Embryology Relevant to Ultrasound Imaging of the Male Genitalia
|
|
|
- Katherine Meghan Jackson
- 6 years ago
- Views:
Transcription
1 Embryology Relevant to Ultrasound Imaging of the Male Genitalia Gideon Richards and Bruce R. Gilbert A basic understanding of the embryologic development of the male genitalia and the male genital blood supply helps guide the interpretation of many abnormalities in both scrotal and penile ultrasound. Presented in this chapter is the embryology relevant to the ultrasound evaluation of male genitalia. There are many excellent textbooks available which present the known elements of male genitourinary development, should the reader desire a comprehensive treatise on the subject [1 4]. Early Genital Developmental Anatomy In the 3-week-old embryo (Fig. 1), primordial germ cells, originating in the wall of the yolk sac near the attachment of the allantois, migrate along the wall of the hindgut and through the dorsal mesentery into the urogenital ridge. The urogenital ridge is a protrusion of intermediate mesoderm that indents the coelomic cavity (precursor to the peritoneal cavity) on each side of the mesentery. The kidney precursors, gonads, and the proximal portions of the reproductive tracts develop from the urogenital ridge. The unilateral absence of the male reproductive ducts or gonad and reproductive ducts is associated with ipsilateral absence of the kidney in % of cases [5]. It is, therefore, reasonable to evaluate the retroperitoneum for the presence of a kidney in a patient where the unilateral reproductive ducts are absent on ultrasound evaluation. In the 5-week-old embryo (Fig. 2), the two early excretory organ systems (the pronephros and mesonephros) begin to regress. The mesonephros constitutes the lateral portion of the urogenital ridge and consists of mesonephric tubules that inter- G. Richards ( ) B. R. Gilbert Arizona State Urological Institute, Gilbert, AZ 85295, USA gidrichards@gmail.com B. R. Gilbert The Arthur Smith Institute for Urology, North Shore-Long Island Jewish Health System, 450 Lakeville Road, Ste. M41, New Hyde Park, NY, USA bgilbert@gmail.com Springer Science+Business Media New York 2015 B. R. Gilbert (ed.), Ultrasound of the Male Genitalia, DOI / _2 11
2 12 G. Richards and B. R. Gilbert Hindgut Alantois Primordial germ cells Heart Yolk sac a Hindgut Genital ridge Fig. 1 Primordial germ cells at their location in yolk-sac as they begin their migration (a). The primordial germ cells migrating through the mesentery to the genital portion of the urogenital ridge bulging into the coelomic cavity (b) modified after Moore et al. [2] b Fig. 2 Development of the early excretory system. Regression of the pronephros (a) and mesonephros (b) with the development of the metanephric system modified after Moore et al. [2] act with glomeruli-like vessels extending from the aorta at one end, and drain into a mesonephric duct at the other end. The regression begins at the cranial aspects and continues toward the caudal end where the duct joins the cloaca (and at what will eventually diverge from the cloaca into the urogenital sinus). The ureteric bud
3 Embryology Relevant to Ultrasound Imaging of the Male Genitalia 13 Fig. 3 The reproductive ducts and their relationship to the developing gonads after the incorporation of the distal mesonephric ducts into the urogenital sinus modified after Moore et al. [2] (also referred to as the metanephric diverticulum) develops as a dorsal bud of the mesonephric duct near its insertion into the cloaca. The metanephros (precursor to the adult kidney) forms from the interaction of the metanephric diverticulum and a region of cells in the intermediate mesoderm known as the metanephric cell mass. At 7 weeks (Fig. 3), the embryo is devoid of phenotypic manifestations of sexual differentiation. There are two roughly parallel pairs of genital ducts: in addition to the mesonephric (Wolffian) ducts, there are the paramesonephric (Müllerian) ducts, which are located more laterally. Along the medial portion of the urogenital ridge, cords of coelomic epithelium termed sex cords have invaginated in to the ridge and house the primordial germ cells. This portion of the urogenital ridge becomes the gonadal ridge and the most superficial aspects of the sex cord regress to completely separate the sex cords from the rest of the coelomic epithelium. It is the presence of a Y chromosome gene, called the sex-determining region Y gene (SRY) or testis determining factor (TDF), that results in the development of testes and the initiation of phenotypic sexual differentiation. The testis forms in the gonadal ridge and Sertoli cells differentiate from cells within the epithelial sex cords. By week 8, the developing fetal testis produces at least two hormones. The first has been referred to as Müllerian-inhibiting substance or factor (MIS, MIF) and in some reports, anti-müllerian hormone (AMH). It is produced by the fetal Sertoli cells and suppresses the development of the paramesonephric duct (which in the absence of this suppression would develop into the upper female reproductive tract organs). The other, testosterone, stimulates the development of the mesonephric ducts into components of the male genital tract. Vestigial remnants of portions of these ducts (Fig. 4a) often can be visualized sonographically.
