dominated scientific discourse, they may have equivalent clinical long term results and can therefore be considered as a solid treatment
|
|
|
- Nicholas Warner
- 5 years ago
- Views:
Transcription
1 Cronicon OPEN ACCESS ORTHOPAEDICS Research Article Does it have to be done Arthroscopically? Comparison between Open and Arthroscopic Anterior Cruciate Ligament Replacement Using a Bone-Tendon-Bone Autograft A Prospective 5 Year Follow-Up Study Sebastian Gottfried Walter*, Tom Sascha Thomas, Luca Tafuro, Wolfram Thomas Department for Orthopedic Surgery, Arthro-Surgery-Group, Rome, Italy *Corresponding Author: Sebastian Gottfried Walter, Department for Orthopedic Surgery, Arthro-Surgery-Group, Rome, Italy. Received Date: January 25, 2016; Published Date: February 09, 2016 Abstract Purpose: To investigate the outcomes of an open and an arthroscopic technique for the reconstruction of the Anterior Cruciate Ligament (ACL). Methods: This prospective randomized controlled trial includes 126 patients. 65 were assigned to an open ACL replacement and 61 to an arthroscopic ACL replacement, always using Bone-patellar tendon-bone (BPTB) autografts. Outcome assessment included rerupture findings, International Knee Documentation Committee (IKDC) and Lysholm-Tegner scores, KT-1000 arthrometer measurements, Lachman, single-leg hop- and pivot-shift tests as well as range of motion (ROM) control. Results: In the time between April 2008 and May2010 we prospectively evaluated 62 patients using this open approach and 49 patients using an arthroscopic technique. Patients of the open group improved the IKDC score for 46.3 points comparing preoperative values with the 5 year follow-up. After 3 years and more there is no statistical difference between both groups when comparing IKDC score and Lysholm score. In addition, Ligament laxity demonstrated to be almost equal over the complete follow-up period. Conclusion: Although minimal invasive open techniques seem to be widely buried in oblivion and unfashionable in an arthroscopic dominated scientific discourse, they may have equivalent clinical long term results and can therefore be considered as a solid treatment option. Keywords: Anterior Cruciate Ligament Reconstruction; ACL; Bone-tendon-Bone; Autograft; Mini Open Level of evidence: I Introduction Ruptured anterior Cruciate ligaments (ACL) are among the most common diagnoses of the knee joint -especially in young patients [1]. Therefore, a broad spectrum of techniques describing adequate treatment options and procedures has been published. [2-12]. However, there is controversy which technique offers the best outcome in terms of functionality and stability as each of them promises advantages and is associated with certain pitfalls. [12-18] Formerly ACL reconstructions were carried out with open techniques [19] but eventually replaced completely by arthroscopic techniques. Based on our clinical experience and data [20, 21] from the time when arthroscopic techniques were finding their way into standard ACL replacement we believed the mini-open technique to be still a comparable treatment alternative. Thus we hypothesized that there would be no difference in clinical outcome between ACL reconstructions performed under arthroscopic visualization or direct, open visualization.
2 Material and Methods From 2008 to patients with ACL rupture underwent reconstruction with either an open or an arthroscopic method of BPTB-graft insertion. Patients were eligible to participate in the study if 1. They were older than 18 years, 2. Had an established diagnosis based on clinical or radiological features, 3. Declared consent to participate on regular follow-up appointments, and 4. Had no history of neuromuscular or systemic disease. Patients were excluded if a. They had bilateral ACL injuries, b. Multi-ligament injuries, c. Articular cartilage lesions greater than Outerbridge II and d. Previous articular injury to, or surgery on, the affected or contralateral knee. Over a period of 2years, 74 subjects were treated with a minimal invasive open approach using BPTB-autografts and 79 subjects were treated arthroscopically receiving BPTB grafts as well. All interventions were done by one senior surgeon who is experienced in both techniques or under his direct supervision. Prior to the start of the study subjects were randomized by a randomization program. All patients were assessed two experienced, independent and blinded examiners before surgery, as well as 6 weeks, 3, 6, 12, 24, 36 and 60 months after the intervention. Examiners were blinded as they had no access to the randomization list and the operation protocols. Furthermore, the scars on the operated knee were covered with band aids by a nurse previous to the examination in a way that a distinction between open and arthroscopic treatment was not possible and testings could be done without limitations. Demographical data, time interval between the initial injury and the surgical treatment as well as the Tegner scale scores were calculated using median (range) values. Measurements with the KT-1000 (MEDmetric Corp., San Diego, CA, USA), IKDC and Lysholm score evaluated using mean (standard deviation) values. For the KT-1000 measurements, an anteroposterior load of 30 pounds was applied on the knee positioned in 25 of flexion. Subjects were evaluated on the Lachmann test and Pivot- shift test. Four categories were defined for the Lachmann test: 0: mm, 1+: mm, 2+: mm and 3+: >10.0 mm. The same was done for the Pivot-shift test, defining 0: equal, 1+: glide, 2+: clunk and for 3+: gross. As a measurement for the primary outcome the IKDC score was used. Postoperatively extension respective flexion deficits were recorded (Table 2) as well as the single leg hop test (Table 3). Furthermore, a Visual Analogue Scale (VAS) was used to determine the postoperative pain. 234 Open Group Arthroscopic Group p-value Age (years, range) 37 (18;62) 35 (18;59) n.s. Male/Female 32/30 25/24 Right/Left 36/26 30/19 Time from Injury to surgery (months, range) 4 (0,2;17) 3 (0,5; 12) n.s. Cartilagedamage n (%) 20 (32) 19 (39) n.s. Meniscuslesion n (%) 32 (52) 22 (45) n.s. Tegnerpre 5 (3;7) 5 (3;7) n.s Tegner 6 weeks 3 (2;3) 3 (2;3) Tegner 3 months 3 (2;4) 3 (2;4) Tegner 6 months 4 (2;5) 4 (2;5)
3 235 Tegner 12 months 4 (3;7) 4 (3;7) Tegner 24 months 5 (4;7) 5 (3;8) Tegner 36 months 5 (3;7) 5 (3;7) Tegner 60 months 5 (3;7) 5 (3;7) Lysholmpre 47.7 (±7.3) 46.0 (±7.3) n.s. Lysholm 6 weeks 66.3 (±3.6) 63.6 (±4.8) Lysholm 3 months 73.0 (±4.1) 69.7 (±5.1) Lysholm 6 months 83.4 (±4.7) 84.2 (±6.2) Lysholm 12 months 88.7 (±4.3) 89.1 (±3.7) Lysholm 24 months 89.4 (±3.7) 87.4 (±5.4) Lysholm 36 months 89.0 (±4.1) 87.8 (±5.7) Lysholm 60 months 89.0 (±4.4) 86.9 (±6.5) IKDC pre 42.7 (±5.1) 44.7 (±7.0) n.s IKDC 6 weeks 66.0 (±3.1) 64.9 (±4.5) IKDC 3months 73.8 (±3.1) 73.2 (±3.6) IKDC 6 months 82.6 (±3.9) 81.7 (±4.3) IKDC 12 months 87.1 (±3.6) 86.6 (±3.8) IKDC 24 months 89.2 (±3.9) 88.3 (±4.1) IKDC 36 months 89.8 (±3.8) 88.5 (±4.1) IKDC 60 months 89.9 (±4.0) 88.6 (± 4.2) KT-1000 pre 6.2 (±2.3) 6.6 (±2.8) n.s KT months 1.2 (±0.2) 1.0 (±0.5) KT months 1.4 (±0.2) 1.5 (±0.5) KT months 1.4 (±0.1) 1.3 (± 0.7) Table 1: Demographic data of Open and Arthroscopic Group. Values for age, time to intervention and Tegner score are given as the median (range in parentheses). Values for IKDC, Lysholm and KT-1000 are presented as average with standard deviation. p-values resulted from a two sided t-test for comparison with the intervention group. n.s.= non significant Measurement accuracy was set at 0.1 mm, 0.1 point and 1. For statistical analyses SPSS 22.0 (IBM Corporation, New York, USA) was used. Differences between the groups were compared using the independent two sample t test for continuous variables and the Chi-square test for categorical variables. All statistical assessments were two- sided and a p value of < 0.05 was considered as statistically significant. Based on pivot- shift measures a post-hoc power analysis was done. Defining the power as 0.80 and expecting positive pivot-shift rates in 36% [22] it was found that 49 patients would have been required in each group. This study was approved by the ethics committee. All procedures were approved by the institutional review board, and informed consent was obtained from all individual participants prior to inclusion into the study.
