Treatment of periprosthetic femoral fractures after femoral revision using a long stem
|
|
|
- Eustace Cooper
- 5 years ago
- Views:
Transcription
1 Kim et al. BMC Musculoskeletal Disorders (2015) 16:113 DOI /s RESEARCH ARTICLE Open Access Treatment of periprosthetic femoral fractures after femoral revision using a long Youngwoo Kim *, Chiaki Tanaka, Hiroshi Tada, Hiroshi Kanoe and Takaaki Shirai Abstract Background: Periprosthetic femoral fractures are becoming increasingly common and are a major complication of total hip arthroplasty and hemiarthroplasty. The treatment of periprosthetic femoral fracture after femoral revision using a long is more complex and challenging. The purpose of this study was to identify the clinical and radiographical features of periprosthetic femoral fractures after revision using a long. Methods: We report a retrospective review of the outcomes of treatment of 11 periprosthetic fractures after femoral revision using a long. Eleven female patients with a mean age of 79.2 years (70 to 91) were treated for a Vancouver type B1 fracture between 1998 and The mean numbers of previous surgeries were 3.1 (2 to 5). Results: The average follow-up was 58.9 months (8 to 180). We found several important features that might influence the outcome of treatment for periprosthetic femoral fractures after femoral revision using a long : 1) all cases were classified as Vancouver type B1. 2) 6 patients (55%) had a transverse fracture around the tip of the long. 3) 7 patients (64%) had a history of previous fracture of the ipsilateral femur. The type B1 fractures were treated with open reduction and internal fixation in 9 hips, 6 of which were reinforced with bone grafts. Two other periprosthetic fractures were treated with femoral revision. One was revised because of breakage, and the other was a transverse fracture associated with poor bone quality, which received a femoral revision with a long and a plate. All fractures except one achieved primary union. This failed case had a bone defect at the fracture site, and revision surgery using a cementless long and allografts was successful. Conclusions: These findings suggest that most cases of type B1 fracture after revision using a long have been treated successfully with open reduction and internal fixation. However, a transverse fracture with very poor bone quality might be considered as a type B3 fracture, and femoral revision might be a treatment of choice. Keywords: Total hip arthroplasty, Revision, Periprosthetic fracture, Long Background During the past decade, the number of patients requiring total hip arthroplasty (THA) has increased steadily in both younger patients and the more active elderly population [1]. There has been also a marked increase in hemiarthroplasty (HA) as treatment for femoral neck fractures [2]. Subsequently, periprosthetic femoral fractures are also becoming increasingly frequent and are a major complication of THA and HA [1,3,4]. A recent study showed that the incidence of periprosthetic femoral fracture is about 1% after primary THA and 4.2% after revision THA [5,6]. Periprosthetic fractures are also * Correspondence: woochan76@hotmail.co.jp Department of Orthopaedic Surgery, Kyoto City Hospital, 1-2 Mibu,higashitakada-cho, Nakagyo, Kyoto , Japan more common in patients who have sustained a hip fracture before arthroplasty [7]. The treatment of these fractures is complex and challenging, and requires the skills of both trauma surgery and revision arthroplasty [8]. The Vancouver classification developed by Duncan and Masri has become the universally accepted classification and has been validated recently in the European setting [9,10]. The site of the fracture, stability of the prosthesis, and the quality of bone stock are the three most important parameters used in the Vancouver classification to guide the surgeon in making a decision about the treatment of these fractures. Treatment is made more difficult by comorbid factors such as fragility or severe osteoporosis in elderly patients [11] Kim et al.; licensee BioMed Central. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Kim et al. BMC Musculoskeletal Disorders (2015) 16:113 Page 2 of 7 The risk factors for periprosthetic femoral fracture include poor bone stock, age, chronic use of corticosteroid, inflammatory arthropathy, stress risers, whether iatrogenic or caused by local osteolysis, previously surgery, excessively stiff joints, and various neurological conditions [1,6,12,13]. Because of the increase in the incidence of arthroplasty and life expectancy, revision arthroplasty is becoming more frequent. Long revision of the femoral component achieves immediate mechanical fixation by bypassing to the distal femoral bone stock in the case of aseptic loosening and periprosthetic fractures [14,15]. Orthopaedic surgeons are now frequently confronted with periprosthetic fractures in elderly patients after revision surgery using a long. The purpose of this study was to identify the clinical and radiographical features of periprosthetic femoral fractures after revision surgery using a long. Methods We retrospectively reviewed a consecutive series of 11 periprosthetic femoral fractures that occurred after revision hip arthroplasty using a long between 1998 and The Institutional Review Board of Kyoto City Hospital approved the protocol for this study, and informed consent was obtained from each patient. The patients were all women with a mean age at the time of fracture of 79.2 years (70 to 91 years), as shown in Table 1. The status of the initial arthroplasty was THA in 5 patients and HA in 6 patients. The original diagnosis was femoral neck fracture in 5 patients, osteoarthritis in 5 patients, and avascular necrosis of femoral head in 1 patient. Seven patients had had a cemented femoral component and 4 had had a cementless femoral component. The mean numbers of previous surgeries were 3.1 (2 to 5). A previous history of fracture in the same femur was found in 7 hips including 5 femoral neck fractures, 3 periprosthetic fractures (Vancouver type B1: 1 hip, type B2: 2 hips). The status of the femur just before the latest revision was a cemented long in 2 patients, a cemented standard in four patients, a cementless standard in 3 patients and resection arthroplasty after infection in 2 patients. The cause of the latest revision surgery was aseptic loosening in 6 hips, periprosthetic fracture in 3 hips, and infection in 2 hips. The status of the femoral component after the latest revision was a cemented long in 8 patients, a cementless long in 2 patients, and a cemented standard with impaction bone grafting technique in 1 patient. Nine patients had sustained a clear mechanical fall, and 2 had sustained a spontaneous or insufficiency fracture. The fractures were classified according to the Vancouver classification. The management algorithm of the Vancouver classification sy was generally applied, but it was modified in some cases according to the surgeon s decision and the operative field. We have added bone grafting in cases of transverse fracture or short oblique fracture with comminution. The bone quality of these fractures Table 1 Demographic data Case Gender age Original diagnosis Primary treatment Fixation Previous operations Previous fractures Femoral status just before the latest revision Revision diagnosis Femoral component after the latest revision 1 F 87 FNF BHA Cemented 3 FNF, SCF Removal of the Infection Cemented long 2 F 73 OA THA Cemented 3 PPFx. B1 Cemented long PPFx. B1 Cemented long 3 F 73 FNF BHA Cemented 5 FNF Cemented long Cemented standard 4 F 73 OA THA Cemented 3 PPFx. B2 Cemented standard PPFx. B2 Cementless long 5 F 70 OA THA Cemented 3 - Cemented standard 6 F 79 OA THA Cemented 2 - Cemented standard Cemented long Cemented long 7 F 71 ANF BHA Cementless 5 - Removal of the Infection Cemented long 8 F 81 FNF BHA Cementless 3 FNF, SCF Cementless standard 9 F 91 OA THA Cemented 2 - Cementless standard 10 F 82 FNF BHA Cementless 2 FNF, SCF Cementless standard 11 F 91 FNF BHA Cementless 3 FNF, PPFx. B2 Cementless standard PPFx. B2 Cemented long Cemented long Cemented long Cementless long FNF, femoral neck fracture; OA, osteoarthritis; ANF, avascular necrosis of femoral head; BHA, bipolar hemiarthroplasty; THA, total hip, arthroplasty; PPF, periprosthetic femoral fracture; SCF, suprachondylar fracture.
