Patellar Luxation. Our guide to dealing with a slipping kneecap. What is a luxating patella? What are the symptoms of patellar luxation?
|
|
|
- Eustace Bradford
- 5 years ago
- Views:
Transcription
1 Patellar Luxation Our guide to dealing with a slipping kneecap What is a luxating patella? The patella is the correct medical name or the kneecap and luxation is a term used to describe something that has moved out of the correct anatomical position. The patella normally sits in a groove (the trochlear groove) on the front of the femur and when the knee (or 'stifle') is moved the patella slides back and forth in this groove. The quadricep muscles on the front of the thigh attach to the patella via the patella ligament which then attaches to the top if the tibia (shin bone). The patella acts to help cushion the passage of this ligament across the front of the knee as the joint flexes and extends in normal motion. In patellar luxation, the patella is pulled out of the correct position so that it glides outside of the groove - most commonly on the inside of the knee (a 'medial ' patella luxation) but sometimes on the outside (a 'lateral' patellar luxation). It some dogs it only pops out of the groove occasionally and usually briefly (a grade 1), in others it pops out very frequently and will often stay out of position (a grade 2) and in the most severe cases the patella is never in the correct position (grade 3 and 4 depending on severity). What are the symptoms of patellar luxation?
2 The lameness caused by a luxating patella is often quite characteristic in that it tends to cause a sudden, intermittent hop which may or may not appear painful. Typically a dog may be running along quite normally and will then lift the affected leg and carry it when the patella luxates before resuming a normal gait when it pops back in. In grade 3 or 4 luxations the patella is located permanently out of the groove so a more persistent lameness is seen and the whole leg may be rotated inwards or outwards due to the pressure of the patella pushing on one side of the knee. What causes the patella to 'luxate'? The luxation is usually caused a twist in the leg at the level of the knee joint caused but either a bend in the femur or a slight deviation in the attachment of the patella ligament to the top of the tibia (the tibial 'tuberosity'). This is a developmental issue that is usually due to individual growth factors and genetics. What breeds and age of dog are affected? Usually smaller breed are affected though not exclusively - it is also fairly common in Staffordshire Bull Terriers and Springer Spaniels as well as some giant breeds. The problem usually first appears in young adults though it can appear in younger and older animals too. How is the condition treated? In grade 1 luxations, medical management is usually acceptable and this may include taking measures to reinforce joint cartilage (such as joint supplements and cartrophen injections) as well hydrotherapy and K-laser to strengthen and support the muscles and tendons around the knee. In grade 2 luxations, many dogs will cope fine for several years but over time the continual movement of the patella in and out of the correct position causes erosion of the cartilage within the knee and eventually leads to arthritis. In grade 3 and 4 luxations, the degree of lameness is usually very debilitating and surgery is needed at a fairly early point to restore normal stifle joint function and prevent long term disability. What does surgical treatment involve? There are usually three steps to correcting a luxating patella: (1) Correcting the alignment of the knee - the tibial tuberosity (or crest ) transposition (TTT) It is important that the groove in the femur (the patellofemoral groove) and the attachment of the patella ligament to the tibial tuberosity (also known as the tibial crest) are aligned in a straight line
3 so that there is no force acting to pull the patella out of position. This usually involves making a cut in the front part of the tibia to separate the tibial tuberosity from the rest of the bone and then moving it sideways to a more central position. A combination of pins and/or wires are then used to anchor it in the new position. In some large breed dogs the patella luxation may occur due to a bow in the femur above the level of the knee joint and in these cases it may be necessary to perform a corrective ostectomy to straighten the femur. This involves cutting the femur, removing a wedge of bone and then tightly securing the cut ends with a strong plate.
4 (2) The sulcoplasty - improving the groove that the patella sits in The front of the femur at the level of the knee has a cartilage-lined groove known as the trochlear groove which forms a channel for the plate to glide in as the knee is flexed and extended. In many cases of patellar luxation the trochlear groove is too shallow, either as a results of not forming properly or due to erosion and bone remodelling from the recurrent displacement of the patella from the groove. In grade 3 or 4 cases the groove may be completely absent. To deepen the groove, a saw is used to cut a wedge of cartilage and bone from the surface of the channel. This wedge is carefully preserved for use as a graft later. The underlying bone is then cut back to deepen the groove, following which the wedge is implanted back into the groove. In this way the cartilage lining the groove is preserved and ensures that the patella will glide smoothly within the newly deepened channel.
5 The cut tibial crest is gently levered to the lateral/outside of the knee (left) and the deepened groove (sulcoplasty) can be seen on the right (3) Soft tissue reconstruction The patella has strong attachments to the soft tissues on either side of the knee joint. However with patella luxation, the attachments on one side can be too tight and on the other side too loose. Therefore to help keep the patella in a central position, these attachments often need to be loosened by stretching or cutting on one side (a 'patella release) and strengthened by adding tightening stitches on the other ('imbrication'). Once surgery has been completed, x-rays are taken to ensure that the metal implants are in the correct position and ensure that the newly adjusted tibial crest, patella and patellofemoral groove are well aligned. The patient is then ready to be woken up and start on the road to recovery.
