Citation for the original published paper (version of record):
|
|
|
- Neal Asher Bryant
- 6 years ago
- Views:
Transcription
1 This is the published version of a paper published in BJU International. Citation for the original published paper (version of record): Carlsson, S., Drevin, L., Loeb, S., Widmark, A., Franck Lissbrant, I. et al. (2016) Population-based study of long-term functional outcomes after prostate cancer treatment. BJU International, 117(6B): E36-E45 Access to the published version may require subscription. N.B. When citing this work, cite the original published paper. Permanent link to this version:
2 Population-based study of long-term functional outcomes after prostate cancer treatment Sigrid Carlsson*, Linda Drevin, Stacy Loeb, Anders Widmark, Ingela Franck Lissbrant**, David Robinson, Eva Johansson,P ar Stattin and Per Fransson *Department of Surgery, Urology Service, Memorial Sloan-Kettering Cancer Center, New York, NY, USA, Department of Urology, Sahlgrenska Academy at G oteborg University, G oteborg, Regional Cancer Center, Uppsala University Hospital, Uppsala, Sweden, New York University and Manhattan Veterans Affairs Medical Center, New York, NY, USA, Department of Radiation Sciences, Oncology, Umea University, Umea, **Department of Oncology, Sahlgrenska Academy at G oteborg University, G oteborg, Department of Surgery and Perioperative Sciences, Urology and Andrology, Umea University Hospital, Umea, Department of Urology, Ryhov County Hospital, J onk oping, Department of Surgical Sciences, University Hospital of Uppsala, Uppsala, and Department of Nursing, Umea University, Umea, Sweden Objective To evaluate long-term urinary, sexual and bowel functional outcomes after prostate cancer treatment at a median (interquartile range) follow-up of 12 (11 13) years. Patients and Methods In this nationwide, population-based study, we identified men diagnosed with localized prostate cancer (clinical local stage T1 2, any Gleason score, prostate-specific antigen <20 ng/ml, NX or N0, MX or M0) between 1997 and 2002 from the National Prostate Cancer Register, Sweden. The men were aged 70 years at diagnosis. A control group of men without prostate cancer were also selected, matched for age and county of residence. Functional outcomes were evaluated with a validated self-reported questionnaire. Results Responses were obtained from 3 937/6 003 cases (66%) and 459/1 000 (46%) controls. At 12 years after diagnosis and at a median age of 75 years, the proportion of cases with adverse symptoms was 87% for erectile dysfunction/sexual inactivity, 20% for urinary incontinence and 14% for bowel disturbances. The corresponding proportions for controls were 62, 6 and 7%, respectively. Men with prostate cancer, except those on surveillance, had an increased risk of erectile dysfunction compared with the men in the control group. Radical prostatectomy was associated with an increased risk of urinary incontinence (odds ratio [OR] 1.89, 95% confidence interval [CI] ) and radiotherapy increased the risk of bowel dysfunction (OR 2.46, 95% CI ) compared with men in the control group. Multimodal treatment, in particular treatment including androgen deprivation therapy (), was associated with the highest risk of adverse effects; for instance, radical prostatectomy followed by radiotherapy and was associated with an OR of 3.74 (95% CI ) for erectile dysfunction and an OR of 3.22 (95% CI ) for urinary incontinence. Conclusion The proportion of men who experienced a long-term impact on functional outcomes after prostate cancer treatment was substantial. Keywords prostate cancer, erectile dysfunction, urinary incontinence, prostatic neoplasms/therapy, quality of life Introduction Erectile dysfunction, urinary incontinence and bowel dysfunction after prostate cancer treatment have been shown to negatively affect quality of life in the short and intermediate term [1]. Two years after primary treatment for prostate cancer, overall sexual health issues caused moderate or severe distress in 43% of men after radical prostatectomy and in 30 37% of men after radiotherapy. The corresponding figures for urinary symptoms were 7 and 11 16%, respectively. Bowel dysfunction caused distress in 11% of men after radiotherapy [1]. In the USA, ~75% of men with localized prostate cancer are treated with radical prostatectomy or radiotherapy [2]. In Sweden, the proportion of men who receive curative treatment is fairly similar for men with intermediate-risk disease, whereas active surveillance is more commonly used among Swedish men with very-low-risk (59%) and low-risk (41%) prostate cancer as compared with the USA [3,4]. Androgen BJU Int 2016; 117: E36 E45 wileyonlinelibrary.com doi: /bju Published by John Wiley & Sons Ltd.
3 Long-term functional outcomes of prostate cancer treatment deprivation therapy () is the primary treatment in 14% of men with localized prostate cancer (mostly intermediate and high risk) in the USA [2] and 10% in Sweden [3]. Men with localized low- and intermediate-risk prostate cancer have a long life expectancy with prostate cancer-specific mortality rates of 3 4% at 10 years after curative treatment or surveillance [5] and 2 10% at 15 years after radical prostatectomy [6]. There is therefore a need for more knowledge regarding the long-term implications of prostate cancer treatment on urinary, sexual and bowel function. In the US Prostate Cancer Outcomes Study, erectile dysfunction or sexual inactivity was almost universal 15 years after treatment, with rates of 87% after radical prostatectomy and 94% after radiotherapy. The prevalence of urinary incontinence was 18 and 9%, and for bowel urgency was 22 and 36%, respectively [7]. A limitation of previous studies is that they mainly included men who underwent primary treatment with curative intent [1,7]. These studies did not include a comparison group and did not address the functional outcomes after secondary therapy other than. A recent study from the US Cancer of the Prostate Strategic Research Endeavor (CaPSURE) registry, which covers men with localized prostate cancer from 45 community-based urology practices, diagnosed between 1995 and 2011, prospectively evaluated functional outcomes up to 10 years after various prostate cancer treatments, including secondary treatments. The study showed significant declines in health-related quality of life over time, adjusting for age, year of treatment, comorbidities, health insurance status, cancer progression risk at diagnosis, Cancer of the Prostate Risk Assessment (or CAPRA) risk score and secondary treatment. Surgery was found to have the greatest impact on sexual and urinary function, radiation had the greatest impact on bowel function and on physical function; however, that study did not include a non-prostate cancer control group, and therefore was unable to assess whether declines in functional outcomes were different from those in men in a similar age group who were free of disease [8]. Because of the scarcity of large-scale population-based studies reporting long-term patient-reported functional outcomes after prostate cancer treatment, our aim was to evaluate these outcomes for men from the National Prostate Cancer Register of Sweden (NPCR). We examined long-term urinary, sexual and bowel function after conservative management, prostatectomy, radiation therapy, and combinations thereof, and compared these results with those in a control group of men free of prostate cancer. Subjects and Methods Subjects Since 1998, prostate cancer cases have been reported to the NPCR. Compared with the Swedish Cancer Registry, to which reporting is mandatory by law, the capture rate is 98% [9]. The NPCR includes information on TNM stage, Gleason score, PSA levels at diagnosis and primary treatment. A detailed description of treatment patterns in the NPCR, such as radiation doses, planned nerve-sparing surgery and type of is available on the NPCR website [3]. The NPCR Follow-Up Study was performed to assess longterm prostate cancer treatment outcomes in men aged 70 years at date of diagnosis, who were diagnosed with localized prostate cancer clinical stage T1 or T2, any Gleason score, PSA < 20 ng/ml and no signs of lymph node metastases (N0 or NX) or bone metastases (M0 or MX) in This study has been described in detail previously [5,9]. Using the unique Swedish personal identification number, we performed registry linkages to obtain information on comorbidities from the National Patient Register and on socio-economic status from the longitudinal database of socio-economic factors [10]. In September 2011, we identified men from the NPCR Follow-Up Study who were alive. We selected prostate cancer-free men matched on age (1 year) and county of residence in the Swedish population in order to create a study-specific comparison group. Linkage with the Swedish Cancer Registry was performed to ensure that the control subjects were free from prostate cancer. No data on comorbidities or socio-economic status were available for control subjects and these important confounders could therefore not be adjusted for in any analysis. Instead, a secondary analysis restricted to men with prostate cancer only was performed, adjusting for age, comorbidities, marital status and education, with men on surveillance as the reference group, which is believed to be most similar with respect to functional outcomes as a control group. Outcome Assessment We assessed the cumulative effect on functional outcomes after various prostate cancer treatments after a median (interquartile range [IQR]) time of 12 (11 13) years after diagnosis. The survey was carried out at varying times after prostate cancer treatment, providing a comprehensive crosssectional picture of the prevalence of long-term functional outcomes in men with prostate cancer. Functional outcomes were evaluated using a patient selfreported questionnaire. Study participants were first asked to complete a web-version of the questionnaire and if no response was received within 1 month, a paper questionnaire was sent by ordinary mail. This questionnaire was based on the Prostate-Cancer Symptom Scale self-assessment, formerly known as the Questionnaire Umea Fransson Widmark 1994, which was E37