4 14 G. Richards and B. R. Gilbert Bladder Prostate utricle Paramesonephric duct Appendix of epididymis Appendix of testes Vas Deferens Paradidymis a b c Fig. 4 Locations of the vestigial remnants of the mesonephric and paramesonephric ducts in the male genitalia (a). Ultrasonic appearance of the appendix testis (b) and appendix epididymis (c) Remnants of the most cranial aspects of the regressed paramesonephric ducts can persist as the appendix of the testis and be demonstrated on ultrasound (Fig. 4b). The most caudal vestigial aspects of the paramesonephric ducts form midline structures and are often found in the prostate, which is derived from the embryonic urogenital sinus. The prostatic utricle is such a structure and can be enlarged and demonstrated on ultrasound. In addition, midline cysts derived from vestiges of the paramesonephric ducts may also be demonstrated. These midline paramesonephric remnants have also been found to obstruct the ejaculatory ducts and result in dilation of the seminal vesicles (anterior posterior (AP) distance greater than 15 mm). The deepest aspects of the sex cords converge on what will become the mediastinum testis. The mesenchyme between each of the cords gives rise to the interstitial cells of Leydig and the septa of the testis that radiate out from the mediastinum testis. The sex cords develop into tubules composted of the germ cells and Sertoli cells and the inner ends of these tubes are referred to as the tubuli recti. The gonadal
5 Embryology Relevant to Ultrasound Imaging of the Male Genitalia 15 ridge, throughout its development, slowly separates from the mesonephros. The mesonephric tubules adjacent to the testis develop into the ductuli efferentia and meet the tubuli recti at the rete testis. The mesonephric ducts develop into the epididymides, vasa defferentia, and ejaculatory ducts. The seminal vesicles develop as a diverticulum of this tube. Residual mesonephric structures can persist as a vestigial remnant of the mesonephric ducts. Those tubules located cranial to the tubules that become the ductuli efferentia of the testis may protrude off the epididymis as a polypoid vestige called the appendix epididymis (Fig. 4c). In addition, remnant mesonephric tubules can persist proximal to those draining the testicle as well. This remnant is known as the paradidymis (a.k.a. organ of Giraldés), a small collection of convoluted tubules lined by ciliated epithelium, that can be found anywhere along the epididymis or vas deferens. Torsion of the appendix testis, appendix epididymis, and paradidymis are all in the differential diagnosis of the acute scrotum. The appendix testis, appendix epididymis, and ectasia of the rete tubules can be visualized during the scrotal ultrasound and their characteristic appearance should be kept in mind to avoid confusion of these structures with testicular and extratesticular masses. Testicular Decent The process of testicular descent begins prior to 7 or 8 weeks in development. At this time, the gonadal position in the dorsal abdominal wall is similar in both sexes. In males, the fetal testis begins to produce MIS from the Sertoli cells. In addition, androgens and an insulin-like hormone 3 (INSL3) are produced from the Leydig cells. These hormones work in concert to control descent of the testis, which is held by a suspensory ligament at the upper pole, and, at the lower pole by the genitoinguinal ligament, or gubernaculum. During the initial phase of descent, the cranial ligament progresses and the gubernaculum thickens allowing the testis to be held near the inguinal region. At this time the inguinal canal forms as the abdominal wall muscles develop around the end of the gubernaculum. At about weeks an out-pouching of the peritoneal membrane, which is known as the processus vaginalis, travels with the testis toward its final position in the scrotum. The processus vaginalis maintains a connection with both the epididymal tail and the lower pole of the testis. At about 25 weeks, testis and attached processus vaginalis begin to pass through the inguinal canal along with fascial coverings from the abdominal wall (Fig. 5). The processus vaginalis is continuous with the peritoneum and tunica vaginalis of the testis. Between 25 and 30 weeks the testis descends rapidly through the inguinal canal and then more slowly across the pubis into the scrotum. The fascial coverings from the abdominal wall that travel with the testis during its descent become the layers covering the spermatic cord and testis. This process is usually completed by 35 weeks of gestation and it is followed by the obliteration of the proximal portion of the processus vaginalis to close the
6 16 G. Richards and B. R. Gilbert Embryonic position Transabdominal phase (8-15 wk) Anchoring Inguinoscrotal phase (25-35 wk) Migration Elongation of cord (0-10 yrs) Fig. 5 The phases of testicular descent. At about 25 weeks, testis and attached processus vaginalis begin to pass through the inguinal canal along with fascial coverings from the abdominal wall connection between the scrotum and peritoneum. Closure may occur during prenatal development or in early infancy. The gubernaculum does not become anchored to the scrotum until descent is completed [6 8]. The embryology of testicular descent becomes important for the sonographer when evaluating the undescended or nonpalpable testis. A majority of undescended testes are found in the inguinal canal which is accessible to diagnostic ultrasound [9 12]. This makes ultrasound examination of the inguinal region essential when a testis is not found on routine scrotal ultrasound. Scrotal Contents The scrotum contains bilateral compartments divided by a septum with multiple fascial layers beneath the skin and dartos fascia. The primary contents of each compartment are a testicle, an epididymis, and a spermatic cord (Fig. 6). The latter contains the ductus deferens, arteries, and veins (the pampiniform plexus). Each testis is covered by a thick, fibrous, connective tissue layer (tunica albuginea). The tunica albuginea is apposed to the visceral tunica vaginalis one of two, thinner connective tissue layers formed from the distal aspects of the processus vaginalis (Fig. 7). The other is the parietal tunica vaginalis which reflects back off the testicle from the visceral tunica vaginalis to surround the anterior, and lateral portions of the testis creating a cavity that normally contains a small amount of fluid. When this cavity contains more than the physiologic amount of fluid (1 2 ml), a hydrocele is present. Failure of the closure of the processus vaginalis allows peritoneal fluid to accumulate in the scrotum when it is in a dependent location, or when the
7 Embryology Relevant to Ultrasound Imaging of the Male Genitalia 17 Ductus deferens, Artery and veins Testicular artery and veins Epididymis Rete testis Tubuli recti Septae Seminiferous tubule Tunica albuginea covered by tunica vaginalis (Visceral layer) Scrotal wall a Tunica vaginalis (Parietal layer) b c Fig. 6 Cross sectional view of a testis demonstrating the locations of the visceral and parietal layers of the tunica vagnialis (a). Ultrasonogram of the testis demonstrating the tunica albugniea, which is apposed to the visceral portion of the tunica vaginalis (b). Photomicrograph of the spermatic tubules and tunica abuginea (c) intra-abdominal pressure rises. This is referred to as a communicating hydrocele. When blood collects in this cavity or in areas outside the parietal vaginalis, it constitutes a hematocele. Cystic dilations of the processus vaginalis maybe found within the spermatic cord on ultrasound examination and are referred to as hydroceles of the cord. Development of the Urogenital Sinus The cloaca is a chamber shared by the allantois (which extends anteriorly from the cloaca into the umbilical cord) and the hindgut. The cloacal membrane makes up the ventral wall of the chamber and is located at the caudal end of the developing hindgut as a bilaminar apposition of ectoderm and the endoderm located on the
8 18 G. Richards and B. R. Gilbert Fig. 7 The contents of the scrotum and spermatic cords. The primary contents of each compartment are a testicle, an epididymis, and a spermatic cord. The latter spermatic cord contains the vas deferens, arteries and veins (the pampiniform plexus) ventral midline. A septum develops as an ingrowth of folds from the lateral walls and a caudal extension of the intervening mesenchyme from the branch point of the allantois and hindgut, which ultimately divides the cloaca into the anterior/ventral urogenital sinus and the posterior/dorsal developing rectum. While the septum develops, mesodermal mesenchyme also encroaches between the two layers of the cloacal membrane. The septum also divides the membrane into a urogenital membrane and anal membrane. These membranes ultimately rupture to create continuity between the ectoderm and both the urogenital sinus and rectum. The mesenchymal tissues that have encroached develop into the muscles and bones of the lower anterior abdomen and pubis. An incompletely understood defect in this process results in the extrophy epispadius complex, a spectrum of abnormalities that can include continuities between the luminal surface of the bladder and the lower abdominal skin. If the defect occurs early enough in the process (before the complete division of the cloaca), a cloacal extrophy can occur which also includes a continuity of the intestinal lumen with the skin and bladder lumen. This is often found on prenatal ultrasound with an appearance that mimics the complete absence of a bladder in the fetus. These findings can also be a found with other penile anomalies.
