A Trial of Calcium and Vitamin D for the Prevention of Colorectal Adenomas
|
|
|
- Berenice Dennis
- 6 years ago
- Views:
Transcription
1 The new england journal of medicine Original Article A Trial of Calcium and Vitamin D for the Prevention of Colorectal Adenomas John A. Baron, M.D., Elizabeth L. Barry, Ph.D., Leila A. Mott, M.S., Judy R. Rees, B.M., B.Ch., Robert S. Sandler, M.D., Dale C. Snover, M.D., Roberd M. Bostick, M.D., M.P.H., Anastasia Ivanova, Ph.D., Bernard F. Cole, Ph.D., Dennis J. Ahnen, M.D., Gerald J. Beck, Ph.D., Robert S. Bresalier, M.D., Carol A. Burke, M.D., Timothy R. Church, Ph.D., Marcia Cruz Correa, M.D., Ph.D., Jane C. Figueiredo, Ph.D., Michael Goodman, M.D., M.P.H., Adam S. Kim, M.D., Douglas J. Robertson, M.D., Richard Rothstein, M.D., Aasma Shaukat, M.D., M.P.H., March E. Seabrook, M.D., and Robert W. Summers, M.D. ABSTRACT BACKGROUND Epidemiologic and preclinical data suggest that higher intake and serum levels of vitamin D and higher intake of calcium reduce the risk of colorectal neoplasia. To further study the chemopreventive potential of these nutrients, we conducted a randomized, double-blind, placebo-controlled trial of supplementation with vitamin D, calcium, or both for the prevention of colorectal adenomas. METHODS We recruited patients with recently diagnosed adenomas and no known colorectal polyps remaining after complete colonoscopy. We randomly assigned 2259 participants to receive daily vitamin D 3 (1000 IU), calcium as carbonate (1200 mg), both, or neither in a partial 2 2 factorial design. Women could elect to receive calcium plus random assignment to vitamin D or placebo. Follow-up colonoscopy was anticipated to be performed 3 or 5 years after the baseline examinations, according to the endoscopist s recommendation. The primary end point was adenomas diagnosed in the interval from randomization through the anticipated surveillance colonoscopy. The authors affiliations are listed in the Appendix. Address reprint requests to Dr. Baron at the University of North Carolina at Chapel Hill, CB #7555, 4160-A Bioinformatics Bldg., 130 Mason Farm Rd., Chapel Hill NC , or at jabaron@ med. unc. edu. N Engl J Med 2015;373: DOI: /NEJMoa Copyright 2015 Massachusetts Medical Society. RESULTS Participants who were randomly assigned to receive vitamin D had a mean net increase in serum 25-hydroxyvitamin D levels of 7.83 ng per milliliter, relative to participants given placebo. Overall, 43% of participants had one or more adenomas diagnosed during follow-up. The adjusted risk ratios for recurrent adenomas were 0.99 (95% confidence interval [CI], 0.89 to 1.09) with vitamin D versus no vitamin D, 0.95 (95% CI, 0.85 to 1.06) with calcium versus no calcium, and 0.93 (95% CI, 0.80 to 1.08) with both agents versus neither agent. The findings for advanced adenomas were similar. There were few serious adverse events. CONCLUSIONS Daily supplementation with vitamin D 3 (1000 IU), calcium (1200 mg), or both after removal of colorectal adenomas did not significantly reduce the risk of recurrent colorectal adenomas over a period of 3 to 5 years. (Funded by the National Cancer Institute; ClinicalTrials.gov number, NCT ) n engl j med 373;16 nejm.org October 15,
2 The new england journal of medicine Vitamin D, an essential nutrient that is important for bone mineralization and calcium homeostasis, 1 also has effects beyond bone and calcium. Many studies have shown it to be antineoplastic, particularly in the colorectum. In in vitro studies, vitamin D and its analogues have been shown to inhibit proliferation, induce differentiation, inhibit angiogenesis, and promote apoptosis in epithelial tissues. 2,3 High vitamin D intake inhibits experimental carcinogenesis, 2,3 even in animals that are vitamin D replete. 4 Observational studies of vitamin D intake 5-7 and serum levels of 25-hydroxyvitamin D 8-10 have shown inverse associations between these measures and the risk of colorectal cancer or adenoma Trials of vitamin D supplementation have not shown a decrease in the incidence of colorectal cancer in association with supplementation, but these studies were limited by small numbers of events, low vitamin D doses, 14 and relatively short follow-up periods for invasive cancer end points High calcium intake is also associated with lower risks of colorectal neoplasia. Increases in dietary calcium have been shown to inhibit largebowel carcinogenesis in animal models, 15 and epidemiologic studies have shown lower risks of colorectal cancer and adenomas in association with higher calcium intake. 16 Trials of calcium supplementation for adenoma prevention have shown reduced risks Moreover, calcium and vitamin D may have synergistic chemopreventive effects against colorectal neoplasia. 20,21 To further investigate the chemopreventive potential of vitamin D and calcium, we conducted a randomized trial of supplementation with calcium, vitamin D 3, or both for the prevention of new colorectal adenomas in persons with a recent history of adenomas. We hypothesized that supplementation would reduce the risk of adenoma and that both agents together would reduce the risk more than calcium alone. Our secondary hypotheses addressed the relationship between vitamin D supplementation and the risk of advanced adenoma, as well as the effects of vitamin D supplementation among persons with baseline 25-hydroxyvitamin D levels in blood that were below the study median, as compared with the effects in persons with levels above the median. Methods Participants We conducted this randomized, multicenter, double-blind, placebo-controlled trial at 11 academic medical centers and associated medical practices in the United States. Enrollment of patients took place from July 2004 through July Staff members at each center enrolled patients 45 to 75 years of age who had at least one colorectal adenoma removed within 120 days before enrollment, had no remaining polyps after a complete colonoscopy, and were anticipated to undergo a 3-year or 5-year colonoscopic followup examination recommended by the treating endoscopist. Eligible patients were in good general health and did not have familial colorectal cancer syndromes or serious intestinal disease. We did not include patients who had conditions that indicated that the study agents would pose a health risk (e.g., a history of kidney stones or hyperparathyroidism) or who had conditions that would indicate a need for either agent (e.g., osteoporosis). We also did not include patients who had a serum calcium level that was outside the normal range, a creatinine level that was more than 20% above the upper limit of the normal range, or a 25-hydroxyvitamin D level that was lower than 12 ng per milliliter or higher than 90 ng per milliliter. Study Design and Oversight In a partial factorial design, we evaluated four regimens, all of which involved two identical tablets taken daily: 1000 IU of vitamin D 3, 1200 mg of calcium as carbonate, both agents, or placebo. Women could elect to be randomly assigned to receive either calcium or calcium plus vitamin D (two-group randomization); all other patients were randomly assigned to receive one of the four regimens (full factorial randomization). The doses of study agents were chosen to increase the total intake substantially, with a margin of safety below the highest mean daily intake level believed unlikely to cause adverse effects in most people at the time that the trial began (2000 IU of vitamin D and 2.5 g of calcium). 22 In accordance with the protocol, study treatment was to continue until the anticipated 3-year or 5-year colonoscopic examination n engl j med 373;16 nejm.org October 15, 2015
3 Calcium and Vitamin D for the Prevention of Adenomas At enrollment, participants provided information regarding demographic data, medical history, medications, nutritional supplements, behavioral factors, and diet (using the Block Brief 2000 food frequency questionnaire [Nutritionquest]). Enrollment was followed by a placebo run-in period of 56 to 84 days to identify and exclude participants who were considered unlikely to follow study procedures. Subsequent randomization by the coordinating center was performed with the use of computer-generated random numbers with permuted blocks and stratification according to clinical center, sex, anticipated colonoscopic examination at 3 years or 5 years, and full factorial or two-group randomization. All study staff were unaware of the treatment assignments, with the exception of the data analyst and statistician, some of the programmers, and pharmacy personnel. Participants agreed to avoid taking study agents outside the trial. However, because of increasing publicity regarding the possible benefits of these supplements (especially vitamin D), daily personal use of up to 1000 IU of vitamin D, 400 mg of elemental calcium, or both were permitted, although discouraged, from April 2008 onward. Participants were contacted by telephone every 6 months and queried regarding adherence to study agents, illnesses, medication and supplement use, dietary calcium intake (see the Supplementary Appendix, available with the full text of this article at NEJM.org), and colorectal procedures. Records were collected that included data on major medical events, colorectal surgical procedures, and endoscopic examinations. Two physicians who were unaware of the study group assignments adjudicated the diagnosis of adverse events. Bottles of study tablets were mailed to participants every 4 months. Patients who wanted to take a multivitamin were offered a special preparation that did not include calcium and vitamin D. The study intervention ended on August 31, 2013; the treatment-phase follow-up continued until November 30, 2013, to accommodate the final 5-year participants. Blood levels of 25-hydroxyvitamin D, calcium, and creatinine were measured at baseline and at year 1, as well as at year 3 for participants with 5-year surveillance cycles. The level of 25-hydroxyvitamin D was also measured shortly before the end-of-treatment examination. The laboratory methods are described in the Supplementary Appendix. Levels of 25-hydroxyvitamin D were seasonally adjusted according to the month in which the blood was drawn (see the Supplementary Appendix). The net change in 25-hydroxyvitamin D levels was defined as the posttreatment level minus the pretreatment level in participants who received vitamin D, minus that difference in participants who were given no vitamin D. The study end points included all adenomas that were diagnosed in any colorectal endoscopic or surgical procedure at least 1 year after randomization and up to 6 months after the anticipated 3-year or 5-year colonoscopic examination. A single study pathologist who was unaware of the treatment assignments reviewed the slides for all excised colorectal lesions. We distinguished between lesions that were proximal to the splenic flexure and lesions that were more distal. Advanced adenomas were defined as those with cancer, high-grade dysplasia, more than 25% villous features, or an estimated diameter of at least 1 cm. Study diagnoses were compared with the diagnoses made by the pathologists at the clinical centers. Discrepancies were resolved by means of a detailed adjudication procedure (see the Supplementary Appendix). The study was conducted and reported in accordance with the study protocol, which is available at NEJM.org. The authors designed the study, analyzed the data, wrote the manuscript, and vouch for the completeness and accuracy of the data and analysis. Pfizer Consumer Healthcare provided the study agents. No institution or company affected the analysis or the decision to submit the manuscript for publication. All participants provided written informed consent; the research was approved by the institutional review board at each center. An independent data and safety monitoring committee oversaw the study. Statistical Analysis In our primary analysis, we compared the risk of one or more adenomas after randomization to vitamin D versus no vitamin D, calcium versus no calcium, and calcium plus vitamin D versus calcium alone. Participants who did not undergo n engl j med 373;16 nejm.org October 15,
