Robotic Radical Prostatectomy
|
|
|
- Annabelle Waters
- 6 years ago
- Views:
Transcription
1 Robotic Radical Prostatectomy 13 Kevin M. Slawin & Naveen Kella Over the past 5 years, the areas of debate regarding the treatment of localized prostate cancer have shifted dramatically. Prior to this period, there were many strong advocates resisting PSA-based screening for prostate cancer and questioning the role of treatment for localized disease in the absence of randomized trials proving a survival benefit. However, with the striking declines in advanced disease associated with screening programs, most dramatically in Tyrol, Austria, together with the unequivocal randomized data from Sweden proving a survival benefit from radical prostatectomy for clinically localized prostate cancer, the value of surgery for these patients is less frequently challenged. Key efforts now are focused on determining the appropriate PSA cutpoints for prostate cancer screening and on addressing the problem of overtreatment of patients with disease of lower grade and volume. Variables often discussed now are the efficacy and morbidity of various treatment options for clinically localized prostate cancer. Treatment decisions require that patients and physicians weigh the risks and benefits of each option. Newer, minimally invasive options for the treatment of prostate cancer, such as robotic prostatectomy, impact this equation by offering high cancer control rates similar to those achieved with open, radical prostatectomy, but with a lower short-term, and potentially longterm, morbidity. The first great strides in addressing the morbidity of prostate cancer surgery were made through a better understanding of the surgical anatomy of the prostate, urinary sphincter, and neurovascular bundles, along with increased experience, as the number of radical prostatectomies performed ballooned in the late 1980s and 1990s [1]. These efforts led to a steady improvement in cancer control along with an improved quality of life for patients in the areas of urinary and sexual functions after surgery for prostate cancer. More recently, technical advances in instrumentation, primarily in support of a laparoscopic approach to surgery, have supported a second revolution in radical prostatectomy surgery. Whereas laparoscopic approaches to the kidney gained acceptance by urologists, laparoscopic prostatectomy initially remained less popular because of the high degree of technical difficulty of this complex operation, and the long and steep learning curve associated with achieving its mastery. Challenges with laparoscopic prostate surgery include lack of depth perception, antiintuitive reverse motion of the instruments, amplification of hand tremor, diminished dexterity in fine movements with the use of laparoscopic instruments due to the limited degrees of freedom (4 versus 6 for a surgeon s
2 own hands), awkward ergonomics for the operating physician and a reduction in tactile feedback. Despite these challenges, a small cadre of talented surgeons, many of whom were expert laparoscopic surgeons but with limited training in oncology, became adept at laparoscopic prostatectomy, surging to the forefront of the field of surgical management of prostate cancer. However, through the relentless drive of technology in the fields of computers and microelectronics, robotic techniques have emerged to provide a viable pathway for classically trained oncologic surgeons, skilled in open radical prostatectomy after years of practice and experience, to translate these skills into a minimally invasive approach to radical prostatectomy. This has leveled the field for all surgeons interested in pursuing minimally invasive approaches to prostate cancer surgery. The DaVinci robotic system (Intuitive Surgical, Inc., Mountain View, CA) allows surgeons to sit comfortably at a console and immerse themselves in a magnified (up to ten-fold) and 3-dimensional view of the surgical field. At the console, the surgeon controls instruments located on the surgical cart, which is the apparatus located patient-side. The surgeon has control of the stereoscopic camera as well as up to three robotic arms, which can wield various and interchangeable instruments. The instruments are able to articulate with wrist-like movements that allow six degrees of motion compared with four degrees possible with conventional laparoscopic instruments. Computer-filtration can eliminate surgeon tremor and finely scale a surgeon s motions up to 5:1, if desired. Moreover, instrument motions occur without perceptible delay to the surgeon. Because tactile feedback is limited, the surgeon is forced to rely on visual cues while dissecting and handling tissue. The first robotic radical prostatectomies were performed by Binder and Kramer in Germany in May 2000 [2]. The advantages provided by robotic assistance for this highly complex and demanding surgical procedure have resulted in an increase in the number of surgeons performing the procedure. In 2004, robotic assistance was used in nearly 10% of all radical prostatectomies performed in the United States.. However, the learning curve is still significant for performing a robotic-assisted laparoscopic prostatectomy. A study by Ahlering et al showed that 20 robotic cases were needed to achieve four-hour proficiency by a surgeon experienced in open procedures. For the initial 45 patients, the mean operating time was 3.45 hours (range hours) [3]. Another requirement in laparoscopic surgery is a skilled assistant. Whereas many DaVinci robotic systems have an additional instrument arm, which allows the surgeon himself to help provide retraction, an experienced assistant is still invaluable for providing suction, irrigation, additional retraction, rapid instrument changes and occasional surgical cart troubleshooting. GENERAL BENEFITS OF ROBOTIC SURGERY Clear benefits of robotic surgery are the reduction in postoperative pain and length of hospitalization because of the minimally invasive nature of the procedure. Generally, our experience is that 90% of patients are ready for discharge the day after surgery. Reports in the literature corroborate our finding. Tewari et al. noted that 93% of their patients are ready for discharge within 24 hours of surgery [8]. Decreased blood loss associated with laparoscopic and robotic-assisted surgery is well documented in the literature. Blood loss in reported series has consistently been less than 200 cc and transfusion rates have been negligible. Narcotic usage is minimal, and many patients may not need patient-controlled analgesia with morphine. Many centers, including ours, find that a 24 hour course of ketorolac is sufficient for pain control during hospitalization followed by Tylenol and hydrocodone tablets afterwards. The Foley catheter remains in situ for one week. Earlier removal is possible but raises the risk of urinary retention. Return to work or return to baseline activities seems anecdotally to occur earlier with robotic-operated patients. We allow patients to return to work and regular activities in as early as one to two weeks after surgery, especially those men who are not physical laborers. Atlas of the Prostate 172
3 URINARY CONTINENCE AND ROBOTIC SURGERY Reports indicate that urinary continence returns earlier with a robotic prostatectomy. Tewari et al. observed that 50% of patients achieved continence within 44 days after robotic surgery compared to 160 days with open surgery [8]. In our experience, it is not unusual for patients to report wearing zero to one pad shortly after removal of the Foley catheter at one week, but we have not yet fully analyzed and reported our continence rates with validated questionnaires. Further evaluation of continence rates is even more interesting when examining the rates of continence achieved by highly experienced open surgeons. For example, Ahlering et al. compared a sequential series of 60 robotics patients (starting after his 45 th robotic case) with the last 60 patients (out of hundreds) who had open surgery. From the robotics group, 76% of patients were completely continent 3 months after surgery, a proportion similar to that for his last group of 60 patients who underwent open radical prostatectomy [9]. With the robotic approach, excellent visualization at the prostatic apex results in maximal preservation of urethral length and minimizes inadvertent cautery damage to surrounding musculature and nerves. Whereas definite data are lacking, many consider preservation of urethral length as a contributor to return of continence [10]. Another aspect of the robotic approach is the ability to construct a watertight anastomosis. Again, whether urinary extravasation truly contributes to incontinence is an unanswered question. However, the ability to prevent urinary leaks does allow earlier removal of the catheter and perhaps reduces the incidence of bladder neck contracture due to urinary extravasation. Indeed, the reported incidence of bladder neck contracture in the robotic literature is extremely low. In summary, promising data suggest an advantage in speed of return of continence and possibly total rate of return of continence with robotics. Additionally, as in open surgery, a surgeon s technique may ultimately be the driving factor in urinary continence. Robotics may better allow preservation of urethral length, construction of a watertight anastomosis, and bladder neck sparing, but surgeon skill and experience are still vital for consistent outcomes for urinary continence. SEXUAL POTENCY AFTER ROBOTIC SURGERY In laparoscopy, dissection of the prostate proceeds primarily in an antegrade fashion. The posterolateral neurovascular bundles are generally thickest proximally at the base of the prostate. As they are dissected under direct vision, they can be swept away towards the apex of the gland. Once at the apex, vision with robotics is superior to that with open surgery as long as the field is relatively bloodless. This visualization allows precise dissection of the neurovascular bundle away from the prostate at its apex. In total, these efforts likely contribute to preservation of sexual function. Of course, principles of nerve preservation during open surgery also apply to robotic surgery. Along with knowledge of the anatomy of the neurovascular bundles, minimal use of cautery and gentle handling of the neurovascular bundles are important. Long-term data are available from some institutions that adopted robotics relatively early. For example, Tewari et al. indicated that robotic surgery patients had an earlier return of erections than patients who had open surgery (50% return at a mean of 180 days versus 440 days for open radical prostatectomy patients). Undoubtedly, as with urinary continence, surgical technique and surgeon experience, rather than the use of the robot, will still be the primary factor determining the eventual success of nervesparing surgery. COSTS OF ROBOTIC SURGERY Robotic Radical Prostatectomy 173 On a simplistic level, assessing the robotic prostatectomy from a cost-profit standpoint generally shows a poor financial return for the hospital. For example, in one report, a single center in the United States performed 174 procedures over a period of 18 months. The total hospital cost per radical prostatectomy was greater than the reimbursement per case by $148. In addition, this figure does not even account for the initial investment and annual maintenance for the robot, typically over 1 million dollars and 100,000 dollars, respectively [11]. At The Methodist Hospital in Houston, Texas, robotic prostatectomy produces net revenue, although over the past three years, open radical prostatectomy generated approximately $1000 more per case for the hospital. With growing experience and the currently decreasing time in the operating room achieved more recently, this differential in revenue will narrow. Further studies may also need to look beyond the hospital s finances and examine the cost of a radical prostatectomy from society s standpoint. Factors such as an earlier return to work, an earlier return of continence, and improved sexual function should be investigated to determine whether they are sufficient to justify the overall higher cost of robotic prostatectomy.