4 Carlsson et al. developed and validated by two of the authors [11]. It includes a question regarding urinary incontinence assessing the use of pads, as well as validated questions regarding bowel function [12], health-related quality of life [13], the International Index of Erectile Function-5 (IIEF-5) [14] and the IPSS [15]. The main endpoints were: urinary incontinence; erectile dysfunction or sexual inactivity; and bowel dysfunction. Secondary endpoints were urinary urgency and health-related quality of life. We used a composite outcome to assess sexual dysfunction defined as erectile dysfunction (an IIEF-5 score 17 and/or reported use of alprostadil) or sexual inactivity. The use of phosphodiesterase type 5 inhibitors was not used for classification. The threshold score of 17 has previously been used [16], and follows the classification suggested by Rosen et al. [14], who developed the questionnaire for distinguishing between severe to moderate (scores 5 16) and mild (scores 17 21) and no erectile dysfunction (scores 22 25). In addition, we considered an IIEF-5 score of 17 to be an appropriate threshold for the older age group under study, as opposed to the higher threshold of 21. Urinary continence was defined as no leakage or occasional use of a protective pad, and urinary incontinence was defined as regular use of pads or diapers. Bowel dysfunction was assessed through three validated questions inquiring about blood in stools, mucus discharge and faecal incontinence, each on a modified linear analogue scale. Bowel problems were then dichotomized and defined as no problems vs problems ( a little, quite a bit or much ). Ethics The Research Ethics Board at Gothenburg University Hospital and Umea University Hospital approved the study. Statistical Analysis To investigate the association between treatment modality and functional outcome, logistic regression analysis adjusting for age was applied and 95% CIs were calculated around point estimates. A descriptive analysis of non-responders was performed. To minimize any bias associated with conducting a complete case analysis only, missing values in the four outcome variables (erectile dysfunction, urgency, urinary incontinence and bowel dysfunction), were imputed, both for non-responders to the questionnaire as well as for responders with missing values, both for cases and controls, using multivariate imputation by chained equations following the method described by van Buuren [17]. Two alternative methods of imputing missing outcome values were used: imputation based on age only (primary) and imputation based on the variables age, comorbidity, marital status and education, excluding the men without prostate cancer. Separate analyses were performed restricted to treated patients with prostate cancer, adjusting for age, comorbidity status, marital status and education. The statistical analyses were conducted using the R statisticalprogrampackage, version2.15.1(r Foundation for StatisticalComputing, Vienna, Austria). Results Functional outcomes were assessed at a median (IQR) time of 12 (11 13) years after diagnosis. Responses to the survey were obtained from 3 937/6 003 cases (66%) and 459/1 000 (46%) controls (Fig. 1). At the date of survey, the median (IQR) age was 75 (70 79) years for cases and 74 (70 78) years for controls. Men who had undergone radical prostatectomy as primary treatment were younger (median age 74 years at follow-up) and had fewer comorbidities than men who received radiotherapy (median age 76 years) or primary (median age 80 years). There were no material differences in socioeconomic status, education or marital status between men undergoing different treatments (Table 1). A substantial proportion of men (23%, 1 383/5 944) received secondary treatment at varying time points after primary treatment. A higher proportion of men with high-risk cancer (53%, 128/243) underwent multiple treatments compared with men with low-risk cancer (15%, 500/3 300), whereas surveillance was more often used in men with low-risk cancer (16%, 526/3 300) than in men with high-risk cancer (2%, 6/243; Table 1). At follow-up, a substantial proportion of men who had received any curative treatment or experienced a negative impact on sexual, urinary and bowel function. In all, 87% of the men had erectile dysfunction or were sexually inactive, 20% reported urinary incontinence and 14% had bowel symptoms. The corresponding proportions for the men in the control group were 62, 6 and 7%, respectively. Sexual and Urinary Dysfunction Compared with the men in the control group, the men treated for prostate cancer had an increased risk of erectile dysfunction. There was no statistically significant difference in men with erectile dysfunction among men on surveillance compared with the men in the control group: odds ratio (OR) 1.24 (95% CI ). The risk was higher for men who had undergone radical prostatectomy (OR 2.29 [95% CI ]) and single-mode radiotherapy (OR 1.56 [95% CI ]; Fig. 2). The risk of urinary incontinence was higher for men who underwent radical prostatectomy (OR 1.89 [95% CI E38
5 Long-term functional outcomes of prostate cancer treatment Fig. 1 Flow chart of study participants. Background population Eligibility & matching Men with prostate cancer assessed for eligibility (n=7 782) All men in the National Prostate Cancer Register (NPCR) with localized prostate cancer diagnosed in : stage T1-2, N0/X, M0/X, PSA < 20 ng/ml and 70 years at diagnosis Cancer-free controls (n=1 000) matched on age and county of residence Excluded (n=1 779) - Deceased or emigrated before questionnaire was sent out (n=1 777) - Wrong address (n=2) Eligible (n=6 003) Questionnaire (sent year 2011) - responders (n=3 937) paper (n=2 060) web (n=1 877) - non-responders (n=2 066) Surveyed Questionnaire (sent year 2011) - responders (n=459) - non-responders (n=541) Analyzed (n=5 944) - responders (n=3 906) paper (n=2 044) Excluded from analysis (n=16) - N1 (n=14) - missing treatment info (n=2) web (n=1 862) Excluded from analysis (n=15) - N1 (n=12) - missing treatment info (n=3) - non-responders (n=2 038) Excluded from analysis (n=28) - N1 (n=19) - missing treatment info (n=9) Analysis Analyzed (n=1 000) - responders (n=459) - non-responders (n=541) Excluded from analysis (n=0) ]), and men who had prostatectomy followed by radiotherapy and had a threefold higher risk of incontinence compared with the control group (OR 3.22 [95% CI ]) (Fig. 2). The risk of urinary urgency symptoms was higher after radiotherapy (OR 1.32 [95% CI ]), but lower after radical prostatectomy (OR 0.79 [95% CI ]) (Fig. 2). Occurrence of erectile dysfunction, sexual inactivity and urinary incontinence after treatment was more common with increasing age at the time of the survey (Tables 2 and 3). Bowel Dysfunction Radiotherapy increased the risk of bowel symptoms, whereas the frequency of bowel dysfunction after radical E39
6 Carlsson et al. Table 1 Patient characteristics by treatment. Surveillance (n = 670) RP (n = 2 640) RT (n = 857) RP + RT (n = 281) (n = 394) RP + (n = 357) RT + (n = 549) RT + RT + (n = 196) All (n = 5 944) Median (IQR) 65 (61 68) 61 (57 65) 64 (60 67) 61 (57 65) 68 (65 69) 63 (59 66) 65 (60 67) 61 (57 65) 63 (59 67) age at diagnosis, years Median (IQR) age at follow-up, years 78 (74 81) 74 (69 78) 76 (72 80) 73 (69 77) 80 (77 82) 75 (71 79) 77 (73 80) 73 (69 77) 75 (71 79) Age group at follow-up, n (%) <70 years 69 (10.3) 671 (25.4) 128 (14.9) 82 (29.2) 10 (2.5) 74 (20.7) 68 (12.4) 52 (26.5) (19.4) years 114 (17.0) 799 (30.3) 213 (24.9) 83 (29.5) 31 (7.9) 75 (21.0) 135 (24.6) 61 (31.1) (25.4) 75 years 487 (72.7) (44.3) 516 (60.2) 116 (41.3) 353 (89.6) 208 (58.3) 346 (63.0) 83 (42.3) (55.2) Year of diagnosis, n (%) (11.5) 169 (6.4) 39 (4.6) 12 (4.3) 30 (7.6) 23 (6.4) 29 (5.3) 6 (3.1) 385 (6.5) (13.7) 277 (10.5) 76 (8.9) 21 (7.5) 49 (12.4) 50 (14.0) 55 (10.0) 13 (6.6) 633 (10.6) (14.3) 387 (14.7) 133 (15.5) 25 (8.9) 60 (15.2) 78 (21.8) 89 (16.2) 20 (10.2) 888 (14.9) (16.1) 498 (18.9) 182 (21.2) 62 (22.1) 90 (22.8) 68 (19.0) 94 (17.1) 26 (13.3) (19.0) (21.6) 571 (21.6) 225 (26.3) 75 (26.7) 74 (18.8) 65 (18.2) 132 (24.0) 57 (29.1) (22.6) (22.7) 738 (28.0) 202 (23.6) 86 (30.6) 91 (23.1) 73 (20.4) 150 (27.3) 74 (37.8) (26.3) Socio-economic status, n (%) Low 318 (47.5) (42.7) 384 (44.8) 127 (45.2) 205 (52.0) 160 (44.8) 267 (48.6) 86 (43.9) (45.0) High 345 (51.5) (56.4) 468 (54.6) 154 (54.8) 185 (47.0) 195 (54.6) 277 (50.5) 110 (56.1) (54.2) Other 7 (1.0) 24 (0.9) 5 (0.6) 0 (0.0) 4 (1.0) 2 (0.6) 5 (0.9) 0 (0.0) 47 (0.8) Charlson comorbidity index, n (%) (73.9) (84.8) 664 (77.5) 243 (86.5) 280 (71.1) 301 (84.3) 432 (78.7) 160 (81.6) (81.0) (16.7) 273 (10.3) 121 (14.1) 29 (10.3) 65 (16.5) 44 (12.3) 78 (14.2) 21 (10.7) 743 (12.5) 2 45 (6.7) 106 (4.0) 49 (5.7) 7 (2.5) 32 (8.1) 10 (2.8) 29 (5.3) 13 (6.6) 291 (4.9) (2.7) 22 (0.8) 23 (2.7) 2 (0.7) 17 (4.3) 2 (0.6) 10 (1.8) 2 (1.0) 96 (1.6) Education, n (%) Low 257 (38.4) 829 (31.4) 308 (35.9) 87 (31.0) 180 (45.7) 121 (33.9) 210 (38.3) 68 (34.7) (34.7) Middle 259 (38.7) (40.3) 328 (38.3) 122 (43.4) 140 (35.5) 145 (40.6) 210 (38.3) 82 (41.8) (39.6) High 152 (22.7) 733 (27.8) 218 (25.4) 72 (25.6) 73 (18.5) 89 (24.9) 129 (23.5) 46 (23.5) (25.4) Missing 2 (0.3) 13 (0.5) 3 (0.4) 0 (0.0) 1 (0.3) 2 (0.6) 0 (0.0) 0 (0.0) 21 (0.4) Marital status, n (%) Married 476 (71.0) (78.6) 634 (74.0) 223 (79.4) 296 (75.1) 273 (76.5) 424 (77.2) 151 (77.0) (76.6) Divorced 102 (15.2) 298 (11.3) 132 (15.4) 29 (10.3) 47 (11.9) 47 (13.2) 71 (12.9) 30 (15.3) 756 (12.7) Widower 35 (5.2) 69 (2.6) 28 (3.3) 9 (3.2) 17 (4.3) 12 (3.4) 22 (4.0) 5 (2.6) 197 (3.3) Never married 57 (8.5) 198 (7.5) 63 (7.4) 20 (7.1) 34 (8.6) 25 (7.0) 32 (5.8) 10 (5.1) 439 (7.4) Risk group*, n (%) Low risk 526 (78.5) (61.6) 478 (55.8) 123 (43.8) 171 (43.4) 125 (35.0) 182 (33.2) 70 (35.7) (55.5) Intermediate risk 138 (20.6) 947 (35.9) 351 (41.0) 146 (52.0) 210 (53.3) 193 (54.1) 312 (56.8) 104 (53.1) (40.4) High risk 6 (0.9) 68 (2.6) 28 (3.3) 12 (4.3) 13 (3.3) 39 (10.9) 55 (10.0) 22 (11.2) 243 (4.1) RP, radical prostatectomy; RT, radiotherapy;, androgen deprivation therapy. * Risk group at diagnosis defined as: low risk; T1 2 and Gleason score 6 and PSA < 10 ng/ml; intermediate risk: T1-2 and Gleason score 7 and/or PSA ng/ml, high risk; T3, and/or Gleason score 8-10 and/or PSA ng/ml. Patients with regionally metastatic disease (N1 and/or PSA ng/ml and no distant metastases, M0 or MX) and patients with distant metastasis (M1 and/or PSA 100 ng/ml) were not eligible. There were no missing data for risk group. prostatectomy or in men on surveillance was no different from that in the men in the control group (Fig. 2). Health-Related Quality of Life Study participants were asked about sexual, urinary and bowel function separately: If you were to spend the rest of your life with your condition just the way it is now, how would you feel about that?. The proportion of men who responded mostly dissatisfied, unhappy or terrible regarding sexual function was 35% for all men treated for prostate cancer as compared with 18% for men in the control group. The corresponding proportions were 11 vs 10% for urinary function and 7 vs 4% for bowel function. Sensitivity Analyses Patient and tumour characteristics for non-responders were compared with responders. Non-responders tended to be older, have more comorbidities, a lower educational level and were more often managed with surveillance and treated with hormonal therapy, although differences were small (data not shown); however, in a multivariable analysis performed in cases only including age, comorbidity, martial status and educational level (as we did not have these data for control subjects), with active surveillance as reference, the increases in risk for men in each of the active treatment groups remained similar (Fig. S1). This was true for both imputation alternatives. E40