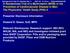
4 The new england journal of medicine Subgroup Vitamin D Relative Risk (95% CI) P Value Calcium Relative Risk (95% CI) P Value Overall Baseline serum 25-hydroxyvitamin D ng/ml >23.16 ng/ml Baseline dietary calcium 597 mg/day >597 mg/day Sex Male Female BMI < Baseline supplement use <400 IU/day vitamin D or mg/day calcium 400 IU/day vitamin D or mg/day calcium Cigarette smoking Never or former Current Alcohol use 0 drinks/day drinks/day >1 drink/day Baseline NSAID or aspirin use <4 days/wk 4 days/wk Anticipated surveillance interval 3 yr 5 yr 0.99 ( ) 1.05 ( ) 0.94 ( ) 0.91 ( ) 1.02 ( ) 0.99 ( ) 0.98 ( ) 0.88 ( ) 1.02 ( ) 1.03 ( ) 0.94 ( ) 1.04 ( ) 0.98 ( ) 0.99 ( ) 0.85 ( ) 1.10 ( ) 0.98 ( ) 1.02 ( ) 0.95 ( ) 1.04 ( ) 0.93 ( ) ( ) 1.01 ( ) 0.88 ( ) 0.90 ( ) 0.97 ( ) 0.93 ( ) 1.03 ( ) 0.75 ( ) 0.93 ( ) 1.08 ( ) 0.95 ( ) 0.87 ( ) 0.93 ( ) 1.28 ( ) 0.87 ( ) 1.12 ( ) 0.83 ( ) 0.96 ( ) 0.92 ( ) 0.98 ( ) 0.90 ( ) Figure 1. Subgroup Analysis of the Effects of Supplementation with Calcium or Vitamin D on the Development of One or More Adenomas. The body-mass index (BMI) is the weight in kilograms divided by the square of the height in meters. NSAID denotes nonsteroidal antiinflammatory drug. the anticipated colonoscopic examination at 3 years or 5 years were included in the analysis if they had had a colonoscopic examination performed at least 1 year after randomization. The sample size and statistical power considerations are described in the Supplementary Appendix. In the prespecified primary analysis, contingency tables and standard chi-square tests were used for the comparison of adenoma occurrence among randomized groups. The calcium analyses included only the participants who underwent full-factorial randomization. Subsequent multivariable generalized linear models for binary data were used to estimate adjusted risk ratios and confidence intervals. The covariates were age, sex, clinical center, number of baseline adenomas (one, two, or three or more), anticipated 3-year versus 5-year surveillance interval, and two-group versus full-factorial randomization. Clinical centers were grouped geographically when necessary because of sparse data. One subgroup analysis was prespecified: the effects of vitamin D in participants with baseline 25-hydroxyvitamin D levels below the overall median level were compared with the effects in those with levels above the median level. Eight additional post hoc subgroup analyses were conducted, as described in Figure 1. Interactions were assessed with the use of Wald tests. For interactions with variables that had more than two levels, we used a one-degree-of-freedom test for trend over medians within strata. In all analyses of randomly assigned treatments, participants were evaluated according to their assigned treat n engl j med 373;16 nejm.org October 15, 2015
5 Calcium and Vitamin D for the Prevention of Adenomas ment group, regardless of their adherence to the study treatment and procedures. Sensitivity analyses were conducted with imputation of missing end points as either adenomas or no adenomas. In a post hoc observational analysis, we similarly assessed associations between adenoma risk and baseline serum 25-hydroxyvitamin D levels among participants who were not randomly assigned to take vitamin D, as well as the association between adenoma risk and baseline calcium intake among participants who were not randomly assigned to receive calcium. The analyses were adjusted for a number of covariates, including (but not limited to) age, clinical center, surveillance interval (3 or 5 years), and number of baseline adenomas (one, two, or three or more). Two-sided P values of less than 0.05 were considered to indicate statistical significance. Statistical analyses were conducted with the use of SAS software, version 9.4 (SAS Institute), and STATA software, version 12 (StataCorp). Results Participants During the period from July 2004 through July 2008, the study staff screened colonoscopy and pathology reports and found 19,083 apparently eligible patients (Fig. S1 in the Supplementary Appendix). Ultimately, 2813 participants entered the run-in period, and 2259 underwent randomization. The study population was middle-aged or older; most patients were non-hispanic men, and more than 35% of the patients were obese (Table 1). A total of 11% of the participants had three or more adenomas at baseline, and 18% had one or more advanced adenomas. There were no material differences between treatment groups with regard to personal characteristics (Table 1). Fifteen patients who underwent randomization and were included in the analysis were later found not to have met all eligibility criteria (see the Supplementary Appendix). Adherence to the Study Procedures The reported adherence to colonoscopy was excellent. Only 67 participants (3.0%) did not have a colonoscopic examination with associated histologic data at least 1 year after randomization, and 104 participants (4.6%) dropped out of the study, were lost to follow-up, or died; this left 2088 participants (92.4%) in the analysis (Fig. S1 in the Supplementary Appendix). Only approximately 1% of the colonoscopic examinations failed to reach the cecum; in 2.0% of procedures, the preparation of the colon was deemed poor, and in 6.8% it was deemed fair. The times to final colonoscopic examination are summarized in Table S2 in the Supplementary Appendix. A total of 1598 participants (77%) had a surveillance colonoscopic examination within 6 months before or after the anticipated 3-year or 5-year follow-up examination. A total of 60 participants (2.9%) had more than one colonoscopic examination during follow-up. During the first year after randomization, 1974 of the 2259 participants who underwent randomization (87.4%) reported taking 80% or more of the study tablets; in the final year of treatment, 1663 participants (73.6%) reported this level of adherence. During the treatment period, 1719 participants (76.1%) reported taking at least 80% of the study tablets, and 1949 (86.3%) reported taking at least 50%. Only 98 of 2251 participants for whom data on personal vitamin supplementation were available (4.4%) reported on two or more semiannual interviews that they took personal vitamin D supplements of 1000 IU or more daily, 74 (3.3%) reported that they took 400 mg or more of calcium daily, and 78 (3.5%) reported that they took 500 to less than 1000 IU of vitamin D. The mean (±SD) net increase in serum 25-hydroxyvitamin D among participants randomly assigned to vitamin D was 7.83±13.4 ng per milliliter in a blood sample drawn shortly before the end of treatment. Occurrence of Adenomas In follow-up examinations, 3131 lesions that were potentially neoplastic were seen in 1301 participants. Pathological evaluations were available for 3012 lesions in 1280 participants. For 119 lesions, the tissue was lost, fulgurated without biopsy, or unsuitable for diagnosis; this left 2059 (99%) of the examined participants for whom we could determine adenoma status. Adenomas were diagnosed in 880 participants (43%). Effects of Supplementation The study interventions, alone or in combination, did not have a significant effect on the risk of adenoma (Table 2). The adjusted risk ratio for any adenoma among patients taking vitamin D as compared with patients who did not take vita- n engl j med 373;16 nejm.org October 15,
6 The new england journal of medicine Table 1. Selected Baseline Characteristics According to Treatment Assignment.* Characteristic Full Factorial Randomization Two-Group Randomization Placebo (N = 415) Calcium (N = 419) Vitamin D (N = 420) Vitamin D plus Calcium (N = 421) Calcium plus Placebo (N = 295) Calcium plus Vitamin D (N = 289) Sex no. (%) Female 60 (14.5) 63 (15.0) 62 (14.8) 67 (15.9) 295 (100) 289 (100) Male 355 (85.5) 356 (85.0) 358 (85.2) 354 (84.1) 0 0 Age yr 58.2± ± ± ± ± ±6.6 Race no./total no. (%) White 357/402 (88.8) 354/404 (87.6) 364/404 (90.1) 350/404 (86.6) 238/275 (86.5) 237/271 (87.5) Black 27/402 (6.7) 33/404 (8.2) 25/404 (6.2) 46/404 (11.4) 28/275 (10.2) 25/271 (9.2) Asian or Pacific Islander 10/402 (2.5) 10/404 (2.5) 12/404 (3.0) 6/404 (1.5) 8/275 (2.9) 7/271 (2.6) Other 8/402 (2.0) 7/404 (1.7) 3/404 (0.7) 2/404 (0.5) 1/275 (0.4) 2/271 (0.7) Non-Hispanic ethnic background no./total no. (%) 395/414 (95.4) 395/418 (94.5) 396/420 (94.3) 394/420 (93.8) 267/295 (90.5) 263/289 (91.0) Family history of colorectal cancer no./total no. (%) 59/378 (15.6) 77/395 (19.5) 66/391 (16.9) 75/393 (19.1) 52/279 (18.6) 43/270 (15.9) BMI 29.0± ± ± ± ± ±5.4 BMI 30 no./total no. (%) 147/414 (35.5) 165/419 (39.4) 163/420 (38.8) 144/421 (34.2) 112/294 (38.1) 92/288 (31.9) Smoking status no. (%) Never smoked 187 (45.1) 212 (50.6) 217 (51.7) 204 (48.5) 205 (69.5) 169 (58.5) Former smoker 193 (46.5) 174 (41.5) 164 (39.0) 169 (40.1) 62 (21.0) 88 (30.4) Current smoker 35 (8.4) 33 (7.9) 39 (9.3) 48 (11.4) 28 (9.5) 32 (11.1) At least one advanced adenoma at baseline no./total no. (%) 69/399 (17.3) 79/399 (19.8) 80/398 (20.1) 76/404 (18.8) 56/289 (19.4) 47/281 (16.7) Alcohol intake drinks/day 0.89± ± ± ± ± ±0.69 Dietary calcium intake mg/day 672± ± ± ± ± ± n engl j med 373;16 nejm.org October 15, 2015
7 Calcium and Vitamin D for the Prevention of Adenomas Characteristic Full Factorial Randomization Two-Group Randomization Placebo (N = 415) Calcium (N = 419) Vitamin D (N = 420) Vitamin D plus Calcium (N = 421) Calcium plus Placebo (N = 295) Calcium plus Vitamin D (N = 289) Baseline supplemental calcium intake no./total no. (%) None 201/387 (51.9) 199/393 (50.6) 207/396 (52.3) 212/400 (53.0) 64/257 (24.9) 56/255 (22.0) elemental mg/day 173/387 (44.7) 172/393 (43.8) 172/396 (43.4) 169/400 (42.2) 94/257 (36.6) 86/255 (33.7) 500 elemental mg/day 13/387 (3.4) 22/393 (5.6) 17/396 (4.3) 19/400 (4.8) 99/257 (38.5) 113/255 (44.3) Baseline dietary vitamin D intake IU/day 138±97 146±96 131± ±92 124±96 134±98 Baseline supplemental vitamin D intake no./total no. (%) None 204/391 (52.2) 203/389 (52.2) 209/397 (52.6) 210/397 (52.9) 84/246 (34.1) 71/233 (30.5) IU/day 175/391 (44.8) 170/389 (43.7) 162/397 (40.8) 175/397 (44.1) 120/246 (48.8) 110/233 (47.2) 500 IU/day 12/391 (3.1) 16/389 (4.1) 26/397 (6.5) 12/397 (3.0) 42/246 (17.1) 52/233 (22.3) Baseline serum 25-hydroxyvitamin D level ng/ml 24.24± ± ± ± ± ±7.71 Baseline aspirin use no. (%) <4 days/wk 255 (61.4) 249 (59.4) 255 (60.7) 270 (64.1) 227 (76.9) 206 (71.3) 4 days/wk 160 (38.6) 170 (40.6) 165 (39.3) 151 (35.9) 68 (23.1) 83 (28.7) Baseline non-aspirin NSAID use no. (%) <4 days/wk 372 (89.6) 367 (87.6) 379 (90.2) 388 (92.2) 261 (88.5) 253 (87.5) 4 days/wk 43 (10.4) 52 (12.4) 41 (9.8) 33 (7.8) 34 (11.5) 36 (12.5) * Plus minus values are means ±SD. The table includes all participants who underwent randomization. Women could elect to be randomly assigned to receive either calcium plus placebo or calcium plus vitamin D (two-group randomization); all other patients were randomly assigned to receive one of four regimens: vitamin D, calcium, both agents, or placebo (full factorial randomization). NSAID denotes nonsteroidal antiinflammatory drug. Race and ethnic background were self-reported. The body-mass index (BMI) is the weight in kilograms divided by the square of the height in meters. A BMI of 30 or higher indicates obesity. Supplemental values include those from separate supplements and multivitamins. Participants were asked to stop taking these personal supplements at enrollment as a condition of study entry. However, from April 2008 onward, daily personal use of up to 1000 IU of vitamin D, 400 mg of elemental calcium, or both were permitted, although discouraged. Patients who wanted to take a multivitamin were offered a special preparation that did not include calcium and vitamin D. n engl j med 373;16 nejm.org October 15,