4 PREOPERATIVE CONSIDERATIONS In general, radical prostatectomy is a treatment option for men with a life expectancy of 10 years or more. Any patient who is a candidate for open extirpation may also be a candidate for a laparoscopic robotic procedure. Conditions making laparoscopy more challenging include previous prostate surgery, whether open or endoscopic; abdominal surgeries, especially with usage of mesh; and adjuvant or salvage treatment, whether after radiation, hormonal therapy, or cryotherapy. The presence of a known median lobe calls for a surgeon who has achieved a higher level of expertise and comfort with this operation. Less experienced surgeons would be more likely to leave a portion of the median lobe behind, or have more difficulty in reconstructing the potentially wide bladder neck. Repair can be done posteriorly or anteriorly on the bladder neck depending on surgeon preference. The technique for performing the bladder neck reconstruction robotically is similar to the technique used in open surgery, but it can be difficult for the inexperienced robotic surgeon. Furthermore, a large prostate tends to lead to longer operating time because of the difficulty inherent in manipulating and placing traction on the prostate in a reduced space. However, we have successfully removed prostates over 130 grams in size. Removal of pelvic lymph nodes is recommended for patients with higher PSA or Gleason Score. Surgeons can perform pelvic lymph node dissection laparoscopically with the DaVinci system, although a more complete node dissection can be achieved through the more standard, open procedure. The pneumoretroperitoneum can flatten the iliac veins, and dissection must be done delicately to avoid injury. Although a transperitoneal approach reduces the risk of a lymphocele, we exclusively utilize a retroperitoneal approach for robotic prostatectomy. PREOPERATIVE PREPARATION Surgeons need to discuss with their patients the risks of laparoscopy and traditional open surgery as well as the possibility of a robotic malfunction, which have been noted but are rare. Bowel preparations can be administered according to surgeon preference, although a simple enema on the morning of surgery is the only preparation we recommend for both robotic and open prostatectomy. Especially during the transition period for newly minted robotic surgeons, patients should be keenly made aware that the surgeon may convert the case to an open approach if he for any reason, he feels the patient s interests favor conversion. Series Positive Margin Rates of Multiple Published Series Soloway (review of several centers) Lepor Scardino Walsh Guillonneau Abbou Rassweiler Turk Bollens Sulser Menon Ahlering Patel V (Open) (Open) (Open, 1154 cases) (498 cases) (Open, 4683 cases from ) (Laparoscopic, 400 cases at MSKCC) (Laparoscopic) (Laparoscopic) (Laparoscopic) (Laparoscopic) (Laparoscopic) (Robotic, >100 cases) (Robotic, 140 cases) (Robotic, 450 cases) Positive margins, % pt2 7.8 pt All 9.2 pt pt2 6.4 pt , 17, FIGURE Positive margin rates of multiple published series. In oncology, a positive margin means an incomplete excision of the tumor. Whereas half or more of prostate cancer patients with a positive margin will remain cancerfree with long-term follow-up, efforts to reduce positive margins clearly lead to better biochemical progression-free rates [4]. In a study by Epstein et al, patients with positive margins had 10-year biochemical progression-free rates of 55%, whereas patients with negative margins had progression-free rates of 80% [5]. With open surgery, it has been shown that surgical technique is an independent predictor of positive margin status [6]. In robotics, the surgeon s technique also influences surgical margin rates. The improvement in visualization and precise movements during a robotic procedure come at the expense of tactile sensation, which some surgeons rely on to detect the presence of tumor extension [7]. Early series in robotics appear to show positive margin rates, which are at least comparable with many open and laparoscopic surgical series. Atlas of the Prostate 174
5 Baylor College of Medicine Single Surgeon Positive Margin Rate with Robotic Prostatectomy (n=117 cases) (Unpublished) pt2 % + SM pt3 % + SM First 50 cases 42 (50)=84% 3 (42)=7% 8 (50)=16% 2 (8)=25% Second 50 cases 32 (50)=64% 1 (32)=3% 13 (50)=26% 3 (13)=23% Last 17 cases 16 (17)=94% 0 (16)=0% 1 (17)=5.9% 0 (1)=0% FIGURE Baylor College of Medicine single surgeon positive margin rate with robotic prostatectomy. Positive margins typically are encountered at the prostatic apex or along the posterolateral aspect of the prostate where the neurovascular bundles are located. Interestingly, these are both locations where the robotic or laparoscopic approach can provide excellent visualization. With a straight (0 degree) or angled down (30 degree down) lens, surgical detail generally unappreciated in open surgery can be visualized to allow a more anatomical dissection, especially at the apex and alongside the neurovascular bundles. As surgeons experienced with radical prostatectomy migrate to the robotic platform, positive margin rates should improve. At Baylor College of Medicine, the single surgeon positive margin rate shows continuing improvement with experience, as shown in this table, and is comparable to those reported for open radical prostatectomy at our center, as well as at other centers of excellence, as shown in Table 1. More importantly, data regarding long-term PSA PFS with robotic prostatectomy will require maturation of data to compare this more clinically significant outcome measure. FIGURE Patient positioning. The patient is positioned supine in lithotomy position, or with split legs, to allow access for the robot between the legs of the patient. Arms are padded and tucked to the sides. This allows space for the assistant to work freely and also avoids possible interference with the optional fourth arm of the DaVinci robot. Depending on whether the approach is transperitoneal or extraperitoneal, the patient is placed maximally to moderately in Trendelenburg position. The surgical prep covers the genitalia to the xiphoid process and stretches laterally to just beyond the anterior superior iliac spines. For a four-arm system, the fourth arm is typically routed below the patient s left leg, or in some institutions, the right leg. The master-slave system of the DaVinci surgical system is comprised of the following: a surgeon s console with a 3-dimensional viewer, the surgical robot with either two or three working arms, and a camera arm. A patient-side assistant attaches instruments to the robotic arms and can change them throughout the course of the procedure. The assistant typically controls one or two laparoscopic ports for suctioning, retraction, suture passing, and eventual entrapment of the prostate in a specimen bag. At the console, the surgeon continually uses his hands and feet to move the instruments, to activate monopolar or bipolar electrocautery, and to position the camera. Robotic Radical Prostatectomy 175 FIGURE Port placement. Two factors, the route of the procedure and the anatomy of the pubic bone, pubic rami, and anterior superior iliac spines primarily determine port placement. The decision to perform surgery transperitoneally or extraperitoneally dictates placement of the camera port 1 or 2 cm above the umbilicus if transperitoneal, or just below the umbilicus if extraperitoneal. The remaining ports are placed in a semicircular fashion, but the pubis should be used as the frame of reference, rather than the camera port [12]. The robotic arms have a finite length and positioning them further than 18 cm away from the pubis (measured when insufflated) risks making them unavailable for performance of the apical dissection or for the anastomosis. At the same time, the DaVinci arms need to be positioned sufficiently distant from the pubis to allow the anterior bladder takedown or a pelvic lymph node dissection. The robotic arms also need to be placed far enough apart to prevent instrument interaction. An 8 to 10 cm distance between each port (insufflated) appears ideal for avoiding interaction. In order to properly position the ports, we initially map out on the patient s skin the superior border of the pubic bone and the anterior superior iliac spines. After placement of the camera port, the primary right and left robotic arm positions are measured and marked on the lower abdomen. The position of the fourth arm is marked on the abdomen laterally to the left of the primary robotic trocar on the left side, all the way to the anterior iliac spine. Finally, a 5 mm assistant port in marked, two-finger breadths above the pubic bone, just to the right of the midline, and a 12 mm port between the camera port and the right sided robotic trocar are positioned. The 12 mm port is needed for passing needles, suctioning, and potentially for stapling the dorsal vein, as well as for entrapping the specimen.