6 AFTERCARE What to expect? Your pet will almost certainly be hospitalised with us overnight following the surgery so we can give them medication, intravenous fluids and pain relief as required so be prepared to collect them the day following surgery. It is important to remember that your pet will be recovering from a major surgical procedure and the after effects of the anaesthetic can make them a bit subdued and disorientated for few days so do not worry if they seem out of sorts and are not their normal self during this period. They will almost certainly also be feeling rather sore and uncomfortable so will need to be encouraged to settle quietly in a warm, familiar spot and sleep it off. The first few days are always the hardest in this respect but once the first 4 to 5 days have passed their behaviour should slowly return to normal. A thick duvet or memory foam mattress should be provided for bedding to help cushion the area and any bedding should be thoroughly washed to reduce the risk of infection. They will need to be kept in a very clean, dry environment at all times during the first 14 days whilst the skin incision heals to minimise the risk of any infection entering the wound. They may also be a bit nauseous for a day or two so we usually recommend dividing their usual portion into several smaller meals for the first couple of days. Offering something palatable and easily digested like cooked chicken, white fish, cottage cheese or a chopped boiled egg with either rice, pasta or mashed potato is often advised - we can provide you with a tasty, high energy tinned diet for this period if requested. It is quite normal after being starved for an anaesthetic for animals not to pass any stools for a few days so this should not be concern as long as they are eating well and drinking and urinating normally. They must also not be allowed to lick the area excessively. A small t-shirt or buster collar must be used to keep the area protected if they are left alone for long periods. The surgical site will need to be checked regularly in the first few days - at least twice a day. A slight ooze of blood is normal in the first two to three days and a degree of redness, bruising and a fluidy swelling may develop over a period of 4 to 5 days. This can be quite marked around the ankle area as gravity causes the fluid to gather below the operation site and is nothing to worry about. However if the ooze of blood seems excessive or the wounds appears to be opening up then we should be contacted. Any discharge can be cleaned away with cotton wool and a saline solution made by adding two teaspoons of salt to a pint of cool, previously boiled water. Any adhesive dressings applied to the wound post operatively may come unstuck in the days following surgery and there is no need to replace them as long as the incision looks clean and dry.
7 Post-op checks These are often carried out by a veterinary nurse after 4-5 days and then again after days by a vet. We will then usually see them at 8 weeks for follow-up x-rays before a final check at 12 weeks to hopefully sign them off and give the green light to be let off the lead! The check-ups may be more frequent if concerns arise or if we administer cartrophen injections or laser therapy post-operatively (see later). REHABILITATION: ICE/COLD THERAPY (DAYS 1 to 3): To reduce swelling and discomfort we recommend applying a soft ice pack to the area for the first 3 days. A suitable ice pack can be made from a bag of peas wrapped in a clean hand towel and should be applied to the area for 10 minutes three times a day. Alternatively an ice cube can be gently moved across the skin surface around the outside of the wound. WARM COMPRESS (DAY 5-14): This can be started after the first op check and only if the incision is clean and dry. Use a hot water bottle (with cover on ie not too hot - it should be comfortable to touch) to warm the knee for 10 minutes. RANGE OF MOTION EXERCISES (DAY 5-28): These should be very gentle with no attempt to go beyond what is comfortable. Get them to lie on their good side and gently flex and extend the affected knee while supporting the leg. Being very patient and careful, perform 10 slow repetitions. Repeat this three times daily. You should only do this is if it is within your pet s comfort level. CONTROLLED EXERCISE PROGRAM: Your pet will need to be restricted to house and garden rest for the first 14 days following surgery. They should be encouraged to get up and walk around every few hours rather than lying completely still as this will help reduce stiffness and improve the circulation to the area. They should be kept on a lead when visiting the garden to avoid any sudden movements. They should also be carried up any high steps or staircases for the first 6 weeks and any sofas/chairs etc should be out of bounds during this time as well. Exercise in the form of controlled lead walking should be introduced as follows (days following surgery): 0-14: House/garden rest only (taken outside every few hours as above)
8 Expect a fair amount of swelling and very little weight-bearing on the leg in the first 7 days; over the course of the second week they should be increasingly happy to put the leg to the ground and use it when walking days (2-4 weeks): 5-10 minutes slow lead walking two to three times a day. During this period they will begin to use the leg most of the time but will be stiff and sore after resting days (4-6 weeks): minutes lead walking two to three times a day. You can also start doing some sit/stand exercises to improve the range of motion and reduce stiffness by getting them to repeatedly sit and stand for 10 repetitions twice daily. Use of a small treat can help with this! This should only be performed voluntarily - do not push down on the rump. During this period they can be expected to be increasingly confident on the leg, generally using it fairly normally and will be gradually less stiff on it days (6-8 weeks): minutes lead walking twice a day By now they will begin to think that they can go back to normal but it is still very important to keep to the exercise plan as healing of cut bone and cartilage grafts will not be complete. Follow up x-rays are normally performed at the end of this period days (8-12 weeks): Allowed off the lead but exercise should be controlled (no balls or chasing squirrels etc) and limited to a maximum of 30 minutes two to three times a day for a further 4 weeks. Gentle swimming may be permitted during this period but only if it can be carefully controlled in a proper pool with clean water and if they can be carefully led into the water avoiding any big leaps etc. After 12 weeks: They should be weight bearing fully on the leg now and can gradually go back to normal levels of exercise. Remember that every dog is different and some take longer to recover than others if there is a lot of arthritis present in the joint then recovery can take much longer and there may be a need for ongoing treatment for lameness. Likewise some dogs are very comfortable on the leg within a matter of days and may feel like using the leg normally. However always remember that with an osteotomy and sulcoplasty the cut bone and cartilage takes at least a couple of months to heal - the consequences of over exertion could be very serious indeed so stick to the exercise plan!
