Local resection of the mass to treat the osteochondroma of the mandibular condyle: Indications and different methods with 38-case series
|
|
|
- Myrtle Hardy
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Local resection of the mass to treat the osteochondroma of the mandibular condyle: Indications and different methods with 38-case series Min-Jie Chen, MD, 1 Chi Yang, MD, 1 * Ya-Ting Qiu, MD, 1 Dong-Mei He, MD, 1 Qin Zhou, DDS, 1 Dong Huang, DDS, 1 Hui-Min Shi, MD 2,3 1 Department of Oral and Maxillofacial Surgery, Ninth People s Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai Key Laboratory of Stomatology, Shanghai, China, 2 Department of Oral and Maxillofacial Surgery, First Teaching Hospital of Xinjiang Medical University, Urumuqi Xinjiang, China, 3 Department of Radiology, Ninth People s Hospital, Shanghai Jiao Tong University, School of Medicine, Shanghai, China. Accepted 28 September 2012 Published online 18 March 2013 in Wiley Online Library (wileyonlinelibrary.com). DOI /hed ABSTRACT: Background. Local resection of the mass was reported to treat the condylar osteochodroma in some cases. The purpose of this study was to evaluate the feasibility and the indications of the local resection. Methods. In all, 47 patients with osteochondroma of the mandibular condyle were treated from January 2002 to March The decision to perform local resection depended on 2 factors: there was a stalk existing between the mass and the condyle, and the condylar surface was involved less than 1/2. Results. Local resection of the mass was performed in 38 cases (80.1%). These masses were removed by 4 methods: direct removal (18 cases), pushed-out by a screw and steel wire (14 cases), excision in multiple pieces (3 cases), and temporary osteotomy of the zygomatic arch (3 cases). In the follow-up period, there was no recurrence. Conclusion. Local resection of the mass was a more conservative procedure to treat the solitary osteochondroma with a stalk. VC 2013 Wiley Periodicals, Inc. Head Neck 36: , 2014 KEY WORDS: osteochondroma, mandibular condyle, local resection of the mass, indication, method INTRODUCTION The World Health Organization defines the osteochondroma as a "cartilage-capped bony protrusion on the external surface of bone. It represents approximately 35% to 50% of all benign bone tumors and 8% to 15% of all primary bone tumors. 1 The most common sites of the craniofacial region are the mandibular condyle and the coronoid process. In 2010, Ord et al 2 identified 67 cases of this tumor to be documented. Roychoudhury et al 3 made it more accurate to say that by 2011 at least 108 cases had been reported in the English-language literature. The number of single case reports is 48; the largest case series is Surgical resection is an acceptable treatment. Total condylectomy and conservative subtotal condylectomy were often used in the treatment of the condylar osteochondroma. Immediate or delayed reconstruction was performed by This article was published online on 18 March An error was subsequently identified. This notice is included in the online and print versions to indicate that both have been corrected [16 December 2013]. *Corresponding author: C. Yang, Department of Oral and Maxillofacial Surgery, Ninth People s Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai Key Laboratory of Stomatology, Shanghai, China. yangchi63@hotmail.com Contract grant sponsor: National Natural Science Foundation of China; contract grant number: ; contract grant sponsor: Program for Innovative Research Team of Shanghai Municipal Education Commission. several methods, such as sagittal split ramus osteotomy (SSRO) and superior advancement, a costchondral graft (CCG) or iliac bone graft. Due to its benign nature, there was an extremely low recurrence. 5 However, could the surgery have been even more conservatively performed? Cottrell 6 proposed to save as much of the condyle as possible. Some single case reports were found to use local resection of the mass There were some queries about the procedure of local resection of the mass, such as: (1) Will it result in a high rate of recurrence? (2) What kind of condylar osteochondroma was appreciated for local resection of the mass? and (3) How is the mass released if it was huge and deep? There were no large case series to answer these questions. Presented here is a report of 38 cases of the osteochondroma of the mandibular condyle treated by local resection of the mass with the condylar head preserved in our unit from January 2002 to March The purpose of this report was to discuss the feasibility and the indication of local resection of the mass. The methods of resection were also introduced. MATERIALS AND METHODS The records of 47 patients with osteochondroma of the mandibular condyle at our unit from January 2002 to March 2012 were retrospectively analyzed. Local resection of the mass was performed in 38 cases (80.1%), total condylectomy in 5 cases (10.6%), and subtotal condylectomy in 4 cases (8.5%). CCG reconstruction, temporary zygomatic arch osteotomy, or orthognathic surgical HEAD & NECK DOI /HED FEBRUARY
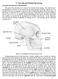
2 CHEN ET AL. TABLE 1. General characteristics of the patients who had local resection of the mass performed. TABLE 2. Operative findings of the patients who had local resection of the mass performed. Characteristic Value Characteristic Value Age at surgery, y Median 41.5 Average 43.7 Sex, n (%) Male 10 (26.3%) Female 28 (73.7%) Side of symptom, n (%) Right 22 (57.9%) Left 16 (42.1%) Preoperative duration of symptom, y Median 1.0 Average 2.93 Symptoms, n (%) Mandible asymmetry 26 (68.4%) Maxilla and mandible asymmetry 5 (13.2%) Preauricular pain 13 (34.2%) Preauricular swelling 17 (44.7%) Ipsilateral hearing loss 2 (5.3%) Recurrent luxation 2 (5.3%) Joint noise 17 (44.7%) Limitation of the open mouth (30 mm) 18 (47.4%) Malocclusion 31 (81.6%) procedures, if indicated, were then concomitantly performed to optimize occlusion, function, and esthetics. The study protocol was approved by and in accord with the recommendations of the human research committee at our institution. Prior to scanning and surgical procedures all patients gave written consent. In all, 38 cases with local resection of the mass and preservation of the condylar head were the core concerns of this report. The decision to perform local resection depended on 2 factors: there was a stalk existing between the mass and the condylar head, and the condylar surface was involved less than half. The variables studied were age, sex, side, duration, symptoms, and treatment. Panoramic radiographs, standardized frontal and lateral cephalometric