultaneous Atypical Small Acinar Proliferation and Prostate Cancer Kwang
PATTERN OF PROSTRATE DISEASES- A HISTOPATHOLOGICAL STUDY IN JAMMU
 PATTERN OF PROSTRATE DISEASES- A HISTOPATHOLOGICAL STUDY IN JAMMU *Neha Angurana Dayanand Medical College & Hospital, Ludhiana- 141008 Punjab, India *Author for Correspondence ABSTRACT Benign hypertrophic
PATTERN OF PROSTRATE DISEASES- A HISTOPATHOLOGICAL STUDY IN JAMMU *Neha Angurana Dayanand Medical College & Hospital, Ludhiana- 141008 Punjab, India *Author for Correspondence ABSTRACT Benign hypertrophic
Outcomes Following Negative Prostate Biopsy for Patients with Persistent Disease after Radiotherapy for Prostate Cancer
 Clinical Urology Post-radiotherapy Prostate Biopsy for Recurrent Disease International Braz J Urol Vol. 36 (1): 44-48, January - February, 2010 doi: 10.1590/S1677-55382010000100007 Outcomes Following Negative
Clinical Urology Post-radiotherapy Prostate Biopsy for Recurrent Disease International Braz J Urol Vol. 36 (1): 44-48, January - February, 2010 doi: 10.1590/S1677-55382010000100007 Outcomes Following Negative
PERSPECTIVE. Abstract. and Glen Kristiansen. Yuri Tolkach*
 Journal of Pathology J Pathol 2018; 244: 389 393 Published online 7 March 2018 in Wiley Online Library (wileyonlinelibrary.com) DOI: 10.1002/path.5045 PERSPECTIVE Is high-grade prostatic intraepithelial
Journal of Pathology J Pathol 2018; 244: 389 393 Published online 7 March 2018 in Wiley Online Library (wileyonlinelibrary.com) DOI: 10.1002/path.5045 PERSPECTIVE Is high-grade prostatic intraepithelial
Ductal adenocarcinoma of the prostate: A clinicopathological study
 20 B. SATHESAN, S. A. S. GOONEWARDENA, H. W. D. ANURUDDHIKA AND M. V. C. DE SILVA Sri Lanka Journal of Urology, 2008, 9, 20-24 Original Article Ductal adenocarcinoma of the prostate: A clinicopathological
20 B. SATHESAN, S. A. S. GOONEWARDENA, H. W. D. ANURUDDHIKA AND M. V. C. DE SILVA Sri Lanka Journal of Urology, 2008, 9, 20-24 Original Article Ductal adenocarcinoma of the prostate: A clinicopathological
Supplemental Information
 Supplemental Information Prediction of Prostate Cancer Recurrence using Quantitative Phase Imaging Shamira Sridharan 1, Virgilia Macias 2, Krishnarao Tangella 3, André Kajdacsy-Balla 2 and Gabriel Popescu
Supplemental Information Prediction of Prostate Cancer Recurrence using Quantitative Phase Imaging Shamira Sridharan 1, Virgilia Macias 2, Krishnarao Tangella 3, André Kajdacsy-Balla 2 and Gabriel Popescu
In 2005, International Society of Urological Pathology
 ORIGINAL ARTICLE Gleason Score 3+4=7 Prostate Cancer With Minimal Quantity of Gleason Pattern 4 on Needle Biopsy Is Associated With Low-risk Tumor in Radical Prostatectomy Specimen Cheng Cheng Huang, MD,*
ORIGINAL ARTICLE Gleason Score 3+4=7 Prostate Cancer With Minimal Quantity of Gleason Pattern 4 on Needle Biopsy Is Associated With Low-risk Tumor in Radical Prostatectomy Specimen Cheng Cheng Huang, MD,*
Radical prostatectomy is the most widely used treatment. Partial Sampling of Radical Prostatectomy Specimens
 ORIGINAL ARTICLE Detection of Positive Margins and Extraprostatic Extension Viacheslav Iremashvili, MD, PhD,* Soum D. Lokeshwar,* Mark S. Soloway, MD,* Lise tpelaez,md,w Saleem A. Umar, MD,w Murugesan
ORIGINAL ARTICLE Detection of Positive Margins and Extraprostatic Extension Viacheslav Iremashvili, MD, PhD,* Soum D. Lokeshwar,* Mark S. Soloway, MD,* Lise tpelaez,md,w Saleem A. Umar, MD,w Murugesan
Outline (1) Outline (2) Concepts in Prostate Pathology. Peculiarities of Prostate Cancer. Peculiarities of Prostate Cancer
 Concepts in Prostate Pathology Murali Varma Cardiff, UK wptmv@cf.ac.uk Sarajevo Nov 2013 Outline (1) Peculiarities of prostate cancer Peculiarities of prostate needle biopsy Needle bx vs. TURP Prostate
Concepts in Prostate Pathology Murali Varma Cardiff, UK wptmv@cf.ac.uk Sarajevo Nov 2013 Outline (1) Peculiarities of prostate cancer Peculiarities of prostate needle biopsy Needle bx vs. TURP Prostate
Kathmandu University Medical Journal (2010), Vol. 8, No. 2, Issue 30,
 Kathmandu University Medical Journal (2010), Vol. 8, No. 2, Issue 30, 158-163 Original Research Article Correlation of serum free prostate-specific antigen level with histological findings in patients
Kathmandu University Medical Journal (2010), Vol. 8, No. 2, Issue 30, 158-163 Original Research Article Correlation of serum free prostate-specific antigen level with histological findings in patients
3/23/2017. Significant Changes in Prostate Cancer Classification, Grading, Staging and Reporting. Disclosure of Relevant Financial Relationships
 Disclosure of Relevant Financial Relationships Staging and Reporting of Prostate Cancer: Major Changes in 8 th Edition AJCC Staging and CAP Cancer Checklists USCAP requires that all planners (Education
Disclosure of Relevant Financial Relationships Staging and Reporting of Prostate Cancer: Major Changes in 8 th Edition AJCC Staging and CAP Cancer Checklists USCAP requires that all planners (Education