9 Embryology Relevant to Ultrasound Imaging of the Male Genitalia 19 Fig. 8 Ultrasound of the bladder with the typical findings associated with posterior urethral valves including a thickened wall and dilated posterior urethra known as the keyhole sign [13] The urethra, prostate, and bladder all develop from the urogenital sinus. The remnants of the caudal ends of the mesonephric ducts become incorporated into the urogenital sinus (Mullerian Tubercle, Fig. 3) and become aspects of the trigone and posterior urethra. The incorporated portions of the mesonephric ducts include the branch points of the metanephric ducts, which become the ureteral orifices. The unincorporated portions of the mesonephric ducts end up entering the urethra at the prostatic urethra as the ejaculatory ducts. Ridges in the urethra, called plicae colliculi, remain along the path of the fusion of the mesonephric ducts as they become incorporated with the urogenital sinus and migrate while the sinus develops. It is hypothesized that abnormalities in this process result in the fusion of the plicae colliculi that is seen in the majority of posterior urethral valves. The remainder of posterior urethral valves are thought to result from an incomplete rupture of the urogenital membrane. Posterior urethral valves are associated with a dilated posterior urethra and thickened bladder wall on ultrasound (Fig. 8). The bladder is often distended with marked hydroureteronephrosis also demonstrated on ultrasound examination. Development of the Male External Genitalia and Phallus Up until the eighth or ninth week of gestational age, the development of the external male genitalia is indistinguishable with that of the female genitalia. It involves the development of the genital tubercles at the craniolateral edges of cloacal membrane. They develop from mesoderm as it infiltrates the cloacal membrane. As the cloaca membrane divides into the urogenital membrane, the tubercles fuse in the midline. This fusion can be disrupted and results in the bifid phallus that is sometimes seen in extrophy. The urogenital membranes and ultimately the urogenital sinus are flanked
10 20 G. Richards and B. R. Gilbert Fig. 9 The male external genital development progressing clockwise from the left. The genital tubercle develops into the glans penis. The upper right panel shows the urogenital sinus opening within the urogenital folds, which are between the scrotal swellings by collections of infiltrating mesoderm termed as the urogenital folds with labial scrotal swellings located laterally on either side (Fig. 9). Masculinization of the indifferent external genitalia occurs under the influence of testosterone produced by the interstitial cells of the fetal testis [14 16]. The tubercle becomes the future phallus and glans. The terminal part of the phallus destined to be the glans becomes solid. The grove between the urogenital folds, which extend onto the underside and with the tubercle as the tubercle grows, is termed the urogenital groove. The urogenital sinus extends to the under surface of the genital tubercle where it opens in this grove. Apical ridges of the urogenital folds grow toward each other and the walls of the phallic portion come together and fuse which creates a tubular extension of the urogenital sinus on the caudal aspect of the developing phallus. This opening is for a while the primitive urogenital opening, and it extends forward to the corona glandis and the final urethral meatus. The corpora cavernosa of the penis as well as the spongiosum surrounding the urethra arise from the mesodermal tissue in the phallus. They are at first dense structures, but later, vascular spaces appear in them, and they gradually become cavernous. A solid plate of ectoderm grows over the superficial part of the phallus. A bilayer of tissue is formed by a breakdown of the more centrally situated cells forming the prepuce. The scrotum is formed by extension of the labioscrotal swellings between the pelvic portion and the anus. With testicular decent these labioscrotal swellings form the scrotal sac.
11
under its influence, male development occurs; in its absence, female development is established.
 Sex differentiation is a complex process that involves many genes, including some that are autosomal. The key to sexual dimorphism is the Y chromosome, which contains the testis determining gene called
Sex differentiation is a complex process that involves many genes, including some that are autosomal. The key to sexual dimorphism is the Y chromosome, which contains the testis determining gene called
Development of the Genital System
 Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
10. Development of genital system. Gonads. Genital ducts. External genitalia.
 10. Development of genital system. Gonads. Genital ducts. External genitalia. Gonads, genital ducts and the external genital organs initially pass through an indifferent period of development, which is
10. Development of genital system. Gonads. Genital ducts. External genitalia. Gonads, genital ducts and the external genital organs initially pass through an indifferent period of development, which is
Development of the urogenital system
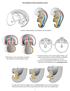 Development of the urogenital system Location of the pronephros, mesonephros and metanephros Differentiation of the intermedierm mesoderm into nephrotome and mesonephric tubules Connection between aorta
Development of the urogenital system Location of the pronephros, mesonephros and metanephros Differentiation of the intermedierm mesoderm into nephrotome and mesonephric tubules Connection between aorta
Urogenital system - Development. Aleš Hampl
 Urogenital system - Development Aleš Hampl cloaca Urogenital system Overall picture Urogenital system Reminder Urogenital system Intermediate mesoderm Urogenital system Early forms of kidneys - Pronephros
Urogenital system - Development Aleš Hampl cloaca Urogenital system Overall picture Urogenital system Reminder Urogenital system Intermediate mesoderm Urogenital system Early forms of kidneys - Pronephros
Urogenital System. PUMC Dept. of Anat. Hist. & Embry. 钱晓菁 XIAO-JING QIAN Dept. of Anatomy, Histology & Embryology Peking Union Medical College
 Urogenital System 钱晓菁 XIAO-JING QIAN Dept. of Anatomy, Histology & Embryology Peking Union Medical College intermediate mesoderm urogenital ridge mesonephric ridge genital ridge I. Urinary System 1. kidney
Urogenital System 钱晓菁 XIAO-JING QIAN Dept. of Anatomy, Histology & Embryology Peking Union Medical College intermediate mesoderm urogenital ridge mesonephric ridge genital ridge I. Urinary System 1. kidney
Urinary system development. Male ( ) and Female ( ) Reproductive Systems Development
 Urinary system development Male ( ) and Female ( ) Reproductive Systems Development Urogenital system develops from mesodermal uro-genital ridge (intermediate mesoderm) development of male and female genital
