The ability of the kidneys to regulate extracellular fluid volume by altering sodium
|
|
|
- Eunice Peters
- 5 years ago
- Views:
Transcription
1 REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi The ability of the kidneys to regulate extracellular fluid volume by altering sodium excretion is important for maintaining adequate volume within the vascular system. Sodium excretion is controlled by integrating physical, neural, and hormonal regulatory systems. The major systems involved in retaining sodium include the renin-angiotensin-aldosterone and sympathetic systems, whereas natriuretic factors such as atrial natriuretic peptide and nitric oxide are important in promoting sodium excretion. In response to increased sodium intake, the sodium-retaining systems are inhibited and natriuretic hormones are activated. Pressures and flows within the microcirculation of the kidney, in concert with neural and hormonal systems, interact to regulate sodium excretion. The quantitative importance of each of these systems in regulating sodium balance is variable and is determined by the physiological or pathiophysiological condition. AM. J. PHYSIOL. 275 (ADV. PHYSIOL. EDUC. 20): S157 S168, EXTRACELLULAR FLUID VOLUME IS DETERMINED BY BALANCE BETWEEN SODIUM INTAKE AND RENAL EXCRETION OF SODIUM The ability of the kidneys to regulate extracellular fluid volume by altering sodium excretion is important for maintaining adequate volume within the vascular system. This ensures that appropriate tissue perfusion occurs under various physiological conditions. Provided that the antidiuretic and thirst systems are functional, changes in the balance between sodium intake and sodium output determined the total quantity of sodium in the body and the volume of the extracellular compartment (11, 12). For example, when sodium intake exceeds sodium output by the kidneys, total body sodium (not Na concentration) and extracellular fluid volume increases. Conversely, when renal excretion of sodium exceeds sodium intake, total body sodium and extracellular fluid volume decrease. Thus the maintenance of a constant extracellular fluid volume depends on the body s ability to regulate the amount of NaCl in the compartment. The body achieves this important regulatory function by varying sodium excretion to match the level of sodium intake. CHANGES IN SODIUM BALANCE ARE SENSED BY VOLUME-DEPENDENT RECEPTORS To maintain a constant extracellular fluid volume, the body monitors the volume of this compartment by sensors or receptors in different regions of the body (11, 12). In response to the sensory output, effector mechanisms are activated to make appropriate adjustments in the renal output of sodium. The portion of the extracellular fluid compartment that is sensed by these receptors is plasma volume. Plasma volume determines the magnitude of various hemodynamic variables that are sensed by volume and/or pressure receptors. For example, changes in plasma volume can cause changes in the distending pressures in certain regions of the cardiovascular system. Volume / 98 $5.00 COPYRIGHT 1998 THE AMERICAN PHYSIOLOGICAL SOCIETY S157
2 receptors are located in the low- and high-pressure portions of the cardiovascular system. The low-pressure receptors are found in the pulmonary vasculature and in the atria. An increase in atrial pressure in response to an increase in plasma volume activates two effector mechanisms that enhance sodium excretion (10, 11, 12). An increase in atrial pressure decreases renal sympathetic nerve activity via a neural reflex mechanism and increases the release of atrial natriuretic peptide (ANP) from atrial myocytes (3, 4). Conversely, a decrease in plasma volume reduces atrial pressure, which leads to enhanced renal sympathetic nerve activity and decreased ANP secretion. Under certain conditions, an increase in plasma volume leads to increases in arterial pressure. Changes in arterial pressure are sensed by high-pressure receptors located in the aortic arch and the carotid sinus (3). Increases in arterial pressure result in baroreceptormediated reductions in renal sympathetic nerve activity, whereas a decrease in arterial pressure leads to enhanced renal sympathetic nerve activity and sodium retention. Changes in plasma volume can also be sensed by two different types of intrarenal volume-dependent receptors (10, 11, 12). Changes in arterial pressure are sensed by pressure receptors located in the afferent arterioles. Decreases in arterial pressure at the level of the afferent arteriole lead to renin secretion and enhanced formation of angiotensin II (ANG II), which is a sodium-retaining hormone. Changes in plasma volume can also lead to alterations in NaCl delivery to macula densa cells, which in turn alters renin secretion. Increases in plasma volume lead to an increase