The XY Gonadal Agenesis Syndrome
|
|
|
- Blake Owens
- 5 years ago
- Views:
Transcription
1 Journal of Medical Genetics (1973). 10, 288. The XY Gonadal Agenesis Syndrome GLORIA E. SARTO and JOHN M. OPITZ Departments of Gynecology and Obstetrics, Pediatrics and Medical Genetics, Health Sciences and Medical School, Madison, Wisconsin, USA University of Wisconsin Center for Summary. A patient with a 46,XY chromosome constitution showed the following main characteristics: eunuchoidal body habitus, lack of secondary sexual development, normal female external genitalia with absence of vagina, no gonadal structures, and complete lack of internal genitalia except for rudimentary ductal structures defined by histological examination. Her condition is clearly different from that of feminizing testis syndrome and Swyer syndrome individuals. We would like to include her and six similar patients from the literature in a newly defined 'XY gonadal agenesis' syndrome. In mammals, the male sex determining 'factor(s)' is located on the Y chromosome. Though the presence of a Y chromosome is able to overcome the effects of more than one X chromosome in determining the male sex, a number of genes, not on the Y chromosome, are able to disturb this role. The best known examples of this phenomenon are the feminizing testis syndrome (FTS) and the Swyer syndrome, in which non-mosaic 46,XY individuals have a female phenotype. The present paper describes another condition, 'the gonadal agenesis syndrome' characterized by a 46,XY sex chromosome constitution and a female phenotype. The present case is compared to similar ones found in the literature. Case Report MS was first seen elsewhere at the age of 16 years for primary amenorrhoea and intermittent abdominal pain. Examination then (in 1960) showed a rather stocky habitus, no axillary and scant pubic hair, no breast development, a normal clitoris, immature labia majora and minora, and absence of the vagina; uterus and gonads could not be palpated. Breast development occurred only after oestrogen therapy. Cyclically recurrent abdominal pain led to hospitalization in 1961, when she was found to excrete normal amounts of 17-ketosteroids and to be X-chromatin nega- Received 18 December Research aided in part by NIH grants Nos. HD , GM 08217, GM 15422, 5 KO 4 HD (Career Development Award J.M.O.), and by grants from the National Foundation-March of Dimes, and Racine Health Fund. tive. Intravenous pyelography disclosed no abnormalities of kidneys, ureters, or bladder. At exploratory laparotomy, no internal genitalia or gonads were found. At the left pelvic wall was a small mass of tissue (measuring 1 0 x 0 5 cm) to which was attached a rudimentary fallopian tube. Similar, but smaller structures were present on the right; microscopic examination of these confirmed the diagnosis of a rudimentary fallopian tube. The patient was first seen at the University of Wisconsin Hospitals in The history of primary amenorrhoea and failure of breast development until after exogenous oestrogen treatment, was confirmed. She was born after an uneventful pregnancy of normal duration, weighing 3062 g and measuring 46 cm in length. Her health during childhood and adolescence was good, and she was of normal intelligence. Her height was around the third centile (for girls) until treatment with sex steroids at the age of 16 years. During the period of hormonal therapy she claims to have increased in height from 150 (fifth centile for girls) to 160 cm ( > 10< 25th centile for girls). Family History This is essentially unremarkable. She was the first of her mother's seven pregnancies which resulted in the birth of three sisters (now 20, 17, and 8 years old) and two brothers (13 and 11 years old). The seventh pregnancy resulted in a spontaneous abortion. All girls are of normal height. They matured at the usual age for their sex; they are of normal intelligence and have no anomalies like those of the patient. The 20-year-old sister is married and has one child; the 17-year-old sister is menstruating normally. Mother and father were 30 and 31 years old respectively when the patient 288
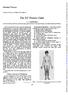
2 was born; they are apparently not related to each other and they are of normal intelligence and stature (161-5 and cm, respectively). No relative is known to have had problems like those of the patient. FIG. 1 FIG. 2 FIGS. 1 and 2. Face and general appearance of the patient; age 21 years. The XY Gonadal Agenesis Syndrome Physical Examination of the Proposita At the age of 21 years (Figs. 1 and 2) her height was 160 cm and she weighed g. She had slightly eunuchoidal body proportions. In addition to the genital malformations, she manifested several minor anomalies including a rather low posterior scalpline, a high, arched palate, bilateral ptosis with true mongolian upper lids, slightly oblong corneae with a suggestion of heterochromia iridis (right iris brown, left greenish-grey), nystagmus, a distal axial palmar triradius (50%') on the right with a relatively low* finger tip total dermatoglyphic ridge count (nine ulnar loops and one radial loop with a total ridge count of 112). Her skin was dry and the subcutaneous veins were prominently visible. The scalp hair was unusually coarse and there was hirsutism of arms and legs. Her face was covered with innumerable small freckles. She did not show shortness of metacarpals or metatarsals, nail defects, webbing of the neck, cubitus valgus, or signs of congenital heart disease. The rest of the physical examination was unremarkable. Cytogenetic Studies Feulgen stained buccal mucosal cells did not show any X-chromatin bodies. Analysis of 33 lymphocytes and of 10 fibroblasts revealed a 46,XY chromosome constitution. The Y chromosome showed a typical appearance and characteristic fluorescence pattern (Fig. 3). It was fairly large, and agreed in size with the Y chromosome of the father and her two brothers. FIG. 3. X and Y chromosomes from four metaphases from the patient, showing the characteristic fluorescence patterns. Clinical Considerations The major manifestations of the present patient are listed in Table I, and compared to other cases in the literature which have been variously discussed under such titles as: 'true agonadism' (Overzier and Linden, 1956), 'pseudohermaphroditism with multiple congenital anomalies' (Schoen * For a 46,XY constitution. 289
3 290 TABLE CHARACTERISTICS OF PRESENT CASE AND PREVIOUSLY REPORTED Present Patients Emson and Buckwold (1965) Dewhurst et al (1963) Age (yr) Body habitus; height Eunuchoid; 155 cm 145 cm Eunuchoid; 169 cm Breast development Absent Absent Minimal Extragenital High, arched palate; bilateral None; full scale IQ 97, 94 No gross anomalies; nipples widely anomalies ptosis; mongolian upper lids, etc spaced (see text) Family history Unremarkable; two normal brothers; Six sisters: normal; three brothers: Only child; mother 35 yr at birth of no consanguinity normal the patient Sex of rearing Female Male Female External genitalia Female: absent vagina; normal Ambiguous;? absent vagina;? slightly Female; absent vagina; minute blind clitoris; infantile labia enlarged clitoris; two lateral folds pit in region of introitus; normal resembling labia majora; no scrotum; clitoris; labia majora: single perineal urethral opening underdeveloped; labia minora: 2-5 cm deep posterior urethral fused outpouching Internal genitalia Gross examination No uterus: no gonadal tissue; small No genital organs; no testes or ovaries; No uterus; two tiny remnants on structure on lateral pelvic walls 'two ovoid bodies' in region of lateral walls; no gonadal tissue intemal ring Histological Rudimentary fallopian tubes 'Tubular structures of 3 types'; 'Small tubular structure resembling a examination immature fallopian tubes; uterine horn; tubules of Wolffian epididymis-like 'paraovarian duct' tubules' X-chromatin Negative Negative Negative Chromosomes 46,XY 46,XY 46,XY et al, 1955), 'an XY female with absent gonads and vestigial pelvic organs' (Dewhurst, Paine, and Blank, 1963), 'agonadism' (Emson and Buckwold, 1965), and 'gonadal dysgenesis with androgenic manifestations' (Chaptal et al, 1958). Only those cases with some evidence for a male sex chromosome constitution (eg, absence of Barr bodies) are included; only three of the reported cases, including the present one, had a chromosome analysis. It is evident from the data in Table I that the present case and those previously reported are similar in many respects. All were X-chromatin negative and, where studied, had an XY constitution. All, except the prepubertal cases (Schoen et al, 1955; Chaptal et al, 1958; Emson and Buckwold, 1965), had eunuchoidal body measurements; except for one case (Dewhurst et al, 1963) all lacked breast development. The sex of rearing was female in all except the case of Emson and Buckwold (1965). Although the present patient and the case of Schoen et al (1955) showed several