Urinary system development Male ( ) and Female ( ) Reproductive Systems Development Urogenital system develops from mesodermal uro-genital ridge (intermediate mesoderm) development of male and female genital
W.S. O University of Hong Kong
 W.S. O University of Hong Kong Development of the Genital System 1. Sexual differentiation 2. Differentiation of the gonads a. Germ cells extragonadal in origin b. Genital ridge intermediate mesoderm consisting
W.S. O University of Hong Kong Development of the Genital System 1. Sexual differentiation 2. Differentiation of the gonads a. Germ cells extragonadal in origin b. Genital ridge intermediate mesoderm consisting
Development of Urinary System
 Jordan University Faculty Of Medicine Development of Urinary System Dr. Ahmed Salman Assistant professor of anatomy & embryology Development of the upper urinary system It is developed from the intraembryonic
Jordan University Faculty Of Medicine Development of Urinary System Dr. Ahmed Salman Assistant professor of anatomy & embryology Development of the upper urinary system It is developed from the intraembryonic
Sexual differentiation is sequential process:
 Genital lsystem J. H. Lue Sexual differentiation is sequential process:.genetic (chromosomal) sex -- determined at fertilization.gonad sex -- is differentiated after 7th week.phenotypic sex -- under normal
Genital lsystem J. H. Lue Sexual differentiation is sequential process:.genetic (chromosomal) sex -- determined at fertilization.gonad sex -- is differentiated after 7th week.phenotypic sex -- under normal
Development of Urinary System
 Jordan University Faculty Of Medicine Development of Urinary System DR. AHMED SALMAN ASSISTANT PROFESSOR OF ANATOMY & EMBRYOLOGY Development of The kidney Dr Ahmed Salman Development of the upper urinary
Jordan University Faculty Of Medicine Development of Urinary System DR. AHMED SALMAN ASSISTANT PROFESSOR OF ANATOMY & EMBRYOLOGY Development of The kidney Dr Ahmed Salman Development of the upper urinary
Midgut. Over its entire length the midgut is supplied by the superior mesenteric artery
 Gi Embryology 3 Midgut the midgut is suspended from the dorsal abdominal wall by a short mesentery and communicates with the yolk sac by way of the vitelline duct or yolk stalk Over its entire length the
Gi Embryology 3 Midgut the midgut is suspended from the dorsal abdominal wall by a short mesentery and communicates with the yolk sac by way of the vitelline duct or yolk stalk Over its entire length the
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE
 ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
M. Al-Mohtaseb. Tala Saleh. Faisal Nimri
 4 5 M. Al-Mohtaseb Tala Saleh Faisal Nimri Inguinal Hernia - An abdominal hernia is the protrusion of part of the abdominal content beyond the normal confines of the abdominal wall through weak points
4 5 M. Al-Mohtaseb Tala Saleh Faisal Nimri Inguinal Hernia - An abdominal hernia is the protrusion of part of the abdominal content beyond the normal confines of the abdominal wall through weak points
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM
 Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Biology 224 Human Anatomy and Physiology II Week 9; Lecture 2; Wednesday Stuart Sumida. Development and Structure, of the Reproductive System
 Biology 224 Human Anatomy and Physiology II Week 9; Lecture 2; Wednesday Stuart Sumida Development and Structure, of the Reproductive System Don t forget the relationships of the structures of the layers
Biology 224 Human Anatomy and Physiology II Week 9; Lecture 2; Wednesday Stuart Sumida Development and Structure, of the Reproductive System Don t forget the relationships of the structures of the layers
Development of the urinary system
 Development of the urinary system WSO School of Biomedical Sciences, University of Hong Kong. 3 sets of kidneys developing in succession (temporally and spatially) : Pronephros ] Mesonephros ]- Intermediate
Development of the urinary system WSO School of Biomedical Sciences, University of Hong Kong. 3 sets of kidneys developing in succession (temporally and spatially) : Pronephros ] Mesonephros ]- Intermediate
Embryology /organogenesis/ Week 4 Development and teratology of reproductive system.
 Embryology /organogenesis/ Week 4 Development and teratology of reproductive system. Male or female sex is determined by spermatozoon Y in the moment of fertilization SRY gene, on the short arm of the
Embryology /organogenesis/ Week 4 Development and teratology of reproductive system. Male or female sex is determined by spermatozoon Y in the moment of fertilization SRY gene, on the short arm of the
Male Reproductive System. Dr Maan Al-Abbasi PhD, MSc, MBChB, MD
 Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Development of the Urinary System
 Development of the Urinary System Lecture Objectives Understand the development of the kidney and related organs of the urinary system. Define the pronephrons, mesonephrons and metanephrons. Understand
Development of the Urinary System Lecture Objectives Understand the development of the kidney and related organs of the urinary system. Define the pronephrons, mesonephrons and metanephrons. Understand
Development of the Urinary System. 3 Distinct Embryonic Kidney Structures
 Development of the Urinary System Excretory portion of urinary system derived from intermediate mesoderm Week 4: 1 st nephrons/renal corpuscles form Nephrotomes form and develop hollow lumens to form nephric
Development of the Urinary System Excretory portion of urinary system derived from intermediate mesoderm Week 4: 1 st nephrons/renal corpuscles form Nephrotomes form and develop hollow lumens to form nephric
Obstetrics Content Outline Obstetrics - Fetal Abnormalities
 Obstetrics Content Outline Obstetrics - Fetal Abnormalities Effective February 2007 10 16% renal agenesis complete absence of the kidneys occurs when ureteric buds fail to develop Or degenerate before
Obstetrics Content Outline Obstetrics - Fetal Abnormalities Effective February 2007 10 16% renal agenesis complete absence of the kidneys occurs when ureteric buds fail to develop Or degenerate before
Urinary System. ectoderm. notochord. mesonephric tubules. Nephrogenic Cord (left)
 Urinary System NOTE: Urine proion requires an increased capillary surface area (glomeruli), epithelial s to collect plasma filtrate and extract desirable constituents, and a system to convey urine away
Urinary System NOTE: Urine proion requires an increased capillary surface area (glomeruli), epithelial s to collect plasma filtrate and extract desirable constituents, and a system to convey urine away
DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS
 8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
Animal Science 434 Reproductive Physiology"