7 Long-term functional outcomes of prostate cancer treatment Fig. 2 Odds ratios and 95% confidence intervals for the risk of adverse functional outcomes by treatment compared to controls and adjusted for age. Erectile dysfunction Men without PCa Surveillance RP RT RP+RT RP+ RT+ RP+RT+ Urgency Men without PCa Surveillance RP RT RP+RT RP+ RT+ RP+RT+ Urinary incontinence Men without PCa Surveillance RP RT RP+RT RP+ RT+ RP+RT+ Bowel dysfunction Men without PCa Surveillance RP RT RP+RT RP+ RT+ RP+RT Ref ( ) 2.29 ( ) 1.56 ( ) 3.48 ( ) 2.32 ( ) 3.70 ( ) 2.17 ( ) 3.74 ( ) 1.00 Ref ( ) 0.79 ( ) 1.32 ( ) 1.23 ( ) 1.21 ( ) 1.16 ( ) 1.37 ( ) 1.21 ( ) 1.00 Ref ( ) 1.89 ( ) 1.00 ( ) 2.41 ( ) 0.99 ( ) 2.70 ( ) 1.19 ( ) 3.22 ( ) 1.00 Ref ( ) 0.99 ( ) 2.46 ( ) 2.13 ( ) 1.24 ( ) 1.26 ( ) 2.72 ( ) 2.29 ( ) Odds Ratio We also performed separate analyses for men with lowand intermediate-risk prostate cancer (Fig. S2). Overall, the risks of side effects were similar for both risk groups. Discussion In this large, population-based study in Sweden, the impact on functional outcomes remained substantial for all treatment methods more than a decade after prostate cancer diagnosis. The majority of men experienced erectile dysfunction or were sexually inactive, almost 20% reported urinary incontinence and 14% had bowel symptoms, all of which affected quality of life. A general and consistent pattern throughout all domains (sexual, urinary and bowel function) was that men who E41
8 Carlsson et al. Table 2 Erectile function at survey, stratified by treatment and age group. No erectile dysfunction n (%) Erectile dysfunction* n (%) Not sexually active n (%) Missing n (%) All age groups, n (%) Men without prostate cancer 160 (34.9) 57 (12.4) 200 (43.6) 42 (9.2) Surveillance 69 (20.1) 62 (18.1) 159 (46.4) 53 (15.5) RP 211 (11.4) 261 (14.0) (61.9) 236 (12.7) RT 87 (15.9) 93 (17.0) 297 (54.4) 69 (12.6) RP + RT 15 (7.7) 27 (13.8) 138 (70.8) 15 (7.7) 12 (5.5) 19 (8.8) 138 (63.6) 48 (22.1) RP + 11 (4.6) 16 (6.6) 188 (78.0) 26 (10.8) RT + 35 (9.5) 54 (14.6) 225 (61.0) 55 (14.9) RP + RT + 6 (4.4) 14 (10.3) 100 (73.5) 16 (11.8) Age < 70 years Men without prostate cancer 60 (60.6) 11 (11.1) 22 (22.2) 6 (6.1) Surveillance 10 (25.0) 14 (35.0) 9 (22.5) 7 (17.5) RP 111 (22.7) 94 (19.2) 225 (45.9) 60 (12.2) RT 27 (31.8) 22 (25.9) 27 (31.8) 9 (10.6) RP + RT 6 (10.3) 10 (17.2) 40 (69.0) 2 (3.4) 2 (33.3) 1 (16.7) 3 (50.0) 0 (0.0) RP + 5 (10.0) 4 (8.0) 36 (72.0) 5 (10.0) RT + 8 (16.7) 11 (22.9) 23 (47.9) 6 (12.5) RP + RT + 3 (8.3) 6 (16.7) 25 (69.4) 2 (5.6) Age years Men without prostate cancer 54 (37.8) 16 (11.2) 59 (41.3) 14 (9.8) Surveillance 18 (27.7) 10 (15.4) 29 (44.6) 8 (12.3) RP 57 (9.9) 95 (16.6) 358 (62.5) 63 (11.0) RT 25 (18.2) 25 (18.2) 72 (52.6) 15 (10.9) RP + RT 3 (5.6) 7 (13.0) 38 (70.4) 6 (11.1) 3 (11.5) 2 (7.7) 16 (61.5) 5 (19.2) RP + 2 (3.3) 4 (6.6) 49 (80.3) 6 (9.8) RT + 16 (17.2) 16 (17.2) 52 (55.9) 9 (9.7) RP + RT + 2 (4.1) 5 (10.2) 35 (71.4) 7 (14.3) Age 75 years Men without prostate cancer 46 (21.2) 30 (13.8) 119 (54.8) 22 (10.1) Surveillance 41 (17.2) 38 (16.0) 121 (50.8) 38 (16.0) RP 43 (5.4) 72 (9.0) 568 (71.4) 113 (14.2) RT 35 (10.8) 46 (14.2) 198 (61.1) 45 (13.9) RP + RT 6 (7.2) 10 (12.0) 60 (72.3) 7 (8.4) 7 (3.8) 16 (8.6) 119 (64.3) 43 (23.2) RP + 4 (3.1) 8 (6.2) 103 (79.2) 15 (11.5) RT + 11 (4.8) 27 (11.8) 150 (65.8) 40 (17.5) RP + RT + 1 (2.0) 3 (5.9) 40 (78.4) 7 (13.7) RP, radical prostatectomy; RT, radiotherapy;, androgen deprivation therapy. * International Index of Erectile Function-5 score 17 or alprostadil use. had received multiple treatments, in particular men who received had poor functional outcomes compared with men who received one single curative treatment. Strengths The present study was population-based and captured all treatment modalities provided by all types of healthcare providers in Sweden. We used self-administered and validated questionnaires to assess the patient-reported functional outcomes. Moreover, the present study included disease risk classification and thus enabled us to specifically study men who underwent treatment for localized prostate cancer only. Limitations The present study had several limitations. Data were crosssectional in nature, and not longitudinal, which would have been ideal. The present study did not include a baseline assessment before treatment; however, we did have a comparison group of age- and county-matched men free from prostate cancer. The risk of adverse effects were consistently and significantly higher across all domains among cases compared with controls. The response rates were suboptimal and there was potential bias because we cannot exclude the possibility that response rate was not related to outcome measures. A descriptive analysis of non-responders compared with responders showed E42
9 Long-term functional outcomes of prostate cancer treatment Table 3 Urinary continence at survey, stratified by treatment and age group. Continent n (%) Incontinent n (%) Missing n (%) All age groups Men without prostate cancer 409 (89.1) 24 (5.2) 26 (5.7) Surveillance 276 (80.5) 28 (8.2) 39 (11.4) RP (69.0) 387 (20.8) 189 (10.2) RT 445 (81.5) 50 (9.2) 51 (9.3) RP + RT 130 (66.7) 53 (27.2) 12 (6.2) 160 (73.7) 26 (12.0) 31 (14.3) RP (57.7) 78 (32.4) 24 (10.0) RT (78.3) 46 (12.5) 34 (9.2) RP + RT + 84 (61.8) 45 (33.1) 7 (5.1) Age < 70 years Men without prostate cancer 93 (93.9) 2 (2.0) 4 (4.0) Surveillance 31 (77.5) 4 (10.0) 5 (12.5) RP 375 (76.5) 66 (13.5) 49 (10.0) RT 75 (88.2) 4 (4.7) 6 (7.1) RP + RT 44 (75.9) 12 (20.7) 2 (3.4) 5 (83.3) 1 (16.7) 0 (0.0) RP + 32 (64.0) 11 (22.0) 7 (14.0) RT + 43 (89.6) 2 (4.2) 3 (6.2) RP + RT + 27 (75.0) 8 (22.2) 1 (2.8) Age years Men without prostate cancer 124 (86.7) 9 (6.3) 10 (7.0) Surveillance 51 (78.5) 8 (12.3) 6 (9.2) RP 395 (68.9) 120 (20.9) 58 (10.1) RT 117 (85.4) 9 (6.6) 11 (8.0) RP + RT 36 (66.7) 13 (24.1) 5 (9.3) 20 (76.9) 2 (7.7) 4 (15.4) RP + 36 (59.0) 18 (29.5) 7 (11.5) RT + 77 (82.8) 10 (10.8) 6 (6.5) RP + RT + 31 (63.3) 14 (28.6) 4 (8.2) Age 75 years Men without prostate cancer 192 (88.5) 13 (6.0) 12 (5.5) Surveillance 194 (81.5) 16 (6.7) 28 (11.8) RP 513 (64.4) 201 (25.3) 82 (10.3) RT 253 (78.1) 37 (11.4) 34 (10.5) RP + RT 50 (60.2) 28 (33.7) 5 (6.0) 135 (73.0) 23 (12.4) 27 (14.6) RP + 71 (54.6) 49 (37.7) 10 (7.7) RT (74.1) 34 (14.9) 25 (11.0) RP + RT + 26 (51.0) 23 (45.1) 2 (3.9) RP, radical prostatectomy; RT, radiotherapy;, androgen deprivation therapy. some minor differences in patient and tumour characteristics (data not shown). We addressed this using multivariate imputation by chained equations, and the patterns seen in the primary analysis remained. In sensitivity analyses restricted to treated patients (with surveillance as the reference group), estimates adjusted for age as well as estimates adjusted for age, comorbidity, marital status and education were essentially the same, suggesting that these variables were not important confounders. A limitation of this study is the lack of information on the control group other than age. The results of the present study need to be interpreted in the light of its observational design and the fact that it includes a historical cohort. Older men with more comorbid conditions and who are less fit may be more likely to undergo radiotherapy than radical prostatectomy; therefore, confounding by indication by tumour characteristics and comorbidity cannot be excluded, despite adjusting for age. Moreover, men in this study were diagnosed between 1997 and 2002 and some men received secondary treatments within 12 years. Treatment may have improved over time and contemporary outcomes may be superior. The present study is consistent with previous intermediateand long-term (2 15 years) studies showing declines in sexual, urinary and bowel domains after prostate cancer treatment, especially erectile dysfunction [1,7,18]. Our findings are very similar to those from the Scandinavian Prostate Cancer Group Study Number 4 (SPCG-4) which had a median follow-up of 12 years and median participant age of 77 years at evaluation, which reported a prevalence of erectile dysfunction of 84% after radical prostatectomy, 80% in men on watchful waiting and 46% among control subjects [19]. E43
10 Carlsson et al. Men on surveillance in the present study had similar risks for all four outcomes (erectile dysfunction, urinary urgency, urinary incontinence and bowel dysfunction) compared with the men in the cancer-free control group. The definition and reporting of erectile function after prostate cancer treatment, mainly radical prostatectomy, is inconsistent in the literature [18]. A common definition of potency is erections sufficient for intercourse, with or without phosphodiesterase type 5 inhibitors [18]. The National Institute of Health consensus conference defined erectile dysfunction as the consistent inability to obtain and/ or maintain an erection sufficient for satisfactory sexual performance [20], a definition that did not include any mention of use of medication or other treatment for erectile dysfunction; therefore, men who reported use of phosphodiesterase type 5 inhibitors were included with their reported scores, whereas men who reported use of transurethral suppositories or intracavernous injections used for erectile dysfunction were considered to have erectile dysfunction using the first definition. The present study confirms previous observations made by Sandaetal.[1],whofoundahighriskofurinary incontinence 2 years after radical prostatectomy. Men who received multiple treatments had the highest risk of poor functional outcomes. This finding is consistent with data from the CaPSURE registry, in which men who received multiple treatments had a sharper decline in urinary and sexual function at 2 years compared with men who only received primary treatment [21]. Furthermore, this corroborates previous findings by Sanda et al. [1] that neoadjuvant before radiotherapy was associated with worse scores in multiple quality-of-life domains, especially urinary incontinence. These findings highlight the importance of critically assessing the need for secondary treatment and of informing men about the risks of more side effects. In the SPCG-4 trial, the proportion of men with urinary leakage at least once daily increased with time. At a median follow-up of 12 years, 41% of men who had undergone prostatectomy, 11% of men on watchful waiting and 3% of men in a control group had urinary leakage [19]. In the Prostate Cancer Outcomes Study (PCOS) study, only 14% of men reported frequent urinary leakage or no urinary control 5 years after prostatectomy [22]. In the present study, 23% reported urinary leakage 12 years after diagnosis in all treatment groups combined. Differences in definition of urinary incontinence and follow-up time may contribute to differences in observed estimates. Radical prostatectomy was associated with a significantly lower risk of urinary urgency in the present study, corroborating results from previous studies that radical prostatectomy prevents age-dependent progression of LUTS [23]. In the present study the risk of long-term bowel dysfunction was high after radiotherapy. In the PCOS study, men