minor extragenital anomalies, as a rule there seem to be no consistent major abnormalities. The vagina was absent in all cases; in three cases (Schoen et al, 1955; Overzier Sarto and Opitz and Linden, 1956; Emson and Buckwold, 1965) an enlarged clitoris and variable degrees of labioscrotal fusion were described. In two cases (Overzier and Linden, 1956; Philipp, 1956) a urogenital sinus was present; in another two (Chaptal et al, 1958; Emson and Buckwold, 1965) a small vaginal outpouching from the urethra was noted. The internal genital anomalies are similar in all cases. True internal genital structures such as uterus, fallopian tubes, or gonads are lacking; instead, small structures are located on the lateral pelvic walls and are variably described as 'ovoid bodies', 'gonads', or 'hypoplastic tubes'. Histologically, these structures are tubular and resemble in some instances the epididymis, and in others, the epoophoron, and in our case, the fallopian tube. In his book 'Intersexuality', Overzier (1961) included his sib cases and the cases of Schoen et al (1955), Philipp (1956), and of Chaptal et al (1958) as examples of the same clinical entity. His postulation of a probable sex chromosome abnormality as aetiology of the syndrome has not been confirmed. We have included these and other cases in Table I, and feel that they all represent a distinct nosologic
4 The XY Gonadal Agenesis Syndrome CASES OF PRESUMED XY GONADAL AGENESIS SYNDROME Chaptal et al (1958) Overzier and Linden (1956); Philipp (1956) Schoen et al (1955) Overzier (1961) and ; bone age 8 yr 132 cm Stocky habitus; 161 and 135 cm, respectively Eunuchoid; 169 cm 135 cm (15th centile for age) Absent Absent Absent Absent None None Turricephaly IQ 85-95; alternating esotropia; spina bifida occulta L5; S1; turribrachycephaly; deafness l l right ear 3 sibs: healthy Positive: 2 affected sisters; 4 older healthy sibs Negative 2 normal sisters Female Female Female Female Female; doubtful sex at birth; no Female; absent vagina; enlarged Female; no vagina; hypoplastic Female; absent vagina; clitorisvagina; small clitoris-like phallic phallic organ with small clitoris; hypoplastic labia; like phallic tubercle with tubercle with prepuce; small opening at its base; short urogenital sinus prepuce; no scrotum or labia; outpouching from urethra; urogenital sinus; high male-type urethra labioscrotal fusion; no scrotum perineum with median raphe or labia No uterus; no gonads; Right- No uterus; no gonads; tiny No uterus; no gonads; no tubes No uterus; no gonadal tissue; possibly hypoplastic tube structure on lateral pelvic wall no fallopian tubes Right epididymis and Primitive tube with Not described Left epoophoron; Rightepoophoron-like tubules mesonephric-type tubules epididymis-like tubules Negative Negative Negative '5 X-chromatin positive' Il (probably X-chromatin negative) Not studied Not studied Not studied Not studied entity. We would like to call it 'the XY gonadal agenesis syndrome'. This syndrome is clearly different from the feminizing testis syndrome (FTS) and from the Swyer syndrome; the latter two conditions are also characterized by a non-mosaic 46,XY chromosome constitution and by female external genitalia (Table II) Ṫhe XY gonadal agenesis syndrome is also different from the vaginal atresia syndrome (the socalled Mayer-Rokitansky-Kuster syndrome [Bryan, Nigro, and Counsellor, 1949; Hauser and Schreiner, 1961]), in which a 46,XX sex chromosome constitution is combined with normal ovarian development and maturation of female secondary sex characteristics, and frequently with major anomalies (eg, of kidneys, the cardiovascular system, etc). Developmental Considerations We are impressed with the possibility that this is a (malformation) syndrome on the basis of the associated anomalies that have been observed: skull defects (turricephaly, turribrachycephaly), vertebral 291 anomalies, low posterior hair-line, high, arched palate, ptosis with epicanthic (mongolian) folds, suggestive heterochromia iridis, nystagmus, alternating esotropia, possible dermatoglyphic abnormalities, and borderline intelligence (97, 94 in one case; in another). Also, the unique genital and gonadal findings suggest an unusual pathogenesis. The external genitalia may have a nearly normal female appearance (save for absence of the vagina); more commonly they show hypoplasia of labia, some degree of labioscrotal fusion, a small clitoris-like phallus without urethra but with dorsal prepuce, a small perineal urethral opening, and rarely a small 'pseudovaginal' urethral outpouching (Chaptal et al, 1958; Emson and Buchwold, 1965). Thus, in some cases, the external genital picture does suggest the intrauterine effect of testosterone; however, in no case was a testis found. In human males, normal inhibition of Mullerian duct differentiation and stimulation of Wolffian ducts towards male gonaductal development occurs under the influence of a fetal testis. On the other hand, Mullerian duct development and regression of the Wolffian ducts, does not require ovaries;
5 292 Sarto and Opitz TABLE II CHARACTERISTICS OF THE XY GONADAL AGENESIS SYNDROME COMPARED WITH THE FEMINIZING TESTIS SYNDROME AND SWYER SYNDROME Feminizing Testis Syndrome Swyer Syndrome XY Gonadal Agenesis Syndrome Body habitus Normal or eunuchoid Eunuchoid Eunuchoid Breast development + Family history External genitalia Female Female Female Clitoris Normal Normal; occasionally enlarged Normal; occasionally enlarged Labia Infantile Infantile Infantile, with occasional scrotal fusion Vagina Blind pouch Complete Absent Miillerian duct differentiation None Normal Rudimentary fallopian tubes; no uterus Wolffian duct None None None Gonadal structure Testis Streak Absent Buccal smear-x-chromatin Negative Negative Negative Chromosomes 46,XY 46,XY 46,XY Somatic anomalies None None Occasional minor indeed, it may occur in the absence of any gonadal tissue. As demonstrated by Jost (1947) in rabbits, and other investigators working with rats (Wells and Fralick, 1951) and mice (Raynaud and Frilley, 1947), the fetal testis is required for regression of the Mullerian ducts; early testicular dysgenesis leads to the development of apparently normal female internal genitalia without the simultaneous differentiation of Wolffian duct structures. Also, in the rabbit, Jost noted that if castration of the male was delayed beyond a certain stage, the Miillerian ducts continued to undergo involution as usual. Thus, there is a limited period of time during which involution of the Miillerian ducts is determined, and once this has occurred, the effect is irreversible. The Wolffian duct structures, however, require the testis for continued survival as well as differentiation. In the present patient and in the other reported cases, no gonads could be found to account for the internal genital findings. Perhaps, as in Jost's experiments (1947), the fetal testis was functional for a sufficient time to induce the Miulerian duct inhibition, but not long enough to maintain Wolffian duct development. A short activity of the fetal testis would also account for the partially virilized external genitalia. Another explanation for the genital/gonadal anomalies of this syndrome is a complete primary deficiency of all gonaductal anlagen with severe concomitant deficiency of the fetal testis which functioned either not at all or only long enough to effect a minimal degree of masculinization of the external genitalia. Genetic Considerations The study of the inheritance of various genes which alter or reverse sexual development is difficult because the affected individuals are sterile. Numerous intersex conditions in 46,XY and 46,XX individuals are known; most of these occur as sporadic cases. Some are 'familial disorders'; these can be divided into two groups. First, a class probably representing the homozygous state of autosome recessive mutations (eg, the adrenogenital syndromes, pseudovaginal perineoscrotal hypospadias [PPSH], the uterine hernia syndrome [UHS], and probably the Swyer syndrome); and secondly, a class representing either male-limited autosomal dominant or X-linked recessive inheritance (eg the FTS, the incomplete FTS, Reifenstein syndrome, and some cases of the Swyer syndrome). Some of the conditions in the first group affect both sexes (ie, the adrenogenital syndrome), some are limited in expression to one sex (usually the male sex, eg, the UHS and PPSH). So far, no proven case of an X-linked locus affecting sex development in man is known; however, work on the X-linked Tfm mutation in the mouse (and similar conditions in the rat and cow) suggests that the FTS in man may also be an X-linked recessive mutation (Ohno, Tettenborn, and Dofuku, 1971). However, linkage studies in the FTS have not shown linkage with any known X-linked locus. Sporadic cases of these disorders may represent new mutations, chance isolated cases, or different genetic entities altogether.