 Animal Science 434 Reproductive Physiology" Embryogenesis of the Pituitary and Sexual Development: Part A Development of the Pituitary Gland" Infundibulum" Brain" Rathke s Pouch" Stomodeum" Germ Cell Migration"
Animal Science 434 Reproductive Physiology" Embryogenesis of the Pituitary and Sexual Development: Part A Development of the Pituitary Gland" Infundibulum" Brain" Rathke s Pouch" Stomodeum" Germ Cell Migration"
حسام أبو عوض. -Dr. Mohammad Muhtasib. 1 P a g e
 5 حسام أبو عوض - -Dr. Mohammad Muhtasib 1 P a g e There are two types of inguinal hernia: direct and indirect. Hernia: protrusion of the small intestine or the greater omentum of the intra-abdominal organs
5 حسام أبو عوض - -Dr. Mohammad Muhtasib 1 P a g e There are two types of inguinal hernia: direct and indirect. Hernia: protrusion of the small intestine or the greater omentum of the intra-abdominal organs
11. SEXUAL DIFFERENTIATION. Germinal cells, gonocytes. Indifferent stage INDIFFERENT STAGE
 11. SEXUAL DIFFERENTIATION INDIFFERENT STAGE Early in pregnancy, (within 10-15 % of the pregnancy s expected length) a genital ridge is formed in the sides of the embryonic tissue, ventral to the mesonephros
11. SEXUAL DIFFERENTIATION INDIFFERENT STAGE Early in pregnancy, (within 10-15 % of the pregnancy s expected length) a genital ridge is formed in the sides of the embryonic tissue, ventral to the mesonephros
Primary sex organs (gonads): testes and ovaries. Accessory reproductive organs: ducts, glands, and external genitalia
 Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Embryology of the Female Reproductive Tract
 Embryology of the Female Reproductive Tract Andrew Healey Contents 1 Introduction... 21 2 Embryology of the Female Genitourinary Tract... 22 2.1 Development of the Gonads... 22 2.2 Relationship Between
Embryology of the Female Reproductive Tract Andrew Healey Contents 1 Introduction... 21 2 Embryology of the Female Genitourinary Tract... 22 2.1 Development of the Gonads... 22 2.2 Relationship Between
The Repr duct ve System. Function: producing offspring
 The Repr duct ve System Function: producing offspring Anatomy of male reproductive system Location: The reproductive organs are classified as external and internal genitalia. The external genitalia are
The Repr duct ve System Function: producing offspring Anatomy of male reproductive system Location: The reproductive organs are classified as external and internal genitalia. The external genitalia are
Male Anatomy. testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics
 Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
Animal Science 434 Reproductive Physiology
 Animal Science 434 Reproductive Physiology Development of the Pituitary Gland Lec 5: Embryogenesis of the Pituitary and Sexual Development Stomodeum Brain Infundibulum Rathke s Pouch Germ Cell Migration
Animal Science 434 Reproductive Physiology Development of the Pituitary Gland Lec 5: Embryogenesis of the Pituitary and Sexual Development Stomodeum Brain Infundibulum Rathke s Pouch Germ Cell Migration
Urinary System. J. H. Lue. intermediate mesoderm cloaca coelomic epithelium
 Urinary System J. H. Lue Primordium: intermediate mesoderm cloaca coelomic epithelium 1 3w(18d) 3 w 4w (24d) 4w (26d) 2 Intermediate mesoderm 3 Intermediate mesoderm intermediate mesoderm urogenital ridge
Urinary System J. H. Lue Primordium: intermediate mesoderm cloaca coelomic epithelium 1 3w(18d) 3 w 4w (24d) 4w (26d) 2 Intermediate mesoderm 3 Intermediate mesoderm intermediate mesoderm urogenital ridge
Male Reproductive System Dr. Gary Mumaugh
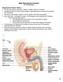 Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception
 PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
أحمد رواجبة- محمود الحربي- أحمد السالمان-
 -6 أحمد رواجبة- محمود الحربي- أحمد السالمان- 1 P a g e The Male Reproductive System The male genital system structures are divided into: Internal structures: 1- Prostate 3-Ejaculatory ducts External structures:
-6 أحمد رواجبة- محمود الحربي- أحمد السالمان- 1 P a g e The Male Reproductive System The male genital system structures are divided into: Internal structures: 1- Prostate 3-Ejaculatory ducts External structures:
Inguinal Canal. It is an oblique passage through the lower part of the anterior abdominal wall. Present in both sexes
 Inguinal canal Inguinal Canal It is an oblique passage through the lower part of the anterior abdominal wall Present in both sexes It allows structures to pass to and from the testis to the abdomen in
Inguinal canal Inguinal Canal It is an oblique passage through the lower part of the anterior abdominal wall Present in both sexes It allows structures to pass to and from the testis to the abdomen in
Pelvis MCQs. Block 1. B. Reproductive organs. C. The liver. D. Urinary bladder. 1. The pelvic diaphragm includes the following muscles: E.
 Pelvis MCQs Block 1 1. The pelvic diaphragm includes the following muscles: A. The obturator internus B. The levator ani C. The coccygeus D. The external urethral sphincter E. The internal urethral sphincter
Pelvis MCQs Block 1 1. The pelvic diaphragm includes the following muscles: A. The obturator internus B. The levator ani C. The coccygeus D. The external urethral sphincter E. The internal urethral sphincter
Development of the Digestive System. W.S. O The University of Hong Kong
 Development of the Digestive System W.S. O The University of Hong Kong Plan for the GI system Then GI system in the abdomen first develops as a tube suspended by dorsal and ventral mesenteries. Blood
Development of the Digestive System W.S. O The University of Hong Kong Plan for the GI system Then GI system in the abdomen first develops as a tube suspended by dorsal and ventral mesenteries. Blood
Genitourinary System Imaging- Based Overview of Anatomy and Embryology. Sameer Ahmed, MS IV 9/8/11
 Genitourinary System Imaging- Based Overview of Anatomy and Embryology Sameer Ahmed, MS IV 9/8/11 ObjecDves Review very high- yield concepts Anatomy test + USMLE Step 1 GU Embryology How it relates directly
Genitourinary System Imaging- Based Overview of Anatomy and Embryology Sameer Ahmed, MS IV 9/8/11 ObjecDves Review very high- yield concepts Anatomy test + USMLE Step 1 GU Embryology How it relates directly
Scrotum Kacey Morrison Amanda Baxter Sabrina Tucker July 18, 2006 SCROTUM
 Scrotum Kacey Morrison Amanda Baxter Sabrina Tucker July 18, 2006 SCROTUM 1) Other Names: Scrotum None Testicles Testes (Curry Tempkin, p. 236, 2/3/2) Ductus deferens spermatic cord (Tempkin, p. 279, Anatomy
Scrotum Kacey Morrison Amanda Baxter Sabrina Tucker July 18, 2006 SCROTUM 1) Other Names: Scrotum None Testicles Testes (Curry Tempkin, p. 236, 2/3/2) Ductus deferens spermatic cord (Tempkin, p. 279, Anatomy
Development of the Digestive System. W.S. O School of Biomedical Sciences, University of Hong Kong.