6 FIGURE Retroperitoneal insufflation. After making a 1 2 cm incision just below the umbilicus, the linea alba is exposed with an Army- Navy retractor, and the anterior rectus sheath is incised with an 11 blade, taking care to leave intact the posterior rectus fascia. Using finger dissection, the Space of Rhetzius is developed. A 2-0 prolene suture is place at the upper apex of the fascial incision and tagged. A kidney-shaped balloon dissection is then placed into the developed space and manually insufflated. After removing the deflated balloon dissector, the mm camera port is inserted and a pneumoretroperitoneum of 13 mm Hg is established. FIGURE Wide angle start. After approximately our first 50 cases, we have switched exclusively to the extraperitoneal approach, which we prefer because it requires less Trendelenburg, avoids the physiologic consequences of a pneumoperitoneum, takes advantage of the peritoneum to retract and protect the small bowel, and is less problematic in the rare event of a urine leak postoperatively. Using an extraperitoneal approach, the bladder is swept posteriorly by the pneumoretroperitoneum and the surgeon has immediate access to the prostate at the outset. FIGURE Clearing of working space. As with conventional laparoscopy, clearing the working space allows improved visualization of surgical planes and diminished problems of clogging the suction device if there is bleeding. The fat is cleared from the endopelvic fascia and puboprostatics to the junction between the prostate and the bladder. Atlas of the Prostate 176
7 A B FIGURE A, Endopelvic fascia, and B, apical dissection. Sharp scissor dissection or electrocautery can start the endopelvic dissection lateral to the prostate. Work is carried proximally to the prostaticovesical junction, which is identifiable by a V shaped tongue of perirectal fat. As the condensations of the endopelvics move distally, they merge into the puboprostatic ligaments. Levator and pubourethral musculature appears to regularly insert into the visceral fascia of the prostate laterally, and forms a sling around the dorsal vein fascia distally. We spare as much musculature as possible by using blunt dissection primarily, and bipolar electrocautery only when necessary. FIGURE Control of dorsal vein complex. The surgeon can decide whether to use a suture ligature or stapler at the apex. An EndoGIA stapler can nicely expose the urethra with minimal bleeding, but requires more dissection of the DVC and puboprostatics to allow placement of the device. Urethral transection theoretically is possible with the stapler. When distinguishing the urethra is difficult, gentle manipulation of the Foley catheter can help in identifying the demarcation between urethra and the dorsal venous complex. This same maneuver is useful when throwing a suture ligature to control the DVC. An advantage of using the stapler is the resulting clear visualization of the urethra. This will allow a precise urethral dissection and potentially reduce iatrogenic apical margins later in the operation [13]. Despite this, in our experience, a simple figure of eight suture using 0-Mersilene, which has a high coefficient of friction and thus resists slippage off of the DVC fascia, is all that is required to effectively control the DVC and is more cost efficient. Robotic Radical Prostatectomy 177 FIGURE Anterior bladder neck dissection. The successful dissection of the bladder neck is critical for creating the conditions for a simple urethrovesical anastomosis at the end of the procedure. The border between the prostate and bladder can be identified visually if the overlying prostatic fat is removed and is best identified at the lateral aspects. The 30 degree down lens provides a good view for this portion of the operation, and the surgeon can use it until the start of the urethral portion of the urethrovesical anastomosis. Moving the Foley catheter all the way into the bladder and then slowly pulling it back can also help identify the proper plane of dissection. An experienced assistant is invaluable for providing irrigation and counter-traction at this step. Our dissection proceeds close to the capsule of the prostate. Starting laterally on each side of prostaticovesicular junction, the surgeon uses the lateral aspect of the prostate as a landmark and starts the creation of a trough towards the midline. Bleeding can occur laterally with perivesicular veins and can occur if dissection occurs into the prostate or too far into the detrusor musculature. A combination of sharp and blunt dissection will identify the bladder neck in the midline, and the proper plan is maintained by staying in the layer of periprostatic fat, present between the bladder neck and prostate laterally. The lateral approach also nicely exposes any median lobe that might be present, thereby facilitating blunt dissection of this lobe off of the posterior aspect of the bladder neck.
8 FIGURE Cut bladder neck. Cutting into the bladder will reveal the Foley catheter, which the fourth arm or the assistant can grasp to provide counter-traction for the posterior bladder neck dissection. FIGURE Posterior bladder neck dissection. After the Foley catheter is elevated by the assistant, the bladder neck mucosa can be seen posteriorly following the contour of the base of the prostate into the urethra. This bladder neck is developed starting laterally with sharp and blunt dissection, sweeping the bladder neck off of the prostate. The detrusor fibers will give way to expose the anterior layer of Denonvillier s fascia. At this point, it is convenient to transect the posterior lip of mucosa forming the bladder neck. Dissection can quickly proceed to the anterior layer of Denonvillier s fascia, already established laterally. If a median lobe is present, the steps are similar except that the mucosa covering the median lobe should be transected at the neck of the median lobe and then bluntly dissected to reach Denonvillier s fascia. If the ureteral orifices are difficult to locate, the anesthesiologist can administer intravenous methylene blue. An important point is to establish the thickness of the bladder neck wall. The thickness usually is the same circumferentially. This can help as a landmark during difficult dissections and can prevent a button-hole dissection into the posterior bladder. FIGURE Seminal vesicles and vasa. Cutting through the Denonvillier s fascia will reveal loose connective tissue encasing the seminal vesicles and vasa. This dissection can appear very deep, especially with a large prostate. To avoid dissecting into a hole, it is helpful to work laterally, as well as to continue to bring the bladder off the prostate. This will also help maintain orientation during this task. We fully remove the seminal vesicles for oncologic purposes, but are careful to use scissor and bipolar dissection or clips to control the vessels to the vasa and the seminal vesicles to minimize injury to the neurovascular bundles. Atlas of the Prostate 178 FIGURE Posterior dissection. To begin the posterior dissection, the seminal vesicles and vasa are grabbed and placed on upwards traction by the assistant. When posterior Denonvillier s fascia is transected close to the base of the prostate, the lobulated perirectal fat becomes apparent. Blunt and sharp dissection can establish the pedicles of the prostate. The plane of dissection should keep the posterior surface of the prostate apparent in order to avoid dissection too close or into the rectum. This posterior dissection can be carried all the way to the urethra if desired.