3 Kim et al. BMC Musculoskeletal Disorders (2015) 16:113 Page 3 of 7 was assessed using cortical index [16]. Gruen have reported that the mean value of cortical index was 50.9% in patients with degenerative joint disease and 43.9% in patients with femoral neck fractures. All fractures were treated surgically. Patients were followed up clinically and radiographically for 6 weeks, and 3, 6, and 12 months postoperatively, and annually thereafter. The time to union was recorded. Clinical union was defined as full weight bearing with only slight or no occasional pain that did not compromise walking or basic daily activities. Union was defined as clinical union in the presence of radiological evidence of bone bridging in both the anteroposterior and lateral views. At the final follow-up, clinical evaluations were performed using the Japanese Orthopedic Association (JOA) score [17]. Complications were recorded with particular reference to infection, refracture, dislocation, and loosening. Postoperative rehabilitation was specific to each patient, but active flexion and extension of the ankle, hip, and knee of the affected side on the first day were common to all. Weight bearing was usually allowed when the fracture callus was visible radiologically and the application of weight was pain free. After 6 weeks, patients were allowed non-weight-bearing movement with a frame or crutch until early signs of healing and then advanced to partial weight bearing at 8 to 12 weeks postoperatively. Once union was confirmed, full weigh bearing was started about 3 to 4 months after surgery. All operations were performed by two experienced senior surgeons (CT and YK). Results The mean time of the radiographic and clinical follow-up was 58.9 months (8 to 180 months). All fractures were classified as Vancouver type B1. The fracture pattern was a transverse fracture in 6 hips and an oblique fracture in 5 hips (Table 2). The mean time from the revision arthroplasty using a long to the fracture was months (12 to 240 months). The mean cortical index was 20.5% (13.8 to 34.0%). In this study, the type B1 fractures were fixed with a plate in 9 patients. Seven patients were treated with a locking compression plate and cerclage wiring and, 2 patients were treated with a Dall Miles sy (Howmedica, Rutherford, NJ). Six patients were treated with bone allografts or autografts to facilitate fracture healing. In the other 2 patients, revision arthroplasty was performed with a cemented long using an impaction bone grafting technique. In one of them, femoral revision was necessary because of breakage (Case 4). In this case, cortical index was 15.3%. Another patient required reinforcement with a locking compression plate fixation (Case3, Figure 1). This patient was a 73-year-old female who had undergone revision surgery using impaction bone grafting because of aseptic loosening of the long after hemiarthroplasty. Six months after revision, this patient sustained a periprosthetic femoral fracture and had required revision arthroplasty using long because of very poor bone quality (cortical index; 13.8%) and had required reinforcement with a locking compression plate fixation because the length of the long available seemed to be insufficient and the reduction of the fracture was not ideal (in valgus alignment). In 1 patient treated with a Dall Miles cable plate and autogarfts, failure occurred because of plate breakage (Case 5, Figure 2). This case was revised with a cementless long (Cannulok revision prosthesis; Orthodynamics, Christchurch, Dorset, UK) in addition to allogeneic tibial plates, which resulted finally in bone union. Union occurred in all patients except one without malunion or infection. This failed case with breakage of the plate had a Table 2 Results Case Fracture type Time to fracture (mo) Treatment Plates Bone graft Time to union (mo) Duration of follow-up (mo) Outcome JOA score 1 Oblique 104 ORIF DFLCP Union 63 2 Transverse 100 ORIF Reverse DFLCP Auto, fibula 6 28 Union 77 3 Transverse 75 Revision (IBG) +ORIF LCP Allo, auto, iliac Union 68 4 Transverse 88 Revision (IBG) - Allo 4 45 Union 77 (with fracture) 5 Transverse 78 ORIF Dall-Miles plate Auto, fibula Nonunion* 53 6 Oblique 99 ORIF LCF Auto, iliac 4 74 Union 60 7 Transverse 12 ORIF Dall-Miles plate Auto, fibula Union 67 8 Oblique 120 ORIF DFLCP Allo 4 35 Union 60 9 Oblique 142 ORIF DFLCP Union Transverse 114 ORIF Reverse DFLCP Auto, iliac 6 12 Union Oblique 240 ORIF DFLCP Union 81 *Breakage of the plate; ORIF, open reduction and internal fixation; IBG, impaction bone grafting; DFLCP, distal femur locking compression plate; LCP, locking compression plate; auto, autograft; allo, allograft.
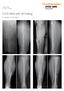
4 Kim et al. BMC Musculoskeletal Disorders (2015) 16:113 Page 4 of 7 Figure 1 Case 3, A seventy-three-years-old woman who sustained a Vancouver type-b1 periprosthetic femoral fracture seventy five months after revision surgery using a long. A Anteroposterior radiograph of the right hip showing the loosening of long. B Anteroposterior radiograph of the right hip made just after revision surgery using a standard with impaction bone grafting. C Anteroposterior radiograph of the right hip showing the Vancouver type B1 fracture pattern six months after revision surgery. D Anteroposterior radiograph of the right hip made one year after operation. Incorporation of the fracture site can be observed. bone defect at the fracture site, and revision surgery using a cementless long and allografts was successful. The mean time to weight bearing for these patients was 8 weeks. Complete fracture union occurred in all patients at an average of 5 months (2 to 8 months). None of the implants were radiolographically loose at final follow-up. The final mean functional score of the patients was JOA hip score Discussion Our study is among the first to report on the clinical and radiographic assessment of periprosthetic femoral fractures after femoral revision using a long. Most studies on periprosthetic femoral fractures deal with standard cemented or cementless s [18-20]. We think that there is a slight difference between periprosthetic fractures with a standard and periprosthetic fractures after revision surgery using a long. We found several important features that might influence the outcome of treatment for periprosthetic femoral fractures after femoral revision using a long. First, all cases in our series were classified as Vancouver type B1. In general, Vancouver type B1 fracture should be treated with open reduction and internal fixation. However, good fixation was less easily achieved in the presence of osteoporosis, which is common in this group of patients [11]. Second, 6 patients (55%) had a transverse fracture around the tip of the long. The rate of transverse fracture in our series is higher than that reported by other recent series [18]. Recent study of short oblique or transverse Vancouver type B1 fracture reported less satisfactory results and concluded that locking plate alone are insufficient for the treatment of periprosthetic femoral fracture and should be supplemented with cortical strut grafts [21]. Third, in our series, 7 patients (64%) had a history of previous fracture of the ipsilateral femur. Five femoral neck fractures, 3 periprosthetic fractures, and 3 suprachondylar fractures were included. The age at the index operation was 79.2 years, and previous surgeries were performed 3.1 on average. These facts mean that most
5 Kim et al. BMC Musculoskeletal Disorders (2015) 16:113 Page 5 of 7 Figure 2 Case 5, A seventy- years-old woman who sustained a Vancouver type-b1 periprosthetic femoral fracture seventy eight months after revision surgery using a long. A Anteroposterior radiograph of the left hip showing the Vancouver type-b1 frcture pattern. B Anteroposterior radiograph of the left hip made just after operation. C Anteroposterior radiograph of the left hip showing the nonunion with breakage of the plate. D Anteroposterior radiograph of the left hip made one year after operation. Incorporation of the fracture site can be observed. patients had poor bone quality because of osteoporosis and previous surgeries. According to the Vancouver classification, type B1 fractures are recommended to be treated with open reduction and internal fixation (ORIF) without revision of the femoral component. In our patients, 9 periprosthetic femoral fractures were treated with ORIF using conventional or locking compression plate and cerclage wiring with or without bone grafts. Five of the 9 fractures were oblique fractures and were treated successfully with this method. Bone grafting was performed in 2 because they involved oblique fracture with comminution. Four of 9 fractures were transverse fractures. Bone grafting was associated with ORIF because a stable long increases the stress at the distal end, which can make bone union very difficult. In 3 patients, the bone united without problems as shown in Figure 3, but in 1 of these patients, bone union failed because of breakage of the plate (Figure 2). This failure was associated with a bone defect at the fracture site. The high stress concentration at the end of the stable long combined with this bone defect might have caused the failure despite the bone grafting. Revision surgery was performed with a cementless long in addition to allogeneic tibial bone plates with success. Two other periprosthetic fractures were transverse fractures and were treated by femoral revision. Femoral revision was necessary for 1 fracture because of breakage and for the other because of very poor bone quality (cortical index; 13.8%). This latter case had required revision previously with impaction bone grafting and conversion of the long to a standard because of loosening of the long cemented. Six months after this revision, the transverse fracture occurred at the zone with very poor bone quality. Femoral revision was performed using a long cemented, bone grafts, and a locking plate. This fracture united 6 months after the femoral revision. In our patients, 7 periprosthetic fractures were treated with locking compression plates, and all patients achieved union. Recent studies have shown that locking compression plates represent a valuable advance in fracture treatment because they provide angular stability and stiffness in axial loading and torsion, help preserve the vascular
6 Kim et al. BMC Musculoskeletal Disorders (2015) 16:113 Page 6 of 7 Figure 3 Case 2, A seventy-three-years-old woman who sustained a Vancouver type-b1 periprosthetic femoral fracture one handred months after revision surgery using a long. A Anteroposterior radiograph of the left hip showing the Vancouver type-b1 frcture pattern. B Anteroposterior radiograph of the left hip made just after operation. C Anteroposterior radiograph of the left hip made one year after operation. Incorporation of the fracture site can be observed. supply, allow for the possible use of minimally invasive insertion techniques, require less plate-contouring compared with conventional plates, and provide better stability in osteoporotic bone [22-28]. Bi- or unicortical screw fixation at the level of the femoral shaft is effective against rotational stress. We used a reverse anatomic distal femoral locking compression plate, which involves use of an upside-down distal femoral plate of the contralateral side. The reverse use of the plate was intended to achieve multiple proximal trochanteric bicortical screw fixation [29]. This technique was very effective. Our results also show that plate pullout was not observed because cerclage wiring had been used routinely. Several authors have reported that plate fixation without cerclage wiring failed in 21% of patients because of plate pullout [21]. Usually bone grafting is not considered necessary for type B1 fractures if the fixation is stable. However, the authors recommend bone grafting for fractures after femoral revision using a long in cases involving transverse fracture or the short oblique fracture with comminution to improve fracture healing and increase bone stock. Stress concentration at the end of the stable seems to be much higher that of the standard [30,31]. And the bone quality is mostly poor because of multiple previous surgeries. Furthermore the patients in our series had a greater degree of osteoporosis (mean cortical index; 20.5%) than a matched group whose primary surgery had been performed for osteoarthritis (11hips, female n = 11, mean age; 78.1, mean cortical index; 53.7%). These aspects make bone union by ORIF more difficult. A transverse fracture with very poor bone quality (cortical index < 20) or bone loss might be considered as a type B3 fracture, and femoral revision might be the treatment of choice. Some authors have reported that revision for transverse type B1 fractures is considered because this fracture configuration is difficult to control with single plating, and fixation with a long is necessary to achieve axial stability and healing [19,25]. In addition, impaction bone grafting with long can be used successfully for treatment of type B2 and B3 periprposthetic femoral fracture [15]. There were several limitations to this study. First, this study was retrospective design and the lack of a patient control group for comparison. Secondly, the series was too small and the follow up period was too short.