8 The new england journal of medicine Table 2. Risk Ratios for Colorectal Adenoma Outcomes According to Treatment Assignment.* Treatment Assignment One or More Adenomas One or More Advanced Adenomas No. of Patients/ Total No. (%) Risk Ratio (95% CI) No. of Patients/ Total No. (%) Risk Ratio (95% CI) Vitamin D vs. no vitamin D No vitamin D 442/1035 (42.7) Reference 98/1042 (9.4) Reference Vitamin D 438/1024 (42.8) 0.99 ( ) 98/1032 (9.5) 0.99 ( ) Calcium vs. no calcium No calcium 362/761 (47.6) Reference 77/764 (10.1) Reference Calcium 345/762 (45.3) 0.95 ( ) 81/773 (10.5) 1.02 ( ) Calcium plus vitamin D vs. calcium alone Calcium 259/655 (39.5) Reference 63/662 (9.5) Reference Calcium plus vitamin D 259/643 (40.3) 1.01 ( ) 56/648 (8.6) 0.89 ( ) Calcium plus vitamin D vs. neither agent Neither calcium nor vitamin D 183/380 (48.2) Reference 35/380 (9.2) Reference Calcium plus vitamin D 174/381 (45.7) 0.93 ( ) 37/387 (9.6) 0.99 ( ) * The analyses of vitamin D versus no vitamin D included all participants who underwent randomization. The analyses of calcium versus no calcium and of vitamin D plus calcium versus neither agent were restricted to participants who underwent full factorial randomization. The analyses of vitamin D plus calcium versus calcium did not include participants who underwent full factorial randomization and were assigned to receive placebo or vitamin D alone. P values, calculated with the use of a chi-square contingency-table test, are as follows: vitamin D versus no vitamin D, P = 0.98; calcium versus no calcium, P = 0.37; vitamin D plus calcium versus calcium, P = 0.79; and vitamin D plus calcium versus neither agent, P = Denominators differ between adenomas and advanced adenomas because of missing data for lesion size and an assumption that small lesions (<6 mm) with missing pathological data are not advanced adenomas (see the Supplementary Appendix). Risk ratios were adjusted for age, clinical center, anticipated surveillance interval (3 or 5 years), a three-level variable for sex and type of randomization (male, female and two-group randomization, female and full factorial randomization), and number of baseline adenomas (1, 2, or 3). min D was 0.99 (95% confidence interval [CI], 0.89 to 1.09), and the adjusted risk ratio among patients taking calcium as compared with those who did not take calcium was 0.95 (95% CI, 0.85 to 1.06). Among patients taking vitamin D plus calcium versus those taking calcium alone, the adjusted risk ratio was 1.01 (95% CI, 0.88 to 1.15). The adjusted risk ratio among patients taking vitamin D plus calcium versus those taking neither agent was 0.93 (95% CI, 0.80 to 1.08). The findings for advanced adenomas also did not suggest meaningful effects. The results for proximal adenomas were similar to those for distal adenomas (Table S3 in the Supplementary Appendix). In the subgroup analyses, we found almost no significant effects of supplementation (Fig. 1, and Fig. S2 in the Supplementary Appendix). The findings were similar among participants with baseline 25-hydroxyvitamin D levels below the study median of 23.2 ng per milliliter and those with levels above the study median. However, body-mass index (BMI) appeared to modify the effects of calcium on adenoma risk (P = 0.02): the lower the BMI, the greater the response to calcium supplementation. Findings with respect to advanced adenomas were broadly similar to those for all adenomas (Fig. 1, and Fig. S2 in the Supplementary Appendix). The findings did not differ significantly between participants who were using vitamin D or calcium supplements at baseline and those who were not or between those who had advanced adenomas at baseline and those who did not (Tables S4, S5, and S6 in the Supplementary Appendix). There were no indications of effects in a per-protocol analysis, nor was there an association between adenoma risk and changes in 25-hydroxyvitamin D levels 1526 n engl j med 373;16 nejm.org October 15, 2015
9 Calcium and Vitamin D for the Prevention of Adenomas Table 3. Adverse Events.* Adverse Event Vitamin D versus No Vitamin D Calcium versus No Calcium No Vitamin D (N = 1129) Vitamin D (N = 1130) P Value No Calcium (N = 835) Calcium (N = 840) P Value number (percent) number (percent) Death 12 (1.1) 15 (1.3) (1.4) 13 (1.5) 0.85 Myocardial infarction with or without 7 (0.6) 8 (0.7) (1.1) 2 (0.2) 0.03 revascularization Revascularization without myocardial 11 (1.0) 12 (1.1) (1.0) 12 (1.4) 0.38 infarction Stroke 5 (0.4) 9 (0.8) (0.6) 3 (0.4) 0.51 Transient ischemic attack 1 (0.1) 3 (0.3) (0.4) Cancer Any 61 (5.4) 47 (4.2) (5.5) 46 (5.5) 0.98 Colorectal 2 (0.2) 3 (0.3) (0.2) 0.50 Urolithiasis 28 (2.5) 19 (1.7) (1.8) 20 (2.4) 0.40 Hypercreatininemia 67 (6.0) 57 (5.1) (4.9) 58 (7.0) 0.06 Hypercalcemia 28 (2.5) 25 (2.2) (0.6) 17 (2.0) 0.01 Hypercalcemia after albumin 4 (0.4) 3 (0.3) (0.2) 0.50 correction Fracture 64 (5.7) 55 (4.9) (5.1) 37 (4.4) 0.47 * The table includes all confirmed events up to 30 days after the cessation of study treatment in all participants who underwent randomization. Data are the numbers of participants who had one or more occurrences of an adverse event and their percentage among all participants who were randomly assigned to the given group. Hypercreatininemia was defined as a creatinine level in the blood sample drawn at year 1 (all participants) or year 3 (participants with a 5-year follow-up) that was above the normal range among participants who had creatinine levels in the normal range at baseline; 31 participants had baseline creatinine levels that were above the normal range. Data were available for 1113 participants in the group that received no vitamin D, 1115 participants in the group that received vitamin D, 822 participants in the group that received no calcium, and 825 participants in the group that received calcium. Hypercalcemia was defined as a calcium level in the blood sample drawn at year 1 or year 3 that was above the normal range, before albumin correction. Albumin correction was not available for 12 participants. or total calcium intake from baseline to shortly before the end of treatment (Tables S7 and S8 in the Supplementary Appendix). However, there was a suggestion that supplementation with vitamin D or calcium conferred lower risks among participants with longer surveillance (and treatment) intervals, although the differences were not significant (Fig. 1, and Table S9 in the Supplementary Appendix). The sensitivity analysis did not suggest that missing data distorted the primary analyses (Table S10 in the Supplementary Appendix). Adverse events are shown in Table 3. Calcium supplementation was associated with a small, nonsignificantly greater risk of urolithiasis than no calcium supplementation, and vitamin D supplementation was associated with a nonsignificantly lower risk of urolithiasis than no vitamin D supplementation. Participants who were randomly assigned to take calcium had slightly higher serum creatinine levels than did participants who were not assigned to take calcium; the difference was of borderline significance. In addition, participants assigned to take calcium had significantly fewer myocardial infarctions than participants who were assigned to no calcium supplementation. The observational associations between adenoma occurrence and baseline serum 25-hydroxyvitamin D level or baseline calcium intake roughly paralleled the findings for supplementation with vitamin D or calcium (Table 4). Among participants who were not given vitamin D, baseline 25-hydroxyvitamin D levels were not significantly associated with adenoma risk (risk ratio, quartile 4 vs. quartile 1, 0.98; 95% CI, 0.79 to 1.21). n engl j med 373;16 nejm.org October 15,
10 The new england journal of medicine Table 4. Observational Association of Baseline Serum 25-Hydroxyvitamin D Level and Dietary Calcium Intake with Risk of Colorectal Adenoma. Quartile of Level or Intake* Baseline Serum 25-Hydroxyvitamin D Level Baseline Dietary Calcium Intake Participants with one or more adenomas No. of Patients/ Total No. (%) Adjusted Risk Ratio (95% CI) Adjusted Risk Ratio per 10 ng/ml (95% CI) 0.98 ( ) No. of Patients/ Total No. (%) Adjusted Risk Ratio (95% CI) Quartile 1 108/256 (42.2) Reference 89/179 (49.7) Reference Quartile 2 115/271 (42.4) 1.02 ( ) Quartile 3 117/257 (45.5) 1.06 ( ) Quartile 4 102/251 (40.6) 0.98 ( ) Participants with one or more advanced adenomas 0.91 ( ) 94/170 (55.3) 1.17 ( ) 69/170 (40.6) 0.85 ( ) 84/184 (45.7) 0.95 ( ) Quartile 1 25/257 (9.7) Reference 21/176 (11.9) Reference Quartile 2 28/270 (10.4) 1.11 ( ) Quartile 3 21/263 (8.0) 0.83 ( ) Quartile 4 24/252 (9.5) 1.06 ( ) 15/176 (8.5) 0.72 ( ) 19/170 (11.2) 0.96 ( ) 18/185 (9.7) 0.82 ( ) Adjusted Risk Ratio per 200 mg (95% CI) 0.99 ( ) 0.94 ( ) * For 25-hydroxyvitamin D, quartiles of seasonally adjusted values were as follows: quartile 1, IU; quartile 2, to IU; quartile 3, to IU; and quartile 4, IU. For calcium intake, the quartiles were as follows: quartile 1, up to mg; quartile 2, to mg; quartile 3, to mg; and quartile 4, mg. The analysis was restricted to participants who did not receive study vitamin D supplementation; risk ratios were adjusted for age, clinical center, anticipated surveillance interval (3 or 5 years), a three-level variable for sex and type of randomization (male, female and two-group randomization, female and full factorial randomization), number of baseline adenomas (one, two, or three or more), and calcium treatment assignment (participants who underwent two-group randomization are grouped with participants who underwent full factorial randomization and received calcium). The analysis was restricted to participants who underwent full factorial randomization and did not receive study calcium supplementation; risk ratios were adjusted for age, clinical center, anticipated surveillance interval (3 or 5 years), sex, number of baseline adenomas (one, two, or three or more), and vitamin D treatment assignment; because of sparse data for advanced adenomas, clinical centers are grouped geographically into southeast (Georgia, North Carolina, South Carolina, and Puerto Rico), north (Ohio, New Hampshire, Iowa, and Minnesota), and west (Colorado, Texas, and California). The P value for trend for adenomas was 0.86, and the P value for trend for advanced adenomas was The P value for trend for adenomas was 0.33, and the P value for trend for advanced adenomas was Denominators differ between adenomas and advanced adenomas because of missing data on lesion size and an assumption that small lesions (<6 mm) with missing pathological data are not advanced adenomas (see the Supplementary Appendix). The results for baseline calcium intake among participants who were not given calcium were similar (risk ratio, quartile 4 vs. quartile 1, 0.95; 95% CI, 0.75 to 1.19). We also found no observational associations between the risk of advanced adenomas and baseline serum 25-hydroxyvitamin D level or baseline calcium intake. Discussion Contrary to our hypotheses, neither 1000 IU of vitamin D 3 nor 1200 mg of calcium, taken daily alone or in combination, reduced the risk of colorectal adenomas. The findings were similar with regard to the risk of advanced adenomas, and vitamin D supplementation was ineffective even among participants who had lower baseline serum 25-hydroxyvitamin D levels. Unplanned subgroup analyses based on participant characteristics at baseline yielded similar results, with the exception of a lower risk of adenomas in association with calcium supplementation among participants with lower BMIs. Because of the number of subgroups examined, this finding may be due to chance. In observational analyses, we also found no association between either baseline 1528 n engl j med 373;16 nejm.org October 15, 2015