 Development of the Digestive System W.S. O School of Biomedical Sciences, University of Hong Kong. Organization of the GI tract: Foregut (abdominal part) supplied by coeliac trunk; derivatives include
Development of the Digestive System W.S. O School of Biomedical Sciences, University of Hong Kong. Organization of the GI tract: Foregut (abdominal part) supplied by coeliac trunk; derivatives include
PHYSIOLOGY AND PATHOLOGY OF SEXUAL DIFFERENTIATION
 PHYSIOLOGY AND PATHOLOGY OF SEXUAL DIFFERENTIATION Prof. Dr med. Jolanta Słowikowska-Hilczer Department of Andrology and Reproductive Endocrinology Medical University of Łódź, Poland Sexual determination
PHYSIOLOGY AND PATHOLOGY OF SEXUAL DIFFERENTIATION Prof. Dr med. Jolanta Słowikowska-Hilczer Department of Andrology and Reproductive Endocrinology Medical University of Łódź, Poland Sexual determination
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
DEVELOPMENT OF THE ADRENAL GLAND; TESTES AND MESONEPHRIC DUCT. Reading Assignment: The Developing Human, Clinically Oriented Embryology pp
 Developmental Anatomy Steven M. Hill, Ph.D. 9/16/13 DEVELOPMENT OF THE ADRENAL GLAND; TESTES AND MESONEPHRIC DUCT Reading Assignment: The Developing Human, Clinically Oriented Embryology pp. 264-273. Objectives:
Developmental Anatomy Steven M. Hill, Ph.D. 9/16/13 DEVELOPMENT OF THE ADRENAL GLAND; TESTES AND MESONEPHRIC DUCT Reading Assignment: The Developing Human, Clinically Oriented Embryology pp. 264-273. Objectives:
FORMS OF EMBRYONIC PRIMORDIA
 FORMS OF EMBRYONIC PRIMORDIA BY PROF. ANTHONY OBIOMA NWAOPARA UNIVERSITY OF MEDICAL SCIENCES ONDO CITY, ONDO STATE LEARNING OBJECTIVES To recognise the different forms of embryonic primordia. To recognise
FORMS OF EMBRYONIC PRIMORDIA BY PROF. ANTHONY OBIOMA NWAOPARA UNIVERSITY OF MEDICAL SCIENCES ONDO CITY, ONDO STATE LEARNING OBJECTIVES To recognise the different forms of embryonic primordia. To recognise
MALE REPRODUCTIVE SYSTEM
 MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
Reproductive System. Where it all begins
 Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
The Male Reproductive System
 The Male Reproductive System YONG-MEI CHEN ( 陈咏梅 ) Dept. of Anatomy, Histology & Embryology Peking Union Medical College Tel:69156461 E-mail address: pumc_he@126.com Content Spermatogenesis Spermiogenesis
The Male Reproductive System YONG-MEI CHEN ( 陈咏梅 ) Dept. of Anatomy, Histology & Embryology Peking Union Medical College Tel:69156461 E-mail address: pumc_he@126.com Content Spermatogenesis Spermiogenesis
Anatomy Lecture Notes Chapter 24
 primary sex organs = gonads produce gametes secrete hormones that control reproduction secondary sex organs = accessory structures Development and Differentiation A. gonads develop from mesoderm starting
primary sex organs = gonads produce gametes secrete hormones that control reproduction secondary sex organs = accessory structures Development and Differentiation A. gonads develop from mesoderm starting
The Reproductive System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
The Reproductive System
 16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
Sexual differentiation:
 Abnormal Development of Female Genitalia Dr. Maryam Fetal development of gonads, external genitalia, Mullerian ducts and Wolffian ducts can be disrupted at a variety of points, leading to a wide range
Abnormal Development of Female Genitalia Dr. Maryam Fetal development of gonads, external genitalia, Mullerian ducts and Wolffian ducts can be disrupted at a variety of points, leading to a wide range
The functional anatomy of the urinary system. Human Anatomy Department Dr. Anastasia Bendelic
 The functional anatomy of the urinary system Human Anatomy Department Dr. Anastasia Bendelic Plan Development of the kidneys and their abnormalities Development of the urinary ways and their abnormalities
The functional anatomy of the urinary system Human Anatomy Department Dr. Anastasia Bendelic Plan Development of the kidneys and their abnormalities Development of the urinary ways and their abnormalities
Sex Determination and Development of Reproductive Organs
 Sex Determination and Development of Reproductive Organs Sex determination The SRY + gene is necessary and probably sufficient for testis development The earliest sexual difference appears in the gonad
Sex Determination and Development of Reproductive Organs Sex determination The SRY + gene is necessary and probably sufficient for testis development The earliest sexual difference appears in the gonad
Male Reproductive System
 Male Reproductive System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Male Reproductive System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Embryology - GIT - Lecture 2
 Embryology - GIT - Lecture 2 Last time we talked about embryology of the GIT. We said that the development of the stomach is accompanied with the development of the duodenum and the pancreas. Also we talked
Embryology - GIT - Lecture 2 Last time we talked about embryology of the GIT. We said that the development of the stomach is accompanied with the development of the duodenum and the pancreas. Also we talked
The Male and Female Internal Genitalia. Dr Oluwadiya Kehinde
 The Male and Female Internal Genitalia Dr Oluwadiya Kehinde www.oluwadiya.com Overview The reproductive role of the male is to produce sperm, deliver them to the female Primary sex organs are the gonads
The Male and Female Internal Genitalia Dr Oluwadiya Kehinde www.oluwadiya.com Overview The reproductive role of the male is to produce sperm, deliver them to the female Primary sex organs are the gonads
Fig General Structural Features of a kidney
 Chapter 11 Development of the Mesodermal Organs in Vertebrates 11.1. Subdivisions of the Mesoderm There are 4 subdivisions of the mesoderm: 1. The Notochord develops into the centrum of the vertebral column.
Chapter 11 Development of the Mesodermal Organs in Vertebrates 11.1. Subdivisions of the Mesoderm There are 4 subdivisions of the mesoderm: 1. The Notochord develops into the centrum of the vertebral column.