6 The seven cases which represent the present 'gonadal agenesis syndrome' are sporadic except for the two sibs described by Overzier and Linden (1956). We consider the gonadal agenesis syndrome to be a genetic disorder; however, at the present time no conclusions can be drawn concerning the mode of inheritance of this condition. We would like to thank John L. Claude, MD, Oconomowoc, Wisconsin, for referring the patient, and Dr E. Therman, and Professor K. Patau for the chromosome fluorescence studies. REFERENCES Bryan, A. L., Nigro, J. A., and Counseller, V. S. (1949). One hundred cases of congenital absence of the vagina. Surgery, Gynecology and Obstetrics, 88, Chaptal, J., Jean, R., Pages, P., Campo, C., Bonnet, H., and Duntze, F. (1958). Sur un cas de dysgenesie gonadique avec manifestations androgeniques. Archives Franfaises de Pidiatrie, 15, Dewhurst, C. J., Paine, C. G., and Blank, C. E. (1963). An XY female with absent gonads and vestigial pelvic organs. Journal of The XY Gonadal Agenesis Syndrome 293 Obstetrics and Gynaecology of the British Commonwealth, 70, Emson, H. E. and Buckwold, A. E. (1965). Agonadism. Canadian Medical Association Journal, 93, Hauser, G. A. and Schreiner, W. E. (1961). Das Mayer-Rokitansky- Kuster Syndrom. Schweizerische medizinische Wochenschrift, 91, Jost, A. (1947). Recherches sur la differenciation sexuelle de l'embryon de lapin. II. Action des androgenes synthese sur l'histogenese genitale. Archives d'anatomie Microscopique et de Morphologie Experimentale. 36, Ohno, S., Tettenborn, U., and Dofuku, R. (1971). Molecular biology of sex differentiation. Hereditas, Genetiskt Arkiv, 69, Overzier, C. (1961). Echter Agonadismus. In Intersexualitat, pp , ed. by C. Overzier. Georg Thieme, Stuttgart. Overzier, C. and Linden, H. (1956). Echter Agonadismus (Anorchismus) bei Geschwistern. Gynaecologia, 142, Philipp, E. (1956). Die Fehlbildungen der Keimdruse. Deutsche medizinische Wochenschrift, 81, Raynaud, A. and Frilley, M. (1947). Destruction des glandes genitales de l'embryon de souris, par une irradiation au moyen des rayons X, a l'age de treize jours. Annales d'endocrinologie, 8, Schoen, E. J., King, A. L., Baritell, A. LaM., and Knigge, W. F. (1955). Pseudohermaphroditism with multiple congenital anomalies. Report of a case. Pediatrics, 16, Wells, L. J. and Fralick, R. (1951). Production of androgen by the testes of fetal rats. American_Journal of Anatomy, 89, J Med Genet: first published as /jmg on 1 September Downloaded from on 21 July 2018 by guest. Protected by copyright.
Testicular feminization. The features of this syndrome in its typical form are these (Fig. 1): (1) Female bodily configuration.
 Personal Practice Archives of Disease in Childhood, 1970, 45, 595. The XY Female Child C. J. DEWHURST From the Institute of Obstetrics and Gynaecology, Queen Charlotte's Maternity Hospital, and Chelsea
Personal Practice Archives of Disease in Childhood, 1970, 45, 595. The XY Female Child C. J. DEWHURST From the Institute of Obstetrics and Gynaecology, Queen Charlotte's Maternity Hospital, and Chelsea
Normal and Abnormal Development of the Genital Tract. Dr.Raghad Abdul-Halim
 Normal and Abnormal Development of the Genital Tract Dr.Raghad Abdul-Halim objectives: Revision of embryology. Clinical presentation, investigations and clinical significance of most common developmental
Normal and Abnormal Development of the Genital Tract Dr.Raghad Abdul-Halim objectives: Revision of embryology. Clinical presentation, investigations and clinical significance of most common developmental
Sexual differentiation:
 Abnormal Development of Female Genitalia Dr. Maryam Fetal development of gonads, external genitalia, Mullerian ducts and Wolffian ducts can be disrupted at a variety of points, leading to a wide range
Abnormal Development of Female Genitalia Dr. Maryam Fetal development of gonads, external genitalia, Mullerian ducts and Wolffian ducts can be disrupted at a variety of points, leading to a wide range
DEFINITION: Masculinization of external genitalia in patients with normal 46XX karyotype.
 INTERSEX DISORDERS DEFINITION: Masculinization of external genitalia in patients with normal 46XX karyotype. - Degree of masculinization variable: - mild clitoromegaly - complete fusion of labia folds
INTERSEX DISORDERS DEFINITION: Masculinization of external genitalia in patients with normal 46XX karyotype. - Degree of masculinization variable: - mild clitoromegaly - complete fusion of labia folds
Ethiopian patients and a brief review
 Postgraduate Medical Journal (November 1979) 55, 844-848 Testicular feminization syndrome: a report of three Ethiopian patients and a brief review EDEMARIAM TSEGA M.D., D.C.M.T.(L), F.R.C.P.(C) Summary
Postgraduate Medical Journal (November 1979) 55, 844-848 Testicular feminization syndrome: a report of three Ethiopian patients and a brief review EDEMARIAM TSEGA M.D., D.C.M.T.(L), F.R.C.P.(C) Summary
IN SUMMARY HST 071 NORMAL & ABNORMAL SEXUAL DIFFERENTIATION Fetal Sex Differentiation Postnatal Diagnosis and Management of Intersex Abnormalities
 Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 Title: Fetal Sex Differentiation Postnatal Diagnosis
Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 Title: Fetal Sex Differentiation Postnatal Diagnosis
Let s Talk About Hormones!