11 Calcium and Vitamin D for the Prevention of Adenomas 25-hydroxyvitamin D levels or dietary calcium intake and the risk of adenomas or advanced adenomas. Our study dose of vitamin D (1000 IU per day) exceeded the currently recommended intake for adults up to 70 years of age (600 IU per day). However, a higher dose would have raised 25-hydroxyvitamin D levels in serum more markedly and provided a more sensitive test of vitamin D chemoprevention. Meta-analyses have summarized the observational association between serum 25-hydroxyvitamin D level and colorectal cancer as relative risks of 0.74 per 10 ng per milliliter, per 10 ng per milliliter, 23 and 0.96 per 100 IU per liter 5 (0.85 per 10 ng per milliliter). These associations suggest that the net mean increase of 7.83 ng per milliliter in serum 25-hydroxyvitamin D levels in our study might yield a relative risk between 0.80 and 0.88, which is outside our confidence limits for all adenomas. In this sense, our findings provide evidence against the strong observational association reported in these meta-analyses. A report of increasing colorectal cancer risk with increasing 25-hydroxyvitamin D levels 24 was included in one meta-analysis 9 that yielded a summary relative risk of 0.94 per 10 nmol per liter (0.90 per 10 ng per milliliter). This suggests that the increase of 7.83 ng per milliliter in 25-hydroxyvitamin D levels in our study might yield a relative risk of 0.92, which is within our confidence intervals and so statistically consistent with our data. Meta-analyses of the relationship between adenoma risk and serum 25-hydroxyvitamin D levels 8,10 have shown summary relative risks between 0.82 and 0.93 per 20 ng per milliliter (0.93 to 0.97 per 7.75 ng per milliliter). Again, our data are consistent with this weaker association. 8,10 A larger sample size, higher vitamin D dose, or perhaps a longer intervention might have been required to detect these associations. Also, the fact that vitamin D may have a weaker relationship with adenomas than with colorectal cancer might imply that vitamin D acts at a later stage of carcinogenesis than that at which adenomas develop. In view of the strong data supporting a chemopreventive effect of calcium supplementation on colorectal carcinogenesis 15,16,18,19 (including findings in our own previous trial), 17 it is surprising that we found no effect of calcium. However, the lack of association between baseline dietary calcium intake and adenoma risk observed in our study population supports the negative findings for calcium in our trial. Whether the high prevalence of obesity in our study population explains the lack of a calcium effect requires further investigation. Important adverse events in the trial were generally uncommon. However, calcium supplementation resulted in an unexpected, small increase in serum creatinine level, 25 which was of uncertain clinical significance. There was a significantly lower risk of myocardial infarction among participants randomly assigned to receive calcium, a finding that contrasts with recent evidence. 26 The lower cancer risk associated with vitamin D supplementation and the smaller number of participants receiving vitamin D or calcium in whom fractures occurred were all compatible with chance. Our trial had several strengths. It was large enough to detect modest chemopreventive effects, adherence to study treatment was high, and participants largely avoided taking vitamin D and calcium in substantial amounts outside the study. We obtained findings from a follow-up colonoscopic examination in a high proportion of participants, and virtually all lesions underwent central pathological review. However, the vitamin D dose was lower than the dose many experts now recommend, and it was used for a limited time. The trial was conducted among patients with a recent history of colorectal adenomas, and the results might not apply to persons without such a history. In summary, contrary to our expectation, supplementation with 1000 IU of vitamin D 3, 1200 mg of calcium, or both did not significantly affect the risk of colorectal adenomas over a period of 3 to 5 years. We have no ready explanation for the finding with regard to calcium supplementation, but the lack of an observational association between the risk of adenomas and baseline dietary calcium intake in our population supports it. Our findings with regard to vitamin D are not inconsistent with a modest chemopreventive potential, but they do not support the more marked chemopreventive effect that has sometimes been posited. Supported by a grant from the National Institutes of Health, National Cancer Institute (CA098286, to Dr. Baron). Disclosure forms provided by the authors are available with the full text of this article at NEJM.org. n engl j med 373;16 nejm.org October 15,
12 Calcium and Vitamin D for the Prevention of Adenomas Appendix The authors affiliations are as follows: the Departments of Medicine (J.A.B., D.J.R., R.R.) and Epidemiology (J.A.B., E.L.B., L.A.M., J.R.R.), Geisel School of Medicine at Dartmouth, Hanover, and Department of Medicine, Dartmouth Hitchcock Medical Center, Lebanon (D.J.R., R.R.) both in New Hampshire; the Departments of Medicine (J.A.B., R.S.S.) and Biostatistics (A.I.), University of North Carolina at Chapel Hill, Chapel Hill; the Department of Pathology, Fairview Southdale Hospital, Edina (D.C.S.), and the Division of Environmental Health Sciences, University of Minnesota School of Public Health (T.R.C.), Minnesota Gastroenterology (A.S.K.), Department of Medicine, University of Minnesota (A.S.), and Minneapolis Veterans Affairs (VA) Medical Center (A.S.), Minneapolis all in Minnesota; the Department of Epidemiology, Rollins School of Public Health, Emory University and Winship Cancer Institute, Emory University, Atlanta (R.M.B., M.G.); the Department of Mathematics and Statistics, University of Vermont, Burlington (B.F.C.), and VA Outcomes Group, White River Junction (D.J.R.) both in Vermont; the Department of Medicine, University of Colorado School of Medicine, Denver (D.J.A.); the Departments of Quantitative Health Sciences (G.J.B.) and Gastroenterology and Hepatology (C.A.B.), Cleveland Clinic, Cleveland; the Department of Gastroenterology, Hepatology, and Nutrition, University of Texas M.D. Anderson Cancer Center, Houston (R.S.B.); Puerto Rico Cancer Center, Medical Sciences Campus, University of Puerto Rico, San Juan (M.C.-C.); the Department of Preventive Medicine, Keck School of Medicine, University of Southern California, Los Angeles (J.C.F.); Consultants in Gastroenterology, West Columbia, SC (M.E.S.); and the Department of Internal Medicine, University of Iowa Carver College of Medicine, Iowa City (R.W.S.). References 1. Brown AJ, Dusso A, Slatopolsky E. Vitamin D. Am J Physiol 1999; 277: F157-F Leyssens C, Verlinden L, Verstuyf A. Antineoplastic effects of 1,25(OH)2D3 and its analogs in breast, prostate and colorectal cancer. Endocr Relat Cancer 2013; 20: R31-R Feldman D, Krishnan AV, Swami S, Giovannucci E, Feldman BJ. The role of vitamin D in reducing cancer risk and progression. Nat Rev Cancer 2014; 14: Harris DM, Go VL. Vitamin D and colon carcinogenesis. J Nutr 2004; 134: Suppl: 3463S-3471S. 5. Touvier M, Chan DS, Lau R, et al. Meta-analyses of vitamin D intake, 25- hydroxyvitamin D status, vitamin D receptor polymorphisms, and colorectal cancer risk. Cancer Epidemiol Biomarkers Prev 2011; 20: Ma Y, Zhang P, Wang F, Yang J, Liu Z, Qin H. Association between vitamin D and risk of colorectal cancer: a systematic review of prospective studies. J Clin Oncol 2011; 29: Wei MY, Garland CF, Gorham ED, Mohr SB, Giovannucci E. Vitamin D and prevention of colorectal adenoma: a metaanalysis. Cancer Epidemiol Biomarkers Prev 2008; 17: Lee JE. Circulating levels of vitamin D, vitamin D receptor polymorphisms, and colorectal adenoma: a meta-analysis. Nutr Res Pract 2011; 5: Chung M, Lee J, Terasawa T, Lau J, Trikalinos TA. Vitamin D with or without calcium supplementation for prevention of cancer and fractures: an updated metaanalysis for the U.S. Preventive Services Task Force. Ann Intern Med 2011; 155: Yin L, Grandi N, Raum E, Haug U, Arndt V, Brenner H. Meta-analysis: serum vitamin D and colorectal adenoma risk. Prev Med 2011; 53: Avenell A, MacLennan GS, Jenkinson DJ, et al. Long-term follow-up for mortality and cancer in a randomized placebocontrolled trial of vitamin D(3) and/or calcium (RECORD trial). J Clin Endocrinol Metab 2012; 97: Lappe JM, Travers-Gustafson D, Davies KM, Recker RR, Heaney RP. Vitamin D and calcium supplementation reduces cancer risk: results of a randomized trial. Am J Clin Nutr 2007; 85: Trivedi DP, Doll R, Khaw KT. Effect of four monthly oral vitamin D3 (cholecalciferol) supplementation on fractures and mortality in men and women living in the community: randomised double blind controlled trial. BMJ 2003; 326: Wactawski-Wende J, Kotchen JM, Anderson GL, et al. Calcium plus vitamin D supplementation and the risk of colorectal cancer. N Engl J Med 2006; 354: Pence BC. Role of calcium in colon cancer prevention: experimental and clinical studies. Mutat Res 1993; 290: Huncharek M, Muscat J, Kupelnick B. Colorectal cancer risk and dietary intake of calcium, vitamin D, and dairy products: a meta-analysis of 26,335 cases from 60 observational studies. Nutr Cancer 2009; 61: Baron JA, Beach M, Mandel JS, et al. Calcium supplements for the prevention of colorectal adenomas. N Engl J Med 1999; 340: Bonithon-Kopp C, Kronborg O, Giacosa A, Räth U, Faivre J. Calcium and fibre supplementation in prevention of colorectal adenoma recurrence: a randomised intervention trial. Lancet 2000; 356: Chu DZ, Hussey MA, Alberts DS, et al. Colorectal Chemoprevention Pilot Study (SWOG-9041), randomized and placebo controlled: the importance of multiple luminal lesions. Clin Colorectal Cancer 2011; 10: Beaty MM, Lee EY, Glauert HP. Influence of dietary calcium and vitamin D on colon epithelial cell proliferation and 1,2-dimethylhydrazine-induced colon carcinogenesis in rats fed high fat diets. J Nutr 1993; 123: Grau MV, Baron JA, Sandler RS, et al. Vitamin D, calcium supplementation, and colorectal adenomas: results of a randomized trial. J Natl Cancer Inst 2003; 95: Institute of Medicine Standing Committee on the Scientific Evaluation of Dietary Reference Intakes. Dietary reference intakes for calcium, phosphorus, magnesium, vitamin D and fluoride. Washington, DC: National Academies Press, Gandini S, Boniol M, Haukka J, et al. Meta-analysis of observational studies of serum 25-hydroxyvitamin D levels and colorectal, breast and prostate cancer and colorectal adenoma. Int J Cancer 2011; 128: Weinstein SJ, Yu K, Horst RL, Ashby J, Virtamo J, Albanes D. Serum 25-hydroxyvitamin D and risks of colon and rectal cancer in Finnish men. Am J Epidemiol 2011; 173: Barry EL, Mott LA, Melamed ML, et al. Calcium supplementation increases blood creatinine concentration in a randomized controlled trial. PLoS One 2014; 9(10): e Bolland MJ, Avenell A, Baron JA, et al. Effect of calcium supplements on risk of myocardial infarction and cardiovascular events: meta-analysis. BMJ 2010; 341: c3691. Copyright 2015 Massachusetts Medical Society n engl j med 373;16 nejm.org October 15, 2015
HHS Public Access Author manuscript N Engl J Med. Author manuscript; available in PMC 2016 April 15.