treated with radiation therapy initially had more bowel urgency compared with radical prostatectomy, but there were no significant differences between the groups by 15 years [7]. As the patient population in the present study stemmed from a truly population-based, nationwide sample, and were not preselected patients, results are likely to represent the real-life scenario. Furthermore, outcomes assessed through questionnaires give a fair view of the patients perspective and may protect against bias that might arise, for example, when patients minimize symptoms when asked by their physician. The present study showed a substantial risk of poor functional outcomes 12 years after the initial treatment, underlining the need for consistent improvement in the delivery of curative treatment in order to reduce the rate of adverse effects. Because the treatments were delivered more than a decade ago and by all types of healthcare providers, including low-volume centres, our results probably represent a worst-case scenario, as cancers currently diagnosed are more likely to be low risk and treatment delivery has improved, including greater centralization of care [24]. In conclusion, a high proportion of men treated for localized prostate cancer with curative intent experienced sexual, urinary and bowel dysfunction >12 years after treatment and men who received several treatments were at particularly high risk of poor functional outcomes. Our findings highlight the importance of careful patient selection and underline the need for a consistent improvement in the delivery of curative treatment given the potential long-term functional implications. Acknowledgements We thank the Swedish Research Council and the Swedish Cancer Foundation , V asterbotten County Council and Lion 0 s Cancer Research Foundation at Umea University. S.C. is supported by grants from AFA Insurance, the Swedish Cancer Society, the Sweden America Foundation, the Swedish Council for Working Life and Social Research, the Swedish Society for Medical Research and the Swedish Prostate Cancer Foundation. S.L. is supported by the National Institutes of Health under Award Number K07CA The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. The funders had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript. The project was made possible by the continuous work of the National Prostate Cancer Register of Sweden steering group: P ar Stattin (chairman), Anders Widmark, Camilla Thellenberg, Ove Andren, Anna Bill-Axelsson, Ann-Sofi Fransson, Magnus T ornblom, Stefan Carlsson, Marie Hj alm-eriksson, Bodil Westman, Bill Pettersson, David Robinson, Mats Anden, Jan- E44
11 Long-term functional outcomes of prostate cancer treatment Erik Damber, Jonas Hugosson, Ingela Frank-Lissbrant, Maria Nyberg, G oran Ahlgren, Ola Bratt, Rene Blom, Lars Egevad, Calle Waller, Olof Akre, Per Fransson, Eva Johansson, Fredrik Sandin, Hans Garmo, Mats Lambe, Karin Hellstr om, Annette Wigertz and Erik Holmberg. Conflict of Interest None declared. References 1 Sanda MG, Dunn RL, Michalski J et al. Quality of life and satisfaction with outcome among prostate-cancer survivors. N Engl J Med 2008; 358: Cooperberg MR, Broering JM, Carroll PR. Time trends and local variation in primary treatment of localized prostate cancer. J Clin Oncol 2010; 28: Prostate Cancer National quality report, Regional cancer centre, Uppsala Orebro, Sweden. Available at: /04/ NPCR-Rapport-2013-FINAL-ENG.pdf Date. Accessed January Loeb S, Berglund A, Stattin P. Population based study of use and determinants of active surveillance and watchful waiting for low and intermediate risk prostate cancer. J Urol 2013; 190: Stattin P, Holmberg E, Johansson JE, Holmberg L, Adolfsson J, Hugosson J. Outcomes in localized prostate cancer: National Prostate Cancer Register of Sweden follow-up study. J Natl Cancer Inst 2010; 102: Stephenson AJ, Kattan MW, Eastham JA et al. Prostate cancer-specific mortality after radical prostatectomy for patients treated in the prostatespecific antigen era. J Clin Oncol 2009; 27: Resnick MJ, Koyama T, Fan KH et al. Long-term functional outcomes after treatment for localized prostate cancer. N Engl J Med 2013; 368: PunnenS, CowanJE, ChanJM, CarrollPR, CooperbergMR. Long-term health-relatedqualityoflifeafterprimarytreatmentforlocalizedprostate cancer: resultsfromthecapsureregistry. EurUrol2014.[Epubaheadof print]. doi: /j.eururo Stattin P, Holmberg E, Bratt O, Adolfsson J, Johansson JE, Hugosson J; National Prostate Cancer Register. Surveillance and deferred treatment for localized prostate cancer. Population based study in the National Prostate Cancer Register of Sweden. J Urol 2008; 180: Van Hemelrijck M, Wigertz A, Sandin F et al. NPCR and PCBaSe Sweden. Cohort profile: the National Prostate Cancer Register of Sweden and Prostate Cancer data base Sweden 2.0. Int J Epidemiol 2013; 42: Fransson P, Tavelin B, Widmark A. Reliability and responsiveness of a prostate cancer questionnaire for radiotherapy-induced side effects. Support Care Cancer 2001; 9: Reidunsdatter RJ, Lund JA, Fransson P, Widmark A, Fossa SD, Kaasa S. Validation of the intestinal part of the prostate cancer questionnaire QUFW94 : psychometric properties, responsiveness, and content validity. Int J Radiat Oncol Biol Phys 2010; 77: Hamoen EH, De Rooij M, Witjes JA, Barentsz JO, Rovers MM. Measuring health-related quality of life in men with prostate cancer: a systematic review of the most used questionnaires and their validity. Urol Oncol 2014; 33: 69.e Rosen RC, Cappelleri JC, Smith MD, Lipsky J, Pe~na BM. Development and evaluation of an abridged, 5-item version of the International Index of Erectile Function (IIEF-5) as a diagnostic tool for erectile dysfunction. Int J Impot Res 1999; 11: Barry MJ, Fowler FJ Jr, O Leary MP et al. The American Urological Association symptom index for benign prostatic hyperplasia. The Measurement Committee of the American Urological Association. J Urol 1992; 148: Carlsson S, Aus G, Bergdahl S et al. The excess burden of side-effects from treatment in men allocated to screening for prostate cancer. The G oteborg randomised population-based prostate cancer screening trial. Eur J Cancer 2011; 47: van Buuren S. Flexible Imputation of Missing Data. Boca Raton, FL: Chapman & Hall/CRC, ISBN Mulhall JP. Defining and reporting erectile function outcomes after radical prostatectomy: challenges and misconceptions. J Urol 2009; 181: Johansson E, Steineck G, Holmberg L et al. Long-term quality-of-life outcomes after radical prostatectomy or watchful waiting: the Scandinavian Prostate Cancer Group-4 randomised trial. Lancet Oncol 2011; 12: NIH Consensus Conference. Impotence. NIH consensus development panel on impotence. JAMA 1993; 270: Wu AK, Cooperberg MR, Sadetsky N et al. Health related quality of life in patients treated with multimodal therapy for prostate cancer. J Urol 2008; 180: Penson DF, McLerran D, Feng Z et al. 5-year urinary and sexual outcomes after radical prostatectomy: results from the prostate cancer outcomes study. J Urol 2005; 173: Prabhu V, Taksler GB, Sivarajan G, Laze J, Makarov DV, Lepor H. Radical prostatectomy improves and prevents age dependent progression of lower urinary tract symptoms. J Urol 2014; 191: Anderson CB, Penson DF, Ni S, Makarov DV, Barocas DA. Centralization of radical prostatectomy in the United States. J Urol 2013; 189: Correspondence: Sigrid Carlsson, Memorial Sloan-Kettering Cancer Center, Department of Epidemiology and Biostatistics, 485 Lexington ave, 2nd floor, New York, NY 10017, USA. carlssos@mskcc.org Abbreviations: OR, odds ratio;, androgen deprivation therapy; CaPSURE, Cancer of the Prostate Strategic Research Endeavor; NPCR, National Prostate Cancer Register of Sweden; IQR, interquartile range; IIEF-5, International Index of Erectile Function-5; SPCG-4, Scandinavian Prostate Cancer Group Study Number 4; PCOS, Prostate Cancer Outcomes Study. Supporting Information Additional Supporting Information may be found in the online version of this article: Fig S1. Odds ratios and 95% confidence intervals for the risk of adverse functional outcomes by treatment, adjusted for age (imputation alternative 1) and adjusted for age, comorbidity, marital status and education (imputation alternative 2). Fig S2. Odds ratios and 95% confidence intervals for the risk of adverse functional outcomes by treatment and risk group, and adjusting for age, comorbidity, marital status and education. E45
Family History and Probability of Prostate Cancer, Differentiated by Risk Category: A Nationwide Population-Based Study
 JNCI J Natl Cancer Inst (2016) 108(10): djw110 doi: 10.1093/jnci/djw110 First published online July 10, 2016 Article Family History and Probability of Prostate Cancer, Differentiated by Risk Category:
JNCI J Natl Cancer Inst (2016) 108(10): djw110 doi: 10.1093/jnci/djw110 First published online July 10, 2016 Article Family History and Probability of Prostate Cancer, Differentiated by Risk Category:
Cohort Profile Update: The National Prostate Cancer Register of Sweden and Prostate Cancer data Base a refined prostate cancer trajectory
 International Journal of Epidemiology, 216, 73 82 doi: 1.193/ije/dyv35 Advance Access Publication Date: 11 December 215 Cohort Profile Update Cohort Profile Update Cohort Profile Update: The National Prostate
International Journal of Epidemiology, 216, 73 82 doi: 1.193/ije/dyv35 Advance Access Publication Date: 11 December 215 Cohort Profile Update Cohort Profile Update Cohort Profile Update: The National Prostate
Long-term adverse effects after retropubic and robot-assisted radical prostatectomy. Nationwide, population-based study
 Received: 11 April 2017 Accepted: 1 May 2017 DOI: 10.1002/jso.24687 RESEARCH ARTICLE Long-term adverse effects after retropubic and robot-assisted radical prostatectomy. Nationwide, population-based study
Received: 11 April 2017 Accepted: 1 May 2017 DOI: 10.1002/jso.24687 RESEARCH ARTICLE Long-term adverse effects after retropubic and robot-assisted radical prostatectomy. Nationwide, population-based study
Citation for the original published paper (version of record):
 http://www.diva-portal.org This is the published version of a paper published in International Journal of Cancer. Citation for the original published paper (version of record): Crawley, D., Garmo, H.,
http://www.diva-portal.org This is the published version of a paper published in International Journal of Cancer. Citation for the original published paper (version of record): Crawley, D., Garmo, H.,
Prognostic Value of the ISUP 2015 Gleason Grade Groupings
 Prognostic Value of the ISUP 2015 Gleason Grade Groupings Yasin Folkvaljon Department of Statistics Uppsala University Supervisors: Lisbeth Hansson and Hans Garmo 2015 Abstract Background: New prognostic
Prognostic Value of the ISUP 2015 Gleason Grade Groupings Yasin Folkvaljon Department of Statistics Uppsala University Supervisors: Lisbeth Hansson and Hans Garmo 2015 Abstract Background: New prognostic
Urological Oncology. Sam Ladjevardi, Anders Berglund*, Eberhard Varenhorst, Ola Bratt, Anders Widmark and Gabriel Sandblom.