7 Kim et al. BMC Musculoskeletal Disorders (2015) 16:113 Page 7 of 7 Thirdly, the strategies of treatment for fractures were heterogeneous (e.g., Dall-miles sy, locking plate, cementless long, and cemented long ). Conclusions In conclusion ORIF is the first choice of treatment for a type B1 fracture after revision using a long. If it is associated with poor bone quality ORIF also should be recommended in combination with bone grafts especially for transverse B1 fractures. However, a transverse fracture with very poor bone quality or bone loss might be considered as a type B3 fracture, and femoral revision might be the treatment of choice. The long-term effects and complications should be examined to determine whether these results can be maintained over time. Competing interests The authors declare that they have no competing interests. Authors contributions YK wrote the manuscript, collected the data and examined the patients. ST, HT and HK contributed to examination of patients and data collection. CT performed study planning and reviewed the manuscript. All authors read and approved the final manuscript. Acknowledgments The authors did not receive any outside funding or grants in support of their research for or preparation of this work. Received: 21 November 2014 Accepted: 27 April 2015 References 1. Berry DJ. Epidemiology: hip and knee. Orthop Clin North Am. 1999;30: Papadimitropoulos EA, Coyte PC, Josse RG, Greenwood CE. Current and projected rates of hip fracture in Canada. CMAJ. 1997;157: Singh JA, Jensen MR, Lewallen DG. Patient factors predict periprosthetic fractures after revision total hip arthroplasty. J Arthroplasty. 2012;8: Haddad FS, Masri BA, Garbuz DS, Duncan CP. The prevention of periprosthetic fractures in total hip and knee arthroplasty. Orthop Clin North Am. 1999;30: Springer BD, Berry DJ, Lewallen DG. Treatment of periprosthetic femoral fractures following total hip arthroplasty with femoral component revision. J Bone Joint Surg Am. 2003;85-A: Meek RMD, Norwood T, Smith R, Brenkel IJ, Howie CR. The risk of peri-prosthetic fracture after primary and revision total hip and knee replacement. J Bone Joint Surg (Br). 2011;93: Schwarzkopf R, Oni JK, Marwin SE. Total hip arthroplasty periprosthetic femoral fractures. Bull Hosp Jt Dis. 2013;71: Tsiridis E, Haddad FS, Gie GA. The management of periprosthetic femoral fractures around hip replacements. Injury. 2003;34: Duncan CP, Masri BA. Fractures of the femur after hip replacement. Instr Course Lect. 1995;44: Rayan F, Dodd M, Haddad FS. European validation of the Vancouver classification of periprosthetic proximal femoral fractures. J Bone Joint Surg (Br). 2008;90: Marsland D, Mears SC. A review of periprosthetic femoral fractures associated with total hip arthroplasty. Geriatr Orthop Surg Rehabil. 2012;3: Berry DJ. Periprosthetic fractures associated with osteolysis: a problem on the rise. J Arthroplasty. 2003;18: Franklin J, Malchau H. Risk factors for periprosthetic femoral fracture. Injury. 2007;38: So K, Kuroda Y, Matsuda S, Akiyama H. Revision total hip replacement with a cemented long femoral component: minimum 9-year follow-up results. Arch Orthop Trauma Surg. 2013;133: Tsiridis E, Narvani AA, Haddad FS, Timperley JA, Gie GA. Impaction femoral allografting and cemented revision for periprosthetic femoral fractures. J Bone Joint Surg (Br). 2004;86: Gruen T. A simple assessment of bone quality prior to hip arthroplasty: Cortical index revisited. In: Acta Orthopaedica Belgica, vol p Kuribayashi M, Takahashi KA, Fujioka M, Ueshima K, Inoue S, Kubo T. Reliability and validity of the Japanese orthopaedic association hip score. J Orthop Sci. 2010;15: Corten K, Vanrykel F, Bellemans J, Frederix PR, Simon J-P, Broos PLO. An algorithm for the surgical treatment of periprosthetic fractures of the femur around a well-fixed femoral component. J Bone Joint Surg (Br). 2009;91: Pavlou G, Panteliadis P, Macdonald D, Timperley JA, Gie G, Bancroft G, et al. A review of 202 periprosthetic fractures revision and allograft improves outcome for type B fractures. Hip Int. 2011;21: Xue H, Tu Y, Cai M, Yang A. Locking compression plate and cerclage band for type B1 periprosthetic femoral fractures preliminary results at average 30-month follow-up. J Arthroplasty. 2011;26(3): e Buttaro MA, Farfalli G, Paredes Núñez M, Comba F, Piccaluga F. Locking compression plate fixation of Vancouver type-b1 periprosthetic femoral fractures. J Bone Joint Surg Am. 2007;89: Demos HA, Briones MS, White PH, Hogan KA, Barfield WR. A biomechanical comparison of periprosthetic femoral fracture fixation in normal and osteoporotic cadaveric bone. J Arthroplasty. 2012;5: Ehlinger M, Adam P, Moser T, Delpin D, Bonnomet F. Type C periprosthetic fractures treated with locking plate fixation with a mean follow up of 2.5 years. Orthop Traumatol Surg Res. 2010;96: Chakravarthy J, Bansal R, Cooper J. Locking plate osteosynthesis for Vancouver type B1 and type C periprosthetic fractures of femur: a report on 12 patients. Injury. 2007;38: Graham SM, Moazen M, Leonidou A, Tsiridis E. Locking plate fixation for Vancouver B1 periprosthetic femoral fractures: a critical analysis of 135 cases. J Orthop Sci. 2013;18: Froberg L, Troelsen A, Brix M. Periprosthetic Vancouver type B1 and C fractures treated by locking-plate osteosynthesis: fracture union and reoperations in 60 consecutive fractures. Acta Orthop. 2012;83: Pike J, Davidson D, Garbuz D, Duncan CP, O Brien PJ, Masri BA. Principles of treatment for periprosthetic femoral shaft fractures around well-fixed total hip arthroplasty. J Am Acad Orthop Surg. 2009;17: Abhaykumar S, Elliott DS. Percutaneous plate fixation for periprosthetic femoral fractures a preliminary report. Injury. 2000;31: Ehlinger M, Brinkert D, Besse J, Adam P, Arlettaz Y, Bonnomet F. Reversed anatomic distal femur locking plate for periprosthetic hip fracture fixation. Orthop Traumatol Surg Res. 2011;97: Bobyn JD, Mortimer ES, Glassman AH, Engh CA, Miller JE, Brooks CE. Producing and avoiding stress shielding: laboratory and clinical observations of noncemented total hip arthroplasty. Clin Orthop Relat Res. 1992;274: Engh CA, Bobyn JD. The influence of size and extent of porous coating on femoral bone resorption after primary cementless hip arthroplasty. Clin Orthop Relat Res. 1988;231:7 28. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Outcomes of Surgical Treatment of Periprosthetic Femoral Fractures in Cementless Hip Arthroplasty
 ORIGINAL ARTICLE Hip Pelvis 27(3): 146-151, 2015 http://dx.doi.org/10.5371/hp.2015.27.3.146 Print ISSN 2287-3260 Online ISSN 2287-3279 Outcomes of Surgical Treatment of Periprosthetic Femoral Fractures
ORIGINAL ARTICLE Hip Pelvis 27(3): 146-151, 2015 http://dx.doi.org/10.5371/hp.2015.27.3.146 Print ISSN 2287-3260 Online ISSN 2287-3279 Outcomes of Surgical Treatment of Periprosthetic Femoral Fractures
Repeated Periprosthethic Femoral Fracture in a Below Knee Amputee with Ipsilateral Cementless Total Hip Arthroplasty - A Case Report -
 CASE REPORT Hip Pelvis 24(4): 322-327, 2012 http://dx.doi.org/10.5371/hp.2012.24.4.322 Print ISSN 2287-3260 Online ISSN 2287-3279 Repeated Periprosthethic Femoral Fracture in a Below Knee Amputee with
CASE REPORT Hip Pelvis 24(4): 322-327, 2012 http://dx.doi.org/10.5371/hp.2012.24.4.322 Print ISSN 2287-3260 Online ISSN 2287-3279 Repeated Periprosthethic Femoral Fracture in a Below Knee Amputee with
Treatment of Periprosthetic Femoral Fractures Following Hip Arthroplasty
 ORIGINAL ARTICLE Hip Pelvis 30(2): 78-85, 2018 http://dx.doi.org/10.5371/hp.2018.30.2.78 Print ISSN 2287-3260 Online ISSN 2287-3279 Treatment of Periprosthetic Femoral Fractures Following Hip Arthroplasty
ORIGINAL ARTICLE Hip Pelvis 30(2): 78-85, 2018 http://dx.doi.org/10.5371/hp.2018.30.2.78 Print ISSN 2287-3260 Online ISSN 2287-3279 Treatment of Periprosthetic Femoral Fractures Following Hip Arthroplasty
A 42-year-old patient presenting with femoral
 Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Could Patient Undergwent Surgical Treatment for Periprosthetic Femoral Fracture after Hip Arthroplasty Return to Their Status before Trauma?