 Let s Talk About Hormones! This lesson was created by Serena Reves and Nichelle Penney, with materials from the BCTF and The Pride Education Network. Hormones are responsible for the regulation of many
Let s Talk About Hormones! This lesson was created by Serena Reves and Nichelle Penney, with materials from the BCTF and The Pride Education Network. Hormones are responsible for the regulation of many
Development of the Genital System
 Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
Approach to Disorders of Sex Development (DSD)
 Approach to Disorders of Sex Development (DSD) Old name: The Approach to Intersex Disorders Dr. Abdulmoein Al-Agha, FRCP Ass. Professor & Consultant Pediatric Endocrinologist, KAUH, Erfan Hospital & Ibn
Approach to Disorders of Sex Development (DSD) Old name: The Approach to Intersex Disorders Dr. Abdulmoein Al-Agha, FRCP Ass. Professor & Consultant Pediatric Endocrinologist, KAUH, Erfan Hospital & Ibn
Development of the urogenital system
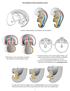 Development of the urogenital system Location of the pronephros, mesonephros and metanephros Differentiation of the intermedierm mesoderm into nephrotome and mesonephric tubules Connection between aorta
Development of the urogenital system Location of the pronephros, mesonephros and metanephros Differentiation of the intermedierm mesoderm into nephrotome and mesonephric tubules Connection between aorta
1) Intersexuality - Dr. Huda
 1) Intersexuality - Dr. Huda DSD (Disorders of sex development) occur when there is disruption of either: Gonadal differentiation Fetal sex steroid production or action Mullerian abnormalities and Wolffian
1) Intersexuality - Dr. Huda DSD (Disorders of sex development) occur when there is disruption of either: Gonadal differentiation Fetal sex steroid production or action Mullerian abnormalities and Wolffian
Intersex Genital Mutilations in ICD-10 Zwischengeschlecht.org / StopIGM.org 2014 (v2.1)
 Intersex Genital Mutilations in ICD-10 Zwischengeschlecht.org / StopIGM.org 2014 (v2.1) ICD-10 Codes and Descriptions: http://apps.who.int/classifications/icd10/browse/2010/en 1. Reference: 17 Most Common
Intersex Genital Mutilations in ICD-10 Zwischengeschlecht.org / StopIGM.org 2014 (v2.1) ICD-10 Codes and Descriptions: http://apps.who.int/classifications/icd10/browse/2010/en 1. Reference: 17 Most Common
W.S. O University of Hong Kong
 W.S. O University of Hong Kong Development of the Genital System 1. Sexual differentiation 2. Differentiation of the gonads a. Germ cells extragonadal in origin b. Genital ridge intermediate mesoderm consisting
W.S. O University of Hong Kong Development of the Genital System 1. Sexual differentiation 2. Differentiation of the gonads a. Germ cells extragonadal in origin b. Genital ridge intermediate mesoderm consisting
Chapter 18 Development. Sexual Differentiation
 Chapter 18 Development Sexual Differentiation There Are Many Levels of Sex Determination Chromosomal Sex Gonadal Sex Internal Sex Organs External Sex Organs Brain Sex Gender Identity Gender Preference
Chapter 18 Development Sexual Differentiation There Are Many Levels of Sex Determination Chromosomal Sex Gonadal Sex Internal Sex Organs External Sex Organs Brain Sex Gender Identity Gender Preference
PHYSIOLOGY AND PATHOLOGY OF SEXUAL DIFFERENTIATION
 PHYSIOLOGY AND PATHOLOGY OF SEXUAL DIFFERENTIATION Prof. Dr med. Jolanta Słowikowska-Hilczer Department of Andrology and Reproductive Endocrinology Medical University of Łódź, Poland Sexual determination
PHYSIOLOGY AND PATHOLOGY OF SEXUAL DIFFERENTIATION Prof. Dr med. Jolanta Słowikowska-Hilczer Department of Andrology and Reproductive Endocrinology Medical University of Łódź, Poland Sexual determination
Goals. Disorders of Sex Development (Intersex): An Overview. Joshua May, MD Pediatric Endocrinology
 Disorders of Sex Development (Intersex): An Overview Joshua May, MD Pediatric Endocrinology Murphy, et al., J Ped Adol Gynecol, 2011 Goals Objectives: Participants will be able to: 1. Apply the medical
Disorders of Sex Development (Intersex): An Overview Joshua May, MD Pediatric Endocrinology Murphy, et al., J Ped Adol Gynecol, 2011 Goals Objectives: Participants will be able to: 1. Apply the medical
Disordered Sex Differentiation Mixed gonadal dysgenesis Congenital adrenal hyperplasia Mixed gonadal dysgenesis
 Disordered Sex Differentiation DSD has superceded intersex in describing genital anomalies in childhood DSD results from hormonal imbalances due to (i) abnormal genetic status, (ii) enzyme defects, or
Disordered Sex Differentiation DSD has superceded intersex in describing genital anomalies in childhood DSD results from hormonal imbalances due to (i) abnormal genetic status, (ii) enzyme defects, or
4.05 Remember the structures of the reproductive system
 4.05 Remember the structures of the reproductive system 4.05 Remember the structures of the reproductive system Essential question What are the structures of the reproductive system? 2 Structures of the
4.05 Remember the structures of the reproductive system 4.05 Remember the structures of the reproductive system Essential question What are the structures of the reproductive system? 2 Structures of the
Sex Determination and Development of Reproductive Organs
 Sex Determination and Development of Reproductive Organs Sex determination The SRY + gene is necessary and probably sufficient for testis development The earliest sexual difference appears in the gonad
Sex Determination and Development of Reproductive Organs Sex determination The SRY + gene is necessary and probably sufficient for testis development The earliest sexual difference appears in the gonad
When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood
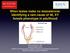 When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood Gardner DG, Shoback D. Greenspan's Basic & Clinical Endocrinology, 10e; 2017 Sira Korpaisarn, MD Endocrinology
When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood Gardner DG, Shoback D. Greenspan's Basic & Clinical Endocrinology, 10e; 2017 Sira Korpaisarn, MD Endocrinology
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
FLASH CARDS. Kalat s Book Chapter 11 Alphabetical
 FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 11 Alphabetical alpha-fetoprotein alpha-fetoprotein Alpha-Fetal Protein (AFP) or alpha-1- fetoprotein. During a prenatal sensitive period, estradiol
FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 11 Alphabetical alpha-fetoprotein alpha-fetoprotein Alpha-Fetal Protein (AFP) or alpha-1- fetoprotein. During a prenatal sensitive period, estradiol
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
AMBIGUOUS GENITALIA. Dr. HAKIMI, SpAK. Dr. MELDA DELIANA, SpAK
 AMBIGUOUS GENITALIA (DISORDERS OF SEXUAL DEVELOPMENT) Dr. HAKIMI, SpAK Dr. MELDA DELIANA, SpAK Dr. SISKA MAYASARI LUBIS, SpA Pediatric Endocrinology division USU/H. ADAM MALIK HOSPITAL 1 INTRODUCTION Normal
AMBIGUOUS GENITALIA (DISORDERS OF SEXUAL DEVELOPMENT) Dr. HAKIMI, SpAK Dr. MELDA DELIANA, SpAK Dr. SISKA MAYASARI LUBIS, SpA Pediatric Endocrinology division USU/H. ADAM MALIK HOSPITAL 1 INTRODUCTION Normal
AND TREATMENT OF HERMAPHRODITISM*
 THE DIAGNOSIS AND TREATMENT OF HERMAPHRODITISM* BY C. C. WINKEL SMITH From the Paediatric Surgical Department, Rigshospitalet, University of Copenhagen, Denmark (RECEIVED FOR PUBLICATION OCTOBER 8, 1959)
THE DIAGNOSIS AND TREATMENT OF HERMAPHRODITISM* BY C. C. WINKEL SMITH From the Paediatric Surgical Department, Rigshospitalet, University of Copenhagen, Denmark (RECEIVED FOR PUBLICATION OCTOBER 8, 1959)
Urogenital System. PUMC Dept. of Anat. Hist. & Embry. 钱晓菁 XIAO-JING QIAN Dept. of Anatomy, Histology & Embryology Peking Union Medical College
 Urogenital System 钱晓菁 XIAO-JING QIAN Dept. of Anatomy, Histology & Embryology Peking Union Medical College intermediate mesoderm urogenital ridge mesonephric ridge genital ridge I. Urinary System 1. kidney
Urogenital System 钱晓菁 XIAO-JING QIAN Dept. of Anatomy, Histology & Embryology Peking Union Medical College intermediate mesoderm urogenital ridge mesonephric ridge genital ridge I. Urinary System 1. kidney
DEVELOPMENT (DSD) 1 4 DISORDERS OF SEX
 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 4. Disorders of sex development (DSD). Horm Res 2007;68(suppl 2):21 24 ESPE Code Diagnosis OMIM ICD 10 4 DISORDERS
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 4. Disorders of sex development (DSD). Horm Res 2007;68(suppl 2):21 24 ESPE Code Diagnosis OMIM ICD 10 4 DISORDERS
10. Development of genital system. Gonads. Genital ducts. External genitalia.
 10. Development of genital system. Gonads. Genital ducts. External genitalia. Gonads, genital ducts and the external genital organs initially pass through an indifferent period of development, which is
10. Development of genital system. Gonads. Genital ducts. External genitalia. Gonads, genital ducts and the external genital organs initially pass through an indifferent period of development, which is
11. SEXUAL DIFFERENTIATION. Germinal cells, gonocytes. Indifferent stage INDIFFERENT STAGE
 11. SEXUAL DIFFERENTIATION INDIFFERENT STAGE Early in pregnancy, (within 10-15 % of the pregnancy s expected length) a genital ridge is formed in the sides of the embryonic tissue, ventral to the mesonephros
11. SEXUAL DIFFERENTIATION INDIFFERENT STAGE Early in pregnancy, (within 10-15 % of the pregnancy s expected length) a genital ridge is formed in the sides of the embryonic tissue, ventral to the mesonephros