4 236 Table 2: Presented is the development of Lachmann and Pivot-shift test over time for both groups. Also average values for extension and flexion deficits are shown. Open Group Arthr. Group p-value Grade A Grade B Grade C Grade A Grade B Grade C Single leg hop test n (%) n.s. 6 months 51 (82) 7 (12) 4 (6) 37 (76) 5 (10) 7 (14) 12 months 59 (95) 3 (5) 0 (0) 43 (88) 5 (10) 1 (2) 24 months 58 (94) 4 (6) 0 (0) 44 (90) 5 (10) 0 (0) 36 months 59 (97) 2 (3) 0 (0) 45 (92) 4 (8) 0 (0) 60 months 59 (97) 2 (3) 0 (0) 46 (94) 3 (6) 0 (0) Table 3: Shown are the results of the single leg hop test for Open and Arthroscopic Surgery. Three possible levels are indicated: Grade A:> 90 %of the distance jumped on the contralateral (uninvolved) limb; Grade B: 75-90% and Grade C:< 75%. Postoperative Pain 1 st day 3 months 6 months Open Group 3.7 ± ± ± 1.1 Arthroscopic Group 3.0 ± ± ± 1.5 p- Value n.s n.s. Table 4: Postoperative Pain Scores on a VAS scale from Pain scores were evaluated on the first post-operative day as well as 3 months and 6 months after the intervention. After 3 months pain scores are significantly higher for the open group. Surgical approach The patients underwent either general inhalational or spinal block anaesthesia and were then brought into a supine position thus allowing the knee to be moved passively over the whole Range of Motion (ROM). The ACL deprived knee joint is primarily examined arthroscopically to detect -and if necessary treat- concomitant injuries such as Meniscus lesions or cartilage defects [23]. While meniscal
5 lesions were treated with partial menisectomy, cartilage defects were treated either with abrasion or matrix-induced autologous chondrocyte implantation (MACI). However, this was done only if there were radiologic or clinical signs suspicious for such damages. 237 A midline incision of the skin reaching from the center of the patella to the tibial tubercle was made thus presenting the patellar ligament beneath [17] Before resecting the BTB graft, one hole (0.8 mm) is drilled into each osseous part to be harvested. Thereafter the graft is harvested having a diameter of 8-10 mm, consisting of a mm long osseous block of the distal patella, the patellar ligament and a 20 mm long block of the tibial tubercle. While the later is a mobilized using chisel the patellar part of the graft is sawed with a bone cutter. Before removing the BPTB-graft, it is attached proximally and distally to a guiding thread. It is then completely dissected and shaped by an assisting surgeon. Meanwhile the surgeon mobilizes the Hoffa fat body ventrally, leaving it attached as much as possible. An insertion guide is placed onto the tibial footprint of the ACL, and then the correct angle of the jig under simulation of the full ROM is determined assuring that there is no impingement. Eventually this position is fixed by inserting a K wire through the appropriately inclined tibia into the femur. According to the diameter of the BPTB-graft, the insertion tunnel is drilled using the K wire as guide. On the femur the tunnel depth is limited to mm in order to guarantee an optimal fit of the graft. At this point, another insertion guide (DePuyMitek Inc., Raynham, MA, USA) is adjusted in order to prepare the insertion channels for the Rigidfix Pins (DePuyMitek Inc., Raynham, MA, USA) in the femur. The BPTB-graft is now inserted from distal and pulled into its final position. ROM is now tested for the second time. The femoral part of the BPTB-graft is then mounted by placing parallelly two 2.7 mm RIGIDfix Crosspins from lateral into the osseous part using a femoral insertion guide. To fix the tibial part of the graft an ABSOLUTE interference screw (DePuy Mitek Inc., Raynham, MA, USA) is inserted from distal. The joint is now again controlled for a complete ROM. The Hoffa fat body is then restored in its original position. The wound is closed in layers starting with the split patellar ligament followed by the closure of the skin. The other two entry spots for placing the BPTB-graft are closed with single stitch sutures. Finally, sutures and joint are covered by sterile wound dressing. The arthroscopic control group was treated with the same technique. However, after harvesting the BPTB autograft, the patellar tendon was closed and all further steps made arthroscopically. [24] Postoperative treatment After the operation, the knee joint is mobilized on a continuous passive motion machine and is provided a cryocuff. A knee joint brace with limited flexion of 60 is applied for 4 weeks. Sutures are removed after 10 days. After 4 weeks the patients are encouraged to gain a full active range of motion primarily which is accompanied by a physiotherapeutic progression to strengthening program by focusing on isometric quadriceps reinforcement. Stationary bike, proprioception exercises are important parts of this concept that are expanded to jogging, swimming in straight line and bicycling after 3 months. After 6 months pivot sports such as ski, tennis and squash are allowed if the criteria of full range of motion, no effusion, normal muscle strength and knee stability are met. Contact sports are supposed to be omitted until the eighth month. Results In the time between 04/2008 and 05 /2010, we operated 74subjects using the described open approach. Of these 65 were included into the study and 62 of those were included in the final analysis, with30 of them being female and 32 male. 1 subject was lost to followup as he moved out of country. We operated 36 right and 26 left knee joints. The median age of the patients at the time of operation was 37(18;62) years. Subjects were operated in the median after 4 (0.2;17) months after the initial event. The mean duration of this type of surgery was 43 min (37-65 min). As a control we used data of 49 patients that were treated arthroscopically (Table 1). In this group 7 subjects were lost to follow-up as 3 of them moved out of country, 1 died, 1 was subject to imprisonment and 2 declined to participate on further regular visitations. Demographic data of this group did not show statistical significant differences compared to the open group as the median age was 35 (18; 59). In this group 25 male and 24 female subjects were treated, 30 on the right and 19 on the left side. With a mean of 69 min (55-78 min) the arthroscopic procedure took longer than the open technique. In all cases, rehabilitation went without infections. 2 subjects of the open group (3%) and 5 of the arthroscopic group (10%) needed a revision. In each, the open group as well in as in the
6 arthroscopic group there was one case of patella fracture in the early postoperative phase detected. The other case to be revised in the open group (11 months) and another three cases in the arthroscopic group (after 6, 10 and 16 months)had to undergo revision due to traumatic damages of the ACL caused by sportive activities. In one arthroscopically treated case, the BTB graft loosened after 6 weeks as the interference screw was not placed appropriately. 238 The preoperative Tegner Score Value described the status before the event that lead to the ACL rupture. After 12 months, patients became an MRI for radiologic proof of intactness of the ACL. There we found no evidence for a secondary loosening or anew lesion. The development of the Lysholm score and the IKDC score values are shown in Table 1. Subjects treated with the open technique stated a median Tegner score of 5 (3;7) before tearing their ACl. 6 weeks after surgery it was 3 (2;3), slightly improving its range to 2-4 after 3 months. After 6 months Tegner score was found at 4 (2;7); p = 0.04 and after 12 months at 5 (3; 8); p = This level was maintained also after 24 months (3;8), 36 months (3;7) and after 60 months (3; 7). The anteroposterior tibial translation was measured with the KT arthrometer by exerting 135 N. The preoperative anteroposterior tibial translation was 6.2 (± 2.3), which significantly decreased after 12 months to 1.2 (± 0.2), p = and to eventually increased slightly to 1.4 (± 0.1) after 36 months. Similar results were found in the arthroscopically treated group, too. There the mean preoperative anteroposterior tibial translation was 6.6 (± 2.8) and 1.0 (± 0.5) after 12 months. After 36 months the tibial translation was 1.5 (± 0.3). Furthermore subjects were clinically evaluated using the Pivot-shift test and Lachmann test with between group differences but tremendous improvements in the postoperative phase (Table 2). In all operated knees, postoperative extension deficits remained under 5 and flexion deficits under 10, thus achieving a normal ROM. The results of the single leg hop test did not show any significant difference, too. (Table 3) Figure 1: Participant flowchart. One patient in the Open Group and seven patients in the Arthroscopic Group were lost to follow-up. Among these patients, four (Arthroscopic group) relocated and lost contact. In another 4 cases patients were satisfied with their outcomes and declined to continue to participate in follow-up. Seven patients experienced re-ruptures. Five of these were caused by injury during sports. One injury (Arthroscopic Group) occurred 50 months after reconstruction and the other one (Open Group) happened 4 months after the intervention.