tomograms, and CT scans before surgery, immediately after surgery, and at the follow-up period were assessed. The diagnosis of osteochondroma was confirmed by histopathologic examination. The facial symmetry, temporomandibular joint (TMJ) pain, mouth opening, occlusion, and radiologic examination were evaluated during the follow-up period. RESULTS The general characteristics of 38 patients performed local resection of the mass are presented in Table 1. Gender predilection (male:female) was 1:2.8. Right:left side predilection was 1.4:1. Only 2 cases had trauma history. Age range was 21 to 74 years, with a mean of 43.7 years. Preoperative duration was 2 months to 15 years, with a mean of 2.93 years. The first symptom noticed was a gradual development of asymmetry and chin deviation, then followed by TMJ dysfunction, swelling, and pain. In all 38 patients, CT revealed the mass protruding from the condyle with less than half of the condyle involved. Location of the mass, n (%) Anterior/anteromedial 25 (65.8%) Posterior/posteromedial 3 (7.9%) Medial 8 (21.1%) Lateral 2 (5.3%) Treatment, n (%) Local resection of the mass 33 (86.8%) Local resection with temporary 3 (7.9%) zygomatic arch osteotomy Local resection with bilateral sagittal 1 (2.6%) split ramus osteotomy Local resection with genioplasty 1 (2.6%) Method of removal of the mass, n (%) Direct removal 18 (47.4%) Distraction by a screw and steel wire 14 (36.8%) Excision in multiple pieces 3 (7.9%) Temporary zygomatic arch osteotomy 3 (7.9%) In accord with CT scans and the operative findings, the location of the mass relative to the condylar head was as follows (Table 2): anterior/anteromedial in 25 cases (65.8%), posterior/posteromedial in 3 cases (7.9%), medial in 8 cases (21.1%), and lateral in 2 cases (5.3%). In 33 patients (86.8%) local resection of the mass only was performed. One case was combined with bilateral SSRO; 1 case was combined with genioplasty. FIGURE 1. Reoperated patient with residue stalk (arrow). 274 HEAD & NECK DOI /HED FEBRUARY 2014
3 FEASIBILITY AND INDICATIONS OF THE LOCAL RESECTION (see Figure 1). The residual stalk was removed to correct the stable occlusion and to avoid the recurrence. Among 38 patients, stable occlusion or minimal occlusion discrepancy was regained immediately after the operation in 26 patients, maxillomandibular elastic bands were applied in 7 patients, and orthodontic therapy was done in 1 patient. However, 4 patients without good occlusion refused to do any subsequent therapy. The follow-up averaged 23.8 months with a range of 1 to 84 months. Twelve cases were lost to follow-up; 6 patients were followed up for at least 5 years; 10 were 1 to 2 years postoperatively; and 10 were less than half a year. TMJ pain, swelling, and hearing loss disappeared. The facial symmetry was almost regained in 34 cases. In the 26 patients who were followed-up, CT scans were examined every year during the follow-up period. No recurrence was encountered except roughness of the bony cut-line occurred in 2 cases. FIGURE 2. Preoperative appearance. (A) Frontal view showing elongation of the left mandible and deviation of the chin to the right. (B) Deviation of the mandibular dental midline to the right by 6 mm. [Color figure can be viewed in the online issue, which is available at wileyonlinelibrary.com.] These masses were removed by 4 methods (Table 2): direct removal in 18 cases, pushed-out by a screw and steel wire in 14 cases, excision in multiple pieces in 3 cases, and temporary osteotomy of the zygomatic arch with masseter muscle attachment in 3 cases. If the mass was too big to be grasped by a forceps, it could be pushed out with assistance of a screw and steel wire. Before fixing the screw, the direction and the length of the screw should be evaluated in accord with the dimension of the mass. The screw should not be longer than the dimension of the mass to avoid damaging the maxilla artery. An obvious differentiable stalk could be found in all of the 38 cases. The largest tumor was cm and the smallest was cm. Two patients were operated on twice because the residual stalk was found by the immediate postoperative CT scan FIGURE 3. Preoperative CT scans. (A) Axial CT scan showing the mass arising from the medial portion of the condylar surface (arrow). (B) Coronal CT scan showing the mass extending superomedially into the infratemporal fossa (arrow). HEAD & NECK DOI /HED FEBRUARY
4 CHEN ET AL. FIGURE 4. Operative photographs. (A) The condyle (white arrow) was pushed infra-anteriorly to expose the mass (thick dark arrow). (B) The cutline (thin black arrow) on the stalk of the mass. (C) The mass was released with preservation of the condyle. (D) The gross specimen with multiple nodes. [Color figure can be viewed in the online issue, which is available at wileyonlinelibrary.com.] Case presentation A 46-year-old woman presented in 2010 with complaint of facial asymmetry and malocclusion. Examination of the patient revealed elongation of the left mandible with deviation of the chin to the right (Figure 2A). Her mouth opening was 10 mm, and mandibular dental midline was deviated to the right by 6 mm. There was a left posterior open bite and a right cross bite (Figure 2B). CT scan showed the mass extended superomedially into the infratemporal fossa (Figures 3A, 3B). Preoperative model analysis showed that a good occlusion could be obtained. The patient was operated on under general anesthesia via a preauricular and infratemporal approach to the joint. The superficial temporal fascia and periosteum overlying the zygomatic arch were incised, leaving the superficial neurovascular structures behind. The inferior compartment was opened. The insertion of the lateral pterygoid muscle was cut to expose the tumor. A screw twining with a steel wire was inserted into the mass (Figure 4A). The stalk of the mass was cut with a motor saw (Figure 4B). The mass with the screw-steel elevator was freed and dissected from the surrounding soft tissue (Figures 4C, 4D). Histopathologic examination of the resected specimen revealed a thickened cartilaginous cap over the mass and islands of subchondral ossification (see Figure 5), thereby confirming the diagnosis of osteochondroma. Maxillomandibular elastic bands were applied postoperatively for 1 month. By 1 year after the 276 HEAD & NECK DOI /HED FEBRUARY 2014