 A Trial of Calcium and Vitamin D for the Prevention of Colorectal Adenomas John A. Baron, M.D., Elizabeth L. Barry, Ph.D., Leila A. Mott, M.S., Judy R. Rees, B.M., B.Ch., Robert S. Sandler, M.D., Dale
A Trial of Calcium and Vitamin D for the Prevention of Colorectal Adenomas John A. Baron, M.D., Elizabeth L. Barry, Ph.D., Leila A. Mott, M.S., Judy R. Rees, B.M., B.Ch., Robert S. Sandler, M.D., Dale
Fat, Fiber, Meat and the Risk of Colorectal Adenomas
 American Journal of Gastroenterology ISSN 0002-9270 C 2005 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2005.00336.x Published by Blackwell Publishing Fat, Fiber, Meat and the Risk of Colorectal
American Journal of Gastroenterology ISSN 0002-9270 C 2005 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2005.00336.x Published by Blackwell Publishing Fat, Fiber, Meat and the Risk of Colorectal
removal of adenomatous polyps detects important effectively as follow-up colonoscopy after both constitute a low-risk Patients with 1 or 2
 Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Vitamin D Supplements and Prevention of Cancer and Cardiovascular Disease
 Original Article Vitamin D Supplements and Prevention of Cancer and Cardiovascular Disease JoAnn E. Manson, M.D., Dr.P.H., Nancy R. Cook, Sc.D., I Min Lee, M.B., B.S., Sc.D., William Christen, Sc.D., Shari
Original Article Vitamin D Supplements and Prevention of Cancer and Cardiovascular Disease JoAnn E. Manson, M.D., Dr.P.H., Nancy R. Cook, Sc.D., I Min Lee, M.B., B.S., Sc.D., William Christen, Sc.D., Shari
How to Design, Conduct, and Analyze Vitamin D Clinical Trials
 How to Design, Conduct, and Analyze Vitamin D Clinical Trials William B. Grant, PhD Sunlight, Nutrition and Health Research Center wbgrant@infionline.net Disclosure I receive funding from Bio-Tech Pharmacal,
How to Design, Conduct, and Analyze Vitamin D Clinical Trials William B. Grant, PhD Sunlight, Nutrition and Health Research Center wbgrant@infionline.net Disclosure I receive funding from Bio-Tech Pharmacal,
Calcium Supplementation Increases Blood Creatinine Concentration in a Randomized Controlled Trial
 Calcium Supplementation Increases Blood Creatinine Concentration in a Randomized Controlled Trial Elizabeth L. Barry, Geisel School of Medicine at Dartmouth Leila A. Mott, Geisel School of Medicine at
Calcium Supplementation Increases Blood Creatinine Concentration in a Randomized Controlled Trial Elizabeth L. Barry, Geisel School of Medicine at Dartmouth Leila A. Mott, Geisel School of Medicine at
Chemoprevention of Colorectal Cancer: Where We Stand
 Chemoprevention of Colorectal Cancer: Where We Stand Andrew T. Chan, MD, MPH Division of Gastroenterology Massachusetts General Hospital 2 nd World Congress on Controversies in Gastroenterology Xi an,
Chemoprevention of Colorectal Cancer: Where We Stand Andrew T. Chan, MD, MPH Division of Gastroenterology Massachusetts General Hospital 2 nd World Congress on Controversies in Gastroenterology Xi an,
Bariatric Surgery versus Intensive Medical Therapy for Diabetes 3-Year Outcomes
 The new england journal of medicine original article Bariatric Surgery versus Intensive Medical for Diabetes 3-Year Outcomes Philip R. Schauer, M.D., Deepak L. Bhatt, M.D., M.P.H., John P. Kirwan, Ph.D.,
The new england journal of medicine original article Bariatric Surgery versus Intensive Medical for Diabetes 3-Year Outcomes Philip R. Schauer, M.D., Deepak L. Bhatt, M.D., M.P.H., John P. Kirwan, Ph.D.,
Vitamin D and Calcium Therapy: how much is enough
 Vitamin D and Calcium Therapy: how much is enough Daniel D Bikle, MD, PhD Professor of Medicine VA Medical Center and University of California San Francisco DISCLOSURE Nothing to disclose 1 RECOMMENDATIONS
Vitamin D and Calcium Therapy: how much is enough Daniel D Bikle, MD, PhD Professor of Medicine VA Medical Center and University of California San Francisco DISCLOSURE Nothing to disclose 1 RECOMMENDATIONS
The Endocrine Society Guidelines
 Vitamin D and Calcium Therapy: how much is enough DISCLOSURE Daniel D Bikle, MD, PhD Professor of Medicine VA Medical Center and University of California San Francisco Nothing to disclose RECOMMENDATIONS
Vitamin D and Calcium Therapy: how much is enough DISCLOSURE Daniel D Bikle, MD, PhD Professor of Medicine VA Medical Center and University of California San Francisco Nothing to disclose RECOMMENDATIONS
Update on vitamin D. J Chris Gallagher Professor of Medicine and Endocrinology Creighton University Omaha,Nebraska USA
 Update on vitamin D J Chris Gallagher Professor of Medicine and Endocrinology Creighton University Omaha,Nebraska 68131 USA Cali, Colombia 2016 definitions DRIs are the recommended dietary reference intakes
Update on vitamin D J Chris Gallagher Professor of Medicine and Endocrinology Creighton University Omaha,Nebraska 68131 USA Cali, Colombia 2016 definitions DRIs are the recommended dietary reference intakes
Clinical Guidelines. Annals of Internal Medicine. Annals of Internal Medicine
 Annals of Internal Medicine Clinical Guidelines Screening for High Blood Pressure: U.S. Preventive Services Task Force Reaffirmation Recommendation Statement U.S. Preventive Services Task Force* Description:
Annals of Internal Medicine Clinical Guidelines Screening for High Blood Pressure: U.S. Preventive Services Task Force Reaffirmation Recommendation Statement U.S. Preventive Services Task Force* Description:
Effect of Vitamin D and Calcium Supplementation on Cancer Incidence in Older Women A Randomized Clinical Trial
 Research JAMA Original Investigation Effect of Vitamin D and Calcium Supplementation on Cancer Incidence in Older Women A Randomized Clinical Trial Joan Lappe, PhD, RN; Patrice Watson, PhD; Dianne Travers-Gustafson,
Research JAMA Original Investigation Effect of Vitamin D and Calcium Supplementation on Cancer Incidence in Older Women A Randomized Clinical Trial Joan Lappe, PhD, RN; Patrice Watson, PhD; Dianne Travers-Gustafson,
The Association between Vitamin D and Lung Cancer Risk in Finnish Male Smokers. Julia Burkley Briarcliff High School
 The Association between Vitamin D and Lung Cancer Risk in Finnish Male Smokers. Julia Burkley Briarcliff High School 2 Burkley Table of Contents Introduction~ Pg. 2 Methods~ Pg. 4 Ethics Statement~ Pg.
The Association between Vitamin D and Lung Cancer Risk in Finnish Male Smokers. Julia Burkley Briarcliff High School 2 Burkley Table of Contents Introduction~ Pg. 2 Methods~ Pg. 4 Ethics Statement~ Pg.
Protocol. This trial protocol has been provided by the authors to give readers additional information about their work.
 Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: Baron JA, Barry EL, Mott LA, et al. A trial of calcium and vitamin D
Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: Baron JA, Barry EL, Mott LA, et al. A trial of calcium and vitamin D
Aspirin for the Chemoprevention of Colorectal Adenomas: Meta-analysis of the Randomized Trials
 JNCI Journal of the National Cancer Institute Advance Access published February 10, 2009 ARTICLE Aspirin for the Chemoprevention of Colorectal Adenomas: Meta-analysis of the Randomized Trials Bernard F.
JNCI Journal of the National Cancer Institute Advance Access published February 10, 2009 ARTICLE Aspirin for the Chemoprevention of Colorectal Adenomas: Meta-analysis of the Randomized Trials Bernard F.
Vitamin D and Cancer Prevention
 Curr Nutr Rep (2012) 1:24 29 DOI 10.1007/s13668-011-0005-8 CANCER (MF LEITZMANN, SECTION EDITOR) Vitamin D and Cancer Prevention Hajo Zeeb Published online: 17 January 2012 # Springer Science+Business
Curr Nutr Rep (2012) 1:24 29 DOI 10.1007/s13668-011-0005-8 CANCER (MF LEITZMANN, SECTION EDITOR) Vitamin D and Cancer Prevention Hajo Zeeb Published online: 17 January 2012 # Springer Science+Business
THE TRUTH ABOUT THE VITAL STUDY ON OMEGA-3 and VITAMIN D
 THE TRUTH ABOUT THE VITAL STUDY ON OMEGA-3 and VITAMIN D There have been two recent publications regarding the findings from the VITAL study that have gotten a lot of media attention because of their conclusions
THE TRUTH ABOUT THE VITAL STUDY ON OMEGA-3 and VITAMIN D There have been two recent publications regarding the findings from the VITAL study that have gotten a lot of media attention because of their conclusions
Smoking categories. Men Former smokers. Current smokers Cigarettes smoked/d ( ) 0.9 ( )
 Table 2.44. Case-control studies on smoking and colorectal Colon Rectal Colorectal Ji et al. (2002), Shanghai, China Cases were permanent Shanghai residents newly diagnosed at ages 30-74 years between
Table 2.44. Case-control studies on smoking and colorectal Colon Rectal Colorectal Ji et al. (2002), Shanghai, China Cases were permanent Shanghai residents newly diagnosed at ages 30-74 years between
A Randomized Trial of a Multivitamin (MVM) in the Prevention of Cardiovascular Disease in Men: The Physicians Health Study (PHS) II
 A Randomized Trial of a Multivitamin (MVM) in the Prevention of Cardiovascular Disease in Men: The Physicians Health Study (PHS) II Presenter Disclosure Information Howard D. Sesso, ScD, MPH Relevant Disclosures:
A Randomized Trial of a Multivitamin (MVM) in the Prevention of Cardiovascular Disease in Men: The Physicians Health Study (PHS) II Presenter Disclosure Information Howard D. Sesso, ScD, MPH Relevant Disclosures:
CALCIUM SUPPLEMENTS FOR THE PREVENTION OF COLORECTAL ADENOMAS CALCIUM SUPPLEMENTS FOR THE PREVENTION OF COLORECTAL ADENOMAS
 SUPPLEMENTS FOR THE PREVENTION OF COLORECTAL ADENOMAS J.A. BARON, M.D., M. BEACH, M.D., PH.D., J.S. MANDEL, PH.D., R.U. VAN STOLK, M.D., R.W. HAILE, DR.P.H., R.S. SANDLER, M.D., M.P.H., R. ROTHSTEIN, M.D.,
SUPPLEMENTS FOR THE PREVENTION OF COLORECTAL ADENOMAS J.A. BARON, M.D., M. BEACH, M.D., PH.D., J.S. MANDEL, PH.D., R.U. VAN STOLK, M.D., R.W. HAILE, DR.P.H., R.S. SANDLER, M.D., M.P.H., R. ROTHSTEIN, M.D.,
The Canadian Cancer Society estimates that in
 How Do I Screen For Colorectal Cancer? By Ted M. Ross, MD, FRCS(C); and Naomi Ross, RD, BSc To be presented at the University of Toronto s Primary Care Today sessions (October 3, 2003) The Canadian Cancer
How Do I Screen For Colorectal Cancer? By Ted M. Ross, MD, FRCS(C); and Naomi Ross, RD, BSc To be presented at the University of Toronto s Primary Care Today sessions (October 3, 2003) The Canadian Cancer
Observational Studies vs. Randomized Controlled Trials
 Observational Studies vs. Randomized Controlled Trials Edward Giovannucci, MD, ScD Harvard School of Public Health Harvard Medical School Boston MA 02115 (1)The relevance of observational data as compared
Observational Studies vs. Randomized Controlled Trials Edward Giovannucci, MD, ScD Harvard School of Public Health Harvard Medical School Boston MA 02115 (1)The relevance of observational data as compared
Colonoscopy with polypectomy significantly reduces colorectal
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:562 567 Utilization and Yield of Surveillance Colonoscopy in the Continued Follow-Up Study of the Polyp Prevention Trial ADEYINKA O. LAIYEMO,*, PAUL F. PINSKY,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:562 567 Utilization and Yield of Surveillance Colonoscopy in the Continued Follow-Up Study of the Polyp Prevention Trial ADEYINKA O. LAIYEMO,*, PAUL F. PINSKY,
CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO
 OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO Amy Ferketich, PhD Ling Wang, MPH The Ohio State University College of Public Health
OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO Amy Ferketich, PhD Ling Wang, MPH The Ohio State University College of Public Health
Dietary Fatty Acids and the Risk of Hypertension in Middle-Aged and Older Women
 07/14/2010 Dietary Fatty Acids and the Risk of Hypertension in Middle-Aged and Older Women First Author: Wang Short Title: Dietary Fatty Acids and Hypertension Risk in Women Lu Wang, MD, PhD, 1 JoAnn E.