9 MEDICATION AND ONGOING CARE Your pet will be sent home with some anti-inflammatory medication, painkillers and antibiotics which should be given as advised - be sure to check when each medication should be given and complete the full course prescribed. We usually recommend giving a course of weekly Cartrophen injections to assist the healing process commencing with the second post-operative check-up. This has a multitude of benefits including stimulating the production and repair of cartilage, joint fluid and ligaments. It also helps reduce scar tissue and inflammation as well as limiting the development of arthritis in later years. We are now also offering post-operative K-laser therapy which can improve healing times and reduce pain following the surgery. K-laser can be used alongside the cartrophen for maximum benefit - visit for more. If arthritis is already present in the stifle joint then good quality glucosamine and chondroitin supplements as well as oils rich in Omega 3 can help manage this condition going forward. Many contain additional ingredients such as the natural anti-inflammatory (Boswelia) which can provide additional benefits ask us for advice on which products might be suitable for your pet. COMPLICATIONS With any surgery complications can and do occur - these are a rare but normal occurrence in a minority of cases (<5%) and are frustrating for all concerned. They often incur additional fees if further medication or surgery is required but we will keep you informed of these throughout. The main symptom of a complication would be if your pet was suddenly a lot more painful on the leg again and did not improve after 24 hours or so. Perhaps the most common complication in the first few weeks following surgery is something known as a 'tibial tuberosity avulsion' which occurs when the pins that secure the cut part of the tibial bone work loose - often due to excessive exercise or repeated jumping up etc. The cut section of tibia is then pulled upwards due to the force of the quadricep muscles and patella ligament acting above. Revision surgery to anchor the tibial tuberosity in the correct position again is nearly always needed. Excessive activity can also lead to loosening of the cartilage implant in the newly deepened groove that the patella sits in and this does usually require surgery if the graft becomes badly displaced. Despite every attention to sterility, surgical site infections can occur in approximately 2-3% of cases. These usually resolve with antibiotics but may require revision surgery if severe or persistent. Later down the line, it is not unusual for the body to reject the pins and/or wires securing the tibial transposition. Typically a soft swelling will appear over the front of the knee and your pet may become acutely lame on the leg. Having long since healed the implants are no longer needed at this stage and surgery to remove the implants is fairly straightforward.
10 A proportion of dogs (5-10%) may require further surgery if the patella continues to luxate i.e. slip out of position. Even with the corrective measures as described above, the pull of the quadriceps muscles on the patella is a dynamic force and further adjustments may be needed further down the line. Also be prepared for the fact that patella luxation is a condition that often affects both legs and even though one side may only cause problems initially there is a good chance (up to 50%) that the other side may need corrective surgery as well so try to prepare yourself both emotionally and financially for this eventuality! As with all major joint problems, arthritis can be expected to progress in time but this will be much less severe than would have been the case without the surgery. We will of course help you manage this should the need arise in the future. As mentioned above, these issues are recognised, normal situations that can arise with the condition and not an indication of any fault or error on behalf of the practice. As such they may incur additional costs but we will endeavour to keep you informed of these throughout.