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
2. Which male target tissues respond to testosterone, and which require dihydrotestosterone?
 308 PHYSIOLOGY CASES AND PROBLEMS Case 56 Male Pseudohermaphroditism: Sa-Reductase Deficiency Fourteen years ago, Wally and Wanda Garvey, who live in rural North Carolina, had their first child. The baby
308 PHYSIOLOGY CASES AND PROBLEMS Case 56 Male Pseudohermaphroditism: Sa-Reductase Deficiency Fourteen years ago, Wally and Wanda Garvey, who live in rural North Carolina, had their first child. The baby
4.05 Remember the structures of the reproductive system
 4.05 Remember the structures of the reproductive system Scrub In The external area between the vulva and the anus is the : a. Cervix b. Endometrium c. Perineum d. Vagina What structure connects the testes
4.05 Remember the structures of the reproductive system Scrub In The external area between the vulva and the anus is the : a. Cervix b. Endometrium c. Perineum d. Vagina What structure connects the testes
OVOTESTIS Background Pathophysiology
 OVOTESTIS Background Ovotestis refers to the histology of a gonad that contains both ovarian follicles and testicular tubular elements. Such gonads are found exclusively in people with ovotesticular disorder
OVOTESTIS Background Ovotestis refers to the histology of a gonad that contains both ovarian follicles and testicular tubular elements. Such gonads are found exclusively in people with ovotesticular disorder
Sexual Development. 6 Stages of Development
 6 Sexual Development 6 Stages of Development Development passes through distinct stages, the first of which is fertilization, when one sperm enters one ovum. To enter an ovum, a sperm must undergo the
6 Sexual Development 6 Stages of Development Development passes through distinct stages, the first of which is fertilization, when one sperm enters one ovum. To enter an ovum, a sperm must undergo the
ISSN International Journal of Innovative and Applied Research (2017) Journal home page: RESEARCH ARTICLE
 Journal home page: http://www.journalijiar.com RESEARCH ARTICLE MAYER-ROKITANSKY-KUSTER-HAUSER SYNDROME II (Rare Case). * Dr. Verinder Dhar 1 and Dr. Renu Hashia 2. 1. MD(Medicine), DM(Endo),Medicare Nursing
Journal home page: http://www.journalijiar.com RESEARCH ARTICLE MAYER-ROKITANSKY-KUSTER-HAUSER SYNDROME II (Rare Case). * Dr. Verinder Dhar 1 and Dr. Renu Hashia 2. 1. MD(Medicine), DM(Endo),Medicare Nursing
under its influence, male development occurs; in its absence, female development is established.
 Sex differentiation is a complex process that involves many genes, including some that are autosomal. The key to sexual dimorphism is the Y chromosome, which contains the testis determining gene called
Sex differentiation is a complex process that involves many genes, including some that are autosomal. The key to sexual dimorphism is the Y chromosome, which contains the testis determining gene called
CHROMOSOMAL NUMERICAL ABERRATIONS INSTITUTE OF BIOLOGY AND MEDICAL GENETICS OF THE 1 ST FACULTY OF MEDICINE
 CHROMOSOMAL NUMERICAL ABERRATIONS INSTITUTE OF BIOLOGY AND MEDICAL GENETICS OF THE 1 ST FACULTY OF MEDICINE CHROMOSOMAL ABERRATIONS NUMERICAL STRUCTURAL ANEUPLOIDY POLYPLOIDY MONOSOMY TRISOMY TRIPLOIDY
CHROMOSOMAL NUMERICAL ABERRATIONS INSTITUTE OF BIOLOGY AND MEDICAL GENETICS OF THE 1 ST FACULTY OF MEDICINE CHROMOSOMAL ABERRATIONS NUMERICAL STRUCTURAL ANEUPLOIDY POLYPLOIDY MONOSOMY TRISOMY TRIPLOIDY
MANAGEMENT AND REPORT OF A CASE OF INTERSEX. By N. JOHN WILDE, D.D.S., M.D., JUAN J. TUR, M.D. and FRED W. BIEKER, M.D.
 MANAGEMENT AND REPORT OF A CASE OF INTERSEX By N. JOHN WILDE, D.D.S., M.D., JUAN J. TUR, M.D. and FRED W. BIEKER, M.D. Fresno, California, U.S.A. DURING man's embryological development, the analogues of
MANAGEMENT AND REPORT OF A CASE OF INTERSEX By N. JOHN WILDE, D.D.S., M.D., JUAN J. TUR, M.D. and FRED W. BIEKER, M.D. Fresno, California, U.S.A. DURING man's embryological development, the analogues of
Bios 90/95. Jennifer Swann, PhD
 Sexual Differentiation Fall 2007 Bios 90/95 Jennifer Swann, PhD Dept Biol Sci, Lehigh University Why have sexes? What determines sex? Environment Genetics Hormones What causes these differences? The true
Sexual Differentiation Fall 2007 Bios 90/95 Jennifer Swann, PhD Dept Biol Sci, Lehigh University Why have sexes? What determines sex? Environment Genetics Hormones What causes these differences? The true
Obstetrics Content Outline Obstetrics - Fetal Abnormalities
 Obstetrics Content Outline Obstetrics - Fetal Abnormalities Effective February 2007 10 16% renal agenesis complete absence of the kidneys occurs when ureteric buds fail to develop Or degenerate before
Obstetrics Content Outline Obstetrics - Fetal Abnormalities Effective February 2007 10 16% renal agenesis complete absence of the kidneys occurs when ureteric buds fail to develop Or degenerate before
Embryology /organogenesis/ Week 4 Development and teratology of reproductive system.
 Embryology /organogenesis/ Week 4 Development and teratology of reproductive system. Male or female sex is determined by spermatozoon Y in the moment of fertilization SRY gene, on the short arm of the
Embryology /organogenesis/ Week 4 Development and teratology of reproductive system. Male or female sex is determined by spermatozoon Y in the moment of fertilization SRY gene, on the short arm of the
Hearing on SJR13 -- Proposes to amend the Nevada Constitution by repealing the limitation on the recognition of marriage.
 Written statement of Lauren A. Scott- Executive Director Equality Nevada. 1350 Freeport Blvd, #107 Sparks, Nevada 89431 Testimony and Statement for the Record of Hearing on SJR13 -- Proposes to amend the
Written statement of Lauren A. Scott- Executive Director Equality Nevada. 1350 Freeport Blvd, #107 Sparks, Nevada 89431 Testimony and Statement for the Record of Hearing on SJR13 -- Proposes to amend the
The Biology of Sex: How We Become Male or Female.
 The Biology of Sex: How We Become Male or Female. Dr. Tamatha Barbeau, Dept. of Biology Guest Lecture for Gender 200 March 2017 Objectives: 1. Sex vs. Gender defined. 2. Biological sex based on inheritance
The Biology of Sex: How We Become Male or Female. Dr. Tamatha Barbeau, Dept. of Biology Guest Lecture for Gender 200 March 2017 Objectives: 1. Sex vs. Gender defined. 2. Biological sex based on inheritance
Chromosome pathology
 Chromosome pathology S. Dahoun Department of Gynecology and Obstetrics, University Hospital of Geneva Cytogenetics is the study of chromosomes and the related disease states caused by abnormal chromosome
Chromosome pathology S. Dahoun Department of Gynecology and Obstetrics, University Hospital of Geneva Cytogenetics is the study of chromosomes and the related disease states caused by abnormal chromosome
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Female Reproduction. Ova- Female reproduction cells stored in the ovaries
 Reproduction Puberty stage of growth and development where males and females become capable of producing offspring. Time of physical and emotional changes. Female *occurs between ages 8 -- 15 *estrogen
Reproduction Puberty stage of growth and development where males and females become capable of producing offspring. Time of physical and emotional changes. Female *occurs between ages 8 -- 15 *estrogen
Development of the female Reproductive System. Dr. Susheela Rani
 Development of the female Reproductive System Dr. Susheela Rani Genital System Gonads Internal genitals External genitals Determining sex chronology of events Genetic sex Determined at fertilization Gonadal
Development of the female Reproductive System Dr. Susheela Rani Genital System Gonads Internal genitals External genitals Determining sex chronology of events Genetic sex Determined at fertilization Gonadal
CHAPTER-VII : SUMMARY AND CONCLUSIONS
 CHAPTER-VII : SUMMARY AND CONCLUSIONS 199 SUMMARY AND CONCLUSIONS t The rapid development of human genetics during the past couple of decades and the discovery of numerous cytogenetic abnormalities have
CHAPTER-VII : SUMMARY AND CONCLUSIONS 199 SUMMARY AND CONCLUSIONS t The rapid development of human genetics during the past couple of decades and the discovery of numerous cytogenetic abnormalities have
Hearing on SJR13 -- Proposes to amend the Nevada Constitution by repealing the limitation on the recognition of marriage.