in sodium delivery [via a decrease in proximal tubule reabsorption and/or increase in glomerular filtration rate (GFR)] to macula densa cells, which in turn suppresses renin release. Conversely, a decrease in plasma volume leads to a decrease in sodium delivery to macula densa cells and enhanced renin secretion and angiotensin formation. Thus changes in extracellular fluid volume are detected by various sensors in the body, which activate effector mechanisms that adjust sodium excretion appropriately to return extracellular fluid volume to normal levels. The effector mechanisms involved in adjusting sodium excretion involve neural and hormonal factors. These factors alter the rate of sodium excretion by influencing the main determinants of sodium excretion, GFR, and tubule sodium reabsorption. The quantity of sodium excreted is determined by the difference between the filtered load of sodium and the amount of sodium reabsorbed along the nephron. Thus an increase in sodium excretion can occur via an increase in glomerular filtration or a decrease in sodium reabsorption. Conversely, a decrease in sodium excretion can occur via a decrease in glomerular filtration or an increase in sodium reabsorption. The remaining part of this brief review will focus on how specific neurohormonal effector mechanisms regulate sodium excretion via alterations in glomerular filtration and tubular sodium reabsorption. CHANGES IN PERITUBULAR CAPILLARY PHYSICAL FACTORS INFLUENCE SODIUM REABSORPTION BY ALTERING INTERSTITIAL HYDROSTATIC PRESSURE An imbalance between hydrostatic and colloid osmotic forces governs the rate of reabsorption across the peritubular capillaries, just as these physical forces control filtration in the glomerular capillaries (11, 12). Thus changes in renal hemodynamics and colloid osmotic pressure can alter peritubular capillary fluid and solute reabsorption, interstitial fluid hydrostatic and colloid osmotic pressure, and, ultimately, reabsorption from the renal tubules. Likewise, primary changes in tubular reabsorption also influence the hydrostatic and colloid osmotic forces of the interstitial compartment and, ultimately, peritubular capillary reabsorption. Thus the hydrostatic and colloid osmotic forces of the renal interstitium provide an important link between circulatory function and renal tubular reabsorption (7). Interstitial fluid volume (and, therefore, interstitial fluid hydrostatic pressure) is determined by the difference between the rate of volume inflow to the interstitium due to tubular reabsorption and outflow due to peritubular capillary reabsorption. In the steady state, peritubular capillary reabsorption must equal renal tubular reabsorption. Thus, from anatomic considerations alone, it is clear that physical forces in the peritubular capillaries and renal interstitium influence renal tubular reabsorption. S158
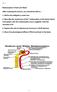
3 Expansion of the extracellular fluid volume compartment results in an increases in peritubular capillary hydrostatic pressure (due to renal vasodilation and/or increases in arterial pressure) and a decrease in colloid osmotic pressure (due to a decrease in filtration fraction). These changes result in a reduced rate of sodium and water reabsorption in the proximal tubules (7, 11, 12). Conversely, when extracellular fluid volume is contracted, decreases in peritubular capillary hydrostatic pressure and increases in colloid osmotic pressure enhance the rate of sodium reabsorption in the proximal tubule. Changes in peritubular capillary physical forces are thought to influence sodium reabsorption by changes in renal interstitial volume or hydrostatic pressure (see Fig. 1). Numerous physiological perturbations that increase sodium excretion such as increases in renal perfusion pressure or extracellular fluid volume expansion are associated with significant elevations in renal interstitial hydrostatic pressure (RIHP) (6, 7). Furthermore, renal vasodilators that cause natriuresis also increase RIHP (7). In contrast, renal vasodilators, such as secretin, that do not increase sodium excretion also do not increase RIHP (7). Finally, when RIHP is FIG. 1. Mechanism whereby renal interstitial hydrostatic pressure reduces sodium reabsorption in response to extracellular fluid volume expansion. S159