5 FEASIBILITY AND INDICATIONS OF THE LOCAL RESECTION DISCUSSION Osteochondroma is the most common benign bone tumor. Osteochondroma of mandibular condyle has been reported earlier under different confusing terminologies, such as osteoma, unilateral hypertrophy of the mandibular condyle, benign hyperplasia, and exostosis. The publication by Kanthak and Harkins, titled Unilateral Hypertrophy of the Mandibular Condyle Associated with Chondroma, has been designated as the first case in all the literature reviews. 6 Until 2011, in all there were 108 cases of mandibular condylar osteochondroma in the Englishlanguage literature. 3 Our report is the largest series of osteochondroma of mandibular condyle. Compared with Roychoudhury s review, 3 correlation of trauma was not obvious in our report (2/38), and the occurrence was much likely trend to the female (28/ 38). Clinical symptomatology of patients with osteochondromas may include 1 or more of the following: vertical elongation of the mandible on the affected side, progressively increasing facial asymmetry, malocclusion, TMJ dysfunction, swelling, pain, and, rarely, hearing loss. In consideration of the benign nature of the tumor and its extremely low likelihood of recurrence, the aim of treatment was excision of the tumor and a swing back of the mandible to near normal occlusion and facial midline correction. In the literature, there are 3 kinds of treatment to the mandibular condylar osteochondroma. Traditional treatment of 76.67% 12 reported cases was the radical resection of the tumor and total condylectomy, 3,13 17 with/without reconstruction of superiorly repositioned vertical ramus, 1,2,4,18 21 CCG, 2,22 or iliac bone harvest. 23 CCG and iliac bone harvest need a donor invasion. Some reports introduced a conservative subtotal condylectomy. 3,5,24 Although the shape of the condyle would be similar to that of the normal one, the loss of the superficial chondrocytes increased the risk of osteoarthritis. A few case reports chose local resection of the mass. Due to its conservative superiority, we accepted it as our basic treatment. Although being worried about the added risk of recurrence, Cottrell 6 proposed to save as much of the condyle as possible and to base the excision on the clinical apparent margin with removal of the cartilage cap. Before Cottrell, Iizuka et al 7 in 1996 (1 case), 7 Koole et al 8 in 1996 (1 case), Rivera et al 9 in 1998 (1 case), Kurita et al 10 in 1999 (1 case), and Aydin et al 11 in 2001 (2 cases) had preferred excision of the mass and the involved FIGURE 5. Histopathologic examination showing a thickened cartilaginous cap (black arrow) and islands of subchondral ossification (white arrow) (hematoxylin and eosin stain, original magnification 200). [Color figure can be viewed in the online issue, which is available at wileyonlinelibrary.com.] surgery, the patient demonstrated good aesthetic and functional stability (Figures 6A, 6B). CT revealed no recurrence (Figures 7A, 7B). FIGURE 6. Postoperative appearances 1 year after the surgery. (A) Frontal view showing the correction of asymmetry. (B) Restored occlusion with midline correction. [Color figure can be viewed in the online issue, which is available at wileyonlinelibrary.com.] HEAD & NECK DOI /HED FEBRUARY
6 CHEN ET AL. only 3 cases recurred out of the condylar osteocondroma, there was no recurrence found in the reports of local resection. Our excellent follow-up results supported the feasibility of the local resection. Axial and coronal CT scans were the important foundation to decide the indication of local resection of the mass. Our radiologic indications include 2 conditions. The first is that a stalk exists between the mass and the condylar head and the second is that the normal condylar surface is more than half. Preoperative CT scans are also necessary to decide the direction and the method of the resection. Immediate postoperative CT scans can show whether the resection of the mass is complete or incomplete. We had 2 patients who suffered from incomplete resection. CT scans immediately after the surgery revealed the mistake. The remaining mass was resected under local anesthesia before the patient went back home. CONCLUSION The use of the technique of local resection of the mass is a more conservative procedure to treat the solitary osteochondroma with a stalk. It could be accomplished by direct removal, distraction by a screw and steel wire, excision in multiple pieces, and temporary osteotomy of the zygomatic arch with masseter muscle attachment. This procedure gives excellent results with regard to facial symmetry, occlusion, and TMJ function. Note added in proof Maimaitituxun Tuerdi, MD, was erroneously listed as an author in the initial online publication. The current version of the article includes the correct author list. REFERENCES FIGURE 7. Postoperative CT scans showing no recurrence (arrow). (A) Axial CT scan. (B) Coronal scan. portion of the condyle. In our unit, 38 cases were performed on local resection of the mass. The advantages were as follows: preservation of the condylar head, which was important to keep the vertical height and the TMJ function; minimal invasion; simple manipulation. All patients did not need additional reconstruction of the condyle. The good results of the facial symmetry and stable occlusion were found. However, some reports argued that the disadvantages of the local resection were the difficult removal of the big or deep masses and incomplete resection of the mass, resulting in recurrence. In our report, distraction by a screw and steel wire were used in 14 cases, excision in multiple pieces in 3 cases, and temporary osteotomy of the zygomatic arch in 3 cases. So, the difficulties of removing the mass from the deeper structures could be overcome by distraction with a screw and steel wire, excising in multiple pieces, or temporary zygomatic arch osteotomy. Although the recurrence rate for the solitary osteochondroma in long bones is 2% 5,6 and 1. Karras SC, Wolford LM, Cottrell DA. Concurrent osterchondroma of the mandible condyle and ipsilateral cranial base resulting in TMJ ankylosis. Report of a case and review of the literature. J Oral Maxillofac Surg 1996; 54: Ord RA, Warburton G, Caccamese JF. Osteochondroma of the condyle: review of 8 cases. Int J Oral Maxillofac Surg 2010;39: Roychoudhury A, Bhatt K, Yadav R, Bhutia O, Roychoudhury S. Review of osteochondroma of mandibular condyle and report of a case series. J Oral Maxillofac Surg 2011;69: Yang X, Hu J, Zhu S, Liang X, Li J, Luo E. Computer-assisted surgical planning and simulation for condylar reconstruction in patients with osteochondroma. Br J Oral Maxillofac Surg 2011;49: Wolford LM, Mehra P, Franco P. Use of conservative condylectomy for treatment of osteochondroma of the mandibular condyle. J Oral Maxillofac Surg 2002;60: Cottrell DA. Discussion: use of conservative condylectomy for treatment of osterchondroma of the mandible condyle. J Oral Maxillofac Surg 