7 239 Figure 2: Development of the IKDC-Score values in the open as well as in the intervention group plotted over time. Lines joining the boxes represent the mean values for each group. The boxes represent the data distribution between 25 % and 75 % of the sample; whiskers represent between 5 % and 95 % of the sample. For illustration purposes the data for the open group were slightly shifted to the right. Discussion After harvesting the BPTB-autograft the only anatomical structure hindering the surgeon from gaining a direct access to the damaged ACL is the Hoffa Body. Thus, a mobilization of that structure seems to be a logic consequence. This principle provides the sight and space necessary to place the ACL functionally and anatomically correctly. The exact placement of the BTB-transplant is essential for satisfying functional outcomes and long term biomechanical stability. [25] Although arthroscopic methods can deliver just as good results in terms of Graft-Placement, the process may be exhausting due to an awkward handling of arthroscopic devices and imprecise judgment of the ACL movement during ROM control. Soft tissues -apart from the Hoffa body- are not more manipulated than in arthroscopic procedures. Although this is discussed controversially [26-28], were commend a refilling of the osseous defects on patella and tibia with cancellous bone and the use of Mitek pins for the femoral fixation. Yet, a further development of this technique might consider the possibility of inserting the BTB-graft through the joint window respective trans-ligamentary approach instead of pulling it through the working tunnel, that way creating an all-inside solution. We made the experience that especially physical active patients profited from the intervention as they returned to demanding sportive activities no later than one year after the intervention in a manner as they used to exercise this activity previously to the trauma. When comparing the non-arthroscopic group with the arthroscopic control group one will note outcomes that are largely congruent. In terms of functional long-term results there seems to be no difference (Table 1). Interestingly almost 18 years ago Gerich., et al. [21] concluded both arthroscopic and open procedure to have similar clinical outcomes although they used different methods and other operation techniques. Sadoghi., et al. [29] compared the Bone-Tendon-Bone autografts with doubled hamstrings and found similar functional results for the BPTB group as presented in this study, also they used cross pin fixation for the femoral part and an interference screw on the tibia. However, follow-up was 2 years only. Harilainen., et al. [30] stated slightly better results for the Lysholm score after 5 years (95%), but a greater laxity in terms of anteroposterior tibial translation (1. 5 ± 3. 0). Although the subject number was similar, fixation technique differed by using an interference screw for the femoral part as well. Another study done by Zaffagnini., et al. [22] showed somewhat lower results for the mean IKDC (82%) after 5 years. In contrast
8 240 to our study the preoperative median Tegner score was higher -which could be explained by less heterogeneity of the presented cohort. With regard to larger systematic review data of arthroscopic techniques the functional long term results of the open technique presented in this study seem to be comparable and similar with those of arthroscopic methods for the BTB replacement. [31] However this needs to be backed up by further research. Duffee., et al. [32] found a relatively high proportion of revisions necessary when drilling the femoral tunnel transtibially. This was explained by the diverse angel of the graft inside the femoral tunnel in relation to its orientation inside the joint and an increased likeliness of an impingement. In contrast other data suggest that this is cannot be the only argument as similar clinical outcomes were found when comparing the anteromedial transportal and modified transtibial technique. [33] A lower rate of revision in this study could be caused by the intraoperative ROM testing for graft impingement previously to the drilling. As in the open group the mean intervention time was shorter and the fact that cost-intensive arthroscopic operation devices were not necessarily requireda study investigating whether the open method is more cost efficient compared to arthroscopic methods would be an attractive field for near future research. Shortcomings of this study are the smaller number of subjects of the arthroscopically treated control group. Although the same postoperative rehabilitation protocol was prescribed to all patients, the quality and consistency of rehabilitation may have varied without strict supervision. Incomplete follow-up radiographic material may limit the ability of this study to draw important conclusions. There were no significant differences observed in the preoperative parameters but difficult to control clinical and individual factors may have had an important impact. Yet the number of patients included in the open-technique-group may be sufficient for this study but needs to be enlarged in further studies to increase validity. Strength of this study is the presentation of recently open/ non-arthroscopically treated subjects with a meaningful follow-up time of 5 years. Conclusion Although this technique seems to be widely buried in oblivion and unfashionable in an arthroscopic dominated scientific discourse, it has demonstrated satisfying clinical results that bear a comparison with arthroscopic techniques and therefore a consideration as one solid alternative to other established techniques is recommended. Bibliography 1. Griffin LY., et al. Understanding and preventing noncontact anterior cruciate ligament injuries: a review of the Hunt Valley II meeting, January The American journal of sports medicine 34.9 (2006): Guglielmetti L., et al. Anterior cruciate ligament reconstruction: a new cortical suspension device for femoral fixation with transtibial and transportal techniques. Journal of orthopaedic surgery and research 9 (2014) Jones KG. Reconstruction of the Anterior Cruciate Ligament. A Technique Using the Central One-Third of the Patellar Ligament. The Journal of bone and joint surgery. American volume 45 (1963): Kartus J., et al. Donor-site morbidity and anterior knee problems after anterior cruciate ligament reconstruction using autografts. Arthroscopy : the journal of arthroscopic & related surgery : official publication of the Arthroscopy Association of North America and the International Arthroscopy Association 17.9 (2001): Lee RJ and Ganley TJ. The 5-strand hamstring graft in anterior cruciate ligament reconstruction. Arthroscopy techniques 3.5 (2014): e627-e Sarzaeem MM., et al. ACL reconstruction using bone-patella tendon-bone autograft: press-fit technique vs. interference screw fixation. Archives of orthopaedic and trauma surgery (2014): Hirzinger C., et al. ACL injuries and stem cell therapy. Archives of orthopaedic and trauma surgery (2014): Mahalingam VD., et al. Fresh Versus Frozen Engineered Bone-Ligament-Bone Grafts for Sheep Anterior Cruciate Ligament Repair. Tissue engineering. Part C, Methods 21.6 (2014):