4 prevented from increasing during renal vasodilatation or acute saline volume expansion, natriuresis is markedly attenuated or even abolished (7). Thus RIHP appears to link changes in peritubular capillary hemodynamics to sodium reabsorption. Although the exact mechanism whereby RIHP influences the reabsorption of sodium and water is unclear, it is thought that RIHP decreases sodium absorption in the proximal tubule by inhibiting passive sodium and water transport (7). One hypothesis is that increased renal interstitial volume and/or pressure raises the permeability of the tight junctional complexes of the proximal tubule. This effect would, in turn, increase the back leak of sodium from the interstitium into the tubule lumen. The net effect would be a reduction of sodium and water reabsorption across the proximal tubule. Conversely, a decrease in RIHP would reduce back leak of sodium from the interstitium and enhance proximal tubule sodium reabsorption. CHANGES IN MEDULLARY BLOOD FLOW INFLUENCE SODIUM REABSORPTION IN LOOP OF HENLE In addition to the influence of the cortical peritubular microcirculation on sodium reabsorption, it has been shown that alterations in medullary hemodynamics affect passive sodium transport in the loop of Henle (10, 11, 15). An increase in medullary blood flow leads to a washout of medullary interstitial hypertonicity (see Fig. 2). Consequently, water abstraction out of the thin descending limb of Henle s loop, which is relatively impermeable to sodium, is reduced. Thus an increased volume of fluid with the same quantity of sodium but decreased sodium concentration is delivered to the water-impermeable thin ascending limb of Henle s loop. The reduced sodium concentration decreases sodium reabsorption in that nephron segment, and more sodium is delivered to the distal tubules and eventually excreted. In contrast, reductions in medullary blood flow would decrease sodium excretion by increasing medullary interstitial tonicity, water abstraction out of the thin descending loop of Henle, and sodium concentration in the thin ascending limb of Henle s loop. The FIG. 2. Mechanism whereby increases in medullary blood flow decreases sodium reabsorption and enhances sodium excretion. TDLH, thin descending limb of loop of Henle; JM, juxtamedullary; TALH, thick ascending limb of loop of Henle. increased sodium concentration would increase passive sodium reabsorption in this nephron segment. A variety of neurohumoral factors, such as angiotensin, norepinephrine, and ANP, and local autocoid factors, such as prostaglandins and nitric oxide (NO), influence medullary blood flow (15). Thus the effects S160
5 of these factors on sodium excretion could, in part, be due to alterations in medullary hemodynamics. CHANGES IN RENAL ARTERY PRESSURE INFLUENCE SODIUM REABSORPTION VIA ALTERATIONS IN INTRARENAL HEMODYNAMICS Increases in renal perfusion pressure enhance sodium excretion, a phenomenon commonly referred to as renal pressure natriuresis (2, 6, 8). Changes in sodium excretion in response to changes in renal perfusion pressure are thought to be due to alterations in tubular reabsorption of sodium, because GFR and the filtered load of sodium are usually well autoregulated. Although renal pressure natriuresis plays a critical role in the long-term regulation of extracellular fluid volume and arterial pressure, the mechanisms whereby changes in renal perfusion pressure influence sodium excretion and, specifically, sodium reabsorption, have not been fully elucidated (2, 8, 10). Research investigations during recent years, however, have provided new insights into possible mechanisms of pressure natriuresis and have suggested that physical factors, especially renal interstitial pressure, may be primary mediators of pressure natriuresis (7). Because pressure natriuresis can occur in the absence of discernible changes in renal blood flow and peritubular capillary hydrostatic and oncotic pressures, the mechanisms responsible for sustained increased RIHP have been unclear. Recent studies, however, have provided evidence that renal medullary hemodynamics are closely linked to changes in RIHP (7). Increases in renal perfusion pressure raise vasa recta flow and hydrostatic pressure, possibly reducing fluid uptake across the vasa recta capillary wall and increasing medullary interstitial volume and medullary interstitial hydrostatic pressure (see Fig. 3). The increase in medullary interstitial hydrostatic pressure is then thought to be transmitted throughout the kidney, including the cortex (15). Why papillary plasma flow increases when renal perfusion pressure is elevated and cortical blood flow is effectively autoregulated is unknown. It is possible that endothelial (NO) or interstitial factors (ANG II, prostaglandins, kinins) are released into the medulla with increased renal perfusion pressure (7, 15). Once released, these intrarenal factors could then alter medullary hemodynamics and override intrinsic autoregulatory mechanisms in the inner medulla. Some investigators have argued against a role for RIHP in mediating pressure natriuresis, because renal blood flow and/or peritubular capillary hydrostatic pressure is usually autoregulated in response to changes in renal perfusion pressure (7). Direct measurement of RIHP, however, indicates that increased RIHP may occur despite efficient autoregulation of whole kidney renal blood flow and peritubular capillary hydrostatic pressure (7). Moreover, preventing RIHP from increasing in response to increased renal perfusion pressure markedly attenuates pressure natriuresis (7). Direct increases in RIHP, comparable to those measured in response to increased renal perfusion pressure, also significantly decrease proximal tubular sodium reabsorption and increase sodium excretion. FIG. 3. Mechanisms whereby increases in renal perfusion pressure enhances sodium excretion. PT, proximal tubule. S161