2002; 60: Iizuka T, Schroth G, Laeng RH, L adrach K. Osteochondroma of the mandibular condyle: report of a case. J Oral Maxillofac Surg 1996;54: Koole R, Steenks MH, Witkamp TD, Slootweg PJ, Shaefer J. Osteochondroma of the mandibular condyle. A case report. Int J Oral Maxillofac Surg 1996;25: Rivera H, Bastidas R, Acevedo AM. A conservative surgical approach of osteochondroma affecting the mandibular condyle. Invest Clin 1998;39: Kurita K, Ogi N, Echiverre NV, Yoshida K. Osteochondroma of the mandibular condyle. A case report. Int J Oral Maxillofac Surg 1999;28: Aydin MA, Küçükçelebi A, Sayilkan S, Celebioğlu S. Osteochondroma of the mandibular condyle: report of 2 cases treated with conservative surgery. J Oral Maxillofac Surg 2001;59: Vezeau PJ, Fridrich KL, Vincent SD. Literature review and report of two atypical cases. J Oral Maxillofac Surg 1995;53: Kumar VV. Large osteochondroma of the mandibular condyle treated by condylectomy using a transzygomatic approach. Int J Oral Maxillofac Surg 2010;39: Ortakoglu K, Akcam T, Sencimen M, Karakoc O, Ozyigit HA, Bengi O. Osteochondroma of the mandible causing severe facial asymmetry: a case 278 HEAD & NECK DOI /HED FEBRUARY 2014
7 FEASIBILITY AND INDICATIONS OF THE LOCAL RESECTION report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007;103: e21 e Koga M, Toyofuku S, Nakamura Y, Yoshiura K, Kusukawa J, Nakamura Y. Osteochondroma in the mandibular condyle that caused facial asymmetry: a case report. Cranio 2006;24: Cimino R, Steenks MH, Michelotti A, Farella M, PierFrancesco N. Mandibular condyle osteochondroma. Review of the literature and report of a misdiagnosed case. J Orofac Pain 2003;17: Saito T, Utsunomiya T, Furutani M, Yamamoto H. Osteochondroma of the mandibular condyle: a case report and review of the literature. J Oral Sci 2001;43: Gonzalez-Otero S, Navarro-Cuellar C, Escrig-de Teigeiro M, Fernandez- Alba-Luengo J, Navarro-Vila C. Osteochondroma of the mandibular condyle: resection and reconstruction using vertical sliding osteotomy of the mandibular ramus. Med Oral Patol Oral Cir Bucal 2009;14: E194 E Ribas Mde O, Martins WD, de Sousa MH, Zanferrari FL, Lanzoni T. Osteochondroma of the mandibular condyle: literature review and report of a case. J Contemp Dent Pract 2007;8: Holmlund AB, Gynther GW, Reinholt FP. Surgical treatment of osteochondroma of the mandibular condyle in the adult. A 5-year follow-up. Int J Oral Maxillofac Surg 2004;33: Martinez-Lage JL, Gonzalez J, Pineda A, Alvarez I. Condylar reconstruction by oblique sliding vertical-ramus osteotomy. J Craniomaxillofac Surg 2004;32: Gingrass DJ, Sadeghi EM. Osteochondroma of the mandibular condyle mimicking TMJ syndrome: clinical and therapeutic appraisal of a case. J Orofac Pain 1993;7: Seki H, Fukuda M, Takahashi T, Iino M. Condylar osteochondroma with complete hearing loss: report of a case. J Oral Maxillofac Surg 2003;61: Peroz I, Scholman HJ, Hell B. Osteochondroma of the mandibular condyle: a case report. Int J Oral Maxillofac Surg 2002;31: HEAD & NECK DOI /HED FEBRUARY
Osteochondroma of Mandibular condyle: Review of the literature and case Report
 American Journal of Advances in Medical Science www.arnaca.com eissn: 2347-2766 Case Report Ajaz Shah 1, Afreen Nadaf 2, Shahid Hassan 1*, Irshad Ahmad 1, Syed Wakeel 1 1 Department of Oral and Maxillofacial
American Journal of Advances in Medical Science www.arnaca.com eissn: 2347-2766 Case Report Ajaz Shah 1, Afreen Nadaf 2, Shahid Hassan 1*, Irshad Ahmad 1, Syed Wakeel 1 1 Department of Oral and Maxillofacial
Osteochondroma of the mandibular condyle cured by conservative resection
 Journal of Dental Sciences (2014) 9, 91e95 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Osteochondroma of the mandibular condyle cured by conservative resection
Journal of Dental Sciences (2014) 9, 91e95 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Osteochondroma of the mandibular condyle cured by conservative resection
Osteochondroma of the mandibular condyle: A case report
 www.edoriumjournals.com case REPORT PEER REVIEWED OPEN ACCESS Osteochondroma of the mandibular condyle: A case report Jayakumar K., Soumithran C.S., Manoj Joseph Michael, Pallav Kumar Kinra, Ambadas Kulkarni,
www.edoriumjournals.com case REPORT PEER REVIEWED OPEN ACCESS Osteochondroma of the mandibular condyle: A case report Jayakumar K., Soumithran C.S., Manoj Joseph Michael, Pallav Kumar Kinra, Ambadas Kulkarni,
A case report of osteochondroma of the mandibular condyle
 Derya et al. 1 case report peer Reviewed open OPEN ACCESS A case report of osteochondroma of the mandibular condyle Icoz Derya, Akgunlu Faruk, Demir Esin, Karabağlı Pınar, Ozturk Kayhan Abstract Introduction:
Derya et al. 1 case report peer Reviewed open OPEN ACCESS A case report of osteochondroma of the mandibular condyle Icoz Derya, Akgunlu Faruk, Demir Esin, Karabağlı Pınar, Ozturk Kayhan Abstract Introduction:
Recurrent osteochondroma of the mandibular condyle: A case report
 Imaging Science in Dentistry 2017; 47: 57-62 https://doi.org/10.5624/isd.2017.47.1.57 Recurrent osteochondroma of the mandibular condyle: case report Young-Eun Kwon 1, Karp-Shik Choi 1, Chang-Hyeon n 1,
Imaging Science in Dentistry 2017; 47: 57-62 https://doi.org/10.5624/isd.2017.47.1.57 Recurrent osteochondroma of the mandibular condyle: case report Young-Eun Kwon 1, Karp-Shik Choi 1, Chang-Hyeon n 1,
Intraoral mandibular distraction osteogenesis in facial asymmetry patients with unilateral temporomandibular joint bony ankylosis
 Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Original Article Factors affecting the outcomes of non-surgical treatment for intracapsular condylar fractures
 Int J Clin Exp Med 2016;9(6):10847-10855 www.ijcem.com /ISSN:1940-5901/IJCEM0021362 Original Article Factors affecting the outcomes of non-surgical treatment for intracapsular condylar fractures Bao-Li
Int J Clin Exp Med 2016;9(6):10847-10855 www.ijcem.com /ISSN:1940-5901/IJCEM0021362 Original Article Factors affecting the outcomes of non-surgical treatment for intracapsular condylar fractures Bao-Li
Osteocartilagenous Exostosis of Mandibular Condyle: A Rarity that is Explored!!: Case Report
 I J Pre Clin Dent Res 2015;2(4):84-88 Oct-Dec All rights reserved International Journal of Preventive & Clinical Dental Research Osteocartilagenous Exostosis of Mandibular Condyle: A Rarity that is Explored!!:
I J Pre Clin Dent Res 2015;2(4):84-88 Oct-Dec All rights reserved International Journal of Preventive & Clinical Dental Research Osteocartilagenous Exostosis of Mandibular Condyle: A Rarity that is Explored!!:
Early View Article: Online published version of an accepted article before publication in the final form.
 Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Dentistry Type of Article: Case Report Title:
Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Dentistry Type of Article: Case Report Title:
Unusual Solitary Osteoma Coronoid Process And Aesthetic Facial Correction
 ISPUB.COM The Internet Journal of Head and Neck Surgery Volume 3 Number 2 Unusual Solitary Osteoma Coronoid Process And Aesthetic Facial Correction Z Núñez-Gil Citation Z Núñez-Gil.. The Internet Journal
ISPUB.COM The Internet Journal of Head and Neck Surgery Volume 3 Number 2 Unusual Solitary Osteoma Coronoid Process And Aesthetic Facial Correction Z Núñez-Gil Citation Z Núñez-Gil.. The Internet Journal
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization
 Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi. E. mail:
 The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The mandibular condyle fracture is a common mandibular
 ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle
 Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
The America Association of Oral and Maxillofacial Surgeons classify occlusion/malocclusion in to the following three categories:
 Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Osteoma of Mandibular Condyle as Ca Title Pain and Limited-mouth-opening: Cas. Yonezu, H; Wakoh, M; Otonari, T; Sa Author(s) Hashimoto, S; Uchiyama, T
 Osteoma of Mandibular Condyle as Ca Title Pain and Limited-mouth-opening: Cas Yonezu, H; Wakoh, M; Otonari, T; Sa Author(s) Hashimoto, S; Uchiyama, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/417
Osteoma of Mandibular Condyle as Ca Title Pain and Limited-mouth-opening: Cas Yonezu, H; Wakoh, M; Otonari, T; Sa Author(s) Hashimoto, S; Uchiyama, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/417
Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient with facial asymmetry
 CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.1.32 pissn 2234-7550 eissn 2234-5930 Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient
CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.1.32 pissn 2234-7550 eissn 2234-5930 Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Synovial Chondromatosis of the Temporomandibular Joint: Long-Term Postoperative Follow-Up of the Residual Calcification
 J Med Dent Sci 2003; 50: 133 137 Case Report Synovial Chondromatosis of the Temporomandibular Joint: Long-Term Postoperative Follow-Up of the Residual Calcification Junichi Ishii 1, Koji Kino 2, Junji
J Med Dent Sci 2003; 50: 133 137 Case Report Synovial Chondromatosis of the Temporomandibular Joint: Long-Term Postoperative Follow-Up of the Residual Calcification Junichi Ishii 1, Koji Kino 2, Junji
Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty
 Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty Abstract A case of true bilateral ankylosis of the temporomandibular joint (TMJ)
Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty Abstract A case of true bilateral ankylosis of the temporomandibular joint (TMJ)
Case Report Digital resection and reconstruction of TMJ synovial chondrosarcoma involving the skull base: report of a case
 Int J Clin Exp Med 2015;8(7):11589-11593 www.ijcem.com /ISSN:1940-5901/IJCEM0010297 Case Report Digital resection and reconstruction of TMJ synovial chondrosarcoma involving the skull base: report of a
Int J Clin Exp Med 2015;8(7):11589-11593 www.ijcem.com /ISSN:1940-5901/IJCEM0010297 Case Report Digital resection and reconstruction of TMJ synovial chondrosarcoma involving the skull base: report of a
MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS. FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy
 MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy MBBS MDS FDSRCS (Edin) FDSRCS (Eng) PhD Dr. Dr. Rajgopal Reddy
MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy MBBS MDS FDSRCS (Edin) FDSRCS (Eng) PhD Dr. Dr. Rajgopal Reddy
Research report for MSc Dent. University of Witwatersrand. Faculty of health science. Dr J Beukes. Student number: h
 Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Simultaneous gap arthroplasty and intraoral distraction and secondary contouring surgery for unilateral temporomandibular joint ankylosis
 Sharma et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:12 DOI 10.1186/s40902-016-0058-0 CASE REPORT Open Access Simultaneous gap arthroplasty and intraoral distraction and secondary contouring
Sharma et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:12 DOI 10.1186/s40902-016-0058-0 CASE REPORT Open Access Simultaneous gap arthroplasty and intraoral distraction and secondary contouring
3. The Jaw and Related Structures
 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery
 European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
Oral & Maxillofacial Surgery
 Chapter 2 Oral & Maxillofacial Surgery Ruchi Singhal 1 ; Virendra Singh 2 ; Amrish Bhagol* 1 Jaipur Dental College, Jaipur, India 2 Senior Professor, PGIDS, Rohtak, India Amrish Bhagol Condylar Fractures
Chapter 2 Oral & Maxillofacial Surgery Ruchi Singhal 1 ; Virendra Singh 2 ; Amrish Bhagol* 1 Jaipur Dental College, Jaipur, India 2 Senior Professor, PGIDS, Rohtak, India Amrish Bhagol Condylar Fractures
TRIFID MANDIBULAR CONDYLE: REPORT OF A RARE CASE
 TRIFID MANDIBULAR CONDYLE: REPORT OF A RARE CASE Khushboo Singh, MDS 1, Dr. Sujata Mohanty, MDS 2, Mahesh Verma, MDS, MBA, PhD 3, Sunita Gupta, MDS, MBA (HCA) 4, Sujoy Ghosh, MDS 5, and Meera Choudhary,
TRIFID MANDIBULAR CONDYLE: REPORT OF A RARE CASE Khushboo Singh, MDS 1, Dr. Sujata Mohanty, MDS 2, Mahesh Verma, MDS, MBA, PhD 3, Sunita Gupta, MDS, MBA (HCA) 4, Sujoy Ghosh, MDS 5, and Meera Choudhary,
Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study
 Regeneration, Reconstruction & Restoration Reconstruction Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study Mohammad Taghi Kiani a*, Mohammad Bayat b, Maryam Ajami
Regeneration, Reconstruction & Restoration Reconstruction Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study Mohammad Taghi Kiani a*, Mohammad Bayat b, Maryam Ajami
Temporomandibular joint reconstruction with alloplastic prosthesis: the outcomes of four cases
 Park et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:6 DOI 10.1186/s40902-017-0103-7 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Temporomandibular joint reconstruction
Park et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:6 DOI 10.1186/s40902-017-0103-7 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Temporomandibular joint reconstruction
ORTHOGNATHIC SURGERY
 ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
Original Article Analysis of neurologic complications after modified temporomandibular joint disc anchorage surgery
 Int J Clin Exp Med 2017;10(3):5440-5444 www.ijcem.com /ISSN:1940-5901/IJCEM0041511 Original Article Analysis of neurologic complications after modified temporomandibular joint disc anchorage surgery Jin-Ze
Int J Clin Exp Med 2017;10(3):5440-5444 www.ijcem.com /ISSN:1940-5901/IJCEM0041511 Original Article Analysis of neurologic complications after modified temporomandibular joint disc anchorage surgery Jin-Ze
Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor
 Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Q2Q3 Reza Movahed, DMD a, *, Larry Wolford, DMD b,c. oralmaxsurgery.theclinics.com KEYWORDS KEY POINTS
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 56 Protocol for Concomitant Temporomandibular
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 56 Protocol for Concomitant Temporomandibular
Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report
 Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report Abstract When diagnosing patients with temporomandibular disorder (TMD) symptoms, the possibility of unusual causes
Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report Abstract When diagnosing patients with temporomandibular disorder (TMD) symptoms, the possibility of unusual causes
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Original Article Three-dimensional printing automatic registration navigational template for mandibular angle osteotomy surgery