TIBIAL PLATEAU LEVELING OSTEOTOMY (TPLO)
 TIBIAL PLATEAU LEVELING OSTEOTOMY (TPLO) Cruciate disease in the dog Cranial cruciate ligament (CCL) disease is the most common cause of hindlimb lameness in the dog. It affects the stifle joint, the equivalent
TIBIAL PLATEAU LEVELING OSTEOTOMY (TPLO) Cruciate disease in the dog Cranial cruciate ligament (CCL) disease is the most common cause of hindlimb lameness in the dog. It affects the stifle joint, the equivalent
Medial Patella Luxation
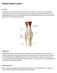 Medial Patella Luxation Anatomy The Patella is the large sesamoid bone (Kneecap) in the stifle joint. It forms part of the quadriceps muscle mechanism which is the main muscle group responsible for extension
Medial Patella Luxation Anatomy The Patella is the large sesamoid bone (Kneecap) in the stifle joint. It forms part of the quadriceps muscle mechanism which is the main muscle group responsible for extension
CRUCIATE DISEASE - LATERAL SUTURE STABILISATION (LSS)
 CRUCIATE DISEASE - LATERAL SUTURE STABILISATION (LSS) Cruciate disease in the dog Cranial cruciate ligament (CCL) disease is the most common cause of hindlimb lameness in the dog. It affects the stifle
CRUCIATE DISEASE - LATERAL SUTURE STABILISATION (LSS) Cruciate disease in the dog Cranial cruciate ligament (CCL) disease is the most common cause of hindlimb lameness in the dog. It affects the stifle
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
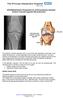 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
Patellar Ligament Disease.
 Patellar Ligament Disease. The patellar ligament disease is a condition of the stifle where the cartilage keeping the patella in place over knee joint is weakened or damaged. The patella is held in place
Patellar Ligament Disease. The patellar ligament disease is a condition of the stifle where the cartilage keeping the patella in place over knee joint is weakened or damaged. The patella is held in place
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament (ACL)
 Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Advice: After the Removal of a Lower Leg Cast
 Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Northumbria Healthcare NHS Foundation Trust. Knee Arthroscopy. Issued by the Orthopaedic Department
 Northumbria Healthcare NHS Foundation Trust Knee Arthroscopy Issued by the Orthopaedic Department Introduction This guide has been produced to provide you with information regarding your knee arthroscopy
Northumbria Healthcare NHS Foundation Trust Knee Arthroscopy Issued by the Orthopaedic Department Introduction This guide has been produced to provide you with information regarding your knee arthroscopy
Patellofemoral Joint Allison Mourad December 20, 2013
 Patellofemoral Joint Allison Mourad December 20, 2013 The patellofemoral joint is located in the hind leg of a canine and plays a key role in dynamic mobility. This joint enables the dog to sit, walk,
Patellofemoral Joint Allison Mourad December 20, 2013 The patellofemoral joint is located in the hind leg of a canine and plays a key role in dynamic mobility. This joint enables the dog to sit, walk,
ACL Reconstruction. Role of the Anterior Cruciate Ligament. Treatment of ACL tears. ACL Reconstruction
 Role of the Anterior Cruciate Ligament The ACL stabilizes the knee when jumping, pivoting, or cutting. It prevents the shinbone (tibia) from sliding forward on the thigh bone (femur). ACL tears often occur
Role of the Anterior Cruciate Ligament The ACL stabilizes the knee when jumping, pivoting, or cutting. It prevents the shinbone (tibia) from sliding forward on the thigh bone (femur). ACL tears often occur
Patellar Instability. OrthoInfo Patella Instability Page 1 of 5
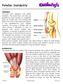 Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY
 A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
Arthroscopy Day Case. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Arthroscopy Day Case An information guide Arthroscopy Day Case Arthroscopy Day case Post-operative regime The post-operative rehabilitation
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Arthroscopy Day Case An information guide Arthroscopy Day Case Arthroscopy Day case Post-operative regime The post-operative rehabilitation
Advice and exercises for managing knee and hip osteoarthritis October 2018 V1.2 April 2018 April 2021
 Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella)
 Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella) Patellar Tendinitis The most common tendinitis about the knee is irritation of the patellar tendon.
Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella) Patellar Tendinitis The most common tendinitis about the knee is irritation of the patellar tendon.
How do you do exercises for patellar tracking disorder?
 To print: Use your web browser's print feature. Close this window after printing. Patellar Tracking Disorder: Exercises Table of Contents Patellar Tracking Disorder: Exercises Patellar Tracking Disorder:
To print: Use your web browser's print feature. Close this window after printing. Patellar Tracking Disorder: Exercises Table of Contents Patellar Tracking Disorder: Exercises Patellar Tracking Disorder:
Arthroscopy of the Knee
 Arthroscopy of the Knee The information contained within this leaflet is only a guide and the timings and activities will depend upon your specific circumstances and Mr Hartley s individual instructions.
Arthroscopy of the Knee The information contained within this leaflet is only a guide and the timings and activities will depend upon your specific circumstances and Mr Hartley s individual instructions.