6 ACTIVATION OF RENAL SYMPATHETIC NERVOUS SYSTEM REDUCES SODIUM EXCRETION BY DECREASING GFR AND ENHANCING SODIUM REABSORPTION Because the kidneys receive extensive sympathetic innervation, alterations in renal nerve traffic are believed to play an important role in the regulation of sodium excretion and extracellular fluid volume (3, 10, 11, 12). The renal sympathetic nervous system is activated via peripheral and central reflex mechanisms. In response to acute reductions in extracellular fluid volume, for example, intrathoracic volume/ pressure receptors are thought to initiate a neural reflex that, in turn, enhances renal sympathetic nerve activity and reduces sodium excretion. Conversely, increases in central volume lead to a reduction in renal nerve traffic and natriuresis. Direct renal nerve stimulation reduces sodium excretion, whereas acute renal denervation enhances pressure natriuresis (3). Increases in renal sympathetic nerve activity could reduce sodium excretion by increasing tubular reabsorption or decreasing the filtered load of sodium (see Fig. 4). Renal nerves are known to act directly on the tubule to increase sodium reabsorption via an -adrenergic receptor. In addition, increases in renal sympathetic nerve activity influence tubule reabsorption by activating the renin FIG. 4. Mechanism whereby activation of sympathetic nervous system reduces sodium excretion in response to extracellular fluid volume contraction. S162
7 angiotensin system. Marked increases in renal sympathetic nerve activity may also raise renal vascular resistance and decrease GFR, medullary blood flow, and renal interstitial pressure, changes that could all contribute to the sodium-retaining effects of renal nerve activation. Most of the experimental evidence suggests that this system plays a role in regulating sodium excretion under conditions associated with marked sodium retention, such as in congestive heart failure, cirrhosis, and a low-sodium diet (3, 10, 11, 12). There is also evidence to suggest that excessive activation of the sympathetic nervous system may play a role in the pathogenesis of certain forms of hypertension such as in obesity-related hypertension. ALDOSTERONE ENHANCES SODIUM REABSORPTION IN CORTICAL COLLECTING DUCT Aldosterone is a potent sodium-retaining hormone that is synthesized in the zona glomerulosa of the adrenal cortex. Although several factors (plasma K and Na, ACTH, and ANP) influence its secretion, ANG II is the most important in controlling aldosterone secretion in response to changes in extracellular fluid volume. Increases in plasma ANG II enhance aldosterone secretion, whereas reduced plasma ANG II decreases aldosterone secretion. There is also a strong inverse relationship between sodium intake and plasma aldosterone concentration. A low-sodium diet is associated with high levels of plasma aldosterone. Conversely, plasma aldosterone concentration approaches zero in individuals with a high sodium intake. Aldosterone decreases sodium excretion by enhancing renal sodium reabsorption. Aldosterone increases sodium reabsorption in principal cells of the collecting duct by increasing the sodium permeability of the luminal membrane and by stimulating Na -K -ATPase activity. Aldosterone permeates the cell membrane of the principal cells and binds to a cytosolic receptor (11). The aldosterone/receptor complex is translocated into the nucleus, where it activates the transcription of specific mrna. The newly formed proteins called aldosterone-induced proteins are involved in mediating the increase in sodium permeability of the luminal membrane and Na -K -ATPase activity. Spironolactone, an aldosterone receptor antagonist, is used clinically to promote sodium loss in sodium retaining states such as congestive heart failure, cirrhosis, and hyperaldosteronism. ANG II ENHANCES SODIUM REABSORPTION VIA A DIRECT EFFECT ON TUBULE TRANSPORT AND BY INDIRECT HEMODYNAMIC MECHANISMS The renin-angiotensin system is the most thoroughly studied, and perhaps most important, system primarily responsible for the regulation of sodium excretion (9). During extracellular fluid volume contraction, renin is released from the kidneys. Renin acts on a substrate to release ANG