07/14/2010 Dietary Fatty Acids and the Risk of Hypertension in Middle-Aged and Older Women First Author: Wang Short Title: Dietary Fatty Acids and Hypertension Risk in Women Lu Wang, MD, PhD, 1 JoAnn E.
Nutrition and gastrointestinal cancer: An update of the epidemiological evidence
 Nutrition and gastrointestinal cancer: An update of the epidemiological evidence Krasimira Aleksandrova, PhD MPH Nutrition, Immunity and Metabolsim Start-up Lab Department of Epidemiology German Institute
Nutrition and gastrointestinal cancer: An update of the epidemiological evidence Krasimira Aleksandrova, PhD MPH Nutrition, Immunity and Metabolsim Start-up Lab Department of Epidemiology German Institute
Prevalence of Self-Reported Obesity Among U.S. Adults by State and Territory. Definitions Obesity: Body Mass Index (BMI) of 30 or higher.
 Prevalence of Self-Reported Obesity Among U.S. Adults by State and Territory Definitions Obesity: Body Mass Index (BMI) of 30 or higher. Body Mass Index (BMI): A measure of an adult s weight in relation
Prevalence of Self-Reported Obesity Among U.S. Adults by State and Territory Definitions Obesity: Body Mass Index (BMI) of 30 or higher. Body Mass Index (BMI): A measure of an adult s weight in relation
Viral hepatitis and Hepatocellular Carcinoma
 Viral hepatitis and Hepatocellular Carcinoma Hashem B. El-Serag, MD, MPH Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Houston VA & Baylor College of Medicine Houston, TX Outline
Viral hepatitis and Hepatocellular Carcinoma Hashem B. El-Serag, MD, MPH Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Houston VA & Baylor College of Medicine Houston, TX Outline
The U.S. Preventive Services Task Force (USPSTF) makes
 Annals of Internal Medicine Clinical Guideline Screening for Testicular Cancer: U.S. Preventive Services Task Force Reaffirmation Recommendation Statement U.S. Preventive Services Task Force* Description:
Annals of Internal Medicine Clinical Guideline Screening for Testicular Cancer: U.S. Preventive Services Task Force Reaffirmation Recommendation Statement U.S. Preventive Services Task Force* Description:
Prevention of cancer the influence of diet
 Prevention of cancer the influence of diet Food Network, 2010 Anne Tjønneland Institut for Epidemiologisk Kræftforskning, Kræftens Bekæmpelse Risk of cancer Indien / USA Aldersspecifik brystkræftincidens
Prevention of cancer the influence of diet Food Network, 2010 Anne Tjønneland Institut for Epidemiologisk Kræftforskning, Kræftens Bekæmpelse Risk of cancer Indien / USA Aldersspecifik brystkræftincidens
Electronic Supplementary Material
 Electronic Supplementary Material Effects of chemopreventive agents on the incidence of recurrent colorectal adenomas: A systematic review with network meta-analysis of randomized controlled trials Sajesh
Electronic Supplementary Material Effects of chemopreventive agents on the incidence of recurrent colorectal adenomas: A systematic review with network meta-analysis of randomized controlled trials Sajesh
Vitamin D for Cancer Prevention: Global Perspective. Annals of Epidemiology Volume 19, Issue 7, July 2009, Pages
 Vitamin D for Cancer Prevention: Global Perspective 1 Annals of Epidemiology Volume 19, Issue 7, July 2009, Pages 468-483 Cedric F. Garland Dr PH, Edward D. Gorham MPH, PhD, Sharif B. Mohr MPH, Frank C.
Vitamin D for Cancer Prevention: Global Perspective 1 Annals of Epidemiology Volume 19, Issue 7, July 2009, Pages 468-483 Cedric F. Garland Dr PH, Edward D. Gorham MPH, PhD, Sharif B. Mohr MPH, Frank C.
Vitamin D. Vitamin functioning as hormone. Todd A Fearer, MD FACP
 Vitamin D Vitamin functioning as hormone Todd A Fearer, MD FACP Vitamin overview Vitamins are organic compounds that are essential in small amounts for normal metabolism They are different from minerals
Vitamin D Vitamin functioning as hormone Todd A Fearer, MD FACP Vitamin overview Vitamins are organic compounds that are essential in small amounts for normal metabolism They are different from minerals
FOR CONSUMERS AND PATIENTS
 AVAILABILITY OF VITAMIN D FOR CONSUMERS AND PATIENTS Prof. Heike A. Bischoff-Ferrari, MD, DrPH Centre on Aging and Mobility, University of Zurich Dept. of Rheumatology, University Hospital Zurich Overview
AVAILABILITY OF VITAMIN D FOR CONSUMERS AND PATIENTS Prof. Heike A. Bischoff-Ferrari, MD, DrPH Centre on Aging and Mobility, University of Zurich Dept. of Rheumatology, University Hospital Zurich Overview
Improving Outcomes from Colorectal Cancer: Diet, Lifestyle, and Chemoprevention
 Improving Outcomes from Colorectal Cancer: Diet, Lifestyle, and Chemoprevention Kimmie Ng, MD, MPH Director of Clinical Research Director, GI Biobank and Biospecimen Research Gastrointestinal Cancer Center
Improving Outcomes from Colorectal Cancer: Diet, Lifestyle, and Chemoprevention Kimmie Ng, MD, MPH Director of Clinical Research Director, GI Biobank and Biospecimen Research Gastrointestinal Cancer Center
A Proposed Randomized Trial of Cocoa Flavanols and Multivitamins in the Prevention of Cardiovascular Disease and Cancer
 A Proposed Randomized Trial of Cocoa Flavanols and Multivitamins in the Prevention of Cardiovascular Disease and Cancer JoAnn E. Manson, MD, DrPH Howard D. Sesso, ScD, MPH Brigham and Women's Hospital
A Proposed Randomized Trial of Cocoa Flavanols and Multivitamins in the Prevention of Cardiovascular Disease and Cancer JoAnn E. Manson, MD, DrPH Howard D. Sesso, ScD, MPH Brigham and Women's Hospital
Original Article. Elizabeth Kos, MD 1 ; Mary Jo Liszek, MD 2 ; Mary Ann Emanuele, MD 3 ; Ramon Durazo-Arvizu, PhD 4 ; Pauline Camacho, MD, FACE 3
 Original Article Elizabeth Kos, MD 1 ; Mary Jo Liszek, MD 2 ; Mary Ann Emanuele, MD 3 ; Ramon Durazo-Arvizu, PhD 4 ; Pauline Camacho, MD, FACE 3 ABSTRACT Objective: To determine the effect of metformin
Original Article Elizabeth Kos, MD 1 ; Mary Jo Liszek, MD 2 ; Mary Ann Emanuele, MD 3 ; Ramon Durazo-Arvizu, PhD 4 ; Pauline Camacho, MD, FACE 3 ABSTRACT Objective: To determine the effect of metformin
Smoking-associated risks of conventional adenomas and serrated polyps in the colorectum
 Cancer Causes Control (2015) 26:377 386 DOI 10.1007/s10552-014-0513-0 ORIGINAL PAPER Smoking-associated risks of conventional adenomas and serrated polyps in the colorectum Jane C. Figueiredo Seth D. Crockett
Cancer Causes Control (2015) 26:377 386 DOI 10.1007/s10552-014-0513-0 ORIGINAL PAPER Smoking-associated risks of conventional adenomas and serrated polyps in the colorectum Jane C. Figueiredo Seth D. Crockett
ORIGINAL INVESTIGATION. C-Reactive Protein Concentration and Incident Hypertension in Young Adults
 ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
The COSMOS Trial. (COcoa Supplement and Multivitamins Outcomes Study) JoAnn E. Manson, MD, DrPH Howard D. Sesso, ScD, MPH
 COSMOS Trial The COSMOS Trial (COcoa Supplement and Multivitamins Outcomes Study) JoAnn E. Manson, MD, DrPH Howard D. Sesso, ScD, MPH Brigham and Women's Hospital Harvard Medical School Garnet L. Anderson,
COSMOS Trial The COSMOS Trial (COcoa Supplement and Multivitamins Outcomes Study) JoAnn E. Manson, MD, DrPH Howard D. Sesso, ScD, MPH Brigham and Women's Hospital Harvard Medical School Garnet L. Anderson,
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Bolland MJ, Grey A, Gamble GD, Reid IR. The
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Bolland MJ, Grey A, Gamble GD, Reid IR. The
Androgen deprivation therapy for treatment of localized prostate cancer and risk of
 Androgen deprivation therapy for treatment of localized prostate cancer and risk of second primary malignancies Lauren P. Wallner, Renyi Wang, Steven J. Jacobsen, Reina Haque Department of Research and
Androgen deprivation therapy for treatment of localized prostate cancer and risk of second primary malignancies Lauren P. Wallner, Renyi Wang, Steven J. Jacobsen, Reina Haque Department of Research and
Cirrhosis and Liver Cancer Mortality in the United States : An Observational Study Supplementary Material
 Cirrhosis and Liver Cancer Mortality in the United States 1999-2016: An Observational Study Supplementary Material Elliot B. Tapper MD (1,2) and Neehar D Parikh MD MS (1,2) 1. Division of Gastroenterology
Cirrhosis and Liver Cancer Mortality in the United States 1999-2016: An Observational Study Supplementary Material Elliot B. Tapper MD (1,2) and Neehar D Parikh MD MS (1,2) 1. Division of Gastroenterology
Brietta M Oaks, Kevin W Dodd, Cari L Meinhold, Li Jiao, Timothy R Church, and Rachael Z Stolzenberg-Solomon
 Folate intake, post folic acid grain fortification, and pancreatic cancer risk in the Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial 1 3 Brietta M Oaks, Kevin W Dodd, Cari L Meinhold, Li
Folate intake, post folic acid grain fortification, and pancreatic cancer risk in the Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial 1 3 Brietta M Oaks, Kevin W Dodd, Cari L Meinhold, Li
Selenium and Vitamin E Cancer Prevention Trial (SELECT): Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Selenium and Vitamin E
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Selenium and Vitamin E
The Role of Observational Studies. Edward Giovannucci, MD, ScD Departments of Nutrition and Epidemiology
 The Role of Observational Studies Edward Giovannucci, MD, ScD Departments of Nutrition and Epidemiology Disclosure Information As required, I would like to report that I have no financial relationships
The Role of Observational Studies Edward Giovannucci, MD, ScD Departments of Nutrition and Epidemiology Disclosure Information As required, I would like to report that I have no financial relationships
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 340 J ANUARY 21, 1999 NUMBER 3 DIETARY FIBER AND THE RISK OF COLORECTAL CANCER AND ADENOMA IN WOMEN CHARLES
The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 340 J ANUARY 21, 1999 NUMBER 3 DIETARY FIBER AND THE RISK OF COLORECTAL CANCER AND ADENOMA IN WOMEN CHARLES
Statin use does not prevent recurrent adenomatous polyp formation in a VA population
 Indian J Gastroenterol (2010) 29:106 111 DOI 10.1007/s12664-010-0032-1 ORIGINAL ARTICLE Statin use does not prevent recurrent adenomatous polyp formation in a VA population Nikki Parker-Ray & Jehad Barakat
Indian J Gastroenterol (2010) 29:106 111 DOI 10.1007/s12664-010-0032-1 ORIGINAL ARTICLE Statin use does not prevent recurrent adenomatous polyp formation in a VA population Nikki Parker-Ray & Jehad Barakat