 Urological Oncology Treatment with curative intent and survival in men with high-risk prostate cancer. A population-based study of 11 380 men with serum PSA level 20 100 ng/ml Sam Ladjevardi, Anders Berglund*,
Urological Oncology Treatment with curative intent and survival in men with high-risk prostate cancer. A population-based study of 11 380 men with serum PSA level 20 100 ng/ml Sam Ladjevardi, Anders Berglund*,
Effects of Prostate-Specific Antigen Testing on Familial Prostate Cancer Risk Estimates
 DOI: 10.1093/jnci/djq265 Advance Access publication on August 19, 2010. The Author 2010. Published by Oxford University Press. All rights reserved. For Permissions, please e-mail: journals.permissions@oxfordjournals.org.
DOI: 10.1093/jnci/djq265 Advance Access publication on August 19, 2010. The Author 2010. Published by Oxford University Press. All rights reserved. For Permissions, please e-mail: journals.permissions@oxfordjournals.org.
Prostate Cancer Mortality in Areas With High and Low Prostate Cancer Incidence
 DOI:10.1093/jnci/dju007 First published online March 4, 2014 Article Oxford University Press 2014. This is an Open Access article distributed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs
DOI:10.1093/jnci/dju007 First published online March 4, 2014 Article Oxford University Press 2014. This is an Open Access article distributed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs
Outcomes in Localized Prostate Cancer: National Prostate Cancer Register of Sweden Follow-up Study
 JNCI Journal of the National Cancer Institute Advance Access published June 18, 2010 DOI: 10.1093/jnci/djq154 Article The Author 2010. Published by Oxford University Press. This is an Open Access article
JNCI Journal of the National Cancer Institute Advance Access published June 18, 2010 DOI: 10.1093/jnci/djq154 Article The Author 2010. Published by Oxford University Press. This is an Open Access article
Treatment of localized prostate cancer in elderly patients
 Editorial Treatment of localized prostate cancer in elderly patients Mohammed Haseebuddin, Marc C. Smaldone Department of Urologic Oncology, Fox Chase Cancer Center, Philadelphia, PA, USA Correspondence
Editorial Treatment of localized prostate cancer in elderly patients Mohammed Haseebuddin, Marc C. Smaldone Department of Urologic Oncology, Fox Chase Cancer Center, Philadelphia, PA, USA Correspondence
Radical Prostatectomy or Watchful Waiting in Early Prostate Cancer
 The new england journal of medicine original article Radical Prostatectomy or Watchful Waiting in Early Prostate Cancer Anna Bill-Axelson, M.D., Ph.D., Lars Holmberg, M.D., Ph.D., Hans Garmo, Ph.D., Jennifer
The new england journal of medicine original article Radical Prostatectomy or Watchful Waiting in Early Prostate Cancer Anna Bill-Axelson, M.D., Ph.D., Lars Holmberg, M.D., Ph.D., Hans Garmo, Ph.D., Jennifer
2017 American Medical Association. All rights reserved.
 Supplementary Online Content Borocas DA, Alvarez J, Resnick MJ, et al. Association between radiation therapy, surgery, or observation for localized prostate cancer and patient-reported outcomes after 3
Supplementary Online Content Borocas DA, Alvarez J, Resnick MJ, et al. Association between radiation therapy, surgery, or observation for localized prostate cancer and patient-reported outcomes after 3
Long- term quality of life after definitive treatment for prostate cancer: patient- reported outcomes in the second posttreatment decade
 Cancer Medicine ORIGINAL RESEARCH Open Access Long- term quality of life after definitive treatment for prostate cancer: patient- reported outcomes in the second posttreatment decade Joanne W. Jang 1,2,
Cancer Medicine ORIGINAL RESEARCH Open Access Long- term quality of life after definitive treatment for prostate cancer: patient- reported outcomes in the second posttreatment decade Joanne W. Jang 1,2,
Irreversible Electroporation for the Treatment of Recurrent Prostate Cancer
 Irreversible Electroporation for the Treatment of Recurrent Prostate Cancer after prostatectomy, radiation therapy and HiFU R. Schwartzberg, E. Günther, N. Klein, S. Zapf, R. El-Idrissi, J. Cooper, B.
Irreversible Electroporation for the Treatment of Recurrent Prostate Cancer after prostatectomy, radiation therapy and HiFU R. Schwartzberg, E. Günther, N. Klein, S. Zapf, R. El-Idrissi, J. Cooper, B.
Introduction. Methods. Original Article: Clinical Investigation
 International Journal of Urology (218) 25, 366--371 doi: 1.1111/iju.1353 Original Article: Clinical Investigation Impact of age on quality of life in patients with localized prostate cancer treated with
International Journal of Urology (218) 25, 366--371 doi: 1.1111/iju.1353 Original Article: Clinical Investigation Impact of age on quality of life in patients with localized prostate cancer treated with
Survivorship Beyond Convalescence: 48-Month Quality-of-Life Outcomes After Treatment for Localized Prostate Cancer
 BRIEF COMMUNICATION Survivorship Beyond Convalescence: 48-Month Quality-of-Life Outcomes After Treatment for Localized Prostate Cancer John L. Gore, Lorna Kwan, Steve P. Lee, Robert E. Reiter, Mark S.
BRIEF COMMUNICATION Survivorship Beyond Convalescence: 48-Month Quality-of-Life Outcomes After Treatment for Localized Prostate Cancer John L. Gore, Lorna Kwan, Steve P. Lee, Robert E. Reiter, Mark S.
Mortality following Hip Fracture in Men with Prostate Cancer
 Mortality following Hip Fracture in Men with Prostate Cancer Mieke Van Hemelrijck 1,2 *, Hans Garmo 1,3, Karl Michaëlsson 4, Andreas Thorstenson 5,6, Olof Akre 7, Pär Stattin 8,9, Lars Holmberg 1,3,10,
Mortality following Hip Fracture in Men with Prostate Cancer Mieke Van Hemelrijck 1,2 *, Hans Garmo 1,3, Karl Michaëlsson 4, Andreas Thorstenson 5,6, Olof Akre 7, Pär Stattin 8,9, Lars Holmberg 1,3,10,
Prostate Cancer Innovations in Surgical Strategies Update 2007!
 Prostate Cancer Innovations in Surgical Strategies Update 2007! Curtis A. Pettaway, M.D. Professor Department of Urology The University of Texas M. D. Anderson Cancer Center Radical Prostatectomy Pathologic
Prostate Cancer Innovations in Surgical Strategies Update 2007! Curtis A. Pettaway, M.D. Professor Department of Urology The University of Texas M. D. Anderson Cancer Center Radical Prostatectomy Pathologic
NIH Public Access Author Manuscript World J Urol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
ERECTILE DYSFUNCTION AND SEXUAL PROBLEM 2-3YEARS AFTER PROSTATECTOMY AMONG AMERICAN, NORWEGIAN AND SPANISH PATIENTS
 ERECTILE DYSFUNCTION AND SEXUAL PROBLEM 2-3YEARS AFTER PROSTATECTOMY AMONG AMERICAN, NORWEGIAN AND SPANISH PATIENTS Storås AH, Sanda MG, Garin O, Patil D, Chang P, Crociani C, Suarez F, Cvancarova M, Loge
ERECTILE DYSFUNCTION AND SEXUAL PROBLEM 2-3YEARS AFTER PROSTATECTOMY AMONG AMERICAN, NORWEGIAN AND SPANISH PATIENTS Storås AH, Sanda MG, Garin O, Patil D, Chang P, Crociani C, Suarez F, Cvancarova M, Loge
Citation for the original published paper (version of record): N.B. When citing this work, cite the original published paper.
 http://www.diva-portal.org This is the published version of a paper published in International Journal of Cancer. Citation for the original published paper (version of record): Häggström, C., Van Hemelrijck,
http://www.diva-portal.org This is the published version of a paper published in International Journal of Cancer. Citation for the original published paper (version of record): Häggström, C., Van Hemelrijck,
J Clin Oncol 28: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 28 NUMBER 1 JANUARY 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Clinical Results of Long-Term Follow-Up of a Large, Active Surveillance Cohort With Localized Prostate Cancer
VOLUME 28 NUMBER 1 JANUARY 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Clinical Results of Long-Term Follow-Up of a Large, Active Surveillance Cohort With Localized Prostate Cancer
PROSTATE CANCER SURVEILLANCE
 PROSTATE CANCER SURVEILLANCE ESMO Preceptorship on Prostate Cancer Singapore, 15-16 November 2017 Rosa Nadal National Cancer Institute, NIH Bethesda, USA DISCLOSURE No conflicts of interest to declare
PROSTATE CANCER SURVEILLANCE ESMO Preceptorship on Prostate Cancer Singapore, 15-16 November 2017 Rosa Nadal National Cancer Institute, NIH Bethesda, USA DISCLOSURE No conflicts of interest to declare
High Risk Localized Prostate Cancer Treatment Should Start with RT
 High Risk Localized Prostate Cancer Treatment Should Start with RT Jason A. Efstathiou, M.D., D.Phil. Assistant Professor of Radiation Oncology Massachusetts General Hospital Harvard Medical School 10
High Risk Localized Prostate Cancer Treatment Should Start with RT Jason A. Efstathiou, M.D., D.Phil. Assistant Professor of Radiation Oncology Massachusetts General Hospital Harvard Medical School 10
INTERNATIONAL JOURNAL OF ONCOLOGY 46: , 2015
 INTERNATIONAL JOURNAL OF ONCOLOGY 46: 381-388, 2015 Long-term health-related quality of life after curative treatment for prostate cancer: A regional cross-sectional comparison of two standard treatment
INTERNATIONAL JOURNAL OF ONCOLOGY 46: 381-388, 2015 Long-term health-related quality of life after curative treatment for prostate cancer: A regional cross-sectional comparison of two standard treatment
Citation for the original published paper (version of record):
 http://www.diva-portal.org This is the published version of a paper published in PLoS ONE. Citation for the original published paper (version of record): Wiren, S., Drevin, L., Akre, O., Robinson, D.,
http://www.diva-portal.org This is the published version of a paper published in PLoS ONE. Citation for the original published paper (version of record): Wiren, S., Drevin, L., Akre, O., Robinson, D.,
Best Papers. F. Fusco
 Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer
 Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer Preliminary Results from the National Program of Cancer Registries Patterns of Care Study (PoC1) NAACCR Annual Meeting
Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer Preliminary Results from the National Program of Cancer Registries Patterns of Care Study (PoC1) NAACCR Annual Meeting
Pre-test. Prostate Cancer The Good News: Prostate Cancer Screening 2012: Putting the PSA Controversy to Rest
 Pre-test Matthew R. Cooperberg, MD, MPH UCSF 40 th Annual Advances in Internal Medicine Prostate Cancer Screening 2012: Putting the PSA Controversy to Rest 1. I do not offer routine PSA screening, and
Pre-test Matthew R. Cooperberg, MD, MPH UCSF 40 th Annual Advances in Internal Medicine Prostate Cancer Screening 2012: Putting the PSA Controversy to Rest 1. I do not offer routine PSA screening, and
Erectile Function Before and After Non-Nerve-Sparing Retropubic Radical Prostatectomy
 Archives of Urology ISSN: 2638-5228 Volume 1, Issue 2, 2018, PP: 5-9 Erectile Function Before and After Non-Nerve-Sparing Retropubic Radical Prostatectomy Jørgen Bjerggaard Jensen, MD 1, Jørgen K. Johansen,
Archives of Urology ISSN: 2638-5228 Volume 1, Issue 2, 2018, PP: 5-9 Erectile Function Before and After Non-Nerve-Sparing Retropubic Radical Prostatectomy Jørgen Bjerggaard Jensen, MD 1, Jørgen K. Johansen,
Radical Prostatectomy versus Watchful Waiting in Early Prostate Cancer
 The new england journal of medicine original article Radical Prostatectomy versus Watchful Waiting in Early Prostate Cancer Anna Bill-Axelson, M.D., Lars Holmberg, M.D., Ph.D., Mirja Ruutu, M.D., Ph.D.,
The new england journal of medicine original article Radical Prostatectomy versus Watchful Waiting in Early Prostate Cancer Anna Bill-Axelson, M.D., Lars Holmberg, M.D., Ph.D., Mirja Ruutu, M.D., Ph.D.,
Prostate-Specific Antigen Based Screening for Prostate Cancer Evidence Report and Systematic Review for the US Preventive Services Task Force
 Clinical Review & Education JAMA US Preventive Services Task Force EVIDENCE REPORT Prostate-Specific Antigen Based Screening for Prostate Cancer Evidence Report and Systematic Review for the US Preventive
Clinical Review & Education JAMA US Preventive Services Task Force EVIDENCE REPORT Prostate-Specific Antigen Based Screening for Prostate Cancer Evidence Report and Systematic Review for the US Preventive
Prognostic value of the Gleason score in prostate cancer
 BJU International (22), 89, 538 542 Prognostic value of the Gleason score in prostate cancer L. EGEVAD, T. GRANFORS*, L. KARLBERG*, A. BERGH and P. STATTIN Department of Pathology and Cytology, Karolinska
BJU International (22), 89, 538 542 Prognostic value of the Gleason score in prostate cancer L. EGEVAD, T. GRANFORS*, L. KARLBERG*, A. BERGH and P. STATTIN Department of Pathology and Cytology, Karolinska
Controversies in Prostate Cancer Screening
 Controversies in Prostate Cancer Screening William J Catalona, MD Northwestern University Chicago Disclosure: Beckman Coulter, a manufacturer of PSA assays, provides research support PSA Screening Recommendations
Controversies in Prostate Cancer Screening William J Catalona, MD Northwestern University Chicago Disclosure: Beckman Coulter, a manufacturer of PSA assays, provides research support PSA Screening Recommendations
A Competing Risk Analysis of Men Age Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer
 A Competing Risk Analysis of Men Age 55-74 Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer Peter C. Albertsen, MD 1 James A. Hanley, PhD 2 Donald F.Gleason, MD, PhD 3
A Competing Risk Analysis of Men Age 55-74 Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer Peter C. Albertsen, MD 1 James A. Hanley, PhD 2 Donald F.Gleason, MD, PhD 3
EUROPEAN UROLOGY 63 (2013)
 EUROPEAN UROLOGY 63 (2013) 101 107 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Laurence Klotz on pp. 108 110 of this issue
EUROPEAN UROLOGY 63 (2013) 101 107 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Laurence Klotz on pp. 108 110 of this issue
Long-Term Functional Outcomes after Treatment for Localized Prostate Cancer
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Long-Term Functional Outcomes after Treatment for Localized Prostate Cancer Matthew J. Resnick, M.D., Tatsuki Koyama, Ph.D., Kang-Hsien
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Long-Term Functional Outcomes after Treatment for Localized Prostate Cancer Matthew J. Resnick, M.D., Tatsuki Koyama, Ph.D., Kang-Hsien
Radical Prostatectomy versus Watchful Waiting in Early Prostate Cancer
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Prostatectomy versus Waiting in Early Prostate Cancer Anna Bill-Axelson, M.D., Ph.D., Lars Holmberg, M.D., Ph.D., Mirja Ruutu, M.D.,
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Prostatectomy versus Waiting in Early Prostate Cancer Anna Bill-Axelson, M.D., Ph.D., Lars Holmberg, M.D., Ph.D., Mirja Ruutu, M.D.,
Introduction. Original Article
 bs_bs_banner International Journal of Urology (2015) 22, 363 367 doi: 10.1111/iju.12704 Original Article Prostate-specific antigen level, stage or Gleason score: Which is best for predicting outcomes after
bs_bs_banner International Journal of Urology (2015) 22, 363 367 doi: 10.1111/iju.12704 Original Article Prostate-specific antigen level, stage or Gleason score: Which is best for predicting outcomes after
Key Words. Curative therapy Cancer-specific mortality Localized disease High risk
 The Oncologist Is Radical Prostatectomy a Useful Therapeutic Option for High-Risk Prostate Cancer in Older Men? MARKUS GRAEFEN,THORSTEN SCHLOMM Martini Clinic, Prostate Cancer Centre, University Hospital
The Oncologist Is Radical Prostatectomy a Useful Therapeutic Option for High-Risk Prostate Cancer in Older Men? MARKUS GRAEFEN,THORSTEN SCHLOMM Martini Clinic, Prostate Cancer Centre, University Hospital
10th anniversary of 1st validated CaPspecific
 Quality of Life after Treatment of Localised Prostate Cancer Dr Jeremy Grummet Clinical Uro-Oncology Fellow May 28, 2008 1 Why? This is important May be viewed as soft science Until we know which treatment
Quality of Life after Treatment of Localised Prostate Cancer Dr Jeremy Grummet Clinical Uro-Oncology Fellow May 28, 2008 1 Why? This is important May be viewed as soft science Until we know which treatment
MATERIALS AND METHODS
 Primary Triple Androgen Blockade (TAB) followed by Finasteride Maintenance (FM) for clinically localized prostate cancer (CL-PC): Long term follow-up and quality of life (QOL) SJ Tucker, JN Roundy, RL
Primary Triple Androgen Blockade (TAB) followed by Finasteride Maintenance (FM) for clinically localized prostate cancer (CL-PC): Long term follow-up and quality of life (QOL) SJ Tucker, JN Roundy, RL
Radical Prostatectomy:
 Overtreatment and undertreatment Radical Prostatectomy: An Emerging Standard of Care for High Risk Prostate Cancer Matthew R. Cooperberg, MD,MPH UCSF Radiation Oncology Update San Francisco, CA April 2,
Overtreatment and undertreatment Radical Prostatectomy: An Emerging Standard of Care for High Risk Prostate Cancer Matthew R. Cooperberg, MD,MPH UCSF Radiation Oncology Update San Francisco, CA April 2,
Prostate cancer: intervention comparisons
 National Institute for Health and Care Excellence Guideline version (Draft) Prostate cancer: intervention comparisons [G] Evidence reviews for active surveillance, radical prostatectomy or radical radiotherapy
National Institute for Health and Care Excellence Guideline version (Draft) Prostate cancer: intervention comparisons [G] Evidence reviews for active surveillance, radical prostatectomy or radical radiotherapy
VALUE AND ROLE OF PSA AS A TUMOUR MARKER OF RESPONSE/RELAPSE
 Session 3 Advanced prostate cancer VALUE AND ROLE OF PSA AS A TUMOUR MARKER OF RESPONSE/RELAPSE 1 PSA is a serine protease and the physiological role is believed to be liquefying the seminal fluid PSA
Session 3 Advanced prostate cancer VALUE AND ROLE OF PSA AS A TUMOUR MARKER OF RESPONSE/RELAPSE 1 PSA is a serine protease and the physiological role is believed to be liquefying the seminal fluid PSA
How to select the right patient for the right treatment: What role does sexuality play in Pca treatment?
 How to select the right patient for the right treatment: What role does sexuality play in Pca treatment? Andrea Salonia, MD, PhD, FECSM Università Vita-Salute San Raffaele Director, URI-Urological Research
How to select the right patient for the right treatment: What role does sexuality play in Pca treatment? Andrea Salonia, MD, PhD, FECSM Università Vita-Salute San Raffaele Director, URI-Urological Research
Elevated PSA. Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017
 Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY
 BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY AZHAN BIN YUSOFF AZHAN BIN YUSOFF 2013 SCENARIO A 66 year old man underwent Robotic Radical Prostatectomy for a T1c Gleason 4+4, PSA 15 ng/ml prostate
BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY AZHAN BIN YUSOFF AZHAN BIN YUSOFF 2013 SCENARIO A 66 year old man underwent Robotic Radical Prostatectomy for a T1c Gleason 4+4, PSA 15 ng/ml prostate
UC San Francisco UC San Francisco Previously Published Works
 UC San Francisco UC San Francisco Previously Published Works Title Positive surgical margins in radical prostatectomy patients do not predict long-term oncological outcomes: Results from the Shared Equal
UC San Francisco UC San Francisco Previously Published Works Title Positive surgical margins in radical prostatectomy patients do not predict long-term oncological outcomes: Results from the Shared Equal
HIGH MORTALITY AND POOR SURVIVAL OF MEN WITH PROSTATE CANCER IN RURAL AND REMOTE AUSTRALIA
 HIGH MORTALITY AND POOR SURVIVAL OF MEN WITH PROSTATE CANCER IN RURAL AND REMOTE AUSTRALIA The prostate is a small gland the size of a walnut which produces fluid to protect and lubricate the sperm It
HIGH MORTALITY AND POOR SURVIVAL OF MEN WITH PROSTATE CANCER IN RURAL AND REMOTE AUSTRALIA The prostate is a small gland the size of a walnut which produces fluid to protect and lubricate the sperm It
concordance indices were calculated for the entire model and subsequently for each risk group.