I, which is rapidly converted to ANG II by a converting enzyme located in the pulmonary circulation and in the kidney itself. For many years ANG II was thought to affect sodium excretion solely through the release of aldosterone, which acts on the cortical tubules to enhance sodium reabsorption (9). However, more recent studies have provided evidence that ANG II can stimulate sodium reabsorption through a direct action on ANG II receptors located on the renal tubules and by reducing medullary blood flow and renal interstitial hydrostatic pressure (see Fig. 5). The importance of the renin-angiotensin-aldosterone system in regulating sodium excretion has been elucidated with the use of a specific receptor antagonist to ANG II and converting-enzyme inhibitors that block the formation of ANG II (9). ANG II appears to play a role in controlling sodium excretion over a wide range of physiological and pathophysiological conditions. For example, suppression of renin release and reduced ANG II formation in response to increases in dietary sodium intake has been shown to play a critical role in allowing the body to maintain sodium balance without increasing arterial pressure (9). ANG II also has powerful vasoconstrictor effects, which, in combination with the sodium-retaining actions of ANG II, play a crucial role in regulating extracellular fluid volume and arterial pressure. Receptor antagonists to ANG II and converting-enzyme inhibitors are widely used in clinical situations that are associated with abnormalities in volume regulation such as in hypertension and congestive heart failure. S163
8 FIG. 5. Mechanism whereby activation of renin-angiotensin system reduces sodium excretion in response to extracellular fluid volume contraction. IN RESPONSE TO ATRIAL DISTENTION, THE HEART RELEASES A HORMONE THAT ENHANCES SODIUM EXCRETION ANP is a 28-amino acid peptide hormone that is synthesized by atrial myocytes and secreted in response to increased atrial distention. Conversely, ANP secretion is reduced in response to reductions in atrial pressure (1, 3, 5). Figure 6 shows pathways whereby ANP is released and then acts through direct and indirect mechanisms to enhance sodium excretion. ANP increases sodium excretion by increasing GFR and reducing sodium reabsorption; however, an increase in GFR is not essential for the natriuresis. Inhibition of sodium reabsorption occurs through direct and indirect effects on the renal tubules. ANP directly inhibits S164
9 FIG. 6. Mechanism whereby atrial natriuretic peptide enhances sodium excretion in response to extracellular fluid volume expansion. sodium reabsorption in the collecting duct via a cgmp-mediated reduction in sodium permeability. ANP decreases sodium reabsorption indirectly by increasing medullary blood flow and inhibiting the formation of ANG II and aldosterone. The quantitative importance of ANP in controlling sodium excretion is uncertain due to the lack of effort via experimental tools to block the synthesis or effector site of ANP. Increases in dietary sodium intake result in relatively small increases in plasma ANP concentration. Thus its importance in regulation sodium balance in response to increments in sodium intake is unclear. ANP is thought to play an important role in controlling sodium excretion under conditions of severe volume overload such as congestive heart failure. Under these conditions ANP is believed to play a role in protecting the body from severe volume retention and edema formation. NITRIC OXIDE IS SYNTHESIZED BY RENAL ENDOTHELIAL AND TUBULE CELLS AND PROMOTES SODIUM EXCRETION NO is synthesized from the amino acid L-arginine in endothelial as well as other renal tubule cells by the action of NO synthase (13, 14). The characterization and cloning of constitutive and inducible NO-synthesizing enzymes and the development of specific inhibitors of the L-arginine-NO pathway have provided powerful tools to examine the role of NO in the regulation of renal hemodynamics and sodium excretion (13, 14, 16). NO is believed to enhance sodium excretion by increasing glomerular filtration and by S165