9 9. Proffen BL., et al. Bio-Enhanced Repair of the Anterior Cruciate Ligament. Arthroscopy : the journal of arthroscopic & related surgery : official publication of the Arthroscopy Association of North America and the International Arthroscopy Association 31.5 (2015): Lenschow S., et al. Comparison of outside-in and inside-out technique for tibial fixation of a soft-tissue graft in ACL reconstruction using the Shim technique. Archives of orthopaedic and trauma surgery (2014): Dawson AG., et al. Is Anterior Cruciate Reconstruction Superior to Conservative Treatment? The journal of knee surgery 29.1 (2014): Shelbourne KD., et al. Anterior Cruciate Ligament Reconstruction With Contralateral Autogenous Patellar Tendon Graft: Evaluation of Donor Site Strength and Subjective Results. The American journal of sports medicine 43.3 (2014): Xie X., et al. A meta-analysis of bone-patellar tendon-bone autograft versus four-strand hamstring tendon autograft for anterior cruciate ligament reconstruction. The Knee 22.2 (2014): Sohn OJ., et al. Comparison of the Modified Transtibial Technique, Anteromedial Portal Technique and Outside-in Technique in ACL Reconstruction. Knee surgery & related research 26.4 (2014): Slone HS., et al. Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: A Comprehensive Review of Current Literature and Systematic Review of Clinical Results. Arthroscopy : the journal of arthroscopic & related surgery : official publication of the Arthroscopy Association of North America and the International Arthroscopy Association 31.3 (2014): Andernord D., et al. Patient Predictors of Early Revision Surgery After Anterior Cruciate Ligament Reconstruction: A Cohort Study of 16,930 Patients With 2-Year Follow-up. The American journal of sports medicine 43.1 (2015): Kartus J., et al. Comparison of traditional and subcutaneous patellar tendon harvest. A prospective study of donor site-related problems after anterior cruciate ligament reconstruction using different graft harvesting techniques. The American journal of sports medicine 28.3 (2000): Group M. Effect of graft choice on the outcome of revision anterior cruciate ligament reconstruction in the Multicenter ACL Revision Study (MARS) Cohort. The American journal of sports medicine (2014): Fergusson CM. Anterior cruciate ligament reconstruction: middle-third bone/patella tendon/bone autograft. Journal of the Royal College of Surgeons of Edinburgh (2000): Gerich TG., et al. [Endoscopic versus limited open technique for replacement of the anterior cruciate ligament. 4 years outcome of a prospective study]. Unfallchirurg (1998): Gerich TG., et al. One- versus two-incision technique for anterior cruciate ligament reconstruction with patellar tendon graft. Results on early rehabilitation and stability. Knee surgery, sports traumatology, arthroscopy : official journal of the ESSKA 5.4 (1997): Zaffagnini S., et al. Prospective and randomized evaluation of ACL reconstruction with three techniques: a clinical and radiographic evaluation at 5 years follow-up. Knee surgery, sports traumatology, arthroscopy : official journal of the ESSKA (2006): Cox CL., et al. Are articular cartilage lesions and meniscus tears predictive of IKDC, KOOS, and Marx activity level outcomes after anterior cruciate ligament reconstruction? A 6-year multicenter cohort study. The American journal of sports medicine 42.5 (2014): Guo L., et al. Anterior cruciate ligament reconstruction with bone-patellar tendon-bone graft: comparison of autograft, freshfrozen allograft, and gamma-irradiated allograft. Arthroscopy : the journal of arthroscopic & related surgery : official publication of the Arthroscopy Association of North America and the International Arthroscopy Association 28.2 (2012): Biggs A., et al. Rehabilitation for Patients Following ACL Reconstruction: A Knee Symmetry Model. North American journal of sports physical therapy : NAJSPT 4.1 (2009): DuMontier TA., et al. Patella fracture after anterior cruciate ligament reconstruction with the patellar tendon: a comparison between different shaped bone block excisions. The american journal of knee surgery 14.1 (2001):
10 27. Frank RM., et al. Closure of patellar tendon defect in anterior cruciate ligament reconstruction with bone-patellar tendon-bone autograft: systematic review of randomized controlled trials. Arthroscopy : the journal of arthroscopic & related surgery : official publication of the Arthroscopy Association of North America and the International Arthroscopy Association 31.2 (2015): Jones KJ., et al. Quantitative assessment of patellar vascularity following bone-patellar tendon-bone autograft harvest for ACL reconstruction. Knee surgery, sports traumatology, arthroscopy : official journal of the ESSKA Sadoghi P., et al. Reconstruction of the anterior cruciate ligament: a clinical comparison of bone-patellar tendon-bone single bundle versus semitendinosus and gracilis double bundle technique. International orthopaedics 35.1 (2011): Harilainen A., et al. Randomized prospective study of ACL reconstruction with interference screw fixation in patellar tendon autografts versus femoral metal plate suspension and tibial post fixation in hamstring tendon autografts: 5-year clinical and radiological follow-up results. Knee surgery, sports traumatology, arthroscopy : official journal of the ESSKA 14.6 (2006): Xie X., et al. A meta-analysis of bone-patellar tendon-bone autograft versus four-strand hamstring tendon autograft for anterior cruciate ligament reconstruction. The Knee 22.2 (2015): Duffee A., et al. Transtibial ACL femoral tunnel preparation increases odds of repeat ipsilateral knee surgery. The Journal of bone and joint surgery. American volume (2013): Lee JK., et al. Anatomic single-bundle ACL reconstruction is possible with use of the modified transtibial technique: a comparison with the anteromedial transportal technique. The Journal of bone and joint surgery. American volume 96.8 (2014): Volume 3 Issue 1 February 2016 All rights are reserved by Sebastian Gottfried Walter., et al.
OMICS - 3rd Int. Conference & 2
 KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
Human ACL reconstruction
 Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear Search Terms
 Moksnes eappendix Page 1 of 15 TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear ch Search Terms No. of Studies #1 Anterior cruciate ligament [MeSH] 7768 #2 Child [MeSH] 1,371,559
Moksnes eappendix Page 1 of 15 TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear ch Search Terms No. of Studies #1 Anterior cruciate ligament [MeSH] 7768 #2 Child [MeSH] 1,371,559
Anterior Cruciate Ligament Surgery
 Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact)
 STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Torn ACL - Anatomic Footprint ACL Reconstruction
 Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System
 Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Cronicon ORTHOPAEDICS
 Cronicon OPEN ACCESS ORTHOPAEDICS Research Article Evaluation of Arthroscopic posterior Cruciate ligament reconstruction by using Quadrable hamstring tendon autograft and endobutton fixation: minimal 2
Cronicon OPEN ACCESS ORTHOPAEDICS Research Article Evaluation of Arthroscopic posterior Cruciate ligament reconstruction by using Quadrable hamstring tendon autograft and endobutton fixation: minimal 2
INDIVIDUALISED, ANATOMIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 ACL RECONSTRUCTION INDIVIDUALISED, ANATOMIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Written by Thierry Pauyo, Marcio Bottene Villa Albers and Freddie H. Fu, USA Anterior cruciate ligament (ACL) reconstruction
ACL RECONSTRUCTION INDIVIDUALISED, ANATOMIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Written by Thierry Pauyo, Marcio Bottene Villa Albers and Freddie H. Fu, USA Anterior cruciate ligament (ACL) reconstruction
Current Concepts for ACL Reconstruction
 Current Concepts for ACL Reconstruction David R. McAllister, MD Associate Team Physician UCLA Athletic Department Chief, Sports Medicine Service Professor Department of Orthopaedic Surgery David Geffen
Current Concepts for ACL Reconstruction David R. McAllister, MD Associate Team Physician UCLA Athletic Department Chief, Sports Medicine Service Professor Department of Orthopaedic Surgery David Geffen
ACL Rehabilitation and Return To Play
 ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
3/13/2018. Common Options. ACL Graft Selection in When my Cojones Are On the Line - What I Do in ACL Reconstruction
 ACL Graft Selection in 2018 James P Bradley, MD Clinical Professor UPMC Head Team Physician Pittsburgh Steelers Consultant Miami Marlins Michael S Nickoli, MD University of Pittsburgh Sports Fellow When
ACL Graft Selection in 2018 James P Bradley, MD Clinical Professor UPMC Head Team Physician Pittsburgh Steelers Consultant Miami Marlins Michael S Nickoli, MD University of Pittsburgh Sports Fellow When
Mædica - a Journal of Clinical Medicine