 Written statement of Lauren A. Scott- Executive Director Equality Nevada 1350 Freeport Blvd, #107 Sparks, Nevada 89431 Testimony and Statement for the Record of Hearing on SJR13 -- Proposes to amend the
Written statement of Lauren A. Scott- Executive Director Equality Nevada 1350 Freeport Blvd, #107 Sparks, Nevada 89431 Testimony and Statement for the Record of Hearing on SJR13 -- Proposes to amend the
Chromosome Studies in 150 Sexually Abnormal Patients (A Summarized Report)1,2
 1966 349 Studies in 150 Sexually Abnormal Patients (A Summarized Report)1,2 Part II Received October 12, 1965 Sajiro Makino Zoological Institute, Hokkaido University, Sapporo, Japan Part II describes cytogenetical
1966 349 Studies in 150 Sexually Abnormal Patients (A Summarized Report)1,2 Part II Received October 12, 1965 Sajiro Makino Zoological Institute, Hokkaido University, Sapporo, Japan Part II describes cytogenetical
Please Take Seats by Gender as Shown Leave Three Seats Empty in the Middle
 Please Take Seats by Gender as Shown Leave Three Seats Empty in the Middle Women Men Sexual Differentiation & Development Neal G. Simon, Ph.D. Professor Dept. of Biological Sciences Signaling Cascade &
Please Take Seats by Gender as Shown Leave Three Seats Empty in the Middle Women Men Sexual Differentiation & Development Neal G. Simon, Ph.D. Professor Dept. of Biological Sciences Signaling Cascade &
Biology 224 Human Anatomy and Physiology II Week 9; Lecture 2; Wednesday Stuart Sumida. Development and Structure, of the Reproductive System
 Biology 224 Human Anatomy and Physiology II Week 9; Lecture 2; Wednesday Stuart Sumida Development and Structure, of the Reproductive System Don t forget the relationships of the structures of the layers
Biology 224 Human Anatomy and Physiology II Week 9; Lecture 2; Wednesday Stuart Sumida Development and Structure, of the Reproductive System Don t forget the relationships of the structures of the layers
Urinary system development. Male ( ) and Female ( ) Reproductive Systems Development
 Urinary system development Male ( ) and Female ( ) Reproductive Systems Development Urogenital system develops from mesodermal uro-genital ridge (intermediate mesoderm) development of male and female genital
Urinary system development Male ( ) and Female ( ) Reproductive Systems Development Urogenital system develops from mesodermal uro-genital ridge (intermediate mesoderm) development of male and female genital
A CHROMOSOME STUDY IN 20 SEXUALLY ABNORMAL PATIENTS>> WOSAMU MARUYAMA, HACHIRO SHIMBA AND SET-ICHI KOHNO
 JAPAN. J. GENETICS Vol. 43, No. 4: 289-298 (1968) A CHROMOSOME STUDY IN 20 SEXUALLY ABNORMAL PATIENTS>> WOSAMU MARUYAMA, HACHIRO SHIMBA AND SET-ICHI KOHNO Received May 9, 1968 Zoological Institute, Hokkaido
JAPAN. J. GENETICS Vol. 43, No. 4: 289-298 (1968) A CHROMOSOME STUDY IN 20 SEXUALLY ABNORMAL PATIENTS>> WOSAMU MARUYAMA, HACHIRO SHIMBA AND SET-ICHI KOHNO Received May 9, 1968 Zoological Institute, Hokkaido
Chapter 7 DEVELOPMENT AND SEX DETERMINATION
 Chapter 7 DEVELOPMENT AND SEX DETERMINATION Chapter Summary The male and female reproductive systems produce the sperm and eggs, and promote their meeting and fusion, which results in a fertilized egg.
Chapter 7 DEVELOPMENT AND SEX DETERMINATION Chapter Summary The male and female reproductive systems produce the sperm and eggs, and promote their meeting and fusion, which results in a fertilized egg.
46 XY gonadal dysgenesis in adulthood pitfalls of late diagnosis
 Reminder of important clinical lesson 46 XY gonadal dysgenesis in adulthood pitfalls of late diagnosis Jarna Naing Hamin,1 Francis Raymond P Arkoncel,2 Frances Lina Lantion-Ang,1 Mark Anthony S Sandoval1
Reminder of important clinical lesson 46 XY gonadal dysgenesis in adulthood pitfalls of late diagnosis Jarna Naing Hamin,1 Francis Raymond P Arkoncel,2 Frances Lina Lantion-Ang,1 Mark Anthony S Sandoval1
Animal Science 434 Reproductive Physiology"
 Animal Science 434 Reproductive Physiology" Embryogenesis of the Pituitary and Sexual Development: Part A Development of the Pituitary Gland" Infundibulum" Brain" Rathke s Pouch" Stomodeum" Germ Cell Migration"
Animal Science 434 Reproductive Physiology" Embryogenesis of the Pituitary and Sexual Development: Part A Development of the Pituitary Gland" Infundibulum" Brain" Rathke s Pouch" Stomodeum" Germ Cell Migration"
normally developed. Copenhagen, Denmark (Prof. dr. med. Dyre Trolle) By Krzysztof Boczkowski, John Philip
 Endocrine Department (Doc. dr. med. J. Teter) First Clinic of Obstetrics and Gynaecology, Medical Academy in Warsaw, Poland (Prof. dr. med. T. Bulski) and University Department of Obstetrics and Gynaecology,
Endocrine Department (Doc. dr. med. J. Teter) First Clinic of Obstetrics and Gynaecology, Medical Academy in Warsaw, Poland (Prof. dr. med. T. Bulski) and University Department of Obstetrics and Gynaecology,
ANATOMY AND PHYSIOLOGY HOMEWORK CHAPTER 15 AND 16
 ANATOMY AND PHYSIOLOGY HOMEWORK CHAPTER 15 AND 16 Name Identify the following: 1) The ureter is indicated by letter 2) The renal pyramid is indicated by letter 3) The fibrous capsule is indicated by letter
ANATOMY AND PHYSIOLOGY HOMEWORK CHAPTER 15 AND 16 Name Identify the following: 1) The ureter is indicated by letter 2) The renal pyramid is indicated by letter 3) The fibrous capsule is indicated by letter
Action of reproductive hormones through the life span 9/22/99
 Action of reproductive hormones through the life span Do reproductive hormones affect the life span? One hypothesis about the rate of aging asserts that there is selective pressure for either high rate
Action of reproductive hormones through the life span Do reproductive hormones affect the life span? One hypothesis about the rate of aging asserts that there is selective pressure for either high rate
Pseudohermaphroditism due to Congenital Adrenal Hyperplasia
 Pseudohermaphroditism due to Congenital Adrenal Hyperplasia Byoung Uk Park Universidad Francisco Marroquín October 19, 2015 Agenda 1. Case Presentation 2. Image Findings 3. Discussion I. Definition/Incidence
Pseudohermaphroditism due to Congenital Adrenal Hyperplasia Byoung Uk Park Universidad Francisco Marroquín October 19, 2015 Agenda 1. Case Presentation 2. Image Findings 3. Discussion I. Definition/Incidence
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System
 Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
Ambiguous genitalia: An approach to its diagnosis
 Ambiguous genitalia: An approach to its diagnosis Poster No.: C-2828 Congress: ECR 2010 Type: Topic: Scientific Exhibit Pediatric Authors: E. Doménech Abellán, C. Serrano García, A. Gilabert Úbeda, F.
Ambiguous genitalia: An approach to its diagnosis Poster No.: C-2828 Congress: ECR 2010 Type: Topic: Scientific Exhibit Pediatric Authors: E. Doménech Abellán, C. Serrano García, A. Gilabert Úbeda, F.