9 A FIGURE A, Control of vascular pedicles and neurovascular bundle dissection. Anatomically, the vascular pedicles originate lateral to the seminal vesicles. Electrocautery or Weck clips are used to control the pedicles. With the increased magnification provided by the robot, the individual branches originating from the inferior vesicular artery can be coagulated precisely with bipolar cautery. As the pedicles are dropped, the B neurovascular bundles can be dissected away from the prostate. Moving in an antegrade fashion allows the bundles to be brought away from the prostate under direct vision. The bundles travel posterolaterally along the prostate and then are lateral and posterolateral to the urethra. B demonstrates a nerve-sparing approach, left. FIGURE Urethral transection and entrapment of prostate. Apical positive margins can be minimized and the urethral length can be maximized if the urethral transection is done under hemostatic conditions. The dorsal venous complex can occasionally start bleeding again due to slippage of the DVC suture, and a second hemostatic stitch should be placed in this circumstance to ensure bloodless visualization during this portion of the procedure. The fourth arm of the robot is useful at this stage to provide traction on the midprostatic suture anteriorally and cephalad. Transection through the uncut portion of the DVC staple line is done with a scissor, which is used to transect the urethra as well. Skilled open surgeons will find it comfortable to complete the distal portion of the neurovascular bundle dissection at this stage, in a retrograde fashion. A specimen sack is deployed to bag the prostate and which is then removed through the camera port incision. For larger prostates, this incision is extended slightly to allow specimen removal, and then shortened again with a 2-0 prolene suture to allow a tight seal when the camera port is replaced in order to complete the operation. Robotic Radical Prostatectomy 179
10 FIGURE Non-nerve sparing approach, right. In a small percentage of cases, the tumor grade and extent requires a non-nerve sparing approach unilaterally. The proximal and distal extent of the resected nerve is marked with clips. A B FIGURE A, Proximal collagen graft, and B, distal collagen graft. For those patients requiring nerve grafting, the proximal and distal cut ends of the NVB are stuffed into the ends of a collagen tube allograft (Neuragen, OriginBiomedicinals, Inc., Nova Scotia, Canada) and secured with 5-0 prolene sutures. Atlas of the Prostate 180
11 A C B FIGURE A, B, and C. Urethrovesical anastomosis. Perhaps the best example of the advantage of robotic surgery over conventional laparoscopy is in the performance of the anastomosis. The needle drivers can articulate at the wrist and thus allow sutures to be thrown precisely and with minimal trauma to surrounding tissues. A running, doublearmed stitch popularized by Van Velthoven et al. results in a watertight anastomosis [14]. A few important points can make the anastomosis portion of the case move smoothly. Monocryl suture is useful because it can slide smoothly through tissue and thus accommodate the occasional tightening of the running anastomosis to prevent leaks. The fourth arm or the assistant can hold traction on the other arm of the stitch to prevent too much loosening of the anastomosis. If bladder neck reconstruction is needed, it can be done on the anterior or posterior portion of the bladder. If the tension required to bring the bladder down to the urethra seems to be too much, the best course of action is to place a few more throws before attempting to bring the anastomosis together. Multiple throws will dissipate the tension across the suture line and allow increased force to bring the anastomosis together. A B FIGURE A, Bladder neck suspension, and B, completion of procedure. Finally, a surgeon s knot is important to prevent the closure ties from coming apart. We typically approximate the DVC fascia to the anterior bladder neck with a final 2-0 Vicryl mattress suture to complete the procedure. Robotic Radical Prostatectomy 181
12 FUTURE Almost 10% of all radical prostatectomy surgeries were performed robotically in As more surgeons surmount the learning curve, this percentage will increase. Implementation of training programs will be challenging but important to train the next generation of urologists to perform robotic surgery. The benefits of robotic surgery include quicker recovery, diminished blood loss, and the faster recovery of continence. Data on sexual potency appear encouraging, but longer-term data from more robotic series are needed. Nerve-sparing is possible with robotics and will likely be technique dependent, just as in open surgery. Surgical positive margin rates appear to be comparable to or better than published rates from open series. However, most importantly, the use of the DaVinci system will not magically transform surgeons with limited knowledge or skill performing prostate cancer surgery into expert surgeons, or instantly improve their outcomes. Improved outcomes come only with experience and attention to the surgical anatomy of the prostate and an understanding of the biology of prostate cancer, regardless of the method used. Conversely, the DaVinci system can allow surgeons already adept at open radical prostatectomy after years of experience and hundreds or even thousands of cases to more readily translate this hard-won skill into minimally invasive surgery for prostate cancer. REFERENCES 1. Walsh PC: Anatomic radical prostatectomy: evolution of the surgical technique. J Urol 1998, 160(6 Pt 2): Binder J, Kramer W: Robotically-assisted laparoscopic radical prostatectomy. BJU Int 2001, 87(4): Ahlering TE, Skarecky D, Lee D: Successful transfer of open surgical skills to a laparoscopic environment using a robotic interface: initial experience with laparoscopic radical prostatectomy. J Urol 2003, 170: Grossfeld GD, Chang JJ, Broering JM, et al.: Impact of positive surgical margins on prostate cancer recurrence and the use of secondary cancer treatment: data from the CaPSURE database. Urology 2000, 163: Epstein JI, Partin AW, Sauvageot J, et al.: Prediction of progression following radical prostatectomy. A multivariate analysis of 721 men with long-term followup. Am J Surg Path 1996, 20: Eastham JA, Kattan MW, Riedel E, et al.: Variations among individual surgeons in the rate of positive surgical margins in radical prostatectomy specimens. J Urol 2003, 170: Hernandez DJ, Epstein JI, Trock BJ, et al.: Radical retropubic prostatectomy. How often do experienced surgeons have positive surgical margins when there is extraprostatic extension in the region of the neurovascular bundle? J Urol 2005, 173: Tewari A, Srivasatava A, Menon M; Members of the VIP Team: A prospective comparison of radical retropubic and robot-assisted prostatectomy: experience in one institution. BJU Int : Ahlering TE, Woo D, Eichel L, et al.: Robot-assisted versus open radical prostatectomy: a comparison of one surgeon s outcomes. Urology 2004, 63: Coakley FV, Eberhardt S, Kattan MW, et al.: Urinary continence after radical retropubic prostatectomy: relationship with membranous urethral length on preoperative endorectal magnetic resonance imaging. J Urol 2002, 168: Jean J: Cost-profit analysis of davinci robotic surgery: Is it worth it? J Urol 2005, 173(4 suppl): Pick DL, Lee DI, Skarecky DW, et al.: Anatomic guide for port placement for davinci robotic radical prostatectomy. J Endourol 2004, 18: Ahlering TE, Eichel L, Edwards RA, et al.: Robotic radical prostatectomy: a technique to reduce pt2 positive margins. Urology 2004, 64: Van Velthoven RF, Ahlering TE, Peltier A, et al.: Technique for laparoscopic running urethrovesical anastomosis: the single knot method. Urology 2003, 61: Atlas of the Prostate 182
da Vinci Prostatectomy
 da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
da Vinci Prostatectomy My Greek personal experience
 da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
Robotic Surgery for Prostate Cancer: A Realistic Approach to Getting Started The Evolution of a Robotic Surgeon
 Robotic Surgery for Prostate Cancer: A Realistic Approach to Getting Started The Evolution of a Robotic Surgeon Douglas S. Scherr, M.D. Clinical Director, Urologic Oncology Weill Medical College of Cornell
Robotic Surgery for Prostate Cancer: A Realistic Approach to Getting Started The Evolution of a Robotic Surgeon Douglas S. Scherr, M.D. Clinical Director, Urologic Oncology Weill Medical College of Cornell
Clinical Study Retrograde Robotic Radical Prostatectomy: Description of a New Technique and Early Perioperative Outcomes
 ISRN Urology, Article ID 945604, 5 pages http://dx.doi.org/10.1155/2014/945604 Clinical Study Retrograde Robotic Radical Prostatectomy: Description of a New Technique and Early Perioperative Outcomes Gino
ISRN Urology, Article ID 945604, 5 pages http://dx.doi.org/10.1155/2014/945604 Clinical Study Retrograde Robotic Radical Prostatectomy: Description of a New Technique and Early Perioperative Outcomes Gino
Robotics, Laparoscopy & Endosurgery
 Robotics, Laparoscopy and Endosurgery Robotics, Laparoscopy & Endosurgery How to preserve bladder neck during robotic radical prostatectomy? Abdullah Erdem Canda* Department of Urology, Yildirim Beyazit
Robotics, Laparoscopy and Endosurgery Robotics, Laparoscopy & Endosurgery How to preserve bladder neck during robotic radical prostatectomy? Abdullah Erdem Canda* Department of Urology, Yildirim Beyazit