 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS The Advantage of Arthroscopic Anterior Cruciate Ligament Reconstruction with Autograft from the Tendons of the Semitendinosus Gracilis Muscles for
Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS The Advantage of Arthroscopic Anterior Cruciate Ligament Reconstruction with Autograft from the Tendons of the Semitendinosus Gracilis Muscles for
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Bone patellar tendon bone autograft versus LARS artificial ligament for anterior cruciate ligament reconstruction
 Eur J Orthop Surg Traumatol (2013) 23:819 823 DOI 10.1007/s00590-012-1073-1 ORIGINAL ARTICLE Bone patellar tendon bone autograft versus LARS artificial ligament for anterior cruciate ligament reconstruction
Eur J Orthop Surg Traumatol (2013) 23:819 823 DOI 10.1007/s00590-012-1073-1 ORIGINAL ARTICLE Bone patellar tendon bone autograft versus LARS artificial ligament for anterior cruciate ligament reconstruction
ACL repair in proximal lesions Vs. ACL reconstruction
 ACL repair in proximal lesions Vs. ACL reconstruction G.L. Canata, V. Casale Centre of Sports Traumatology, Koelliker Hospital, Torino Institute of Sports Medicine, Torino, Italy Gian Luigi Canata, MD
ACL repair in proximal lesions Vs. ACL reconstruction G.L. Canata, V. Casale Centre of Sports Traumatology, Koelliker Hospital, Torino Institute of Sports Medicine, Torino, Italy Gian Luigi Canata, MD
Minimally Invasive ACL Surgery
 Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES
 ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES WHAT IS THE ACL? The ACL is a very strong ligament on the inside of the knee. It runs from the femur (thigh bone) obliquely down to the Tibia (shin bone). The
ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES WHAT IS THE ACL? The ACL is a very strong ligament on the inside of the knee. It runs from the femur (thigh bone) obliquely down to the Tibia (shin bone). The
Disclosures. Outline. The Posterior Cruciate Ligament 5/3/2016
 The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
BioRCI Screw System. Surgical Technique for Hamstring and Patellar Tendon Grafts
 BioRCI Screw System Surgical Technique for Hamstring and Patellar Tendon Grafts Surgical Technique for Hamstring and Patellar Tendon Grafts Using the BioRCI Screw System The Smith & Nephew BioRCI cruciate
BioRCI Screw System Surgical Technique for Hamstring and Patellar Tendon Grafts Surgical Technique for Hamstring and Patellar Tendon Grafts Using the BioRCI Screw System The Smith & Nephew BioRCI cruciate
Transtibial PCL Reconstruction. Surgical Technique. Transtibial PCL Reconstruction
 Transtibial PCL Reconstruction Surgical Technique Transtibial PCL Reconstruction The Arthrex Transtibial PCL Reconstruction System includes unique safety features for protecting posterior neurovascular
Transtibial PCL Reconstruction Surgical Technique Transtibial PCL Reconstruction The Arthrex Transtibial PCL Reconstruction System includes unique safety features for protecting posterior neurovascular
Five year results of the first ten ACL patients treated with dynamic intraligamentary stabilisation
 Eggli et al. BMC Musculoskeletal Disorders (2016) 17:105 DOI 10.1186/s12891-016-0961-7 RESEARCH ARTICLE Open Access Five year results of the first ten ACL patients treated with dynamic intraligamentary
Eggli et al. BMC Musculoskeletal Disorders (2016) 17:105 DOI 10.1186/s12891-016-0961-7 RESEARCH ARTICLE Open Access Five year results of the first ten ACL patients treated with dynamic intraligamentary
Grant H Garcia, MD Sports and Shoulder Surgeon
 What to Expect from your Anterior Cruciate Ligament Reconstruction Surgery A Guide for Patients Grant H Garcia, MD Sports and Shoulder Surgeon Important Contact Information Grant Garcia, MD Wallingford:
What to Expect from your Anterior Cruciate Ligament Reconstruction Surgery A Guide for Patients Grant H Garcia, MD Sports and Shoulder Surgeon Important Contact Information Grant Garcia, MD Wallingford:
What is new in CrCl surgery in humans
 What is new in CrCl surgery in humans ESVOT meeting, Lodi, Italy September 12, 2015 Stephen Bresina, Sc.D. Kyon & Scyon Orthpoaedics Failure Mechansim 30 % in USA due to contact (American Football) Non-contact
What is new in CrCl surgery in humans ESVOT meeting, Lodi, Italy September 12, 2015 Stephen Bresina, Sc.D. Kyon & Scyon Orthpoaedics Failure Mechansim 30 % in USA due to contact (American Football) Non-contact
All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes
 All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes William Godfrey, BS Aaron Gebrelul, BA; John Xerogeanes, MD; Ajay
All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes William Godfrey, BS Aaron Gebrelul, BA; John Xerogeanes, MD; Ajay
Treatment of meniscal lesions and isolated lesions of the anterior cruciate ligament of the knee in adults
 QUICK REFERENCE GUIDE Treatment of meniscal s and isolated s of the anterior cruciate ligament of the knee in adults June 2008 AIM OF THE GUIDELINES To encourage good practices in the areas of meniscal
QUICK REFERENCE GUIDE Treatment of meniscal s and isolated s of the anterior cruciate ligament of the knee in adults June 2008 AIM OF THE GUIDELINES To encourage good practices in the areas of meniscal
ACL INJURIES WHEN TO OPERATE
 ACL INJURIES WHEN TO OPERATE Ziali Sivardeen BMedSci, (MRCS), AFRCS, FRCS (Tr & Orth) Consultant Trauma and Orthopaedic Surgeon (Shoulder, Knee and Sports Injuries) ziali@theolympiaclinic.com www.theolympiaclinic.com
ACL INJURIES WHEN TO OPERATE Ziali Sivardeen BMedSci, (MRCS), AFRCS, FRCS (Tr & Orth) Consultant Trauma and Orthopaedic Surgeon (Shoulder, Knee and Sports Injuries) ziali@theolympiaclinic.com www.theolympiaclinic.com
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Why anteromedial portal is the best
 Controversies in ACL Reconstruction Why anteromedial portal is the best Robert A. Gallo, MD Associate Professor Nothing to disclose Case presentation 20-year-old Division III track athlete sustained ACL
Controversies in ACL Reconstruction Why anteromedial portal is the best Robert A. Gallo, MD Associate Professor Nothing to disclose Case presentation 20-year-old Division III track athlete sustained ACL
Appendix 2: KNGF Evidence Statement for anterior cruciate ligament reconstruction rehabilitation
 Appendix 2: KNGF Evidence Statement for anterior cruciate ligament reconstruction rehabilitation Inclusion and exclusion criteria for rehabilitation according to the Evidence Statement Inclusion of patients
Appendix 2: KNGF Evidence Statement for anterior cruciate ligament reconstruction rehabilitation Inclusion and exclusion criteria for rehabilitation according to the Evidence Statement Inclusion of patients
FIXED PERFORMANCE. Soft Tissue ACL Reconstruction
 ADJUSTABLE CONVENIENCE, FIXED PERFORMANCE Soft Tissue ACL Reconstruction Surgical Technique The RIGIDLOOP Adjustable Cortical System The RIGIDLOOP Adjustable Cortical System is an innovative technology
ADJUSTABLE CONVENIENCE, FIXED PERFORMANCE Soft Tissue ACL Reconstruction Surgical Technique The RIGIDLOOP Adjustable Cortical System The RIGIDLOOP Adjustable Cortical System is an innovative technology
ACL RECONSTRUCTION SPORTS REHABILITATION. Written by Bart Sas, Qatar
 ACL RECONSTRUCTION PREDICTORS AND PROGNOSIS OF OUTCOME POST RECONSTRUCTION Written by Bart Sas, Qatar Injury to the anterior cruciate ligament (ACL) is arguably the most devastating injury that an athlete
ACL RECONSTRUCTION PREDICTORS AND PROGNOSIS OF OUTCOME POST RECONSTRUCTION Written by Bart Sas, Qatar Injury to the anterior cruciate ligament (ACL) is arguably the most devastating injury that an athlete
Primary Tunnel Dilatation in Tibia, An Unrecognised Complication of ACL Reconstruction
 Abstract # 18074 Primary Tunnel Dilatation in Tibia, An Unrecognised Complication of ACL Reconstruction Prakash Ayyadurai, Suresh Perumal, Parthiban Jeganathan, Karthik Parachur, Arumugam Sivaraman Sri
Abstract # 18074 Primary Tunnel Dilatation in Tibia, An Unrecognised Complication of ACL Reconstruction Prakash Ayyadurai, Suresh Perumal, Parthiban Jeganathan, Karthik Parachur, Arumugam Sivaraman Sri