Management of gonads in DSD
 Management of gonads in DSD Martine Cools, paediatric endocrinologist, Katja Wolffenbuttel and Piet Hoebeke, paediatric urologists, all at University Hospital Ghent, Belgium Sten Drop, paediatric endocrinologist
Management of gonads in DSD Martine Cools, paediatric endocrinologist, Katja Wolffenbuttel and Piet Hoebeke, paediatric urologists, all at University Hospital Ghent, Belgium Sten Drop, paediatric endocrinologist
Topic 13 Sex. Being Male and Female
 Topic 13 Sex Being Male and Female Reproduction Asexual (1 individual): more efficient, low genetic variation Sexual: prevalent (2 sexes, separate or not) High genetic variation, need 2 Approaches: External
Topic 13 Sex Being Male and Female Reproduction Asexual (1 individual): more efficient, low genetic variation Sexual: prevalent (2 sexes, separate or not) High genetic variation, need 2 Approaches: External
Ambiguous genitalia (Disorders of sex development); is any case in which the external genitalia do not appear completely male or completely female.
 Ambiguous genitalia (Disorders of sex development); is any case in which the external genitalia do not appear completely male or completely female. Disorders of sex development (DSD); True hermaphrodite;
Ambiguous genitalia (Disorders of sex development); is any case in which the external genitalia do not appear completely male or completely female. Disorders of sex development (DSD); True hermaphrodite;
A Young Asian Girl with MRKH Type B Syndrome: A Case Report
 A Young Asian Girl with MRKH Type B Syndrome: A Case Report Nidhi Jain 1, Pardaman Singh 2, Deepak Goel 3, Jyotsna kamra 4 1,4 Department of Obstetrics and Gynecology, Maharaja Agarsein Medical College,
A Young Asian Girl with MRKH Type B Syndrome: A Case Report Nidhi Jain 1, Pardaman Singh 2, Deepak Goel 3, Jyotsna kamra 4 1,4 Department of Obstetrics and Gynecology, Maharaja Agarsein Medical College,
Genitalia And Identity Crisis The state of being neither male nor female may be
 25 Genitalia And Identity Crisis The state of being neither male nor female may be understood in relation to the individual s biological sex, gender role, gender identity or sexual orientation. In sociology,
25 Genitalia And Identity Crisis The state of being neither male nor female may be understood in relation to the individual s biological sex, gender role, gender identity or sexual orientation. In sociology,
Sexual differentiation is sequential process:
 Genital lsystem J. H. Lue Sexual differentiation is sequential process:.genetic (chromosomal) sex -- determined at fertilization.gonad sex -- is differentiated after 7th week.phenotypic sex -- under normal
Genital lsystem J. H. Lue Sexual differentiation is sequential process:.genetic (chromosomal) sex -- determined at fertilization.gonad sex -- is differentiated after 7th week.phenotypic sex -- under normal
CONGENITAL ABNORMALITIES OF GENITAL TRACT - VAGINAL DEFECTS
 CONGENITAL ABNORMALITIES OF GENITAL TRACT - VAGINAL DEFECTS Abstract Pages with reference to book, From 256 To 261 Asif Zia Akhtar ( Department of Obstetric and Gynaecology, Abbasi Shaheed Hospital, Karachi.
CONGENITAL ABNORMALITIES OF GENITAL TRACT - VAGINAL DEFECTS Abstract Pages with reference to book, From 256 To 261 Asif Zia Akhtar ( Department of Obstetric and Gynaecology, Abbasi Shaheed Hospital, Karachi.
17. Sex. Being Male and Female
 17. Sex Being Male and Female Reproduction Asexual: more efficient (Only 1 sex) Low genetic variation Sexual: prevalent (2 sexes, separate or not) High genetic variation Need 2 members of the same species
17. Sex Being Male and Female Reproduction Asexual: more efficient (Only 1 sex) Low genetic variation Sexual: prevalent (2 sexes, separate or not) High genetic variation Need 2 members of the same species
Written re-exam Bachelor in Medicine/MedIS. Exam date: Time: 09:00-11:00. Important information:
 Written re-exam 2016 Course title: Program: Semester: Reproductive endocrinology Bachelor in Medicine/MedIS 4 semester Exam date: 04-08-16 Time: 09:00-11:00 Evaluation form 7-point scale Important information:
Written re-exam 2016 Course title: Program: Semester: Reproductive endocrinology Bachelor in Medicine/MedIS 4 semester Exam date: 04-08-16 Time: 09:00-11:00 Evaluation form 7-point scale Important information:
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception
 PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
Martin Ritzén. bioscience explained Vol 7 No 2. Girl or boy: What guides gender development and how can this be a problem within
 Martin Ritzén Professor emeritus, Karolinska Institutet, Stockholm, Sweden Girl or boy: What guides gender development and how can this be a problem within sport? Introduction During the 2009 athletics
Martin Ritzén Professor emeritus, Karolinska Institutet, Stockholm, Sweden Girl or boy: What guides gender development and how can this be a problem within sport? Introduction During the 2009 athletics
Animal Science 434 Reproductive Physiology
 Animal Science 434 Reproductive Physiology Development of the Pituitary Gland Lec 5: Embryogenesis of the Pituitary and Sexual Development Stomodeum Brain Infundibulum Rathke s Pouch Germ Cell Migration
Animal Science 434 Reproductive Physiology Development of the Pituitary Gland Lec 5: Embryogenesis of the Pituitary and Sexual Development Stomodeum Brain Infundibulum Rathke s Pouch Germ Cell Migration
HORMONAL SEX REVERSAL IN A FEMALE
 HORMONAL SEX REVERSAL IN A FEMALE BY W. J. MATHESON and E. M. WARD From the Children's Hospital and Pathological Department, Leicester Royal Infirmary (RECEIVED FOR PUBLICATION SEPTEMBER 15, 1953) The
HORMONAL SEX REVERSAL IN A FEMALE BY W. J. MATHESON and E. M. WARD From the Children's Hospital and Pathological Department, Leicester Royal Infirmary (RECEIVED FOR PUBLICATION SEPTEMBER 15, 1953) The
Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True Hermaphrodite
 Clin Pediatr Endocrinol 1994; 3(2): 91-95 Copyright (C) 1994 by The Japanese Society for Pediatric Endocrinology Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True
Clin Pediatr Endocrinol 1994; 3(2): 91-95 Copyright (C) 1994 by The Japanese Society for Pediatric Endocrinology Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True
Yutaka; SAKAMOTO, Hiromi. Citation 泌尿器科紀要 (1986), 32(10):
 Title46XX male; report of case OKUYAMA, Akihiko; KONDO, Nobuyuki; Author(s) NAKAMURA, Masahiro; SONODA, Takao; Yutaka; SAKAMOTO, Hiromi Citation 泌尿器科紀要 (1986), 32(10): 1539-1542 Issue Date 1986-10 URL
Title46XX male; report of case OKUYAMA, Akihiko; KONDO, Nobuyuki; Author(s) NAKAMURA, Masahiro; SONODA, Takao; Yutaka; SAKAMOTO, Hiromi Citation 泌尿器科紀要 (1986), 32(10): 1539-1542 Issue Date 1986-10 URL
Grade 9 Science - Human Reproduction
 Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Intersex among Africans in Rhodesia
 Arch. Dis. Childh., 1966, 41, 102. Intersex among Africans in Rhodesia J. I. FORBES and B. HAMMAR From Harari Hospital, Salisbury, Southern Rhodesia According to a Greek myth, preserved for us in Ovid
Arch. Dis. Childh., 1966, 41, 102. Intersex among Africans in Rhodesia J. I. FORBES and B. HAMMAR From Harari Hospital, Salisbury, Southern Rhodesia According to a Greek myth, preserved for us in Ovid
Professor, Prasad Institute of Medical Sciences, Lucknow, India. ABSTRACT. Online Access and Article Informtaion
 Original Research Article Disorders of Sexual Differentiation: A study on the Incidence and Types of Female Pseudo Hermaphrodites J.Radhika * 1, C.Bhuvaneswari 2, Arudyuti Chowdhury 3. *1 Associate Professor,
Original Research Article Disorders of Sexual Differentiation: A study on the Incidence and Types of Female Pseudo Hermaphrodites J.Radhika * 1, C.Bhuvaneswari 2, Arudyuti Chowdhury 3. *1 Associate Professor,
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM
 Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
EMBRYOLOGIC BASIS OF FEMALE CONGENITAL TRACT MALFORMATIONS
 EMBRYOLOGIC BASIS OF FEMALE CONGENITAL TRACT MALFORMATIONS Prof. Pedro Acién, MD, FRCOG Maribel Acién, MD San Juan University Hospital/ Miguel Hernández University Campus of San Juan. Alicante. Spain Instituto
EMBRYOLOGIC BASIS OF FEMALE CONGENITAL TRACT MALFORMATIONS Prof. Pedro Acién, MD, FRCOG Maribel Acién, MD San Juan University Hospital/ Miguel Hernández University Campus of San Juan. Alicante. Spain Instituto
Male and Female Reproduction
 Male and Female Reproduction Similarities / Differences Develop very similar structures of sex glands Two genital tubes Manufacture the hormones of the other sex. Hormones of one sex are often used to
Male and Female Reproduction Similarities / Differences Develop very similar structures of sex glands Two genital tubes Manufacture the hormones of the other sex. Hormones of one sex are often used to
Intersex is a group of conditions where there is a discrepancy between the external genitals and the internal genitals (the testes and ovaries).