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Department of Urology, Cochin hospital Paris Descartes University
 Technical advances in the treatment of localized prostate cancer Pr Michaël Peyromaure Department of Urology, Cochin hospital Paris Descartes University Introduction Curative treatments of localized prostate
Technical advances in the treatment of localized prostate cancer Pr Michaël Peyromaure Department of Urology, Cochin hospital Paris Descartes University Introduction Curative treatments of localized prostate
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
Citation for published version (APA): Haber, G. P. (2010). Application of emerging technologies to urologic oncology
 UvA-DARE (Digital Academic Repository) Application of emerging technologies to urologic oncology Haber, G.P. Link to publication Citation for published version (APA): Haber, G. P. (2010). Application of
UvA-DARE (Digital Academic Repository) Application of emerging technologies to urologic oncology Haber, G.P. Link to publication Citation for published version (APA): Haber, G. P. (2010). Application of
PERTINENT ISSUES RELATED TO LAPAROSCOPIC RADICAL PROSTATECTOMY
 Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology LAPAROSCOPIC RADICAL PROSTATECTOMY Vol. 29 (6): 489-496, November - December, 2003 PERTINENT ISSUES RELATED
Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology LAPAROSCOPIC RADICAL PROSTATECTOMY Vol. 29 (6): 489-496, November - December, 2003 PERTINENT ISSUES RELATED
Improvements in Robot-Assisted Prostatectomy: The Effect of Surgeon Experience and Technical Changes on Oncologic and Functional Outcomes
 JOURNAL OF ENDOUROLOGY Volume 24, Number 7, July 2010 ª Mary Ann Liebert, Inc. Pp. 1105 1110 DOI: 10.1089=end.2010.0136 Improvements in Robot-Assisted Prostatectomy: The Effect of Surgeon Experience and
JOURNAL OF ENDOUROLOGY Volume 24, Number 7, July 2010 ª Mary Ann Liebert, Inc. Pp. 1105 1110 DOI: 10.1089=end.2010.0136 Improvements in Robot-Assisted Prostatectomy: The Effect of Surgeon Experience and
The importance of maximal restoration of peri-prostatic support
 Providing the best evidence for each surgical option in organ confined prostate cancer The importance of maximal restoration of peri-prostatic support A. Mottrie ORSI-Academy Melle Belgium OLV Hospital
Providing the best evidence for each surgical option in organ confined prostate cancer The importance of maximal restoration of peri-prostatic support A. Mottrie ORSI-Academy Melle Belgium OLV Hospital
Learning Curve of Robotic-assisted Radical Prostatectomy With 60 Initial Cases by a Single Surgeon
 Original Article Learning Curve of Robotic-assisted Radical Prostatectomy With 60 Initial Cases by a Single Surgeon Yen-Chuan Ou, 1 Chi-Rei Yang, 1 John Wang, 2 Chen-Li Cheng 1 and Vipul R. Patel, 3 1
Original Article Learning Curve of Robotic-assisted Radical Prostatectomy With 60 Initial Cases by a Single Surgeon Yen-Chuan Ou, 1 Chi-Rei Yang, 1 John Wang, 2 Chen-Li Cheng 1 and Vipul R. Patel, 3 1
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Laparoscopic Surgery. The Da Vinci Robot. Limits of Laparoscopy. What Robotics Offers. Robotic Urologic Surgery: A New Era in Patient Care
 Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Open Prostatectomy is Best
 Open Prostatectomy is Best William J. Catalona, M.D. The Trifecta Trifecta Cure Continence Potency Northwestern University Feinberg School of Medicine Eastham, J et al, JUrol 179:2207 Continence (Pad Free
Open Prostatectomy is Best William J. Catalona, M.D. The Trifecta Trifecta Cure Continence Potency Northwestern University Feinberg School of Medicine Eastham, J et al, JUrol 179:2207 Continence (Pad Free
Facing Prostate Cancer?
 The Enabling Technology: The da Vinci Surgical System Your doctor is one of the growing number of surgeons worldwide offering da Vinci Surgery for a range of complex conditions. The da Vinci Surgical System
The Enabling Technology: The da Vinci Surgical System Your doctor is one of the growing number of surgeons worldwide offering da Vinci Surgery for a range of complex conditions. The da Vinci Surgical System
Inception Cohort. Center for Evidence-Based Medicine, Oxford VIP-- Inception Cohort (2008) Nov Dec
 VIP-- Inception Cohort (28) Robotic Prostatectomy: Oncological and Functional Outcomes after 4 cases The Donald Smith Lecture Nov 2- Dec 28---- ----42 patients Patient 1 to patient 38 PSA follow-up -------3481
VIP-- Inception Cohort (28) Robotic Prostatectomy: Oncological and Functional Outcomes after 4 cases The Donald Smith Lecture Nov 2- Dec 28---- ----42 patients Patient 1 to patient 38 PSA follow-up -------3481
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Intussusception of the bladder neck does not promote early restoration to urinary continence after non-nervesparing radical retropubi c prostatectomy
 Blackwell Science, LtdOxford, UKIJUInternational Journal of Urology0919-81722004 Blackwell Publishing Asia Pty LtdMarch 2004123275279Original ArticleIntussusception of the bladder neck and early continencei
Blackwell Science, LtdOxford, UKIJUInternational Journal of Urology0919-81722004 Blackwell Publishing Asia Pty LtdMarch 2004123275279Original ArticleIntussusception of the bladder neck and early continencei
DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis.
 DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
Citation Acta medica Nagasakiensia. 1963, 8(
 NAOSITE: Nagasaki University's Ac Title Radical Operation For Prostatic Car Author(s) Kondoh, Atushi Citation Acta medica Nagasakiensia. 1963, 8( Issue Date 1963-12-25 URL http://hdl.handle.net/10069/15473
NAOSITE: Nagasaki University's Ac Title Radical Operation For Prostatic Car Author(s) Kondoh, Atushi Citation Acta medica Nagasakiensia. 1963, 8( Issue Date 1963-12-25 URL http://hdl.handle.net/10069/15473
TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy
 TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy Nam Kyu Kim M.D., Ph.D., FACS, FRCS, FASCRS Professor Department of Surgery Yonsei University College of Medicine Seoul,
TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy Nam Kyu Kim M.D., Ph.D., FACS, FRCS, FASCRS Professor Department of Surgery Yonsei University College of Medicine Seoul,
Laparoscopic Instruments for Urology
 Laparoscopic Instruments for Urology Urology Growing importance Laparoscopic Methods in Urology The laparoscopic method is increasingly gaining importance in the treatment of identified carcinomas in the
Laparoscopic Instruments for Urology Urology Growing importance Laparoscopic Methods in Urology The laparoscopic method is increasingly gaining importance in the treatment of identified carcinomas in the
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation 3D HD Vision 3D HD visualization facilitates accurate
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation 3D HD Vision 3D HD visualization facilitates accurate
INTERNATIONAL JOURNAL OF ONCOLOGY 38: ,
 INTERNATIONAL JOURNAL OF ONCOLOGY 38: 293-304, 2011 293 Utility of transrectal ultrasonography guidance and seven key elements of operative skill for early recovery of urinary continence after laparoscopic
INTERNATIONAL JOURNAL OF ONCOLOGY 38: 293-304, 2011 293 Utility of transrectal ultrasonography guidance and seven key elements of operative skill for early recovery of urinary continence after laparoscopic
Pathologic Outcomes during the Learning Curve for Robotic-Assisted Laparoscopic Radical Prostatectomy
 Clinical Urology Pathologic Outcomes While Learning RALP International Braz J Urol Vol. 34 (2): 159-163, March - April, 2008 Pathologic Outcomes during the Learning Curve for Robotic-Assisted Laparoscopic
Clinical Urology Pathologic Outcomes While Learning RALP International Braz J Urol Vol. 34 (2): 159-163, March - April, 2008 Pathologic Outcomes during the Learning Curve for Robotic-Assisted Laparoscopic
disfunzioni sessuali ed urinarie: come evitarle? D. Mascagni
 disfunzioni sessuali ed urinarie: come evitarle? D. Mascagni Cattedra di Chirurgia Generale Direttore: Prof. A. Filippini Verona, 2010 CHIRURGIA RADICALE PER CANCRO DEL RETTO SOTTOPERITONEALE 5cm 2 cm
disfunzioni sessuali ed urinarie: come evitarle? D. Mascagni Cattedra di Chirurgia Generale Direttore: Prof. A. Filippini Verona, 2010 CHIRURGIA RADICALE PER CANCRO DEL RETTO SOTTOPERITONEALE 5cm 2 cm
DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT OF URETERAL STENT: SIMPLIFICATION OF THE TECHNIQUE
 Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
Robotic Laparoscopic Radical Prostatectomy
 State of the Art Robotic Laparoscopic Radical Prostatectomy Assaad El-Hakim, MD Ashutosh Tewari, MD Prostate cancer is the most common non-skin cancer in the United States and is the second leading cause
State of the Art Robotic Laparoscopic Radical Prostatectomy Assaad El-Hakim, MD Ashutosh Tewari, MD Prostate cancer is the most common non-skin cancer in the United States and is the second leading cause
Chapter 2. Simple Nephrectomy. Please Give Three Tips for Laparoscopic Simple Nephrectomy. Dr. de la Rosette
 Chapter 2 Simple Nephrectomy Please Give Three Tips for Laparoscopic Simple Nephrectomy............. 39 How Does One Find the Renal Hilum during Transperitoneal Laparoscopic Nephrectomy?.................
Chapter 2 Simple Nephrectomy Please Give Three Tips for Laparoscopic Simple Nephrectomy............. 39 How Does One Find the Renal Hilum during Transperitoneal Laparoscopic Nephrectomy?.................