ACL Reconstruction Cross-Pin Technique
 ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
Evolution of Technique: 90 s
 Anterior Medial and Accessory Portal Techniques: ACL Reconstruction Charles A. Bush Joseph, MD Rush University Medical Center Chicago, IL Evolution of Technique: 80 s Open and 2 incision methods produced
Anterior Medial and Accessory Portal Techniques: ACL Reconstruction Charles A. Bush Joseph, MD Rush University Medical Center Chicago, IL Evolution of Technique: 80 s Open and 2 incision methods produced
Double Bundle PCL Reconstruction. Surgical Technique
 Double Bundle PCL Reconstruction Surgical Technique Double Bundle PCL Reconstruction With recent interest in double tunnel endoscopic PCL reconstruction, Arthrex has created a series of Femoral PCL Drill
Double Bundle PCL Reconstruction Surgical Technique Double Bundle PCL Reconstruction With recent interest in double tunnel endoscopic PCL reconstruction, Arthrex has created a series of Femoral PCL Drill
STUDY ON FUNCTIONAL OUTCOME WITH VARIOUS GRAFT FIXATION OPTIONS IN ARTHROSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 STUDY ON FUNCTIONAL OUTCOME WITH VARIOUS GRAFT FIXATION OPTIONS IN ARTHROSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Clinical Article Orthopaedics P. Radhakrishnan 1, C. Kamalanathan 2, A.M. Shantha
STUDY ON FUNCTIONAL OUTCOME WITH VARIOUS GRAFT FIXATION OPTIONS IN ARTHROSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Clinical Article Orthopaedics P. Radhakrishnan 1, C. Kamalanathan 2, A.M. Shantha
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Kohei Kawaguchi, Shuji Taketomi, Hiroshi Inui, Ryota Yamagami, Kenichi Kono, Keiu Nakazato, Kentaro Takagi, Manabu Kawata, Sakae Tanaka
 Chronological changes in anterior knee stability after anatomical anterior cruciate ligament reconstruction using bone-patellar tendon-bone graft and hamstrings graft Kohei Kawaguchi, Shuji Taketomi, Hiroshi
Chronological changes in anterior knee stability after anatomical anterior cruciate ligament reconstruction using bone-patellar tendon-bone graft and hamstrings graft Kohei Kawaguchi, Shuji Taketomi, Hiroshi
Knee Surg Relat Res 2011;23(4): pissn eissn Knee Surgery & Related Research
 Original Article Knee Surg Relat Res 2011;23(4):213-219 http://dx.doi.org/10.5792/ksrr.2011.23.4.213 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Anatomic Single Bundle Anterior Cruciate
Original Article Knee Surg Relat Res 2011;23(4):213-219 http://dx.doi.org/10.5792/ksrr.2011.23.4.213 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Anatomic Single Bundle Anterior Cruciate
Biologics in ACL: What s the Data?
 Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
ADJUSTABLE CONVENIENCE, FIXED PERFORMANCE
 ADJUSTABLE CONVENIENCE, FIXED PERFORMANCE Soft Tissue ACL Reconstruction This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE THE RIGIDLOOP ADJUSTABLE CORTICAL SYSTEM The RIGIDLOOP
ADJUSTABLE CONVENIENCE, FIXED PERFORMANCE Soft Tissue ACL Reconstruction This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE THE RIGIDLOOP ADJUSTABLE CORTICAL SYSTEM The RIGIDLOOP
ARTICLE IN PRESS. Technical Note
 Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN. Guy BELLIER PARIS France
 BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN Guy BELLIER PARIS France TREATMENT OF ACL TEARS IN CHILDREN CONTROVERSIAL DIAGNOSIS clinical exam X-rays (stress) M.R.I. arthroscopy ACL TEARS
BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN Guy BELLIER PARIS France TREATMENT OF ACL TEARS IN CHILDREN CONTROVERSIAL DIAGNOSIS clinical exam X-rays (stress) M.R.I. arthroscopy ACL TEARS
Incidence. Avoiding Complications of ACL Surgery. ACL Complications 6/10/2011. Not if, but when
 Avoiding Complications of ACL Surgery Thomas J. Gill, MD Chief, MGH Sports Medicine Service Dept of Orthopedic Surgery Massachusetts General Hospital Associate Professor of Orthopedic Surgery Harvard Medical
Avoiding Complications of ACL Surgery Thomas J. Gill, MD Chief, MGH Sports Medicine Service Dept of Orthopedic Surgery Massachusetts General Hospital Associate Professor of Orthopedic Surgery Harvard Medical
3/21/2011 PCL INJURY WITH OPERATIVE TREATMENT A CASE STUDY PCL PCL MECHANISM OF INJURY PCL PREVALENCE
 PCL PCL INJURY WITH OPERATIVE TREATMENT A CASE STUDY K. Anderson, S. Hjortedal, Y. Jingi, E. Sutcliffe & S. Witschen Washington State University Origin Posterior aspect of tibia Insertion Medial femoral
PCL PCL INJURY WITH OPERATIVE TREATMENT A CASE STUDY K. Anderson, S. Hjortedal, Y. Jingi, E. Sutcliffe & S. Witschen Washington State University Origin Posterior aspect of tibia Insertion Medial femoral
Darren L. Johnson, M.D. Professor and Chairman Medical Director of Sports Medicine University of Kentucky School of Medicine
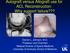 Autograft versus Allograft use for ACL Reconstruction: Why support failure??? Darren L. Johnson, M.D. Professor and Chairman Medical Director of Sports Medicine University of Kentucky School of Medicine
Autograft versus Allograft use for ACL Reconstruction: Why support failure??? Darren L. Johnson, M.D. Professor and Chairman Medical Director of Sports Medicine University of Kentucky School of Medicine
Extensor Mechanism Rupture
 Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
Does Cortical Non-Contact or Delayed Contact of an Adjustable-loop Femoral Button Affect Knee Stability after ACL Reconstruction?
 Does Cortical Non-Contact or Delayed Contact of an Adjustable-loop Femoral Button Affect Knee Stability after ACL Reconstruction? 2008. 1. 16 Kim CK, Sohn SE, Koh IJ, Kim MS, Song KY, In Y Seoul St. Mary
Does Cortical Non-Contact or Delayed Contact of an Adjustable-loop Femoral Button Affect Knee Stability after ACL Reconstruction? 2008. 1. 16 Kim CK, Sohn SE, Koh IJ, Kim MS, Song KY, In Y Seoul St. Mary
A Patient s Guide to Posterior Cruciate Ligament Injuries
 A Patient s Guide to Posterior Cruciate Ligament Injuries 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Posterior Cruciate Ligament Injuries 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
ACL Reconstruction for BTB Grafts
 Transtibial ACL Reconstruction System for BTB Grafts Surgical Technique Designed in conjunction with John C. Garrett, M.D., Atlanta, GA ACL Reconstruction for BTB Grafts Reference Anatomical Constants
Transtibial ACL Reconstruction System for BTB Grafts Surgical Technique Designed in conjunction with John C. Garrett, M.D., Atlanta, GA ACL Reconstruction for BTB Grafts Reference Anatomical Constants
Disclosure. ACL Reconstruction with Allograft is Controversial. UCSF Pioneered Research on Allograft ACL Reconstruction
 Disclosure Allograft ACL Reconstruction in the Adolescent Steve J. Barad, MD and Stephen M. Howell, MD Private Practice Orthopedic Surgery, Sacramento, CA Professor of Mechanical Engineering, UC Davis
Disclosure Allograft ACL Reconstruction in the Adolescent Steve J. Barad, MD and Stephen M. Howell, MD Private Practice Orthopedic Surgery, Sacramento, CA Professor of Mechanical Engineering, UC Davis
CROSS PIN TECHNOLOGY FOR AN ANATOMIC ACL
 CROSS PIN TECHNOLOGY FOR AN ANATOMIC ACL INTRODUCTION The RIGIDFIX Curve Cross Pin System is designed specifically for use with the anteromedial (AM) portal approach to achieve a more anatomic soft tissue
CROSS PIN TECHNOLOGY FOR AN ANATOMIC ACL INTRODUCTION The RIGIDFIX Curve Cross Pin System is designed specifically for use with the anteromedial (AM) portal approach to achieve a more anatomic soft tissue
Medical Diagnosis for Michael s Knee
 Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION
 ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft
 384 Clinicale Evaluation Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft Swaroop Patel, Resident, Vijendra D. Chauhan, Professor, Anil Juyal, Professor, Rajesh
384 Clinicale Evaluation Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft Swaroop Patel, Resident, Vijendra D. Chauhan, Professor, Anil Juyal, Professor, Rajesh
Figure 3 Figure 4 Figure 5
 Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
ACL Reconstruction: What is the Role of Sex and Sport in Graft Choice?