Leveraging Prospective Cohort Studies to Advance Colorectal Cancer Prevention, Treatment and Biology
 Leveraging Prospective Cohort Studies to Advance Colorectal Cancer Prevention, Treatment and Biology Charles S. Fuchs, MD, MPH Director, Yale Cancer Center Physician-in-Chief, Smilow Cancer Hospital New
Leveraging Prospective Cohort Studies to Advance Colorectal Cancer Prevention, Treatment and Biology Charles S. Fuchs, MD, MPH Director, Yale Cancer Center Physician-in-Chief, Smilow Cancer Hospital New
C olorectal adenomas are reputed to be precancerous
 568 COLORECTAL CANCER Incidence and recurrence rates of colorectal adenomas estimated by annually repeated colonoscopies on asymptomatic Japanese Y Yamaji, T Mitsushima, H Ikuma, H Watabe, M Okamoto, T
568 COLORECTAL CANCER Incidence and recurrence rates of colorectal adenomas estimated by annually repeated colonoscopies on asymptomatic Japanese Y Yamaji, T Mitsushima, H Ikuma, H Watabe, M Okamoto, T
The prevalence of obesity has increased markedly in
 Brief Communication Use of Prescription Weight Loss Pills among U.S. Adults in 1996 1998 Laura Kettel Khan, PhD; Mary K. Serdula, MD; Barbara A. Bowman, PhD; and David F. Williamson, PhD Background: Pharmacotherapy
Brief Communication Use of Prescription Weight Loss Pills among U.S. Adults in 1996 1998 Laura Kettel Khan, PhD; Mary K. Serdula, MD; Barbara A. Bowman, PhD; and David F. Williamson, PhD Background: Pharmacotherapy
To estimate the population attributable cancer risk associated with excess salt and
 Appendix 1 (as supplied by the authors): Supplementary Material 1: Methods for Population Attributable Cancer Risks for Excess Salt and Insufficient Calcium and Vitamin D To estimate the population attributable
Appendix 1 (as supplied by the authors): Supplementary Material 1: Methods for Population Attributable Cancer Risks for Excess Salt and Insufficient Calcium and Vitamin D To estimate the population attributable
Nutritional concepts for the prevention and treatment of osteoporosis: what, for whom, when? Objectives
 Nutritional concepts for the prevention and treatment of osteoporosis: what, for whom, when? Bess Dawson-Hughes, MD Disclosures: Amgen, DSM, Nestle, Opko, Pfizer, Roche, Tricida Interrelationships of muscle
Nutritional concepts for the prevention and treatment of osteoporosis: what, for whom, when? Bess Dawson-Hughes, MD Disclosures: Amgen, DSM, Nestle, Opko, Pfizer, Roche, Tricida Interrelationships of muscle
Vitamin D and Inflammation
 Vitamin D and Inflammation Susan Harris, D.Sc. Jean Mayer USDA Human Nutrition Research Center on Aging at Tufts University Boston, MA Vitamin D Liver 25(OH)D storage form nmol/l=ng/ml x 2.5 Renal 1,25(OH)
Vitamin D and Inflammation Susan Harris, D.Sc. Jean Mayer USDA Human Nutrition Research Center on Aging at Tufts University Boston, MA Vitamin D Liver 25(OH)D storage form nmol/l=ng/ml x 2.5 Renal 1,25(OH)
How to Design, Conduct, and Analyze Vitamin D Clinical Trials
 How to Design, Conduct, and Analyze Vitamin D Clinical Trials William B. Grant, PhD Sunlight, Nutrition and Health Research Center wbgrant@infionline.net Disclosure I receive funding from Bio-Tech Pharmacal,
How to Design, Conduct, and Analyze Vitamin D Clinical Trials William B. Grant, PhD Sunlight, Nutrition and Health Research Center wbgrant@infionline.net Disclosure I receive funding from Bio-Tech Pharmacal,
Screening & Surveillance Guidelines
 Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
The effect of supplementation with vitamin D on recurrent ischemic events and sudden cardiac death in patients with acute coronary syndrome
 CRC IRB Proposal Matthew Champion PGY-1 8/29/12 The effect of supplementation with vitamin D on recurrent ischemic events and sudden cardiac death in patients with acute coronary syndrome Study Purpose
CRC IRB Proposal Matthew Champion PGY-1 8/29/12 The effect of supplementation with vitamin D on recurrent ischemic events and sudden cardiac death in patients with acute coronary syndrome Study Purpose
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE
 SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
Cardiovascular Risk of Celecoxib in 6 Randomized Placebo-controlled Trials: The Cross Trial Safety Analysis
 Cardiovascular Risk of Celecoxib in 6 Randomized Placebo-controlled Trials: The Cross Trial Safety Analysis Scott D. Solomon, MD, Janet Wittes, PhD, Ernest Hawk, MD, MPH for the Celecoxib Cross Trials
Cardiovascular Risk of Celecoxib in 6 Randomized Placebo-controlled Trials: The Cross Trial Safety Analysis Scott D. Solomon, MD, Janet Wittes, PhD, Ernest Hawk, MD, MPH for the Celecoxib Cross Trials
Modifying effect of calcium/magnesium intake ratio and mortality: a populationbased
 Open Access To cite: Dai Q, Shu X-O, Deng X, et al. Modifying effect of calcium/magnesium intake ratio and mortality: a population-based cohort study. BMJ Open 2013;3: e002111. doi:10.1136/ bmjopen-2012-002111
Open Access To cite: Dai Q, Shu X-O, Deng X, et al. Modifying effect of calcium/magnesium intake ratio and mortality: a population-based cohort study. BMJ Open 2013;3: e002111. doi:10.1136/ bmjopen-2012-002111
Chapter Two Incidence & prevalence
 Chapter Two Incidence & prevalence Science is the observation of things possible, whether present or past. Prescience is the knowledge of things which may come to pass, though but slowly. LEONARDO da Vinci
Chapter Two Incidence & prevalence Science is the observation of things possible, whether present or past. Prescience is the knowledge of things which may come to pass, though but slowly. LEONARDO da Vinci
The Vitamin D Gap. Vitamin D intake guidelines were established to prevent. Estimating an adequate intake of vitamin D. FEATURE VITAMIN D GAP
 The Vitamin D Gap Estimating an adequate intake of vitamin D. By Laurence Montgomery, ND and George Tardik, ND Vitamin D intake guidelines were established to prevent rickets in children and osteomalacia
The Vitamin D Gap Estimating an adequate intake of vitamin D. By Laurence Montgomery, ND and George Tardik, ND Vitamin D intake guidelines were established to prevent rickets in children and osteomalacia
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Personalized Aspirin Therapy
 Personalized Aspirin Therapy Nadir Arber, MD, MSc, MHA Head - Integrated Cancer Prevention Center Tel Aviv Medical Centre and Tel Aviv University Heidelberg 2014 CRC is Preventable Early detection Chemoprevention
Personalized Aspirin Therapy Nadir Arber, MD, MSc, MHA Head - Integrated Cancer Prevention Center Tel Aviv Medical Centre and Tel Aviv University Heidelberg 2014 CRC is Preventable Early detection Chemoprevention
Obesity Trends:
 Obesity Trends: 1985-2014 Compiled by the Centers for Disease Control and Prevention Retrieved from http://www.cdc.gov/obesity/data/prevalencemaps.html Organized into two groupings due to methodological
Obesity Trends: 1985-2014 Compiled by the Centers for Disease Control and Prevention Retrieved from http://www.cdc.gov/obesity/data/prevalencemaps.html Organized into two groupings due to methodological
Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer
 Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer David A. Lieberman, 1 Douglas K. Rex, 2 Sidney J. Winawer,
Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer David A. Lieberman, 1 Douglas K. Rex, 2 Sidney J. Winawer,
Colorectal Cancer Screening: Recommendations for Physicians and Patients from the U.S. Multi-Society Task Force on Colorectal Cancer
 Colorectal Cancer Screening: Recommendations for Physicians and Patients from the U.S. Multi-Society Task Force on Colorectal Cancer Douglas K. Rex, MD, MACG 1, C. Richard Boland, MD 2, Jason A. Dominitz,
Colorectal Cancer Screening: Recommendations for Physicians and Patients from the U.S. Multi-Society Task Force on Colorectal Cancer Douglas K. Rex, MD, MACG 1, C. Richard Boland, MD 2, Jason A. Dominitz,
Economic Analyses of Nutrient Interventions for Chronic Disease Prevention Paul M. Coates, Ph.D. Director
 Economic Analyses of Nutrient Interventions for Chronic Disease Prevention Paul M. Coates, Ph.D. Director Office of Dietary Supplements National Institutes of Health Overview What is the science telling
Economic Analyses of Nutrient Interventions for Chronic Disease Prevention Paul M. Coates, Ph.D. Director Office of Dietary Supplements National Institutes of Health Overview What is the science telling
Research Article Vitamin D Levels in Subjects with Prostate Cancer Compared to Age-Matched Controls
 Prostate Cancer Volume 2012, Article ID 524206, 4 pages doi:10.1155/2012/524206 Research Article Vitamin D Levels in Subjects with Prostate Cancer Compared to Age-Matched Controls Subhashini Yaturu, 1
Prostate Cancer Volume 2012, Article ID 524206, 4 pages doi:10.1155/2012/524206 Research Article Vitamin D Levels in Subjects with Prostate Cancer Compared to Age-Matched Controls Subhashini Yaturu, 1
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kaminski MF, Regula J, Kraszewska E, et al. Quality indicators
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kaminski MF, Regula J, Kraszewska E, et al. Quality indicators
FORTE: Five or Ten Year Colonoscopy for 1-2 Non-Advanced Adenomas
 FORTE: Five or Ten Year Colonoscopy for 1-2 Non-Advanced Adenomas CRC Screening is Increasing Up to date with recommended screening in U.S.: 54% in 2002 65% in 2010 80% goal for 2018 More people are getting
FORTE: Five or Ten Year Colonoscopy for 1-2 Non-Advanced Adenomas CRC Screening is Increasing Up to date with recommended screening in U.S.: 54% in 2002 65% in 2010 80% goal for 2018 More people are getting
Emerging Areas Relating Vitamin D to Health
 ILSI SEA Region Vit D Conference, Australia, June 2012 (www.ilsi.org/sea Region) Emerging Areas Relating Vitamin D to Health Peter R Ebeling MD FRACP NorthWest Academic Centre and Dept Endocrinology The
ILSI SEA Region Vit D Conference, Australia, June 2012 (www.ilsi.org/sea Region) Emerging Areas Relating Vitamin D to Health Peter R Ebeling MD FRACP NorthWest Academic Centre and Dept Endocrinology The
Benefits of Vitamin D for Cancer and Pregnancy/Birth Outcomes. William B. Grant, PhD Sunlight, Nutrition and Health Research Center, San Francisco
 Benefits of Vitamin D for Cancer and Pregnancy/Birth Outcomes William B. Grant, PhD Sunlight, Nutrition and Health Research Center, San Francisco Disclosure I receive funding from Bio Tech Pharmacal, Inc.