 ORIGINAL ARTICLE Hip Pelvis 28(2): 90-97, 2016 http://dx.doi.org/10.5371/hp.2016.28.2.90 Print ISSN 2287-3260 Online ISSN 2287-3279 Could Patient Undergwent Surgical Treatment for Periprosthetic Femoral
ORIGINAL ARTICLE Hip Pelvis 28(2): 90-97, 2016 http://dx.doi.org/10.5371/hp.2016.28.2.90 Print ISSN 2287-3260 Online ISSN 2287-3279 Could Patient Undergwent Surgical Treatment for Periprosthetic Femoral
Total hip arthroplasty (THA) is a
 Review Article Principles of Treatment for Periprosthetic Femoral Shaft Fractures Around Well-fixed Total Hip Arthroplasty Jeffrey Pike, MD Darin Davidson, MD, MHSc Donald Garbuz, MD, MHSc, FRCSC Clive
Review Article Principles of Treatment for Periprosthetic Femoral Shaft Fractures Around Well-fixed Total Hip Arthroplasty Jeffrey Pike, MD Darin Davidson, MD, MHSc Donald Garbuz, MD, MHSc, FRCSC Clive
Unified Classification System (UCS) for peri-prosthetic fractures (PPFx)
 Unified Classification System (UCS) for peri-prosthetic fractures (PPFx) Waleed A Abdulwahid Consultant surgeon Medical City, Iraq 6th Emirates International Orthopedic Congress Dubai, UAE May 3-5, 2018
Unified Classification System (UCS) for peri-prosthetic fractures (PPFx) Waleed A Abdulwahid Consultant surgeon Medical City, Iraq 6th Emirates International Orthopedic Congress Dubai, UAE May 3-5, 2018
CIRCUMFERENTIAL PROXIMAL FEMORAL ALLOGRAFTS IN REVISION SURGERY ON TOTAL HIP ARTHROPLASTY: CASE REPORTS WITH A MINIMUM FOLLOW-UP OF 20 YEARS
 CASE REPORT CIRCUMFERENTIAL PROXIMAL FEMORAL ALLOGRAFTS IN REVISION SURGERY ON TOTAL HIP ARTHROPLASTY: CASE REPORTS WITH A MINIMUM FOLLOW-UP OF 20 YEARS Bruno Dutra Roos 1, Milton Valdomiro Roos 2, Antero
CASE REPORT CIRCUMFERENTIAL PROXIMAL FEMORAL ALLOGRAFTS IN REVISION SURGERY ON TOTAL HIP ARTHROPLASTY: CASE REPORTS WITH A MINIMUM FOLLOW-UP OF 20 YEARS Bruno Dutra Roos 1, Milton Valdomiro Roos 2, Antero
PERIPROSTHETIC FRACTURES FOLLOWING TOTAL HIP ARTHOPLASTY
 PERIPROSTHETIC FRACTURES FOLLOWING TOTAL HIP ARTHOPLASTY Jon Minter, DO Arthritis and Total Joint Specialists Atlanta, Georgia ArthritisAndTotalJoint.Com Intra Op Incidence of Periprosthetic Hip Fractures
PERIPROSTHETIC FRACTURES FOLLOWING TOTAL HIP ARTHOPLASTY Jon Minter, DO Arthritis and Total Joint Specialists Atlanta, Georgia ArthritisAndTotalJoint.Com Intra Op Incidence of Periprosthetic Hip Fractures
Surgical Management of Repeated Low-Energy Periprosthetic Femur Fractures - A Case Report -
 10.5371/jkhs.2011.23.1.66 Case Report Surgical Management of Repeated Low-Energy Periprosthetic Femur Fractures - Case Report - Taek-Rim Yoon, MD, Kyung-Soon Park, MD, Karupiah Thevarajan, MD, Nam-Young
10.5371/jkhs.2011.23.1.66 Case Report Surgical Management of Repeated Low-Energy Periprosthetic Femur Fractures - Case Report - Taek-Rim Yoon, MD, Kyung-Soon Park, MD, Karupiah Thevarajan, MD, Nam-Young
Treatment of Peri-Implant Fractures of the Femur
 Treatment of Peri-Implant Fractures of the Femur Steven I. Rabin Dreyer Medical Clinic Created January 2006 Revised August 2009 Fractures around Implants Pose Unique Fixation Challenges Number of Implants
Treatment of Peri-Implant Fractures of the Femur Steven I. Rabin Dreyer Medical Clinic Created January 2006 Revised August 2009 Fractures around Implants Pose Unique Fixation Challenges Number of Implants
Periprosthetic fractures around the femoral stem: overcoming challenges and avoiding pitfalls
 Review Article Page 1 of 13 Periprosthetic fractures around the femoral stem: overcoming challenges and avoiding pitfalls Andrew N. Fleischman, Antonia F. Chen Rothman Institute Department of Orthopaedic
Review Article Page 1 of 13 Periprosthetic fractures around the femoral stem: overcoming challenges and avoiding pitfalls Andrew N. Fleischman, Antonia F. Chen Rothman Institute Department of Orthopaedic
Use Of A Long Femoral Stem In The Treatment Of Proximal Femoral Fractures: A Report Of Four Cases
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 5 Number 1 Use Of A Long Femoral Stem In The Treatment Of Proximal Femoral Fractures: A Report Of Four Cases C Yu, V Singh Citation C Yu, V Singh..
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 5 Number 1 Use Of A Long Femoral Stem In The Treatment Of Proximal Femoral Fractures: A Report Of Four Cases C Yu, V Singh Citation C Yu, V Singh..
Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication?
 CASE REPORT Open Access Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication? A case report Timothy R Judkins, Michael R Dayton * Abstract
CASE REPORT Open Access Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication? A case report Timothy R Judkins, Michael R Dayton * Abstract
The complex problem of the interprosthetic femoral fracture in the elderly patient
 Acta Orthop. Belg., 2010, 76, 636-643 OriGiNal STUDY The complex problem of the interprosthetic femoral fracture in the elderly patient Yusuf MiCHLA, Lynnette SPALDiNG, James P. HOLLAND, David J. DEEHAN
Acta Orthop. Belg., 2010, 76, 636-643 OriGiNal STUDY The complex problem of the interprosthetic femoral fracture in the elderly patient Yusuf MiCHLA, Lynnette SPALDiNG, James P. HOLLAND, David J. DEEHAN
Medium- to Long-term Results of Strut Allografts Treating Periprosthetic Bone Defects
 ORIGINAL ARTICLE http://dx.doi.org/10.5371/hp.2018.30.1.23 Print ISSN 2287-3260 Online ISSN 2287-3279 Medium- to Long-term Results of Strut Allografts Treating Periprosthetic Bone Defects Jun Sung Park,
ORIGINAL ARTICLE http://dx.doi.org/10.5371/hp.2018.30.1.23 Print ISSN 2287-3260 Online ISSN 2287-3279 Medium- to Long-term Results of Strut Allografts Treating Periprosthetic Bone Defects Jun Sung Park,
Crossed Steinmann Pin Fixation In Supracondylar Femur Fractures In Adults A Case Series
 Article ID: WMC005027 ISSN 2046-1690 Crossed Steinmann Pin Fixation In Supracondylar Femur Fractures In Adults A Case Series Peer review status: No Corresponding Author: Dr. Mohit K Jindal, Senior Resident,
Article ID: WMC005027 ISSN 2046-1690 Crossed Steinmann Pin Fixation In Supracondylar Femur Fractures In Adults A Case Series Peer review status: No Corresponding Author: Dr. Mohit K Jindal, Senior Resident,
Locked plating constructs are creating a challenge for surgeons.