 Int J Clin Exp Med 2016;9(7):13065-13069 www.ijcem.com /ISSN:1940-5901/IJCEM0021585 Original Article Three-dimensional printing automatic registration navigational template for mandibular angle osteotomy
Int J Clin Exp Med 2016;9(7):13065-13069 www.ijcem.com /ISSN:1940-5901/IJCEM0021585 Original Article Three-dimensional printing automatic registration navigational template for mandibular angle osteotomy
Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy
 1 Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy J. Beukes 1,, J. P. Reyneke 1,2,3,4, P. J. Becker 5,6
1 Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy J. Beukes 1,, J. P. Reyneke 1,2,3,4, P. J. Becker 5,6
Interesting Case Series. Virtual Surgical Planning in Orthognathic Surgery
 Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
ORTHOGNATHIC SURGERY
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Changes in the temporomandibular joint after mandibular lengthening with different rates of distraction
 Shujuan Zou, DDS, MS Department of Orthodontics Jing Hu, DDS, MS, PhD Dazhang Wang, DDS, FICD Jihua Li, DDS, MS Zhenglong Tang, DDS, MS Department of Oral and Maxillofacial Surgery Huaxi School of Stomatology
Shujuan Zou, DDS, MS Department of Orthodontics Jing Hu, DDS, MS, PhD Dazhang Wang, DDS, FICD Jihua Li, DDS, MS Zhenglong Tang, DDS, MS Department of Oral and Maxillofacial Surgery Huaxi School of Stomatology
Reconstruction of large mandibular defects
 Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Orthodontics-surgical combination therapy for Class III skeletal malocclusion
 [Downloaded free from http://www.contempclindent.org on Tuesday, July 16, 2013, IP: 164.100.31.82] Click here to download free Android application for this jou Orthodontics-surgical combination therapy
[Downloaded free from http://www.contempclindent.org on Tuesday, July 16, 2013, IP: 164.100.31.82] Click here to download free Android application for this jou Orthodontics-surgical combination therapy
Navigation-Guided Lateral Gap Arthroplasty as the Treatment of Temporomandibular Joint Ankylosis
 CRANIOMAXILLOFACIAL DEFORMITIES/COSMETIC SURGERY Navigation-Guided Lateral Gap Arthroplasty as the Treatment of Temporomandibular Joint Ankylosis Haijun Gui, MD, DDS,* Jinyang Wu, DDS,y Steve G. F. Shen,
CRANIOMAXILLOFACIAL DEFORMITIES/COSMETIC SURGERY Navigation-Guided Lateral Gap Arthroplasty as the Treatment of Temporomandibular Joint Ankylosis Haijun Gui, MD, DDS,* Jinyang Wu, DDS,y Steve G. F. Shen,
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL
 What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y
 TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y Cranio : the journal of craniomandi Journal 20(1): 67-71 URL http://hdl.handle.net/10130/1098 Right
TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y Cranio : the journal of craniomandi Journal 20(1): 67-71 URL http://hdl.handle.net/10130/1098 Right
Oral cavity landmarks
 By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
Journal of Cranio-Maxillo-Facial Surgery
 Journal of Cranio-Maxillo-Facial Surgery 42 (2014) 1078e1082 Contents lists available at SciVerse ScienceDirect Journal of Cranio-Maxillo-Facial Surgery journal homepage: www.jcmfs.com A retrospective
Journal of Cranio-Maxillo-Facial Surgery 42 (2014) 1078e1082 Contents lists available at SciVerse ScienceDirect Journal of Cranio-Maxillo-Facial Surgery journal homepage: www.jcmfs.com A retrospective
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Temporomandibular Joint. Dr Noman ullah wazir
 Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
Correction of Dentofacial Deformities (Orthognathic Surgery)
 Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
An Isolated, Giant Infratemporal Fossa Schwannoma: Removal By Transmandibular Transpterygoid Approach
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 5 Number 2 An Isolated, Giant Infratemporal Fossa Schwannoma: Removal By Transmandibular Transpterygoid Rijuneeta, P Kumar Parida, V Mshesha,
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 5 Number 2 An Isolated, Giant Infratemporal Fossa Schwannoma: Removal By Transmandibular Transpterygoid Rijuneeta, P Kumar Parida, V Mshesha,
Patient information booklet Orthognathic Surgery
 Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
Topic: Orthognathic Surgery Date of Origin: October 5, Section: Surgery Last Reviewed Date: December 2013
 Medical Policy Manual Topic: Orthognathic Surgery Date of Origin: October 5, 2004 Section: Surgery Last Reviewed Date: December 2013 Policy No: 137 Effective Date: March 1, 2014 IMPORTANT REMINDER Medical
Medical Policy Manual Topic: Orthognathic Surgery Date of Origin: October 5, 2004 Section: Surgery Last Reviewed Date: December 2013 Policy No: 137 Effective Date: March 1, 2014 IMPORTANT REMINDER Medical
Case Report Decompression of the inferior alveolar nerve to treat the pain of the mandible caused by fibrous dysplasia-case report
 Int J Clin Exp Med 2015;8(10):19535-19539 www.ijcem.com /ISSN:1940-5901/IJCEM0014642 Case Report Decompression of the inferior alveolar nerve to treat the pain of the mandible caused by fibrous dysplasia-case
Int J Clin Exp Med 2015;8(10):19535-19539 www.ijcem.com /ISSN:1940-5901/IJCEM0014642 Case Report Decompression of the inferior alveolar nerve to treat the pain of the mandible caused by fibrous dysplasia-case
2018 Dental Code Set For dates of service from 1/1/ /31/2018
 D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
2018 Dental Code Set
 D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Muscles of mastication [part 1]
![Muscles of mastication [part 1] Muscles of mastication [part 1]](/thumbs/76/73586850.jpg) Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Magnetic resonance imaging assessment of temporomandibular joint soft tissue injuries of intracapsular condylar fracture,
 Available online at www.sciencedirect.com British Journal of Oral and Maxillofacial Surgery 51 (2013) 133 137 Magnetic resonance imaging assessment of temporomandibular joint soft tissue injuries of intracapsular
Available online at www.sciencedirect.com British Journal of Oral and Maxillofacial Surgery 51 (2013) 133 137 Magnetic resonance imaging assessment of temporomandibular joint soft tissue injuries of intracapsular
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Outcomes of surgical versus nonsurgical treatment of mandibular condyle fractures
 International Surgery Journal Ragupathy K. Int Surg J. 2016 Feb;3(1):47-51 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151508
International Surgery Journal Ragupathy K. Int Surg J. 2016 Feb;3(1):47-51 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151508
The Temporomandibular joint: Anatomy, Mechanics, Pathology. Aditya Bahel, DO
 The Temporomandibular joint: Anatomy, Mechanics, Pathology Aditya Bahel, DO Outline Anatomy Mechanics and function Indications for TMJ imaging MR Protocols and pitfalls Pathology Treatment options Anatomy
The Temporomandibular joint: Anatomy, Mechanics, Pathology Aditya Bahel, DO Outline Anatomy Mechanics and function Indications for TMJ imaging MR Protocols and pitfalls Pathology Treatment options Anatomy
MAHP Orthognathic Surgery Guidelines. Medical Policy Statement. Criteria
 Introduction The word orthognathic comes from the Greek words for straighten and jaw. Orthognathic surgery is the surgical correction of abnormalities of the mandible and/or maxilla. 1 It involves the
Introduction The word orthognathic comes from the Greek words for straighten and jaw. Orthognathic surgery is the surgical correction of abnormalities of the mandible and/or maxilla. 1 It involves the
Facelift approach for mandibular resection and reconstruction
 ORIGINAL ARTICLE Facelift approach for mandibular resection and reconstruction Bernardo Bianchi, MD, Andrea Ferri, MD, * Silvano Ferrari, MD, Chiara Copelli, MD, Enrico Sesenna, MD Maxillo-Facial Surgery
ORIGINAL ARTICLE Facelift approach for mandibular resection and reconstruction Bernardo Bianchi, MD, Andrea Ferri, MD, * Silvano Ferrari, MD, Chiara Copelli, MD, Enrico Sesenna, MD Maxillo-Facial Surgery
Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap.
 Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note
 Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
Condylar Movement Assessment is Severe Attrition Patient Undergoing Orthodontic Treatment: Joint Vibrant Analysis Procedure
 Case Report imedpub Journals http://www.imedpub.com Journal of Dental and Craniofacial Research DOI: 10.21767/2576-392X.100004 Condylar Movement Assessment is Severe Attrition Patient Undergoing Orthodontic
Case Report imedpub Journals http://www.imedpub.com Journal of Dental and Craniofacial Research DOI: 10.21767/2576-392X.100004 Condylar Movement Assessment is Severe Attrition Patient Undergoing Orthodontic
Condylar positioning changes following unilateral sagittal split ramus osteotomy in patients with mandibular prognathism
 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:36 DOI 10.1186/s40902-015-0036-y CASE REPORT Open Access Condylar positioning changes following unilateral sagittal split ramus osteotomy
Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:36 DOI 10.1186/s40902-015-0036-y CASE REPORT Open Access Condylar positioning changes following unilateral sagittal split ramus osteotomy
Qestions often arise regarding the appropriate
 CLINICAL REVIEW C E Considerations for orthognathic surgery during growth, Part 1: Mandibular deformities Larry M. Wolford, DMD, a Spiro C. Karras, DDS, b and Pushkar Mehra, DMD c Dallas, Tex Management
CLINICAL REVIEW C E Considerations for orthognathic surgery during growth, Part 1: Mandibular deformities Larry M. Wolford, DMD, a Spiro C. Karras, DDS, b and Pushkar Mehra, DMD c Dallas, Tex Management
Bones Ethmoid bone Inferior nasal concha Lacrimal bone Maxilla Nasal bone Palatine bone Vomer Zygomatic bone Mandible
 splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
Sample Case #1. Disclaimer
 ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
The Melbourne Temporomandibular Total Joint Replacement System
 The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
Total Prosthetic Replacement of the Temporomandibular Joint (TMJ)
 Total Prosthetic Replacement of the Temporomandibular Joint (TMJ) VERSION CONTROL Version: 2.0 Ratified by: Governing Body Date ratified: 13 November 2013 Name of originator/author: Name of responsible
Total Prosthetic Replacement of the Temporomandibular Joint (TMJ) VERSION CONTROL Version: 2.0 Ratified by: Governing Body Date ratified: 13 November 2013 Name of originator/author: Name of responsible
Treatment of Chronic Mandibular Dislocations: A Comparison Between Eminectomy and Miniplates
 J Oral Maxillofac Surg 67:2599-2604, 2009 Treatment of Chronic Mandibular Dislocations: A Comparison Between Eminectomy and Miniplates Belmiro Cavalcanti do Egito Vasconcelos, DDS, PhD,* and Gabriela Granja
J Oral Maxillofac Surg 67:2599-2604, 2009 Treatment of Chronic Mandibular Dislocations: A Comparison Between Eminectomy and Miniplates Belmiro Cavalcanti do Egito Vasconcelos, DDS, PhD,* and Gabriela Granja
The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting
 44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document.
 ORTHOGNATHIC SURGERY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
ORTHOGNATHIC SURGERY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Clinical evaluation of temporomandibular joint disorder after orthognathic surgery in skeletal class II malocclusion patients
 ORIGINAL ARTICLE http://dx.doi.org/10.5125/jkaoms.2012.38.3.139 pissn 22347550 eissn 22345930 Clinical evaluation of temporomandibular joint disorder after orthognathic surgery in skeletal class II malocclusion
ORIGINAL ARTICLE http://dx.doi.org/10.5125/jkaoms.2012.38.3.139 pissn 22347550 eissn 22345930 Clinical evaluation of temporomandibular joint disorder after orthognathic surgery in skeletal class II malocclusion
TEMPORO-MANDIBULAR JOINT DISORDERS
 Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Mixed-reality simulation for orthognathic surgery
 Fushima and Kobayashi Maxillofacial Plastic and Reconstructive Surgery (2016) 38:13 DOI 10.1186/s40902-016-0059-z METHODOLOGY Mixed-reality simulation for orthognathic surgery Kenji Fushima 1* and Masaru
Fushima and Kobayashi Maxillofacial Plastic and Reconstructive Surgery (2016) 38:13 DOI 10.1186/s40902-016-0059-z METHODOLOGY Mixed-reality simulation for orthognathic surgery Kenji Fushima 1* and Masaru
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
Surgically assisted rapid palatal expansion (SARPE) prior to combined Le Fort I and sagittal osteotomies: A case report
 200 Carlos Alberto E. Tavares, DDS, MS, DOrth Professor Department of Orthodontics Associação Brasileira de Odontologia - RS Porto Alegre, Brazil Miguel Scheffer, DDS, MS Chairman Department of Oral and
200 Carlos Alberto E. Tavares, DDS, MS, DOrth Professor Department of Orthodontics Associação Brasileira de Odontologia - RS Porto Alegre, Brazil Miguel Scheffer, DDS, MS Chairman Department of Oral and
Bone scintigraphy of human temporomandibular joints during Herbst treatment: a case report
 European Journal of Orthodontics 20 (1998) 369-374 1998 European Orthodontic Society Bone scintigraphy of human temporomandibular joints during Herbst treatment: a case report H. U. Paulsen, A. Habel and
European Journal of Orthodontics 20 (1998) 369-374 1998 European Orthodontic Society Bone scintigraphy of human temporomandibular joints during Herbst treatment: a case report H. U. Paulsen, A. Habel and
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
Case Report A ring-like soft tissue osteoma in the temporomandibular joint capsule: case report
 Int J Clin Exp Med 2019;12(2):1992-1996 www.ijcem.com /ISSN:1940-5901/IJCEM0086715 Case Report A ring-like soft tissue osteoma in the temporomandibular joint capsule: case report Xu-Zhuo Chen 1*, Abdelrehem
Int J Clin Exp Med 2019;12(2):1992-1996 www.ijcem.com /ISSN:1940-5901/IJCEM0086715 Case Report A ring-like soft tissue osteoma in the temporomandibular joint capsule: case report Xu-Zhuo Chen 1*, Abdelrehem
KEY WORDS: orthognathic surgery, mandibular condylar hyperplasia, condylectomy, facial asymmetry.