Robotic Surgery for Upper Tract Urothelial Carcinoma. Li-Ming Su, MD
 Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
Clinical Pearls: The Approach to the Management of Difficult Anatomy and Common Operative and Postoperative Problems
 14 Clinical Pearls: The Approach to the Management of Difficult Anatomy and Common Operative and Postoperative Problems Vipul R. Patel The task of learning robotic prostatectomy can be quite challenging
14 Clinical Pearls: The Approach to the Management of Difficult Anatomy and Common Operative and Postoperative Problems Vipul R. Patel The task of learning robotic prostatectomy can be quite challenging
Robotic radical prostatectomy Technique and results of nerve sparing approach EAU 2009 March 19 th 2009
 Robotic radical prostatectomy Technique and results of nerve sparing approach EAU 2009 March 19 th 2009 J.H. Witt Department of Urology and Pediatric Urology Prostate Center Northwest St. Antonius-Hospital
Robotic radical prostatectomy Technique and results of nerve sparing approach EAU 2009 March 19 th 2009 J.H. Witt Department of Urology and Pediatric Urology Prostate Center Northwest St. Antonius-Hospital
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery
 Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
LATERAL PEDICLE CONTROL DURING LAPAROSCOPIC RADICAL PROSTATECTOMY: REFINED TECHNIQUE
 RAPID COMMUNICATION LATERAL PEDICLE CONTROL DURING LAPAROSCOPIC RADICAL PROSTATECTOMY: REFINED TECHNIQUE INDERBIR S. GILL, OSAMU UKIMURA, MAURICIO RUBINSTEIN, ANTONIO FINELLI, ALIREZA MOINZADEH, DINESH
RAPID COMMUNICATION LATERAL PEDICLE CONTROL DURING LAPAROSCOPIC RADICAL PROSTATECTOMY: REFINED TECHNIQUE INDERBIR S. GILL, OSAMU UKIMURA, MAURICIO RUBINSTEIN, ANTONIO FINELLI, ALIREZA MOINZADEH, DINESH
Laparoscopic Radical Prostatectomy
 1 2 3 3 Laparoscopic Radical Prostatectomy 4 5 Sidney C. Abreu, Andrew P. Steinberg, and Inderbir S. Gill Cleveland Clinic Foundation, Cleveland, Ohio, USA 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22
1 2 3 3 Laparoscopic Radical Prostatectomy 4 5 Sidney C. Abreu, Andrew P. Steinberg, and Inderbir S. Gill Cleveland Clinic Foundation, Cleveland, Ohio, USA 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22
Collaborative Stage Coding Prostate Cases
 PROSTATE CASE 1 History & Physical 7/2 The patient is a 63 year old male with normal physical exam. Digital rectal exam showed normal seminal vesicles. Prostate smooth with no palpable nodules. Biopsy
PROSTATE CASE 1 History & Physical 7/2 The patient is a 63 year old male with normal physical exam. Digital rectal exam showed normal seminal vesicles. Prostate smooth with no palpable nodules. Biopsy
Robot Assisted-Radical Prostatectomy (RARP) and
 Narrowing of the Dorsal Vein Complex Technique during Laparoscopic Radical Prostatectomy: A Simple Trick to Simplify the Control of Venous Plexus Alejandro García-Segui,* Manuel Sánchez, Aleixandre Verges,
Narrowing of the Dorsal Vein Complex Technique during Laparoscopic Radical Prostatectomy: A Simple Trick to Simplify the Control of Venous Plexus Alejandro García-Segui,* Manuel Sánchez, Aleixandre Verges,
Transition from open to robotic-assisted radical prostatectomy: 7 years experience at Hackensack University Medical Center
 J Robotic Surg (27) 1:155 159 DOI 1.7/s1171-7-23- ORIGINAL ARTICLE Transition from open to robotic-assisted radical prostatectomy: 7 years experience at Hackensack University Medical Center Ravi Munver
J Robotic Surg (27) 1:155 159 DOI 1.7/s1171-7-23- ORIGINAL ARTICLE Transition from open to robotic-assisted radical prostatectomy: 7 years experience at Hackensack University Medical Center Ravi Munver
BJUI. Surgery Illustrated Surgical Atlas Robot-assisted ascending-descending laparoscopic nerve-sparing prostatectomy
 et al. a Surgeon b Assistant Anaesthesia Scrub Nurse Assistant 5 mm Port 12 mm Port 8 mm Robotic Ports 12 mm Camera Port 8 mm Port (4th arm) GILLITZER ET AL. BJUI BJU INTERNATIONAL Surgery Illustrated
et al. a Surgeon b Assistant Anaesthesia Scrub Nurse Assistant 5 mm Port 12 mm Port 8 mm Robotic Ports 12 mm Camera Port 8 mm Port (4th arm) GILLITZER ET AL. BJUI BJU INTERNATIONAL Surgery Illustrated
Urinary Bladder. Prof. Imran Qureshi
 Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
EndoBlade Soft Tissue Release System
 Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
8 A SIMPLE FISTULA REPAIR, STEP BY STEP
 8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
Laparoscopic Right Colectomy
 Laparoscopic Right Colectomy Shawnee Mission Medical Center February 22, 2011 Hi, and welcome to the program. My name is Dr. Sanjay Thekkeurumbil, and I m a colorectal surgeon at Shawnee Mission Medical
Laparoscopic Right Colectomy Shawnee Mission Medical Center February 22, 2011 Hi, and welcome to the program. My name is Dr. Sanjay Thekkeurumbil, and I m a colorectal surgeon at Shawnee Mission Medical
Cover Page. The following handle holds various files of this Leiden University dissertation:
 Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Laparoscopic radical prostatectomy, first described in the early
 ORIGINAL RESEARCH Initial experience with robotic-assisted laparoscopic radical prostatectomy in the Canadian health care system Joseph L. Chin, MD; * Patrick P. Luke, MD; * Stephen E. Pautler, MD See
ORIGINAL RESEARCH Initial experience with robotic-assisted laparoscopic radical prostatectomy in the Canadian health care system Joseph L. Chin, MD; * Patrick P. Luke, MD; * Stephen E. Pautler, MD See
Prostate Cancer. David Wilkinson MD Gulfshore Urology
 Prostate Cancer David Wilkinson MD Gulfshore Urology What is the Prostate? Male Sexual Gland Adds nutrients and fluids for sperm This fluid is added to sperm during ejaculation Urethra (urine channel)
Prostate Cancer David Wilkinson MD Gulfshore Urology What is the Prostate? Male Sexual Gland Adds nutrients and fluids for sperm This fluid is added to sperm during ejaculation Urethra (urine channel)
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery.
 This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery. 1 The border of the anterior abdominal wall is defined superiorly by the
This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery. 1 The border of the anterior abdominal wall is defined superiorly by the
Radical Cystectomy A Patient s Guide
 Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Stepwise Description and Outcomes of Bladder Neck Sparing During Robot-Assisted Laparoscopic Radical Prostatectomy
 Stepwise Description and Outcomes of Bladder Neck Sparing During Robot-Assisted Laparoscopic Radical Prostatectomy David F. Friedlander, Mehrdad Alemozaffar, Nathanael D. Hevelone, Stuart R. Lipsitz and
Stepwise Description and Outcomes of Bladder Neck Sparing During Robot-Assisted Laparoscopic Radical Prostatectomy David F. Friedlander, Mehrdad Alemozaffar, Nathanael D. Hevelone, Stuart R. Lipsitz and
AATS Focus on Thoracic Surgery: Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017?
 AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Robotic distal ureterectomy with psoas hitch and ureteroneocystostomy: Surgical technique and outcomes
 Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
The Surgical Procedure Is the Most Important Factor Affecting Continence Recovery after Laparoscopic Radical Prostatectomy
 pissn: 2287-4208 / eissn: 2287-4690 World J Mens Health 2013 August 31(2): 163-169 http://dx.doi.org/10.5534/wjmh.2013.31.2.163 Original Article The Surgical Procedure Is the Most Important Factor Affecting
pissn: 2287-4208 / eissn: 2287-4690 World J Mens Health 2013 August 31(2): 163-169 http://dx.doi.org/10.5534/wjmh.2013.31.2.163 Original Article The Surgical Procedure Is the Most Important Factor Affecting
Nasser Simforoosh, Ahmad Javaherforooshzadeh, Alireza Aminsharifi, Ali Tabibi
 Laparoscopic Urology Early Continence After Open and Laparoscopic Radical Prostatectomy With Sutureless Vesicourethral Alignment An Alternative Technique, 8 Years Experience Nasser Simforoosh, Ahmad Javaherforooshzadeh,
Laparoscopic Urology Early Continence After Open and Laparoscopic Radical Prostatectomy With Sutureless Vesicourethral Alignment An Alternative Technique, 8 Years Experience Nasser Simforoosh, Ahmad Javaherforooshzadeh,
Minimally invasive surgery in urology oncology. Dr. Tongchai Nakamont 23 Jan 2014
 Minimally invasive surgery in urology oncology Dr. Tongchai Nakamont 23 Jan 2014 Urology oncology Renal cell carcinoma ( RCC) Transitional cell carcinoma (TCC) Kidney Ureter Bladder Prostate cancer Urological
Minimally invasive surgery in urology oncology Dr. Tongchai Nakamont 23 Jan 2014 Urology oncology Renal cell carcinoma ( RCC) Transitional cell carcinoma (TCC) Kidney Ureter Bladder Prostate cancer Urological
Lecture 56 Kidney and Urinary System
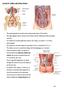 Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Asian Journal of Andrology (2013) 15, ß 2013 AJA, SIMM & SJTU. All rights reserved X/13 $ ORIGINAL ARTICLE
 (2013) 15, 513 517 ß 2013 AJA, SIMM & SJTU. All rights reserved 1008-682X/13 $32.00 www.nature.com/aja ORIGINAL ARTICLE A matched-pair comparison between bilateral intrafascial and interfascial nerve-sparing
(2013) 15, 513 517 ß 2013 AJA, SIMM & SJTU. All rights reserved 1008-682X/13 $32.00 www.nature.com/aja ORIGINAL ARTICLE A matched-pair comparison between bilateral intrafascial and interfascial nerve-sparing
Laparoscopic radical prostatectomy
 Review Article Laparoscopic radical prostatectomy Michael Lipke, Chandru P. Sundaram Department of Urology, Indiana University School of Medicine, Indianapolis, Indiana, USA Address for correspondence:
Review Article Laparoscopic radical prostatectomy Michael Lipke, Chandru P. Sundaram Department of Urology, Indiana University School of Medicine, Indianapolis, Indiana, USA Address for correspondence:
Robot-Assisted Radical Prostatectomy
 John W. Davis Editor Robot-Assisted Radical Prostatectomy Beyond the Learning Curve 123 Apex: The Crossroads of Functional Recovery and Oncologic Control 10 Fatih Atug I nt rod u c ti on Prostate cancer
John W. Davis Editor Robot-Assisted Radical Prostatectomy Beyond the Learning Curve 123 Apex: The Crossroads of Functional Recovery and Oncologic Control 10 Fatih Atug I nt rod u c ti on Prostate cancer
Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer
 Technical Note Page 1 of 8 Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer Gong Chen, Rong-Xin Zhang, Zhi-Tao Xiao Department of Colorectal Surgery, Sun Yat-sen University
Technical Note Page 1 of 8 Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer Gong Chen, Rong-Xin Zhang, Zhi-Tao Xiao Department of Colorectal Surgery, Sun Yat-sen University
Open Radical Cystectomy Tips and Tricks in Males and Females
 Open Radical Cystectomy Tips and Tricks in Males and Females Seth P. Lerner, MD, FACS Professor of Urology Beth and Dave Swalm Chair in Urologic Oncology Scott Department of Urology Baylor College of Medicine
Open Radical Cystectomy Tips and Tricks in Males and Females Seth P. Lerner, MD, FACS Professor of Urology Beth and Dave Swalm Chair in Urologic Oncology Scott Department of Urology Baylor College of Medicine
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Open RRP versus LRP in Asian Men. International Braz J Urol Vol. 35 (2): , March - April, 2009
 Clinical Urology Open RRP versus LRP in Asian Men International Braz J Urol Vol. 35 (2): 151-157, March - April, 2009 Perioperative Outcomes of Open Radical Prostatectomy versus Laparoscopic Radical Prostatectomy
Clinical Urology Open RRP versus LRP in Asian Men International Braz J Urol Vol. 35 (2): 151-157, March - April, 2009 Perioperative Outcomes of Open Radical Prostatectomy versus Laparoscopic Radical Prostatectomy
Intraoperative Identification and Monitoring of the Somatic Nerves Critical to Potency Preservation during da Vinci Prostatectomy
 Intraoperative Identification and Monitoring of the Somatic Nerves Critical to Potency Preservation during da Vinci Prostatectomy J. Rasmussen, J. Schneider Background Since Walsh and Donker first introduced
Intraoperative Identification and Monitoring of the Somatic Nerves Critical to Potency Preservation during da Vinci Prostatectomy J. Rasmussen, J. Schneider Background Since Walsh and Donker first introduced
Oncological and functional results of extraperitoneal laparoscopic radical prostatectomy
 ONCOLOGY LETTERS 4: 351-357, 2012 Oncological and functional results of extraperitoneal laparoscopic radical prostatectomy TAO ZHENG, XU ZHANG, XIN MA, HONG-ZHAO LI, JIANG-PIN GAO, WEI CAI, GUANG-FU CHEN,
ONCOLOGY LETTERS 4: 351-357, 2012 Oncological and functional results of extraperitoneal laparoscopic radical prostatectomy TAO ZHENG, XU ZHANG, XIN MA, HONG-ZHAO LI, JIANG-PIN GAO, WEI CAI, GUANG-FU CHEN,
SCIENTIFIC PAPER ABSTRACT INTRODUCTION METHODS
 SCIENTIFIC PAPER Patient-Reported Validated Functional Outcome After Extraperitoneal Robotic-Assisted Nerve-Sparing Radical Prostatectomy Ralph Madeb, MD, Dragan Golijanin, MD, Joy Knopf, MD, Ivelisse
SCIENTIFIC PAPER Patient-Reported Validated Functional Outcome After Extraperitoneal Robotic-Assisted Nerve-Sparing Radical Prostatectomy Ralph Madeb, MD, Dragan Golijanin, MD, Joy Knopf, MD, Ivelisse
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS
 8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
Surgery Illustrated Surgical Atlas Millin Retropubic Prostatectomy
 BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Millin Retropubic Prostatectomy John M. Fitzpatrick Mater Misericordiae University Hospital Dublin & University College Dublin, Ireland Accepted
BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Millin Retropubic Prostatectomy John M. Fitzpatrick Mater Misericordiae University Hospital Dublin & University College Dublin, Ireland Accepted
BICEPTOR Tenodesis System
 BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
RADICAL PROSTATECTOMY
 Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
How-To Booklet: Pediatric Spay-Neuter. Surgical Techniques Pictorial
 How-To Booklet: Pediatric Spay-Neuter Surgical Techniques Pictorial Brenda Griffin, DVM, MS, DACVIM 1. Approach to Scrotal Neuter for Puppies 2. Cord Tie 3. Figure 8 Knot 4. Ovarian Pedicle Tie 5. Modified
How-To Booklet: Pediatric Spay-Neuter Surgical Techniques Pictorial Brenda Griffin, DVM, MS, DACVIM 1. Approach to Scrotal Neuter for Puppies 2. Cord Tie 3. Figure 8 Knot 4. Ovarian Pedicle Tie 5. Modified
Open Radical Retropubic Prostatectomy
 european urology 52 (2007) 71 80 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Open Radical Retropubic Prostatectomy Christian Barré * Service d Urologie,
european urology 52 (2007) 71 80 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Open Radical Retropubic Prostatectomy Christian Barré * Service d Urologie,
Evolution of Robotic Radical Prostatectomy. BACKGROUND. Robotic-assisted radical prostatectomy (RAP) is the dominant
 1951 Evolution of Robotic Radical Prostatectomy Assessment After 2766 Procedures Ketan K. Badani, MD Sanjeev Kaul, MD Mani Menon, MD Vattikuti Urology Institute, Henry Ford Hospital, Detroit, Michigan.
1951 Evolution of Robotic Radical Prostatectomy Assessment After 2766 Procedures Ketan K. Badani, MD Sanjeev Kaul, MD Mani Menon, MD Vattikuti Urology Institute, Henry Ford Hospital, Detroit, Michigan.