 ACL Reconstruction: What is the Role of Sex and Sport in Graft Choice? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior
ACL Reconstruction: What is the Role of Sex and Sport in Graft Choice? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
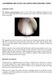 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION INTRODUCTION The anterior cruciate ligament (ACL) is one of the major stabilising ligaments in the knee. It is a strong rope like structure located in the centre
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION INTRODUCTION The anterior cruciate ligament (ACL) is one of the major stabilising ligaments in the knee. It is a strong rope like structure located in the centre
*smith&nephew ENDOBUTTON CL. Knee Series Technique Guide. Fixation System
 Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System Double Bundle ACL Reconstruction using the Smith & Nephew ACUFEX Director Set for Anatomic ACL Reconstruction French Anatomic ACL-R
Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System Double Bundle ACL Reconstruction using the Smith & Nephew ACUFEX Director Set for Anatomic ACL Reconstruction French Anatomic ACL-R
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Anterolateral Ligament. Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine
 Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Impact of surgical timing on the clinical outcomes of anatomic double-bundle anterior cruciate ligament reconstruction
 ISAKOS 2019 12 th -16 th May Cancun, Mexico Impact of surgical timing on the clinical outcomes of anatomic double-bundle anterior cruciate ligament reconstruction Baba R. 1, Kondo E. 2, Iwasaki K. 1, Joutoku
ISAKOS 2019 12 th -16 th May Cancun, Mexico Impact of surgical timing on the clinical outcomes of anatomic double-bundle anterior cruciate ligament reconstruction Baba R. 1, Kondo E. 2, Iwasaki K. 1, Joutoku
Autograft versus Allograft Failure in Anterior Cruciate Ligament Reconstruction of Young Athletic Patients
 James Madison University JMU Scholarly Commons Physician Assistant Capstones The Graduate School 8-1-2016 Autograft versus Allograft Failure in Anterior Cruciate Ligament Reconstruction of Young Athletic
James Madison University JMU Scholarly Commons Physician Assistant Capstones The Graduate School 8-1-2016 Autograft versus Allograft Failure in Anterior Cruciate Ligament Reconstruction of Young Athletic
What is an ACL Tear?...2. Treatment Options...3. Surgical Techniques...4. Preoperative Care...5. Preoperative Requirements...6
 Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Clarkstown Division This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Clarkstown Division This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
SURGICAL TECHNIQUE VISUALIZE FEMORAL FIXATION 360 GRAFT TO BONE CONTACT INCREASED PULL-OUT STRENGTH
 SURGICAL TECHNIQUE VISUALIZE FEMORAL FIXATION 360 GRAFT TO BONE CONTACT INCREASED PULL-OUT STRENGTH PINN-ACL CROSSPIN SYSTEM SURGICAL TECHNIQUE INTRODUCTION The ConMed Linvatec Pinn-ACL CrossPin System
SURGICAL TECHNIQUE VISUALIZE FEMORAL FIXATION 360 GRAFT TO BONE CONTACT INCREASED PULL-OUT STRENGTH PINN-ACL CROSSPIN SYSTEM SURGICAL TECHNIQUE INTRODUCTION The ConMed Linvatec Pinn-ACL CrossPin System
Graft choice for anterior cruciate ligament (ACL)
 Technical Note Arthroscopic Anterior Cruciate Ligament Reconstruction Using Quadriceps Tendon Autograft and Bioabsorbable Cross-Pin Fixation Emmanuel Antonogiannakis, M.D., Christos K. Yiannakopoulos,
Technical Note Arthroscopic Anterior Cruciate Ligament Reconstruction Using Quadriceps Tendon Autograft and Bioabsorbable Cross-Pin Fixation Emmanuel Antonogiannakis, M.D., Christos K. Yiannakopoulos,
Torn ACL Hamstring Graft
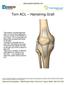 Torn ACL Hamstring Graft The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects the femur to the tibia.
Torn ACL Hamstring Graft The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects the femur to the tibia.
ACL Injury: Does It Require Surgery?-OrthoInfo - AAOS
 ACL Injury: Does It Require Surgery?-OrthoInfo - AAOS ACL Injury: Does It Require Surgery? The following article provides in-depth information about treatment for anterior cruciate ligament injuries. The
ACL Injury: Does It Require Surgery?-OrthoInfo - AAOS ACL Injury: Does It Require Surgery? The following article provides in-depth information about treatment for anterior cruciate ligament injuries. The
Bioabsorbable Versus Titanium Screws in ACL Reconstruction. A Randomised Controlled Trial with 13 years Follow-up
 Bioabsorbable Versus Titanium Screws in ACL Reconstruction. A Randomised Controlled Trial with 13 years Follow-up Justin Roe, Keran Sundaraj, Emma Heath, Lucy Salmon, Leo Pinczewski North Sydney Orthopaedic
Bioabsorbable Versus Titanium Screws in ACL Reconstruction. A Randomised Controlled Trial with 13 years Follow-up Justin Roe, Keran Sundaraj, Emma Heath, Lucy Salmon, Leo Pinczewski North Sydney Orthopaedic
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
as described by J. Emory Chapman, Jr., MD
 PROCEDURAL PERSPECTIVES SOFT TISSUE ACL RECONSTRUCTION PROCEDURE as described by J. Emory Chapman, Jr., MD RIGIDFIX ST SURGICAL TECHNIQUE PROCEDURAL PERSPECTIVE J. EMORY CHAPMAN, JR., MD For more information,
PROCEDURAL PERSPECTIVES SOFT TISSUE ACL RECONSTRUCTION PROCEDURE as described by J. Emory Chapman, Jr., MD RIGIDFIX ST SURGICAL TECHNIQUE PROCEDURAL PERSPECTIVE J. EMORY CHAPMAN, JR., MD For more information,
RIGIDfix. Soft Tissue. Surgical Technique for Mitek RIGIDfix ACL Reconstruction PRODUCTS. Daniel J. McKernan, M.D. TISSUE SOFT.