The Scrotum & Testes Prof. Dr. Imran Qureshi
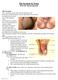 The Scrotum & Testes Prof. Dr. Imran Qureshi The Scrotum It is a cutaneous pouch of the anterior abdominal wall. Most layers of the abdominal wall are represented in its structure. It contains the testes
The Scrotum & Testes Prof. Dr. Imran Qureshi The Scrotum It is a cutaneous pouch of the anterior abdominal wall. Most layers of the abdominal wall are represented in its structure. It contains the testes
Systematic Anatomy. Shanghai Medical College,Fudan University. Dr.Hongqi Zhang ( 张红旗 )
 Systematic Anatomy Department of Anatomy,Histology & Embryology Shanghai Medical College,Fudan University Dr.Hongqi Zhang ( 张红旗 ) Email: zhanghq58@yahoo.com.cn Office: Building 9,Room308, 54237151-9308
Systematic Anatomy Department of Anatomy,Histology & Embryology Shanghai Medical College,Fudan University Dr.Hongqi Zhang ( 张红旗 ) Email: zhanghq58@yahoo.com.cn Office: Building 9,Room308, 54237151-9308
MALE REPRODUCTIVE SYSTEM
 MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
Lab #9: Kidney: Gross Anatomy & Histology
 Name Date Lab #9: Kidney: Gross Anatomy & Histology Lab #10: Male Reproductive System: Human Models & Histology Lab #11: Female Reproductive System: Human Models & Histology Stuff to Know Dr. L. Bacha
Name Date Lab #9: Kidney: Gross Anatomy & Histology Lab #10: Male Reproductive System: Human Models & Histology Lab #11: Female Reproductive System: Human Models & Histology Stuff to Know Dr. L. Bacha
SUBJECTS 2nd year, 1st semester I. 1. Primitive gut - limits, derivatives 2. Foregut -limits, evolution, derivatives 3. Midgut -limits, evolution,
 SUBJECTS 2nd year, 1st semester I. 1. Primitive gut - limits, derivatives 2. Foregut -limits, evolution, derivatives 3. Midgut -limits, evolution, derivatives 4. Hindgut- limits, evolution, derivatives
SUBJECTS 2nd year, 1st semester I. 1. Primitive gut - limits, derivatives 2. Foregut -limits, evolution, derivatives 3. Midgut -limits, evolution, derivatives 4. Hindgut- limits, evolution, derivatives
Development of the female Reproductive System. Dr. Susheela Rani
 Development of the female Reproductive System Dr. Susheela Rani Genital System Gonads Internal genitals External genitals Determining sex chronology of events Genetic sex Determined at fertilization Gonadal
Development of the female Reproductive System Dr. Susheela Rani Genital System Gonads Internal genitals External genitals Determining sex chronology of events Genetic sex Determined at fertilization Gonadal
Development of the Urinary System
 Development of the Urinary System ## every things is written in this sheet so u don t have to go back to the slide. ## I write everything and I hope everything will be clear,, if some note doesn t clear
Development of the Urinary System ## every things is written in this sheet so u don t have to go back to the slide. ## I write everything and I hope everything will be clear,, if some note doesn t clear
REPRODUCTIVE SYSTEM By Dr.Ahmed Salman
 The University Of Jordan Faculty Of Medicine Anatomy Department REPRODUCTIVE SYSTEM By Dr.Ahmed Salman Assistant Professor of Anatomy &embryology Male genital system Learning Objectives 1. Identify External
The University Of Jordan Faculty Of Medicine Anatomy Department REPRODUCTIVE SYSTEM By Dr.Ahmed Salman Assistant Professor of Anatomy &embryology Male genital system Learning Objectives 1. Identify External
Embryology of the Midgut and Hind gut
 Embryology of the Midgut and Hind gut Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E-mail: abdulameerh@yahoo.com Abdominal organs www.google.co.uk/search? Development of Duodenum The
Embryology of the Midgut and Hind gut Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E-mail: abdulameerh@yahoo.com Abdominal organs www.google.co.uk/search? Development of Duodenum The
Pelvis Perineum MCQs. Block 1.1. A. Urinary bladder. B. Rectum. C. Reproductive organs. D. The thigh
 Pelvis Perineum MCQs Block 1.1 1. The pelvic diaphragm includes the following muscles: A. The coccygeus B. The levator ani C. The external urethral sphincter D. The internal urethral sphincter E. The obturator
Pelvis Perineum MCQs Block 1.1 1. The pelvic diaphragm includes the following muscles: A. The coccygeus B. The levator ani C. The external urethral sphincter D. The internal urethral sphincter E. The obturator
Anatomy & Physiology: Testis Penis. Hosam Serag ST7 Urology University Hospital of Wales
 Anatomy & Physiology: Testis Penis Hosam Serag ST7 Urology University Hospital of Wales Testis Dimensions: 4 to 5 cm long 3 cm wide 2.5 cm deep volume of 30 ml Prader Orchidometer Layers Visceral tunica
Anatomy & Physiology: Testis Penis Hosam Serag ST7 Urology University Hospital of Wales Testis Dimensions: 4 to 5 cm long 3 cm wide 2.5 cm deep volume of 30 ml Prader Orchidometer Layers Visceral tunica
The Acute Scrotum: Sonographic Findings
 The Acute Scrotum: Sonographic Findings 가천의대길병원방사선과 양달모 Gachon Medical School Introduction Many diseases presenting as acute scrotal pain DDx is important for determining the appropriate treatment US with
The Acute Scrotum: Sonographic Findings 가천의대길병원방사선과 양달모 Gachon Medical School Introduction Many diseases presenting as acute scrotal pain DDx is important for determining the appropriate treatment US with
LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM
 LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM Slide #101 (1096). Testis, rat. sustentacular ( Sertoli ) cells Nuclei of Sustentacular cells Leydig cells Spermatogonia Spermatocytes Spermatids pale
LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM Slide #101 (1096). Testis, rat. sustentacular ( Sertoli ) cells Nuclei of Sustentacular cells Leydig cells Spermatogonia Spermatocytes Spermatids pale
Surgical management of the undescended testis is performed
 Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase
 Human Sexuality Exam II Review Material Gametogenesis: Oogenesis 1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase 2. Know the relative
Human Sexuality Exam II Review Material Gametogenesis: Oogenesis 1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase 2. Know the relative
The embryonic endoderm initially is widely connected with the yolk sac. As a consequence of cephalocaudal and lateral folding, a portion of the
 DIGESTIVE SYSTEM The embryonic endoderm initially is widely connected with the yolk sac. As a consequence of cephalocaudal and lateral folding, a portion of the endoderm-lined yolk sac cavity is incorporated
DIGESTIVE SYSTEM The embryonic endoderm initially is widely connected with the yolk sac. As a consequence of cephalocaudal and lateral folding, a portion of the endoderm-lined yolk sac cavity is incorporated
Yes, cranially with ovarian, caudally with vaginal. Yes, with uterine artery (collateral circulation between abdominal +pelvic source)
 Blood supply to internal female genitalia: uterine Internal iliac Sup. large branch: uterus, inf. Small branch: cervix+ sup. Vagina Yes, cranially with ovarian, caudally with vaginal Medially in base of
Blood supply to internal female genitalia: uterine Internal iliac Sup. large branch: uterus, inf. Small branch: cervix+ sup. Vagina Yes, cranially with ovarian, caudally with vaginal Medially in base of
Lab Schedule for Rest of Semester