 ; 2010 Urological Oncology ACCURACY OF KATTAN NOMOGRAM KORETS ET AL. BJUI Accuracy of the Kattan nomogram across prostate cancer risk-groups Ruslan Korets, Piruz Motamedinia, Olga Yeshchina, Manisha Desai
; 2010 Urological Oncology ACCURACY OF KATTAN NOMOGRAM KORETS ET AL. BJUI Accuracy of the Kattan nomogram across prostate cancer risk-groups Ruslan Korets, Piruz Motamedinia, Olga Yeshchina, Manisha Desai
Causes of death in men with prostate cancer: an analysis of men from the Thames Cancer Registry
 Causes of death in men with prostate cancer: an analysis of 5 men from the Thames Cancer Registry Simon Chowdhury, David Robinson, Declan Cahill*, Alejo Rodriguez-Vida, Lars Holmberg and Henrik Møller
Causes of death in men with prostate cancer: an analysis of 5 men from the Thames Cancer Registry Simon Chowdhury, David Robinson, Declan Cahill*, Alejo Rodriguez-Vida, Lars Holmberg and Henrik Møller
Individualized Estimation of the Benefit of Radical Prostatectomy from the Scandinavian Prostate Cancer Group Randomized Trial
 EUROPEAN UROLOGY 62 (2012) 204 209 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Massimo Lazzeri and Francesco Montorsi on
EUROPEAN UROLOGY 62 (2012) 204 209 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Massimo Lazzeri and Francesco Montorsi on
Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer
 Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Elsevier Editorial System(tm) for European Urology Manuscript Draft
 Elsevier Editorial System(tm) for European Urology Manuscript Draft Manuscript Number: EURUROL-D-13-00306 Title: Post-Prostatectomy Incontinence and Pelvic Floor Muscle Training: A Defining Problem Article
Elsevier Editorial System(tm) for European Urology Manuscript Draft Manuscript Number: EURUROL-D-13-00306 Title: Post-Prostatectomy Incontinence and Pelvic Floor Muscle Training: A Defining Problem Article
TREATMENT OPTIONS FOR LOCALIZED PROSTATE CANCER: QUALITY-ADJUSTED LIFE YEARS AND THE EFFECTS OF LEAD-TIME
 ADULT UROLOGY TREATMENT OPTIONS FOR LOCALIZED PROSTATE CANCER: QUALITY-ADJUSTED LIFE YEARS AND THE EFFECTS OF LEAD-TIME VIBHA BHATNAGAR, SUSAN T. STEWART, WILLIAM W. BONNEY, AND ROBERT M. KAPLAN ABSTRACT
ADULT UROLOGY TREATMENT OPTIONS FOR LOCALIZED PROSTATE CANCER: QUALITY-ADJUSTED LIFE YEARS AND THE EFFECTS OF LEAD-TIME VIBHA BHATNAGAR, SUSAN T. STEWART, WILLIAM W. BONNEY, AND ROBERT M. KAPLAN ABSTRACT
Prostate Cancer Incidence
 Prostate Cancer: Prevention, Screening and Treatment Philip Kantoff MD Dana-Farber Cancer Institute Professor of fmedicine i Harvard Medical School Prostate Cancer Incidence # of patients 350,000 New Cases
Prostate Cancer: Prevention, Screening and Treatment Philip Kantoff MD Dana-Farber Cancer Institute Professor of fmedicine i Harvard Medical School Prostate Cancer Incidence # of patients 350,000 New Cases
Int. J. Cancer: 120, (2006)
 Int. J. Cancer: 120, 170 174 (2006) ' 2006 Wiley-Liss, Inc. PSA doubling time predicts the outcome after active surveillance in screening-detected prostate cancer: Results from the European randomized
Int. J. Cancer: 120, 170 174 (2006) ' 2006 Wiley-Liss, Inc. PSA doubling time predicts the outcome after active surveillance in screening-detected prostate cancer: Results from the European randomized
National Trends in the Management of Low and Intermediate Risk Prostate Cancer in the United States
 National Trends in the Management of Low and Intermediate Risk Prostate Cancer in the United States Adam B. Weiner, Sanjay G. Patel, Ruth Etzioni and Scott E. Eggener* From the Pritzker School of Medicine
National Trends in the Management of Low and Intermediate Risk Prostate Cancer in the United States Adam B. Weiner, Sanjay G. Patel, Ruth Etzioni and Scott E. Eggener* From the Pritzker School of Medicine
Correspondence should be addressed to Taha Numan Yıkılmaz;
 Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
Inguinal Hernia After Radical Prostatectomy for Prostate Cancer: Results From a Randomized Setting and a Nonrandomized Setting
 EUROPEAN UROLOGY 58 (2010) 719 726 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Inguinal Hernia After Radical Prostatectomy for Prostate Cancer: Results
EUROPEAN UROLOGY 58 (2010) 719 726 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Inguinal Hernia After Radical Prostatectomy for Prostate Cancer: Results
Radical Prostatectomy: Management of the Primary From Localized to Oligometasta:c Disease
 Radical Prostatectomy: Management of the Primary From Localized to Oligometasta:c Disease Disclosures I do not have anything to disclose Sexual function causes moderate to severe distress 2 years after
Radical Prostatectomy: Management of the Primary From Localized to Oligometasta:c Disease Disclosures I do not have anything to disclose Sexual function causes moderate to severe distress 2 years after
Racial variation in receipt of quality radiation therapy for prostate cancer
 https://doi.org/10.1007/s10552-018-1065-5 BRIEF REPORT Racial variation in receipt of quality for prostate cancer Daniel J. Lee 1 Zhiguo Zhao 2 Li Ching Huang 2 Tatsuki Koyoma 2 Matthew J. Resnick 1 David
https://doi.org/10.1007/s10552-018-1065-5 BRIEF REPORT Racial variation in receipt of quality for prostate cancer Daniel J. Lee 1 Zhiguo Zhao 2 Li Ching Huang 2 Tatsuki Koyoma 2 Matthew J. Resnick 1 David
Measuring the value of healthcare activities. Susan Rollason, Director of Finance and Strategy
 Measuring the value of healthcare activities Susan Rollason, Director of Finance and Strategy Items covered What are we doing and why? What have we done so far? What challenges have we faced? What are
Measuring the value of healthcare activities Susan Rollason, Director of Finance and Strategy Items covered What are we doing and why? What have we done so far? What challenges have we faced? What are
GUIDELINES ON PROSTATE CANCER
 10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
Outcomes Following Negative Prostate Biopsy for Patients with Persistent Disease after Radiotherapy for Prostate Cancer
 Clinical Urology Post-radiotherapy Prostate Biopsy for Recurrent Disease International Braz J Urol Vol. 36 (1): 44-48, January - February, 2010 doi: 10.1590/S1677-55382010000100007 Outcomes Following Negative
Clinical Urology Post-radiotherapy Prostate Biopsy for Recurrent Disease International Braz J Urol Vol. 36 (1): 44-48, January - February, 2010 doi: 10.1590/S1677-55382010000100007 Outcomes Following Negative
Prostate Cancer Treatment for Economically Disadvantaged Men
 Prostate Cancer Treatment for Economically Disadvantaged Men A Comparison of County Hospitals and Private Providers J. Kellogg Parsons, MD, MHS 1,2 ; Lorna Kwan, MPH 3 ; Sarah E. Connor, MPH 4 ; David
Prostate Cancer Treatment for Economically Disadvantaged Men A Comparison of County Hospitals and Private Providers J. Kellogg Parsons, MD, MHS 1,2 ; Lorna Kwan, MPH 3 ; Sarah E. Connor, MPH 4 ; David
Treatment Failure After Primary and Salvage Therapy for Prostate Cancer
 307 Treatment Failure After Primary and Salvage Therapy for Prostate Cancer Likelihood, Patterns of Care, and Outcomes Piyush K. Agarwal, MD 1 Natalia Sadetsky, MD, MPH 2 Badrinath R. Konety, MD, MBA 2
307 Treatment Failure After Primary and Salvage Therapy for Prostate Cancer Likelihood, Patterns of Care, and Outcomes Piyush K. Agarwal, MD 1 Natalia Sadetsky, MD, MPH 2 Badrinath R. Konety, MD, MBA 2
PSA-based Early Detection in the US:
 PSA-based Early Detection in the US: What Went Wrong, and How to Screen Smarter Matthew R. Cooperberg, MD, MPH Departments of Urology and Epidemiology & Biostatistics @dr_coops PAHO/WHO Consultation on
PSA-based Early Detection in the US: What Went Wrong, and How to Screen Smarter Matthew R. Cooperberg, MD, MPH Departments of Urology and Epidemiology & Biostatistics @dr_coops PAHO/WHO Consultation on
Prostate cancer. Treatments Side effects and management in the community setting
 Prostate cancer Treatments Side effects and management in the community setting Kristoffer Ohlin CNS Urology Janice Minter Lead Cancer Nurse St George s Hospital Agenda Prostate cancer treatments Radiotherapy
Prostate cancer Treatments Side effects and management in the community setting Kristoffer Ohlin CNS Urology Janice Minter Lead Cancer Nurse St George s Hospital Agenda Prostate cancer treatments Radiotherapy
A case-control study of lower urinary-tract infections, associated antibiotics and the risk of developing prostate cancer using PCBaSe 3.
 RESEARCH ARTICLE A case-control study of lower urinary-tract infections, associated antibiotics and the risk of developing prostate cancer using PCBaSe 3.0 Beth Russell 1 *, Hans Garmo 1,2, Kerri Beckmann
RESEARCH ARTICLE A case-control study of lower urinary-tract infections, associated antibiotics and the risk of developing prostate cancer using PCBaSe 3.0 Beth Russell 1 *, Hans Garmo 1,2, Kerri Beckmann
Health state utilities among contemporary prostate cancer patients on active surveillance
 Original Article Health state utilities among contemporary prostate cancer patients on active surveillance Stacy Loeb 1,2,3, Caitlin Curnyn 1,2, Dawn Walter 1,2, Angela Fagerlin 4, Uwe Siebert 5,6,7,8,
Original Article Health state utilities among contemporary prostate cancer patients on active surveillance Stacy Loeb 1,2,3, Caitlin Curnyn 1,2, Dawn Walter 1,2, Angela Fagerlin 4, Uwe Siebert 5,6,7,8,
Validation of the 2015 Prostate Cancer Grade Groups for Predicting Long-Term Oncologic Outcomes in a Shared Equal-Access Health System
 Original Article Validation of the 2015 Prostate Cancer Grade Groups for Predicting Long-Term Oncologic Outcomes in a Shared Equal-Access Health System Ariel A. Schulman, MD 1 ; Lauren E. Howard, MS 2
Original Article Validation of the 2015 Prostate Cancer Grade Groups for Predicting Long-Term Oncologic Outcomes in a Shared Equal-Access Health System Ariel A. Schulman, MD 1 ; Lauren E. Howard, MS 2
Prostate Cancer: Is There Standard Treatment? Who has prostate cancer? In this article:
 Focus on CME at l Université de Montréal Prostate Cancer: Is There Standard Treatment? Pierre I. Karakiewicz, MD, FRCSC; Paul Perrotte, MD, FRCSC; Fred Saad, MD, FRCSC In this article: 1. Risk factors
Focus on CME at l Université de Montréal Prostate Cancer: Is There Standard Treatment? Pierre I. Karakiewicz, MD, FRCSC; Paul Perrotte, MD, FRCSC; Fred Saad, MD, FRCSC In this article: 1. Risk factors
MORE THAN 140,000 men in the United States annually
 Time Course and Predictors of Symptoms After Primary Prostate Cancer Therapy By James A. Talcott, Judith Manola, Jack A. Clark, Irving Kaplan, Clair J. Beard, Sonya P. Mitchell, Ronald C. Chen, Michael
Time Course and Predictors of Symptoms After Primary Prostate Cancer Therapy By James A. Talcott, Judith Manola, Jack A. Clark, Irving Kaplan, Clair J. Beard, Sonya P. Mitchell, Ronald C. Chen, Michael
2015 myresearch Science Internship Program: Applied Medicine. Civic Education Office of Government and Community Relations
 2015 myresearch Science Internship Program: Applied Medicine Civic Education Office of Government and Community Relations Harguneet Singh Science Internship Program: Applied Medicine Comparisons of Outcomes
2015 myresearch Science Internship Program: Applied Medicine Civic Education Office of Government and Community Relations Harguneet Singh Science Internship Program: Applied Medicine Comparisons of Outcomes
Hormone Therapy for Prostate Cancer: Guidelines versus Clinical Practice
 european urology supplements 5 (2006) 362 368 available at www.sciencedirect.com journal homepage: www.europeanurology.com Hormone Therapy for Prostate Cancer: Guidelines versus Clinical Practice Antonio
european urology supplements 5 (2006) 362 368 available at www.sciencedirect.com journal homepage: www.europeanurology.com Hormone Therapy for Prostate Cancer: Guidelines versus Clinical Practice Antonio
EUROPEAN UROLOGY 62 (2012)
 EUROPEAN UROLOGY 62 (2012) 745 752 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Allison S. Glass, Matthew R. Cooperberg and
EUROPEAN UROLOGY 62 (2012) 745 752 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Allison S. Glass, Matthew R. Cooperberg and
Chapter 6. Long-Term Outcomes of Radical Prostatectomy for Clinically Localized Prostate Adenocarcinoma. Abstract
 Chapter 6 Long-Term Outcomes of Radical Prostatectomy for Clinically Localized Prostate Adenocarcinoma Vijaya Raj Bhatt 1, Carl M Post 2, Sumit Dahal 3, Fausto R Loberiza 4 and Jue Wang 4 * 1 Department
Chapter 6 Long-Term Outcomes of Radical Prostatectomy for Clinically Localized Prostate Adenocarcinoma Vijaya Raj Bhatt 1, Carl M Post 2, Sumit Dahal 3, Fausto R Loberiza 4 and Jue Wang 4 * 1 Department
Management of Prostate Cancer
 Clinical Decisions Interactive at www.nejm.org Management of Prostate Cancer This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed by specific clinical
Clinical Decisions Interactive at www.nejm.org Management of Prostate Cancer This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed by specific clinical
UCSF UC San Francisco Previously Published Works
 UCSF UC San Francisco Previously Published Works Title Patterns of practice in the United States: insights from CaPSURE on prostate cancer management. Permalink https://escholarship.org/uc/item/24j7405c
UCSF UC San Francisco Previously Published Works Title Patterns of practice in the United States: insights from CaPSURE on prostate cancer management. Permalink https://escholarship.org/uc/item/24j7405c
PSA is rising: What to do? After curative intended radiotherapy: More local options?