 RIGIDfix A C L C R O S S P I N S Y S T E M Daniel J. McKernan, M.D. Toledo, Ohio SOFT TISSUE Surgical Technique for Mitek RIGIDfix ACL Reconstruction Soft Tissue PRODUCTS SURGICAL TECHNIQUE RIGIDfix A
RIGIDfix A C L C R O S S P I N S Y S T E M Daniel J. McKernan, M.D. Toledo, Ohio SOFT TISSUE Surgical Technique for Mitek RIGIDfix ACL Reconstruction Soft Tissue PRODUCTS SURGICAL TECHNIQUE RIGIDfix A
Anterior Cruciate Ligament (ACL) Tears
 WASHINGTON UNIVERSITY ORTHOPEDICS Anterior Cruciate Ligament (ACL) Tears Knowing what to expect for ACL surgery is key for a healthy surgery and recovery. Our sports medicine specialists are committed
WASHINGTON UNIVERSITY ORTHOPEDICS Anterior Cruciate Ligament (ACL) Tears Knowing what to expect for ACL surgery is key for a healthy surgery and recovery. Our sports medicine specialists are committed
Remnant Preservation in ACL Reconstruction: Is it Worth Doing?
 Remnant Preservation in ACL Reconstruction: Is it Worth Doing? 1. Presentation (4 x approx. 5min.) i. Mitsuo Ochi ii. Freddie Fu, iii. Takeshi Muneta iv. Rainer Siebold, 2. Debate (approx. 10 min.) 1 ACL
Remnant Preservation in ACL Reconstruction: Is it Worth Doing? 1. Presentation (4 x approx. 5min.) i. Mitsuo Ochi ii. Freddie Fu, iii. Takeshi Muneta iv. Rainer Siebold, 2. Debate (approx. 10 min.) 1 ACL
Rehabilitation Protocol for Anterior Cruciate Ligament Reconstruction
 Rehabilitation Protocol for Anterior Cruciate Ligament Reconstruction Orthopedic Services by Stephen M. Howell, MD ALIGN WITH THE BEST Brace-Free Rehabilitation Protocol for Anterior Cruciate Ligament
Rehabilitation Protocol for Anterior Cruciate Ligament Reconstruction Orthopedic Services by Stephen M. Howell, MD ALIGN WITH THE BEST Brace-Free Rehabilitation Protocol for Anterior Cruciate Ligament
Jonathan T. Bravman, MD
 Jonathan T. Bravman, MD Assistant Professor Director of Sports Medicine Research Division of Sports Medicine and Shoulder Surgery Department of Orthopedics University of Colorado Team Physician for CU
Jonathan T. Bravman, MD Assistant Professor Director of Sports Medicine Research Division of Sports Medicine and Shoulder Surgery Department of Orthopedics University of Colorado Team Physician for CU
Jennifer L. Cook, MD
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
QuadsTape System TM. For Quadriceps Tendon Reconstruction. Surgical Technique Manual
 QuadsTape System TM For Quadriceps Tendon Reconstruction Surgical Technique Manual 0086 Introduction QuadsTape System TM The QuadsTape System comprises a wide open weave Poly-Tape prosthesis with associated
QuadsTape System TM For Quadriceps Tendon Reconstruction Surgical Technique Manual 0086 Introduction QuadsTape System TM The QuadsTape System comprises a wide open weave Poly-Tape prosthesis with associated
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
ACL Reconstruction Protocol (Allograft)
 ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
Comparison of effects of Mckenzie exercises and conventional therapy in ACL reconstruction on knee range of motion and functional ability
 2018; 4(4): 415-420 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(4): 415-420 www.allresearchjournal.com Received: 25-02-2018 Accepted: 26-03-2018 Riya Sadana BPTh Student,
2018; 4(4): 415-420 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(4): 415-420 www.allresearchjournal.com Received: 25-02-2018 Accepted: 26-03-2018 Riya Sadana BPTh Student,
Bio-TransFix ACL Reconstruction. Surgical Technique
 Bio-TransFix ACL Reconstruction Surgical Technique Bio-TransFix ACL Reconstruction 1 Semitendinosus and gracilis tendon autografts or tibialis tendon allografts are mounted on the GraftPro workstation.
Bio-TransFix ACL Reconstruction Surgical Technique Bio-TransFix ACL Reconstruction 1 Semitendinosus and gracilis tendon autografts or tibialis tendon allografts are mounted on the GraftPro workstation.
Disclosures. Background. Background
 Kinematic and Quantitative MR Imaging Evaluation of ACL Reconstructions Using the Mini-Two Incision Method Compared to the Anteromedial Portal Technique Drew A. Lansdown, MD Christina Allen, MD Samuel
Kinematic and Quantitative MR Imaging Evaluation of ACL Reconstructions Using the Mini-Two Incision Method Compared to the Anteromedial Portal Technique Drew A. Lansdown, MD Christina Allen, MD Samuel
IKDC DEMOGRAPHIC FORM
 IKDC DEMOGRAPHIC FORM Your Full Name Your Date of Birth / / Your Social Security Number - - Your Gender: Male Female Occupation Today s Date / / The following is a list of common health problems. Please
IKDC DEMOGRAPHIC FORM Your Full Name Your Date of Birth / / Your Social Security Number - - Your Gender: Male Female Occupation Today s Date / / The following is a list of common health problems. Please
Incidence of graft rupture 15 years after bilateral anterior cruciate ligament reconstructions
 M. Goddard, L. Salmon, A. Waller, E. Papapetros, L. A. Pinczewski From North Sydney Orthopaedic and Sports Medicine Centre, Sydney, Australia M. Goddard, FRCS(Tr & Orth), Orthopaedic Surgeon L. Salmon,
M. Goddard, L. Salmon, A. Waller, E. Papapetros, L. A. Pinczewski From North Sydney Orthopaedic and Sports Medicine Centre, Sydney, Australia M. Goddard, FRCS(Tr & Orth), Orthopaedic Surgeon L. Salmon,
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
ACL reconstruction with the ACUFEX Director Drill Guide and. ENDOBUTTON CL Fixation System. *smith&nephew. Knee Series Technique Guide ENDOBUTTON CL
 Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System ACL reconstruction with the ACUFEX Director Drill Guide and ENDOBUTTON CL Fixation System Thomas D. Rosenberg, MD ACL Reconstruction
Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System ACL reconstruction with the ACUFEX Director Drill Guide and ENDOBUTTON CL Fixation System Thomas D. Rosenberg, MD ACL Reconstruction
)264( COPYRIGHT 2015 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE
 )264( COPYRIGHT 2015 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Functional Outcome Following Arthroscopic ACL Reconstruction with Rigid Fix: A Retrospective Observational Study Satish Shervegar,
)264( COPYRIGHT 2015 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Functional Outcome Following Arthroscopic ACL Reconstruction with Rigid Fix: A Retrospective Observational Study Satish Shervegar,
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
Primary transosseous ACL repair in proximal lesions
 Primary transosseous ACL repair in proximal lesions G.L. Canata, V. Casale Centre of Sports Traumatology, Koelliker Hospital, Torino Institute of Sports Medicine, Torino, Italy Gian Luigi Canata, MD I
Primary transosseous ACL repair in proximal lesions G.L. Canata, V. Casale Centre of Sports Traumatology, Koelliker Hospital, Torino Institute of Sports Medicine, Torino, Italy Gian Luigi Canata, MD I
What to Expect from your Anterior Cruciate Ligament (ACL) Reconstruction Surgery A Guide for Patients
 What to Expect from your Anterior Cruciate Ligament (ACL) Reconstruction Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://www.orthoinfo.org/informedpatient.cfm http://www.sportsmed.org/patient/
What to Expect from your Anterior Cruciate Ligament (ACL) Reconstruction Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://www.orthoinfo.org/informedpatient.cfm http://www.sportsmed.org/patient/
REHABILITATION GUIDELINES
 REHABILITATION GUIDELINES Autologous Chondrocyte Implantation using Carticel (autologous cultured chondrocytes) Michael M. Reinold, PT, ATC* Kevin E. Wilk, PT* Jeffrey R. Dugas, MD* E. Lyle Cain, MD* Scott
REHABILITATION GUIDELINES Autologous Chondrocyte Implantation using Carticel (autologous cultured chondrocytes) Michael M. Reinold, PT, ATC* Kevin E. Wilk, PT* Jeffrey R. Dugas, MD* E. Lyle Cain, MD* Scott