 Locked plating constructs are creating a challenge for surgeons. Three recent studies examining supracondylar femur fractures show concern for the high degree of stiffness of locked plating constructs
Locked plating constructs are creating a challenge for surgeons. Three recent studies examining supracondylar femur fractures show concern for the high degree of stiffness of locked plating constructs
Revision hip arthroplasty with S-ROM prosthesis: a study of clinical outcomes and implant stability
 J Orthopaed Traumatol () 7:1 1 DOI 1.17/s1195--15- ORIGINAL M. El-Deen S. Zahid D.T. Miller A. Nargol R. Logishetty Revision hip arthroplasty with S-ROM prosthesis: a study of clinical outcomes and implant
J Orthopaed Traumatol () 7:1 1 DOI 1.17/s1195--15- ORIGINAL M. El-Deen S. Zahid D.T. Miller A. Nargol R. Logishetty Revision hip arthroplasty with S-ROM prosthesis: a study of clinical outcomes and implant
Locked Plating: Clinical Indications
 Techniques in Orthopaedics 22(3):181 185 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Clinical Indications Kyle F. Dickson, M.D., M.B.A., John Munz, M.D. Summary: As shown in the previous article,
Techniques in Orthopaedics 22(3):181 185 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Clinical Indications Kyle F. Dickson, M.D., M.B.A., John Munz, M.D. Summary: As shown in the previous article,
Primary total hip arthroplasty after acetabular fracture using intra-acetabular bended plates
 Acta Orthop. Belg., 2017, 83, 93-97 ORIGINAL STUDY Primary total hip arthroplasty after acetabular fracture using intra-acetabular bended plates Valentinas Uvarovas, Igoris Šatkauskas, Giedrius Petryla,
Acta Orthop. Belg., 2017, 83, 93-97 ORIGINAL STUDY Primary total hip arthroplasty after acetabular fracture using intra-acetabular bended plates Valentinas Uvarovas, Igoris Šatkauskas, Giedrius Petryla,
RESULTS OF TREATMENT OF PERIPROSTHETIC FEMORAL FRACTURES AFTER TOTAL HIP ARTHROPLASTY
 Original articles RESULTS OF TREATMENT OF PERIPROSTHETIC FEMORAL FRACTURES AFTER TOTAL HIP ARTHROPLASTY Martin Korbel, Pavel Šponer, Tomáš Kučera, Egon Procházka, Tomáš Proček Charles University in Prague,
Original articles RESULTS OF TREATMENT OF PERIPROSTHETIC FEMORAL FRACTURES AFTER TOTAL HIP ARTHROPLASTY Martin Korbel, Pavel Šponer, Tomáš Kučera, Egon Procházka, Tomáš Proček Charles University in Prague,
EVOS MINI with IM Nailing
 Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Distal femoral fracture with subsequent ipsilateral proximal femoral fracture
 Distal femoral fracture with subsequent ipsilateral proximal femoral fracture by M Agarwal, MS FRCS, AA Syed, FRCSI, PV Giannoudis (!), BSc,MB,MD,EEC(Orth) Dept. of Orthopaedics and Trauma, St.James University
Distal femoral fracture with subsequent ipsilateral proximal femoral fracture by M Agarwal, MS FRCS, AA Syed, FRCSI, PV Giannoudis (!), BSc,MB,MD,EEC(Orth) Dept. of Orthopaedics and Trauma, St.James University
Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture
 Case Reports in Orthopedics, Article ID 745083, 4 pages http://dx.doi.org/10.1155/2014/745083 Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture Marcos Carvalho,
Case Reports in Orthopedics, Article ID 745083, 4 pages http://dx.doi.org/10.1155/2014/745083 Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture Marcos Carvalho,
Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy: a case report
 Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
CASE REPORT COMPLETE BONE REMODELING AFTER CALCAR RECONSTRUCTION WITH METAL WIRE MESH AND IMPACTION BONE GRAFTING: A CASE REPORT
 Nagoya J. Med. Sci. 75. 287 ~ 293, 2013 CASE REPORT COMPLETE BONE REMODELING AFTER CALCAR RECONSTRUCTION WITH METAL WIRE MESH AND IMPACTION BONE GRAFTING: A CASE REPORT Toshiki Iwase, M.D., Ph.D., Atsushi
Nagoya J. Med. Sci. 75. 287 ~ 293, 2013 CASE REPORT COMPLETE BONE REMODELING AFTER CALCAR RECONSTRUCTION WITH METAL WIRE MESH AND IMPACTION BONE GRAFTING: A CASE REPORT Toshiki Iwase, M.D., Ph.D., Atsushi
Level of Evidence: Prognostic Level II. See Instructions to Authors for a complete description of levels of evidence.
 1215 COPYRIGHT 2006 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Three Hundred and Twenty-one Periprosthetic Femoral Fractures BY HANS LINDAHL, MD, GÖRAN GARELLICK, MD, PHD, HANS REGNÉR, MD,
1215 COPYRIGHT 2006 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Three Hundred and Twenty-one Periprosthetic Femoral Fractures BY HANS LINDAHL, MD, GÖRAN GARELLICK, MD, PHD, HANS REGNÉR, MD,
Periprosthetic fractures of the femur: our experience
 Acta Biomed 2014; Vol. 85, N. 1: 35-43 Mattioli 1885 Original Article Periprosthetic fractures of the femur: our experience Roberto Valentini, Marcellino Martino, Giovanni De Fabrizio, Giovanni Fancellu
Acta Biomed 2014; Vol. 85, N. 1: 35-43 Mattioli 1885 Original Article Periprosthetic fractures of the femur: our experience Roberto Valentini, Marcellino Martino, Giovanni De Fabrizio, Giovanni Fancellu
Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts
 Original Article 268 Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts Lin-Hsiu Weng, MD; Jun-Wen Wang, MD Background: In this study,
Original Article 268 Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts Lin-Hsiu Weng, MD; Jun-Wen Wang, MD Background: In this study,
Failed Subtrochanteric Fracture How I Decide What to Do?
 Failed Subtrochanteric Fracture How I Decide What to Do? Gerald E. Wozasek Thomas M. Tiefenboeck 5 October 2016, Washington Medical University of Vienna, Department of Trauma Surgery ordination @wozasek.at
Failed Subtrochanteric Fracture How I Decide What to Do? Gerald E. Wozasek Thomas M. Tiefenboeck 5 October 2016, Washington Medical University of Vienna, Department of Trauma Surgery ordination @wozasek.at
Extensively Porous-coated Stems for Femoral Revision: Reliable Choice for Stem Revision in Paprosky Femoral Type III Defects
 Extensively Porous-coated Stems for Femoral Revision: Reliable Choice for Stem Revision in Paprosky Femoral Type III Defects Lien-Hsiang Chung, MD; Po-Kuei Wu, MD; Cheng-Fong Chen, MD; Wei-Ming Chen, MD;
Extensively Porous-coated Stems for Femoral Revision: Reliable Choice for Stem Revision in Paprosky Femoral Type III Defects Lien-Hsiang Chung, MD; Po-Kuei Wu, MD; Cheng-Fong Chen, MD; Wei-Ming Chen, MD;
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture.
 Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
Revision Total Hip Arthroplasty Using an Extensively Porous Coated Femoral Stem
 Original Article Clinics in Orthopedic Surgery 2009;1:105-109 doi:10.4055/cios.2009.1.2.105 Revision Total Hip Arthroplasty Using an Extensively Porous Coated Femoral Stem Kyoung Ho Moon, MD, Joon Soon
Original Article Clinics in Orthopedic Surgery 2009;1:105-109 doi:10.4055/cios.2009.1.2.105 Revision Total Hip Arthroplasty Using an Extensively Porous Coated Femoral Stem Kyoung Ho Moon, MD, Joon Soon
Salvage of failed dynamic hip screw fixation of intertrochanteric fractures
 Injury, Int. J. Care Injured (2005) xxx, xxx xxx 1 www.elsevier.com/locate/injury 2 3 4 5 6 7 8 8 9 10 11 12 13 14 15 Salvage of failed dynamic hip screw fixation of intertrochanteric s G.Z. Said, O. Farouk
Injury, Int. J. Care Injured (2005) xxx, xxx xxx 1 www.elsevier.com/locate/injury 2 3 4 5 6 7 8 8 9 10 11 12 13 14 15 Salvage of failed dynamic hip screw fixation of intertrochanteric s G.Z. Said, O. Farouk
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Clinico-radiological outcome of closed reduction and percutaneous fixation of proximal humerus fractures
 2018; 4(1): 614-618 ISSN: 2395-1958 IJOS 2018; 4(1): 614-618 2018 IJOS www.orthopaper.com Received: 10-11-2017 Accepted: 11-12-2017 Dr. Dharmendra Kumar Assistant Professor, KGMU, Lucknow, Dr. Neerav Anand
2018; 4(1): 614-618 ISSN: 2395-1958 IJOS 2018; 4(1): 614-618 2018 IJOS www.orthopaper.com Received: 10-11-2017 Accepted: 11-12-2017 Dr. Dharmendra Kumar Assistant Professor, KGMU, Lucknow, Dr. Neerav Anand
3.5 mm Locking Attachment Plate
 For Treatment of Periprosthetic Fractures 3.5 mm Locking Attachment Plate Surgical Technique Table of Contents Introduction 3.5 mm Locking Attachment Plate 2 Indications 4 Surgical Technique Preparation
For Treatment of Periprosthetic Fractures 3.5 mm Locking Attachment Plate Surgical Technique Table of Contents Introduction 3.5 mm Locking Attachment Plate 2 Indications 4 Surgical Technique Preparation
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Fixation in osteoporotic bone. Jeppe Barckman Ortopædkirugisk afd. Aarhus Universitetshospital
 Fixation in osteoporotic bone Jeppe Barckman Ortopædkirugisk afd. Aarhus Universitetshospital Objective Highlight current principles of fixation for osteoporotic fractures Woman 75 year Who to fix? The
Fixation in osteoporotic bone Jeppe Barckman Ortopædkirugisk afd. Aarhus Universitetshospital Objective Highlight current principles of fixation for osteoporotic fractures Woman 75 year Who to fix? The
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
The risk of peri-prosthetic fracture after primary and revision total hip and knee replacement
 The risk of peri-prosthetic fracture after primary and revision total hip and knee replacement R. M. D. Meek, T. Norwood, R. Smith, I. J. Brenkel, C. R. Howie From the Scottish Arthroplasty Project, Edinburgh,
The risk of peri-prosthetic fracture after primary and revision total hip and knee replacement R. M. D. Meek, T. Norwood, R. Smith, I. J. Brenkel, C. R. Howie From the Scottish Arthroplasty Project, Edinburgh,
operative technique Kent Hip
 operative technique Kent Hip The Kent Hip Operative Technique The Kent Hip was developed by Mr Cliff Stossel, FRCS in Maidstone, Kent, UK and first implanted in 1986. It was designed to deal with problems