Cruciate ligament injury
 Cruciate ligament injury This is an extremely common injury in dogs, less so in cats. Let s start by looking at the anatomy of the stifle (knee) joint of the dog. The important differences between the
Cruciate ligament injury This is an extremely common injury in dogs, less so in cats. Let s start by looking at the anatomy of the stifle (knee) joint of the dog. The important differences between the
High Tibial Osteotomy (HTO) Rehabilitation Protocols
 High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET
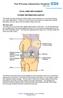 TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Knee arthroscopy. Physiotherapy Department. Patient information leaflet
 Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Advice for patients following a Rotator Cuff Repair
 Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Advice for patients following a Rotator Cuff Repair Patient Advice and Liaison Service (PALS): 0151 430 1376 St Helens Hospital Marshall
Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Advice for patients following a Rotator Cuff Repair Patient Advice and Liaison Service (PALS): 0151 430 1376 St Helens Hospital Marshall
Patellofemoral Pain Syndrome
 What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
The best way to deal with back pain
 The best way to deal with back pain The best way to deal with back pain Back pain is common and can be very painful but, serious or permanent damage is rare. The Facts Most back pain is not due to any
The best way to deal with back pain The best way to deal with back pain Back pain is common and can be very painful but, serious or permanent damage is rare. The Facts Most back pain is not due to any
Patellar Luxation. The Patella. Dr. PJ Rocheleau, DVM and Associates 138 Tudhope St, Espanola ON, P5E 1S6
 Patellar Luxation The Patella The patella (equivalent to the knee cap ) is one of several structures in the stifle (equivalent to our knee) that provide joint stability and allow normal function. The stifle
Patellar Luxation The Patella The patella (equivalent to the knee cap ) is one of several structures in the stifle (equivalent to our knee) that provide joint stability and allow normal function. The stifle
Anterior Cruciate Ligament (ACL) Reconstruction. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Anterior Cruciate Ligament (ACL) Reconstruction An information guide Anterior Cruciate Ligament (ACL) Reconstruction Post-operative regime
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Anterior Cruciate Ligament (ACL) Reconstruction An information guide Anterior Cruciate Ligament (ACL) Reconstruction Post-operative regime
Knee Arthroscopy: Postoperative Instructions
 Knee Arthroscopy: Postoperative Instructions John P. Woll, MD Knee arthroscopy is a commonly performed procedure that is much less invasive than previous open techniques, but it is still an operation,
Knee Arthroscopy: Postoperative Instructions John P. Woll, MD Knee arthroscopy is a commonly performed procedure that is much less invasive than previous open techniques, but it is still an operation,
Anterior Cruciate Ligament Reconstruction
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Anterior Cruciate Ligament Reconstruction Patient Information
 Anterior Cruciate Ligament Reconstruction Patient Information This information sheet is designed to help you to understand what an Anterior Cruciate Ligament (ACL) Reconstruction involves. I perform ACL
Anterior Cruciate Ligament Reconstruction Patient Information This information sheet is designed to help you to understand what an Anterior Cruciate Ligament (ACL) Reconstruction involves. I perform ACL
Lateral Collateral Ligament Sprain
 What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
Anterior Cruciate Ligament (ACL) Reconstruction
 Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
Advice for patients following a Slap Repair
 Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Patient Advice and Liaison Service (PALS): 0151 430 1376 Advice for patients following a Slap Repair St Helens Hospital Marshall Cross
Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Patient Advice and Liaison Service (PALS): 0151 430 1376 Advice for patients following a Slap Repair St Helens Hospital Marshall Cross
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Cheilectomy. Your guide to a successful outcome following surgery. Orthopaedic Department. Royal Surrey County Hospital. Patient information leaflet
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Cheilectomy Your guide to a successful outcome following surgery Orthopaedic Department What is Cheilectomy? This is surgery
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Cheilectomy Your guide to a successful outcome following surgery Orthopaedic Department What is Cheilectomy? This is surgery
ACL Reconstruction Physiotherapy advice for patients
 ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction of your anterior cruciate
ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction of your anterior cruciate
How is 1st MTP joint fusion carried out? Patient Information: Big Toe Fusion Metatarsophalangeal (MTP)
 Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
Patella Instability in Children and Adolescents
 Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
This advice and exercises have been selected to help you manage the symptoms of your arthritis
 This advice and exercises have been selected to help you manage the symptoms of your arthritis 1. GENERAL ADVICE Movement is good for your arthritic knee it helps to keep the tissue healthy, increases
This advice and exercises have been selected to help you manage the symptoms of your arthritis 1. GENERAL ADVICE Movement is good for your arthritic knee it helps to keep the tissue healthy, increases