10 FIG. 7. Mechanism whereby nitric oxide increases sodium excretion in response to extracellular fluid volume expansion. GFR, glomerular filtration rate. inhibiting tubular sodium reabsorption (see Fig. 7). NO directly inhibits sodium transport in the collecting duct (13, 16). In addition, NO decreases tubular reabsorption by enhancing medullary blood flow ad increasing renal interstitial hydrostatic pressure (13, 16). NO may also decrease tubular odium reabsorption by antagonizing the renal tubular actions of ANG II studies (13, 16). Recent studies indicate that NO may be important in the regulation of sodium excretion (13, 16). All three isoforms of NO synthase are found in the kidney, and there is evidence to suggest that NO synthesis increases in response to increases in sodium intake and other stimuli that increase sodium excretion such as increases in renal perfusion pressure. The mechanism whereby increases in extracellular fluid volume increase NO production, however, has yet been fully elucidated. Blockade of endogenous NO formation reduces sodium excretion. In addition, chronic blockade of NO synthesis results in a saltsensitive form of hypertension. Thus it appears that NO is involved in the normal regulation of extracellular fluid volume and arterial pressure. SODIUM EXCRETION RESPONSE TO ELEVATIONS IN SODIUM INTAKE INVOLVES INTEGRATION OF NEURAL, HORMONAL, AND PHYSICAL FACTORS The integration of control systems regulating sodium excretion under normal conditions can be summarized by examining the homeostatic response to progressive increases in dietary sodium intake (see Fig. 8). The primary purpose of the homeostatic response is to enhance sodium excretion and maintain a balance between sodium intake and renal sodium output. As sodium intake is increased, sodium output initially lags behind intake. This time delay in sodium excretion results in a positive cumulative sodium balance and an increase, albeit small, in extracellular S166
11 FIG. 8. Integrated response to increases in dietary sodium intake. ANF, atrial natriuretic factor. fluid volume. It is this small increase in extracellular fluid volume that triggers various volume and/or low-pressure receptors in the body to increase sodium excretion. Activating these receptors suppresses sodium-retaining systems and activates sodium-losing systems. Under normal conditions, progressive increases in sodium intake reduce renin release, ANG II formation, and aldosterone secretion. The elevation in extracellular fluid volume may also lead to a reduction in renal sympathetic nerve activity. In contrast to the sodium-retaining systems, natriuretic systems, such as the ANP and NO systems, are likely to be activated during progressive increases in dietary sodium intake. The combined activation of natriuretic systems and suppression of sodium-retaining systems leads to an increase in sodium excretion, partly through reductions in sodium reabsorption and increases in glomerular filtration. These systems act on the kidneys to decrease sodium reabsorption directly by inhibiting sodium transport and indirectly by increasing RIHP and medullary blood flow. Maintaining sodium balance during chronic increases in sodium intake normally occurs without marked increases in renal perfusion pressure. Thus the neural and hormonal systems are sufficiently effective under normal conditions to maintain sodium balance without marked increases in S167
12 renal perfusion pressure. Thus the neural and hormonal systems are sufficiently effective under normal conditions to maintain sodium balance without excessive volume retention and hypertension. However, when a derangement in an important regulatory system occurs, activation of other natriuretic mechanisms, such as a rise in arterial pressure, becomes an important compensatory mechanism for maintaining sodium balance. The importance of pressure/natriuresis can be illustrated in the homeostatic response to increased sodium intake when ANG II production is unable to be suppressed. Because ANG II is unable to respond to further increments in sodium intake, more sodium is retained, causing increases in extracellular fluid volume and arterial pressure that help to restore sodium balance. Another possible factor for maintaining sodium balance may be the release of natriuretic factors, such as atrial natriuretic factor (ANF). Circulatory levels of this natriuretic substance are elevated under these conditions; however, its quantitative importance in achieving sodium balance has not been determined. Thus sodium excretion is controlled by integrating physical, neural, and hormonal regulatory systems. The major systems involved in retaining sodium include the renin-angiotensin-aldosterone and sympathetic systems, whereas natriuretic factors such as ANP and NO are important in promoting sodium excretion. In response to increased sodium intake, the sodium-retaining systems are inhibited and natriuretic hormones are activated. Pressures and flows within the microcirculation of the kidney, in concert with neural and hormonal systems, interact to regulate sodium excretion. The quantitative importance of each of these systems in regulating sodium balance is variable and is determined by the physiological or pathophysiological condition. This work is supported in part by National Heart, Lung, and Blood Intitute Grants HL-3499 and HL Address for reprint requests: J. P. Granger, Dept. of Physiology and Biophysics, Univ. of Mississippi Medical Center, 2500 N. State St., Jackson, MS References 1. Burnett, J. C., Jr., J. P. Granger, and T. J. Opgenorth. Effects of synthetic atrial natriuretic factor on renal function and renin release. Am. J. Physiol. 