 Int. J. Odontostomat., 10(2):207-213, 2016. Surgical Treatment of Condylar Hyperplasia Associated with Dentofacial Deformity: Low Condylectomy, Articular Disc Repositioning, and Orthognathic Surgery Tratamiento
Int. J. Odontostomat., 10(2):207-213, 2016. Surgical Treatment of Condylar Hyperplasia Associated with Dentofacial Deformity: Low Condylectomy, Articular Disc Repositioning, and Orthognathic Surgery Tratamiento
Postoperative mandibular stability after orthognathic surgery in patients with mandibular protrusion and mandibular deviation
 Wenli Lai, DDS, PhD Lecturer Department of Orthodontics West China College of Stomatology Sichuan University Chengdu, China Kazuhiro Yamada, DDS, PhD Lecturer Division of Orthodontics Department of Oral
Wenli Lai, DDS, PhD Lecturer Department of Orthodontics West China College of Stomatology Sichuan University Chengdu, China Kazuhiro Yamada, DDS, PhD Lecturer Division of Orthodontics Department of Oral
Severe Malocclusion: Appropriately Timed Treatment. This article discusses challenging issues clinicians face when treating
 Severe Malocclusion: The Importance of Appropriately Timed Treatment A Synchronized and Simultaneous Interdisciplinary Plan Using Cosmetic Dentistry Principles David M. Sarver, DMD, MS Abstract This article
Severe Malocclusion: The Importance of Appropriately Timed Treatment A Synchronized and Simultaneous Interdisciplinary Plan Using Cosmetic Dentistry Principles David M. Sarver, DMD, MS Abstract This article
Parotid Gland, Temporomandibular Joint and Infratemporal Fossa
 M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
Osteomas of the craniofacial region
 Imaging Science in Dentistry 2011; 41 : 107-13 http://dx.doi.org/10.5624/isd.2011.41.3.107 Department of Oral and Maxillofacial Radiology, School of Dentistry, Pusan National University, usan, Korea STRCT
Imaging Science in Dentistry 2011; 41 : 107-13 http://dx.doi.org/10.5624/isd.2011.41.3.107 Department of Oral and Maxillofacial Radiology, School of Dentistry, Pusan National University, usan, Korea STRCT
Scholars Journal of Medical Case Reports
 DOI: 10.21276/sjmcr.2016.4.11.17 Scholars Journal of Medical Case Reports Sch J Med Case Rep 2016; 4(11):863-868 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher
DOI: 10.21276/sjmcr.2016.4.11.17 Scholars Journal of Medical Case Reports Sch J Med Case Rep 2016; 4(11):863-868 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher
Concomitant Temporomandibular Joint and Orthognathic Surgery
 CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 61:1198-1204, 2003 Concomitant Temporomandibular Joint and Orthognathic Surgery Larry M. Wolford, DMD* *Clinical
CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 61:1198-1204, 2003 Concomitant Temporomandibular Joint and Orthognathic Surgery Larry M. Wolford, DMD* *Clinical
Dislocation of the temporomandibular joint occurs when
 Rev Bras Otorrinolaringol. V.71, n.1, 32-7, jan./feb. 2005 ARTIGO ORIGINAL ORIGINAL ARTICLE Comparative study of eminectomy and use of bone miniplate in the articular eminence for the treatment of recurrent
Rev Bras Otorrinolaringol. V.71, n.1, 32-7, jan./feb. 2005 ARTIGO ORIGINAL ORIGINAL ARTICLE Comparative study of eminectomy and use of bone miniplate in the articular eminence for the treatment of recurrent
Stability and Relapse in Orthognathic Surgery
 Stability and Relapse in Orthognathic Surgery Neeraj Panchal, DDS, MD, MA Christine Ellis, DDS, MSD Paul Tiwana, DDS, MD, MS, FACS INTRODUCTION The long-term success of orthognathic reconstructive surgery
Stability and Relapse in Orthognathic Surgery Neeraj Panchal, DDS, MD, MA Christine Ellis, DDS, MSD Paul Tiwana, DDS, MD, MS, FACS INTRODUCTION The long-term success of orthognathic reconstructive surgery
06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.]
![06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.] 06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.]](/thumbs/84/91182117.jpg) Reference #: MC/B002 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS)
Reference #: MC/B002 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS)
Jaw locking after maxillofacial trauma
 106 Jaw locking after maxillofacial trauma David B. Kamadjaja and R. Soesanto Department of Oral and Maxillofacial Surgery Faculty of Dentistry Airlangga University Surabaya - Indonesia abstract The purpose
106 Jaw locking after maxillofacial trauma David B. Kamadjaja and R. Soesanto Department of Oral and Maxillofacial Surgery Faculty of Dentistry Airlangga University Surabaya - Indonesia abstract The purpose
NC Medicaid Dental Reimbursement Rates General Dentist, Oral Surgeon, Pediatric Dentist, Periodontist, & Orthodontist Effective Date: January 1, 2017
 NC Dental Reimbursement s Refer to the NC and Health Choice Clinical Coverage Policies on the DMA website. D0120 Periodic oral evaluation 24.51 D0140 Limited oral evaluation - problem focused 34.94 D0145
NC Dental Reimbursement s Refer to the NC and Health Choice Clinical Coverage Policies on the DMA website. D0120 Periodic oral evaluation 24.51 D0140 Limited oral evaluation - problem focused 34.94 D0145
A Rare Case of Cheerleader Syndrome, Case Report
 47 A Rare Case of Cheerleader Syndrome, Case Report Dr. Ayad AL mudarris, FIBMS (1) and Dr. Shifaa Hussain, MSc (2) (1)Head of Maxillofacial Surgical Department. Al Imamain Al Kadhemain Medical City; (2)
47 A Rare Case of Cheerleader Syndrome, Case Report Dr. Ayad AL mudarris, FIBMS (1) and Dr. Shifaa Hussain, MSc (2) (1)Head of Maxillofacial Surgical Department. Al Imamain Al Kadhemain Medical City; (2)
SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 02 SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT Amit Dahiya 1,Minakshi
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 02 SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT Amit Dahiya 1,Minakshi