 Laboratory 9 Cat Dissection II Respiratory Urinary/Reproductive Systems Lab Schedule for Rest of Semester Cat dissection labs Dissection II (today) Respiratory (Ex. 57 in Hole) Human Reproductive Systems
Laboratory 9 Cat Dissection II Respiratory Urinary/Reproductive Systems Lab Schedule for Rest of Semester Cat dissection labs Dissection II (today) Respiratory (Ex. 57 in Hole) Human Reproductive Systems
Development of pancreas and Small Intestine. ANATOMY DEPARTMENT DR.SANAA AL-AlSHAARAWY DR.ESSAM Eldin Salama
 Development of pancreas and Small Intestine ANATOMY DEPARTMENT DR.SANAA AL-AlSHAARAWY DR.ESSAM Eldin Salama OBJECTIVES At the end of the lecture, the students should be able to : Describe the development
Development of pancreas and Small Intestine ANATOMY DEPARTMENT DR.SANAA AL-AlSHAARAWY DR.ESSAM Eldin Salama OBJECTIVES At the end of the lecture, the students should be able to : Describe the development
The Male Reproductive System
 The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
Comparative Anatomy Urogenital System. Note Set 11 Chapter 15
 Comparative Anatomy Urogenital System Note Set 11 Chapter 15 Urogenital System Ducts of excretory and reproductive systems are intimately associated Figure 14.1: Embryonic and evolutionary development
Comparative Anatomy Urogenital System Note Set 11 Chapter 15 Urogenital System Ducts of excretory and reproductive systems are intimately associated Figure 14.1: Embryonic and evolutionary development
Chapter 2 Development of the Male Reproductive System
 Chapter 2 Development of the Male Reproductive System 1 2 Pravin K. Rao and Arthur L. Burnett 3 Abstract Male and female reproductive systems develop in close relation to the urinary tract. Until approximately
Chapter 2 Development of the Male Reproductive System 1 2 Pravin K. Rao and Arthur L. Burnett 3 Abstract Male and female reproductive systems develop in close relation to the urinary tract. Until approximately
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Male Reproductive System
 Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Chapter 26: Reproductive Systems. Male 11/29/2015. Male reproductive system is composed of... BIO 218 Fall Gonads (testes)
 Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 22 Reproductive Systems. Male Reproductive Organs. Male Reproductive Organs. Specialized to produce, maintain the male sex cells (sperm)
 Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
Normal and Abnormal Development of the Genital Tract. Dr.Raghad Abdul-Halim
 Normal and Abnormal Development of the Genital Tract Dr.Raghad Abdul-Halim objectives: Revision of embryology. Clinical presentation, investigations and clinical significance of most common developmental
Normal and Abnormal Development of the Genital Tract Dr.Raghad Abdul-Halim objectives: Revision of embryology. Clinical presentation, investigations and clinical significance of most common developmental
MALE REPRODUCTIVE SYSTEM
 1 MALE REPRODUCTIVE SYSTEM SCPA 602 Anatomical Basis for Pathological Study Updated: 20.09.2018 Lect. Nisamanee Charoenchon, PhD nisamanee.cha@mahidol.ac.th Department of Pathobiology, Mahidol University
1 MALE REPRODUCTIVE SYSTEM SCPA 602 Anatomical Basis for Pathological Study Updated: 20.09.2018 Lect. Nisamanee Charoenchon, PhD nisamanee.cha@mahidol.ac.th Department of Pathobiology, Mahidol University
Development of the Liver and Pancreas
 Development of the Liver and Pancreas Professor Alfred Cuschieri Department of Anatomy University of Malta Three glandular buds arise from the distal end of the foregut during the fourth week Day 22 -The
Development of the Liver and Pancreas Professor Alfred Cuschieri Department of Anatomy University of Malta Three glandular buds arise from the distal end of the foregut during the fourth week Day 22 -The
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
The Urinary System Pearson Education, Inc.
 26 The Urinary System Introduction The urinary system does more than just get rid of liquid waste. It also: Regulates plasma ion concentrations Regulates blood volume and blood pressure Stabilizes blood
26 The Urinary System Introduction The urinary system does more than just get rid of liquid waste. It also: Regulates plasma ion concentrations Regulates blood volume and blood pressure Stabilizes blood
Biology of Reproduction-Biol 326
 Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
Biology 340 Comparative Embryology Lecture 10 Dr. Stuart Sumida. Further Development of the Mesoderm (and Endoderm)
 Biology 340 Comparative Embryology Lecture 10 Dr. Stuart Sumida Further Development of the Mesoderm (and Endoderm) Further Development: Digestive System Foregut, Midgut, Hindgut Heart and Aortic Arches
Biology 340 Comparative Embryology Lecture 10 Dr. Stuart Sumida Further Development of the Mesoderm (and Endoderm) Further Development: Digestive System Foregut, Midgut, Hindgut Heart and Aortic Arches
Lesson 31. Lesson Outline:
 Lesson 31 Lesson Outline: The Urogenital System Urinary System o Embryonic Origins o Phylogenetic Trends Function Urinary Bladder Implications for the Evolution of the Vertebrates o Freshwater or Seawater
Lesson 31 Lesson Outline: The Urogenital System Urinary System o Embryonic Origins o Phylogenetic Trends Function Urinary Bladder Implications for the Evolution of the Vertebrates o Freshwater or Seawater
Chapter 6: Genitourinary and Gastrointestinal Systems 93
 Chapter 6: Genitourinary and Gastrointestinal Systems 93 Chapter 6 Genitourinary and Gastrointestinal Systems Embryology Three sets of excretory organs or kidneys develop in human embryos: Pronephros:
Chapter 6: Genitourinary and Gastrointestinal Systems 93 Chapter 6 Genitourinary and Gastrointestinal Systems Embryology Three sets of excretory organs or kidneys develop in human embryos: Pronephros:
Imaging Ejaculatory Disorders and Hematospermia
 ATHENS 4-6 October 2018 European Society of Urogenital Radiology Imaging Ejaculatory Disorders and Hematospermia Parvati Ramchandani, MD Professor, Radiology and Surgery University of Pennsylvania Medical
ATHENS 4-6 October 2018 European Society of Urogenital Radiology Imaging Ejaculatory Disorders and Hematospermia Parvati Ramchandani, MD Professor, Radiology and Surgery University of Pennsylvania Medical
BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS
 BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS External oblique muscle Muscular portion Aponeurotic portion Superficial inguinal ring Lateral (inferior) crus Medial
BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS External oblique muscle Muscular portion Aponeurotic portion Superficial inguinal ring Lateral (inferior) crus Medial
2. Which of the following factors does not contribute to ion selectivity?
 General Biology Summer 2014 Exam II Sample Answers 1. Which of the following is TRUE about a neuron at rest? A. The cytosol is positive relative to the outside B. Na+ concentrations are higher inside C.
General Biology Summer 2014 Exam II Sample Answers 1. Which of the following is TRUE about a neuron at rest? A. The cytosol is positive relative to the outside B. Na+ concentrations are higher inside C.
Human Sexuality - Ch. 2 Sexual Anatomy (Hock)
 Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Histology of Male Reproductive system (1)
 Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