Achilles Tendonitis and Tears
 Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Going home after major gynaecological surgery. Information for patients Gynaecology
 Going home after major gynaecological surgery Information for patients Gynaecology Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice about what
Going home after major gynaecological surgery Information for patients Gynaecology Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice about what
TIBIAL PLATEAU FRACTURE
 TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
Physiotherapy Services. Physiotherapy Guide. Hip Replacement
 Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
BIG TOE FUSION. Patient Information
 Patient Information BIG TOE FUSION This may have been caused by an old injury, previous surgery or a long-standing bunion deformity. Pain at the joint can start to affect your daily activities and even
Patient Information BIG TOE FUSION This may have been caused by an old injury, previous surgery or a long-standing bunion deformity. Pain at the joint can start to affect your daily activities and even
Arthroscopic capsular release. Information for patients Orthopaedics - Upper Limb
 Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
Your Arthroscopic Capsular Release (Arthrolysis) Information for Patients
 Your Arthroscopic Capsular Release (Arthrolysis) Information for Patients This leaflet will provide you with general information about capsular release surgery. It will briefly explain the operation procedure
Your Arthroscopic Capsular Release (Arthrolysis) Information for Patients This leaflet will provide you with general information about capsular release surgery. It will briefly explain the operation procedure
Knee Replacement PROGRAM. Nightingale. Home Healthcare
 Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
DISCOID MENISCUS. Description
 DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
Acute Lower Back Pain. Physiotherapy department
 Acute Lower Back Pain Physiotherapy department Back pain is a common condition and in the UK it affects 7 out of 10 people at some point in their lives. Back pain can be very uncomfortable but it is not
Acute Lower Back Pain Physiotherapy department Back pain is a common condition and in the UK it affects 7 out of 10 people at some point in their lives. Back pain can be very uncomfortable but it is not
A Guide to Common Ankle Injuries
 A Guide to Common Ankle Injuries Learn About: Common ankle injuries Feet and Ankle Diagnosis and Treatment Ankle exercises Beginning your recovery Frequently asked questions Do s and Don t s Arthroscopy
A Guide to Common Ankle Injuries Learn About: Common ankle injuries Feet and Ankle Diagnosis and Treatment Ankle exercises Beginning your recovery Frequently asked questions Do s and Don t s Arthroscopy
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron
 Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron Orthopaedic Department Patient information leaflet This patient information booklet is designed to provide you with information
Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron Orthopaedic Department Patient information leaflet This patient information booklet is designed to provide you with information
Ankle Arthroscopy PATIENT INFORMATION. What is an ankle arthroscopy? Common disorders in which ankle arthroscopy is useful.
 PATIENT INFORMATION Ankle Arthroscopy What is an ankle arthroscopy? Ankle arthroscopy is also known as keyhole surgery or minimally invasive ankle surgery. Ankle arthroscopy involves using very small incisions
PATIENT INFORMATION Ankle Arthroscopy What is an ankle arthroscopy? Ankle arthroscopy is also known as keyhole surgery or minimally invasive ankle surgery. Ankle arthroscopy involves using very small incisions
Reversed geometry shoulder replacement
 Information and exercises Reversed geometry shoulder replacement Introduction The reversed geometry total shoulder replacement is designed for use in shoulders that have a deficient rotator cuff, arthritis
Information and exercises Reversed geometry shoulder replacement Introduction The reversed geometry total shoulder replacement is designed for use in shoulders that have a deficient rotator cuff, arthritis
Knee Replacement Patient Information
 Knee Replacement Patient Information This information sheet is designed to help you to understand what a knee replacement involves. I perform knee replacements frequently, several times each week, and
Knee Replacement Patient Information This information sheet is designed to help you to understand what a knee replacement involves. I perform knee replacements frequently, several times each week, and
What to expect after Dupuytren's surgery and what to do to get the best possible results.
 What to expect after Dupuytren's surgery and what to do to get the best possible results. Directly after surgery: You can expect a bulky bandage covering the palm and the fingers that were operated on.
What to expect after Dupuytren's surgery and what to do to get the best possible results. Directly after surgery: You can expect a bulky bandage covering the palm and the fingers that were operated on.
Mosaicplasty and OATS Rehabilitation Protocol
 Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
It is most common in people between the age of 40 and 70 years and has been estimated to affect at least one person in 50 every year.
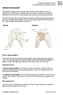 FROZEN SHOULDER The shoulder is designed to have a large amount of movement so that we can use our hands/arms in a wide variety of positions. Some movement occurs between the shoulder blade and chest wall.
FROZEN SHOULDER The shoulder is designed to have a large amount of movement so that we can use our hands/arms in a wide variety of positions. Some movement occurs between the shoulder blade and chest wall.