 Intersex to use the sharing features on this page, please enable JavaScript. Share on facebookshare on IwitterBookmark & SharePrintcr-lnendly version Intersex is a group of conditions where
Intersex to use the sharing features on this page, please enable JavaScript. Share on facebookshare on IwitterBookmark & SharePrintcr-lnendly version Intersex is a group of conditions where
Grand Rounds Mullerian Anomalies. Sara Schaenzer, PGY-3 9/26/18
 Grand Rounds Mullerian Anomalies Sara Schaenzer, PGY-3 9/26/18 Background Congenital uterine anomalies occur in 2-4% of women Three times more common in women with recurrent pregnancy loss True incidence
Grand Rounds Mullerian Anomalies Sara Schaenzer, PGY-3 9/26/18 Background Congenital uterine anomalies occur in 2-4% of women Three times more common in women with recurrent pregnancy loss True incidence
Unit B Understanding Animal Body Systems. Lesson 6 Anatomy and Physiology of Animal Reproduction Systems
 Unit B Understanding Animal Body Systems Lesson 6 Anatomy and Physiology of Animal Reproduction Systems 1 Terms Alimentary canal Bladder Cervix Clitoris Cloaca Copulation Cowper s gland Epididymis Fallopian
Unit B Understanding Animal Body Systems Lesson 6 Anatomy and Physiology of Animal Reproduction Systems 1 Terms Alimentary canal Bladder Cervix Clitoris Cloaca Copulation Cowper s gland Epididymis Fallopian
6.7 IN. Continuity through Reproduction. What are the differences between male and female gametes? Discuss their formation and physical attributes.
 6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
C. Patrick Shahan, MD University of Tennessee Health Science Center Department of Surgery
 C. Patrick Shahan, MD University of Tennessee Health Science Center Department of Surgery Drop use of hermaphrodite and derivatives 1 in 15,000 live births Congenital Adrenal Hyperplasia Mixed Gonadal
C. Patrick Shahan, MD University of Tennessee Health Science Center Department of Surgery Drop use of hermaphrodite and derivatives 1 in 15,000 live births Congenital Adrenal Hyperplasia Mixed Gonadal
Sexual Differentiation Fall 2008 Bios 90
 Sexual Differentiation Fall 2008 Bios 90 Jennifer Swann, Professor Dept Biol Sci, Lehigh University Asexual reproduction Budding : offspring develop as a growth on the body of the parent jellyfishes, echinoderms,
Sexual Differentiation Fall 2008 Bios 90 Jennifer Swann, Professor Dept Biol Sci, Lehigh University Asexual reproduction Budding : offspring develop as a growth on the body of the parent jellyfishes, echinoderms,
Reproductive System. Where it all begins
 Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
ISSN CHROMOSOME STUDY IN SUSPECTED CASES OF TURNER S SYNDROME FROM JAMMU REGION OF JAMMU & KASHMIR
 J. Adv. Zool. 2018: 39(1): 32-36 ISSN-0253-7214 CHROMOSOME STUDY IN SUSPECTED CASES OF TURNER S SYNDROME FROM JAMMU REGION OF JAMMU & KASHMIR Wahied Khawar Balwan and Neelam Saba *Department of Zoology,
J. Adv. Zool. 2018: 39(1): 32-36 ISSN-0253-7214 CHROMOSOME STUDY IN SUSPECTED CASES OF TURNER S SYNDROME FROM JAMMU REGION OF JAMMU & KASHMIR Wahied Khawar Balwan and Neelam Saba *Department of Zoology,
The Genital Anomaly Associated with Prenatal Exposure to Progestogens
 The Genital Anomaly Associated with Prenatal Exposure to Progestogens Howard W. Jones, Jr., M.D., and Lawson Wilkins, M.D. THE GREAT MAJORITY of individuals with positive (female) sex chromatin and masculinized
The Genital Anomaly Associated with Prenatal Exposure to Progestogens Howard W. Jones, Jr., M.D., and Lawson Wilkins, M.D. THE GREAT MAJORITY of individuals with positive (female) sex chromatin and masculinized
Embryology of the Female Reproductive Tract
 Embryology of the Female Reproductive Tract Andrew Healey Contents 1 Introduction... 21 2 Embryology of the Female Genitourinary Tract... 22 2.1 Development of the Gonads... 22 2.2 Relationship Between
Embryology of the Female Reproductive Tract Andrew Healey Contents 1 Introduction... 21 2 Embryology of the Female Genitourinary Tract... 22 2.1 Development of the Gonads... 22 2.2 Relationship Between
Growth pattern of the sex ducts in foetal mouse hermaphrodites
 /. Embryol. exp. Morph. 73, 59-68, 1983 59 Printed in Great Britain The Company of Biologists Limited 1983 Growth pattern of the sex ducts in foetal mouse hermaphrodites By C. YDING ANDERSEN 1, A. G. BYSKOV
/. Embryol. exp. Morph. 73, 59-68, 1983 59 Printed in Great Britain The Company of Biologists Limited 1983 Growth pattern of the sex ducts in foetal mouse hermaphrodites By C. YDING ANDERSEN 1, A. G. BYSKOV
LYMPHANGIOGRAPHY AND CHROMOSOME STUDIES IN FEMALES WITH LYMPHOEDEMA AND POSSIBLE OVARIAN DYSGENESIS
 Arch. Dis. Childh., 1965, 40, 27. LYMPHANGIOGRAPHY AND CHROMOSOME STUDIES IN FEMALES WITH LYMPHOEDEMA AND POSSIBLE OVARIAN DYSGENESIS BY P. F. BENSON, M. H. GOUGH, and P. E. POLANI From the Paediatric
Arch. Dis. Childh., 1965, 40, 27. LYMPHANGIOGRAPHY AND CHROMOSOME STUDIES IN FEMALES WITH LYMPHOEDEMA AND POSSIBLE OVARIAN DYSGENESIS BY P. F. BENSON, M. H. GOUGH, and P. E. POLANI From the Paediatric
Defining Sex and Gender & The Biology of Sex
 Defining Sex and Gender & The Biology of Sex Today: -Defining Sex and Gender -Conception of a Child -Chromosomes -Defects in Chromosomes Often we hear the terms sex and gender used in our society interchangeably,
Defining Sex and Gender & The Biology of Sex Today: -Defining Sex and Gender -Conception of a Child -Chromosomes -Defects in Chromosomes Often we hear the terms sex and gender used in our society interchangeably,
Case Report Role of Imaging in the Diagnosis and Management of Complete Androgen Insensitivity Syndrome in Adults
 Hindawi Publishing Corporation Case Reports in Radiology Volume 2013, Article ID 158484, 6 pages http://dx.doi.org/10.1155/2013/158484 Case Report Role of Imaging in the Diagnosis and Management of Complete
Hindawi Publishing Corporation Case Reports in Radiology Volume 2013, Article ID 158484, 6 pages http://dx.doi.org/10.1155/2013/158484 Case Report Role of Imaging in the Diagnosis and Management of Complete
Urogenital system - Development. Aleš Hampl
 Urogenital system - Development Aleš Hampl cloaca Urogenital system Overall picture Urogenital system Reminder Urogenital system Intermediate mesoderm Urogenital system Early forms of kidneys - Pronephros
Urogenital system - Development Aleš Hampl cloaca Urogenital system Overall picture Urogenital system Reminder Urogenital system Intermediate mesoderm Urogenital system Early forms of kidneys - Pronephros