operative technique Kent Hip The Kent Hip Operative Technique The Kent Hip was developed by Mr Cliff Stossel, FRCS in Maidstone, Kent, UK and first implanted in 1986. It was designed to deal with problems
PERIPROSTHETIC FEMUR FRACTURES AFTER THA: Treatment with Revision
 PERIPROSTHETIC FEMUR FRACTURES AFTER THA: Treatment with Revision Daniel J. Berry, MD LZ Gund Professor Department of Orthopedic Surgery Mayo Clinic Rochester, MN Presenter Disclosure Information The author
PERIPROSTHETIC FEMUR FRACTURES AFTER THA: Treatment with Revision Daniel J. Berry, MD LZ Gund Professor Department of Orthopedic Surgery Mayo Clinic Rochester, MN Presenter Disclosure Information The author
ISSUES FROM AN ORTHOPEDIC PERSPECTIVE
 ISSUES FROM AN ORTHOPEDIC PERSPECTIVE John Brown, MD The Core Institute Objectives: Understand the common orthopedic problems of the geriatric population. Describe the standard treatment algorithms for
ISSUES FROM AN ORTHOPEDIC PERSPECTIVE John Brown, MD The Core Institute Objectives: Understand the common orthopedic problems of the geriatric population. Describe the standard treatment algorithms for
For Commercial products, please refer to the following policy: Preauthorization via Web-Based Tool for Procedures
 Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Orthopedics in Motion Tristan Hartzell, MD January 27, 2016
 Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Femoral Revision Algorithm. A practical guide for the use of the CORAIL Hip System in femoral revision surgery
 Femoral Revision Algorithm A practical guide for the use of the CORAIL Hip System in femoral revision surgery Introduction The principles that govern the mode of prosthetic fixation, implant stability
Femoral Revision Algorithm A practical guide for the use of the CORAIL Hip System in femoral revision surgery Introduction The principles that govern the mode of prosthetic fixation, implant stability
Distal Femur Fractures in The Elderly The Ideal Construct
 Distal Femur Fractures in The Elderly The Ideal Construct Tak-Wing Lau Department of Orthopaedics and Traumatology Queen Mary Hospital The University of Hong Kong Singapore Trauma 2015 Trauma Through the
Distal Femur Fractures in The Elderly The Ideal Construct Tak-Wing Lau Department of Orthopaedics and Traumatology Queen Mary Hospital The University of Hong Kong Singapore Trauma 2015 Trauma Through the
Peri-prosthetic fractures around the hip
 Vineet Sharma MS *, Aaron G Rosenberg MD** *Consultant, Advanced Hip and Knee Clinic, Chandigarh **Chief of Adult Reconstruction, Rush University Medical Center, 1725 West Harrison Street, Suite 1063 Chicago,
Vineet Sharma MS *, Aaron G Rosenberg MD** *Consultant, Advanced Hip and Knee Clinic, Chandigarh **Chief of Adult Reconstruction, Rush University Medical Center, 1725 West Harrison Street, Suite 1063 Chicago,
Types of Plates 1. New Dynamic Compression Plate: Diaphyseal fracture: Radius, Ulna, Humerus, Rarely tibia
 Types of Plates 1. New Dynamic Compression Plate: DCP Diaphyseal fracture: Radius, Ulna, Humerus, Rarely tibia 1. Undercut adjacent to the holes low contact: less stress shield 2. Undercut at the undersurface
Types of Plates 1. New Dynamic Compression Plate: DCP Diaphyseal fracture: Radius, Ulna, Humerus, Rarely tibia 1. Undercut adjacent to the holes low contact: less stress shield 2. Undercut at the undersurface
Locked Plating: Biomechanics and Biology
 Techniques in Orthopaedics 22(4):E1 E6 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Biomechanics and Biology Kyle F. Dickson, M.D., M.B.A., John W. Munz, M.D. Summary: Since the early ideas
Techniques in Orthopaedics 22(4):E1 E6 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Biomechanics and Biology Kyle F. Dickson, M.D., M.B.A., John W. Munz, M.D. Summary: Since the early ideas
Case Reports RETROGRADE INTRAMEDULLARY NAILING FOR NONUNIONS OF SUPRACONDYLAR FEMUR FRACTURE OF OSTEOPOROTIC BONES
 J.L. Pao and C.C. Jiang RETROGRADE INTRAMEDULLARY NAILING FOR NONUNIONS OF SUPRACONDYLAR FEMUR FRACTURE OF OSTEOPOROTIC BONES Jwo-Luen Pao 1 and Ching-Chuan Jiang 2 Abstract: Nonunion of supracondylar
J.L. Pao and C.C. Jiang RETROGRADE INTRAMEDULLARY NAILING FOR NONUNIONS OF SUPRACONDYLAR FEMUR FRACTURE OF OSTEOPOROTIC BONES Jwo-Luen Pao 1 and Ching-Chuan Jiang 2 Abstract: Nonunion of supracondylar
LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia.
 LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia. LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia.
LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia. LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia.
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY
 EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
The shape and size of femoral components in revision total hip arthroplasty among Chinese patients
 Journal of Orthopaedic Surgery 2003: 11(1): 53 58 The shape and size of femoral components in revision total hip arthroplasty among Chinese patients KY Chiu, TP Ng, WM Tang Department of Orthopaedic Surgery,
Journal of Orthopaedic Surgery 2003: 11(1): 53 58 The shape and size of femoral components in revision total hip arthroplasty among Chinese patients KY Chiu, TP Ng, WM Tang Department of Orthopaedic Surgery,
Difficult Hosts. Treatment Options. Distal Femoral Replacement for Distal Femur Fractures When is it the Best Choice
 Distal Femoral Replacement for Distal Femur Fractures When is it the Best Choice Walter W. Virkus, MD IU Health Methodist Hospital Indianapolis, IN Difficult Hosts Distal femur fractures common Distal
Distal Femoral Replacement for Distal Femur Fractures When is it the Best Choice Walter W. Virkus, MD IU Health Methodist Hospital Indianapolis, IN Difficult Hosts Distal femur fractures common Distal
BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES
 BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES Mohammad Abul kalam, Pradeep Kumar, Mohammad Afzal Hussain and Iqbal Ahmad Abstract A prospective study of forty comminuted femoral shaft fractures,
BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES Mohammad Abul kalam, Pradeep Kumar, Mohammad Afzal Hussain and Iqbal Ahmad Abstract A prospective study of forty comminuted femoral shaft fractures,
Elbow Fractures ORIF VS Arthroplasty
 Elbow Fractures ORIF VS Arthroplasty Oke Anakwenze, M.D. Olympus Orthopedics No disclosures Disclosures Distal humerus fractures 0.5-0.7% of all fractures 30% of all elbow fractures Bimodal etiology Young
Elbow Fractures ORIF VS Arthroplasty Oke Anakwenze, M.D. Olympus Orthopedics No disclosures Disclosures Distal humerus fractures 0.5-0.7% of all fractures 30% of all elbow fractures Bimodal etiology Young
76 F: Plays tennis, lives independently, told she has weak bone
 Femoral Neck Fractures In the ELDERLY What to do, when and why Frank Liporace, MD Chairman & VP, Dept of Orthopaedics Chief of Trauma & Adult Reconstruction Jersey City Medical Center / RWJ Barnabas Health
Femoral Neck Fractures In the ELDERLY What to do, when and why Frank Liporace, MD Chairman & VP, Dept of Orthopaedics Chief of Trauma & Adult Reconstruction Jersey City Medical Center / RWJ Barnabas Health
IJCRI 2011;2(5): Manikam et. al. 21
 IJCRI 2011;2(5):21-25. Manikam et. al. 21 CASE REPORT OPEN ACCESS Reversed tibial locking plates in management of traumatic ipsilateral periprosthetic fractures of the distal femur and proximal tibia after
IJCRI 2011;2(5):21-25. Manikam et. al. 21 CASE REPORT OPEN ACCESS Reversed tibial locking plates in management of traumatic ipsilateral periprosthetic fractures of the distal femur and proximal tibia after
Revision Arthroplasty Using a MUTARS Prosthesis in Comminuted Periprosthetic Fracture of the Distal Femur
 Technical Report Yonsei Med J 2016 Nov;57(6):1517-1522 pissn: 0513-5796 eissn: 1976-2437 Revision Arthroplasty Using a MUTARS Prosthesis in Comminuted Periprosthetic Fracture of the Distal Femur Hyung-Suk
Technical Report Yonsei Med J 2016 Nov;57(6):1517-1522 pissn: 0513-5796 eissn: 1976-2437 Revision Arthroplasty Using a MUTARS Prosthesis in Comminuted Periprosthetic Fracture of the Distal Femur Hyung-Suk
DISCLOSURE FNFX ORIF OR ARTHROPLASTY? 11/21/2016 FEMORAL NECK FRACTURES: ORIF OR ARTHROPLASTY? ROYALTIES DEPUY, BIOMET
 FEMORAL NECK FRACTURES: ORIF OR ARTHROPLASTY? GEORGE HAIDUKEWYCH, MD ORLANDO, FLORIDA DISCLOSURE ROYALTIES DEPUY, BIOMET CONSULTING DEPUY, SYNTHES, BIOMET, RESPONSIVE ORTHOPEDICS STOCK OWNERSHIP ORTHOPEDIATRICS
FEMORAL NECK FRACTURES: ORIF OR ARTHROPLASTY? GEORGE HAIDUKEWYCH, MD ORLANDO, FLORIDA DISCLOSURE ROYALTIES DEPUY, BIOMET CONSULTING DEPUY, SYNTHES, BIOMET, RESPONSIVE ORTHOPEDICS STOCK OWNERSHIP ORTHOPEDIATRICS
Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based screw insertion into locking plates
 Ioannou et al. Journal of Orthopaedic Surgery and Research (2016) 11:118 DOI 10.1186/s13018-016-0458-y RESEARCH ARTICLE Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based
Ioannou et al. Journal of Orthopaedic Surgery and Research (2016) 11:118 DOI 10.1186/s13018-016-0458-y RESEARCH ARTICLE Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based
Plate Fixation Options
 Distal tibia extra-articular fractures can be difficult to treat Tenuous soft tissue Complex fracture patterns Plate Fixation Options Medial plating: Minimally invasive approach Technical ease Anterolateral
Distal tibia extra-articular fractures can be difficult to treat Tenuous soft tissue Complex fracture patterns Plate Fixation Options Medial plating: Minimally invasive approach Technical ease Anterolateral
Technique Guide. Locking Attachment Plate. For treatment of periprosthetic fractures.