Patient Education GANZ PERIACETABULAR OSTEOTOMY
 GANZ PERIACETABULAR OSTEOTOMY Thank you for the opportunity of allowing us to take care of you. We understand that there are many questions regarding your hip surgery for you and your parents. This information
GANZ PERIACETABULAR OSTEOTOMY Thank you for the opportunity of allowing us to take care of you. We understand that there are many questions regarding your hip surgery for you and your parents. This information
Returning to fitness after birth
 Returning to fitness after birth This leaflet is designed for all women, whether you have given birth vaginally or by Caesarean section. During pregnancy your body undergoes many changes to adapt to your
Returning to fitness after birth This leaflet is designed for all women, whether you have given birth vaginally or by Caesarean section. During pregnancy your body undergoes many changes to adapt to your
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (Immediate) Post-Op Home Exercise Program
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (Immediate) Post-Op Home Exercise Program The knee brace must be worn locked in extension (straight) while walking and sleeping. You may take the brace off when
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (Immediate) Post-Op Home Exercise Program The knee brace must be worn locked in extension (straight) while walking and sleeping. You may take the brace off when
Cranial Cruciate Ligament Disease
 24- hour Emergency Service 01635 47170 The Tibial Tuberosity Advancement (TTA) procedure is one of the advanced procedures for the treatment of cranial cruciate ligament disease in dogs. TTA is now available
24- hour Emergency Service 01635 47170 The Tibial Tuberosity Advancement (TTA) procedure is one of the advanced procedures for the treatment of cranial cruciate ligament disease in dogs. TTA is now available
PATELLA INSTABILITY AND REALIGNMENT
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS
 OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long 614-566-8691 Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS Shoulder Arthroscopy with Labral Repair (SLAP/Bankart/Posterior) Latarjet Procedure
OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long 614-566-8691 Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS Shoulder Arthroscopy with Labral Repair (SLAP/Bankart/Posterior) Latarjet Procedure
PLICA SYNDROME. Contents What is Plica Syndrome?... 3
 Contents What is Plica Syndrome?........................................................... 3 What are Plicae?..................................................................... 3 YOUR GUIDE TO PLICA
Contents What is Plica Syndrome?........................................................... 3 What are Plicae?..................................................................... 3 YOUR GUIDE TO PLICA
SIMITRI STABLE IN STRIDE POST-OPERATIVE CARE
 Copyright 2016 NGD. All rights reserved Neil Embleton, B.Sc., DVM and Veronica Barkowski, DVM Helivet Mobile Surgical Services, Sundre, AB, Canada July 2016 SIMITRI STABLE IN STRIDE POST-OPERATIVE CARE
Copyright 2016 NGD. All rights reserved Neil Embleton, B.Sc., DVM and Veronica Barkowski, DVM Helivet Mobile Surgical Services, Sundre, AB, Canada July 2016 SIMITRI STABLE IN STRIDE POST-OPERATIVE CARE
Hip Pain. Anatomy of the hip
 Hip Pain Anatomy of the hip The hip is a ball and socket joint, the ball is on the head of femur (the top of the thigh bone) and the socket (acetabulum) is a part of the pelvis. It s surrounded by tendons
Hip Pain Anatomy of the hip The hip is a ball and socket joint, the ball is on the head of femur (the top of the thigh bone) and the socket (acetabulum) is a part of the pelvis. It s surrounded by tendons
Rehabilitation programme after hemiarthroplasty surgery
 Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Key words: Laser, sprain, strain, lameness, tendon
 MLS Master Class - Veterinary Imaging Presented by CelticSMR Ltd Free Phone (UK): 0800 279 9050 International: +44 (0) 1646 603150 AUTHOR DETAILS Carl Gorman BVSc MRCVS PUBLISHER DETAILS Mike Howe B Vet
MLS Master Class - Veterinary Imaging Presented by CelticSMR Ltd Free Phone (UK): 0800 279 9050 International: +44 (0) 1646 603150 AUTHOR DETAILS Carl Gorman BVSc MRCVS PUBLISHER DETAILS Mike Howe B Vet
(Also known as a, Lateral Cartilage Tear,, Bucket Handle Tear of the Lateral Meniscus, Torn Cartilage)
 Lateral Meniscus Tear (Also known as a, Lateral Cartilage Tear,, Bucket Handle Tear of the Lateral Meniscus, Torn Cartilage) What is a lateral meniscus tear? The knee joint comprises of the union of two
Lateral Meniscus Tear (Also known as a, Lateral Cartilage Tear,, Bucket Handle Tear of the Lateral Meniscus, Torn Cartilage) What is a lateral meniscus tear? The knee joint comprises of the union of two
POST-SURGERY INSTRUCTIONS: LIPOSUCTION
 POST-SURGERY INSTRUCTIONS: LIPOSUCTION Once your surgery is completed, you must follow all the instructions given to you in order to heal properly and have a good outcome. The following instructions are
POST-SURGERY INSTRUCTIONS: LIPOSUCTION Once your surgery is completed, you must follow all the instructions given to you in order to heal properly and have a good outcome. The following instructions are
DISCOID MENISCUS. Description
 Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
DRAFT. The best way to deal with back pain
 Services provided by Essex Parntership University NHS Foundation Trust and West Essex NHS Clinical Commissioning Group niversity The best way to deal with back pain The best way to deal with back pain
Services provided by Essex Parntership University NHS Foundation Trust and West Essex NHS Clinical Commissioning Group niversity The best way to deal with back pain The best way to deal with back pain
PATIENT INFORMATION Cartiva implant surgery
 PATIENT INFORMATION Cartiva implant surgery Introduction This leaflet will explain what will happen when you come to the hospital for an operation to have a Cartiva implant inserted into your toe joint.