Retrograde Nerve-Sparing (NS) Laparoscopic Radical Prostatectomy (LRP): Technical Aspects and Early Results
 european urology supplements 5 (2006) 925 933 available at www.sciencedirect.com journal homepage: www.europeanurology.com Retrograde Nerve-Sparing (NS) Laparoscopic Radical Prostatectomy (LRP): Technical
european urology supplements 5 (2006) 925 933 available at www.sciencedirect.com journal homepage: www.europeanurology.com Retrograde Nerve-Sparing (NS) Laparoscopic Radical Prostatectomy (LRP): Technical
CLOSE-UP VIEW OF ROBOTIC SURGERY FOR PROSTATE CANCER THOMAS JEFFERSON UNIVERSITY HOSPITAL, PHILADELPHIA, PENNSYLVANIA Broadcast January 19, 2006
 CLOSE-UP VIEW OF ROBOTIC SURGERY FOR PROSTATE CANCER THOMAS JEFFERSON UNIVERSITY HOSPITAL, PHILADELPHIA, PENNSYLVANIA Broadcast January 19, 2006 00:00:16.000 NARRATOR: The American Cancer Society reports
CLOSE-UP VIEW OF ROBOTIC SURGERY FOR PROSTATE CANCER THOMAS JEFFERSON UNIVERSITY HOSPITAL, PHILADELPHIA, PENNSYLVANIA Broadcast January 19, 2006 00:00:16.000 NARRATOR: The American Cancer Society reports
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Totally thoracoscopic left upper lobe tri-segmentectomy
 Masters of Cardiothoracic Surgery Totally thoracoscopic left upper lobe tri-segmentectomy Dominique Gossot Thoracic Department, Institut Mutualiste Montsouris, Paris, France Correspondence to: Dominique
Masters of Cardiothoracic Surgery Totally thoracoscopic left upper lobe tri-segmentectomy Dominique Gossot Thoracic Department, Institut Mutualiste Montsouris, Paris, France Correspondence to: Dominique
Comparative Analysis Research of Robotic Assisted Laparoscopic Prostatectomy
 Comparative Analysis Research of Robotic Assisted Laparoscopic Prostatectomy By: Jonathan Barlaan; Huy Nguyen Mentor: Julio Powsang, MD Reader: Richard Wilder, MD May 2, 211 Abstract Introduction: The
Comparative Analysis Research of Robotic Assisted Laparoscopic Prostatectomy By: Jonathan Barlaan; Huy Nguyen Mentor: Julio Powsang, MD Reader: Richard Wilder, MD May 2, 211 Abstract Introduction: The
Inferior Pelvic Border
 Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Prostate Cancer Case Study 1. Medical Student Case-Based Learning
 Prostate Cancer Case Study 1 Medical Student Case-Based Learning The Case of Mr. Powers Prostatic Nodule The effervescent Mr. Powers is found by his primary care provider to have a prostatic nodule. You
Prostate Cancer Case Study 1 Medical Student Case-Based Learning The Case of Mr. Powers Prostatic Nodule The effervescent Mr. Powers is found by his primary care provider to have a prostatic nodule. You
Intrafascial Nerve-Sparing Endoscopic Extraperitoneal Radical Prostatectomy
 european urology 53 (2008) 931 940 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Intrafascial Nerve-Sparing Endoscopic Extraperitoneal Radical Prostatectomy
european urology 53 (2008) 931 940 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Intrafascial Nerve-Sparing Endoscopic Extraperitoneal Radical Prostatectomy
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
7/11/17. The Surgeon s Operative Report: Tools and Tips to Enhance Abstraction. Stopwoundinfection.com. Impact to Healthcare
 1. Scott, R. Douglas. The Direct Medical Costs of Healthcare-Associated Infections in U.S. Hospitals and the Benefits of Prevention. March 2009. http://www.cdc.gov/hai/pdfs/hai/scott_costpaper.pdf. 2.
1. Scott, R. Douglas. The Direct Medical Costs of Healthcare-Associated Infections in U.S. Hospitals and the Benefits of Prevention. March 2009. http://www.cdc.gov/hai/pdfs/hai/scott_costpaper.pdf. 2.
Peritoneal Dialysis Catheter Placement. Peritoneal Dialysis Catheter Placement. Peritoneal Dialysis Catheter Placement
 ASDIN Advanced Techniques Pre-course Feb. 24, 2012 New Orleans, La Randall L. Rasmussen, MD Special thank you to Drs. Rajeev Narayan, San Antonio, Tx and Hemant Dhingra, Fresno Ca for lending me slides
ASDIN Advanced Techniques Pre-course Feb. 24, 2012 New Orleans, La Randall L. Rasmussen, MD Special thank you to Drs. Rajeev Narayan, San Antonio, Tx and Hemant Dhingra, Fresno Ca for lending me slides
Transperitoneal Robotic-Assisted Laparoscopic Prostatectomy After Prosthetic Mesh Herniorrhaphy
 SCIENTIFIC PAPER Transperitoneal Robotic-Assisted Laparoscopic Prostatectomy After Prosthetic Mesh Herniorrhaphy Costas D. Lallas, MD, Mark L. Pe, MD, Jitesh V. Patel, MD, Pranav Sharma, Leonard G. Gomella,
SCIENTIFIC PAPER Transperitoneal Robotic-Assisted Laparoscopic Prostatectomy After Prosthetic Mesh Herniorrhaphy Costas D. Lallas, MD, Mark L. Pe, MD, Jitesh V. Patel, MD, Pranav Sharma, Leonard G. Gomella,
Clinical Study A Comparison of Radical Perineal, Radical Retropubic, and Robot-Assisted Laparoscopic Prostatectomies in a Single Surgeon Series
 Prostate Cancer Volume 2011, Article ID 878323, 6 pages doi:10.1155/2011/878323 Clinical Study A Comparison of Radical Perineal, Radical Retropubic, and Robot-Assisted Laparoscopic Prostatectomies in a
Prostate Cancer Volume 2011, Article ID 878323, 6 pages doi:10.1155/2011/878323 Clinical Study A Comparison of Radical Perineal, Radical Retropubic, and Robot-Assisted Laparoscopic Prostatectomies in a
Laparoscopic Radical Nephrectomy- the current gold standard
 Laparoscopic Radical Nephrectomy- the current gold standard Anoop M. Meraney, M.D Director, Urologic Oncology, Helen and Harry Gray Cancer Center, Hartford Hospital and Connecticut Surgical Group. Is it
Laparoscopic Radical Nephrectomy- the current gold standard Anoop M. Meraney, M.D Director, Urologic Oncology, Helen and Harry Gray Cancer Center, Hartford Hospital and Connecticut Surgical Group. Is it
Endoscopic Component Separation November Philip Omotosho, MD Assistant Professor of Surgery Duke University School of Medicine
 Endoscopic Component Separation November 2014 Philip Omotosho, MD Assistant Professor of Surgery Duke University School of Medicine Abdominal Wall Anatomy External Oblique Rectus Abdominus Internal Oblique
Endoscopic Component Separation November 2014 Philip Omotosho, MD Assistant Professor of Surgery Duke University School of Medicine Abdominal Wall Anatomy External Oblique Rectus Abdominus Internal Oblique
Operative Technique: Karen Horvath, MD, FACS. SCOAP Retreat June 17, 2011
 Operative Technique: Total Mesorectal Excision Karen Horvath, MD, FACS University it of Washington, Seattle SCOAP Retreat June 17, 2011 No Disclosures Purpose What is Total Mesorectal Excision (TME)? How
Operative Technique: Total Mesorectal Excision Karen Horvath, MD, FACS University it of Washington, Seattle SCOAP Retreat June 17, 2011 No Disclosures Purpose What is Total Mesorectal Excision (TME)? How
Urethral catheter removal 3 days after radical retropubic prostatectomy is feasible and desirable
 Urethral catheter 3 days after radical retropubic prostatectomy is feasible and desirable (2002) 5, 291 295 ß 2002 Nature Publishing Group All rights reserved 1365 7852/02 $25.00 www.nature.com/pcan JM
Urethral catheter 3 days after radical retropubic prostatectomy is feasible and desirable (2002) 5, 291 295 ß 2002 Nature Publishing Group All rights reserved 1365 7852/02 $25.00 www.nature.com/pcan JM
Surgery Illustrated Surgical Atlas
 Surgery Illustrated SURGERY ILLUSTRATEDMURPHY ET AL MURPHY ET AL. BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Robotically assisted laparoscopic pyeloplasty Declan Murphy, Ben Challacombe,
Surgery Illustrated SURGERY ILLUSTRATEDMURPHY ET AL MURPHY ET AL. BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Robotically assisted laparoscopic pyeloplasty Declan Murphy, Ben Challacombe,