 Technique Guide Locking Attachment Plate. For treatment of periprosthetic fractures. Table of Contents Introduction Locking Attachment Plate 2 Indications 4 Surgical Technique Patient Positioning 5 Preparation
Technique Guide Locking Attachment Plate. For treatment of periprosthetic fractures. Table of Contents Introduction Locking Attachment Plate 2 Indications 4 Surgical Technique Patient Positioning 5 Preparation
Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Conflict of Interest 9/24/2015
 Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Cory Collinge, MD Professor of Orthopedic Surgery Vanderbilt University Medical Center Nashville, TN Conflict of Interest Consultant: Smith
Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Cory Collinge, MD Professor of Orthopedic Surgery Vanderbilt University Medical Center Nashville, TN Conflict of Interest Consultant: Smith
Long-stem revision prosthesis for salvage of failed fixation of extracapsular proximal femoral fractures
 Acta Orthop. Belg., 2009, 75, 340-345 ORIGINAL STUDY Long-stem revision prosthesis for salvage of failed fixation of extracapsular proximal femoral fractures Rory J. SHARVILL, Nicholas A. FERRAN, Huw G.
Acta Orthop. Belg., 2009, 75, 340-345 ORIGINAL STUDY Long-stem revision prosthesis for salvage of failed fixation of extracapsular proximal femoral fractures Rory J. SHARVILL, Nicholas A. FERRAN, Huw G.
REVISING THE DEFICIENT PROXIMAL FEMUR
 REVISING THE DEFICIENT PROXIMAL FEMUR by David Mattingly, Boston, MA Joseph McCarthy, Boston, MA Benjamin E. Bierbaum, Boston, MA Hugh P. Chandler, Boston, MA Roderick H. Turner, Boston, MA Hugh U. Cameron,
REVISING THE DEFICIENT PROXIMAL FEMUR by David Mattingly, Boston, MA Joseph McCarthy, Boston, MA Benjamin E. Bierbaum, Boston, MA Hugh P. Chandler, Boston, MA Roderick H. Turner, Boston, MA Hugh U. Cameron,
Bone Bangalore
 Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital, Whitefield,
Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital, Whitefield,
Autologous bone grafting plus bio-absorbable pin fixation for medial tibial defects in total knee arthroplasty
 Autologous bone grafting plus bio-absorbable pin fixation for medial tibial defects in total knee arthroplasty Showa University Fujigaoka Hospital, Yokohama SHIN KATO, Hiroshi Takagi, Jun Oike, Takayuki
Autologous bone grafting plus bio-absorbable pin fixation for medial tibial defects in total knee arthroplasty Showa University Fujigaoka Hospital, Yokohama SHIN KATO, Hiroshi Takagi, Jun Oike, Takayuki
Optimum implant geometry
 Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
A comparative study of less invasive stabilization system and titanium elastic nailing for subtrochanteric femur fractures in older children
 Acta Orthop. Belg., 2015, 81, 123-130 ORIGINAL STUDY A comparative study of less invasive stabilization system and titanium elastic nailing for subtrochanteric femur fractures in older children Liao-Jun
Acta Orthop. Belg., 2015, 81, 123-130 ORIGINAL STUDY A comparative study of less invasive stabilization system and titanium elastic nailing for subtrochanteric femur fractures in older children Liao-Jun
Fixation with cancellous screws and fibular strut grafts for neglected femoral neck fractures
 Journal of Orthopaedic Surgery 2014;22(2):181-5 Fixation with cancellous screws and fibular strut grafts for neglected femoral neck fractures Chandra Prakash Pal, 1 Binod Kumar, 2 Karuna Shankar Dinkar,
Journal of Orthopaedic Surgery 2014;22(2):181-5 Fixation with cancellous screws and fibular strut grafts for neglected femoral neck fractures Chandra Prakash Pal, 1 Binod Kumar, 2 Karuna Shankar Dinkar,
Fibula bone grafting in infected gap non union: A prospective case series
 2019; 3(1): 06-10 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2019; 3(1): 06-10 Received: 03-11-2018 Accepted: 06-12-2018 Dr. Mohammed Nazim M.S (Ortho),
2019; 3(1): 06-10 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2019; 3(1): 06-10 Received: 03-11-2018 Accepted: 06-12-2018 Dr. Mohammed Nazim M.S (Ortho),
Extended Trochanteric Osteotomy Followed by Cemented Impaction Allografting in Revision Hip Arthroplasty
 The Journal of Arthroplasty Vol. 28 No. 1 2013 Extended Trochanteric Osteotomy Followed by Cemented Impaction Allografting in Revision Hip Arthroplasty John Charity, MD, MRCS,* Eleftherios Tsiridis, MD,
The Journal of Arthroplasty Vol. 28 No. 1 2013 Extended Trochanteric Osteotomy Followed by Cemented Impaction Allografting in Revision Hip Arthroplasty John Charity, MD, MRCS,* Eleftherios Tsiridis, MD,
A prospective study of treatment of distal femur fractures with locking condylar plate
 International Journal of Research in Orthopaedics Rekha YB et al. Int J Res Orthop. 2017 Nov;3(6):1117-1121 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20174699
International Journal of Research in Orthopaedics Rekha YB et al. Int J Res Orthop. 2017 Nov;3(6):1117-1121 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20174699
Comparison of two modality of fixation in unstable trochantric fractures in elderly patients
 Original article Comparison of two modality of fixation in unstable trochantric fractures in elderly patients 1Dr. Vipin Garg, 2 Dr. Anjul Agarwal 1MS Orhtopaedics, Assistant professor, Department of orthopaedics,
Original article Comparison of two modality of fixation in unstable trochantric fractures in elderly patients 1Dr. Vipin Garg, 2 Dr. Anjul Agarwal 1MS Orhtopaedics, Assistant professor, Department of orthopaedics,
Hip arthroplasty after failed fixation of trochanteric and subtrochanteric
 Acta Orthopaedica 2012; 83 (5): 493 498 493 Hip arthroplasty after failed fixation of trochanteric and subtrochanteric fractures A cohort study with 5 11 year follow-up of 88 consecutive patients Anders
Acta Orthopaedica 2012; 83 (5): 493 498 493 Hip arthroplasty after failed fixation of trochanteric and subtrochanteric fractures A cohort study with 5 11 year follow-up of 88 consecutive patients Anders
Clinical outcome of endoprosthetic replacement for failed treatment of intertrochanteric fractures: A retrospective case series
 Original Article Open Access Clinical outcome of endoprosthetic replacement for failed treatment of intertrochanteric fractures: A retrospective case series Wei Feng 1, Ting Hao 2, Wan-lin Liu 3, Yan-fei
Original Article Open Access Clinical outcome of endoprosthetic replacement for failed treatment of intertrochanteric fractures: A retrospective case series Wei Feng 1, Ting Hao 2, Wan-lin Liu 3, Yan-fei
Technique Guide. LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System.
 Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
A comparative study of 30 cases of trochanteric fracture femur treated with dynamic hip screw and proximal femoral nailing
 Original Article A comparative study of 30 cases of trochanteric fracture femur treated with dynamic hip screw and proximal femoral nailing Jaswinder Pal Singh Walia *, Himanshu Tailor**, H S Mann ***,
Original Article A comparative study of 30 cases of trochanteric fracture femur treated with dynamic hip screw and proximal femoral nailing Jaswinder Pal Singh Walia *, Himanshu Tailor**, H S Mann ***,
Olecranon fracture. Lonnie Froberg, MD, Ph.D Rigshospitalet, Copenhagen University Hospital
 Olecranon fracture Lonnie Froberg, MD, Ph.D Rigshospitalet, Copenhagen University Hospital 20% of forearm fracture 12 per 100.000 persons per year Low-energy fall Increased risk >50 years 90% AO 21.B1.1
Olecranon fracture Lonnie Froberg, MD, Ph.D Rigshospitalet, Copenhagen University Hospital 20% of forearm fracture 12 per 100.000 persons per year Low-energy fall Increased risk >50 years 90% AO 21.B1.1
3A ODEP rating, demonstrating 99.5% survivorship at 3 years for aseptic loosening
 The evidence base 3A ODEP rating, demonstrating 99.5% survivorship at 3 years for aseptic loosening Total number of patients 175 (89 male; 86 female) Mean age 59.15 (33-72) Mean follow-up 3.2 years (0.01-4.5)
The evidence base 3A ODEP rating, demonstrating 99.5% survivorship at 3 years for aseptic loosening Total number of patients 175 (89 male; 86 female) Mean age 59.15 (33-72) Mean follow-up 3.2 years (0.01-4.5)
Management of periprosthetic fractures in patients treated with a megaprosthesis for malignant bone tumours around the knee
 Acta Orthop. Belg., 2012, 78, 558-563 CASE REPORT Management of periprosthetic fractures in patients treated with a megaprosthesis for malignant bone tumours around the knee Michael GEBHARt, Félix SHuMElInSky
Acta Orthop. Belg., 2012, 78, 558-563 CASE REPORT Management of periprosthetic fractures in patients treated with a megaprosthesis for malignant bone tumours around the knee Michael GEBHARt, Félix SHuMElInSky
OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3
 OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3 HOW TO CITE THIS ARTICLE: Karan Mehta, Prashanth G. Shiblee Siddiqui,
OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3 HOW TO CITE THIS ARTICLE: Karan Mehta, Prashanth G. Shiblee Siddiqui,
DifficultTibialNailRemovalusingtheExtendedTrochantericOsteotomyTechniquePriortoTotalKneeArthroplasty
 : H Orthopedic and Musculoskeletal System Volume 14 Issue 3 Version 1.0 Year 2014 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online ISSN: 2249-4618
: H Orthopedic and Musculoskeletal System Volume 14 Issue 3 Version 1.0 Year 2014 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online ISSN: 2249-4618
Knee Revision. Portfolio
 Knee Revision Portfolio I use the DePuy Revision Knee System because of its versatility. With this system I can solve nearly any situation I encounter in the OR. Dr. Thomas Fehring, OrthoCarolina Hip and
Knee Revision Portfolio I use the DePuy Revision Knee System because of its versatility. With this system I can solve nearly any situation I encounter in the OR. Dr. Thomas Fehring, OrthoCarolina Hip and
Convertibilité. Ph. Valenti. Paris Shoulder Unit Clinique Bizet (Paris, France)
 Convertibilité Ph. Valenti Paris Shoulder Unit Clinique Bizet (Paris, France) Disclosures Arthroplasty Consultant : FH orthopaedics receive royalties Arthroscopy Consultant : Zimmer Biomet Arthrex In Last
Convertibilité Ph. Valenti Paris Shoulder Unit Clinique Bizet (Paris, France) Disclosures Arthroplasty Consultant : FH orthopaedics receive royalties Arthroscopy Consultant : Zimmer Biomet Arthrex In Last
AOTrauma / AORecon Masters Course Periprosthetic Fractures (Course with Anatomical Specimen)
 Sunday, 13 May 2018 (Day 1) 15:00 17:00 Other Registration of participants 17:00 18:00 Opening remarks Opening ceremony 18:00 19:00 Other AOTRAUMA RECEPTION 120 1 / 10 Monday, 14 May 2018 (Day 2) 08:00
Sunday, 13 May 2018 (Day 1) 15:00 17:00 Other Registration of participants 17:00 18:00 Opening remarks Opening ceremony 18:00 19:00 Other AOTRAUMA RECEPTION 120 1 / 10 Monday, 14 May 2018 (Day 2) 08:00
The long term fate of the fibula when used as an intraosseous graft
 Acta Orthop. Belg., 2004, 70, 322-326 The long term fate of the fibula when used as an intraosseous graft Onkar N. NAGI, Mandeep S. DHILLON, Sameer AGGARWAL From the Post Graduate Institute of Medical
Acta Orthop. Belg., 2004, 70, 322-326 The long term fate of the fibula when used as an intraosseous graft Onkar N. NAGI, Mandeep S. DHILLON, Sameer AGGARWAL From the Post Graduate Institute of Medical
Osteotomy in artificial femoral component revision with severe greater trochanter osteolysis.
 Biomedical Research 2017; 28 (13): 6007-6012 ISSN 0970-938X www.biomedres.info Osteotomy in artificial femoral component revision with severe greater trochanter osteolysis. Xiao-hui Gu 1,2, Jun-ying Sun
Biomedical Research 2017; 28 (13): 6007-6012 ISSN 0970-938X www.biomedres.info Osteotomy in artificial femoral component revision with severe greater trochanter osteolysis. Xiao-hui Gu 1,2, Jun-ying Sun
Comparitive Study between Proximal Femoral Nailing and Dynamic Hip Screw in Intertrochanteric Fracture of Femur *
 Open Journal of Orthopedics, 2013, 3, 291-295 Published Online November 2013 (http://www.scirp.org/journal/ojo) http://dx.doi.org/10.4236/ojo.2013.37053 291 Comparitive Study between Proximal Femoral Nailing
Open Journal of Orthopedics, 2013, 3, 291-295 Published Online November 2013 (http://www.scirp.org/journal/ojo) http://dx.doi.org/10.4236/ojo.2013.37053 291 Comparitive Study between Proximal Femoral Nailing
Management Of Acetabular Deficiency In Total Hip Arthroplasty: A Series Of 15 Cases
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 21 Number 2 Management Of Acetabular Deficiency In Total Hip Arthroplasty: A Series Of 15 Cases G Khanna, R Sharma, D Singh, T A Chandy Citation
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 21 Number 2 Management Of Acetabular Deficiency In Total Hip Arthroplasty: A Series Of 15 Cases G Khanna, R Sharma, D Singh, T A Chandy Citation
Autosomal Dominant Type I Osteopetrosis Is Related with Iatrogenic Fractures in Arthroplasty
 Case Report Clinics in Orthopedic Surgery 2014;6:484-488 http://dx.doi.org/10.4055/cios.2014.6.4.484 Autosomal Dominant Type I Osteopetrosis Is Related with Iatrogenic Fractures in Arthroplasty Ruud P.
Case Report Clinics in Orthopedic Surgery 2014;6:484-488 http://dx.doi.org/10.4055/cios.2014.6.4.484 Autosomal Dominant Type I Osteopetrosis Is Related with Iatrogenic Fractures in Arthroplasty Ruud P.
The Lateral Trochanteric Wall A Key Element in the Reconstruction of Unstable Pertrochanteric Hip Fractures
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 425, pp. 82 86 2004 Lippincott Williams & Wilkins The Lateral Trochanteric Wall A Key Element in the Reconstruction of Unstable Pertrochanteric Hip Fractures
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 425, pp. 82 86 2004 Lippincott Williams & Wilkins The Lateral Trochanteric Wall A Key Element in the Reconstruction of Unstable Pertrochanteric Hip Fractures
Tibial deformity correction by Ilizarov method
 International Journal of Research in Orthopaedics http://www.ijoro.org Case Report DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180422 Tibial deformity correction by Ilizarov method Robert
International Journal of Research in Orthopaedics http://www.ijoro.org Case Report DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180422 Tibial deformity correction by Ilizarov method Robert
Use of the Extended Trochanteric Osteotomy in Treating Prosthetic Hip Infection
 The Journal of Arthroplasty Vol. 24 No. 1 2009 Use of the Extended Trochanteric Osteotomy in Treating Prosthetic Hip Infection Brett R. Levine, MD, MS,* Craig J. Della Valle, MD,y Mark Hamming, BA,y Scott
The Journal of Arthroplasty Vol. 24 No. 1 2009 Use of the Extended Trochanteric Osteotomy in Treating Prosthetic Hip Infection Brett R. Levine, MD, MS,* Craig J. Della Valle, MD,y Mark Hamming, BA,y Scott