PATIENT INFORMATION Cartiva implant surgery Introduction This leaflet will explain what will happen when you come to the hospital for an operation to have a Cartiva implant inserted into your toe joint.
Inner side of knee. Outer side of knee. PCL - Posterior cruciate ligament. Femur Articular cartilage. ACL - Anterior cruciate ligament
 ACL surgery Outer side of knee Inner side of knee PCL - Posterior cruciate ligament Femur Articular cartilage LCL - Lateral collateral ligament Lateral meniscus Tibia ACL - Anterior cruciate ligament MCL
ACL surgery Outer side of knee Inner side of knee PCL - Posterior cruciate ligament Femur Articular cartilage LCL - Lateral collateral ligament Lateral meniscus Tibia ACL - Anterior cruciate ligament MCL
Information for Patients having Total Knee Replacement Surgery
 Information for Patients having Total Knee Replacement Surgery Hello You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written this booklet to give you information
Information for Patients having Total Knee Replacement Surgery Hello You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written this booklet to give you information
Lumbar Decompression GUIDELINES FOR PATIENTS HAVING A. Lumbar Decompression
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
Guidelines for patients having. Achilles Tendon Repair. Achilles Tendon Repair
 Guidelines for patients having ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Achilles Tendon Repair Please stick addressograph
Guidelines for patients having ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Achilles Tendon Repair Please stick addressograph
This booklet has been developed to help guide you through your post-operative rehabilitation.
 Patient Information Physiotherapy following Breast Surgery Physiotherapy Directorate Keep this booklet as a reminder with your exercises long term. If you start to develop stiffness, pain, weakness, or
Patient Information Physiotherapy following Breast Surgery Physiotherapy Directorate Keep this booklet as a reminder with your exercises long term. If you start to develop stiffness, pain, weakness, or
Knee Pain Solutions. Assess Your Pain. Make a Plan. Take Action
 Knee Pain Solutions Assess Your Pain Make a Plan Take Action By Jared Evans Certified Strength and Conditioning Specialist Giammalva Fitness Director There are many different causes of knee pain and understanding
Knee Pain Solutions Assess Your Pain Make a Plan Take Action By Jared Evans Certified Strength and Conditioning Specialist Giammalva Fitness Director There are many different causes of knee pain and understanding
Surgery to reconstruct the anterior cruciate ligament of the knee (ACL reconstruction)
 Surgery to reconstruct the anterior cruciate ligament of the knee (ACL reconstruction) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery
Surgery to reconstruct the anterior cruciate ligament of the knee (ACL reconstruction) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery
SHOULDER ACROMIOPLASTY
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A SHOULDER ACROMIOPLASTY Please stick addressograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A SHOULDER ACROMIOPLASTY Please stick addressograph
Information Following Ankle Injury
 Patient & Family Guide Information Following Ankle Injury 2016 www.nshealth.ca Information Following Ankle Injury Physiotherapy Department Date Physiotherapist What to expect after cast/bandage removal:
Patient & Family Guide Information Following Ankle Injury 2016 www.nshealth.ca Information Following Ankle Injury Physiotherapy Department Date Physiotherapist What to expect after cast/bandage removal:
A Patient information guide to. Bunion Correction. Foot and Ankle Unit. Mr Amit Amin Mr Ali Abbasian BUNION CORRECTION (SCARF/AKIN) JAN
 A Patient information guide to Bunion Correction Foot and Ankle Unit Mr Amit Amin Mr Ali Abbasian BUNION CORRECTION (SCARF/AKIN) JAN 2016 1 What does surgery involve? Surgery to correct a bunion is not
A Patient information guide to Bunion Correction Foot and Ankle Unit Mr Amit Amin Mr Ali Abbasian BUNION CORRECTION (SCARF/AKIN) JAN 2016 1 What does surgery involve? Surgery to correct a bunion is not
KUCHING SPECIALIST HOSPITAL - Arthritis and Sports Injury Centre -
 KUCHING SPECIALIST HOSPITAL - Arthritis and Sports Injury Centre - ARTHROSCOPY FOR TORN MENISCI You have had problems with your knee and your orthopaedic surgeon suspects that you may have a torn meniscus,
KUCHING SPECIALIST HOSPITAL - Arthritis and Sports Injury Centre - ARTHROSCOPY FOR TORN MENISCI You have had problems with your knee and your orthopaedic surgeon suspects that you may have a torn meniscus,
Exercises following Copeland Surface Replacement Arthroplasty (CSRA)
 Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
A Patient s Guide to Patellofemoral Problems
 A Patient s Guide to Patellofemoral Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Patellofemoral Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
Discharge Information following Bowel Surgery
 Discharge Information following Bowel Surgery Here is some information to help with your recovery at home and advice about returning to normal activities following bowel surgery. We hope this will be helpful
Discharge Information following Bowel Surgery Here is some information to help with your recovery at home and advice about returning to normal activities following bowel surgery. We hope this will be helpful