247 (Renal Fluid Electrolyte Physiol. 16): F863 F866, Cowley, A. W., Jr. Long-term control of arterial blood pressure. Physiol. Rev. 72: , DiBona, G. F. The functions of the renal nerves. Rev. Physiol. Biochem. Pharmacol. 94: , Genest, J., and M. Cantin. Regulation of body fluid volume: the atrial natriuretic factor. News Physiol. Sci. 1: 3 5, Granger, J. P. Inhibitors of ANF metabolism: potential therapeutic agents in cardiovascular disease. Circulation 82: , Granger, J. P. Pressure-natriuresis: role of renal interstitial hydrostatic pressure. Hypertension 19: I9 I17, Granger, J. P. Role of renal interstitial hydrostatic pressure in the regulation of sodium excretion. Federation Proc. 45: , Guyton, A. C., T. G. Coleman, A. W. Cowley, Jr., K. W. Scheel, R. D. Manning, and R. A. Norman. Arterial pressure regulation: overriding dominance of the kidneys in long-term regulation and in hypertension. Am. J. Med. 52: , Hall, J. E. Control of sodium excretion by angiotensin II: intrarenal mechanisms and blood pressure regulation. Am. J. Physiol. 250 (Regulatory Integrative Comp. Physiol. 19): R960 R972, Hall, J. E., and J. P. Granger. Role of sodium and fluid excretion in hypertension. In: Textbook of Hypertension, edited by J. D. Swales. Oxford, UK: Blackwell Scientific, 1994, p Knox, F. G., and J. P. Granger. Control of sodium excretion: an integrative approach. In: Handbook of Renal Physiology, edited by E. Windhager. New York: Oxford Univ. Press, 1992, p Knox, F. G., and J. P. Granger. Control of sodium excretion: the kidney produces under pressure. News Physiol. Sci. 2: 26 29, Kone, B. C., and C. Baylis. Biosynthesis and homeostatic roles of nitric oxide in the normal kidney. Am. J. Physiol. 272 (Renal Physiol. 41): F561 F578, Moncada, S., R. M. J. Palmer, and E. A. Higgs. Nitric oxide: physiology, pathophysiology and pharmacology. Pharmacol. Rev. 43: , Roman, R. J., and A.-P. Zou. Influence of the renal medullary circulation on the control of sodium excretion. Am. J. Physiol. 265 (Regulatory Integrative Comp. Physiol. 14): R963 R973, Schnackenberg, C. G., K. Kirchner, A. Patel, and J. P. Granger. Nitric oxide, the kidney, and hypertension. Clin. Exp. Pharmacol. Physiol. 24: , S168
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Counter-Current System Regulation of Renal Functions
 Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
MAJOR FUNCTIONS OF THE KIDNEY
 MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM
 RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY
 RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
Functions of the kidney
 Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Chapter 23. The Nephron. (functional unit of the kidney
 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D.
 Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
8. URINE CONCENTRATION
 8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
RENAL PHYSIOLOGY. Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM
 RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte,
RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte,
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
RENAL PHYSIOLOGY. Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM
 RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte, H
RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte, H
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19
![QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19](/thumbs/80/80449526.jpg) 1 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion, excretion
1 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion, excretion
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
Physiology (4) 2/4/2018. Wael abu-anzeh
 Physiology (4) 2/4/2018 Wael abu-anzeh In the previous lectures we have discussed the filtration and the reabsorption processes but in this lecture we will talk about the factor that will regulate or control
Physiology (4) 2/4/2018 Wael abu-anzeh In the previous lectures we have discussed the filtration and the reabsorption processes but in this lecture we will talk about the factor that will regulate or control
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
Physiology (6) 2/4/2018. Rahmeh Alsukkar
 Physiology (6) 2/4/2018 Rahmeh Alsukkar **unfortunately the sheet does not involve the slides. ** the doctor repeat a lot of things from the previous lecture so this sheet will begin from slide 139 to
Physiology (6) 2/4/2018 Rahmeh Alsukkar **unfortunately the sheet does not involve the slides. ** the doctor repeat a lot of things from the previous lecture so this sheet will begin from slide 139 to
Na + Transport 1 and 2 Linda Costanzo, Ph.D.
 Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Faculty version with model answers
 Faculty version with model answers Urinary Dilution & Concentration Bruce M. Koeppen, M.D., Ph.D. University of Connecticut Health Center 1. Increased urine output (polyuria) can result in a number of
Faculty version with model answers Urinary Dilution & Concentration Bruce M. Koeppen, M.D., Ph.D. University of Connecticut Health Center 1. Increased urine output (polyuria) can result in a number of
Identify and describe. mechanism involved in Glucose reabsorption
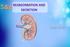 Define tubular reabsorption, tubular secretion, transcellular and paracellular transport. Identify and describe mechanism involved in Glucose reabsorption Describe tubular secretion with PAH transport
Define tubular reabsorption, tubular secretion, transcellular and paracellular transport. Identify and describe mechanism involved in Glucose reabsorption Describe tubular secretion with PAH transport
CASE 13. What neural and humoral pathways regulate arterial pressure? What are two effects of angiotensin II?
 CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Diagram of the inner portions of the kidney
 Excretory and Endocrine functions of the kidney The kidneys are the main excretory organs which eliminate in the urine, most metabolites primarily those containing nitrogen such as ammonia, urea and creatinine.
Excretory and Endocrine functions of the kidney The kidneys are the main excretory organs which eliminate in the urine, most metabolites primarily those containing nitrogen such as ammonia, urea and creatinine.
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018 Intercalated cells Intercalated cells secrete either H + (Typ A) or HCO 3- (Typ B). In intercalated cells Typ A can be observed
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018 Intercalated cells Intercalated cells secrete either H + (Typ A) or HCO 3- (Typ B). In intercalated cells Typ A can be observed
Kidney Structure. Renal Lobe = renal pyramid & overlying cortex. Renal Lobule = medullary ray & surrounding cortical labryinth.
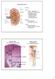 Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Chapter 17: Urinary System
 Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
I. Metabolic Wastes Metabolic Waste:
 I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
BLOCK REVIEW Renal Physiology. May 9, 2011 Koeppen & Stanton. EXAM May 12, Tubular Epithelium
 BLOCK REVIEW Renal Physiology Lisa M. HarrisonBernard, Ph.D. May 9, 2011 Koeppen & Stanton EXAM May 12, 2011 Tubular Epithelium Reabsorption Secretion 1 1. 20, 40, 60 rule for body fluid volumes 2. ECF
BLOCK REVIEW Renal Physiology Lisa M. HarrisonBernard, Ph.D. May 9, 2011 Koeppen & Stanton EXAM May 12, 2011 Tubular Epithelium Reabsorption Secretion 1 1. 20, 40, 60 rule for body fluid volumes 2. ECF
Class XI Chapter 19 Excretory Products and their Elimination Biology
 Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
Waste Products & Kidney Function
 Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
Chapter 24: The Urinary System
 Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
URINE CONCENTRATION AND REGULATION OF ECF OSMOLARITY
 URINE CONCENTRATION AND REGULATION OF ECF OSMOLARITY Dilute and concentrated urine 1-Dilute urine : Nephron function continuous reabsorption. Solutes while failing to reabsorbe water in distal tubule and
URINE CONCENTRATION AND REGULATION OF ECF OSMOLARITY Dilute and concentrated urine 1-Dilute urine : Nephron function continuous reabsorption. Solutes while failing to reabsorbe water in distal tubule and
Renal Physiology - Lectures
 Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
Fluid and electrolyte balance, imbalance
 Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Other Factors Affecting GFR. Chapter 25. After Filtration. Reabsorption and Secretion. 5 Functions of the PCT
 Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
19. RENAL PHYSIOLOGY ROLE OF THE URINARY SYSTEM THE URINARY SYSTEM. Components and function. V BS 122 Physiology II 151 Class of 2011
 19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
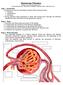 Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19
![QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19](/thumbs/77/74887026.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
Basic Functions of the Kidneys
 Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Kidneys in regulation of homeostasis
 Kidneys in regulation of homeostasis Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important terms
Kidneys in regulation of homeostasis Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important terms
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Renal Physiology. April, J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine.
 Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Hyperaldosteronism: Conn's Syndrome
 RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
BODY FLUID. Outline. Functions of body fluid Water distribution in the body Maintenance of body fluid. Regulation of fluid homeostasis
 BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
Chapter 26 The Urinary System
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
After studying this lecture, you should be able to...
 Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
PHGY210 Renal Physiology
 PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
Lab Activity 31. Anatomy of the Urinary System. Portland Community College BI 233
 Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
The kidneys are excretory and regulatory organs. By
 exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
osmoregulation mechanisms in gills, salt glands, and kidneys
 Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