 Klinik und Poliklinik für Urologie und Kinderurologie Direktor: Prof. Dr. H. Riedmiller PSA is rising: What to do? After curative intended radiotherapy: More local options? Klinische und molekulare Charakterisierung
Klinik und Poliklinik für Urologie und Kinderurologie Direktor: Prof. Dr. H. Riedmiller PSA is rising: What to do? After curative intended radiotherapy: More local options? Klinische und molekulare Charakterisierung
When radical prostatectomy is not enough: The evolving role of postoperative
 When radical prostatectomy is not enough: The evolving role of postoperative radiation therapy Dr Tom Pickles Clinical Associate Professor, UBC. Chair, Provincial Genito-Urinary Tumour Group BC Cancer
When radical prostatectomy is not enough: The evolving role of postoperative radiation therapy Dr Tom Pickles Clinical Associate Professor, UBC. Chair, Provincial Genito-Urinary Tumour Group BC Cancer
The New England Journal of Medicine QUALITY OF LIFE AFTER RADICAL PROSTATECTOMY OR WATCHFUL WAITING
 QUALITY OF LIFE AFTER OR GUNNAR STEINECK, M.D., FRED HELGESEN, M.D., JAN ADOLFSSON, M.D., PAUL W. DICKMAN, PH.D., JAN-ERIK JOHANSSON, M.D., BO JOHAN NORLÉN, M.D., AND LARS HOLMBERG, M.D., FOR THE SCANDINAVIAN
QUALITY OF LIFE AFTER OR GUNNAR STEINECK, M.D., FRED HELGESEN, M.D., JAN ADOLFSSON, M.D., PAUL W. DICKMAN, PH.D., JAN-ERIK JOHANSSON, M.D., BO JOHAN NORLÉN, M.D., AND LARS HOLMBERG, M.D., FOR THE SCANDINAVIAN
Health-related Quality of Life After Primary Treatment for Localized Prostate Cancer: A Systematic Review of the Literature. Sara E.
 Health-related Quality of Life After Primary Treatment for Localized Prostate Cancer: A Systematic Review of the Literature By Sara E. Wobker A Master's Paper submitted to the faculty of the University
Health-related Quality of Life After Primary Treatment for Localized Prostate Cancer: A Systematic Review of the Literature By Sara E. Wobker A Master's Paper submitted to the faculty of the University
Prostate Cancer: 2010 Guidelines Update
 Prostate Cancer: 2010 Guidelines Update James L. Mohler, MD Chair, NCCN Prostate Cancer Panel Associate Director for Translational Research, Professor and Chair, Department of Urology, Roswell Park Cancer
Prostate Cancer: 2010 Guidelines Update James L. Mohler, MD Chair, NCCN Prostate Cancer Panel Associate Director for Translational Research, Professor and Chair, Department of Urology, Roswell Park Cancer
Screening for Prostate Cancer US Preventive Services Task Force Recommendation Statement
 Clinical Review & Education JAMA US Preventive Services Task Force RECOMMENDATION STATEMENT Screening for Prostate Cancer US Preventive Services Task Force Recommendation Statement US Preventive Services
Clinical Review & Education JAMA US Preventive Services Task Force RECOMMENDATION STATEMENT Screening for Prostate Cancer US Preventive Services Task Force Recommendation Statement US Preventive Services
State-of-the-art: vision on the future. Urology
 State-of-the-art: vision on the future Urology Francesco Montorsi MD FRCS Professor and Chairman Department of Urology San Raffaele Hospital Vita-Salute San Raffaele University Milan, Italy Disclosures
State-of-the-art: vision on the future Urology Francesco Montorsi MD FRCS Professor and Chairman Department of Urology San Raffaele Hospital Vita-Salute San Raffaele University Milan, Italy Disclosures
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION LESS IS MORE Risk Profiles and Treatment Patterns Among Men Diagnosed as Having Prostate Cancer and a Prostate-Specific Antigen Level Below 4. ng/ml Yu-Hsuan Shao, PhD; Peter C.
ORIGINAL INVESTIGATION LESS IS MORE Risk Profiles and Treatment Patterns Among Men Diagnosed as Having Prostate Cancer and a Prostate-Specific Antigen Level Below 4. ng/ml Yu-Hsuan Shao, PhD; Peter C.
Survival outcomes for men in rural and remote NSW. Trend in prostate cancer incidence and mortality rates in Australia. The prostate cancer conundrum
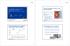 7/8/20 7/8/20 Using PROMS to better understand prostate cancer outcomes: The NSW Prostate Cancer Care and Outcomes Study David Smith Research Fellow Cancer Research Division Monash Uni, 26 th June 20 Survival
7/8/20 7/8/20 Using PROMS to better understand prostate cancer outcomes: The NSW Prostate Cancer Care and Outcomes Study David Smith Research Fellow Cancer Research Division Monash Uni, 26 th June 20 Survival
WITHOUT UNDERSTANDing
 ORIGINAL CONTRIBUTION Natural History of Early, Localized Prostate Cancer Jan-Erik Johansson, MD, PhD Ove Andrén, MD Swen-Olof Andersson, MD, PhD Paul W. Dickman, PhD Lars Holmberg, MD, PhD Anders Magnuson,
ORIGINAL CONTRIBUTION Natural History of Early, Localized Prostate Cancer Jan-Erik Johansson, MD, PhD Ove Andrén, MD Swen-Olof Andersson, MD, PhD Paul W. Dickman, PhD Lars Holmberg, MD, PhD Anders Magnuson,
Effective Health Care Program
 Comparative Effectiveness Review Number 146 Effective Health Care Program Therapies for Clinically Localized Prostate Cancer: Update of a 2008 Systematic Review Executive Summary Background Prostate cancer
Comparative Effectiveness Review Number 146 Effective Health Care Program Therapies for Clinically Localized Prostate Cancer: Update of a 2008 Systematic Review Executive Summary Background Prostate cancer
Prostate Cancer Dashboard
 Process Risk Assessment Risk assessment: family history assessment of family history of prostate cancer Best Observed: 97 %1 ; Ideal Benchmark:100% measure P8 2 Process Appropriateness of Care Pre-treatment
Process Risk Assessment Risk assessment: family history assessment of family history of prostate cancer Best Observed: 97 %1 ; Ideal Benchmark:100% measure P8 2 Process Appropriateness of Care Pre-treatment
ACTIVE SURVEILLANCE OR WATCHFUL WAITING
 Prostate Cancer ACTIVE SURVEILLANCE OR WATCHFUL WAITING María Teresa Bourlon, MD MS Head, Urologic Oncology Clinic Hemato-Oncology Department Instituto Nacional de Ciencias Médicas y Nutrición Salvador
Prostate Cancer ACTIVE SURVEILLANCE OR WATCHFUL WAITING María Teresa Bourlon, MD MS Head, Urologic Oncology Clinic Hemato-Oncology Department Instituto Nacional de Ciencias Médicas y Nutrición Salvador
ABOUT MEN WILL BE
 ORIGINAL CONTRIBUTION Comparison of ations by Urologists and Oncologists for Treatment of Clinically Localized Prostate Cancer Floyd J. Fowler, Jr, PhD Mary McNaughton Collins, MD, MPH Peter C. Albertsen,
ORIGINAL CONTRIBUTION Comparison of ations by Urologists and Oncologists for Treatment of Clinically Localized Prostate Cancer Floyd J. Fowler, Jr, PhD Mary McNaughton Collins, MD, MPH Peter C. Albertsen,
A comparative study of radical prostatectomy and permanent seed brachytherapy for low- and intermediate-risk prostate cancer
 ORIGINAL RESEARCH A comparative study of radical prostatectomy and permanent seed brachytherapy for low- and intermediate-risk prostate cancer Daniel Taussky, MD; 1 Véronique Ouellet, MD; 2 Guila Delouya,
ORIGINAL RESEARCH A comparative study of radical prostatectomy and permanent seed brachytherapy for low- and intermediate-risk prostate cancer Daniel Taussky, MD; 1 Véronique Ouellet, MD; 2 Guila Delouya,
PSA testing in New Zealand general practice
 PSA testing in New Zealand general practice Ross Lawrenson, Charis Brown, Fraser Hodgson. On behalf of the Midland Prostate Cancer Study Group Academic Steering Goup: Zuzana Obertova, Helen Conaglen, John
PSA testing in New Zealand general practice Ross Lawrenson, Charis Brown, Fraser Hodgson. On behalf of the Midland Prostate Cancer Study Group Academic Steering Goup: Zuzana Obertova, Helen Conaglen, John
Prostatectomy as salvage therapy. Cases. Paul Cathcart - Guy s & St Thomas NHS Trust, London
 Prostatectomy as salvage therapy Cases Paul Cathcart - Guy s & St Thomas NHS Trust, London Attributes of brachytherapy appeal to young men who place high utility on genitourinary function At risk of
Prostatectomy as salvage therapy Cases Paul Cathcart - Guy s & St Thomas NHS Trust, London Attributes of brachytherapy appeal to young men who place high utility on genitourinary function At risk of
PCA MORTALITY VS TREATMENTS
 PCA MORTALITY VS TREATMENTS Terrence P McGarty White Paper No 145 July, 2017 In a recent NEJM paper the authors argue that there is no material difference between a prostatectomy and just "observation"
PCA MORTALITY VS TREATMENTS Terrence P McGarty White Paper No 145 July, 2017 In a recent NEJM paper the authors argue that there is no material difference between a prostatectomy and just "observation"
Prospective assessment of the quality of life before, during and after image guided intensity modulated radiotherapy for prostate cancer
 Sveistrup et al. Radiation Oncology (2016) 11:117 DOI 10.1186/s13014-016-0689-4 RESEARCH Open Access Prospective assessment of the quality of life before, during and after image guided intensity modulated
Sveistrup et al. Radiation Oncology (2016) 11:117 DOI 10.1186/s13014-016-0689-4 RESEARCH Open Access Prospective assessment of the quality of life before, during and after image guided intensity modulated