Benefits of Vitamin D for Cancer and Pregnancy/Birth Outcomes William B. Grant, PhD Sunlight, Nutrition and Health Research Center, San Francisco Disclosure I receive funding from Bio Tech Pharmacal, Inc.
Chemoprevention of colorectal cancer in individuals with previous colorectal neoplasia: systematic review and network meta-analysis
 open access Chemoprevention of colorectal cancer in individuals with previous colorectal neoplasia: systematic review and network meta-analysis Parambir S Dulai, 1 Siddharth Singh, 1,2 Evelyn Marquez,
open access Chemoprevention of colorectal cancer in individuals with previous colorectal neoplasia: systematic review and network meta-analysis Parambir S Dulai, 1 Siddharth Singh, 1,2 Evelyn Marquez,
Trends in colorectal cancer incidence in younger Canadians,
 Trends in colorectal cancer incidence in younger Canadians, 1969-2010 Prithwish De, MHSc, PhD 1,2 ; Parth Patel, MPH 2 1 Surveillance & Ontario Cancer Registry, Cancer Care Ontario 2 Dalla Lana School
Trends in colorectal cancer incidence in younger Canadians, 1969-2010 Prithwish De, MHSc, PhD 1,2 ; Parth Patel, MPH 2 1 Surveillance & Ontario Cancer Registry, Cancer Care Ontario 2 Dalla Lana School
 PATCH Analysis Plan v1.2.doc Prophylactic Antibiotics for the Treatment of Cellulitis at Home: PATCH Analysis Plan for PATCH I and PATCH II Authors: Angela Crook, Andrew Nunn, James Mason and Kim Thomas,
PATCH Analysis Plan v1.2.doc Prophylactic Antibiotics for the Treatment of Cellulitis at Home: PATCH Analysis Plan for PATCH I and PATCH II Authors: Angela Crook, Andrew Nunn, James Mason and Kim Thomas,
B&T Format. New Measures. 2 CAHPS is a registered trademark of the Agency for Healthcare Research and Quality (AHRQ).
 TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February 4, 2018 RE: 2018 Accreditation Benchmarks and Thresholds This document reports national benchmarks and
TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February 4, 2018 RE: 2018 Accreditation Benchmarks and Thresholds This document reports national benchmarks and
Five-Year Risk of Colorectal Neoplasia after Negative Screening Colonoscopy
 The new england journal of medicine original article Five-Year Risk of Colorectal Neoplasia after Negative Screening Colonoscopy Thomas F. Imperiale, M.D., Elizabeth A. Glowinski, R.N., Ching Lin-Cooper,
The new england journal of medicine original article Five-Year Risk of Colorectal Neoplasia after Negative Screening Colonoscopy Thomas F. Imperiale, M.D., Elizabeth A. Glowinski, R.N., Ching Lin-Cooper,
Susan Steck, Ph.D., M.P.H., R.D.
 Susan Steck, Ph.D., M.P.H., R.D. Associate Professor Department of Epidemiology and Biostatistics Cancer Prevention and Control Program Center for Research in Nutrition and Health Disparities Arnold School
Susan Steck, Ph.D., M.P.H., R.D. Associate Professor Department of Epidemiology and Biostatistics Cancer Prevention and Control Program Center for Research in Nutrition and Health Disparities Arnold School
Zeenat Ali, PGY3 Joseph Grisanti, MD June 7 th, 2012
 A Randomized Open Label Trial to Evaluate the Efficacy of Different Dosage Forms of Vitamin D in Patients with Vitamin D Deficiency, and the Effect of Food on Vitamin D Absorption. Zeenat Ali, PGY3 Joseph
A Randomized Open Label Trial to Evaluate the Efficacy of Different Dosage Forms of Vitamin D in Patients with Vitamin D Deficiency, and the Effect of Food on Vitamin D Absorption. Zeenat Ali, PGY3 Joseph
MEDICAL POLICY EFFECTIVE DATE: 08/21/14 REVISED DATE: 04/16/15, 06/16/16, 07/20/17 SUBJECT: SCREENING FOR VITAMIN D DEFICIENCY
 MEDICAL POLICY SUBJECT: SCREENING FOR VITAMIN D DEFICIENCY A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not
MEDICAL POLICY SUBJECT: SCREENING FOR VITAMIN D DEFICIENCY A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not
Vitamin D Deficiency. Decreases renal calcium excretion. Increases intestinal absorption Calcium. Increases bone resorption of calcium
 Vitamin D Deficiency Deborah Gordish, MD Assistant Professor of Clinical Internal Medicine Lead Physician Lewis Center Primary Care Associate Division Director General Internal Medicine The Ohio State
Vitamin D Deficiency Deborah Gordish, MD Assistant Professor of Clinical Internal Medicine Lead Physician Lewis Center Primary Care Associate Division Director General Internal Medicine The Ohio State
B&T Format. New Measures. Better health care. Better choices. Better health.
 1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: August 13,
1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: August 13,
Citation Characteristics of Research Published in Emergency Medicine Versus Other Scientific Journals
 ORIGINAL CONTRIBUTION Citation Characteristics of Research Published in Emergency Medicine Versus Other Scientific From the Division of Emergency Medicine, University of California, San Francisco, CA *
ORIGINAL CONTRIBUTION Citation Characteristics of Research Published in Emergency Medicine Versus Other Scientific From the Division of Emergency Medicine, University of California, San Francisco, CA *
Vitamin D, skin cancer and all-cause mortality
 Vitamin D, skin cancer and all-cause mortality 3rd International UV and Skin Cancer Prevention Conference - Melbourne 2015 Sara Gandini, PhD Senior staff scientist Vice-director Division of Epidemiology
Vitamin D, skin cancer and all-cause mortality 3rd International UV and Skin Cancer Prevention Conference - Melbourne 2015 Sara Gandini, PhD Senior staff scientist Vice-director Division of Epidemiology
Supplementary Figure 1. Principal components analysis of European ancestry in the African American, Native Hawaiian and Latino populations.
 Supplementary Figure. Principal components analysis of European ancestry in the African American, Native Hawaiian and Latino populations. a Eigenvector 2.5..5.5. African Americans European Americans e
Supplementary Figure. Principal components analysis of European ancestry in the African American, Native Hawaiian and Latino populations. a Eigenvector 2.5..5.5. African Americans European Americans e
Application of New Cholesterol Guidelines to a Population-Based Sample
 The new england journal of medicine original article Application of New Cholesterol to a Population-Based Sample Michael J. Pencina, Ph.D., Ann Marie Navar-Boggan, M.D., Ph.D., Ralph B. D Agostino, Sr.,
The new england journal of medicine original article Application of New Cholesterol to a Population-Based Sample Michael J. Pencina, Ph.D., Ann Marie Navar-Boggan, M.D., Ph.D., Ralph B. D Agostino, Sr.,
Application of New Cholesterol Guidelines to a Population-Based Sample
 The new england journal of medicine original article Application of New Cholesterol to a Population-Based Sample Michael J. Pencina, Ph.D., Ann Marie Navar-Boggan, M.D., Ph.D., Ralph B. D Agostino, Sr.,
The new england journal of medicine original article Application of New Cholesterol to a Population-Based Sample Michael J. Pencina, Ph.D., Ann Marie Navar-Boggan, M.D., Ph.D., Ralph B. D Agostino, Sr.,
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines
 Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
No effect of exercise on insulin-like growth factor (IGF)-1, insulin and glucose in young women participating in a 16-week randomized controlled trial
 University of North Florida UNF Digital Commons Nutrition and Dietetics Faculty Publications Department of Nutrition and Dietetics 11-2010 No effect of exercise on insulin-like growth factor (IGF)-1, insulin
University of North Florida UNF Digital Commons Nutrition and Dietetics Faculty Publications Department of Nutrition and Dietetics 11-2010 No effect of exercise on insulin-like growth factor (IGF)-1, insulin
B&T Format. New Measures. Better health care. Better choices. Better health.
 1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February
1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February
Subgroup Analysis of the MARINA Study of Ranibizumab in Neovascular Age-Related Macular Degeneration
 Subgroup Analysis of the MARINA Study of in Neovascular Age-Related Macular Degeneration David S. Boyer, MD, 1 Andrew N. Antoszyk, MD, 2 Carl C. Awh, MD, 3 Robert B. Bhisitkul, MD, PhD, 4 Howard Shapiro,
Subgroup Analysis of the MARINA Study of in Neovascular Age-Related Macular Degeneration David S. Boyer, MD, 1 Andrew N. Antoszyk, MD, 2 Carl C. Awh, MD, 3 Robert B. Bhisitkul, MD, PhD, 4 Howard Shapiro,
The epidemiology of vitamin D and colorectal cancer: recent findings Edward Giovannucci a,b,c
 The epidemiology of vitamin D and colorectal cancer: recent findings Edward Giovannucci a,b,c Purpose of review To highlight the human studies published over the past year examining the influence of vitamin
The epidemiology of vitamin D and colorectal cancer: recent findings Edward Giovannucci a,b,c Purpose of review To highlight the human studies published over the past year examining the influence of vitamin
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Weintraub WS, Grau-Sepulveda MV, Weiss JM, et al. Comparative
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Weintraub WS, Grau-Sepulveda MV, Weiss JM, et al. Comparative
The U.S. Preventive Services Task Force (USPSTF) makes
 Annals of Internal Medicine Clinical Guideline Vitamin D and Calcium Supplementation to Prevent Fractures in Adults: U.S. Preventive Services Task Force Recommendation Statement Virginia A. Moyer, MD,
Annals of Internal Medicine Clinical Guideline Vitamin D and Calcium Supplementation to Prevent Fractures in Adults: U.S. Preventive Services Task Force Recommendation Statement Virginia A. Moyer, MD,
V t i amin i n D a nd n d Calc l iu i m u : Rol o e l in i n Pr P eve v nt n io i n and n d Tr T eatment n of o Fr F actur u es and n d Fa F ll l s
 Vitamin D and Calcium: Role in Prevention and Treatment of Fractures and Falls Osteoporosis 21: New Insights In Research, Diagnosis, and Clinical Care Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic
Vitamin D and Calcium: Role in Prevention and Treatment of Fractures and Falls Osteoporosis 21: New Insights In Research, Diagnosis, and Clinical Care Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic
